Cultivation of Keratinocytes and Fibroblasts in a Three-Dimensional Bovine Collagen-Elastin Matrix (Matriderm®) and Application for Full Thickness Wound Coverage in Vivo
Abstract
:1. Introduction
1.1. Clinical Background
1.2. Skin Substitutes as an Alternative for Skin Transplants
2. Results and Discussion
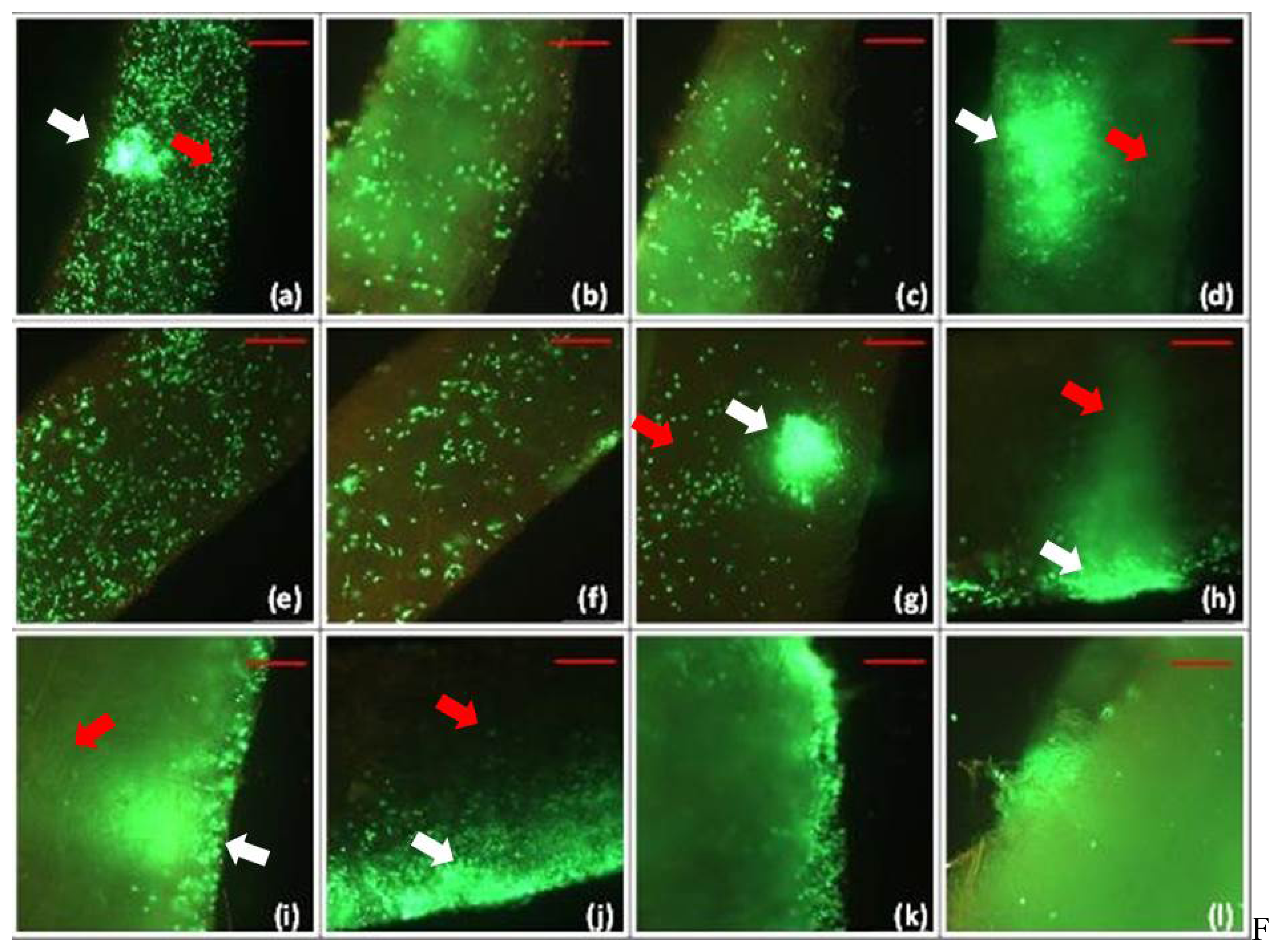
2.1. Viability of Keratinocytes and Fibroblasts Transplanted into Matriderm®
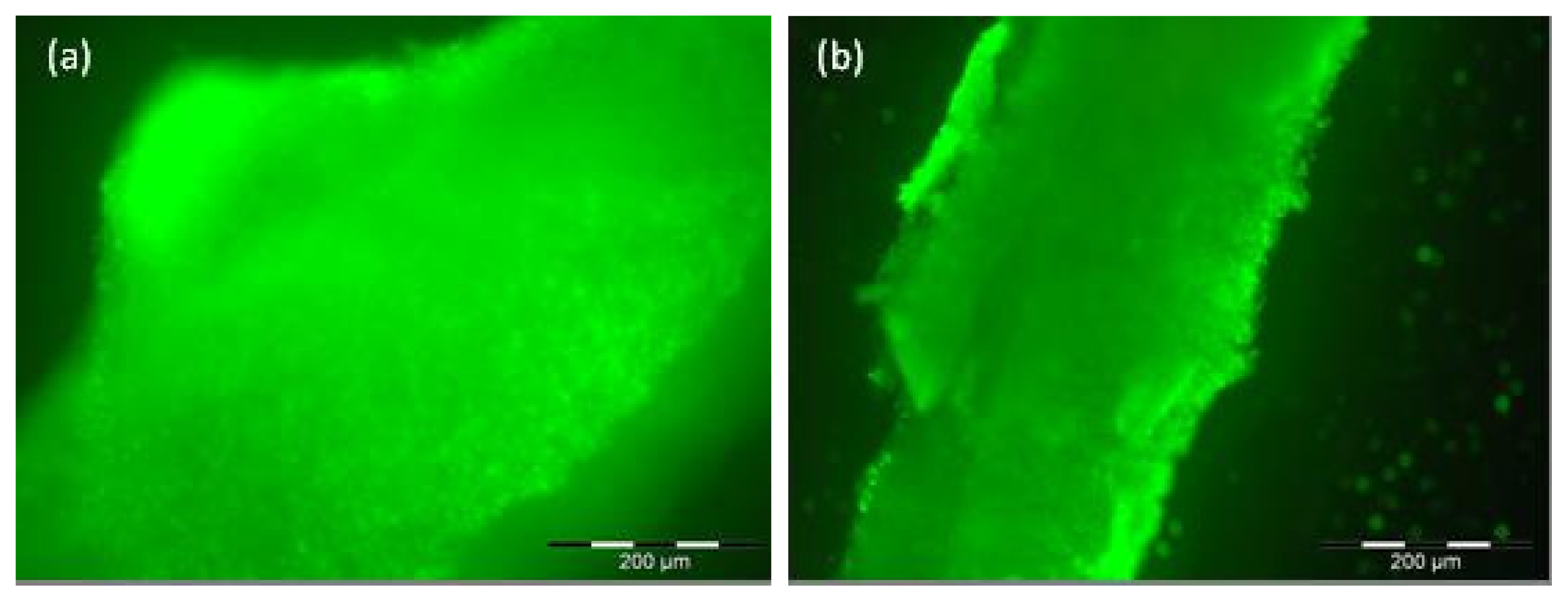
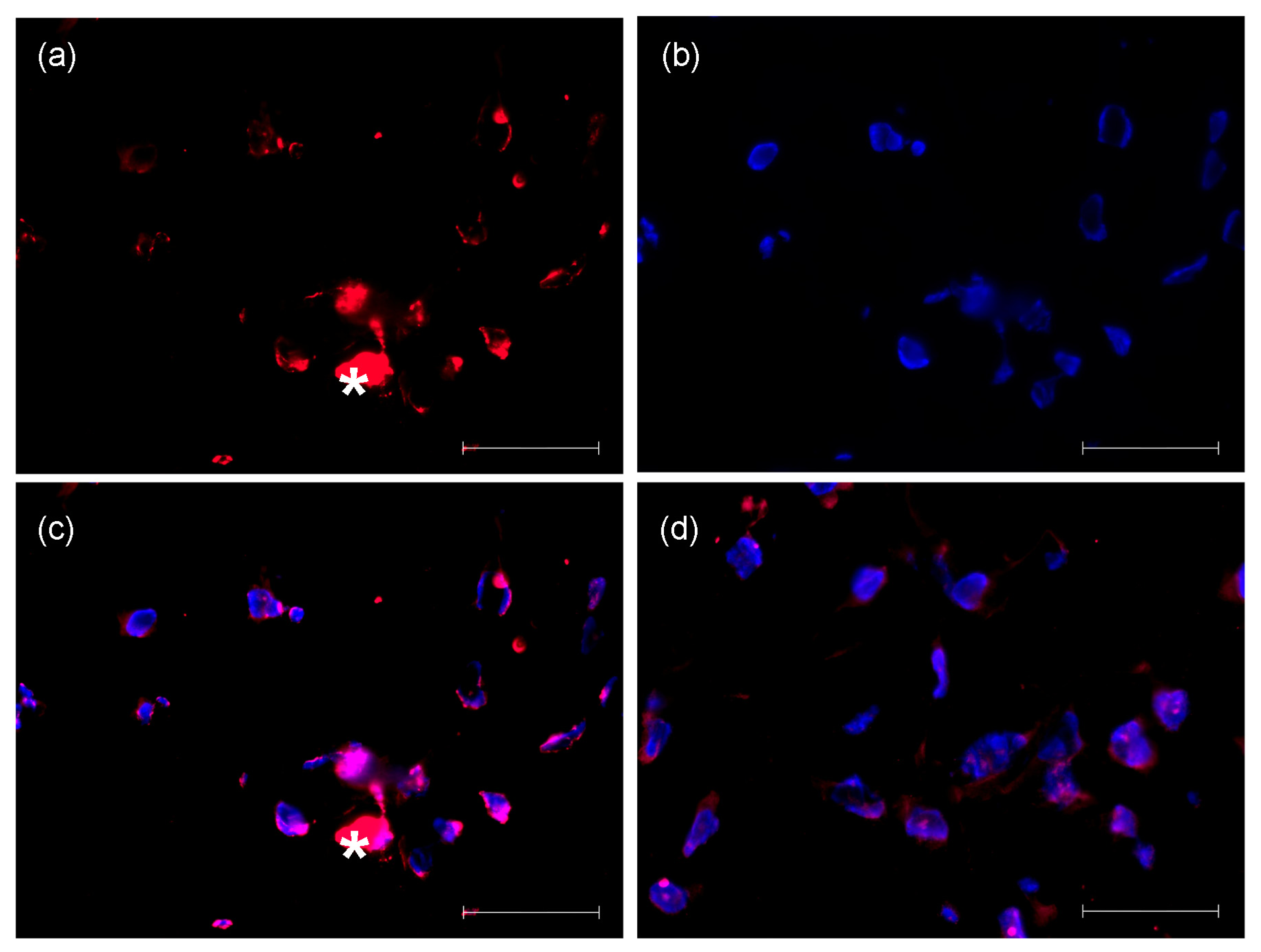
2.2. Proliferation
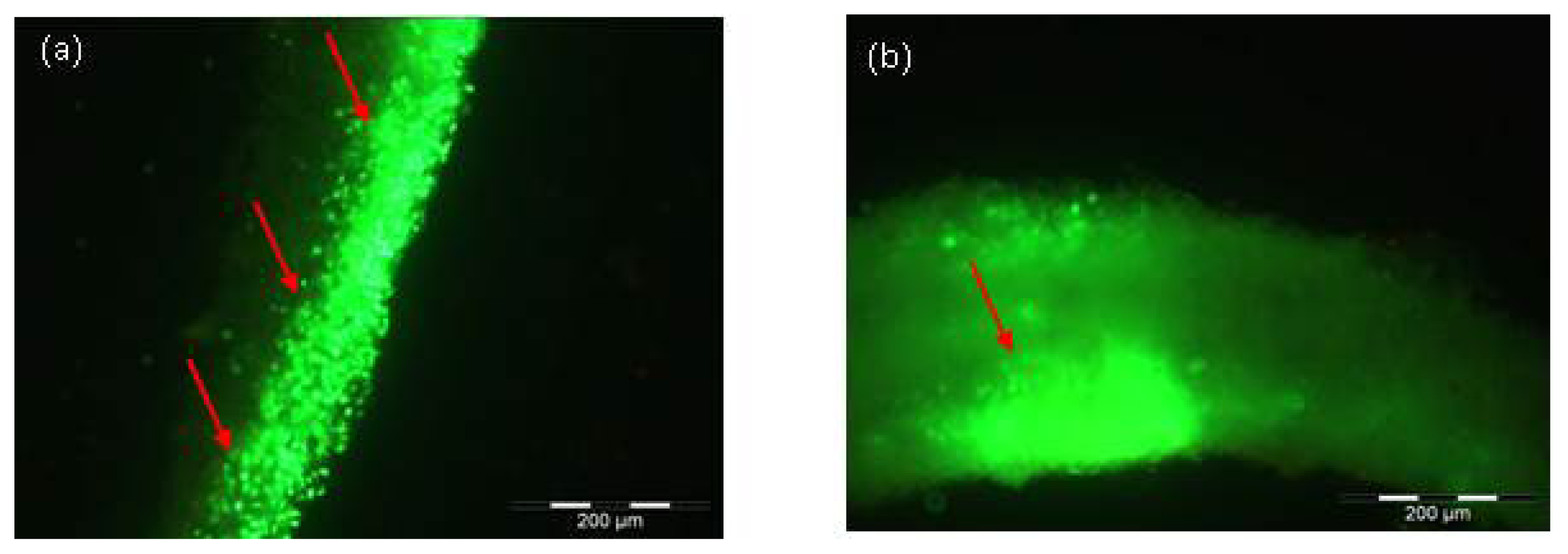
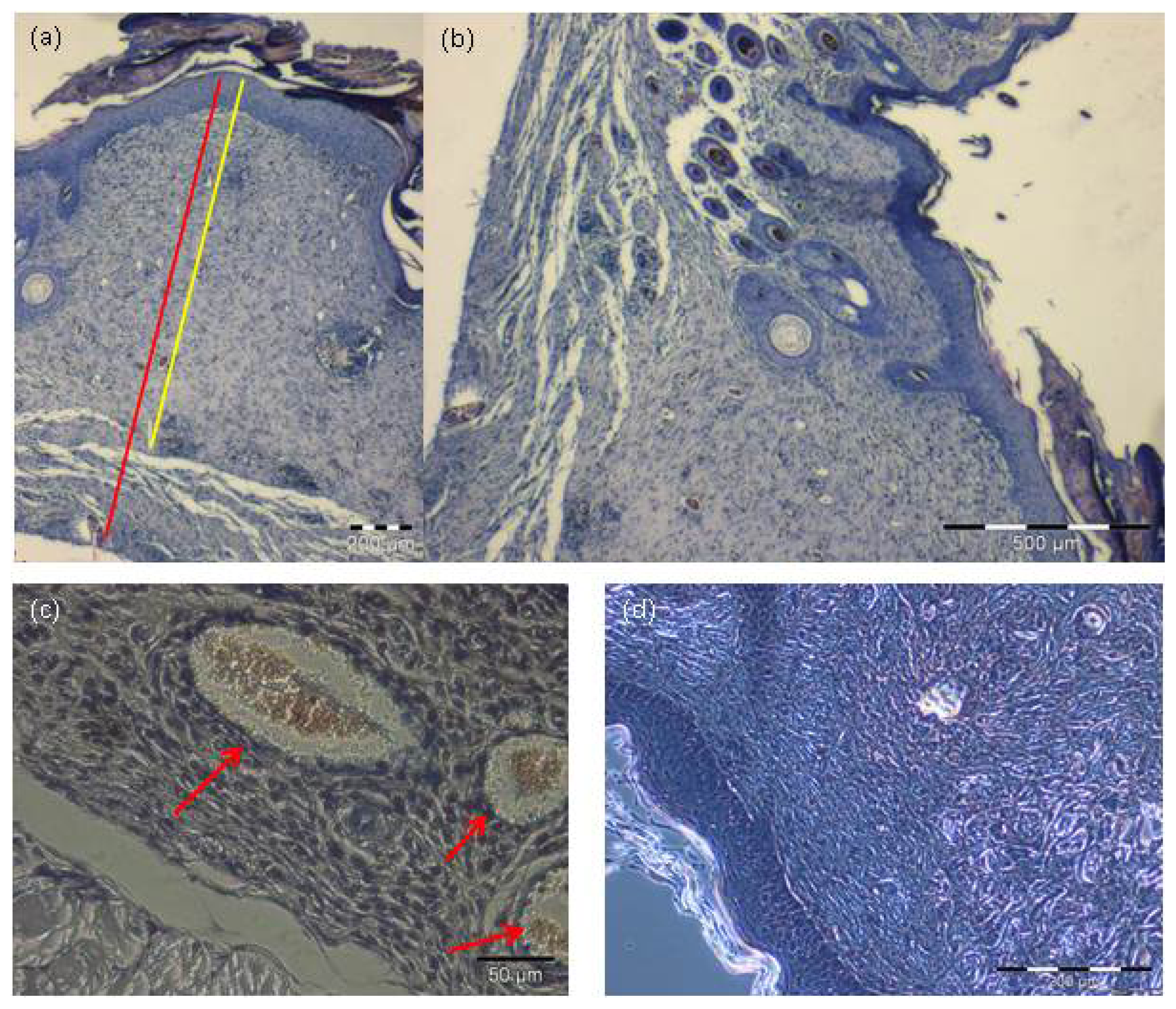
2.3. Integration of the Skin Substitute in Vivo
3. Experimental Section
3.1. Matriderm®
3.2. Cell Culture
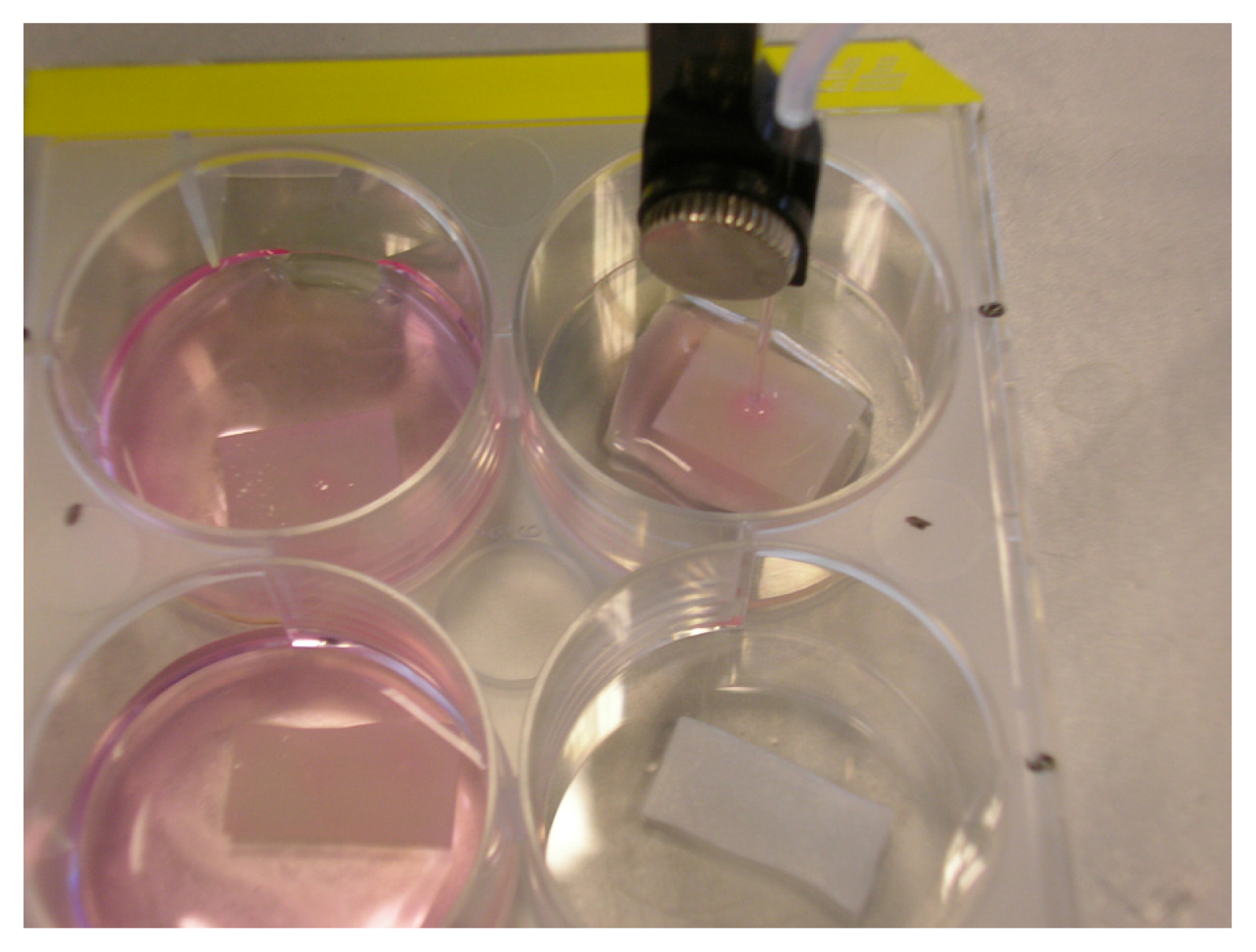
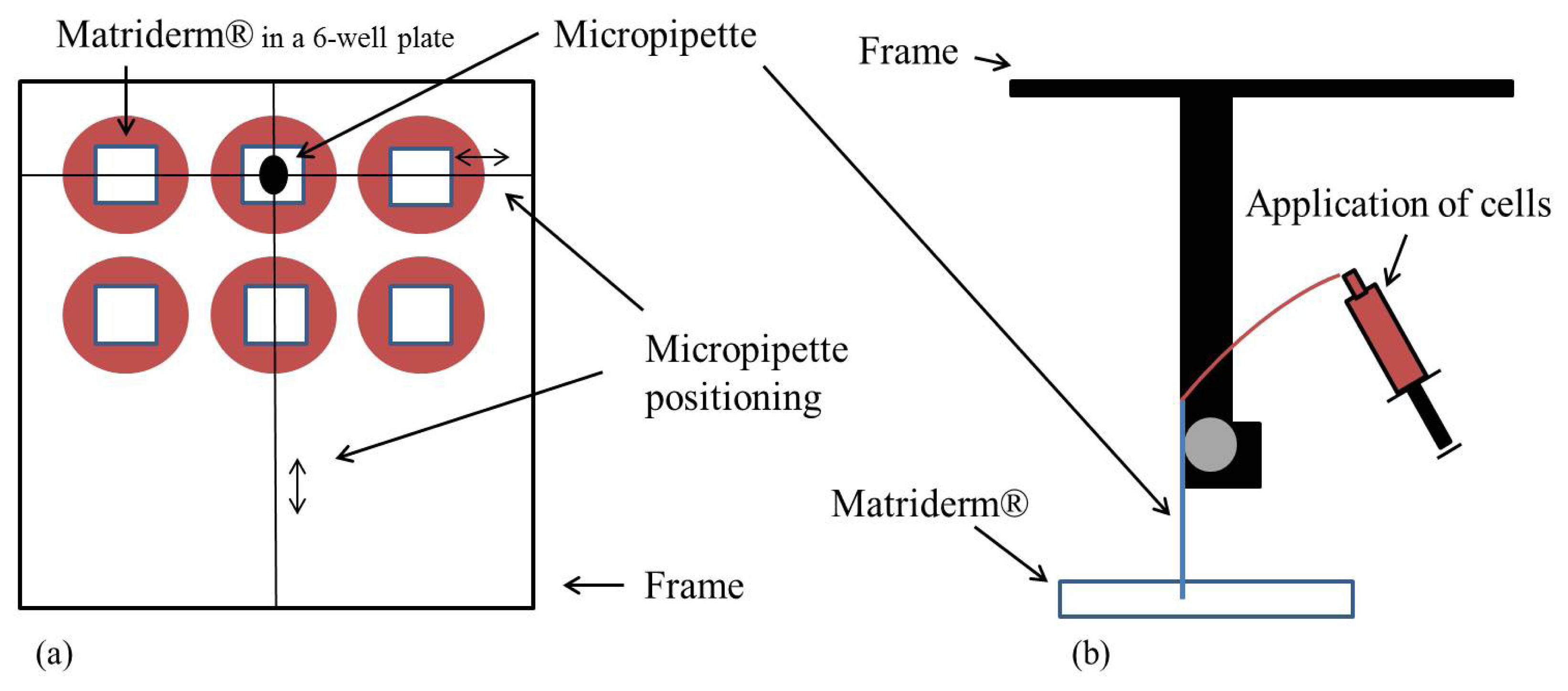
3.3. Injection in Matriderm®
3.4. LIVE/DEAD Assay
3.5. Immunofluorescence
3.6. Insertion of the Skin Substitute in Mice
3.7. Histological Analysis
3.8. Animal and Ethics Statement
4. Conclusions
Acknowledgments
Conflict of Interest
References
- Spies, M.; Vogt, P.M. Verbrennungen (in German). In Chirurgie, 3nd ed.; Henne-Bruhns, D., Ed.; Thieme: Stuttgart, Germany, 2008; pp. 912–915. [Google Scholar]
- Aust, M.; Reimers, K.; Sorg, H. Biologische Grundlagen der Wundheilung (in German). In Praxis der Plastischen Chirurgie, 1st ed; Vogt, P.M., Ed.; Springer Medizin: Heidelberg, Germany, 2011; pp. 4–8. [Google Scholar]
- Alexander, J.W.; MacMillan, B.G.; Law, E.; Kittur, D.S. Treatment of severe burns with widely meshed skin autograft and meshed skin allograft overlay. J. Trauma 1981, 21, 433–438. [Google Scholar]
- Kolokythas, P.; Aust, M.C. Verbrennungsverletzungen (in German). In Praxis Der Plastischen Chirurgie, 1st ed; Vogt, P.M., Ed.; Springer Medizin: Berlin/Heidelberg, Germany, 2011; pp. 662–664. [Google Scholar]
- Fletcher, J.L.; Caterson, E.J.; Hale, R.G.; Cancio, L.C.; Renz, E.M.; Chan, R.K. Characterization of skin allograft use in thermal injury. J. Burn Care Res 2013, 34, 168–175. [Google Scholar]
- Kremer, M.; Berger, A. Perspektiven des kunstlichen Hautersatzes: Vom biologischen verband zur künstlichen haut (in German). Deutsches Ärzteblatt-Ärztliche Mitteilungen-Ausgabe A 2000, 97, 1222–1227. [Google Scholar]
- Vogt, P.M.; Kolokythas, P.; Niederbichler, A.; Knobloch, K.; Reimers, K.; Choi, C.Y. Innovative wundtherapie und hautersatz bei verbrennungen (in German). Chirurg 2007, 335–342. [Google Scholar]
- Felder, J.M., III; Goyal, S.S.; Attinger, C.E. A systematic review of skin substitutes for foot ulcers. Plast. Reconstr. Surg. 2012, 130, 145–164. [Google Scholar]
- Cronin, H.; Goldstein, G. Biologic skin substitutes and their applications in dermatology. Dermatol. Surg 2013, 39, 30–34. [Google Scholar]
- Shores, J.T.; Hiersche, M.; Gabriel, A.; Gupta, S. Tendon coverage using an artificial skin substitute. J. Plast. Reconstr. Aesthet. Surg 2012, 65, 1544–1550. [Google Scholar]
- Schneider, J.; Biedermann, T.; Widmer, D.; Montano, I.; Meuli, M.; Reichmann, E.; Schiestl, C. Matriderm® versus Integra®: A comparative experimental study. Burns 2009, 35, 51–57. [Google Scholar]
- Guthrie, K.M.; Agarwal, A.; Tackes, D.S.; Johnson, K.W.; Abbott, N.L.; Murphy, C.J.; Czuprynski, C.J.; Kierski, P.R.; Schurr, M.J.; McAnulty, J.F. Antibacterial efficacy of silver-impregnated polyelectrolyte multilayers immobilized on a biological dressing in a murine wound infection model. Ann. Surg 2012, 256, 371–377. [Google Scholar]
- Frew, Q.; Philp, B.; Shelley, O.; Myers, S.; Navsaria, H.; Dziewulski, P. The use of Biobrane®as a delivery method for cultured epithelial autograft in burn patients. Burns 2013, in press. [Google Scholar]
- Wendt, H.; Hillmer, A.; Reimers, K.; Kuhbier, J.W.; Schafer-Nolte, F.; Allmeling, C.; Kasper, C.; Vogt, P.M. Artificial skin—Culturing of different skin cell lines for generating an artificial skin substitute on cross-weaved spider silk fibres. PLoS One 2011, 6, e21833. [Google Scholar]
- Jin, G.; Prabhakaran, M.P.; Kai, D.; Annamalai, S.K.; Arunachalam, K.D.; Ramakrishna, S. Tissue engineered plant extracts as nanofibrous wound dressing. Biomaterials 2013, 34, 724–734. [Google Scholar]
- Falanga, V.; Iwamoto, S.; Chartier, M.; Yufit, T.; Butmarc, J.; Kouttab, N.; Shrayer, D.; Carson, P. Autologous bone marrow-derived cultured mesenchymal stem cells delivered in a fibrin spray accelerate healing in murine and human cutaneous wounds. Tissue Eng 2007, 13, 1299–1312. [Google Scholar]
- Akela, A.; Nandi, S.K.; Banerjee, D.; Das, P.; Roy, S.; Joardar, S.N.; Mandal, M.; Das, P.K.; Pradhan, N.R. Evaluation of autologous bone marrow in wound healing in animal model: A possible application of autologous stem cells. Int. Wound J 2012, 9, 505–516. [Google Scholar]
- Saha, P.; Chen, J.; Thome, K.C.; Lawlis, S.J.; Hou, Z.H.; Hendricks, M.; Parvin, J.D.; Dutta, A. Human CDC6/Cdc18 associates with Orc1 and Cyclin-cdk and is selectively eliminated from the nucleus at the onset of S phase. Mol. Cell. Biol 1998, 18, 2758–2767. [Google Scholar]
- Golinski, P.A.; Zoller, N.; Kippenberger, S.; Menke, H.; Bereiter-Hahn, J.; Bernd, A. Development of an engraftable skin equivalent based on matriderm with human keratinocytes and fibroblasts. Handchir. Mikrochir. Plast. Chir 2009, 41, 327–332. [Google Scholar]
- Reichenberger, M.A.; Mueller, W.; Schafer, A.; Heimer, S.; Leimer, U.; Lass, U.; Germann, G.; Kollensperger, E. Fibrin-embedded adipose derived stem cells enhance skin flap survival. Stem Cell. Rev 2012, 8, 844–853. [Google Scholar]
- Leng, X.; Zhang, Q.; Zhai, X.; Chen, Z. Local transplant of human umbilical cord matrix stem cells improves skin flap survival in a mouse model. Tohoku J. Exp. Med 2012, 227, 191–197. [Google Scholar]
- Salem, H.; Ciba, P.; Rapoport, D.H.; Egana, J.T.; Reithmayer, K.; Kadry, M.; Machens, H.G.; Kruse, C. The influence of pancreas-derived stem cells on scaffold based skin regeneration. Biomaterials 2009, 30, 789–796. [Google Scholar]
- Keck, M.; Haluza, D.; Selig, H.F.; Jahl, M.; Lumenta, D.B.; Kamolz, L.P.; Frey, M. Adipose tissue engineering: Three different approaches to seed preadipocytes on a collagen-elastin matrix. Ann. Plast. Surg 2011, 67, 484–488. [Google Scholar]
- Hateboer, G.; Wobst, A.; Petersen, B.O.; Le Cam, L.; Vigo, E.; Sardet, C.; Helin, K. Cell cycle-regulated expression of mammalian CDC6 is dependent on E2F. Mol. Cell. Biol 1998, 18, 6679–6697. [Google Scholar]
- Kapuscinski, J. DAPI: A DNA-specific fluorescent probe. Biotech. Histochem 1995, 70, 220–233. [Google Scholar]


© 2013 by the authors; licensee MDPI, Basel, Switzerland This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/3.0/).
Share and Cite
Killat, J.; Reimers, K.; Choi, C.Y.; Jahn, S.; Vogt, P.M.; Radtke, C. Cultivation of Keratinocytes and Fibroblasts in a Three-Dimensional Bovine Collagen-Elastin Matrix (Matriderm®) and Application for Full Thickness Wound Coverage in Vivo. Int. J. Mol. Sci. 2013, 14, 14460-14474. https://doi.org/10.3390/ijms140714460
Killat J, Reimers K, Choi CY, Jahn S, Vogt PM, Radtke C. Cultivation of Keratinocytes and Fibroblasts in a Three-Dimensional Bovine Collagen-Elastin Matrix (Matriderm®) and Application for Full Thickness Wound Coverage in Vivo. International Journal of Molecular Sciences. 2013; 14(7):14460-14474. https://doi.org/10.3390/ijms140714460
Chicago/Turabian StyleKillat, Jasper, Kerstin Reimers, Claudia Y. Choi, Sabrina Jahn, Peter M. Vogt, and Christine Radtke. 2013. "Cultivation of Keratinocytes and Fibroblasts in a Three-Dimensional Bovine Collagen-Elastin Matrix (Matriderm®) and Application for Full Thickness Wound Coverage in Vivo" International Journal of Molecular Sciences 14, no. 7: 14460-14474. https://doi.org/10.3390/ijms140714460




