New Developments in Medical Applications of Hybrid Hydrogels Containing Natural Polymers
Abstract
:1. Introduction
1.1. Polymers Used in Hybrid Hydrogels
1.1.1. Microgel
1.1.2. Hybrid Nanogels
1.1.3. Multifunctional Hybrid Nanogels
1.1.4. Hybrid Polymer Nanogel/Hydrogels
1.1.5. Physical Hydrogels
1.1.6. Chemically or Covalently Crosslinked Hydrogels
1.1.7. Self-Assembling Hybrid Hydrogels
1.1.8. Interpenetrated and Semi-Interpenetrated Polymer Networks
1.1.9. Core-Shell Polymer Networks
1.1.10. Supramolecular Hydrogel
2. Preparation Procedures for Polymeric Hybrid Hydrogels
2.1. Routes to Obtain Hybrid Hydrogels
2.1.1. Chemical Modifications
2.1.2. Functionalization
2.1.3. Stealth Functionalization
2.1.4. PEGylation
2.2. Processing Methods
3. Properties
3.1. Swelling
3.2. Mechanical Properties
3.3. Responsiveness
3.4. Porosity and Permeation
4. Applications
5. Homopolysaccharides-Based Hybrid Hydrogels
5.1. Ability of Homopolysaccharides to Form Hybrid Hydrogels
5.2. Biomedical Applications of Homopolysaccharides-Based Hydrogels
5.2.1. Tissue Engineering
5.2.2. Wound Dressing
5.2.3. Drug Delivery
5.2.4. Other Biomedical Applications
6. Heteropolysaccharides-Based Hybrid Hydrogels
6.1. Ability of Heteropolysaccharides to Form Hybrid Hydrogels
6.2. Biomedical Applications of Heteropolysaccharides-Based Hybrid Hydrogels
6.2.1. Tissue Engineering
6.2.2. Wound Dressing
6.2.3. Drug Delivery
7. Hybrid Proteins Based Hydrogels for Biomedical Applications
7.1. Ability of Proteins/Peptides to Form Hybrid Hydrogels
7.2. Properties of Proteins to Form Hybrid Hydrogels for Biomedical Applications
7.2.1. Collagen
7.2.2. Gelatin
7.2.3. Keratin
7.2.4. Bovine Serum Albumin
7.2.5. Silk
7.2.6. Resilin
7.2.7. Whey Proteins
7.2.8. Soy Protein Isolate
7.2.9. Elastin
7.3. Biomedical Applications of Protein Based Hybrid Hydrogels
7.3.1. Tissue Engineering
7.3.2. Bone Tissue Engineering
7.3.3. Cartilage Tissue Engineering
7.3.4. Wound Healing
7.3.5. Drug and Molecule Delivery
8. Nucleic Acids Based Hybrid Hydrogels for Biomedical Applications
8.1. Nucleic Acids Ability to Form Hydrogels
8.2. Biomedical Applications of Nucleic Acids-Containing Hybrid Hydrogels
8.2.1. Drug Delivery
8.2.2. Immunotherapy
8.2.3. Biosensing Applications
9. Hybrid Hydrogels Containing Lignin for Biomedical Applications
9.1. Bioactive Compounds Delivery
9.2. Applications as Antimicrobial, Antioxidant, Antifungal materials
10. Conclusions and Future Trends
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
Abbreviations
| AAc—acrylic acid | LCST—lower critical phase transition temperature |
| AAm—acrylamide | LMWG—low-molecular-weight gelator |
| Alg—alginate | MA—maleic anhydride |
| APS—ammonium persulfate | MAA—methacrylic acid |
| ATRP—atom transfer radical polymerization | MACMC—methacrylate carboxymethyl cellulose |
| BC—bacterial cellulose | MBA—N,N′-methylene bisacrylamide |
| bFGF—basic fibroblast growth factor | MS—microspheres |
| BIS—N,N-Methylene bisacrylamide | MW—molecular weight |
| JuanuaryBMSCs—bone mesenchymal stem cells | MGG—methacrylated gellan gum |
| BSA—bovine serum albumin | MA—maleic anhydride |
| CA—crosslinking agent | NanoCliP—nanogel-crosslinked porous |
| CaM—Calmodulin | NIPAAm—N-isopropylacrylamide |
| CBA—N,N′-bis(acryloyl)cystamine | PAA—polyacrylic acid |
| CBMA—carboxybetaine methacrylate | PAAm—polyacrylamide |
| CE-chitosan—carboxyethyl chitosan | PAN—polyacrylonitrile |
| CG—Carrageenan | PCL—poly(ε-caprolactone) |
| Cel—cellulose | PDEA—poly(diethylacrylamide) |
| CHP—cholesterol-bearing pullulan | PDMAEMA—poly 2-(dimethylamino) ethyl methacrylate |
| CHP—cholesteryl-modified pullulan | PDMS—poly(dimethylsiloxane) |
| CHPANG—acrylate group-modified cholesterol-bearing pullulan | PEG—poly (ethylene glycol) |
| CHPOA—acryloyl group modified-cholesterol-bearing pullulan | PEGDA—polyethylene glycol diacrylate |
| CMC—carboxymethyl cellulose | PEG-Nor—norbornene immobilized tetra-arm PEG |
| CM-chitosan—N-O-carboxymethyl chitosan | PEI—polyethylenimine |
| CMP—carboxymethyl pullulan | PEO—poly(ethylene oxide) |
| CMPVA—carboxymethyl polyvinyl alcohol | PET—poly (ethylene terephthalate) |
| CMS—carboxymethyl starch | PG—polymer gelator |
| CNCs—cellulose nanocrystals | PGA—poly(glycolic acid) |
| CNF—cellulose nanofiber | PHB—poly(3-hydroxybutyrate) |
| CPUNs—cationic polyurethane nanoparticles | PHEA—poly(N-hydroxyethyl acrylamide) |
| CS—chitosan | PHEMA—poly(2-hydroxyethyl methacrylate) |
| CTS—chondroitin sulfate | PLA—poly (lactic acid) |
| CUR—curcumin | PLGA—poly(lactic-co-glycolic acid) |
| DDS—drug delivery system | PLLA—poly(l-lactide) |
| DN—double network | PMAA—poly(methacrylic acid) |
| DNA—deoxyribonucleic acid | PMMA—poly(methyl methacrylate) |
| DP—difunctionalized PEG | PNIPAAm—poly(N-isopropylacrylamide) |
| DPC-DN—dual physically cross-linked double network | PoH—poloxamer-heparin |
| DTT—dithiothreitol | PPO—poly(propylene oxide) |
| EBI—electron beam irradiation | PPy—polypyrrole |
| ECM—extracellular matrix | PTX—paclitaxel |
| EDAC—1-ethyl-3-(3- dimethylaminopropyl) carbodiimide | PU—polyurethane |
| EDC—1-(3-Dimethyl aminopropyl)-3-ethylcarbodiimide Hydrochloride | PULMA—methacrylated pullulan |
| EDTA—ethylene diamine tetraacetic acid | PUU—polyurethane-urea |
| EGDA—ethylene glycol diacrylate | PVP—polyvinylpyrrolidone |
| EGDMA—ethylene glycol dimethacrylate | Q-chitosan—quaternary chitosan |
| ELPs—elastin-like polypeptides | rBMSCs—bone marrow stem cells isolated from rabbits |
| FK—feather keratin | rMSCs—marrow stem cells isolated from rabbits |
| FT—freeze–thawing | RAFT—reversible addition–fragmentation chain-transfer polymerization |
| GA—glutaraldehyde | RNA—ribonucleic acid |
| GAG—glycosaminoglycan | RITP—iodine-mediated polymerization |
| GC—glycol chitosan | RLPs—resilin-like polypeptides |
| GC-DP—hydrogels based on glycol chitosan and difunctionalized PEG | RT-PCR—reverse transcription polymerase chain reaction |
| GG—gellan gum | SA—sodium alginate |
| GI tract—gastrointestinal tract | SAPCs—superabsorbent polymer composites |
| HA—hyaluronic acid | SF—silk fibroin |
| Hce—hemicellulose | SGF—simulated gastric fluid |
| Hep—Heparin | SIF—simulated intestinal fluid |
| hBMSCs—human bone marrow stromal cell | sIPNs—semi-IPNs |
| HDI—hexamethylene diisocyanate | siRNA—small interfering RNA |
| HEC—hydroxyethyl cellulose | SP—soy protein |
| HEMA—2-hydroxyethyl methacrylate | SPI—soy protein isolate |
| HHP—high hydrostatic pressure | SPION—super paramagnetic iron oxide nanoparticles |
| HLC—human like collagen | SS—silk sericin |
| hMSCs—human mesenchymal stem cells | TEMED—N,N,N′,N′-tetramethylethylenediamine |
| hBMSCs—human bone marrow stromal cell | TG—transglutaminase |
| HP—homopolysaccharides | TGFβ1—transforming growth factor β1 |
| HPA—hydroxyphenyl propionic acid | |
| HPC—hydroxypropyl cellulose | THPC—tetrakis(hydroxymethyl)phosphonium chloride |
| HPMA—2-hydroxypropyl methacrylate | TIPS—thermally induced phase separation |
| HSP27—heat shock protein 27 | VEGF—vascular endothelial growth factor |
| HRP—horseradish peroxidase | VP—vinyl pyrrolidone |
| ICH—intracerebral hemorrhage | WP—whey protein |
| IPN—interpenetrated network | WPC—whey protein concentrates |
| KOS—keratose | WPH—whey protein hydrolysates |
| KTN—kerateine | WPI—whey protein isolates |
| KPS—potassium persulfate | XG—xanthan gum |
| LZ—leucine zipper | |
References
- Kumar, A.; Han, S.S. PVA-based hydrogels for tissue engineering: A review. Int. J. Polym. Mater. Polym. Biomater. 2017, 66, 159–182. [Google Scholar] [CrossRef]
- Budama-Kilinc, Y.; Cakir-Koc, R.; Aslan, B.; Özkan, B.; Mutlu, H.; Üstün, E. Chapter 12: Hydrogels in Regenerative Medicine. In Biomaterials in Regenerative Medicine; Dobrzański, L.A., Ed.; IntechOpen: London, UK, 2018; pp. 277–301. [Google Scholar]
- Durmaz, S.; Okay, O. Acrylamide/2-acrylamido-2-methylpropane sulfonic acid sodium salt-based hydrogels: Synthesis and characterization. Polymer 2000, 41, 3693–3704. [Google Scholar] [CrossRef]
- Ekici, S.; Saraydin, D. Synthesis, characterization and evaluation of IPN hydrogels for antibiotic release. Drug Deliv. 2004, 11, 381–388. [Google Scholar] [CrossRef] [PubMed]
- Peppas, N.P.; Leobandung, W.; Ichikawa, H. Hydrogels in pharmaceutical formulations. Eur. J. Pharm. Biopharm. 2000, 50, 27–46. [Google Scholar] [CrossRef]
- Swami, S.N. Radiation synthesis of polymeric hydrogels for swelling-controlled drug release studies. Ph.D. Thesis, Western Sydney University, Sydney, Australia, 2004. Available online: http://handle.uws.edu.au:8081/1959.7/698 (accessed on 7 January 2020).
- Katime, I.; Novoa, R.; Zuluaga, F. Swelling kinetics and release studies of theophylline and aminophylline from acrylic acid/n-alkyl methacrylate hydrogels. Eur. Polym. J. 2001, 37, 1465–1471. [Google Scholar] [CrossRef]
- Zhang, T.; Yang, R.; Yang, S.; Guan, J.; Zhang, D.; Ma, Y.; Liu, H. Research progress of self-assembled nanogel and hybrid hydrogel systems based on pullulan derivatives. Drug Deliv. 2018, 25, 278–292. [Google Scholar] [CrossRef]
- Kopeček, J.; Tang, A.; Wang, C.; Stewart, R.J. De novo design of biomedical polymers. Hybrids from synthetic macromolecules and genetically engineered protein domains. Macomol. Symp. 2001, 174, 31–42. [Google Scholar] [CrossRef]
- Molina, M.; Asadian-Birjand, M.; Balach, J.; Bergueiro, J.; Miceliac, E.; Calderon, M. Stimuli-responsive nanogel composites and their application in nanomedicine. Chem. Soc. Rev. 2015, 44, 6161–6186. [Google Scholar] [CrossRef] [Green Version]
- Jia, X.; Kiick, K.L. Hybrid multicomponent hydrogels for tissue engineering. Macromol. Biosci. 2009, 9, 140–156. [Google Scholar] [CrossRef] [Green Version]
- Myung, D.; Waters, D.; Wiseman, M.; Duhamel, P.E.; Noolandi, J.; Ta, C.N.; Frank, C.W. Progress in the development of interpenetrating polymer network hydrogels. Polym. Adv. Technol. 2008, 19, 647–657. [Google Scholar] [CrossRef] [Green Version]
- Jonker, A.M.; Löwik, D.W.P.M.; van Hest, J.C.M. Peptide- and protein-based hydrogels. Chem. Mater. 2012, 24, 759–773. [Google Scholar] [CrossRef]
- Lau, H.K.; Kiick, K.L. Opportunities for multicomponent hybrid hydrogels in biomedical applications. Biomacromolecules 2015, 16, 28–42. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Maisani, M.; Pezzoli, D.; Chassande, O.; Mantovani, D. Cellularizing hydrogel-based scaffolds to repair bone tissue: How to create a physiologically relevant micro-environment? J. Tissue Eng. 2017, 8. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Joseph, C.A.; McCarthy, C.W.; Tyo, A.; Hubbard, K.; Fisher, H.; Altscheffel, J.; He, W.; Pinnaratip, R.; Lui, Y.; Lee, B.P.; et al. Development of an injectable nitric oxide releasing poly(ethylene) glycol-Fibrin adhesive hydrogel. ACS Biomater. Sci. Eng. 2019, 5, 959–969. [Google Scholar] [CrossRef] [PubMed]
- Hoffman, A.S. Hydrogels for biomedical applications. Ann. N. Y. Acad. Sci. 2001, 944, 62–73. [Google Scholar] [CrossRef] [PubMed]
- Yang, G.; Lin, H.; Rothrauff, B.B.; Yu, S.; Tuan, R.S. Multilayered polycaprolactone/gelatin fiber-hydrogel composite for tendon tissue engineering. Acta Biomater. 2016, 35, 68–76. [Google Scholar] [CrossRef] [Green Version]
- Patel, D.; Sharma, S.; Screen, H.R.C.; Bryant, S.J. Effects of cell adhesion motif, fiber stiffness, and cyclic strainon tenocyte gene expression in a tendon mimetic fiber composite hydrogel. Biochem. Biophys. Res. Commun. 2018, 499, 642–647. [Google Scholar] [CrossRef]
- Kopeček, J. Hydrogel Biomaterials: A Smart Future? Biomaterials 2007, 28, 5185–5192. [Google Scholar] [CrossRef] [Green Version]
- Liang, Y.; Liu, W.; Han, B.; Yang, C.; Ma, Q.; Song, F.; Bi, Q. An in situ formed biodegradable hydrogel for reconstruction of the corneal endothelium. Colloids Surf. B: Biointerfaces 2011, 82, 1–7. [Google Scholar] [CrossRef]
- Ehrick, J.D.; Deo, S.K.; Browning, T.W.; Bachas, L.G.; Madou, M.J.; Daunert, S. Genetically engineered protein in hydrogels tailors stimuli-responsive characteristics. Nat. Mater. 2005, 4, 298–302. [Google Scholar] [CrossRef]
- Sengupta, D.; Heilshorn, S.C. Protein-engineered biomaterials: Highly tunable tissue engineering scaffolds. Tissue Eng. Part B: Rev. 2010, 16, 285–293. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Foo, W.P.C.T.; Lee, J.S.; Mulyasasmita, W.; Parisi-Amon, A.; Heilshorn, S.C. Two-component protein-engineered physical hydrogels for cell encapsulation. Proc. Natl. Acad. Sci. USA 2009, 106, 22067–22072. [Google Scholar]
- Sakai, S.; Hirose, K.; Taguchi, K.; Ogushi, Y.; Kawakami, K. An injectable, in situ enzymatically gellable, gelatin derivative for drug delivery and tissue engineering. Biomaterials 2009, 30, 3371–3377. [Google Scholar] [CrossRef] [PubMed]
- Xing, Y.; Cheng, E.; Yang, Y.; Chen, P.; Zhang, T.; Sun, Y.; Yang, Z.; Liu, D. Self-assembled DNA hydrogels with designable thermal and enzymatic responsiveness. Adv. Mater. 2011, 23, 1117–1121. [Google Scholar] [CrossRef] [PubMed]
- Davidenko, N.; Campbell, J.J.; Thian, E.S.; Watson, C.J.; Cameron, R.E. Collagen–hyaluronic acid scaffolds for adipose tissue engineering. Acta Biomater. 2010, 6, 3957–3968. [Google Scholar] [CrossRef]
- Raschip, I.E.; Hitruc, G.E.; Vasile, C.; Popescu, M.C. Effect of the lignin type on the morphology and thermal properties of xanthan/lignin hydrogels. Int. J. Biol. Macromol. 2013, 54, 230–237. [Google Scholar] [CrossRef]
- Raschip, I.E.; Hitruc, E.G.; Vasile, C. Semi-interpenetrating polymer networks containing polysaccharides. II. Xanthan/lignin network: A spectral and thermal characterization. High Perform. Polym. 2011, 23, 219–229. [Google Scholar] [CrossRef]
- Hejčl, A.; Sedý, J.; Kapcalová, M.; Toro, D.A.; Amemori, T.; Lesný, P.; Likavcanová-Mašínová, K.; Krumbholcová, E.; Prádný, M.; Michálek, J.; et al. HPMA-RGD hydrogels seeded with mesenchymal stem cells improve functional outcome in chronic spinal cord injury. Stem Cells Dev. 2010, 19, 1535–1546. [Google Scholar] [CrossRef]
- Beamish, J.A.; Zhu, J.; Kottke-Marchant, K.; Marchant, R.E. The effects of monoacrylated poly(ethylene glycol) on the properties of poly (ethylene glycol) diacrylate hydrogels used for tissue engineering. J. Biomed. Mater. Res. Part A 2010, 92, 441–450. [Google Scholar] [CrossRef] [Green Version]
- Zustiak, S.P.; Leach, J.B. Hydrolytically degradable poly (ethylene glycol) hydrogel scaffolds with tunable degradation and mechanical properties. Biomacromolecules 2010, 11, 1348–1357. [Google Scholar] [CrossRef] [Green Version]
- Silva, A.K.A.; Richard, C.; Bessodes, M.; Scherman, D.; Merten, O.-W. Growth factor delivery approaches in hydrogels. Biomacromolecules 2008, 10, 9–18. [Google Scholar] [CrossRef] [PubMed]
- Varghese, S.; Elisseeff, J.H. Hydrogels for musculoskeletal tissue engineering. Adv. Polym. Sci. 2006, 203, 95–144. [Google Scholar]
- Jiang, Z.; Hao, J.; You, Y.; Liu, Y.; Wang, Z.; Deng, X. Biodegradable and thermoreversible hydrogels of poly (ethylene glycol)-poly (ε-caprolactone-co-glycolide)-poly (ethylene glycol) aqueous solutions. J. Biomed. Mater. Res. Part A 2008, 87, 45–51. [Google Scholar] [CrossRef] [PubMed]
- Deshmukh, M.; Singh, Y.; Gunaseelan, S.; Gao, D.; Stein, S.; Sinko, P.J. Biodegradable poly (ethylene glycol) hydrogels based on a self-elimination degradation mechanism. Biomaterials 2010, 31, 6675–6684. [Google Scholar] [CrossRef] [Green Version]
- Schmedlen, R.H.; Masters, K.S.; West, J.L. Photocrosslinkable polyvinyl alcohol hydrogels that can be modified with cell adhesion peptides for use in tissue engineering. Biomaterials 2002, 23, 4325–4332. [Google Scholar] [CrossRef]
- Ossipov, D.A.; Brännvall, K.; Forsberg-Nilsson, K.; Hilborn, J. Formation of the first injectable poly (vinyl alcohol) hydrogel by mixing of functional PVA precursors. J. Appl. Polym. Sci. 2007, 106, 60–70. [Google Scholar] [CrossRef]
- Higuchi, A.; Aoki, N.; Yamamoto, T.; Miyazaki, T.; Fukushima, H.; Tak, T.M.; Jyujyoji, S.; Egashira, S.; Matsuoka, Y.; Natori, S.H. Temperature-induced cell detachment on immobilized pluronic surface. J. Biomed. Mater. Res. Part A 2006, 79, 380–392. [Google Scholar] [CrossRef]
- Zhu, J. Bioactive modification of poly (ethylene glycol) hydrogels for tissue engineering. Biomaterials 2010, 31, 4639–4656. [Google Scholar] [CrossRef] [Green Version]
- Geckil, H.; Xu, F.; Zhang, X.; Moon, S.; Demirci, U. Engineering hydrogels as extracellular matrix mimics. Nanomedicine 2010, 5, 469–484. [Google Scholar] [CrossRef] [Green Version]
- Matsumoto, T.; Isogawa, Y.; Tanaka, T.; Kondo, A. Streptavidin-hydrogel prepared by sortase A-assisted click chemistry for enzyme immobilization on an electrode. Biosens. Bioelectron. 2018, 99, 56. [Google Scholar] [CrossRef] [Green Version]
- Ito, F.; Usui, K.; Kawahara, D.; Suenaga, A.; Maki, T.; Kidoaki, S.; Suzuki, H.; Taiji, M.; Itoh, M.; Hayashizaki, Y.; et al. Reversible hydrogel formation driven by protein-peptide-specific interaction and chondrocyte entrapment. Biomaterials 2009, 31, 58–66. [Google Scholar] [CrossRef] [PubMed]
- Ramirez, M.; Guan, D.; Ugaz, V.; Chen, Z. Intein-triggered artificial protein hydrogels that support the immobilization of bioactive proteins. J. Am. Chem. Soc. 2013, 135, 5290. [Google Scholar] [CrossRef] [PubMed]
- Krishna, O.D.; Kiick, K.L. Protein- and peptide-modified synthetic polymeric biomaterials. Biopolymers 2010, 94, 32–48. [Google Scholar] [CrossRef] [Green Version]
- Pamfil, D.; Vasile, C.; Tarțău, L.; Vereștiuc, L.; Poieată, A. pH-Responsive 2-hydroxyethyl methacrylate/citraconic anhydride-modified collagen hydrogels as ciprofloxacin carriers for wound dressings. J. Bioact. Compat. Polym. 2017, 32, 355–381. [Google Scholar] [CrossRef]
- Dorwal, D. Nanogels as Novel and versatile pharmaceutics. J. Pharm. Pharm. Sci. 2012, 4, 67–74. [Google Scholar]
- Yadav, H.K.S.; Al Halabi, N.A.; Alsalloum, G.A. Nanogels as Novel Drug Delivery Systems-A Review. J. Pharm. Pharm. Res. 2017, 1, 1–8. [Google Scholar]
- Tahara, Y.; Akiyoshi, K. Current advances in self-assembled nanogel delivery systems for immunotherapy. Adv. Drug Deliv. Rev. 2015, 95, 65–76. [Google Scholar] [CrossRef]
- Bencherif, S.A.; Siegwart, D.J.; Srinivasan, A.; Horkay, F.; Hollinger, J.O.; Washburn, N.R.; Matyjaszewski, K. Nanostructured hybrid hydrogels prepared by a combination of atom transfer radical polymerization and free radical polymerization. Biomaterials 2009, 30, 5270–5278. [Google Scholar] [CrossRef] [Green Version]
- Sahiner, N.; Godbey, W.T.; McPherson, G.L.; John, V.T. Microgel, nanogel and hydrogel–hydrogel semi-IPN composites for biomedical applications: Synthesis and characterization. Colloid Polym. Sci. 2006, 284, 1121–1129. [Google Scholar] [CrossRef]
- Wu, W.; Zhou, S. Hybrid micro-/nanogels for optical sensing and intracellular imaging. Nano Rev. 2010, 1, 5730. [Google Scholar] [CrossRef]
- Lohani, A.; Singh, G.; Sankar Bhattacharya, S.; Verma, A. Interpenetrating Polymer Networks as Innovative Drug Delivery Systems. J. Drug Deliv. 2014, 2014, 583612. [Google Scholar] [CrossRef] [Green Version]
- Hoare, T.R.; Kohane, D.S. Hydrogels in drug delivery: Progress and challenges. Polymer 2008, 49, 1993–2007. [Google Scholar] [CrossRef] [Green Version]
- Ebara, M.; Kotsuchibashi, Y.; Narain, R.; Idota, N.; Kim, Y.J.; Hoffman, J.M.; Uto, K.; Aoyagit, T. Smart Biomaterials; Springer: Tokyo, Japan, 2014; ISBN 978-4-431-54400-5. [Google Scholar]
- Amini, A.A.; Nair, L.S. Injectable hydrogels for bone and cartilage repair. Biomed. Mater. 2012, 7, 024105. [Google Scholar] [CrossRef] [PubMed]
- Jin, R. Chapter 2: In-Situ Forming Biomimetic Hydrogels for Tissue Regeneration. In Biomedicine; Lin, C., Ed.; INTECH Open Access Publisher: London, UK, 2012; pp. 35–58. [Google Scholar]
- Augst, A.D.; Kong, H.J.; Mooney, D.J. Alginate hydrogels as biomaterials. Macromol. Biosci. 2006, 6, 623–633. [Google Scholar] [CrossRef] [PubMed]
- Czarnecki, S.; Rossow, T.; Seiffert, S. Hybrid Polymer-Network Hydrogels with Tunable Mechanical Response. Polymers 2016, 8, 82. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Sun, J.-Y.; Zhao, X.; Illeperuma, W.R.K.; Chaudhuri, O.; Oh, K.H.; Mooney, D.J.; Vlassak, J.J.; Suo, Z. Highly stretchable and tough hydrogels. Nature 2012, 489, 133–136. [Google Scholar] [CrossRef]
- Lin, P.; Ma, S.; Wang, X.; Zhou, F. Molecularly engineered dual-crosslinked hydrogel with ultrahigh mechanical strength, toughness, and good self-recovery. Adv. Mater. 2015, 27, 2054–2059. [Google Scholar] [CrossRef]
- Narita, T.; Mayumi, K.; Ducouret, G.; Hébraud, P. Viscoelastic properties of poly(vinyl alcohol) hydrogels having permanent and transient cross-links studied by microrheology, classical rheometry, and dynamic light scattering. Macromolecules 2013, 46, 4174–4183. [Google Scholar] [CrossRef]
- Kondo, S.; Hiroi, T.; Han, Y.S.; Kim, T.H.; Shibayama, M.; Chung, U.I.; Sakai, T. Reliable hydrogel with mechanical “fuse link” in an aqueous environment. Adv. Mater. 2015, 27, 7407–7411. [Google Scholar] [CrossRef]
- Sletten, E.M.; Bertozzi, C.R. Bioorthogonal chemistry: Fishing for selectivity in a sea of functionality. Angew. Chem. Int. Ed. 2009, 48, 6974–6998. [Google Scholar] [CrossRef] [Green Version]
- Kopeček, J.; Yang, J. Smart Self-Assembled Hybrid Hydrogel Biomaterials. Angew. Chem. Int. Ed. 2012, 51, 7396–7417. [Google Scholar] [CrossRef] [PubMed]
- Rodriguez, L.M.D.L.; Hemar, Y.; Cornish, J.; Brimble, M.A. Structure–mechanical property correlations of hydrogel forming β-sheet peptides. Chem. Soc. Rev. 2016, 45, 4797. [Google Scholar] [CrossRef] [PubMed]
- Baker, B.M.; Chen, C.S. Deconstructing the third dimension–how 3D culture microenvironments alter cellular cues. J. Cell Sci. 2012, 125, 3015–3024. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Yang, J.; Xu, C.; Wang, C.; Kopeček, J. Refolding hydrogels self-assembled from N-(2-hydroxypropyl)methacrylamide graft copolymers by antiparallel coiled-coil formation. Biomacromolecules 2006, 7, 1187–1195. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Ren, N.; Sun, R.; Xia, K.; Zhang, Q.; Li, W.; Wang, F.; Zhang, X.; Ge, Z.; Wang, L.; Fan, C.; et al. DNA-Based Hybrid Hydrogels Sustain Water-Insoluble Ophthalmic Therapeutic Delivery against Allergic Conjunctivitis. ACS Appl. Mater. Interfaces 2019, 11, 26704–26710. [Google Scholar] [CrossRef] [PubMed]
- Mundargi, R.C.; Patil, S.A.; Kulkarni, P.V.; Mallikarjuna, N.N.; Aminabhavi, T.M. Sequential interpenetrating polymer network hydrogel microspheres of poly(methacrylic acid) and poly(vinyl alcohol) for oral controlled drug delivery to intestine. J. Microencapsul. 2008, 25, 228–240. [Google Scholar] [CrossRef]
- Liu, X.; Guo, H.; Zha, L. Study of pH/temperature dual stimuli-responsive nanogels with interpenetrating polymer network structure. Polym. Int. 2012, 61, 1144–1150. [Google Scholar] [CrossRef]
- Blackburn, W.H.; Dickerson, E.B.; Smith, M.H.; McDonald, J.F.; Lyon, L.A. Peptide-Functionalized Nanogels for Targeted siRNA Delivery. Bioconjug. Chem. 2009, 20, 960–968. [Google Scholar] [CrossRef] [Green Version]
- Schachschal, S.; Balaceanu, A.; Melian, C.; Demco, D.E.; Eckert, T.; Richtering, W.; Pich, A. Polyampholyte Microgels with Anionic Core and Cationic Shell. Macromolecules 2010, 43, 4331–4339. [Google Scholar] [CrossRef]
- Zhang, W.; Yao, R.; Tao, W.; He, H.; Shui, S. Preparation of monodisperse HPMC/PAA hybrid nanogels via surfactant-free seed polymerization. Colloid Polym. Sci. 2013, 292, 317–324. [Google Scholar] [CrossRef]
- Nayak, S.; Lee, H.; Chmielewski, J.; Lyon, L.A. Folate-Mediated Cell Targeting and Cytotoxicity Using Thermoresponsive Microgels. J. Am. Chem. Soc. 2004, 126, 10258–10259. [Google Scholar] [CrossRef] [PubMed]
- Dickerson, E.; Blackburn, W.; Smith, M.; Kapa, L.; Lyon, L.A.; McDonald, J. Chemosensitization of cancer cells by siRNA using targeted nanogel delivery. BMC Cancer 2010, 10, 10. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Lapeyre, V.; Ancla, C.; Catargi, B.; Ravaine, V. Glucose-responsive microgels with a core-shell structure. J. Colloid Interface Sci. 2008, 327, 316–323. [Google Scholar] [CrossRef]
- Zieris, A.; Prokoph, S.; Levental, K.R.; Welzel, P.B.; Grimmer, M.; Freudenberg, Y.; Werner, C. FGF-2 and VEGF functionalization of starPEG–heparin hydrogels to modulate biomolecular and physical cues of angiogenesis. Biomaterials 2010, 31, 7985–7994. [Google Scholar] [CrossRef] [PubMed]
- Jin, R.; Moreira Teixeira, L.S.; Krouwels, A.; Dijkstra, P.J.; van Blitterswijk, C.A.; Karperien, M.; Feijen, J. Synthesis and characterization of hyaluronic acid–poly (ethylene glycol) hydrogels via Michael addition: An injectable biomaterial for cartilage repair. Acta Biomater. 2010, 6, 1968–1977. [Google Scholar] [CrossRef] [PubMed]
- Li, F.; Griffith, M.; Li, Z.; Tanodekaew, S.; Sheardown, H.; Hakim, M.; Carlsson, D.J. Recruitment of multiple cell lines by collagen-synthetic copolymer matrices in corneal regeneration. Biomaterials 2005, 26, 3093–3104. [Google Scholar] [CrossRef] [PubMed]
- Nistor, M.T.; Vasile, C.; Tatia, R.; Chiriac, A. Hybrid collagen/pNIPAAM hydrogel nanocomposites for tissue engineering application. Colloid Polym. Sci. 2018, 296, 1555–1571. [Google Scholar]
- Nistor, M.T.; Chiriac, A.P.; Nita, L.E.; Vasile, C. Characterization of the semi-interpenetrated network based on collagen and poly(N-isopropyl acrylamide-co-diethylene glycol diacrylate). Int. J. Pharm. 2013, 452, 92–101. [Google Scholar] [CrossRef]
- Cheaburu, C.N.; Vasile, C. Responsive freeze-drying interpolymeric associations of alginic acid and PNIPAM. II. Transition and temperature dependence on pH and composition. Cell. Chem. Technol. 2008, 42, 207–212. [Google Scholar]
- Radvar, E.; Azevedo, H.S. Supramolecular Peptide/Polymer Hybrid Hydrogels for Biomedical Applications. Macromol. Biosci. 2019, 19, 1800221. [Google Scholar] [CrossRef] [Green Version]
- Vandermeulen, G.W.M.; Klok, H.A. Peptide/protein hybrid materials: Enhanced control of structure and impropved performance through conjugation of biological and synthetic polymers. Macromol. Biosci. 2004, 4, 383–398. [Google Scholar] [CrossRef] [PubMed]
- Gulrez, S.K.H.; Al-Assaf, S.; Phillips, G.O. Hydrogels: Methods of Preparation, Characterisation and Applications. In Progress in Molecular and Environmental Bioengineering. Analysis and Modeling to Technology Applications; Carpi, A., Ed.; IntechOpen: Rijeka, Croatia, 2011. [Google Scholar]
- Khademhosseini, A.; Langer, R. Microengineered hydrogels for tissue engineering. Biomaterials 2007, 28, 5087–5092. [Google Scholar] [CrossRef] [PubMed]
- Barner-Kowollik, C. Handbook of RAFT Polymerization; Wiley-VCH Verlag GmbH & Co.: Weinheim, Germany, 2008; ISBN 978-3-527-31924-4. [Google Scholar]
- Wang, C.; Kopeček, J.; Stewart, R.J. Hybrid hydrogels crosslinked by genetically engineered coiled-coil block proteins. Biomacromolecules 2001, 2, 912–920. [Google Scholar] [CrossRef] [PubMed]
- Lim, S.; Jung, G.A.; Muckom, R.J.; Glover, D.J.; Clark, D.S. Engineering bioorthogonal protein–polymer hybrid hydrogel as a functional protein immobilization platform. Chem. Commun. 2019, 55, 806–809. [Google Scholar] [CrossRef]
- Sierra-Martin, B.; Fernandez-Barbero, A. Multifunctional hybrid nanogels for theranostic applications. Soft Matter 2015, 14, 8205–8216. [Google Scholar] [CrossRef] [PubMed]
- Sanson, N.; Rieger, J. Synthesis of nanogels/microgels by conventional and controlled radical crosslinking copolymerization. Polym. Chem. 2010, 1, 96577. [Google Scholar] [CrossRef]
- Kabanov, A.V.; Vinogradov, S.V. Nanogels as pharmaceutical carriers: Finite networks of infinite capabilities. Angew. Chem. Int. Ed. 2009, 48, 5418–5429. [Google Scholar] [CrossRef] [Green Version]
- Wu, H.Q.; Wang, C.C. Biodegradable smart nanogels: A new platform for targeting drug delivery and biomedical diagnostics. Langmuir 2016, 32, 6211–6225. [Google Scholar] [CrossRef]
- Karg, M. Functional Materials Design through Hydrogel Encapsulation of Inorganic Nanoparticles: Recent Developments and Challenges. Macromol. Chem. Phys. 2016, 217, 242–255. [Google Scholar] [CrossRef]
- Eslami, P.; Rossi, F.; Fedeli, S. Review Hybrid Nanogels: Stealth and Biocompatible Structures for Drug Delivery Applications. Pharmaceutics 2019, 11, 71. [Google Scholar] [CrossRef] [Green Version]
- Grover, G.N.; Rao, N.; Christman, K.L. Myocardial Matrix-Polyethylene Glycol Hybrid Hydrogels for Tissue Engineering. Nanotechnology 2014, 25, 014011. [Google Scholar] [CrossRef] [PubMed]
- Foster, J. Chapter 12: PEGylation and BioPEGylation of Polyhydroxyalkanoates: Synthesis, Characterisation and Applications. In Biopolymers; Elnashar, M., Ed.; IntevhOpen: Rijeka, Croatia, 2010; pp. 243–256. [Google Scholar]
- Jiang, Y.; Chen, J.; Deng, C.; Suuronen, E.J.; Zhong, Z. Click hydrogels, microgels and nanogels: Emerging platforms for drug delivery and tissue engineering. Biomaterials 2014, 35, 4969–4985. [Google Scholar] [CrossRef] [PubMed]
- Chirani, N.; Yahia, L.H.; Gritsch, L.; Motta, F.L.; Chirani, S.; Faré, S. History and Applications of Hydrogels. J. Biomed. Sci. 2015, 4, 32. [Google Scholar] [CrossRef]
- Zhou, M.; Smith, A.M.; Das, A.K.; Hodson, N.W.; Collins, R.F.; Ulijn, R.V.; Gough, J.E. Self-assembled peptide-based hydrogels as scaffolds for anchorage-dependent cells. Biomaterials 2009, 30, 2523–2530. [Google Scholar] [CrossRef]
- Palmese, L.L.; Thapa, R.K.; Sullivan, M.O.; Kiick, K.L. Hybrid hydrogels for biomedical applications. Curr. Opin. Chem. Eng. 2019, 24, 143–157. [Google Scholar] [CrossRef]
- Bakarich, S.E.; Balding, P.; Gorkin, R.; Spinks, G.M. Printed ioniccovalent entanglement hydrogels from carrageenan and an epoxy amine. RSC Adv. 2014, 4, 38088–38092. [Google Scholar] [CrossRef] [Green Version]
- Tan, H.; Marra, K.G. Injectable, Biodegradable Hydrogels for Tissue Engineering Applications. Materials 2010, 3, 1746–1767. [Google Scholar] [CrossRef]
- Peppas, N.A.; Hilt, J.Z.; Khademhosseini, A.; Langer, R. Hydrogels in biology and medicine: From molecular principles to bionanotechnology. Adv. Mater. 2006, 18, 1345–1360. [Google Scholar] [CrossRef]
- Weber, L.M.; Lopez, C.G.; Anseth, K.S. Effects of PEG hydrogel crosslinking density on protein diffusion and encapsulated islet survival and function. J. Biomed. Mater. Res. A 2009, 90, 720–729. [Google Scholar] [CrossRef] [Green Version]
- Fujioka-Kobayashi, M.; Ota, M.S.; Shimoda, A.; Nakahama, K.; Akiyoshi, K.; Miyamoto, Y.; Iseki, S. Cholesteryl group- and acryloyl group-bearing pullulan nanogel to deliver BMP2 and FGF18 for bone tissue engineering. Biomaterials 2012, 33, 7613–7620. [Google Scholar] [CrossRef]
- Shimoda, A.; Chen, Y.; Akiyoshi, K. Nanogel containing electrospun nanofibers as a platform for stable loading of proteins. RSC Adv. 2016, 6, 40811–40817. [Google Scholar] [CrossRef]
- Shimoda, A.; Sawada, S.-i.; Akiyoshi, K. Intracellular protein delivery using self-assembled amphiphilic polysaccharide nanogels. In Intracellular Delivery II: Fundamentals and Applications; Prokop, A., Iwasaki, Y., Harada, A., Eds.; Springer: Dordrecht, The Netherlands, 2014; pp. 265–274. [Google Scholar]
- Molinos, M.; Carvalho, V.; Silva, D.M.; Gama, F.M. Development of a Hybrid Dextrin Hydrogel Encapsulating Dextrin Nanogel As Protein Delivery Systems. Biomacromolecules 2012, 13, 517–527. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Lee, S.C.; Kwon, I.K.; Park, K. Hydrogels for delivery of bioactive agents: A historical perspective. Adv. Drug Deliv. Rev. 2013, 65, 17–20. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Buwalda, S.J.; Boere, K.W.; Dijkstra, P.J.; Feijen, J.; Vermonden, T.; Hennink, W.E. Hydrogels in a historical perspective: From simple networks to smart materials. J. Control. Release 2014, 190, 254–273. [Google Scholar] [CrossRef] [PubMed]
- Yom-Tov, O.; Neufeld, L.; Seliktar, D.; Bianco-Peled, H. A novel design of injectable porous hydrogels with in situ pore formation. Acta Biomater. 2014, 10, 4236–4246. [Google Scholar] [CrossRef] [PubMed]
- Abebe, D.G.; Fujiwara, T. Controlled thermoresponsive hydrogels by stereocomplexed PLA-PEG-PLAprepared via hybrid micelles of premixed copolymers with different PEG lengths. Biomacromolecules 2012, 13, 1828–1836. [Google Scholar] [CrossRef]
- Sefton, M.V.; May, M.H.; Lahooti, S.; Babensee, J.E. Making microencapsulation work: Conformal coating, immobilization gels and in vivo performance. J. Control. Release 2000, 65, 173–186. [Google Scholar] [CrossRef]
- Wang, L.; Guo, S.; Dong, J.; Cui, J.; Hao, J. Microgels in biomaterials and nanomedicines. Adv. Colloid Interface Sci. 2019, 266, 1–20. [Google Scholar] [CrossRef]
- Fu, L.-H.; Qi, C.; Ma, M.-G.; Wan, P. Multifunctional cellulose-based hydrogels for biomedical applications. J. Mater. Chem. B 2019, 7, 1541–1562. [Google Scholar] [CrossRef]
- Ismail, H.; Irani, M.; Ahmad, Z. Starch-based bydrogels: Present status and applications. Int. J. Polym. Mater. Polym. Biomat. 2013, 62, 411–420. [Google Scholar] [CrossRef]
- Sıvoli, L.; Perez, E.; Caraballo, D.; Rodrıguez, J.P.; Rodrıguez, D.; Moret, J.; Sojo, F.; Arvelo, F.; Tapia, M.; Colina, M.; et al. Cytocompatibility of a matrix of methylated cassava starch and chitosan. J. Cell Plast. 2013, 49, 507–520. [Google Scholar] [CrossRef]
- Kara, S.; Tamerler, C.; Bermek, H.; Pekcan, O. Cation effects on sol-gel and gel-sol phase transitions of κ-carrageenan-water system. Int. J. Biol. Macromol. 2003, 31, 177–185. [Google Scholar] [CrossRef]
- Osmałek, T.; Froelich, A.; Tasarek, S. Application of gellan gum in pharmacy and medicine. Int. J. Pharm. 2014, 466, 328–340. [Google Scholar] [CrossRef] [PubMed]
- Anirudhan, T.S.; Rejeena, S.R. Poly(acrylic acid-co-acrylamide-co-2-acrylamido-2-methyl-1-propanesulfonic acid)-grafted nanocellulose/poly(vinyl alcohol) composite for the in vitro gastrointestinal release of amoxicillin. J. Appl. Polym. Sci. 2014, 131, 40699. [Google Scholar] [CrossRef]
- Morales Hurtado, M.; de Vriesa, E.G.; Zeng, X.; van der Heide, E. A tribo-mechanical analysis of PVA-based building-blocks for implementation in a 2D-layered skin model. J. Mech. Behav. Biomed. Mater. 2016, 62, 319–332. [Google Scholar] [CrossRef] [PubMed]
- Jiang, P.; Li, G.; Lv, L.; Ji, H.; Li, Z.; Chen, S.; Chu, S. Effect of DMAEMA content and polymerization mode on morphologies and properties of pH and temperature double-sensitive cellulose-based hydrogels. J. Macromol. Sci. A 2020, 57, 207–216. [Google Scholar] [CrossRef]
- Yang, J.; Han, C.R. Mechanically viscoelastic properties of cellulose nanocrystals skeleton reinforced hierarchical composite hydrogels. ACS Appl. Mater. Interfaces 2016, 8, 25621–25630. [Google Scholar] [CrossRef]
- Chen, C.; Li, D.; Abe, K.; Yano, H. Formation of high strength double-network gels from cellulose nanofiber/polyacrylamide via NaOH gelation treatment. Cellulose 2018, 25, 5089–5097. [Google Scholar] [CrossRef]
- Huang, W.; Wang, Y.; McMullen, L.M.; McDermott, M.T.; Deng, H.; Du, Y.; Chen, L.; Zhang, L. Stretchable, tough, self-recoverable, and cytocompatible chitosan/cellulose nanocrystals/polyacrylamide hybrid hydrogels. Carbohyd. Polym. 2019, 222, 114977. [Google Scholar] [CrossRef]
- Pandey, M.; Mohamad, N.; Amin, M.C.I.M. Bacterial cellulose/acrylamide pH-sensitive smart hydrogel: Development, characterization, and toxicity studies in ICR mice model. Mol. Pharm. 2014, 11, 3596–3608. [Google Scholar] [CrossRef]
- Ahmad, N.; Amin, M.C.I.M.; Mahali, S.M.; Ismail, I.; Chuang, V.T.G. Biocompatible and mucoadhesive bacterial cellulose-g-poly(acrylic acid) for oral protein delivery. Mol. Pharm. 2014, 11, 4130–4142. [Google Scholar] [CrossRef] [PubMed]
- Mohd Amin, M.C.I.; Ahmad, N.; Pandey, M.; Jue Xin, C. Stimuli-responsive bacterial cellulose-g-poly(acrylic acid-co-acrylamide) hydrogels for oral controlled release drug delivery. Drug Dev. Ind. Pharm. 2014, 40, 1340–1349. [Google Scholar] [CrossRef] [PubMed]
- Hobzova, R.; Hrib, J.; Sirc, J.; Karpushkin, E.; Michalek, J.; Janouskova, O.; Gatenholm, P. Embedding of bacterial cellulose nanofibers within PHEMA hydrogel matrices: Tunable stiffness composites with potential for biomedical applications. J. Nanomater. 2018, 2018, 5217095. [Google Scholar] [CrossRef] [Green Version]
- Dai, L.; Fang, B.; Liang, C.; Zeng, R.; Tu, M.; Zhao, J. Preparation of bacterial cellulose/poly γ-glutamic acid composite hydrogels via 60Co γ-irradiation crosslinking and their properties. Polym. Mater. Sci. Eng. 2017, 33, 167–171. [Google Scholar] [CrossRef]
- Alosmanov, R.; Wolski, K.; Zapotoczny, S. Grafting of thermosensitive poly(N-isopropylacrylamide) from wet bacterial cellulose sheets to improve its swelling drying ability. Cellulose 2017, 24, 285–293. [Google Scholar] [CrossRef] [Green Version]
- Yang, J.Y.; Zhou, X.S.; Fang, J. Synthesis and characterization of temperature sensitive hemicellulose-based hydrogels. Carbohyd. Polym. 2011, 86, 1113–1117. [Google Scholar] [CrossRef]
- Bai, Y.; Zhang, Z.; Zhang, A.; Chen, L.; He, C.; Zhuang, X.; Chen, X. Novel thermo- and pH-responsive hydroxypropyl cellulose- and poly (l-glutamic acid)-based microgels for oral insulin controlled release. Carbohyd. Polym. 2012, 89, 1207–1214. [Google Scholar] [CrossRef]
- Li, Q.; Gong, J.; Zhang, J. Rheological properties and microstructures of hydroxyethyl cellulose/poly(acrylic acid) blend hydrogels. J. Macromol. Sci. B 2015, 54, 1132–1143. [Google Scholar] [CrossRef]
- Dutta, S.; Samanta, P.; Dhara, D. Temperature, pH and redox responsive cellulose based hydrogels for protein delivery. Int. J. Biol. Macromol. 2016, 87, 92–100. [Google Scholar] [CrossRef]
- Dahlan, N.A.; Pushpamalar, J.; Veeramachineni, A.K.; Muniyandy, S. Smart hydrogel of carboxymethyl cellulose grafted carboxymethyl polyvinyl alcohol and properties studied for future material applications. J. Polym. Environ. 2018, 26, 2061–2071. [Google Scholar] [CrossRef]
- Salama, A.; El-Sakhawy, M.; Kamel, S. Carboxymethyl cellulose based hybrid material for sustained release of protein drugs. Int. J. Biol. Macromol. 2016, 93, 1647–1652. [Google Scholar] [CrossRef] [PubMed]
- Lee, S.; Park, Y.H.; Ki, C.S. Fabrication of PEG-carboxymethyl cellulose hydrogel by thiol-norbornene photo-click Chemistry. Int. J. Biol. Macromol. 2016, 83, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Lee, S.Y.; Bang, S.; Kim, S.; Jo, S.Y.; Kim, B.-C.; Hwang, Y.; Noh, I. Synthesis and in vitro characterizations of porous carboxymethyl cellulose-poly(ethylene oxide) hydrogel film. Biomater. Res. 2015, 19, 12. [Google Scholar] [CrossRef] [Green Version]
- Bajpai, S.K.; Saxena, S. Enzymatically degradable and pH-sensitive hydrogels for colon-targeted oral drug delivery. I. Synthesis and characterization. J. Appl. Polym. Sci. 2004, 92, 3630–3643. [Google Scholar] [CrossRef]
- Zhang, X.; Zhuo, R. Synthesis of temperature-sensitive poly(N- isopropylacrylamide) hydrogel with improved surface property. J. Colloid Interface Sci. 2000, 223, 311–313. [Google Scholar] [CrossRef] [PubMed]
- Zhang, L.M.; Wang, G.H.; Lu, H.W. A new class of starch based hydrogels incorporating acrylamide and vinyl pyrrolidone: Effects of reaction variables on water sorption behavior. J. Bioact. Compat. Polym. 2005, 20, 2005. [Google Scholar] [CrossRef]
- Li, Y.; Liu, C.; Tan, Y.; Xu, K.; Lu, C.; Wang, P. In situ hydrogel constructed by starch-based nanoparticles via a Schiff base reaction. Carbohydr. Polym. 2014, 110, 87–94. [Google Scholar] [CrossRef]
- Geresh, S.; Gilboa, Y.; Peisahov-Korol, J.; Gdalevsky, G.; Voorspoels, J.; Remon, J.P.; Kost, J. Preparation and characterization of bioadhesive grafted starch copolymers as platforms for controlled drug delivery. J. Appl. Polym. Sci. 2002, 86, 1157–1162. [Google Scholar] [CrossRef]
- Zhai, M.; Yoshii, F.; Kume, T.; Hashim, K. Syntheses of PVA/Starch grafted hydrogels by irradiation. Carbohydr. Polym. 2002, 50, 295–303. [Google Scholar] [CrossRef]
- Bhuniya, S.P.; Rahman, S.; Satyanand, A.J.; Gharia, M.M.; Dave, A.M. Novel route to synthesis of allyl starch and biodegradable hydrogel by copolymerizing allyl-modified starch with methacrylic acid and acrylamide. J. Polym. Sci. A: Polym. Chem. 2003, 41, 1650–1658. [Google Scholar] [CrossRef]
- Saboktakin, M.R.; Maharramov, A.; Ramazanov, M.A. pH-sensitive starch hydrogels via free radical graft copolymerization, synthesis and properties. Carbohydr. Polym. 2009, 77, 634–638. [Google Scholar] [CrossRef]
- Seo, S.; Lee, C.S.; Jung, Y.S.; Na, K. Thermo-sensitivity and triggered drug release of polysaccharide nanogels derived from pullulan-g-poly(L-lactide) copolymers. Carbohydr. Polym. 2012, 87, 1105–1111. [Google Scholar] [CrossRef]
- Shitole, A.A.; Raut, P.W.; Khandwekar, A.; Sharma, N.; Baruah, M. Design and engineering of polyvinyl alcohol based biomimetic hydrogels for wound healing and repair. J. Polym. Res. 2019, 26, 201. [Google Scholar] [CrossRef]
- Baron, R.I.; Culica, M.E.; Biliuta, G.; Bercea, M.; Gherman, S.; Zavastin, D.; Ochiuz, L.; Avadanei, M.; Coseri, S. Physical hydrogels of oxidized polysaccharides and poly(vinyl alcohol) for wound dressing applications. Materials 2019, 12, 1569. [Google Scholar] [CrossRef] [Green Version]
- Masci, G.; Bontempo, D.; Crescenzi, V. Synthesis and characterization of thermoresponsive N-isopropylacrylamide/methacrylated pullulan hydrogels. Polymer 2002, 43, 5587–5593. [Google Scholar] [CrossRef]
- Asmarandei, I.; Fundueanu, G.; Cristea, M.; Harabagiu, V.; Constantin, M. Thermo- and pH sensitive interpenetrating poly(N-isopropylacrylamide)/carboxymethyl pullulan network for drug delivery. J. Polym. Res. 2013, 20, 293. [Google Scholar] [CrossRef]
- Morimoto, N.; Winnik, F.M.; Akiyoshi, K. Botryoidal assembly of cholesteryl−pullulan/poly(N-isopropylacrylamide) nanogels. Langmuir 2007, 23, 217–223. [Google Scholar] [CrossRef]
- Akiyoshi, K.; Kang, E.-C.; Kurumada, S.; Sunamoto, J.; Principi, T.; Winnik, F.M. Controlled association of amphiphilic polymers in water: Thermosensitive nanoparticles formed by self-assembly of hydrophobically modified pullulans and poly(Nisopropylacrylamides). Macromolecules 2000, 33, 3244–3249. [Google Scholar] [CrossRef]
- Hasegawa, U.; Sawada, S.; Shimizu, T.; Kishida, T.; Otsuji, E.; Mazda, O.; Akiyoshi, K. Raspberry-like assembly of cross-linked nanogels for protein delivery. J. Control. Release 2009, 140, 312–317. [Google Scholar] [CrossRef]
- Cinay, G.E.; Erkoc, P.; Alipour, M.; Hashimoto, Y.; Sasaki, Y.; Akiyoshi, K.; Kizilel, S. Nanogel-integrated pH responsive composite hydrogels for controlled drug delivery. ACS Biomater. Sci. Eng. 2017, 3, 370–380. [Google Scholar] [CrossRef]
- Hashimoto, Y.; Mukai, S.; Sawada, S.; Sasaki, Y.; Akiyoshi, K. Nanogel tectonic porous gel loading biologics, nanocarriers, and cells for advanced scaffold. Biomaterials 2015, 37, 107–115. [Google Scholar] [CrossRef] [Green Version]
- Liu, Y.; Zhu, Y.-Y.; Wei, G.; Lu, W.-Y. Effect of carrageenan on poloxamer-based in situ gel for vaginal use: Improved in vitro and in vivo sustained-release properties. Eur. J. Pharm. Sci. 2009, 37, 306–312. [Google Scholar] [CrossRef] [PubMed]
- Zhang, Y.; Ye, L.; Cui, M.; Yang, B.; Li, J.; Sun, H.; Yao, F. Physically crosslinked poly (vinyl alcohol)-carrageenan composite hydrogels: Pore structure stability and cell adhesive ability. RSC Adv. 2015, 5, 78180–78191. [Google Scholar] [CrossRef]
- Kawata, K.; Hanawa, T.; Endo, N.; Suzuki, M.; Oguchi, T. Formulation study on retinoic acid gel composed of iota-carrageenan, polyethylene oxide and Emulgen®408. Chem. Pharm. Bull. 2012, 60, 825–830. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Kulkarni, R.V.; Boppana, R.; Krishna Mohan, G.; Mutalik, S.; Kalyane, N.V. pH-responsive interpenetrating network hydrogel beads of poly(acrylamide)-g-carrageenan and sodium alginate for intestinal targeted drug delivery: Synthesis, in vitro and in vivo evaluation. J. Colloid Interface Sci. 2012, 367, 509–517. [Google Scholar] [CrossRef]
- Chan, A.H.; Boughton, P.C.; Ruys, A.J.; Oyen, M.L. An interpenetrating network composite for a regenerative spinal disc application. J. Mech. Behav. Biomed. Mater. 2017, 65, 842–848. [Google Scholar] [CrossRef] [Green Version]
- Chen, J.; Liu, M.; Jin, S.; Liu, H. Synthesis and characterization of κ- carrageenan/poly(N,N-diethylacrylamide) semi-interpenetrating polymer network hydrogels with rapid response to temperature. Polym. Adv. Technol. 2008, 17, 395–418. [Google Scholar] [CrossRef]
- Mohanan, A.; Vishalakshi, B.; Ganesh, S. Swelling and diffusion characteristics of stimuli-responsive N-isopropylacrylamide and κ-carrageenan semi-IPN hydrogels. Int. J. Polym. Mater. Polym. Biomat. 2011, 60, 787–798. [Google Scholar] [CrossRef]
- Deng, Y.; Huang, M.; Sun, D.; Hou, Y.; Li, Y.; Dong, T.; Wang, X.; Zhang, L.; Yang, W. Dual physically cross-linked κ-carrageenan-based double network hydrogels with superior self-healing performance for biomedical application. ACS Appl. Mater. Interfaces 2018, 10, 37544–37554. [Google Scholar] [CrossRef] [Green Version]
- Bardajee, G.R.; Hooshyar, Z.; Rastgo, F. Kappa carrageenan-g-poly (acrylic acid)/SPION nanocomposite as a novel stimuli-sensitive drug delivery system. Colloid Polym. Sci. 2013, 291, 2791–2803. [Google Scholar] [CrossRef]
- De Silva, D.A.; Hettiarachchi, B.U.; Nayanajith, L.D.C.; Milani, M.D.Y.; Motha, J.T.S. Development of a PVP / kappa-carrageenan / PEG hydrogel dressing for wound healing applications in Sri Lanka. J. Natl. Sci. Found. Sri Lanka 2011, 39, 25–33. [Google Scholar] [CrossRef]
- Bakarich, S.E.; Pidcock, G.C.; Balding, P.; Stevens, L.; Calvert, P.; Panhuis, M. Recovery from applied strain in interpenetrating polymer network hydrogels with ionic and covalent cross-links. Soft Matter 2012, 8, 9985–9988. [Google Scholar] [CrossRef]
- Kim, H.S.; Kim, D.; Jeong, Y.W.; Choi, M.J.; Lee, G.W.; Thangavelu, M.; Song, J.E.; Khang, G. Engineering retinal pigment epithelial cells regeneration for transplantation in regenerative medicine using PEG/Gellan gum hydrogels. Int. J. Biol. Macromol. 2019, 130, 220–228. [Google Scholar] [CrossRef] [PubMed]
- Li, W.; Wu, D.; Hu, D.; Zhu, S.; Pan, C.; Jiao, Y.; Li, L.; Luo, B.; Zhou, C.; Lu, L. Stress-relaxing double-network hydrogel for chondrogenic differentiation of stem cells. Mater. Sci. Eng.: C 2020, 107, 110333. [Google Scholar] [CrossRef] [PubMed]
- Choi, J.H.; Choi, O.K.; Lee, J.; Noh, J.; Lee, S.; Park, A.; Rim, M.A.; Reis, R.L.; Khang, G. Evaluation of double network hydrogel of poloxamer-heparin/gellan gum for bone marrow stem cells delivery carrier. Colloid Surf. B 2019, 181, 879–889. [Google Scholar] [CrossRef]
- Agnihotri, S.A.; Aminabhavi, T.M. Development of novel interpenetrating network gellan gum-poly(vinyl alcohol) hydrogel microspheres for the controlled release of carvedilol. Drug Dev. Ind. Pharm. 2005, 31, 491–503. [Google Scholar] [CrossRef]
- Hamcerencu, M.; Desbrieres, J.; Khoukh, A.; Popa, M.; Riess, G. Synthesis and characterization of new unsaturated esters of gellan gum. Carbohydr. Polym. 2008, 71, 92–100. [Google Scholar] [CrossRef]
- Hamcerencu, M.; Desbrieres, J.; Popa, M.; Riess, G. Thermo-sensitive gellan maleate/N-isopropylacrylamide hydrogels: Initial “in vitro” and “in vivo” evaluation as ocular inserts. Polym. Bull. 2020, 77, 741–755. [Google Scholar] [CrossRef]
- Sahraro, M.; Barikani, M.; Daemi, H. Mechanical reinforcement of Gellan gum polyelectrolyte hydrogels by cationic polyurethane soft nanoparticles. Carbohydr. Polym. 2018, 187, 102–109. [Google Scholar] [CrossRef]
- Wu, M.; Bao, B.; Yoshii, F.; Makuuchi, K. Irradiation of crosslinked, poly(vinyl alcohol) blended hydrogel for wound dressing. J. Radioanal. Nucl. Chem. 2001, 250, 391–395. [Google Scholar] [CrossRef]
- Dadoo, N.; Landry, S.B.; Bomar, J.D.; Gramlich, W.M. Synthesis and spatiotemporal modification of biocompatible and stimuli-responsive carboxymethyl cellulose hydrogels using thiol-norbornene chemistry. Macromol. Biosci. 2017, 17, 589–599. [Google Scholar] [CrossRef] [PubMed]
- Constantin, M.; Bucatariu, S.; Stoica, I.; Fundueanu, G. Smart nanoparticles based on pullulan-g-poly(N-isopropylacrylamide) for controlled delivery of indomethacin. Int. J. Biol. Macromol. 2017, 94, 698–708. [Google Scholar] [CrossRef] [PubMed]
- Jayaramudu, T.; Raghavendra, G.M.; Varaprasad, K.; Sadiku, R.; Ramam, K.; Raju, K.M. Iota-Carrageenan-based biodegradable Ag0 nanocomposite hydrogels for the inactivation of bacteria. Carbohydr. Polym. 2013, 95, 188–194. [Google Scholar] [CrossRef]
- Lee, K.Y.; Mooney, D.J. Alginate: Properties and biomedical applications. Prog. Polym. Sci. 2012, 37, 106–126. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Newsom, J.P.; Payne, K.A.; Krebs, M.D. Microgels: Modular, tunable constructs for tissue regeneration. Acta Biomater. 2019, 88, 32–41. [Google Scholar] [CrossRef] [PubMed]
- Piras, C.C.; Slavik, P.; Smith, D.K. Self-Assembling Supramolecular Hybrid Hydrogel Beads, Supramolecular Chemistry. Angew. Chem. Int. Ed. 2020, 59, 853–859. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Vieira, V.M.P.; Hay, L.L.; Smith, D.K. Multi-component hybrid hydrogels – understanding the extent of orthogonal assembly and its impact on controlled release. Chem. Sci. 2017, 8, 6981–6990. [Google Scholar] [CrossRef] [Green Version]
- Passemard, S.; Szabó, L.; Noverraz, F.; Montanari, E.; Gonelle-Gispert, C.; Bühler, L.H.; Wandrey, C.; Gerber-Lemaire, S. Synthesis Strategies to Extend the Variety of Alginate-Based Hybrid Hydrogels for Cell Microencapsulation. Biomacromolecules 2017, 18, 2747–2755. [Google Scholar] [CrossRef] [Green Version]
- Chaterji, S.; Kwon, I.K.; Park, K. Smart polymeric gels: Redefining the limits of biomedical devices. Prog. Polym. Sci. 2007, 32, 1083–1122. [Google Scholar] [CrossRef] [Green Version]
- Ahmadi, F.; Oveisi, Z.; Samani, M.; Amoozgar, Z. Chitosan based hydrogels: Characteristics and pharmaceutical applications. Res. Pharm. Sci. 2015, 10, 1–16. [Google Scholar]
- Chen, C.; Liu, L.; Huang, T.; Wang, Q.; Fang, Y.E. Bubble template fabrication of chitosan/poly(vinyl alcohol) sponges for wound dressing applications. Int. J. Biol. Macromol. 2013, 62, 188–193. [Google Scholar] [CrossRef]
- Fraser, J.R.E.; Laurent, T.C.; Laurent, U.B.G. Hyaluronan: Its nature, distribution, functions and turnover. J. Intern. Med. 1997, 242, 27–33. [Google Scholar] [CrossRef] [PubMed]
- Lam, J.; Truong, N.F.; Segura, T. Design of cell-matrix interactions in hyaluronic acid hydrogel scaffolds. Acta Biomater. 2014, 10, 1571–1580. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Kim, K.O.; Akada, Y.; Kai, W.; Kim, B.S.; Kim, I.S. Cells Attachment Property of PVA Hydrogel Nanofibers Incorporating Hyaluronic Acid for Tissue Engineering. J. Biomater. Nanobiotechnol. 2011, 2, 353–360. [Google Scholar] [CrossRef] [Green Version]
- Benoit, D.S.; Durney, A.R.; Anseth, K.S. The effect of heparin-functionalized PEG hydrogels on three-dimensional human mesenchymal stem cell osteogenic differentiation. Biomaterials 2007, 28, 66–77. [Google Scholar] [CrossRef]
- Slaughter, B.V.; Khurshid, S.S.; Fisher, O.Z.; Khademhosseini, A.; Peppas, N.A. Hydrogels in Regenerative Medicine. Adv. Mater. 2009, 21, 3307–3329. [Google Scholar] [CrossRef] [Green Version]
- Skilling, K.J.; Citossi, F.; Bradshaw, T.D.; Ashford, M.; Kellam, B.; Marlow, M. Insights into low molecular mass organic gelators: A focus on drug delivery and tissue engineering applications. Soft Matter 2014, 10, 237–256. [Google Scholar] [CrossRef]
- Cho, S.H.; Oh, S.H.; Lee, J.H. Fabrication and characterization of porous alginate/polyvinyl alcohol hybrid scaffolds for 3D cell culture. J. Biomater. Sci. Polym. Ed. 2005, 16, 933–947. [Google Scholar] [CrossRef]
- Kim, J.O.; Park, J.K.; Kim, J.H.; Jin, S.G.; Yonga, C.S.; Li, D.X.; Choi, J.Y.; Woo, J.S.; Yoo, B.K.; Lyoo, W.S.; et al. Development of polyvinyl alcohol–sodium alginate gel matrix-based wound dressing system containing nitrofurazone. Int. J. Pharm. 2008, 359, 79–86. [Google Scholar] [CrossRef]
- Kim, J.O.; Choi, J.Y.; Park, J.K.; Kim, J.H.; Jin, S.G.; Chang, S.W.; Li, D.X.; Hwang, M.-R.; Woo, J.S.; Kim, J.-A.; et al. Development of Clindamycin-Loaded Wound Dressing with Polyvinyl Alcohol and Sodium Alginate. Biol. Pharm. Bull. 2008, 31, 2277–2282. [Google Scholar] [CrossRef] [Green Version]
- Stone, S.A.; Gosavi, P.; Athauda, T.J.; Ozer, R.R. In situ citric acid crosslinking of alginate/polyvinyl alcohol electrospun nanofibers. Mater. Lett. 2013, 112, 32–35. [Google Scholar] [CrossRef]
- Tarun, K.; Gobi, N. Calcium alginate/PVA blended nano fiber matrix for wound dressing. Indian J. Fibre Text. Res. 2012, 37, 127–132. [Google Scholar]
- Kumar, A.; Negi, Y.S.; Choudhary, V.; Bhardwaj, N.K. Characterization of Cellulose Nanocrystals Produced by Acid-Hydrolysis from Sugarcane Bagasse as Agro-Waste. J. Mater. Phys. Chem. 2014, 2, 1–8. [Google Scholar]
- Kumar, A.; Lee, Y.; Kim, D.; Rao, K.M.; Kim, J.; Park, S.; Haider, A.; Lee, D.H.; Han, S.S. Effect of crosslinking functionality on microstructure, mechanical properties, and in vitro cytocompatibility of cellulose nanocrystals reinforced poly (vinyl alcohol)/sodium alginate hybrid scaffolds. Int. J. Biol. Macromol. 2017, 95, 962–973. [Google Scholar] [CrossRef] [PubMed]
- Anjum, F.; Lienemann, P.S.; Metzger, S.; Biernaskie, J.; Kallos, M.S.; Ehrbar, M. Enzyme responsive GAG-based natural-synthetic hybrid hydrogel for tunable growth factor delivery and stem cell differentiation. Biomaterials 2016, 87, 104–117. [Google Scholar] [CrossRef] [Green Version]
- Zhao, L.; Gwon, H.-J.; Lim, Y.-M.; Nho, Y.-C.; Kim, S.Y. Hyaluronic acid/chondroitin sulfate-based hydrogel prepared by gamma irradiation technique. Carbohydr. Polym. 2014, 102, 598–605. [Google Scholar] [CrossRef]
- Huang, X.; Brazel, C.S. Review On the importance and mechanisms of burst release in matrix-controlled drug delivery systems. J. Control. Release 2001, 73, 121–136. [Google Scholar] [CrossRef]
- El-Salmawi, K.M. Gamma radiation-induced crosslinked PVA/chitosan blends for wound dressing. J. Macromol. Sci. Part A: Pure Appl. Chem. 2007, 44, 541–545. [Google Scholar] [CrossRef]
- Yang, X.; Liu, Q.; Chen, X.; Yu, F.; Zhu, Z. Investigation of PVA/ws-chitosan hydrogels prepared by combined gama-irradiation and freeze–thawing. Carbohydr. Polym. 2008, 73, 401–408. [Google Scholar] [CrossRef]
- Yang, X.; Yang, K.; Wu, S.; Chen, X.; Yu, F.; Li, J.; Ma, M.; Zhu, Z. Cytotoxicity and wound healing properties of PVA/ws Chitosan/glycerol hydrogels made by irradiation followed by freeze–thawing. Radiat. Phys. Chem. 2010, 79, 606–611. [Google Scholar] [CrossRef]
- Jiang, Y.; Meng, X.; Wu, Z.; Qi, X. Modified chitosan thermosensitive hydrogel enables sustained and efficient anti-tumor therapy via intratumoral injection. Carbohydr. Polym. 2016, 144, 245–253. [Google Scholar] [CrossRef] [PubMed]
- Yang, J.M.; Su, W.Y.; Leu, T.L.; Yang, M.C. Evaluation of chitosan/PVA blended hydrogel membranes. J. Membr. Sci. 2004, 236, 39–51. [Google Scholar] [CrossRef]
- Sung, J.H.; Hwang, M.R.; Kim, J.O.; Lee, J.H.; Kim, Y.I.; Kim, J.H.; Change, S.W.; Jin, S.G.; Kim, J.A.; Lyoo, W.S.; et al. Gel characterization and in vivo evaluation of minocycline-loaded wound dressing with enhanced wound healing using polyvinyl alcohol and chitosan. Int. J. Pharm. 2010, 392, 232–240. [Google Scholar] [CrossRef] [PubMed]
- Zu, Y.; Zhang, Y.; Zhao, X.; Shan, C.; Zu, S.; Wang, K.; Li, Y.; Ge, Y. Preparation and Characterization of Chitosan–polyvinyl Alcohol Blend Hydrogels for the Controlled Release of Nano-Insulin. Int. J. Biol. Macromol. 2012, 50, 82–87. [Google Scholar] [CrossRef]
- Charernsriwilaiwat, N.; Rojanarata, T.; Ngawhirunpat, T.; Opanasopit, P. Electrospun Chitosan/polyvinyl Alcohol Nanofibre Mats for Wound Healing. Int. Wound J. 2014, 11, 215–222. [Google Scholar] [CrossRef]
- Shamloo, A.; Sarmadi, M.; Aghababaie, Z.; Vossoughi, M. Accelerated full-thickness wound healing via sustained bFGF delivery based on a PVA/chitosan/gelatin hydrogel incorporating PCL microspheres. Int. J. Pharm. 2018, 537, 278–289. [Google Scholar] [CrossRef]
- Fan, L.; Yang, H.; Yang, J.; Peng, M.; Hu, J. Preparation and Characterization of Chitosan/gelatin/PVA Hydrogel for Wound Dressings. Carbohydr. Polym. 2016, 146, 427–434. [Google Scholar] [CrossRef]
- Tsai, R.-Y.; Kuo, T.-Y.; Hung, S.-C.; Lin, C.-M.; Hsien, T.-Y.; Wang, D.-M.; Hsieh, H.-J. Use of Gum Arabic to Improve the Fabrication of Chitosan–gelatin-based Nanofibers for Tissue Engineering. Carbohydr. Polym. 2015, 115, 525–532. [Google Scholar] [CrossRef]
- Rodriguez-Rodriguez, R.; Garcia-Carvajal, Z.; Jimenez-Palomar, I.; Jimenez-Avalos, J.; Espinosa-Andrews, H. Development of Gelatin/chitosan/PVA Hydrogels: Thermal stability, water state, viscoelasticity, and cytotoxicity assays. J. Appl. Polym. Sci. 2018, 136, 47149. [Google Scholar] [CrossRef]
- Khan, F.; Tare, R.S.; Oreffo, R.O.C.; Bradley, M. Versatile biocompatible polymer hydrogels: Scaffolds for cell growth. Angew. Chem. Int. Ed. 2009, 48, 978–982. [Google Scholar] [CrossRef] [Green Version]
- Bhattarai, N.; Ramay, H.R.; Gunn, J.; Matsen, F.A.; Zhang, M.Q. PEG-grafted chitosan as an injectable thermosensitive hydrogel for sustained protein release. J. Control. Release 2005, 103, 609–624. [Google Scholar] [CrossRef] [PubMed]
- Bhattarai, N.; Gunn, J.; Zhang, M. Chitosan-based hydrogels for controlled, localized drug delivery. Adv. Drug Deliv. Rev. 2010, 62, 83–99. [Google Scholar] [CrossRef]
- Hong, Y.; Gong, Y.; Gao, C.; Shen, J. Collagen-coated polylactide microcarriers/chitosan hydrogel composite: Injectable scaffold for cartilage regeneration. J. Biomed. Mater. Res. Part A 2008, 85, 628–637. [Google Scholar] [CrossRef] [PubMed]
- Sadeghi, A.; Moztarzadeh, F.; Mohandesi, J.A. Investigating the effect of chitosan on hydrophilicity and bioactivity of conductive electrospun composite scaffold for neural tissue engineering. Int. J. Biol. Macromol. 2018, 121, 625–632. [Google Scholar] [CrossRef] [PubMed]
- Elcin, Y.M.; Dixit, V.; Gitnick, G. Hepatocyte attachment on biodegradable modified chitosan membranes: In vitro evaluation for the development of liver organoids. Artif. Organs 1998, 22, 837–846. [Google Scholar] [CrossRef]
- Zhao, L.; Mitomo, H.; Zhai, M.; Yoshii, F.; Nagasawa, N.; Kume, T. Synthesis of Antibacterial PVA/CM-chitosan Blend Hydrogels with Electron Beam Irradiation. Carbohydr. Polym. 2003, 53, 439–446. [Google Scholar] [CrossRef]
- Afshari, M.J.; Sheikh, N.; Afarideh, H. PVA/CM-chitosan/honey hydrogels prepared by using the combined technique of irradiation followed by freeze-thawing. Radiat. Phys. Chem. 2015, 113, 28–35. [Google Scholar] [CrossRef]
- Xiao, C.; Zhou, G. Synthesis and properties of degradable poly(vinyl alcohol) hydrogel. Polym. Degrad. Stab. 2003, 81, 297–301. [Google Scholar] [CrossRef]
- Ignatova, M.; Starbova, K.; Manolova, N.; Rashkov, I. Electrospun nano-fibre mats with antibacterial properties from quaternized chitosan and poly(vinyl alcohol). Carbohydr. Res. 2006, 341, 2098–2107. [Google Scholar] [CrossRef]
- Zhao, X.; Li, P.; Guo, B.; Ma, P.X. Antibacterial and conductive injectable hydrogels based on quaternized chitosan-graft-polyaniline/oxidized dextran for tissue engineering. Acta Biomater. 2015, 26, 236–248. [Google Scholar] [CrossRef]
- Fan, L.; Yang, J.; Wu, H.; Hu, Z.; Yi, J.; Tong, J.; Zhu, X. Preparation and Characterization of Quaternary Ammonium Chitosan Hydrogel with Significant Antibacterial Activity. Int. J. Biol. Macromol. 2015, 79, 830–836. [Google Scholar] [CrossRef] [PubMed]
- Kim, S.; Cui, Z.K.; Kim, P.J.; Jung, L.Y.; Lee, M. Design of hydrogels to stabilize and enhance bone morphogenetic protein activity by heparin mimetics. Acta Biomater. 2018, 72, 45–54. [Google Scholar] [CrossRef] [PubMed]
- Ding, C.X.; Liu, F.Y.; Cheng, J.; Gu, J.X.; Dan, S.; Liu, C.Y.; Qu, X.Z.; Yang, Z.Z. Dually responsive injectable hydrogel prepared by in situ cross-linking of glycol chitosan and benzaldehyde-capped PEO-PPO-PEO. Biomacromolecules 2010, 11, 1043–1051. [Google Scholar] [CrossRef] [PubMed]
- Park, K.M.; Lee, S.Y.; Joung, Y.K.; Na, J.S.; Lee, M.C.; Park, K.D. Thermosensitive chitosan–Pluronic hydrogel as an injectable cell delivery carrier for cartilage regeneration. Acta Biomater. 2009, 5, 1956–1965. [Google Scholar] [CrossRef] [PubMed]
- Kim, J.Y.; Choi, W.I.; Kim, Y.H.; Tae, G. Brain-targeted delivery of protein using chitosan- and RVG peptide-conjugated, pluronic-based nano-carrier. Biomaterials 2013, 34, 1170–1178. [Google Scholar] [CrossRef] [PubMed]
- Choi, J.S.; Yoo, H.S. Pluronic/chitosan hydrogels containing epidermal growth factor with wound-adhesive and photo-crosslinkable properties. J. Biomed. Mater. Res. Part A 2010, 95, 564–573. [Google Scholar] [CrossRef]
- Farahani, B.V.; Ghasemzaheh, H.; Afraz, S. Intelligent semi-IPN chitosan-PEG-PAAm hydrogel for closed-loop insulin delivery and kinetic modeling. RSC Adv. 2016, 6, 26590–26598. [Google Scholar] [CrossRef]
- Li, Q.; Williams, C.G.; Sun, D.D.N.; Wang, J.; Leong, K.; Elisseeff, J.H.J. Photocrosslinkable polysaccharides based on chondroitin sulfate. Biomed. Mater. Res. 2004, 68, 28–33. [Google Scholar] [CrossRef]
- Zhang, C.; Dong, Q.; Liang, K.; Zhou, D.; Yang, H.; Liu, X.; Xu, W.; Zhou, Y.; Xiao, P. Photopolymerizable thiol-acrylate maleiated hyaluronic acid/thiol-terminated poly(ethylene glycol) hydrogels as potential in-situ formable scaffolds. Int. J. Biol. Macromol. 2018, 119, 270–277. [Google Scholar] [CrossRef]
- Sharma, B.; Williams, C.G.; Khan, M.; Manson, P.; Elisseeff, J.H. In vivo Chondrogenesis of Mesenchymal Stem Cells in a Photopolymerized Hydrogel. Plast. Reconstr. Surg. 2007, 119, 112–120. [Google Scholar] [CrossRef]
- Bae, K.H.; Yoon, J.J.; Park, T.G. Fabrication of Hyaluronic Acid Hydrogel Beads for Cell Encapsulation. Biotechnol. Prog. 2006, 22, 297–302. [Google Scholar] [CrossRef] [PubMed]
- Vignesh, S.; Sivashanmugam, A.; Mohandas, A.; Janarthanan, R.; Iyer, S.; Nair, S.V.; Jayakumar, R. Injectable deferoxamine nanoparticles loaded chitosan–hyaluronic acid coacervate hydrogel for therapeutic angiogenesis. Colloids Surf. B Biointerfaces 2018, 161, 129–138. [Google Scholar]
- Na, K.; Kim, S.; Woo, D.G.; Sun, B.K.; Yang, H.N.; Chung, H.M.; Park, K.H. Combination material delivery of dexamethasone and growth factor in hydrogel blended with hyaluronic acid constructs for neocartilage formation. J. Biomed. Mater. Res. Part A 2007, 83, 779–786. [Google Scholar] [CrossRef] [PubMed]
- Leone, G.; Consumi, M.; Lamponi, S.; Bonechi, C.; Tamassi, G.; Donati, A.; Rossi, C.; Magnani, A. Hybrid PVA-xanthan gum hydrogels as nucleus pulposus substitutes. Int. J. Polym. Materi. Polym. Biomater. 2018, 68, 681–690. [Google Scholar] [CrossRef]
- Elizalde-Peña, E.A.; Zarate-Triviño, D.G.; Nuño-Donlucas, S.M.; Medina-Torres, L.; Gough, J.E.; Sanchez, I.C.; Villaseñor, F.; Luna-Barcenas, G. Synthesis and characterization of a hybrid (chitosan-g-glycidyl methacrylate)–xanthan hydrogel. J. Biomater. Sci. Polym. Ed. 2013, 24, 1426–1442. [Google Scholar] [CrossRef]
- Shah, S.S.; Kim, M.; Cahill-Thompson, K.; Tae, G.; Revzin, A. Micropatterning of bioactive heparin-based hydrogels. Soft Matter 2011, 7, 3133–3140. [Google Scholar] [CrossRef]
- Kim, M.; Shin, Y.; Hong, B.-H.; Kim, Y.-J.; Chun, J.-S.; Tae, G.; Kim, Y.H. In vitro Chondrocyte Culture in a Heparin-Based Hydrogel for Cartilage Regeneration. Tissue Eng. Part C: Meth. 2009, 16, 1–10. [Google Scholar] [CrossRef]
- Kim, M.; Lee, J.Y.; Jones, C.N.; Revzin, A.; Tae, G. Heparin-based hydrogel as a matrix for encapsulation and cultivation of primary hepatocytes. Biomaterials 2010, 31, 3596–3603. [Google Scholar] [CrossRef] [Green Version]
- Goh, M.C.; Hwang, Y.; Tae, G. Epidermal growth factor loaded heparin-based hydrogel sheet for skin wound healing. Carbohydr. Polym. 2016, 147, 251–260. [Google Scholar] [CrossRef]
- Xu, H.-L.; Tian, F.-R.; Xiao, J.; Chen, P.-P.; Xu, J.; Fan, Z.-L.; Yang, J.-J.; Lu, C.-T.; Zhao, Y.-Z. Sustained-release of FGF-2 from a hybrid hydrogel of heparin-poloxamer and decellular matrix promotes the neuroprotective effects of proteins after spinal injury. Int. J. Nanomed. 2018, 13, 681–694. [Google Scholar] [CrossRef] [Green Version]
- Ahmed, S.; Annu, A.A.; Sheikh, J. A review on chitosan centred scaffolds and their applications in tissue engineering. Int. J. Biol. Macromol. 2018, 116, 849–862. [Google Scholar] [CrossRef] [PubMed]
- Martins, J.G.; Camargo, S.E.A.; Bishop, T.T.; Popat, K.C.; Kipper, M.J.; Martins, A.F. Pectin-chitosan membrane scaffold imparts controlled stem cell adhesion and proliferation. Carbohydr. Polym. 2018, 197, 47–56. [Google Scholar] [CrossRef] [PubMed]
- Tiwari, S.; Patil, R.; Bahadur, P. Polysaccharide based scaffolds for soft tissue engineering applications. Polymers 2019, 11, 1. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Li, X.; Sun, Q.; Li, Q.; Kawazoe, N.; Chen, G. Functional Hydrogels With Tunable Structures and Properties for Tissue Engineering Applications. Front. Chem. 2018, 6, 499. [Google Scholar] [CrossRef] [Green Version]
- Qasim, S.B.; Husain, S.; Huang, Y.; Pogorielov, M.; Deineka, V.; Lyndin, M.; Rawlinson, A.; Rehman, I.U. In vitro and in vivo Degradation Studies of Freeze Gelated Porous Chitosan Composite Scaffolds for Tissue Engineering Applications. Polym. Degrad. Stab. 2017, 136, 31–38. [Google Scholar] [CrossRef]
- Pok, S.; Myers, J.D.; Madihally, S.V.; Jacot, J.G. A multilayered scaffold of a chitosan and gelatin hydrogel supported by a PCL core for cardiac tissue engineering. Acta Biomater. 2013, 9, 5630–5642. [Google Scholar] [CrossRef] [Green Version]
- Negishi, J.; Nam, K.; Kimura, T.; Hashimoto, Y.; Funamoto, S.; Higami, T.; Fujisato, S.; Kishida, A. Fabrication of a heparin–PVA complex hydrogel for application as a vascular access. J. Biomed. Mater. Res. B Appl. Biomater. 2014, 102, 1426–1433. [Google Scholar] [CrossRef]
- Homandberg, G.A.; Hui, F.; Wen, C.; Kuettner, K.E.; Williams, J.M. Hyaluronic acid suppresses fibronectin fragment mediated cartilage chondrolysis: I. In vitro. Osteoarthr. Cartil. 1997, 5, 309–319. [Google Scholar] [CrossRef] [Green Version]
- Shimazu, A.; Jikko, A.; Iwamoto, M.; Koike, T.; Yan, W.; Okada, Y.; Shinmei, M.; Nakamura, S.; Kato, Y. Effects of hyaluronic acid on the release of proteoglycan from the cell matrix in rabbit chondrocyte cultures in the presence and absence of cytokines. Arthritis Rheum. 1993, 36, 247–253. [Google Scholar] [CrossRef]
- Morris, E.A.; Wilcon, S.; Treadwell, B.V. Inhibition of interleukin 1-mediated proteoglycan degradation in bovine articular cartilage explants by addition of sodium hyaluronate. Am. J. Vet. Res. 1992, 53, 1977–1982. [Google Scholar]
- Balakrishnan, B.; Banerjee, R. Biopolymer-Based Hydrogels for Cartilage Tissue Engineering. Chem. Rev. 2011, 111, 4453–4474. [Google Scholar] [CrossRef] [PubMed]
- Fan, H.; Hu, Y.; Zhang, C.; Li, X.; Lv, R.; Qin, L.; Zhu, R. Cartilage regeneration using mesenchymal stem cells and a PLGA-gelatin/chondroitin/hyaluronate hybrid scaffold. Biomaterials 2006, 27, 4573–4580. [Google Scholar] [CrossRef] [PubMed]
- Bichara, D.A.; Zhao, X.; Hwang, N.S.; Bodugoz-Senturk, H.; Yaremchuk, M.J.; Randolph, M.A.; Muratoglu, O.K. Porous Poly(vinyl alcohol)-Alginate Gel Hybrid Construct for Neocartilage Formation Using Human Nasoseptal Cells. J. Surg. Res. 2010, 163, 331–336. [Google Scholar] [CrossRef] [PubMed]
- Kunisch, E.; Knauf, A.-K.; Hesse, E.; Freudenberg, U.; Werner, C.; Bothe, F. StarPEG/heparin-hydrogel based in vivo engineering of stable bizonal cartilage with a calcified bottom layer. Biofabrication 2018, 11, 015001. [Google Scholar] [CrossRef] [PubMed]
- Tan, H.; Ramirez, C.M.; Miljkovic, N.; Li, H.; Rubin, J.P.; Marra, K.G. Thermosensitive injectable hyaluronic acid hydrogel for adipose tissue engineering. Biomaterials 2009, 30, 6844–6853. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Lin, Y.-K.; Chen, K.-H.; Kuan, C.-Y. The synthesis and characterization of a thermally responsive hyaluronic acid/Pluronic copolymer and an evaluation of its potential as an artificial vitreous substitute. J. Bioact. Compat. Pol. 2013, 28, 355–367. [Google Scholar] [CrossRef]
- Liu, Y.; Hsu, S. Synthesis and Biomedical Applications of Self-healing Hydrogels. Front. Chem. 2018, 6, 449. [Google Scholar] [CrossRef] [Green Version]
- Tseng, T.C.; Tao, L.; Hsieh, F.Y.; Wei, Y.; Chiu, I.M.; Hsu, S.H. An injectable, self-healing hydrogel to repair the central nervous system. Adv. Mater. 2015, 27, 3518–3524. [Google Scholar] [CrossRef]
- Hsieh, F.-Y.; Tao, L.; Wei, Y.; Hsu, S.H. A novel biodegradable self healing hydrogel to induce blood capillary formation. Npg Asia Mater. 2017, 9, e363. [Google Scholar] [CrossRef] [Green Version]
- Fares, M.M.; Sani, E.S.; Lara, R.P.; Oliveira, R.B.; Khademhosseini, A.; Annabi, N. Interpenetrating network gelatin methacryloyl (GelMA) and pectin-g-PCL hydrogels with tunable properties for tissue engineering. Biomater. Sci. 2018, 6, 2938–2950. [Google Scholar] [CrossRef] [Green Version]
- Niu, R.; Qin, Z.; Ji, F.; Xu, M.; Tian, X.; Li, J.; Yao, F. Hybrid pectin-Fe3+/polyacrylamide double network hydrogels with excellent strength, high stiffness, superior toughness and notch-insensitivity. Soft Matter 2017, 13, 9237–9245. [Google Scholar] [CrossRef] [PubMed]
- Temenoff, J.S.; Mikos, A.G. Injectable biodegradable materials for orthopedic tissue engineering. Biomaterials 2000, 21, 2405–2412. [Google Scholar] [CrossRef]
- Khunmanee, S.; Jeong, Y.; Park, H. Crosslinking method of hyaluronic-based hydrogel for biomedical applications. J. Tissue Eng. 2017, 8, 1–16. [Google Scholar] [CrossRef] [Green Version]
- Liu, M.; Zeng, X.; Ma, C.; Yi, H.; Ali, Z.; Mou, X.; Li, S.; Deng, Y.; He, N. Injectable hydrogels for cartilage and bone tissue engineering. Bone Res. 2017, 5, 17014. [Google Scholar] [CrossRef] [PubMed]
- Chircov, C.; Grumezescu, A.M.; Bejenaru, L.E. Hyaluronic acid-based scaffolds for tissue engineering. Rom. J. Morphol. Embryol. 2018, 59, 71–76. [Google Scholar] [PubMed]
- Baican, M.; Vasile, C. Chitosan containing biomaterials for tissue engineering applications. In Advances in Polymers for Biomedical Applications; Deepak, P., Bhuvanesh, G., Eds.; Nova Science Publishers, Inc.: Hauppauge, NY, USA, 2018; pp. 221–279. [Google Scholar]
- Jayakumar, R.; Prabaharan, M.; Sudheesh Kumar, P.T.; Nair, S.V.; Tamura, H. Biomaterials based on chitin and chitosan in wound dressing applications. Biotechnol. Adv. 2011, 29, 322–337. [Google Scholar] [CrossRef] [PubMed]
- Fahmy, A.; Kamoun, E.A.; El-Eisawy, R.; El-Fakharany, E.M.; Taha, T.H.; El-Damhougy, B.K.; Abdelhai, F. Poly(vinyl alcohol)-hyaluronic acid membranes for wound dressing applications: Synthesis and in vitro bio-evaluations. J. Braz. Chem. Soc. 2015, 26, 1466–1474. [Google Scholar] [CrossRef]
- Phuc, D.H.; Hiep, N.T.; Phuc Chau, N.D.; Hoai, N.T.T.; Khon, H.C.; Toi, V.V.; Hai, N.D.; Bao, B.C. Fabrication of hyaluronan-poly(vinylphosphonic acid)-chitosan hydrogel for wound healing application. Int. J. Polym. Sci. 2016, 2016, 6723716. [Google Scholar]
- Hoffman, A.S. Hydrogels for biomedical applications. Adv. Drug Deliv. Rev. 2002, 54, 3–12. [Google Scholar] [CrossRef]
- Hamedi, H.; Moradi, S.; Hudson, S.M.; Tonelli, A.E. Chitosan based hydrogels and their applications for drug delivery in wound dressings: A review. Carbohydr. Polym. 2018, 199, 445–460. [Google Scholar] [CrossRef]
- Wu, J.; Wei, W.; Wang, L.Y.; Su, Z.G.; Ma, G.H. A thermosensitive hydrogel based on quaternized chitosan and poly(ethylene glycol) for nasal drug delivery system. Biomaterials 2007, 28, 2220–2232. [Google Scholar] [CrossRef] [PubMed]
- Dyer, A.M.; Hinchcliffe, M.; Watts, P.; Castile, J.; Jabbal-Gill, I.; Nankervis, R.; Smith, A.; Illum, L. Nasal delivery of insulin using novel chitosan based formulations: A comparative study in two animal models between simple chitosan formulations and chitosan nanoparticles. Pharm. Res. 2002, 19, 998–1008. [Google Scholar] [CrossRef] [PubMed]
- Buranachai, T.; Praphairaksit, N.; Muangesin, N. Chitosan/polyethylene glycol beads crosslinked with tripolyphosphate and glutaraldehyde for gasterointestinal drug delivery. AAPS Pharm. Sci. Tech. 2010, 11, 1128–1137. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Hassani, N.A.; Abdouss, M.; Faghihi, S. Synthesis and evaluation of PEG-O-chitosan nanoparticles for delivery of poor water soluble drugs: Lbuprofen. Mater. Sci. Eng. C Mater. Biol. Appl. 2014, 41, 91–99. [Google Scholar] [CrossRef] [PubMed]
- Ito, T.; Yoshida, C.; Murakami, Y. Design of novel sheet-shaped chitosan hydrogel for wound healing: A hybrid biomaterial consisting of both PEG-grafted chitosan and crosslinkable polymeric micelles acting as drug containers. Mater. Sci. Eng. C Mater. Biol. Appl. 2013, 33, 3697–3703. [Google Scholar] [CrossRef] [PubMed]
- Chan, P.; Kurisawa, M.; Chung, J.E.; Yang, Y.Y. Synthesis and characterization of chitosan-g-poly (ethylene glycol)-folate as a non-viral carrier for tumor-targeted gene delivery. Biomaterials 2007, 28, 540–549. [Google Scholar] [CrossRef]
- Patel, V.; Amiji, M. Preparation and characterization of freeze-dried chitosan-poly (ethylene oxide) hydrogels for site-specific antibiotic delivery in the stomach. Pharm. Res. 1996, 13, 588–593. [Google Scholar] [CrossRef]
- Gong, S.; Tu, H.; Zheng, H.; Xu, H.; Yin, Y. Chitosan-g-PAA hydrogels for colon-specific drug delivery: Preparation, swelling behavior and in vitro degradability. J. Wuhan Univ. Technol. Mater. Sci. Ed. 2010, 25, 248–251. [Google Scholar] [CrossRef]
- Zhou, T.; Xiao, C.; Fan, J.; Chen, S.; Shen, J.; Wu, W.; Zhou, S. A nanogel of on-site tunable pH-response for efficient anticancer drug delivery. Acta Biomater. 2013, 9, 4546–4557. [Google Scholar] [CrossRef]
- Åhlén, M.; Tummala, G.K.; Mihranyan, A. Nanoparticle-loaded hydrogels as a pathway for enzymetriggered drug release in ophthalmic applications. Int. J. Pharm. 2018, 536, 73–81. [Google Scholar]
- Jamal, A.; Shahzadi, L.; Ahtzaz, S.; Zahid, S.; Chaudhry, A.A.; Rehman, I.U.; Yar, M. Identification of anti-cancer potential of doxazocin: Loading into chitosan based biodegradable hydrogels for on-site delivery to treat cervical cancer. Mater. Sci. Eng. C. Mater. Biol. Appl. 2018, 82, 102–109. [Google Scholar] [CrossRef] [PubMed]
- Islam, A.; Yasin, T. Controlled Delivery of Drug from pH Sensitive Chitosan/poly (vinyl Alcohol) Blend. Int. J. Biol. Macromol. 2012, 88, 1055–1060. [Google Scholar] [CrossRef]
- Yang, L.; Li, Y.S.; Gou, Y.Z.; Wang, X.; Zhao, X.M.; Tao, L. Improving tumor chemotherapy effect using an injectable self-healing hydrogel as drug carrier. Polym. Chem. 2017, 8, 3071–3076. [Google Scholar] [CrossRef]
- Wang, J.Y.; Wang, D.; Yan, H.; Tao, L.; Wei, Y.; Li, Y.; Wang, X.; Zhao, W.; Zhang, Y.; Zhao, L.; et al. An injectable ionic hydrogel inducing high temperature hyperthermia for microwave tumor ablation. J. Mater. Chem. B 2017, 5, 4110–4120. [Google Scholar] [CrossRef]
- Luckanagul, J.A.; Pitakchatwong, C.; Bhuket, P.R.N.; Muangnoi, C.; Rojsitthisak, P.; Chirachanchai, S.; Wang, Q.; Rojsitthisak, P. Chitosan-based polymer hybrids for thermo-responsive nanogel delivery of curcumin. Carbohydr. Polym. 2018, 181, 1119–1127. [Google Scholar] [CrossRef]
- Luo, Z.; Xue, K.; Zhang, X.; Lim, J.Y.C.; Lai, X.; Young, D.J.; Zhang, Z.-X.; Wu, Y.-L.; Loh, X.J. Thermogelling chitosan-based polymers for the treatment of oral mucosa ulcers. Biomater. Sci. 2020, 8, 1364–1379. [Google Scholar] [CrossRef] [PubMed]
- Lee, J.; Cha, M.-J.; Lim, K.S.; Kim, J.-K.; Lee, S.-K.; Kim, Y.-H.; Hwang, K.-C.; Lee, K.Y. Injectable microsphere/hydrogel hybrid system containing heat shock protein as therapy in a murine myocardial infarction model. J. Drug Target. 2013, 21, 822–829. [Google Scholar] [CrossRef] [PubMed]
- Dumitriu, R.P.; Oprea, A.M.; Vasile, C. A drug delivery system based on stimuli-responsive alginate/N-isopropylacryl amide hydrogel. Cell. Chem. Technol. 2009, 43, 251–262. [Google Scholar]
- Chen, Y.-Y.; Wu, H.-C.; Sun, J.-S.; Dong, G.-C.; Wang, T.-W. Injectable and thermoresponsive self-assembled nanocomposite hydrogel for long-term anticancer drug delivery. Langmuir 2013, 29, 3721–3729. [Google Scholar] [CrossRef]
- Fujita, S.; Hara, S.; Hosono, A.; Sugihara, S.; Uematsu, H.; Suye, S. Hyaluronic Acid Hydrogel Crosslinked with Complementary DNAs. Hindawi Adv. Polym. Technol. 2020, 2020, 1470819. [Google Scholar] [CrossRef]
- Roberts, J.J.; Farrugia, B.L.; Green, R.A.; Kovacina, J.R.; Martens, P.J. In situ formation of poly(vinyl alcohol)–heparin hydrogels for mild encapsulation and prolonged release of basic fibroblast growth factor and vascular endothelial growth factor. J. Tissue Eng. 2016, 7, 1–10. [Google Scholar] [CrossRef] [PubMed]
- He, C.; Ji, H.; Qian, Y.; Wang, Q.; Liu, X.; Zhao, W.; Zhao, C. Heparin-based and heparin-inspired hydrogels: Size-effect, gelation and biomedical applications. J. Mater. Chem. B 2019, 7, 1186–1208. [Google Scholar] [CrossRef]
- Li, J.; Chen, G.; Xu, X.; Abdou, P.; Jiang, Q.; Shi, D.; Gu, Z. Advances of injectable hydrogel-based scaffolds for cartilage regeneration. Regen. Biomater. 2019, 129–140. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Ma, X.; Sun, X.; Chen, J.; Lei, Y. Natural or Natural-Synthetic Hybrid Polymer-Based Fluorescent Polymeric Materials for Bio-imaging-Related Applications. Appl. Biochem. Biotechnol. 2017, 183, 461–487. [Google Scholar] [CrossRef] [PubMed]
- Liu, Z.; Tang, Z.; Zhu, L.; Lu, S.; Chen, F.; Tang, C.; Sun, H.; Yang, J.; Qin, G.; Chen, Q. Natural protein-based hydrogels with high strength and rapid self-recovery. Int. J. Biol. Macromol. 2019, 141, 108–116. [Google Scholar] [CrossRef] [PubMed]
- Chen, J.; Cai, Z.; Wei, Q.; Wang, D.; Wu, J.; Tan, Y.; Lu, J.; Ai, H. Proanthocyanidin-crosslinked collagen/konjac glucomannan hydrogel with improved mechanical properties and MRI trackable biodegradation for potential tissue engineering scaffolds. Mater. Chem. B 2020, 8, 316–331. [Google Scholar] [CrossRef]
- Eslahi, N.; Simchi, A.; Mehrjoo, M.; Shokrgozar, M.A.; Bonakdar, S. Hybrid cross-linked hydrogels based on fibrous protein/block copolymers and layered silicate nanoparticles: Tunable thermosensitivity, biodegradability and mechanical durability. RSC Adv. 2016, 6, 62944. [Google Scholar] [CrossRef]
- Pamfil, D.; Schick, C.; Vasile, C. New Hydrogels Based on Substituted Anhydride Modified Collagen and 2-Hydroxyethyl Methacrylate. Synthesis and Characterization. Ind. Eng. Chem. Res. 2014, 53, 11239–11248. [Google Scholar] [CrossRef]
- Lotz, C.; Schmid, F.F.; Oechsle, E.; Monaghan, M.; Walles, H.; Groeber-Becker, F.K. A Crosslinked Collagen Hydrogel Matrix Resisting Contraction to Facilitate Full-thickness Skin Equivalents. ACS Appl. Mater. Interfaces 2017, 9, 20417–20425. [Google Scholar] [CrossRef]
- Dinescu, S.; Albu Kaya, M.; Chitoiu, L.; Ignat, S.; Kaya, D.A.; Costache, M. Collagen-Based Hydrogels and Their Applications for Tissue Engineering and Regenerative Medicine. In Cellulose-Based Superabsorbent Hydrogels. Polymers and Polymeric Composites: A Reference Series; Mondal, M., Ed.; Springer International Publishing: Cham, Switzerland, 2018. [Google Scholar]
- Ucar, B.; Humpel, C. Collagen for brain repair: Therapeutic perspectives. Neural. Regen. Res. 2018, 13, 595–598. [Google Scholar] [CrossRef]
- Gómez-Guillén, M.C.; Giménez, B.; López-Caballero, M.E.; Montero, M.P. Functional and bioactive properties of collagen and gelatin from alternative sources: A review. Food Hydrocoll. 2011, 25, 1813–1827. [Google Scholar] [CrossRef] [Green Version]
- Farris, S.; Song, J.; Huang, Q. Alternative Reaction Mechanism for the Cross-Linking of Gelatin with Glutaraldehyde. J. Agric. Food Chem. 2010, 58, 998–1003. [Google Scholar] [CrossRef]
- Nagarajan, S.; Radhakrishnan, S.; Kalkura, S.N.; Balme, S.; Miele, P.; Bechelany, M. Overview of Protein-Based Biopolymers for Biomedical Application. Macromol. Chem. Phys. 2019, 220, 1900126. [Google Scholar] [CrossRef]
- Ni, N.; Dumont, M.-J. Protein-Based Hydrogels Derived from Industrial Byproducts Containing Collagen, Keratin, Zein and Soy. Waste Biomass Valor. 2017, 8, 285–300. [Google Scholar] [CrossRef]
- Neves, N.M.; Reis, R.L. Biomaterials from Nature for Advanced Devices and Therapies; John Wiley & Sons, Inc.: Hoboken, NJ, USA, 2016. [Google Scholar]
- de Guzman, R.C.; Merrill, M.R.; Richter, J.R.; Hamzi, R.I.; Greengauz-Roberts, O.K.; Van Dyke, M.E. Mechanical and biological properties of keratose biomaterials. Biomaterials 2011, 32, 8205–8217. [Google Scholar] [CrossRef] [PubMed]
- Cohen, D.J.; Hyzy, S.L.; Haque, S.; Olson, L.C.; Boyan, B.D.; Saul, J.M.; Schwartz, Z. Effects of Tunable Keratin Hydrogel Erosion on rhBMP-2 Release, Bioactivity, and Bone Induction. Tissue Eng. Part A 2018, 24, 1616–1630. [Google Scholar] [CrossRef] [PubMed]
- Kumaran, P.; Gupta, A.; Sharma, S. Synthesis of wound-healing keratin hydrogels using chicken feathers proteins and its properties. Int. J. Pharm. Sci. 2017, 9, 171–178. [Google Scholar] [CrossRef] [Green Version]
- Ma, X.; Sun, X.; Hargrove, D.; Chen, J.; Song, D.; Dong, Q.; Lu, X.; Fan, T.; Fu, Y.; Lei, Y. A Biocompatible and Biodegradable Protein Hydrogel with Green and Red Autofluorescence: Preparation, Characterization and In vivo Biodegradation Tracking and Modeling. Sci. Rep. 2016, 6, 19370. [Google Scholar] [CrossRef]
- Pandey, V.; Haider, T.; Jain, P.; Gupta, P.N.; Soni, V. Silk as a leading-edge biological macromolecule for improved drug delivery. J. Drug Deliv. Sci. Technol. 2020, 55, 101294. [Google Scholar] [CrossRef]
- Liu, B.; Song, Y.W.; Jin, L.; Wang, Z.J.; Pu, D.Y.; Lin, S.Q.; Zhou, C.; You, H.J.; Ma, Y.; Li, J.M.; et al. Silk structure and degradation. Colloids Surf. B Biointerfaces 2015, 131, 122–128. [Google Scholar] [CrossRef] [Green Version]
- Li, Z.; Song, J.; Zhang, J.; Hao, K.; Liu, L.; Wu, B.; Zheng, X.; Xiao, B.; Tong, X.; Dai, F. Topical application of silk fibroin-based hydrogel in preventing hypertrophic scars. Colloids Surf. B Biointerfaces 2020, 185, 110735. [Google Scholar] [CrossRef] [PubMed]
- Yin, Z.; Wu, F.; Xing, T.; Yadavalli, V.K.; Kunduc, S.C.; Lu, S. A silk fibroin hydrogel with reversible sol–gel transition. RSC Adv. 2017, 7, 24085. [Google Scholar] [CrossRef] [Green Version]
- Xu, M. Development of protein based hydrogels as encapsulation matrices for Lactobacillus casei ATCC 393. Master’s Thesis, McGill University, Macdonald Campus, Montreal, QC, Canada, 2015. Available online: https://escholarship.mcgill.ca/concern/theses/c247dw09t?locale=en (accessed on 24 February 2020).
- Nagarkar, S.; Nicolai, T.; Chassenieux, C.; Lele, A. Structure and gelation mechanism of silk hydrogels. Phys. Chem. Chem. Phys. 2010, 12, 3834–3844. [Google Scholar] [CrossRef] [PubMed]
- Abascal, N.C.; Regan, L. The past, present and future of protein based materials. Open Biol. 2018, 8, 180113. [Google Scholar] [CrossRef] [Green Version]
- Wong, D.C.; Pearson, R.D.; Elvin, C.M.; Merritt, D.J. Expression of the rubber-like protein, resilin, in developing and functional insect cuticle determined using a Drosophila anti-rec 1 resilin antibody. Dev. Dyn. 2012, 241, 333–339. [Google Scholar] [CrossRef]
- de Castro, R.J.S.; Domingues, M.A.F.; Ohara, A.; Okuro, P.K.; dos Santos, J.G.; Brexó, R.P.; Sato, H.H. Whey protein as a key component in food systems: Physicochemical properties, production technologies and applications. Food Struct. 2017, 14, 17–29. [Google Scholar] [CrossRef]
- Tansaz, S.; Boccaccini, A.R. Biomedical applications of soy protein: A brief overview. Mater. Res. Part A 2016, 104, 553–569. [Google Scholar] [CrossRef]
- Tian, K.; Shao, Z.; Chen, X. Natural electroactive hydrogel from soy protein isolation. Biomacromolecules 2010, 11, 3638–3643. [Google Scholar] [CrossRef]
- Lin, H.; Hsieh, F.; Tseng, C.; Hsu, S. Preparation and characterization of biodegradable polyurethane hydrogel and the hybrid gel with soy protein for 3D cell-laden bioprinting. J. Mater. Chem. B 2016, 4, 6694–6705. [Google Scholar] [CrossRef]
- Meikle, S.T.; Standen, G.; Salvage, J.; De Santis, R.; Nicolais, L.; Ambrosio, L.; Santin, M. Synthesis and Characterization of Soybean-Based Hydrogels with an Intrinsic Activity on Cell Differentiation. Tissue Eng. Part A 2012, 18, 1932–1939. [Google Scholar] [CrossRef]
- Ali, A.; Ahmed, S. Recent Advances in Edible Polymer Based Hydrogels as a Sustainable Alternative to Conventional Polymers. J. Agric. Food Chem. 2018, 66, 6940–6967. [Google Scholar] [CrossRef] [PubMed]
- Li, H.; Kong, N.; Laver, B.; Liu, J. Hydrogels Constructed from Engineered Proteins. Small 2016, 12, 973–987. [Google Scholar] [CrossRef] [PubMed]
- Cook, W.J.; Walter, L.J.; Walter, M.R. Drug binding by calmodulin: Crystal structure of a calmodulin-trifluoperazine complex. Biochemistry 1994, 33, 15259–15265. [Google Scholar] [CrossRef] [PubMed]
- Daamen, W.F.; Hafmans, T.; Veerkamp, J.H.; van Kuppevelt, T.H. Comparison of five procedures for the purification of insoluble elastin. Biomaterials 2001, 22, 1997–2005. [Google Scholar] [CrossRef]
- Mithieux, S.M.; Rasko, J.E.J.; Weiss, A.S. Synthetic elastin hydrogels derived from massive elastic assemblies of self-organized human protein monomers. Biomaterials 2004, 25, 4921–4927. [Google Scholar] [CrossRef]
- Leach, J.B.; Wolinsky, J.B.; Stone, P.J.; Wong, J.Y. Crosslinked alpha-elastin biomaterials: Towards a processable elastin mimetic scaffold. Acta Biomater. 2005, 1, 155–164. [Google Scholar] [CrossRef]
- Lim, D.W.; Nettles, D.L.; Setton, L.A.; Chilkoti, A. In situ cross-linking of elastin-like polypeptide block copolymers for tissue repair. Biomacromolecules 2008, 9, 222–230. [Google Scholar] [CrossRef] [Green Version]
- Haider, M.; Megeed, Z.; Ghandehari, H. Genetically engineered polymers: Status and prospects for controlled release. J. Control. Release 2004, 95, 1–26. [Google Scholar] [CrossRef]
- Petka, W.A.; Harden, J.L.; McGrath, K.P.; Wirtz, D.; Tirrell, D.A. Reversible hydrogels from self-assembling artificial proteins. Science 1998, 281, 389–392. [Google Scholar] [CrossRef]
- Banta, S.; Wheeldon, I.R.; Blenner, M. Protein Engineering in the Development of Functional Hydrogels. Annu. Rev. Biomed. Eng. 2010, 12, 167–186. [Google Scholar] [CrossRef] [Green Version]
- Cao, Y.; Li, H. Engineering tandem modular protein based reversible hydrogels. Chem. Commun. 2008, 4144–4146. [Google Scholar] [CrossRef] [PubMed]
- Huang, C.; Ravindran, S.; Yin, Z.; George, A. 3-D self-assembling leucine zipper hydrogel with tunable properties for tissue engineering. Biomaterials 2014, 35, 5316–5326. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Shu, J.Y.; Tan, C.; DeGrado, W.F.; Xu, T. New design of helix bundle peptide-polymer conjugates. Biomacromolecules 2008, 9, 2111–2117. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Posritong, S.; Flores Chavez, R.; Chu, T.G.; Bruzzaniti, A. A Pyk2 inhibitor incorporated into a PEGDA-gelatin hydrogel promotes osteoblast activity and mineral deposition. Biomed. Mater. 2019, 14, 025015. [Google Scholar] [CrossRef]
- Wang, Y.; Ma, M.; Wang, J.; Zhang, W.; Lu, W.; Gao, Y.; Zhang, B.; Guo, Y. Development of a Photo-Crosslinking, Biodegradable GelMA/PEGDA Hydrogel for Guided Bone Regeneration Materials. Materials 2018, 11, 1345. [Google Scholar] [CrossRef] [Green Version]
- Singh, D.; Zo, S.M.; Singh, D.; Han, S.S. Interpenetrating Alginate on Gelatin- Poly (2-hydroxyethyl Methacrylate) as a Functional Polymeric Matrix for Cartilage Tissue Engineering. Int. J. Polym. Mater. Po. 2019, 68, 551–563. [Google Scholar] [CrossRef]
- Kim, D.H.; Heo, S.-J.; Shin, J.-W.; Mun, C.W. Preparation of Thermosensitive Gelatin-Pluronic Copolymer for Cartilage Tissue Engineering. Macromol. Res. 2010, 18, 387–391. [Google Scholar] [CrossRef]
- Han, L.; XU, J.; LU, X.; Gan, D.; Wang, Z.; WANG, K.F.; Zhang, H.; Yuan, H.; Weng, J. Biohybrid methacrylated gelatin/ polyacrylamide hydrogels for cartilage repair. J. Mater. Chem. B 2017, 5, 731–741. [Google Scholar] [CrossRef]
- Saghebasl, S.; Davaran, S.; Rahbarghazi, R.; Montaseri, A.; Salehi, R.; Ramazani, A. Synthesis and in vitro evaluation of thermosensitive hydrogel scaffolds based on (PNIPAAm-PCL-PEG-PCL-PNIPAAm)/Gelatin and (PCL-PEGPCL)/ Gelatin for use in cartilage tissue engineering. J. Biomater. Sci. Polym. Ed. 2018, 29, 1185–1206. [Google Scholar] [CrossRef]
- Temofeew, N.A.; Hixon, K.R.; McBride-Gagyi, S.H.; Sell, S.A. The fabrication of cryogel scaffolds incorporated with poloxamer 407 for potential use in the regeneration of the nucleus pulposus. J. Mater. Sci. Mater. Med. 2017, 28, 36. [Google Scholar] [CrossRef]
- Marin, S.; Albu Kaya, M.G.; Ghica, M.V.; Dinu-Pîrvu, C.; Popa, L.; Udeanu, D.I.; Mihai, G.; Enachescu, M. Collagen-Polyvinyl Alcohol-Indomethacin Biohybrid Matrices as Wound Dressings. Pharmaceutics 2018, 10, 224. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Pan, H.; Fan, D.; Duan, Z.; Zhu, C.; Fu, R.; Li, X. Non-stick hemostasis hydrogels as dressings with bacterial barrier activity for cutaneous wound healing. Mater. Sci. Eng. C 2019, 105, 110118. [Google Scholar] [CrossRef] [PubMed]
- Norouzi, M.R.; Ghasemi-Mobarakeh, L.; Gharibi, H.; Meamar, R.; Ajalloueian, F.; Chronakis, I.S. Surface modification of poly (ethylene terephthalate) fabric by soy protein isolate hydrogel for wound dressing application. Int. J. Polym. Mater. Polym. Biomater. 2018, 68, 1–9. [Google Scholar] [CrossRef]
- Snyders, R.; Shingel, K.I.; Zabeida, O.; Roberge, C.; Faure, M.-P.; Martinu, L.; Klemberg-Sapieha, J.E. Mechanical and microstructural properties of hybrid poly(ethylene glycol)–soy protein hydrogels for wound dressing applications. J. Biomed. Mater. Res. Part A 2007, 83, 88–97. [Google Scholar] [CrossRef]
- Demeter, M.; Virgolici, M.; Vancea, C.; Scarisoreanu, A.; Kaya, M.G.A.; Meltzer, V. Network structure studies on γ–irradiated Collagen–PVP superabsorbent hydrogels. Radiat. Phys. Chem. 2017, 131, 51–59. [Google Scholar] [CrossRef]
- Noppakundilograt, S.; Choopromkaw, S.; Kiatkamjornwong, S. Hydrolyzed collagen-grafted-poly[(acrylic acid)-co-(methacrylic acid)] hydrogel for drug delivery. J. Appl. Polym. Sci. 2018, 135, 45654. [Google Scholar] [CrossRef] [Green Version]
- Pupkaite, J.; Rosenquist, J.; Hilborn, J.; Samanta, A. Injectable Shape-Holding Collagen Hydrogel for Cell Encapsulation and Delivery Cross-linked Using Thiol-Michael Addition Click Reaction. Biomacromolecules 2019, 20, 3475–3484. [Google Scholar] [CrossRef]
- Bini, R.A.; Silva, M.F.; Varanda, L.C.; da Silva, M.; Dreiss, C.A. Soft nanocomposites of gelatin and poly(3-hydroxybutyrate) nanoparticles for dual drug release. Colloids Surf. B Biointerfaces 2017, 157, 191–198. [Google Scholar] [CrossRef] [Green Version]
- Lai, T.; Yu, J.; Tsai, W. Gelatin Methacrylate/Carboxybetaine Methacrylate Hydrogels with Tunable Crosslinking for Controlled Drug Release. J. Mater. Chem. B 2016, 4, 2304–2313. [Google Scholar] [CrossRef]
- Anirudhan, T.S.; Mohan, A.M. Novel pH sensitive dual drug loaded-gelatin methacrylate/methacrylic acid hydrogel for the controlled release of antibiotics. Int. J. Biol Macromol. 2018, 110, 167–178. [Google Scholar] [CrossRef]
- Yu, M.; Yao, Q.; Zhang, Y.; Chen, H.; He, H.; Zhang, Y.; Yin, T.; Tang, X.; Xu, H. Core/shell PLGA microspheres with controllable in vivo release profile via rational core phase design. Artif. Cells Nanomed. Biotechnol. 2018, 46, 1070–1079. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Guo, J.; Pan, S.; Yin, X.; He, Y.-F.; Li, T.; Wang, R.-M. pH-Sensitive keratin-based polymer hydrogel and its controllable drug-release behavior. J. Appl. Polym. Sci. 2015, 132, 41572. [Google Scholar] [CrossRef]
- Liu, Y.; Cui, Y.; Liao, M. pH and temperature-responsive IPN hydrogels based on soy protein and poly(N-isopropylacrylamide-co-sodium acrylate). J. Appl. Polym. Sci. 2015, 131, 39781. [Google Scholar] [CrossRef]
- He, N.; Chen, X.; Wang, L.; Wen, J.; Li, Y.; Cao, Q.; Liu, Z.; Li, B. Fabrication of composite hydrogels based on soy protein isolate and their controlled globular protein delivery. Glob. Chall. 2019, 3, 1900030. [Google Scholar] [CrossRef]
- Aderibigbe, B.A.; Mhlwatika, Z. Dual release kinetics of antimalarials from soy protein isolate-carbopol-polyacrylamide based hydrogels. J. Appl. Polym. Sci. 2016, 133, 43918. [Google Scholar] [CrossRef]
- Zhu, Q.; Gong, Y.; Guo, T.; Deng, J.; Ji, J.; Wang, B.; Hao, S. Thermo-sensitive keratin hydrogel against iron-induced brain injury after experimental intracerebral hemorrhage. Int. J. Pharm. 2019, 566, 342–351. [Google Scholar] [CrossRef]
- Vijayavenkataraman, S.; Vialli, N.; Fuh, J.Y.H.; Lu, W.F. Conductive collagen/PPy-b-PCL hydrogel for bioprinting of neural tissue constructs. Int. J. Bioprint. 2019, 5, 229. [Google Scholar] [CrossRef]
- Chen, K.; Fan, X.; Tang, K.; Wan, G.; He, X.; Li, X.; Chen, Q.; Shen, M.; Lv, Y.; Wang, F. A morphology-controllable collagen/poly(2-hydroxyethyl methacrylate) porous hydrogel with paraffin microsphere as template. ACS Appl. Bio. Mater. 2018, 1, 1311–1318. [Google Scholar] [CrossRef]
- Wang, C.; Chen, C.; Guo, M.; Li, B.; Han, F.; Chen, W. Stretchable collagen-coated polyurethane-urea hydrogel seeded with bladder smooth muscle cells for urethral defect repair in a rabbit model. J. Mater. Sci.: Mater. Med. 2019, 30, 135. [Google Scholar] [CrossRef]
- Wakuda, Y.; Nishimoto, S.; Suye, S.; Fujita, S. Native collagen hydrogel nanofibres with anisotropic structure using core-shell electrospinning. Sci. Rep. 2018, 8, 6248. [Google Scholar] [CrossRef]
- Sarkar, J.; Kamble, S.C.; Patil, R.; Kumar, A.; Gosavi, S.W. Gelatin interpenetration in poly N-isopropylacrylamide network reduces the compressive modulus of the scaffold: A property employed to mimic hepatic matrix stiffness. Biotechnol. Bioeng. 2020, 117, 567–579. [Google Scholar] [CrossRef] [PubMed]
- Yu, L.; Gu, L. Hydrolyzed polyacrylonitrile-blend-soy protein hydrogel fibers: A study of structure and dynamic pH response. Polym. Int. 2009, 58, 66–73. [Google Scholar] [CrossRef]
- Vishnoi, T.; Singh, A.; Teotia, A.K.; Kumar, A. Chitosan-Gelatin-Polypyrrole Cryogel Matrix for Stem Cell Differentiation into Neural Lineage and Sciatic Nerve Regeneration in Peripheral Nerve Injury Model. ACS Biomater. Sci. Eng. 2019, 5, 3007–3021. [Google Scholar] [CrossRef]
- Li, G.; Kong, Y.; Zhao, Y.; Zhao, Y.; Zhang, L.; Yang, Y. Fabrication and characterization of polyacrylamide/silk fibroin hydrogels for peripheral nerve regeneration. J. Biomater. Sci. Polym. Ed. 2015, 26, 899–916. [Google Scholar] [CrossRef]
- Sui, Z.; King, W.J.; Murphy, W.L. Dynamic Materials Based on a Protein Conformational Change. Adv. Mater. 2007, 19, 3377–3380. [Google Scholar] [CrossRef]
- Tan, H.; Jin, D.; Qu, X.; Liu, H.; Yin, M.; Liu, C. A PEG-Lysozyme hydrogel harvests multiple functions as a fit-to-shape tissue sealant for internal-use of body. Biomaterials 2019, 192, 392–404. [Google Scholar] [CrossRef]
- Park, K.M.; Lee, Y.; Son, J.Y.; Oh, D.H.; Lee, J.S.; Park, K.D. Synthesis and characterizations of in situ cross-linkable gelatin and 4-arm-PPO-PEO hybrid hydrogels via enzymatic reaction for tissue regenerative medicine. Biomacromolecules 2012, 13, 604–611. [Google Scholar] [CrossRef]
- Zheng, Z.; Wu, J.; Liu, M.; Wang, H.; Li, C.; Rodriguez, M.J.; Li, G.; Wang, X.; Kaplan, D.L. 3D Bioprinting of Self-Standing Silk-Based Bioink. Adv. Healthcare Mater. 2018, 7, 1701026. [Google Scholar] [CrossRef]
- McGann, C.L.; Akins, R.E.; Kiick, K.L. Resilin-PEG hybrid hydrogels yield degradable elastomeric scaffolds with heterogeneous microstructure. Biomacromolecules 2016, 17, 128–140. [Google Scholar] [CrossRef] [Green Version]
- Liu, B.; Lewis, A.K.; Shen, W. Physical Hydrogels Photo-Cross-Linked from Self-Assembled Macromers for Potential Use in Tissue Engineering. Biomacromolecules 2009, 10, 3182–3187. [Google Scholar] [CrossRef]
- Visser, J.; Melchels, F.P.W.; Jeon, J.E.; van Bussel, E.M.; Kimpton, L.S.; Byrne, H.M.; Dhert, W.J.A.; Dalton, P.D.; Hutmacher, D.W.; Malda, J. Reinforcement of hydrogels using three-dimensionally printed microfibres. Nat. Commun. 2015, 6, 6933. [Google Scholar] [CrossRef] [PubMed]
- De Mori, A.; Fernández, M.P.; Blunn, G.; Tozzi, G.; Roldo, M. 3D Printing and Electrospinning of Composite Hydrogels for Cartilage and Bone Tissue Engineering. Polymers 2018, 10, 285. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Liu, W.; Zhan, J.; Su, Y.; Wu, T.; Ramakrishna, S.; Liao, S.; Mo, X. Injectable hydrogel incorporating with nanoyarn for bone regeneration. J. Biomater. Sci. Polym. Ed. 2014, 25, 168–180. [Google Scholar] [CrossRef] [PubMed]
- Gan, Y.; Li, P.; Wang, L.; Mo, X.; Song, L.; Xu, Y.; Zhao, C.; Ouyang, B.; Tu, B.; Luo, L.; et al. An interpenetrating network-strengthened and toughened hydrogel that supports cell-based nucleus pulposus regeneration. Biomaterials 2017, 136, 12–28. [Google Scholar] [CrossRef]
- Wang, X.; Partlow, B.; Liu, J.; Zheng, Z.; Su, B.; Wang, Y.; Kaplan, D.L. Injectable silk-polyethylene glycol hydrogels. Acta Biomater. 2015, 12, 51–61. [Google Scholar] [CrossRef]
- Xu, Y.; Peng, J.; Richards, G.; Lu, S.; Eglin, D. Optimization of electrospray fabrication of stem cell-embedded alginate-gelatin microspheres and their assembly in 3D- printed poly(ε-caprolactone) scaffold for cartilage tissue engineering. J. Orthop. Transl. 2019, 18, 128–141. [Google Scholar] [CrossRef]
- Asadi, N.; Alizadeh, E.; Bakhshayesh, A.R.D.; Mostafavi, E.; Akbarzadeh, A.; Davaran, S. Fabrication and in vitro Evaluation of Nanocomposite Hydrogel Scaffolds Based on Gelatin/PCL−PEG−PCL for Cartilage Tissue Engineering. ACS Omega. 2019, 4, 449–457. [Google Scholar] [CrossRef]
- Lee, J.M.; Sultan, M.T.; Kim, S.H.; Kumar, V.; Yeon, Y.K.; Lee, O.J.; Park, C.H. Artificial Auricular Cartilage Using Silk Fibroin and Polyvinyl Alcohol Hydrogel. Int. J. Mol. Sci. 2017, 18, 1707. [Google Scholar] [CrossRef] [Green Version]
- Bektas, C.K.; Kimiz, I.; Urkmez, A.S.; Hasirci, V.; Hasirci, N. A Bilayer Scaffold Prepared from Collagen and Carboxymethyl Cellulose for Skin Tissue Engineering Applications. J. Biomater. Sci. Polym. Ed. 2018, 29, 1764–1784. [Google Scholar] [CrossRef]
- Park, M.; Kim, B.-S.; Shin, H.K.; Park, S.-J.; Kim, H.-Y. Preparation and characterization of keratin-based biocomposite hydrogels prepared by electron beam irradiation. Mater. Sci. Eng. C 2013, 33, 5051–5057. [Google Scholar] [CrossRef]
- Park, M.; Shin, H.K.; Kim, B.-S.; Kim, M.J.; Kim, I.-S.; Park, B.-Y.; Kim, H.-Y. Effect of discarded keratin-based biocomposite hydrogels on the wound healing process in vivo. Mater. Sci. Eng. C 2015, 55, 88–94. [Google Scholar] [CrossRef] [PubMed]
- Punyamoonwongsa, P.; Klayya, S.; Sajomsang, W.; Kunyanee, C.; Aueviriyavit, S. Silk sericin semi-interpenetrating network hydrogels based on PEG-Diacrylate for wound healing treatment. Int. J. Polym. Sci. 2019, 2019, 4740765. [Google Scholar] [CrossRef]
- Aramwit, P.; Sereemaspun, A.; Yamdech, R. Sericin Ameliorates the Properties of Poly(VinylAlcohol) Hydrogel Prepared by Simple Repeated Freeze-Thaw Process without the Use of Chemical Crosslinking. IJRS 2018, 4, 6–11. [Google Scholar] [CrossRef]
- Ross, S.; Yooyod, M.; Limpeanchob, N.; Mahasaranon, S.; Suphrom, N.; Ross, G.M. Novel 3D porous semi-IPN hydrogel scaffolds of silk sericin and poly(N-hydroxyethyl acrylamide) for dermal reconstruction. Express Polym. Lett. 2017, 11, 719–730. [Google Scholar] [CrossRef]
- Kundu, B.; Kundu, S.C. Silk sericin/polyacrylamide in situ forming hydrogels for dermal reconstruction. Biomaterials 2012, 33, 7456–7467. [Google Scholar] [CrossRef] [PubMed]
- Youngblood, R.L.; Truong, N.F.; Segura, T.; Shea, L.D. It’s All in the Delivery: Designing Hydrogels for Cell and Non-viral Gene Therapies. Mol. Ther. 2018, 26, 2087–2106. [Google Scholar] [CrossRef] [Green Version]
- Krebs, M.D.; Jeon, O.; Alsberg, E. Localized and sustained delivery of silencing RNA from macroscopic biopolymer hydrogels. J. Am. Chem. Soc. 2009, 131, 9204–9206. [Google Scholar] [CrossRef]
- Peng, H.; Yang, H.; Song, L.; Zhou, Z.; Sun, J.; Du, Y.; Lu, K.; Li, T.; Yin, A.; Xu, J.; et al. Sustained delivery of siRNA/PEI complex from in situ forming hydrogels potently inhibits the proliferation of gastric cancer. J. Exp. Clin. Cancer Res. 2016, 35, 57. [Google Scholar] [CrossRef] [Green Version]
- Pamfil, D.; Vasile, C. Chapter 4: Nanogels of natural polymers. In Polymer Gels: Science and Fundamentals. Gels Horizons: From Science to Smart Materials; Thakur, V., Thakur, M.K., Voicu, S., Eds.; Springer Nature: Singapore, 2018; pp. 71–110. [Google Scholar] [CrossRef]
- Tran, D.-H.N.; Nguyen, T.H.; Vo, T.N.N.; Pham, L.P.T.; Vo, D.M.H.; Nguyen, C.K.; Bach, L.G.; Nguyen, D.H. Self-assembled poly(ethylene glycol) methyl ether-grafted gelatin nanogels for efficient delivery of curcumin in cancer treatment. J. Appl. Polym. Sci. 2019, 136, 47544. [Google Scholar] [CrossRef] [Green Version]
- Ge, J.; Min, S.-H.; Kim, D.M.; Lee, D.C.; Park, K.C.; Yeom, Y.I. Selective gene delivery to cancer cells secreting matrix metalloproteinases using a gelatin/polyethylenimine/DNA complex. Biotechnol. Bioprocess. Eng. 2012, 17, 160–167. [Google Scholar] [CrossRef]
- Truong-Le, V.L.; Walsh, S.M.; Schweibert, E.; Mao, Q.H.; Guggino, W.B.; August, J.T.; Leong, K.W. Gene transfer by DNA-gelatin nanospheres. Arch. Biochem. Biophys. 1999, 361, 47–56. [Google Scholar] [CrossRef] [PubMed]
- Rumschöttel, J.; Baus, S.; Kosmella, S.; Appelhans, D.; Koetz, J. Incorporation of DNA/PEI polyplexes into gelatin/chitosan hydrogel scaffolds: A μ-DSC study. Compos. Interfaces 2018, 25, 1–11. [Google Scholar] [CrossRef]
- Chao, G.; Deng, H.; Huang, Q.; Jia, W.; Huang, W.; Gu, Y.; Tan, H.; Fan, L.; Liu, C.; Huang, A.; et al. Preparation and Characterization of pH Sensitive Semi-interpenetrating Network Hydrogel Based on Methacrylic Acid, Bovine Serum Albumin (BSA), and PEG. J. Polym. Res. 2006, 13, 349–355. [Google Scholar] [CrossRef]
- Gayet, J.-C.; Fortier, G. High water content BSA-PEG hydrogel for controlled release device: Evaluation of the drug release properties. J. Control. Release 1996, 38, 177–184. [Google Scholar] [CrossRef]
- Li, X.; Qin, J.; Ma, J. Silk fibroin/poly (vinyl alcohol) blend scaffolds for controlled delivery of curcumin. Regen. Biomater. 2015, 2, 97–105. [Google Scholar] [CrossRef]
- Zhong, T.; Jiang, Z.; Wang, P.; Bie, S.; Zhang, F.; Zuo, B. Silk fibroin/copolymer composite hydrogels for the controlled and sustained release of hydrophobic/hydrophilic drugs. Int. J. Pharm. 2015, 494, 264–270. [Google Scholar] [CrossRef]
- Farooq, M.A.; Aquib, M.; Ghayas, S.; Bushra, R.; Khan, D.H.; Parveen, A.; Wang, B. Whey protein: A functional and promising material for drug delivery systems recent developments and future prospects. Polym. Adv. Technol. 2019, 30, 2183–2191. [Google Scholar] [CrossRef]
- Aderibigbe, B.A.; Ndwabu, S. Evaluation of whey protein isolate-graft-carbopolpolyacrylamide pH-sensitive composites for controlled release of pamidronate. Polym. Bull. 2017, 74, 5129–5144. [Google Scholar] [CrossRef]
- Seeman, N. DNA in a material world. Nature 2003, 421, 427–431. [Google Scholar] [CrossRef]
- Stoleru, E.; Vasile, C. Chapter 6: Nucleic acids-based bionanomaterials for drug and gene therapy. In Micro and Nano Technologies; Vasile, C., Ed.; Elsevier: Amsterdam, The Netherlands, 2019; pp. 235–259. [Google Scholar]
- Gačanin, J.; Synatschke, C.V.; Weil, T. Biomedical applications of DNA-based hydrogels. Adv. Funct. Mater. 2020, 30, 1906253. [Google Scholar] [CrossRef] [Green Version]
- Costa, D.; Valente, A.J.M.; Queiroz, J. Chapter 13: DNA-Based Hydrogels: An Approach for Multifunctional Bioapplications. In Hydrogels, Gels Horizons: From Science to Smart Materials; Thakur, V.K., Thakur, M.K., Eds.; Springer Nature Singapore Pte Ltd.: Singapore, 2018. [Google Scholar]
- Lia, J.; Mo, L.; Lu, C.-H.; Fu, T.; Yang, H.-H.; Tan, W. Functional nucleic acid-based hydrogels for bioanalytical and biomedical applications. Chem. Soc. Rev. 2016, 45, 1410–1431. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Um, S.H.; Lee, J.B.; Park, N.; Kwon, S.Y.; Umbach, C.C.; Luo, D. Enzyme-catalysed assembly of DNA hydrogel. Nat. Mater. 2006, 5, 797–801. [Google Scholar] [CrossRef] [PubMed]
- Cheng, E.; Xing, Y.; Chen, P.; Yang, Y.; Sun, Y.; Zhou, D.; Xu, L.; Fan, Q.; Liu, D. A pH-Triggered, fast-responding DNA hydrogel. Angew. Chem. Int. Ed. 2009, 48, 7660–7663. [Google Scholar] [CrossRef] [PubMed]
- Ding, L.; Li, J.; Wu, C.; Yan, F.; Li, X.; Zhang, S. A self-assembled RNA-triple helix hydrogel drug delivery system targeting triple-negative breast cancer. J. Mater. Chem. B 2020. [Google Scholar] [CrossRef]
- Lin, D.C.; Yurke, B.; Langrana, N.A. Mechanical properties of a reversible, DNA-crosslinked polyacrylamide hydrogel. J. Biomech. Eng. 2004, 126, 104–110. [Google Scholar] [CrossRef]
- Soontornworajit, B.; Zhou, J.; Zhang, Z.; Wang, Y. Aptamer-functionalized in situ injectable hydrogel for controlled protein release. Biomacromolecules 2010, 11, 2724. [Google Scholar] [CrossRef]
- Li, S.; Chen, N.; Gaddes, E.R.; Zhang, X.; Dong, C.; Wang, Y. A Drosera-bioinspired hydrogel for catching and killing cancer cells. Sci. Rep. 2015, 5, 14297. [Google Scholar] [CrossRef] [Green Version]
- Zhang, X.-Z.; Zeng, X.; Sun, Y.-X.; Zhuo, R.-X. Bioactive materials in gene therapy. In Bioactive Materials in Medicine; Zhao, X., Courtney, J.M., Qian, H., Eds.; Woodhead Publishing Limited: Cambridge, UK, 2011. [Google Scholar]
- Korolev, N.; Lyubartsev, A.; Nordenskiold, L. Cation-induced polyelectrolyte-polyelectrolyte attraction in solutions of DNA and nucleosome core particles. Adv. Colloid Interface Sci. 2010, 158, 32–47. [Google Scholar] [CrossRef]
- Costa, D.; Valente, A.J.M.; Queiroz, J. Plasmid DNA nanogels as photoresponsive materials for multifunctional bio-applications. J. Biotechnol. 2015, 20, 98–104. [Google Scholar] [CrossRef] [Green Version]
- Ding, F.; Huang, X.; Gao, X.; Xie, M.; Pan, G.; Li, Q.; Song, J.; Zhu, X.; Zhang, C. A Non-cationic Nucleic Acid Nanogel for the Delivery of CRISPR/Cas9 Gene Editing Tool. Nanoscale 2019, 11, 17211–17215. [Google Scholar] [CrossRef]
- Mimi, H.; Ho, K.; Siu, Y.; Wu, A.; Li, P. Polyethyleneimine-based core-shell nanogels: A promising siRNA carrier for argininosuccinate synthetase mRNA knockdown in HeLa cells. J. Control. Release 2012, 158, 123–130. [Google Scholar] [CrossRef] [PubMed]
- Li, R.Q.; Wu, W.; Song, H.Q.; Ren, Y.; Yang, M.; Li, J.; Xu, F.J. Well-defined reducible cationic nanogels based on functionalized low-molecular-weight PGMA for effective pDNA and siRNA delivery. Acta Biomater. 2016, 41, 282–292. [Google Scholar] [CrossRef] [PubMed]
- Kang, H.; Liu, H.; Zhang, X.; Yan, J.; Zhu, Z.; Peng, L.; Yang, H.; Kim, Y.; Tan, W. Photoresponsive DNA-Cross-Linked Hydrogels for Controllable Release and Cancer Therapy. Langmuir 2011, 27, 399–408. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Wang, Y.; Zhang, S.; Benoit, D.S.W. Degradable poly(ethylene glycol) (PEG)-based hydrogels for spatiotemporal control of siRNA/nanoparticle delivery. J. Control. Release 2018, 287, 58–66. [Google Scholar] [CrossRef]
- Li, F.; Lyu, D.; Liu, S.; Guo, W. DNA Hydrogels and Microgels for Biosensing and Biomedical Applications. Adv. Mater. 2019, 32, 1–9. [Google Scholar] [CrossRef]
- Dave, N.; Huang, P.-J.J.; Chan, M.Y.; Smith, B.D.; Liu, J. Regenerable DNA-functionalized hydrogels for ultrasensitive, instrument-free mercury(II) detection and removal in water. J. Am. Chem. Soc. 2010, 132, 12668. [Google Scholar] [CrossRef] [Green Version]
- Hu, Y.; Kahn, J.S.; Guo, W.; Huang, F.; Fadeev, M.; Harries, D.; Willner, I. Reversible Modulation of DNA-Based Hydrogel Shapes by Internal Stress Interactions. J. Am. Chem. Soc. 2016, 138, 16112–16119. [Google Scholar] [CrossRef]
- Guo, W.; Lu, C.-H.; Orbach, R.; Wang, F.; Qi, X.-J.; Cecconello, A.; Seliktar, D.; Willner, I. pH-Stimulated DNA Hydrogels Exhibiting Shape-Memory Properties. Adv. Mater. 2015, 27, 73–78. [Google Scholar] [CrossRef]
- Liu, X.; Zhang, J.; Fadeev, M.; Li, Z.; Wulf, V.; Tian, H.; Willner, I. Chemical and photochemical DNA “gears” reversibly control stiffness, shape-memory, self-healing and controlled release properties of polyacrylamide hydrogels. Chem. Sci. 2019, 10, 1008–1016. [Google Scholar] [CrossRef] [Green Version]
- Rico-García, D.; Ruiz-Rubio, L.; Pérez-Alvarez, L.; Hernández-Olmos, S.L.; Guerrero-Ramírez, G.L.; Vilas-Vilela, J.L. Lignin-Based Hydrogels: Synthesis and Applications. Polymers 2020, 12, 81. [Google Scholar] [CrossRef] [Green Version]
- Meng, Y.; Lu, J.; Cheng, Y.; Li, Q.; Wang, H. Lignin-based hydrogels: A review of preparation, properties, and application. Int. J. Biol. Macromol. 2019, 135, 1006–1019. [Google Scholar] [CrossRef] [PubMed]
- Penaranda, J.E.; Sabino, M.A. Effect of the presence of lignin or peat in IPN hydrogels on the sorption of heavy metals. Polym. Bull. 2010, 65, 495–508. [Google Scholar] [CrossRef]
- Jin, C.; Song, W.; Liu, T.; Xin, J.; Hiscox, W.C.; Zhang, J.; Liu, G.; Kong, Z. Temperature and pH responsive hydrogels using methacrylated lignosulfonate cross-linker: Synthesis, characterization, and properties. ACS Sustain. Chem. Eng. 2018, 6, 1763–1771. [Google Scholar] [CrossRef]
- Passauer, L.; Halles, T.; Baucker, E.; Ciesielski, G.; Lebioda, S.; Hamer, U. Biodegradation of hydrogels from oxyethylated lignins in model soils. ACS Sustain. Chem. Eng. 2015, 3, 1955–1964. [Google Scholar] [CrossRef]
- Kai, D.; Low, Z.W.; Liow, S.S.; Karim, A.A.; Ye, H.; Jin, G.; Li, K.; Loh, X.J. Development of lignin supramolecular hydrogels with mechanically responsive and self-healing properties. ACS Sustain. Chem. Eng. 2015, 3, 2160–2169. [Google Scholar] [CrossRef]
- Zhao, H.; Feng, Q.; Xie, Y.; Li, J.; Chen, X. Preparation of biocompatible hydrogel from lignin-carbohydrate complex (LCC) as cell carriers. Bioresources 2017, 12, 8490–8504. [Google Scholar]
- Naficy, S.; Spinks, G.M.; Wallace, G.G. Thin, tough, pH-sensitive hydrogel films with rapid load recovery. Acs Appl. Mater. Interfaces 2014, 6, 4109–4114. [Google Scholar] [CrossRef]
- Oveissi, F.; Naficy, S.; Le, T.Y.L.; Fletcher, D.F.; Dehghani, F. Tough and processable hydrogels based on lignin and hydrophilic polyurethane. ACS Appl. Bio. Mater. 2018, 1, 2073–2081. [Google Scholar] [CrossRef]
- Park, S.; Kim, S.H.; Won, K.; Choi, J.W.; Kim, Y.H.; Kim, H.J.; Yang, Y.-H.; Lee, S.H. Wood mimetic hydrogel beads for enzyme immobilization. Carbohydr. Polym. 2015, 115, 223–229. [Google Scholar] [CrossRef]
- Borisenkov, M.F.; Karmanov, A.P.; Kocheva, L.S.; Markov, P.A.; Istomina, E.I.; Bakutova, L.A.; Litvinets, S.G.; Martinson, E.A.; Durnev, E.A.; Vityazev, F.V.; et al. Adsorption of beta-glucuronidase and estrogens on pectin/lignin hydrogel particles. Int. J. Polym. Mater. Polym. Biomater. 2016, 65, 433–441. [Google Scholar] [CrossRef]
- Figueiredo, P.; Ferro, C.; Kemell, M.; Liu, Z.; Kiriazis, A.; Lintinen, K.; Florindo, H.F.; Yli-Kauhaluoma, J.; Hirvonen, J.; Kostiainen, M.A.; et al. Functionalization of carboxylated lignin nanoparticles for targeted and pH-responsive delivery of anticancer drugs. Nanomedicine 2017, 12, 2581–2596. [Google Scholar] [CrossRef] [PubMed]
- Ciolacu, D.; Oprea, A.M.; Anghel, N.; Cazacu, G.; Cazacu, M. New cellulose-lignin hydrogels and their application in controlled release of polyphenols. Mater. Sci. Eng. C 2012, 32, 452–463. [Google Scholar] [CrossRef]
- Wu, L.; Huang, S.; Zheng, J.; Qiu, Z.; Lin, X.; Qin, Y. Synthesis and characterization of biomass lignin-based PVA super-absorbent hydrogel. Int. J. Biol. Macromol. 2019, 140, 538–545. [Google Scholar] [CrossRef] [PubMed]
- Wang, X.; Zhou, Z.; Guo, X.; He, Q. Ultrasonic-assisted synthesis of sodium lignosulfonate-grafted poly(acrylic acid-co-poly (vinyl pyrrolidone)) hydrogel for drug delivery. RSC Adv. 2016, 6, 35550–35558. [Google Scholar] [CrossRef]
- Spasojevic, D.; Zmejkoski, D.; Glamoclija, J.; Nikolic, M.; Sokovic, M.; Milosevic, V.; Jaric, I.; Stojanovic, M.; Marinkovic, E.; Barisani-Asenbauer, T.; et al. Lignin model compound in alginate hydrogel: A strong antimicrobial agent with high potential in wound treatment. Int. J. Antimicrob. Agents 2016, 48, 732–735. [Google Scholar] [CrossRef]
- Yang, W.; Fortunati, E.; Dominici, F.; Giovanale, G.; Mazzaglia, A.; Balestra, G.M.; Kenny, J.M.; Puglia, D. Effect of cellulose and lignin on disintegration, antimicrobial and antioxidant properties of PLA active films. Int. J. Biol. Macromol. 2016, 89, 360–368. [Google Scholar] [CrossRef]
- Mahata, D.; Jana, M.; Jana, A.; Mukherjee, A.; Mondal, N.; Saha, T.; Sen, S.; Nando, G.B.; Mukhopadhyay, C.K.; Chakraborty, R.; et al. Lignin-graft-polyoxazoline conjugated triazole a novel anti-infective ointment to control persistent inflammation. Sci. Rep. 2017, 7, 46412–46417. [Google Scholar] [CrossRef] [Green Version]
- Ravishankar, K.; Venkatesan, M.; Preeth, R.; Mahalingam, A. Biocompatible hydrogels of chitosan-alkali lignin for potential wound healing applications. Mater. Sci. Eng. C 2019, 102, 447–457. [Google Scholar] [CrossRef]
- Zmejkoski, D.; Spasojevic, D.; Orlovska, I.; Kozyrovska, N.; Sokovic, M.; Glamoclija, J.; Dmitrovic, S.; Matovic, B.; Tasic, N.; Maksimovic, V.; et al. Bacterial cellulose-lignin composite hydrogel as a promising agent in chronic wound healing. Int. J. Biol. Macromol. 2018, 118, 494–503. [Google Scholar] [CrossRef] [Green Version]
- Musilová, L.; Mrácek, A.; Kovalcik, A.; Smolka, P.; Minarík, A.; Humpolícek, P.; Vícha, R.; Ponížil, P. Hyaluronan hydrogels modified by glycinated Kraft lignin: Morphology, swelling, viscoelastic properties and biocompatibility. Carbohydr. Polym. 2018, 181, 394–403. [Google Scholar] [CrossRef]
- Larrañeta, E.; Imízcoz, M.; Toh, J.X.; Irwin, N.J.; Ripolin, A.; Perminova, A.; Dom, J.; Rodr, A.; Donnelly, R.F. Synthesis and Characterization of Lignin Hydrogels for Potential Applications as Drug Eluting Antimicrobial Coatings for Medical Materials. Sustain. Chem. Eng. 2018, 6, 9037–9046. [Google Scholar] [CrossRef]
- Alles, N.; Soysa, N.S.; Hussain, M.D.A.; Tomomatsu, N.; Saito, H.; Baron, R.; Morimoto, N.; Aoki, K.; Akiyoshi, K.; Ohya, K. Polysaccharide nanogel delivery of a TNF-α aand RANKL antagonist peptide allows systemic prevention of bone loss. Eur. J. Pharm. Sci. 2009, 37, 83–88. [Google Scholar] [CrossRef]
- Uenaka, A.; Wada, H.; Isobe, M.; Saika, T.; Tsuji, K.; Sato, E.; Sato, S.; Noguchi, Y.; Kawabata, R.; Yasuda, T.; et al. T cell immunomonitoring and tumor responses in patients immunized with a complex of cholesterol-bearing hydrophobized pullulan (CHP) and NY-ESO-1 protein. Cancer Immunol. 2007, 7, 9–20. [Google Scholar]
- Kageyama, S.; Kitano, S.; Hirayama, M.; Nagata, Y.; Imai, H.; Shiraishi, T.; Akiyoshi, K.; Scott, A.M.; Murphy, R.; Hoffman, E.W.; et al. Humoral immune responses in patients vaccinated with 1-146 HER2 protein complexed with cholesteryl pullulan nanogel. Cancer Sci. 2008, 99, 601–607. [Google Scholar] [CrossRef]
- Kitano, S.; Kageyama, S.; Nagata, Y.; Miyahara, Y.; Hiasa, A.; Naota, H.; Okumura, S.; Imai, H.; Shiraishi, T.; Masuya, M.; et al. HER2-specific T-cell immune responses in patients vaccinated with truncated HER2 protein complexed with nanogels of cholesteryl pullulan. Clin. Cancer Res. 2006, 12, 7397–7405. [Google Scholar] [CrossRef] [Green Version]
- Kawabata, R.; Wada, H.; Isobe, M.; Saika, T.; Sato, S.; Uenaka, A.; Miyata, H.; Yasuda, T.; Doki, Y.; Noguchi, Y.; et al. Antibody response against NY-ESO-1 in CHP-NY-ESO-1 vaccinated patients. Int. J. Cancer 2007, 120, 2178–2184. [Google Scholar] [CrossRef]
- Shingel, K.I.; Di Stabille, L.; Marty, J.P.; Faure, M.P. Inflammatory inert poly(ethylene glycol)–protein wound dressing improves healing responses in partial- and full-thickness wounds. Int. Wound J. 2006, 3, 332–342. [Google Scholar] [CrossRef]
- Nochi, T.; Yuki, Y.; Takahashi, H.; Sawada, S.-I.; Mejima, M.; Kohda, T.; Harada, N.; Kong, I.G.; Sato, A.; Kataoka, N.; et al. Nanogel antigenic protein-delivery system for adjuvant-free intranasal vaccines. Nat. Mater. 2010, 9, 572–578. [Google Scholar] [CrossRef]
- Kanokpanont, S.; Damrongsakkul, S.; Ratanavaraporn, J.; Aramwit, P. An innovative bi-layered wound dressing made of silk and gelatin for accelerated wound healing. Int. J. Pharm. 2012, 436, 141–153. [Google Scholar] [CrossRef]
- Kwiecień, I.; and Kwiecień, M. Application of Polysaccharide-Based Hydrogels as Probiotic Delivery Systems. Gels 2018, 4, 47. [Google Scholar] [CrossRef] [Green Version]


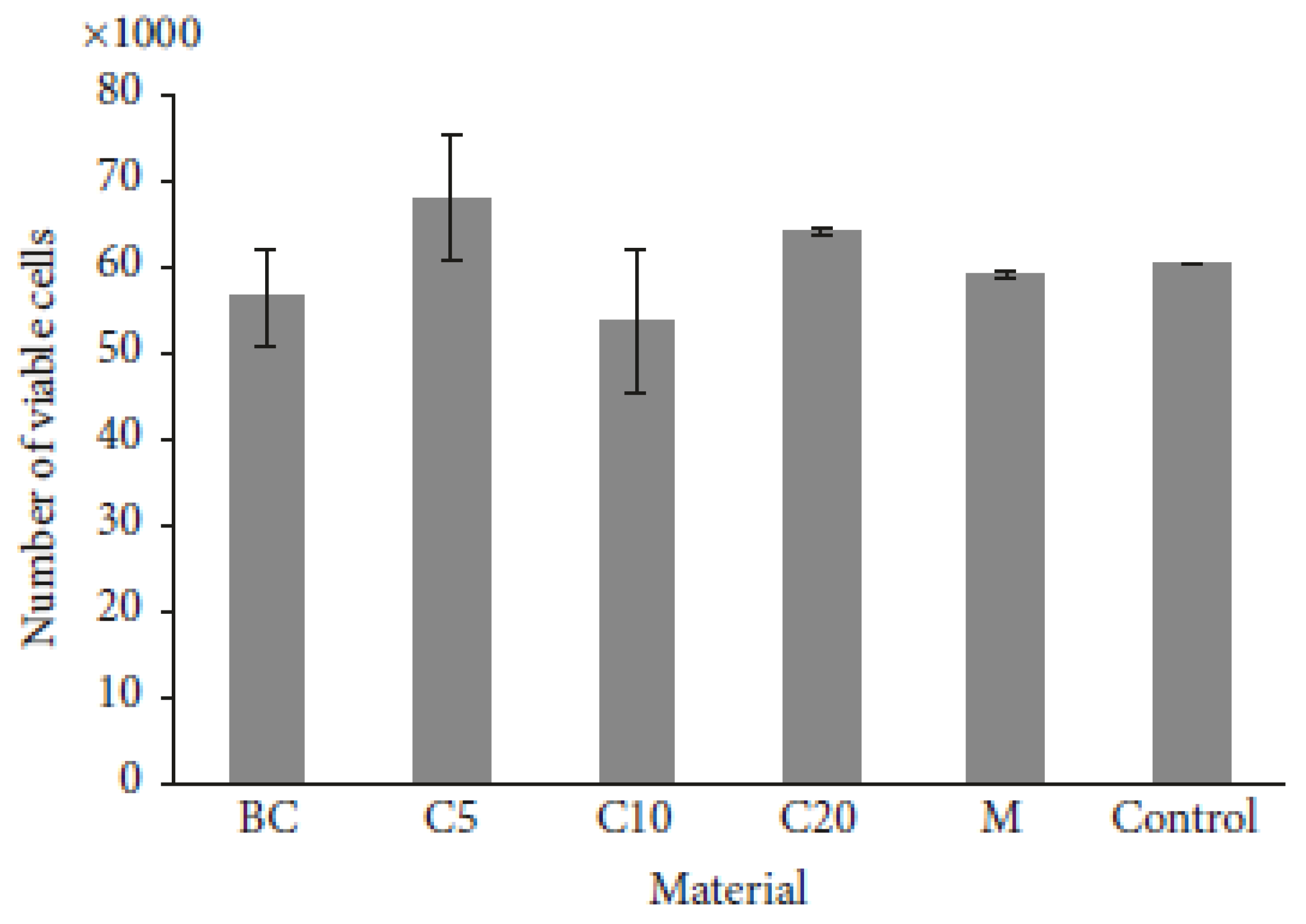
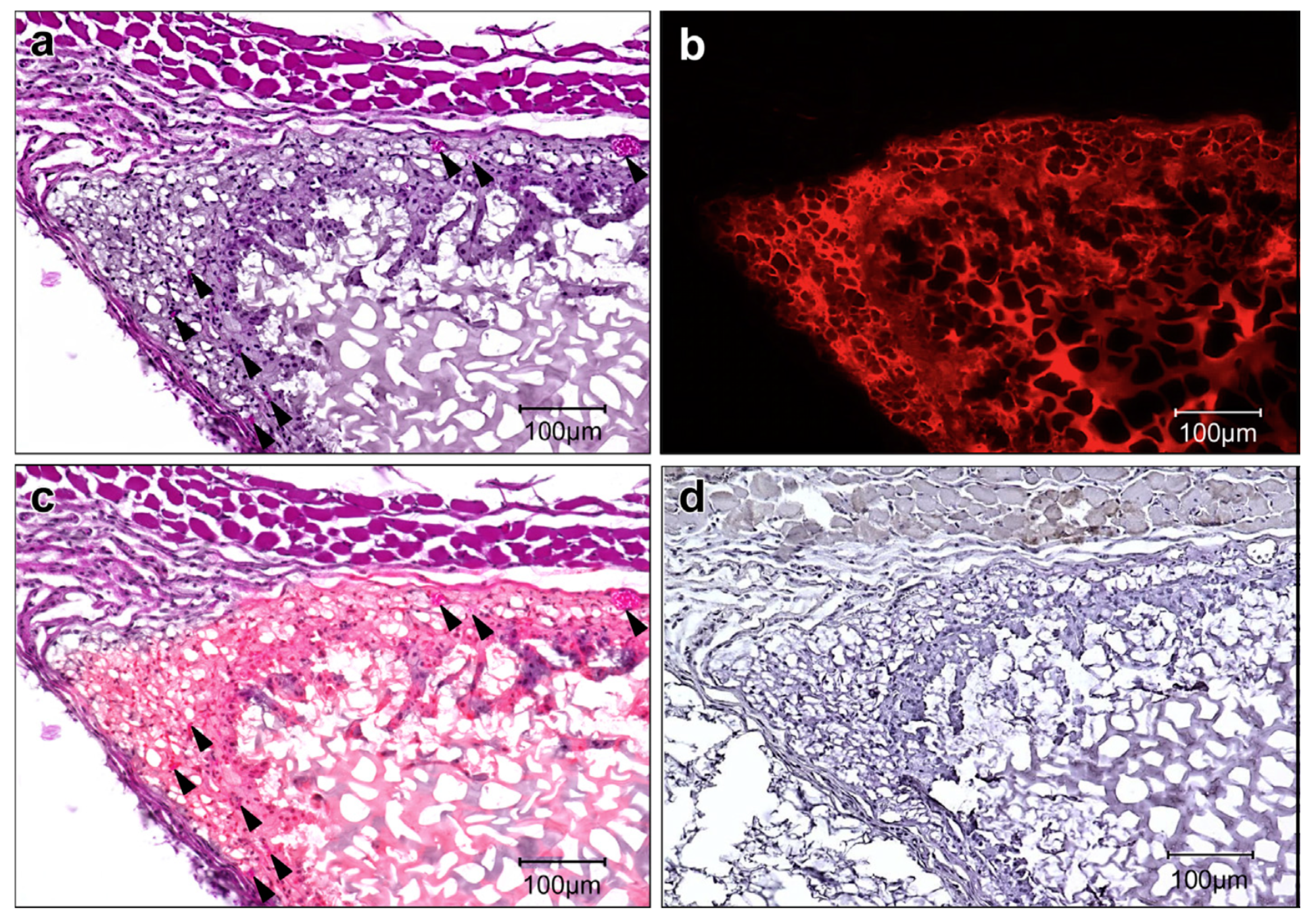
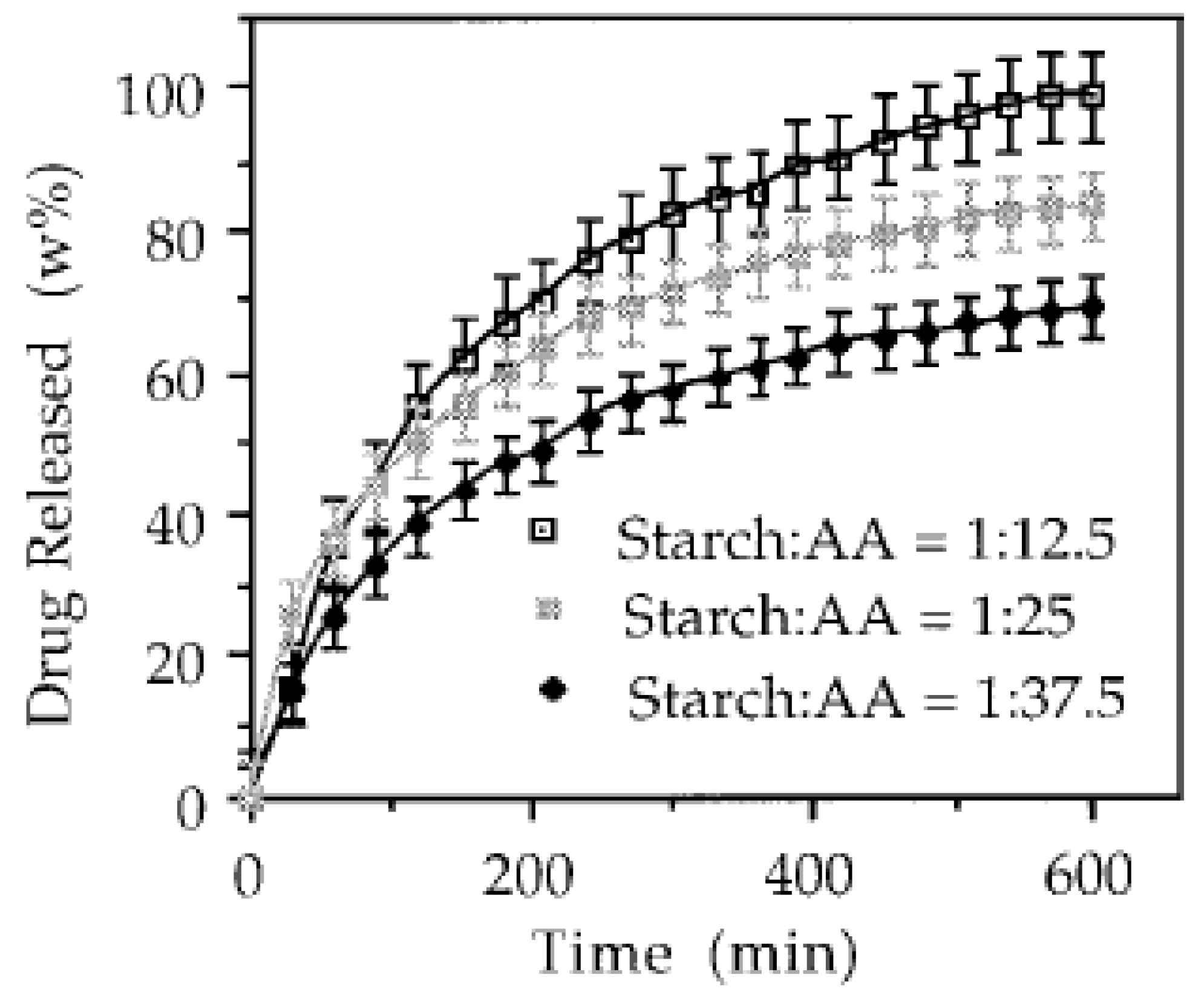

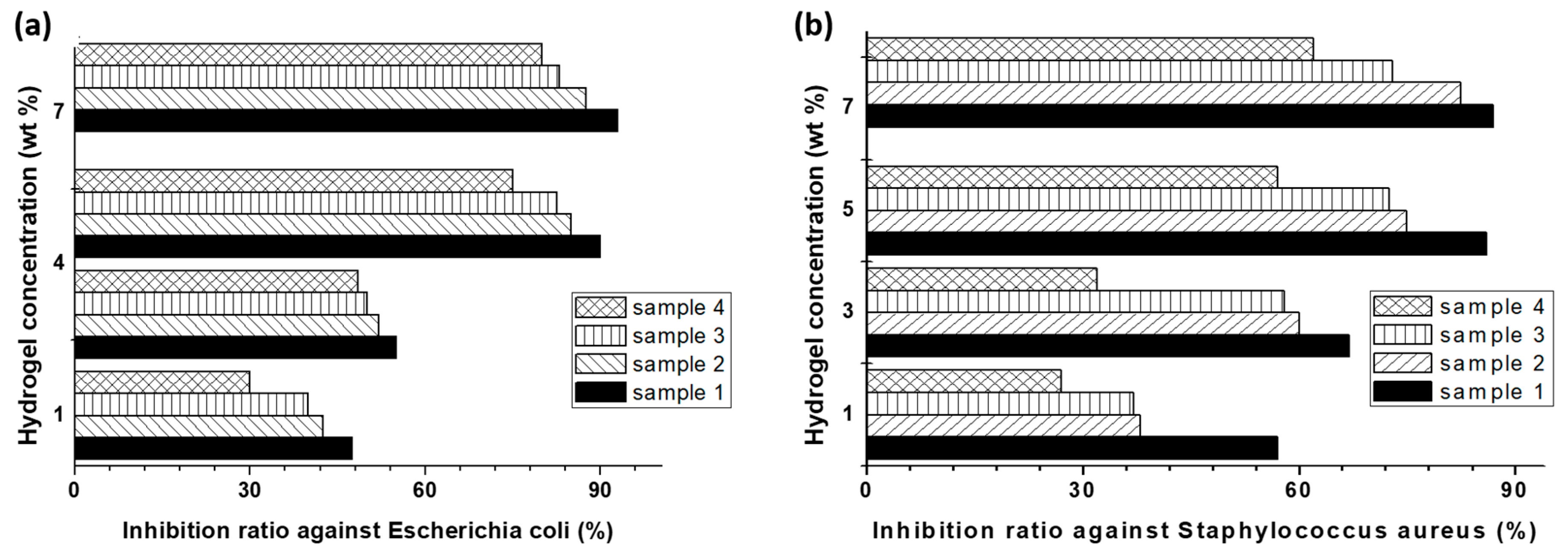

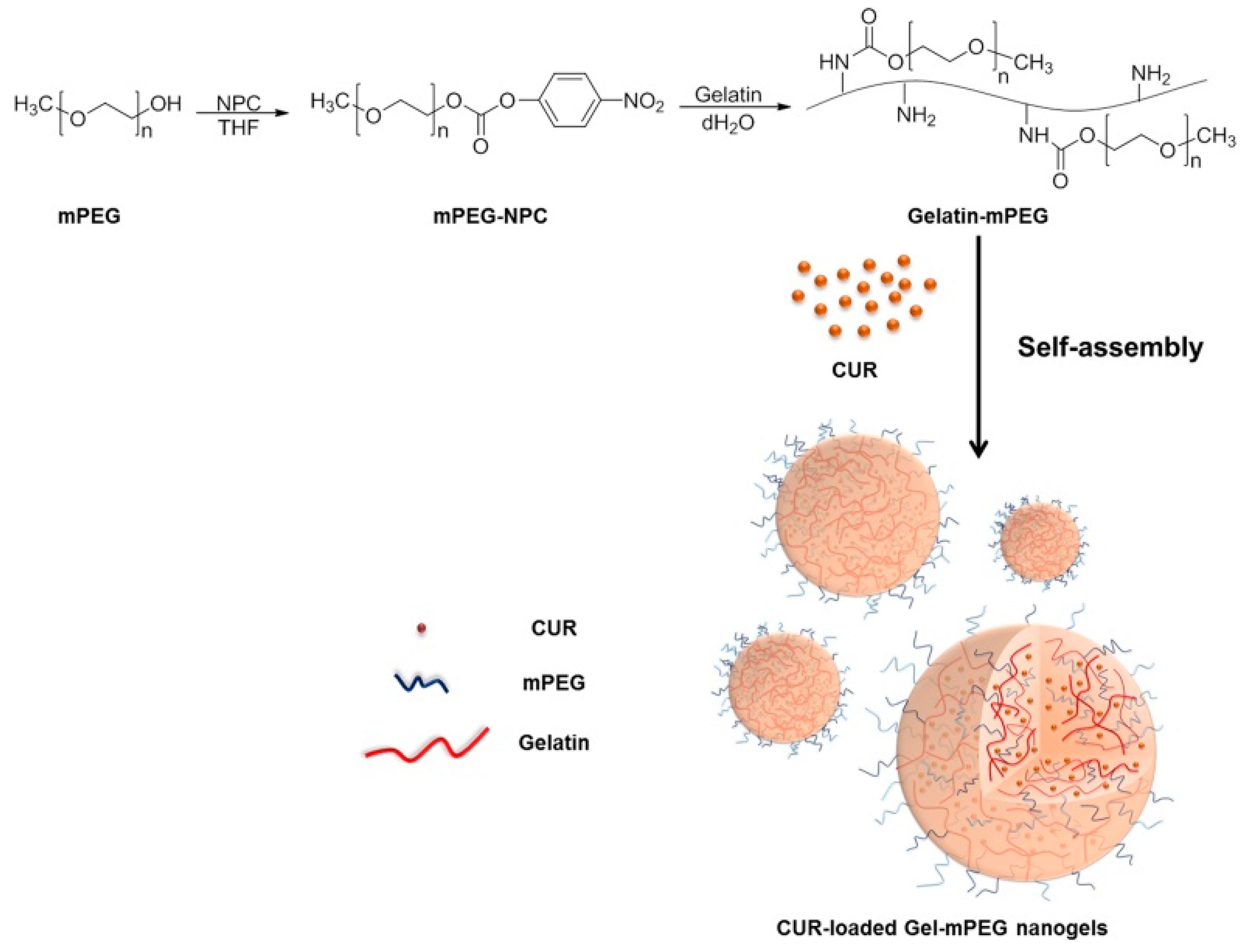
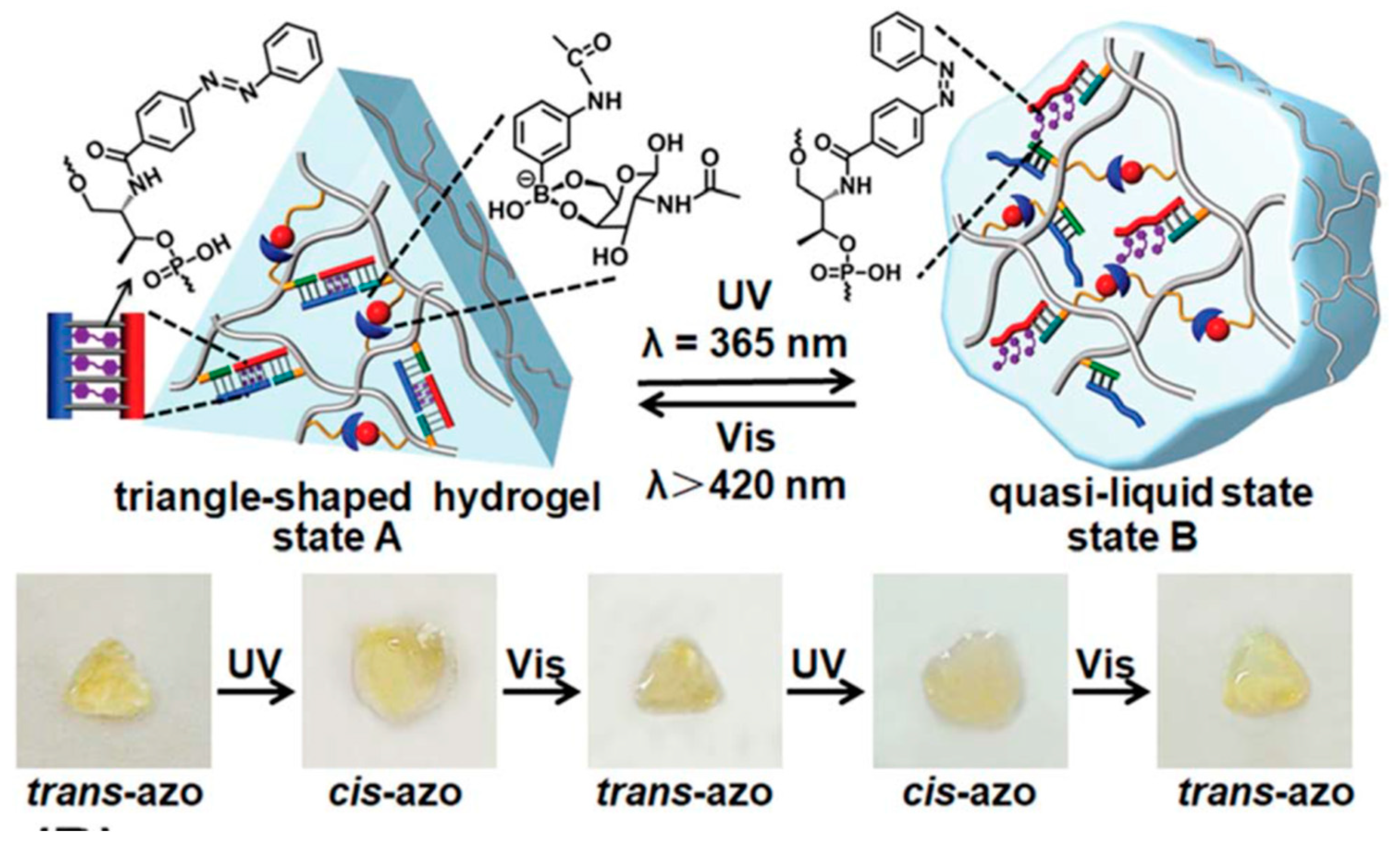
| Polysaccharides | Polypeptides and Proteins | Polynucleotides and Others | |
|---|---|---|---|
| Homopolysaccharides | Heteropolysaccharides | ||
Cellulose and derivatives (carboxymethylcellulose, hydroxyethyl cellulose; hydroxypropylcellulose methylcellulose hydroxypropylmethylcellulose; cellulose acetophphalate)
|
|
|
|
| Homopolysaccharide | Synthetic Component | Obtaining Method | Application | References |
|---|---|---|---|---|
| Cellulose | PVA and poly(acrylic acid-co-acrylamide-co22-acrylamido-2-methyl-1-propanesulfonic acid) | Graft copolymerization | In vitro gastrointestinal release of amoxicillin | [122] |
| PVA | Freezing/thawing (FT) cycles | 2D-layered skin model | [123] | |
| poly 2-(dimethylamino) ethyl methacrylate (PDMAEMA) | In situ radical polymerization | pH/temperature-responsive hydrogel | [124] | |
| Cellulose nanocrystal (CNC) | polyacrylamide (PAAm) | In situ polymerization (hydrophilic cross-linker PEGDA575) | Scaffolds for tissue engineering | [125] |
| Cellulose nanofibers | PAAm | Alkali treatment | Bio-medical load-bearing gel materials | [126] |
| CNC | PAAm and chitosan | Schiff base linkages and covalent crosslinking | Controlled drug release and dye adsorption | [127] |
| Bacterial cellulose (BC) | PAAm | Microwave irradiation | Oral drug delivery vehicles | [128] |
| poly(acrylic acid) (PAA) | Grafting by electron beam irradiation | Oral protein delivery | [129] | |
| poly(acrylic acid-co-acrylamide) | Microwave-assisted graft copolymerization | Controlled drug release | [130] | |
| poly(2-hydroxyethyl methacrylate) (PHEMA) | In situ UV radical polymerization | Cartilage, stent, and certain wound-dressing materials | [131] | |
| PGA | 60Co γ-irradiation crosslinking | Antibacterial contact materials | [132] | |
| poly(N-isopropylacrylamide) (PNIPAAm) | Atom transfer radical polymerization (ATRP) | Thermoresponsive hydrogels | [133] | |
| Hemicellulose grafting maleic anhydride (MA) | N-isopropylacrylamide (NIPAAm) | UV photocrosslinking | Smart biomaterials | [134] |
| Hydroxypropyl cellulose (HPC) | poly (l-glutamic acid-2-hydroxyethyl methacrylate) | Emulsion polymerization | Oral insulin controlled release | [135] |
| Hydroxyethyl cellulose (HEC) | PAA | Physical blending | pH-responsive material | [136] |
| Carboxymethyl cellulose (CMC) | PNIPAAm | Copolymerization | Protein delivery | [137] |
| carboxymethyl polyvinyl alcohol (CMPVA) | Grafting copolymerization (adipic dihydrazide as crosslinker) | Drug delivery and as scaffold in tissue engineering | [138] | |
| poly(dimethylamino ethyl methacrylate) (PDMAEMA) | Chemical grafting | Protein-drug delivery | [139] | |
| PEG (norbornene immobilized tetra-arm PEG) | Chemical cross-linking (dithiothreitol as co-crosslinker) | pH-sensitive protein drug carrier | [140] | |
| CMC acrylate | PEO-hexa-thiols | Michael type addition reaction | Scaffolds for tissue engineering | [141] |
| Methacrylate carboxymethyl cellulose (MACMC) | NIPAAm | Polymerization of NIPAAm in presence of CMC and redox crosslinking | Protein delivery | [137] |
| Starch | AAc | Potassium persulfate (KPS)-initiated graft copolymerization; in the presence of N,N′-methylene bisacrylamide (MBA) as cross-linker | Colon-targeted oral drug delivery | [142] |
| NIPAAm | Polymerization of NIPAAm using ammonium persulfate (APS) and N,N,N′,N′-tetramethylethylenediamine (TEMED) as a pair of redox initiators and MBA as the cross-linker | temperature-sensitive hydrogel | [143] | |
| AAm and vinyl pyrrolidone (VP) | CAN-initiated free radical solution polymerization in the presence of MBA | Drug release | [144] | |
| polyvinylamine | In situ crosslinking using starch decorated with cholesterol group and aldehyde groups | Drug release | [145] | |
| AAc | 60Co-gamma-radiation-induced graft polymerization | Drug delivery | [146] | |
| PVA | Gamma and electron beam radiation | Not tested yet | [147] | |
| Maize starch modified with allyl chloride | methacrylic acid and acrylamide | Copolymerization using KPS as initiator | Not tested yet | [148] |
| Carboxymethyl starch (CMS) | poly methacrylic acid (MAA) | Free radical graft copolymerization using bisacrylamide as a crosslinking agent and persulfate as an initiator | Drug release | [149] |
| Pullulan | Poly(l-lactide) (PLLA) | Graft copolymerization | Triggered drug release | [150] |
| PVA/ Poly-l-Lysine/Gelatin | FT method | Wound healing | [151] | |
| Oxidized pullulan (C6-OOH groups) | PVA | FT method | Wound dressing | [152] |
| Methacrylated pullulan (PULMA) | NIPAAm | Polymerization of NIPAAm using KPS as initiator and N,N,N′,N′-tetramethylethylenediamine as an accelerator | Proposed as temperature-responsive drug delivery system | [153] |
| Carboxymethyl pullulan (CMP) | PNIPAAm | Chemical cross-linking of NIPAAm in the presence of CMP followed by additional reticulation of CMP | Drug delivery | [154] |
| Cholesteryl-modified pullulan (CHP) | PNIPAAm | Graft free-radical copolymerization | Not tested yet | [155] |
| CHP | copolymer of NIPAAm and N-[4-(1-pyrenyl)butyl]-N-n-octadecylacrylamide] (PNIPAAm -C18Py) | Self-assembly | Not tested | [156] |
| Acrylate group-modified cholesterol-bearing pullulan (CHPANG) | Thiol group-modified poly (ethylene glycol) | Michael addition | Protein delivery | [157] |
| Acryloyl group modified-cholesterol-bearing pullulan (CHPOA) | Poly(methacrylic acid-g-ethylene glycol) (P(MAA-g-EG)) | Surface-initiated and bulk photopolymerization | Drug delivery | [158] |
| pentaerythritol tetra (mercaptoethyl) polyoxyethylene | Michael addition followed by freezing-induced phase separation | Advanced scaffold | [159] | |
| CG | poloxamer 407 copolymer (ethylene oxide and propylene oxide blocks) | Blending | Vaginal gel | [160] |
| ι-CG | PVA | FT technique | Cell adhesion | [161] |
| PEO | Blending with retinoic acid gel and Emulgen® 408 | Skin topical treatment | [162] | |
| κ-CG | PAAm and sodium alginate (SA) | Graft-copolymerization | Intestinal targeted drug delivery | [163] |
| PCL | Gel infusion within interpenetrating network (IPN) scaffolds of PCL incorporated with sucrose | Regenerative tissue engineering | [164] | |
| Poly(diethylacrylamide) (PDEA) | Crosslinking with methylene bisacrylamide | Not tested yet | [165] | |
| PNIPAAm | Electron beam radiation technique | Not evaluated yet | [166] | |
| PAAm | Dual physical-crosslinking strategy (hydrophobic associations and potassium ion (K+) cross-linking) | Cell culture | [167] | |
| PAA and super paramagnetic iron oxide nanoparticles (SPION) | Graft-copolymerization | Drug delivery | [168] | |
| poly(vinylpyrrolidone) (PVP) | Gamma irradiation | Wound healing | [169] | |
| PVP and PEG | 60Co gamma irradiation | Wound healing | [169] | |
| poly(oxyalkylene amine) | 3D-printing approach based on ionic-covalent entanglement | Not tested | [103] | |
| GG | PAAm | Cross-linking by Ca ions | Not evaluated | [170] |
| PEG | Ionic cross-linking with CaCl2 | Regenerative tissue engineering | [171] | |
| Polyethylene glycol diacrylate (PEGDA) | UV photo-crosslinking | Stem cells culture | [172] | |
| Poloxamer-Hep copolymer | Ionic cross-linking with CaCl2 | bone marrow stem cells delivery | [173] | |
| PVA | Emulsion cross-linking method | Drug delivery | [174] | |
| Gellan unsaturated esters | NIPAAm | Functionalization of GG with acrylic acid, acryloyl chloride or maleic anhydride and further co-polymerization | Not tested | [175] |
| Gellan maleate | NIPAAm | Free radical grafting/polymerization | Ocular inserts | [176] |
| Methacrylated gellan gum (MGG) | cationic polyurethane nanoparticles (CPUNs) | UV free radical polymerization | Tissue engineering | [177] |
| Hybrid Hydrogel Composite | Obtainment Method | Properties | Application | Reference |
|---|---|---|---|---|
| Alginate-based hybrid hydrogels | ||||
| PVA/alginate (Alg) | Physical crosslinking of PVA, followed by chemical crosslinking with alginate | * highly porous, open-cellular pore structures * pore size very 290–190 μm, depending on PVA concentration * scaffolds softer and more elastic than the control alginate, without affecting the mechanical strength * better cell adhesion and faster growth than the control alginate | Scaffolds for cartilage tissue engineering | [196] |
| PVA/SA hydrogel, containing nitrofurazone | FT method | * increase of SA concentration in PVA hydrogel films increased the swelling ability, elasticity, and thermal stability of PVA/SA hydrogel system * increase of SA content led to significant decreases in gel fraction %, and mechanical properties of PVA/SA hydrogel * low SA content resulted in a decreased protein adsorption, indicating a better blood compatibility | Wound dressing | [197] |
| Biodegradable PVA/SA-clindamycin-loaded hydrogel film | Physical crosslinking conducted by the FT method | * increasing SA concentration decreased the gelation (%), maximum strength and break elongation, but it resulted in an increase in the swelling ability, elasticity and thermal stability of the hydrogel film * SA content had an insignificant effect on the release profile of clindamycin from the PVA/SA film, whereas PVA/SA-clindamycin improved the healing rate of artificial wound in rats | Wound dressing | [198] |
| PVA/Alg (1/1 weight ratio) nanofiber hydrogels | In situ crosslinking using citric acid (5 wt%) + curing at 140 °C, for 2 h + conditioning at room temperature | * enhanced thermal stability and insolubility in both water and simulated body fluid (SBF) for 2 days | Tissue engineering | [199] |
| PVA/calcium alginate nanofiber web | Electrospinning technique | * a maximum calcium alginate content showed the maximum water vapor transmission rate that help in maintaining the local moist environment for accelerating wound healing * apparently new epithelium formation without any harmful reactions, when the wound is covered with the PVA based nanofiber | Wound healing | [200] |
| PVA/Alg reinforced with cellulose nanocrystals (CNCs) | Acidic hydrolysis | * fibrous porous structure (95.2% porosity) and improved mechanical stability * good properties for in vitro cell attachment | Scaffolds with good proliferation for fibroblast cells | [201,202] |
| Chondroitin sulfate-based hybrid hydrogels | ||||
| Chondroitin sulfate (CTS)/PEG | FXIIIa-mediated crosslinking of chondroitin sulfate grafted with PEG | * tuned growth factor binding and release * promoting of stem cell proliferation and osteogenic differentiation | Treatment of osteogenesis | [203] |
| PVA/HA/CTS hydrogels | Gamma irradiation (5–25 kGy) | * hydrogels with a higher content of HA/CTS exhibited higher enzymatic degradation rates * PVA/HA/CTS hydrogels cultures with human keratinocytes (HaCaT) showed higher cell viability (more than 90%), when compared to the control sample | Potential application in skin tissue engineering | [204] |
| Glucan-based hybrid hydrogels | ||||
| PVA/glucan films | Physical blending, followed by drying at 110 °C, without using chemically crosslinking | * no covalent bond between PVA and glucan was found in the formed film; glucan can be released to facilitate wound healing * an increase in glucan content led to a decrease in the tensile strength and an increase of the breaking elongation * a high glucan content with PVA film can hinder the cell mobility and prolong the time of healing * healing time of wound can be shortened by 48%, when glucan content is optimized | Wound dressing | [205] |
| Chitosan (CS) and chitosan derivatives-based hydrogels | ||||
| PVA/CS hydrogels | Crosslinking induced by exposure to different doses of γ-radiation | * gel fraction and mechanical properties of the hydrogels increased with increasing PVA concentration and irradiation dose * swelling ability of the hydrogels increased with increasing the CS content | Prevention of microbiological growth, such as bacteria, fungi and microorganisms, with possible use as wound dressing material | [206] |
| PVA/CS hydrogel membranes | FTcycle, followed by γ-irradiation process | * larger swelling capacity, high mechanical strength, lower water evaporation, and high thermal stability were obtained * good antibacterial activity against Escherichia coli with increasing CS content | Wound dressing | [207] |
| Addition of glycerol into PVA/CS hydrogels | Irradiation followed by FT | * acceleration of the healing process of wounds in a rat model * nontoxicity toward L929 mouse fibroblast cells * mature epidermal architecture was formed after the 11th day postoperatively | Wound dressing | [208] |
| Temperature-sensitive CS/PVA hydrogel | Chemical crosslinking, using glutaraldehyde | * the release of paclitaxel (PTX) in PBS (pH 7.4) is sustainable for 13 days * the antitumor activity of the drug-loaded composite hydrogel is 3.7 fold higher than that of Taxol | Intratumoral delivery of PTX | [209] |
| PVA/CS hydrogel loaded with vitamin B12 | Physical blending between different portions of PVA and water soluble CS, followed by treatment with formaldehyde to convert –NH2 group of CS into -N=C group in PVA/CS membranes | * increasing of CS content increases water content, water vapor transmission, and permeability of loaded vitamin B12 through PVA/CS membranes | Potential biomedical applications | [210] |
| Minocycline loaded PVA/CS hydrogel films | FT method | * high CS concentrations decreased gel fraction, mechanical properties, and thermal stability, and it increased the swelling ability, water vapor transmission, elasticity, and porosity of PVA/CS hydrogel films * faster healing of the wound when compared to the conventional sterile gauze control | Wound dressing | [211] |
| Nano-insulin loaded CS/PVA hydrogel | Chemical crosslinking, using glutaraldehyde as the cross-linking agent | * miscibility of nano-insulin and hydrogel * porous structure, with good deformability and flexibility * constant release of the insulin * high permeation rate of nano-insulin | Transdermal insulin delivery | [212] |
| CS / PVA nanofiber mats | Electrospinning, using different CS salts (CS-hydroxybenzotriazole (HOBt), CS-ethylenediaminetetraacetic acid (EDTA), and CS-thiamin pyrophosphate (TPP)) | * increase of the swelling degree with increasing CS; concentration, whatever the CS salt * no toxic compounds that reduce the cellular growth of fibroblasts * highest antibacterial activity and better healing activity were obtained for CS-EDTA/PVA fiber | Wound healing system | [213] |
| PVA/CS/gelatin hydrogel, incorporating polycaprolactone microspheres | Physically incorporation | * improvement of the mechanical properties by PVA * improvement of cell adhesion by gelatin | Delivery of basic fibroblast growth factor (bFGF) | [214] |
| CS/gelatin/PVA hydrogels | Gamma-irradiation | * increase of the swelling capacity with increasing the CS/gelatin ratio * 3D network structure with a good evaporation rate * about 10–20% water retained in 24 h; * good coagulation effect | Wound dressing | [215] |
| Gelatin/CS/PVA/ Arabic gum nanofibers | Electrospinning | * steady permeability of large molecules (e.g., BSA) * excellent cell attachment and proliferation | Wound healing | [216] |
| Gelatin/CS/PVA hydrogels | FT process | * non-toxic for the HT29-MTX-E12 cell line | Potential for tissue engineering applications | [217] |
| CS/polyethylenimine (PEI) 3D hydrogels | Physical mixture | * stable under cell culture conditions * could support the growth of primary human fetal skeletal cells | Gene transfection agent | [218] |
| CS-PEG co-polymer (CS-g-PEG) | Chemically grafting of monohydroxy PEG onto the CS backbone, using Schiff base and sodium cyanoborohydride chemistry | * obtainment of an injectable, thermoreversible gel * by optimizing PEG content (45–55 wt.%) and PEG molecular weight, the resultant system underwent a thermoreversible transition from an injectable solution at room temperature to a gel at body temperature | Potential carrier matrices for a wide range of biomedical and pharmaceutical applications | [219] |
| Thermo-responsive PEG-grafted CS hydrogel | Physical crosslinking | * steady protein release pattern for a period of 70 h after an initial burst release in the first 5 h * by crosslinking with genipin, it was obtained a prolonged quasi-linear release of the protein for up to 40 days; the initial burst release was reduced | Sustained BSA release | [220] |
| Injectable composite scaffold obtained from collagen-coated polylactide micro carriers/CS hydrogel | Physical crosslinking | * collagen-coated polylactide micro carriers enhanced the mechanical properties * cell metabolic activity increased before 9 days of in vitro chondrocytes growth within the scaffold * after 9–12 days, confluent cell layers were formed | Tissue engineering applications, particularly in orthopedics | [221] |
| CS/Poly(ε-caprolactone) (PCL)/polypyrrole | Electrospun | enhanced attachment and proliferation of PC12 cells | Neural tissue substrate | [222] |
| Maleiated CS/thiol-terminated PVA | Solvent casting | fetal porcine hepatocytes survived at least 14 days | Hepatocyte attachment | [223] |
| PVA/carboxymethyl chitosan (CM)-chitosan hydrogels | Electron beam rosslinking at room temperature | * mechanical properties and swelling degree improved after adding CM-chitosan * considerable antibacterial activity against E. coli for a low CM-chitosan content | Antibacterial activity | [224] |
| PVA/CM/honey | FT method | * inhibition of the growth of Escherichia coli bacteria * presence of honey leads to faster wound healing | Wound dressing | [225] |
| Carboxyethyl chitosan (CE)/PVA nanofiber mats | Electrospinning of aqueous CE-chitosan/PVA solution | * CE-chitosan/PVA nanofiber mat was nontoxic to the L929 cells * good in promoting the L929 cell attachment and proliferation | Skin regeneration and healing | [226] |
| PVA/quaternary chitosan (Q-chitosan mats | Photo-crosslinking electrospinning technique | * efficient inhibition toward growth of Gram-positive and Gram-negative bacteria | Wound dressing applications | [227] |
| Q-chitosan/polyaniline/ oxidized dextran (DEX) | Lyophilization | High antibacterial activity and enhanced proliferation of C2C12 myoblasts | In situ forming antibacterial and electroactive hydrogels | [228] |
| Quaternary ammonium chitosan/PVA hydrogels | Gamma irradiation, at different radiation doses and for different polymer ratios | * very good swelling ability (1000–4000%), water evaporation rate and mechanical properties * for doses <40 kGy, the tensile strength increases with increasing the radiation dose * higher crosslinking degree of the hydrogel with increasing the radiation dose * for doses >40 kGy, the hydrogel degraded * inhibition of the growth of Staphylococcus aureus and Escherichia coli | Antimicrobial system | [229] |
| Poly-4-styrenesulfonic acid/methacrylated glycol CS (MeGC) hydrogel or poly-vinylsulfonic acid/MeGC | Photo-crosslinking | * the initial burst was decreased after adding PSS or PVSA * higher human bone morphogenetic protein-2 (BMP-2)-induced osteogenesis differentiation | Efficient protein delivery | [230] |
| pH and temperature dual-sensitive hydrogel between glycol chitosan and benzaldehyde-modified Pluronic | Schiff base reaction | in physiological conditions, it was obtained the release of doxorubicin (DOX) and prednisolone from the hydrogels, without any initial burst release | Drug delivery system | [231] |
| Thermo-responsive Pluronic grafted CS hydrogel | Grafting of Pluronic onto chitosan using EDC/NHS chemistry | * higher mechanical properties than Pluronic hydrogels * in vitro culture of bovine chondrocytes in the hydrogel showed that the cell number and synthesized glycosaminoglycan (GAG) increased spontaneously over a period of 28 days | Cartilage regeneration | [232] |
| CS-Pluronic nano-hydrogel with targeting peptides | Photo-crosslinking | * high accumulation efficiency in brain tissues | Delivery of β-galactosidase to brain | [233] |
| CS-Pluronic hydrogels with encapsulated recombinant human epidermal growth factor (rhEGF) | Photo-croslinking | * the release of rhEGF is highly related to the degradation rate of the hydrogels * difference in rhEGF release patterns within 1 day, for different photoirradiation time (2 min–5 min) * epidermal differentiation is highly enhanced * good muco-adhesive property with animal skins | Wound curing | [234] |
| Semi-interpenetrating polymer network CS/ PEG/acrylamide (AAm) hydrogels | Chemical crosslinking | * increase of the protein half-life * improvement of the CS biocompatibility * increasing PEG content increased the swelling ratio, protein loading capacity, and entrapment efficiency | Closed-loop insulin delivery | [235] |
| Methacrylate derivative of CS/poly(ethylene oxide diacrylate) (PEODA) | Photo-crosslinking (intensity of UV light ≈ 10 mW/cm2, at a wavelength of 365 nm) | * good mechanical strength * degradation of the gels in the presence of chondroitinase enzyme in a dose-response manner * no degradation in the absence of the enzyme * compatibility with chondrocytes | Cartilage tissue engineering | [236] |
| Hyaluronic acid-based hybrid hydrogels | ||||
| Maleiated HA/thiol-terminated PEG | Mould-casting | quick gelation, porous structures, tunable degradation, and cytocompatibility with L929 cells | In situ formed scaffolds for tissue engineering | [237] |
| HA/PEG-diacrylate coencapsulated with TGF-β-3 | Photo-crosslinking | Cartilage differentiation | Cartilage tissue engineering | [238] |
| Injectable hydrogels of thiolated HA and 4-arm PEG-vinyl sulfone | Michael-type addition reaction | * gelation time decreased with the increase in the molecular weight (45–185 kDa) of HA * degradation time increased (15 days) with the molecular weight of HA and its degree of substitution * degradation in the presence of chondrocytes increased after 14 and 21 days, maybe due to the production of hyaluronidase enzyme by the incorporated chondrocytes | Cartilage tissue engineering | [79] |
| Methacrylated HA/N-vinyl pyrrolidone, using Alg as a temporal spherical mold | Photo-polymerization (long wavelength UV, 7W/cm2—intensity) | * degradable in the presence of hyaluronidase enzyme | Cartilage tissue engineering | [239] |
| Hybrid injectable hydrogel, consisting of deferoxamine-loaded poly(lactic-co-glycolic acid) nanoparticles (NPs) incorporated into a HA/CS hydrogel | Physical crosslinking | * angiogenesis was induced by deferoxamine drug release, but also by the presence of HA/CS hydrogel * cytocompatibility and cell proliferation * maximal blood vessels formation * beneficial effect of deferoxamine for neovascularization after 28 days when compared to HA/CS hydrogel | Suitable support for microvascular extension | [240] |
| Hydrogels of HA with thermosensitive poly(N-isopropyl acrylamide-co-acrylic acid), incorporated with dexamethasone and growth factor TGF β-3 | Temperature-induced crosslinking | * enhancement of chondrogenic differentiation and expression of aggregan, collagen type I and type II | Injectable tissue engineering construct for cartilage repair | [241] |
| Xanthan gum-based hybrid hydrogels | ||||
| PVA and xanthan gum (XG), in different molar ratios | Crosslinking, using trisodium trimetaphosphate | * for a molar ratio of 4:1 between PVA and XG, mechanical, swelling, and thermal properties superimposed with those of human nucleus pulposus (HNP) tissue * the hydrogels did not show any signs of cytotoxicity towards mouse fibroblasts (NIH3T3) | Good candidate as a potential HNP substitute | [242] |
| Hybrid (chitosan-g-glycidyl methacrylate) (CS–g–GMA)/xanthan hydrogel | Dissolved CS-g-GMA was mixed with the xanthan solution, under nitrogen gas flow, while keeping the temperature at 50 ± 1 °C under constant magnetic agitation | viability of fibroblasts when cultured onto the synthesized hydrogels | Potential for use in biomedical engineering applications | [243] |
| Heparin based hybrid hydrogels | ||||
| Hep/PEG hybrid gels | UV-initiated thiolene reaction between thiolated Hep and diacrylated poly(ethylene) glycol (PEG-DA) | * hepatocyte growth factor (HGF) was retained after 5 days in the hybrid Hep/PEG hydrogel microstructures, but was rapidly released from pure PEG gel microstructures * hepatocytes residing next to Hep/PEG hydrogels were producing ∼4 times more albumin at day 7, compared to cells cultured next to inert PEG hydrogels | * Designing cellular microenvironment in vitro * Vehicles for cell transplantation in vivo | [244] |
| Hep-based hydrogel system, formed by thiolated heparin and diacrylated PEG | Michael-type addition reaction | * encapsulation by the Hep -based hydrogel did not affect the chondrocyte viability (better than calcium-induced alginate gel) * hydrogel promoted chondrocyte proliferation, while maintaining chondrogenic nature | Promising material for chondrocyte culture, potentially applicable for cartilage regeneration | [245] |
| Hep/acrylated PEG hydrogel, with rat hepatocytes entrapped | Michael-type addition reaction | * the hydrogel was non-cytotoxic to cells, and promoted the hepatic function * hepatocytes entrapped in the Hep-based hydrogel maintained high levels of albumin and urea synthesis after three weeks in culture * hepatocyte growth factor (HGF) incorporated in the hydrogel was released in a controlled manner (only 40% of GF molecules released after 30 days in culture) | Good characteristics for matrices for in vitro differentiation of hepatocytes or stem cells and as vehicles for transplantation of these cells | [246] |
| Hep-based hydrogel sheet containing thiolated Hep and diacrylated PEG | Photo polymerization | * in vitro sustained release profile of human epidermal growth factor (hEGF) loaded in the hydrogel * acceleration of the wound healing after application of the hydrogels * advanced granulation tissue formation, capillary formation, and epithelialization in wounds treated by hEGF loaded Hep-based hydrogel | Wound healing | [247] |
| Hep-poloxamer/decellular spinal cord extracellular matrix (dscECM), used for fibroblast growth factor-2 (FGF2) attachment | EDC/NHS method | * treatment with FGF2-dscECM-HP hydrogel induced the recovery of the neuron functions and tissue morphology in rats that suffered from spinal cord injury (SCI) | Delivery of macromolecular proteins | [248] |
| Natural Polymer | Synthetic Polymer | Preparation Procedure | Crosslinker (If Applicable) | Properties/Applications | References |
|---|---|---|---|---|---|
| Bone tissue engineering | |||||
| Gelatin | PEGDA | Polymerization by light curing | No crosslinker | Biodegradable hydrogel for the delivery of small molecules, including a Pyk2-targeted inhibitor, in the treatment of craniofacial and appendicular skeletal defects, promoting osteoblast activity and mineral deposition | [346] |
| Methacrylated gelatin | PEGDA | UV photo-crosslinking | No crosslinker | Mouse osteoblasts culture on the hydrogel surface showed high viability, adhesion, and proliferation | [347] |
| Cartilage tissue engineering | |||||
| Gelatin, alginate | PHEMA | PHEMA-gelatin forms a gel after adding GA and ammonium persulfate (APS)/TEMED (free-radical polymerization initiator), and the reaction between the aldehyde groups of the oxidized alginate and the amino group of the gelatin might be due to a Schiff-base reaction | GA | IPN sodium alginate in HEMA-gelatin scaffolds that promotes the proliferation of chondrocytes | [348] |
| Gelatin | Pluronic | Graft copolymerization | EDC/NHS as a coupling reagent | Thermosensitive injectable cell-containing scaffold with thermally reversible properties and good biocompatibility | [349] |
| Methacrylated gelatin | PAAm | Co-polymerization of acrylamide (AAm) and methacrylated gelatin under UV radiation in the presence of a photo-initiator | No crosslinker | Biodegradable hydrogel with sustained growth factors release in articular cartilage defect repair | [350] |
| Gelatin | Three-block PCL-PEG-PCL and penta block PNIPAAm-PCL-PEG-PCL-PNIPAAm copolymers | TIPS (thermally induced phase separation) method using span-80 as an emulsifier | GA | Biodegradable thermosensitive hydrogel scaffolds | [351] |
| Fish skin gelatin | Poloxamer 407 | FT method | GA | Cryogel used in the regeneration of the nucleus pulposus | [352] |
| Wound healing | |||||
| Type I Collagen from bovine skin | PVA | Crosslinking | GA | Biohybrid sponge loaded with indomethacin, a non-steroidal anti-inflammatory drug | [353] |
| Human-like collagen (HLC) | PVA | Repeated FT where Tween80 was used as pore forming agent | No crosslinker | Soft, translucent, flexible hydrogels with smooth surfaces accelerating wound recovery through upregulating the expression of main growth factors of VEGF and TGF-β | [354] |
| Soy protein (SP) | Poly (ethylene terephthalate) (PET) AAc | Radical graft polymerization of AAc on the surface of PET fabric, and then the carboxyl groups available in the structure of AAc were activated using 1-ethyl-3-(3-dimethylaminopropyl) carbodiimide (EDAC) and then SPI was covalent coated on the surface of PET fabric | EDAC | Gabapentin loaded hydrogel as dressing for highly exudate wounds (diabetic ulcer) with neuropathic pain | [355] |
| SP | PEG | Condensation reaction between the carbonated moieties of PEG and amino groups of SP forming stable urethane linkages with subsequent release of p-nitrophenol molecules | No crosslinker | Safe and inflammatory inert moist transdermal drug delivery system for wound healing | [356] |
| Drugs and molecules delivery | |||||
| Acidic Type I Collagen from calf skin | PVP | γ–irradiation in the absence of oxygen | No crosslinker | Superabsorbent hydrogels | [357] |
| Hydrolyzed Collagen with low molecular weight | Poly[(acrylic acid)-co-(methacrylic acid)] (poly(AA-co-MAA)) | Graft polymerization with APS/TEMED initiator couple | N,N′-methylenebisacrylamide | pH- and thermo sensible hydrogels for oral delivery of insulin and methylene blue | [358] |
| Porcine Type I Collagen modified with γ-thiobutyrolactone to introduce thiol groups | 8-arm PEG-maleimide | Thiol-Michael addition click reaction | No crosslinker | Injectable hydrogels for cell delivery | [359] |
| Gelatin | poly(3-hydroxybutyrate) (PHB) | Physical gelation (due to the formation of triple helices at low temperatures) or chemical cross-linking (gelatin enzymatically cross-linked with TG), and embedded with drug loaded PHB nanoparticles prepared by the solvent displacement method | Natural enzyme microbial transglutaminase (TG) | Physical or chemical nanocomposite injectable hydrogels for the dual sustained release of naproxen sodium and curcumin | [360] |
| Methacrylated gelatin | Carboxybetaine methacrylate (CBMA) | Polymerization of vinyl groups of methacrylated gelatin and CBMA initiated by APS and TEMED | No crosslinker | Slow degradable hydrogels for fluorescein isothiocyanate-dextran release | [361] |
| Gelatin methacrylate | MAA | Gelatin methacrylate copolymerized with MAA by a free polymerization in the presence of KPS and ethylene glycol dimethacrylate (EGDMA) | NHS/EDC zero length crosslinker for GS link to polymeric back bone | pH sensitive hydrogel with controlled delivery of Gentamicin and Ampicillin antibiotics; GS, chemically conjugated to the polymer using amide linkage, leads to the slow release of it and high stability over long period | [362] |
| Gelatin | PLGA(lactide:glycolide 75:25) | Double water-in-oil-in-water(w/o/w) emulsification-solvent evaporation | No crosslinker | Injectable core/shell microspheres with gel inner phase for controllable release of Losartan potassium | [363] |
| Feather Keratin (FK) | Poly(methacrylic acid) (PMAA) | After the addition of the monomer (MAA) and crosslinker (BIS), and initiation with APS, the PMAA chains were grafted on the thiol group of the FK chains by grafting copolymerization | N,N-Methylene bisacrylamide (BIS) | pH-sensitive hydrogel for small molecule (rhodamine B) and macromolecule (BSA) release | [364] |
| SP | Poly(N-isopropylacrylamide-co-sodium acrylate) | Interpenetrating polymer network (IPN) method in the presence of APS/TEMED | GA for soy protein crosslinking and BIS for NIPAAm and AA crosslinking | pH- and temperature-responsive IPN hydrogels for BSA release | [365] |
| SPI | PAA | Covalent linking by Schiff base reaction of peptides from SPI with PAA (in the presence of GA) or self-assembly by noncovalent hydrophobic interactions (without GA) | With or without GA | Drug sustained release hydrogels for globular proteins (BSA) with excellent pH sensitivity, good water uptake, and high capacity of BSA absorption | [366] |
| SP | AAc Carbopol MBA AAm | Chemical crosslinking by copolymerization to obtain SPI-carbopol-PAAm hydrogels (in the presence of TEMED/KPS redox initiator) | No crosslinker | Dual (chloroquine diphosphate and curcumin) pH sensitive release hydrogels for antimalaria infection | [367] |
| Brain injury | |||||
| Keratin | PNIPAAm | Oxidative crosslinking method via the thiol-ene ‘click’ reaction between thiol group of the keratin and the ethylene bond of the NIPAAm | No crosslinker | Deferoxamine mesylate loaded thermo-sensitive injectable hydrogel for iron-induced brain injury after intracerebral hemorrhage (ICH); they can fill up the complex shapes of lesion cavities easily due to the sol-gel transition, which provided faster iron adsorption speed, and then relieving the iron overload and brain damage after ICH | [368] |
| Soy protein (SP) | PU | Mixing of PU nanoparticles dispersion (which is stable in water because of the negative charge of dissociated hydrophilic -COOH group) with protein solution in order to shorten the gelation time; the exact interaction between SPI and PU is not specified | No crosslinker | Hybrid thermo-responsive 3D bioprinting ink in neural tissue engineering | [331] |
| Type I Collagen from rat tail | Block copolymer of polypyrrole (PPy), conducting polymer, and PCL | Bioprinting | No crosslinker | Biodegradable and conductive hydrogel for neural tissue engineering | [369] |
| Protein | Synthetic Polymer | Synthesis | Crosslinker (If Applicable) | Application | References |
|---|---|---|---|---|---|
| Type I Collagen from pig skin | PHEMA | PHEMA matrix with inter-connected porous microstructure fabricated by a paraffin template method, which was then used as substrate to adhere collagen fibers to prepare the hydrogel | Without chemical crosslinker | Artificial cornea skirt | [370] |
| Type-I Collagen from bovine | Polyurethane-urea (PUU) | PUU fibrous membrane is fabricated by electrospinning, then PUU is coated by collagen and formed the hydrogel after soaking in collagen solution | Without chemical crosslinker | Urological tissue engineering | [371] |
| Type I Collagen from porcine skin | PVP, a spinnable polymer | Electrospinning. The collagen core was formed by gelation in basic conditions and the shell was PVP | Without chemical or thermal crosslinker | Artificial blood vessels | [372] |
| Gelatin | PNIPAAm | Interpenetrating cryogels | GA | Liver disease modeling (mimic the ECM stiffness of various disease stages of different tissues) | [373] |
| SP | Hydrolyzed polyacrylonitrile (PAN) | Wet-spinning method | GA | Smart artificial muscle with dynamic elongation /contraction pH responsiveness | [374] |
| SP | PEG | Cross-linking with amino and hydroxyl groups in the macromolecular chains of SP | Epichlorohydrin | Smart microsensor and actuator | [330] |
| Gelatin | PPy | Polymerization by FT | GA | 3-D cryogel matrix for peripheral nerve regeneration | [375] |
| SF | PAAm | In situ radical polymerization using ammonia persulfate as a initiator | bis-acrylamide (bis-AM) | Peripheral nerve regeneration | [376] |
| CaM | PEGDA | CaM with two mutated cysteins residues was reacted with PEGDA under UV radiation | No crosslinker | Intelligent actuator hydrogel based on conformational change of CaM in the presence of the ligand leading to a subsequent change in hydrogel volume | [377] |
| Lysozyme | 4-arm-PEG succinimidyl (4-arm-PEG-NHS) | Lysozyme offers free amine groups to rapidly crosslink with PEG | Ethylene diamine tetraacetic acid (EDTA) as an additive | In situ formation of antibacterial cardiothoracic surgical sealants to stop internal fluids leakage | [378] |
| Phase | Hybrid Nanogel/Hydrogel | Application | References |
|---|---|---|---|
| Preclinical | Cholesterol-bearing pullulan (CHP)-W9-peptide | Bone loss disorder | [458] |
| Acryloyl group-modified cholesterol-bearing pullulan and pentaerythritol tetra (mercaptoethyl) polyoxyethylene | Tissue engineering | [159] | |
| Pullulan-g-poly(l-lactide) copolymers | Anticancer drug delivery carrier | [150] | |
| Acrylate group-modified cholesterol-bearing pullulan nanogel (CHPANG) with thiol group-modified poly (ethylene glycol) | Protein delivery | [157] | |
| Clinical | CHP | Vaccines | [459,460,461,462] |
| BioAquacareTM—a novel soft hydrogel based on the poly(ethylene glycol)–soyprotein conjugates | Wound dressing material assessed in partial- and full-thickness wounds in pigs | [463] |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Vasile, C.; Pamfil, D.; Stoleru, E.; Baican, M. New Developments in Medical Applications of Hybrid Hydrogels Containing Natural Polymers. Molecules 2020, 25, 1539. https://doi.org/10.3390/molecules25071539
Vasile C, Pamfil D, Stoleru E, Baican M. New Developments in Medical Applications of Hybrid Hydrogels Containing Natural Polymers. Molecules. 2020; 25(7):1539. https://doi.org/10.3390/molecules25071539
Chicago/Turabian StyleVasile, Cornelia, Daniela Pamfil, Elena Stoleru, and Mihaela Baican. 2020. "New Developments in Medical Applications of Hybrid Hydrogels Containing Natural Polymers" Molecules 25, no. 7: 1539. https://doi.org/10.3390/molecules25071539
APA StyleVasile, C., Pamfil, D., Stoleru, E., & Baican, M. (2020). New Developments in Medical Applications of Hybrid Hydrogels Containing Natural Polymers. Molecules, 25(7), 1539. https://doi.org/10.3390/molecules25071539







