Gastrin and the Moderate Hypergastrinemias
Abstract
:1. Introduction
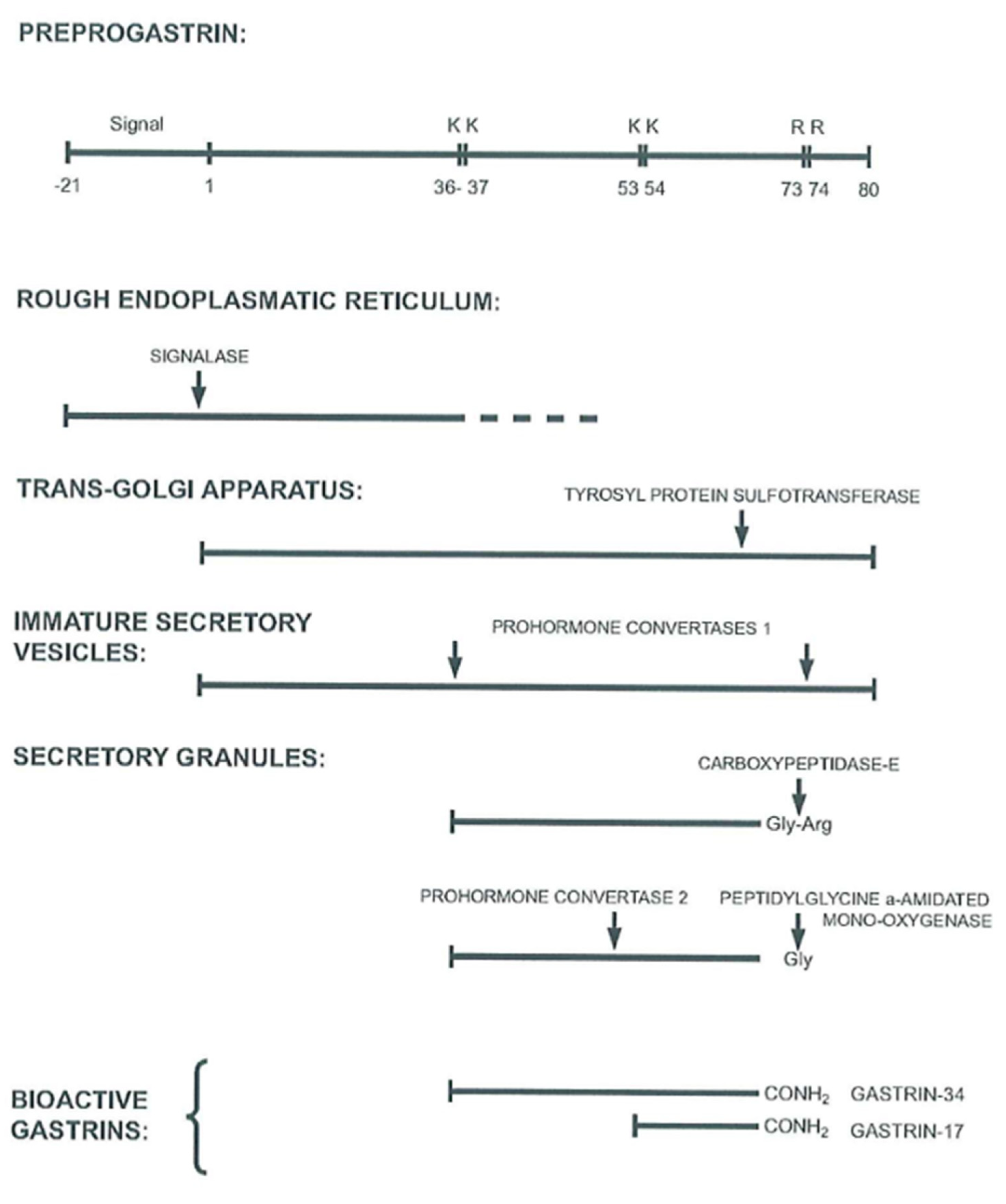
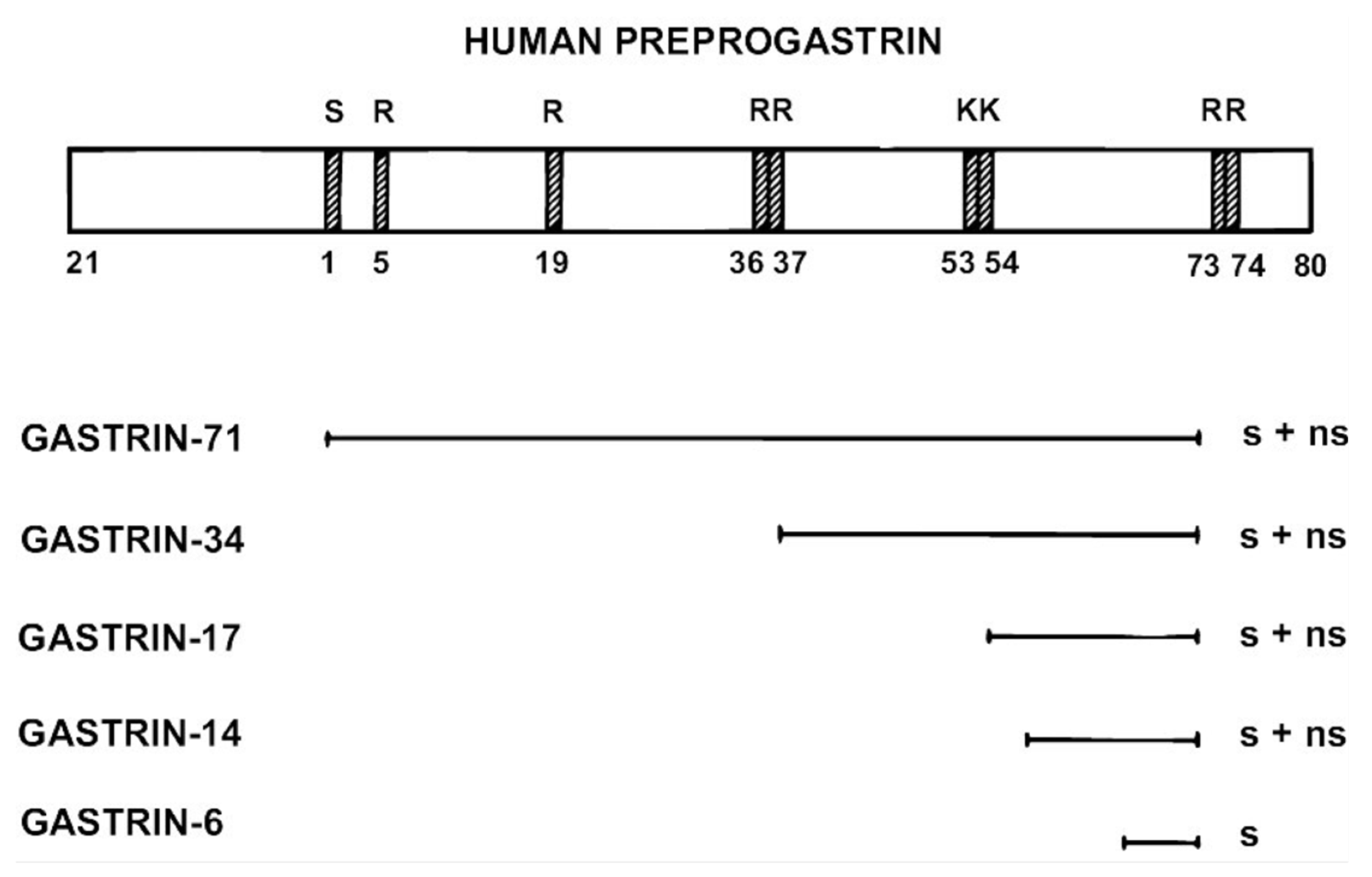
2. G Cell Synthesis of Gastrin
3. Extraintestinal Gastrin Expression
4. Plasma Pattern and Concentration Levels of Gastrin in Hypergastrinemia
5. Measurement of Gastrin in Plasma
6. Helicobacter pylori-Induced Hypergastrinemia
7. Proton-Pump Inhibitor-Induced Hypergastrinemia
8. Problem with Commercial Gastrin Kits
9. Conclusions
Funding
Institutional Review Board Statement
Informed Consent Statement
Acknowledgments
Conflicts of Interest
References
- Waldum, H.L.; Kleveland, P.M.; Fossmark, R. Upper gastrointestinal physiology and diseases. Scand. J. Gastroenterol. 2015, 50, 649–656. [Google Scholar] [CrossRef]
- Schubert, M.L.; Rehfeld, J.F. Gastric peptides—Gastrin and somatostatin. Compr. Physiol. 2020, 10, 197–228. [Google Scholar]
- Koh, T.J.; Goldenring, J.R.; Ito, S.; Mashimo, H.; Kopin, A.S.; Varro, A.; Dockray, G.J.; Wang, T.C. Gastrin deficiency results in altered gastric differentiation and decreased colonic proliferation in mice. Gastroenterology 1997, 113, 1015–1025. [Google Scholar] [CrossRef]
- Friis-Hansen, L.; Sundler, F.; Li, Y.; Gillespie, P.J.; Saunders, T.L.; Greenson, J.K.; Owyang, C.; Rehfeld, J.F.; Samuelson, L.C. Impaired gastric acid secretion in gastrin-deficient mice. Am. J. Physiol. 1998, 274, G561–G568. [Google Scholar] [CrossRef]
- Zavros, Y.; Eaton, K.A.; Kang, W.; Rathinavelu, S.; Katukuri, V.; Kao, J.Y.; Samuelson, L.C.; Merchant, J.L. Chronic gastritis in the hypochlorhydric gastrin-deficient mouse progresses to adenocarcinoma. Oncogene 2005, 24, 2354–2366. [Google Scholar] [CrossRef] [Green Version]
- Friis-Hansen, L.; Rieneck, K.; Nilsson, H.O.; Wadström, T.; Rehfeld, J.F. Gastric inflammation, metaplasia, and tumor development in gastrin-deficient mice. Gastroenterology 2006, 131, 246–258. [Google Scholar] [CrossRef]
- Jensen, R.T. Recent insights from studies of gastrinomas. In Gastrin in the New Millennium; Merchant, J.L., Buchan, A.M.J., Wang, T.C., Eds.; CURE Foundation: Los Angeles, CA, USA, 2004; pp. 339–352. [Google Scholar]
- Rehfeld, J.F.; Gingras, M.H.; Bardram, L.; Hilsted, L.; Goetze, J.P.; Poitras, P. The Zollinger-Ellison syndrome and mismeasurement of gastrin. Gastroenterology 2011, 140, 1444–1453. [Google Scholar] [CrossRef] [PubMed]
- Rehfeld, J.F.; van Solinge, W.W.; Tos, M.; Thomsen, J. Gastrin, cholecystokinin and their precursors in acoustic neuromas. Brain Res. 1990, 530, 235–238. [Google Scholar] [CrossRef]
- Rehfeld, J.F.; Bardram, L.; Hilsted, L. Gastrin in human bronchogenic carcinomas: Constant expression but variable processing of progastrin. Cancer Res. 1989, 49, 2840–2843. [Google Scholar] [PubMed]
- Van Solinge, W.W.; Nielsen, F.C.; Friis-Hansen, L.; Falkmer, U.G.; Rehfeld, J.F. Expression but incomplete maturation of progastrin in colorectal carcinomas. Gastroenterology 1993, 104, 1099–1107. [Google Scholar] [CrossRef]
- Van Solinge, W.W.; Ødum, L.; Rehfeld, J.F. Ovarian cancers express and process progastrin. Cancer Res. 1993, 53, 1823–1828. [Google Scholar]
- Goetze, J.P.; Nielsen, F.C.; Burcharth, F.; Rehfeld, J.F. Closing the gastrin loop in pancreatic carcinoma: Coexpression of gastrin and its receptor in solid human pancreatic adenocarcinoma. Cancer 2000, 88, 2487–2494. [Google Scholar] [CrossRef]
- Goetze, J.P.; Eiland, S.; Svendsen, L.B.; Vainer, B.; Hannibal, J.; Rehfeld, J.F. Characterization of gastrins and their receptor in solid human gastric adenocarcinomas. Scand. J. Gastroenterol. 2013, 48, 688–695. [Google Scholar] [CrossRef]
- Gregory, H.; Hardy, P.M.; Jones, D.S.; Kenner, G.W.; Sheppard, R.C. The antral hormone gastrin. I. Structure of gastrin. Nature 1964, 204, 931–933. [Google Scholar] [CrossRef]
- Rehfeld, J.F.; Stadil, F.; Baden, H.; Fischerman, K. The enteral insulin-stimulation after Whipple’s operation. Diabetologia 1975, 11, 207–210. [Google Scholar] [CrossRef] [Green Version]
- Rehfeld, J.F. Disturbed islet-cell function related to endogenous gastrin release. Studies on insulin secretion and glucose tolerance in pernicious anemia. J. Clin. Investig. 1976, 58, 41–49. [Google Scholar] [CrossRef]
- Levi, S.; Beardshall, K.; Haddad, G.; Playford, R.; Ghosh, P.; Calam, J. Campylobacter pylori and duodenal ulcers: The gastrin link. Lancet 1989, 1, 1167–1168. [Google Scholar] [CrossRef]
- Moss, S.F.; Calam, J. Acid secretion and sensitivity to gastrin in patients with duodenal ulcer: Effect of eradication of Helicobacter pylori. Gut 1993, 34, 888–892. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Olbe, L.; Hamlet, A.; Dalenbäck, J.; Fändriks, L. A mechanism by which Helicobacter pylori infection of the antrum contributes to the development of duodenal ulcer. Gastroenterology 1996, 110, 1386–1394. [Google Scholar] [CrossRef] [PubMed]
- Graham, D.Y.; Go, M.F.; Lew, G.M.; Genta, R.M.; Rehfeld, J.F. Helicobacter pylori infection and exaggerated gastrin release. Effects of inflammation and progastrin processing. Scand. J. Gastroenterol. 1993, 28, 690–694. [Google Scholar] [CrossRef] [PubMed]
- Ødum, L.; Petersen, H.D.; Andersen, I.B.; Hansen, B.F.; Rehfeld, J.F. Gastrin and somatostatin in Helicobacter pylori infected antral mucosa. Gut 1994, 35, 615–618. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Zavros, Y.; Rieder, G.; Ferguson, A.; Samuelson, L.C.; Merchant, J.L. Hypergastrinemia in response to gastric inflammation suppresses somatostatin. Am. J. Physiol. Gastrointest. Liver Physiol. 2002, 282, G175–G183. [Google Scholar] [CrossRef] [PubMed]
- Smolka, A.J.; Schubert, M.L. Helicobacter pylori-induced changes in gastric acid secretion and upper gastrointestinal disease. Curr. Top. Microbiol. Immunol. 2017, 400, 227–252. [Google Scholar]
- Swarovsky, B.; Eissele, R.; Gross, M.; Körtner, G.; Koop, H.; Arnold, R.; Simon, B. Expression of the gastric H+/K+-ATPase and histidine decarboxylase during omeprazole treatment. Digestion 1994, 55, 97–102. [Google Scholar] [CrossRef]
- Waldum, H.L.; Arnestad, J.S.; Brenna, E.; Eide, I.; Syversen, U.; Sandvik, A.K. Marked increase in gastric acid secretory capacity after omeprazole treatment. Gut 1996, 39, 649–653. [Google Scholar] [CrossRef] [Green Version]
- Xu, G.; Sumi, S.; Koike, M.; Tanigawa, K.; Nio, Y.; Tamura, K. Role of endogenous hypergastrinemia in regenerating endocrine pancreas after partial pancreatectomy. Dig. Dis. Sci. 1996, 41, 2433–2439. [Google Scholar] [CrossRef]
- Williams, M.P.; Sercombe, J.; Hamilton, M.I.; Pounder, R.E. A placebo-controlled trial to assess the effects of 8 days of dosing with rabeprazole versus omeprazole on 24-h intragastric acidity and plasma gastrin concentrations in young healthy male subjects. Aliment. Pharmacol. Ther. 1998, 12, 1079–1089. [Google Scholar] [CrossRef]
- Sanduleanu, S.; Stridsberg, M.; Jonkers, D.; Hameeteman, W.; Biemond, I.; Lundqvist, G.; Lamers, C.; Stockbrügger, R.W. Serum gastrin and chromogranin A during medium- and long-term acid suppressive therapy: A case-control study. Aliment. Pharmacol. Ther. 1999, 13, 145–153. [Google Scholar] [CrossRef] [Green Version]
- Bardhan, K.D.; Cherian, P.; Bishop, A.E.; Polak, J.M.; Romanska, H.; Perry, M.J.; Rowland, A.; Thompson, M.; Morris, P.; Schneider, A.; et al. Pantoprazole therapy in the long-term management of severe acid peptic disease: Clinical efficacy, safety, serum gastrin, gastric histology, and endocrine cell studies. Am. J. Gastroenterol. 2001, 96, 1767–1776. [Google Scholar] [CrossRef]
- Fossmark, R.; Johnsen, G.; Johanessen, E.; Waldum, H.L. Rebound acid hypersecretion after long-term inhibition of gastric acid secretion. Aliment. Pharmacol. Ther. 2005, 21, 149–154. [Google Scholar] [CrossRef] [PubMed]
- Hove, K.D.; Brøns, C.; Færch, K.; Lund, S.S.; Petersen, J.S.; Karlsen, A.E.; Rossing, P.; Rehfeld, J.F.; Vaag, A. Effects of 12 weeks’ treatment with a proton pump inhibitor on insulin secretion, glucose metabolism and markers of cardiovascular risk in patients with type 2 diabetes: A randomised double-blind prospective placebo-controlled study. Diabetologia 2013, 56, 22–30. [Google Scholar] [CrossRef]
- Gould, E.; Clements, C.; Reed, A.; Giori, L.; Steiner, M.J.; Lidbury, J.A.; Suchodolski, J.S.; Brand, M.; Moyers, T.; Emery, L. A Prospective, placebo-controlled pilot evaluation of the effect of omeprazole on serum calcium, magnesium, cobalamin, gastrin concentrations, and bone in cats. J. Vet. Intern. Med. 2016, 30, 779–786. [Google Scholar] [CrossRef]
- Brand, S.J.; Klarlund, J.; Schwartz, T.W.; Rehfeld, J.F. Biosynthesis of tyrosine-0-sulfated gastrins in rat antral mucosa. J. Biol. Chem. 1984, 259, 13246–13252. [Google Scholar] [CrossRef]
- Hilsted, L.; Rehfeld, J.F. α-carboxyamidation of antral progastrin: Relation to other post-translational modifications. J. Biol. Chem. 1987, 262, 16953–16957. [Google Scholar] [CrossRef]
- Jensen, S.; Borch, K.; Hilsted, L.; Rehfeld, J.F. Progastrin processing during antral G-cell hypersecretion in humans. Gastroenterology 1989, 96, 1063–1070. [Google Scholar] [CrossRef]
- Rehfeld, J.F. The endoproteolytic maturation of progastrin and procholecystokinin. J. Mol. Med. 2006, 84, 544–550. [Google Scholar] [CrossRef] [PubMed]
- Rehfeld, J.F. The art of measuring gastrin in plasma: A dwindling diagnostic discipline? Scand. J. Clin. Lab. Investig. 2008, 68, 353–361. [Google Scholar] [CrossRef]
- Rehfeld, J.F.; Zhu, X.; Norrbom, C.; Bundgaard, J.R.; Johnsen, A.H.; Nielsen, J.E.; Vikesaa, J.; Stein, J.; Dey, A.; Steiner, D.F.; et al. Prohormone convertases 1/3 and 2 together orchestrate the site-specific cleavages of progastrin to release gastrin -34 and gastrin-17. Biochem. J. 2008, 415, 35–43. [Google Scholar] [CrossRef] [Green Version]
- Eipper, B.A.; Stoffers, D.A.; Mains, R.E. The biosynthesis of neuropeptides: Peptide alpha-amidation. Ann. Rev. Neurosci. 1992, 15, 57–85. [Google Scholar] [CrossRef]
- Dockray, G.J.; Varro, A.; Desmond, H.; Young, J.; Gregory, H.; Gregory, R.A. Posttranslational processing of the porcine gastrin precursor by phosphorylation of the COOH-terminal fragment. J. Biol. Chem. 1987, 262, 8643–8647. [Google Scholar] [CrossRef]
- Rehfeld, J.F.; Johnsen, A.H. Identification of gastrin component I as gastrin-71. The largest possible bioactive progastrin product. Eur. J. Biochem. 1994, 223, 765–773. [Google Scholar] [CrossRef] [PubMed]
- Rehfeld, J.F.; Hansen, C.P.; Johnsen, A.H. Post-poly(Glu) cleavage and degradation modified by O-sulfated tyrosine: A novel posttranslational processing mechanism. EMBO J. 1995, 14, 389–396. [Google Scholar] [CrossRef]
- Papay, K.D.; Falck, V.G.; Poulsen, S.S.; Pannaccione, R.; Rehfeld, J.F.; Storr, M.A. Juvenile polyposis of the stomach—A novel cause of hypergastrinemia. Nat. Rev. Gastroenterol. Hepatol. 2010, 7, 583–588. [Google Scholar] [CrossRef]
- Stadil, F.; Rehfeld, J.F.; Christiansen, L.A.; Malmstrøm, J. Patterns of gastrin components in serum during feeding in normal subjects and duodenal ulcer patients. Scand. J. Gastroenterol. 1975, 10, 863–868. [Google Scholar] [CrossRef]
- Malmstrøm, J.; Stadil, F.; Rehfeld, J.F. Gastrins in tissue: Concentration and component pattern in gastric, duodenal, and jejunal mucosa of normal human subjects and patients with duodenal ulcer. Gastroenterology 1976, 70, 697–704. [Google Scholar] [CrossRef]
- Lüttichau, H.R.; van Solinge, W.W.; Nielsen, F.C.; Rehfeld, J.F. Developmental expression of the gastrin and cholecystokinin genes in rat colon. Gastroenterology 1993, 104, 1092–1098. [Google Scholar] [CrossRef]
- Larsson, L.I.; Rehfeld, J.F.; Sundler, F.; Håkanson, R. Pancreatic gastrin in foetal and neonatal rats. Nature 1976, 262, 609–610. [Google Scholar] [CrossRef]
- Brand, S.J.; Andersen, B.N.; Rehfeld, J.F. Complete tyrosine-O-sulphation of gastrin in neonatal rat pancreas. Nature 1984, 309, 456–458. [Google Scholar] [CrossRef] [PubMed]
- Bardram, L.; Hilsted, L.; Rehfeld, J.F. Progastrin expression in mammalian pancreas. Proc. Natl. Acad. Sci. USA 1990, 87, 298–302. [Google Scholar] [CrossRef] [Green Version]
- Larsson, L.I.; Rehfeld, J.F. Pituitary gastrins occur in corticotrophs and melanotrophs. Science 1981, 213, 768–770. [Google Scholar] [CrossRef]
- Rehfeld, J.F.; Hansen, H.F.; Larsson, L.-I.; Stengaard-Pedersen, K.; Thorn, N.A. Gastrin and cholecystokinin in pituitary neurons. Proc. Natl. Acad. Sci. USA 1984, 81, 1902–1905. [Google Scholar] [CrossRef] [Green Version]
- Rehfeld, J.F. Accumulation of nonamidated preprogastrin and preprocholecystokinin products in porcine pituitary corticotrophs. Evidence of post-translational control of cell differentiation. J. Biol. Chem. 1986, 261, 5841–5847. [Google Scholar] [CrossRef]
- Rehfeld, J.F. Progastrin and its products in the cerebellum. Neuropeptides 1991, 20, 239–245. [Google Scholar] [CrossRef]
- Uvnäs-Wallensten, K.; Rehfeld, J.F.; Larsson, L.I.; Uvnäs, B. Heptadecapeptide gastrin in the vagal nerve. Proc. Natl. Acad. Sci. USA 1977, 74, 5707–5710. [Google Scholar] [CrossRef] [Green Version]
- Bardram, L.; Hilsted, L.; Rehfeld, J.F. Cholecystokinin, gastrin and their precursors in pheochromocytomas. Acta Endocrinol. 1989, 120, 479–484. [Google Scholar] [CrossRef] [PubMed]
- Schalling, M.; Persson, H.; Pelto-Huikko, M.; Ødum, L.; Ekman, P.; Gottlieb, C.; Hökfelt, T.; Rehfeld, J.F. Expression and localization of gastrin messenger RNA and peptide in spermatogenic cells. J. Clin. Investig. 1990, 86, 660–669. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Walsh, J.H.; Isenberg, J.I.; Ansfield, J.; Maxwell, V. Clearance and acid-stimulating action of human big and little gastrins in duodenal ulcer subjects. J. Clin. Investig. 1976, 57, 1125–1131. [Google Scholar] [CrossRef] [Green Version]
- Hansen, C.P.; Stadil, F.; Rehfeld, J.F. Metabolism and influence of gastrin-52 on gastric acid secretion in humans. Am. J. Physiol. 1995, 269, G600–G605. [Google Scholar] [CrossRef]
- Goetze, J.P.; Rehfeld, J.F. Impact of assay epitope specificity in gastrinoma diagnosis. Clin. Chem. 2003, 49, 333–334. [Google Scholar] [CrossRef] [Green Version]
- Blair, A.J.; Richardson, C.T.; Walsh, J.; Feldman, M. Variable contribution of gastrin to gastric acid secretion after a meal in humans. Gastroenterology 1987, 92, 944–949. [Google Scholar] [CrossRef]
- Sjöblom, S.M.; Sipponen, P.; Karonen, S.L.; Järvinen, H.J. Mucosal argyrophil endocrine cells in pernicious anemia and upper gastrointestinal carcinoid tumours. J. Clin. Pathol. 1989, 42, 371–377. [Google Scholar] [CrossRef] [Green Version]
- Kleveland, P.M.; Waldum, H.L.; Larsson, H. Gastric acid secretion in the totally isolated, vasculatory perfused rat stomach: A selectively muscarinic-1 agent does whereas gastrin does not augment maximal histamine-stimulated acid secretion. Scand. J. Gastroenterol. 1987, 22, 705–713. [Google Scholar] [CrossRef]
- Brenna, E.; Waldum, H.L. Trophic effect of gastrin on the enterochromaffin-like cells of the rat stomach: Establishment of a dose response relationship. Gut 1992, 33, 1303–1306. [Google Scholar] [CrossRef] [Green Version]
- McGuigan, J.E. Immunochemical studies with synthetic human gastrin. Gastroenterology 1968, 54, 1005–1011. [Google Scholar] [CrossRef]
- Yalow, R.S.; Berson, S.A. Radioimmunoassay of gastrin. Gastroenterology 1970, 58, 1–14. [Google Scholar] [CrossRef]
- Stadil, F.; Rehfeld, J.F. Radioimmunoassay of gastrin in human serum. Scand. J. Gastroenterol. 1971, 9, 61–65. [Google Scholar]
- Rehfeld, J.F.; Stadil, F.; Rubin, B. Production and evaluation of antibodies for the radioimmunoassay of gastrin. Scand. J. Clin. Lab. Investig. 1972, 30, 221–232. [Google Scholar] [CrossRef]
- Stadil, F.; Rehfeld, J.F. Determination of gastrin in serum. Scand. J. Gastroenterol. 1973, 8, 101–113. [Google Scholar] [CrossRef]
- Warren, J.R.; Marshall, B. Unidentified curved bacilli on gastric epithelium in active chronic gastritis. Lancet 1983, 1, 1273–1275. [Google Scholar]
- Marshall, B.J.; Goodwin, C.S.; Warren, J.R.; Murray, R.; Blincow, E.D.; Blackbourn, S.J.; Phillips, M.; Waters, T.E.; Sanderson, C.R. Prospective double-blind trial of duodenal ulcer relapse after eradication of Campylobacter pylori. Lancet 1988, 2, 1437–1442. [Google Scholar] [CrossRef]
- Feldman, M.; Cryer, B.; Lee, E. Effects of Helicobacter pylori gastritis on gastric secretion in healthy human beings. Am. J. Physiol. 1998, 274, G1011–G1017. [Google Scholar]
- Parsonnet, J.; Friedman, G.D.; Vandersteen, D.P.; Chang, Y.; Vogelman, J.H.; Orentreich, N.; Sibley, R.K. Helicobacter pylori infection and the risk of gastric carcinoma. N. Engl. J. Med. 1991, 325, 1127–1131. [Google Scholar] [CrossRef]
- Larsson, L.I.; Goltermann, N.; de Magistris, L.; Rehfeld, J.F.; Schwartz, T.W. Somatostatin cell processes as pathways for paracrine secretion. Science 1979, 205, 1393–1395. [Google Scholar] [CrossRef]
- Rehfeld, J.F.; Sennels, H.P.; Jørgensen, H.L.; Fahrenkrug, J. Circadian variations in plasma concentrations of cholecystokinin and gastrin in man. Scand. J. Clin. Lab. Investig. 2020, 80, 546–551. [Google Scholar] [CrossRef]
- El-Omar, E.M.; Penman, I.D.; Ardill, J.E.S.; Chitajallu, R.S.; Howie, C.; McColl, K.E.L. Helicobacter pylori infection and abnormalities in patients with duodenal ulcer disease. Gastroenterology 1995, 109, 681–691. [Google Scholar] [CrossRef]
- Hansky, J.; Cain, M.D. Radioimmunoassay of gastrin in human serum. Lancet 1969, 2, 1388–1390. [Google Scholar] [CrossRef]
- Rehfeld, J.F. To study the molecular nature of gastrin—And to know John Walsh: A flashback to the seventies. In Gut-Brain Peptides in the New Millenium: A tribute to John Walsh; Taché, Y., Goto, Y., Lloyd, K., Ohning, G., Yamada, T., Eds.; CURE Foundation: Los Angeles, CA, USA, 2002; pp. 11–21. [Google Scholar]
- Varro, A.; Ardill, J.E.S. Gastrin, an analytical review. Ann. Clin. Biochem. 2003, 40, 472–480. [Google Scholar] [CrossRef]
- Stadil, F. The measurement of gastrin. Scand. J. Clin. Lab. Investig. 2001, 61 (Suppl. 234), 129–132. [Google Scholar] [CrossRef]
- Murphy, G.; Abnet, C.C.; Choo-Wosoba, H.; Vogtmann, E.; Weinstein, S.J.; Taylor, P.R.; Männistö, S.; Albanes, D.; Dawsey, S.M.; Rehfeld, J.F.; et al. Serum gastrin and cholecystokinin are associated with subsequent development of gastric cancer in a prospective cohort of Finnish smokers. Int. J. Epidemiol. 2017, 46, 914–923. [Google Scholar] [CrossRef] [Green Version]
- Niikura, R.; Hayakawa, Y.; Hirata, Y.; Yamada, A.; Fujishiro, M.; Koike, K. Long-term proton pump inhibitor use is a risk factor of gastric cancer after treatment for Helicobacter pylori: A retrospective cohort analysis. Gut 2018, 67, 1908–1910. [Google Scholar] [CrossRef]
- Waldum, H.L.; Rehfeld, J.F. Gastric cancer and gastrin: On the interaction of Helicobacter pylori gastritis and acid inhibitory induced hypergastrinemia. Scand. J. Gastroenterol. 2019, 54, 1118–1123. [Google Scholar] [CrossRef] [PubMed]



| Category | Condition | Basal Plasma Concentration Levels (pmol/L) |
|---|---|---|
| Agastrinemia | Genetically modified animals | 0 |
| Hypogastrinemia | Antroduodenally resected patients Antro-mucosal atrophy patients | 0–5 |
| Normogastrinemia | Fasting normal subjects and mammals | 5–15 |
| Hypergastrinemia (I) (moderate) | Helicobacter pylori-infected subjects Proton-pump inhibitor-treated patients Early gastrinomas | 20–100 |
| Hypergastrinemia (II) (excessive) | Atrophic gastritis Gastrinomas with fulminant Zollinger–Ellison syndrome Gastric polyposis | >100 |
| Gastrinoma Patients | Amidated Gastrins (pmol/L) | Gastrin-17 (pmol/L) |
|---|---|---|
| 1 | 475 | 10 |
| 2 | 235 | 42 |
| 3 | 270 | 90 |
| 4 | 82 | 15 |
| 5 | 57 | 24 |
| 6 | 60 | 26 |
| 7 | 305 | 6 |
| Median | 235 | 24 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the author. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Rehfeld, J.F. Gastrin and the Moderate Hypergastrinemias. Int. J. Mol. Sci. 2021, 22, 6977. https://doi.org/10.3390/ijms22136977
Rehfeld JF. Gastrin and the Moderate Hypergastrinemias. International Journal of Molecular Sciences. 2021; 22(13):6977. https://doi.org/10.3390/ijms22136977
Chicago/Turabian StyleRehfeld, Jens F. 2021. "Gastrin and the Moderate Hypergastrinemias" International Journal of Molecular Sciences 22, no. 13: 6977. https://doi.org/10.3390/ijms22136977





