Abstract
Background: Atherosclerotic cardiovascular diseases are characterized by a dysregulated inflammatory and thrombotic state, leading to devastating complications with increased morbidity and mortality rates. Summary: In this review article, we present the available evidence regarding the impact of inflammation on platelet activation in atherosclerosis. Key messages: In the context of a dysfunctional vascular endothelium, structural alterations by means of endothelial glycocalyx thinning or functional modifications through impaired NO bioavailability and increased levels of von Willebrand factor result in platelet activation. Moreover, neutrophil-derived mediators, as well as neutrophil extracellular traps formation, have been implicated in the process of platelet activation and platelet-leukocyte aggregation. The role of pro-inflammatory cytokines is also critical since their receptors are also situated in platelets while TNF-α has also been found to induce inflammatory, metabolic, and bone marrow changes. Additionally, important progress has been made towards novel concepts of the interaction between inflammation and platelet activation, such as the toll-like receptors, myeloperoxidase, and platelet factor-4. The accumulating evidence is especially important in the era of the coronavirus disease-19 pandemic, characterized by an excessive inflammatory burden leading to thrombotic complications, partially mediated by platelet activation. Lastly, recent advances in anti-inflammatory therapies point towards an anti-thrombotic effect secondary to diminished platelet activation.
1. Introduction
Cardiovascular diseases, the leading cause of death worldwide, are governed by a dysregulated inflammatory and thrombotic milieu, stemming from the cluster of comorbidities that encompasses them, including obesity, diabetes mellitus, and arterial hypertension. Moreover, emotional, environmental, and lifestyle aspects have been implicated in sterile inflammation and atherosclerosis development and progression as additional deleterious risk factors [1,2,3,4].
Despite the progress that has been made towards the antithrombotic aspect [5,6], there is still a lot of ground to cover with regards to the management of low-grade systemic inflammation that has been proven to be a core element of the atherosclerotic process and the residual risk. The interaction of inflammation with platelets has also received scientific interest since several pro-inflammatory conditions and mediators have been associated with platelet activation. In this scoping review, we elaborate on the various inflammatory entities contributing to platelet activation (Figure 1), namely the dysfunctional endothelium, the interaction with leukocytes, and cytokines among others. Moreover, we delve into the platelet hyperactivation complicating the severe acute respiratory syndrome coronavirus-2 (SARS-CoV-2) infection and describe the current progress in the pharmacological management of thromboinflammation with a focus on platelet activation, including both currently available agents and novel molecules in the early phase of experimental development.

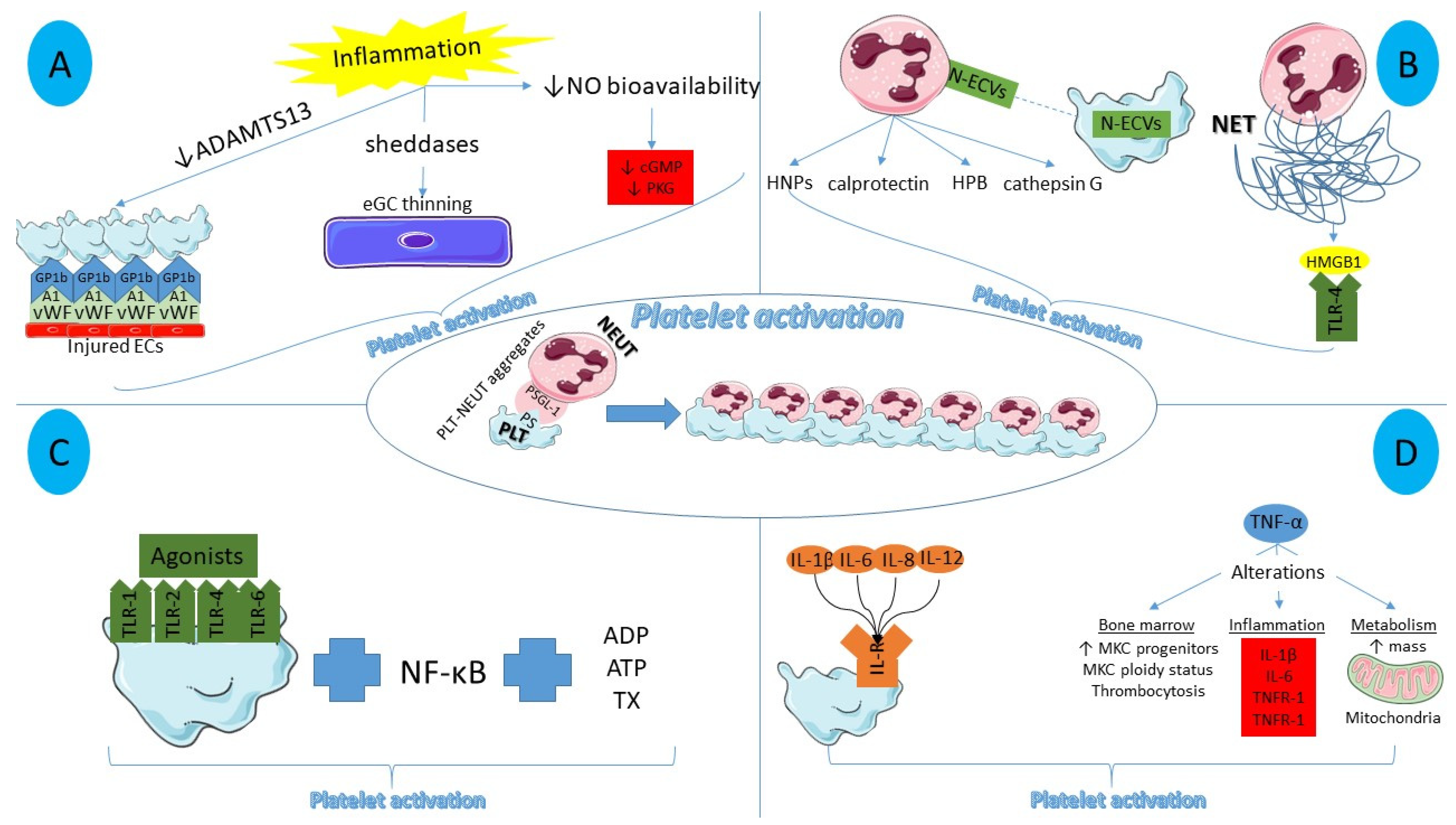
Figure 1.
Main inflammatory mediators of platelet activation. (A) Endothelial dysfunction in the setting of inflammation results in increased platelet–endothelial cell interactions, thinning of endothelial glycocalyx, and reduced nitric oxide bioavailability, contributing to platelet activation. (B) Neutrophil-derived molecules and extracellular vesicles aid platelet activation, together with the pro-thrombotic role of NET histones via a Toll-like receptor 4-related platelet activation. (C) Platelet toll-like receptors cannot directly induce platelet activation but they augment it, stimulated by NF-κB, thromboxane, adenosine diphosphate, and adenosine triphosphate. (D) Pro-inflammatory interleukins bind to interleukin receptors situated on the platelet surface while tumor necrosis factor-alpha promotes alterations in bone marrow, inflammation, and mitochondria, collectively facilitating platelet activation. ADAMTS13: A disintegrin-like and metalloprotease with thrombospondin type-1 repeats-13, NO: nitric oxide, EC: endothelial cells, eGC: endothelial glycocalyx, cGMP: cyclic guanyl monophosphate, PKG: protein kinase G, N-ECV: neutrophil extracellular vesicles, HNP: human neutrophil peptides, HBP: heparin binding protein, NET: neutrophil extraceullar trap, HMGB1: High mobility group box 1, TLR: toll-like receptor, ADP: adenosine diphosphate, ATP: adenosine triphosphate, TX: thromboxane, IL-R: interleukin receptor, MKC: megakaryocyte, TNFR: tumor necrosis factor receptor, PS: P Selectin, PSGL-1: P Selectin glycoprotein ligand-1, NEUT: neutrophil, PLT: platelet.
2. Inflammation and Platelet Activation
2.1. Endothelial Dysfunction and Platelet Activation
The vascular endothelium is a monolayer that consists of squamous cells lining the vessel wall, with a critical role in cardiovascular health. Among its well-described properties are the regulation of vascular tone, the control of cellular adhesion, the proliferation of smooth muscle cells, and the transport of macromolecules across the vessel wall [7]. Moreover, the endothelium acts in anti-thrombotic ways under physiologic situations, preventing platelet adherence and activation.
Several mechanisms have been implicated in this anti-platelet effect. Starting with the endothelial glycocalyx (eGC), its role in vascular integrity and endothelial activation has been recently characterized. The eGC is a 0.5–5 μm thick negatively charged endothelial cell cover floating into the vessel lumen that is composed of proteoglycans (syndecans, versicans), glycolipids, glycoproteins, and glycosaminoglycans (heparan sulfate, chondroitin sulfate, hyaluronan). Physiologically, the balance between the shedding of eGC components, the adsorption of circulating blood molecules, and the formation of novel constituents by endothelial cells leads to the stabilization of the eGC. However, in the setting of inflammation [8], increased shedding of eGC components, namely syndecan-1, hyaluronan, heparan sulfate, and chondroitin sulfate, is observed owing to the action of sheddases (matrix metalloproteinases, heparanase, hyaluronidase, angiopoietin 2) [9,10,11]. It has to been noted that molecules involved in thrombosis and fibrinolysis, such as plasmin and thrombin, have been found to cleave syndecan-4, thereby aiding the eGC degradation [12]. According to a recently reported study, versican might be the main eGC component that promotes an anti-platelet effect, in a dose-dependent manner [13]. Ultimately, increased platelet adhesion to the vessel wall is noted during the atherosclerotic process, owing to the eGC thinning (Figure 1A) [14], since its degradation aids the binding of leukocytes and platelets on the receptors of adhesion molecules and von Willebrand factor, which are consequently released by endothelial cells [15,16]. Additional functions of eCG have been described [17], including the binding of cytokines, the regulation of oxidative stress, and mechanotransduction.
Nitric oxide (NO) is an essential factor implicated in the regulation of platelet activation and aggregation as a physiologic inhibitor, through the activation of soluble guanylate cyclase. The resulting upregulation of intracellular cyclic guanosine monophosphate (cGMP) and protein kinase G (PKG) in platelets leads to lower intracellular calcium within platelets, an ion essential for platelet activation [18]. cGMP levels are also controlled by the platelet cGMP-specific phosphodiesterase type 5 (PDE5A) [19] but, in the absence of PKG, the effect of cGMP on intracellular Ca2+ is largely lost [20], depicted by increased platelet adhesion and aggregation [21]. In the presence of established cardiovascular risk factors (diabetes mellitus, arterial hypertension, dyslipidemia, smoking), the augmented oxidative stress leads to endothelial dysfunction [22]. In this setting, the low availability of NO due to its lower expression, increased degradation, and endothelial NO synthase (eNOS) uncoupling leads to enhanced peroxynitrite production, aiding the thrombotic process among others [23]. It is important to note that platelets are another source of NO as they also contain eNOS [24,25]. Even though the platelet NO production is of a lesser magnitude compared to endothelial cells [26], it is believed that its role is of greater importance as demonstrated in animal experiments [27,28].
Prostacyclin (PGI2) is another endothelial cell-derived molecule with a NO-synergistic effect towards lower platelet activity. By stimulating cell surface prostacyclin receptors, it provokes the activation of adenylate cyclase, the formation of cyclic adenosine monophosphate (cAMP), and the phosphorylation of protein kinase A, ultimately resulting in reduced platelet intracellular calcium [29]. It physiologically opposes the action of the prothrombotic thromboxane A2, which is also produced from endothelial cells apart from platelets [30,31]. The impaired homeostatic balance between PGI2 and thromboxane A2 additionally promotes a prothrombotic state in the setting of endothelial dysfunction.
Von Willebrand factor (vWF), a large multimeric glycoprotein (GP) produced mainly by the endoplasmic reticulum of endothelial cells and stored in the Weibel-Palade bodies [32], is another crucial element of hemostasis by aiding platelet adhesion through bonding of the active A1 domain with platelets via their receptor glycoprotein Ib/V/IX in areas of vascular injury [33]. In healthy states, vWF is cleaved primarily by a disintegrin-like metalloprotease with thrombospondin type-1 repeats-13 (ADAMTS13) at the Tyr1605-Met1606 site of the A2 domain [34]. However, in the presence of inflammation and oxidative stress, the diminished ADAMTS13 levels result in amplified platelet recruitment [35,36]. Interestingly, vWF unfolding at high shear rates over 5000 s−1 observed in areas of vascular stenosis or injury is another stimulus for platelet adhesion [37]. The role of vWF and ADAMTS13 in atherosclerosis has also been recently proven in low-density lipoprotein receptor-deficient mice crossed with mice deficient for ADAMTS13, who were then treated with recombinant ADAMTS13. Following its administration, a reduction in endothelial vWF and platelet adhesion was noted, leading to a significant decrease in aortic plaque size [38].
2.2. Platelet–Neutrophil Interactions in Atherosclerosis
The interaction between platelets and neutrophils has been thoroughly investigated in the setting of inflammation. Following platelet activation, the binding between their surface transmembrane protein P-selectin and its glycoprotein ligand (P-Selectin glycoprotein ligand-1, PSGL-1) on the neutrophil surface represents the main mechanism of neutrophil recruitment, with the interaction between platelet GPIb and integrin aMβ2 on neutrophils or, aided by fibrinogen, the binding of platelet integrin aIIβ3 with integrin aMβ2 as an alternative way [39]. Additionally, platelet-derived cytokines, chemokines, and microparticles have also been implicated in the recruitment and activation of neutrophils. The role of protease-activated receptor 4 in the platelet–neutrophil interactions through the secretion of dense granule contents has also been recently demonstrated experimentally [40]. Moreover, thrombospondin-1, expressed by platelets following their activation, undergoes neutrophil-mediated proteolysis leading to a lower mass molecule that is a potent inducer of platelet activation [41].
On the other hand, in the presence of atherosclerosis, the higher levels of inflammatory cytokines induce the activation of neutrophils which, in turn, overexpress adhesion molecules that promote their binding with platelets, further attenuating the processes of thromboinflammation (Figure 1B) [42]. Several other neutrophil-derived molecules have been implicated in platelet activation including human neutrophil peptides [43,44], heparin binding protein [45], and neutrophil cathepsin G [46]. Novel concepts have also been introduced with regards to neutrophil-mediated platelet activation. To begin with, the neutrophil production of calprotectin has been related to enhanced neutrophil mobilization [47] and platelet activation in experimental studies [48,49]. Moreover, the role of neutrophil cathelicidins in thromboinflammation is being investigated, with LL-37 being an important mediator of platelet activation through the GP VI receptor and downstream signaling via Src/Syk tyrosine kinases and phospholipase C [50]. Lastly, the release of extracellular vesicles from neutrophils and the subsequent entry into platelets could also result in increased thromboxane synthesis and, ultimately, platelet activation [51].
The prothrombotic role of neutrophil extracellular traps (NETs) is also of great importance in the context of atherosclerotic cardiovascular diseases [52]. Based on their composition of DNA, histones, and granular components, NETs can provoke thrombosis either through contact-dependent coagulation [53] or histone-induced platelet recruitment and activation mediated by Toll-like receptors (TLRs) [54]. High-mobility group box 1 (HMGB1) is a damage-associated molecular pattern that has been tightly associated with NET-induced thrombosis [55]. Its involvement in platelet activation has been associated with TLR4 and MyD88-dependent signaling, as well as arterial thrombi [55]. Importantly, NETs were found in abundance in coronary thrombi [56], coronary stent thrombi [57], and cerebrovascular thrombi [58], while their presence was correlated with the degree of infarct [59].
2.3. The Role of Myeloperoxidase and Platelet Toll-Like Receptors
The release of myeloperoxidase (MPO) by activated neutrophils in the setting of inflammation has been associated with atherosclerotic diseases, namely coronary artery disease and its most grievous manifestation, acute coronary syndrome [60,61]. MPO is implicated in alterations of the inflammatory and oxidative processes and the promotion of a stable plaque phenotype [62,63]. Moreover, recent advances have highlighted additional hazardous effects concerning platelet activation. In the study of Kolarova et al., the authors demonstrated that platelets, which are MPO-free following their release from bone marrow, are mildly activated by MPO, as evidenced by their increased production of P-selectin and platelet endothelial cell adhesion molecule-1, the rearrangement of their cytoskeleton, and the released of reactive oxygen species [64]. Interestingly, they did not detect platelet aggregation, thus signifying only partial activation which may, however, enhance the platelet reaction to other stimuli. The effect of MPO on the bioavailability of platelet-derived NO is another fact that has to be taken into account as it is also associated with increased platelet activation and, consequently, adverse cardiovascular outcomes [65].
Platelet TLRs, a cluster of 10 pattern recognition receptors responsible for the identification of molecular patterns, are also involved in the regulation of thromboinflammation (Figure 1C). Previously published studies have reported abnormalities in the levels of platelet TLR 1, 2, 4, and 6 in patients with acute coronary syndromes [66,67], while limited information is available regarding the other representatives of this family.
Starting with platelet TLR2/1, their stimulation by an agonist (Pam3CSK4), exerts pro-thrombotic and pro-inflammatory effects. However, platelet activation is not immediate following their stimulation, requiring either the non-genomic NF-κB activation [68] or the release of adenosine diphosphate or triphosphate and the concomitant release of thromboxane [69,70]. Similar to the above-mentioned complex, platelet TLR4 is incapable of inducing a profound thrombotic effect after the administration of its agonist, lipopolysaccharide, but can augment an established platelet aggregation process [71], while also requiring the presence of other surface molecules such as CD62 [72]. Agonists of platelet TLR2/6 were also deemed unable to activate platelets in physiological doses [67,73], but managed to do so at supra-physiological doses [67]. Along those lines are the observations on other platelet TLR family members such as TLR3 and TLR7 [74,75]. It can be assumed that the main role of these complexes is directed towards inflammation rather than thrombosis [76].
2.4. Cytokines in Platelet Activation
The role of pro-inflammatory cytokines in cardiovascular diseases events has been established with an increased risk of adverse incidents being noted when elevated [77,78]. Unsurprisingly, anti-inflammatory therapies reduced the incidence rate of adverse outcomes in high-risk individuals in the recently completed Canakinumab Antiinflammatory Thrombosis Outcome Study (CANTOS) and Colchicine Cardiovascular Outcomes Trial (COLCOT) [79,80], further cementing the pivotal role of inflammation in the natural history of atherosclerotic cardiovascular diseases.
The excess risk observed in individuals with overproduction of inflammatory cytokines could be attributed to their prothrombotic role (Figure 1D). It should be noted that platelets have receptors for interleukins (ILs), whose stimulation could lead to platelet activation [81,82]. A recent study confirmed this hypothesis, demonstrating enhanced coagulation and platelet hyper-reactivity upon exposure of whole blood from healthy volunteers to IL-1β, IL-6, IL-8, and IL-12 [83,84].
Similar results have been reported for tumor necrosis factor-α (TNF-α) which promoted platelet aggregation and activation [85], while TNF-α inhibitors abrogated platelet activation, platelet-leukocyte interactions, and tissue factor expression in patients with rheumatoid arthritis [86]. Critical insight was provided by the study of Davizon-Castillo et al. in aging-associated inflammation [87]. TNF-α was recognized by the researchers as the primary cytokine involved in platelet hyper-reactivity surrounding this process, eliciting significant alterations at the level of bone marrow (increased megakaryocyte-committed progenitor cells, megakaryocyte ploidy status, and thrombocytosis). Moreover, they reported genetic alterations in inflammatory pathways (signaling of IL-1β, IL-6, TNF receptor-1, and TNF receptor-2), in metabolic pathways, and mitochondrial function evidenced by the augmentation of mitochondrial mass. Those findings were confirmed following administration of recombinant TNF-α in young C57BL/6J mice and reversed after treatment with an anti-TNF-α antibody. It should also be noted that in the absence of functional TNF-α receptors, TNF-α overexpression had no impact on platelet activity and mitochondrial functionality. Strikingly, IL-1β treatment did not result in platelet hyper-reactivity.
2.5. NLRP3 Inflammasome
The nucleotide-binding oligomerization domain, leucine-rich repeat-containing receptor (NLR) family pyrin domain-containing 3 (NLRP3) inflammasome, also consisting of the adaptor apoptosis-associated speck-like protein containing a CARD (ASC) and pro-caspase-1, is well-characterized in atherosclerotic diseases. Several activating factors have been described in the NLRP3 inflammasome assembly in atherosclerosis, including hypoxia [88], NETs [89], cholesterol crystals [90], oxidized low-density lipoprotein cholesterol (LDL-C), and oscillatory shear stress among others [91].
The platelet NLRP3 inflammasome constitutes an important mediator of platelet activation, either not requiring an initial priming signal [92] or being primed in an autocrine or paracrine way in the presence of platelet IL-1 receptor [93]. Murthy et al. showed that the platelet NLRP3 inflammasome was responsible for platelet activation, aggregation, and thrombus formation [94]. Moreover, platelet activation can also induce NLRP3 inflammasome upregulation and subsequent activation of caspase-1 and IL-1β cleavage. Interestingly, they identified platelet Bruton’s tyrosine kinase (BTK) as the mediator of those prothrombotic effects. Vogel et al. shed further light towards this direction by performing BTK or NLRP3 inflammasome inhibition with ibrutinib and MCC950 respectively in sickle cell mice, noting diminished platelet aggregation and thrombus formation [95]. These findings add to the existing knowledge on the platelet activating actions of the platelet NLRP3 inflammasome via the caspase-1-induced thromboinflammatory particles [96].
2.6. Platelet Factor-4
Platelet factor-4 (PF4) is an important mediator of atherogenesis since it has been found in abundance in atherosclerotic plaques and its quantity is related to the severity of the atherosclerotic lesion [97]. Derived from activated platelets, PF4 is laid upon endothelial cells where it recruits monocytes and aids their differentiation into macrophages [98]. Additionally, it interacts with LDL-C by inhibiting the degradation of their receptor and facilitating the uptake of oxidized LDL-C by macrophages [98]. PF4 correlates strongly with the degree of platelet activation evidenced by the platelet-monocyte aggregates, as indicated by the study of Gremmel et al. [99], while its genetic variations are associated with alterations in platelet activation [100]. However, the binding of PF4 with endothelial cell-derived perlecan heparan sulfate chains appears to have an attenuating effect on PF4-induced platelet activation [101].
4. Therapeutic Implications
Inflammation and platelet activation represent crucial therapeutic targets in atherosclerotic cardiovascular diseases and COVID-19 since they are amongst the main etiologies of major adverse events. Even though antiplatelet agents have been established as the cornerstone of atherosclerotic disease management, this has not been the case for anti-inflammatory therapies despite the encouraging results following canakinumab administration in high-risk individuals with elevated levels of high sensitivity C reactive protein [79], which reduced the incidence rate of nonfatal myocardial infarction, non-fatal stroke, and cardiovascular mortality. Colchicine has also demonstrated considerable efficacy in patients with stable coronary artery disease [152] or after myocardial infarction [80], by decreasing the risk of future cardiovascular events when administered in a low dose. Colchicine’s use in cardiovascular disease prevention has been implemented in the latest guidelines of the European Society of Cardiology [153], owing to the positive results of the above mentioned clinical trials and meta-analysis [154]. Of note, low dose methotrexate failed to provide the expected clinical benefit in patients with coronary artery disease with diabetes mellitus or metabolic syndrome in the Cardiovascular Inflammation Reduction Trial (CIRT) [155]. However, inflammatory parameters were not among the inclusion criteria and, thus, the results of this trial should be interpreted with caution.
As highlighted, an interplay between inflammation and platelet activation in the context of atherosclerosis and COVID-19 is highly important and, thus, anti-inflammatory agents have been evaluated with regards to their anti-platelet potential (Table 1). Starting with TNF-α inhibitors, frequently used in autoimmune disorders with speculated cardiovascular benefits [156], their use has been associated with diminished platelet activation through a decrease in platelet–leukocyte interactions and reduced expression of P-Selection [86]. However, a study of etanercept in patients with acute myocardial infarction did not report remarkable alterations in platelet activation parameters [157], while increases in platelet aggregation were mentioned in an in-vitro study of adalimumab [158]. In the studies examining the IL-6 inhibitor tocilizumab, a reduced platelet activity was observed [159], also extending towards COVID-19 anti-thrombotic treatment [128]. Interestingly, when tocilizumab was administered to COVID-19 patients, an early and sustained increase in platelet count was observed, possibly signifying reduced platelet consumption and less thrombosis [160,161]. Finally, colchicine has undoubtedly received the most scientific attention in this aspect, with several studies highlighting its potential as an adjunctive antiplatelet approach [159,162,163,164], which might be responsible for the beneficial effects observed in patients with a recent acute coronary syndrome or chronic coronary syndromes [80,152]. Despite being studied in the setting of COVID-19, the effect of anti-inflammatory agents on established platelet activation parameters has not been assessed in this patient population and can only be speculated on.

Table 1.
Studies evaluating the effect of the available anti-inflammatory agents on platelet activation parameters.
With regards to other experimental therapeutics (Table 2), important progress has been made in NET inhibition. Li et al. noted a decrease in inflammatory cytokines paired with attenuation of platelet activation and thrombus formation following NET degradation with the inhibitor DNAse [168]. In another study, DNAse lessened ATP and ADP-induced thrombus formation in vivo, although it did not affect NET formation [169]. The DNAse inhibitor dornase alfa has recently gained attention towards COVID-19 treatment, with improvement in patient oxygenation being noted following its use in vitro and in vivo [170,171,172], while it remains to be explored whether these agents can influence clinical outcomes by halting platelet activation among other pathways. Chloramidine, a protein-arginine deiminase antagonist known for inhibiting NETosis, was also associated with reduced arterial thrombosis in vivo [173]. Moving to TLR4 inhibition with eritoran, Clark et al. demonstrated its potential in interfering with platelet activation, as shown by the reduced platelet-leukocyte aggregates and platelet-associated NET formation [174]. Resveratrol was also found to possess anti-TLR4 properties, leading to the attenuation of thrombin receptor activated peptide (TRAP)- and collagen-induced platelet aggregation as well as the reduction of CD40L [175]. It is critical to note that currently available antiplatelet agents appear to have minimal effect on platelet TLR4 [176]. Moreover, novel aptamers acting as inhibitors of vWF have been developed (BT200, DTRI-031), which attenuate the platelet-activating properties of vWF in a dose-dependent manner [177,178]. Lastly, the role of NLRP3 inflammasome inhibition is gathering scientific attention, with either direct inhibitors (MCC950) or BTK inhibitors (acalabrutinib, ibrutinib) demonstrating efficacy in attenuating platelet activation, aggregation, and thrombus formation in experimental studies [179,180,181,182].

Table 2.
Studies evaluating the effect of the experimental anti-inflammatory agents on thromboinflammation.
5. Conclusions
The interaction of platelets with the vascular endothelium, the immune cells, and other inflammatory mediators appears to be a central component of thromboinflammation, which adversely affects cardiovascular health by promoting atherogenesis. Moreover, platelet activation as a result of the cytokine storm induced by SARS-CoV-2 infection might be a crucial moderator of the thrombotic complications reported in COVID-19 patients. Ultimately, according to the results of preclinical and clinical studies, anti-inflammatory therapies could represent a reasonable therapeutic option in the reduction of residual cardiovascular risk in the setting of atherosclerotic diseases and COVID-19.
Funding
This research received no external funding.
Institutional Review Board Statement
Not applicable.
Informed Consent Statement
Not applicable.
Data Availability Statement
Not applicable.
Conflicts of Interest
The authors declare no conflict of interest.
References
- Oikonomou, E.; Vogiatzi, G.; Lazaros, G.; Tsalamandris, S.; Goliopoulou, A.; Mystakidou, V.; Theofilis, P.; Christoforatou, E.; Chasikidis, C.; Tousoulis, D. Relationship of depressive symptoms with arterial stiffness and carotid atherosclerotic burden in the Corinthia study. QJM Mon. J. Assoc. Physicians 2020, 113, 633–642. [Google Scholar] [CrossRef]
- Oikonomou, E.; Lazaros, G.; Mystakidi, V.C.; Papaioannou, N.; Theofilis, P.; Vogiatzi, G.; Chasikidis, C.; Fountoulakis, P.; Papakostantinou, M.A.; Assimakopoulos, M.N.; et al. The association of air pollutants exposure with subclinical inflammation and carotid atherosclerosis. Int. J. Cardiol. 2021, 342, 108–114. [Google Scholar] [CrossRef]
- Oikonomou, E.; Lazaros, G.; Christoforatou, E.; Chasikidis, C.; Vavouranaki, G.; Vogiatzi, G.; Papamikroulis, G.A.; Tsalamandris, S.; Gergiopoulos, G.; Mazaris, S.; et al. Breakfast association with arterial stiffness and carotid atherosclerotic burden. Insights from the ‘Corinthia’ study. Nutr. Metab. Cardiovasc. Dis. NMCD 2019, 29, 744–750. [Google Scholar] [CrossRef]
- Oikonomou, E.; Theofilis, P.; Vogiatzi, G.; Lazaros, G.; Tsalamandris, S.; Mystakidi, V.C.; Goliopoulou, A.; Anastasiou, M.; Fountoulakis, P.; Chasikidis, C.; et al. The impact of sleeping duration on atherosclerosis in the community: Insights from the Corinthia study. Sleep Breath. 2021. [Google Scholar] [CrossRef]
- Majithia, A.; Bhatt, D.L. Novel Antiplatelet Therapies for Atherothrombotic Diseases. Arterioscler. Thromb. Vasc. Biol. 2019, 39, 546–557. [Google Scholar] [CrossRef]
- Siasos, G.; Skotsimara, G.; Oikonomou, E.; Sagris, M.; Vasiliki-Chara, M.; Bletsa, E.; Stampouloglou, P.; Theofilis, P.; Charalampous, G.; Tousoulis, D. Antithrombotic Treatment in Diabetes Mellitus: A Review of the Literature about Antiplatelet and Anticoagulation Strategies Used for Diabetic Patients in Primary and Secondary Prevention. Curr. Pharm. Des. 2020, 26, 2780–2788. [Google Scholar] [CrossRef]
- Theofilis, P.; Sagris, M.; Oikonomou, E.; Antonopoulos, A.S.; Siasos, G.; Tsioufis, C.; Tousoulis, D. Inflammatory Mechanisms Contributing to Endothelial Dysfunction. Biomedicines 2021, 9, 781. [Google Scholar] [CrossRef] [PubMed]
- Delgadillo, L.F.; Lomakina, E.B.; Kuebel, J.; Waugh, R.E. Changes in endothelial glycocalyx layer protective ability after inflammatory stimulus. Am. J. Physiol. Cell Physiol. 2021, 320, C216–C224. [Google Scholar] [CrossRef] [PubMed]
- Uchimido, R.; Schmidt, E.P.; Shapiro, N.I. The glycocalyx: A novel diagnostic and therapeutic target in sepsis. Crit. Care 2019, 23, 16. [Google Scholar] [CrossRef] [PubMed]
- Becker, B.F.; Jacob, M.; Leipert, S.; Salmon, A.H.; Chappell, D. Degradation of the endothelial glycocalyx in clinical settings: Searching for the sheddases. Br. J. Clin. Pharmacol. 2015, 80, 389–402. [Google Scholar] [CrossRef] [PubMed]
- Lukasz, A.; Hillgruber, C.; Oberleithner, H.; Kusche-Vihrog, K.; Pavenstadt, H.; Rovas, A.; Hesse, B.; Goerge, T.; Kumpers, P. Endothelial glycocalyx breakdown is mediated by angiopoietin-2. Cardiovasc. Res. 2017, 113, 671–680. [Google Scholar] [CrossRef]
- Schmidt, A.; Echtermeyer, F.; Alozie, A.; Brands, K.; Buddecke, E. Plasmin- and thrombin-accelerated shedding of syndecan-4 ectodomain generates cleavage sites at Lys(114)-Arg(115) and Lys(129)-Val(130) bonds. J. Biol. Chem. 2005, 280, 34441–34446. [Google Scholar] [CrossRef]
- Britten, M.W.; Lumers, L.; Tominaga, K.; Peters, J.; Dirkmann, D. Glycocalyx components affect platelet function, whole blood coagulation, and fibrinolysis: An in vitro study suggesting a link to trauma-induced coagulopathy. BMC Anesthesiol. 2021, 21, 83. [Google Scholar] [CrossRef]
- Reitsma, S.; Oude Egbrink, M.G.; Heijnen, V.V.; Megens, R.T.; Engels, W.; Vink, H.; Slaaf, D.W.; van Zandvoort, M.A. Endothelial glycocalyx thickness and platelet-vessel wall interactions during atherogenesis. Thromb. Haemost. 2011, 106, 939–946. [Google Scholar] [CrossRef]
- Constantinescu, A.A.; Vink, H.; Spaan, J.A. Endothelial cell glycocalyx modulates immobilization of leukocytes at the endothelial surface. Arterioscler. Thromb. Vasc. Biol. 2003, 23, 1541–1547. [Google Scholar] [CrossRef]
- Becker, B.F.; Chappell, D.; Bruegger, D.; Annecke, T.; Jacob, M. Therapeutic strategies targeting the endothelial glycocalyx: Acute deficits, but great potential. Cardiovasc. Res. 2010, 87, 300–310. [Google Scholar] [CrossRef]
- Dogne, S.; Flamion, B.; Caron, N. Endothelial Glycocalyx as a Shield Against Diabetic Vascular Complications: Involvement of Hyaluronan and Hyaluronidases. Arterioscler. Thromb. Vasc. Biol. 2018, 38, 1427–1439. [Google Scholar] [CrossRef]
- Smolenski, A. Novel roles of cAMP/cGMP-dependent signaling in platelets. J. Thromb. Haemost. 2012, 10, 167–176. [Google Scholar] [CrossRef] [PubMed]
- Mellion, B.T.; Ignarro, L.J.; Ohlstein, E.H.; Pontecorvo, E.G.; Hyman, A.L.; Kadowitz, P.J. Evidence for the inhibitory role of guanosine 3′, 5′-monophosphate in ADP-induced human platelet aggregation in the presence of nitric oxide and related vasodilators. Blood 1981, 57, 946–955. [Google Scholar] [CrossRef] [PubMed]
- Eigenthaler, M.; Ullrich, H.; Geiger, J.; Horstrup, K.; Honig-Liedl, P.; Wiebecke, D.; Walter, U. Defective nitrovasodilator-stimulated protein phosphorylation and calcium regulation in cGMP-dependent protein kinase-deficient human platelets of chronic myelocytic leukemia. J. Biol. Chem. 1993, 268, 13526–13531. [Google Scholar] [CrossRef]
- Massberg, S.; Sausbier, M.; Klatt, P.; Bauer, M.; Pfeifer, A.; Siess, W.; Fassler, R.; Ruth, P.; Krombach, F.; Hofmann, F. Increased adhesion and aggregation of platelets lacking cyclic guanosine 3′,5′-monophosphate kinase I. J. Exp. Med. 1999, 189, 1255–1264. [Google Scholar] [CrossRef]
- Hadi, H.A.; Carr, C.S.; Al Suwaidi, J. Endothelial dysfunction: Cardiovascular risk factors, therapy, and outcome. Vasc. Health Risk Manag. 2005, 1, 183–198. [Google Scholar]
- Szabo, C.; Ischiropoulos, H.; Radi, R. Peroxynitrite: Biochemistry, pathophysiology and development of therapeutics. Nat. Rev. Drug Discov. 2007, 6, 662–680. [Google Scholar] [CrossRef]
- Freedman, J.E.; Loscalzo, J.; Barnard, M.R.; Alpert, C.; Keaney, J.F.; Michelson, A.D. Nitric oxide released from activated platelets inhibits platelet recruitment. J. Clin. Investig. 1997, 100, 350–356. [Google Scholar] [CrossRef]
- Berkels, R.; Bertsch, A.; Zuther, T.; Dhein, S.; Stockklauser, K.; Rosen, P.; Rosen, R. Evidence for a NO synthase in porcine platelets which is stimulated during activation/aggregation. Eur. J. Haematol. 1997, 58, 307–313. [Google Scholar] [CrossRef]
- Malinski, T.; Radomski, M.W.; Taha, Z.; Moncada, S. Direct electrochemical measurement of nitric oxide released from human platelets. Biochem. Biophys. Res. Commun. 1993, 194, 960–965. [Google Scholar] [CrossRef] [PubMed]
- Freedman, J.E.; Sauter, R.; Battinelli, E.M.; Ault, K.; Knowles, C.; Huang, P.L.; Loscalzo, J. Deficient platelet-derived nitric oxide and enhanced hemostasis in mice lacking the NOSIII gene. Circ. Res. 1999, 84, 1416–1421. [Google Scholar] [CrossRef] [PubMed]
- Momi, S.; Caracchini, R.; Falcinelli, E.; Evangelista, S.; Gresele, P. Stimulation of platelet nitric oxide production by nebivolol prevents thrombosis. Arterioscler. Thromb. Vasc. Biol. 2014, 34, 820–829. [Google Scholar] [CrossRef]
- Schwarz, U.R.; Walter, U.; Eigenthaler, M. Taming platelets with cyclic nucleotides. Biochem. Pharmacol. 2001, 62, 1153–1161. [Google Scholar] [CrossRef]
- Ramadan, F.M.; Upchurch, G.R., Jr.; Keagy, B.A.; Johnson, G., Jr. Endothelial cell thromboxane production and its inhibition by a calcium-channel blocker. Ann. Thorac. Surg. 1990, 49, 916–919. [Google Scholar] [CrossRef]
- Ooi, B.S.; Cohen, D.J.; Chang, T.H.; Tian, Y.; Papademetrious, V. Stimulation of endothelial cell production of vasoconstrictive substances by hypertensive sera. Am. J. Hypertens. 1998, 11, 240–244. [Google Scholar] [CrossRef][Green Version]
- Wagner, D.D.; Marder, V.J. Biosynthesis of von Willebrand protein by human endothelial cells: Processing steps and their intracellular localization. J. Cell Biol. 1984, 99, 2123–2130. [Google Scholar] [CrossRef] [PubMed]
- Wu, M.D.; Atkinson, T.M.; Lindner, J.R. Platelets and von Willebrand factor in atherogenesis. Blood 2017, 129, 1415–1419. [Google Scholar] [CrossRef]
- Dong, J.F.; Moake, J.L.; Nolasco, L.; Bernardo, A.; Arceneaux, W.; Shrimpton, C.N.; Schade, A.J.; McIntire, L.V.; Fujikawa, K.; Lopez, J.A. ADAMTS-13 rapidly cleaves newly secreted ultralarge von Willebrand factor multimers on the endothelial surface under flowing conditions. Blood 2002, 100, 4033–4039. [Google Scholar] [CrossRef] [PubMed]
- Cao, W.J.; Niiya, M.; Zheng, X.W.; Shang, D.Z.; Zheng, X.L. Inflammatory cytokines inhibit ADAMTS13 synthesis in hepatic stellate cells and endothelial cells. J. Thromb. Haemost. 2008, 6, 1233–1235. [Google Scholar] [CrossRef] [PubMed]
- Chen, J.; Fu, X.; Wang, Y.; Ling, M.; McMullen, B.; Kulman, J.; Chung, D.W.; Lopez, J.A. Oxidative modification of von Willebrand factor by neutrophil oxidants inhibits its cleavage by ADAMTS13. Blood 2010, 115, 706–712. [Google Scholar] [CrossRef]
- Okhota, S.; Melnikov, I.; Avtaeva, Y.; Kozlov, S.; Gabbasov, Z. Shear Stress-Induced Activation of von Willebrand Factor and Cardiovascular Pathology. Int. J. Mol. Sci. 2020, 21, 7804. [Google Scholar] [CrossRef] [PubMed]
- Ozawa, K.; Muller, M.A.; Varlamov, O.; Tavori, H.; Packwood, W.; Mueller, P.A.; Xie, A.; Ruggeri, Z.; Chung, D.; Lopez, J.A.; et al. Proteolysis of Von Willebrand Factor Influences Inflammatory Endothelial Activation and Vascular Compliance in Atherosclerosis. JACC Basic Transl. Sci. 2020, 5, 1017–1028. [Google Scholar] [CrossRef]
- Zucoloto, A.Z.; Jenne, C.N. Platelet-Neutrophil Interplay: Insights Into Neutrophil Extracellular Trap (NET)-Driven Coagulation in Infection. Front. Cardiovasc. Med. 2019, 6, 85. [Google Scholar] [CrossRef]
- Rigg, R.A.; Healy, L.D.; Chu, T.T.; Ngo, A.T.P.; Mitrugno, A.; Zilberman-Rudenko, J.; Aslan, J.E.; Hinds, M.T.; Vecchiarelli, L.D.; Morgan, T.K.; et al. Protease-activated receptor 4 activity promotes platelet granule release and platelet-leukocyte interactions. Platelets 2019, 30, 126–135. [Google Scholar] [CrossRef]
- Seif, K.; Alidzanovic, L.; Tischler, B.; Ibrahim, N.; Zagrapan, B.; Rauscher, S.; Salzmann, M.; Hell, L.; Mauracher, L.M.; Budde, U.; et al. Neutrophil-Mediated Proteolysis of Thrombospondin-1 Promotes Platelet Adhesion and String Formation. Thromb. Haemost. 2018, 118, 2074–2085. [Google Scholar] [CrossRef]
- Oikonomou, E.; Leopoulou, M.; Theofilis, P.; Antonopoulos, A.S.; Siasos, G.; Latsios, G.; Mystakidi, V.C.; Antoniades, C.; Tousoulis, D. A link between inflammation and thrombosis in atherosclerotic cardiovascular diseases: Clinical and therapeutic implications. Atherosclerosis 2020, 309, 16–26. [Google Scholar] [CrossRef]
- Quinn, K.L.; Henriques, M.; Tabuchi, A.; Han, B.; Yang, H.; Cheng, W.E.; Tole, S.; Yu, H.; Luo, A.; Charbonney, E.; et al. Human neutrophil peptides mediate endothelial-monocyte interaction, foam cell formation, and platelet activation. Arterioscler. Thromb. Vasc. Biol. 2011, 31, 2070–2079. [Google Scholar] [CrossRef]
- Horn, M.; Bertling, A.; Brodde, M.F.; Muller, A.; Roth, J.; Van Aken, H.; Jurk, K.; Heilmann, C.; Peters, G.; Kehrel, B.E. Human neutrophil alpha-defensins induce formation of fibrinogen and thrombospondin-1 amyloid-like structures and activate platelets via glycoprotein IIb/IIIa. J. Thromb. Haemost. 2012, 10, 647–661. [Google Scholar] [CrossRef]
- Kaiser, P.; Harenberg, J.; Walenga, J.M.; Huhle, G.; Giese, C.; Prechel, M.; Hoppensteadt, D.; Fareed, J. Effects of a heparin-binding protein on blood coagulation and platelet function. Semin. Thromb. Hemost. 2001, 27, 495–502. [Google Scholar] [CrossRef][Green Version]
- Faraday, N.; Schunke, K.; Saleem, S.; Fu, J.; Wang, B.; Zhang, J.; Morrell, C.; Dore, S. Cathepsin G-dependent modulation of platelet thrombus formation in vivo by blood neutrophils. PLoS ONE 2013, 8, e71447. [Google Scholar] [CrossRef] [PubMed]
- Pruenster, M.; Kurz, A.R.; Chung, K.J.; Cao-Ehlker, X.; Bieber, S.; Nussbaum, C.F.; Bierschenk, S.; Eggersmann, T.K.; Rohwedder, I.; Heinig, K.; et al. Extracellular MRP8/14 is a regulator of beta2 integrin-dependent neutrophil slow rolling and adhesion. Nat. Commun. 2015, 6, 6915. [Google Scholar] [CrossRef] [PubMed]
- Santilli, F.; Paloscia, L.; Liani, R.; Di Nicola, M.; Di Marco, M.; Lattanzio, S.; La Barba, S.; Pascale, S.; Mascellanti, M.; Davi, G. Circulating myeloid-related protein-8/14 is related to thromboxane-dependent platelet activation in patients with acute coronary syndrome, with and without ongoing low-dose aspirin treatment. J. Am. Heart Assoc. 2014, 3. [Google Scholar] [CrossRef] [PubMed]
- Liang, X.; Xiu, C.; Liu, M.; Lin, C.; Chen, H.; Bao, R.; Yang, S.; Yu, J. Platelet-neutrophil interaction aggravates vascular in fl ammation and promotes the progression of atherosclerosis by activating the TLR4/NF-kappaB pathway. J. Cell. Biochem. 2019, 120, 5612–5619. [Google Scholar] [CrossRef] [PubMed]
- Pircher, J.; Czermak, T.; Ehrlich, A.; Eberle, C.; Gaitzsch, E.; Margraf, A.; Grommes, J.; Saha, P.; Titova, A.; Ishikawa-Ankerhold, H.; et al. Cathelicidins prime platelets to mediate arterial thrombosis and tissue inflammation. Nat. Commun. 2018, 9, 1523. [Google Scholar] [CrossRef] [PubMed]
- Rossaint, J.; Kuhne, K.; Skupski, J.; Van Aken, H.; Looney, M.R.; Hidalgo, A.; Zarbock, A. Directed transport of neutrophil-derived extracellular vesicles enables platelet-mediated innate immune response. Nat. Commun. 2016, 7, 13464. [Google Scholar] [CrossRef]
- Thakur, M.; Evans, B.; Schindewolf, M.; Baumgartner, I.; Doring, Y. Neutrophil Extracellular Traps Affecting Cardiovascular Health in Infectious and Inflammatory Diseases. Cells 2021, 10, 1689. [Google Scholar] [CrossRef]
- Noubouossie, D.F.; Whelihan, M.F.; Yu, Y.B.; Sparkenbaugh, E.; Pawlinski, R.; Monroe, D.M.; Key, N.S. In vitro activation of coagulation by human neutrophil DNA and histone proteins but not neutrophil extracellular traps. Blood 2017, 129, 1021–1029. [Google Scholar] [CrossRef] [PubMed]
- Semeraro, F.; Ammollo, C.T.; Morrissey, J.H.; Dale, G.L.; Friese, P.; Esmon, N.L.; Esmon, C.T. Extracellular histones promote thrombin generation through platelet-dependent mechanisms: Involvement of platelet TLR2 and TLR4. Blood 2011, 118, 1952–1961. [Google Scholar] [CrossRef] [PubMed]
- Vogel, S.; Bodenstein, R.; Chen, Q.; Feil, S.; Feil, R.; Rheinlaender, J.; Schaffer, T.E.; Bohn, E.; Frick, J.S.; Borst, O.; et al. Platelet-derived HMGB1 is a critical mediator of thrombosis. J. Clin. Investig. 2015, 125, 4638–4654. [Google Scholar] [CrossRef]
- De Boer, O.J.; Li, X.; Teeling, P.; Mackaay, C.; Ploegmakers, H.J.; van der Loos, C.M.; Daemen, M.J.; de Winter, R.J.; van der Wal, A.C. Neutrophils, neutrophil extracellular traps and interleukin-17 associate with the organisation of thrombi in acute myocardial infarction. Thromb. Haemost. 2013, 109, 290–297. [Google Scholar] [CrossRef] [PubMed]
- Riegger, J.; Byrne, R.A.; Joner, M.; Chandraratne, S.; Gershlick, A.H.; Ten Berg, J.M.; Adriaenssens, T.; Guagliumi, G.; Godschalk, T.C.; Neumann, F.J.; et al. Histopathological evaluation of thrombus in patients presenting with stent thrombosis. A multicenter European study: A report of the prevention of late stent thrombosis by an interdisciplinary global European effort consortium. Eur. Heart J. 2016, 37, 1538–1549. [Google Scholar] [CrossRef] [PubMed]
- Laridan, E.; Denorme, F.; Desender, L.; Francois, O.; Andersson, T.; Deckmyn, H.; Vanhoorelbeke, K.; De Meyer, S.F. Neutrophil extracellular traps in ischemic stroke thrombi. Ann. Neurol. 2017, 82, 223–232. [Google Scholar] [CrossRef]
- Mangold, A.; Alias, S.; Scherz, T.; Hofbauer, M.; Jakowitsch, J.; Panzenbock, A.; Simon, D.; Laimer, D.; Bangert, C.; Kammerlander, A.; et al. Coronary neutrophil extracellular trap burden and deoxyribonuclease activity in ST-elevation acute coronary syndrome are predictors of ST-segment resolution and infarct size. Circ. Res. 2015, 116, 1182–1192. [Google Scholar] [CrossRef]
- Nussbaum, C.; Klinke, A.; Adam, M.; Baldus, S.; Sperandio, M. Myeloperoxidase: A leukocyte-derived protagonist of inflammation and cardiovascular disease. Antioxid. Redox Signal. 2013, 18, 692–713. [Google Scholar] [CrossRef]
- Baldus, S.; Heeschen, C.; Meinertz, T.; Zeiher, A.M.; Eiserich, J.P.; Munzel, T.; Simoons, M.L.; Hamm, C.W.; Investigators, C. Myeloperoxidase serum levels predict risk in patients with acute coronary syndromes. Circulation 2003, 108, 1440–1445. [Google Scholar] [CrossRef] [PubMed]
- Kargapolova, Y.; Geissen, S.; Zheng, R.; Baldus, S.; Winkels, H.; Adam, M. The Enzymatic and Non-Enzymatic Function of Myeloperoxidase (MPO) in Inflammatory Communication. Antioxidants 2021, 10, 562. [Google Scholar] [CrossRef] [PubMed]
- Teng, N.; Maghzal, G.J.; Talib, J.; Rashid, I.; Lau, A.K.; Stocker, R. The roles of myeloperoxidase in coronary artery disease and its potential implication in plaque rupture. Redox Rep. Commun. Free Radic. Res. 2017, 22, 51–73. [Google Scholar] [CrossRef] [PubMed]
- Kolarova, H.; Klinke, A.; Kremserova, S.; Adam, M.; Pekarova, M.; Baldus, S.; Eiserich, J.P.; Kubala, L. Myeloperoxidase induces the priming of platelets. Free. Radic. Biol. Med. 2013, 61, 357–369. [Google Scholar] [CrossRef]
- Freedman, J.E.; Ting, B.; Hankin, B.; Loscalzo, J.; Keaney, J.F., Jr.; Vita, J.A. Impaired platelet production of nitric oxide predicts presence of acute coronary syndromes. Circulation 1998, 98, 1481–1486. [Google Scholar] [CrossRef]
- Gurses, K.M.; Kocyigit, D.; Yalcin, M.U.; Canpinar, H.; Oto, M.A.; Ozer, N.; Tokgozoglu, L.; Guc, D.; Aytemir, K. Enhanced Platelet Toll-like Receptor 2 and 4 Expression in Acute Coronary Syndrome and Stable Angina Pectoris. Am. J. Cardiol. 2015, 116, 1666–1671. [Google Scholar] [CrossRef]
- Hally, K.E.; La Flamme, A.C.; Larsen, P.D.; Harding, S.A. Platelet Toll-like receptor (TLR) expression and TLR-mediated platelet activation in acute myocardial infarction. Thromb. Res. 2017, 158, 8–15. [Google Scholar] [CrossRef]
- Rivadeneyra, L.; Carestia, A.; Etulain, J.; Pozner, R.G.; Fondevila, C.; Negrotto, S.; Schattner, M. Regulation of platelet responses triggered by Toll-like receptor 2 and 4 ligands is another non-genomic role of nuclear factor-kappaB. Thromb. Res. 2014, 133, 235–243. [Google Scholar] [CrossRef]
- Kalvegren, H.; Skoglund, C.; Helldahl, C.; Lerm, M.; Grenegard, M.; Bengtsson, T. Toll-like receptor 2 stimulation of platelets is mediated by purinergic P2X1-dependent Ca2+ mobilisation, cyclooxygenase and purinergic P2Y1 and P2Y12 receptor activation. Thromb. Haemost. 2010, 103, 398–407. [Google Scholar] [CrossRef]
- Klarstrom Engstrom, K.; Brommesson, C.; Kalvegren, H.; Bengtsson, T. Toll like receptor 2/1 mediated platelet adhesion and activation on bacterial mimetic surfaces is dependent on src/Syk-signaling and purinergic receptor P2X1 and P2Y12 activation. Biointerphases 2014, 9, 041003. [Google Scholar] [CrossRef]
- Lopes Pires, M.E.; Clarke, S.R.; Marcondes, S.; Gibbins, J.M. Lipopolysaccharide potentiates platelet responses via toll-like receptor 4-stimulated Akt-Erk-PLA2 signalling. PLoS ONE 2017, 12, e0186981. [Google Scholar] [CrossRef] [PubMed]
- Stahl, A.L.; Svensson, M.; Morgelin, M.; Svanborg, C.; Tarr, P.I.; Mooney, J.C.; Watkins, S.L.; Johnson, R.; Karpman, D. Lipopolysaccharide from enterohemorrhagic Escherichia coli binds to platelets through TLR4 and CD62 and is detected on circulating platelets in patients with hemolytic uremic syndrome. Blood 2006, 108, 167–176. [Google Scholar] [CrossRef]
- de Stoppelaar, S.F.; Claushuis, T.A.; Schaap, M.C.; Hou, B.; van der Poll, T.; Nieuwland, R.; van ‘t Veer, C. Toll-Like Receptor Signalling Is Not Involved in Platelet Response to Streptococcus pneumoniae In Vitro or In Vivo. PLoS ONE 2016, 11, e0156977. [Google Scholar] [CrossRef] [PubMed]
- D’Atri, L.P.; Etulain, J.; Rivadeneyra, L.; Lapponi, M.J.; Centurion, M.; Cheng, K.; Yin, H.; Schattner, M. Expression and functionality of Toll-like receptor 3 in the megakaryocytic lineage. J. Thromb. Haemost. 2015, 13, 839–850. [Google Scholar] [CrossRef]
- Rex, S.; Beaulieu, L.M.; Perlman, D.H.; Vitseva, O.; Blair, P.S.; McComb, M.E.; Costello, C.E.; Freedman, J.E. Immune versus thrombotic stimulation of platelets differentially regulates signalling pathways, intracellular protein-protein interactions, and alpha-granule release. Thromb. Haemost. 2009, 102, 97–110. [Google Scholar] [CrossRef] [PubMed]
- Hally, K.; Fauteux-Daniel, S.; Hamzeh-Cognasse, H.; Larsen, P.; Cognasse, F. Revisiting Platelets and Toll-Like Receptors (TLRs): At the Interface of Vascular Immunity and Thrombosis. Int. J. Mol. Sci. 2020, 21, 6150. [Google Scholar] [CrossRef] [PubMed]
- Tousoulis, D.; Oikonomou, E.; Economou, E.K.; Crea, F.; Kaski, J.C. Inflammatory cytokines in atherosclerosis: Current therapeutic approaches. Eur. Heart J. 2016, 37, 1723–1732. [Google Scholar] [CrossRef]
- Yuan, S.; Lin, A.; He, Q.Q.; Burgess, S.; Larsson, S.C. Circulating interleukins in relation to coronary artery disease, atrial fibrillation and ischemic stroke and its subtypes: A two-sample Mendelian randomization study. Int. J. Cardiol. 2020, 313, 99–104. [Google Scholar] [CrossRef] [PubMed]
- Ridker, P.M.; Everett, B.M.; Thuren, T.; MacFadyen, J.G.; Chang, W.H.; Ballantyne, C.; Fonseca, F.; Nicolau, J.; Koenig, W.; Anker, S.D.; et al. Antiinflammatory Therapy with Canakinumab for Atherosclerotic Disease. N. Engl. J. Med. 2017, 377, 1119–1131. [Google Scholar] [CrossRef]
- Tardif, J.C.; Kouz, S.; Waters, D.D.; Bertrand, O.F.; Diaz, R.; Maggioni, A.P.; Pinto, F.J.; Ibrahim, R.; Gamra, H.; Kiwan, G.S.; et al. Efficacy and Safety of Low-Dose Colchicine after Myocardial Infarction. N. Engl. J. Med. 2019, 381, 2497–2505. [Google Scholar] [CrossRef]
- Tedgui, A.; Mallat, Z. Cytokines in atherosclerosis: Pathogenic and regulatory pathways. Physiol. Rev. 2006, 86, 515–581. [Google Scholar] [CrossRef]
- Regnault, V.; de Maistre, E.; Carteaux, J.P.; Gruel, Y.; Nguyen, P.; Tardy, B.; Lecompte, T. Platelet activation induced by human antibodies to interleukin-8. Blood 2003, 101, 1419–1421. [Google Scholar] [CrossRef] [PubMed]
- Page, M.J.; Bester, J.; Pretorius, E. Interleukin-12 and its procoagulant effect on erythrocytes, platelets and fibrin(ogen): The lesser known side of inflammation. Br. J. Haematol. 2018, 180, 110–117. [Google Scholar] [CrossRef] [PubMed]
- Bester, J.; Pretorius, E. Effects of IL-1beta, IL-6 and IL-8 on erythrocytes, platelets and clot viscoelasticity. Sci. Rep. 2016, 6, 32188. [Google Scholar] [CrossRef] [PubMed]
- Page, M.J.; Bester, J.; Pretorius, E. The inflammatory effects of TNF-alpha and complement component 3 on coagulation. Sci. Rep. 2018, 8, 1812. [Google Scholar] [CrossRef] [PubMed]
- Manfredi, A.A.; Baldini, M.; Camera, M.; Baldissera, E.; Brambilla, M.; Peretti, G.; Maseri, A.; Rovere-Querini, P.; Tremoli, E.; Sabbadini, M.G.; et al. Anti-TNFalpha agents curb platelet activation in patients with rheumatoid arthritis. Ann. Rheum. Dis. 2016, 75, 1511–1520. [Google Scholar] [CrossRef]
- Davizon-Castillo, P.; McMahon, B.; Aguila, S.; Bark, D.; Ashworth, K.; Allawzi, A.; Campbell, R.A.; Montenont, E.; Nemkov, T.; D’Alessandro, A.; et al. TNF-alpha-driven inflammation and mitochondrial dysfunction define the platelet hyperreactivity of aging. Blood 2019, 134, 727–740. [Google Scholar] [CrossRef] [PubMed]
- Folco, E.J.; Sukhova, G.K.; Quillard, T.; Libby, P. Moderate hypoxia potentiates interleukin-1beta production in activated human macrophages. Circ. Res. 2014, 115, 875–883. [Google Scholar] [CrossRef] [PubMed]
- Warnatsch, A.; Ioannou, M.; Wang, Q.; Papayannopoulos, V. Inflammation. Neutrophil extracellular traps license macrophages for cytokine production in atherosclerosis. Science 2015, 349, 316–320. [Google Scholar] [CrossRef] [PubMed]
- Duewell, P.; Kono, H.; Rayner, K.J.; Sirois, C.M.; Vladimer, G.; Bauernfeind, F.G.; Abela, G.S.; Franchi, L.; Nunez, G.; Schnurr, M.; et al. NLRP3 inflammasomes are required for atherogenesis and activated by cholesterol crystals. Nature 2010, 464, 1357–1361. [Google Scholar] [CrossRef]
- Xiao, H.; Lu, M.; Lin, T.Y.; Chen, Z.; Chen, G.; Wang, W.C.; Marin, T.; Shentu, T.P.; Wen, L.; Gongol, B.; et al. Sterol regulatory element binding protein 2 activation of NLRP3 inflammasome in endothelium mediates hemodynamic-induced atherosclerosis susceptibility. Circulation 2013, 128, 632–642. [Google Scholar] [CrossRef] [PubMed]
- Hottz, E.D.; Monteiro, A.P.; Bozza, F.A.; Bozza, P.T. Inflammasome in platelets: Allying coagulation and inflammation in infectious and sterile diseases? Mediat. Inflamm. 2015, 2015, 435783. [Google Scholar] [CrossRef] [PubMed]
- Brown, G.T.; Narayanan, P.; Li, W.; Silverstein, R.L.; McIntyre, T.M. Lipopolysaccharide stimulates platelets through an IL-1beta autocrine loop. J. Immunol. 2013, 191, 5196–5203. [Google Scholar] [CrossRef]
- Murthy, P.; Durco, F.; Miller-Ocuin, J.L.; Takedai, T.; Shankar, S.; Liang, X.; Liu, X.; Cui, X.; Sachdev, U.; Rath, D.; et al. The NLRP3 inflammasome and bruton’s tyrosine kinase in platelets co-regulate platelet activation, aggregation, and in vitro thrombus formation. Biochem. Biophys. Res. Commun. 2017, 483, 230–236. [Google Scholar] [CrossRef]
- Vogel, S.; Kamimura, S.; Arora, T.; Smith, M.L.; Almeida, L.E.F.; Combs, C.A.; Thein, S.L.; Quezado, Z.M.N. NLRP3 inflammasome and bruton tyrosine kinase inhibition interferes with upregulated platelet aggregation and in vitro thrombus formation in sickle cell mice. Biochem. Biophys. Res. Commun. 2021, 555, 196–201. [Google Scholar] [CrossRef]
- Hottz, E.D.; Lopes, J.F.; Freitas, C.; Valls-de-Souza, R.; Oliveira, M.F.; Bozza, M.T.; Da Poian, A.T.; Weyrich, A.S.; Zimmerman, G.A.; Bozza, F.A.; et al. Platelets mediate increased endothelium permeability in dengue through NLRP3-inflammasome activation. Blood 2013, 122, 3405–3414. [Google Scholar] [CrossRef]
- Pitsilos, S.; Hunt, J.; Mohler, E.R.; Prabhakar, A.M.; Poncz, M.; Dawicki, J.; Khalapyan, T.Z.; Wolfe, M.L.; Fairman, R.; Mitchell, M.; et al. Platelet factor 4 localization in carotid atherosclerotic plaques: Correlation with clinical parameters. Thromb. Haemost. 2003, 90, 1112–1120. [Google Scholar] [CrossRef] [PubMed]
- Aidoudi, S.; Bikfalvi, A. Interaction of PF4 (CXCL4) with the vasculature: A role in atherosclerosis and angiogenesis. Thromb. Haemost. 2010, 104, 941–948. [Google Scholar] [CrossRef]
- Gremmel, T.; Ay, C.; Riedl, J.; Kopp, C.W.; Eichelberger, B.; Koppensteiner, R.; Panzer, S. Platelet-specific markers are associated with monocyte-platelet aggregate formation and thrombin generation potential in advanced atherosclerosis. Thromb. Haemost. 2016, 115, 615–621. [Google Scholar] [CrossRef]
- Bhatnagar, P.; Lu, X.; Evans, M.K.; Laveist, T.A.; Zonderman, A.B.; Carter, D.L.; Arking, D.E.; Fletcher, C.A. Genetic variants in platelet factor 4 modulate inflammatory and platelet activation biomarkers. Circ. Cardiovasc. Genet. 2012, 5, 412–421. [Google Scholar] [CrossRef]
- Lord, M.S.; Cheng, B.; Farrugia, B.L.; McCarthy, S.; Whitelock, J.M. Platelet Factor 4 Binds to Vascular Proteoglycans and Controls Both Growth Factor Activities and Platelet Activation. J. Biol. Chem. 2017, 292, 4054–4063. [Google Scholar] [CrossRef] [PubMed]
- Sagris, M.; Theofilis, P.; Antonopoulos, A.S.; Tsioufis, C.; Oikonomou, E.; Antoniades, C.; Crea, F.; Kaski, J.C.; Tousoulis, D. Inflammatory Mechanisms in COVID-19 and Atherosclerosis: Current Pharmaceutical Perspectives. Int. J. Mol. Sci. 2021, 22, 6607. [Google Scholar] [CrossRef] [PubMed]
- Oikonomou, E.; Aznaouridis, K.; Barbetseas, J.; Charalambous, G.; Gastouniotis, I.; Fotopoulos, V.; Gkini, K.P.; Katsivas, A.; Koudounis, G.; Koudounis, P.; et al. Hospital attendance and admission trends for cardiac diseases during the COVID-19 outbreak and lockdown in Greece. Public Health 2020, 187, 115–119. [Google Scholar] [CrossRef] [PubMed]
- Lazaros, G.; Oikonomou, E.; Theofilis, P.; Theodoropoulou, A.; Triantafyllou, K.; Charitos, C.; Charalambous, G.; Papanikolaou, A.; Gastouniotis, I.; Siasos, G.; et al. The impact of COVID-19 pandemic on adult cardiac surgery procedures. Hell. J. Cardiol. 2021, 62, 231–233. [Google Scholar] [CrossRef] [PubMed]
- Klok, F.A.; Kruip, M.; van der Meer, N.J.M.; Arbous, M.S.; Gommers, D.; Kant, K.M.; Kaptein, F.H.J.; van Paassen, J.; Stals, M.A.M.; Huisman, M.V.; et al. Incidence of thrombotic complications in critically ill ICU patients with COVID-19. Thromb. Res. 2020, 191, 145–147. [Google Scholar] [CrossRef] [PubMed]
- Tan, B.K.; Mainbourg, S.; Friggeri, A.; Bertoletti, L.; Douplat, M.; Dargaud, Y.; Grange, C.; Lobbes, H.; Provencher, S.; Lega, J.C. Arterial and venous thromboembolism in COVID-19: A study-level meta-analysis. Thorax 2021, 76, 970–979. [Google Scholar] [CrossRef] [PubMed]
- Choudry, F.A.; Hamshere, S.M.; Rathod, K.S.; Akhtar, M.M.; Archbold, R.A.; Guttmann, O.P.; Woldman, S.; Jain, A.K.; Knight, C.J.; Baumbach, A.; et al. High Thrombus Burden in Patients With COVID-19 Presenting With ST-Segment Elevation Myocardial Infarction. J. Am. Coll. Cardiol. 2020, 76, 1168–1176. [Google Scholar] [CrossRef]
- Rodriguez-Leor, O.; Cid Alvarez, A.B.; Perez de Prado, A.; Rossello, X.; Ojeda, S.; Serrador, A.; Lopez-Palop, R.; Martin-Moreiras, J.; Rumoroso, J.R.; Cequier, A.; et al. In-hospital outcomes of COVID-19 ST-elevation myocardial infarction patients. EuroIntervention 2021, 16, 1426–1433. [Google Scholar] [CrossRef]
- Rapkiewicz, A.V.; Mai, X.; Carsons, S.E.; Pittaluga, S.; Kleiner, D.E.; Berger, J.S.; Thomas, S.; Adler, N.M.; Charytan, D.M.; Gasmi, B.; et al. Megakaryocytes and platelet-fibrin thrombi characterize multi-organ thrombosis at autopsy in COVID-19: A case series. EClinicalMedicine 2020, 24, 100434. [Google Scholar] [CrossRef]
- Portier, I.; Campbell, R.A. Role of Platelets in Detection and Regulation of Infection. Arterioscler. Thromb. Vasc. Biol. 2021, 41, 70–78. [Google Scholar] [CrossRef]
- Fox, S.E.; Akmatbekov, A.; Harbert, J.L.; Li, G.; Quincy Brown, J.; Vander Heide, R.S. Pulmonary and cardiac pathology in African American patients with COVID-19: An autopsy series from New Orleans. Lancet Respir. Med. 2020, 8, 681–686. [Google Scholar] [CrossRef]
- Khismatullin, R.R.; Ponomareva, A.A.; Nagaswami, C.; Ivaeva, R.A.; Montone, K.T.; Weisel, J.W.; Litvinov, R.I. Pathology of lung-specific thrombosis and inflammation in COVID-19. J. Thromb. Haemost. 2021. [Google Scholar] [CrossRef]
- Nauen, D.W.; Hooper, J.E.; Stewart, C.M.; Solomon, I.H. Assessing Brain Capillaries in Coronavirus Disease 2019. JAMA Neurol. 2021, 78, 760–762. [Google Scholar] [CrossRef]
- McMullen, P.; Smith, H.; Pytel, P. Entrapped Megakaryocytes in the Microvasculature of Brain Tissues are not Specific to COVID-19 but can be Seen Across a Spectrum of Acute Lung Injuries. J. Neuropathol. Exp. Neurol. 2021. [Google Scholar] [CrossRef]
- Johnson, J.E.; McGuone, D.; Xu, M.L.; Jane-Wit, D.; Mitchell, R.N.; Libby, P.; Pober, J.S. COVID Coronary Vascular Thrombosis: Correlation with Neutrophil but not Endothelial Activation. Am. J. Pathol. 2021. [Google Scholar] [CrossRef]
- Ackermann, M.; Verleden, S.E.; Kuehnel, M.; Haverich, A.; Welte, T.; Laenger, F.; Vanstapel, A.; Werlein, C.; Stark, H.; Tzankov, A.; et al. Pulmonary Vascular Endothelialitis, Thrombosis, and Angiogenesis in Covid-19. N. Engl. J. Med. 2020, 383, 120–128. [Google Scholar] [CrossRef] [PubMed]
- Maquet, J.; Lafaurie, M.; Sommet, A.; Moulis, G. Thrombocytopenia is independently associated with poor outcome in patients hospitalized for COVID-19. Br. J. Haematol. 2020, 190, e276–e279. [Google Scholar] [CrossRef]
- Xu, P.; Zhou, Q.; Xu, J. Mechanism of thrombocytopenia in COVID-19 patients. Ann. Hematol. 2020, 99, 1205–1208. [Google Scholar] [CrossRef] [PubMed]
- Thachil, J.; Lisman, T. Pulmonary Megakaryocytes in Coronavirus Disease 2019 (COVID-19): Roles in Thrombi and Fibrosis. Semin. Thromb. Hemost. 2020, 46, 831–834. [Google Scholar] [CrossRef] [PubMed]
- Yang, X.; Yang, Q.; Wang, Y.; Wu, Y.; Xu, J.; Yu, Y.; Shang, Y. Thrombocytopenia and its association with mortality in patients with COVID-19. J. Thromb. Haemost. 2020, 18, 1469–1472. [Google Scholar] [CrossRef] [PubMed]
- Wool, G.D.; Miller, J.L. The Impact of COVID-19 Disease on Platelets and Coagulation. Pathobiol. J. Immunopathol. Mol. Cell. Biol. 2021, 88, 15–27. [Google Scholar] [CrossRef]
- Cohen, A.; Harari, E.; Cipok, M.; Laish-Farkash, A.; Bryk, G.; Yahud, E.; Sela, Y.; Lador, N.K.; Mann, T.; Mayo, A.; et al. Immature platelets in patients hospitalized with Covid-19. J. Thromb. Thrombolysis 2021, 51, 608–616. [Google Scholar] [CrossRef]
- Bongiovanni, D.; Santamaria, G.; Klug, M.; Santovito, D.; Felicetta, A.; Hristov, M.; von Scheidt, M.; Aslani, M.; Cibella, J.; Weber, C.; et al. Transcriptome Analysis of Reticulated Platelets Reveals a Prothrombotic Profile. Thromb. Haemost. 2019, 119, 1795–1806. [Google Scholar] [CrossRef]
- Tang, W.H.; Stitham, J.; Gleim, S.; Di Febbo, C.; Porreca, E.; Fava, C.; Tacconelli, S.; Capone, M.; Evangelista, V.; Levantesi, G.; et al. Glucose and collagen regulate human platelet activity through aldose reductase induction of thromboxane. J. Clin. Investig. 2011, 121, 4462–4476. [Google Scholar] [CrossRef] [PubMed]
- Barale, C.; Russo, I. Influence of Cardiometabolic Risk Factors on Platelet Function. Int. J. Mol. Sci. 2020, 21, 623. [Google Scholar] [CrossRef] [PubMed]
- Varga, Z.; Flammer, A.J.; Steiger, P.; Haberecker, M.; Andermatt, R.; Zinkernagel, A.S.; Mehra, M.R.; Schuepbach, R.A.; Ruschitzka, F.; Moch, H. Endothelial cell infection and endotheliitis in COVID-19. Lancet 2020, 395, 1417–1418. [Google Scholar] [CrossRef]
- Qin, Z.; Liu, F.; Blair, R.; Wang, C.; Yang, H.; Mudd, J.; Currey, J.M.; Iwanaga, N.; He, J.; Mi, R.; et al. Endothelial cell infection and dysfunction, immune activation in severe COVID-19. Theranostics 2021, 11, 8076–8091. [Google Scholar] [CrossRef]
- Canzano, P.; Brambilla, M.; Porro, B.; Cosentino, N.; Tortorici, E.; Vicini, S.; Poggio, P.; Cascella, A.; Pengo, M.F.; Veglia, F.; et al. Platelet and Endothelial Activation as Potential Mechanisms Behind the Thrombotic Complications of COVID-19 Patients. JACC Basic Transl. Sci. 2021, 6, 202–218. [Google Scholar] [CrossRef] [PubMed]
- Melkumyants, A.; Buryachkovskaya, L.; Lomakin, N.; Antonova, O.; Serebruany, V. Mild COVID-19 and Impaired Blood Cell-Endothelial Crosstalk: Considering Long-Term Use of Antithrombotics? Thromb. Haemost. 2021. [Google Scholar] [CrossRef]
- Goshua, G.; Pine, A.B.; Meizlish, M.L.; Chang, C.H.; Zhang, H.; Bahel, P.; Baluha, A.; Bar, N.; Bona, R.D.; Burns, A.J.; et al. Endotheliopathy in COVID-19-associated coagulopathy: Evidence from a single-centre, cross-sectional study. Lancet Haematol. 2020, 7, e575–e582. [Google Scholar] [CrossRef]
- Rovas, A.; Osiaevi, I.; Buscher, K.; Sackarnd, J.; Tepasse, P.R.; Fobker, M.; Kuhn, J.; Braune, S.; Gobel, U.; Tholking, G.; et al. Microvascular dysfunction in COVID-19: The MYSTIC study. Angiogenesis 2021, 24, 145–157. [Google Scholar] [CrossRef]
- Stahl, K.; Gronski, P.A.; Kiyan, Y.; Seeliger, B.; Bertram, A.; Pape, T.; Welte, T.; Hoeper, M.M.; Haller, H.; David, S. Injury to the Endothelial Glycocalyx in Critically Ill Patients with COVID-19. Am. J. Respir. Crit. Care Med. 2020, 202, 1178–1181. [Google Scholar] [CrossRef]
- Lambadiari, V.; Mitrakou, A.; Kountouri, A.; Thymis, J.; Katogiannis, K.; Korakas, E.; Varlamos, C.; Andreadou, I.; Tsoumani, M.; Triantafyllidi, H.; et al. Association of COVID-19 with impaired endothelial glycocalyx, vascular function and myocardial deformation 4 months after infection. Eur. J. Heart Fail. 2021. [Google Scholar] [CrossRef]
- Fogarty, H.; Townsend, L.; Morrin, H.; Ahmad, A.; Comerford, C.; Karampini, E.; Englert, H.; Byrne, M.; Bergin, C.; O’Sullivan, J.M.; et al. Persistent endotheliopathy in the pathogenesis of long COVID syndrome. J. Thromb. Haemost. JTH 2021, 19, 2546–2553. [Google Scholar] [CrossRef] [PubMed]
- Cenko, E.; Badimon, L.; Bugiardini, R.; Claeys, M.J.; De Luca, G.; de Wit, C.; Derumeaux, G.; Dorobantu, M.; Duncker, D.J.; Eringa, E.C.; et al. Cardiovascular disease and COVID-19: A consensus paper from the ESC Working Group on Coronary Pathophysiology & Microcirculation, ESC Working Group on Thrombosis and the Association for Acute CardioVascular Care (ACVC), in collaboration with the European Heart Rhythm Association (EHRA). Cardiovasc. Res. 2021. [Google Scholar] [CrossRef]
- Barrett, T.J.; Cornwell, M.; Myndzar, K.; Rolling, C.C.; Xia, Y.; Drenkova, K.; Biebuyck, A.; Fields, A.T.; Tawil, M.; Luttrell-Williams, E.; et al. Platelets amplify endotheliopathy in COVID-19. Sci. Adv. 2021, 7, eabh2434. [Google Scholar] [CrossRef] [PubMed]
- Moore, J.B.; June, C.H. Cytokine release syndrome in severe COVID-19. Science 2020, 368, 473–474. [Google Scholar] [CrossRef] [PubMed]
- Sacchi, A.; Grassi, G.; Notari, S.; Gili, S.; Bordoni, V.; Tartaglia, E.; Casetti, R.; Cimini, E.; Mariotti, D.; Garotto, G.; et al. Expansion of Myeloid Derived Suppressor Cells Contributes to Platelet Activation by L-Arginine Deprivation during SARS-CoV-2 Infection. Cells 2021, 10, 2111. [Google Scholar] [CrossRef] [PubMed]
- Sacchi, A.; Grassi, G.; Bordoni, V.; Lorenzini, P.; Cimini, E.; Casetti, R.; Tartaglia, E.; Marchioni, L.; Petrosillo, N.; Palmieri, F.; et al. Early expansion of myeloid-derived suppressor cells inhibits SARS-CoV-2 specific T-cell response and may predict fatal COVID-19 outcome. Cell Death Dis. 2020, 11, 921. [Google Scholar] [CrossRef]
- Manne, B.K.; Denorme, F.; Middleton, E.A.; Portier, I.; Rowley, J.W.; Stubben, C.; Petrey, A.C.; Tolley, N.D.; Guo, L.; Cody, M.; et al. Platelet gene expression and function in patients with COVID-19. Blood 2020, 136, 1317–1329. [Google Scholar] [CrossRef]
- Barrett, T.J.; Bilaloglu, S.; Cornwell, M.; Burgess, H.M.; Virginio, V.W.; Drenkova, K.; Ibrahim, H.; Yuriditsky, E.; Aphinyanaphongs, Y.; Lifshitz, M.; et al. Platelets contribute to disease severity in COVID-19. J. Thromb. Haemost. 2021. [Google Scholar] [CrossRef] [PubMed]
- Gadanec, L.K.; McSweeney, K.R.; Qaradakhi, T.; Ali, B.; Zulli, A.; Apostolopoulos, V. Can SARS-CoV-2 Virus Use Multiple Receptors to Enter Host Cells? Int. J. Mol. Sci. 2021, 22, 992. [Google Scholar] [CrossRef]
- Cunin, P.; Bouslama, R.; Machlus, K.R.; Martinez-Bonet, M.; Lee, P.Y.; Wactor, A.; Nelson-Maney, N.; Morris, A.; Guo, L.; Weyrich, A.; et al. Megakaryocyte emperipolesis mediates membrane transfer from intracytoplasmic neutrophils to platelets. eLife 2019, 8. [Google Scholar] [CrossRef]
- Hottz, E.D.; Azevedo-Quintanilha, I.G.; Palhinha, L.; Teixeira, L.; Barreto, E.A.; Pao, C.R.R.; Righy, C.; Franco, S.; Souza, T.M.L.; Kurtz, P.; et al. Platelet activation and platelet-monocyte aggregate formation trigger tissue factor expression in patients with severe COVID-19. Blood 2020, 136, 1330–1341. [Google Scholar] [CrossRef] [PubMed]
- Zuo, Y.; Yalavarthi, S.; Shi, H.; Gockman, K.; Zuo, M.; Madison, J.A.; Blair, C.; Weber, A.; Barnes, B.J.; Egeblad, M.; et al. Neutrophil extracellular traps in COVID-19. JCI Insight 2020, 5. [Google Scholar] [CrossRef]
- Middleton, E.A.; He, X.Y.; Denorme, F.; Campbell, R.A.; Ng, D.; Salvatore, S.P.; Mostyka, M.; Baxter-Stoltzfus, A.; Borczuk, A.C.; Loda, M.; et al. Neutrophil extracellular traps contribute to immunothrombosis in COVID-19 acute respiratory distress syndrome. Blood 2020, 136, 1169–1179. [Google Scholar] [CrossRef] [PubMed]
- Petito, E.; Falcinelli, E.; Paliani, U.; Cesari, E.; Vaudo, G.; Sebastiano, M.; Cerotto, V.; Guglielmini, G.; Gori, F.; Malvestiti, M.; et al. Association of Neutrophil Activation, More Than Platelet Activation, With Thrombotic Complications in Coronavirus Disease 2019. J. Infect. Dis. 2021, 223, 933–944. [Google Scholar] [CrossRef] [PubMed]
- Comer, S.P.; Cullivan, S.; Szklanna, P.B.; Weiss, L.; Cullen, S.; Kelliher, S.; Smolenski, A.; Murphy, C.; Altaie, H.; Curran, J.; et al. COVID-19 induces a hyperactive phenotype in circulating platelets. PLoS Biol. 2021, 19, e3001109. [Google Scholar] [CrossRef]
- Cappellano, G.; Raineri, D.; Rolla, R.; Giordano, M.; Puricelli, C.; Vilardo, B.; Manfredi, M.; Cantaluppi, V.; Sainaghi, P.P.; Castello, L.; et al. Circulating Platelet-Derived Extracellular Vesicles Are a Hallmark of Sars-Cov-2 Infection. Cells 2021, 10, 85. [Google Scholar] [CrossRef]
- Fricke, A.; Ullrich, P.V.; Cimniak, A.F.V.; Becherer, C.; Follo, M.; Heinz, J.; Scholber, J.; Herget, G.W.; Hauschild, O.; Wittel, U.A.; et al. Levels of activated platelet-derived microvesicles in patients with soft tissue sarcoma correlate with an increased risk of venous thromboembolism. BMC Cancer 2017, 17, 527. [Google Scholar] [CrossRef]
- Zaid, Y.; Puhm, F.; Allaeys, I.; Naya, A.; Oudghiri, M.; Khalki, L.; Limami, Y.; Zaid, N.; Sadki, K.; Ben El Haj, R.; et al. Platelets Can Associate with SARS-Cov-2 RNA and Are Hyperactivated in COVID-19. Circ. Res. 2020. [Google Scholar] [CrossRef]
- Nidorf, S.M.; Fiolet, A.T.L.; Mosterd, A.; Eikelboom, J.W.; Schut, A.; Opstal, T.S.J.; The, S.H.K.; Xu, X.F.; Ireland, M.A.; Lenderink, T.; et al. Colchicine in Patients with Chronic Coronary Disease. N. Engl. J. Med. 2020, 383, 1838–1847. [Google Scholar] [CrossRef]
- Visseren, F.L.J.; Mach, F.; Smulders, Y.M.; Carballo, D.; Koskinas, K.C.; Back, M.; Benetos, A.; Biffi, A.; Boavida, J.M.; Capodanno, D.; et al. 2021 ESC Guidelines on cardiovascular disease prevention in clinical practice. Eur. Heart J. 2021, 42, 3227–3337. [Google Scholar] [CrossRef]
- Fiolet, A.T.L.; Opstal, T.S.J.; Mosterd, A.; Eikelboom, J.W.; Jolly, S.S.; Keech, A.C.; Kelly, P.; Tong, D.C.; Layland, J.; Nidorf, S.M.; et al. Efficacy and safety of low-dose colchicine in patients with coronary disease: A systematic review and meta-analysis of randomized trials. Eur. Heart J. 2021, 42, 2765–2775. [Google Scholar] [CrossRef]
- Ridker, P.M.; Everett, B.M.; Pradhan, A.; MacFadyen, J.G.; Solomon, D.H.; Zaharris, E.; Mam, V.; Hasan, A.; Rosenberg, Y.; Iturriaga, E.; et al. Low-Dose Methotrexate for the Prevention of Atherosclerotic Events. N. Engl. J. Med. 2019, 380, 752–762. [Google Scholar] [CrossRef]
- Ljung, L.; Rantapaa-Dahlqvist, S.; Jacobsson, L.T.; Askling, J. Response to biological treatment and subsequent risk of coronary events in rheumatoid arthritis. Ann. Rheum. Dis. 2016, 75, 2087–2094. [Google Scholar] [CrossRef] [PubMed]
- Padfield, G.J.; Din, J.N.; Koushiappi, E.; Mills, N.L.; Robinson, S.D.; Cruden Nle, M.; Lucking, A.J.; Chia, S.; Harding, S.A.; Newby, D.E. Cardiovascular effects of tumour necrosis factor alpha antagonism in patients with acute myocardial infarction: A first in human study. Heart 2013, 99, 1330–1335. [Google Scholar] [CrossRef] [PubMed]
- Nielsen, C.B.; Nielsen, C.; Nybo, M.; Just, S.A.; Vinholt, P.J. The in vitro effect of antirheumatic drugs on platelet function. Platelets 2020, 31, 248–257. [Google Scholar] [CrossRef]
- Shah, B.; Allen, N.; Harchandani, B.; Pillinger, M.; Katz, S.; Sedlis, S.P.; Echagarruga, C.; Samuels, S.K.; Morina, P.; Singh, P.; et al. Effect of Colchicine on Platelet-Platelet and Platelet-Leukocyte Interactions: A Pilot Study in Healthy Subjects. Inflammation 2016, 39, 182–189. [Google Scholar] [CrossRef] [PubMed]
- Di Nisio, M.; Potere, N.; Candeloro, M.; Spacone, A.; Pieramati, L.; Ferrandu, G.; Rizzo, G.; La Vella, M.; Di Carlo, S.; Cibelli, D.; et al. Interleukin-6 receptor blockade with subcutaneous tocilizumab improves coagulation activity in patients with COVID-19. Eur. J. Intern. Med. 2021, 83, 34–38. [Google Scholar] [CrossRef] [PubMed]
- Gergi, M.; Cushman, M.; Littenberg, B.; Budd, R.C. Thrombo-inflammation response to Tocilizumab in COVID-19. Res. Pract. Thromb. Haemost. 2020. [Google Scholar] [CrossRef] [PubMed]
- Cirillo, P.; Taglialatela, V.; Pellegrino, G.; Morello, A.; Conte, S.; Di Serafino, L.; Cimmino, G. Effects of colchicine on platelet aggregation in patients on dual antiplatelet therapy with aspirin and clopidogrel. J. Thromb. Thrombolysis 2020, 50, 468–472. [Google Scholar] [CrossRef]
- Cimmino, G.; Tarallo, R.; Conte, S.; Morello, A.; Pellegrino, G.; Loffredo, F.S.; Cali, G.; De Luca, N.; Golino, P.; Trimarco, B.; et al. Colchicine reduces platelet aggregation by modulating cytoskeleton rearrangement via inhibition of cofilin and LIM domain kinase 1. Vasc. Pharmacol. 2018, 111, 62–70. [Google Scholar] [CrossRef] [PubMed]
- Pennings, G.J.; Reddel, C.J.; Traini, M.; Campbell, H.; Chen, V.; Kritharides, L. Colchicine inhibits ROS generation in response to glycoprotein VI stimulation. Sci. Rep. 2021, 11, 11965. [Google Scholar] [CrossRef] [PubMed]
- Di Sabatino, A.; Santilli, F.; Guerci, M.; Simeone, P.; Ardizzone, S.; Massari, A.; Giuffrida, P.; Tripaldi, R.; Malara, A.; Liani, R.; et al. Oxidative stress and thromboxane-dependent platelet activation in inflammatory bowel disease: Effects of anti-TNF-alpha treatment. Thromb. Haemost. 2016, 116, 486–495. [Google Scholar] [CrossRef]
- Menchen, L.; Marin-Jimenez, I.; Arias-Salgado, E.G.; Fontela, T.; Hernandez-Sampelayo, P.; Rodriguez, M.C.; Butta, N.V. Matrix metalloproteinase 9 is involved in Crohn’s disease-associated platelet hyperactivation through the release of soluble CD40 ligand. Gut 2009, 58, 920–928. [Google Scholar] [CrossRef]
- DeSena, A.D.; Do, T.; Schulert, G.S. Systemic autoinflammation with intractable epilepsy managed with interleukin-1 blockade. J. Neuroinflamm. 2018, 15, 38. [Google Scholar] [CrossRef]
- Li, T.; Wang, C.; Liu, Y.; Li, B.; Zhang, W.; Wang, L.; Yu, M.; Zhao, X.; Du, J.; Zhang, J.; et al. Neutrophil Extracellular Traps Induce Intestinal Damage and Thrombotic Tendency in Inflammatory Bowel Disease. J. Crohn’s Colitis 2020, 14, 240–253. [Google Scholar] [CrossRef]
- Carminita, E.; Crescence, L.; Brouilly, N.; Altie, A.; Panicot-Dubois, L.; Dubois, C. DNAse-dependent, NET-independent pathway of thrombus formation in vivo. Proc. Natl. Acad. Sci. USA 2021, 118. [Google Scholar] [CrossRef]
- Okur, H.K.; Yalcin, K.; Tastan, C.; Demir, S.; Yurtsever, B.; Karakus, G.S.; Kancagi, D.D.; Abanuz, S.; Seyis, U.; Zengin, R.; et al. Preliminary report of in vitro and in vivo effectiveness of dornase alfa on SARS-CoV-2 infection. New Microbes New Infect. 2020, 37, 100756. [Google Scholar] [CrossRef]
- Weber, A.G.; Chau, A.S.; Egeblad, M.; Barnes, B.J.; Janowitz, T. Nebulized in-line endotracheal dornase alfa and albuterol administered to mechanically ventilated COVID-19 patients: A case series. Mol. Med. 2020, 26, 91. [Google Scholar] [CrossRef] [PubMed]
- Toma, A.; Darwish, C.; Taylor, M.; Harlacher, J.; Darwish, R. The Use of Dornase Alfa in the Management of COVID-19-Associated Adult Respiratory Distress Syndrome. Crit. Care Res. Pract. 2021, 2021, 8881115. [Google Scholar] [CrossRef]
- Novotny, J.; Chandraratne, S.; Weinberger, T.; Philippi, V.; Stark, K.; Ehrlich, A.; Pircher, J.; Konrad, I.; Oberdieck, P.; Titova, A.; et al. Histological comparison of arterial thrombi in mice and men and the influence of Cl-amidine on thrombus formation. PLoS ONE 2018, 13, e0190728. [Google Scholar] [CrossRef]
- Clark, S.R.; Ma, A.C.; Tavener, S.A.; McDonald, B.; Goodarzi, Z.; Kelly, M.M.; Patel, K.D.; Chakrabarti, S.; McAvoy, E.; Sinclair, G.D.; et al. Platelet TLR4 activates neutrophil extracellular traps to ensnare bacteria in septic blood. Nat. Med. 2007, 13, 463–469. [Google Scholar] [CrossRef]
- Sun, J.; Zhang, M.; Chen, K.; Chen, B.; Zhao, Y.; Gong, H.; Zhao, X.; Qi, R. Suppression of TLR4 activation by resveratrol is associated with STAT3 and Akt inhibition in oxidized low-density lipoprotein-activated platelets. Eur. J. Pharmacol. 2018, 836, 1–10. [Google Scholar] [CrossRef]
- Hally, K.E.; La Flamme, A.C.; Harding, S.A.; Larsen, P.D. The effects of aspirin and ticagrelor on Toll-like receptor (TLR)-mediated platelet activation: Results of a randomized, cross-over trial. Platelets 2019, 30, 599–607. [Google Scholar] [CrossRef]
- Kovacevic, K.D.; Buchtele, N.; Schoergenhofer, C.; Derhaschnig, U.; Gelbenegger, G.; Brostjan, C.; Zhu, S.; Gilbert, J.C.; Jilma, B. The aptamer BT200 effectively inhibits von Willebrand factor (VWF) dependent platelet function after stimulated VWF release by desmopressin or endotoxin. Sci. Rep. 2020, 10, 11180. [Google Scholar] [CrossRef]
- Nimjee, S.M.; Dornbos, D., 3rd; Pitoc, G.A.; Wheeler, D.G.; Layzer, J.M.; Venetos, N.; Huttinger, A.; Talentino, S.E.; Musgrave, N.J.; Moody, H.; et al. Preclinical Development of a vWF Aptamer to Limit Thrombosis and Engender Arterial Recanalization of Occluded Vessels. Mol. Ther. J. Am. Soc. Gene Ther. 2019, 27, 1228–1241. [Google Scholar] [CrossRef]
- Nicolson, P.L.R.; Nock, S.H.; Hinds, J.; Garcia-Quintanilla, L.; Smith, C.W.; Campos, J.; Brill, A.; Pike, J.A.; Khan, A.O.; Poulter, N.S.; et al. Low-dose Btk inhibitors selectively block platelet activation by CLEC-2. Haematologica 2021, 106, 208–219. [Google Scholar] [CrossRef] [PubMed]
- Dobie, G.; Kuriri, F.A.; Omar, M.M.A.; Alanazi, F.; Gazwani, A.M.; Tang, C.P.S.; Sze, D.M.; Handunnetti, S.M.; Tam, C.; Jackson, D.E. Ibrutinib, but not zanubrutinib, induces platelet receptor shedding of GPIb-IX-V complex and integrin alphaIIbbeta3 in mice and humans. Blood Adv. 2019, 3, 4298–4311. [Google Scholar] [CrossRef] [PubMed]
- Ninomoto, J.; Mokatrin, A.; Kinoshita, T.; Marimpietri, C.; Barrett, T.D.; Chang, B.Y.; Sukbuntherng, J.; James, D.F.; Crowther, M. Effects of ibrutinib on in vitro platelet aggregation in blood samples from healthy donors and donors with platelet dysfunction. Hematology 2020, 25, 112–117. [Google Scholar] [CrossRef] [PubMed]
- Cornelius, D.C.; Travis, O.K.; Tramel, R.W.; Borges-Rodriguez, M.; Baik, C.H.; Greer, M.; Giachelli, C.A.; Tardo, G.A.; Williams, J.M. NLRP3 inflammasome inhibition attenuates sepsis-induced platelet activation and prevents multi-organ injury in cecal-ligation puncture. PLoS ONE 2020, 15, e0234039. [Google Scholar] [CrossRef] [PubMed]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).