Fibroblast, Epithelial and Endothelial Cell-Derived Human Cytomegalovirus Strains Display Distinct Neutralizing Antibody Responses and Varying Levels of gH/gL Complexes
Abstract
:1. Introduction
2. Results
2.1. NAb Titer of Sequential Sera from 3 Patients (p-232, p-236, and p-237) vs. Homologous and Heterologous HCMV Strains (VR#1, VR#2, and VR#3, Respectively)
2.2. NAb Titers vs. VR#1814
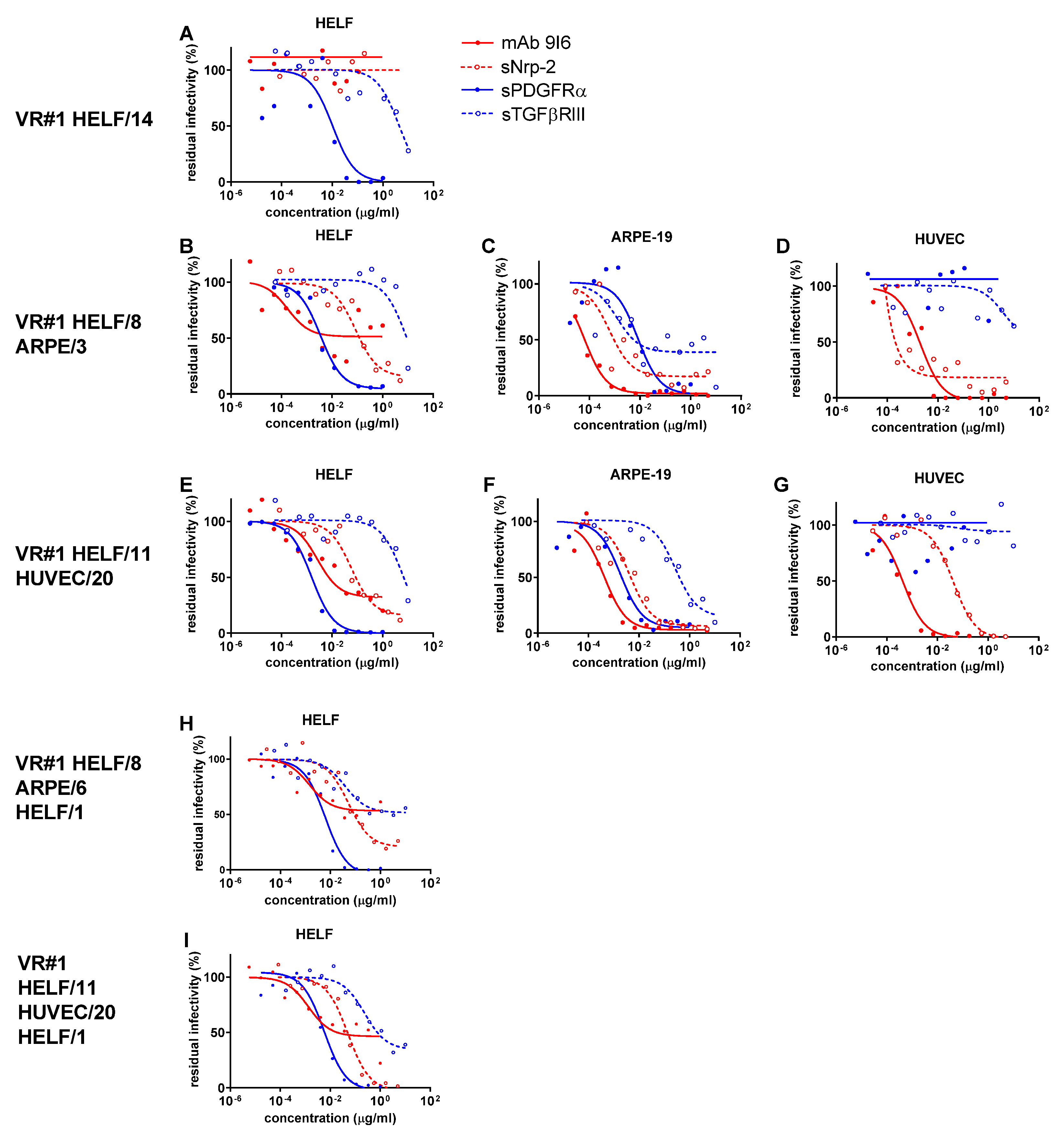
2.3. Residual HCMV Infectivity (VR#1 to VR#3) following NAb Inhibition by PC-Specific and TC-Specific Inhibitors in Different Cell Cultures
2.4. Expression of PC and TC in Different Virus Preparations
2.5. ELISA IgG Antibody Response to gCs
3. Discussion
4. Materials and Methods
4.1. Cell Cultures
4.2. Study Population and HCMV Strains
4.3. Genotyping of HCMV Strains
4.4. Cross-Neutralization Assays
4.5. Inhibition Assays
4.6. Expression of PC and TC on Virus Preparations
4.7. Immunoblotting
4.8. Determination of IgG Antibodies to PC, TC, and gB by ELISA
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Chou, S.W.; Dennison, K.M. Analysis of interstrain variation in cytomegalovirus glycoprotein B sequences encoding neutralization-related epitopes. J. Infect. Dis. 1991, 163, 1229–1234. [Google Scholar] [CrossRef] [PubMed]
- Chou, S.W. Molecular epidemiology of envelope glycoprotein H of human cytomegalovirus. J. Infect. Dis. 1992, 166, 604–607. [Google Scholar] [CrossRef] [PubMed]
- Urban, M.; Britt, W.; Mach, M. The dominant linear neutralizing antibody-binding site of glycoprotein gp86 of human cytomegalovirus is strain-specific. J. Virol. 1992, 66, 1303–1311. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Burkhardt, C.; Himmelein, S.; Britt, W.; Winkler, T.; Mach, M. Glycoprotein N subtypes of human cytomegalovirus induce a strain-specific antibody response during natural infection. J. Gen. Virol. 1992, 90, 1951–1961. [Google Scholar] [CrossRef] [PubMed]
- Pati, S.K.; Novak, Z.; Purser, M.; Arora, N.; Mach, M.; Britt, W.J.; Boppana, S.B. Strain-specific neutralizing antibody responses against human cytomegalovirus envelope glycoprotein N. Clin. Vacc. Immunol. 2012, 19, 909–913. [Google Scholar] [CrossRef] [Green Version]
- Wille, P.T.; Knoche, A.J.; Nelson, J.A.; Jarvis, M.A.; Johnson, D.C. A human cytomegalovirus gO-null mutant fails to incorporate gH/gL into the virion envelope and is unable to enter fibroblasts and epithelial and endothelial cells. J. Virol. 2010, 84, 2585–2596. [Google Scholar] [CrossRef] [Green Version]
- Hahn, G.; Revello, M.G.; Patrone, M.; Percivalle, E.; Campanini, G.; Sarasini, A.; Wagner, M.; Gallina, A.; Milanesi, G.; Koszinowski, U.; et al. Human cytomegalovirus UL131-128 genes are indispensable for virus growth in endothelial cells and virus transfer to leukocytes. J. Virol. 2004, 78, 10023–10033. [Google Scholar] [CrossRef] [Green Version]
- Ryckman, B.J.; Chase, M.C.; Johnson, D.C. HCMV gH/gL/UL128-131 interferes with virus entry into epithelial cell: Evidence for type-specific receptors. Proc. Natl. Acad. Sci. USA 2008, 105, 14118–14123. [Google Scholar] [CrossRef] [Green Version]
- Kabanova, A.; Marcandalli, J.; Zhou, T.; Bianchi, S.; Baxa, U.; Tsybovski, Y.; Lilleri, D.; Silacci-Fregni, C.; Foglierini, M.; Fernandez-Rodriguez, B.M.; et al. Platelet-derived growth factor-alpha receptor is the cellular receptor for human cytomegalovirus gHgLgO trimer. Nat. Microbiol. 2016, 1, 16082. [Google Scholar] [CrossRef] [Green Version]
- Martinez-Martin, N.; Marcandalli, J.; Huang, C.S.; Arthur, C.P.; Perotti, M.; Foglierini, M.; Ho, H.; Dosey, A.M.; Shriver, S.; Payandeh, J.; et al. An unbiased screen for human cytomegalovirus identifies neuropilin-2 as a central viral receptor. Cell 2018, 174, 1158–1171. [Google Scholar] [CrossRef] [Green Version]
- Lilleri, D.; Kabanova, A.; Revello, M.G.; Percivalle, E.; Sarasini, A.; Genini, E.; Sallusto, F.; Lanzavecchia, A.; Corti, D.; Gerna, G. Fetal human cytomegalovirus transmission correlates with delayed maternal antibodies to gH/gL/pUL128-130-131 complex during primary infection. PLoS ONE 2013, 8, e59863. [Google Scholar] [CrossRef] [Green Version]
- Kabanova, A.; Perez, L.; Lilleri, D.; Marcandalli, J.; Agatic, G.; Becattini, S.; Preite, S.; Fuschillo, D.; Percivalle, E.; Sallusto, F.; et al. Antibody-driven design of a human cytomegalovirus gHgLpUL128L subunit vaccine that selectively elicits potent neutralizing antibodies. Proc. Natl. Acad. Sci. USA 2014, 111, 17965–17970. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Fouts, A.E.; Chan, P.; Stefan, J.P.; Vandler, R.; Feierbach, B. Antibodies against the gH/gL/UL128/UL130/UL131 complex comprise the majority of the anti-cytomegalovirus (anti-CMV) neutralizing antibody response in CMV hyperimmune globulin. J. Virol. 2012, 86, 7444–7447. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Macagno, A.; Bernasconi, N.; Vanzetta, F.; Dander, E.; Sarasini, A.; Revello, M.G.; Gerna, G.; Sallusto, F.; Lanzavecchia, A. Isolation of human monoclonal antibodies that potently neutralize HCMV infection by targeting different epitopes on the gH/gL/UL128-131A complex. J. Virol. 2010, 84, 1005–1113. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Vanarsdall, A.L.; Chin, A.L.; Liu, J.; Jardetzky, T.S.; Mudd, J.O.; Orloff, S.L.; Streblow, D.; Mussi-Pinhata, M.M.; Yamamoto, A.Y.; Duarte, G.; et al. HCMV trimer-and pentamer-specific antibodies synergize for virus neutralization but do not correlate with congenital transmission. Proc. Natl. Acad. Sci. USA 2019, 116, 3728–3733. [Google Scholar] [CrossRef] [Green Version]
- Lilleri, D.; Gerna, G.; Furione, M.; Zavattoni, M.; Spinillo, A. Neutralizing and ELISA IgG antibodies to human cytomegalovirus glycoprotein complexes may help date the onset of primary infection in pregnancy. J. Clin. Virol. 2016, 81, 16–24. [Google Scholar] [CrossRef] [PubMed]
- Gerna, G.; Sarasini, A.; Patrone, M.; Percivalle, E.; Fiorina, L.; Campanini, G.; Gallina, A.; Baldanti, F.; Revello, M.G. Human cytomegalovirus serum neutralizing antibodies block virus infection of endothelial/epithelial cells, but not fibroblasts, early during primary infection. J. Gen. Virol. 2008, 89, 853–865. [Google Scholar] [CrossRef]
- Zhou, M.; Yu, Q.; Wechsler, A.; Ryckman, B.J. Comparative analysis of gO isoforms reveals that strains of human cytomegalovirus differ in the ratio of gH/gL/gO and gH/gL/UL128-131 in the virion envelope. J. Virol. 2013, 87, 9680–9690. [Google Scholar] [CrossRef] [Green Version]
- Zhang, L.; Zhou, M.; Stanton, R.; Kamil, J.; Ryckman, B.J. Expression levels of glycoprotein O (gO) vary between strains of human cytomegalovirus, influencing the assembly of gH/gL complexes and virion infectivity. J. Virol. 2018, 92, e00606-18. [Google Scholar] [CrossRef] [Green Version]
- Zhou, M.; Lanchy, J.-M.; Ryckman, B.J. Human cytomegalovirus gH/gL/gO promotes the fusion step of entry into all cell types, whereas gH/gL/UL128-131 broadens virus tropism through a distinct mechanism. J. Virol. 2015, 89, 8999–9009. [Google Scholar] [CrossRef] [Green Version]
- Gerna, G.; Percivalle, E.; Lilleri, D.; Lozza, L.; Fornara, C.; Hahn, G.; Baldanti, F.; Revello, M.G. Dendritic-cell infection by human cytomegalovirus is restricted to strains carrying functional UL131-128 genes and mediates efficient viral antigen presentation to CD8+ T cells. J. Gen. Virol. 2005, 86, 275–284. [Google Scholar] [CrossRef] [PubMed]
- Liu, J.; Jardetzky, T.S.; Chin, A.L.; Johnson, D.C.; Vanarsdall, A.L. The human cytomegalovirus trimer and pentamer promote sequential steps in entry into epithelial and endothelial cells at cell surfaces and endosomes. J. Virol. 2018, 92, e01336-18. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Nguyen, C.C.; Kamil, J.P. Pathogen at the gates: Human cytomegalovirus entry and cell tropism. Viruses 2018, 10, 704. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Kschonsak, M.; Rougè, L.; Arthur, C.P.; Hoangdung, H.; Patel, N.; Kim, I.; Johnson, M.C.; Kraft, E.; Rohou, A.L.; Gill, A.; et al. Structures of HCMV trimer reveal the basis for receptor recognition and cell entry. Cell 2021, 184, 1232–1246. [Google Scholar] [CrossRef] [PubMed]
- Borza, C.M.; Hutt-Fletcher, L.M. Alternate replication in B cells and epithelial cells switches tropism of Epstein-Barr virus. Nat. Med. 2002, 8, 594–599. [Google Scholar] [CrossRef] [PubMed]
- Scrivano, L.; Sinzger, C.; Nitschko, H.; Koszinowski, U.H.; Adler, B. HCMV spread and cell tropism are determined by distinct virus populations. PLoS Pathog. 2011, 7, e1001256. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Schultz, E.P.; Lanchy, J.-M.; Day, L.Z.; Yu, Q.; Peterson, C.; Preece, J.; Ryckman, B.J. Specialization for cell-free or cell-to-cell spread of Bac-cloned human cytomegalovirus strains is determined by factors beyond the UL128-131 and RL13 loci. J. Virol. 2020, 94, e00034-20. [Google Scholar] [CrossRef]
- Furione, M.; Rognoni, V.; Cabano, E.; Baldanti, F. Kinetics of human cytomegalovirus (HCMV) DNAemia in transplanted patients expressed in international units as determined with the Abbott RealTime CMV assay and an in-house assay. J. Clin. Virol. 2012, 50, 317–322. [Google Scholar] [CrossRef]
- Revello, M.G.; Furione, M.; Rognoni, V.; Arossa, A.; Gerna, G. Cytomegalovirus DNAemia in pregnant women. J. Clin. Virol. 2014, 61, 590–592. [Google Scholar] [CrossRef]
- Suarez, N.M.; Wilkie, G.S.; Hage, E.; Camiolo, S.; Holton, M.; Hughes, J.; Maabar, M.; Vattipally, S.B.; Dhingra, A.; Gompels, U.A.; et al. Human cytomegalovirus genomes sequenced directly from clinical material: Variation, multiple-strain infection, recombination, and gene loss. J. Infect. Dis. 2019, 220, 781–791. [Google Scholar] [CrossRef] [Green Version]
- De Vries, J.J.; Wessel, E.; Korver, A.M.; van der Eijk, A.A.; Rusman, L.G.; Kroes, A.C.; Vossen, A.C. Rapid genotyping of cytomegalovirus in dried blood spots by multiplex real-time PCR assays targeting the envelope glycoprotein B and gH genes. J. Clin. Microbiol. 2012, 50, 232–237. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Mattick, C.; Dewin, D.; Polley, S.; Sevilla-Reyes, E.; Pignatelli, S.; Rawlinson, W.; Wilkindson, G.; Dal Monte, P.; Gompels, U.A. Linkage of human cytomegalovirus glycoprotein gO variant groups identified from worldwide clinical isolates with gN genotypes, implications for disease associations and evidence for N-terminal sites of positive selection. Virology 2004, 318, 582–597. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Revello, M.G.; Baldanti, F.; Percivalle, E.; Sarasini, A.; De-Giuli, L.; Genini, E.; Lilleri, D.; Labò, N.; Gerna, G. In vitro selection of human cytomegalovirus variants unable to transfer virus and virus products from infected cells to polymorphonuclear leukocytes and to grow in endothelial cells. J. Gen. Virol. 2001, 82, 1429–1438. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Murrell, I.; Bedford, C.; Ladell, K.; Miners, K.L.; Price, D.A.; Tomasec, P.; Wilkinson, G.W.G.; Stanton, R.J. The pentameric complex drives immunologically covert cell-cell transmission of wild-type human cytomegalovirus. Proc. Natl. Acad. Sci. USA 2017, 114, 6104–6109. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Al Qaffas, A.; Camiolo, S.; Vo, M.; Aguiar, A.; Ourahmane, A.; Sorono, M.; Davison, A.J.; McVoy, M.A.; Hertel, L. Genome sequences of human cytomegalovirus strain TB40/E variants propagated in fibroblasts and epithelial cells. Virol. J. 2021, 18, 112. [Google Scholar] [CrossRef] [PubMed]
- Vo, M.; Aguiar, A.; McVoy, M.A.; Hertel, L. Cytomegalovirus Strain TB40/E Restrictions and Adaptations to Growth in ARPE-19 Epithelial Cells. Microorganisms 2020, 8, 615. [Google Scholar] [CrossRef]
- Lilleri, D.; Kabanova, A.; Lanzavecchia, A.; Gerna, G. Antibodies against neutralization epitopes of human cytomegalovirus gH/gL/pUL128-130-131 complex and virus spreading may correlate with virus control in vivo. J. Clin. Immunol. 2012, 32, 1324–1331. [Google Scholar] [CrossRef]
- E, X.; Meraner, P.; Lu, P.; Perreira, J.M.; Aker, A.M.; McDougall, W.M.; Zhu, R.; Chan, G.C.; Gerstein, R.M.; Caposio, P.; et al. OR14I1 is a receptor for the human cytomegalovirus pentameric complex and defines viral epithelial cell tropism. Proc. Natl. Acad. Sci. USA 2019, 116, 7043–7052. [Google Scholar] [CrossRef] [Green Version]
- Day, L.Z.; Stegman, C.; Schultz, E.P.; Lanchy, J.-M.; Yu, Q.; Ryckman, B.J. Polymorphisms in human cytomegalovirus glycoprotein O (gO) exert epistatic influences on cell-free and cell-to-cell spread and antibody neutralization on gH epitopes. J. Virol. 2020, 94, e02051-19. [Google Scholar] [CrossRef]
- Klein, M.; Schoppel, K.; Amvrossiadis, N.; Mach, M. Strain-specific neutralization of human cytomegalovirus isolates by human sera. J. Virol. 1999, 73, 878–886. [Google Scholar] [CrossRef] [Green Version]
- Ishida, J.H.; Patel, A.; Mehta, A.K.; Gatault, P.; McBride, J.M.; Burgess, T.; Derby, M.A.; Snydman, D.R.; Emu, B.; Feierbach, B.; et al. Phase 2 Randomized, Double-Blind, Placebo-Controlled Trial of RG7667, a Combination Monoclonal Antibody, for Prevention of Cytomegalovirus Infection in High-Risk Kidney Transplant Recipients. Antimicrob. Agents Chemother. 2017, 61, e01794-16. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Maertens, J.; Logan, A.C.; Jang, J.; Long, G.; Tang, J.L.; Hwang, W.Y.K.; Koh, L.P.; Chemaly, R.; Gerbitz, A.; Winkler, J.; et al. Phase 2 Study of Anti-Human Cytomegalovirus Monoclonal Antibodies for Prophylaxis in Hematopoietic Cell Transplantation. Antimicrob. Agents Chemother. 2020, 64, e02467-19. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Martins, J.P.; Andoniou, C.E.; Fleming, P.; Kuns, R.D.; Schuster, I.S.; Voigt, V.; Daly, S.; Varelias, A.; Tey, S.-K.; Degli-Esposti, M.A.; et al. Strain-specific antibody therapy prevents cytomegalovirus reactivation after transplantation. Science 2019, 363, 288–293. [Google Scholar] [CrossRef] [PubMed]
- Gilbert, G.L.; Hayes, K.; Hudson, I.L.; James, J. Prevention of transfusion-acquired cytomegalovirus infection in infants by blood filtration to remove leucocytes. Neonatal Cytomegalovirus Infection Study Group. Lancet 1989, 1, 1228–1231. [Google Scholar] [CrossRef] [PubMed]
- Gerna, G.; Zipeto, D.; Percivalle, E.; Parea, M.; Revello, M.G.; Maccario, R.; Peri, G.; Milanesi, G. Human cytomegalovirus infection of the major leukocyte subpopulations and evidence for initial viral replication in polymorphonuclear leukocytes from viremic patients. J. Infect. Dis. 1992, 166, 1236–1244. [Google Scholar] [CrossRef] [PubMed]
- Gomez-Roman, V.R.; Florese, R.H.; Patterson, L.J.; Peng, B.; Venzon, D.; Aldrich, K.; Robert-Guroff, M. A simplified method for rapid fluorometric assessment of antibody-dependent cell-mediated cytotoxicity. J. Immunol. Methods 2006, 308, 53–67. [Google Scholar] [CrossRef] [PubMed]
- Ackerman, M.E.; Moldt, B.; Wyatt, R.T.; Dugast, A.-S.; McAndrew, E.; Tsoukas, S.; Jost, S.; Berger, C.; Sciarangella, G.; Liu, Q.; et al. A robust, high-throughput assay to determine the phagocyte activity of clinical antibody samples. J. Immunol. Methods 2011, 366, 8–19. [Google Scholar] [CrossRef] [Green Version]
- Chung, A.W.; Ghebremichael, M.; Robinson, H.; Brown, E.; Choi, I.; Lane, S.; Dugast, A.-S.; Schoen, M.K.; Rolland, M.; Suscovich, T.J.; et al. Polyfunctional Fc-effector profiles mediated by IgG subclass selection distinguish RV144 and VAX003 vaccines. Sci. Transl. Med. 2014, 6, 228ra38. [Google Scholar] [CrossRef]
- Chung, A.W.; Kumar, M.P.; Arnold, K.B.; Yu, W.H.; Schoen, M.K.; Dunphy, L.J.; Suscovich, T.J.; Frahm, N.; Linde, C.; Mahan, A.E.; et al. Dissecting polyclonal vaccine-induced humoral immunity against HIV using systems serology. Cell 2015, 163, 988–998. [Google Scholar] [CrossRef] [Green Version]
- Gerna, G.; Percivalle, E.; Perez, L.; Lanzavecchia, A.; Lilleri, D. Monoclonal antibodies to different components of the human cytomegalovirus (HCMV) pentamer gH/gL/pUL128L and trimer gH/gL/gO as well as antibodies elicited during primary HCMV infection prevent epithelial cell syncytium formation. J. Virol. 2016, 90, 6216–6223. [Google Scholar] [CrossRef] [Green Version]
- Schultz, E.P.; Yu, Q.; Stegmann, C.; Day, L.Z.; Lanchy, J.M.; Ryckman, B.J. Mutagenesis of Human Cytomegalovirus Glycoprotein L Disproportionately Disrupts gH/gL/gO over gH/gL/pUL128-131. J. Virol. 2021, 95, e0061221. [Google Scholar] [CrossRef] [PubMed]





| NAb Titers | VR#1/HELF/14 | VR#1/HELF/8-ARPE/3 | VR#1/HELF/11-HUVEC/20 | ||||||
|---|---|---|---|---|---|---|---|---|---|
| HELF | ARPE | HUVEC | HELF | ARPE | HUVEC | HELF | ARPE | HUVEC | |
| Homologous titer | |||||||||
| p-232 (VR#1) | |||||||||
| Serum #1 | <10 | NA | NA | 10 | 1280 | 80 | <10 | 2560 | 640 |
| #2 | <10 | NA | NA | 80 | 1280 | 160 | 20 | 2560 | 1280 |
| #3 | 10 | NA | NA | 160 | 1280 | 640 | 40 | 2560 | 5120 |
| #4 | 320 | NA | NA | 320 | 1280 | 640 | 160 | 10,240 | 10,240 |
| #5 | 2560 | NA | NA | 2560 | 1280 | 1280 | 2560 | 20,480 | 20,480 |
| Heterologous titers | |||||||||
| p-236 (VR#2) | |||||||||
| Serum #1 | <10 | NA | NA | 10 | 160 | 40 | <10 | 640 | 160 |
| #2 | <10 | NA | NA | 40 | 1280 | 80 | <10 | 640 | 640 |
| #3 | 20 | NA | NA | 160 | 2560 | 1280 | 160 | 1280 | 2560 |
| #4 | 80 | NA | NA | 320 | 2560 | 2560 | 160 | 5120 | 5120 |
| #5 | 160 | NA | NA | 1280 | 1280 | 640 | 320 | 5120 | 1280 |
| p-237 (VR#3) | |||||||||
| Serum #1 | <10 | NA | NA | 10 | 160 | 20 | 10 | 640 | 160 |
| #2 | <10 | NA | NA | 20 | 640 | 80 | 40 | 640 | 320 |
| #3 | 10 | NA | NA | 40 | 1280 | 640 | 80 | 1280 | 640 |
| #4 | 20 | NA | NA | 160 | 1280 | 2560 | 160 | 1280 | 160 |
| #5 | 80 | NA | NA | 160 | 640 | 640 | 320 | 1280 | 160 |
| NAb Titers | VR#2/HELF/12 | VR#2/HELF/9-ARPE/4 | VR#2/HELF/4-HUVEC/14 | ||||||
|---|---|---|---|---|---|---|---|---|---|
| HELF | ARPE | HUVEC | HELF | ARPE | HUVEC | HELF | ARPE | HUVEC | |
| Homologous titer | |||||||||
| p-236 (VR#2) | |||||||||
| Serum #1 | <10 | NA | NA | <10 | 1280 | 320 | 80 | 320 | 640 |
| #2 | <10 | NA | NA | 80 | 2560 | 640 | 80 | 640 | 640 |
| #3 | 160 | NA | NA | 1280 | 10,240 | 5120 | 320 | 10,240 | 2560 |
| #4 | 640 | NA | NA | 5120 | 10,240 | 5120 | 320 | 20,480 | 5120 |
| #5 | 2560 | NA | NA | 20,480 | 10,240 | 10,240 | 640 | 10,240 | 10,240 |
| Heterologous titers | |||||||||
| p-232 (VR#1) | |||||||||
| Serum #1 | <10 | NA | NA | 40 | 1280 | 160 | 40 | 640 | 160 |
| #2 | <10 | NA | NA | 160 | 1280 | 640 | 40 | 640 | 640 |
| #3 | 10 | NA | NA | 1280 | 1280 | 640 | 80 | 640 | 640 |
| #4 | 40 | NA | NA | 2560 | 2560 | 2560 | 160 | 2560 | 2560 |
| #5 | 160 | NA | NA | 5120 | 5120 | 2560 | 320 | 2560 | 2560 |
| p-237 (VR#3) | |||||||||
| Serum #1 | <10 | NA | NA | <10 | 40 | 40 | 40 | 160 | 160 |
| #2 | <10 | NA | NA | 160 | 640 | 320 | 160 | 160 | 320 |
| #3 | 10 | NA | NA | 1280 | 2560 | 1280 | 320 | 640 | 640 |
| #4 | 160 | NA | NA | 1280 | 2560 | 2560 | 160 | 640 | 640 |
| #5 | 160 | NA | NA | 1280 | 2560 | 1280 | 160 | 640 | 640 |
| NAb Titers | VR#3/HELF/12 | VR#3/HELF/12-ARPE/4 | VR#3/HELF/10-HUVEC/8 | ||||||
|---|---|---|---|---|---|---|---|---|---|
| HELF | ARPE | HUVEC | HELF | ARPE | HUVEC | HELF | ARPE | HUVEC | |
| Homologous titer | |||||||||
| p-237 (VR#3) | |||||||||
| Serum #1 | <10 | NA | NA | <10 | 320 | 40 | <10 | 160 | 40 |
| #2 | 10 | NA | NA | <10 | 320 | 80 | 10 | 320 | 80 |
| #3 | 20 | NA | NA | 80 | 640 | 160 | 40 | 640 | 160 |
| #4 | 80 | NA | NA | 160 | 640 | 160 | 320 | 1280 | 160 |
| #5 | 1280 | NA | NA | 1280 | 640 | 160 | 2560 | 640 | 160 |
| Heterologous titers | |||||||||
| p-232 (VR#1) | |||||||||
| Serum #1 | <10 | NA | NA | 10 | 1280 | 160 | <10 | 1280 | 160 |
| #2 | 20 | NA | NA | 10 | 1280 | 640 | 10 | 640 | 160 |
| #3 | 10 | NA | NA | 10 | 1280 | 640 | 10 | 320 | 160 |
| #4 | 10 | NA | NA | 80 | 1280 | 320 | 40 | 640 | 160 |
| #5 | 160 | NA | NA | 1280 | 1280 | 320 | 320 | 2560 | 320 |
| p-236 (VR#2) | |||||||||
| Serum #1 | <10 | NA | NA | <10 | 1280 | 40 | <10 | 2560 | 320 |
| #2 | 20 | NA | NA | <10 | 1280 | 160 | <10 | 5120 | 320 |
| #3 | 40 | NA | NA | 40 | 1280 | 1280 | 80 | 2560 | 640 |
| #4 | 40 | NA | NA | 80 | 640 | 1280 | 80 | 5120 | 640 |
| #5 | 160 | NA | NA | 160 | 640 | 320 | 160 | 640 | 640 |
| NAb Titers | VR#1814/HELF/27 | VR#1814/HUVEC/132-ARPE/8 | VR#1814/HUVEC/132 | ||||||
|---|---|---|---|---|---|---|---|---|---|
| HELF | ARPE | HUVEC | HELF | ARPE | HUVEC | HELF | ARPE | HUVEC | |
| Heterologous titers | |||||||||
| p-232 (VR#1) | |||||||||
| Serum #1 | <10 | NA | NA | <10 | 1280 | 320 | <10 | 2560 | 320 |
| #2 | <10 | NA | NA | <10 | 1280 | 320 | <10 | 2560 | 640 |
| #3 | <10 | NA | NA | <10 | 640 | 160 | 10 | 1280 | 320 |
| #4 | 40 | NA | NA | 20 | 640 | 160 | 20 | 1280 | 320 |
| #5 | 640 | NA | NA | 160 | 1280 | 320 | 320 | 2560 | 320 |
| p-236 (VR#2) | |||||||||
| Serum #1 | 10 | NA | NA | <10 | 2560 | 320 | <10 | 5120 | 640 |
| #2 | 10 | NA | NA | <10 | 1280 | 640 | <10 | 2560 | 1280 |
| #3 | 40 | NA | NA | 20 | 1280 | 640 | 40 | 2560 | 1280 |
| #4 | 40 | NA | NA | 20 | 1280 | 640 | 80 | 5120 | 1280 |
| #5 | 80 | NA | NA | 80 | 1280 | 640 | 80 | 5120 | 1280 |
| p-237 (VR#3) | |||||||||
| Serum #1 | <10 | NA | NA | <10 | 320 | 40 | <10 | 1280 | 160 |
| #2 | 10 | NA | NA | <10 | 320 | 160 | <10 | 1280 | 160 |
| #3 | 20 | NA | NA | <10 | 640 | 320 | 10 | 2560 | 320 |
| #4 | 80 | NA | NA | <10 | 640 | 160 | 20 | 1280 | 640 |
| #5 | 320 | NA | NA | 40 | 640 | 160 | 80 | 1280 | 160 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Fornara, C.; Schultz, E.; Lilleri, D.; Baldanti, F.; Ryckman, B.; Gerna, G. Fibroblast, Epithelial and Endothelial Cell-Derived Human Cytomegalovirus Strains Display Distinct Neutralizing Antibody Responses and Varying Levels of gH/gL Complexes. Int. J. Mol. Sci. 2023, 24, 4417. https://doi.org/10.3390/ijms24054417
Fornara C, Schultz E, Lilleri D, Baldanti F, Ryckman B, Gerna G. Fibroblast, Epithelial and Endothelial Cell-Derived Human Cytomegalovirus Strains Display Distinct Neutralizing Antibody Responses and Varying Levels of gH/gL Complexes. International Journal of Molecular Sciences. 2023; 24(5):4417. https://doi.org/10.3390/ijms24054417
Chicago/Turabian StyleFornara, Chiara, Eric Schultz, Daniele Lilleri, Fausto Baldanti, Brent Ryckman, and Giuseppe Gerna. 2023. "Fibroblast, Epithelial and Endothelial Cell-Derived Human Cytomegalovirus Strains Display Distinct Neutralizing Antibody Responses and Varying Levels of gH/gL Complexes" International Journal of Molecular Sciences 24, no. 5: 4417. https://doi.org/10.3390/ijms24054417
APA StyleFornara, C., Schultz, E., Lilleri, D., Baldanti, F., Ryckman, B., & Gerna, G. (2023). Fibroblast, Epithelial and Endothelial Cell-Derived Human Cytomegalovirus Strains Display Distinct Neutralizing Antibody Responses and Varying Levels of gH/gL Complexes. International Journal of Molecular Sciences, 24(5), 4417. https://doi.org/10.3390/ijms24054417








