Oxidant/Antioxidant Status of Breast Cancer Patients in Pre- and Post-Operative Periods
Abstract
1. Introduction
2. Materials and Methods
2.1. Analysis of MDA, Total Glutathione (GSH + GSSG) and GST
2.2. Reagents
2.3. Statistical Analysis
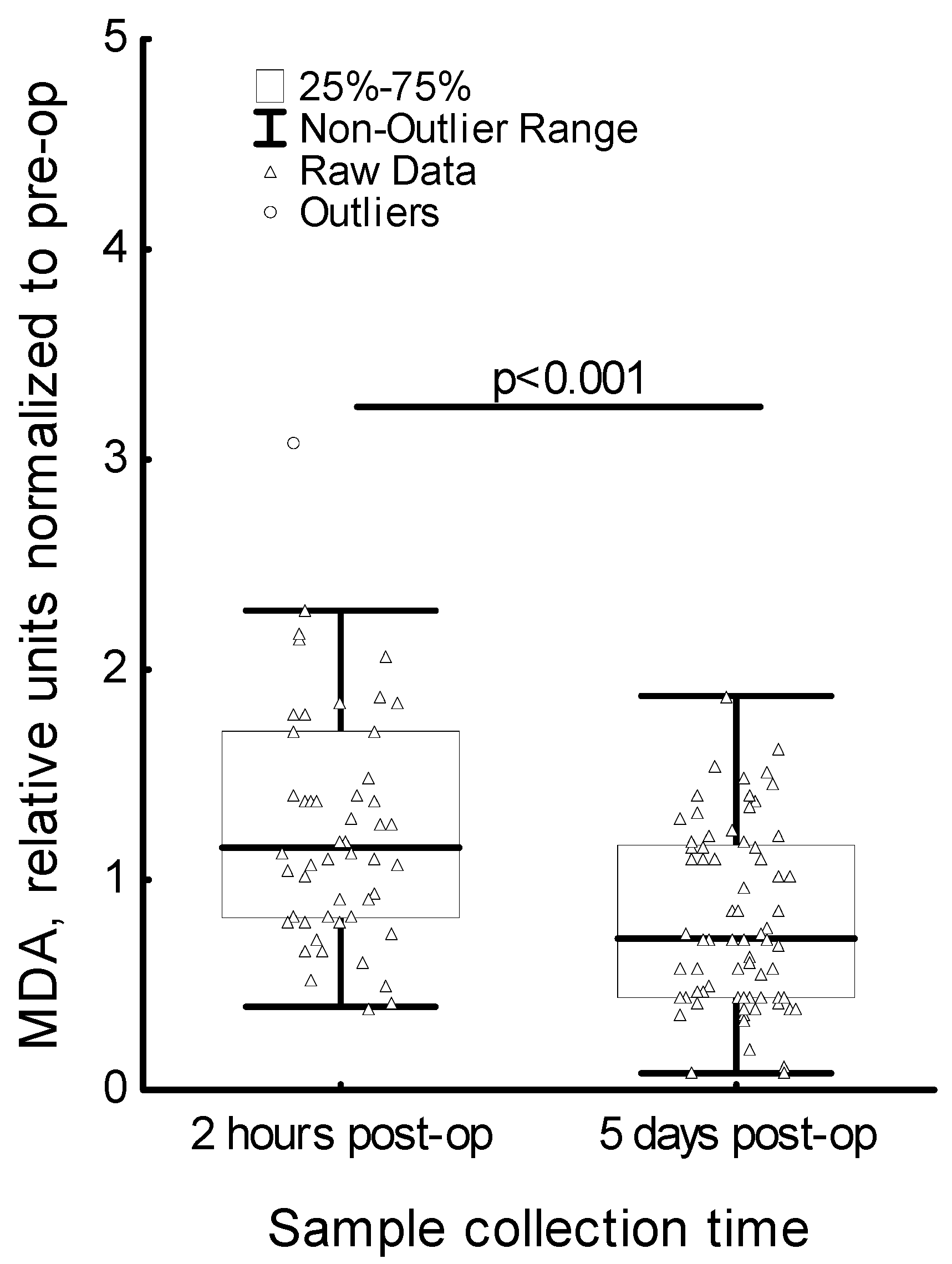
3. Results
4. Discussion
5. Conclusions
Author Contributions
Conflicts of Interest
References
- Available online: http://globocan.iarc.fr/old/FactSheets/cancers/breast-new.asp#MORTALITY (accessed on 25 November 2016).
- McPherson, K.; Steel, C.M.; Dixon, J.M. ABC of breast diseases. Breast cancer-epidemiology, risk factors, and genetics. BMJ 2000, 321, 624–628. [Google Scholar] [CrossRef] [PubMed]
- Franceschini, G.; Martin Sanchez, A.; Di Leone, A.; Magno, S.; Moschella, F.; Accetta, C.; Masetti, R. New trends in breast cancer surgery: A therapeutic approach increasingly efficacy and respectful of the patient. G. Chir. 2015, 36, 145–152. [Google Scholar] [CrossRef] [PubMed]
- Cortazar, P.; Kluetz, P.G. Neoadjuvant breast cancer therapy and drug development. Clin. Adv. Hematol. Oncol. 2015, 13, 755–761. [Google Scholar] [PubMed]
- Anampa, J.; Makower, D.; Sparano, J.A. Progress in adjuvant chemotherapy for breast cancer: An overview. BMC Med. 2015, 13, 195. [Google Scholar] [CrossRef]
- Liou, G.Y.; Storz, P. Reactive oxygen species in cancer. Free Radic. Res. 2010, 44, 479–496. [Google Scholar] [CrossRef]
- Arsalani-Zadeh, R.; Ullah, S.; Khan, S.; MacFie, J. Oxidative stress in laparoscopic versus open abdominal surgery: A systematic review. J. Surg. Res. 2011, 169, 59–68. [Google Scholar] [CrossRef]
- Pande, D.; Negi, R.; Karki, K.; Khanna, S.; Khanna, R.S.; Khanna, H.D. Oxidative damage markers as possible discriminatory biomarkers in breast carcinoma. Transl. Res. 2012, 160, 411–418. [Google Scholar] [CrossRef]
- Lu, S.C. Regulation of glutathione synthesis. Curr. Top. Cell Regul. 2000, 36, 95–116. [Google Scholar]
- Polat, M.F.; Taysi, S.; Gul, M.; Cikman, O.; Yilmaz, I.; Bakan, E.; Erdogan, F. Oxidant/antioxidant status in blood of patients with malignant breast tumour and benign breast disease. Cell. Biochem. Funct. 2002, 20, 327–331. [Google Scholar] [CrossRef]
- Estrela, J.M.; Ortega, A.; Obrador, E. Glutathione in cancer biology and therapy. Crit. Rev. Clin. Lab. Sci. 2006, 43, 143–181. [Google Scholar] [CrossRef]
- Kim, D.; Koo, J.S.; Lee, S. Overexpression of reactive oxygen species scavenger enzymes is associated with a good prognosis in triple-negative breast cancer. Oncology 2015, 88, 9–17. [Google Scholar] [CrossRef] [PubMed]
- Upadhya, S.; Upadhya, S.; Mohan, S.K.; Vanajakshamma, K.; Kunder, M.; Mathias, S. Oxidant-antioxidant status in colorectal cancer patients–before and after treatment. Indian J. Clin. Biochem. 2004, 9, 80–83. [Google Scholar] [CrossRef] [PubMed]
- Sharma, A.; Rajappa, M.; Satyam, A.; Sharma, M. Oxidant/anti-oxidant dynamics in patients with advanced cervical cancer: Correlation with treatment response. Mol. Cell. Biochem. 2010, 341, 65–72. [Google Scholar] [CrossRef] [PubMed]
- Sener, D.E.; Gönenç, A.; Akinci, M.; Torun, M. Lipid peroxidation and total antioxidant status in patients with breast cancer. Cell. Biochem. Funct. 2007, 25, 377–382. [Google Scholar] [CrossRef] [PubMed]
- Prabasheela, B.; Baskaran, S.; Singh, A.K. Antioxidant and lipid peroxidation status in pre- and post-operative breast carcinoma. Int. J. Pharma Bio Sci. 2011, 2, 450–454. [Google Scholar]
- Prabasheela, B.; Baskaran, S. Alteration of glutathione dependent enzymes in pre- and post- operative breast carcinoma. Med. Res. Chron. 2014, 1, 73–77. [Google Scholar]
- El-Hefny, M.A.; Karimova, S.T.; Afandiev, A.F. Lipid peroxidation and antioxidant status in breast cancer patients before and after therapy. Med. J. Cairo Univ. 2009, 77, 37–42. [Google Scholar]
- Buege, J.A.; Aust, S.D. Microsomal lipid peroxidation. Methods Enzymol. 1978, 52, 302–310. [Google Scholar]
- Habig, W.H.; Pabst, M.J.; Jakoby, W.B. Glutathione S-transferases. The first enzymatic step in mercapturic acid formation. J. Biol. Chem. 1974, 249, 7130–7139. [Google Scholar]
- Baker, M.A.; Cerniglia, G.J.; Zaman, A. Microtiter plate assay for the measurement of glutathione and glutathione disulfide in large numbers of biological samples. Anal. Biochem. 1990, 190, 360–365. [Google Scholar] [CrossRef]
- Rosenfeldt, F.; Wilson, M.; Lee, G.; Kure, C.; Ou, R.; Braun, L.; de Haan, J. Oxidative stress in surgery in an ageing population: Pathophysiology and therapy. Exp. Gerontol. 2013, 48, 45–54. [Google Scholar] [CrossRef] [PubMed]
- Salzman, R.; Pácal, L.; Kaňková, K.; Tomandl, J.; Horáková, Z.; Tóthová, E.; Kostřica, R. High perioperative level of oxidative stress as a prognostic tool for identifying patients with a high risk of recurrence of head and neck squamous cell carcinoma. Int. J. Clin. Oncol. 2010, 15, 565–570. [Google Scholar] [CrossRef] [PubMed]
- Gorozhanskaya, E.G.; Sviridova, S.P.; Baykova, V.N.; Zubrikhina, G.N.; Dobrovolskaya, M.M.; Sitov, A.V. Oxidative stress in platelets at an oncopathology. Biomed. Khim. 2015, 61, 519–525. [Google Scholar] [CrossRef] [PubMed]
- Scibior, D.; Skrzycki, M.; Podsiad, M.; Czeczot, H. Glutathione level and glutathione-dependent enzyme activities in blood serum of patients with gastrointestinal tract tumors. Clin. Biochem. 2008, 41, 852–858. [Google Scholar] [CrossRef]
- Beevi, S.S.; Rasheed, M.H.; Geetha, A. Evidence of oxidative and nitrosative stress in patients with cervical squamous cell carcinoma. Clin. Chim. Acta 2007, 75, 119–123. [Google Scholar] [CrossRef]
- Szychta, P.; Zadrozny, M.; Lewinski, A.; Karbownik-Lewinska, M. Increased oxidative damage to membrane lipids following surgery for breast cancer. Neuro Endocrinol. Lett. 2014, 35, 602–607. [Google Scholar]
- Fiaschi, A.I.; Cozzolino, A.; Ruggiero, G.; Giorgi, G. Glutathione, ascorbic acid and antioxidant enzymes in the tumor tissue and blood of patients with oral squamous cell carcinoma. Eur. Rev. Med. Pharmacol. Sci. 2005, 9, 361–367. [Google Scholar]
- Nomani, H.; Ghobadloo, S.M.; Yaghmaei, B.; Rezvanie, N.A.; Yaghmaei, K. Glutathione S-transferases activity in patients with colorectal cancer. Clin. Biochem. 2005, 38, 621–624. [Google Scholar] [CrossRef]
- Abou Ghalia, A.H.; Fouad, I.M. Glutathione and its metabolizing enzymes in patients with different benign and malignant diseases. Clin. Biochem. 2000, 33, 657–662. [Google Scholar] [CrossRef]
- Kadam, C.Y.; Abhang, S.A. Evaluation of serum levels of reduced glutathione, glutathione-s-transferase and nitric oxide in breast cancer patients undergoing adjuvant chemotherapy. Int. J. Cur. Rev. 2013, 5, 51–57. [Google Scholar]
- Franco, R.L.; Schenka, N.G.; Schenka, A.A.; Rezende, L.F.; Gurgel, M.S. Glutathione S-transferase Pi expression in invasive breast cancer and its relation with the clinical outcome. J. BU ON 2012, 17, 259–264. [Google Scholar]

| Parameters | Number of Cases (n) |
|---|---|
| Age | |
| <50 | 34 |
| >50 | 18 |
| Histologic subtype | |
| Ductal carcinoma | 46 |
| Invasive lobular carcinoma | 3 |
| Other | 3 |
| TNM stages | |
| 0 | 3 |
| I | 19 |
| II | 22 |
| III | 8 |
| Lymph node metastasis | |
| Yes | 18 |
| No | 34 |
| Tumor grade | |
| Gx | 6 |
| G1 | 8 |
| G2 | 23 |
| G3 | 15 |
| Type of surgery | |
| Breast conserving surgery | 52 |
| Body mass index under 50 years of age | |
| <18.5 18.5–24.9 25–29.9 30–34.9 35–40 Body mass index over 50 years of age | – 15 12 5 2 |
| <18.5 18.5–24.9 25–29.9 30–34.9 35–40 | – 4 9 4 1 |
| Parameters | Before Surgery | Two Hours after Surgery | Five Days after Surgery | Control |
|---|---|---|---|---|
| MDA, nmol/mL | 11.29 ± 7.69 * | 13.93 ± 8.35 * | 9.83 ± 3.15 ● | 6.73 ± 2.66 ● |
| GST, µmol/mL/min | 0.36 ± 0.16 | 0.37 ± 0.16 | 0.37 ± 0.16 ● | 0.48 ± 0.13 ● |
| GSH + GSSG, µmol/mL | 0.47 ± 0.19 | 0.46 ± 0.3 | 0.48 ± 0.21 ● | 0.79 ± 0.28 ● |
| Under 50 Years of Age | ||||||
| Parameters | n | Before Surgery | Two Hours after Surgery | Five Days after Surgery | n | Control |
| MDA, nmol/mL | 34 | 10.04 ± 5.2 | 11.68 ± 8.39 * | 8.94 ± 4.24 * | 20 | 6.06 ± 1.72 |
| GST, µmol/mL/min | 34 | 0.33 ± 0.16 | 0.34 ± 0.17 | 0.33 ± 0.16 | 20 | 0.41 ± 0.19 |
| GSH + GSSG, µmol/mL | 34 | 0.51 ± 0.21 | 0.46 ± 0.14 | 0.49 ± 0.24 ● | 20 | 0.98 ± 0.13 ● |
| Over 50 Years of Age | ||||||
| Parameters | n | Before Surgery | Two Hours after Surgery | Five Days after Surgery | n | Control |
| MDA, nmol/mL | 18 | 13.67 ± 6.76 * | 18.18 ± 10.76 * | 11.46 ± 6.30 ● | 22 | 7.40 ± 1.83 ● |
| GST, µmol/mL/min | 18 | 0.43 ± 0.13 | 0.44 ± 0.14 | 0.39 ± 0.17 ● | 22 | 0.55 ± 0.16 ● |
| GSH + GSSG, µmol/mL | 18 | 0.41 ± 0.13 | 0.41 ± 0.11 | 0.47 ± 0.15 ● | 22 | 0.60 ± 0.17 ● |
| Stage I | |||||
| Parameters | n | Before Surgery | Two Hours after Surgery | Five Days after Surgery | Control |
| MDA, nmol/mL | 19 | 11.99 ± 9.08 * | 16.04 ± 10.22 * | 10.52 ± 6.11 ● | 6.73 ± 2.66 ● |
| GST, µmol/mL/min | 19 | 0.38 ± 0.15 | 0.39 ± 0.14 | 0.39 ± 0.13 | 0.48 ± 0.23 |
| GSH + GSSG, µmol/mL | 19 | 0.48 ± 0.20 | 0.48 ± 0.09 | 0.51 ± 0.28 ● | 0.79 ± 0.28 ● |
| Stage II | |||||
| MDA, nmol/mL | 22 | 8.91 ± 3.47 | 10.30 ± 4.41 | 8.23 ± 3.27 | 6.73 ± 2.66 |
| GST, µmol/mL/min | 22 | 0.36 ± 0.15 | 0.37 ± 0.15 | 0.37 ± 0.14 | 0.48 ± 0.23 |
| GSH + GSSG, µmol/mL | 22 | 0.48 ± 0.21 | 0.43 ± 0.17 | 0.45 ± 0.17 ● | 0.79 ± 0.28 ● |
| Stage III | |||||
| MDA, nmol/mL | 8 | 17.11 ± 11.04 | 21.66 ± 13.82 | 14.33 ± 5.38 ● | 6.73 ± 2.66 ● |
| GST, µmol/mL/min | 8 | 0.41 ± 0.16 | 0.43 ± 0.17 | 0.43 ± 0.19 | 0.48 ± 0.23 |
| GSH + GSSG, µmol/mL | 8 | 0.48 ± 0.16 | 0.52 ± 0.17 | 0.56 ± 0.10 ● | 0.79 ± 0.28 ● |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Didžiapetrienė, J.; Kazbarienė, B.; Tikuišis, R.; Dulskas, A.; Dabkevičienė, D.; Lukosevičienė, V.; Kontrimavičiūtė, E.; Sužiedėlis, K.; Ostapenko, V. Oxidant/Antioxidant Status of Breast Cancer Patients in Pre- and Post-Operative Periods. Medicina 2020, 56, 70. https://doi.org/10.3390/medicina56020070
Didžiapetrienė J, Kazbarienė B, Tikuišis R, Dulskas A, Dabkevičienė D, Lukosevičienė V, Kontrimavičiūtė E, Sužiedėlis K, Ostapenko V. Oxidant/Antioxidant Status of Breast Cancer Patients in Pre- and Post-Operative Periods. Medicina. 2020; 56(2):70. https://doi.org/10.3390/medicina56020070
Chicago/Turabian StyleDidžiapetrienė, Janina, Birutė Kazbarienė, Renatas Tikuišis, Audrius Dulskas, Daiva Dabkevičienė, Vaida Lukosevičienė, Eglė Kontrimavičiūtė, Kęstutis Sužiedėlis, and Valerijus Ostapenko. 2020. "Oxidant/Antioxidant Status of Breast Cancer Patients in Pre- and Post-Operative Periods" Medicina 56, no. 2: 70. https://doi.org/10.3390/medicina56020070
APA StyleDidžiapetrienė, J., Kazbarienė, B., Tikuišis, R., Dulskas, A., Dabkevičienė, D., Lukosevičienė, V., Kontrimavičiūtė, E., Sužiedėlis, K., & Ostapenko, V. (2020). Oxidant/Antioxidant Status of Breast Cancer Patients in Pre- and Post-Operative Periods. Medicina, 56(2), 70. https://doi.org/10.3390/medicina56020070






