The Role of “Critical” Ultrasound Reassessment in the Decision-Making of Bethesda III Thyroid Nodules
Abstract
:1. Introduction
2. Materials and Methods
2.1. Clinical Management
- -
- any ‘non aggressive’ PTC recruited in BIII diagnostic category (2018–2022);
- -
- US performed by endocrinologist/endocrine surgeon of multidisciplinary team.
- -
- two or more BIII-IV-V-VI nodules;
- -
- US reports not in agreement with ACE/AACE/AME standards;
- -
- cytology reports not in agreement with Bethesda system;
- -
- Grave’s disease and other benign diseases;
- -
- cancers other than PTC;
- -
- aggressive variants of PTC;
- -
- NIFTP and other tumors of uncertain malignant potential;
- -
- PTC ≤ 1 cm.
2.2. Thyroid Ultrasound
2.3. Thyroid Cytology
2.4. Thyroid Surgery
2.5. Variables Analyzed
2.6. Statistical Analysis
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Guth, S.; Theune, U.; Aberle, J.; Galach, A.; Bamberger, C.M. Very high prevalence of thyroid nodules detected by high frequency (13 MHz) ultrasound examination. Eur. J. Clin. Investig. 2009, 39, 699–706. [Google Scholar] [CrossRef]
- Papini, E.; Guglielmi, R.; Bianchini, A.; Crescenzi, A.; Taccogna, S.; Nardi, F.; Panunzi, C.; Rinaldi, R.; Toscano, V.; Pacella, C.M. Risk of malignancy in nonpalpable thyroid nodules: Predictive value of ultrasound and color-Doppler features. J. Clin. Endocrinol. Metab. 2002, 87, 1941–1946. [Google Scholar] [CrossRef]
- Parsa, A.A.; Gharib, H. Epidemiology of Thyroid Nodules. In Thyroid Nodules. Contemporary Endocrinology; Gharib, H., Ed.; Humana Press: Tortowa, NJ, USA, 2018; pp. 1–11. [Google Scholar]
- Hegedüs, L. Clinical practice. The thyroid nodule. N. Engl. J. Med. 2004, 351, 1764–1771. [Google Scholar] [CrossRef]
- Wong, R.; Farrell, S.G.; Grossmann, M. Thyroid nodules: Diagnosis and management. Med. J. Aust. 2018, 209, 92–98. [Google Scholar] [CrossRef]
- Cibas, E.S.; Ali, S. The Bethesda System for Reporting Thyroid Cytopathology. Am. J. Clin. Pathol. 2009, 132, 658–665. [Google Scholar] [CrossRef]
- Cibas, E.S.; Ali, S.Z. The 2017 Bethesda system for reporting thyroid cytopathology. Thyroid 2017, 27, 1341–1346. [Google Scholar] [CrossRef]
- Kim, J.; Shin, J.H.; Oh, Y.L.; Hahn, S.Y.; Park, K.W. Approach to Bethesda system category III thyroid nodules according to US-risk stratification. Endocr. J. 2022, 69, 67–74. [Google Scholar] [CrossRef]
- Song, J.Y.; Chu, Y.C.; Kim In, L.; Park Jee, S.; Joon, Y.H.; Kim, M. Reclassifying Formerly Indeterminate Thyroid FNAs Using the Bethesda System Reduces the Number of Inconclusive Cases. Acta Cytol. 2012, 56, 122–129. [Google Scholar] [CrossRef]
- Ivana Kholová, I.; Ludvíková, M. Thyroid Atypia of Undetermined Significance or Follicular Lesion of Undetermined Significance: An Indispensable Bethesda 2010 Diagnostic Category or Waste Garbage? Acta Cytol. 2014, 58, 319–329. [Google Scholar] [CrossRef]
- Haugen, B.R.; Alexander, E.K.; Bible, K.C.; Doherty, G.M.; Mandel, S.J.; Nikiforov, Y.E.; Pacini, F.; Randolph, G.W.; Sawka, A.M.; Schlumberger, M.; et al. 2015 American Thyroid Association Management guidelines for adult patients with thyroid nodules and differentiated thyroid cancer. Thyroid 2016, 26, 1–33. [Google Scholar] [CrossRef]
- Gao, L.Y.; Wang, Y.; Jiang, Y.X.; Yang, X.; Liu, R.Y.; Xi, X.H.; Zhu, S.L.; Zhao, R.N.; Lai, X.J.; Zhang, X.Y.; et al. Ultrasound is helpful to differentiate Bethesda class III thyroid nodules. A PRISMA-compliant systematic review and meta-analysis. Medicine 2017, 96, e6564. [Google Scholar] [CrossRef]
- Rosario, P.W. Thyroid nodules with atypia or follicular lesions of undetermined significance (Bethesda Category III): Importance of ultrasonography and cytological subcategory. Thyroid 2014, 24, 1115–1120. [Google Scholar] [CrossRef]
- Kovatcheva, R.D.; Shinkov, A.D.; Dimitrova, I.D.; Ivanova, R.B.; Vidinov, K.N.; Ivanova, R.S. Evaluation of the Diagnostic Performance of EU-TIRADS in Discriminating Benign from Malignant Thyroid Nodules: A Prospective Study in One Referral Center. Eur. Thyroid J. 2021, 9, 304–312. [Google Scholar] [CrossRef]
- Cap, J.; Ryska, A.; Rehorkova, P.; Hovorkova, E.; Kerekes, Z.; Pohnetalova, D. Sensitivity and specificity of the fine needle aspiration biopsy of the thyroid: Clinical point of view. Clin. Endocrinol. 1999, 51, 509–515. [Google Scholar] [CrossRef]
- Melfa, G.; Porrello, C.; Cocorullo, G.; Raspanti, C.; Rotolo, G.; Attard, A.; Gullo, R.; Bonventre, S.; Gulotta, G.; Scerrino, G. Surgeon volume and hospital volume in endocrine neck surgery: How many procedures are needed for reaching a safety level and acceptable costs? A systematic narrative review. Il G. Chir. 2018, 39, 5–11. [Google Scholar] [CrossRef]
- Lorenz, K.; Raffaelli, M.; Barczyński, M.; Lorente-Poch, L.; Sancho, J. Volume, outcomes, and quality standards in thyroid surgery: An evidence-based analysis—European Society of Endocrine Surgeons (ESES) positional statement. Langenbeck’s Arch. Surg. 2020, 405, 401–425. [Google Scholar] [CrossRef]
- Gharib, H.; Papini, E.; Garber, J.R.; Duick, D.S.; Harrell, R.M.; Hegedüs, L.; Paschke, R.; Valcavi, R.; Vitti, P. AACE/ACE/AME Task Force on Thyroid Nodules. American Association of Clinical Endocrinologists, American College of Endocrinology, and Associazione Medici Endocrinologi Medical guidelines for clinical practice for the diagnosis and management of thyroid nodules-2016 update. Endocr. Pract. 2016, 22, 622–639. [Google Scholar] [CrossRef]
- McMurtry, V.; Canberk, S.; Deftereos, G. Molecular testing in fine-needle aspiration of thyroid nodules. Diagn. Cytopathol. 2023, 51, 36–50. [Google Scholar] [CrossRef]
- Cohen, Y.; Rosenbaum, E.; Clark, D.P.; Zeiger, M.A.; Umbricht, C.B.; Tufano, R.P.; Sidransky, D.; Westra, W.H. Mutational analysis of BRAF in fine needle aspiration biopsies of the thyroid: A potential application for the preoperative assessment of thyroid nodules. Clin. Cancer Res. 2004, 10, 2761–2765. [Google Scholar] [CrossRef]
- Haugen, B.R.; Sawka, A.M.; Alexander, E.K.; Bible, K.C.; Caturegli, P.; Doherty, G.M.; Mandel, S.J.; Morris, J.C.; Nassar, A.; Pacini, F.; et al. American Thyroid Association Guidelines on the Management of Thyroid Nodules and Differentiated Thyroid Cancer Task Force Review and Recommendation on the Proposed Renaming of Encapsulated Follicular Variant Papillary Thyroid Carcinoma Without Invasion to Noninvasive Follicular Thyroid Neoplasm with Papillary-Like Nuclear Features. Thyroid 2017, 27, 481–483. [Google Scholar]
- Yousefi, E.; Sura, G.H.; Somma, J. The gray zone of thyroid nodules: Using a nomogram to provide malignancy risk assessment and guide patient management. Cancer Med. 2021, 10, 2723–2731. [Google Scholar] [CrossRef]
- Mosca, L.; Ferraz da Silva, L.F.; Campos Carneiro, P.; Azevedo Chacon, D.; Furtado de Araujo-Neto, V.J.; Furtado de Araujo-Filho, V.J.; Cernea, C.R. Malignancy rates for Bethesda III subcategories in thyroid fine needle aspiration biopsy (FNAB). Clinics 2018, 73, e370. [Google Scholar] [CrossRef]
- Kaymaz, E.; Gun, B.D.; Tasdoven, I.; Korkturk, F. Is Subdivision of Atypia of Undetermined Significance AUS/Follicular Lesion of Undetermined Significance Cases According to Detailed Nuclear Features Vital for Assessing the Risk of Malignancy? J. Cytol. 2020, 37, 204–209. [Google Scholar] [CrossRef]
- de Koster, E.J.; de Geus-Oei, L.F.; Dekkers, O.M.; van Engen-van Grunsven, I.; Hamming, J.; Corssmit, E.P.M.; Morreau, H.; Schepers, A.; Smit, J.; Oyen, W.J.G.; et al. Diagnostic Utility of Molecular and Imaging Biomarkers in Cytological Indeterminate Thyroid Nodules. Endocr. Rev. 2018, 39, 154–191. [Google Scholar] [CrossRef]
- Steinmetz, D.; Kim, M.; Choi, J.H.; Yeager, T.; Samuel, K.; Khajoueinejad, N.; Buseck, A.; Imtiaz, S.; Fernandez-Ranvier, G.; Lee, D.; et al. How Effective is the Use of Molecular Testing in Preoperative Decision Making for Management of Indeterminate Thyroid Nodules? World J. Surg. 2022, 46, 3043–3050. [Google Scholar] [CrossRef]
- Shrestha, R.T.; Karunamurthy, A.; Amin, K.; Nikiforov, Y.E.; Caramori, M.L. Multiple Mutations Detected Preoperatively May Predict Aggressive Behavior of Papillary Thyroid Cancer and Guide Management–A Case Report. Thyroid 2015, 25, 1375–1378. [Google Scholar] [CrossRef]
- Marotta, V.; Sapio, M.R.; Guerra, A.; Vitale, M. BRAF mutation in cytology samples as a diagnostic tool for papillary thyroid carcinoma. Expert Opin. Med. Diagn. 2011, 5, 277–290. [Google Scholar] [CrossRef]
- Alzahrani, A.S.; Alsaadi, R.; Murugan, A.K.; Sadiq, B.B. TERT Promoter Mutations in Thyroid Cancer. Horm. Cancer 2016, 7, 165–177. [Google Scholar] [CrossRef]
- Marotta, V.; Bifulco, M.; Vitale, M. Significance of RAS Mutations in Thyroid Benign Nodules and Non-Medullary Thyroid Cancer. Cancers 2021, 13, 3785. [Google Scholar] [CrossRef]
- Mady, L.J.; Grimes, M.C.; Khan, N.I.; Rao, R.H.; Chiosea, S.I.; Yip, L.; Ferris, R.L.; Nikiforov, Y.E.; Carty, S.E.; Duvvuri, U. Molecular Profile of Locally Aggressive Well Differentiated Thyroid Cancers. Sci. Rep. 2020, 10, 8031. [Google Scholar] [CrossRef]
- Bose, S.; Sacks, W.; Walts, A.E. Update on Molecular Testing for Cytologically Indeterminate Thyroid Nodules. Adv. Anat. Pathol. 2019, 26, 114–123. [Google Scholar] [CrossRef]
- Frates, M.C.; Benson, C.B.; Charboneau, J.W.; Cibas, E.S.; Clark, O.H.; Coleman, B.G.; Cronan, J.J.; Doubilet, P.M.; Evans, D.B.; Goellner, J.R.; et al. Management of thyroid nodules detected at US: Society of Radiologists in Ultrasound consensus conference statement. Radiology 2005, 237, 794–800. [Google Scholar] [CrossRef]
- Nabahati, M.; Moazezi, Z.; Fartookzadeh, S.; Mehraeen, R.; Ghaemian, N.; Sharbatdaran, M. The comparison of accuracy of ultrasonographic features versus ultrasound-guided fine-needle aspiration cytology in diagnosis of malignant thyroid nodules. J. Ultrasound. 2019, 22, 315–321. [Google Scholar] [CrossRef]
- Trimboli, P.; Deandrea, M.; Mormile, A.; Ceriani, L.; Garino, F.; Limone, P.; Garino, F.; Limone, P.; Giovanella, L. American Thyroid Association ultrasound system for the initial assessment of thyroid nodules: Use in stratifying the risk of malignancy of indeterminate lesions. Head Neck 2017, 40, 722–727. [Google Scholar] [CrossRef]
- Barbosa, T.L.M.; Junior, C.O.M.; Graf, H.; Cavalvanti, T.; Trippia, M.A.; da Silveira Ugino, R.T.; de Oliveira, G.L.; Granella, V.H.; de Carvalho, G.A. ACR TI-RADS and ATA US scores are helpful for the management of thyroid nodules with indeterminate cytology. BMC Endocr. Disord. 2019, 19, 112. [Google Scholar] [CrossRef]
- Grani, G.; Lamartina, L.; Ascoli, V.; Bosco, D.; Nardi, F.; D’Ambrosio, F.; Rubini, A.; Giacomelli, L.; Biffoni, M.; Filetti, S.; et al. Ultrasonography scoring systems can rule out malignancy in cytologically indeterminate thyroid nodules. Endocrine 2017, 57, 256–261. [Google Scholar] [CrossRef]
- Ahmadi, S.; Herbst, R.; Oyekunle, T.; Jiang, X.; Strickland, K.; Roman, S.; Sosa, J.A. Using the ATA and Acr ti-rads sonographic classifications as adjunctive predictors of malignancy for indeterminate thyroid nodules. Endocr. Pract. 2019, 25, 908–917. [Google Scholar] [CrossRef]
- Scerrino, G.; Cocorullo, G.; Mazzola, S.; Melfa, G.; Orlando, G.; Laise, I.; Corigliano, A.; Lo Brutto, D.; Cipolla, C.; Graceffa, G. Improving Diagnostic Performance for Thyroid Nodules Classified as Bethesda Category III or IV: How and by Whom Ultrasonography Should be Performed. J. Surg. Res. 2021, 262, 203–211. [Google Scholar] [CrossRef]
- Suh, Y.J.; Choi, Y.J. Strategy to reduce unnecessary surgeries in thyroid nodules with cytology of Bethesda category III (AUS/FLUS): A retrospective analysis of 667 patients diagnosed by surgery. Endocrine 2020, 69, 578–586. [Google Scholar] [CrossRef]
- Stoian, D.; Borcan, F.; Petre, I.; Mozos, I.; Varcus, F.; Ivan, V.; Cioca, A.; Apostol, A.; Dehelean, C.A. Strain Elastography as a Valuable Diagnosis Tool in Intermediate Cytology (Bethesda III) Thyroid Nodules. Diagnostics 2019, 9, 119. [Google Scholar] [CrossRef]
- Borlea, A.; Stoian, D.; Cotoi, L.; Sporea, I.; Lazar, F.; Mozos, I. Thyroid Multimodal Ultrasound Evaluation—Impact on Presurgical Diagnosis of Intermediate Cytology Cases. Appl. Sci. 2020, 10, 3439. [Google Scholar] [CrossRef]
- Słowińska-Klencka, D.; Klencki, M.; Duda-Szymańska, J.; Popowicz, B. Optimization of the Management of Category III Thyroid Nodules Using Repeat FNA and TIRADS. Cancers 2022, 14, 4489. [Google Scholar] [CrossRef] [PubMed]
- Liu, X.; Wang, J.; Du, W.; Dai, L.; Fang, Q. Predictors of Malignancy in Thyroid Nodules Classified as Bethesda Category III. Front. Endocrinol. 2022, 13, 806028. [Google Scholar] [CrossRef] [PubMed]
- Xu, X.M.; Angelova, E.; Clement, C.G. Outcome of Atypia of Undetermined Significance/Follicular Lesion of Undetermined Significance in Thyroid Fine- Needle Aspirations: A Six-Year Institutional Experience. Diagn. Cytopathol. 2021, 49, 915–920. [Google Scholar] [CrossRef] [PubMed]
- Zhao, H.; Guo, H.; Zhao, L.; Cao, J.; Sun, Y.; Wang, C.; Zhang, Z. Subclassification of the Bethesda Category III (AUS/FLUS): A Study of Thyroid FNA Cytology Based on ThinPrep Slides From the National Cancer Center in China. Cancer Cytopathol. 2021, 129, 642–648. [Google Scholar] [CrossRef]
- Alshahrani, A.S.; Alamri, A.S.; Balkhoyor, A.H.; Mahzari, M.M.; Alshieban, S.S.; Majed, P.M. The Prediction of Malignancy Risk in Thyroid Nodules Classified as Bethesda System Category III (AUS/FLUS) and the Role of Ultrasound Finding for Prediction of Malignancy Risk. Cureus 2021, 13, e17924. [Google Scholar] [CrossRef]
- Cho, Y.Y.; Chung, Y.J.; Kim, H.S. Malignancy Rate of Bethesda Class III Thyroid Nodules Based on the Presence of Chronic Lymphocytic Thyroiditis in Surgical Patients. Front. Endocrinol. 2021, 12, 745395. [Google Scholar] [CrossRef]
- Puzziello, A.; Guerra, A.; Murino, A.; Izzo, G.; Carrano, M.; Angrisani, E.; Zeppa, P.; Marotta, V.; Faggiano, A.; Vitale, M. Benign thyroid nodules with RAS mutation grow faster. Clin. Endocrinol. 2016, 84, 736–740. [Google Scholar] [CrossRef]
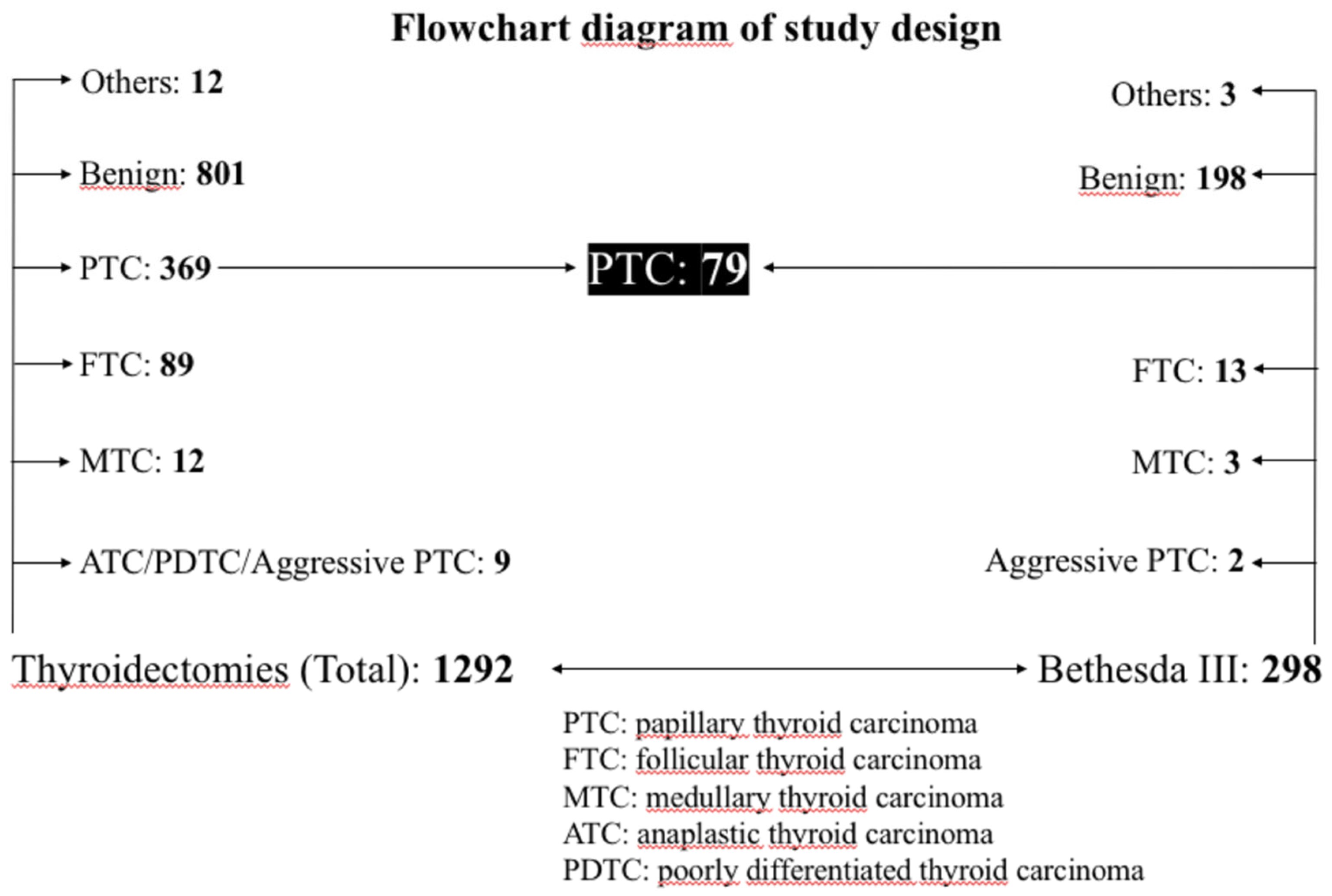


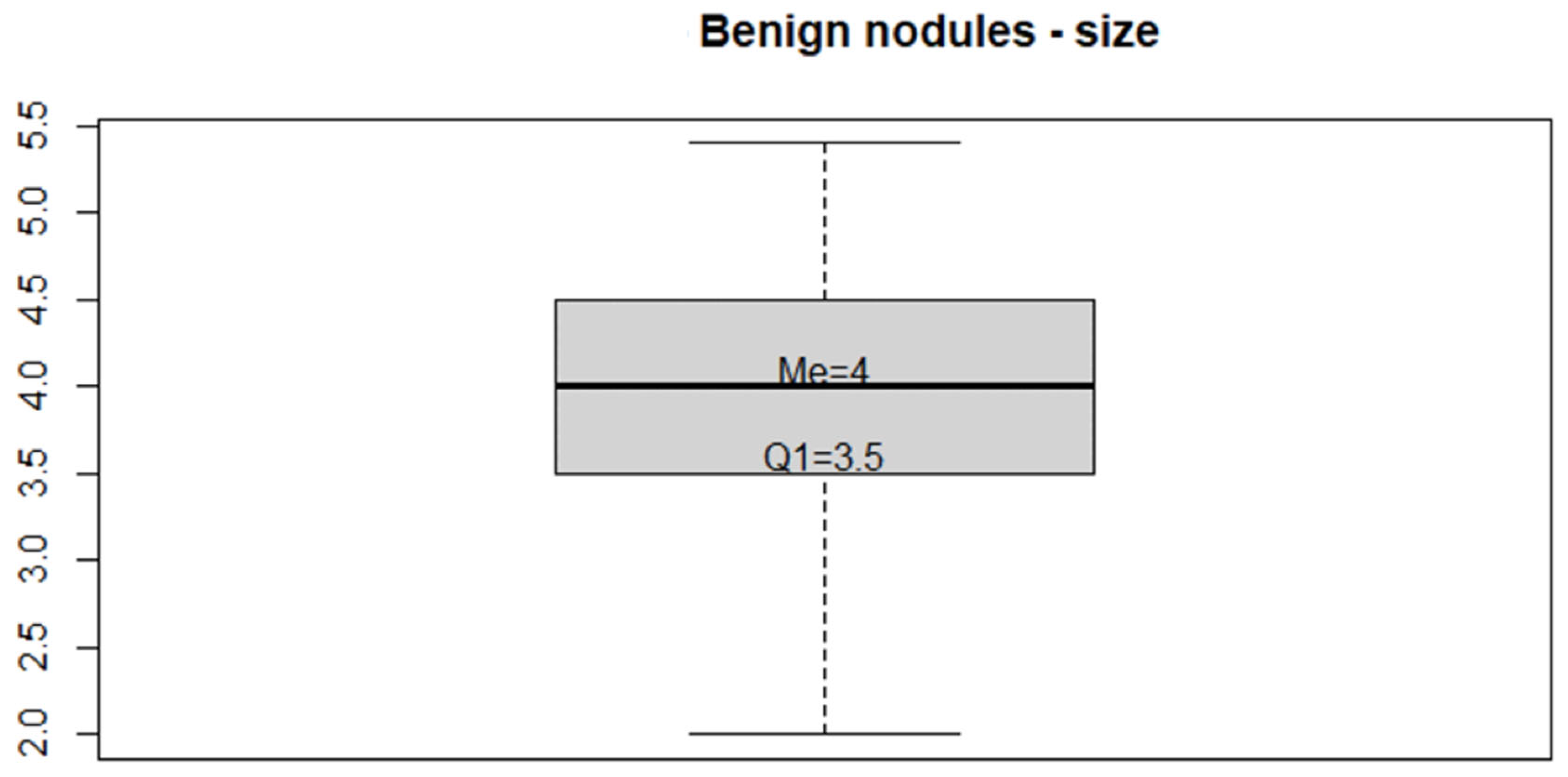
| Variable | Benign | Malignant | OR (CI95%) | p-Value | |
|---|---|---|---|---|---|
| Age | 54 | 55 | 0.4298489 | ||
| Sex | Benign | Malignant | Total | OR (CI95%) | p-value |
| m | 66 (23%) | 22 (7%) | 88 (30%) | 0.895 | 0.7743 |
| f | 153 (51%) | 57 (19%) | 210 (70%) | ||
| Total | 219 (74%) | 79 (26%) | 298 (100%) | ||
| Variable | Benign | Malignant | OR (CI95%) | p-value | |
| Size | 3.85 | 2.3 | <0.00001 | ||
| Cystic | Benign | Malignant | Total | OR (CI95%) | p-value |
| N | 182 (61%) | 78 (26.2%) | 260 (87.2%) | 0.0633 (0.0085–0.4678) | <0.001 |
| Y | 37 (12.5%) | 1 (0.3%) | 38 (12.8%) | ||
| Total | 219 (73.5%) | 79 (26.5%) | 298 (100%) | ||
| Echogenicity | Benign | Malignant | Total | OR (CI95%) | p-value |
| Isohechoic | 60 (20.1%) | 0 (0%) | 60 (20.1%) | 13.9 | 0.000001 |
| Slightly hypohechoic | 108 (36.3%) | 15 (5%) | 123 (41.3%) | ||
| Hypohechoic | 51 (17.1%) | 64 (21.5%) | 115 (38.6%) | ||
| Total | 219 (73.5) | 79 (26.5%) | 298 (100%) | ||
| Intralesional vascularization | Benign | Malignant | Total | OR (CI95%) | p-value |
| N | 108 (36.3%) | 14 (4.7%) | 122 (41%) | 4.5 (2.3–9.2) | 0.000001 |
| Y | 111 (37.2%) | 65 (21.8%) | 176 (59%) | ||
| Total | 219 (73.5%) | 79 (26.5%) | 298 (100%) | ||
| Spiculated margins | Benign | Malignant | Total | OR (CI95%) | p-value |
| N | 209 (70.1%) | 24 (8%) | 233 (78.1%) | 46.7 (20.5–116.9) | 0.000001 |
| Y | 10 (3.4%) | 55 (18.5%) | 65 (21.9%) | ||
| Total | 219 (73.5%) | 79 (26.5%) | 298 (100%) | ||
| Microcalcification | Benign | Malignant | Total | OR (CI95%) | p-value |
| N | 165 (55.4%) | 10 (3.3%) | 175 (58.7%) | 20.8 (9.8–48.6) | 0.000001 |
| Y | 54 (18.1%) | 69 (23.2%) | 123 (41.3%) | ||
| Total | 219 (73.5%) | 79 (26.5%) | 298 (100%) | ||
| Taller than wide | Benign | Malignant | Total | OR (CI95%) | p-value |
| N | 218 (73.2%) | 54 (18.1%) | 272 (91.3%) | 99.2 (15.6–4060.8) | 0.000001 |
| Y | 1 (0.3%) | 25 (8.4%) | 26 (8.7%) | ||
| Total | 219 (73.5%) | 79 (26.5%) | 298 (100%) | ||
| Extra-thyroid growth | Benign | Malignant | Total | OR (CI95%) | p-value |
| N | 219 (73.5%) | 54 (18.1) | 273 (91.6%) | 205.4 (12.3–3427.38) | 0.000001 |
| Y | 0 | 25 (8.4%) | 25 (8.4%) | ||
| Total | 219 (73.5%) | 79 (26.5%) | 298 (100%) | ||
| Increase | Benign | Malignant | Total | OR (CI95%) | p-value |
| N | 66 (22.2%) | 14 (4.7%) | 80 (26.9%) | 2.0 (1.02–4.13) | <0.05 |
| Y | 153 (51.3%) | 65 (21.8%) | 218 (73.1%) | ||
| Total | 219 (73.5%) | 79 (26.5%) | 298 (100%) |
| Reassessment | Benign | Malignant | Total | OR (CI95%) | p-Value |
|---|---|---|---|---|---|
| N | 11 (3.7%) | 0 (0%) | 11 (3.7%) | Inf (0.93-Inf) | 0.05 |
| Y | 208 (69.8%) | 79 (26.5%) | 287 (96.3%) | ||
| Total | 219 (73.5%) | 79 (26.5%) | 298 (100%) | ||
| Change of strategy | Benign | Malignant | Total | OR (CI95%) | p-value |
| N | 197 | 3 | 200 | 218.7 (64.1–1155.2) | <0.00001 |
| Y | 22 | 76 | 98 | ||
| Total | 219 | 79 | 298 |
| Variable | OR | CI (Inf) 95% | CI (Sup) 95% | p-Value |
|---|---|---|---|---|
| Size | 0.193 | 0.081 | 0.404 | <0.00005 *** |
| Spiculated margins + | 5.694 | 1.992 | 10.70 | <0.005 ** |
| Microcalcifications + | 5.050 | 1.542 | 10.88 | <0.01 ** |
| Taller than wide + | 10.16 | 1.006 | 30.09 | 0.07456 |
| Extra-thyroidal growth + | >6000 | >0.001 | <20,000 | 0.98672 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Orlando, G.; Graceffa, G.; Mazzola, S.; Vassallo, F.; Proclamà, M.P.; Richiusa, P.; Radellini, S.; Paladino, N.C.; Melfa, G.; Scerrino, G. The Role of “Critical” Ultrasound Reassessment in the Decision-Making of Bethesda III Thyroid Nodules. Medicina 2023, 59, 1484. https://doi.org/10.3390/medicina59081484
Orlando G, Graceffa G, Mazzola S, Vassallo F, Proclamà MP, Richiusa P, Radellini S, Paladino NC, Melfa G, Scerrino G. The Role of “Critical” Ultrasound Reassessment in the Decision-Making of Bethesda III Thyroid Nodules. Medicina. 2023; 59(8):1484. https://doi.org/10.3390/medicina59081484
Chicago/Turabian StyleOrlando, Giuseppina, Giuseppa Graceffa, Sergio Mazzola, Fabrizio Vassallo, Maria Pia Proclamà, Pierina Richiusa, Stefano Radellini, Nunzia Cinzia Paladino, Giuseppina Melfa, and Gregorio Scerrino. 2023. "The Role of “Critical” Ultrasound Reassessment in the Decision-Making of Bethesda III Thyroid Nodules" Medicina 59, no. 8: 1484. https://doi.org/10.3390/medicina59081484





