Higher C-Reactive Protein to Albumin Ratio Portends Long-Term Mortality in Patients with Chronic Heart Failure and Reduced Ejection Fraction
Abstract
:1. Introduction
2. Materials and Methods
2.1. Study Setting and Participants
2.2. Data Collection
2.3. Follow-Up and Endpoint
2.4. Statistical Analysis
3. Results
4. Discussion
Study Limitations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- McDonagh, T.A.; Metra, M.; Adamo, M.; Gardner, R.S.; Baumbach, A.; Böhm, M.; Burri, H.; Butler, J.; Čelutkienė, J.; Chioncel, O.; et al. 2021 ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure. Eur. Heart J. 2021, 42, 3599–3726. [Google Scholar] [CrossRef] [PubMed]
- Conrad, N.; Judge, A.; Tran, J.; Mohseni, H.; Hedgecott, D.; Crespillo, A.P.; Allison, M.; Hemingway, H.; Cleland, J.G.; McMurray, J.J.V.; et al. Temporal trends and patterns in heart failure incidence: A population-based study of 4 million individuals. Lancet 2018, 391, 572–580. [Google Scholar] [CrossRef] [PubMed]
- Jackson, S.L.; Tong, X.; King, R.J.; Loustalot, F.; Hong, Y.; Ritchey, M.D. National Burden of Heart Failure Events in the United States, 2006 to 2014. Circ. Heart Fail. 2018, 11, e004873. [Google Scholar] [CrossRef] [PubMed]
- Hartupee, J.; Mann, D.L. Neurohormonal activation in heart failure with reduced ejection fraction. Nat. Rev. Cardiol. 2017, 14, 30–38. [Google Scholar] [CrossRef] [PubMed]
- Torre-Amione, G.; Kapadia, S.; Benedict, C.; Oral, H.; Young, J.B.; Mann, D.L. Proinflammatory cytokine levels in patients with depressed left ventricular ejection fraction: A report from the Studies of Left Ventricular Dysfunction (SOLVD). J. Am. Coll. Cardiol. 1996, 27, 1201–1206. [Google Scholar] [CrossRef] [PubMed]
- Deswal, A.; Petersen, N.J.; Feldman, A.M.; Young, J.B.; White, B.G.; Mann, D.L. Cytokines and cytokine receptors in advanced heart failure: An analysis of the cytokine database from the Vesnarinone trial (VEST). Circulation 2001, 103, 2055–2059. [Google Scholar] [CrossRef]
- Anand, I.S.; Latini, R.; Florea, V.G.; Kuskowski, M.A.; Rector, T.; Masson, S.; Signorini, S.; Mocarelli, P.; Hester, A.; Glazer, R.; et al. C-reactive protein in heart failure: Prognostic value and the effect of valsartan. Circulation 2005, 112, 1428–1434. [Google Scholar] [CrossRef]
- Horwich, T.B.; Kalantar-Zadeh, K.; MacLellan, R.W.; Fonarow, G.C. Albumin levels predict survival in patients with systolic heart failure. Am. Heart J. 2008, 155, 883–889. [Google Scholar] [CrossRef]
- Yu, X.; Wen, Y.; Lin, Y.; Zhang, X.; Chen, Y.; Wang, W.; Wang, G.; Zhang, L. The value of preoperative Glasgow Prognostic Score and the C-Reactive Protein to Albumin Ratio as prognostic factors for long-term survival in pathological T1N0 esophageal squamous cell carcinoma. J. Cancer 2018, 9, 807–815. [Google Scholar] [CrossRef] [PubMed]
- Ranzani, O.T.; Zampieri, F.G.; Forte, D.N.; Azevedo, L.C.; Park, M. C-reactive protein/albumin ratio predicts 90-day mortality of septic patients. PLoS ONE 2013, 8, e59321. [Google Scholar] [CrossRef] [PubMed]
- Acet, H.; Güzel, T.; Aslan, B.; Isik, M.A.; Ertas, F.; Catalkaya, S. Predictive Value of C-Reactive Protein to Albumin Ratio in ST-Segment Elevation Myocardial Infarction Patients Treated with Primary Percutaneous Coronary Intervention. Angiology 2021, 72, 244–251. [Google Scholar] [CrossRef] [PubMed]
- Zhang, Y.; Bauersachs, J.; Langer, H.F. Immune mechanisms in heart failure. Eur. J. Heart Fail. 2017, 11, 1379–1389. [Google Scholar] [CrossRef] [PubMed]
- Hedayat, M.; Mahmoudi, M.J.; Rose, N.R.; Rezaei, N. Proinflammatory cytokines in heart failure: Double-edged swords. Heart Fail. Rev. 2010, 15, 543–562. [Google Scholar] [CrossRef] [PubMed]
- Mueller, C.; Laule-Kilian, K.; Christ, A.; Brunner-La Rocca, H.P.; Perruchoud, A.P. Inflammation and long-term mortality in acute congestive heart failure. Am. Heart J. 2006, 151, 845–850. [Google Scholar] [CrossRef] [PubMed]
- Vasan, R.; Sullivan, L.; Roubenoff, R. Inflammatory markers and risk of heart failure in elderly subjects without prior myocardial infarction: The Framingham Heart Study. Circulation 2003, 107, 1486–1491. [Google Scholar] [CrossRef] [PubMed]
- Minami, Y.; Kajimoto, K.; Sato, N.; Hagiwara, N.; Takano, T.; ATTEND Study Investigators. C-reactive protein level on admission and time to and cause of death in patients hospitalized for acute heart failure. Eur. Heart J. Qual. Care Clin. Outcomes 2017, 3, 148–156. [Google Scholar] [CrossRef] [PubMed]
- Park, J.J.; Choi, D.-J.; Yoon, C.-H.; Oh, I.-Y.; Jeon, E.-S.; Kim, J.-J.; Cho, M.-C.; Chae, S.C.; Ryu, K.-H.; Yoo, B.-S.; et al. Prognostic value of C-reactive protein as an inflammatory and N-terminal pro-brain natriuretic peptide as a neurohumoral marker in acute heart failure (from the Korean Heart Failure registry). Am. J. Cardiol. 2014, 113, 511–517. [Google Scholar] [CrossRef]
- Arques, S.; Roux, E.; Stolidi, P.; Gelisse, R.; Ambrosi, P. Usefulness of serum albumin and serum total cholesterol in the prediction of hospital death in older patients with severe, acute heart failure. Arch. Cardiovasc. Dis. 2011, 104, 502–508. [Google Scholar] [CrossRef]
- Ancion, A.; Allepaerts, S.; Robinet, S.; Oury, C.; Pierard, L.A.; Lancellotti, P. Serum albumin level and long-term outcome in acute heart failure. Acta Cardiol. 2019, 74, 465–471. [Google Scholar] [CrossRef]
- Arques, S.; Ambrosi, P. Human serum albumin in the clinical syndrome of heart failure. J. Card. Fail. 2011, 17, 451–458. [Google Scholar] [CrossRef]
- Yoshihisa, A.; Watanabe, S.; Kanno, Y.; Takiguchi, M.; Sato, A.; Yokokawa, T.; Miura, S.; Shimizu, T.; Abe, S.; Sato, T.; et al. The CHA2DS2-VASc score as a predictor of high mortality in hospitalized heart failure patients. ESC Heart Fail. 2016, 3, 261–269. [Google Scholar] [CrossRef]
- Agostoni, P.; Paolillo, S.; Mapelli, M.; Gentile, P.; Salvioni, E.; Veglia, F.; Bonomi, A.; Corrà, U.; Lagioia, R.; Limongelli, G.; et al. Multiparametric prognostic scores in chronic heart failure with reduced ejection fraction: A long-term comparison. Eur. J. Heart Fail. 2018, 20, 700–710. [Google Scholar] [CrossRef] [PubMed]
- Cho, J.Y.; Kim, K.H.; Cho, H.-J.; Lee, H.-Y.; Choi, J.-O.; Jeon, E.-S.; Lee, S.E.; Kim, M.-S.; Kim, J.-J.; Hwang, K.-K.; et al. Nutritional risk index as a predictor of mortality in acutely decompensated heart failure. PLoS ONE 2018, 13, e0209088. [Google Scholar] [CrossRef]
- Nishi, I.; Ibaraki Cardiovascular Assessment Study-Heart Failure Investigators; Seo, Y.; Hamada-Harimura, Y.; Sato, K.; Sai, S.; Yamamoto, M.; Ishizu, T.; Sugano, A.; Obara, K.; et al. Nutritional screening based on the controlling nutritional status (CONUT) score at the time of admission is useful for long-term prognostic prediction in patients with heart failure requiring hospitalization. Heart Vessel. 2017, 32, 1337–1349. [Google Scholar] [CrossRef]
- Fairclough, E.; Cairns, E.; Hamilton, J.; Kelly, C. Evaluation of a modified early warning system for acute medical admissions and comparison with C-reactive protein/albumin ratio as a predictor of patient outcome. Clin. Med. 2009, 9, 30–33. [Google Scholar] [CrossRef]
- Castell, J.V.; Gómez-Lechón, M.J.; David, M.; Andus, T.; Geiger, T.; Trullenque, R.; Fabra, R.; Heinrich, P.C. Interleukin-6 is the major regulator of acute phase protein synthesis in adult human hepatocytes. FEBS Lett. 1989, 242, 237–239. [Google Scholar] [CrossRef] [PubMed]
- Blake, G.J.; Ridker, P.M. Novel clinical markers of vascular wall inflammation. Circ. Res. 2001, 89, 763–771. [Google Scholar] [CrossRef]
- Gruys, E.; Toussaint, M.J.; Niewold, T.A.; Koopmans, S.J. Acute phase reaction and acute phase proteins. J. Zhejiang Univ. Sci. B 2005, 6, 1045–1056. [Google Scholar] [CrossRef]
- Li, L.; Dai, L.; Wang, X.; Wang, Y.; Zhou, L.; Chen, M.; Wang, H.; Karpinsky, G.; Fatyga, A.; Krawczyk, M.A.; et al. Predictive value of the C-reactive protein-to-prealbumin ratio in medical ICU patients. Biomark. Med. 2017, 11, 329–337. [Google Scholar] [CrossRef]
- Kaplan, M.; Ates, I.; Akpinar, M.Y.; Yuksel, M.; Kuzu, U.B.; Kacar, S.; Coskun, O.; Kayacetin, E. Predictive value of C-reactive protein/albumin ratio in acute pancreatitis. Hepatobiliary Pancreat. Dis. Int. 2017, 16, 424–430. [Google Scholar] [CrossRef]
- Wada, H.; Dohi, T.; Miyauchi, K.; Doi, S.; Naito, R.; Konishi, H.; Tsuboi, S.; Ogita, M.; Kasai, T.; Okazaki, S.; et al. Independent and combined effects of serum albumin and C-reactive protein on long-term outcomes of patients undergoing percutaneous coronary intervention. Circ. J. 2017, 81, 1293–1300. [Google Scholar] [CrossRef]
- Karabağ, Y.; Çağdaş, M.; Rencuzogullari, I.; Karakoyun, S.; Artaç, I.; İliş, D.; Atalay, E.; Yesin, M.; Gürsoy, M.O.; Tanboğa, I.H. Relationship between C-reactive protein/albumin ratio and coronary artery disease severity in patients with stable angina pectoris. J. Clin. Lab. Anal. 2018, 32, e22457. [Google Scholar] [CrossRef] [PubMed]
- Çağdaş, M.; Rencüzoğullari, I.; Karakoyun, S.; Karabağ, Y.; Yesin, M.; Artaç, I.; Iliş, D.; Çağdaş, S.; Tezcan, A.H.; Tanboğa, H.I. Assessment of Relationship between C-Reactive Protein to Albumin Ratio and Coronary Artery Disease Severity in Patients with Acute Coronary Syndrome. Angiology 2019, 70, 361–368. [Google Scholar] [CrossRef] [PubMed]
- Çinier, G.; Hayıroğlu, M.İ.; Kolak, Z.; Tezen, O.; Yumurtaş, A.Ç.; Pay, L.; Eren, S.; Çetin, T.; Özcan, S.; Türkkan, C.; et al. The value of C-reactive protein-to-albumin ratio in predicting long-term mortality among HFrEF patients with implantable cardiac defibrillators. Eur. J. Clin. Investig. 2021, 51, e13550. [Google Scholar] [CrossRef]
- Cho, A.; Arfsten, H.; Goliasch, G.; Bartko, P.E.; Wurm, R.; Strunk, G.; Hülsmann, M.; Pavo, N. The inflammation-based modified Glasgow prognostic score is associated with survival in stable heart failure patients. ESC Heart Fail. 2020, 7, 654–662. [Google Scholar] [CrossRef]
- Erdogan, G.; Yenerçağ, M.; Uçar, M.; Öztürk, O.; Şeker, O.O.; Yontar, O.C.; Çakmak, E.Ö.; Karagöz, A.; Şahin, İ.; Arslan, U. Modified Glasgow Prognostıc Score May Be Useful to Predict Major Adverse Cardiac Events in Heart Failure Patients Undergone Cardiac Resynchronization Treatment. Turk. Kardiyol. Dern. Ars. 2023, 51, 104–111. [Google Scholar] [CrossRef] [PubMed]
- Lima, P.C.; Rios, D.M.; de Oliveira, F.P.; Passos, L.R.; Ribeiro, L.B.; Serpa, R.G.; Calil, O.A.; de Barros, L.C.; Barbosa, L.F.M.; Barbosa, R.R. Inflammation as a Prognostic Marker in Heart Failure. Cureus 2022, 14, e28605. [Google Scholar] [CrossRef]
- Murphy, S.P.; Ibrahim, N.E.; Januzzi, J.L., Jr. Heart Failure with Reduced Ejection Fraction: A Review. JAMA 2020, 324, 488–504. [Google Scholar] [CrossRef]
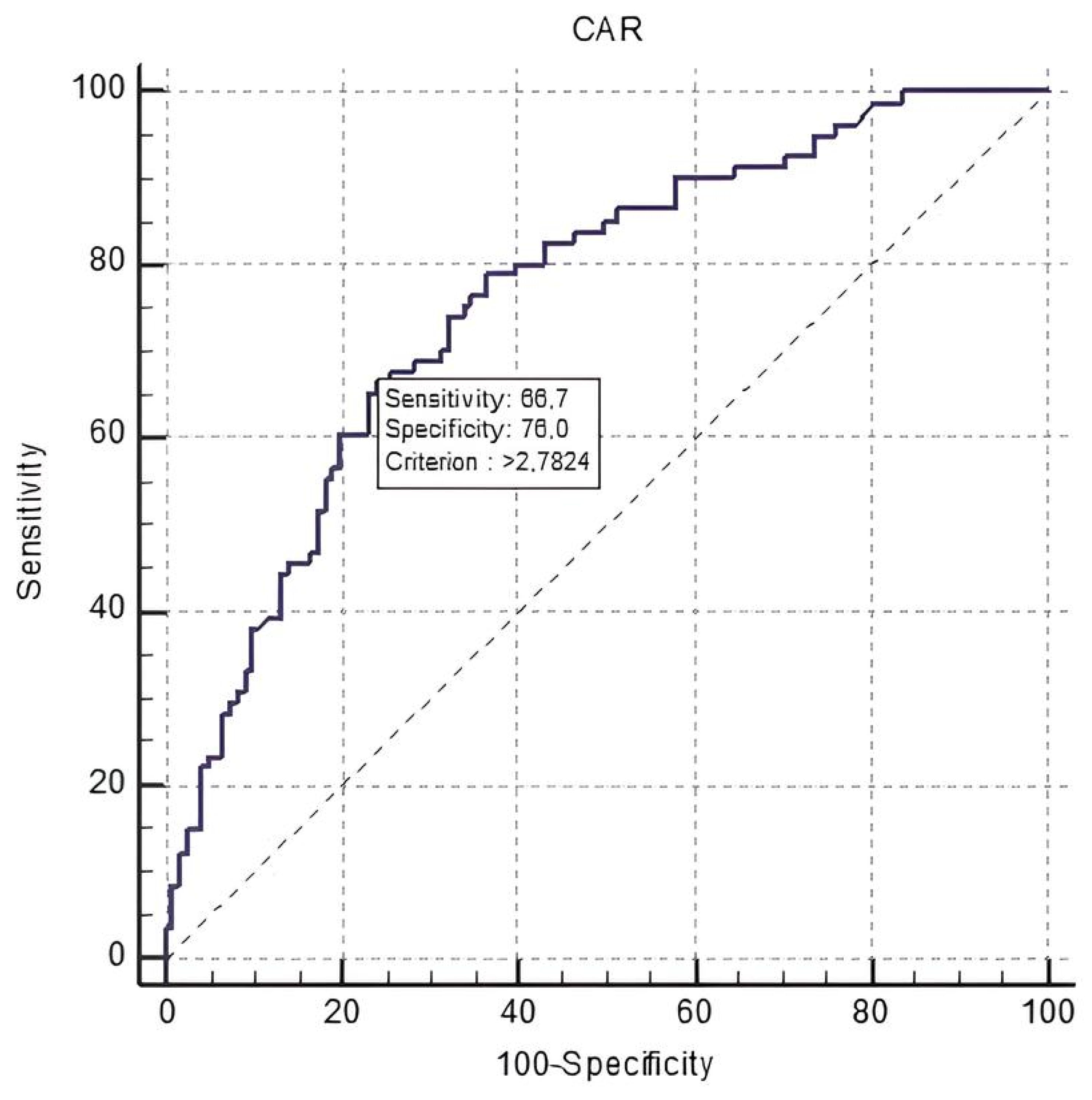
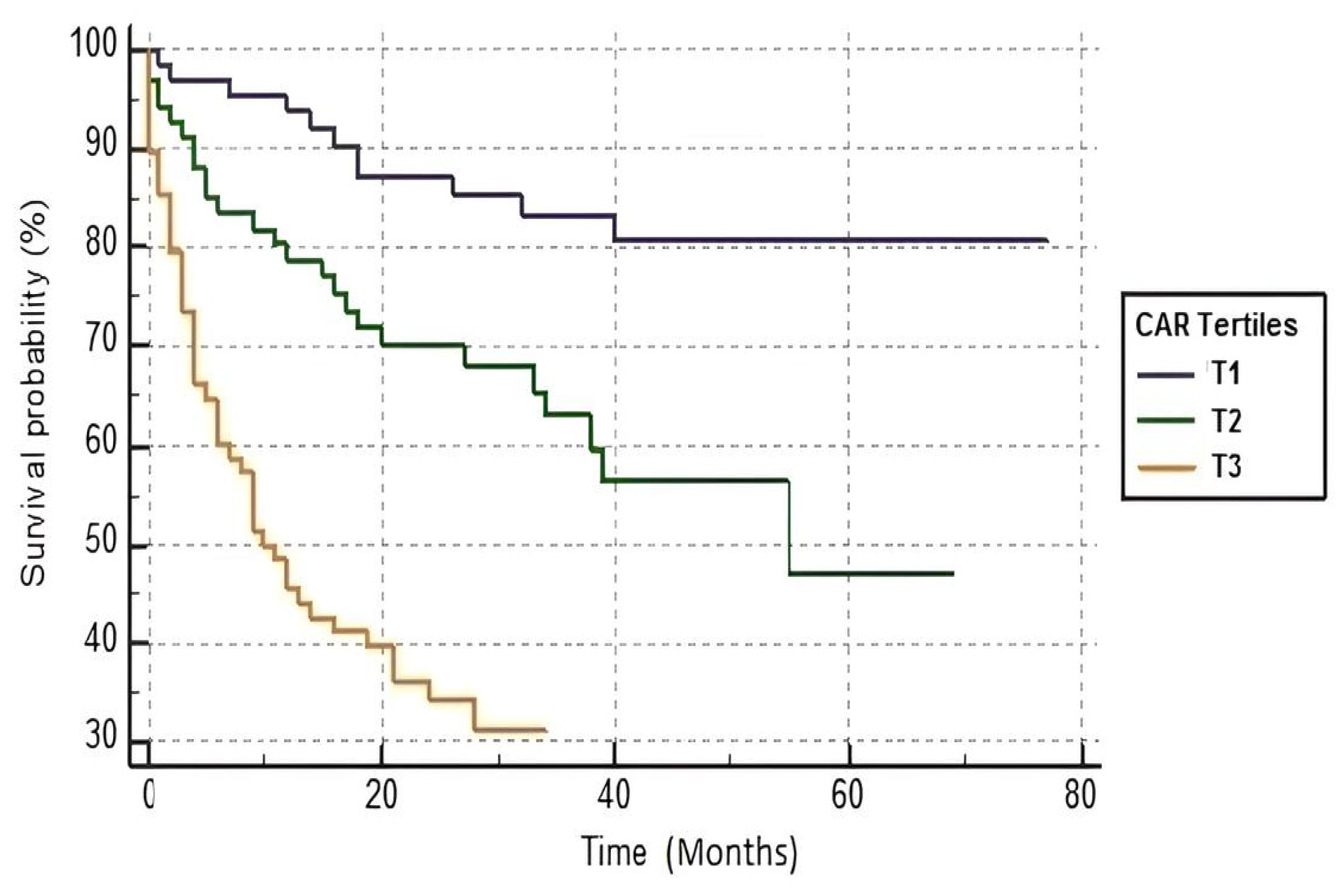
| Survivor Group (n = 242) | Non-Survivor Group (n = 162) | p Value | |
|---|---|---|---|
| Age, years | 55 ± 13 | 66 ± 14 | <0.001 |
| Female gender, n (%) | 74 (30.6) | 50 (30.9) | 0.966 |
| History | |||
| Hypertension, n (%) | 118 (48.8) | 116 (71.6) | 0.001 |
| Diabetes mellitus, n (%) | 92 (38.0) | 56 (34.6) | 0.618 |
| Hyperlipidemia, n (%) | 42 (17.4) | 50 (30.9) | 0.025 |
| Smoking history, n (%) | 134 (55.4) | 80 (49.4) | 0.403 |
| CRF, n (%) | 36 (14.9) | 52 (32.1) | 0.004 |
| CAD, n (%) | 100 (41.3) | 98 (60.5) | 0.008 |
| CVD, n (%) | 16 (6.7) | 14 (8.8) | 0.584 |
| AF, n (%) | 56 (23.1) | 74 (45.7) | 0.001 |
| At admission | |||
| SBP, mmHg | 136 ± 29 | 138 ± 37 | 0.072 |
| Heart rate, bpm | 87 ± 8 | 89 ± 10 | 0.082 |
| LVEF, % | 26 (19–33) | 25 (22–33) | 0.022 |
| Medication | |||
| Beta-blocker, n (%) | 240 (99.2) | 160 (98.8) | 0.774 |
| ACE-i or ARB, n (%) | 222 (91.7) | 134 (82.7) | 0.052 |
| MRA, n (%) | 146 (60.3) | 88 (54.3) | 0.396 |
| P2Y12 inhibitors, n (%) | 32 (13.2) | 38 (23.5) | 0.060 |
| ASA, n (%) | 142 (58.7) | 86 (53.1) | 0.432 |
| Statin, n (%) | 92 (38.0) | 68 (42.0) | 0.573 |
| Digoxin, n (%) | 24 (9.9) | 30 (18.5) | 0.078 |
| VKA, n (%) | 90 (37.2) | 78 (48.1) | 0.121 |
| NOAC, n (%) | 20 (8.3) | 20 (12.3) | 0.341 |
| Laboratory variables | |||
| Glucose, mg/dL | 105 (91–134) | 104 (92–140) | 0.969 |
| NT-pro-BNP, ng/L | 898 (311–1837) | 2575 (1150–8770) | <0.001 |
| Troponin I, ng/dL | 0.03 (0.01–0.07) | 0.05 (0.035–0.12) | 0.040 |
| Creatinine, mg/dL | 1.05 (0.84–1.3) | 1.26 (0.96–1.5) | 0.003 |
| Sodium, mEq/L | 136.4 ± 4.0 | 136.6 ± 4.7 | 0.660 |
| Potassium, mEq/L | 4.3 ± 0.6 | 4.4 ± 0.6 | 0.146 |
| Magnesium, mg/dL | 2.02 ± 0.36 | 2.08 ± 0.29 | 0.335 |
| Total cholesterol, mg/dL | 160 (138–200) | 160 (124–186) | 0.118 |
| Total protein, g/dL | 6.77 ± 0.78 | 6.36 ± 0.83 | <0.001 |
| Albumin, g/dL | 3.80 ± 0.52 | 3.36 ± 0.58 | <0.001 |
| CRP, mg/dL | 2.0 (0.4–10.1) | 22.3 (6.0–67.0) | <0.001 |
| WBC count, cells/µL | 8.9 ± 2.7 | 9.0 ± 3.1 | 0.190 |
| Hemoglobin, g/dL | 12.7 ± 1.8 | 11.9 ± 2.0 | 0.007 |
| Platelet, 103/µL | 243 ± 80 | 223 ± 95 | 0.113 |
| Neutrophil, 103/µL | 5.7 ± 2.5 | 6.3 ± 3.1 | 0.014 |
| Lymphocyte, 103/µL | 2.1 ± 1.3 | 1.7 ± 1.2 | 0.035 |
| CAR, ×100 | 0.6 (0.1–2.6) | 6.7 (1.6–20.4) | <0.001 |
| Cardiac devices (ICD or CRT), n (%) | 168 (69.4) | 74 (45.7) | <0.001 |
| Follow-up duration, months | 34 (24–47) | 7 (2–16) | <0.001 |
| T1 [0 < CAR < 0.4] (n = 132) | T2 [0.4 ≤ CAR < 5.9] (n = 136) | T3 [CAR ≥ 5.9] (n = 136) | p Value | |
|---|---|---|---|---|
| Age, years | 50 ± 11 | 58 ± 14 | 70 ± 11 | <0.001 |
| Female gender, n (%) | 36 (27.3) | 42 (30.9) | 46 (33.8) | 0.713 |
| History | ||||
| Hypertension, n (%) | 36 (27.3) | 78 (57.4) | 120 (88.2) | <0.001 |
| Diabetes mellitus, n (%) | 30 (22.7) | 56 (41.2) | 62 (45.6) | 0.015 |
| Hyperlipidemia, n (%) | 2 (1.5) | 32 (23.5) | 58 (42.6) | <0.001 |
| Smoking history, n (%) | 60 (45.4) | 66 (48.5) | 88 (64.7) | 0.055 |
| CRF, n (%) | 12 (9.1) | 24 (17.6) | 52 (38.2) | <0.001 |
| CAD, n (%) | 34 (25.8) | 76 (55.9) | 88 (64.7) | <0.001 |
| CVD, n (%) | 8 (6.1) | 10 (7.6) | 12 (8.8) | 0.831 |
| AF, n (%) | 28 (21.2) | 38 (27.9) | 64 (47.1) | 0.004 |
| At admission | ||||
| SBP, mmHg | 125 ± 14 | 128 ± 12 | 125 ± 10 | 0.812 |
| Heart rate, bpm | 87 ± 8 | 88 ± 9 | 88 ± 9 | 0.508 |
| LVEF, % | 33 (26–38) | 24 (18–32) | 23 (18–29) | <0.001 |
| Medications | ||||
| Beta-blocker, n (%) | 130 (98.5) | 136 (100) | 134 (98.5) | 0.599 |
| ACE-i or ARB, n (%) | 112 (84.8) | 120 (88.2) | 124 (91.1) | 0.526 |
| MRA, n (%) | 72 (54.5) | 80 (58.8) | 82 (60.2) | 0.783 |
| P2Y12 inhibitors, n (%) | 10 (7.6) | 30 (22.1) | 30 (22.1) | 0.039 |
| ASA, n (%) | 68 (51.5) | 78 (57.4) | 82 (60.3) | 0.581 |
| Statin, n (%) | 20 (15.2) | 70 (51.5) | 70 (51.5) | <0.001 |
| Digoxin, n (%) | 10 (7.6) | 16 (11.8) | 28 (20.6) | 0.077 |
| VKA, n (%) | 52 (39.4) | 64 (47.1) | 52 (38.2) | 0.526 |
| NOAC, n (%) | 12 (9.1) | 14 (10.3) | 14 (10.3) | 0.965 |
| Laboratory results | ||||
| Glucose, mg/dL | 101 (89–128) | 105 (93–131) | 119 (93–149) | 0.230 |
| NT-pro-BNP, ng/L | 609.5 (221–1614) | 1252.5 (552–2575) | 7590 (2950–11,600) | <0.001 |
| Troponin I, ng/dL | 0.025 (0.01–0.08) | 0.04 (0.02–0.075) | 0.06 (0.04–0.165) | <0.001 |
| Creatinine, mg/dL | 0.99 (0.8–1.22) | 1.10 (0.85–1.40) | 1.34 (1.07–1.73) | <0.001 |
| Sodium, mEq/L | 136.3 ± 3.7 | 136.6 ± 4.3 | 136.5 ± 4.7 | 0.828 |
| Potassium, mEq/L | 4.3 ± 0.6 | 4.4 ± 0.5 | 4.3 ± 0.7 | 0.367 |
| Magnesium, mg/dL | 2.08 ± 0.31 | 2.03 ± 0.29 | 1.94 ± 0.48 | 0.079 |
| Total cholesterol, mg/dL | 170 (138–208) | 156 (132–196) | 151 (125–175) | 0.014 |
| Total protein, g/dL | 6.88 ± 0.68 | 6.83 ± 0.87 | 6.12 ± 0.69 | <0.001 |
| Albumin, g/dL | 3.94 ± 0.53 | 3.68 ± 0.52 | 3.26 ± 0.49 | <0.001 |
| CRP, mg/dL | 0.45 ± 0.38 | 7.41 ± 5.46 | 65.98 ± 46.01 | <0.001 |
| WBC count, cells/µL | 8.0 (6.7–9.1) | 8.4 (7.3–10.5) | 9.1 (7.0–11.0) | 0.087 |
| Hemoglobin, g/dL | 13.1 ± 2.0 | 12.4 ± 1.6 | 11.6 ± 1.9 | <0.001 |
| Platelet, 103/µL | 242 ± 79 | 237 ± 77 | 226 ± 101 | 0.267 |
| Neutrophil, 103/µL | 5.0 ± 2.4 | 5.9 ± 2.6 | 7.0 ± 3.0 | <0.001 |
| Lymphocyte, 103/µL | 2.3 ± 1.6 | 2.1 ± 1.3 | 1.4 ± 0.7 | <0.001 |
| CAR, ×100 | 0.1 (0–0.2) | 1.6 (0.9–2.6) | 18.7 (9.2–28.1) | <0.001 |
| Cardiac devices (ICD or CRT), n (%) | 66 (50) | 81 (59.6) | 95 (69.9) | 0.004 |
| Long-term mortality, n (%) | 22 (16.7) | 50 (36.8) | 90 (66.2) | <0.001 |
| Univariate Analysis | Multivariate Analysis | |||
|---|---|---|---|---|
| p Value | HR (95% CI) | p Value | HR (95% CI) | |
| Age (1-year increase) | <0.001 | 2.750 (2.332–3.168) | 0.001 | 2.008 (1.753–2.309) |
| CAD | 0.010 | 1.936 (1.046–3.188) | 0.087 | 1.057 (0.903–1.678) |
| Hypertension | 0.002 | 2.001 (1.462–3.891) | 0.056 | 1.068 (0.958–1.843) |
| Hyperlipidemia | 0.022 | 1.865 (1.059–3.003) | 0.102 | 1.043 (0.874–1.564) |
| CRF | 0.003 | 1.996 (1.349–3.447) | 0.061 | 1.081 (0.916–1.981) |
| AF | 0.001 | 2.205 (1.423–3.418) | 0.051 | 1.071 (0.943–1.780) |
| LVEF (1% decrease) | 0.025 | 1.431 (1.023–1.891) | 0.102 | 1.018 (0.871–1.291) |
| Cardiac devices (absence) | <0.001 | 3.106 (1.488–6.482) | 0.001 | 2.458 (1.592–4.875) |
| Creatinine (0.1 mg/dL increase) | 0.003 | 1.809 (1.236–2.647) | 0.083 | 1.023 (0.805–1.592) |
| NT-pro-BNP (50 pg/mL increase) | <0.001 | 2.987 (1.407–5.003) | 0.002 | 1.967 (1.108–2.709) |
| Troponin I (0.01 ng/dL increase) | 0.042 | 1.657 (0.963–2.850) | 0.456 | 1.006 (0.786–1.342) |
| Hemoglobin (1 g/dL decrease) | 0.010 | 0.857 (0.758–0.968) | 0.090 | 1.064 (0.851–1.302) |
| CAR | <0.001 | 2.927 (1.617–4.987) | 0.005 | 1.852 (1.124–2.581) |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Tanık, V.O.; Akdeniz, E.; Çınar, T.; Şimşek, B.; İnan, D.; Kıvrak, A.; Karabağ, Y.; Çağdaş, M.; Kalkan, K.; Karabay, C.Y.; et al. Higher C-Reactive Protein to Albumin Ratio Portends Long-Term Mortality in Patients with Chronic Heart Failure and Reduced Ejection Fraction. Medicina 2024, 60, 441. https://doi.org/10.3390/medicina60030441
Tanık VO, Akdeniz E, Çınar T, Şimşek B, İnan D, Kıvrak A, Karabağ Y, Çağdaş M, Kalkan K, Karabay CY, et al. Higher C-Reactive Protein to Albumin Ratio Portends Long-Term Mortality in Patients with Chronic Heart Failure and Reduced Ejection Fraction. Medicina. 2024; 60(3):441. https://doi.org/10.3390/medicina60030441
Chicago/Turabian StyleTanık, Veysel Ozan, Evliya Akdeniz, Tufan Çınar, Barış Şimşek, Duygu İnan, Ahmet Kıvrak, Yavuz Karabağ, Metin Çağdaş, Kamuran Kalkan, Can Yücel Karabay, and et al. 2024. "Higher C-Reactive Protein to Albumin Ratio Portends Long-Term Mortality in Patients with Chronic Heart Failure and Reduced Ejection Fraction" Medicina 60, no. 3: 441. https://doi.org/10.3390/medicina60030441






