Abstract
This study was undertaken to determine whether there was an association between coarse particles (PM2.5–10) levels and frequency of hospital admissions for respiratory diseases (RD) in Kaohsiung, Taiwan. Hospital admissions for RD including chronic obstructive pulmonary disease (COPD), asthma, and pneumonia, and ambient air pollution data levels for Kaohsiung were obtained for the period from 2006 to 2010. The relative risk of hospital admissions for RD was estimated using a case-crossover approach, controlling for weather variables, day of the week, seasonality, and long-term time trends. For the single pollutant model (without adjustment for other pollutants), increased rate of admissions for RD were significantly associated with higher coarse PM levels only on cool days (<25 °C), with a 10 µg/m3 elevation in PM2.5–10 concentrations associated with a 3% (95% CI = 1%–5%) rise in COPD admissions, 4% (95% CI = 1%–7%) increase in asthma admissions, and 3% (95% CI = 2%–4%) rise in pneumonia admissions. No significant associations were found between coarse particle levels and the number of hospital admissions for RD on warm days. In the two-pollutant models, PM2.5–10 levels remained significantly correlated with higher rate of RD admissions even controlling for sulfur dioxide, nitrogen dioxide, carbon monoxide, or ozone on cool days. This study provides evidence that higher levels of PM2.5–10 enhance the risk of hospital admissions for RD on cool days.
1. Introduction
Over the past decade, many epidemiologic studies demonstrated positive associations between ambient levels of particulate matter (PM) (generally measured as PM with an aerodynamic diameter < 10µm (PM10)) and daily mortality and hospital admissions or emergency room (ER) visits for cardiovascular and respiratory morbidity [1,2,3,4,5]. PM10 was seen as the most health relevant PM size fraction and therefore measured on a regular basis worldwide.
While previous studies primarily used PM10 as an exposure indicator, fine particles (defined as PM with an aerodynamic diameter less than 2.5 µm; PM2.5) have become a greater health and regulatory concern due to data based upon epidemiologic studies suggesting that PM2.5 might exert greater toxicity than larger particles [6,7,8,9,10]. It is now generally accepted that PM2.5 are more harmful to health than larger particles (PM10) because PM2.5 offer a greater surface area and hence potentially larger concentrations of adsorbed or condensed toxic air pollutants per unit mass [11,12,13]. Most of the prior studies only used PM2.5 or PM10 as particle measurements, leaving the effects of other particle sizes—particularly PM2.5–10—not well understood [6,14].
Fewer studies have examined the potential adverse health effects attributed to the coarse fraction, that is, particles ranging in size from 2.5µm to 10µm in aerodiameter (PM2.5–10) [14]. PM2.5–10 originate mainly from abrasive mechanical processes such as mechanical grinding, windblown dust, and agricultural activities. PM2.5–10 are predominantly composed of crustal-related materials such as calcium (Ca), magnesium (Mg), aluminum (Al), silicon, and iron (Fe), and primary organic materials such as pollen, spores, as well as plant and animal debris [11,15,16]. In contrast, the origin of chemical composition of PM2.5 is combustion-related constituents. PM2.5 are composed of many organic and inorganic compounds, including sulfate, nitrate, organic carbon and elemental carbon, carbonates, metals, and water [17,18]. The adverse health effects associated with ambient exposure to PM2.5–10 may thus differ from those of PM2.5 considering differences in the sites of deposition in the respiratory tract and sources and chemical composition for these two different-sized fractions [19].
Although the association between PM2.5 levels and adverse respiratory health outcomes (RD) is well established [5,12,20,21,22,23,24,25,26,27,28,29,30,31,32], epidemiologic data on the influence of PM2.5–10 on RD morbidity are limited and inconsistent [19,21,24,33,34,35,36,37,38,39,40,41]. More comprehensive knowledge of the health risks associated with exposure to PM2.5–10 is still needed as suggested in a review on this topic by Brunekreef and Forsberg (2005) [14], in which the authors concluded that coarse PM has a stronger or as strong a short-term effect on respiratory health as fine PM. Because above mentioned studies were conducted primarily in America and some European cities, the findings may not be applicable to Taiwan, which has different air pollutant mixtures and environmental conditions.
This study was undertaken to examine the short-term associations of daily concentrations of PM2.5–10 with frequency of hospital admissions for RD including chronic obstructive pulmonary disease (COPD), asthma, and pneumonia among individuals residing in Kaohsiung city, a large industrial city in southwest Taiwan, over a 5 year period from 2006 to 2010, using a case-crossover design.
2. Materials and Methods
2.1. Kaohsiung City
Kaohsiung is the largest commercial harbor and the second largest city in Taiwan, with a population of approximately 1.46 million. It is the chief center of the heavy industry, including China Steel Corporation and China Shipbuilding Corporation, and of the petrochemical industry situated on the southwest coast of Taiwan. The city is considered a symbol of recent success in Taiwan’s economic development.
2.2. Hospital Admission Data
The National Health Insurance (NHI) Program, which provides compulsory universal health insurance, was implemented in Taiwan on 1 March 1995. Most medical institutions (93%) are contracted to the Bureau of NHI (BNHI), and those not contracted provide fewer health services. More than 96% of the population who are covered by NHI used health services at least one time through contracted medical institutions.
Computerized records of daily clinic visits or hospital admissions are available for each contracted medical institution. All medical institutions must submit standard claim documents for medical expenses on a computerized form, which includes the date of admission and discharge, identification number, gender, birthday, and diagnostic code of each admission. Therefore, the information from the NHI database appears to be sufficiently complete, reliable, and accurate for use in epidemiological studies. In total, 15,283,304 admissions were collected for the period of 2006–2010. Of the 15,283,304 admissions, 1,229,455 were recorded in Kaohsiung city (8.04% of all the admissions). Daily counts of hospital admissions with a primary diagnosis of RD were extracted from the medical insurance files for the period 2006–2010. RD outcomes included the following conditions: COPD (International Classification of Diseases, 9th revision (ICD-9) codes 490–492, 494, and 496), asthma (code 493), and pneumonia (codes 480–486). In addition, this study was approved by the ethics review board of Kaohsiung Medical University Hospital (KMUH-IRB-EXEMPT-20130018).
2.3. Pollutant and Meteorological Data
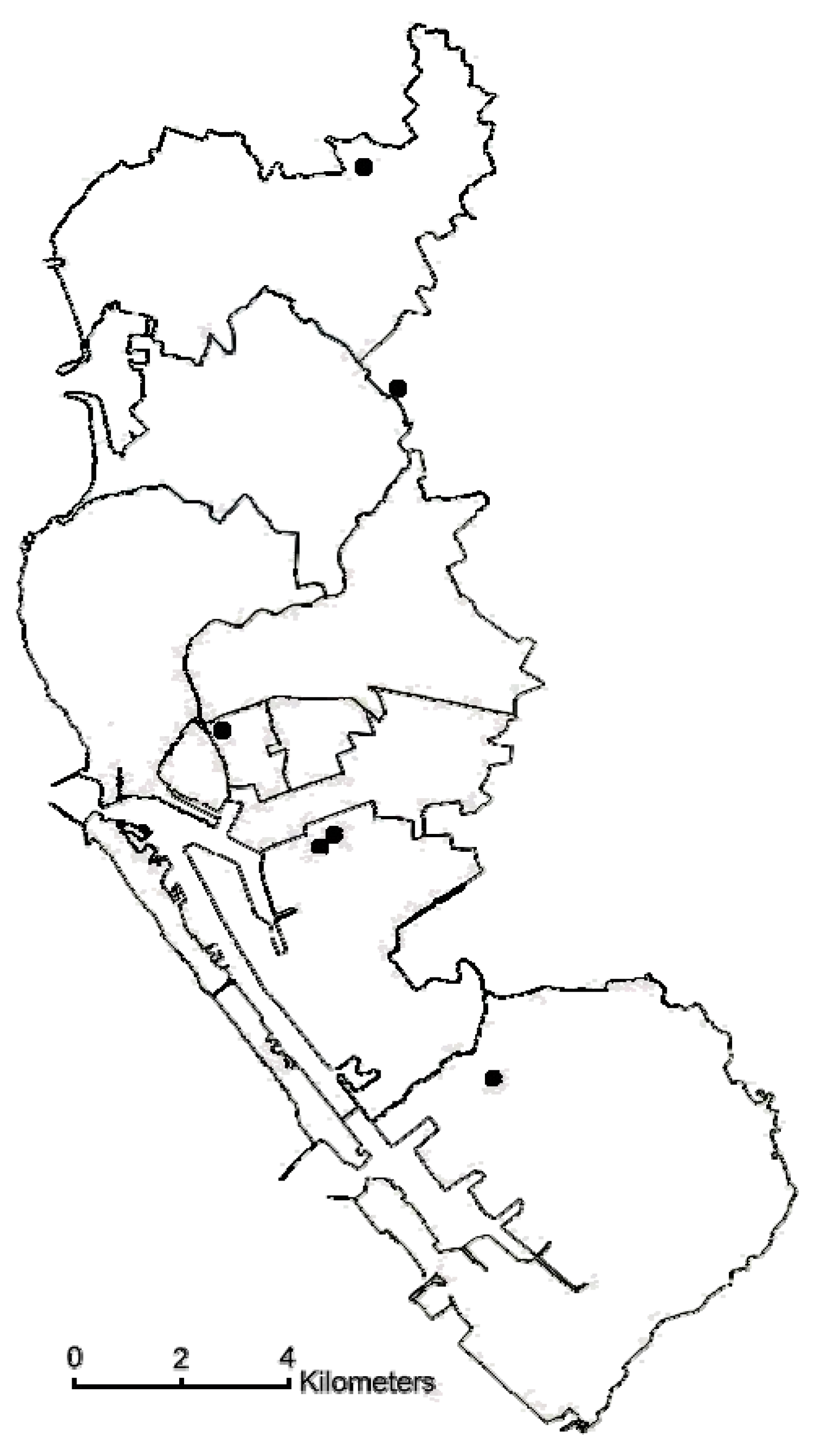
Six air-quality monitoring stations were established in Kaohsiung city by the Taiwanese Environmental Protection Administration (EPA), a central governmental agency in 1994 (Figure 1). The stations used commercial monitoring instruments designated by the USEPA as an equivalent or reference method and manufactured by US Thermo Environmental Instruments, Inc. (Franklin, MA, USA). The monitoring stations were fully automated and routinely monitored 5 “criteria” pollutants including sulfur dioxide (SO2) (by ultraviolet fluorescence); particulate matter (PM10) (by beta-ray absorption); nitrogen dioxide (NO2) (by ultraviolet fluorescence), carbon monoxide (CO) (by nondispersive infrared photometry), and ozone (O3) (by ultraviolet photometry) levels. However, PM2.5 was not regularly monitored. PM2.5 concentrations in Taiwan were measured continuously since 2006. PM2.5 was measured using tapered element oscillating microbalance method samplers. The availability of the monitoring network for PM2.5 and the continuation of PM10 monitoring provided an opportunity to calculate coarse PM concentrations. The concentration of the coarse fraction was calculated by subtracting PM2.5 levels from PM10 levels. For each day, hourly air pollution data were obtained for all of the monitoring stations. After calculating the hourly mean of each pollutant from the 6 stations, the 24-hr average levels of these pollutants were computed. Daily information on mean temperature and mean humidity was provided by the Central Weather Bureau from a station located on the coastline of Kaohsiung Harbor.
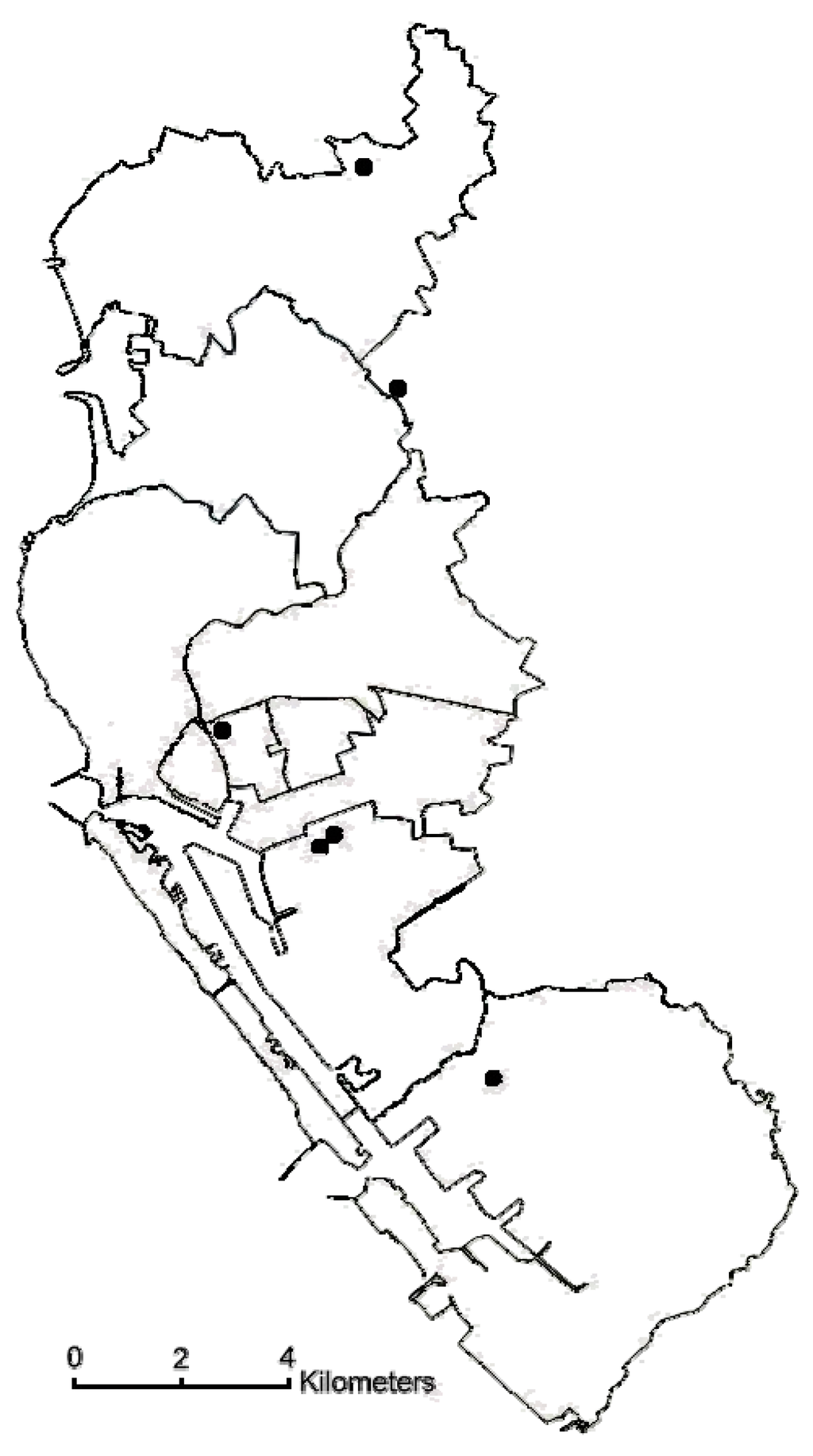
Figure 1.
Map of Kaohsiung city showing location of the air quality monitoring stations.
Figure 1.
Map of Kaohsiung city showing location of the air quality monitoring stations.
2.4. Statistics
Data were analyzed using the case-crossover technique [42,43,44]. This design is an alternative to Poisson time series regression models for studying the short-term effects attributed to air pollutants (Levy et al., 2001). In general, the case-crossover design and the time-series approach yielded almost identical results [45,46].
The time-stratified approach was used for the case-crossover analysis [47]. A stratification of time into separate months was made to select referent days as the days falling on the same day of the week within the same month as the index day. Air pollution levels during the case period were compared with exposures occurring on all referent days. This time-stratified referent selection scheme minimizes bias due to non-stationarity of air pollution time-series data. [48,49,50] Results of previous investigations indicated that increased number of hospital admissions for RD were associated with higher ambient air pollutant levels on the same day or the previous two days [51]. Longer lag times have rarely been described. Thus the cumulative lag period up to 2 previous days (i.e., the average air pollutant levels of the same and previous 2 days) was used. Because pollutants vary considerably by season, especially O3 and PM, seasonal interactions between PM and hospital admissions have often been reported. However, previous studies were conducted mostly in countries where the climates are substantially different from that in Kaohsiung [52,53], which has a tropical climate with no apparent 4-season cycle. Hence in this study the potential interactions of seasonality on the adverse effects of PM were not considered, but temperature was used instead. The adverse health effects of each air pollutant were examined for the “warm” days (days with a mean temperature above 25 °C) and “cool” days (days with a mean temperature below 25 °C) separately.
The associations between hospital admissions for RD and levels of PM were estimated using the odds ratio (OR) and their 95% confidence intervals (CI), which were generated using conditional logistic regression with weights equal to the number of hospital admissions on that day. All statistical analyses were performed using the SAS package (version 9.2; SAS Institute, Inc., Cary, NC). Both single-pollutant models and multi-pollutant models were fitted with a different combination of pollutants (up to two pollutants per model) to assess the stability of the effects of PM. Exposure levels to air pollutants were entered into the models as continuous variables. Meteorological variables such as daily average temperature and humidity on the same day, which might play a confounding role, were included in the model. Inclusion of barometric pressure did not markedly change the effect estimates and therefore was not considered in the final model. ORs were calculated on the basis of an increment in exposure corresponding to the 10 µg/m3 of PM2.5, PM10, and PM2.5–10. The criterion for significance was set at p < 0.05.
3. Results and Discussion
During the 5 years of the study, there were a total of 81,836 hospital admissions for RD (14,136 for COPD, 5222 for asthma, and 62,478 for pneumonia) for the 63 hospitals in Kaohsiung City. The descriptive statistics for hospital admissions and corresponding environmental data are shown in Table 1. The average fine and coarse PM during the study period was 45.88 µg/m3 and 31.65 µg/m3, respectively. Approximately 60% of PM10 mass may be attributed to PM2.5 mass. There was a mean of 44.82 daily hospital admissions for RD (7.74 for COPD, 2.86 for asthma, and 34.22 for pneumonia) in the city over the study period.
Pearson’s correlation coefficients among the air pollutants are presented in Table 2.
Table 3 shows the effect estimates of PM on frequency of hospital admissions for RD in single-pollutant and two-pollutant models. Data demonstrated that the relationship between PM and RD-related hospital admissions differed by season. Generally, no significant associations between PM and number of hospital admissions for RD were observed on warm days.
On cool days, there were consistent significant positive associations with RD-related hospital admissions in single pollutant model (without adjustment for other pollutants) for all PM (PM2.5, PM10, and PM2.5–10), with a 10 µg/m3 increase in PM2.5 associated with a 11% (95% CI = 9%–13%), 10% (95% CI = 6%–13%), and 12% (95% CI = 11%–13%) rise in COPD, asthma, and pneumonia admissions, respectively. A 10 µg/m3 elevation in PM2.5–10 was associated with a 3% (95% CI = 1%–5%) increase in rate of COPD, 4% (95% CI = 1%–7%) asthma, and 3% (95% CI = 2%–4%) increase in pneumonia admissions. For PM10, the corresponding estimates were 5% (95% CI = 3%–6%), 4% (95% CI = 3%–6%), and 5% (95% CI = 4%–5%), respectively. PM2.5 showed more potent effect on RD-related admissions than PM2.5–10 and PM10. In two-pollutant models, the influence of all PM on RD-related admissions generally remained significant after inclusion of other pollutants including SO2, NO2, CO, or O3 in the regression model. Similarly, PM2.5 demonstrated the greatest effect on rate of RD-related admissions. Compared to effect estimate associated with a 10 µg/m3 increase in PM2.5 levels, effect estimates of number of RD-related admissions associated with the same rise in PM2.5–10 and PM10 levels were weaker. However, CI of respective effect estimates for PM2.5–10 and PM10 overlapped.
This study is one of the few that investigated the association between exposure to fine and coarse particles and rate of hospital admissions for RD. Data showed that the levels of fine and coarse particles were correlated with increased risk of hospital admissions for RD including COPD, asthma, and pneumonia, and only on cool days. In addition, PM2.5 demonstrated a stronger effect on RD-related admissions than PM2.5–10.
The correlation between fine and coarse PM was moderate at values of 0.28–0.69 in previous studies with a higher value at 0.69 in Steubenville, USA [54]. In contrast, the relationship between PM10 and fine as well as coarse PM was greater [14]. The implication is that analyses based on PM10 are generally not able to support arguments on the relative importance of fine and coarse PM in the induction of RD. The correlation between fine and coarse PM (r = 0.64) in this study enables separation of the two effects but it was not possible to disentangle the joint effects of coarse and fine PM in a two-pollutant model given their correlation levels. It is unfortunate that thus far, few studies have reported the results from two-pollutant analyses.
Epidemiologic studies on the effects of coarse particles on hospitalizations for RD are limited and inconsistent. A study conducted in 6 French cities, Host et al. [21] found positive association between coarse PM and hospitalizations for respiratory infection, with an excess risk of 4.4% (95% CI = 0.9%–8.0%) per 10 µg/m3 increase in PM2.5–10 levels. Qiu et al. [33] conducted a study in Hong Kong, and reported an interquartile range (IQR = 10.9µg/m3) increase of PM2.5–10 was associated with 1.05% (95% CI = 0.19%–1.91%), 1.78% (0.41%–3.16%), and 0.27% (−2.42% to 3.03%) increase in ER visits for total RD, COPD, and asthma, respectively. A study in Hong Kong by Qiu et al. [34] reported a 3.33% (95% CI = 1.54%–5.15%) increase in ER visits for pneumonia per every 10µg/m3 increment of PM2.5–10 in the past 4 days (lag 3). A study in 35 California counties by Malig et al. [35] reported a 10µg/m3 increment in the level of PM2.5–10 was associated with a 3.3% (95% CI = 2.0%–4.6%) increase in ER visits for asthma. In a large U.S. study of 108 counties, a 10µg/m3 increase in coarse PM was associated with a non-statistically significant unadjusted 0.33% (95% CI = −0.21% to 0.86%) increase in RD admissions and with a 0.26% (95% CI = −0.32% to 0.84%) increase in RD admissions when adjusted for PM2.5 on the same day [19]. A study conducted in 8 Southern European cities within the MED-PARTICLES projects, Stafoggia et al. [41] noted an increase of 1.24% (95% CI = −0.2% to 2.82%) in frequency of RD admissions for an IQR increase (6.3 µg/m3) in coarse PM levels at the cumulative lag0–5. In a Toronto, Canada study, Burnett et al. [37] reported a 4.8% (95% CI = 2.1%–7.6%) increase in the risk of RD admissions per 10 µg/m3 increase in PM2.5–10 level. However, significant associations observed for RD admissions, COPD, and respiratory infections in another Toronto study, were not present in gas-adjusted models [38]. In a study conducted in Vancouver, Chen et al. [36] reported a 1.03 (95% CI = 0.98–1.09) increase for the first RD admission, 1.22 (95% CI = 1.01–1.36) for the second RD admission, and 1.06 (95% CI = 1.02–1.11) for overall RD admissions for an increment of 4.2 µg/m3 in PM2.5–10 concentrations. Two studies conducted in the United Kingdom found no evidence of an association between RD admissions and exposure to PM2.5–10 [39,40]. A study in Helsinki by Halonen et al. [24] reported no evidence of positive associations for pneumonia and asthma-COPD with coarse PM. In this study, a 10 µg/m3 increase in PM2.5–10 in the 3-day moving mean concentrations on cool days was associated with a 3% (95% CI = 1%–5%) elevation in number of COPD admissions, 4% (95% CI = 1%–7%) in asthma admissions, and 3% (95% CI = 2%–4%) in pneumonia admissions. Corresponding relationships with a 10 µg/m3 increase in coarse PM in this study were higher than previously observed [33,34,35]. In addition, the association with PM2.5 concentration is almost three times larger than for coarse PM concentration in the two-pollutant model. This finding is consistent with the investigations that also found fine fraction to be correlated with greater risk per unit mass than the coarse fraction [19,24,41]. However, because coarse PM is obtained as the difference between PM10 and PM2.5, it is affected by measurement error from two sources, and the direction and magnitude of the resulting bias in the associations with hospitalizations cannot be predicted [41].
Only in recent years have researchers begun to separately address the adverse health effects attributed to PM2.5–10, because (1) PM2.5–10 were initially considered as potentially less toxic than PM2.5 due to their large size and small surface area to mass ratio and (2) it is only recently that PM2.5 were measured separately [21]. However, PM2.5–10 may plausibly impact health given their deposition in the lungs, high biological content such as organic matter and microbes, and, in urban areas, high content of heavy metals such as Fe and Al [55]. Further, particle agglomerates that are large enough to be in the coarse fraction may contain many ultrafine particles and other attached constituents [21].
Results from toxicological studies showed that, PM2.5–10 and PM2.5 both produce inflammatory effects, including some evidence that PM2.5–10 may be more inflammatory than PM2.5 [56,57,58,59,60,61]. Controlled exposure to concentrated ambient coarse particles can also produce an increase in neutrophils in healthy humans [62,63]. Such inflammatory responses are a major component of asthmatic disease and may incite or exacerbate other respiratory conditions [64,65].
Major PM2.5–10 components vary by region and by season, but typically include Ca, Mg, Al, silicon, and Fe, and primary organic materials such as pollen, spores, and plant and animal debris [11,15,16]. Despite considerable research, the relative toxicity of different constituents of PM2.5–10 remain unclear but likely vary dependent upon the components [60]. The origin of chemical pollutants in an urban atmosphere is known to be predominantly attributed to road traffic [3]. Concentrations in urban environments are generally more influenced by transportation than in rural conditions, in which agriculture, other sources such as unpaved and construction sites, and wind are key influences [11].
In our study, adverse effects were observed only on cool days. It was possible to confirm that observed PM-induced effects varied by season [8,66]. The observed seasonal variation in effect estimates might be explained by variation in exposure patterns. It might be related to the relatively mild winters in Kaohsiung, where the mean monthly temperatures from December to February ranged from 18.8 to 22.1 °C and the mean daily temperature rarely fell below 15 °C. People in Kaohsiung are therefore more likely to go outdoors and open the windows in the cool than warm season (higher exposure). Thus, monitored concentrations of coarse PM may be closer to personal exposure to PM2.5–10 in the cool than warm season (more reliable exposure assessment). This fact may attenuate the PM2.5–10 induced influence in the warm season. On the other hand, seasonal differences in air pollution mixtures may also modify the effect estimates. Air pollution mixtures may include a greater proportion of toxic components during cooler months. Further, compared with other studies in developed countries, our data demonstrated larger effect estimates per unit increase of PM2.5–10. One potential explanation for this discrepancy is that most published investigations only noted straightforward, pooled effect estimates (lack of effect estimates stratified by season). This may mask inherent differences between different climates and air pollution mixtures. Variations in seasonal and regional effect estimates may in part result from differences in the chemical composition of particles [66,67]. Nevertheless, the seasonal pattern of air pollution adverse health effects needs to be further investigated.
The case-crossover study design was proposed by Maclure [42] to examine the influence of transient, intermittent exposures on the subsequent risk of rare acute-onset events in close temporal proximity to exposure. This design offers the ability to control for many confounders by design rather than by statistical modelling. This design is an adaptation of the case-control study in which each case serves as his or her own referent. Therefore, time-invariant subject-specific variables such as gender, age, underlying chronic disease, or other individual-level characteristics do not act as confounders. In addition, the time-stratified approach was found to be effective in controlling for seasonality [47], time trends, chronic, and slowly varying potential confounders [49,50,68].
For a factor to confound the relationship between coarse PM levels and admissions for RD it needs to be correlated with both variables. It is unlikely that time-variant subject-specific variables such as smoking, diet, and other indoor pollutants confounded the present association since these factors either do not vary significantly over time or vary slowly. In addition, there is no reason to believe that daily variations in the individual risk factors are correlated with changes in PM2.5–10 air pollution [69].
As in other studies in this field, we derived daily average levels of PM2.5–10 from outdoor monitoring stations to represent the personal exposure to PM2.5–10. Numerous factors, such as air conditioning and ventilation rate between indoor and outdoor air, may affect the monitoring results from fixed stations as surrogates of personal exposure to PM2.5–10. PM2.5–10 levels typically are more spatially heterogeneous than PM2.5 due to its higher deposition velocities in the atmosphere for these higher mass particles [19,55]. Concentrations of PM have also been shown to vary across space based on proximity to different sources, making exposure assignment especially difficult given the limited numbers of monitoring stations with data to estimate PM2.5–10 [55]. The potential for exposure measurement error in epidemiologic studies based on monitoring stations is likely to be greater for investigating associations of health indicators with PM2.5–10 than PM2.5 [19]. Larger measurement error relative to PM2.5 may be a plausible explanation for weakened associations for PM2.5–10 in this study. Measurements of PM2.5–10 levels are indirect, estimated through subtraction of PM2.5 from PM10 concentrations measured at the same monitoring station in this study. While past investigations deemed this a reliable approach to estimating PM2.5–10 in urban areas [55], there are inherently errors due to the uncertainty of both filters. PM2.5–10 were assigned from fixed, outdoor monitoring stations to individuals to estimate exposure (assuming that exposure was homogeneous encompassing the entire studied area). Exposure measurement errors resulting from differences between the population average exposure and ambient PM2.5–10 levels are unavoidable. However, this type of error may underestimate the true effect of exposure-response association due to the non-differential misclassification of the exposure [51,70].
This study was conducted in a tropical city. These facts may somewhat restrict the generalizability of these findings to other locations with different meteorological and racial characteristics. Further, behavior such as air conditioning usage or time spent outdoors may affect personal exposures. This might modify the magnitude of the observed associations compared with other geographical locations.

Table 1.
Distribution of daily respiratory diseases admissions, weather conditions, and air pollution variables in Kaohsiung, Taiwan, 2006–2010.
| Variable a | Min | Percentile | Max | Mean | ||
|---|---|---|---|---|---|---|
| 25% | 50% | 75% | ||||
| PM10 (μg/m3) | 19.97 | 45.21 | 72.72 | 104.24 | 607.14 | 77.53 |
| PM2.5 (μg/m3) | 11.44 | 25.57 | 44.30 | 61.88 | 144.37 | 45.88 |
| PM2.5–10(μg/m3) | 4.95 | 17.63 | 27.87 | 42.07 | 489.56 | 31.65 |
| SO2 (ppb) | 1.91 | 6.02 | 7.49 | 9.20 | 22.45 | 7.80 |
| NO2 (ppb) | 4.45 | 15.45 | 21.69 | 28.81 | 53.11 | 22.31 |
| CO (ppm) | 0.13 | 0.41 | 0.56 | 0.71 | 1.34 | 0.57 |
| O3 (ppb) | 4.77 | 18.90 | 27.92 | 37.19 | 72.96 | 29.14 |
| Temperature(°C) | 12.88 | 22.65 | 26.81 | 29.08 | 32.21 | 25.68 |
| Humidity (%) | 40.35 | 68.15 | 72.30 | 75.94 | 93.55 | 72.10 |
| Hospital admissions | ||||||
| COPD | 0 | 5 | 7 | 10 | 25 | 7.74 |
| Asthma | 0 | 1 | 3 | 4 | 12 | 2.86 |
| Pneumonia | 0 | 27 | 34 | 40 | 73 | 34.22 |
Abbreviation: Min, minimum value; Max, maximum value. a 24-hr average.

Table 2.
Correlation coefficients among air pollutants.
| Variable | PM2.5 | PM2.5–10 | SO2 | NO2 | CO | O3 |
|---|---|---|---|---|---|---|
| PM10 | 0.92 * | 0.89 * | 0.25 * | 0.74 * | 0.72 * | 0.37 * |
| PM2.5 | - | 0.64 * | 0.25 * | 0.80 * | 0.81 * | 0.42 * |
| PM2.5–10 | - | - | 0.19 | 0.53 * | 0.47 * | 0.24 * |
| SO2 | - | - | 1.0 | 0.40 * | 0.40 * | −0.02 |
| NO2 | - | - | - | 1.0 | 0.93 * | 0.11 |
| CO | - | - | - | - | 1.0 | 0.14 |
| O3 | - | - | - | - | - | 1.0 |
* p < 0.05.

Table 3.
Percent increase (95% CI) of hospital admissions for respiratory diseases associated with a 10 μg/m3 increase of particulate matter in Kaohsiung, Taiwan, 2006–2010.
| Temperature | PM2.5 | PM2.5-10 | PM10 |
|---|---|---|---|
| ≥ 25 °C (1125 days) | |||
| COPD | |||
| Without adjustment a | 1.00 (0.98–1.03) | 1.02 (1.00–1.03) | 1.01 (1.00–1.02) |
| Adjusted for SO2 | 1.00 (0.98–1.02) | 1.02 (1.00–1.03) | 1.01 (1.00–1.02) |
| Adjusted for NO2 | 0.98 (0.95–1.00) | 1.01 (1.00–1.03) | 1.00 (0.99–1.01) |
| Adjusted for CO | 0.96 (0.93–0.99) | 1.01 (1.00–1.03) | 1.00 (0.99–1.01) |
| Adjusted for O3 | 0.93 (0.90–0.96) | 1.01 (0.99–1.03) | 0.99 (0.98–1.00) |
| Asthma | |||
| Without adjustment a | 1.02 (0.98–1.06) | 1.02 (1.00–1.05) | 1.02 (1.00–1.04) |
| Adjusted for SO2 | 1.02 (0.98–1.06) | 1.02 (0.99–1.05) | 1.01 (1.00–1.03) |
| Adjusted for NO2 | 0.99 (0.95–1.04) | 1.02 (0.99–1.04) | 1.01 (0.99–1.03) |
| Adjusted for CO | 0.97 (0.93–1.02) | 1.02 (0.99–1.04) | 1.00 (0.98–1.03) |
| Adjusted for O3 | 0.95 (0.91–1.00) | 1.01 (0.99–1.04) | 1.00 (0.98–1.02) |
| Pneumonia | |||
| Without adjustment a | 1.00 (0.99–1.01) | 1.02 (1.01–1.03) | 1.01 (1.01–1.02) |
| Adjusted for SO2 | 1.00 (0.99–1.01) | 1.02 (1.01–1.03) | 1.01 (1.01–1.02) |
| Adjusted for NO2 | 0.97 (0.96–0.99) | 1.02 (1.01–1.02) | 1.00 (1.00–1.01) |
| Adjusted for CO | 0.95 (0.94–0.97) | 1.02 (1.01–1.02) | 1.00 (0.99–1.01) |
| Adjusted for O3 | 0.93 (0.92–0.94) | 1.01 (1.01–1.02) | 0.99 (0.99–1.00) |
| < 25 °C (701 days) | |||
| COPD | |||
| Without adjustment a | 1.11 (1.09–1.13) | 1.03 (1.01–1.05) | 1.05 (1.03–1.06) |
| Adjusted for SO2 | 1.13 (1.11–1.16) | 1.03 (1.02–1.05) | 1.05 (1.04–1.06) |
| Adjusted for NO2 | 1.06 (1.03–1.09) | 1.02 (1.00–1.04) | 1.02 (1.01–1.04) |
| Adjusted for CO | 1.05 (1.02–1.08) | 1.02 (1.00–1.03) | 1.02 (1.01–1.03) |
| Adjusted for O3 | 1.09 (1.07–1.12) | 1.03 (1.01–1.04) | 1.04 (1.03–1.05) |
| Asthma | |||
| Without adjustment a | 1.10 (1.06–1.13) | 1.04 (1.01–1.07) | 1.04 (1.03–1.06) |
| Adjusted for SO2 | 1.12 (1.08–1.16) | 1.04 (1.01–1.07) | 1.05 (1.03–1.07) |
| Adjusted for NO2 | 1.05 (1.00–1.09) | 1.02 (0.99–1.05) | 1.02 (1.00–1.04) |
| Adjusted for CO | 1.04 (0.99–1.09) | 1.02 (0.99–1.05) | 1.02 (1.00–1.04) |
| Adjusted for O3 | 1.08 (1.05–1.12) | 1.03 (1.00–1.06) | 1.04 (1.02–1.06) |
| Pneumonia | |||
| Without adjustment a | 1.12 (1.11–1.13) | 1.03 (1.02–1.04) | 1.05 (1.04–1.05) |
| Adjusted for SO2 | 1.14 (1.13–1.15) | 1.03 (1.03–1.04) | 1.05 (1.05–1.06) |
| Adjusted for NO2 | 1.07 (1.06–1.08) | 1.02 (1.01–1.02) | 1.02 (1.02–1.03) |
| Adjusted for CO | 1.06 (1.05–1.08) | 1.01 (1.01–1.02) | 1.02 (1.01–1.03) |
| Adjusted for O3 | 1.10 (1.09–1.11) | 1.03 (1.02–1.03) | 1.04 (1.03–1.04) |
a single pollutant model.
4. Conclusions
In summary, this study provided evidence of associations between short-term exposure to coarse PM and increased risk of rate of hospital admissions for RD. Associations were much more pronounced during the cool period. These findings reinforce the possible role of PM2.5–10 on the number of hospital admissions for RD.
Acknowledgments
This study is based in part on data from the National Insurance Research Database provided by the Bureau of National Health Insurance, Department of Health and managed by National Health Research Institutes. The interpretation and conclusions contained herein do not represent those of Bureau of National Health Insurance, Department of Health or National Health Research Institutes. This study was supported by National Health Research Institutes (EO-104-PP-08) and National Science Council (NSC-102-2314-B-037-065-MY2).
Author Contributions
Meng-Hsuan Cheng wrote the manuscript. Hui-Fen Chiu provided essential insight into the interpretation of the results. Chun-Yuh Yang contributed to study design and interpretation of the data.
Conflicts of Interest
The authors declare no conflict of interest.
References
- Brunekreef, B.; Holgate, S.T. Air pollution and health. Lancet 2002, 360, 1233–1242. [Google Scholar] [CrossRef]
- Samet, J.; Krewski, D. Health effects associated with exposure to ambient air pollution. J. Toxicol. Environ. Health A 2007, 70, 227–242. [Google Scholar] [CrossRef] [PubMed]
- Beckerman, B.S.; Jerrett, M.; Finkelstein, M.; Kanaroglou, P.; Brook, J.R.; Arain, M.A.; Sears, M.R.; Stieb, D.; Balmes, J.; Chapman, K. The association between chronic exposure to traffic-related air pollution and ischemic heart disease. J. Toxicol. Environ. Health Part A 2012, 75, 402–411. [Google Scholar] [CrossRef] [PubMed]
- Costa, S.; Ferreira, J.; Silveira, C.; Costa, C.; Lopes, D.; Relvas, H.; Borrego, C.; Roebeling, P.; Miranda, A.I.; Teixeira, J.P. Integrating health on air quality assessment—Review report on health risks of two major European outdoor air pollutants: PM and NO2. J. Toxicol. Environ. Health Part B 2014, 17, 307–340. [Google Scholar] [CrossRef] [PubMed]
- Tsai, S.S.; Chiu, H.F.; Liou, S.H.; Yang, C.Y. Short-term effects of fine particulate air pollution on hospital admissions for respiratory diseases: A case-crossover study in a tropical city. J. Toxicol. Environ. Health Part A 2014, 77, 1091–1101. [Google Scholar] [CrossRef] [PubMed]
- Cifuentes, L.A.; Vega, J.; Kopfer, K.; Lave, L.B. Effect of the fine fraction of particulate matter versus the coarse mass and other pollutants on daily nortality in Santiago Chile. J. Air Waste Manage. Assoc. 2000, 50, 1287–1298. [Google Scholar] [CrossRef]
- Schwartz, J.; Dockery, D.W.; Neas, L.M. Is daily mortality associated specifically with fine particles? J. Air Waste Manage. Assoc. 1996, 46, 927–939. [Google Scholar] [CrossRef]
- Zanobetti, A.; Franklin, M.; Koutrakis, P.; Schwartz, J. Fine particulate air pollution and its components in association with cause-specific emergency admissions. Environ. Health 2009, 8. [Google Scholar] [CrossRef] [PubMed]
- Liao, D.; Shaffer, M.L.; He, F.; Rodriguez-Colon, S.; Eu, R.; Whitsel, E.A.; Bixler, E.O.; Cascio, W.E. Fine particulate air pollution is associated with higher vulnerability to atrial fibrillation-The APACR study. J. Toxicol. Environ. Health A 2011, 74, 693–705. [Google Scholar] [CrossRef] [PubMed]
- Chang, C.C.; Chen, P.S.; Yang, C.Y. Short-term effects of fine particulate air pollution on hospital admissions for cardiovascular diseases: A case-crossover study in a tropical city. J. Toxicol. Environ. Health Part A 2015, 78, 267–277. [Google Scholar] [CrossRef] [PubMed]
- Wilson, W.E.; Suh, H.H. Fine particles and coarse particles: Concentration relationship relevant to epidemiologic studies. J. Air Waste Manage. Assoc. 1997, 47, 1238–1249. [Google Scholar] [CrossRef]
- Dominici, F.; Peng, R.D.; Bell, M.L.; Pham, L.; McDermott, A.; Zeger, S.L.; Samet, J.M. Fine particulate air pollution and hospital admission for cardiovascular and respiratory diseases. J. Am. Med. Assoc. 2006, 295, 1127–1134. [Google Scholar] [CrossRef] [PubMed]
- Pope, C.A.; Dockery, D.W. Health effects of fine particulate air pollution: Lines that connect. J. Air Waste Manage. Assoc. 2006, 36, 709–742. [Google Scholar]
- Brunekreef, B.; Forsberg, B. Epidemiological evidence of effects of coarse airborne particles on health. Eur. Respir. J. 2005, 26, 309–318. [Google Scholar] [CrossRef] [PubMed]
- Fang, G.C.; Chang, C.N.; Wu, Y.S.; Wang, V.; Fu, P.P.; Yang, D.G. The study of fine and coarse particles, and metallic elements for the daytime and night time in a suburban area of central Taiwan, Taichung. Chemosphere 2000, 41, 639–644. [Google Scholar] [CrossRef]
- Wang, H.; Shooter, D. Source apportionment of fine and coarse atmospheric particles in Auckland, New Zealand. Sci. Total Environ. 2005, 340, 189–198. [Google Scholar] [CrossRef] [PubMed]
- Peng, R.D.; Bell, M.L.; Geyh, A.S.; McDermott, A.; Zeger, S.L.; Samet, J.M.; Dominici, F. Emergency admissions for cardiovascular and respiratory diseases and the chemical composition of fine particle air pollution. Environ. Health Perspect. 2009, 117, 957–963. [Google Scholar] [CrossRef] [PubMed]
- Suh, H.H.; Zanobetti, A.; Schwartz, J.; Coull, B.A. Chemical properties of air pollutants and cause-specific hospital admissions among the elderly in Atlanta, Georgia. Environ. Health Perspect. 2011, 119, 1421–1428. [Google Scholar] [CrossRef] [PubMed]
- Peng, R.D.; Chang, H.H.; Bell, M.L.; McDermott, A.; Zeger, S.L.; Samet, J.M.; Dominici, F. Coarse particulate matter air pollution and hospital admissions for cardiovascular and respiratory diseases among medicare patients. J. Am. Med. Assoc. 2008, 299, 2172–2179. [Google Scholar] [CrossRef] [PubMed]
- Zanobetti, A.; Schwartz, J. Air pollution and emergency admissions in Boston, MA. J. Epidemiol. Community Health 2006, 60, 890–895. [Google Scholar] [CrossRef] [PubMed]
- Host, S.; Larrieu, S.; Pascal, L.; Blanchard, M.; Declercq, C.; Fabre, P.; Jusot, J.F.; Chardon, B.; Le Tertre, A.; Wagner, V.; Prouvost, H.; Lefrance, A. Short-term associations between fine and coarse particles and hospital admissions for cardiorespiratory diseases in six French cities. Occup. Environ. Med. 2008, 65, 544–551. [Google Scholar] [CrossRef] [PubMed]
- Belleudi, V.; Faustini, A.; Stafoggia, M.; Cattani, G.; Marconi, A.; Perucci, C.A.; Forastiere, F. Impact of fine and ultrafine particles on emergency hospital admissions for cardiac and respiratory diseaes. Epidemiology 2010, 21, 414–423. [Google Scholar] [CrossRef] [PubMed]
- Halonen, J.I.; Lanki, T.; Yli-Tuomi, T.; Kulmala, M.; Tiittanen, P.; Pekkanen, J. Urban air pollution and asthma and COPD hospital emergency room visits. Thorax 2008, 63, 635–641. [Google Scholar] [CrossRef] [PubMed]
- Halonen, J.I.; Lanki, T.; Yli-Tuomi, T.; Tiittanen, P.; Kulmala, M.; Pekkanen, J. Particulate air pollution and acute cardiorespiratory hospital admissions and mortality among the elderly. Epidemiology 2009, 20, 143–153. [Google Scholar] [CrossRef] [PubMed]
- Andersen, Z.J.; Wahlin, P.; Raaschou-Nielsen, O.; Ketzel, M.; Scheike, T.; Loft, S. Size distribution and total number concentration of ultrafine and accumulation mode particles and hospital admissions in children and the elderly in Copenhagen, Denmark. Occup. Environ. Med. 2008, 65, 458–466. [Google Scholar] [CrossRef] [PubMed]
- Tecer, L.H.; Alagha, O.; Karaca, F.; Tuncel, G.; Eldes, N. Particulate matter (PM2.5, PM2.5–10, and PM10) and children’s hospital admissions for asthma and respiratory diseases: A bidirectional case-crossover study. J. Toxicol. Environ. Health A 2008, 71, 515–520. [Google Scholar]
- Stieb, D.M.; Szyszkowicz, M.; Rowe, B.H.; Leech, J.A. Air pollution and emergency department visits for cardiac and respiratory conditions: A multi-city time-series analysis. Environ. Health 2009, 8. [Google Scholar] [CrossRef] [PubMed]
- Silverman, R.A.; Ito, K. Age-related association of fine particles and ozone with severe acute asthma in New York city. J. Allergy Clin. Immunol. 2010, 125, 367–373. [Google Scholar] [CrossRef] [PubMed]
- Iskandar, A.; Andersen, Z.J.; Bonnelykke, K.; Ellermann, T.; Andersen, K.K.; Bisgaard, H. Coarse and fine particles but not ultrafine particles in urban air trigger hospital admissions for asthma in children. Thorax 2012, 67, 252–257. [Google Scholar] [CrossRef] [PubMed]
- Tsai, S.S.; Yang, C.Y. Fine particulate air pollution and hospital hospital admissions forpneumonia in a subtropical city: Taipei, Taiwan. J. Toxicol. Environ. Health Part A 2014, 77, 192–201. [Google Scholar] [CrossRef] [PubMed]
- Tsai, S.S.; Chang, C.C.; Yang, C.Y. Fine particulate air pollution and hospital admissions for chronic obstructive pulmonary disease: A case-crossover study in Taipei. Int. J. Environ. Res. Public Health 2013, 10, 6015–6026. [Google Scholar] [CrossRef] [PubMed]
- Cheng, M.H.; Chen, C.C.; Chiu, H.F.; Yang, C.Y. Fine particulate air pollution and hospital hospital admissions for asthma: A case-crossover study in Taipei. J. Toxicol. Environ. Health Part A 2014, 77, 1075–1083. [Google Scholar] [CrossRef] [PubMed]
- Qiu, H.; Yu, T.S.; Tian, L.W.; Wang, X.; Tse, L.A.; Tam, W.; Wong, T.W. Effects of coarse particulate matter on emergency hospital admissions for respiratory diseases: A time-series analysis in Hong Kong. Environ. Health Perspect. 2012, 120, 572–576. [Google Scholar] [CrossRef] [PubMed]
- Qiu, H.; Tian, L.W.; Pun, V.C.; Wong, T.W.; Yu, T.S. Coarse particulate matter associated with increased risk of emergency hospital admissions for pneumonia in Hong Kong. Thorax 2014, 69, 1027–1033. [Google Scholar] [CrossRef] [PubMed]
- Malig, B.J.; Green, S.; Basu, R.; Broadwin, R. Coarse particles and respiratory emergency department visits in California. Am. J. Epidemiol. 2013, 178, 58–69. [Google Scholar] [CrossRef] [PubMed]
- Chen, Y.; Yang, Q.; Krewski, D.; Burnett, R.T.; Shi, Y.; McGrail, K.M. The effect of coarse ambient particulate matter on first, second, and overall hospital admissions for respiratory disease among the elderly. Inhal. Toxicol. 2005, 17, 649–655. [Google Scholar] [CrossRef] [PubMed]
- Burnett, R.T.; Cakmak, S.; Brook, J.R.; Krewski, D. The role of particulate size and chemistry in the association between summertime ambient air pollution and hospitalization for cardiorespiratory diseases. Environ. Health Perspect. 1997, 105, 614–620. [Google Scholar] [CrossRef] [PubMed]
- Burnett, R.T.; Smith-Doiron, M.; Stieb, D.; Cakmak, S.; Brook, J.R. Effects of particulate and gaseous air pollution on cardiorespiratory hospitalizations. Arch. Environ. Health 1999, 54, 130–139. [Google Scholar] [CrossRef] [PubMed]
- Anderson, H.R.; Bremner, S.A.; Atkinson, R.W.; Harrison, R.M.; Walters, S. Particulate matter and daily mortality and hospital admissions in the west midlands conurbation of the United Kingdom: Association with fine and coarse particles, black smoke and sulphate. Occup. Environ. Med. 2001, 58, 504–510. [Google Scholar] [CrossRef] [PubMed]
- Atkinson, R.W.; Fuller, G.W.; Anderson, H.R.; Harrison, R.M.; Armstrong, B. Urban ambient particle metrics and health: A time-series analysis. Epidemiology 2010, 21, 501–511. [Google Scholar] [CrossRef] [PubMed]
- Stafoggia, M.; Samoli, E.; Alessandrini, E.; Cadum, E.; Ostro, B.; Berti, G.; Faustini, A.; Jacquemin, B.; Linares, C.; Pascal, M.; Randi, G.; Ranzi, A.; Stivanello, E.; Forastiere, F. Short-term associations between fine and coarse particulate matter and hospitalizations in southern Europe: Results from the MED-PARTICLES project. Environ. Health Perspect. 2013, 121, 1026–1033. [Google Scholar] [CrossRef] [PubMed]
- Maclure, M. The case-crossover design: A method for studying transient effects on the risk of acute events. Am. J. Epidemiol. 1991, 133, 144–153. [Google Scholar] [PubMed]
- Marshall, R.J.; Jackson, R.T. Analysis of case-crossover designs. Stat. Med. 1993, 12, 2333–2341. [Google Scholar] [CrossRef] [PubMed]
- Mittleman, M.A.; Maclure, M.; Robins, J.M. Control sampling strategies for case-crossover studies: An assessment of relative efficiency. Am. J. Epidemiol. 1995, 142, 91–98. [Google Scholar] [PubMed]
- Neas, L.N.; Schwartz, J.; Dockery, D. A case-crossover analysis of air pollution and mortality in Philadelphia. Environ. Health Perspect. 1999, 107, 629–631. [Google Scholar] [CrossRef] [PubMed]
- Lee, J.T.; Schwartz, J. Reanalysis of the effects of air pollution on daily mortality in Seoul, Korea: A case-crossover design. Environ. Health Perspect. 1999, 107, 633–636. [Google Scholar] [CrossRef] [PubMed]
- Levy, D.; Lumley, T.; Sheppard, L.; Kaufman, J.; Checkoway, H. Referent selection in case-crossover analyses of acute health effects of air pollution. Epidemiology 2001, 12, 186–192. [Google Scholar] [CrossRef] [PubMed]
- Levy, J.I.; Hammitt, J.K.; Spengler, J.D. Estimating the mortality impacts of particulate matter: What can be learned from between-study variability? Environ. Health Perspect. 2000, 108, 109–117. [Google Scholar] [CrossRef] [PubMed]
- Janes, H.; Sheppard, L.; Lumley, T. Case-crossover analyses of air pollution exposure data: Referent selection strategies and their implications for bias. Epidemiology 2005, 16, 717–726. [Google Scholar] [CrossRef] [PubMed]
- Mittleman, M.A. Optimal referent selection strategies in case-crossover studies: A settled issue. Epidemiology 2005, 16, 15–16. [Google Scholar] [CrossRef]
- Katsouyanni, K.; Touloumi, G.; Spix, C.; Schwartz, J.; Balducci, F.; Medina, S.; Rossi, G.; Wojtyniak, B.; Sunyer, J.; Bacharova, L.; Schouten, J.P.; Ponka, A.; Anderson, H.R. Short term effects of ambient sulphur dioxide and particulate matter on mortality in 12 European cities: Results from time series data from the APHEA project. Br. Med. J. 1997, 314, 1658–1663. [Google Scholar] [CrossRef]
- Tsai, S.S.; Huang, C.H.; Goggins, W.B.; Wu, T.N.; Yang, C.Y. Relationship between air pollution and daily mortality in a tropical city: Kaohsiung, Taiwan. J. Toxicol. Environ. Health A 2003, 66, 1341–1349. [Google Scholar] [CrossRef] [PubMed]
- Yang, C.Y.; Chen, Y.S.; Yang, C.H.; Ho, S.C. Relationship between ambient air pollution and hospital admissions for cardiovascular diseases in Kaohsiung, Taiwan. J. Toxicol. Environ. Health A 2004, 67, 483–493. [Google Scholar] [CrossRef] [PubMed]
- Dockery, D.W.; Pope, C.A. An association between air pollution and mortality in six U.S. cities. N. Engl. J. Med. 1994, 329, 1753–1759. [Google Scholar] [CrossRef] [PubMed]
- Adar, S.D.; Filigrana, P.A.; Clements, N.; Peel, J.L. Ambient coarse particulate matter and human health: A systematic review and meta-analysis. Curr. Environ. Health Rep. 2014, 1, 258–274. [Google Scholar] [CrossRef] [PubMed]
- Schins, R.P.; Lightbody, J.H.; Borm, P.J.; Shi, T.M.; Donaldson, K.; Stone, V. Inflammatory effects of coarse and fine particulate matter in relation to chemical and biological constituents. Toxicol. Appl. Pharmacol. 2004, 195, 1–11. [Google Scholar] [CrossRef] [PubMed]
- Becker, S.; Soukup, J.M.; Sioutas, C.; Cassee, F.R. Response of human alveolar macrophages to ultrafine, fine, and coarse urban air pollution particles. Exp. Lung Res. 2003, 29, 29–44. [Google Scholar] [CrossRef] [PubMed]
- Happo, M.S.; Salonen, R.O.; Halinen, A.I.; Jalava, P.I.; Pennanen, A.S.; Kosma, V.M.; Sillanpaa, M.; Hillamo, R.; Brunekreef, B.; Katasouyanni, K.; Sunyer, J.; Hirvonen, M.R. Dose and time dependency of inflammatory responses in the mouse lung to urban air coarse, fine, and ultrafine particles from six European cities. Inhal. Toxicol. 2007, 19, 227–246. [Google Scholar] [CrossRef] [PubMed]
- Wegesser, T.C.; Last, J.A. Lung response to coarse PM: bioassay in mice. Toxicol. Appl. Pharmacol. 2008, 230, 159–166. [Google Scholar] [CrossRef] [PubMed]
- Ghio, A.J.; Carraway, M.S.; Madden, M.C. Composition of air pollution particles and oxidative stress in cells, tissues, and living systems. J. Toxicol. Environ. Health Part B 2012, 15, 1–21. [Google Scholar] [CrossRef] [PubMed]
- Amatullah, H.; North, M.L.; Akhtar, U.S.; Rastogi, N.; Urch, B.; Silverman, F.S.; Chow, C.W.; Evans, G.J.; Scott, J.A. Comparative cardiopulmonary effects of size-fractionated airborne particulate matter. Inhal. Toxicol. 2012, 24, 161–171. [Google Scholar] [CrossRef] [PubMed]
- Alexis, N.E.; Lay, J.C.; Zeman, K.; Bennett, W.E.; Peden, D.B.; Soukup, J.M.; Devlin, R.B.; Becker, S. Biological material on inhaled coarse fraction particulate matter activates airway phagocytes in vivo in healthy volunteers. J. Allergy Clin. Immunol. 2006, 117, 1396–1403. [Google Scholar] [CrossRef] [PubMed]
- Graff, D.W.; Cascio, W.E.; Rappold, A.; Zhou, H.B.; Huang, Y.C.; Delvin, R.B. Exposure to concentrated coarse air pollution particles causes mild cardiopulmonary effects in healthy young adults. Environ. Health Perspect. 2009, 117, 1089–1094. [Google Scholar] [CrossRef] [PubMed]
- Barbato., A.; Turato, G.; Baraldo, S.; Bazzan, E.; Calabrese, F.; Tura, M.; Zuin, R.; Beghe, B.; Maestrelli, P.; Fabbri, L.M.; Saetta, M. Airway inflammation in childhood asthma. Am. J. Respir. Crit. Care Med. 2003, 168, 798–803. [Google Scholar] [CrossRef] [PubMed]
- Brussel, G.G.; Joos, G.F.; Bracke, K.R. Chronic obstructive pulmonary disease 1. New insights into the immunology of chronic obstructive pulmonary disease. Lancet 2011, 378, 1015–1026. [Google Scholar] [CrossRef]
- Bell, M.L.; Ebisu, K.; Peng, R.D.; Walker, J.; Samet, J.M.; Zeger, S.L.; Dominici, F. Seasonal and regional short-term effects of fine particles on hospital admissions in 202 US counties, 1999–2005. Am. J. Epidemiol. 2008, 168, 1301–1310. [Google Scholar] [CrossRef] [PubMed]
- Zeka, A.; Zanobetti, A.; Schwartz, J. Individual-level modifiers of the effects of particulate matter on daily mortality. Am. J. Epidemiol. 2006, 163, 849–859. [Google Scholar] [CrossRef] [PubMed]
- Lumley, T.; Levy, D. Bias in the case-crossover design: Implications for studies of air pollution. Environmetrics 2000, 11, 689–704. [Google Scholar] [CrossRef]
- Schwartz, J.; Marcus, A. Mortality and air pollution in London: A time series analysis. Am. J. Epidemiol. 1990, 131, 185–194. [Google Scholar] [PubMed]
- Zeger, S.L.; Thomas, D.; Dominici, F.; Samet, J.M.; Schwartz, J.; Dockery, D.; Cohen, A. Exposure measurement error in time-series studies of air pollution: Concepts and consequences. Environ. Health Perspect. 2000, 108, 419–426. [Google Scholar] [CrossRef] [PubMed]
© 2015 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/4.0/).
