Pelvic Floor Muscle Training for Urinary Incontinence with or without Biofeedback or Electrostimulation in Women: A Systematic Review
Abstract
:1. Introduction
2. Material and Method
2.1. Search Strategy
2.2. Study Selection and Criteria
2.3. Data Extraction, Quality Assessment, Data Synthesis
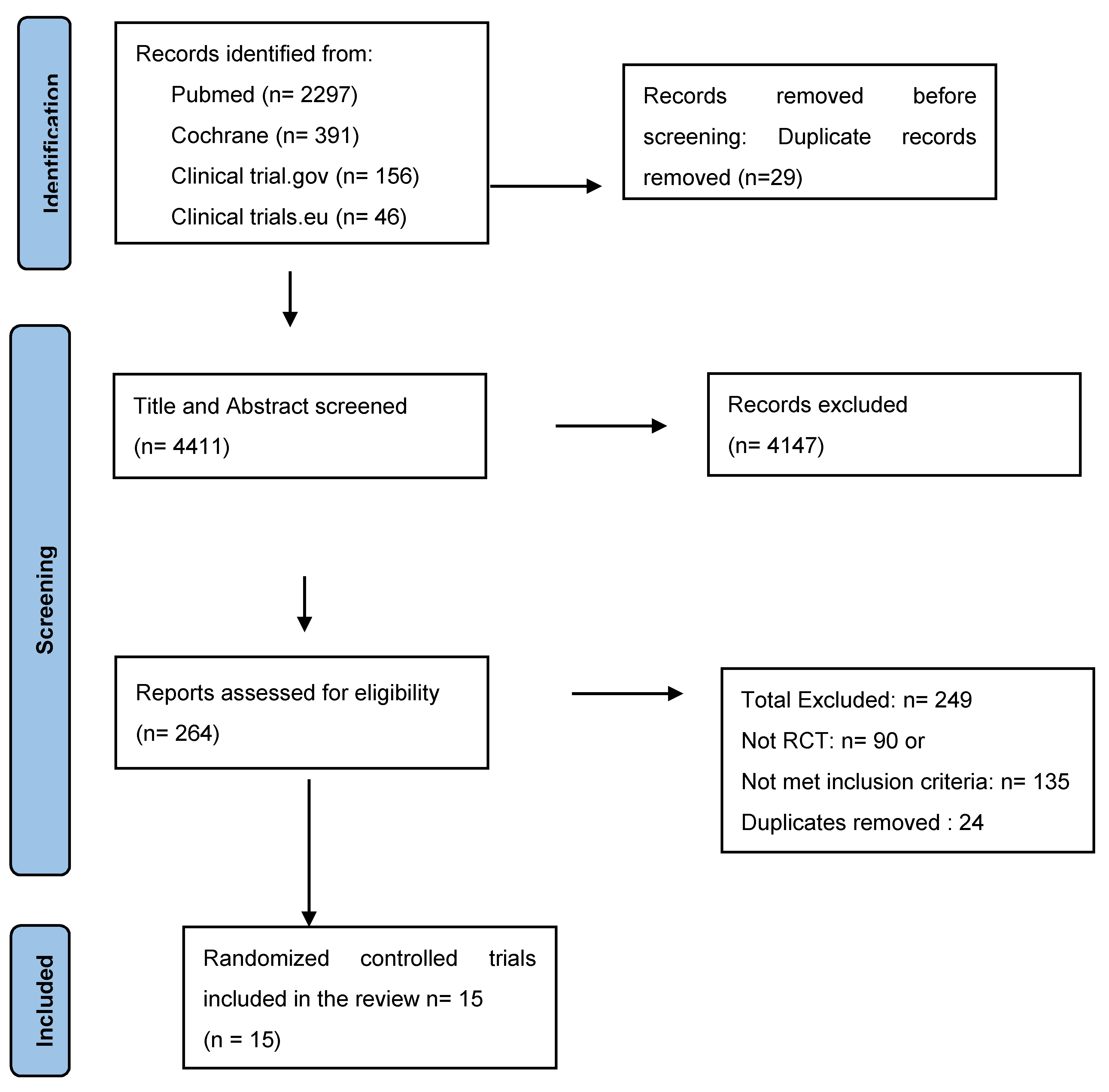
3. Results
Study Selection
4. Narrative Synthesis
4.1. Study and Population Characteristics
4.2. Overall Quality and Risk of Bias Assessing of Studies
4.3. Study Outcome
4.4. Sensitivity and Subgroup Synthesis
5. Discussion
Strengths and Limitations of the Study
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Weber-Rajek, M.; Strączyńska, A.; Strojek, K.; Piekorz, Z.; Pilarska, B.; Podhorecka, M.; Sobieralska-Michalak, K.; Goch, A.; Radzimińska, A. Assessment of the Effectiveness of Pelvic Floor Muscle Training (PFMT) and Extracorporeal Magnetic Innervation (ExMI) in Treatment of Stress Urinary Incontinence in Women: A Randomized Controlled Trial. BioMed Res. Int. 2020, 2020, 1019872. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Leong, B.S.; Mok, N.W. Effectiveness of a new standardized Urinary Continence Physiotherapy Program for community-dwelling older women in Hong Kong. Hong Kong Med. J. 2015, 21, 30–37. [Google Scholar] [PubMed]
- Castro, R.A.; Arruda, R.M.; Zanetti, M.R.D.; Santos, P.D.; Sartori, M.G.F.; Girão, M.J.B.C. Single-blind, randomized, controlled trial of pelvic floor muscle training, electrical stimulation, vaginal cones, and no active treatment in the management of stress urinary incontinence. Clinics 2008, 63, 465–472. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Åhlund, S.; Nordgren, B.; Wilander, E.-L.; Wiklund, I.; Fridén, C. Is home-based pelvic floor muscle training effective in treatment of urinary incontinence after birth in primiparous women? A randomized controlled trial. Acta Obstet. Et Gynecol. Scand. 2013, 92, 909–915. [Google Scholar] [CrossRef]
- Pereira, V.S.; De Melo, M.V.; Correia, G.N.; Driusso, P. Long-term effects of pelvic floor muscle training with vaginal cone in post-menopausal women with urinary incontinence: A randomized controlled trial. Neurourol. Urodyn. 2012, 32, 48–52. [Google Scholar] [CrossRef]
- Luginbuehl, H.; Lehmann, C.; Koenig, I.; Kuhn, A.; Buergin, R.; Radlinger, L. Involuntary reflexive pelvic floor muscle training in addition to standard training versus standard training alone for women with stress urinary incontinence: A randomized controlled trial. Int. Urogynecology J. 2021, 1–10. [Google Scholar] [CrossRef]
- Kargar Jahromi, M.; Talebizadeh, M.; Mirzaei, M. The effect of pelvic muscle exercises on urinary incontinency and self-esteem of elderly females with stress urinary incontinency, 2013. Glob. J. Health Sci. 2014, 7, 71–79. [Google Scholar] [CrossRef] [Green Version]
- Gameiro, M.O.; Moreira, E.H.; Gameiro, F.O.; Moreno, J.C.; Padovani, C.R.; Amaro, J.L. Vaginal weight cone versus assisted pelvic floor muscle training in the treatment of female urinary incontinence. A prospective, single-blind, randomized trial. Int. Urogynecology J. 2010, 21, 395–399. [Google Scholar] [CrossRef]
- Farzinmehr, A.; Moezy, A.; Koohpayehzadeh, J.; Kashanian, M. A comparative study of whole-body vibration training and pelvic floor muscle training on women’s stress urinary incontinence: Three-month follow-up. J. Fam. Reprod. Health 2015, 9, 147. [Google Scholar]
- Dumoulin, C.; Lemieux, M.-C.; Bourbonnais, D.; Gravel, D.; Bravo, G.; Morin, M. Physiotherapy for Persistent Postnatal Stress Urinary Incontinence: A Randomized Controlled Trial. Obstet. Gynecol. 2004, 104, 504–510. [Google Scholar] [CrossRef] [Green Version]
- Hagen, S.; Elders, A.; Stratton, S.; Sergenson, N.; Bugge, C.; Dean, S.; Hay-Smith, J.; Kilonzo, M.; Dimitrova, M.; Abdel-Fattah, M.; et al. Effectiveness of pelvic floor muscle training with and without electromyographic biofeedback for urinary incontinence in women: Multicentre randomised controlled trial. BMJ 2020, 371, m3719. [Google Scholar] [CrossRef]
- Bø, K.; Talseth, T.; Vinsnes, A. Randomized controlled trial on the effect of pelvic floor muscle training on quality of life and sexual problems in genuine stress incontinent women. Acta Obstet Gynecol Scand. 2000, 4, 598–603. [Google Scholar]
- McLean, L.; Varette, K.; Gentilcore-Saulnier, E.; Harvey, M.-A.; Baker, K.; Sauerbrei, E. Pelvic floor muscle training in women with stress urinary incontinence causes hypertrophy of the urethral sphincters and reduces bladder neck mobility during coughing. Neurourol. Urodyn. 2013, 32, 1096–1102. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Wagg, A.; Chowdhury, Z.; Galarneau, J.-M.; Haque, R.; Kabir, F.; MacDonald, D.; Naher, K.; Yasui, Y.; Cherry, N. Exercise intervention in the management of urinary incontinence in older women in villages in Bangladesh: A cluster randomised trial. Lancet Glob. Health 2019, 7, e923–e931. [Google Scholar] [CrossRef] [Green Version]
- Dumoulin, C.; Morin, M.; Danieli, C.; Cacciari, L.; Mayrand, M.-H.; Tousignant, M.; Abrahamowicz, M.; Urinary Incontinence and Aging Study Group. Group-Based vs. Individual Pelvic Floor Muscle Training to Treat Urinary Incontinence in Older Women: A Randomized Clinical Trial. JAMA Intern. Med. 2020, 180, 1284–1293. [Google Scholar] [CrossRef]
- Gumussoy, S.; Kavlak, O.; Yeniel, A.O. Effects of Biofeedback-Guided Pelvic Floor Muscle Training with and without Extracorporeal Magnetic Innervation Therapy on Stress Incontinence: A Randomized Controlled Trial. J. Wound Ostomy Cont. Nurs. 2021, 48, 153–161. [Google Scholar] [CrossRef]
- Dumoulin, C.; Cacciari, L.P.; Hay-Smith, E.J.C. Pelvic floor muscle training versus no treatment, or inactive control treatments, for urinary incontinence in women (Review). Cochrane Database Syst. Rev. 2018, 10, CD005654. [Google Scholar]
- Bø, K.; Talseth, T.; Holme, I. Single blind, randomised controlled trial of pelvic floor exercises, electrical stimulation, vaginal cones, and no treatment in management of genuine stress incontinence in women. BMJ 1999, 318, 487–493. [Google Scholar] [CrossRef] [Green Version]
- Brennen, R.; Frawley, H.C.; Martin, J.; Haines, T.P. Group-based pelvic floor muscle training for all women during pregnancy is more cost-effective than postnatal training for women with urinary incontinence: Cost-effectiveness analysis of a systematic review. J. Physiother. 2021, 67, 105–114. [Google Scholar] [CrossRef]
- Radzimińska, A.; Strączyńska, A.; Weber-Rajek, M.; Styczyńska, H.; Strojek, K.; Piekorz, Z. The impact of pelvic floor muscle training on the quality of life of women with urinary incontinence: A systematic literature review. Clin. Interv. Aging. 2018, 13, 957–965. [Google Scholar] [CrossRef] [Green Version]
- Ayeleke, R.O.; Hay-Smith, E.J.C.; Omar, M.I. Pelvic floor muscle training added to another active treatment versus the same active treatment alone for urinary incontinence in women (Review). Cochrane Database Syst. Rev. 2015, 2015, CD010551. [Google Scholar] [CrossRef] [PubMed]
- Talasz, H.; Jansen, S.C.; Kofler, M.; Lechleitner, M. High prevalence of pelvic floor muscle dysfunction in hospitalized elderly women with urinary incontinence. Int. Urogynecology J. 2012, 23, 1231–1237. [Google Scholar] [CrossRef] [PubMed]
- Kim, S.; Wong, V.; Moore, K.H. Why are some women with pelvic floor dysfunction unable to contract their pelvic floor muscles? Aust. N. Z. J. Obstet. Gynaecol. 2013, 53, 574–579. [Google Scholar] [CrossRef]
- Steensma, A.B.; Konstantinovic, M.L.; Burger, C.W.; De Ridder, D.; Timmerman, D.; Deprest, J. Prevalence of major levator abnormalities in symptomatic patients with an underactive pelvic floor contraction. Int. Urogynecology J. 2010, 21, 861–867. [Google Scholar] [CrossRef] [Green Version]
- Dietz, H.P.; Shek, C. Levator avulsion and grading of pelvic floor muscle strength. Int. Urogynecology J. 2007, 19, 633–636. [Google Scholar] [CrossRef]
- Yang, S.-J.; Liu, Y.-T.; Lo, S.-S.; Tsai, C.-C.; Pan, P.-J. Effect of a Comprehensive Rehabilitation Program for Community Women with Urinary Incontinence: A Retrospect Cohort Study. Healthcare 2021, 9, 1686. [Google Scholar] [CrossRef] [PubMed]
- Miller, J.; Ashton-Miller, J.; DeLancey, J.O.L. A Pelvic Muscle Precontraction Can Reduce Cough-Related Urine Loss in Selected Women with Mild SUI. J. Am. Geriatr. Soc. 1998, 46, 870–874. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Tosun, O.C.; Mutlu, E.K.; Ergenoglu, A.M.; Yeniel, A.; Tosun, G.; Malkoc, M.; Askar, N.; Itil, I.M. Does pelvic floor muscle training abolish symptoms of urinary incontinence? A randomized controlled trial. Clin. Rehabil. 2014, 29, 525–537. [Google Scholar] [CrossRef]
- Luginbuehl, H.; Baeyens, J.-P.; Taeymans, J.; Maeder, I.-M.; Kuhn, A.; Radlinger, L. Pelvic floor muscle activation and strength components influencing female urinary continence and stress incontinence: A systematic review. Neurourol. Urodyn. 2015, 34, 498–506. [Google Scholar] [CrossRef]
- Thompson, J.A.; O’Sullivan, P.B.; Briffa, N.K.; Neumann, P. Assessment of voluntary pelvic floor muscle contraction in continent and incontinent women using transperineal ultrasound, manual muscle testing and vaginal squeeze pressure measurements. Int. Urogynecology J. 2006, 17, 624–630. [Google Scholar] [CrossRef]
- Cho, S.T.; Kim, K.H. Pelvic floor muscle exercise and training for coping with urinary incontinence. J. Exerc. Rehabil. 2021, 17, 379–387. [Google Scholar] [CrossRef] [PubMed]
- Veldman, M.; Gondin, J.; Place, N.; Maffiuletti, N.A. Effects of Neuromuscular Electrical Stimulation Training on Endurance Performance. Front. Physiol. 2016, 7, 544. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Woodley, S.J.; Lawrenson, P.; Boyle, R.; Cody, J.D.; Mørkved, S.; Kernohan, A.; Hay-Smith, E.J.C. Pelvic floor muscle training for preventing and treating urinary and faecal incontinence in antenatal and postnatal women. Cochrane Database Syst. Rev. 2020, 2021, CD007471. [Google Scholar] [CrossRef]
- Bech, S.R.; Villadsen, D.; Laursen, H.H.; Toft, A.; Reinau, H.S.; Raasted, T.H.; Christensen, K.W.; Corfitzen, L.H.; Christensen, S.W.M. The effect of group or individualised pelvic floor exercises with or without ultrasonography guidance for urinary incontinence in elderly women—A pilot study. J. Bodyw. Mov. Ther. 2021, 28, 34–41. [Google Scholar] [CrossRef]


| Criteria | Inclusion | Exclusion |
|---|---|---|
| Population | Women/Female Mixed population Pre- and post-menopause women Postpartum women | Post-surgical patients Pregnant women Animal Male |
| Intervention | Physiotherapy Pelvic floor muscle training (PFMT) PFMT with electrostimulation | Other interventions Pharmacological interventions |
| Comparator | Any comparator Placebo | Pharmacological PFMT with pharmacological Pharmacological with electrostimulation |
| Outcome | Muscle strength Endurance Urinary incontinence Urinary leakage | Any other clinical or biochemical outcome |
| Study | RCT | Analytical study Non-randomized study Qualitative study Narrative review Laboratory study |
| Language | English | Non-English |
| Year | 2000–Present | Before 2000 |
| Study Name Authors | Country | Study Type | Inclusion Criteria | Sample Randomized | Intervention Groups (Sample Size) | Duration of Study | Study Outcome | Drop out |
|---|---|---|---|---|---|---|---|---|
| Gumussoy et al. [16] 20 | Turkey | RCT | Women with SIU. | 51 | 26 EMG-BF 25 EMG-BF + ExMI. | 8 weeks | 1 h pad test (grams of urine loss) 3-day bladder diary I Qol pelvic floor muscle contraction force measured via a perineometer and Modified Oxford Scale (MOS). | 23 |
| Dumoulin et al. [15] 2020 | Canada | RCT | Stress or mixed UI in older women. | 362 | Group PFMT (178) vs. individual PFMT (184) | 12 weeks 1-year follow-up | %reduction in UI episodes in 1 year I Qol | 43 |
| Weber-Razek et al. [1] 2020 [1] | Poland | RCT | Women patients with urinary incontinence. | 128 | PFMT (44) ExMI (44) Control (40) | 4 weeks | Urinary incontinence, severity, QoL | 17 |
| Farzinmehr et al. [9] 2015 | Iran | RCT | Women patients with 4.5-year history of urinary incontinence. | 46 | WBVT (24) PFMT (22) | 3 months (13 weeks) | Urinary incontinence, severity, PFM strength | 3 |
| Chantale et al. 2004 [10] | Canada | RCT | Women patients exhibiting symptoms of stress urinary incontinence at least once per week for 3 months or more after their last delivery. | 64 | PFMT (21) PFM + AMT (23) Control (20) | 8 weeks | PFM function, muscle strength, endurance, rapidity of contraction, urine leakage incontinence | 2 |
| Hagen et al. [11] 2020 | UK | RCT | Women patients aged 18 years or older and newly presenting with clinically diagnosed stress or mixed urinary incontinence and urine leakage. | 600 | PFMT + Biofeedback (300) PFMT (300) | 24 months (104 weeks) | Incontinence, severity, symptoms, QoL, endurance, PFM strength | 7 |
| Ahlund et al. [4]. 2013. | Sweden | RCT | Women patients having urinary incontinence after 10–16 weeks postpartum. | 98 | PFMT (49) Control (49) | 6 months (26 weeks) | PFM strength, endurance, incontinence, symptoms, vaginal squeeze pressure | 16 |
| Castro et al. [3] 2008 | Brazil | RCT | Women patients having had urodynamic stress incontinence of at least 3 stress incontinence episodes in a week. | 118 | PFMT (31) ES (30) VC (27) Control (30) | 6 months (26 weeks) | QoL, urine leakage, urodynamic test | 17 |
| Jahromi et al. 2013 [7] | Iran | RCT | Women having Quid score for incontinence type (stress score ≥ 4, clinical symptoms of urinary incontinence within the last 6 months). | 50 | PFMT (25) Control (25) | 2 months (8.5 weeks) | Urinary incontinency, urine leakage, self-esteem, QoL, self-esteem | 2 |
| Gameiro et al. [8] 2010 | Brazil | RCT | Women patients having symptoms of SUI and urge incontinence. | 103 | VC (51) PFMT (51) | 12 weeks | Urinary leakage, PFM contraction | 0 |
| Wagg et al. [14] 2019 | Bangladesh | RCT | Women patients having current urinary incontinence, with a positive response of urinary leakage with urgency, stress, or drops of urine loss. | 625 | PFMT + Education (335) Education (290) | 24 weeks | Urinary leakage | 46 |
| Bo et al. [12] 2000 | Norway | RCT | Women patients having history of stress urinary incontinence and >4 g of urine leakage. | 59 | PFMT (29) Control (30) | 6 months (26 weeks) | Incontinence, symptoms, QOL | 6 |
| McLean et al. [13] 2013 | Canada | RCT | Women patients having symptoms of SUI with or without urge incontinence. | 40 | PFMT (20) Control (20) | 12 weeks | Incontinence, urinary flow | 5 |
| Pereira et al. [5] 2013 | Brazil | RCT | 12-month post-menopausal women patients having at least one episode of SUI symptom. | 45 | PFMT (15) VC (15) Control (15) | 12 months (52 weeks) | Urinary leakage, PFM strength, QoL | 4 |
| Leong et al. [2] 2015 | Hong Kong | RCT | Women patients having a clinical diagnosis of SUI, UUI, or MUI. | 55 | PFMT + BT + Education (27) Education (28) | 12 weeks | QoL incontinence episodes | 0 |
| Study Name | Scales Used for Measuring Outcomes | Risk of Bias | Age (Years) | Result for Muscle Contraction | Result for Endurance | Result for Urinary Incontinence |
|---|---|---|---|---|---|---|
| Gumussoy et al. [16] 2021 | Pad test, 3-day bladder diary I Qol PFMC with a perineometer and Modified Oxford Scale | Some concern. | 50.92 years (SD 8.88). | Pelvic floor muscle contraction force significantly increased in both groups. | Both groups achieved reductions in urine loss during treatment. -The rate of decrease in pad test values of the EMG-BF + ExMI group was higher. - Significant differences in the number of urinations on a daily basis (9 vs. 8 for the EMG-BF and 9 vs. 7 in the EMG − BF + ExMI group. | |
| Dumoulin et al. [15] 2020 | %reduction in UI episodes in 1 year, 7-day bladder diary Qol | Low risk. | Age, 67.9 [5.8] years | Significant reduction in leakage episode frequency at 12 weeks and 1 year for both groups’ median percentage reduction in urinary incontinence episodes at 1 year of 70% in individual PFMT compared with a 74% reduction in group-based PFMT. | ||
| Weber-Razek et al. [1] | RUIS, KHQ | Low risk. | Mean (Range): 68.77 (45 to 78) | Statistical improvement in urinary incontinence severity in PFMT | ||
| Farzinmehr et al. [9] | VAS, I-QOL | Low risk. | Range: 36 to 48 | WBVT was effective in PFM strength similar to PFMT. | WBVT was effective in reducing the severity of incontinence similar to PFMT. Increasing I-QOL questionnaire score. No significant difference was observed between the WBVT and PFMT groups. | |
| Dumoulin et al. [10] | Pad test, VAS, UDI, IIQ, pelvic floor muscle dynamometer | Some concern. | <45 | No significant improvement was observed between the PFMT, PFM + AT, and control group. | Significant improvement was observed in the PFMT and PFM + AT group compared with control. | |
| Hagen et al. [11] | ICIQ-UI SF, PGII | Some concern. No objective measure of urinary leakage. | Mean (SD) PFMT + Biofeedback: 48.2(11.6) PFMT: 47.3(11.4) | No significant difference was found between the PFMT + biofeedback (8.5%) and PFMT group (6%) at 6 months. | No clinical or significant difference was observed between PFMT + biofeedback and PFMT groups. 60% in the PFMT + biofeedback and 62.6% in the PFMT group reported improvement in symptoms at 24 months. | |
| Ahlund et al. [4] | BFLUT Symptoms Module ICIQ FLUTS Perineometer OGS | Low risk both groups received instructions on how to contract PFM and, vaginal palpation. | Mean (SD) 33 (3.6) | Muscle strength: No statistically significant difference was observed between PFMT and Control group. However, a significant increase was observed from baseline in both groups. | No significant difference was observed between PFMT and Control groups. However, there was an increase in endurance from baseline in both groups. | Significant improvement was observed in both PFMT and control group from baseline. |
| Castro et al. [3] | Pad test I-QOL OGS | Low risk. | Mean ± SD PFMT: 56.2 ± 12.5 ES: 55.2 ± 12.8 VC: 52.6 ± 11.2 Control: 52.6 ± 11.2 | Significant improvement was observed in the PFMT compared with the ES and VC groups. | Significant decrease in pad weight or improvement in urinary leakage in PFMT, ES, and VC group compared with control. However, no significant difference between ES, VC, and PFMT. | |
| Jahromi et al. [7] | QUID ICIQ Self-esteem questionnaires | High risk. | 60–74 years | Significant difference was observed between the PFMT and the control group for frequency of urine leakage. | ||
| Gameiro et al. [8] | VAS Pad test Perineometer | Low risk. | Mean VWC: 49 PFMT 48 | No statistical difference Was observed between the VWC and PFMT group. | Significant improvement was observed from baseline in both the groups at 6 months but not at 12 months. NS difference between the VWC and PFMT group. | |
| Wagg et al. [14] | EuroQoL Questionnaire EQ5D | Some concern. | Mean (SD) PFMT + Education: 64.5 (4.2) Education: 64.7 (4.1) | A significant decrease in leakage was observed in the PFMT + education group compared with the only education group. | ||
| Bo et al. [12] | QoLS-N B-FLUTS | High risk. | Mean (SD) PFMT: 49.6 (10.0) Control: 51.7 (8.8) | Significant improvement in sex-life, social life, and physical activity in PFMT group. NS difference between the groups. | ||
| McLean et al. [13] | Pad test UDI-6 IIQ-7 3-day bladder diary | High risk. | Mean ± SD PFMT: 49.5 ± 8.2 Control: 54.0 ± 8.4 | Significant improvements in in PFMT group on the impact of SUI compared with the control group. Pad test NS difference between the PFMT group and the control group. | ||
| Pereira et al. [5] | Pad test Perina Stim device | Low risk. | Median (min, max) PFMT: 62 (51, 85) VC: 64 (52, 83) Control: 62(51, 80) | Significant decrease in urinary leakage in PFMT and VC group from baseline compared with the control group. | ||
| Leong et al. [2] | IIQ-SF-7 UI7 | Some concern. | Mean (± SD) 74.3 ± 4.6 | Significant reduction in urinary leakage (>90%) in the PFMT + BT + education group compared with the education group (7.2%). |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Alouini, S.; Memic, S.; Couillandre, A. Pelvic Floor Muscle Training for Urinary Incontinence with or without Biofeedback or Electrostimulation in Women: A Systematic Review. Int. J. Environ. Res. Public Health 2022, 19, 2789. https://doi.org/10.3390/ijerph19052789
Alouini S, Memic S, Couillandre A. Pelvic Floor Muscle Training for Urinary Incontinence with or without Biofeedback or Electrostimulation in Women: A Systematic Review. International Journal of Environmental Research and Public Health. 2022; 19(5):2789. https://doi.org/10.3390/ijerph19052789
Chicago/Turabian StyleAlouini, Souhail, Sejla Memic, and Annabelle Couillandre. 2022. "Pelvic Floor Muscle Training for Urinary Incontinence with or without Biofeedback or Electrostimulation in Women: A Systematic Review" International Journal of Environmental Research and Public Health 19, no. 5: 2789. https://doi.org/10.3390/ijerph19052789






