Technology-Based Mental Health Interventions for Domestic Violence Victims Amid COVID-19
Highlights
- A growing array of technology-based mental health interventions is available to domestic violence victims.
- However, a lack of empirical evidence and oversight compromises these solutions’ ability to help the victims.
- Limited guardrails are in place to prevent technology-based help from turning into technology-facilitated harm.
- Rigorous research is needed to ensure the quality, safety, and security of mental health technologies for the victims.
- Domestic violence is a stain on humanity and a threat to global solidarity.
- Advanced technologies require more profound oversight to ensure they, first, do no harm, and second, do help.
- A whole-society approach is needed to safeguard victims’ mental health and eradicate domestic violence in the long run.
- Collective actions could make society more resistant to malaises such s domestic violence, amid COVID-19 and beyond.
Abstract
:1. Introduction
2. Materials and Methods
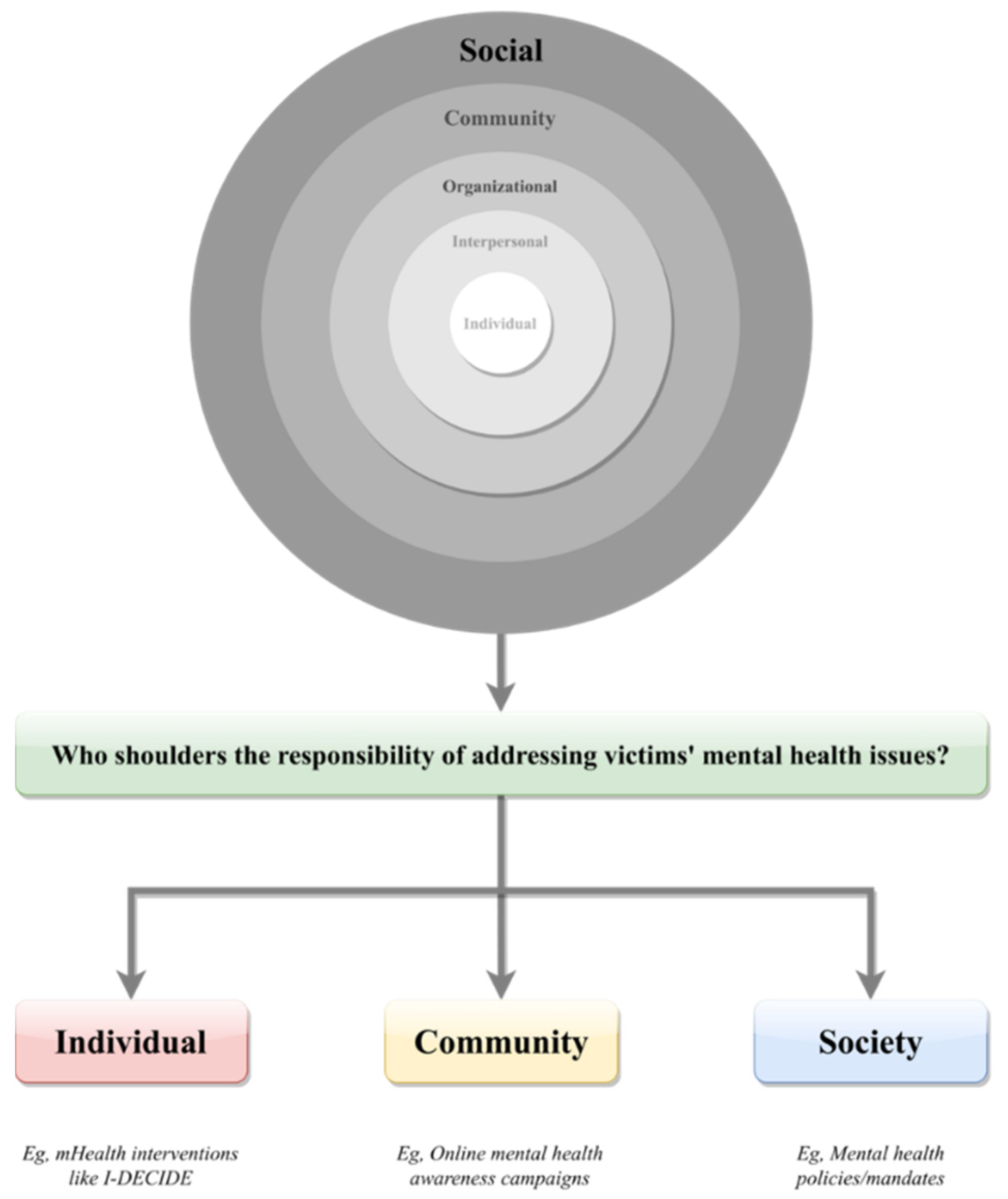
The Social Ecological Model
3. Results
4. Discussion
4.1. Benefits of Technology-Based Interventions
4.2. Risks Associated with Technology-Based Interventions
4.3. The Pronounced Need for More Rigorous Technology-Based Interventions
4.4. Limitations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- United Nations. Declaration on the Elimination of Violence against Women; United Nations: New York, NY, USA, 1993. [Google Scholar]
- World Health Organization. Preventing Intimate Partner and Sexual Violence against Women: Taking Action and Generating Evidence; World Health Organization: Geneva, Switzerland, 2010. [Google Scholar]
- Stöckl, H.; Devries, K.; Rotstetin, A.; Abrahams, N.; Campbell, J.; Watts, C.; Moreno, C.G. The global prevalence of intimate partner homicide: A systematic review. Lancet 2013, 382, 859–865. [Google Scholar] [CrossRef] [Green Version]
- Su, Z.; McDonnell, D.; Cheshmehzangi, A.; Ahmad, J.; Chen, H.; Šegalo, S.; Cai, Y. What “family affair”? Domestic violence awareness in China. Front. Public Health 2022, 10, 795841. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. Violence against Women. 2021. Available online: https://www.who.int/news-room/fact-sheets/detail/violence-against-women (accessed on 17 October 2021).
- Sardinha, L.; Maheu-Giroux, M.; Stöckl, H.; Metyer, S.R.; Galrcía-Moreno, C. Global, regional, and national prevalence estimates of physical or sexual, or both, intimate partner violence against women in 2018. Lancet 2022, 399, 803–813. [Google Scholar] [CrossRef]
- Sanchez, O.A.; Vivas, J.N.L.; Cardenas, D.R.; Cano, M.d.P.R. Sexual Violence against Women in the Context of the Colombian armed Conflict 2001–2009; Campaign ‘Rape and Other Violence: Leave my Body out of the War’: Bogota, Colombia, 2011. [Google Scholar]
- Oram, S.; Khalifeh, H.; Howard, L.M. Violence against women and mental health. Lancet Psychiatry 2017, 4, 159–170. [Google Scholar] [CrossRef] [Green Version]
- Ellsberg, M.; Watts, C.; Yoshihama, M.; Kiss, L.; Schraiber, L.B.; Deyessa, N.; WHO Multi-Country Study. Intimate partner violence and women’s physical and mental health in the WHO multi-country study on women’s health and domestic violence: An observational study. Lancet 2008, 371, 1165–1172. [Google Scholar] [CrossRef]
- Indu, P.V.; Remadevi, S.; Vidhukumar, K.; Navas, P.M.S.; Anilkumar, T.V.; Subha, N. Domestic violence as a risk factor for attempted suicide in married women. J. Interpers. Violence 2017, 35, 5753–5771. [Google Scholar] [CrossRef]
- Devries, K.; Watts, C.; Yoshihama, M.; Kiss, L.; Schraiber, L.B.; Deyessa, N.; Heise, L.; Durand, J.; Mbwambo, J.; Jansen, H.; et al. Violence against women is strongly associated with suicide attempts: Evidence from the WHO multi-country study on women’s health and domestic violence against women. Soc. Sci. Med. 2011, 73, 79–86. [Google Scholar] [CrossRef]
- Sediri, S.; Zgueb, Y.; Ouanets, S.; Ouali, U.; Bourgou, S.; Jomli, R.; Nacef, F. Women’s mental health: Acute impact of COVID-19 pandemic on domestic violence. Arch. Women’s Ment. Health 2020, 23, 749–756. [Google Scholar] [CrossRef]
- Hsu, L.-C.; Henke, A. COVID-19, staying at home, and domestic violence. Rev. Econ. Househ. 2021, 19, 145–155. [Google Scholar] [CrossRef]
- McLay, M.M. When “shelter-in-place” isn’t shelter that’s safe: A rapid analysis of domestic violence case differences during the COVID-19 pandemic and stay-at-home orders. J. Fam. Violence 2021. [CrossRef]
- Cancino, R.S.; Su, Z.; Mesa, R.; E Tomlinson, G.; Walng, J. The impact of COVID-19 on cancer screening: Challenges and opportunities. JMIR Cancer 2020, 6, e21697. [Google Scholar] [CrossRef] [PubMed]
- Baker, M.; Ivory, D. Why Public Health Faces a Crisis across the U.S. 2021. Available online: https://www.nytimes.com/2021/10/18/us/coronavirus-public-health.html (accessed on 19 October 2021).
- Constantino, R.E.; Braxter, B.; Ren, D.; Burroughs, J.D.; Doswell, W.M.; Wu, L.; Hwang, J.G.; Klem, M.; Joshi, J.B.D.; Greene, W.B. Comparing online with face-to-face HELPP intervention in women experiencing intimate partner violence. Issues Ment. Health Nurs. 2015, 36, 430–438. [Google Scholar] [CrossRef] [PubMed]
- van Gelder, N.; Ligthart, S.; Ten Elzen, J.; Prins, J.; van Rosmalen-Nooijens, K.; Oertelt-Prigione, S. “If I’d had something like SAFE at the time, maybe I would’ve left him sooner.”—Essential features of eHealth interventions for women exposed to intimate partner violence: A qualitative study. J. Interpers. Violence 2021, 08862605211036108. [Google Scholar] [CrossRef] [PubMed]
- Koziol-McLain, J.; Vandal, A.C.; Wilson, D.; Nada-Raja, S.; Dobbs, T.; McLean, C.; Sisk, R.; Eden, K.B.; E Glass, N. Efficacy of a Web-Based Safety Decision Aid for Women Experiencing Intimate Partner Violence: Randomized Controlled Trial. J. Med Internet Res. 2018, 19, e426. [Google Scholar] [CrossRef]
- Tarzia, L.; Cornelio, R.; Forsdike, K.; Hegarty, K. Women’s Experiences Receiving Support Online for Intimate Partner Violence: How Does it Compare to Face-to-Face Support from a Health Professional? Interact. Comput. 2018, 30, 433–443. [Google Scholar] [CrossRef]
- Ogbe, E.; Harmon, S.; Bergh, R.V.D.; Degomme, O. A systematic review of intimate partner violence interventions focused on improving social support and/mental health outcomes of survivors. PLoS ONE 2020, 15, e0235177. [Google Scholar] [CrossRef]
- Su, Z.; Li, X.; McDonnell, D.; A Fernandez, A.; E Flores, B.; Wang, J. Technology-Based Interventions for Cancer Caregivers: A Concept Analysis. JMIR Cancer 2021, 7, e22140. [Google Scholar] [CrossRef]
- Golden, S.D.; Earp, J.A.L. Social ecological approaches to individuals and their contexts: Twenty years of health education & behavior health promotion interventions. Health Educ. Behav. 2012, 39, 364–372. [Google Scholar]
- Cowan, E.; Khan, M.R.; Shastry, S.; Edelman, E.J. Conceptualizing the effects of the COVID-19 pandemic on people with opioid use disorder: An application of the social ecological model. Addict. Sci. Clin. Pr. 2021, 16, 4. [Google Scholar] [CrossRef]
- Stone, R.; Campbell, J.K.; Kinney, D.; Rothman, E.F. “He would take my shoes and all the baby’s warm winter gear so we couldn’t leave”: Barriers to safety and recovery experienced by a sample of Vermont women with partner violence and opioid use disorder experiences. J. Rural Health 2021, 37, 35–44. [Google Scholar] [CrossRef]
- Sullivan, C.M. Understanding How Domestic Violence Support Services Promote Survivor Well-being: A Conceptual Model. J. Fam. Violence 2018, 33, 123–131. [Google Scholar] [CrossRef]
- Kuskoff, E.; Parsell, C. Striving for Gender Equality: Representations of Gender in “Progressive” Domestic Violence Policy. Violence Women 2021, 27, 470–488. [Google Scholar] [CrossRef] [PubMed]
- Su, Z.; McDonnell, D.; Roth, S.; Li, Q.; Šegalo, S.; Shi, F.; Wagers, S. Mental health solutions for domestic violence victims amid COVID-19: A review of the literature. Glob. Health 2021, 17, 67. [Google Scholar] [CrossRef] [PubMed]
- Mazza, M.; Marano, G.; Lai, C.; Janiri, L.; Sani, G. Danger in danger: Interpersonal violence during COVID-19 quarantine. Psychiatry Res. 2020, 289, 113046. [Google Scholar] [CrossRef] [PubMed]
- Fegert, J.M.; Vitiello, B.; Plener, P.L.; Clemens, V. Challenges and burden of the Coronavirus 2019 (COVID-19) pandemic for child and adolescent mental health: A narrative review to highlight clinical and research needs in the acute phase and the long return to normality. Child Adolesc. Psychiatry Ment. Health 2020, 14, 20. [Google Scholar] [CrossRef]
- Emezue, C. Digital or Digitally Delivered Responses to Domestic and Intimate Partner Violence During COVID-19. JMIR Public Health Surveill 2020, 6, e19831. [Google Scholar] [CrossRef]
- Bennett, E.R.; Snyder, S.; Cusano, J.; McMahon, S.; Zijdel, M.; Camerer, K.; Howley, C. Supporting survivors of campus dating and sexual violence during COVID-19: A social work perspective. Soc. Work Health Care 2021, 60, 106–116. [Google Scholar] [CrossRef]
- Bradley, N.L.; DiPasquale, A.M.; Dillabough, K.; Schneider, P.S. Health care practitioners’ responsibility to address intimate partner violence related to the COVID-19 pandemic. Can. Med. Assoc. J. 2020, 192, E609–E610. [Google Scholar] [CrossRef]
- Barbara, G.; Facchin, F.; Micci, L.; Rendiniello, M.; Giulini, P.; Cattaneo, C.; Vercellini, P.; Kustermann, A. COVID-19, Lockdown, and Intimate Partner Violence: Some Data from an Italian Service and Suggestions for Future Approaches. J. Women’s Health (Larchmt) 2020, 29, 1239–1242. [Google Scholar] [CrossRef]
- Sauerborn, E.; Eisenhut, K.; Ganguli-Mitra, A.; Wild, V. Digitally supported public health interventions through the lens of structural injustice: The case of mobile apps responding to violence against women and girls. Bioethics 2021, 36, 71–76. [Google Scholar] [CrossRef]
- Su, Z.; McDonnell, D.; Liang, B.; Kue, J.; Li, X.; Šegalo, S.; Advani, S.; Flores, B.E.; Wang, J. Technology-based health solutions for cancer caregivers to better shoulder the impact of COVID-19: A systematic review protocol. Syst. Rev. 2021, 10, 43. [Google Scholar] [CrossRef] [PubMed]
- Su, Z.; Cheshmehzangi, A.; McDonnell, D.; Šegalo, S.; Ahmad, J.; Bennett, B. Gender inequality and health disparity amid COVID-19. Nurs. Outlook 2021, 70, 89–95. [Google Scholar] [CrossRef] [PubMed]
- Leigh, J.K.; Peña, L.D.; Anurudran, A.; Pai, A. “Are you safe to talk?”: Perspectives of Service Providers on Experiences of Domestic Violence During the COVID-19 Pandemic. J. Fam. Violence 2022. [Google Scholar] [CrossRef] [PubMed]
- Flor, L.S.; Friedman, J.; Spencer, C.N.; Cagney, J.; Arrieta, A.; E Herbert, M.; Stein, C.; Mullany, E.C.; Hon, J.; Patwardhan, V.; et al. Quantifying the effects of the COVID-19 pandemic on gender equality on health, social, and economic indicators: A comprehensive review of data from March, 2020, to September, 2021. Lancet 2022. [Google Scholar] [CrossRef]
- Morton, A.; Adams, C. Health visiting in England: The impact of the COVID-19 pandemic. Public Health Nurs. 2022. [Google Scholar] [CrossRef]
- Panovska-Griffiths, J.; Szilassy, E.; Johnson, M.; Dixon, S.; De Simoni, A.; Wileman, V.; Dowrick, A.; Emsley, E.; Griffiths, C.; Barbosa, E.C.; et al. Impact of the first national COVID-19 lockdown on referral of women experiencing domestic violence and abuse in England and Wales. BMC Public Health 2022, 22, 504. [Google Scholar] [CrossRef]
- Shah, S.S.; Mufeed, S.A. Urgency and relevance of feminist social work to curb domestic violence amid COVID-19. Int. Soc. Work 2022, 00208728211066833. [Google Scholar] [CrossRef]
- Tarzia, L.; Iyer, D.; Thrower, E.; Hegarty, K. “Technology doesn’t judge you”: Young Australian women’s views on using the internet and smartphones to address intimate partner violence. J. Technol. Hum. Serv. 2017, 35, 199–218. [Google Scholar] [CrossRef]
- Anderson, E.J.; Krause, K.C.; Krause, C.M.; Welter, A.; McClelland, D.J.; Garcia, D.O.; Ernst, K.; Lopez, E.C.; Koss, M.P. Web-Based and mHealth Interventions for Intimate Partner Violence Victimization Prevention: A Systematic Review. Trauma Violence Abus. 2019, 22, 870–884. [Google Scholar] [CrossRef]
- Murta, S.G.; Parada, P.D.O.; Meneses, S.; Medeiros, J.V.V.; Balbino, A.; Rodrigues, M.C.; Miura, M.A.; Dos Santos, T.A.A.; De Vries, H. Dating SOS: A systematic and theory-based development of a web-based tailored intervention to prevent dating violence among Brazilian youth. BMC Public Health 2020, 20, 391. [Google Scholar] [CrossRef] [Green Version]
- Clayson, P.E.; Carbine, K.A.; Baldwin, S.A.; Larson, M.J. Methodological reporting behavior, sample sizes, and statistical power in studies of event-related potentials: Barriers to reproducibility and replicability. Psychophysiology 2019, 56, e13437. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Thomas, C.R.; Miller, G.; Hartshorn, J.C.; Speck, N.C.; Walker, G. Telepsychiatry Program for Rural Victims of Domestic Violence. Telemed. J. e-Health 2005, 11, 567–573. [Google Scholar] [CrossRef] [PubMed]
- Women’s Aid. The Survivor’s Handbook: Information in Other Languages. 2021. Available online: https://www.womensaid.org.uk/the-survivors-handbook/different-languages/ (accessed on 20 October 2021).
- Mason, O.J.; Stevenson, C.; Freedman, F. Ever-present threats from information technology: The Cyber-Paranoia and Fear Scale. Front. Psychol. 2014, 5, 1298. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Kaya, A.Y.; Ata, F. New Media and Digital Paranoia: Extreme Skepticism in Digital Communication. In Handbook of Research on Cyberchondria, Health Literacy, and the Role of Media in Society’s Perception of Medical Information; Aker, H., Aiken, M., Eds.; IGI Global: Hershey, PA, USA, 2022; pp. 330–343. [Google Scholar]
- Zimaitis, I.; Degutis, M.; Urbonavicius, S. Social media use and paranoia: Factors that matter in online shopping. Sustainability 2020, 12, 904. [Google Scholar] [CrossRef] [Green Version]
- Winfield, A. Ethical standards in robotics and AI. Nat. Electron. 2019, 2, 46–48. [Google Scholar] [CrossRef]
- Keskinbora, K.H. Medical ethics considerations on artificial intelligence. J. Clin. Neurosci. 2019, 64, 277–282. [Google Scholar] [CrossRef]
- Hunt, X.; Tomlinson, M.; Sikander, S.; Skeen, S.; Marlow, M.; Du Toit, S.; Eisner, M. Artificial Intelligence, Big Data, and mHealth: The Frontiers of the Prevention of Violence Against Children. Front. Artif. Intell. 2020, 3, 106550. [Google Scholar] [CrossRef]
- Su, Z.; McDonnell, D.; Bentley, B.L.; He, J.; Shi, F.; Cheshmehzangi, A.; Ahmad, J.; Jia, P. Addressing Biodisaster X Threats with Artificial Intelligence and 6G Technologies: Literature Review and Critical Insights. J. Med. Internet Res. 2021, 23, e26109. [Google Scholar] [CrossRef]
- Jacobson, N.C.; Bentley, K.H.; Walton, A.; Wang, S.B.; Fortgang, R.G.; Millner, A.J.; Coombs, G.; Rodman, A.M.; Coppersmith, D.D.L. Ethical dilemmas posed by mobile health and machine learning in psychiatry research. Bull. World Health Organ. 2020, 98, 270–276. [Google Scholar] [CrossRef]
- Davison, T. Cyberthreats are going mobile and it’s time to take action. Comput. Fraud. Secur. 2021, 2021, 18–19. [Google Scholar] [CrossRef]
- Parsons, C.; Molnar, A.; Dalek, J.; Knockel, J.; Kenyon, M.; Haselton, B.; Khoo, C.; Deibert, R. The Predator in Your Pocket: A Multidisciplinary Assessment of the Stalkerware Application Industry; Lab, C., Ed.; University of Toronto: Toronto, ON, Canada, 2021. [Google Scholar]
- Jattamart, A.; Kwangsawad, A. What awareness variables are associated with motivation for changing risky behaviors to prevent recurring victims of cyberbullying? Heliyon 2021, 7, 08121. [Google Scholar] [CrossRef] [PubMed]
- Lopes Gomes Pinto Ferreira, G. Technology as both a facilitator of and response to youth intimate partner violence: Perspectives from advocates in the global-south. In The Emerald International Handbook of Technology-Facilitated Violence and Abuse; Bailey, J., Flynn, A., Henry, N., Eds.; Emerald Publishing Limited: Bingley, UK, 2021; pp. 427–446. [Google Scholar]
- Bauerly, B.C.; Mccord, R.F.; Hulkower, R.; Pepin, D. Broadband Access as a Public Health Issue: The Role of Law in Expanding Broadband Access and Connecting Underserved Communities for Better Health Outcomes. J. Law Med. Ethics 2019, 47 (Suppl. 2), 39–42. [Google Scholar] [CrossRef] [PubMed]
- Huckvale, K.; Torous, J.; Larsen, M.E. Assessment of thedata sharing and privacy practices of smartphone apps for depression and smoking cessation. JAMA Netw. Open 2019, 2, e192542. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Montag, C.; Elhai, J.D. Discussing digital technology overuse in children and adolescents during the COVID-19 pandemic and beyond: On the importance of considering Affective Neuroscience Theory. Addict. Behav. Rep. 2020, 12, 100313. [Google Scholar] [CrossRef]
- Schueller, S.M.; Hunter, J.F.; Figueroa, C.; Aguilera, A. Use of Digital Mental Health for Marginalized and Underserved Populations. Curr. Treat. Options Psychiatry 2019, 6, 243–255. [Google Scholar] [CrossRef]
- Pappas, S. Providing Care in Innovative Ways. 2021. Available online: https://www.apa.org/monitor/2020/01/cover-trends-innovative-ways (accessed on 24 October 2021).
- The Psychology Interjurisdictional Compact. Map. 2021. Available online: https://psypact.site-ym.com/general/custom.asp?page=psypactmap (accessed on 24 October 2021).
- Bradbury-Jones, C.; Isham, L. The pandemic paradox: The consequences of COVID-19 on domestic violence. J. Clin. Nurs. 2020, 29, 2047–2049. [Google Scholar] [CrossRef] [Green Version]
- Vaci, N.; Liu, Q.; Kormilitzin, A.; De Crescenzo, F.; Kurtulmus, A.; Harvey, J.; O’Dell, B.; Innocent, S.; Tomlinson, A.; Cipriani, A.; et al. Natural language processing for structuring clinical text data on depression using UK-CRIS. Évid. Based Ment. Health 2020, 23, 21–26. [Google Scholar] [CrossRef]
- Annapragada, A.V.; Donaruma-Kwoh, M.M.; Annapragada, A.V.; Starosolski, Z.A. A natural language processing and deep learning approach to identify child abuse from pediatric electronic medical records. PLoS ONE 2021, 16, e0247404. [Google Scholar] [CrossRef]
- Ni, Y.; Barzman, D.; Bachtel, A.; Griffey, M.; Osborn, A.; Sorter, M. Finding warning markers: Leveraging natural language processing and machine learning technologies to detect risk of school violence. Int. J. Med. Inform. 2020, 139, 104137. [Google Scholar] [CrossRef]
- Subramani, S.; Wang, H.; Vu, H.Q.; Li, G. Domestic violence crisis identification from facebook posts based on deep learning. IEEE Access 2018, 6, 54075–54085. [Google Scholar] [CrossRef]
- Howard, L.M.; Trevillion, K.; Agnew-Davies, R. Domestic violence and mental health. Int. Rev. Psychiatry 2010, 22, 525–534. [Google Scholar] [CrossRef] [PubMed]
- Campbell, J.C. Health consequences of intimate partner violence. Lancet 2002, 359, 1331–1336. [Google Scholar] [CrossRef]
- Graham, S.; Depp, C.; Lee, E.E.; Nebeker, C.; Tu, X.; Kim, H.-C.; Jeste, D.V. Artificial Intelligence for Mental Health and Mental Illnesses: An Overview. Curr. Psychiatry Rep. 2019, 21, 116. [Google Scholar] [CrossRef] [PubMed]
- Lovejoy, C.A.; Buch, V.; Maruthappu, M. Technology and mental health: The role of artificial intelligence. Eur. Psychiatry 2019, 55, 1–3. [Google Scholar] [CrossRef] [PubMed]
- Kolenik, T.; Gams, M. Persuasive Technology for Mental Health: One Step Closer to (Mental Health Care) Equality? IEEE Technol. Soc. Mag. 2021, 40, 80–86. [Google Scholar] [CrossRef]
- Ragavan, M.I.; Thomas, K.; Medzhitova, J.; Brewer, N.; Goodman, L.A.; Bair-Merritt, M. A systematic review of community-based research interventions for domestic violence survivors. Psychol. Violence 2019, 9, 139–155. [Google Scholar] [CrossRef]
- Johnson, L.; Stylianou, A.M. Coordinated Community Responses to Domestic Violence: A Systematic Review of the Literature. Trauma Violence Abus. 2020, 23, 506–522. [Google Scholar] [CrossRef] [PubMed]
| Theme | Search String |
|---|---|
| Domestic violence | “domestic violence” [MeSH] OR “domestic violence” [TIAB] OR “intimate partner violence” [MeSH] OR “intimate partner violence” [TIAB] OR “domestic violence” OR “intimate partner violence” OR “violence against women” OR “violence against woman” |
| Mental health | “mental health” [MeSH] OR “mental health” [TIAB] OR “mental wellbeing” OR “mental well-being” OR “psychological health” OR “psychological wellbeing” OR “psychological well-being” |
| Technology-based interventions | “technology” [MeSH] OR “technology” [TIAB] OR “eHealth” [TIAB] OR “telemedicine” [MeSH] OR “telemedicine” [TIAB] OR “tele-medicine” [MeSH] OR “tele-medicine” [TIAB] OR “telehealth” [TIAB] OR “tele-health” [TIAB] OR “connected health” [TIAB] OR “digital health” [TIAB] OR “mHealth” [TIAB] OR “mobile health” [TIAB] |
| COVID-19 | “COVID-19” [MeSH] OR “COVID-19” [TIAB] OR “SAS-CoV-2” OR “coronavirus disease 2019” |
| Category | Inclusion Criteria |
|---|---|
| Language | English |
| Focus | Provide insights on technology-based mental health interventions for domestic violence victims |
| Scope | Published within the context of COVID-19 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Su, Z.; Cheshmehzangi, A.; McDonnell, D.; Chen, H.; Ahmad, J.; Šegalo, S.; da Veiga, C.P. Technology-Based Mental Health Interventions for Domestic Violence Victims Amid COVID-19. Int. J. Environ. Res. Public Health 2022, 19, 4286. https://doi.org/10.3390/ijerph19074286
Su Z, Cheshmehzangi A, McDonnell D, Chen H, Ahmad J, Šegalo S, da Veiga CP. Technology-Based Mental Health Interventions for Domestic Violence Victims Amid COVID-19. International Journal of Environmental Research and Public Health. 2022; 19(7):4286. https://doi.org/10.3390/ijerph19074286
Chicago/Turabian StyleSu, Zhaohui, Ali Cheshmehzangi, Dean McDonnell, Hengcai Chen, Junaid Ahmad, Sabina Šegalo, and Claudimar Pereira da Veiga. 2022. "Technology-Based Mental Health Interventions for Domestic Violence Victims Amid COVID-19" International Journal of Environmental Research and Public Health 19, no. 7: 4286. https://doi.org/10.3390/ijerph19074286










