Implementation of a Comprehensive and Personalised Approach for Older People with Psychosocial Frailty in Valencia (Spain): Study Protocol for a Pre–Post Controlled Trial
Abstract
:1. Introduction
Objectives
- (a)
- To compare the benefits of the ValueCare intervention deployed in the Valencia pilot vs. usual care for older people in terms of frailty, loneliness, social support, health-related quality of life, and healthy lifestyle behaviour.
- (b)
- To evaluate the benefits of the ValueCare approach deployed in the Valencia pilot centre in terms of reducing the use of outpatient and inpatient health and social care among older people.
- (c)
- To evaluate the satisfaction of the target population with the ValueCare intervention deployed in the Valencia pilot centre.
2. Materials and Methods
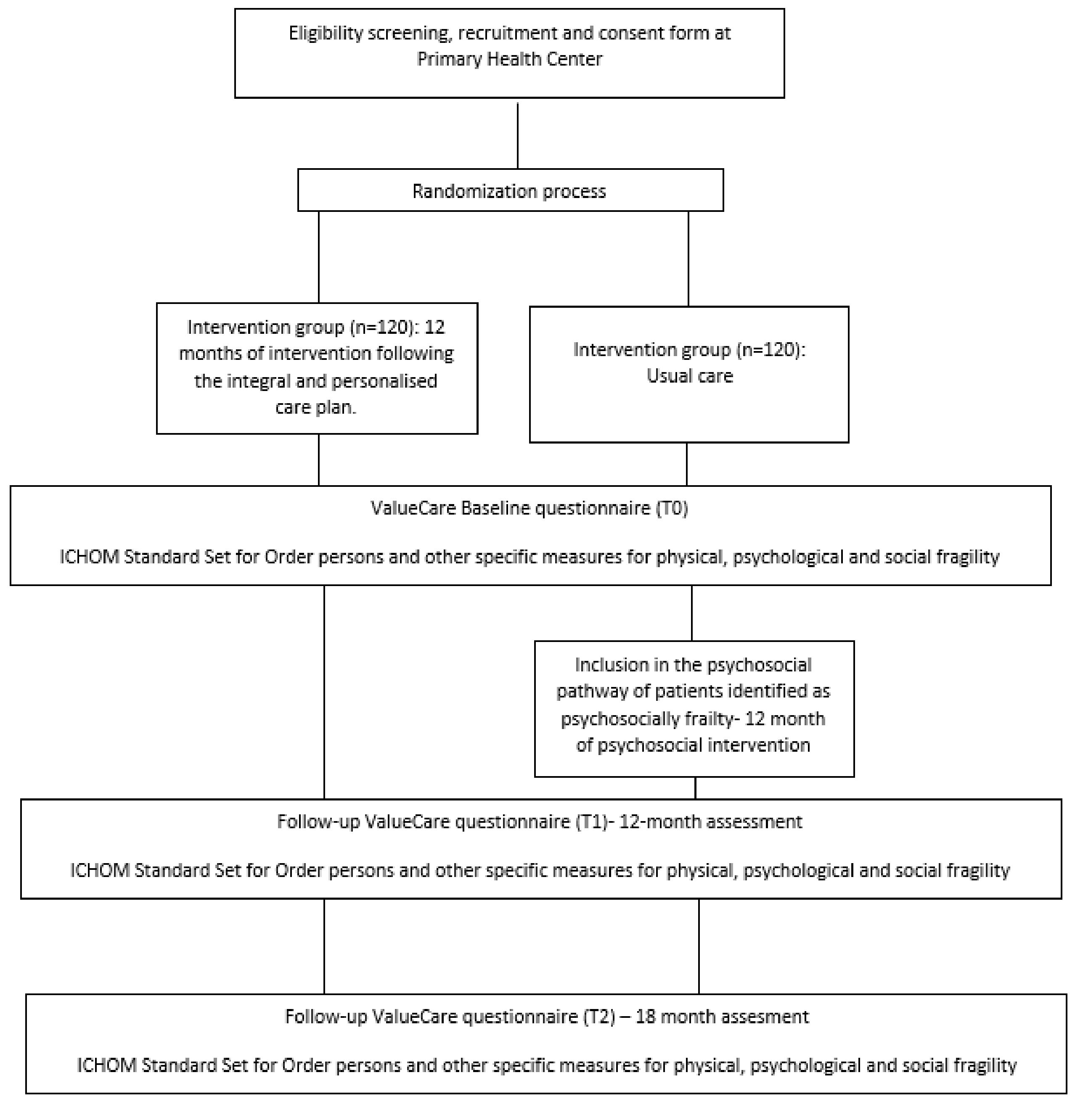
2.1. Design
2.2. Study Participants: Inclusion and Exclusion Criteria
2.3. Recruitment and Randomization
2.4. Data Collection Process
2.5. Description of the Intervention: Design and Implementation
2.6. Control Group
2.7. Outcomes
2.8. Ethics
3. Registration and Dissemination
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Prince, M.J.; Wu, F.; Guo, Y.; Robledo, L.M.G.; O’Donnell, M.; Sullivan, R.; Yusuf, S. The burden of disease in older people and implications for health policy and practice. Lancet 2015, 385, 549–562. [Google Scholar] [CrossRef] [PubMed]
- Rudnicka, E.; Napierała, P.; Podfigurna, A.; Męczekalski, B.; Smolarczyk, R.; Grymowicz, M. The World Health Organization (WHO) approach to healthy ageing. Maturitas 2020, 139, 6–11. [Google Scholar] [CrossRef] [PubMed]
- Lette, M.; Stoop, A.; Gadsby, E.; Ambugo, E.A.; Mateu, N.C.; Reynolds, J.; Nijpels, G.; Baan, C.; De Bruin, S.R. Supporting older people to live safely at home–findings from thirteen case studies on integrated care across Europe. Int. J. Integr. Care 2020, 20, 1. [Google Scholar] [CrossRef]
- Dogra, S.; Dunstan, D.W.; Sugiyama, T.; Stathi, A.; Gardiner, P.; Owen, N. Active aging and public health: Evidence, implications, and opportunities. Annu. Rev. Public Health 2022, 43, 439–459. [Google Scholar] [CrossRef] [PubMed]
- Liberale, L.; Badimon, L.; Montecucco, F.; Lüscher, T.; Libby, P.; Camici, G. Inflammation, aging, and cardiovascular disease: JACC review topic of the week. J. Am. Coll. Cardiol. 2022, 79, 837–847. [Google Scholar] [CrossRef]
- Pons Raventos, M.; Rebollo Rubio, A.; Jiménez Ternero, J. Fragilidad: ¿Cómo podemos detectarla? Enfermería Nefrológica 2016, 19, 170–173. [Google Scholar] [CrossRef]
- Brivio, P.; Paladini, M.; Racagni, G.; Riva, M.; Calabrese, F.; Molteni, R. From healthy aging to frailty: In search of the underlying mechanisms. Curr. Med. Chem. 2019, 26, 3685–3701. [Google Scholar] [CrossRef]
- Martin, F.; O’Halloran, A. Tools for assessing frailty in older people: General concepts. In Frailty and Cardiovascular Diseases: Research into an Elderly Population; Springer: Cham, Switzerland, 2020; pp. 9–19. [Google Scholar]
- Zhao, L.; Wu, L. The association between social participation and loneliness of the Chinese older adults over time—The mediating effect of social support. Int. J. Environ. Res. Public Health 2022, 19, 815. [Google Scholar] [CrossRef]
- Davies, K.; Maharani, A.; Chandola, T.; Todd, C.; Pendleton, N. The longitudinal relationship between loneliness, social isolation, and frailty in older adults in England: A prospective analysis. Lancet Healthy Longev. 2021, 2, e70–e77. [Google Scholar] [CrossRef]
- Sancho, P.; Sentandreu-Mañó, T.; Fernández, I.; Tomás, J. El impacto de la soledad y la fragilidad en el bienestar de los mayores europeos. Rev. Latinoam. Psicol. 2022, 54, 86–93. [Google Scholar] [CrossRef]
- Hoogendijk, E.; Suanet, B.; Dent, E.; Deeg, D.; Aartsen, M. Adverse effects of frailty on social functioning in older adults: Results from the Longitudinal Aging Study Amsterdam. Maturitas 2016, 83, 45–50. [Google Scholar] [CrossRef] [PubMed]
- Gale, C.; Westbury, L.; Cooper, C. Social isolation and loneliness as risk factors for the progression of frailty: The English Longitudinal Study of Ageing. Age Ageing 2018, 47, 392–397. [Google Scholar] [CrossRef] [PubMed]
- Park, C.; Majeed, A.; Gill, H.; Tamura, J.; Ho, R.C.; Mansur, R.B.; Nasri, F.; Lee, Y.; Rosenblat, J.D.; Wong, E.; et al. The effect of loneliness on distinct health outcomes: A comprehensive review and meta-analysis. Psychiatry Res. 2020, 294, 113514. [Google Scholar] [CrossRef] [PubMed]
- Altintas, H.; Coban, S.; Cantekin, I. Relationship between frailty and loneliness among community-dwelling Turkish older people. Psychogeriatrics 2023, 23, 243–251. [Google Scholar] [CrossRef] [PubMed]
- Gordon, E.H.; Hubbard, R.E. Differences in frailty in older men and women. Med. J. Aust. 2020, 212, 183–188. [Google Scholar] [CrossRef] [PubMed]
- Rivas-Ruiz, F.; Machón, M.; Contreras-Fernández, E.; Vrotsou, K.; Padilla-Ruiz, M.; Diez Ruiz, A.I.; de Mesa Berenguer, Y.; Vergara, I.; Group GIFEA. Prevalence of frailty among community-dwelling elderly persons in Spain and factors associated with it. Eur. J. Gen. Pract. 2019, 25, 190–196. [Google Scholar] [CrossRef] [PubMed]
- Menéndez-González, L.; Izaguirre-Riesgo, A.; Tranche-Iparraguirre, S.; Montero-Rodríguez, Á.; Orts-Cortés, M.I. Prevalencia y factores asociados de fragilidad en adultos mayores de 70 años en la comunidad. Atención Primaria 2021, 53, 102128. [Google Scholar] [CrossRef]
- O’Caoimh, R.; Sezgin, D.; O’Donovan, M.; Molloy, D.; Clegg, A.; Rockwood, K.; Liew, A. Prevalence of frailty in 62 countries across the world: A systematic review and meta-analysis of population-level studies. Age Ageing 2021, 50, 96–104. [Google Scholar] [CrossRef]
- Manfredi, G.; Midão, L.; Paúl, C.; Cena, C.; Duarte, M.; Costa, E. Prevalence of frailty status among the European elderly population: Findings from the Survey of Health, Aging and Retirement in Europe. Geriatr. Gerontol. Int. 2019, 19, 723–729. [Google Scholar] [CrossRef]
- Vermeiren, S.; Vella-Azzopardi, R.; Beckwee, D.; Habbig, A.K.; Scafoglieri, A.; Jansen, B.; Bautmans, I.; Verté, D.; Beyer, I.; Petrovic, M.; et al. Frailty and the prediction of negative health outcomes: A meta-analysis. J. Am. Med. Dir. Assoc. 2016, 17, 1163-e1. [Google Scholar] [CrossRef]
- Wleklik, M.; Uchmanowicz, I.; Jankowska, E.A.; Vitale, C.; Lisiak, M.; Drozd, M.; Pobrotyn, P.; Tkaczyszyn, M.; Lee, C. Multidimensional approach to frailty. Front. Psychol. 2020, 11, 564. [Google Scholar] [CrossRef] [PubMed]
- Ge, L.; Yap, C.; Heng, B. Associations of social isolation, social participation, and loneliness with frailty in older adults in Singapore: A panel data analysis. BMC Geriatr. 2022, 22, 26. [Google Scholar] [CrossRef] [PubMed]
- Fürstenau, D.; Haneke, H.; Spies, C.; Walz, T.; Schewina, K.; Höft, M.; Mörgeli, R.; Balzer, F. Tackling the frailty burden with an integrative value-based approach: Results from a mixed-methods study. J. Public Health 2022, 30, 99–110. [Google Scholar] [CrossRef]
- Boreskie, K.F.; Hay, J.L.; Boreskie, P.E.; Arora, R.C.; Duhamel, T.A. Frailty-aware care: Giving value to frailty assessment across different healthcare settings. BMC Geriatr. 2022, 22, 13. [Google Scholar] [CrossRef]
- Di Pollina, L.; Guessous, I.; Petoud, V.; Combescure, C.; Buchs, B.; Schaller, P.; Kossovsky, M.; Gaspoz, J.M. Integrated care at home reduces unnecessary hospitalizations of community-dwelling frail older adults: A prospective controlled trial. BMC Geriatr. 2017, 17, 53. [Google Scholar] [CrossRef]
- Abbasi, M.; Khera, S.; Dabravolskaj, J.; Chevalier, B.; Parker, K. The seniors’ community hub: An integrated model of care for the identification and management of frailty in primary care. Geriatrics 2021, 6, 18. [Google Scholar] [CrossRef] [PubMed]
- Sun, J.; Kong, X.; Li, H.; Chen, J.; Yao, Q.; Li, H.; Zhou, F.; Hu, H. Does social participation decrease the risk of frailty? Impacts of diversity in frequency and types of social participation on frailty in middle-aged and older populations. BMC Geriatr. 2022, 22, 553. [Google Scholar] [CrossRef] [PubMed]
- Paquet, C.; Whitehead, J.; Shah, R.; Adams, A.M.; Dooley, D.; Spreng, R.N.; Dubé, L. Social prescription interventions addressing social isolation and loneliness in older adults: Meta-review integrating on-the-ground resources. J. Med. Internet Res. 2023, 25, e40213. [Google Scholar] [CrossRef] [PubMed]
- O’Rourke, H.M.; Collins, L.; Sidani, S. Interventions to address social connectedness and loneliness for older adults: A scoping review. BMC Geriatr. 2018, 18, 214. [Google Scholar] [CrossRef]
- Miller, W.; Rollnick, S. Motivational interviewing: Preparing people for change. Book Review. J. Stud. Alcohol. 2002, 63, 776–777. [Google Scholar]
- Guillaumes, S.; O’Callaghan, C. Versión en español del software gratuito OxMaR para minimización y aleatorización de estudios clínicos. Gac. Sanit. 2019, 33, 395–397. [Google Scholar] [CrossRef] [PubMed]
- Akpan, A.; Roberts, C.; Bandeen-Roche, K.; Batty, B.; Bausewein, C.; Bell, D.; Bramley, D.; Bynum, J.; Cameron, I.D.; Chen, L.K.; et al. Standard set of health outcome measures for older persons. BMC Geriatr. 2018, 18, 36. [Google Scholar] [CrossRef] [PubMed]
- Gobbens, R.J.; van Assen, M.A.; Luijkx, K.G.; Wijnen-Sponselee, M.T.; Schols, J.M. The Tilburg frailty indicator: Psychometric properties. J. Am. Med. Dir. Assoc. 2010, 11, 344–355. [Google Scholar] [CrossRef] [PubMed]
- Hughes, M.; Waite, L.; Hawkley, L.; Cacioppo, J. A short scale for measuring loneliness in large surveys: Results from two population-based studies. Res. Aging 2004, 26, 655–672. [Google Scholar] [CrossRef] [PubMed]
- Prochaska, J.O.; DiClemente, C. Toward a comprehensive model of change. In Treating Addictive Behaviors: Processes of Change; Springer: Boston, MA, USA, 1986; pp. 3–27. [Google Scholar]
- Rempel, E.; Wilson, E.; Durrant, H.; Barnett, J. Preparing the prescription: A review of the aim and measurement of social referral programmes. BMJ Open 2017, 7, e017734. [Google Scholar] [CrossRef] [PubMed]
- Bickerdike, L.; Booth, A.; Wilson, P.; Farley, K.; Wright, K. Social prescribing: Less rhetoric and more reality. A systematic review of the evidence. BMJ Open 2017, 7, e013384. [Google Scholar] [CrossRef] [PubMed]
- Vidovic, D.; Reinhardt, G.Y.; Hammerton, C. Can social prescribing foster individual and community well-being? A systematic review of the evidence. Int. J. Environ. Res. Public Health 2021, 18, 5276. [Google Scholar] [CrossRef] [PubMed]
- Pescheny, J.; Randhawa, G.; Pappas, Y. The impact of social prescribing services on service users: A systematic review of the evidence. Eur. J. Public Health 2020, 30, 664–673. [Google Scholar] [CrossRef] [PubMed]
- Gauthier, A.; Lagarde, C.; Mourey, F.; Manckoundia, P. Use of digital tools, social isolation, and lockdown in people 80 years and older living at home. Int. J. Environ. Res. Public Health 2022, 19, 2908. [Google Scholar] [CrossRef]
- Vodafone Innovus. Available online: https://www.vodafoneinnovus.com/ (accessed on 16 November 2023).
- Sanz, M.F.; Acha, B.V.; García, M.F. Co-design for people-centred care digital solutions: A literature review. Int. J. Integr. Care 2021, 21, 16. [Google Scholar] [CrossRef]
- Vidavo, S.A. Available online: https://www.vidavo.eu/ (accessed on 16 November 2023).
- Fondazione Bruno Kessler. Available online: https://www.fbk.eu/en/ (accessed on 16 November 2023).
- Van Kan, G.; Rolland, Y.; Bergman, H.; Morley, J.; Kritchevsky, S.; Vellas, B. Geriatric Advisory Panel. The IANA Task Force on frailty assessment of older people in clinical practice. J. Nutr. Health Aging 2018, 12, 29–37. [Google Scholar] [CrossRef] [PubMed]
- Gleason, L.; Benton, E.; Alvarez-Nebreda, M.; Weaver, M.; Harris, M.; Javedan, H. FRAIL questionnaire screening tool and short-term outcomes in geriatric fracture patients. J. Am. Med. Dir. Assoc. 2017, 18, 1082–1086. [Google Scholar] [CrossRef] [PubMed]
- Collin, C.; Wade, D.T.; Davies, S.; Horne, V. The Barthel ADL Index: A reliability study. Int. Disabil. Stud. 1988, 10, 61–63. [Google Scholar] [CrossRef] [PubMed]
- Pfeiffer, E. A short portable mental status questionnaire for the assessment of organic brain deficit in elderly patients. J. Am. Geriatr. Soc. 1975, 23, 433–441. [Google Scholar] [CrossRef] [PubMed]
- Katzan, I.; Lapin, B. PROMIS GH (patient-reported outcomes measurement information system global health) scale in stroke: A validation study. Stroke 2018, 49, 147–154. [Google Scholar] [CrossRef] [PubMed]
- EuroQol Research F Research Foundation. EQ-5D-5L User Guide Version 3.0: Basic Information on How to Use the EQ-5D-5L Instrument. 2019. Available online: https://euroqol.org/publications/user-guides (accessed on 1 February 2024).
- Scheffer, A.; Schuurmans, M.; van Dijk, N.; Van Der Hooft, T.; De Rooij, S. Reliability and validity of the visual analogue scale for fear of falling in older persons. J. Am. Geriatr. Soc. 2010, 58, 2228. [Google Scholar] [CrossRef] [PubMed]
- Levy, H. Self-administered medication-risk questionnaire in an elderly population. Ann. Pharmacother. 2003, 37, 982–987. [Google Scholar] [CrossRef] [PubMed]
- Zhang, S.; Meng, L.; Qiu, F.; Yang, J.; Sun, S. Medication-related risk factors associated with health-related quality of life among community-dwelling elderly in China. Patient Prefer. Adherence 2018, 12, 529–537. [Google Scholar] [CrossRef] [PubMed]
- Wijnhoven, H.; Elstgeest, L.; de Vet, H.; Nicolaou, M.; Snijder, M.; Visser, M. Development and validation of a short food questionnaire to screen for low protein intake in community-dwelling older adults: The Protein Screener 55+(Pro55+). PLoS ONE 2018, 13, e0196406. [Google Scholar] [CrossRef]
- Guralnik, J.M.; Simonsick, E.M.; Ferrucci, L.; Glynn, R.J.; Berkman, L.F.; Blazer, D.G.; Scherr, P.A.; Wallace, R.B. A short physical performance battery assessing lower extremity function: Association with self-reported disability and prediction of mortality and nursing home admission. J. Gerontol. 1994, 49, M85–M94. [Google Scholar] [CrossRef]
- Romero-Ortuno, R. The Frailty Instrument of the Survey of Health, Ageing and Retirement in Europe (SHARE-FI) predicts mortality beyond age, comorbidities, disability, self-rated health, education and depression. Eur. Geriatr. Med. 2011, 2, 323–326. [Google Scholar] [CrossRef] [PubMed]
- Wijnhoven, H.A.; Schilp, J.; de Vet, H.C.; Kruizenga, H.M.; Deeg, D.J.; Ferrucci, L.; Visser, M. Development and validation of criteria for determining undernutrition in community-dwelling older men and women: The Short Nutritional Assessment Questionnaire 65+. Clin. Nutr. 2012, 31, 351–358. [Google Scholar] [CrossRef] [PubMed]
- Ng, T.P.; Feng, L.; Nyunt, M.S.Z.; Feng, L.; Niti, M.; Tan, B.Y.; Chan, G.; Khoo, S.A.; Chan, S.M.; Yap, P.; et al. Nutritional, physical, cognitive, and combination interventions and frailty reversal among older adults: A randomized controlled trial. Am. J. Med. 2015, 128, 1225–1236. [Google Scholar] [CrossRef] [PubMed]
- Strandberg, T.; Pitkälä, K.; Tilvis, R. Frailty in older people. Eur. Geriatr. Med. 2011, 2, 344–355. [Google Scholar] [CrossRef]
- Dedeyne, L.; Deschodt, M.; Verschueren, S.; Tournoy, J.; Gielen, E. Effects of multi-domain interventions in (pre) frail elderly on frailty, functional, and cognitive status: A systematic review. Clin. Interv. Aging 2017, 12, 873–896. [Google Scholar] [CrossRef] [PubMed]
- Bloch, F.; Charasz, N. Attitudes of older adults to their participation in clinical trials: A pilot study. Drugs Aging 2014, 31, 373–377. [Google Scholar] [CrossRef]
- Pitkala, H.; Strandberg, T. Clinical trials in older people. Age Ageing 2022, 51, afab282. [Google Scholar] [CrossRef]
| Outcome | Outcome Measure (s) | Methods and Instruments |
|---|---|---|
| Health, well-being, and quality of life | Physical HR-QoL | PROMIS-10 [45] |
| Mental HR-QoL | ||
| Self-perceived health | EQ-5D-5L [46] | |
| Frailty | Tilburg Frailty Indicator [30] | |
| Comorbidities | ICHOM Older Person Set [29] | |
| Loneliness | UCLA 3-Item Loneliness Scale [31] | |
| Activities of daily living | Modified 10-item Barthel Index [43] | |
| Falls | Visual Analogue Scale for Fear of Falling [47] | |
| Lifestyle behaviour | BMI | ICHOM Older Person Set [29] |
| Smoking status | ICHOM Older Person Set [29] | |
| Alcohol consumption | ICHOM Older Person Set [29] | |
| Sitting time | One Internal Physical Activity Questionnaire (IPAQ) | |
| Physical activity | One item of the SHARE-Frailty [57] | |
| Nutrition and undernutrition | SNAQ + 65 [58] | |
| Medication use | Medication intake | Medication Risk Questionnaire (MRQ-10) [48] |
| Care use | Care utilisation | Modified SMRC Health Care Utilization Questionnaire [49] |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Fernández-Salido, M.; Alhambra-Borrás, T.; Garcés-Ferrer, J. Implementation of a Comprehensive and Personalised Approach for Older People with Psychosocial Frailty in Valencia (Spain): Study Protocol for a Pre–Post Controlled Trial. Int. J. Environ. Res. Public Health 2024, 21, 715. https://doi.org/10.3390/ijerph21060715
Fernández-Salido M, Alhambra-Borrás T, Garcés-Ferrer J. Implementation of a Comprehensive and Personalised Approach for Older People with Psychosocial Frailty in Valencia (Spain): Study Protocol for a Pre–Post Controlled Trial. International Journal of Environmental Research and Public Health. 2024; 21(6):715. https://doi.org/10.3390/ijerph21060715
Chicago/Turabian StyleFernández-Salido, Mirian, Tamara Alhambra-Borrás, and Jorge Garcés-Ferrer. 2024. "Implementation of a Comprehensive and Personalised Approach for Older People with Psychosocial Frailty in Valencia (Spain): Study Protocol for a Pre–Post Controlled Trial" International Journal of Environmental Research and Public Health 21, no. 6: 715. https://doi.org/10.3390/ijerph21060715





