Adjuvant Treatment of Stage I–II Serous Endometrial Cancer: A Single Institution 20-Year Experience
Abstract
1. Introduction
2. Materials and Methods
2.1. Design and Participants
2.2. Data Collection
2.3. Outcomes
2.4. Statistical Analysis
3. Results
3.1. Patient and Treatment Characteristics
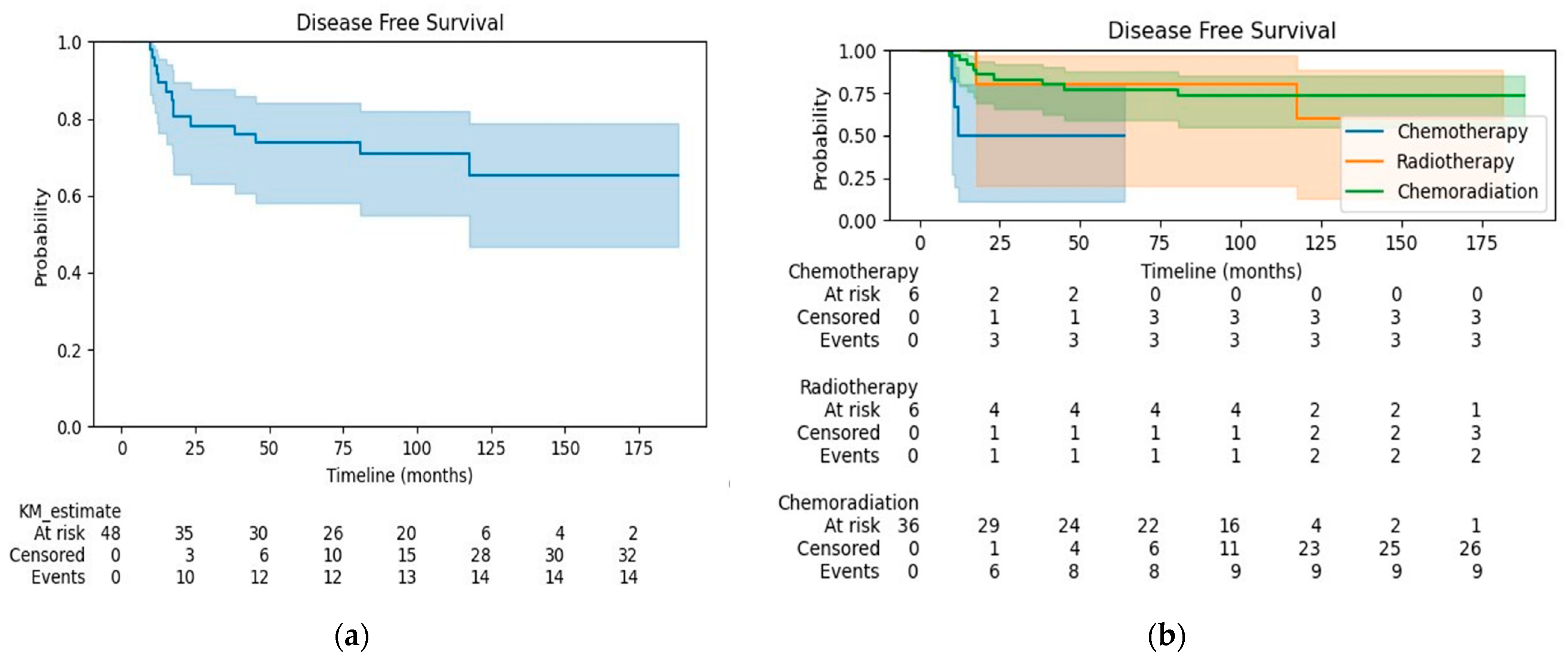
3.2. Survival Outcomes
3.3. Patterns of Recurrence
3.4. Toxicity Outcomes and Treatment Compliance
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Brenner, D.; Poirier, A.; Smith, L.; Aziz, L.S.; Ellison, L.; Fitzgerald, N.; Saint-Jacques, N.; Turner, D.; Weir, H.K.; Woods, R.; et al. Canadian Cancer Statistics Advisory Committee in Collaboration with the Canadian Cancer Society, Statistics Canana and the Public Health Agency of Canada. Canadian Cancer Statistics 2021. Canadian Cancer Society. 2021. Available online: http://cancer.ca/Canadian-Cancer-Statistics-2021-EN (accessed on 1 May 2024).
- Felix, A.S.; Weissfeld, J.L.; Stone, R.A.; Bowser, R.; Chivukula, M.; Edwards, R.P.; Linkov, F. Factors Associated with Type I and Type II Endometrial Cancer. Cancer Causes Control CCC 2010, 21, 1851–1856. [Google Scholar] [CrossRef] [PubMed]
- Sagae, S.; Susumu, N.; Viswanathan, A.N.; Aoki, D.; Backes, F.J.; Provencher, D.M.; Vaughan, M.; Creutzberg, C.L.; Kurzeder, C.; Kristensen, G.; et al. Gynecologic Cancer InterGroup (GCIG) Consensus Review for Uterine Serous Carcinoma. Int. J. Gynecol. Cancer Off. J. Int. Gynecol. Cancer Soc. 2014, 24, S83–S89. [Google Scholar] [CrossRef] [PubMed]
- Boruta, D.M.; Gehrig, P.A.; Fader, A.N.; Olawaiye, A.B. Management of Women with Uterine Papillary Serous Cancer: A Society of Gynecologic Oncology (SGO) Review. Gynecol. Oncol. 2009, 115, 142–153. [Google Scholar] [CrossRef] [PubMed]
- Hamilton, C.A.; Cheung, M.K.; Osann, K.; Chen, L.; Teng, N.N.; Longacre, T.A.; Powell, M.A.; Hendrickson, M.R.; Kapp, D.S.; Chan, J.K. Uterine Papillary Serous and Clear Cell Carcinomas Predict for Poorer Survival Compared to Grade 3 Endometrioid Corpus Cancers. Br. J. Cancer 2006, 94, 642–646. [Google Scholar] [CrossRef] [PubMed]
- Concin, N.; Matias-Guiu, X.; Vergote, I.; Cibula, D.; Mirza, M.R.; Marnitz, S.; Ledermann, J.; Bosse, T.; Chargari, C.; Fagotti, A.; et al. ESGO/ESTRO/ESP Guidelines for the Management of Patients with Endometrial Carcinoma. Radiother. Oncol. 2021, 154, 327–353. [Google Scholar] [CrossRef] [PubMed]
- Berek, J.S.; Matias-Guiu, X.; Creutzberg, C.; Fotopoulou, C.; Gaffney, D.; Kehoe, S.; Lindemann, K.; Mutch, D.; Concin, N.; FIGO Women’s Cancer Committee. FIGO Staging of Endometrial Cancer: 2023. Int. J. Gynecol. Obstet. 2023, 162, 383–394. [Google Scholar] [CrossRef] [PubMed]
- Boyraz, G.; Salman, M.C.; Basaran, D.; Ozgul, N.; Turan, T.; Turkmen, O.; Kimyon, G.C.; Ozkan, N.T.; Cagan, M.; Gungor, T.; et al. Extrauterine Spread, Adjuvant Treatment, and Prognosis in Noninvasive Uterine Papillary Serous Carcinoma of the Endometrium: A Retrospective Multicenter Study. Int. J. Gynecol. Cancer Off. J. Int. Gynecol. Cancer Soc. 2017, 27, 102–108. [Google Scholar] [CrossRef] [PubMed]
- Slomovitz, B.M.; Burke, T.W.; Eifel, P.J.; Ramondetta, L.M.; Silva, E.G.; Jhingran, A.; Oh, J.C.; Atkinson, E.N.; Broaddus, R.R.; Gershenson, D.M.; et al. Uterine Papillary Serous Carcinoma (UPSC): A Single Institution Review of 129 Cases. Gynecol. Oncol. 2003, 91, 463–469. [Google Scholar] [CrossRef] [PubMed]
- Casarin, J.; Multinu, F.; Tortorella, L.; Cappuccio, S.; Weaver, A.L.; Ghezzi, F.; Cliby, W.; Kumar, A.; Langstraat, C.; Glaser, G.; et al. Sentinel Lymph Node Biopsy for Robotic-Assisted Endometrial Cancer Staging: Further Improvement of Perioperative Outcomes. Int. J. Gynecol. Cancer 2020, 30, 41–47. [Google Scholar] [CrossRef]
- Casarin, J.; Multinu, F.; Ubl, D.S.; Dowdy, S.C.; Cliby, W.A.; Glaser, G.E.; Butler, K.A.; Ghezzi, F.; Habermann, E.B.; Mariani, A. Adoption of Minimally Invasive Surgery and Decrease in Surgical Morbidity for Endometrial Cancer Treatment in the United States. Obstet. Gynecol. 2018, 131, 304–311. [Google Scholar] [CrossRef]
- Blake, P.; Swart, A.M.; Orton, J.; Kichener, H.; Whelan, T.; Lukka, H.; Eisenhauer, E.; Bacon, M.; Tu, D.; Parman, M.K. Adjuvant External Beam Radiotherapy in the Treatment of Endometrial Cancer (MRC ASTEC and NCIC CTG EN. 5 Randomised Trials): Pooled Trial Results, Systematic Review, and Meta-Analysis. Lancet 2009, 373, 137–146. [Google Scholar] [PubMed]
- de Boer, S.M.; Powell, M.E.; Mileshkin, L.; Katsaros, D.; Bessette, P.; Haie-Meder, C.; Ottevanger, P.B.; Ledermann, J.A.; Khaw, P.; D’Amico, R.; et al. Adjuvant Chemoradiotherapy versus Radiotherapy Alone in Women with High-Risk Endometrial Cancer (PORTEC-3): Patterns of Recurrence and Post-Hoc Survival Analysis of a Randomised Phase 3 Trial. Lancet Oncol. 2019, 20, 1273–1285. [Google Scholar] [CrossRef] [PubMed]
- National Comprehensive Cancer Network. NCCN Clinical Practice Guidelines in Oncology: Uterine Neoplasms V.2.2024; National Comprehensive Cancer Network: Plymouth Meeting, PA, USA, 2024; Available online: https://www.nccn.org/guidelines/guidelines-detail?category=1&id=1473 (accessed on 1 May 2024).
- Tortorella, L.; Langstraat, C.L.; Weaver, A.L.; McGree, M.E.; Bakkum-Gamez, J.N.; Dowdy, S.C.; Cliby, W.A.; Keeney, G.L.; Sherman, M.E.; Weroha, S.J.; et al. Uterine Serous Carcinoma: Reassessing Effectiveness of Platinum-Based Adjuvant Therapy. Gynecol. Oncol. 2018, 149, 291–296. [Google Scholar] [CrossRef] [PubMed]
- Fader, A.N.; Drake, R.D.; O’Malley, D.M.; Gibbons, H.E.; Huh, W.K.; Havrilesky, L.J.; Gehrig, P.A.; Tuller, E.; Axtell, A.E.; Zanotti, K.M.; et al. Platinum/Taxane-Based Chemotherapy with or without Radiation Therapy Favorably Impacts Survival Outcomes in Stage I Uterine Papillary Serous Carcinoma. Cancer 2009, 115, 2119–2127. [Google Scholar] [CrossRef] [PubMed]
- Velker, V.; D’Souza, D.; Prefontaine, M.; McGee, J.; Leung, E. Role of Adjuvant Therapy for Stage IA Serous and Clear Cell Uterine Cancer: Is Observation a Valid Strategy? Int. J. Gynecol. Cancer Off. J. Int. Gynecol. Cancer Soc. 2016, 26, 491–496. [Google Scholar] [CrossRef] [PubMed]
- Qu, X.M.; Velker, V.M.; Leung, E.; Kwon, J.S.; Elshaikh, M.A.; Kong, I.; Logie, N.A.; Mendez, L.C.; van der Putten, L.J.; Donovan, E.K.; et al. The Role of Adjuvant Therapy in Stage IA Serous and Clear Cell Uterine Cancer: A Multi-Institutional Pooled Analysis. Gynecol. Oncol. 2018, 149, 283–290. [Google Scholar] [CrossRef] [PubMed]
- Nasioudis, D.; Roy, A.G.; Ko, E.M.; Cory, L.; Giuntoli Ii, R.L.; Haggerty, A.F.; Kim, S.H.; Morgan, M.A.; Latif, N.A. Adjuvant Treatment for Patients with FIGO Stage I Uterine Serous Carcinoma Confined to the Endometrium. Int. J. Gynecol. Cancer Off. J. Int. Gynecol. Cancer Soc. 2020, 30, 1089–1094. [Google Scholar] [CrossRef] [PubMed]
- Kurnit, K.C.; Nobre, S.P.; Fellman, B.M.; Iglesias, D.A.; Lindemann, K.; Jhingran, A.; Eriksson, A.G.Z.; Ataseven, B.; Glaser, G.E.; Mueller, J.J.; et al. Adjuvant Therapy in Women with Early Stage Uterine Serous Carcinoma: A Multi-Institutional Study. Gynecol. Oncol. 2022, 167, 452–457. [Google Scholar] [CrossRef] [PubMed]
- Keys, H.M.; Roberts, J.A.; Brunetto, V.L.; Zaino, R.J.; Spirtos, N.M.; Bloss, J.D.; Pearlman, A.; Maiman, M.A.; Bell, J.G. A Phase III Trial of Surgery with or without Adjunctive External Pelvic Radiation Therapy in Intermediate Risk Endometrial Adenocarcinoma: A Gynecologic Oncology Group Study. Gynecol. Oncol. 2004, 92, 744–751. [Google Scholar] [CrossRef]
- Creutzberg, C.L.; Nout, R.A.; Lybeert, M.L.; Warlam-Rodenhuis, C.C.; Jobsen, J.J.; Mens, J.W.; Lutgens, L.C.; Pras, E.; van de Poll-Franse, L.V.; van Putten, W.L.; et al. Fifteen-Year Radiotherapy Outcomes of the Randomized PORTEC-1 Trial for Endometrial Carcinoma. Int. J. Radiat. Oncol. Biol. Phys. 2011, 81, e631–e638. [Google Scholar] [CrossRef]
- Nout, R.A.; Smit, V.; Putter, H.; Juergenliemk-Schulz, I.M.; Jobsen, J.J.; Lutgens, L.; van der Steen-Banasik, E.M.; Mens, J.W.M.; Slot, A.; Kroese, M.S. Vaginal Brachytherapy versus Pelvic External Beam Radiotherapy for Patients with Endometrial Cancer of High-Intermediate Risk (PORTEC-2): An Open-Label, Non-Inferiority, Randomised Trial. Lancet 2010, 375, 816–823. [Google Scholar] [CrossRef] [PubMed]
- Randall, M.E.; Filiaci, V.; McMeekin, D.S.; Von Gruenigen, V.; Huang, H.; Yashar, C.M.; Mannel, R.S.; Kim, J.-W.; Salani, R.; Disilvestro, P.A.; et al. Phase III Trial: Adjuvant Pelvic Radiation Therapy Versus Vaginal Brachytherapy Plus Paclitaxel/Carboplatin in High-Intermediate and High-Risk Early-Stage Endometrial Cancer. J. Clin. Oncol. 2019, 37, 1810–1818. [Google Scholar] [CrossRef] [PubMed]
- Matei, D.; Filiaci, V.; Randall, M.E.; Mutch, D.; Steinhoff, M.M.; Disilvestro, P.A.; Moxley, K.M.; Kim, Y.M.; Powell, M.A.; O’Malley, D.M.; et al. Adjuvant Chemotherapy plus Radiation for Locally Advanced Endometrial Cancer. N. Engl. J. Med. 2019, 380, 2317–2326. [Google Scholar] [CrossRef] [PubMed]
- Lancellotta, V.; De Felice, F.; Vicenzi, L.; Antonacci, A.; Cerboneschi, V.; Costantini, S.; di Cristino, D.; Tagliaferri, L.; Cerrotta, A.; Vavassori, A.; et al. The Role of Vaginal Brachytherapy in Stage I Endometrial Serous Cancer: A Systematic Review. J. Contemp. Brachyther. 2020, 12, 61–66. [Google Scholar] [CrossRef] [PubMed]
- Creasman, W.T.; Kohler, M.F.; Odicino, F.; Maisonneuve, P.; Boyle, P. Prognosis of Papillary Serous, Clear Cell, and Grade 3 Stage I Carcinoma of the Endometrium. Gynecol. Oncol. 2004, 95, 593–596. [Google Scholar] [CrossRef] [PubMed]
- De Boer, S.M.; Powell, M.E.; Mileshkin, L.; Katsaros, D.; Bessette, P.; Haie-Meder, C.; Ottevanger, P.B.; Ledermann, J.A.; Khaw, P.; Colombo, A.; et al. Adjuvant Chemoradiotherapy versus Radiotherapy Alone for Women with High-Risk Endometrial Cancer (PORTEC-3): Final Results of an International, Open-Label, Multicentre, Randomised, Phase 3 Trial. Lancet Oncol. 2018, 19, 295–309. [Google Scholar] [CrossRef]
- Leon-Castillo, A.; De Boer, S.M.; Powell, M.E.; Mileshkin, L.R.; Mackay, H.J.; Leary, A.; Nijman, H.W.; Singh, N.; Pollock, P.M.; Bessette, P.; et al. Molecular Classification of the PORTEC-3 Trial for High-Risk Endometrial Cancer: Impact on Prognosis and Benefit From Adjuvant Therapy. J. Clin. Oncol. 2020, 38, 3388–3397. [Google Scholar] [CrossRef]

| All Patients (n = 50) | CT (n = 6) | RT (n = 6) | CRT (n = 36) | Observation (n = 2) | |
|---|---|---|---|---|---|
| Age at diagnosis, median (min–max) | 69 (46–92) | 70.5 (67–92) | 65.5 (48–81) | 66.5 (46–83) | 89 (86–92) |
| BMI, median (min–max) | 31.2 (20.6–48.9) | 30.8 (21.5–33.8) | 28.8 (23.9–48.9) | 31.5 (20.6–47.6) | 35.9 (32–39.8) |
| CEA at diagnosis (n = 35), median (min–max) | 1.7 (0.4–6.5) | 2.55 (1.4–3.6) | 2.5 (1.6–3.6) | 1.7 (0.4–6.5) | 1.3 |
| Ca-125 at diagnosis (N = 47), median (min–max) | 14 (5–119) | 13.5 (7–57) | 14 (9–26) | 14 (5–119) | 19 (16–22) |
| ECOG Score 0, n | 42 | 6 | 6 | 30 | 0 |
| ECOG Score ≥1, n | 8 | 0 | 0 | 6 | 2 |
| Pelvic lymphadenectomy, n (%) | 41 (82) | 2 (33.3) | 5 (83.3) | 33 (92) | 1 (50) |
| Para-aortic lymphadenectomy, n (%) | 18 (36) | 1 (16.7) | 1 (16.7) | 16 (44.4) | 0 |
| SNLD, n (%) | 10 (20) | 3 (50) | 0 | 6 (17) | 1 (50) |
| Follow-up (months), median | 90.9 | 28.3 | 141.9 | 97.6 | 10 |
| Radiation Type | |||||
| pEBRT, n (%), N = 42 | 10 (24) | N/A | 3 (50) | 7 (19) | N/A |
| VBT, n (%), N = 42 | 21 (50) | N/A | 2 (33) | 19 (53) | N/A |
| pEBRT + VBT, n (%), N = 42 | 11 (26) | N/A | 1 (17) | 10 (28) | N/A |
| Tumor Characteristics | |||||
| Figo 2009 Stage IA, n (%) | 30 (60) | 4 (67) | 3 (50) | 22 (61.1) | 1 (50) |
| Figo 2009 Stage IB, n (%) | 12 (24) | 2 (33) | 2 (33) | 7 (19.4) | 1 (50) |
| Figo 2009 Stage II, n (%) | 8 (16) | 0 | 1 (17) | 7 (19.4) | 0 |
| ER+ (>5%), n (%), N = 41 | 32 (78) * | 3/6 (50) | 2/4 (50) * | 26/29 (89.7) * | 1/2 (50) |
| PR+ (>5%), n (%), N = 40 | 32 (80) * | 3/6 (50) | 3/4 (75) * | 20/28 (71.4) * | 0/2 |
| P16+, n (%), N = 38 | 38 (100) * | 6/6 (100) | 2/2 (100) * | 28/28 (100) * | 2/2 (100) |
| P53+, n (%), N = 42 | 40 (95.2) * | 6/6 (100) | 4/4 (100) * | 28/30 (93.3) * | 2/2 (100) |
| LVI | |||||
| Negative, n | 23 | 2 | 5 | 16 | 0 |
| Focal, n | 6 | 0 | 0 | 5 | 1 |
| Extensive, n | 21 | 4 | 1 | 15 | 1 |
| First Site of Recurrence | CT (n = 6) N (%) | RT (n = 6) N (%) | CRT (n = 36) N (%) |
|---|---|---|---|
| Loco-regional | 2 (33) | 0 | 0 |
| Distant | 1 (17) | 0 | 8 (22) |
| Loco-regional + distant | 0 | 2 (33) | 1 (3) |
| FIGO 2009 Stage | LVI Status | Adjuvant Treatment | Site(s) of Recurrence | Time to First Recurrence (Months) | Salvage Therapy | Months Alive after Recurrence | Mortality Status |
|---|---|---|---|---|---|---|---|
| IA | Extensive | CRT | Distant (lung, para-aortic LN, inguinal LN, mediastinum) | 82 | CT | 8.5 | Dead |
| II | Extensive | CRT | Distant (field border para-aortic LN) | 10 | RT | 49.4 | Dead |
| II | Extensive | CRT | Distant (lung, non-para-aortic LN) | 14 | Observed | 1.8 | Dead |
| IB | Extensive | CT | Locoregional (vagina, LN) | 10 | Observed | 12.7 | Dead |
| IA | Focal | CRT | Distant (lung, brain) | 39 | SRS to brain only; lung observed | 5.2 | Dead |
| IB | None | CRT | Distant (liver) | 20 | Megestrol and tamoxifen | 16.8 | Dead |
| IA | None | RT | Locoregional (pelvic LN) Distant (peritoneal carcinomatosis) | 14 | CRT | 15.1 | Dead |
| IB | Extensive | CT | Locoregional (vagina) | 12 | Surgery, CT | 20.6 | Dead |
| IA | None | CRT | Locoregional (external iliac LN) Distant (inguinal LN) | 46 | RT | 13 | Dead |
| IA | Extensive | CT | Distant (liver, peritoneal carcinomatosis, para-aortic-, periportal-, hepatogastric LN) | 12 | CT | 5.1 | Dead |
| IA | None | RT | Loco-regional (out-of-field vagina, above-field common iliac LN) Distant (inguinal LN) | 119 | Surgery, CRT | 129.4 | Alive |
| IA | Extensive | CRT | Distant (lung) | 18 | RT | 76.4 | Alive |
| IA | Extensive | CRT | Distant (peritoneal carcinomatosis) | 17 | Chemo | 7.3 | Dead |
| II | Extensive | CRT | Distant (lung) | 24 | Chemo, RUBY trial (placebo vs. dostarlimab) | 24 | Alive |
| Toxicity | None * N | G1 N | G2 N | G3 N | G4 N | G5 N |
|---|---|---|---|---|---|---|
| Acute | ||||||
| GU | 41 | 7 | 0 | 0 | 1 | 0 |
| GI | 12 | 30 | 5 | 2 | 0 | 0 |
| Hematological | 10 | 12 | 15 | 7 | 5 | 0 |
| Late | ||||||
| GU | 43 | 4 | 1 | 0 | 1 | 0 |
| GI | 41 | 6 | 2 | 0 | 0 | 0 |
| Hematological | 36 | 9 | 2 | 2 | 0 | 0 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Akingbade, A.; Fabi, F.; Cartes, R.; Tsui, J.; Alfieri, J. Adjuvant Treatment of Stage I–II Serous Endometrial Cancer: A Single Institution 20-Year Experience. Curr. Oncol. 2024, 31, 3758-3770. https://doi.org/10.3390/curroncol31070277
Akingbade A, Fabi F, Cartes R, Tsui J, Alfieri J. Adjuvant Treatment of Stage I–II Serous Endometrial Cancer: A Single Institution 20-Year Experience. Current Oncology. 2024; 31(7):3758-3770. https://doi.org/10.3390/curroncol31070277
Chicago/Turabian StyleAkingbade, Aquila, François Fabi, Rodrigo Cartes, James Tsui, and Joanne Alfieri. 2024. "Adjuvant Treatment of Stage I–II Serous Endometrial Cancer: A Single Institution 20-Year Experience" Current Oncology 31, no. 7: 3758-3770. https://doi.org/10.3390/curroncol31070277
APA StyleAkingbade, A., Fabi, F., Cartes, R., Tsui, J., & Alfieri, J. (2024). Adjuvant Treatment of Stage I–II Serous Endometrial Cancer: A Single Institution 20-Year Experience. Current Oncology, 31(7), 3758-3770. https://doi.org/10.3390/curroncol31070277





