Dietary Patterns and Quality of Life in Older Adults: A Systematic Review
Abstract
1. Introduction
2. Methods
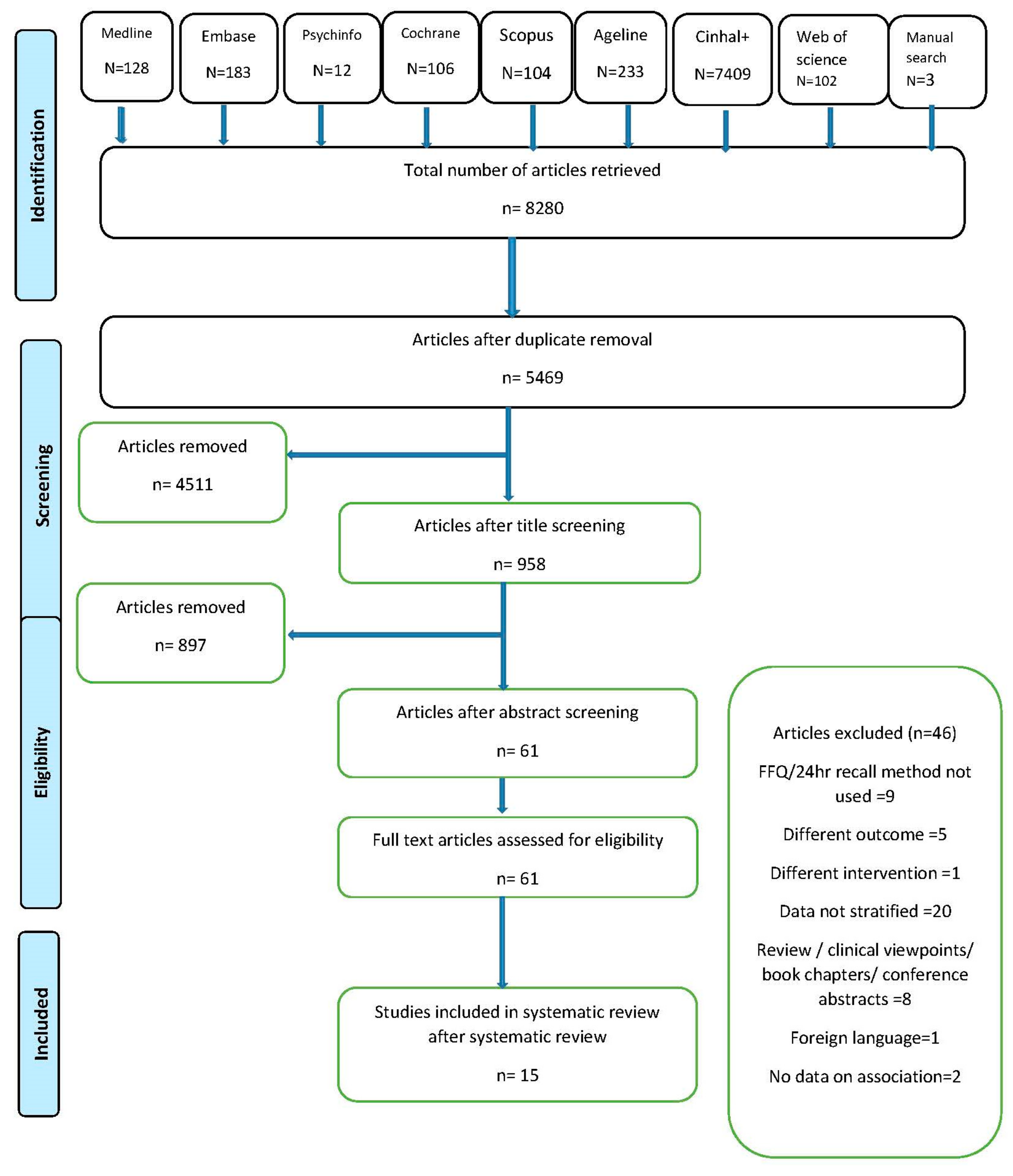
2.1. Search Strategy
2.2. Inclusion and Exclusion Criteria
2.3. Data Extraction
2.4. Overall Quality of Studies
3. Results
4. Discussion
Strengths and Limitations of This Study
5. Recommendations
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- United Nations, Department of Economic and Social Affairs, Population Division. World Population Ageing 2015; (ST/ESA/SER.A/390); United Nations: New York, NY, USA, 2015. [Google Scholar]
- World Health Organization. Whoqol-Bref: Introduction, Administration, Scoring and Generic Version of the Assessment; Programme on Mental Health, World Health Organization: Geneva, Switzerland, 1996. [Google Scholar]
- Felce, D.; Perry, J. Quality of life: Its definition and measurement. Res. Dev. Disabil. 1995, 16, 51–74. [Google Scholar] [CrossRef]
- Dimenas, E.S.; Dahlof, C.G.; Jern, S.C.; Wiklund, I.K. Defining quality of life in medicine. Scand. J. Prim. Health Care 1990, 1 (Suppl.), 7–10. [Google Scholar]
- Rubin, R.R.; Peyrot, M. Quality of life and diabetes. Diabetes Metab. Res. Rev. 1999, 15, 205–218. [Google Scholar] [CrossRef]
- Campos, A.C.; Ferreira, E.F.; Vargas, A.M.; Albala, C. Aging, Gender and Quality of Life (AGEQOL) study: Factors associated with good quality of life in older Brazilian community-dwelling adults. Health Qual. Life Outcomes 2014, 12, 166. [Google Scholar] [CrossRef] [PubMed]
- Kim, H.K.; Hisata, M.; Kai, I.; Lee, S.K. Social support exchange and quality of life among the Korean elderly. J. Cross Cult. Gerontol. 2000, 15, 331–347. [Google Scholar] [CrossRef] [PubMed]
- Gandek, B.; Ware, J.E.; Aaronson, N.K.; Apolone, G.; Bjorner, J.B.; Brazier, J.E.; Bullinger, M.; Kaasa, S.; Leplege, A.; Prieto, L.; et al. Cross-validation of item selection and scoring for the sf-12 health survey in nine countries: Results from the IQOLA project. International quality of life assessment. J. Clin. Epidemiol. 1998, 51, 1171–1178. [Google Scholar] [CrossRef]
- Ware, J.E., Jr.; Sherbourne, C.D. The mos 36-item short-form health survey (SF-36). I. Conceptual framework and item selection. Med. Care 1992, 30, 473–483. [Google Scholar] [CrossRef] [PubMed]
- Alexandre, T.D.S.; Cordeiro, R.C.; Ramos, L.R. Factors associated to quality of life in active elderly. Revista de Saúde Pública 2009, 43, 613–621. [Google Scholar] [CrossRef]
- Pearlman, R.A.; Uhlmann, R.F. Quality of life in chronic diseases: Perceptions of elderly patients. J. Gerontol. 1988, 43, M25–M30. [Google Scholar] [CrossRef] [PubMed]
- Addington-Hall, J.; Kalra, L. Who should measure quality of life? BMJ 2001, 322, 1417–1420. [Google Scholar] [CrossRef] [PubMed]
- Tajvar, M.; Arab, M.; Montazeri, A. Determinants of health-related quality of life in elderly in Tehran, Iran. BMC Public Health 2008, 8, 323. [Google Scholar] [CrossRef] [PubMed]
- Dalton, D.S.; Cruickshanks, K.J.; Klein, B.E.K.; Klein, R.; Wiley, T.L.; Nondahl, D.M. The impact of hearing loss on quality of life in older adults. Gerontologist 2003, 43, 661–668. [Google Scholar] [CrossRef] [PubMed]
- Locker, D.; Matear, D.; Stephens, M.; Jokovic, A. Oral health-related quality of life of a population of medically compromised elderly people. Community Dent. Health 2002, 19, 90–97. [Google Scholar] [PubMed]
- Bize, R.; Johnson, J.A.; Plotnikoff, R.C. Physical activity level and health-related quality of life in the general adult population: A systematic review. Prev. Med. 2007, 45, 401–415. [Google Scholar] [CrossRef] [PubMed]
- Amarantos, E.; Martinez, A.; Dwyer, J. Nutrition and quality of life in older adults. J. Gerontol. A Biol. Sci. Med. Sci. 2001, 56, 54–64. [Google Scholar] [CrossRef] [PubMed]
- Keller, H.H.; Østbye, T.; Goy, R. Nutritional risk predicts quality of life in elderly community-living Canadians. J. Gerontol. A Biol. Sci. Med. Sci. 2004, 59, M68–M74. [Google Scholar] [CrossRef]
- Darwiche, G.; Höglund, P.; Roth, B.; Larsson, E.; Sjöberg, T.; Wohlfart, B.; Steen, S.; Ohlsson, B. An Okinawan-based Nordic diet improves anthropometry, metabolic control, and health-related quality of life in Scandinavian patients with type 2 diabetes: A pilot trial. Food Nutr. Res. 2016, 60. [Google Scholar] [CrossRef] [PubMed]
- Ruano, C.; Henriquez, P.; Martínez-González, M.Á.; Bes-Rastrollo, M.; Ruiz-Canela, M.; Sánchez-Villegas, A. Empirically derived dietary patterns and health-related quality of life in the sun project. PLoS ONE 2013, 8, e61490. [Google Scholar] [CrossRef] [PubMed]
- Veronese, N.; Stubbs, B.; Noale, M.; Solmi, M.; Luchini, C.; Maggi, S. Adherence to the Mediterranean diet is associated with better quality of life: Data from the osteoarthritis initiative Am. J. Clin. Nutr. 2016, 104, 1403–1409. [Google Scholar] [CrossRef] [PubMed]
- Perez-Tasigchana, R.F.; Leon-Munoz, L.M.; Lopez-Garcia, E.; Banegas, J.R.; Rodriguez-Artalejo, F.; Guallar-Castillon, P. Mediterranean diet and health-related quality of life in two cohorts of community-dwelling older adults. PLoS ONE 2016, 11, e0151596. [Google Scholar]
- Kiefte-De Jong, J.C.; Mathers, J.C.; Franco, O.H. Nutrition and healthy ageing: The key ingredients. Proc. Nutr. Soc. 2014, 73, 249–259. [Google Scholar] [CrossRef] [PubMed]
- Mathers, J.C. Food, nutrition and healthy ageing. Food Sci. Technol. 2013, 27, 34–36. [Google Scholar]
- Hu, F.B. Dietary pattern analysis: A new direction in nutritional epidemiology. Curr. Opin. Lipidol. 2002, 13, 3–9. [Google Scholar] [CrossRef] [PubMed]
- Fung, T.T.; Rimm, E.B.; Spiegelman, D.; Rifai, N.; Tofler, G.H.; Willett, W.C.; Hu, F.B. Association between dietary patterns and plasma biomarkers of obesity and cardiovascular disease risk. Am. J. Clin. Nutr. 2001, 73, 61–67. [Google Scholar] [CrossRef] [PubMed]
- Dietary Guidelines Advisory Committee. Scientific Report of the 2015 Dietary Guidelines Advisory Committee; Departments of Health and Human Services, Ed.; United States Department of Agriculture (USDA): Washington, DC, USA, 2015. [Google Scholar]
- Tucker, K.L. Dietary patterns, approaches, and multicultural perspective, Can we identify culture-specific healthful dietary patterns among diverse populations undergoing nutrition transition? Appl. Physiol. Nutr. Metab. 2010, 35, 211–218. [Google Scholar] [CrossRef] [PubMed]
- McNaughton, S.A. Dietary patterns and diet quality: Approaches to assessing complex exposures in nutrition. Australas Epidemiol. 2010, 17, 35–37. [Google Scholar]
- Evidence Analysis Library Division, Centre for Nutrition Policy and Promotion. A Series of Systematic Reviews on the Relationship between Dietary Patterns and Health Outcomes; 2014. Available online: https://www.cnpp.usda.gov/nutrition-evidence-library-dietary-patterns-systematic-review-project (accessed on 3 March 2018).
- Mohammadifard, N.; Talaei, M.; Sadeghi, M.; Oveisegharan, S.; Golshahi, J.; Esmaillzadeh, A.; Sarrafzadegan, N. Dietary patterns and mortality from cardiovascular disease: Isfahan cohort study. Eur. J. Clin. Nutr. 2017, 71, 252–258. [Google Scholar] [CrossRef] [PubMed]
- Livingstone, K.M.; McNaughton, S.A. Dietary patterns by reduced rank regression are associated with obesity and hypertension in Australian adults. Br. J. Nutr. 2017, 117, 248–259. [Google Scholar] [CrossRef] [PubMed]
- Lee, H.S.; Lee, K.B.; Hyun, Y.Y.; Chang, Y.; Ryu, S.; Choi, Y. Dash dietary pattern and chronic kidney disease in elderly Korean adults. Eur. J. Clin. Nutr. 2017, 71, 755–761. [Google Scholar] [CrossRef] [PubMed]
- Asghari, G.; Yuzbashian, E.; Mirmiran, P.; Hooshmand, F.; Najafi, R.; Azizi, F. Dietary approaches to stop hypertension (dash) dietary pattern is associated with reduced incidence of metabolic syndrome in children and adolescents. J. Pediatr. 2016, 174, 178–184.e171. [Google Scholar] [CrossRef] [PubMed]
- Adriano, L.S.; Sampaio, H.A.; Arruda, S.P.; Portela, C.L.; Melo, M.L.; Carioca, A.A.; Soares, N.T. Healthy dietary pattern is inversely associated with non-alcoholic fatty liver disease in elderly. Br. J. Nutr. 2016, 115, 2189–2195. [Google Scholar] [CrossRef] [PubMed]
- Myles, I.A. Fast food fever: Reviewing the impacts of the Western diet on immunity. Nutr. J. 2014, 13, 61. [Google Scholar] [CrossRef] [PubMed]
- Brigham, E.P.; Kolahdooz, F.; Hansel, N.; Breysse, P.N.; Davis, M.; Sharma, S.; Matsui, E.C.; Diette, G.; McCormack, M.C. Association between Western diet pattern and adult asthma: A focused review. Ann. Allergy Asthma Immunol. 2015, 114, 273–280. [Google Scholar] [CrossRef] [PubMed]
- Danaei, G.; Singh, G.M.; Paciorek, C.J.; Lin, J.K.; Cowan, M.J.; Finucane, M.M.; Farzadfar, F.; Stevens, G.A.; Riley, L.M.; Lu, Y.; et al. The global cardiovascular risk transition: Associations of four metabolic risk factors with national income, urbanization, and western diet in 1980 and 2008. Circulation 2013, 127, 1493–1502. [Google Scholar] [CrossRef] [PubMed]
- O’Dea, K. Diabetes in Australian Aborigines: Impact of the western diet and life style. J. Intern. Med. 1992, 232, 103–117. [Google Scholar] [CrossRef] [PubMed]
- Slattery, M.L.; Potter, J.D.; Ma, K.N.; Caan, B.J.; Leppert, M.; Samowitz, W. Western diet, family history of colorectal cancer, nat2, gstm-1 and risk of colon cancer. Cancer Causes Control 2000, 11, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Iqbal, R.; Anand, S.; Ounpuu, S.; Islam, S.; Zhang, X.; Rangarajan, S.; Chifamba, J.; Al-Hinai, A.; Keltai, M.; Yusuf, S. Dietary patterns and the risk of acute myocardial infarction in 52 countries. Results of the INTERHEART Study. Circulation 2008, 118, 1929–1937. [Google Scholar] [CrossRef] [PubMed]
- Marshall, T.A.; Stumbo, P.J.; Warren, J.J.; Xie, X.-J. Inadequate nutrient intakes are common and are associated with low diet variety in rural, community-dwelling elderly. J. Nutr. 2001, 131, 2192–2196. [Google Scholar] [CrossRef] [PubMed]
- Sharkey, J.R.; Branch, L.G.; Zohoori, N.; Giuliani, C.; Busby-Whitehead, J.; Haines, P.S. Inadequate nutrient intakes among homebound elderly and their correlation with individual characteristics and health-related factors. Am. J. Clin. Nutr. 2002, 76, 1435–1445. [Google Scholar] [CrossRef] [PubMed]
- Ryan, A.S.; Craig, L.D.; Finn, S.C. Nutrient intakes and dietary patterns of older Americans: A national study. J. Gerontol. 1992, 47, M145–M150. [Google Scholar] [CrossRef] [PubMed]
- Ho, S.C.; Donnan, S.; Sham, A. Dietary intake among elderly Chinese in Hong Kong. J. Hum. Nutr. Diet. 1988, 1, 205–215. [Google Scholar] [CrossRef]
- Agarwalla, R.; Saikia, A.M.; Baruah, R. Assessment of the nutritional status of the elderly and its correlates. J. Fam. Community Med. 2015, 22, 39–43. [Google Scholar] [CrossRef] [PubMed]
- Han, Y.; Li, S.; Zheng, Y. Predictors of nutritional status among community-dwelling older adults in Wuhan, China. Public Health Nutr. 2009, 12, 1189–1196. [Google Scholar] [CrossRef] [PubMed]
- Mokhber, N.; Majdi, M.R.; Ali-Abadi, M.; Shakeri, M.T.; Kimiagar, M.; Salek, R.; Moghaddam, P.A.; Sakhdari, A.; Azimi-Nezhad, M.; Ghayour-Mobarhan, M.; et al. Association between malnutrition and depression in elderly people in Razavi Khorasan: A population based-study in Iran. Iran. J. Public Health 2011, 40, 67–74. [Google Scholar] [PubMed]
- Watanabe, R.; Hanamori, K.; Kadoya, H.; Nishimuta, M.; Miyazaki, H. Nutritional intakes in community-dwelling older japanese adults: High intakes of energy and protein based on high consumption of fish, vegetables and fruits provide sufficient micronutrients. J. Nutr. Sci. Vitaminol. 2004, 50, 184–195. [Google Scholar] [CrossRef] [PubMed]
- Nnakwe, N.E. Nutrient intakes of healthy independent living elderly persons consuming self-selected diets. FASEB J. 1997, 11, 1095. [Google Scholar]
- Elsner, R.J. Changes in eating behavior during the aging process. Eat Behav. 2002, 3, 15–43. [Google Scholar] [CrossRef]
- Shahar, D.R.; Schultz, R.; Shahar, A.; Wing, R.R. The effect of widowhood on weight change, dietary intake, and eating behavior in the elderly population. J. Aging Health 2001, 13, 186–199. [Google Scholar] [CrossRef]
- Rosenbloom, C.A.; Whittington, F.J. The effects of bereavement on eating behaviors and nutrient intakes in elderly widowed persons. J. Gerontol. 1993, 48, S223–S229. [Google Scholar] [CrossRef] [PubMed]
- McIntosh, W.A.; Shifflett, P.A.; Picou, J.S. Social support, stressful events, strain, dietary intake, and the elderly. Med. Care 1989, 27, 140–153. [Google Scholar] [CrossRef] [PubMed]
- Nicklett, E.J.; Kadell, A.R. Fruit and vegetable intake among older adults: A scoping review. Maturitas 2013, 75, 305–312. [Google Scholar] [CrossRef] [PubMed]
- Oros, R.I.; Popescu, C.A.; Iova, S.O.; Mihancea, P.; Iova, C.A. Depression, activities of daily living and quality of life in elderly stroke patients. Hum. Vet. Med. 2016, 8, 24–28. [Google Scholar]
- Neto, J.A.F.; Reis, L.M.C.B.; Veras, M.R.; Queiroz, L.L.C.; Nunes, K.P.L.N.; Miranda, P.O.; Santos, A.F.D.; Nunes, J.K.V.R.S. Impact of cardiovascular interventions on the quality of life in the elderly. Braz. J. Cardiovasc. Surg. 2015, 30, 626–630. [Google Scholar]
- Liu, M.H.; Wang, C.H.; Huang, Y.Y.; Cherng, W.J.; Wang, K.W.K. A correlational study of illness knowledge, self-care behaviors, and quality of life in elderly patients with heart failure. J. Nurs. Res. 2014, 22, 136–145. [Google Scholar] [CrossRef] [PubMed]
- Tarride, J.E.; Burke, N.; Leslie, W.D.; Morin, S.N.; Adachi, J.D.; Papaioannou, A.; Bessette, L.; Brown, J.P.; Pericleous, L.; Muratov, S.; et al. Loss of health related quality of life following low-trauma fractures in the elderly. BMC Geriatr. 2016, 16, 84. [Google Scholar] [CrossRef] [PubMed]
- Assaf, A.R.; Beresford, S.A.; Risica, P.M.; Aragaki, A.; Brunner, R.L.; Bowen, D.J.; Naughton, M.; Rosal, M.C.; Snetselaar, L.; Wenger, N. Low-fat dietary pattern intervention and health-related quality of life: The Women’s Health Initiative randomized controlled dietary modification trial. J. Acad. Nutr. Diet. 2016, 116, 259–271. [Google Scholar] [CrossRef] [PubMed]
- Thomas, B.H.; Ciliska, D.; Dobbins, M.; Micucci, S. A process for systematically reviewing the literature: Providing the research evidence for public health nursing interventions. Worldviews Evid. Based Nurs. 2004, 1, 176–184. [Google Scholar] [CrossRef] [PubMed]
- Armijo-Olivo, S.; Stiles, C.R.; Hagen, N.A.; Biondo, P.D.; Cummings, G.G. Assessment of study quality for systematic reviews: A comparison of the Cochrane Collaboration risk of bias tool and the effective public health practice project quality assessment tool: Methodological research. J. Eval. Clin. Pract. 2012, 18, 12–18. [Google Scholar] [CrossRef] [PubMed]
- Shamseer, L.; Moher, D.; Clarke, M.; Ghersi, D.; Liberati, A.; Petticrew, M.; Shekelle, P.; Stewart, L.A. Preferred reporting items for systematic review and meta-analysis protocols (prisma-p) 2015: Elaboration and explanation. BMJ 2015, 349. [Google Scholar] [CrossRef] [PubMed]
- Moher, D.; Liberati, A.; Tetzlaff, J.; Altman, D.G. Preferred reporting items for systematic reviews and meta-analyses: The prisma statement. PLoS Med. 2009, 6, e1000097. [Google Scholar] [CrossRef] [PubMed]
- Rifai, L.; Pisano, C.; Hayden, J.; Sulo, S.; Silver, M.A. Impact of the dash diet on endothelial function, exercise capacity, and quality of life in patients with heart failure. Bayl. Univ. Med. Center Proc. 2015, 28, 151–156. [Google Scholar] [CrossRef]
- Woo, J.; Chan, R.; Leung, J.; Wong, M. Relative contributions of geographic, socioeconomic, and lifestyle factors to quality of life, frailty, and mortality in elderly. PLoS ONE 2010, 5. [Google Scholar] [CrossRef] [PubMed]
- Haveman-Nies, A.; de Groot, L.C.P.; van Staveren, W.A. Relation of dietary quality, physical activity, and smoking habits to 10-year changes in health status in older Europeans in the Seneca study. Am. J. Public Health 2003, 93, 318–323. [Google Scholar] [CrossRef] [PubMed]
- Schlesinger, S.; Walter, J.; Hampe, J.; von Schonfels, W.; Hinz, S.; Kuchler, T.; Jacobs, G.; Schafmayer, C.; Nothlings, U. Lifestyle factors and health-related quality of life in colorectal cancer survivors. Cancer Causes Control 2014, 25, 99–110. [Google Scholar] [CrossRef] [PubMed]
- Gopinath, B.; Russell, J.; Flood, V.M.; Burlutsky, G.; Mitchell, P. Adherence to dietary guidelines positively affects quality of life and functional status of older adults. J. Acad. Nutr. Diet. 2014, 114, 220–229. [Google Scholar] [CrossRef] [PubMed]
- Milte, C.M.; Thorpe, M.G.; Crawford, D.; Ball, K.; McNaughton, S.A. Associations of diet quality with health-related quality of life in older Australian men and women. Exp. Gerontol. 2015, 64, 8–16. [Google Scholar] [CrossRef] [PubMed]
- Zaragoza-Martí, A.; Ferrer-Cascales, R.; Hurtado-Sánchez, J.A.; Laguna-Pérez, A.; Cabañero-Martínez, M.J. Relationship between adherence to the Mediterranean diet and health-related quality of life and life satisfaction among older adults. J. Nutr. Health Aging 2018, 22, 89–96. [Google Scholar] [CrossRef] [PubMed]
- Lewis, C.M.; Wolf, W.A.; Xun, P.; Sandler, R.S.; He, K. Racial differences in dietary changes and quality of life after a colorectal cancer diagnosis: A follow-up of the study of outcomes in colorectal cancer survivors cohort. Am. J. Clin. Nutr. 2016, 103, 1523–1530. [Google Scholar] [CrossRef] [PubMed]
- Alcubierre, N.; Martinez-Alonso, M.; Valls, J.; Rubinat, E.; Traveset, A.; Hernández, M.; Martínez-González, M.D.; Granado-Casas, M.; Jurjo, C.; Vioque, J.; et al. Relationship of the adherence to the Mediterranean diet with health-related quality of life and treatment satisfaction in patients with type 2 diabetes mellitus: A post-hoc analysis of a cross-sectional study. Health Qual. Life Outcomes 2016, 14, 1–6. [Google Scholar] [CrossRef] [PubMed]
- Sanchez-Aguadero, N.; Alonso-Dominguez, R.; Garcia-Ortiz, L.; Agudo-Conde, C.; Rodriguez-Martin, C.; de Cabo-Laso, A.; Sanchez-Salgado, B.; Ramos, R.; Maderuelo-Fernandez, J.A.; Gomez-Marcos, M.A.; et al. Diet and physical activity in people with intermediate cardiovascular risk and their relationship with the health-related quality of life: Results from the mark study. Health Qual. Life Outcomes 2016, 14, 169. [Google Scholar] [CrossRef] [PubMed]
- Mosher, C.E.; Sloane, R.; Morey, M.C.; Snyder, D.C.; Cohen, H.J.; Miller, P.E.; Demark-Wahnefried, W. Associations between lifestyle factors and quality of life among older long-term breast, prostate, and colorectal cancer survivors. Cancer 2009, 115, 4001–4009. [Google Scholar] [CrossRef] [PubMed]
- Ford, D.W.; Jensen, G.L.; Still, C.; Wood, C.; Mitchell, D.C.; Erickson, P.; Bailey, R.; Smiciklas-Wright, H.; Coffman, D.L.; Hartman, T.J. The associations between diet quality, body mass index (BMI) and health and activity limitation index (halex) in the Geisinger Rural Aging Study (GRAS). J. Nutr. Health Aging 2014, 18, 167–170. [Google Scholar] [CrossRef] [PubMed]
- Samieri, C.; Jutand, M.-A.; Féart, C.; Capuron, L.; Letenneur, L.; Barberger-Gateau, P. Dietary patterns derived by hybrid clustering method in older people: Association with cognition, mood, and self-rated health. J. Am. Diet. Assoc. 2008, 108, 1461–1471. [Google Scholar] [CrossRef] [PubMed]
- Trichopoulou, A.; Orfanos, P.; Norat, T.; Bueno-de-Mesquita, B.; Ocké, M.C.; Peeters, P.H.M.; van der Schouw, Y.T.; Boeing, H.; Hoffmann, K.; Boffetta, P.; et al. Modified mediterranean diet and survival: Epic-elderly prospective cohort study. BMJ 2005, 330, 991. [Google Scholar] [CrossRef] [PubMed]
- Schroder, H.; Fito, M.; Estruch, R.; Martinez-Gonzalez, M.A.; Corella, D.; Salas-Salvado, J.; Lamuela-Raventos, R.; Ros, E.; Salaverria, I.; Fiol, M.; et al. A short screener is valid for assessing mediterranean diet adherence among older Spanish men and women. J. Nutr. 2011, 141, 1140–1145. [Google Scholar] [CrossRef] [PubMed]
- Panagiotakos, D.B.; Pitsavos, C.; Stefanadis, C. Dietary patterns: A mediterranean diet score and its relation to clinical and biological markers of cardiovascular disease risk. Nutr. Metab. Cardiovasc. Dis. 2006, 16, 559–568. [Google Scholar] [CrossRef] [PubMed]
- Buckland, G.; González, C.A.; Agudo, A.; Vilardell, M.; Berenguer, A.; Amiano, P.; Ardanaz, E.; Arriola, L.; Barricarte, A.; Basterretxea, M.; et al. Adherence to the Mediterranean diet and risk of coronary heart disease in the Spanish EPIC cohort study. Am. J. Epidemiol. 2009, 170, 1518–1529. [Google Scholar] [CrossRef] [PubMed]
- National Health and Medical Research Council. Dietary Guidelines for Australian Adults; National Health and Medical Research Council: Canberra, Australia, 2003. [Google Scholar]
- Folsom, A.R.; Parker, E.D.; Harnack, L.J. Degree of concordance with DASH diet guidelines and incidence of hypertension and fatal cardiovascular disease. Am. J. Hypertens. 2007, 20, 225–232. [Google Scholar] [CrossRef] [PubMed]
- Lai, J.S.; Hiles, S.; Bisquera, A.; Hure, A.J.; McEvoy, M.; Attia, J. A systematic review and meta-analysis of dietary patterns and depression in community-dwelling adults. Am. J. Clin. Nutr. 2013, 99, 181–197. [Google Scholar] [CrossRef] [PubMed]
- Magalhães, B.; Peleteiro, B.; Lunet, N. Dietary patterns and colorectal cancer: Systematic review and meta-analysis. Eur. J. Cancer Prev. 2012, 21, 15–23. [Google Scholar] [CrossRef] [PubMed]
- Brennan, S.F.; Cantwell, M.M.; Cardwell, C.R.; Velentzis, L.S.; Woodside, J.V. Dietary patterns and breast cancer risk: A systematic review and meta-analysis. Am. J. Clin. Nutr. 2010, 91, 1294–1302. [Google Scholar] [CrossRef] [PubMed]
- Kant, A.K. Dietary patterns and health outcomes. J. Am. Diet. Assoc. 2004, 104, 615–635. [Google Scholar] [CrossRef] [PubMed]
- Milte, C.M.; McNaughton, S.A. Dietary patterns and successful ageing: A systematic review. Eur. J. Nutr. 2016, 55, 423–450. [Google Scholar] [CrossRef] [PubMed]
- Guenther, P.M.; Kirkpatrick, S.I.; Reedy, J.; Krebs-Smith, S.M.; Buckman, D.W.; Dodd, K.W.; Casavale, K.O.; Carroll, R.J. The healthy eating index-2010 is a valid and reliable measure of diet quality according to the 2010 dietary guidelines for Americans. J. Nutr. 2014, 144, 399–407. [Google Scholar] [CrossRef] [PubMed]
- Patterson, R.E.; Haines, P.S.; Popkin, B.M. Diet quality index: Capturing a multidimensional behavior. J. Am. Diet. Assoc. 1994, 94, 57–64. [Google Scholar] [CrossRef]
- Kim, S.; Haines, P.S.; Siega-Riz, A.M.; Popkin, B.M. The diet quality index-international (dqi-i) provides an effective tool for cross-national comparison of diet quality as illustrated by China and the United States. J. Nutr. 2003, 133, 3476–3484. [Google Scholar] [CrossRef] [PubMed]
- Willett, W.C. Overview and perspective in human nutrition. Asia Pac. J. Clin. Nutr. 2008, 17, 1–4. [Google Scholar] [PubMed]
- Klipstein-Grobusch, K.; den Breeijen, J.H.; Goldbohm, R.A.; Geleijnse, J.M.; Hofman, A.; Grobbee, D.E.; Witteman, J.C. Dietary assessment in the elderly: Validation of a semiquantitative food frequency questionnaire. Eur. J. Clin. Nutr. 1998, 52, 588–596. [Google Scholar] [CrossRef] [PubMed]
- Bauer, J.M.; Kaiser, M.J.; Sieber, C.C. Evaluation of nutritional status in older persons: Nutritional screening and assessment. Curr. Opin. Clin. Nutr. Metab. Care 2010, 13, 8–13. [Google Scholar] [CrossRef] [PubMed]
- Van Staveren, W.A.; de Groot, L.C.; Blauw, Y.H.; van der Wielen, R.P. Assessing diets of elderly people: Problems and approaches. Am J. Clin. Nutr. 1994, 59, 221s–223s. [Google Scholar] [CrossRef] [PubMed]
- Ortiz-Andrellucchi, A.; Sanchez-Villegas, A.; Doreste-Alonso, J.; de Vries, J.; de Groot, L.; Serra-Majem, L. Dietary assessment methods for micronutrient intake in elderly people: A systematic review. BJN 2009, 102 (Suppl. 1), S118–S149. [Google Scholar] [CrossRef] [PubMed]
- De Vries, J.H.; de Groot, L.C.; van Staveren, W.A. Dietary assessment in elderly people: Experiences gained from studies in the Netherlands. Eur. J. Clin. Nutr. 2009, 63 (Suppl. 1), S69–S74. [Google Scholar] [CrossRef] [PubMed]
- Honda, M.; Wakita, T.; Onishi, Y.; Nunobe, S.; Miura, A.; Nishigori, T.; Kusanagi, H.; Yamamoto, T.; Boddy, A.; Fukuhara, S. Development and validation of a disease-specific instrument to measure diet-targeted quality of life for postoperative patients with esophagogastric cancer. Ann. Surg. Oncol. 2015, 22, 848–854. [Google Scholar] [CrossRef] [PubMed]
- Grunert, K.G.; Dean, M.; Raats, M.M.; Nielsen, N.A.; Lumbers, M. A measure of satisfaction with food-related life. Appetite 2007, 49, 486–493. [Google Scholar] [CrossRef] [PubMed]
| Study and Setting | Study Design | Sample Size | Mean Age 1 | (A)Dietary Intake Assessment (B) Pattern Analysis Method (C) Adjustment Variables | QoL Measure | Results | Study Quality 2 |
|---|---|---|---|---|---|---|---|
| Woo, J. et al. [66] Hong Kong | Cross sectional | 3378 | 72.5 ± 5.2 | (A):FFQ (B): DQI-I with 4 aspects—variety, adequacy, moderation and overall balance: Range 0–94, high scores better quality (C): Age, sex, socioeconomic status and districts | SF-12 | Better dietary quality is associated with better self-rated physical and mental health. PCS: β = 0.0689 (p < 0.0001) MCS: β = 0.0693 (p < 0.0001) | moderate |
| Haveman-Nies et al., SENECA [67] Europe (Belgium, Denmark, Italy, The Netherlands, Portugal, Spain and Switzerland) | Longitudinal | 480 | 72.6 ± 1.6 | (A) Diet history (B) Modified Mediterranean score: Range 0–7, high scores indicate better quality. (C): Age, country | Self-rated health status | No association observed between diet quality and risk of deterioration of health status. Risk of deterioration in health status resulting from low dietary quality: OR (95% CI): Men 1.1 (0.5, 2.3); women 1.4 (0.7, 2.7) | weak |
| Schlesinger et al. [68] Northern Germany | Cross sectional | 1389 | 69 (64–73) | (A): 112 item web-based FFQ/ (B): Dietary Index: Two indices namely ’favorable‘ and ’unfavorable‘ were generated (C): Age sex and SES | EORTC QLQ-C30 | Those with a favorable’ diet had a reduced odds of having a low gHRQoL; OR (95% CI): 0.79 (0.63–0.99) | moderate |
| Perez-Tasigchana et al., UAM-cohort, & Seniors-ENRICA [22] Spain | Longitudinal | 2376 | ≥60 | (A):14 item paper-based FFQ (B): Mediterranean dietary pattern index (UAM-MDP): Range −2 to 6, low score indicates less healthy diet. (C): Age, sex, level of education, smoking, BMI, physical activity, comorbidities | SF-36 (Spanish version) | No significant association between UAM-MDP and PCS and MCS. | strong |
| 1911 | ≥60 | (A): Dietary history-Enrica (B): PREDIMED score: Range 0–14 high scores better adherence MDS :Range 0–9 high scores better adherence (C): Age, sex, level of education, smoking, BMI, physical activity, comorbidities | SF-12 | Higher PREDIMED score was associated with slightly better PCS score. Compared to those in the lowest tertile, PCS: b = 0.55 (−0.48 to 1.59) for tertile 2, 1.34 (0.21 to 2.47) for tertile 3PREDIMED score not significantly associated with a better MCS score. [/MCS: tertile 2, b = −0.25 (−1.31 to 0.80) and tertile 3, b = 0.56 (−0.58 to 1.71)] | |||
| MDS not associated with PCS or MCS | |||||||
| Gopinath et al., BMES [69] Australia | Longitudinal | 895 | 67.1 ± 7.4 | (A): 145 item FFQ (B): Total Diet Score to assess adherence to dietary guidelines for Australian adults: Range 0–20, higher scores better adherence (C): Age, sex, receipt of pension payment, home ownership, admission to hospitals, walking disability, living alone, 5 or more co morbidities, cognitive and visual impairment | SF-36 and FACT-C | Adherence to dietary guidelines at baseline was associated with significantly better QoL in four domains after 5 years. Participants in the highest vs. lowest quartile of baseline total diet scores had adjusted mean scores 5.6, 4.0, 5.3, and 2.6 units higher in these SF36 domains 5 years later | moderate |
| Milte et al., WELL [70] Australia | Longitudinal | 2457 | 59.9 (65–55) | (A): 111 item FFQ (B): DGI: Range 0–130 higher scores reflect greater compliance with dietary guidelines RFS: Range 0–49, with higher scores associated with greater diet quality MDS: Range 0–8, higher scores reflecting greater adherence to Mediterranean diet. (C): Model 1: adjusted for age, sex, education and urban/rural location. Model 2: additionally adjusted for smoking and total physical activity. Model 3: additionally adjusted for BMI | RAND 36 | Older adults with better quality diets report better health-related QoL, with additional associations with emotional wellbeing observed in women. Better diet quality by DGI was associated with better self-reported HRQoL on the physical function (OR = 1.56, 95% confidence intervals (CI): 1.22–1.99), bodily pain (OR = 1.29, CI: 1.01, 1.63), general health (OR = 1.72, CI: 1.36, 2.19), energy (OR = 1.51, CI: 1.19, 1.92), emotional wellbeing (OR = 1.36, CI: 1.08, 1.72) and PCS (OR = 1.46, CI: 1.15, 1.86). | strong |
| A higher RFS was associated with better HRQoL on the physical function (OR = 1.43, CI: 1.13–1.82), general health (OR = 1.41, CI: 1.12, 1.78), energy (OR = 1.55, CI: 1.22, 1.96) and emotional wellbeing (OR = 1.41, CI: 1.12, 1.77) | |||||||
| MDS score in the top quartile was associated with a better score on the energy scale (OR = 1.53, CI: 1.11, 2.10). An association between MDS and general health was also observed after adjustment for smoking and physical activity (OR = 1.52, CI: 1.11, 2.08) | |||||||
| Zaragoza-marti et al. [71] Spain | Cross sectional | 351 | 71.06 | (A): MEDIS-FFQ (B): MDS: Range 0–9, higher the score higher the adherence (C): Age, hours of physical activity, educational level, BMI, blood cholesterol, blood glucose levels and blood pressure | SF 12 | Adherence to MD is positively related to both PCS and MCS of SF12 for both sexes. Regression coefficients for the relationship between Mediterranean diet score with women (MCS (0.07, CI:(−0.96–0.23, p < 0.001) and PCS (0.19, CI (0.04–0.34, p = 0.020)) and men (MCS (0.01, CI: −0.12–0.29, p = 0.004 and PCS (0.05, CI: 0.17–0.20, p = 0.060)) | moderate |
| Veronese et al., Osteoarthritis Initiative [21] United States | Cross sectional (sub study of a large longitudinal study) | 4470 | 61.3 ± 9.2 | (A): 77 item Block brief 2000 FFQ (B): Modified MDS: Range: 0–55 high scores better adherence (C): Age, sex, race, BMI, education, smoking status, total energy intake, Charlson co morbidity index, use of analgesic drugs, annual income | SF-12 | Higher adherence to med diet is associated with better QOL. Those with higher aMED showed significantly higher PCS (quintile 5: 50 ± 8.5 compared to quintile 1: 47.2 ± 9.8; p < 0.0001) and MCS (quintile 5: 54.5 ± 7.6 compared to quintile 1: 53.2 ± 8.8; p < 0.0001) | moderate |
| Lewis et al. [72] United States | Longitudinal | 265 | 64.5 ± 10.3 (Caucasians)/60.7 ± 10.2 (African American) | (A): 44 item Diet history questionnaire (B): Dietary index scored from −30 to 30 Higher scores better adherence. (C): Age, sex, follow up time, education, Socio economic factors, BMI, alcohol consumption, smoking and physical activity | SF-12 | Subjects who improved dietary quality exhibited positive changes in QOL-significant changes observed in functional wellbeing (0.14, CI: 0.05–0.07, p ≤ 0.01), functional assessment of cancer therapy-general total score (0.19, CI: 0.01, 0.37, p = 0.04) and Physical composite score of SF12 (0.23,CI: 0.05–0.41, p = 0.01) | strong |
| Alcubierre et al. [73] Spain | Cross sectional | 294 (146 DR and 148 NDR) | No Diabetic retinopathy: 57.9 ± 10.3 | (A) Semi quantitative FFQ 101 items (B): rMED: Range, 0–18 Adherence was rated as low (0–6), medium (7–10) and high (11–18) (C):Adjustments varied for different components of the QoL domain and included age, ethnicity, insulin treatment, retinopathy, diabetes duration another diabetes related factors | ADDQOL-19 | rMED was significantly associated with HRQOL dimensions of travels, self-confidence, freedom to eat and freedom to drink. rMED > 8, positively associated with self confidence (p = 0.015), freedom to eat 0.839 (p = 0.037) and freedom to drink 1.150 (p = 0.015) | moderate |
| Diabetic retinopathy: 60.5 ± 8.8 | |||||||
| Rifai et al. [65] United States | Randomised controlled trial | 48 | DASH group (60) and comparison group (64) | (A): FFQ/food diaries (B): DASH diet index: Range 0 to 11, with higher scores indicating higher levels of concordance. (C): N/A | MLHF | Adhering to the DASH diet improved QoL scores at 3 months; improved MLHFQ scores at 3-month follow-up (21 vs. 39; p = 0.006) | strong |
| Sanchez-Aguadero et al. MARK study [74] Spain | Longitudinal | 314 | 61.1 ± 8.4 (35–74) | (A): FFQ with 18 food groups divided into three categories (B): DQI: Range 18–54, with higher scores associated with better diet quality. aMED: Score ≥ 5 meaning good compliance (C): Age, sex, hypertension, dyslipidaemia and Charlson Comorbidity Index | Spanish version of the SF-12 v.2 | In those at intermediate cardiovascular risk, DQI was directly related to the mental component score (r = 0.127, p < 0.05) and mental health (r = 0.121, p < 0.05), in bivariate analyses | moderate |
| Greater adherence to the Mediterranean diet was associated with higher scores on the SF-12 mental component, social functioning and vitality and DQI showed an association with the mental component score. Bivariate correlation: The Mediterranean Diet (total score) was related to the mental component (r = 0.164, p < 0.01) as well as social functioning (r = 0.172, p < 0.01) and vitality (r = 0.122, p < 0.05). Multiple linear regression: 1.177 point increase in the mental component for each increase of 1 point in the Mediterranean diet adherence score (p < 0.01), Vitality (β = 0.958 and 0.990) and Social Functioning (p < 0.05 and p < 0.01) domains maintained association post adjustments. | |||||||
| Mosher et al., RENEW [75] United States, UK and Canada | Cross sectional | 641 | 73 ± 5 | (A): 24 h dietary recalls (B): HEI05: Range 0–100 with scores above 80 indicating good diet quality. (C): age, race, level of education, and number of comorbidities | SF-36 | Diet quality was positively associated with physical functioning (β = 0.10, Ps < 0.005) and vitality (β = 0.095, Ps = 0.01) | moderate |
| Ford et al., GRAS [76] United States | Cross sectional | 4009 | Males: 81.3 ± 4.2, Females: 81.5 ± 4.5 | (A): DST (B): HEI 05: Range :0–100 (<60 considered “unhealthy”, 60–75 “borderline”, and >75 “healthy”) (C): BMI, disease burden, sex, education, age, smoking status, living situation and self-vs. proxy report | HALex | Poor diet quality, as assessed by the DST, is associated with lower HRQoL. HALex scores were significantly lower for participants with dietary intakes categorized as unhealthy (<60) (0.70, 95% CI 0.69, 0.72, p < 0.05) or borderline (60–75) (0.71, 95% CI 0.70, 0.73, p < 0.05) compared to those scoring in the healthy range (>75) (0.75, 95% CI 0.73, 0.77). | moderate |
| Sameiri et al., Three City Study [77] France | Cross-sectional | 1724 | 76.0 ± 4.9 | (A): 148 item FFQ (B): Mixed method combining hybrid clusters to derive sex-specific dietary patterns. Five dietary patterns were identified in men and women each. (C): Sociodemographic variables, and comorbidities | Self-rated health status | Men in the “pasta eaters” cluster had greater risk of reporting poor health (odds ratio [OR] 1.91; 95% CI, 1.21–3.01) than the “healthy” cluster. Women in the “biscuits and snacking” cluster (n = 162; 15%) had greater risk of poor perceived health (OR 1.69; 95% CI, 1.15–2.48) compared to “healthy” eaters. | moderate |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Govindaraju, T.; Sahle, B.W.; McCaffrey, T.A.; McNeil, J.J.; Owen, A.J. Dietary Patterns and Quality of Life in Older Adults: A Systematic Review. Nutrients 2018, 10, 971. https://doi.org/10.3390/nu10080971
Govindaraju T, Sahle BW, McCaffrey TA, McNeil JJ, Owen AJ. Dietary Patterns and Quality of Life in Older Adults: A Systematic Review. Nutrients. 2018; 10(8):971. https://doi.org/10.3390/nu10080971
Chicago/Turabian StyleGovindaraju, Thara, Berhe W. Sahle, Tracy A. McCaffrey, John J. McNeil, and Alice J. Owen. 2018. "Dietary Patterns and Quality of Life in Older Adults: A Systematic Review" Nutrients 10, no. 8: 971. https://doi.org/10.3390/nu10080971
APA StyleGovindaraju, T., Sahle, B. W., McCaffrey, T. A., McNeil, J. J., & Owen, A. J. (2018). Dietary Patterns and Quality of Life in Older Adults: A Systematic Review. Nutrients, 10(8), 971. https://doi.org/10.3390/nu10080971






