Simple Summary
To this day, cancer remains a medical challenge despite the development of cutting-edge diagnostic methods and therapeutics. Thus, there is a continual demand for improved therapeutic options for managing cancer patients. However, novel drug development requires decade-long time commitment and financial investments. Repurposing approved and market-available drugs for cancer therapy is a way to reduce cost and the timeframe for developing new therapies. Nelfinavir is an anti-infective agent that has extensively been used to treat acquired immunodeficiency syndrome (AIDS) in adult and pediatric patients. In addition to its anti-infective properties, nelfinavir has demonstrated potent off-target anti-cancer effects, suggesting that it could be a suitable candidate for drug repurposing for cancer. In this review, we systematically compiled the therapeutic benefits of nelfinavir against cancer as a single drug or in combination with chemoradiotherapy, and outlined the possible underlying mechanistic pathways contributing to the anti-cancer effects.
Abstract
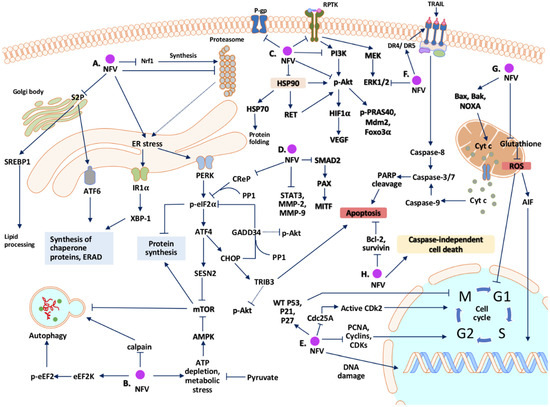
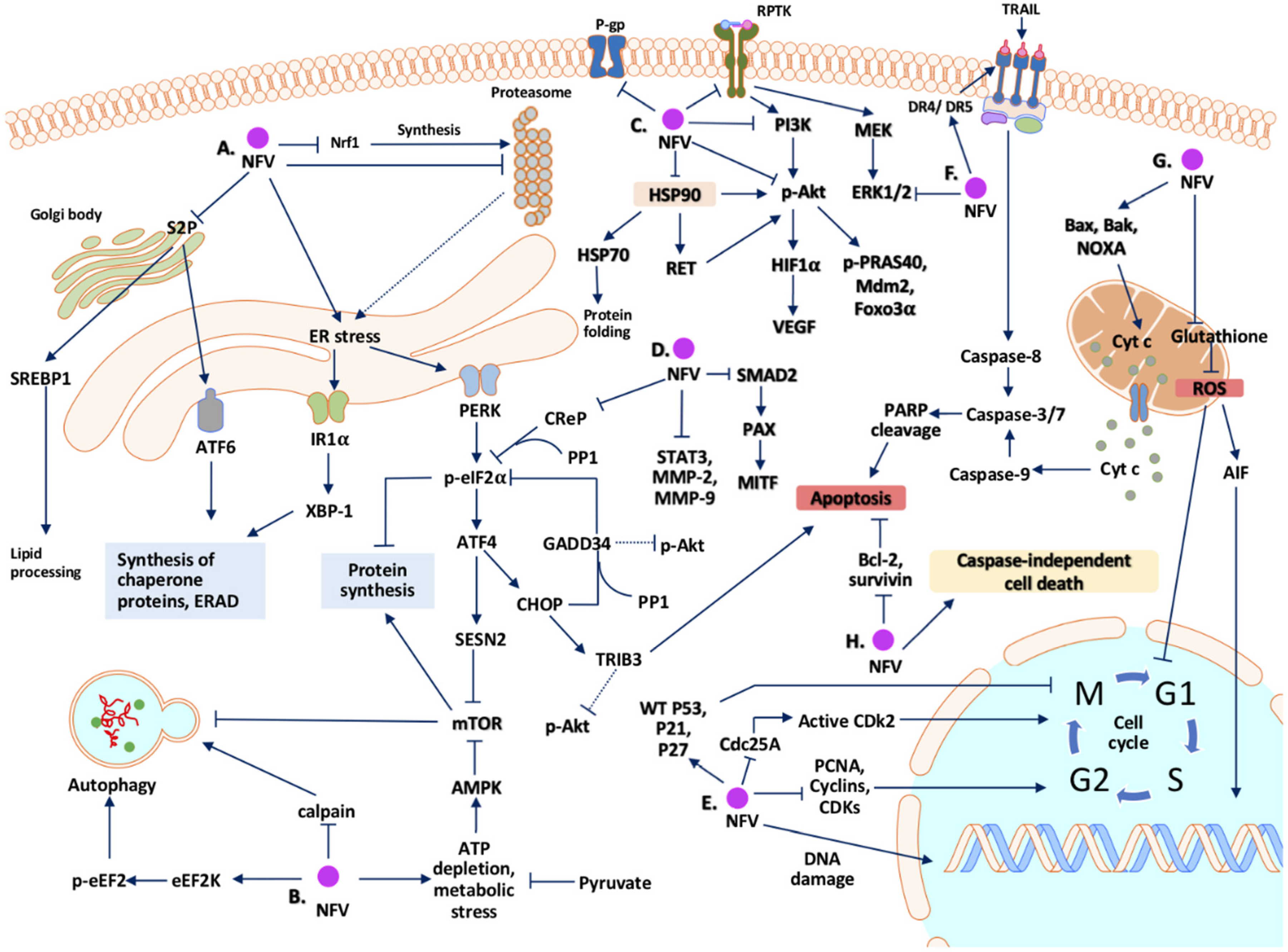
Traditional cancer treatments may lose efficacy following the emergence of novel mutations or the development of chemoradiotherapy resistance. Late diagnosis, high-cost of treatment, and the requirement of highly efficient infrastructure to dispense cancer therapies hinder the availability of adequate treatment in low-income and resource-limited settings. Repositioning approved drugs as cancer therapeutics may reduce the cost and timeline for novel drug development and expedite the availability of newer, efficacious options for patients in need. Nelfinavir is a human immunodeficiency virus (HIV) protease inhibitor that has been approved and is extensively used as an anti-infective agent to treat acquired immunodeficiency syndrome (AIDS). Yet nelfinavir has also shown anti-cancer effects in in vitro and in vivo studies. The anti-cancer mechanism of nelfinavir includes modulation of different cellular conditions, such as unfolded protein response, cell cycle, apoptosis, autophagy, the proteasome pathway, oxidative stress, the tumor microenvironment, and multidrug efflux pumps. Multiple clinical trials indicated tolerable and reversible toxicities during nelfinavir treatment in cancer patients, either as a monotherapy or in combination with chemo- or radiotherapy. Since orally available nelfinavir has been a safe drug of choice for both adult and pediatric HIV-infected patients for over two decades, exploiting its anti-cancer off-target effects will enable fast-tracking this newer option into the existing repertoire of cancer chemotherapeutics.
1. Introduction
Human immunodeficiency virus (HIV) protease inhibitors (PIs) are a group of drugs designed to target the aspartyl protease enzyme of the virus. The ribonucleic acid (RNA) in HIV encodes for two polyproteins—gag and gag-pol—which are cleaved at specific regions by an aspartyl protease for the maturation of the nascent virions through morphologic changes and condensation of the nucleoprotein core [1]. To date, ten HIV-PIs have been approved by the United States Food and Drug Administration (FDA); they contain a synthetic analogue of the gag-pol polyprotein, having a sequence of phenylalanine-proline at 167 and 168 regions [2,3]. The HIV-PIs currently available in the market are nelfinavir, saquinavir, ritonavir, indinavir, amprenavir, fosamprenavir, lopinavir, atazanavir, darunavir, and tipranavir [3,4]. The HIV-PIs exert their therapeutic benefit by inhibiting subsequent HIV infection in a patient; however, they do not exert any action on cells already carrying integrated proviral DNA [1]. Thus, HIV-PIs have been in use in combination with reverse transcriptase inhibitors to treat HIV-infected patients, constituting the standard protocol of highly active antiretroviral treatment (HAART) [5].
Rational drug design of the HIV-PIs as peptidomimetics—based on the amino acid sequence recognized by the HIV aspartyl protease—was intended to drive competitive binding of the drug at the active site of the enzyme and disrupt the enzyme–substrate reaction [6]. Mammalian aspartyl proteases are weaker in cleaving and inhibiting maturation of HIV polyproteins than the HIV-residing enzyme; thus, it was expected that the HIV-PIs would spare the human proteases and induce minimal toxicity. However, soon after the introduction of the HIV-PIs in the HAART protocol, pleiotropic off-target effects of the HIV-PIs were reported. The emergence of reports of remission from AIDS-associated cancers suggested anti-neoplastic properties of HIV-PIs to be a potentially important off-target effect. For instance, Niehuse et al. reported a case of complete regression of AIDS-associated Kaposi’s sarcoma (KS) in a 5-year-old child undergoing HAART regimen consisting of HIV-PI nelfinavir and reverse transcriptase inhibitors zidovudine and lamivudine [7]. Lebbé [8] and Krischer [9] also reported regression of KS in HIV-infected adults undergoing combination therapies of HIV-PIs and reverse transcriptase inhibitors. Initially, the reduction in AIDS-associated cancers was attributed to the immune reconstitution of the body as a result of improved CD4+ T cell count and the reduction in overall viral load; however, later reports suggested that direct off-target anti-cancer action by HIV-PIs could be possible. Sgadari et al. suggested that the antiangiogenic properties of indinavir and saquinavir contributed to the regression of Kaposi’s sarcoma in mice models [10,11], whereas Schmidtke et al. demonstrated that ritonavir could affect the cellular proteasome activity in addition to its immunomodulatory and virus-reducing actions [12]. Thus, multiple preclinical reports suggesting the pleotropic effects of HIV-PIs initiated the research for their possible anti-neoplastic properties.
Nelfinavir is a first-generation HIV-PI, which was approved by the FDA in March 1997 [13,14] for treating HIV infection. Due to the emergence of second- and third-generation HIV-PIs, nelfinavir has been progressively displaced from the HAART protocol [15]; however, nelfinavir exhibited maximum anti-neoplastic efficiency among the HIV-PIs. Wu et al. suggested that a unique cis-decahydroisoquinoline-2 carboxamide moiety may be responsible for the higher anti-neoplastic efficiency of nelfinavir. Analysis through a bioinformatical virtual docking system suggested that nelfinavir can potentially bind at the ATP binding site of the EGFR (ERBB1) protein, which was structurally compared with the same-site binding of the EGFR inhibitor lapatinib [16]. Further molecular docking approaches predicted the probability of binding of nelfinavir with cellular kinases [17] and Hsp90β protein [18], which may also contribute to its anti-cancer properties. In 2007, in a landmark paper by Gills et al., the preclinical anti-neoplastic efficiency of nelfinavir was demonstrated in the NCI60 cancer cell panel [19].
Long-term treatment with nelfinavir in HIV-infected patients led to adverse events such as hyperglycemia, insulin resistance, and lipodystrophy, denoting mechanisms of action of nelfinavir disparate from its anti-viral activity [1]. One of the mechanisms by which insulin resistance is triggered in the body is by the inhibition of the IGF/Akt pathway, which is upregulated in many cancers. Thus, from the observation of insulin resistance, it was postulated that nelfinavir could act as an inhibitor of the Akt pathway in cancer, which was later demonstrated in preclinical studies [19]. To date, multiple research groups have used multipronged approaches to understand and implement the anti-cancer properties of nelfinavir in preclinical settings and clinical trials, with the aim of repositioning the drug as a potential chemotherapeutic agent against a multitude of cancers.
Repositioning already approved drugs for cancer therapeutics is desirable for two reasons: to reduce the timeframe of the drug development pipeline, and to increase the affordability of chemotherapeutics for patients. At present, it takes approximately a decade to go from target identification to FDA approval of a new drug, and these new drugs themselves remain cost prohibitive for large segments of the population, especially in low-income countries. Data available from preclinical studies and toxicity profiling may contribute to the rapid repurposing of nelfinavir in the clinical setting. Furthermore, the recent emergence of nelfinavir in generic form [20] following patent expiration may reduce the cost of treatment as a result of drug repurposing. Minimal toxicity in clinical trials and ease of introduction through oral route may also be an important consideration for repurposing nelfinavir.
This review offers a systematic analysis of the studies investigating the role and efficiency of nelfinavir against a plethora of cancers in preclinical settings and clinical trials.
4. Current Status of Clinical Trials
Promising preclinical data regarding nelfinavir, as a single agent or in combination with other cancer therapies, on multiple cancers, prompted a series of clinical trials. For instance, Rengan and colleagues reported the outcome of a phase I/II trial of nelfinavir with concurrent chemoradiotherapy on locally advanced unresectable stage IIIa/IIIb NSCLC [133,134]. In the phase I study, the maximum tolerated dose of nelfinavir was determined to be 1250 mg per oral route twice daily. Nelfinavir was administered 7 to 14 days prior to and concurrently with cisplatin, etoposide, and radiotherapy at a 66.6 Gy dose. No significant predetermined dose-limiting toxicity was observed. Five of the nine evaluable patients showed complete response, whereas the remaining four patients showed partial response in post-treatment positron emission tomography (PET)-derived metabolic evaluation [133]. The phase I study progressed into a phase II study where 35 patients with locally advanced unresectable stage IIIa/IIIb NSCLC were treated with nelfinavir with concurrent chemoradiotherapy. Observed median survival was 41.1 months and a median progression-free survival was 11.7 months without any unexpected grade 3 or 4 toxicities beyond those of standard chemoradiotherapy [134].
Radiotherapy is a front-line management option for inoperable locally advanced pancreatic cancer (LAPC); however, resistance to radiation is frequent and local disease progression leads to the demise of patients. In the preclinical setting, nelfinavir was shown to increase the sensitivity to radiation via the downregulation of Akt [96], reducing hypoxia [103], and improving tumor microvasculature [120]. Brunner et al. first reported a phase I trial with the use of nelfinavir in conjunction with chemoradiotherapy in inoperable LAPC patients [107]. In this study, 12 patients started nelfinavir three days before the initiation of radiation therapy and chemotherapy with cisplatin and gemcitabine. Of the 10 evaluable patients, 5 showed complete metabolic response in PET and 6 underwent secondary resection. The median overall survival was 18 months, and most patients showed downregulation of p-Akt in PBMCs. Nelfinavir did not contribute to additional or unexpected toxicity to the regimen [107]. The study escalated into phase II, where 23 patients with estimated life expectancy ≥ 12 weeks received nelfinavir 1250 mg twice daily prior to and concurrently with radiotherapy and chemotherapy (cisplatin and gemcitabine) [135]. In this study, the median overall survival time was 17.4 months, (90%CI: 12.8–18.8%) and one-year overall survival rate was 73.4% (90% CI: 54.5–85.5%). Four of the six recruited patients for a sub-study showed reduced hypoxia in 18F-fluoromisonidazole positron emission tomography (FMISO-PET) with a concurrent increase in computed tomography (CT) perfusion denoting increased blood flow. Additionally, 8 of 13 evaluable patients demonstrated the downregulation of p-Akt following initial nelfinavir treatment. However, a high incidence of grade 3 or above gastrointestinal toxicity raised concern, which was attributed to the gemcitabine-cisplatin combination with concurrent large-field radiotherapy [135,136]. To address the need to optimize the chemoradiation regime for LAPC, a large-scale multicenter randomized study SCALOP-2 began in March 2016. The study aims at investigating the benefit of induction-chemotherapy by gemcitabine and nab-paclitaxel followed by escalating doses of radiation with or without the radiosensitizer nelfinavir [136]. Recently, Lin et al. reported two trials testing the simultaneous use of nelfinavir with stereotactic body radiotherapy (SBRT) on patients having locally advanced or unresectable pancreatic adenocarcinoma [137,138]. In the phase I study, patients received three-week cycles of gemcitabine/leucovorin/fluorouracil followed by combinations of nelfinavir and escalating doses of radiation therapy. In this study, a median overall survival was estimated to be 14.4 months, and the maximum tolerated dose combination was deemed SBRT (40 Gy)/nelfinavir (1250 BID) [137]. Additionally, in a prematurely terminated trial, Lin et al. tested a chemoimmunotherapy combination gemcitabine/leucovorin/fluorouracil/oregovomab followed by SBRT (40 Gy)/nelfinavir (1250 BID) in LAPC patients [138].
In a few studies, nelfinavir was tried as a monotherapy, unlike the mostly tested regimen of nelfinavir in combination with chemotherapy and with or without radiation therapy. Hoover et al. reported a phase II clinical trial in patients with recurrent adenoid cystic carcinoma who no longer responded to the available standard therapeutic options. Patients received doses of 1250 mg of nelfinavir twice daily; however, the progression-free survival did not improve significantly [109]. Conversely, in a phase I study conducted by Pan et al., 6 patients out of 20 (30%), having recurrent, metastatic or unresectable liposarcoma, showed clinical benefits at different dose levels of nelfinavir [139]. Nelfinavir was reasonably tolerated without any dose-limiting toxicity, and dose escalation was effective up to 3000 mg due to auto-induction of increased plasma clearance at higher doses [139]. Blumenthal et al. investigated the effects of nelfinavir monotherapy on adults having advanced solid refractory tumors of different origins [57]. Patients showed well tolerability to nelfinavir with manageable toxicities and the maximum tolerated dose was determined at 3125 mg. Dose-limiting toxicity was reported as grade 4 neutropenia at a high dose level (3750 mg), which was reversible quickly upon temporary discontinuation of the treatment. Out of 28 patients, one showed partial response, three showed minor response and six showed stable disease on tumor evaluation. Importantly, this study reported the beneficial effect of nelfinavir on a neuroendocrine tumor (NET). Patients showed decreased p-Akt, enhanced p-eIF2α and enhanced expression of ATF3 and CHOP analyzed from PBMCs following nelfinavir treatment [57].
Decreased UPR, especially silencing of IRE1α/XBP1 in MM cells has been shown to confer resistance to proteasome inhibitor bortezomib [140]. In a phase I study, Driessen et al. observed the upregulation of UPR proteins in response to nelfinavir—with or without bortezomib—in PBMCs of advanced MM patients [75]. Among six bortezomib and lenalidomide refractory MM patients, three showed partial response, and two demonstrated minor response to the combination of nelfinavir (2 × 2500 mg) and bortezomib. Nelfinavir also showed mild inhibition of proteasome activity, which was further enhanced by bortezomib [20,75]. In a phase II trial 34 patients of bortezomib-refractory MM, a twice daily dose of 2500 mg of nelfinavir lead to an objective response rate of 65% (90% CI, 49–76%) and was observed with 12 weeks of progression-free survival and a median overall survival of 12 months [20]. Recently, Hitz et al. reported a regime of nelfinavir/lenalidomide/dexamethasone, a triad of orally given drugs, tried on 29 patients with lenalidomide refractory MM [76]. Ten of the 29 patients had lenalidomide-bortezomib double-refractory MM; 16 patients showed minor response or better (55%, 95% CI 36–74%), and 9 patients showed partial response (31%, 95% CI 15–51%), with median overall survival of 21.6 months. Lenalidomide and nelfinavir both act as substrates for multidrug-resistant 1 (MDR-1) pump which may have caused competing interaction and inhibited drug efflux, thereby increasing intracellular concentration and clinical effects [76].
Hill et al. conducted a clinical trial of combining nelfinavir and radiotherapy on 10 patients having advanced metastatic rectal cancer. Unlike previous studies, nelfinavir (1250 mg twice daily) was combined with hypofractionated radiotherapy without the addition of chemotherapy. Five patients demonstrated tumor regression as per MRI imaging, and dynamic imaging (p-CT, DCI-MRI) hinted increased perfusion in the tumor area [141]. In another small cohort of 11 patients, Buijsen et al. investigated the tolerability of nelfinavir with standard radiotherapy and capecitabine (825 mg/2) in locally advanced rectal cancer patients. Three patients showed pathological complete response and 4 other patients showed major response. Diarrhea appeared to be the most frequent adverse event, which was speculated to be related to the high plasma level of nelfinavir due to inhibition of CYP2C9—a metabolizer enzyme of nelfinavir—by capecitabine. The maximum tolerated dose of nelfinavir was deemed 750 mg twice daily [142]. In patients diagnosed with glioblastoma multiforme (GBM), in order to determine the dose limiting toxicity and maximum tolerated dose of nelfinavir, in conjunction with temozolomide and radiotherapy, Alonso-Basnata and colleagues conducted a phase I trial on 21 patients. Nelfinavir was deemed to be safe when administered with temozolomide (75 mg/m2) and radiotherapy (6000 cGy to the gross tumor volume), and the maximum tolerated dose was 1250 mg, similar to the standard dose of HIV infected patients [143]. The bulk of clinical trial data are compiled in Table 2.

Table 2.
Updated clinical trial list including nelfinavir (2020).
5. Conclusions
Despite promising advancement in cancer therapeutics, the emergence of novel mutations and resistance to chemoradiotherapy results in low survival rates. Additionally, increased cost and requirement of highly efficient setup for chemoradiotherapy hinders patient access to efficacious treatments within low-income populations and areas with limited resources. Drug repurposing for cancer therapy can maximize the optimal use of the existing drug repertoire and lower the time and cost of developing new therapies. An anti-HIV protease inhibitor, nelfinavir, has been proven efficacious, as a monotherapy, against a variety of cancers in both preclinical settings and clinical trials. Furthermore, nelfinavir sensitized cancer cells to existing regimens of chemotherapy and radiotherapy. Nelfinavir has been in use as an anti-infective agent against HIV for more than two decades, demonstrating good safety profile and tolerable toxicities. The main toxicities associated with long-term frequent dosing of nelfinavir are impairment of glucose metabolism and lipodystrophy, which are reversible upon discontinuation; hence, the potential anti-tumor benefits may outweigh the associated risk of toxicities. As nelfinavir is an orally administered drug, it may lead to good patient compliance and be a preferred drug of choice in resource-limited settings.
Nelfinavir can target a number of mechanisms in mammalian cancer cells; however, definitive identification of the primary cellular target responsible for anti-tumor efficacy is still needed. Analysis of reports indicating probable intracellular pathways suggests that the mechanisms to impart anti-cancer properties by nelfinavir may be cell type and cancer-specific. A number of phase I and II clinical trials have proven the safety, tolerability and positive outcome of nelfinavir in cancer patients, with or without co-treatments, especially against pancreatic cancer, NSCLC, and MM [75,107,134]. So far, the completed clinical trials have been single arm and open-labelled involving small cohorts and the available data warrants randomized controlled trials on larger population groups. Accordingly, two large scale randomized trials are currently ongoing to test the efficacy of nelfinavir with radiotherapy against locally advanced pancreatic cancer (NCT02024009) and cervical cancer (NCT03256916).
Anti-infective dosing of nelfinavir in HIV-infected patients results in a maximum plasma concentration of 7–9 μmol/L, and reports have shown that anti-cancer effects can be achieved within this range [16,19,21]. However, higher plasma concentration may be needed to elicit anti-cancer properties by nelfinavir against some cancers [41]. As nelfinavir is an inducer and substrate of metabolic enzyme CYP34A, autoinduction of plasma clearance in high doses is initiated, which prevents increment of plasma concentration during dose escalation, leading to non-linear pharmacokinetics [139]. Enhanced plasma concentration and tissue availability of nelfinavir can be achieved through molecular modification, drug combination, or nano-particle-based administration. Molecular modification through nitric oxide (NO) hybridization of HIV-PIs have emerged as an alternative strategy to increase the anti-cancer efficacy in lower doses, especially in case of saquinavir [4]. Metabolism of nelfinavir by the enzyme CYP2C19 yields the pharmacologically active metabolite M8 responsible for suppressing the viral replication. M8 has also shown comparable anti-tumor activity to nelfinavir [61]. Kattel et al. reported enhanced systemic exposure of nelfinavir due to genetic polymorphism of CYP2C19 in locally advanced pancreatic cancer patients, suggesting that stratification of patients according to the genotype could identify the population likely to be benefitted from nelfinavir treatment [145].
Overall, the anti-tumor effects of nelfinavir have been tested on an array of cancers, with positive results rationalizing its suitability as a potential candidate for drug repurposing for cancer.
Author Contributions
Writing—original draft preparation, M.R.S.; cartoon eliciting mechanisms of action of nelfinavir, M.R.S.; graphical abstract, M.R.S. and C.M.T.; conceptualization, and writing—review and editing, C.M.T. Both authors have read and agreed to the published version of the manuscript.
Funding
This article was supported with funds from the Department of Pathology, McGill University, a grant from the Canadian Foundation for Innovation, and funds from the Rivkin Center for Ovarian Cancer (all to CT).
Acknowledgments
The authors thank Nahuel Telleria for editing the manuscript.
Conflicts of Interest
The authors declare no conflict of interests.
Abbreviations
| ABC | ATP-binding cassette |
| AIDS | Acquired immunodeficiency syndrome |
| AIF | Apoptosis-inducing factor |
| AML | Acute myeloid leukemia |
| AMPK | 5′-AMP-activated protein kinase |
| ATF3 | Activating transcription factor 3 |
| ATF6 | Activating transcription factor 6 |
| ATP | Adenosine triphosphate |
| BrdU | Bromodeoxyuridine |
| CDK | Cyclin-dependent kinase |
| CHOP | CCAAT enhancer-binding protein homologous protein |
| CML | Chronic myeloid leukemia |
| CT | Computer tomography |
| DR | Death receptors |
| DEN | Diethylnitrosamine |
| DMC | Dimethylcelecoxib |
| eIF2α | Eukaryotic initiation factor 2α |
| eEF2 | Eukaryotic elongation factor |
| eEF2K | Eukariotic elongation factor 2 kinase |
| EGFR | Epidermal growth factor receptor |
| ER | Endoplasmic reticulum |
| ERp44 | Endoplasmic reticulum resident protein 44 |
| ERO1-Lα | Endoplasmic reticulum oxidoreductin-1-like protein α |
| FACS | Fluorescence-activated cell sorting |
| FADD | Fas-associated protein with death domain |
| FAK | Focal adhesion kinase |
| FAS | Fatty acid synthase |
| FDA | Food and Drug Administration |
| FMISO-PET | 18F-fluoromisonidazole positron emission tomography |
| GADD34 | Growth arrest and DNA damage inducible protein 34 |
| GBM | Glioblastoma multiforme |
| GFP | Green fluorescent protein |
| GRP78 | Glucose-regulated protein of 78 kDa |
| GSH | Glutathione |
| HAART | Highly active antiretroviral treatment |
| HCC | Hepatocarcinoma cells |
| HDAC | Histone deacetylase |
| HER2 | Human epidermal factor receptor 2 |
| HIF1α | Hypoxia-inducible factor 1α |
| HIV | Human immunodeficiency virus |
| HPV | Human papillomavirus |
| hPSC | Human pancreatic stellate cells |
| HSP90 | Heat shock protein 90 |
| H2O2 | Hydrogen peroxide |
| IGFR | Insulin-like growth factor receptor |
| IRE1α | Inositol-requiring enzyme 1-α |
| ISR | Integrated stress response |
| KS | Kaposi’s sarcoma |
| LAPC | Locally advanced pancreatic cancer |
| MAPK | Mitogen-activated protein kinase pathway |
| 3MA | 3-methyladenosine |
| mTOR | Mammalian target of rapamycin |
| 3-MA | 3-methyladenine |
| MDR | Multidrug resistance |
| MDR1 | Multidrug-resistant 1 |
| MRP-4 | Multidrug resistance protein 4 |
| MEF | Mouse embryonic fibroblasts |
| MM | Multiple myeloma |
| mPTP | Mitochondria permeability transition pore |
| MMP-2 | Matrix metalloproteinase-2 |
| MMP-9 | Matrix metalloproteinase-3 |
| NAC | N-acetylcysteine |
| NET | Neuroendocrine tumor |
| NO | Nitric oxide |
| NSCLC | Non-small-cell lung carcinoma |
| PARP | Poly ADP-ribose polymerase |
| PBMC | Peripheral blood mononuclear cells |
| PCNA | Proliferating cell nuclear antigen |
| PDI | Protein disulfide isomerase |
| PE | Phosphatidyl ethanolamine |
| PERK | Protein kinase RNA-like endoplasmic reticulum kinase |
| PET | Positron emission tomography |
| P-gp | P-glycoprotein |
| PI | Protease inhibitors |
| PTEN | Phosphate and tensin homologue |
| RIP | Regulated intramembrane proteolysis |
| RNA | Ribonucleic acid |
| ROS | Reactive oxygen species |
| SBRT | Stereotactic body radiotherapy |
| SIRT3 | Sirtuin-3 |
| STAT3 | Signal transducer and activator of transcription 3 |
| S1P | Site-1 protease |
| S2P | Site-2 protease |
| SESN2 | Sestrin-2 |
| SRC | Tyrosine kinase Src |
| SREBP1 | Sterol regulatory binding protein-1 |
| siRNA | Small interference RNA |
| TNBC | Triple-negative breast cancer |
| TNF | Tumor necrosis factor |
| TRAIL | Tumor necrosis factor-related apoptosis-inducing ligand |
| TRIB-3 | Tribbles homolog-3 |
| TSC | Tuberous sclerosis complex |
| TUNEL | Terminal deoxynucleotidyl transferase (TdT) dUTP Nick-End Labeling |
| UPR | Unfolded protein response |
| VEGF | Vascular endothelial growth factor |
| XBP-1 | X-box binding protein-1 |
References
- Flexner, C. HIV-protease inhibitors. N. Engl. J. Med. 1998, 338, 1281–1292. [Google Scholar] [CrossRef]
- Debouck, C. The HIV-1 protease as a therapeutic target for AIDS. AIDS Res. Hum. Retrovir. 1992, 8, 153–164. [Google Scholar] [CrossRef] [PubMed]
- Lv, Z.; Chu, Y.; Wang, Y. HIV protease inhibitors: A review of molecular selectivity and toxicity. HIV AIDS (Auckl) 2015, 7, 95–104. [Google Scholar] [PubMed]
- Maksimovic-Ivanic, D.; Fagone, P.; McCubrey, J.; Bendtzen, K.; Mijatovic, S.; Nicoletti, F. HIV-protease inhibitors for the treatment of cancer: Repositioning HIV protease inhibitors while developing more potent NO-hybridized derivatives? Int. J. Cancer 2017, 140, 1713–1726. [Google Scholar] [CrossRef] [PubMed]
- Carpenter, C.C.; Fischl, M.A.; Hammer, S.M.; Hirsch, M.S.; Jacobsen, D.M.; Katzenstein, D.A.; Montaner, J.S.; Richman, D.D.; Saag, M.S.; Schooley, R.T.; et al. Antiretroviral therapy for HIV infection in 1998: Updated recommendations of the International AIDS Society-USA Panel. JAMA 1998, 280, 78–86. [Google Scholar] [CrossRef] [PubMed]
- Zhang, K.E.; Wu, E.; Patick, A.K.; Kerr, B.; Zorbas, M.; Lankford, A.; Kobayashi, T.; Maeda, Y.; Shetty, B.; Webber, S. Circulating metabolites of the human immunodeficiency virus protease inhibitor nelfinavir in humans: Structural identification, levels in plasma, and antiviral activities. Antimicrob. Agents Chemother. 2001, 45, 1086–1093. [Google Scholar] [CrossRef]
- Niehues, T.; Horneff, G.; Megahed, M.; Schroten, H.; Wahn, V. Complete regression of AIDS-related Kaposi’s sarcoma in a child treated with highly active antiretroviral therapy. AIDS 1999, 13, 1148–1149. [Google Scholar] [CrossRef]
- Lebbe, C.; Blum, L.; Pellet, C.; Blanchard, G.; Verola, O.; Morel, P.; Danne, O.; Calvo, F. Clinical and biological impact of antiretroviral therapy with protease inhibitors on HIV-related Kaposi’s sarcoma. AIDS 1998, 12, F45–F49. [Google Scholar] [CrossRef]
- Krischer, J.; Rutschmann, O.; Hirschel, B.; Vollenweider-Roten, S.; Saurat, J.H.; Pechere, M. Regression of Kaposi’s sarcoma during therapy with HIV-1 protease inhibitors: A prospective pilot study. J. Am. Acad. Dermatol. 1998, 38, 594–598. [Google Scholar] [CrossRef]
- Sgadari, C.; Barillari, G.; Toschi, E.; Carlei, D.; Bacigalupo, I.; Baccarini, S.; Palladino, C.; Leone, P.; Bugarini, R.; Malavasi, L.; et al. HIV protease inhibitors are potent anti-angiogenic molecules and promote regression of Kaposi sarcoma. Nat. Med. 2002, 8, 225–232. [Google Scholar] [CrossRef]
- Sgadari, C.; Monini, P.; Barillari, G.; Ensoli, B. Use of HIV protease inhibitors to block Kaposi’s sarcoma and tumour growth. Lancet Oncol. 2003, 4, 537–547. [Google Scholar] [CrossRef]
- Schmidtke, G.; Holzhutter, H.G.; Bogyo, M.; Kairies, N.; Groll, M.; de Giuli, R.; Emch, S.; Groettrup, M. How an inhibitor of the HIV-I protease modulates proteasome activity. J. Biol. Chem. 1999, 274, 35734–35740. [Google Scholar] [CrossRef] [PubMed]
- Pai, V.B.; Nahata, M.C. Nelfinavir mesylate: A protease inhibitor. Ann. Pharm. 1999, 33, 325–339. [Google Scholar] [CrossRef] [PubMed]
- Koltai, T. Nelfinavir and other protease inhibitors in cancer: Mechanisms involved in anticancer activity. F1000Res 2015, 4, 9. [Google Scholar] [CrossRef]
- Gantt, S.; Casper, C.; Ambinder, R.F. Insights into the broad cellular effects of nelfinavir and the HIV protease inhibitors supporting their role in cancer treatment and prevention. Curr. Opin. Oncol. 2013, 25, 495–502. [Google Scholar] [CrossRef]
- Wu, W.; Zhang, R.; Salahub, D.R. Nelfinavir: A magic bullet to annihilate cancer cells? Cancer Biol. Ther. 2009, 8, 233–235. [Google Scholar] [CrossRef]
- Xie, L.; Evangelidis, T.; Xie, L.; Bourne, P.E. Drug Discovery Using Chemical Systems Biology: Weak Inhibition of Multiple Kinases May Contribute to the Anti-Cancer Effect of Nelfinavir. PLoS Comput. Biol. 2011, 7, e1002037. [Google Scholar] [CrossRef]
- Arodola, O.A.; Soliman, M.E. Could the FDA-approved anti-HIV PR inhibitors be promising anticancer agents? An answer from enhanced docking approach and molecular dynamics analyses. Drug Des. Devel. Ther. 2015, 9, 6055–6065. [Google Scholar]
- Gills, J.J.; Lopiccolo, J.; Tsurutani, J.; Shoemaker, R.H.; Best, C.J.; Abu-Asab, M.S.; Borojerdi, J.; Warfel, N.A.; Gardner, E.R.; Danish, M.; et al. Nelfinavir, A lead HIV protease inhibitor, is a broad-spectrum, anticancer agent that induces endoplasmic reticulum stress, autophagy, and apoptosis in vitro and in vivo. Clin. Cancer Res. 2007, 13, 5183–5194. [Google Scholar] [CrossRef]
- Driessen, C.; Muller, R.; Novak, U.; Cantoni, N.; Betticher, D.; Mach, N.; Rufer, A.; Mey, U.; Samaras, P.; Ribi, K.; et al. Promising activity of nelfinavir-bortezomib-dexamethasone in proteasome inhibitor-refractory multiple myeloma. Blood 2018, 132, 2097–2100. [Google Scholar] [CrossRef]
- Bruning, A.; Burger, P.; Vogel, M.; Rahmeh, M.; Gingelmaiers, A.; Friese, K.; Lenhard, M.; Burges, A. Nelfinavir induces the unfolded protein response in ovarian cancer cells, resulting in ER vacuolization, cell cycle retardation and apoptosis. Cancer Biol. Ther. 2009, 8, 226–232. [Google Scholar] [CrossRef] [PubMed]
- Bruning, A.; Rahmeh, M.; Gingelmaier, A.; Friese, K. The mitochondria-independent cytotoxic effect of nelfinavir on leukemia cells can be enhanced by sorafenib-mediated mcl-1 downregulation and mitochondrial membrane destabilization. Mol. Cancer 2010, 9, 19. [Google Scholar] [CrossRef] [PubMed]
- Bruning, A.; Vogel, M.; Mylonas, I.; Friese, K.; Burges, A. Bortezomib targets the caspase-like proteasome activity in cervical cancer cells, triggering apoptosis that can be enhanced by nelfinavir. Curr. Cancer Drug Targets 2011, 11, 799–809. [Google Scholar] [CrossRef] [PubMed]
- Chow, W.A.; Guo, S.; Valdes-Albini, F. Nelfinavir induces liposarcoma apoptosis and cell cycle arrest by upregulating sterol regulatory element binding protein-1. Anticancer Drugs 2006, 17, 891–903. [Google Scholar] [CrossRef] [PubMed]
- Jiang, W.; Mikochik, P.J.; Ra, J.H.; Lei, H.; Flaherty, K.T.; Winkler, J.D.; Spitz, F.R. HIV protease inhibitor nelfinavir inhibits growth of human melanoma cells by induction of cell cycle arrest. Cancer Res. 2007, 67, 1221–1227. [Google Scholar] [CrossRef]
- Jensen, K.; Bikas, A.; Patel, A.; Kushchayeva, Y.; Costello, J.; McDaniel, D.; Burman, K.; Vasko, V. Nelfinavir inhibits proliferation and induces DNA damage in thyroid cancer cells. Endocr. Relat. Cancer 2017, 24, 147–156. [Google Scholar] [CrossRef][Green Version]
- Sato, A.; Asano, T.; Okubo, K.; Isono, M.; Asano, T. Nelfinavir and Ritonavir Kill Bladder Cancer Cells Synergistically by Inducing Endoplasmic Reticulum Stress. Oncol. Res. 2018, 26, 323–332. [Google Scholar] [CrossRef]
- Okubo, K.; Sato, A.; Isono, M.; Asano, T.; Asano, T. Nelfinavir Induces Endoplasmic Reticulum Stress and Sensitizes Renal Cancer Cells to TRAIL. Anticancer Res. 2018, 38, 4505–4514. [Google Scholar] [CrossRef]
- Okubo, K.; Isono, M.; Asano, T.; Sato, A. Panobinostat and Nelfinavir Inhibit Renal Cancer Growth by Inducing Endoplasmic Reticulum Stress. Anticancer Res. 2018, 38, 5615–5626. [Google Scholar] [CrossRef]
- Soprano, M.; Sorriento, D.; Rusciano, M.R.; Maione, A.S.; Limite, G.; Forestieri, P.; D’Angelo, D.; D’Alessio, M.; Campiglia, P.; Formisano, P.; et al. Oxidative Stress Mediates the Antiproliferative Effects of Nelfinavir in Breast Cancer Cells. PLoS ONE 2016, 11, e0155970. [Google Scholar] [CrossRef] [PubMed]
- Sun, L.; Niu, L.; Zhu, X.; Hao, J.; Wang, P.; Wang, H. Antitumour effects of a protease inhibitor, nelfinavir, in hepatocellular carcinoma cancer cells. J. Chemother. 2012, 24, 161–166. [Google Scholar] [CrossRef] [PubMed]
- Veschi, S.; De Lellis, L.; Florio, R.; Lanuti, P.; Massucci, A.; Tinari, N.; De Tursi, M.; di Sebastiano, P.; Marchisio, M.; Natoli, C.; et al. Effects of repurposed drug candidates nitroxoline and nelfinavir as single agents or in combination with erlotinib in pancreatic cancer cells. J. Exp. Clin. Cancer Res. 2018, 37, 236. [Google Scholar] [CrossRef] [PubMed]
- Xiang, T.; Du, L.; Pham, P.; Zhu, B.; Jiang, S. Nelfinavir, an HIV protease inhibitor, induces apoptosis and cell cycle arrest in human cervical cancer cells via the ROS-dependent mitochondrial pathway. Cancer Lett. 2015, 364, 79–88. [Google Scholar] [CrossRef] [PubMed]
- Xia, C.; Chen, R.; Chen, J.; Qi, Q.; Pan, Y.; Du, L.; Xiao, G.; Jiang, S. Combining metformin and nelfinavir exhibits synergistic effects against the growth of human cervical cancer cells and xenograft in nude mice. Sci. Rep. 2017, 7, 43373. [Google Scholar] [CrossRef]
- Bruning, A.; Burger, P.; Vogel, M.; Gingelmaier, A.; Friese, K.; Burges, A. Nelfinavir induces mitochondria protection by ERK1/2-mediated mcl-1 stabilization that can be overcome by sorafenib. Investig. New Drugs 2010, 28, 535–542. [Google Scholar] [CrossRef]
- Cande, C.; Cecconi, F.; Dessen, P.; Kroemer, G. Apoptosis-inducing factor (AIF): Key to the conserved caspase-independent pathways of cell death? J. Cell Sci. 2002, 115, 4727–4734. [Google Scholar] [CrossRef]
- Bono, C.; Karlin, L.; Harel, S.; Mouly, E.; Labaume, S.; Galicier, L.; Apcher, S.; Sauvageon, H.; Fermand, J.P.; Bories, J.C.; et al. The human immunodeficiency virus-1 protease inhibitor nelfinavir impairs proteasome activity and inhibits the proliferation of multiple myeloma cells in vitro and in vivo. Haematologica 2012, 97, 1101–1109. [Google Scholar] [CrossRef]
- Kushchayeva, Y.; Jensen, K.; Recupero, A.; Costello, J.; Patel, A.; Klubo-Gwiezdzinska, J.; Boyle, L.; Burman, K.; Vasko, V. The HIV protease inhibitor nelfinavir down-regulates RET signaling and induces apoptosis in medullary thyroid cancer cells. J. Clinl. Endocrinol. Metabol. 2014, 99, E734–E745. [Google Scholar] [CrossRef]
- Bruning, A.; Friese, K.; Burges, A.; Mylonas, I. Tamoxifen enhances the cytotoxic effects of nelfinavir in breast cancer cells. Breast Cancer Res. 2010, 12, R45. [Google Scholar] [CrossRef]
- Cho, H.Y.; Thomas, S.; Golden, E.B.; Gaffney, K.J.; Hofman, F.M.; Chen, T.C.; Louie, S.G.; Petasis, N.A.; Schonthal, A.H. Enhanced killing of chemo-resistant breast cancer cells via controlled aggravation of ER stress. Cancer Lett. 2009, 282, 87–97. [Google Scholar] [CrossRef]
- Thomas, S.; Sharma, N.; Golden, E.B.; Cho, H.; Agarwal, P.; Gaffney, K.J.; Petasis, N.A.; Chen, T.C.; Hofman, F.M.; Louie, S.G.; et al. Preferential killing of triple-negative breast cancer cells in vitro and in vivo when pharmacological aggravators of endoplasmic reticulum stress are combined with autophagy inhibitors. Cancer Lett. 2012, 325, 63–71. [Google Scholar] [CrossRef] [PubMed]
- Davis, M.A.; Delaney, J.R.; Patel, C.B.; Storgard, R.; Stupack, D.G. Nelfinavir is effective against human cervical cancer cells in vivo: A potential treatment modality in resource-limited settings. Drug Des. Devel. Ther. 2016, 10, 1837–1846. [Google Scholar] [PubMed]
- Bruning, A.; Rahmeh, M.; Friese, K. Nelfinavir and bortezomib inhibit mTOR activity via ATF4-mediated sestrin-2 regulation. Mol. Oncol. 2013, 7, 1012–1018. [Google Scholar] [CrossRef] [PubMed]
- Meier-Stephenson, V.; Riemer, J.; Narendran, A. The HIV protease inhibitor, nelfinavir, as a novel therapeutic approach for the treatment of refractory pediatric leukemia. Onco. Targets Ther. 2017, 10, 2581–2593. [Google Scholar] [CrossRef]
- Liu, W.; Meng, Q.; Sun, Y.; Wang, C.; Huo, X.; Liu, Z.; Sun, P.; Sun, H.; Ma, X.; Liu, K. Targeting P-Glycoprotein: Nelfinavir Reverses Adriamycin Resistance in K562/ADR Cells. Cell Physiol. Biochem. 2018, 51, 1616–1631. [Google Scholar] [CrossRef]
- Mathur, A.; Abd Elmageed, Z.Y.; Liu, X.; Kostochka, M.L.; Zhang, H.; Abdel-Mageed, A.B.; Mondal, D. Subverting ER-stress towards apoptosis by nelfinavir and curcumin coexposure augments docetaxel efficacy in castration resistant prostate cancer cells. PLoS ONE 2014, 9, e103109. [Google Scholar] [CrossRef]
- Yang, Y.; Ikezoe, T.; Nishioka, C.; Bandobashi, K.; Takeuchi, T.; Adachi, Y.; Kobayashi, M.; Takeuchi, S.; Koeffler, H.P.; Taguchi, H. NFV, an HIV-1 protease inhibitor, induces growth arrest, reduced Akt signalling, apoptosis and docetaxel sensitisation in NSCLC cell lines. Br. J. Cancer 2006, 95, 1653–1662. [Google Scholar] [CrossRef]
- Yang, Y.; Ikezoe, T.; Takeuchi, T.; Adachi, Y.; Ohtsuki, Y.; Takeuchi, S.; Koeffler, H.P.; Taguchi, H. HIV-1 protease inhibitor induces growth arrest and apoptosis of human prostate cancer LNCaP cells in vitro and in vivo in conjunction with blockade of androgen receptor STAT3 and AKT signaling. Cancer Sci. 2005, 96, 425–433. [Google Scholar] [CrossRef]
- Vandewynckel, Y.P.; Coucke, C.; Laukens, D.; Devisscher, L.; Paridaens, A.; Bogaerts, E.; Vandierendonck, A.; Raevens, S.; Verhelst, X.; Van Steenkiste, C.; et al. Next-generation proteasome inhibitor oprozomib synergizes with modulators of the unfolded protein response to suppress hepatocellular carcinoma. Oncotarget 2016, 7, 34988–35000. [Google Scholar] [CrossRef]
- Gupta, V.; Samuleson, C.G.; Su, S.; Chen, T.C. Nelfinavir potentiation of imatinib cytotoxicity in meningioma cells via survivin inhibition. Neurosurg. Focus 2007, 23, E9. [Google Scholar] [CrossRef]
- Elmore, S. Apoptosis: A review of programmed cell death. Toxicol. Pathol. 2007, 35, 495–516. [Google Scholar] [CrossRef] [PubMed]
- Tian, X.; Ye, J.; Alonso-Basanta, M.; Hahn, S.M.; Koumenis, C.; Dorsey, J.F. Modulation of CCAAT/enhancer binding protein homologous protein (CHOP)-dependent DR5 expression by nelfinavir sensitizes glioblastoma multiforme cells to tumor necrosis factor-related apoptosis-inducing ligand (TRAIL). J. Biol. Chem. 2011, 286, 29408–29416. [Google Scholar] [CrossRef] [PubMed]
- Bruning, A.; Vogel, M.; Burger, P.; Rahmeh, M.; Gingelmaier, A.; Friese, K.; Lenhard, M.; Burges, A. Nelfinavir induces TRAIL receptor upregulation in ovarian cancer cells. Biochem. Biophys. Res. Commun. 2008, 377, 1309–1314. [Google Scholar] [CrossRef] [PubMed]
- Wang, W.A.; Groenendyk, J.; Michalak, M. Endoplasmic reticulum stress associated responses in cancer. Biochim. Biophys. Acta 2014, 1843, 2143–2149. [Google Scholar] [CrossRef]
- Corazzari, M.; Gagliardi, M.; Fimia, G.M.; Piacentini, M. Endoplasmic Reticulum Stress, Unfolded Protein Response, and Cancer Cell Fate. Front Oncol. 2017, 7, 78. [Google Scholar] [CrossRef] [PubMed]
- Kawabata, S.; Gills, J.J.; Mercado-Matos, J.R.; Lopiccolo, J.; Wilson, W., 3rd; Hollander, M.C.; Dennis, P.A. Synergistic effects of nelfinavir and bortezomib on proteotoxic death of NSCLC and multiple myeloma cells. Cell Death Dis. 2012, 3, e353. [Google Scholar] [CrossRef]
- Blumenthal, G.M.; Gills, J.J.; Ballas, M.S.; Bernstein, W.B.; Komiya, T.; Dechowdhury, R.; Morrow, B.; Root, H.; Chun, G.; Helsabeck, C.; et al. A phase I trial of the HIV protease inhibitor nelfinavir in adults with solid tumors. Oncotarget 2014, 5, 8161–8172. [Google Scholar] [CrossRef]
- Pyrko, P.; Kardosh, A.; Wang, W.; Xiong, W.; Schonthal, A.H.; Chen, T.C. HIV-1 protease inhibitors nelfinavir and atazanavir induce malignant glioma death by triggering endoplasmic reticulum stress. Cancer Res. 2007, 67, 10920–10928. [Google Scholar] [CrossRef]
- Mahameed, M.; Boukeileh, S.; Obiedat, A.; Darawshi, O.; Dipta, P.; Rimon, A.; McLennan, G.; Fassler, R.; Reichmann, D.; Karni, R.; et al. Pharmacological induction of selective endoplasmic reticulum retention as a strategy for cancer therapy. Nat. Commun. 2020, 11, 1304. [Google Scholar] [CrossRef]
- Chakravarty, G.; Mathur, A.; Mallade, P.; Gerlach, S.; Willis, J.; Datta, A.; Srivastav, S.; Abdel-Mageed, A.B.; Mondal, D. Nelfinavir targets multiple drug resistance mechanisms to increase the efficacy of doxorubicin in MCF-7/Dox breast cancer cells. Biochimie 2016, 124, 53–64. [Google Scholar] [CrossRef]
- Guan, M.; Fousek, K.; Jiang, C.; Guo, S.; Synold, T.; Xi, B.; Shih, C.C.; Chow, W.A. Nelfinavir induces liposarcoma apoptosis through inhibition of regulated intramembrane proteolysis of SREBP-1 and ATF6. Clin. Cancer Res. 2011, 17, 1796–1806. [Google Scholar] [CrossRef]
- Guan, M.; Fousek, K.; Chow, W.A. Nelfinavir inhibits regulated intramembrane proteolysis of sterol regulatory element binding protein-1 and activating transcription factor 6 in castration-resistant prostate cancer. FEBS J. 2012, 279, 2399–2411. [Google Scholar] [CrossRef]
- Sakakura, Y.; Shimano, H.; Sone, H.; Takahashi, A.; Inoue, N.; Toyoshima, H.; Suzuki, S.; Yamada, N. Sterol regulatory element-binding proteins induce an entire pathway of cholesterol synthesis. Biochem. Biophys. Res. Commun. 2001, 286, 176–183. [Google Scholar] [CrossRef] [PubMed]
- Brown, M.S.; Ye, J.; Rawson, R.B.; Goldstein, J.L. Regulated intramembrane proteolysis: A control mechanism conserved from bacteria to humans. Cell 2000, 100, 391–398. [Google Scholar] [CrossRef]
- Guan, M.; Su, L.; Yuan, Y.C.; Li, H.; Chow, W.A. Nelfinavir and nelfinavir analogs block site-2 protease cleavage to inhibit castration-resistant prostate cancer. Sci. Rep. 2015, 5, 9698. [Google Scholar] [CrossRef] [PubMed]
- De Gassart, A.; Martinon, F. Translating the anticancer properties of eEF2K. Cell Cycle. 2017, 16, 299–300. [Google Scholar] [CrossRef]
- De Gassart, A.; Demaria, O.; Panes, R.; Zaffalon, L.; Ryazanov, A.G.; Gilliet, M.; Martinon, F. Pharmacological eEF2K activation promotes cell death and inhibits cancer progression. EMBO Rep. 2016, 17, 1471–1484. [Google Scholar] [CrossRef] [PubMed]
- De Gassart, A.; Bujisic, B.; Zaffalon, L.; Decosterd, L.A.; Di Micco, A.; Frera, G.; Tallant, R.; Martinon, F. An inhibitor of HIV-1 protease modulates constitutive eIF2α dephosphorylation to trigger a specific integrated stress response. Proc. Natl. Acad. Sci. USA 2016, 113, E117–E126. [Google Scholar] [CrossRef]
- Johnson, C.E.; Hunt, D.K.; Wiltshire, M.; Herbert, T.P.; Sampson, J.R.; Errington, R.J.; Davies, D.M.; Tee, A.R. Endoplasmic reticulum stress and cell death in mTORC1-overactive cells is induced by nelfinavir and enhanced by chloroquine. Mol. Oncol. 2015, 9, 675–688. [Google Scholar] [CrossRef]
- Johnson, C.E.; Dunlop, E.A.; Seifan, S.; McCann, H.D.; Hay, T.; Parfitt, G.J.; Jones, A.T.; Giles, P.J.; Shen, M.H.; Sampson, J.R.; et al. Loss of tuberous sclerosis complex 2 sensitizes tumors to nelfinavir-bortezomib therapy to intensify endoplasmic reticulum stress-induced cell death. Oncogene 2018, 37, 5913–5925. [Google Scholar] [CrossRef]
- Dunlop, E.A.; Johnson, C.E.; Wiltshire, M.; Errington, R.J.; Tee, A.R. Targeting protein homeostasis with nelfinavir/salinomycin dual therapy effectively induces death of mTORC1 hyperactive cells. Oncotarget 2017, 8, 48711–48724. [Google Scholar] [CrossRef] [PubMed]
- McCann, H.D.; Johnson, C.E.; Errington, R.J.; Davies, D.M.; Dunlop, E.A.; Tee, A.R. Energy Stress-Mediated Cytotoxicity in Tuberous Sclerosis Complex 2-Deficient Cells with Nelfinavir and Mefloquine Treatment. Cancers 2018, 10, 375. [Google Scholar] [CrossRef] [PubMed]
- Kraus, M.; Bader, J.; Overkleeft, H.; Driessen, C. Nelfinavir augments proteasome inhibition by bortezomib in myeloma cells and overcomes bortezomib and carfilzomib resistance. Blood Cancer J. 2013, 3, e103. [Google Scholar] [CrossRef] [PubMed]
- Kraus, M.; Muller-Ide, H.; Ruckrich, T.; Bader, J.; Overkleeft, H.; Driessen, C. Ritonavir, nelfinavir, saquinavir and lopinavir induce proteotoxic stress in acute myeloid leukemia cells and sensitize them for proteasome inhibitor treatment at low micromolar drug concentrations. Leuk Res. 2014, 38, 383–392. [Google Scholar] [CrossRef]
- Driessen, C.; Kraus, M.; Joerger, M.; Rosing, H.; Bader, J.; Hitz, F.; Berset, C.; Xyrafas, A.; Hawle, H.; Berthod, G.; et al. Treatment with the HIV protease inhibitor nelfinavir triggers the unfolded protein response and may overcome proteasome inhibitor resistance of multiple myeloma in combination with bortezomib: A phase I trial (SAKK 65/08). Haematologica 2016, 101, 346–355. [Google Scholar] [CrossRef]
- Hitz, F.; Kraus, M.; Pabst, T.; Hess, D.; Besse, L.; Silzle, T.; Novak, U.; Seipel, K.; Rondeau, S.; Studeli, S.; et al. Nelfinavir and lenalidomide/dexamethasone in patients with lenalidomide-refractory multiple myeloma. A phase I/II Trial (SAKK 39/10). Blood Cancer J. 2019, 9, 70. [Google Scholar] [CrossRef]
- Mahoney, E.; Maddocks, K.; Flynn, J.; Jones, J.; Cole, S.L.; Zhang, X.; Byrd, J.C.; Johnson, A.J. Identification of endoplasmic reticulum stress-inducing agents by antagonizing autophagy: A new potential strategy for identification of anti-cancer therapeutics in B-cell malignancies. Leuk Lymphoma. 2013, 54, 2685–2692. [Google Scholar] [CrossRef]
- Yoshii, S.R.; Mizushima, N. Monitoring and Measuring Autophagy. Int. J. Mol. Sci. 2017, 18, 1865. [Google Scholar] [CrossRef]
- Mizushima, N.; Yoshimori, T. How to interpret LC3 immunoblotting. Autophagy 2007, 3, 542–545. [Google Scholar] [CrossRef]
- Gills, J.J.; Lopiccolo, J.; Dennis, P.A. Nelfinavir, a new anti-cancer drug with pleiotropic effects and many paths to autophagy. Autophagy 2008, 4, 107–109. [Google Scholar] [CrossRef]
- Escalante, A.M.; McGrath, R.T.; Karolak, M.R.; Dorr, R.T.; Lynch, R.M.; Landowski, T.H. Preventing the autophagic survival response by inhibition of calpain enhances the cytotoxic activity of bortezomib in vitro and in vivo. Cancer Chemother. Pharmacol. 2013, 71, 1567–1576. [Google Scholar] [CrossRef] [PubMed]
- Demarchi, F.; Bertoli, C.; Copetti, T.; Tanida, I.; Brancolini, C.; Eskelinen, E.-L.; Schneider, C. Calpain is required for macroautophagy in mammalian cells. J. Cell Biol. 2006, 175, 595–605. [Google Scholar] [CrossRef] [PubMed]
- Navon, A.; Ciechanover, A. The 26 S proteasome: From basic mechanisms to drug targeting. J. Biol. Chem. 2009, 284, 33713–33718. [Google Scholar] [CrossRef] [PubMed]
- Dimopoulos, M.A.; Moreau, P.; Palumbo, A.; Joshua, D.; Pour, L.; Hajek, R.; Facon, T.; Ludwig, H.; Oriol, A.; Goldschmidt, H.; et al. Carfilzomib and dexamethasone versus bortezomib and dexamethasone for patients with relapsed or refractory multiple myeloma (ENDEAVOR): A randomised, phase 3, open-label, multicentre study. Lancet Oncol. 2016, 17, 27–38. [Google Scholar] [CrossRef]
- Groll, M.; Berkers, C.R.; Ploegh, H.L.; Ovaa, H. Crystal structure of the boronic acid-based proteasome inhibitor bortezomib in complex with the yeast 20S proteasome. Structure 2006, 14, 451–456. [Google Scholar] [CrossRef] [PubMed]
- Demo, S.D.; Kirk, C.J.; Aujay, M.A.; Buchholz, T.J.; Dajee, M.; Ho, M.N.; Jiang, J.; Laidig, G.J.; Lewis, E.R.; Parlati, F.; et al. Antitumor activity of PR-171, a novel irreversible inhibitor of the proteasome. Cancer Res. 2007, 67, 6383–6391. [Google Scholar] [CrossRef]
- Besse, A.; Stolze, S.C.; Rasche, L.; Weinhold, N.; Morgan, G.J.; Kraus, M.; Bader, J.; Overkleeft, H.S.; Besse, L.; Driessen, C. Carfilzomib resistance due to ABCB1/MDR1 overexpression is overcome by nelfinavir and lopinavir in multiple myeloma. Leukemia 2018, 32, 391–401. [Google Scholar] [CrossRef]
- Shim, J.S.; Rao, R.; Beebe, K.; Neckers, L.; Han, I.; Nahta, R.; Liu, J.O. Selective inhibition of HER2-positive breast cancer cells by the HIV protease inhibitor nelfinavir. J. Natl. Cancer Inst. 2012, 104, 1576–1590. [Google Scholar] [CrossRef]
- Gupta, A.K.; Li, B.; Cerniglia, G.J.; Ahmed, M.S.; Hahn, S.M.; Maity, A. The HIV protease inhibitor nelfinavir downregulates Akt phosphorylation by inhibiting proteasomal activity and inducing the unfolded protein response. Neoplasia 2007, 9, 271–278. [Google Scholar] [CrossRef]
- Pajonk, F.; Himmelsbach, J.; Riess, K.; Sommer, A.; McBride, W.H. The human immunodeficiency virus (HIV)-1 protease inhibitor saquinavir inhibits proteasome function and causes apoptosis and radiosensitization in non-HIV-associated human cancer cells. Cancer Res. 2002, 62, 5230–5235. [Google Scholar]
- Piccinini, M.; Rinaudo, M.T.; Anselmino, A.; Buccinnà, B.; Ramondetti, C.; Dematteis, A.; Ricotti, E.; Palmisano, L.; Mostert, M.; Tovo, P.A. The HIV protease inhibitors nelfinavir and saquinavir, but not a variety of HIV reverse transcriptase inhibitors, adversely affect human proteasome function. Antivir. Ther. 2005, 10, 215–223. [Google Scholar] [PubMed]
- Fassmannová, D.; Sedlák, F.; Sedláček, J.; Špička, I.; Grantz Šašková, K. Nelfinavir Inhibits the TCF11/Nrf1-Mediated proteasome recovery pathway in multiple myeloma. Cancers 2020, 12, 1065. [Google Scholar] [CrossRef] [PubMed]
- Alfano, L.; Guida, T.; Provitera, L.; Vecchio, G.; Billaud, M.; Santoro, M.; Carlomagno, F. RET is a heat shock protein 90 (HSP90) client protein and is knocked down upon HSP90 pharmacological block. J. Clin. Endocrinol. Metab. 2010, 95, 3552–3557. [Google Scholar] [CrossRef] [PubMed]
- Carlomagno, F.; Guida, T.; Anaganti, S.; Vecchio, G.; Fusco, A.; Ryan, A.J.; Billaud, M.; Santoro, M. Disease associated mutations at valine 804 in the RET receptor tyrosine kinase confer resistance to selective kinase inhibitors. Oncogene 2004, 23, 6056–6063. [Google Scholar] [CrossRef] [PubMed]
- Petrich, A.M.; Leshchenko, V.; Kuo, P.Y.; Xia, B.; Thirukonda, V.K.; Ulahannan, N.; Gordon, S.; Fazzari, M.J.; Ye, B.H.; Sparano, J.A.; et al. Akt inhibitors MK-2206 and nelfinavir overcome mTOR inhibitor resistance in diffuse large B-cell lymphoma. Clin. Cancer Res. 2012, 18, 2534–2544. [Google Scholar] [CrossRef]
- Gupta, A.K.; Cerniglia, G.J.; Mick, R.; McKenna, W.G.; Muschel, R.J. HIV protease inhibitors block Akt signaling and radiosensitize tumor cells both in vitro and in vivo. Cancer Res. 2005, 65, 8256–8265. [Google Scholar] [CrossRef]
- Goda, J.S.; Pachpor, T.; Basu, T.; Chopra, S.; Gota, V. Targeting the AKT pathway: Repositioning HIV protease inhibitors as radiosensitizers. Indian J. Med. Res. 2016, 143, 145–159. [Google Scholar] [CrossRef]
- Bernhard, E.J.; Brunner, T.B. Progress towards the use of HIV protease inhibitors in cancer therapy. Cancer Biol. Ther. 2008, 7, 636–637. [Google Scholar] [CrossRef]
- Gupta, A.K.; Lee, J.H.; Wilke, W.W.; Quon, H.; Smith, G.; Maity, A.; Buatti, J.M.; Spitz, D.R. Radiation response in two HPV-infected head-and-neck cancer cell lines in comparison to a non-HPV-infected cell line and relationship to signaling through AKT. Int. J. Radiat. Oncol. Biol. Phys. 2009, 74, 928–933. [Google Scholar] [CrossRef]
- Jiang, Z.; Pore, N.; Cerniglia, G.J.; Mick, R.; Georgescu, M.M.; Bernhard, E.J.; Hahn, S.M.; Gupta, A.K.; Maity, A. Phosphatase and tensin homologue deficiency in glioblastoma confers resistance to radiation and temozolomide that is reversed by the protease inhibitor nelfinavir. Cancer Res. 2007, 67, 4467–4473. [Google Scholar] [CrossRef]
- Kimple, R.J.; Vaseva, A.V.; Cox, A.D.; Baerman, K.M.; Calvo, B.F.; Tepper, J.E.; Shields, J.M.; Sartor, C.I. Radiosensitization of epidermal growth factor receptor/HER2-positive pancreatic cancer is mediated by inhibition of Akt independent of ras mutational status. Clin. Cancer Res. 2010, 16, 912–923. [Google Scholar] [CrossRef] [PubMed]
- Cuneo, K.C.; Tu, T.; Geng, L.; Fu, A.; Hallahan, D.E.; Willey, C.D. HIV protease inhibitors enhance the efficacy of irradiation. Cancer Res. 2007, 67, 4886–4893. [Google Scholar] [CrossRef] [PubMed]
- Pore, N.; Gupta, A.K.; Cerniglia, G.J.; Jiang, Z.; Bernhard, E.J.; Evans, S.M.; Koch, C.J.; Hahn, S.M.; Maity, A. Nelfinavir down-regulates hypoxia-inducible factor 1alpha and VEGF expression and increases tumor oxygenation: Implications for radiotherapy. Cancer Res. 2006, 66, 9252–9259. [Google Scholar] [CrossRef] [PubMed]
- Pore, N.; Gupta, A.K.; Cerniglia, G.J.; Maity, A. HIV protease inhibitors decrease VEGF/HIF-1alpha expression and angiogenesis in glioblastoma cells. Neoplasia 2006, 8, 889–895. [Google Scholar] [CrossRef]
- Zeng, J.; See, A.P.; Aziz, K.; Thiyagarajan, S.; Salih, T.; Gajula, R.P.; Armour, M.; Phallen, J.; Terezakis, S.; Kleinberg, L.; et al. Nelfinavir induces radiation sensitization in pituitary adenoma cells. Cancer Biol. Ther. 2011, 12, 657–663. [Google Scholar] [CrossRef][Green Version]
- Plastaras, J.P.; Vapiwala, N.; Ahmed, M.S.; Gudonis, D.; Cerniglia, G.J.; Feldman, M.D.; Frank, I.; Gupta, A.K. Validation and toxicity of PI3K/Akt pathway inhibition by HIV protease inhibitors in humans. Cancer Biol. Ther. 2008, 7, 628–635. [Google Scholar] [CrossRef]
- Brunner, T.B.; Geiger, M.; Grabenbauer, G.G.; Lang-Welzenbach, M.; Mantoni, T.S.; Cavallaro, A.; Sauer, R.; Hohenberger, W.; McKenna, W.G. Phase I trial of the human immunodeficiency virus protease inhibitor nelfinavir and chemoradiation for locally advanced pancreatic cancer. J. Clin. Oncol. 2008, 26, 2699–2706. [Google Scholar] [CrossRef]
- Gupta, A.K.; Wilke, W.W.; Taylor, E.N.; Bodeker, K.L.; Hoffman, H.T.; Milhem, M.M.; Buatti, J.M.; Robinson, R.A. Signaling pathways in adenoid cystic cancers: Implications for treatment. Cancer Biol. Ther. 2009, 8, 1947–1951. [Google Scholar] [CrossRef]
- Hoover, A.C.; Milhem, M.M.; Anderson, C.M.; Sun, W.; Smith, B.J.; Hoffman, H.T.; Buatti, J.M. Efficacy of nelfinavir as monotherapy in refractory adenoid cystic carcinoma: Results of a phase II clinical trial. Head Neck 2015, 37, 722–726. [Google Scholar] [CrossRef]
- Liebscher, S.; Koi, L.; Lock, S.; Muders, M.H.; Krause, M. The HIV protease and PI3K/Akt inhibitor nelfinavir does not improve the curative effect of fractionated irradiation in PC-3 prostate cancer in vitro and in vivo. Clin. Transl. Radiat. Oncol. 2017, 2, 7–12. [Google Scholar] [CrossRef][Green Version]
- Bruning, A. Targeting the off-targets: A computational bioinformatics approach to understanding the polypharmacology of nelfinavir. Expert Rev. Clin. Pharmacol. 2011, 4, 571–573. [Google Scholar] [CrossRef] [PubMed]
- Ikezoe, T.; Saito, T.; Bandobashi, K.; Yang, Y.; Koeffler, H.P.; Taguchi, H. HIV-1 protease inhibitor induces growth arrest and apoptosis of human multiple myeloma cells via inactivation of signal transducer and activator of transcription 3 and extracellular signal-regulated kinase 1/2. Mol. Cancer Ther. 2004, 3, 473–479. [Google Scholar] [PubMed]
- Smith, M.P.; Brunton, H.; Rowling, E.J.; Ferguson, J.; Arozarena, I.; Miskolczi, Z.; Lee, J.L.; Girotti, M.R.; Marais, R.; Levesque, M.P.; et al. Inhibiting Drivers of Non-mutational Drug Tolerance Is a Salvage Strategy for Targeted Melanoma Therapy. Cancer Cell 2016, 29, 270–284. [Google Scholar] [CrossRef] [PubMed]
- Bali, P.; Pranpat, M.; Bradner, J.; Balasis, M.; Fiskus, W.; Guo, F.; Rocha, K.; Kumaraswamy, S.; Boyapalle, S.; Atadja, P.; et al. Inhibition of histone deacetylase 6 acetylates and disrupts the chaperone function of heat shock protein 90: A novel basis for antileukemia activity of histone deacetylase inhibitors. J. Biol. Chem. 2005, 280, 26729–26734. [Google Scholar] [CrossRef]
- Liu, J.; Wang, Z. Increased Oxidative Stress as a Selective Anticancer Therapy. Oxid. Med. Cell Longev. 2015, 2015, 294303. [Google Scholar] [CrossRef]
- Kushchayeva, Y.; Jensen, K.; Burman, K.D.; Vasko, V. Repositioning therapy for thyroid cancer: New insights on established medications. Endocr. Relat. Cancer 2014, 21, R183–R194. [Google Scholar] [CrossRef]
- Xia, C.; He, Z.; Liang, S.; Chen, R.; Xu, W.; Yang, J.; Xiao, G.; Jiang, S. Metformin combined with nelfinavir induces SIRT3/mROS-dependent autophagy in human cervical cancer cells and xenograft in nude mice. Eur. J. Pharmacol. 2019, 848, 62–69. [Google Scholar] [CrossRef]
- Chen, Y.; Fu, L.L.; Wen, X.; Wang, X.Y.; Liu, J.; Cheng, Y.; Huang, J. Sirtuin-3 (SIRT3), a therapeutic target with oncogenic and tumor-suppressive function in cancer. Cell Death Dis. 2014, 5, e1047. [Google Scholar] [CrossRef]
- Rockwell, S.; Dobrucki, I.T.; Kim, E.Y.; Marrison, S.T.; Vu, V.T. Hypoxia and radiation therapy: Past history, ongoing research, and future promise. Curr. Mol. Med. 2009, 9, 442–458. [Google Scholar] [CrossRef]
- Qayum, N.; Im, J.; Stratford, M.R.; Bernhard, E.J.; McKenna, W.G.; Muschel, R.J. Modulation of the tumor microvasculature by phosphoinositide-3 kinase inhibition increases doxorubicin delivery in vivo. Clin. Cancer Res. 2012, 18, 161–169. [Google Scholar] [CrossRef]
- Bourlier, V.; Zakaroff-Girard, A.; De Barros, S.; Pizzacalla, C.; de Saint Front, V.D.; Lafontan, M.; Bouloumie, A.; Galitzky, J. Protease inhibitor treatments reveal specific involvement of matrix metalloproteinase-9 in human adipocyte differentiation. J. Pharmacol. Exp. Ther. 2005, 312, 1272–1279. [Google Scholar] [CrossRef] [PubMed]
- Kast, R.E.; Halatsch, M.E. Matrix metalloproteinase-2 and -9 in glioblastoma: A trio of old drugs-captopril, disulfiram and nelfinavir-are inhibitors with potential as adjunctive treatments in glioblastoma. Arch. Med. Res. 2012, 43, 243–247. [Google Scholar] [CrossRef] [PubMed]
- Al-Assar, O.; Bittner, M.I.; Lunardi, S.; Stratford, M.R.; McKenna, W.G.; Brunner, T.B. The radiosensitizing effects of Nelfinavir on pancreatic cancer with and without pancreatic stellate cells. Radiother. Oncol. 2016, 119, 300–305. [Google Scholar] [CrossRef] [PubMed]
- Darini, C.Y.; Martin, P.; Azoulay, S.; Drici, M.D.; Hofman, P.; Obba, S.; Dani, C.; Ladoux, A. Targeting cancer stem cells expressing an embryonic signature with anti-proteases to decrease their tumor potential. Cell Death. Dis. 2013, 4, e706. [Google Scholar] [CrossRef]
- Giardino Torchia, M.L.; Ciaglia, E.; Masci, A.M.; Vitiello, L.; Fogli, M.; la Sala, A.; Mavilio, D.; Racioppi, L. Dendritic cells/natural killer cross-talk: A novel target for human immunodeficiency virus type-1 protease inhibitors. PLoS ONE 2010, 5, e11052. [Google Scholar] [CrossRef] [PubMed]
- Rees, D.C.; Johnson, E.; Lewinson, O. ABC transporters: The power to change. Nat. Rev. Mol. Cell Biol. 2009, 10, 218–227. [Google Scholar] [CrossRef] [PubMed]
- Misra, S.; Ghatak, S.; Toole, B.P. Regulation of MDR1 expression and drug resistance by a positive feedback loop involving hyaluronan, phosphoinositide 3-kinase, and ErbB2. J. Biol. Chem. 2005, 280, 20310–20315. [Google Scholar] [CrossRef]
- Kim, J.Y.; Park, Y.J.; Lee, B.M.; Yoon, S. Co-treatment With HIV Protease Inhibitor Nelfinavir Greatly Increases Late-phase Apoptosis of Drug-resistant KBV20C Cancer Cells Independently of P-Glycoprotein Inhibition. Anticancer Res. 2019, 39, 3757–3765. [Google Scholar] [CrossRef]
- Lucia, M.B.; Anu, R.; Handley, M.; Gillet, J.P.; Wu, C.P.; De Donatis, G.M.; Cauda, R.; Gottesman, M.M. Exposure to HIV-protease inhibitors selects for increased expression of P-glycoprotein (ABCB1) in Kaposi’s sarcoma cells. Br. J. Cancer 2011, 105, 513–522. [Google Scholar] [CrossRef]
- Perloff, M.D.; von Moltke, L.L.; Fahey, J.M.; Daily, J.P.; Greenblatt, D.J. Induction of P-glycoprotein expression by HIV protease inhibitors in cell culture. AIDS 2000, 14, 1287–1289. [Google Scholar] [CrossRef]
- Gupta, A.; Zhang, Y.; Unadkat, J.D.; Mao, Q. HIV protease inhibitors are inhibitors but not substrates of the human breast cancer resistance protein (BCRP/ABCG2). J. Pharmacol. Exp. Ther. 2004, 310, 334–341. [Google Scholar] [CrossRef] [PubMed]
- Fukuda, Y.; Takenaka, K.; Sparreboom, A.; Cheepala, S.B.; Wu, C.P.; Ekins, S.; Ambudkar, S.V.; Schuetz, J.D. Human immunodeficiency virus protease inhibitors interact with ATP binding cassette transporter 4/multidrug resistance protein 4: A basis for unanticipated enhanced cytotoxicity. Mol. Pharmacol. 2013, 84, 361–371. [Google Scholar] [CrossRef] [PubMed]
- Rengan, R.; Mick, R.; Pryma, D.; Rosen, M.A.; Lin, L.L.; Maity, A.M.; Evans, T.L.; Stevenson, J.P.; Langer, C.J.; Kucharczuk, J.; et al. A phase I trial of the HIV protease inhibitor nelfinavir with concurrent chemoradiotherapy for unresectable stage IIIA/IIIB non-small cell lung cancer: A report of toxicities and clinical response. J. Thorac. Oncol. 2012, 7, 709–715. [Google Scholar] [CrossRef] [PubMed]
- Rengan, R.; Mick, R.; Pryma, D.A.; Lin, L.L.; Christodouleas, J.; Plastaras, J.P.; Simone, C.B., 2nd; Gupta, A.K.; Evans, T.L.; Stevenson, J.P.; et al. Clinical Outcomes of the HIV Protease Inhibitor Nelfinavir With Concurrent Chemoradiotherapy for Unresectable Stage IIIA/IIIB Non-Small Cell Lung Cancer: A Phase 1/2 Trial. JAMA Oncol. 2019, 5, 1464–1472. [Google Scholar] [CrossRef] [PubMed]
- Wilson, J.M.; Fokas, E.; Dutton, S.J.; Patel, N.; Hawkins, M.A.; Eccles, C.; Chu, K.Y.; Durrant, L.; Abraham, A.G.; Partridge, M.; et al. ARCII: A phase II trial of the HIV protease inhibitor Nelfinavir in combination with chemoradiation for locally advanced inoperable pancreatic cancer. Radiother. Oncol. 2016, 119, 306–311. [Google Scholar] [CrossRef]
- Strauss, V.Y.; Shaw, R.; Virdee, P.S.; Hurt, C.N.; Ward, E.; Tranter, B.; Patel, N.; Bridgewater, J.; Parsons, P.; Radhakrishna, G.; et al. Study protocol: A multi-centre randomised study of induction chemotherapy followed by capecitabine +/− nelfinavir with high- or standard-dose radiotherapy for locally advanced pancreatic cancer (SCALOP-2). BMC Cancer 2019, 19, 121. [Google Scholar] [CrossRef]
- Lin, C.; Verma, V.; Ly, Q.P.; Lazenby, A.; Sasson, A.; Schwarz, J.K.; Meza, J.L.; Are, C.; Li, S.; Wang, S.; et al. Phase I trial of concurrent stereotactic body radiotherapy and nelfinavir for locally advanced borderline or unresectable pancreatic adenocarcinoma. Radiother. Oncol. 2019, 132, 55–62. [Google Scholar] [CrossRef]
- Lin, C.; Verma, V.; Lazenby, A.; Ly, Q.P.; Berim, L.D.; Schwarz, J.K.; Madiyalakan, M.; Nicodemus, C.F.; Hollingsworth, M.A.; Meza, J.L.; et al. Phase I/II Trial of Neoadjuvant Oregovomab-based Chemoimmunotherapy Followed by Stereotactic Body Radiotherapy and Nelfinavir For Locally Advanced Pancreatic Adenocarcinoma. Am. J. Clin. Oncol. 2019, 42, 755–760. [Google Scholar] [CrossRef]
- Pan, J.; Mott, M.; Xi, B.; Hepner, E.; Guan, M.; Fousek, K.; Magnusson, R.; Tinsley, R.; Valdes, F.; Frankel, P.; et al. Phase I study of nelfinavir in liposarcoma. Cancer Chemother. Pharmacol. 2012, 70, 791–799. [Google Scholar] [CrossRef]
- Leung-Hagesteijn, C.; Erdmann, N.; Cheung, G.; Keats, J.J.; Stewart, A.K.; Reece, D.E.; Chung, K.C.; Tiedemann, R.E. Xbp1s-negative tumor B cells and pre-plasmablasts mediate therapeutic proteasome inhibitor resistance in multiple myeloma. Cancer Cell 2013, 24, 289–304. [Google Scholar] [CrossRef]
- Hill, E.J.; Roberts, C.; Franklin, J.M.; Enescu, M.; West, N.; MacGregor, T.P.; Chu, K.Y.; Boyle, L.; Blesing, C.; Wang, L.M.; et al. Clinical Trial of Oral Nelfinavir before and during Radiation Therapy for Advanced Rectal Cancer. Clin. Cancer Res. 2016, 22, 1922–1931. [Google Scholar] [CrossRef] [PubMed]
- Buijsen, J.; Lammering, G.; Jansen, R.L.; Beets, G.L.; Wals, J.; Sosef, M.; Den Boer, M.O.; Leijtens, J.; Riedl, R.G.; Theys, J.; et al. Phase I trial of the combination of the Akt inhibitor nelfinavir and chemoradiation for locally advanced rectal cancer. Radiother. Oncol. 2013, 107, 184–188. [Google Scholar] [CrossRef] [PubMed]
- Bernstein, W.B.; Dennis, P.A. Repositioning HIV protease inhibitors as cancer therapeutics. Curr. Opin. HIV AIDS 2008, 3, 666–675. [Google Scholar] [CrossRef] [PubMed]
- Alonso-Basanta, M.; Fang, P.; Maity, A.; Hahn, S.M.; Lustig, R.A.; Dorsey, J.F. A phase I study of nelfinavir concurrent with temozolomide and radiotherapy in patients with glioblastoma multiforme. J. Neurooncol. 2014, 116, 365–372. [Google Scholar] [CrossRef]
- Kattel, K.; Evande, R.; Tan, C.; Mondal, G.; Grem, J.L.; Mahato, R.I. Impact of CYP2C19 polymorphism on the pharmacokinetics of nelfinavir in patients with pancreatic cancer. Br. J. Clin. Pharmacol. 2015, 80, 267–275. [Google Scholar] [CrossRef]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).