Abstract
The severe acute respiratory syndrome coronavirus-2 (SARS-CoV-2) has recently emerged in China and caused a disease called coronavirus disease 2019 (COVID-19). The virus quickly spread around the world, causing a sustained global outbreak. Although SARS-CoV-2, and other coronaviruses, SARS-CoV and Middle East respiratory syndrome CoV (MERS-CoV) are highly similar genetically and at the protein production level, there are significant differences between them. Research has shown that the structural spike (S) protein plays an important role in the evolution and transmission of SARS-CoV-2. So far, studies have shown that various genes encoding primarily for elements of S protein undergo frequent mutation. We have performed an in-depth review of the literature covering the structural and mutational aspects of S protein in the context of SARS-CoV-2, and compared them with those of SARS-CoV and MERS-CoV. Our analytical approach consisted in an initial genome and transcriptome analysis, followed by primary, secondary and tertiary protein structure analysis. Additionally, we investigated the potential effects of these differences on the S protein binding and interactions to angiotensin-converting enzyme 2 (ACE2), and we established, after extensive analysis of previous research articles, that SARS-CoV-2 and SARS-CoV use different ends/regions in S protein receptor-binding motif (RBM) and different types of interactions for their chief binding with ACE2. These differences may have significant implications on pathogenesis, entry and ability to infect intermediate hosts for these coronaviruses. This review comprehensively addresses in detail the variations in S protein, its receptor-binding characteristics and detailed structural interactions, the process of cleavage involved in priming, as well as other differences between coronaviruses.
1. Introduction
A novel coronavirus (severe acute respiratory syndrome coronavirus-2, or SARS-CoV-2) emerged in China in 2019. It causes illness in humans termed coronavirus disease 2019 (COVID-19). The symptoms of this disease are similar to those of SARS-CoV in humans, and can lead to fatal respiratory tract infection. Phylogenetic studies have shown that SARS-CoV-2 is a beta-coronavirus [1] that belongs to a group of SARS-CoV and SARS-like bat-derived viruses (ZC45 and ZCX21) [2]. Coronaviruses are composed of short-strand ribonucleic acid (ssRNA) as genetic material. The RNA strands in coronaviruses range in length from 26 to 32 kbs [3].
In the early weeks of the COVID-19 pandemic, the WHO expected that the production of an effective vaccine against SARS-CoV-2 would probably require 18 months of development. This encouraged researchers to assess the potential antiviral effects of existing drugs against COVID-19, as such, an approach could be cost- and time-effective amid the current situation [4]. Extensive trials have been performed to investigate the possibility of repurposing currently-used FDA approved drugs to treat COVID-19. There are also many drugs in development to target the virus directly. For example, a protease inhibitor, camostat mesylate, has been demonstrated to inhibit SARS-CoV-2 infection and prevent the entry of the virus mediated by the spike (S) protein into primary human lung cells [5,6]. The S proteins offer a good druggable target, since they cover the virus surface, and are key to initiate binding to the host cell receptors angiotensin converting enzyme 2 (ACE2) and the transmembrane serine protease (TMPRSS2), leading to subsequent internalization and infection.
ACE2 is a type I membrane zinc-containing enzyme that is expressed on the surface of endothelial cells in the lungs, as well as some other cell types and tissues [7]. Specifically, ACE2 is attached to the cell membrane of main pulmonary type II cells, the entericytes of the small intestines, arterial and vein endothelial cells and smooth arterial muscle cells in most organs. The protein of ACE2 contains the N-terminal peptidase M2 domain and the C-terminal amino acid collectrin transporter domain [8].
The amino acids that interact at the ACE2 and SARS-CoV-2 receptor-binding domain (RBD) interface have been analyzed through the crystal structure (PDB IDs: 6LZG and 6M17) [2,9,10]. In total, 15 residues from ACE2 interact with the RBD: residues Gln24, Thr27, Asp30, Lys31, His34, Glu35, Glu37, Asp38, Tyr41 and Gln42 are in α1, one residue (residue Met82) comes from α2, while the residues Lys353, Gly354, Asp355 and Arg357 come from the linker between β3 and β4. Therefore, these 15 amino acids in ACE2 can be labelled as critical amino acids for binding, and the α1, α2, β3, and β4 secondary structure elements as ACE2 critical binding components to the S protein [9].
Many studies have been performed to design a therapeutic peptide based on ACE2, which could act as an antagonist for binding. In one study, it was found that the single α1-helix used in inhibitor 1 was somewhat unstable, whereas the α1 and α2-helices that were used in inhibitors 2–4 supported each other and retained their bent shape, which provided a conformational match to the RBD of SARS-CoV-2, and fully covered the RBD surface. Precise conformational matching between the designed peptides and the virus provides an opportunity to further improve the binding affinity, which should be considered in future inhibitor design protocols [9]. Moreover, Battle and associates also proposed the use of the already available recombinant ACE2 to intercept COVID-19 and, therefore, to attenuate infection [11,12].
Studies have shown that proteins of different coronaviruses display sequence variations that cause differences in the three dimensional (3D) structures, and, thus, in the shape of their binding contacts [13]. The current review compares the structure of S protein from SARS-CoV-2, SARS-CoV and MERS-CoV, and shows the genetic variability between them, with pinpointing potentially significant variations capable of altering binding contacts. Understanding the potential effects of these variations would be helpful towards determining the range of available intermediate hosts, as well as their effects on immunogenicity and treatment. Structural information at this atomic level has the potential to improve our understanding of the interactions between SARS-CoV-2 and its variants with infection susceptible cells, help identify robust target regions for neutralizing antibodies and assist with structure-based drug and vaccine design, urgently needed in the fight against SARS-CoV-2 [6].
3. Differences in Transcriptome
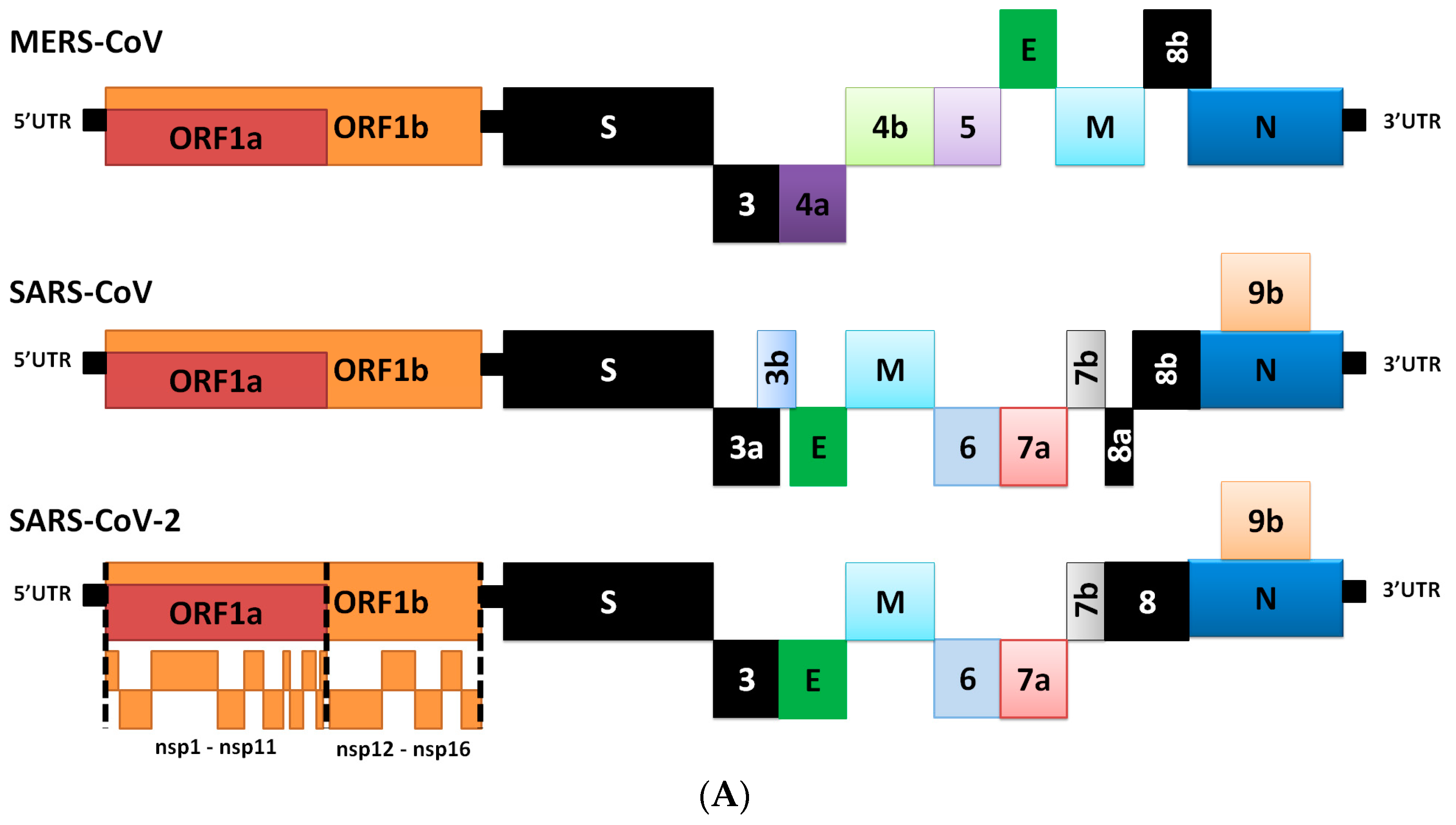
Each coronaviral RNA contains a standard 50 nt lead sequence that is fused from the downstream genome of the body sequence [19]. The coronavirus genome is used as the template for replication and transcription mediated by nsp12 (harboring RNA dependent RNA polymerase (RdRp) activity). Negative-sense RNA intermediates are generated to serve as the templates for the synthesis of positive-sense genomic RNA (gRNA) and subgenomic RNAs (sgRNAs) [14]. The gRNA is packaged by the structural proteins to produce new progeny virions. Shorter sgRNAs encode conserved structural proteins (including S, E, M, N and accessory proteins). SARS-CoV-2 has at least six accessory proteins (3a, 6, 7a, 7b, 8 and 10). However, SARS-CoV-2 ORFs have not yet been experimentally verified for expression. Therefore, it is currently unclear which accessory genes are actually expressed from this compact genome [14].
During negative-strand synthesis, RdRp pauses when it crosses a transcription regulatory sequence (TRS) in the body (TRS-B) and switches to the TRS in the leader (TRS-L), which results in discontinuous transcription leading to the leader-body fusion. This pause results in discontinuous transcription that results in leader-body fusion during negative-strand synthesis. Positive-strand mRNAs are transcribed from the fused negative-strand intermediates. These components can be used to develop diagnostic and therapeutic tools based on the SARS-CoV-2 genome organization. It is unclear whether the general mechanism is applicable to SARS-CoV-2. ORFs that have been deleted or frameshifted may produce short proteins that are distinct from known viral proteins. In addition to the 10 canonical RNA (one genomic and nine subgenomic), SARS-CoV-2 produces transcripts encoding unknown ORFs with fusion, deletion and/or frameshift. In the future, it will be interesting to examine whether these unknown ORFs are translated and whether they produce functional products [14].
The tail of SARS-CoV-2 RNAs has a median length of 47 nt. The full-length gRNA has a longer tail than do sub-genomic RNAs (sgRNAs). SgRNAs have, in particular, two tail populations: a minor of 30 nt and a major of 45 nt [14]. It has already been noted that poly(A) tail lengths change from 45 nt immediately after infection to 65 nt after six to nine hours of infection and to 30 nt after 140 h of infection [24]. It has been shown that nsp8 has an adenylyltransferase activity, which may extend the poly(A) tail of viral RNA [25,26]. The poly(A) tail of mRNA is also critical to control stability and translation through its interaction with poly(A) binding proteins (PABPs). The tail is likely to play multiple roles in translation and replication.
A minimum of 41 sites have been reported to display substantial differences in the transcripts of SARS-CoV-2. Such variety indicates potential RNA modifications. The motif that has been most commonly reported among these modification sites is AAGAA. Change sites that form an “AAGAA-like” pattern (including A/G rich sequences) are especially enriched in 28.5 to 29.5 kb genomic positions. Long viral transcripts (gRNA, S, 3a, E and M) are more frequently modified than short RNAs (6, 7a, 7b, 8 and N), which suggests a modification mechanism that is specific to certain RNA species. Interestingly, modified RNA molecules have shorter poly(A) tails than unmodified ones, which suggests that there is a link between the internal modification and 3′-end tail, and, thus, with viral RNA stability control. It is also plausible that RNA modification is a mechanism to evade host-immune response [14]. It will be interesting, in the future, to identify the chemical nature, enzymology and biological functions of these modifications. The new ORFs may serve as a source of accessory proteins that modulate viral replication and host-immune response. The RNA modifications may also contribute to viral survival and evasion of immunity in infected tissues, as the innate immune system is less sensitive to RNAs with nucleoside modification than to those without modification [14].
4. Role of S Protein in Pathogenesis
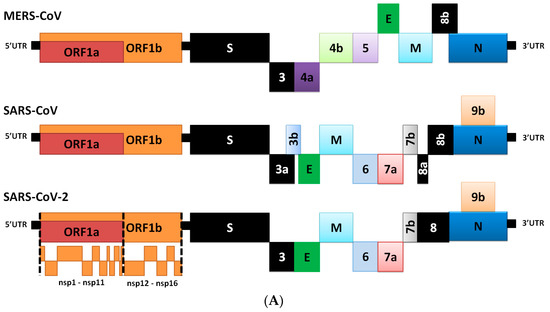
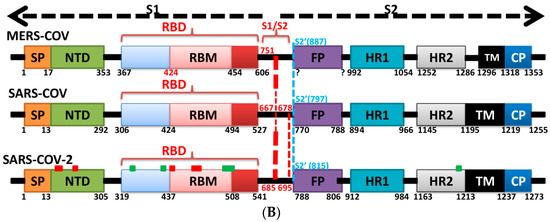
The outer surface of the coronavirus SARS-CoV-2 is made up of four structural proteins: S, E, M and N (Table 1 and Figure 1A) [17]. The S protein (~1200 aa long, about 180 kDa) [27] mediates the interaction of the virus with the host cell-surface receptors and their subsequent fusion. Coronavirus replication begins with attachment and entrance of the virus into the host cell, through interactions between the S protein and its receptor. After the receptor attachment to ACE2, the host-cell cytosol enters the virus by the cleavage of S protein (cleavage of S1 from S2) by a protease enzyme (i.e., transmembrane protease serine 2 (TMPRSS2)). This procedure is followed by fusion of the virus and the host-cell membranes. The next step is the translation of the replicase enzyme from the virion genomic RNA, and the translation and assembly of the viral replicase complexes. Encapsidation results in the formation of the mature virus after replication and the subgenomic RNA synthesis. Virions are then transported in vesicles to the cell surface and released through exocytosis [28] (Figure 2). Cryo-electron microscopy studies of the SARS-CoV S protein and its interaction with the cell receptor ACE2 have demonstrated that S1 and ACE2 binding prompts the S2 section to move from a metastable pre-fusion state, to a more stable post-fusion state, which is essential for membrane fusion [6].
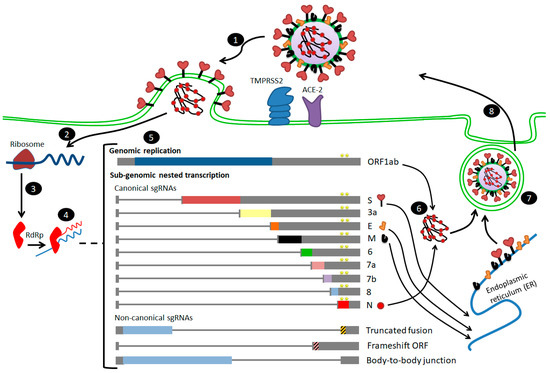
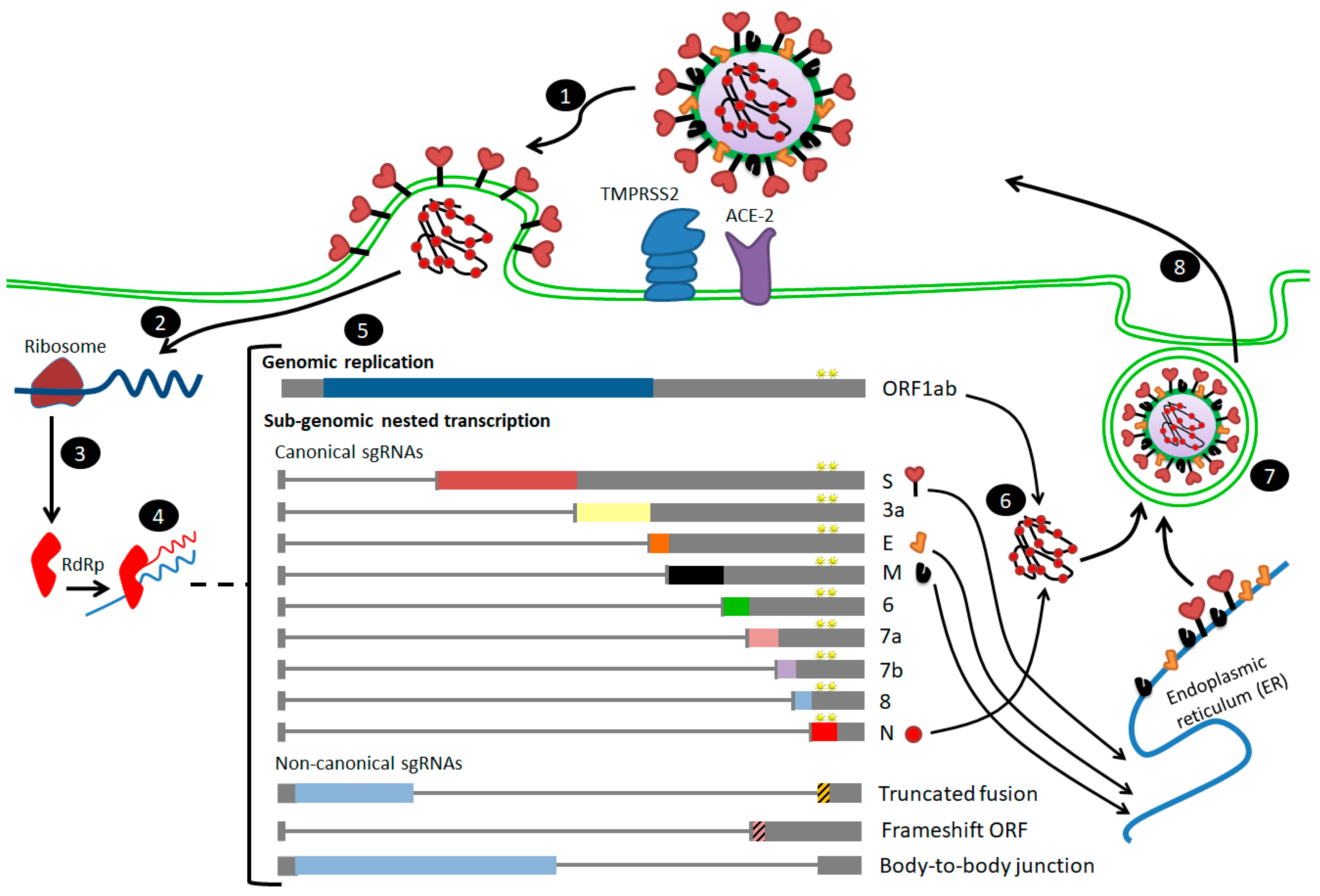
Figure 2.
Steps of SARS-CoV-2 infection and entry to the host cell [14,29]. (1) After receptor (angiotensin-converting enzyme 2 (ACE2)) binding, the virus enters host cell cytosol via cleavage of S protein by a protease enzyme (transmembrane protease serine 2 (TMPRSS2)), followed by fusion of the viral and cellular membranes. (2) Upon cell entry, the genomic RNA is translated to produce non-structural proteins from two open reading frames, ORF1a and ORF1b. (3) Some of the nsps have RNA-dependent RNA polymerase (RdRp) activity (nsp12). (4) Negative-sense RNA intermediates are generated to serve as the templates for the synthesis of positive-sense genomic RNA (gRNA), and (5) sub-genomic RNAs (sgRNAs). (6) The gRNA is packaged by the structural proteins to assemble progeny virions. Shorter sgRNAs encode conserved structural proteins (S, E, M and N), and several accessory proteins. SARS-CoV-2 is known to have at least six accessory proteins (3a, 6, 7a, 7b, 8 and 10), and non-canonical sgRNAs are also shown in the figure. The AAGAA-type modification clusters in gRNA and sgRNAs are shown with yellow stars annotations. (7,8) budding and exocytosis of the virus occur.
Several mutated amino-acid residues in the HR1 domain may be associated with enhanced interactions with the HR2 domain and, thus, enhanced membrane fusion [21]. The presence of a furin-like cleavage site in SARS-CoV-2 has also been found to facilitate the priming of the S protein, and to improve the efficiency of the spread of SARS-CoV-2 compared with other beta coronaviruses [30]. Plasmin and other proteases have been shown to cleave a newly inserted furin site extracellularly in the S protein of SARS-CoV 2, and this procedure increases the virus’ infectivity and virulence. The plasmin system may offer a promising therapeutic target to combat SARS-CoV-2 infection [31]. Collectively, these results indicate SARS-CoV-2 is closely related to SARS-CoV, and suggest SARS-CoV-2 may use various novel glycosylation sites, which may contribute to its pandemic spread, owing to its antigenic discrepancy to previous coronaviruses [32].
6. Is ACE2 the Receptor for S Protein?
It has been reported that the spike glycoprotein of SARS-CoV-2 is modified via homologous recombination and is a mixture of bat SARS-CoV and an unknown Beta-CoV [3,32]. Superimposition of the cryo-EM structure of the RBD of SARS-514 CoV-2 onto a previously reported SARS RBD structure revealed a root-mean-square deviation (RMSD) of 3.8 Å over 959 Cα atoms [2], which indicates highly similar 3D protein structures [63,64,65].
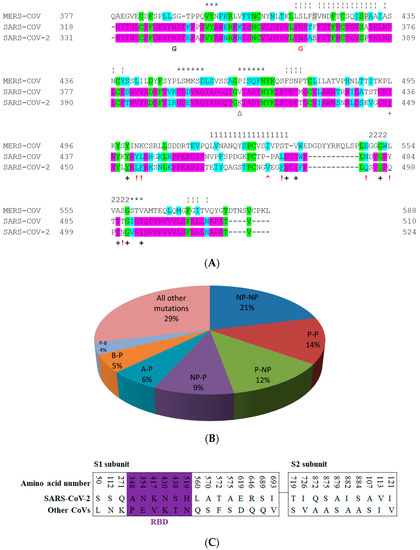
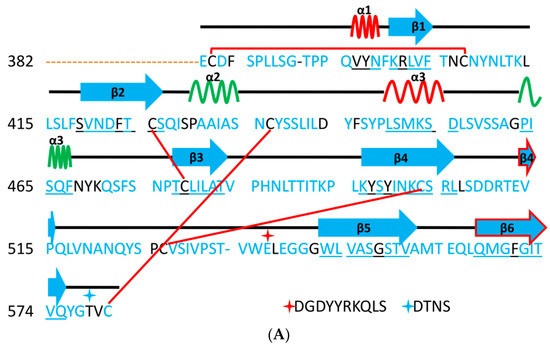
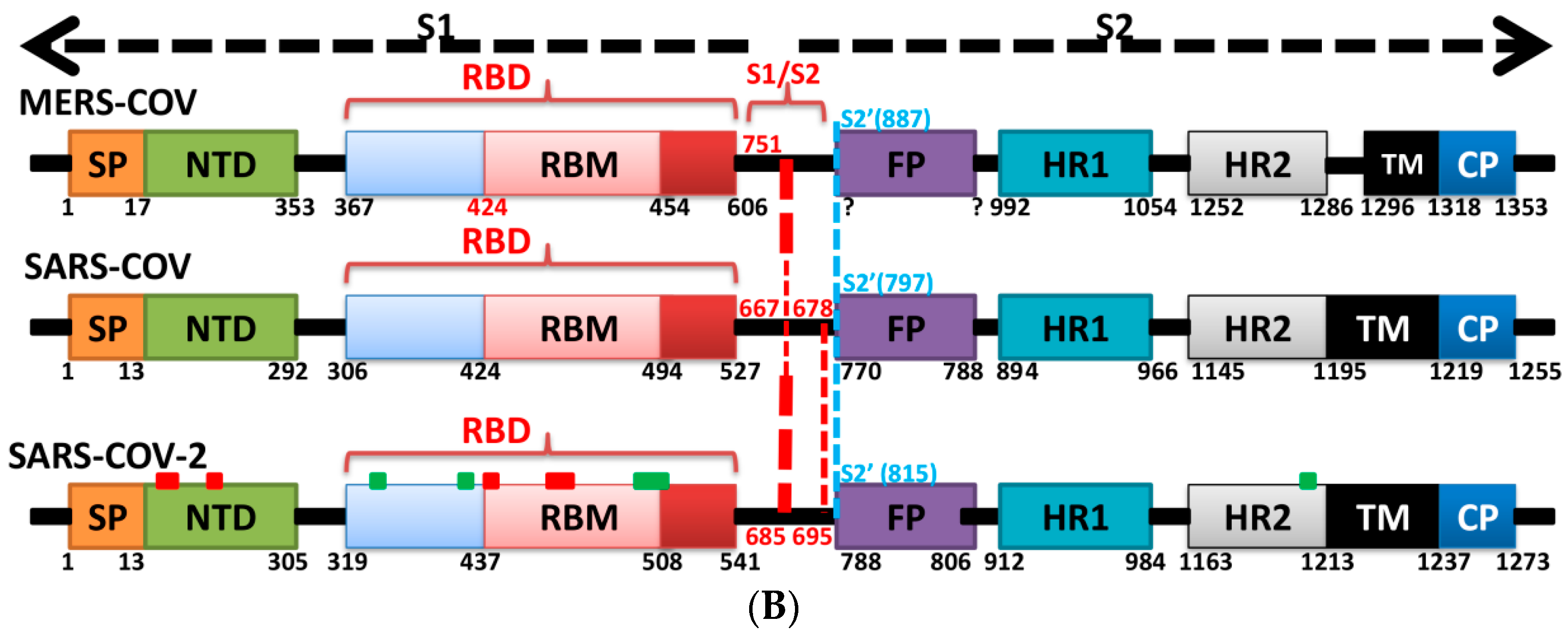
Sequence similarities between SARS-CoV-2 and SARS-CoV spikes imply that they share the same ACE2 receptor. Importantly, compared with the SARS-CoV RBM, the SARS-CoV-2 RBM does not contain any deletion or insertion, except for a single-residue (Val483) insertion in TR1 (Figure 3A and Figure 4K). This information provides additional evidence that SARS-CoV-2 uses ACE2 as its receptor [1,66]. Other evidence that ACE2 is the receptor for SARS-CoV-2 is that, among the 14 ACE2 contacting residues in the RBD, nine are fully conserved and four are partially conserved in SARS-CoV-2 and SARS-CoV (Figure 3) [1,27].
However, it has been reported that there are no data on the relationship between ACE2 activity and SARS-CoV-2 mortality [67]. On the other hand, it has been reported that some cell types in the host that express ACE2 beyond lung epithelial cells, are not attacked by the SARS-CoV-2 virus, while cells that lack ACE2 can bind the SARS-CoV-2 virus [68]. The differences in S protein may have implications for the virulence of SARS-CoV-2 and its binding affinity, which will affect vaccine and therapy development; for example, polyclonal anti-SARS S1 antibodies T62 inhibit entry of SARS-CoV S, but not SARS-CoV-2 S pseudo-virions [69]. The S protein is a homotrimeric glycoprotein fusion class I (Figure 7), which, in a metastable conformation prefusion, undergoes a substantial structural rearrangement in order to fuse the viral membrane and the host cell membrane [2,15,27,70,71,72,73].
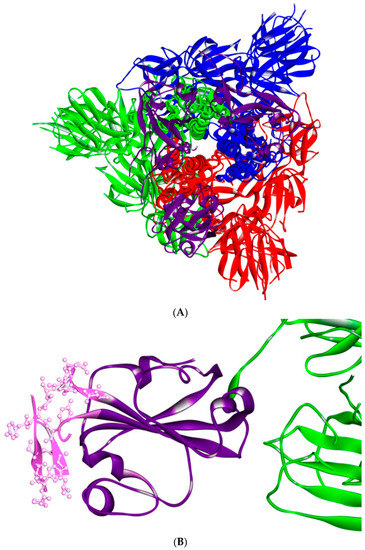
Figure 7.
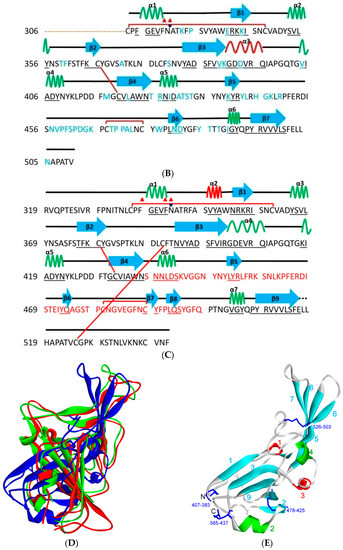
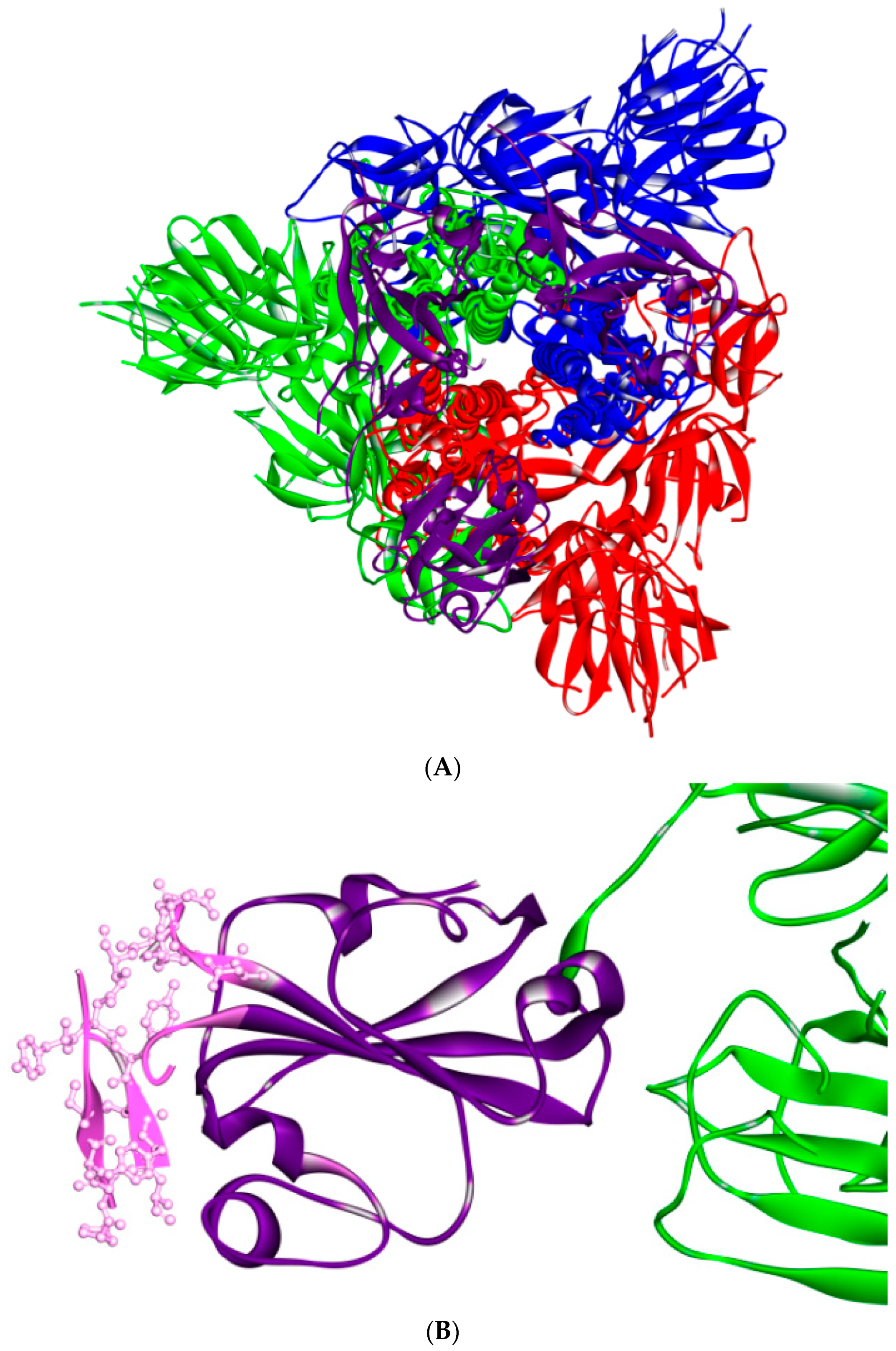
Structure of S protein (PDB ID: 6vsb) [14]. (A) RBD is shown in violet. (B) Close side view of RBD in violet, with receptor-binding motif (RBM) annotated in pink. Three-dimensional models were created using Discovery Studio (version 2.5.5, Biovia, San Diego, CA, USA).
This process is triggered when the S1 subunit binds to a host-cell receptor. Receptor binding destabilizes the pre-fusion trimer (in which receptor binding to RBDs leads to an unstable RBD up-conformation) and the result is the shedding of the S1 subunit and transition of the S2 subunit to a stable post-fusion conformation. It has been shown that the RBD of SARS-CoV-2 S1 undergoes hinge-like conformational movements (which are also a feature that is found in SARS-CoV, MERS-CoV and some alpha-coronaviruses) that transiently hide or expose the determinants of receptor binding. These two states are referred to as the “down” conformation and the “up” conformation, in which the “down” conformation corresponds to the receptor-inaccessible state [15]. The ACE2 host receptor can only interact with the RBD when it is in the up conformation, since the down conformation is inaccessible to ACE2 [60]. Moreover, SARS-CoV-2 has been shown to use the TMPRSS2 serine protease to prime the S protein. A TMPRSS2 inhibitor has been shown to block entry; it has been approved for clinical use and might constitute a treatment option [39,74].
There is no evidence that S protein immunogenicity or its link with the ACE2 receptor is affected by either the absence or the presence of other structural proteins. This condition is a critical initial stage for viruses to access the host cell [75]. Differences in the S protein affect recognition by the ACE2 receptor and other proteins or ligands. For example, it was found that a panel of monoclonal antibodies and murine polyclonal antisera against SARS-S1/RBD are unable to bind to the SARS-CoV-2 S protein [2]. This finding suggests that researchers must investigate the previously developed SARS-RBD-based vaccine candidates for any clinical benefit for SARS-CoV-2 prophylaxis.
The position of RBDs in their respective down conformations is one of the significant differences between SARS-CoV and SARS-CoV-2S1 structures (although a relatively small difference). The SARS-CoV RBD is closer to the NTD of the neighboring protomer in the down conformation than in the up, whereas the SARS-CoV-2 RBD is placed at a sharp angle into the down conformation towards the central cavity of the trimer. However, when the individual structural domains of SARS-CoV-2 are aligned with their counterparts from the SARS-CoV S, they reflect the high degree of structural homology between the two proteins [15].
7. Differences in Furin-Like Protease Recognition Pattern
Seven pro-protein convertases (PCs) cleave precursor proteins at specific single or paired basic amino acids within the motif (R/K)-(2X)n-(R/K)↓(canonically, R-X-(R/K)-R), in which n = 0, 1, 2 or 3 spacer amino acids [1,76]. PCs, in particular furin [77,78,79], have been involved in viral infections due to their role in the processing of many critical surface-cell proteins.
Furin is used by a number of pathogens in other roles. For example, the envelope proteins of viruses such as human immunodeficiency virus (HIV), influenza, dengue fever, several filoviruses, including ebola and marburg viruses, and possibly the spike protein of SARS-CoV-2 [1,77,78,79], must be cleaved by furin or furin-like proteases to become fully functional. Inhibitors of furin are under consideration as therapeutic agents to treat anthrax infection [80]. ProP [81] and PiTou [82] are two bioinformatics methods that can be used to predict furin substrates and locations of furin cleavage sites in protein sequences. The S1/S2 processing sites exhibit different motifs among coronaviruses; many of them display cleavage sites after a basic residue. It is, thus, likely that the priming process is ensured by different host-cell proteases, the choice of which depends on the sequence of the S1/S2 cleavage site. Accordingly, the MERS-CoV S protein that contains the RSVR↓SV motif can be cleaved by furin during viral egress [83,84]. The SARS-CoV-2 S protein contains a putative furin recognition motif (PRRARSV) (Figure 8 and Figure 9) that is similar to that of MERS-CoV.
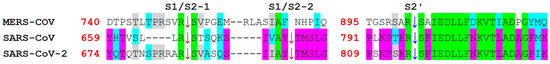
Figure 8.
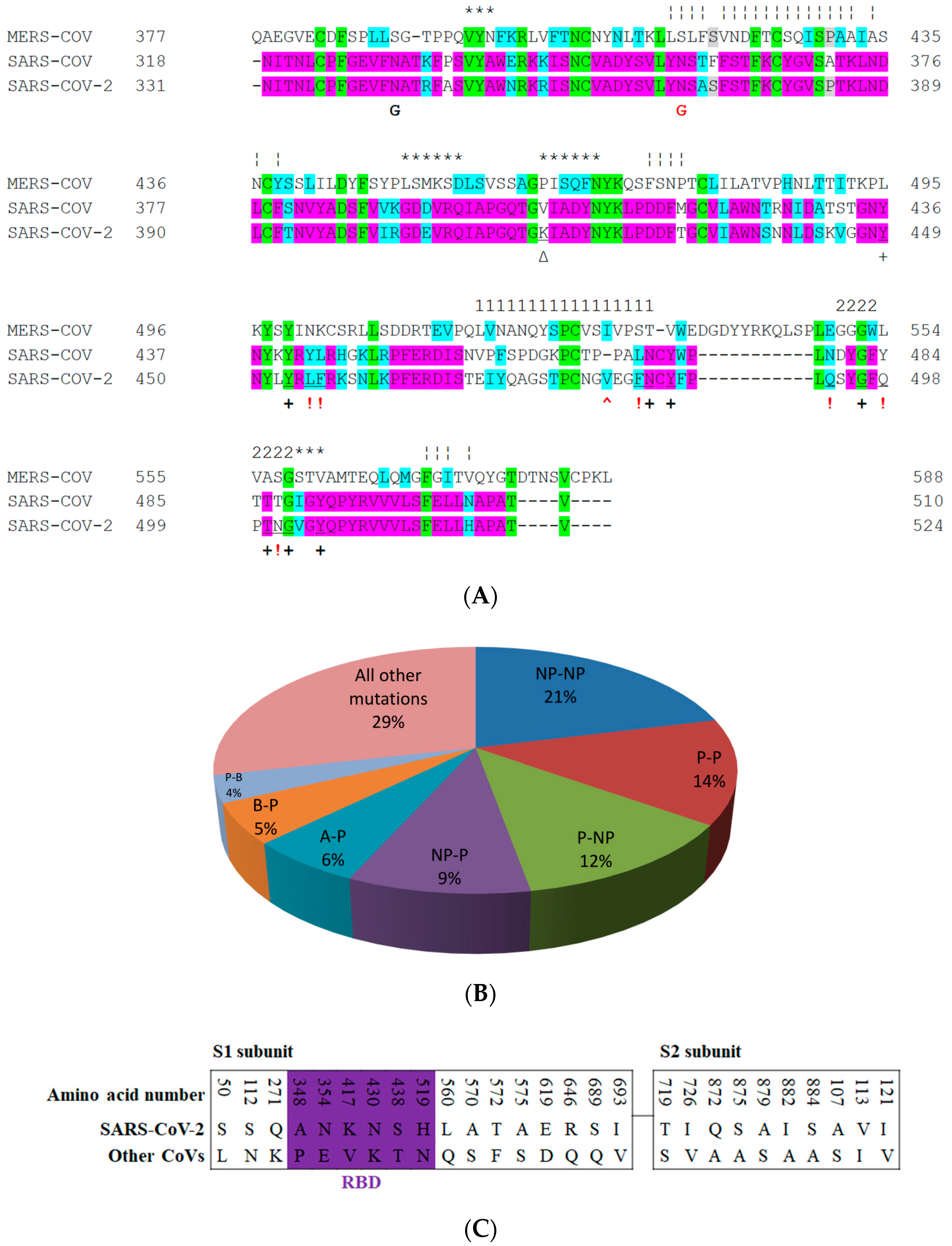
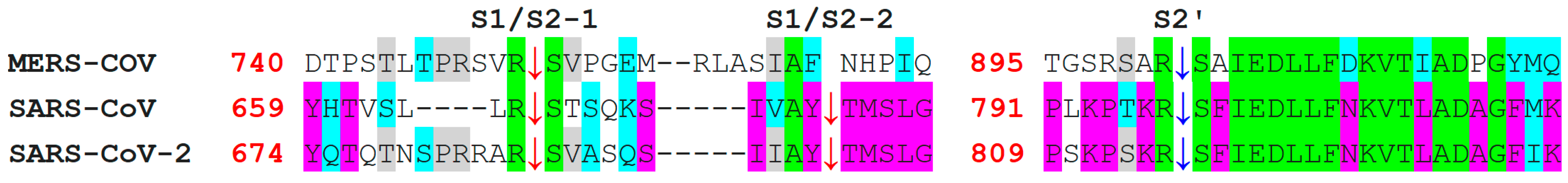
Aligned sequences (performed by use of Clustalw) of furin-like cleavage sites for SARS-CoV-2 that are aligned with those of SARS-CoV and MERS-CoV. Green color indicates positions that have a single, fully conserved residue between the three sequences. Pink indicates amino acids that are conserved between SARS-CoV-2 and SARS-CoV, while grey color indicates those that are conserved between SARS-CoV-2 and MERS-CoV. Cyan indicates conservation between groups that exhibit strongly similar properties and score > 0.5 in the Gonnet PAM 250 matrix [85]. The red arrowheads indicate S1/S2 possible cleavage sites, while the blue arrow shows a S2′ cleavage site. The first S1/S2 site is very similar between SARS-CoV-2 and MERS-CoV, while the second S1/S2 is found only in SARS-CoV and SARS-CoV-2. The S2′ cleavage site in SARS-CoV-2 is similar to that of SARS-CoV.
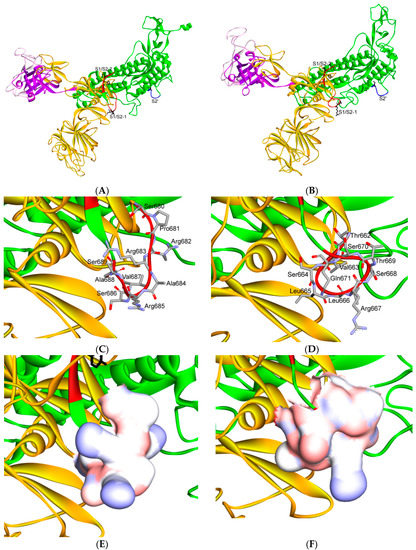
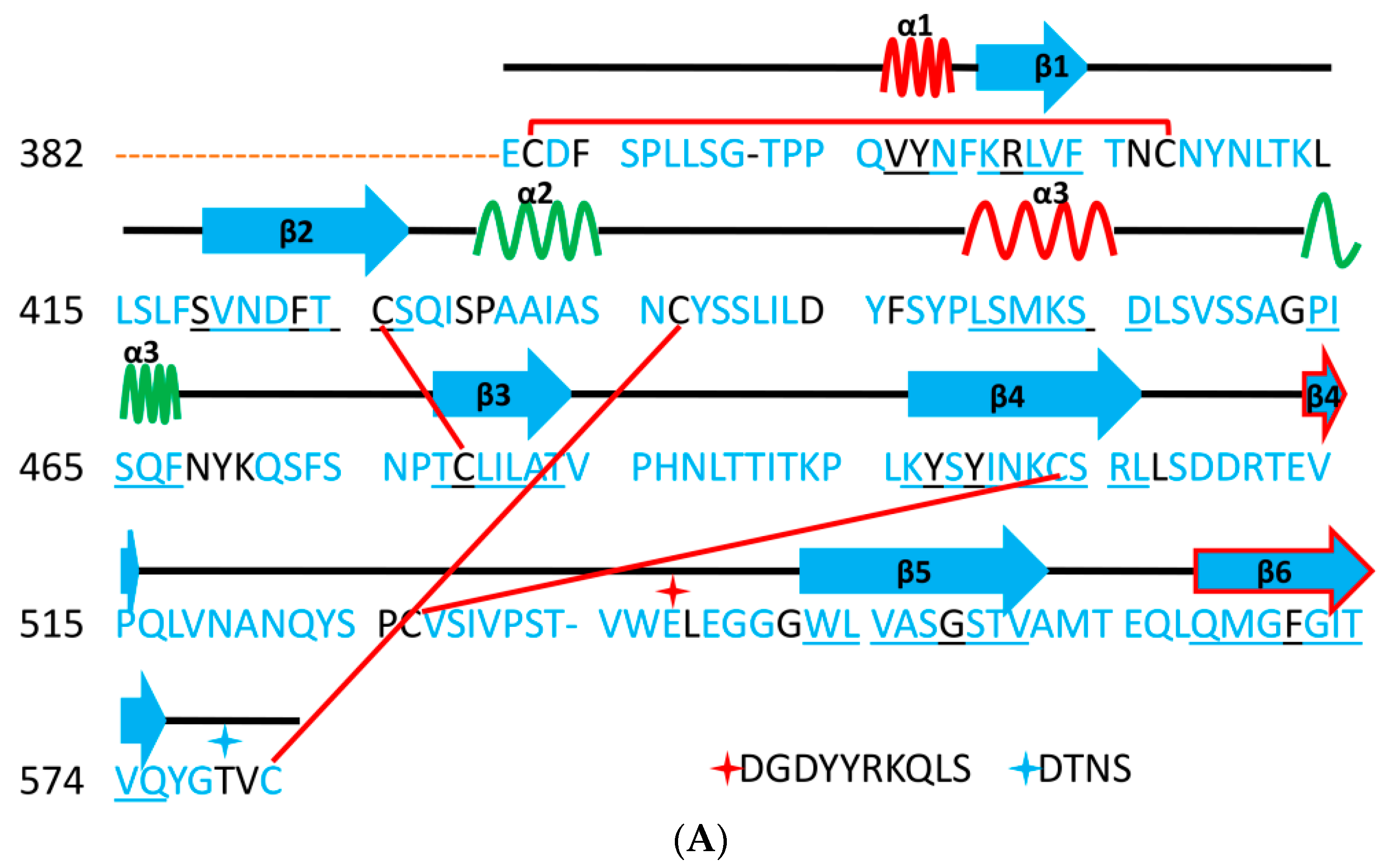
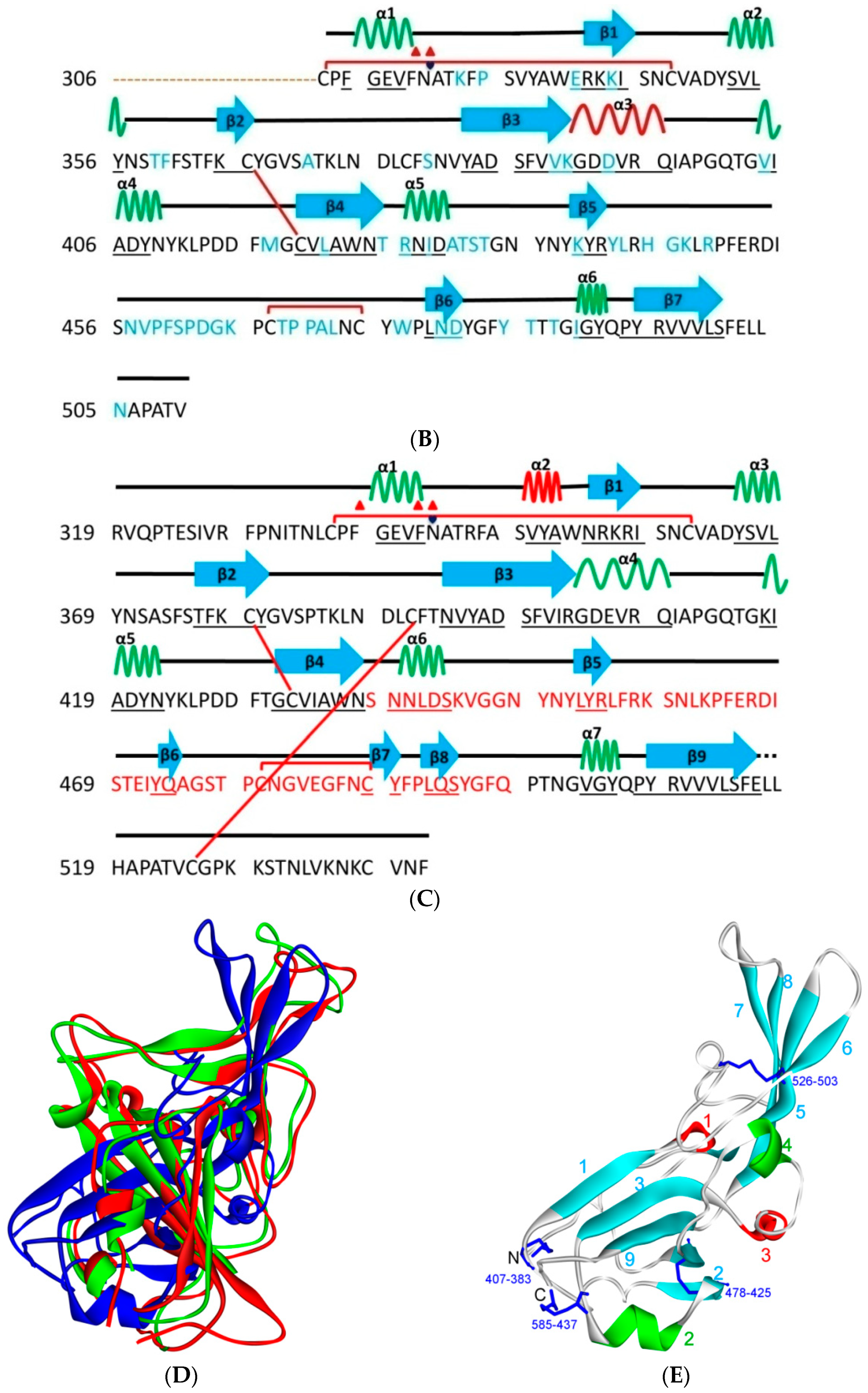
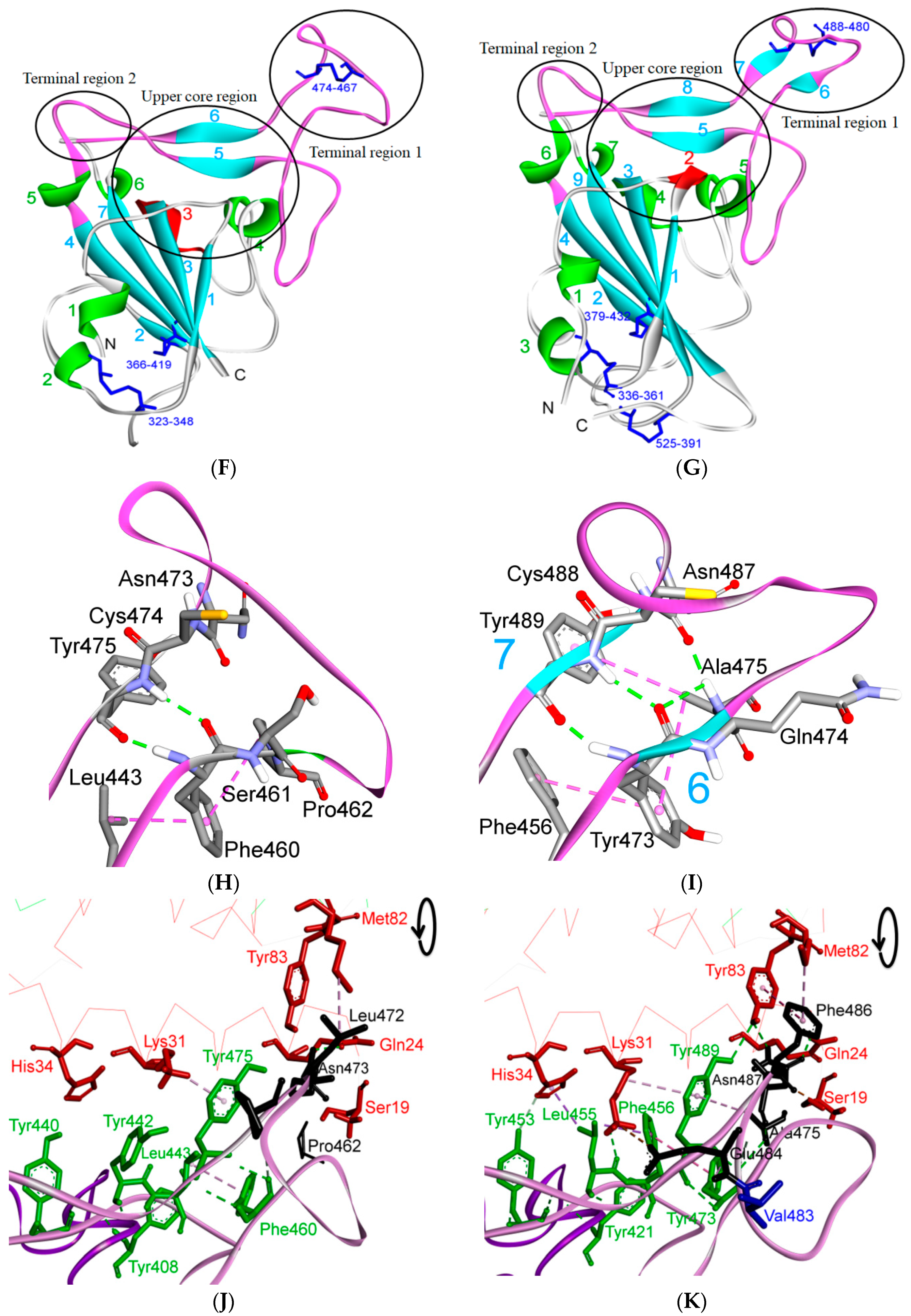
Figure 9.
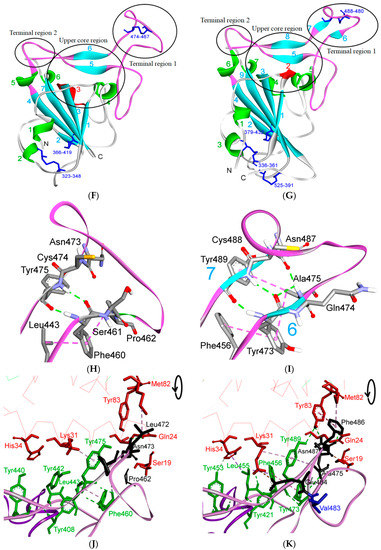
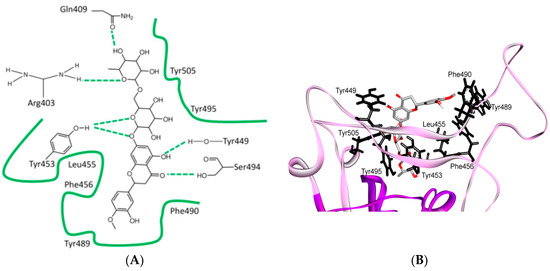
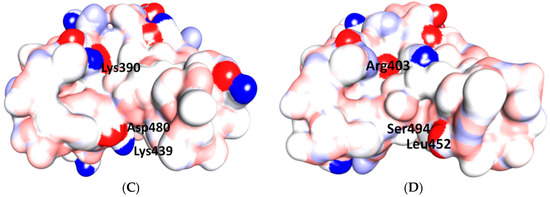
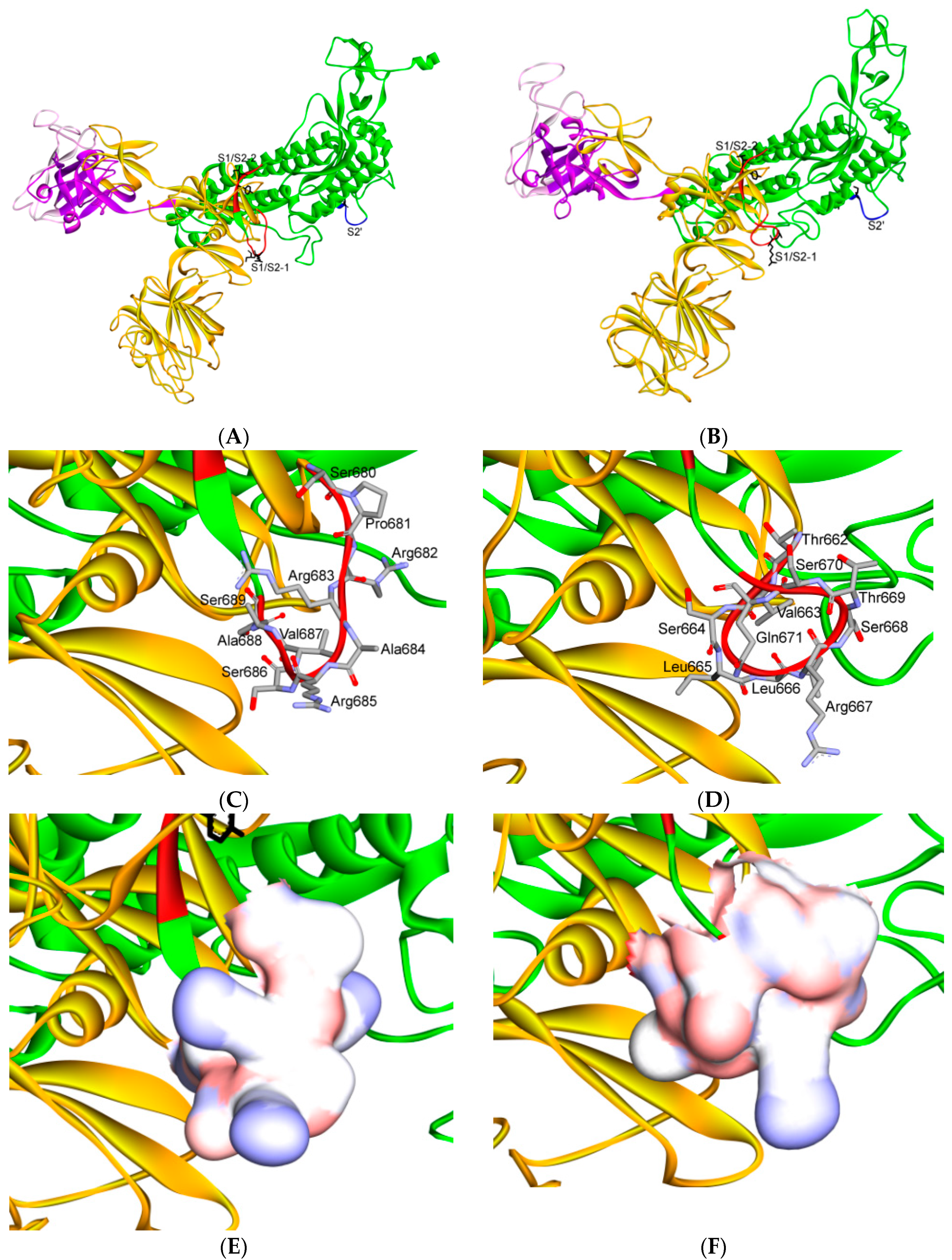
Three-dimensional structure of different furin-like cleavage sites for SARS-CoV and SARS-CoV-2. (A,B) show 3D models of the S protein of SARS-CoV and SARS-CoV-2, respectively. These have been predicted by homology modeling that used Swiss-model software, based on the S protein sequence obtained from Genbank (accession numbers: MT192773 and AY278741 for SARS-CoV and SARS-CoV-2, respectively). The models were predicted through use of PDB IDs 6ACD and 6VYB for SARS-CoV and SARS-CoV-2, respectively. The S2 unit, RBD, RBM, S1/S2 and S2′ potential cleavage sites are shown in green, violet, pink, red and blue, respectively. The S1/S2-1 is more exposed to solvent than the S1/S2-2 site, so it is more easily accessed and cleaved by furin in SARS-CoV-2. Therefore, it is a more potential effective priming site. (C,D) show the detailed amino acid compositions of the S1/S2-1 cleavage sites of SARS-CoV and SARS-CoV-2, respectively. (E,F) show the surface of the S1/S2-1 cleavage sites of SARS-CoV and SARS-CoV-2, respectively. There are more basic groups in the S1/S2-1 cleavage site of SARS-CoV-2 (shown in light blue color) than in that of SARS-CoV. 3D models were created using Discovery Studio (version 2.5.5, Biovia, San Diego, CA, USA).
It has been shown that the spike protein is cleaved at the S1/S2 cleavage site to generate the subunits S1 and S2. Many viruses display the canonical (R/K)-(2X)n-(R/K)↓ motif (Figure 8). Further, the variation around the viral envelope glycoprotein cleavage site has been shown to play a role in cellular tropism and pathogenesis [76,77,78,79]. Conversely, the S protein of SARS-CoV remains largely uncleaved after biosynthesis, possibly due to the lack of a favorable furin-like cleavage site (SLLRST). In this case, it has been reported that, after receptor binding, the virus coerces the proteases of target cells such as elastase, cathepsin L or TMPRSS2 to cleave the S protein at a conserved sequence AYT↓M (located 10 amino acids downstream of SLLRST). As the priming event is essential for virus entry, the efficacy and extent of this activation step by the proteases of the target cells should regulate cellular tropism and viral pathogenesis. In the case of the SARS-CoV-2 S protein, the conserved site 2 (S1/S2-2) sequence AYT↓M may still be cleaved, possibly after the preferred furin cleavage at the site 1 [27]. The 3D model of the three cleavage sites of SARS-CoV and SARS-CoV-2 are shown in Figure 9.
Strikingly, the SARS-CoV-2 S protein sequence contains 12 additional nucleotides upstream of the single Arg↓ cleavage site 1 (S1/S2-1) compared with the same site on the SARS-CoV S protein. This addition forms a predicted solvent-exposed PRRAR↓SV sequence, which corresponds with a canonical furin-like cleavage site (Figure 8 and Figure 9) [27,86,87,88]. This furin-like cleavage site should be cleaved during virus egress [83] in order to promote S protein “priming” and it may provide a gain-of-function to the SARS-CoV-2 virus for efficient spread in the human population, compared with other lineage b beta coronaviruses. If this site is not processed, it is expected that the S protein is cleaved at site 2 during virus endocytosis, as has been observed for the SARS-CoV virus. The furin-like S2′ cleavage site at KR↓SF, which contains P1 and P2 basic residues and a “P4” hydrophobic Phe [83], is identical between SARS-CoV and SARS-CoV-2.
In the MERS-CoV S protein, the sequence is replaced by RXXR↓SA at the S2′ site, where P1 and P4 are basic residues and an alanine is found at P6. This sequence suggests a less favorable cleavage by furin. However, processing at S1/S2-1 in SARS-CoV-2 is expected to be a key part of the final activation of the S protein. These observations suggest that inhibitors of furin-like enzymes may contribute to the inhibition of virus propagation [27].
A comparable type of modification (insertion) alters the H5N1 influenza virus and other avian viruses into more pathogenic variants. The origin of the high pathogenicity of avian influenza H5N1 due to the RRRKK insertion at the cleavage loop of the haemagglutin in H5 has been studied and compared with those of the non-inserted H5 and H3 that are bound to the furin active site. The highly pathogenic H5 cleavage loop has been found to be strongly bound to the furin cavity as a proteolytic conformation. Experimentally, the RRRKK insertion also increases the amount of haemagglutinin cleavage by furin [89].
Moreover, the RRXR sequence has been shown by many studies to be a putative furin cleavage site. TGF-β has been shown to be cleaved from its pro-peptide by furin-like endo-proteinases at the RRXR sequence during secretion [90]. Additionally, in the ADAM metallo-peptidase domain 17 (ADAM17), also called TACE, the pro-domain is cleaved from the catalytic domain at the RRXR site [91]. MT1-MMP is synthesized as a latent zymogen. The zymogen requires proteolytic cleavage of the N-terminal prodomain peptide sequence [92,93]. The main activation mechanism of MT1-MMP has been suggested for cleavage at one or both RRXR-furin sites [94].
Dahms et al. have searched for inhibitory peptides that have similar sequences to that of the S1/S1-1 cleavage site [76]. They have reported the inhibition activity of three different peptides, namely: I1: H-Arg-Arg-Arg-Val-Arg-4-aminomethyl-benzamidine (R-R-R-V-R-X1); I2: phenylacetyl-citrulline-Arg-Val-Arg-4-aminomethyl-benzamidine (X2-R-V-R-X1); and I3: 4-aminomethyl-phenylacetyl-Arg-Tle-Arg-4-aminomethyl-benzamidine (X3-R-tL-R-X1). Their inhibition constants were reported to be 33.7 pM, 238 nM and 22.4 pM, respectively; I1 and I3 were the most active [76].
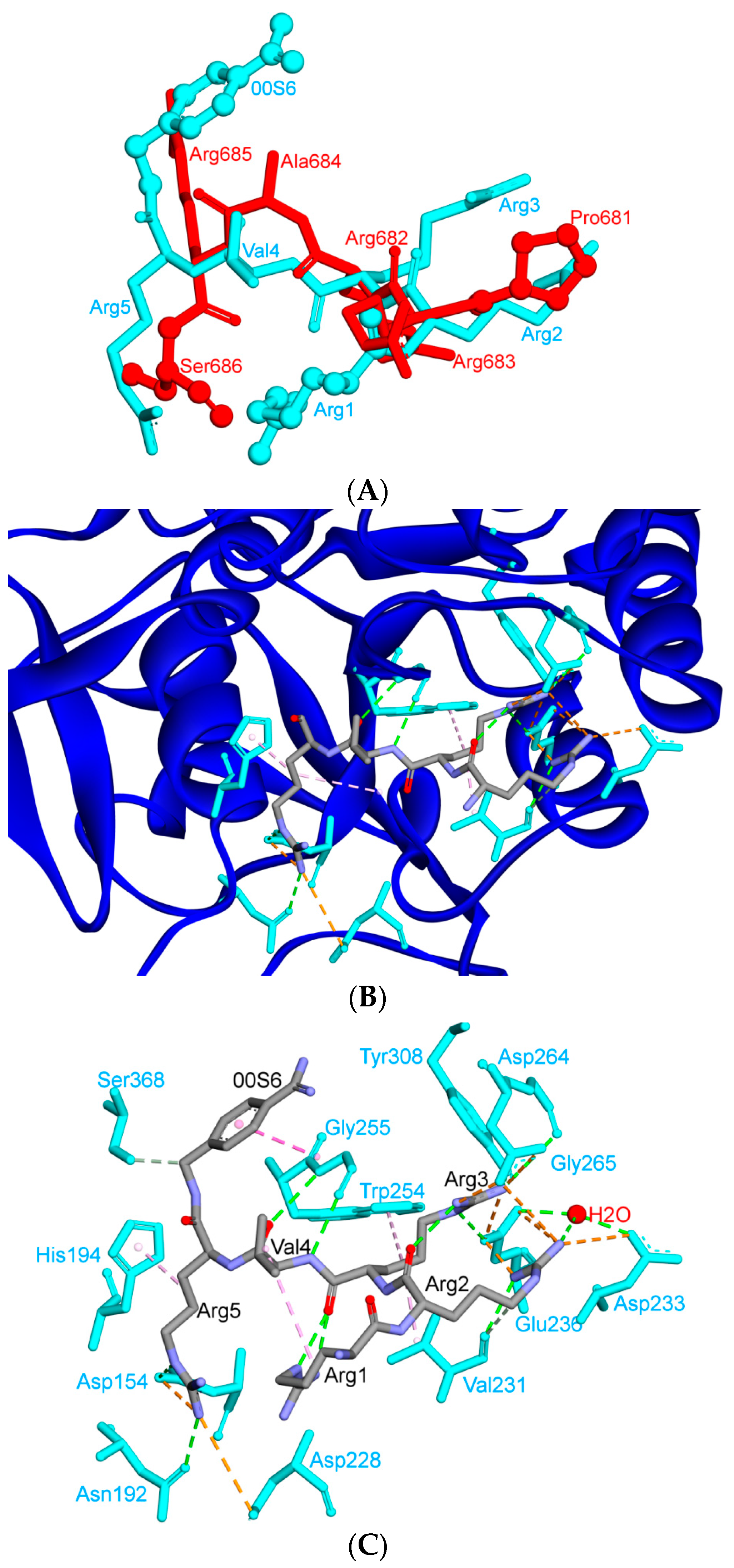
Inhibitory peptide I1 has a core sequence (RRXR) that is closely related to that of the S1/S2-1 cleavage site of SARS-CoV-2 (R-R-A-R), with the X position filled by a hydrophobic, small amino acid. Interactions of I1 that have been observed at the Arg3 position involve typical hydrogen bonds with Tyr308 and charge-assisted hydrogen bonds with Asp264 and Glu236. The guanidino group of the Arg2 residue also mediates electrostatic interactions with Glu236. Additional Arg2 interactions include hydrogen bonds to the carbonyloxygen of Val231 and to a specific water molecule that is tightly bound by the side chains of Asp233 and Glu236 and by the amide nitrogen of Ala267 [76].
An intra-molecular hydrogen bond has been observed between the Arg2 carbonyloxygen and the Arg3 guanidino group. As a result of the extensive interaction network, the backbone conformation of this peptide bond is largely restricted. This backbone conformation of the inhibitor is also stabilized by water-bridged interactions between the Arg2 carbonyloxygen and the amide nitrogen of Glu257 as well as between the Arg2 amide nitrogen and the amide nitrogen of Val231 (Figure 10) [76].
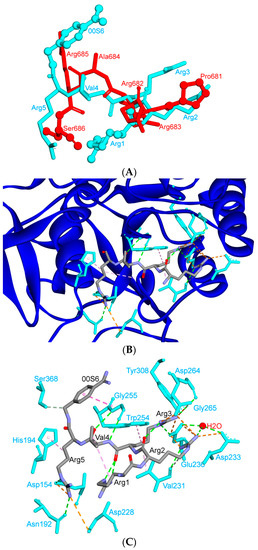
Figure 10.
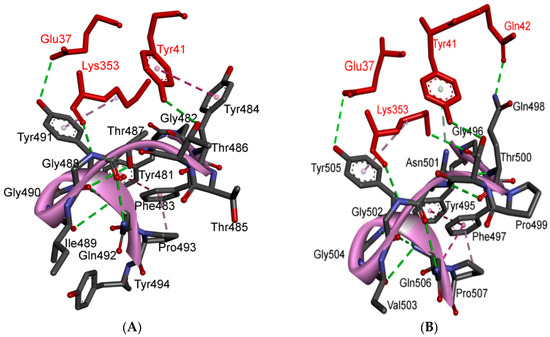
S1/S2-1 furin cleavage site and its similarity to the I1 inhibitory peptide. (A) The alignment of the SARS-CoV-2 S1/S2-1 site in SARS-CoV-2 with the I1 peptide. (B) The binding mode of the furin active site with the I1 inhibitory peptide. (C) The interactions of the I1 inhibitory peptide with the amino acids of the furin active site; same interactions are expected with the S1/S2-1 cleavage site. Three-dimensional models were created using Discovery Studio (version 2.5.5, Biovia, San Diego, CA, USA).
The RRXR sequence (POS-POS-X-POS) in general has an S score of 0.84 [55], which means it is disordered, but in the structure of S1/S2-1, the backbone might be affected by the presence of proline (Pro681) upstream of the cleavage site, which is likely to increase the amount of order in the site.
The bulky Arg1 residue of I1 (which corresponds to Pro681 in the S1/S2-1 site) replaces water molecules from the active site cleft of furin (which are believed to be replaced by flanking amino acids in the S1/S2-1 cleavage site of SARS-CoV-2). Several ordered solvent molecules have been observed to bind in close proximity to Arg1 in structures that involve inhibitors that lackan Arg1 residue. Some of these water molecules show conserved binding sites. The liberation of bound solvent molecules by the inhibitor at Arg1 is, hence, expected to increase the entropy of binding and therefore productively contribute to the binding energy.
More interestingly, the PRRXR sequence (which is equivalent to the S1/S2-1 cleavage site of SARS-CoV-2) has been reported to be apat7 nuclear localization signal (NLS). The pat7 NLS starts with proline and is followed within three residues by a segment that contains three basic residues out of four. The presence of this NLS has been confirmed by use of the computer program PSORT [95]. Even though replication of many viruses is restricted to the cytoplasm, the N proteins of several viruses have been reported to localize to the nucleolus during infection by NLSs [96,97,98,99]. Viral proteins have the capacity to modulate the nucleolar function, and this modulation can be a viral strategy that diverts biosynthetic resources from the dividing nucleus to the cytoplasm, the site of virus replication [44,85,99,100,101]. The ability of S protein in the cytoplasm to perform such a function requires verification [102].
8. Effect of the S Protein and ACE2 Differences on the Binding Contacts, Affinity and Virulence
It has been shown that in SARS-CoV-2, the presence of glutamine, asparagine, leucine, phenylalanine and serine amino acids enhances ACE2 binding [103]. Several studies have proposed that the increased virulence of SARS-CoV-2 compared with that of other coronaviruses is due to its higher binding affinity to the ACE2 receptor [1,45,85,104]. Yan et al. have proposed that the mutation of Val404 to Lys417 may result in a higher binding affinity, due to the salt bridge between K417 and D30, whereas the mutation of Arg426 to Asn439 would weaken the interaction with Glu329 [45]. However, it was shown by simulations that the Val404 to Lys417 mutation increased the binding affinities, due to favorable electrostatic interactions that were greater than the energy losses that were induced by the Arg426 to Asn439 mutation.
Additionally, it was proposed that the mutation of Leu472 to Phe486 would weaken the Van der Waals (vdw) contact with Met82 of ACE2 [45]. It was found that two main residues (Asn479 and Asn487) were associated with hACE2 [105], and enabled virus progression and tropism [11]. In addition, a single mutation in Asn501 position has been found to enhance the binding capacity of the SARS-CoV-2 RBD with the human ACE2 and this evolution in infected patients should be monitored [38,44,105].
Nearly 20-fold increased binding energy between ACE2 and the SARS-CoV-2 spike trimer has been reported (KD of 14.7 nM), compared with that between ACE2 and the SD1 site of the SARS-CoV RBD (KD of 325 nM). This is perhaps due to experimental issues, such as the different proteins that were used in the assay. Nevertheless, the binding affinity alone is unlikely to explain the unusual transmissibility of SARS-CoV-2. Other factors such as the unique RRAR furin cleavage site at the S1/S2 boundary of the SARS-CoV-2 spike may play more important roles in the facilitation of rapid human-to-human transmission [6,39,44,82,85].
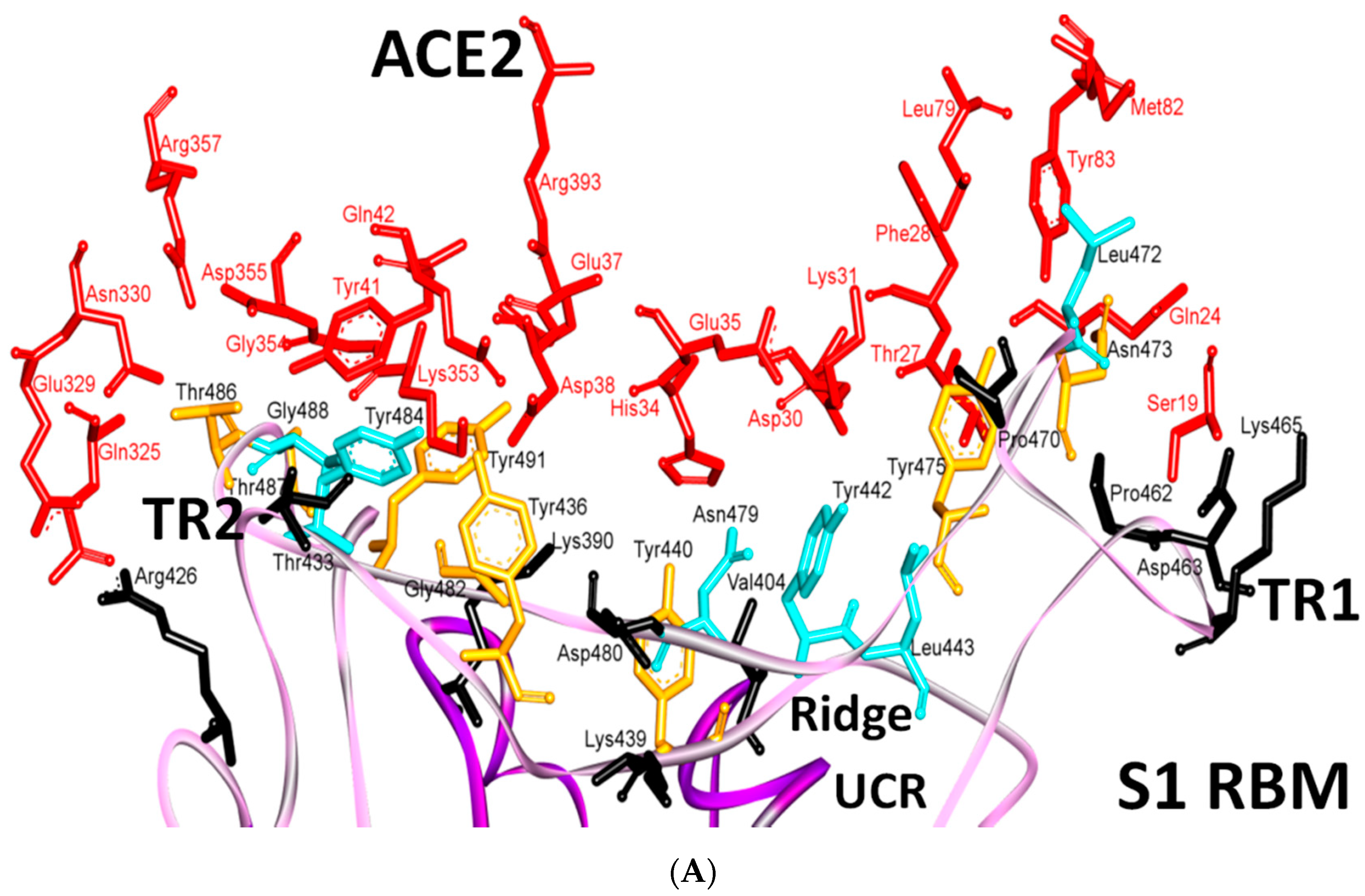
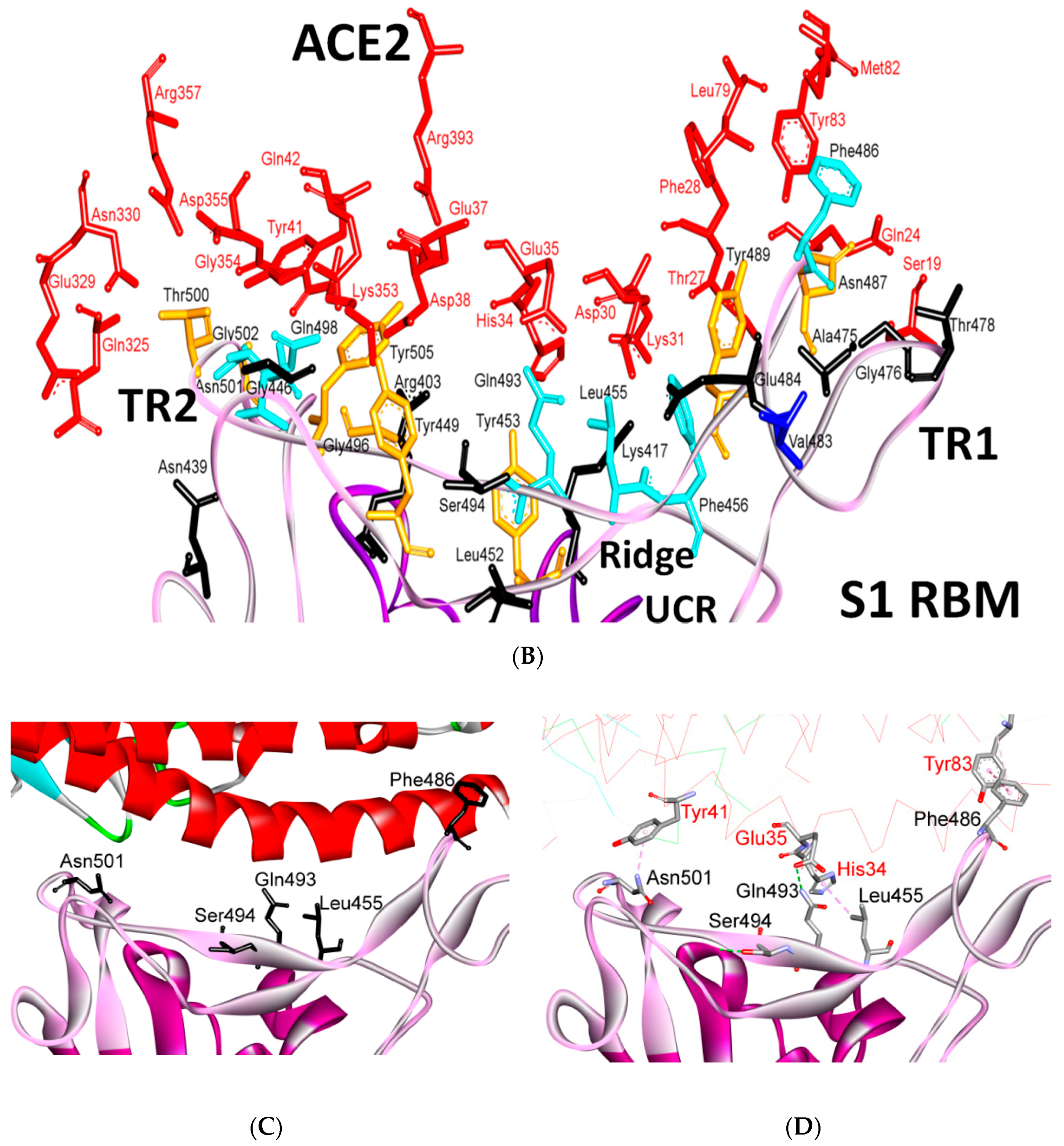
Several naturally selected RBM mutations occur near the virus-binding hot regions, and these residues largely determine the host range of SARS-CoV and binding affinity. Furthermore, specific amino acids have been determined at the 442,472, 479, 480 and 487 positions of SARS-CoV (which correspond to the 455, 486, 493, 494 and 501 positions in SARS-CoV-2) that enhance viral binding to hACE2. Importantly, when all these five hACE2-favoring residues have been combined into one RBD, this RBD binds to hACE2 with super affinity and the corresponding spike protein mediates viral entry into human cells with very high efficiency [1]. Table 2 shows the changes at these five critical positions for SARS-CoV and SARS-CoV-2. Studies have highlighted positions 3 and 5 (namely Q493 and N501 in SARS-CoV-2) as the most critical residues in the binding process. Figure S2 shows the contacting ACE2 residues with RBM region, the interacting residues in the RBM region of SARS-CoV and SARS-CoV-2 are shown in Figure 11A,B, respectively. Figure 11C shows the residues that are reported in Table 2 in black (the RBD is shown in violet while the RBM is shown in pink). The contacts between these residues in SARS-CoV-2 and the corresponding ACE2 that have been observed in X-ray [2] structure are shown in Figure 11D, which shows stacking between Asn501 of the RMB and Tyr41 of ACE2, hydrogen bonding between Gln493 of the RBM with Glu35 of ACE2, stacking between Leu455 of the RBM and His34 of ACE2, and stacking between Phe486 of the RBM with Tyr83 of ACE2.

Table 2.
The variants of RBM at five critical positions in SARS-CoV (442, 472, 479, 480 and 487).
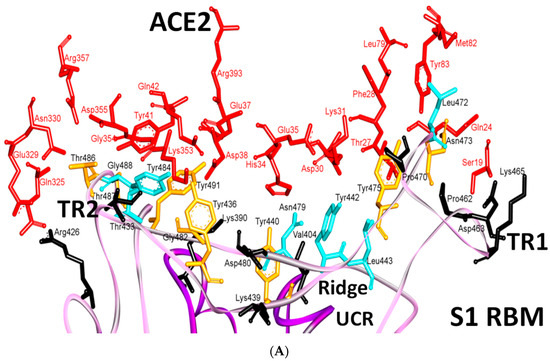
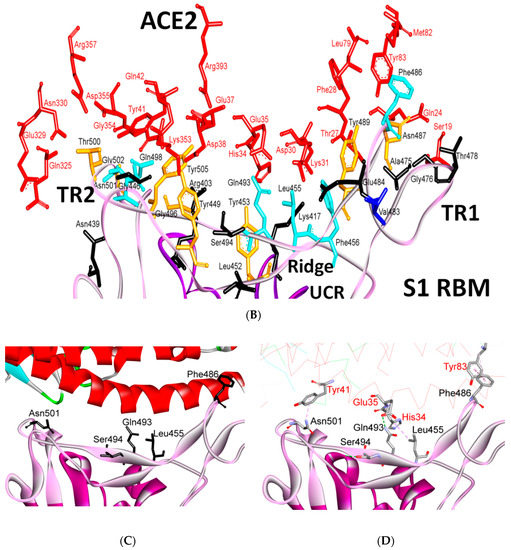
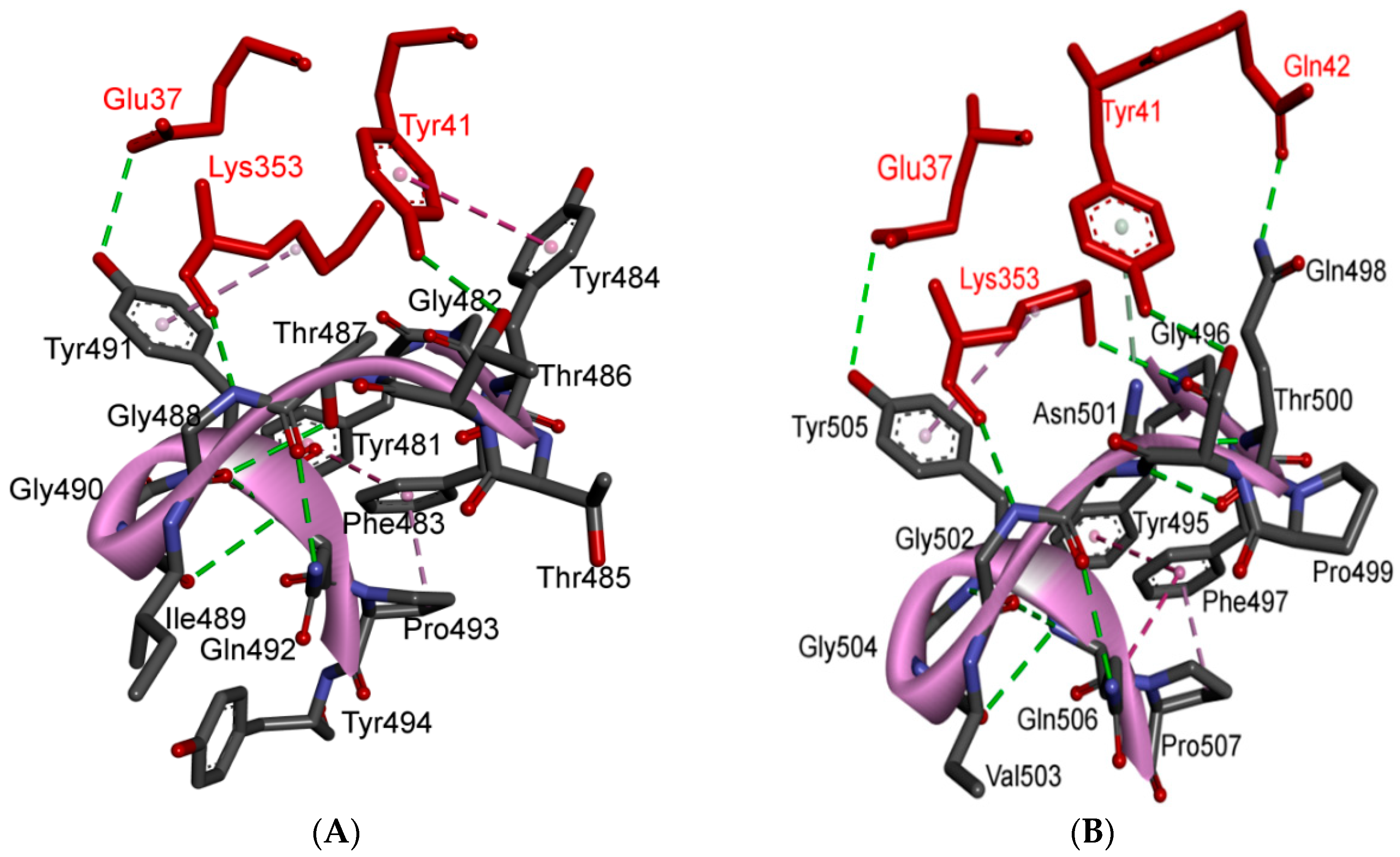
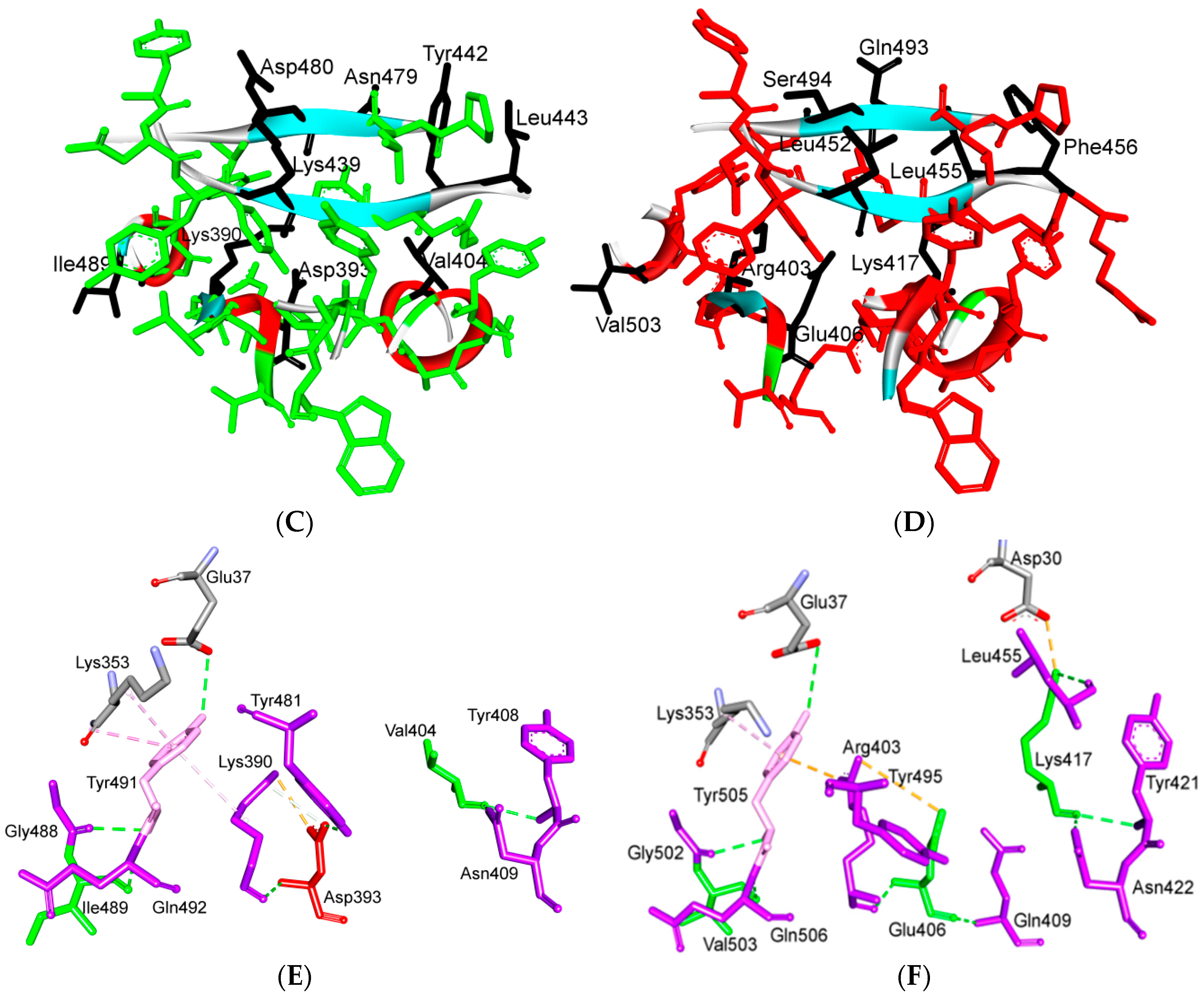
Figure 11.
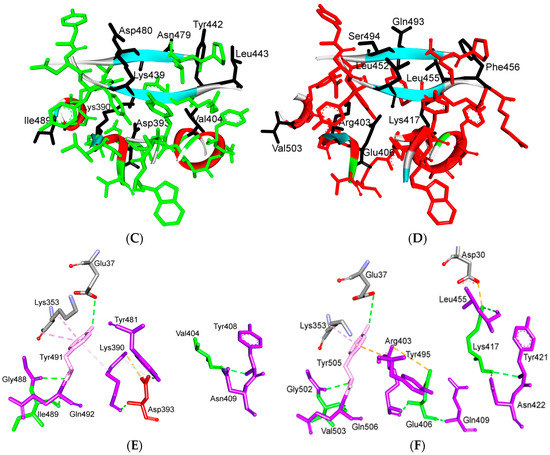
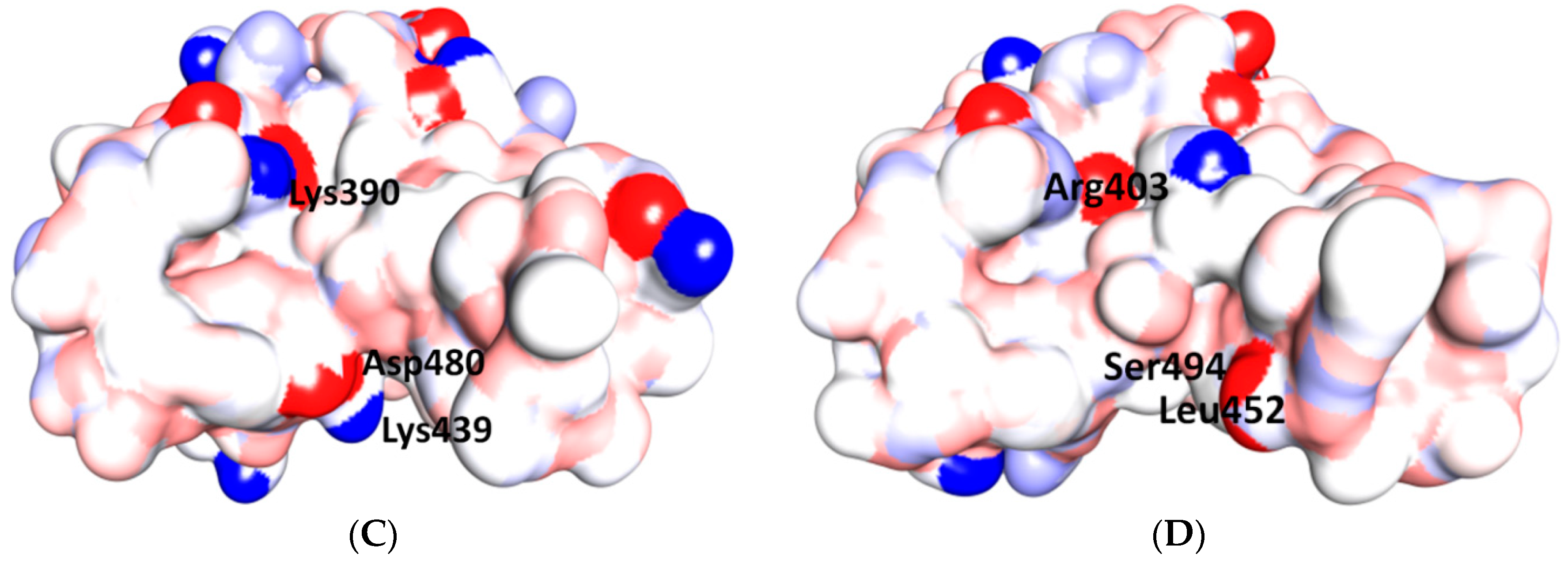
Binding interface and interactions between RBM of SARS-CoV and SARS-CoV-2 with ACE2. (A,B) interacting residues between the RBM and ACE2 for SARS-CoV and SARS-CoV-2, respectively. Red, orange, cyan and black colors indicate the interacting amino acids from ACE2, identical residues between SARS-CoV and SARS-CoV-2, different residues with partially conserved contacts, and different residues with different contacts, respectively. Ridge: region between TR1 and TR2. UCR: Upper core region. A Leu to Phe486 mutation (in addition to Pro to Ala475, Pro to Glu484, Lys to Thr478, Asp to Gly476 mutations and a Val483 insertion) in TR1 increases its hydrophobicity and the order of its structure, while mutations in the ridge region of Val to Lys417 (which makes electrostatic interactions), Asn to Gln493 (more hydrogen bonding), Asp to Ser494 and Lys to Leu452 (which increase the hydrophobicity of the shallow pit) give SARS-CoV-2 an advantage to bind mainly through these regions. Arg426, Thr433 and Tyr484 in SARS-CoV (instead of Asn439, Gly446 and Gln498 in SARS-CoV-2) produce more electrostatic, hydrogen bonding and stacking interactions, respectively, which give SARS-CoVan advantage to bind mainly through TR2. The use of different regions for binding may explain the differences in affinity and pathogenesis between SARS-CoV and SARS-CoV-2. (C) shows the five critical binding residues that are shown in Table 2. (D) shows the interacting residues from ACE2 with these critical residues. Three-dimensional models were created using Discovery Studio (version 2.5.5, Biovia, San Diego, CA, USA).
It has been determined that at position 1, phenylalanine shows more affinity to ACE2 than tyrosine does in the human, while tyrosine shows more affinity to ACE2 than phenylalanine does at the same position in the civet. For position 2 in the human, phenylalanine has more affinity to ACE2 than leucine, which, in turn, has more affinity than proline. In contrast, in the civet, proline and leucine have the same affinity to ACE2, which is greater than that of phenylalanine. Position 3 shows similar affinity in the human to ACE2 when it contains either asparagine or arginine, and either of these shows much more affinity than lysine. For civet at the same position, arginine has more affinity than either lysine or asparagine. At position 4, aspartate has more affinity than glycine in the human and vice versa in civet. Finally, at position 5, threonine has much more affinity for ACE2 than serine in the human, with a lesser difference in civet [1].
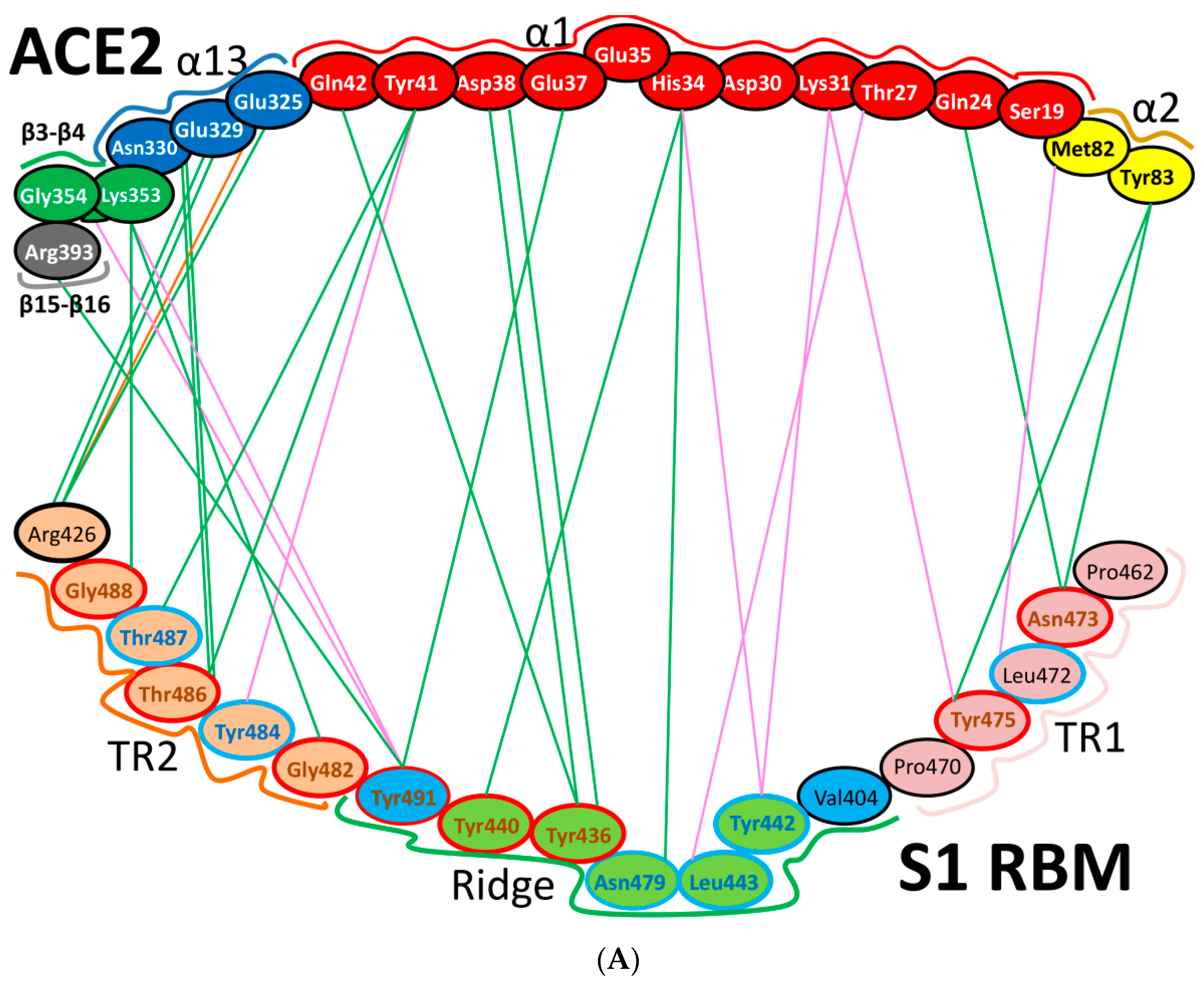
Further detailed comparison of the receptor-binding interface between the two coronaviruses reveals that, among the 24 residues in ACE2 that make vdw contacts with either RBD, 15 amino acids display more contacts with the SARS-CoV-2 RBD than with the SARS-CoV RBD. The SARS-CoV-2 RBD binding interface also has more residues than the SARS-CoV RBD (21 vs. 17) that directly interact with ACE2. These interacting residues form more vdw contacts (288 vs. 213) as well as more hydrogen bonds (16 vs. 11). Specifically, F486 in the RBD of SARS-CoV-2, in contrast to I472 in the SARS-CoV RBD, forms strong aromatic-aromatic interactions with hACE2 Y83 (Figure 11 and Figure 12). Similarly, E484 in the SARS-CoV-2 RBD, instead of P470 in the SARS-CoV RBD, forms ionic interactions with K31 [14] (Figure 11 and Figure 12 and Table 3). Interestingly, it has been observed that a single K353A mutation in ACE2 insufficient to abolish these interactions in SARS-CoV-2 [2].
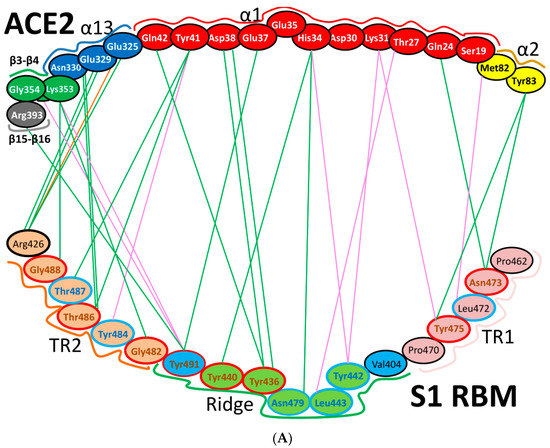
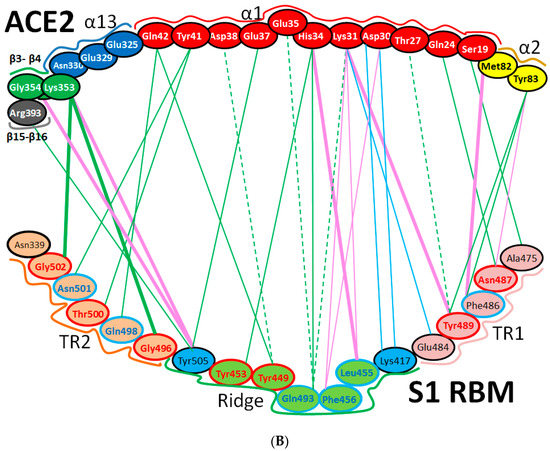
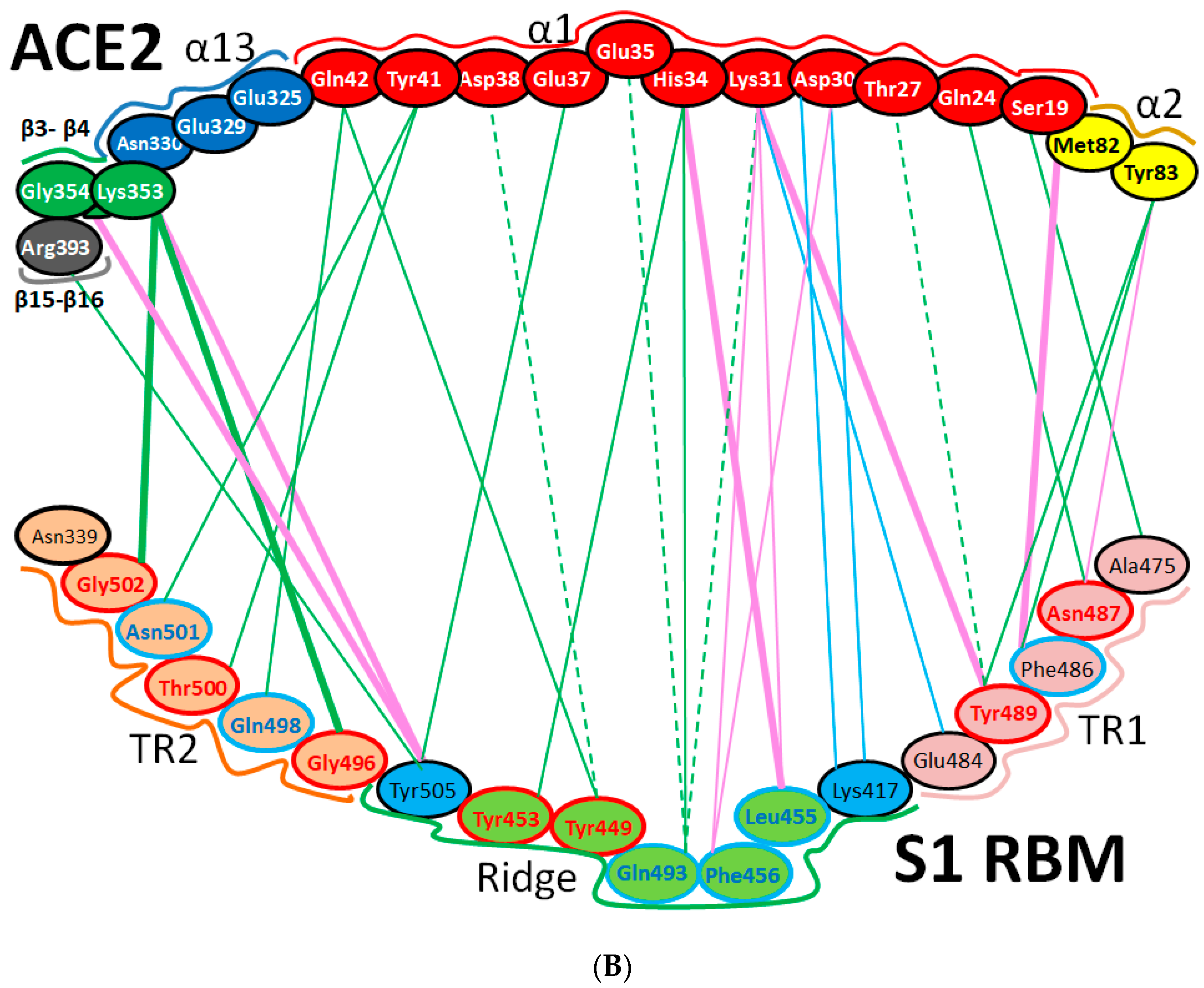
Figure 12.
Cartoon representation of the interactions between ACE2 and the RBM of SARS-CoV and SARS-CoV-2. (A) SARS-CoV (based on PDB: 2AJF) and (B) SARS-CoV-2 (based on PDBs: 6LZG and 6M17). Hydrogen bonding interactions, hydrophobic interactions, and electrostatic interactions are shown by green, pink and orange lines, respectively. In the RBM regions, residues with red outlines are identical, while residues with cyan outlines are different amino acids with partially conserved contacts. The black outlines show different amino acids with different contacts. For interactions that are shown for SARS-CoV-2, the solid lines are attributed to interactions monitored in PDB:2AJF, while the dashed lines are attributed to those in PDB:6M17. Thick lines represent the common interactions between the two SARS-CoV-2 PDBs. “α” and “β” refer to alpha helix and beta sheet, respectively.

Table 3.
Interactions between amino acids in the RBDs of SARS-CoV-2 and SARS-CoV with ACE2.
The major electrostatic contributions are observed for the (RBMR426)/(ACE2 E329) salt bridge with SARS-CoV and (RBMK404)/(ACE2 D30) with SARS-CoV-2, as shown in (Table 3, Figure 11 and Figure 12) [104]. However, the latter exhibits a higher electrostatic interaction by 1.4 Kcal/mol. The contribution in the free-energy formation of the salt-bridges (∆G) is dominated by the pairwise acid/base interactions [104]. The total electrostatic interaction between SARS-CoV-2 and ACE2 is 3 Kcal/mol higher than that between SARS-CoV and ACE2. The contribution of a single mutation to the electrostatic binding energies is small. However, these mutations induce structural changes that increase the favorable vdw interactions in SARS-CoV-2. The total vdw contribution to the binding energy is 4 Kcal/mol, which illustrates the overall structural changes in the S protein in SARS-CoV-2. It has been found that the total binding energy in the case of SARS-CoV-2 is stronger than that in SARS-CoV, as the electrostatic and vdw interactions are greater in SARS-CoV-2 by 3 Kcal/mol and 1 Kcal/mol, respectively, than in the case of SARS-CoV [104].
In summary, SARS-CoV-2 seems to involve in more interactions with ACE2 than SARS-CoV (Figure 11 and Figure 12). There are significant differences in the TR1, middle ridge region and TR2 of the RBM in SARS-CoV-2, compared with the same RBMs parts of MERS-CoV and SARS-CoV. Thanks to these differences, SARS-CoV-2 has acquired the advantage of binding mainly through the RBM by using hydrophobic, hydrogen-bonded and electrostatic interactions in TR1 and the middle ridge. This differs from SARS-CoV, which interacts through more electrostatic links in TR2 of the RBM, together with hydrogen bonds and stacking interactions. Different types and numbers of interactions and different regions of binding between SARS-CoV-2 and SARS-CoV may explain many of their different tendencies for infection. SARS-CoV-2 and SARS-CoV both bind through TR1, middle ridge and TR2. However, SARS-COV-2 manifests more interactions (i.e., hydrophobic, hydrogen-bonded and electrostatic interactions) in TR1 and middle ridge, while SARS-CoV shows more preference for TR2 (i.e., it has more electrostatic interactions in this region than SARS-CoV-2). Furthermore, it seems that proline plays an important role in both TR1 and TR2, as it is involved in important motifs in these regions, including motifs that were well reported to affect the flexibility and disorder of the comprised regions [2,22,45,53,55,56,57].
Water solvation may play a significant role in the determination of the dynamics of the S protein in different parts, and the overall rigidities of the S protein in the two viruses may contribute to the differences between the two types. The TR1 (also referred as loop 3, L3) is markedly more rigid in the SARS-CoV-2/ACE2 adduct as compared to that of SARS-CoV [22]. Indeed, TR1 in SARS-CoV-2 possesses a more defined secondary structure (composed by small β-sheets), which is preserved along the MD simulations. Ostensibly, TR1’s length is different in the two SARS variants, being characterized by the insertion of Gly482, in SARS-CoV-2. This makes TR1 longer and more structured, enabling it to gain stabilizing interactions (namely, the mutated residues Gly485 with Cys488 and Gln474 with Gly476) in the SARS-CoV-2/ACE2 adduct. This amino acid insertion, along with other amino acidic mutations, stunningly convert an unessential part of the RBM into a strikingly effective recognition grasp for ACE2, allowing SARS-CoV-2 to stiffen, by establishing stronger interfacial interactions [22]. The presence of potent S1/S2-1 furin-like cleavage sites in SARS-CoV-2 and certain glycosylation tendencies may have critical roles in the tropism and pathogenesis of COVID-19. It is also possible, but thus far unproven, that other mutations that are distal from the RBM may contribute to such differences, and affect the binding.
9. S Protein and ACE2 Differences Determine the Risk of Being an Intermediate Host
Amino acids in RBM region of S protein and their contacts are critical for the binding of viruses in human and other animal reservoirs, and they can be used to assess potential intermediate hosts. For example, it was mentioned in Section 9 that a single K353A mutation in ACE2 was sufficient to abolish the interactions of ACE2 with SARS-CoV-2. Interestingly, most mammals (human, civet, bat, pig, ferret, cat, orangutan and monkey) have lysine at this position, but some mammals, such as mouse and rat, have histidine instead of lysine at this position. This difference requires assessment of the effect on their risk of being intermediate hosts [1].
On the basis of structural information regarding the complex of hACE2 and the RBD of SARS-CoV-2, the affinity to the S protein of the 20 key residues in ACE2 from mammal, bird, turtle and snake has been analyzed. Several ACE2 proteins from primates, bovidae, cricetidae and cetacea have been found to maintain the majority of key residues in ACE2 that associate with the SARS-CoV-2 RBD. Simulated structures have indicated that ACE2 proteins from bovidae and cricetidae are able to associate with the SARS-CoV-2 RBD, which suggests that bovidae and cricetidae should be included in the screening of intermediate hosts for SARS-CoV-2 [47]. Moreover, it has been found that nearly half of the key residues in turtle, snake and bird are changed. The simulated structures show that several key contacts with the SARS-CoV-2 RBD in turtle and snake ACE2 are eliminated. This finding indicates that neither snakes nor turtles maybe intermediate hosts for SARS-CoV-2, which further reinforces the concept that reptiles are resistant to infection by coronaviruses. However, other studies have indicated that interaction between the key amino acids of the S protein RBD and ACE2 in turtles may lead to these animals acting as potential intermediate hosts that can transmit SARS-CoV-2 to humans [46]. It has also been previously suggested that pangolins and snakes may act as intermediate hosts.
It has also been found that most mammals, including pets (dog and cat), pangolins and Cricetidae mammals retain the most key residues in ACE2 for association with the S protein from SARS-CoV and SARS-CoV-2. The interaction interface between the ACE2 of these mammals and the SARS-CoV/SARS-CoV-2 S protein has been manipulated through homology modeling. These studies identified a closer contact between Asn82 in ACE2 and the SARS-CoV-2 S protein than that between M82 in human ACE2 and the SARS-CoV-2 S protein. These findings provide important insights into the host range of SARS-CoV-2 and a new strategy to design an optimized ACE2 for SARS-CoV-2 infection [34,47].
10. Conclusions
SARS-CoV-2 has become known across the world in the last few months. It shows a pathogenesis spectrum and affinity to host receptors that are different from those of SARS-CoV and MERS-CoV. SARS-CoV-2 shares high similarity with SARS-CoV, nevertheless, small differences between them might be used to explain differences in behavior. Noticeably, the RBM of the SARS-CoV-2 S protein shows significant differences from those of SASR-CoV and MERS-CoV. For instance, the mutation of Leu to Phe486 (in addition to Pro to Ala475, Pro to Glu484, Lys to Thr478, Asp to Gly476 and a Val483 insertion) in the TR1 region makes it a more hydrophobic and ordered structure than that present in the other coronaviruses. The changes in the ridge region of Val to Lys417 (which increases the electrostatic interactions), Asn to Gln493 (which increases the number of hydrogen bonds), Asp to Ser494 and Lys to Leu452 (which make the shallow pit more hydrophobic) may give SARS-CoV-2 an advantage to bind mainly through these regions. In comparison, the presence of Arg426, Thr433 and Tyr484 in SARS-CoV, instead of Asn439, Gly446 and Gln498 in SARS-CoV-2, increases the number of electrostatic interactions, hydrogen bonds and stacking interactions in the TR2 region, respectively, and these alterations give SARS-CoV an advantage to bind mainly through TR2. Different types and numbers of interactions and different regions between SARS-CoV and SARS-CoV-2 may explain many of their different tendencies for infecting different hosts and for binding particular host receptors in specific ways. Moreover, it seems that proline plays a central role in TR1 and TR2 structure and interactions (through the appearance or disappearance of important motifs in these regions, and its role in the formation of different ordered structures). Solvation might play significant roles in the determination of the dynamics of the protein in different parts. The overall rigidity, flexibility and disorder of the different regions of S protein in the two viruses may additionally contribute to such differences. The presence of additional potent furin cleavage site (S1/S2-1) in SARS-CoV-2 and different glycosylation propensities may play critical roles in the tropism, pathogenesis and binding of the protein with drugs and antibodies. More studies are needed to investigate the effects of combinations of these factors, and computational studies may provide information to elucidate many of these concerns.
Supplementary Materials
The following are available online at https://www.mdpi.com/2073-4409/9/12/2638/s1, Figure S1. Structural alignment of TR2 for both SARS-CoV (green) and SARS-CoV-2 (red); the annotated amino acids represent those that differ between the two viruses; Figure S2. The main contacting residues from ACE2 with RBM region.
Author Contributions
Conceptualization, M.M.H.; investigation, M.M.H.; writing—original draft preparation, M.M.H.; writing—review and editing, W.A., M.A.I.A.-H., M.H., O.S., M.O.T., A.J.O., J.C.B., R.M. and M.P. All authors have read and agreed to the published version of the manuscript.
Funding
This research received no external funding.
Acknowledgments
M.M.H. would like to thank The Hashemite University for providing financial support, and IMAN1 Center (Jordan’s National Supercomputing Center) for providing computational tools and high-performance computing system to perform the analyses, special thanks to Eng. Zaid Abudayyeh from IMAN1 Center for providing technical support. M.A.I.A.-H. would like to acknowledge the Universiti Sains Malaysia (USM) Fellowship Scheme for providing financial support. M.P. is an NHMRC Senior Research Fellow.
Conflicts of Interest
The authors declare no conflict of interest.
References
- Wan, Y.; Shang, J.; Graham, R.; Baric, R.S.; Li, F. Receptor recognition by the novel coronavirus from Wuhan: An analysis based on decade-long structural studies of SARS coronavirus. J. Virol. 2020, 94, 94. [Google Scholar] [CrossRef] [PubMed]
- Wang, Q.; Zhang, Y.; Wu, L.; Niu, S.; Song, C.; Zhang, Z.; Lu, G.; Qiao, C.; Hu, Y.; Yuen, K.-Y. Structural and functional basis of SARS-CoV-2 entry by using human ACE2. Cell 2020, 181, 894–904.e9. [Google Scholar] [CrossRef] [PubMed]
- Shereen, M.A.; Khan, S.; Kazmi, A.; Bashir, N.; Siddique, R. COVID-19 infection: Origin, transmission, and characteristics of human coronaviruses. J. Adv. Res. 2020, 24, 91–98. [Google Scholar] [CrossRef] [PubMed]
- The, L.I.D. Challenges of coronavirus disease 2019. Lancet Infect. Dis. 2020, 20, 261. [Google Scholar]
- Huang, J.; Song, W.; Huang, H.; Sun, Q. Pharmacological therapeutics targeting RNA-dependent RNA polymerase, proteinase and spike protein: From mechanistic studies to clinical trials for COVID-19. J. Clin. Med. 2020, 9, 1131. [Google Scholar] [CrossRef] [PubMed]
- Lan, J.; Ge, J.; Yu, J.; Shan, S.; Zhou, H.; Fan, S.; Zhang, Q.; Shi, X.; Wang, Q.; Zhang, L. Structure of the SARS-CoV-2 spike receptor-binding domain bound to the ACE2 receptor. Nature 2020, 581, 215–220. [Google Scholar] [CrossRef]
- Fehr, A.R.; Perlman, S. Coronaviruses: An Overview of Their Replication and Pathogenesis. In Coronaviruses: Methods and Protocols; Maier, H.J., Bickerton, E., Britton, P., Eds.; Springer: New York, NY, USA, 2015; pp. 1–23. [Google Scholar]
- Turner, A. Chapter 25-ACE2 cell biology, regulation, and physiological functions. In The Protective Arm of the Renin Angiotensin System (RAS): Functional Aspects; Academic Press: Cambridge, MA, USA, 2015. [Google Scholar]
- Han, Y.; Král, P. Computational Design of ACE2-Based Peptide Inhibitors of SARS-CoV-2. ACS Nano 2020, 14, 5143–5147. [Google Scholar] [CrossRef]
- Deng, X.; Cao, M.; Zhang, J.; Hu, K.; Yin, Z.; Zhou, Z.; Xiao, X.; Yang, Y.; Sheng, W.; Wu, Y. Hyaluronic acid-chitosan nanoparticles for co-delivery of MiR-34a and doxorubicin in therapy against triple negative breast cancer. Biomaterials 2014, 35, 4333–4344. [Google Scholar] [CrossRef]
- Magrone, T.; Magrone, M.; Jirillo, E. Focus on Receptors for Coronaviruses with Special Reference to Angiotensin-converting Enzyme 2 as a Potential Drug Target—A Perspective. Endocr. Metab. Immune Disord. Drug Targets 2020, 20, 807–811. [Google Scholar] [CrossRef]
- Batlle, D.; Wysocki, J.; Satchell, K. Soluble angiotensin-converting enzyme 2: A potential approach for coronavirus infection therapy? Clin. Sci. 2020, 134, 543–545. [Google Scholar] [CrossRef]
- Robson, B. COVID-19 Coronavirus spike protein analysis for synthetic vaccines, a peptidomimetic antagonist, and therapeutic drugs, and analysis of a proposed achilles’ heel conserved region to minimize probability of escape mutations and drug resistance. Comput. Biol. Med. 2020, 121, 103749. [Google Scholar] [CrossRef] [PubMed]
- Kim, D.; Lee, J.-Y.; Yang, J.-S.; Kim, J.W.; Kim, V.N.; Chang, H. The architecture of SARS-CoV-2 transcriptome. Cell 2020, 181, 914–921.e10. [Google Scholar] [CrossRef] [PubMed]
- Wrapp, D.; Wang, N.; Corbett, K.S.; Goldsmith, J.A.; Hsieh, C.-L.; Abiona, O.; Graham, B.S.; McLellan, J.S. Cryo-EM structure of the 2019-nCoV spike in the prefusion conformation. Science 2020, 367, 1260–1263. [Google Scholar] [CrossRef]
- Lu, R.; Zhao, X.; Li, J.; Niu, P.; Yang, B.; Wu, H.; Wang, W.; Song, H.; Huang, B.; Zhu, N.; et al. Genomic characterisation and epidemiology of 2019 novel coronavirus: Implications for virus origins and receptor binding. Lancet 2020, 395, 565–574. [Google Scholar] [CrossRef]
- Wu, A.; Peng, Y.; Huang, B.; Ding, X.; Wang, X.; Niu, P.; Meng, J.; Zhu, Z.; Zhang, Z.; Wang, J. Genome composition and divergence of the novel coronavirus (2019-nCoV) originating in China. Cell Host Microbe 2020, 27, 325–328. [Google Scholar] [CrossRef]
- Snijder, E.; Decroly, E.; Ziebuhr, J. The nonstructural proteins directing coronavirus RNA synthesis and processing. In Advances in Virus Research; Elsevier: Amsterdam, The Netherlands, 2016; Volume 96, pp. 59–126. [Google Scholar]
- Sola, I.; Almazan, F.; Zuniga, S.; Enjuanes, L. Continuous and discontinuous RNA synthesis in coronaviruses. Annu. Rev. Virol. 2015, 2, 265–288. [Google Scholar] [CrossRef]
- Guruprasad, L. Evolutionary relationships and sequence-structure determinants in human SARS coronavirus-2 spike proteins for host receptor recognition. Proteins 2020, 88, 1387–1393. [Google Scholar] [CrossRef]
- Xia, S.; Liu, M.; Wang, C.; Xu, W.; Lan, Q.; Feng, S.; Qi, F.; Bao, L.; Du, L.; Liu, S. Inhibition of SARS-CoV-2 (previously 2019-nCoV) infection by a highly potent pan-coronavirus fusion inhibitor targeting its spike protein that harbors a high capacity to mediate membrane fusion. Cell Res. 2020, 30, 343–355. [Google Scholar] [CrossRef] [PubMed]
- Spinello, A.; Saltalamacchia, A.; Magistrato, A. Is the Rigidity of SARS-CoV-2 Spike Receptor-Binding Motif the Hallmark for Its Enhanced Infectivity? Insights from All-Atom Simulations. J. Phys. Chem. Lett. 2020, 11, 4785–4790. [Google Scholar] [CrossRef] [PubMed]
- Snijder, E.J.; Decroly, E.; Ziebuhr, J. The Nonstructural Proteins Directing Coronavirus RNA Synthesis and Processing. Adv. Virus. Res. 2016, 96, 59–126. [Google Scholar] [CrossRef] [PubMed]
- Wu, H.-Y.; Ke, T.-Y.; Liao, W.-Y.; Chang, N.-Y. Regulation of coronaviral poly (A) tail length during infection. PLoS ONE 2013, 8, e70548. [Google Scholar] [CrossRef] [PubMed]
- He, Y.; Zheng, C. Replication and transmission mechanisms of highly pathogenic human coronaviruses. Zhejiang Da Xue Xue Bao Yi Xue ban J. Zhejiang Univ. Med Sci. 2020, 49, 324–339. [Google Scholar]
- Tvarogová, J.; Madhugiri, R.; Bylapudi, G.; Ferguson, L.J.; Karl, N.; Ziebuhr, J. Identification and characterization of a human coronavirus 229E nonstructural protein 8-associated RNA 3′-terminal adenylyltransferase activity. J. Virol. 2019, 93, 93. [Google Scholar] [CrossRef] [PubMed]
- Coutard, B.; Valle, C.; de Lamballerie, X.; Canard, B.; Seidah, N.; Decroly, E. The spike glycoprotein of the new coronavirus 2019-nCoV contains a furin-like cleavage site absent in CoV of the same clade. Antivir. Res. 2020, 176, 104742. [Google Scholar] [CrossRef]
- Malik, Y.A. Properties of Coronavirus and SARS-CoV-2. Malays. J. Pathol. 2020, 42, 3–11. [Google Scholar] [PubMed]
- Al-Hatamleh, M.A.I.; Hatmal, M.M.; Sattar, K.; Ahmad, S.; Mustafa, M.Z.; Bittencourt, M.D.C.; Mohamud, R. Antiviral and Immunomodulatory Effects of Phytochemicals from Honey against COVID-19: Potential Mechanisms of Action and Future Directions. Molecules 2020, 25, 5017. [Google Scholar] [CrossRef] [PubMed]
- Rabaan, A.A.; Al-Ahmed, S.H.; Haque, S.; Sah, R.; Tiwari, R.; Malik, Y.S.; Dhama, K.; Yatoo, M.I.; Bonilla-Aldana, D.K.; Rodriguez-Morales, A.J. SARS-CoV-2, SARS-CoV, and MERS-CoV: A comparative overview. Infez. Med. 2020, 28, 174–184. [Google Scholar]
- Ji, H.-L.; Zhao, R.; Matalon, S.; Matthay, M.A. Elevated plasmin (ogen) as a common risk factor for COVID-19 susceptibility. Physiol. Rev. 2020, 100, 1065–1075. [Google Scholar] [CrossRef]
- Kumar, S.; Maurya, V.K.; Prasad, A.K.; Bhatt, M.L.; Saxena, S.K. Structural, glycosylation and antigenic variation between 2019 novel coronavirus (2019-nCoV) and SARS coronavirus (SARS-CoV). Virusdisease 2020, 31, 13–21. [Google Scholar] [CrossRef]
- Yin, C. Genotyping coronavirus SARS-CoV-2: Methods and implications. Genomics 2020, 112, 3588–3596. [Google Scholar] [CrossRef]
- Xia, S.; Liu, Q.; Wang, Q.; Sun, Z.; Su, S.; Du, L.; Ying, T.; Lu, L.; Jiang, S. Middle East respiratory syndrome coronavirus (MERS-CoV) entry inhibitors targeting spike protein. Virus Res. 2014, 194, 200–210. [Google Scholar] [CrossRef] [PubMed]
- Lu, G.; Wang, Q.; Gao, G.F. Bat-to-human: Spike features determining ‘host jump’of coronaviruses SARS-CoV, MERS-CoV, and beyond. Trends Microbiol. 2015, 23, 468–478. [Google Scholar] [CrossRef] [PubMed]
- Jaimes, J.A.; André, N.M.; Chappie, J.S.; Millet, J.K.; Whittaker, G.R. Phylogenetic analysis and structural modeling of SARS-CoV-2 spike protein reveals an evolutionary distinct and proteolytically-sensitive activation loop. J. Mol. Biol. 2020, 432, 3309–3325. [Google Scholar] [CrossRef] [PubMed]
- Hulswit, R.; De Haan, C.; Bosch, B.-J. Coronavirus spike protein and tropism changes. In Advances in Virus Research; Elsevier: Amsterdam, The Netherlands, 2016; Volume 96, pp. 29–57. [Google Scholar]
- Zhou, P.; Yang, X.-L.; Wang, X.-G.; Hu, B.; Zhang, L.; Zhang, W.; Si, H.-R.; Zhu, Y.; Li, B.; Huang, C.-L. A pneumonia outbreak associated with a new coronavirus of probable bat origin. Nature 2020, 579, 270–273. [Google Scholar] [CrossRef] [PubMed]
- Hoffmann, M.; Kleine-Weber, H.; Schroeder, S.; Krüger, N.; Herrler, T.; Erichsen, S.; Schiergens, T.S.; Herrler, G.; Wu, N.-H.; Nitsche, A. SARS-CoV-2 cell entry depends on ACE2 and TMPRSS2 and is blocked by a clinically proven protease inhibitor. Cell 2020, 181, 271–280.e8. [Google Scholar] [CrossRef]
- Li, F.; Li, W.; Farzan, M.; Harrison, S.C. Structure of SARS coronavirus spike receptor-binding domain complexed with receptor. Science 2005, 309, 1864–1868. [Google Scholar] [CrossRef]
- Chang, T.-J.; Yang, D.-M.; Wang, M.-L.; Liang, K.-H.; Tsai, P.-H.; Chiou, S.-H.; Lin, T.-H.; Wang, C.-T. Genomic analysis and comparative multiple sequences of SARS-CoV2. J. Chin. Med. Assoc. 2020, 83, 537–543. [Google Scholar] [CrossRef]
- Tai, W.; He, L.; Zhang, X.; Pu, J.; Voronin, D.; Jiang, S.; Zhou, Y.; Du, L. Characterization of the receptor-binding domain (RBD) of 2019 novel coronavirus: Implication for development of RBD protein as a viral attachment inhibitor and vaccine. Cell. Mol. Immunol. 2020, 17, 613–620. [Google Scholar] [CrossRef]
- Bahar, I.; Atilgan, A.R.; Erman, B. Direct evaluation of thermal fluctuations in proteins using a single-parameter harmonic potential. Fold. Des. 1997, 2, 173–181. [Google Scholar] [CrossRef]
- Rowland, R.R.; Yoo, D. Nucleolar-cytoplasmic shuttling of PRRSV nucleocapsid protein: A simple case of molecular mimicry or the complex regulation by nuclear import, nucleolar localization and nuclear export signal sequences. Virus Res. 2003, 95, 23–33. [Google Scholar] [CrossRef]
- Yan, R.; Zhang, Y.; Li, Y.; Xia, L.; Guo, Y.; Zhou, Q. Structural basis for the recognition of SARS-CoV-2 by full-length human ACE2. Science 2020, 367, 1444–1448. [Google Scholar] [CrossRef] [PubMed]
- Liu, Z.; Xiao, X.; Wei, X.; Li, J.; Yang, J.; Tan, H.; Zhu, J.; Zhang, Q.; Wu, J.; Liu, L. Composition and divergence of coronavirus spike proteins and host ACE2 receptors predict potential intermediate hosts of SARS-CoV-2. J. Med. Virol. 2020, 92, 595–601. [Google Scholar] [CrossRef] [PubMed]
- Luan, J.; Lu, Y.; Jin, X.; Zhang, L. Spike protein recognition of mammalian ACE2 predicts the host range and an optimized ACE2 for SARS-CoV-2 infection. Biochem. Biophys. Res. Commun. 2020, 526, 165–169. [Google Scholar] [CrossRef] [PubMed]
- Carugo, O. How large B-factors can be in protein crystal structures. BMC Bioinform. 2018, 19, 61. [Google Scholar] [CrossRef] [PubMed]
- Wang, Y.; Liu, M.; Gao, J. Enhanced receptor binding of SARS-CoV-2 through networks of hydrogen-bonding and hydrophobic interactions. Proc. Natl. Acad. Sci. USA 2020, 117, 13967–13974. [Google Scholar] [CrossRef] [PubMed]
- Joshi, S.; Joshi, M.; Degani, M.S. Tackling SARS-CoV-2: Proposed targets and repurposed drugs. Future Med. Chem. 2020, 12, 1579–1601. [Google Scholar] [CrossRef] [PubMed]
- Ibrahim, I.M.; Abdelmalek, D.H.; Elshahat, M.E.; Elfiky, A.A. COVID-19 spike-host cell receptor GRP78 binding site prediction. J. Infect. 2020, 80, 554–562. [Google Scholar] [CrossRef]
- Dahanayake, J.N.; Mitchell-Koch, K.R. How does solvation layer mobility affect protein structural dynamics? Front. Mol. Biosci. 2018, 5, 65. [Google Scholar] [CrossRef]
- Kay, B.K.; Williamson, M.P.; Sudol, M. The importance of being proline: The interaction of proline-rich motifs in signaling proteins with their cognate domains. FASEB J. 2000, 14, 231–241. [Google Scholar] [CrossRef]
- Sudol, M.; Bedford, M.T. Competitive Binding of Proline-Rich Sequences by SH3, WW, and Other Functionally Related Protein Domains. In Proteomics and Protein-Protein Interactions: Biology, Chemistry, Bioinformatics, and Drug Design; Waksman, G., Ed.; Springer: Boston, MA, USA, 2005; pp. 185–201. [Google Scholar]
- Lise, S.; Jones, D. Sequence patterns associated with disordered regions in proteins. PROTEINS Struct. Funct. Bioinform. 2005, 58, 144–150. [Google Scholar] [CrossRef]
- Iakoucheva, L.M.; Kimzey, A.L.; Masselon, C.D.; Bruce, J.E.; Garner, E.C.; Brown, C.J.; Dunker, A.K.; Smith, R.D.; Ackerman, E.J. Identification of intrinsic order and disorder in the DNA repair protein XPA. Protein Sci. 2001, 10, 560–571. [Google Scholar] [CrossRef] [PubMed]
- Bright, J.N.; Sansom, M.S. The flexing/twirling helix: Exploring the flexibility about molecular hinges formed by proline and glycine motifs in transmembrane helices. J. Phys. Chem. B 2003, 107, 627–636. [Google Scholar] [CrossRef]
- Chowdhury, R.; Maranas, C.D. Biophysical characterization of the SARS-CoV-2 spike protein binding with the ACE2 receptor explains increased COVID-19 pathogenesis. bioRxiv 2020. preprint. [Google Scholar] [CrossRef]
- Wu, C.; Liu, Y.; Yang, Y.; Zhang, P.; Zhong, W.; Wang, Y.; Wang, Q.; Xu, Y.; Li, M.; Li, X. Analysis of therapeutic targets for SARS-CoV-2 and discovery of potential drugs by computational methods. Acta Pharm. Sin. B 2020, 10, 766–788. [Google Scholar] [CrossRef] [PubMed]
- Yuan, M.; Wu, N.C.; Zhu, X.; Lee, C.-C.D.; So, R.T.; Lv, H.; Mok, C.K.; Wilson, I.A. A highly conserved cryptic epitope in the receptor binding domains of SARS-CoV-2 and SARS-CoV. Science 2020, 368, 630–633. [Google Scholar] [CrossRef] [PubMed]
- Fantini, J.; Di Scala, C.; Chahinian, H.; Yahi, N. Structural and molecular modeling studies reveal a new mechanism of action of chloroquine and hydroxychloroquine against SARS-CoV-2 infection. Int. J. Antimicrob. Agents 2020, 55, 105960. [Google Scholar] [CrossRef] [PubMed]
- Brufsky, A. Distinct Viral Clades of SARS-CoV-2: Implications for Modeling of Viral Spread. J. Med. Virol. 2020, 92, 1386–1390. [Google Scholar] [CrossRef]
- Reva, B.A.; Finkelstein, A.V.; Skolnick, J. What is the probability of a chance prediction of a protein structure with an rmsd of 6 A? Fold. Des. 1998, 3, 141–147. [Google Scholar] [CrossRef]
- Hatmal, M.M.; Taha, M.O. Combining Stochastic Deformation/Relaxation and Intermolecular Contacts Analysis for Extracting Pharmacophores from Ligand-Receptor Complexes. J. Chem. Inf. Model. 2018, 58, 879–893. [Google Scholar] [CrossRef]
- Maiorov, V.N.; Crippen, G.M. Significance of root-mean-square deviation in comparing three-dimensional structures of globular proteins. J. Mol. Biol. 1994, 235, 625–634. [Google Scholar] [CrossRef]
- Kannan, S.; Ali, P.S.S.; Sheeza, A.; Hemalatha, K. COVID-19 (Novel Coronavirus 2019)-recent trends. Eur. Rev. Med. Pharmacol. Sci. 2020, 24, 2006–2011. [Google Scholar] [PubMed]
- Kuster, G.M.; Pfister, O.; Burkard, T.; Zhou, Q.; Twerenbold, R.; Haaf, P.; Widmer, A.F.; Osswald, S. SARS-CoV2: Should inhibitors of the renin–angiotensin system be withdrawn in patients with COVID-19? Eur. Heart J. 2020, 41, 1801–1803. [Google Scholar] [CrossRef] [PubMed]
- Gu, J.; Korteweg, C. Pathology and pathogenesis of severe acute respiratory syndrome. Am. J. Pathol. 2007, 170, 1136–1147. [Google Scholar] [CrossRef] [PubMed]
- Ou, X.; Liu, Y.; Lei, X.; Li, P.; Mi, D.; Ren, L.; Guo, L.; Guo, R.; Chen, T.; Hu, J. Characterization of spike glycoprotein of SARS-CoV-2 on virus entry and its immune cross-reactivity with SARS-CoV. Nat. Commun. 2020, 11, 1–12. [Google Scholar] [CrossRef] [PubMed]
- Delmas, B.; Laude, H. Assembly of coronavirus spike protein into trimers and its role in epitope expression. J. Virol. 1990, 64, 5367–5375. [Google Scholar] [CrossRef]
- Kim, E.; Erdos, G.; Huang, S.; Kenniston, T.W.; Balmert, S.C.; Carey, C.D.; Raj, V.S.; Epperly, M.W.; Klimstra, W.B.; Haagmans, B.L. Microneedle array delivered recombinant coronavirus vaccines: Immunogenicity and rapid translational development. EBioMedicine 2020, 55, 102743. [Google Scholar] [CrossRef] [PubMed]
- Li, F. Structure, function, and evolution of coronavirus spike proteins. Annu. Rev. Virol. 2016, 3, 237–261. [Google Scholar] [CrossRef] [PubMed]
- Bosch, B.J.; Van Der Zee, R.; De Haan, C.A.M.; Rottier, P.J.M. The coronavirus spike protein is a class I virus fusion protein: Structural and functional characterization of the fusion core complex. J. Virol. 2003, 77, 8801–8811. [Google Scholar] [CrossRef] [PubMed]
- Wang, K.; Chen, W.; Zhou, Y.-S.; Lian, J.-Q.; Zhang, Z.; Du, P.; Gong, L.; Zhang, Y.; Cui, H.-Y.; Geng, J.-J.; et al. SARS-CoV-2 invades host cells via a novel route: CD147-spike protein. bioRxiv 2020. preprint. [Google Scholar] [CrossRef]
- Dhama, K.; Sharun, K.; Tiwari, R.; Dadar, M.; Malik, Y.S.; Singh, K.P.; Chaicumpa, W. COVID-19, an emerging coronavirus infection: Advances and prospects in designing and developing vaccines, immunotherapeutics, and therapeutics. Hum. Vaccines Immunother. 2020, 16, 1232–1238. [Google Scholar] [CrossRef] [PubMed]
- Dahms, S.O.; Hardes, K.; Steinmetzer, T.; Than, M.E. X-ray structures of the proprotein convertase furin bound with substrate analogue inhibitors reveal substrate specificity determinants beyond the s4 pocket. Biochemistry 2018, 57, 925–934. [Google Scholar] [CrossRef] [PubMed]
- Elshuber, S.; Mandl, C.W. Resuscitating mutations in a furin cleavage-deficient mutant of the flavivirus tick-borne encephalitis virus. J. Virol. 2005, 79, 11813–11823. [Google Scholar] [CrossRef] [PubMed]
- Shiryaev, S.A.; Chernov, A.V.; Golubkov, V.S.; Thomsen, E.R.; Chudin, E.; Chee, M.S.; Kozlov, I.A.; Strongin, A.Y.; Cieplak, P. High-resolution analysis and functional mapping of cleavage sites and substrate proteins of furin in the human proteome. PLoS ONE 2013, 8, e54290. [Google Scholar] [CrossRef]
- Follis, K.E.; York, J.; Nunberg, J.H. Furin cleavage of the SARS coronavirus spike glycoprotein enhances cell–cell fusion but does not affect virion entry. Virology 2006, 350, 358–369. [Google Scholar] [CrossRef]
- Shiryaev, S.A.; Remacle, A.G.; Ratnikov, B.I.; Nelson, N.A.; Savinov, A.Y.; Wei, G.; Bottini, M.; Rega, M.F.; Parent, A.; Desjardins, R. Targeting host cell furin proprotein convertases as a therapeutic strategy against bacterial toxins and viral pathogens. J. Biol. Chem. 2007, 282, 20847–20853. [Google Scholar] [CrossRef]
- Duckert, P.; Brunak, S.; Blom, N. Prediction of proprotein convertase cleavage sites. Protein Eng. Des. Sel. 2004, 17, 107–112. [Google Scholar] [CrossRef]
- Tian, S.; Huajun, W.; Wu, J. Computational prediction of furin cleavage sites by a hybrid method and understanding mechanism underlying diseases. Sci. Rep. 2012, 2, 261. [Google Scholar] [CrossRef]
- Millet, J.K.; Whittaker, G.R. Host cell entry of Middle East respiratory syndrome coronavirus after two-step, furin-mediated activation of the spike protein. Proc. Natl. Acad. Sci. USA 2014, 111, 15214–15219. [Google Scholar] [CrossRef]
- Zhang, T.; Wu, Q.; Zhang, Z. Probable pangolin origin of SARS-CoV-2 associated with the COVID-19 outbreak. Curr. Biol. 2020, 30, 1346–1351. [Google Scholar] [CrossRef]
- Letko, M.; Marzi, A.; Munster, V. Functional assessment of cell entry and receptor usage for SARS-CoV-2 and other lineage B betacoronaviruses. Nat. Microbiol. 2020, 5, 562–569. [Google Scholar] [CrossRef]
- Braun, E.; Sauter, D. Furin-mediated protein processing in infectious diseases and cancer. Clin. Transl. Immunol. 2019, 8, e1073. [Google Scholar] [CrossRef] [PubMed]
- Izaguirre, G. The proteolytic regulation of virus cell entry by furin and other proprotein convertases. Viruses 2019, 11, 837. [Google Scholar] [CrossRef] [PubMed]
- Seidah, N.G.; Prat, A. The biology and therapeutic targeting of the proprotein convertases. Nat. Rev. Drug Discov. 2012, 11, 367–383. [Google Scholar] [CrossRef] [PubMed]
- Decha, P.; Rungrotmongkol, T.; Intharathep, P.; Malaisree, M.; Aruksakunwong, O.; Laohpongspaisan, C.; Parasuk, V.; Sompornpisut, P.; Pianwanit, S.; Kokpol, S. Source of high pathogenicity of an avian influenza virus H5N1: Why H5 is better cleaved by furin. Biophys. J. 2008, 95, 128–134. [Google Scholar] [CrossRef][Green Version]
- Schwab, M. Encyclopedia of Cancer; Springer: Berlin/Heidelberg, Germany, 2011. [Google Scholar]
- Bottomley, K.M.; Bradshaw, D.; Nixon, J.S. Metalloproteinases as Targets for Anti-Inflammatory Drugs; Springer: Basel, Switzerland, 1999; Volume 14. [Google Scholar]
- Nagase, H.; Woessner, J.F. Matrix metalloproteinases. J. Biol. Chem. 1999, 274, 21491–21494. [Google Scholar] [CrossRef]
- Hernandez-Barrantes, S.; Bernardo, M.; Toth, M.; Fridman, R. Regulation of membrane type-matrix metalloproteinases. Semin. Cancer Biol. 2002, 12, 131–138. [Google Scholar] [CrossRef]
- Deryugina, E.I.; Ratnikov, B.I.; Yu, Q.; Baciu, P.C.; Rozanov, D.V.; Strongin, A.Y. Prointegrin maturation follows rapid trafficking and processing of MT1-MMP in Furin-Negative Colon Carcinoma LoVo Cells. Traffic 2004, 5, 627–641. [Google Scholar] [CrossRef]
- Nakai, K.; Kanehisa, M. A knowledge base for predicting protein localization sites in eukaryotic cells. Genomics 1992, 14, 897–911. [Google Scholar] [CrossRef]
- Rowland, R.R.; Kervin, R.; Kuckleburg, C.; Sperlich, A.; Benfield, D.A. The localization of porcine reproductive and respiratory syndrome virus nucleocapsid protein to the nucleolus of infected cells and identification of a potential nucleolar localization signal sequence. Virus. Res. 1999, 64, 1–12. [Google Scholar] [CrossRef]
- Rowland, R.R.; Schneider, P.; Fang, Y.; Wootton, S.; Yoo, D.; Benfield, D.A. Peptide domains involved in the localization of the porcine reproductive and respiratory syndrome virus nucleocapsid protein to the nucleolus. Virology 2003, 316, 135–145. [Google Scholar] [CrossRef]
- Tijms, M.A.; van der Meer, Y.; Snijder, E.J. Nuclear localization of non-structural protein 1 and nucleocapsid protein of equine arteritis virus. J. Gen. Virol. 2002, 83, 795–800. [Google Scholar] [CrossRef] [PubMed]
- Yoo, D.; Wootton, S.K.; Li, G.; Song, C.; Rowland, R.R. Colocalization and interaction of the porcine arterivirus nucleocapsid protein with the small nucleolar RNA-associated protein fibrillarin. J. Virol. 2003, 77, 12173–12183. [Google Scholar] [CrossRef] [PubMed]
- Hiscox, J. The nucleolus—A gateway to viral infection? Arch. Virol. 2002, 147, 1077–1089. [Google Scholar] [CrossRef]
- Hiscox, J.A.; Wurm, T.; Wilson, L.; Britton, P.; Cavanagh, D.; Brooks, G. The coronavirus infectious bronchitis virus nucleoprotein localizes to the nucleolus. J. Virol. 2001, 75, 506–512. [Google Scholar] [CrossRef] [PubMed]
- Rowland, R.R.; Chauhan, V.; Fang, Y.; Pekosz, A.; Kerrigan, M.; Burton, M.D. Intracellular localization of the severe acute respiratory syndrome coronavirus nucleocapsid protein: Absence of nucleolar accumulation during infection and after expression as a recombinant protein in vero cells. J. Virol. 2005, 79, 11507–11512. [Google Scholar] [CrossRef] [PubMed]
- Satarker, S.; Nampoothiri, M. Structural Proteins in Severe Acute Respiratory Syndrome Coronavirus-2. Arch. Med. Res. 2020, 51, 482–491. [Google Scholar] [CrossRef] [PubMed]
- Amin, M.; Sorour, M.K.; Kasry, A. Comparing the binding interactions in the receptor binding domains of SARS-CoV-2 and SARS-CoV. J. Phys. Chem. Lett. 2020, 11, 4897–4900. [Google Scholar] [CrossRef]
- Ortega, J.T.; Serrano, M.L.; Pujol, F.H.; Rangel, H.R. Role of changes in SARS-CoV-2 spike protein in the interaction with the human ACE2 receptor: An in silico analysis. EXCLI J. 2020, 19, 410. [Google Scholar]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).