Sensitivity of SARS-CoV-2 towards Alcohols: Potential for Alcohol-Related Toxicity in Humans
Abstract
:1. Introduction
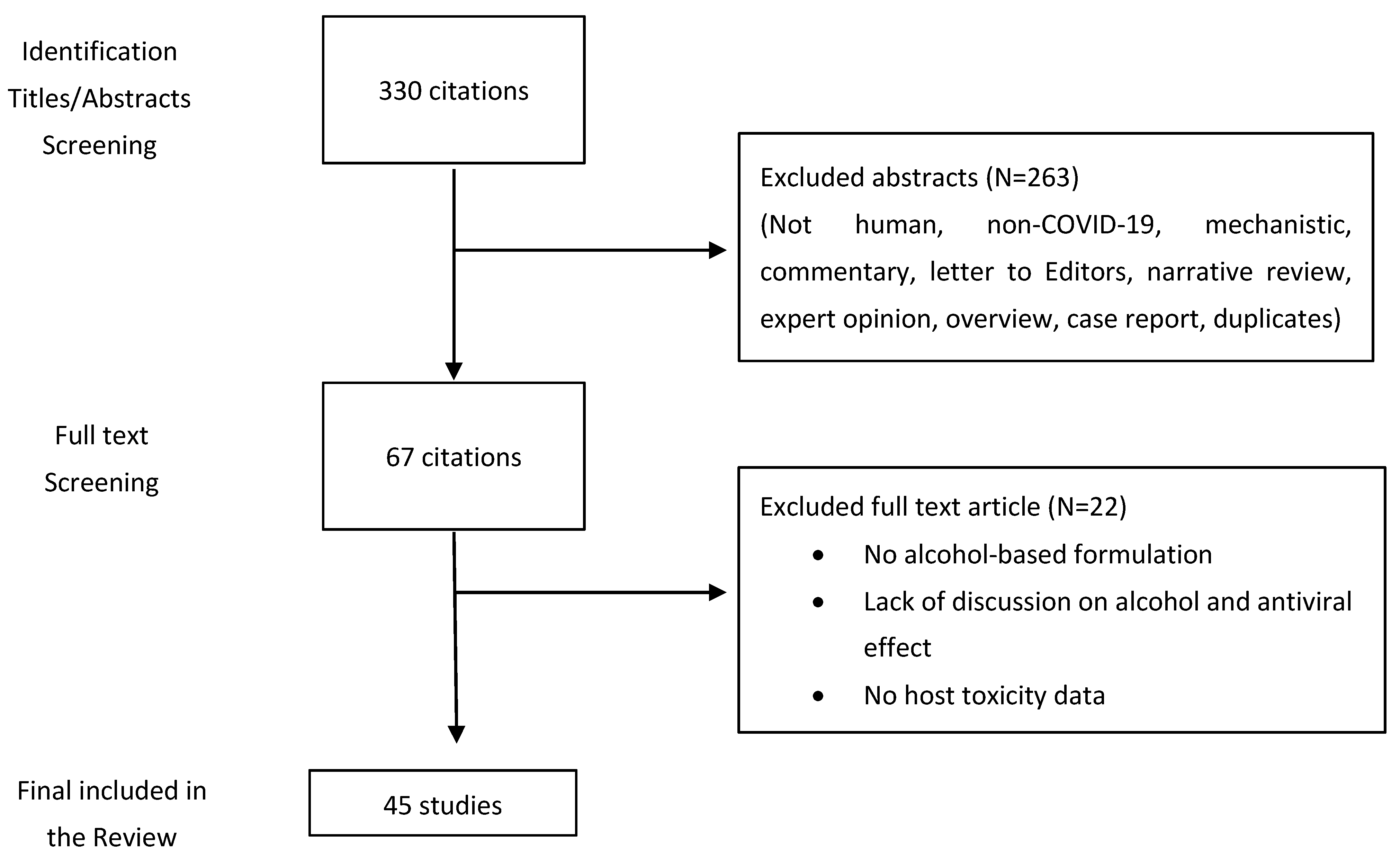
2. Methods
3. Characteristics of SARS-Cov-2 and Other Coronaviruses
4. Alcohol-Based Formulations of Hand Sanitizers
5. Effects of Different Alcohols on Coronavirus Family
6. Oral, Dermal, and Pulmonary Absorption of Alcohols and Their Related Toxicities
7. Alternatives and Precautions to ABHS
8. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- World Health Organization (WHO). Coronavirus Disease (COVID-19) Pandemic. 2020. Available online: https://www.who.int/emergencies/diseases/novel-coronavirus-2019 (accessed on 27 November 2021).
- Rodriguez-Morales, A.J.; Cardona-Ospina, J.A.; Gutierrez-Ocampo, E.; Villamizar-Pena, R.; Holguin-Rivera, Y.; Escalera-Antezana, J.P.; Alvarado-Arnez, L.E.; Bonilla-Aldana, D.K.; Franco-Paredes, C.; Henao-Martinez, A.F.; et al. Clinical, laboratory and imaging features of COVID-19: A systematic review and meta-analysis. Travel Med. Infect. Dis. 2020, 34, 101623. [Google Scholar] [CrossRef] [PubMed]
- Liu, K.; Chen, Y.; Lin, R.; Han, K. Clinical features of COVID-19 in elderly patients: A comparison with young and middle-aged patients. J. Infect. 2020, 80, e14–e18. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Yang, J.; Zheng, Y.; Gou, X.; Pu, K.; Chen, Z.; Guo, Q.; Ji, R.; Wang, H.; Wang, Y.; Zhou, Y. Prevalence of comorbidities and its effects in patients infected with SARS-CoV-2: A systematic review and meta-analysis. Int. J. Infect. Dis. 2020, 94, 91–95. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization (WHO). WHO Coronavirus Disease (COVID-19) Dashboard. Available online: https://covid19.who.int/ (accessed on 27 November 2021).
- U.S. Food and Drug Administration. Coronavirus (COVID-19) Update: FDA Issues Emergency Use Authorization for Potential COVID-19 Treatment. Available online: https://www.fda.gov/news-events/press-announcements/coronavirus-covid-19-update-fda-issues-emergency-use-authorization-potential-covid-19-treatment#:~:text=The%20emergency%20use%20authorization%20allows,children%20hospitalized%20with%20severe%20disease (accessed on 27 November 2021).
- Health Canada. Drug and Vaccine Authorizations for COVID-19: List of Authorized Drugs, Vaccines and Expanded Indications. Available online: https://www.canada.ca/en/health-canada/services/drugs-health-products/covid19-industry/drugs-vaccines-treatments/authorization/list-drugs.html#wb-auto-4 (accessed on 27 November 2021).
- European Medicines Agency (EMA). COVID-19 Treatments. Available online: https://www.ema.europa.eu/en/human-regulatory/overview/public-health-threats/coronavirus-disease-covid-19/treatments-vaccines/covid-19-treatments (accessed on 27 November 2021).
- Centers for Disease Control and Prevention (CDC). Core Infection Prevention and Control Practices for Safe Healthcare Delivery in All Settings—Recommendations of the Healthcare Infection Control Practices Advisory Committee. Available online: https://www.cdc.gov/hicpac/recommendations/core-practices.html (accessed on 27 November 2021).
- Centers for Disease Control and Prevention (CDC). People Who Are at Higher Risk for Severe Illness. Available online: https://www.cdc.gov/coronavirus/2019-ncov/need-extra-precautions/groups-at-higher-risk.html (accessed on 8 April 2021).
- Dellanno, C.; Vega, Q.; Boesenberg, D. The antiviral action of common household disinfectants and antiseptics against murine hepatitis virus, a potential surrogate for SARS coronavirus. Am. J. Infect. Control 2009, 37, 649–652. [Google Scholar] [CrossRef] [Green Version]
- McDonnell, G.; Russell, A.D. Antiseptics and disinfectants: Activity, action, and resistance. Clin. Microbiol. Rev. 1999, 12, 147–179. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Chen, J. Pathogenicity and transmissibility of 2019-nCoV-A quick overview and comparison with other emerging viruses. Microbes Infect. 2020, 22, 69–71. [Google Scholar] [CrossRef] [PubMed]
- Yin, Y.; Wunderink, R.G. MERS, SARS and other coronaviruses as causes of pneumonia. Respirology 2018, 23, 130–137. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Mihindukulasuriya, K.A.; Wu, G.; St Leger, J.; Nordhausen, R.W.; Wang, D. Identification of a novel coronavirus from a beluga whale by using a panviral microarray. J. Virol. 2008, 82, 5084–5088. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Woo, P.C.; Lau, S.K.; Lam, C.S.; Lai, K.K.; Huang, Y.; Lee, P.; Luk, G.S.; Dyrting, K.C.; Chan, K.H.; Yuen, K.Y. Comparative analysis of complete genome sequences of three avian coronaviruses reveals a novel group 3c coronavirus. J. Virol. 2009, 83, 908–917. [Google Scholar] [CrossRef] [Green Version]
- Chan, J.F.; Kok, K.H.; Zhu, Z.; Chu, H.; To, K.K.; Yuan, S.; Yuen, K.Y. Genomic characterization of the 2019 novel human-pathogenic coronavirus isolated from a patient with atypical pneumonia after visiting Wuhan. Emerg. Microbes Infect. 2020, 9, 221–236. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Wu, A.; Peng, Y.; Huang, B.; Ding, X.; Wang, X.; Niu, P.; Meng, J.; Zhu, Z.; Zhang, Z.; Wang, J.; et al. Genome composition and divergence of the novel coronavirus (2019-nCoV) originating in China. Cell Host Microbe 2020, 27, 325–328. [Google Scholar] [CrossRef] [Green Version]
- Gordon, D.E.; Jang, G.M.; Bouhaddou, M.; Xu, J.; Obernier, K.; White, K.M.; O’Meara, M.J.; Rezelj, V.V.; Guo, J.Z.; Swaney, D.L.; et al. A SARS-CoV-2 protein interaction map reveals targets for drug repurposing. Nature 2020, 583, 459–468. [Google Scholar] [CrossRef] [PubMed]
- Marra, M.A.; Jones, S.J.; Astell, C.R.; Holt, R.A.; Brooks-Wilson, A.; Butterfield, Y.S.; Khattra, J.; Asano, J.K.; Barber, S.A.; Chan, S.Y.; et al. The genome sequence of the SARS-associated coronavirus. Science 2003, 300, 1399–1404. [Google Scholar] [CrossRef] [Green Version]
- Ruan, Y.J.; Wei, C.L.; Ee, A.L.; Vega, V.B.; Thoreau, H.; Su, S.T.; Chia, J.M.; Ng, P.; Chiu, K.P.; Lim, L.; et al. Comparative full-length genome sequence analysis of 14 SARS coronavirus isolates and common mutations associated with putative origins of infection. Lancet 2003, 361, 1779–1785. [Google Scholar] [CrossRef] [Green Version]
- Wong, S.K.; Li, W.; Moore, M.J.; Choe, H.; Farzan, M. A 193-amino acid fragment of the SARS coronavirus S protein efficiently binds angiotensin-converting enzyme 2. J. Biol. Chem. 2004, 279, 3197–3201. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Coutard, B.; Valle, C.; de Lamballerie, X.; Canard, B.; Seidah, N.G.; Decroly, E. The spike glycoprotein of the new coronavirus 2019-nCoV contains a furin-like cleavage site absent in CoV of the same clade. Antivir. Res. 2020, 176, 104742. [Google Scholar] [CrossRef] [PubMed]
- Guo, J.P.; Petric, M.; Campbell, W.; McGeer, P.L. SARS corona virus peptides recognized by antibodies in the sera of convalescent cases. Virology 2004, 324, 251–256. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Wang, J.; Wen, J.; Li, J.; Yin, J.; Zhu, Q.; Wang, H.; Yang, Y.; Qin, E.; You, B.; Li, W.; et al. Assessment of immunoreactive synthetic peptides from the structural proteins of severe acute respiratory syndrome coronavirus. Clin. Chem. 2003, 49, 1989–1996. [Google Scholar] [CrossRef] [Green Version]
- Zhu, N.; Zhang, D.; Wang, W.; Li, X.; Yang, B.; Song, J.; Zhao, X.; Huang, B.; Shi, W.; Lu, R.; et al. A novel coronavirus from patients with pneumonia in China, 2019. N. Engl. J. Med. 2020, 382, 727–733. [Google Scholar] [CrossRef] [PubMed]
- Ren, L.L.; Wang, Y.M.; Wu, Z.Q.; Xiang, Z.C.; Guo, L.; Xu, T.; Jiang, Y.Z.; Xiong, Y.; Li, Y.J.; Li, X.W.; et al. Identification of a novel coronavirus causing severe pneumonia in human: A descriptive study. Chin. Med. J. 2020, 133, 1015–1024. [Google Scholar] [CrossRef] [PubMed]
- Lu, R.; Zhao, X.; Li, J.; Niu, P.; Yang, B.; Wu, H.; Wang, W.; Song, H.; Huang, B.; Zhu, N.; et al. Genomic characterisation and epidemiology of 2019 novel coronavirus: Implications for virus origins and receptor binding. Lancet 2020, 395, 565–574. [Google Scholar] [CrossRef] [Green Version]
- Zhou, P.; Yang, X.L.; Wang, X.G.; Hu, B.; Zhang, L.; Zhang, W.; Si, H.R.; Zhu, Y.; Li, B.; Huang, C.L.; et al. A pneumonia outbreak associated with a new coronavirus of probable bat origin. Nature 2020, 579, 270–273. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Andersen, K.G.; Rambaut, A.; Lipkin, W.I.; Holmes, E.C.; Garry, R.F. The proximal origin of SARS-CoV-2. Nat. Med. 2020, 26, 450–452. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Wrobel, A.G.; Benton, D.J.; Xu, P.; Roustan, C.; Martin, S.R.; Rosenthal, P.B.; Skehel, J.J.; Gamblin, S.J. SARS-CoV-2 and bat RaTG13 spike glycoprotein structures inform on virus evolution and furin-cleavage effects. Nat. Struct. Mol. Biol. 2020, 27, 763–767. [Google Scholar] [CrossRef]
- Cui, J.; Li, F.; Shi, Z.L. Origin and evolution of pathogenic coronaviruses. Nat. Rev. Microbiol. 2019, 17, 181–192. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Huang, C.; Wang, Y.; Li, X.; Ren, L.; Zhao, J.; Hu, Y.; Zhang, L.; Fan, G.; Xu, J.; Gu, X.; et al. Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China. Lancet 2020, 395, 497–506. [Google Scholar] [CrossRef] [Green Version]
- Zumla, A.; Chan, J.F.; Azhar, E.I.; Hui, D.S.; Yuen, K.Y. Coronaviruses—Drug discovery and therapeutic options. Nat. Rev. Drug Discov. 2016, 15, 327–347. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Vermeil, T.; Peters, A.; Kilpatrick, C.; Pires, D.; Allegranzi, B.; Pittet, D. Hand hygiene in hospitals: Anatomy of a revolution. J. Hosp. Infect. 2019, 101, 383–392. [Google Scholar] [CrossRef] [PubMed]
- Singh, D.; Joshi, K.; Samuel, A.; Patra, J.; Mahindroo, N. Alcohol-based hand sanitisers as first line of defence against SARS-CoV-2: A review of biology, chemistry and formulations. Epidemiol. Infect. 2020, 148, e229. [Google Scholar] [CrossRef] [PubMed]
- Kratzel, A.; Todt, D.; V’Kovski, P.; Steiner, S.; Gultom, M.; Thao, T.T.N.; Ebert, N.; Holwerda, M.; Steinmann, J.; Niemeyer, D.; et al. Inactivation of severe acute respiratory syndrome coronavirus 2 by WHO-recommended hand rub formulations and alcohols. Emerg. Infect. Dis. 2020, 26, 1592–1595. [Google Scholar] [CrossRef] [PubMed]
- U.S. Food and Drug Administration. Policy for Temporary Compounding of Certain Alcohol-Based Hand Sanitizer Products During the Public Health Emergency. Available online: https://www.fda.gov/regulatory-information/search-fda-guidance-documents/policy-temporary-compounding-certain-alcohol-based-hand-sanitizer-products-during-public-health (accessed on 27 November 2021).
- Jing, J.L.J.; Pei Yi, T.; Bose, R.J.C.; McCarthy, J.R.; Tharmalingam, N.; Madheswaran, T. Hand sanitizers: A review on formulation aspects, adverse effects, and regulations. Int. J. Environ. Res. Public Health 2020, 17, 3326. [Google Scholar] [CrossRef]
- Song, X.; Vossebein, L.; Zille, A. Efficacy of disinfectant-impregnated wipes used for surface disinfection in hospitals: A review. Antimicrob. Resist. Infect. Control 2019, 8, 139. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- United States Pharmacopeia (USP). Compounding Alcohol-Based Hand Sanitizer during COVID-19 Pandemic. Available online: https://www.usp.org/sites/default/files/usp/document/about/public-policy/usp-covid19-handrub.pdf (accessed on 27 November 2021).
- Kampf, G.; Todt, D.; Pfaender, S.; Steinmann, E. Persistence of coronaviruses on inanimate surfaces and their inactivation with biocidal agents. J. Hosp. Infect. 2020, 104, 246–251. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Siddharta, A.; Pfaender, S.; Vielle, N.J.; Dijkman, R.; Friesland, M.; Becker, B.; Yang, J.; Engelmann, M.; Todt, D.; Windisch, M.P.; et al. Virucidal activity of World Health Organization—Recommended formulations against enveloped viruses, including zika, ebola, and emerging coronaviruses. J. Infect. Dis. 2017, 215, 902–906. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Kampf, G. Efficacy of ethanol against viruses in hand disinfection. J. Hosp. Infect. 2018, 98, 331–338. [Google Scholar] [CrossRef] [PubMed]
- Leslie, R.A.; Zhou, S.S.; Macinga, D.R. Inactivation of SARS-CoV-2 by commercially available alcohol-based hand sanitizers. Am. J. Infect. Control. 2021, 49, 401–402. [Google Scholar] [CrossRef] [PubMed]
- Van Doremalen, N.; Bushmaker, T.; Munster, V.J. Stability of Middle East respiratory syndrome coronavirus (MERS-CoV) under different environmental conditions. Eurosurveillance 2013, 18, 20590. [Google Scholar] [CrossRef] [Green Version]
- Duan, S.M.; Zhao, X.S.; Wen, R.F.; Huang, J.J.; Pi, G.H.; Zhang, S.X.; Han, J.; Bi, S.L.; Ruan, L.; Dong, X.P.; et al. Stability of SARS coronavirus in human specimens and environment and its sensitivity to heating and UV irradiation. Biomed. Environ. Sci. 2003, 16, 246–255. [Google Scholar]
- Rabenau, H.F.; Cinatl, J.; Morgenstern, B.; Bauer, G.; Preiser, W.; Doerr, H.W. Stability and inactivation of SARS coronavirus. Med. Microbiol. Immunol. 2005, 194, 1–6. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Chan, K.H.; Peiris, J.S.; Lam, S.Y.; Poon, L.L.; Yuen, K.Y.; Seto, W.H. The Effects of temperature and relative humidity on the viability of the SARS coronavirus. Adv. Virol. 2011, 2011, 734690. [Google Scholar] [CrossRef] [PubMed]
- Rabenau, H.F.; Kampf, G.; Cinatl, J.; Doerr, H.W. Efficacy of various disinfectants against SARS coronavirus. J. Hosp. Infect. 2005, 61, 107–111. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Lai, M.Y.; Cheng, P.K.; Lim, W.W. Survival of severe acute respiratory syndrome coronavirus. Clin. Infect. Dis. 2005, 41, e67–e71. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Centers for Disease Control and Prevention (CDC). Guideline for Disinfection and Sterilization in Healthcare Facilities. 2008. Available online: https://www.cdc.gov/infectioncontrol/guidelines/disinfection/index.html (accessed on 27 November 2021).
- Price, P.B. Reevaluation of ethyl alcohol as a germicide. Arch. Surg. 1950, 60, 492–502. [Google Scholar] [CrossRef] [PubMed]
- Ingram, L.O. Adaptation of membrane lipids to alcohols. J. Bacteriol. 1976, 125, 670–678. [Google Scholar] [CrossRef] [Green Version]
- Wanderlingh, U.; D’Angelo, G.; Nibali, V.C.; Crupi, C.; Rifici, S.; Corsaro, C.; Sabatino, G. Interaction of alcohol with phospholipid membrane: NMR and XRD investigations on DPPC–hexanol system. Spectroscopy 2010, 24, 375–380. [Google Scholar] [CrossRef]
- Das, S.; Meinel, M.K.; Wu, Z.; Muller-Plathe, F. The role of the envelope protein in the stability of a coronavirus model membrane against an ethanolic disinfectant. J. Chem. Phys. 2021, 154, 245101. [Google Scholar] [CrossRef] [PubMed]
- Martin-Gonzalez, N.; Vieira Goncalves, L.; Condezo, G.N.; San Martin, C.; Rubiano, M.; Fallis, I.; Rubino, J.R.; Ijaz, M.K.; Maillard, J.Y.; De Pablo, P.J. Virucidal action mechanism of alcohol and divalent cations against human adenovirus. Front. Mol. Biosci. 2020, 7, 570914. [Google Scholar] [CrossRef] [PubMed]
- Sato, S.; Matsumoto, N.; Hisaie, K.; Uematsu, S. Alcohol abrogates human norovirus infectivity in a pH-dependent manner. Sci. Rep. 2020, 10, 15878. [Google Scholar] [CrossRef] [PubMed]
- Lin, Q.; Lim, J.Y.; Xue, K.; Yew, P.Y.M.; Owh, C.; Chee, P.L.; Loh, X.J. Sanitizing agents for virus inactivation and disinfection. VIEW 2020, 1, e16. [Google Scholar] [CrossRef] [PubMed]
- Rabenau, H.F.; Rapp, I.; Steinmann, J. Can vaccinia virus be replaced by MVA virus for testing virucidal activity of chemical disinfectants? BMC Infect. Dis. 2010, 10, 185. [Google Scholar] [CrossRef] [Green Version]
- Golin, A.P.; Choi, D.; Ghahary, A. Hand sanitizers: A review of ingredients, mechanisms of action, modes of delivery, and efficacy against coronaviruses. Am. J. Infect. Control. 2020, 48, 1062–1067. [Google Scholar] [CrossRef] [PubMed]
- Holford, N.H. Clinical pharmacokinetics of ethanol. Clin. Pharmacokinet. 1987, 13, 273–292. [Google Scholar] [CrossRef]
- Martinez, T.T.; Jaeger, R.W.; de Castro, F.J.; Thompson, M.W.; Hamilton, M.F. A comparison of the absorption and metabolism of isopropyl alcohol by oral, dermal and inhalation routes. Vet. Hum. Toxicol. 1986, 28, 233–236. [Google Scholar] [PubMed]
- MacLean, R.R.; Valentine, G.W.; Jatlow, P.I.; Sofuoglu, M. Inhalation of alcohol vapor: Measurement and implications. Alcohol Clin. Exp. Res. 2017, 41, 238–250. [Google Scholar] [CrossRef] [PubMed]
- Cederbaum, A.I. Alcohol metabolism. Clin. Liver Dis. 2012, 16, 667–685. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Heier, C.; Xie, H.; Zimmermann, R. Nonoxidative ethanol metabolism in humans-from biomarkers to bioactive lipids. IUBMB Life 2016, 68, 916–923. [Google Scholar] [CrossRef]
- Santos, C.; Kieszak, S.; Wang, A.; Law, R.; Schier, J.; Wolkin, A. Reported adverse health effects in children from ingestion of alcohol-based hand sanitizers—United States, 2011–2014. MMWR Morb. Mortal. Wkly. Rep. 2017, 66, 223–226. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Jones, A.W. Alcohol, its absorption, distribution, metabolism, and excretion in the body and pharmacokinetic calculations. WIREs Forensic Sci. 2019, 1, e1340. [Google Scholar] [CrossRef]
- Lachenmeier, D.W. Safety evaluation of topical applications of ethanol on the skin and inside the oral cavity. J. Occup. Med. Toxicol. 2008, 3, 26. [Google Scholar] [CrossRef] [Green Version]
- Siegel, I.A.; Izutsu, K.T.; Burkhart, J. Transfer of alcohols and ureas across the oral mucosa measured using streaming potentials and radioisotopes. J. Pharm. Sci. 1976, 65, 129–131. [Google Scholar] [CrossRef]
- Gaudet, M.P.; Fraser, G.L. Isopropanol ingestion: Case report with pharmacokinetic analysis. Am. J. Emerg. Med. 1989, 7, 297–299. [Google Scholar] [CrossRef]
- Miller, M.A.; Rosin, A.; Levsky, M.E.; Patel, M.M.; Gregory, T.J.; Crystal, C.S. Does the clinical use of ethanol-based hand sanitizer elevate blood alcohol levels? A prospective study. Am. J. Emerg. Med. 2006, 24, 815–817. [Google Scholar] [CrossRef] [PubMed]
- Turner, P.; Saeed, B.; Kelsey, M.C. Dermal absorption of isopropyl alcohol from a commercial hand rub: Implications for its use in hand decontamination. J. Hosp. Infect. 2004, 56, 287–290. [Google Scholar] [CrossRef]
- Peavy, H.H.; Summer, W.R.; Gurtner, G. The effects of acute ethanol ingestion on pulmonary diffusing capacity. Chest 1980, 77, 488–492. [Google Scholar] [CrossRef] [PubMed]
- Luisada, A.A.; Goldmann, M.A.; Weyl, R. Alcohol vapor by inhalation in the treatment of acute pulmonary edema. Circulation 1952, 5, 363–369. [Google Scholar] [CrossRef] [Green Version]
- Mehta, A.J.; Guidot, D.M. Alcohol and the lung. Alcohol Res. 2017, 38, 243–254. [Google Scholar] [PubMed]
- Ahmed-Lecheheb, D.; Cunat, L.; Hartemann, P.; Hautemaniere, A. Dermal and pulmonary absorption of ethanol from alcohol-based hand rub. J. Hosp. Infect. 2012, 81, 31–35. [Google Scholar] [CrossRef] [PubMed]
- Brewer, C.; Streel, E. Is alcohol in hand sanitizers absorbed through the skin or lungs? Implications for disulfiram treatment. Alcohol Alcohol. 2020, 55, 354–356. [Google Scholar] [CrossRef] [PubMed]
- Ghosh, A.; Mahintamani, T.; Balhara, Y.P.S.; Roub, F.E.; Basu, D.; Bn, S.; Mattoo, S.K.; Mishra, E.; Sharma, B. Disulfiram ethanol reaction with alcohol-based hand sanitizer: An exploratory study. Alcohol Alcohol. 2021, 56, 42–46. [Google Scholar] [CrossRef]
- Mahmood, A.; Eqan, M.; Pervez, S.; Alghamdi, H.A.; Tabinda, A.B.; Yasar, A.; Brindhadevi, K.; Pugazhendhi, A. COVID-19 and frequent use of hand sanitizers; human health and environmental hazards by exposure pathways. Sci. Total Environ. 2020, 742, 140561. [Google Scholar] [CrossRef]
- Trummel, J.; Ford, M.; Austin, P. Ingestion of an unknown alcohol. Ann. Emerg. Med. 1996, 27, 368–374. [Google Scholar] [CrossRef]
- Vonghia, L.; Leggio, L.; Ferrulli, A.; Bertini, M.; Gasbarrini, G.; Addolorato, G. Acute alcohol intoxication. Eur. J. Intern. Med. 2008, 19, 561–567. [Google Scholar] [CrossRef]
- Zaman, F.; Pervez, A.; Abreo, K. Isopropyl alcohol intoxication: A diagnostic challenge. Am. J. Kidney Dis. 2002, 40, E12. [Google Scholar] [CrossRef]
- Alves, S.M.; Arendse, A.J.; Kannenberg, S.M.H. COVID-19 collateral damage: Alcohol rub dermatitis as an emerging problem. S. Afr. Med. J. 2020, 110, 13135. [Google Scholar] [CrossRef]
- Emami, A.; Javanmardi, F.; Keshavarzi, A.; Pirbonyeh, N. Hidden threat lurking behind the alcohol sanitizers in COVID-19 outbreak. Dermatol. Ther. 2020, 33, e13627. [Google Scholar] [CrossRef] [PubMed]
- Winnefeld, M.; Richard, M.A.; Drancourt, M.; Grob, J.J. Skin tolerance and effectiveness of two hand decontamination procedures in everyday hospital use. Br. J. Dermatol. 2000, 143, 546–550. [Google Scholar] [CrossRef] [PubMed]
- Pourmand, A.; Ghassemi, M.; Frasure, S.E.; Kreisman, A.; Shesser, R. Hand sanitizer intoxication in the emergency department. Cureus 2021, 13, e17906. [Google Scholar] [CrossRef]
- Hohl, D.H.; Coltro, P.S.; Silva, G.M.A.; Silveira, V.G.; Farina, J.A.J. Covid-19 quarantine has increased the incidence of ethyl alcohol burns. Burns 2021, 47, 1212. [Google Scholar] [CrossRef]
- Yip, L.; Bixler, D.; Brooks, D.E.; Clarke, K.R.; Datta, S.D.; Dudley, S., Jr.; Komatsu, K.K.; Lind, J.N.; Mayette, A.; Melgar, M.; et al. Serious adverse health events, including death, associated with ingesting alcohol-based hand sanitizers containing methanol—Arizona and New Mexico, May–June 2020. MMWR Morb. Mortal. Wkly. Rep. 2020, 69, 1070–1073. [Google Scholar] [CrossRef] [PubMed]
- McCulley, L.; Cheng, C.; Mentari, E.; Diak, I.L.; Michele, T. Alcohol-based hand sanitizer exposures and effects on young children in the U.S. during the COVID-19 pandemic. Clin. Toxicol. 2021, 59, 355–356. [Google Scholar] [CrossRef]
- Dev Kumar, G.; Mishra, A.; Dunn, L.; Townsend, A.; Oguadinma, I.C.; Bright, K.R.; Gerba, C.P. Biocides and novel antimicrobial agents for the mitigation of coronaviruses. Front. Microbiol. 2020, 11, 1351. [Google Scholar] [CrossRef]
- Lingayya, H.; Aayushi, H.; Alisha, M.; Jacqueline, A.; Ryna, S.S.; Sriraksha, B.K. Biocides for textiles against SARS-CoV 2. J. Textile Sci. Eng 2020, 10, 7. [Google Scholar] [CrossRef]
- Moon, J.M.; Chun, B.J.; Min, Y.I. Hemorrhagic gastritis and gas emboli after ingesting 3% hydrogen peroxide. J. Emerg. Med. 2006, 30, 403–406. [Google Scholar] [CrossRef] [PubMed]
- Yari, S.; Moshammer, H.; Asadi, A.F.; Mosavi Jarrahi, A. Side effects of using disinfectants to fight covid-19. Asian Pac. J. Environ. Cancer 2020, 3, 9–13. [Google Scholar] [CrossRef]
- Kalidoss, V.K.; Bakshi, S.S. Has the use of hand sanitiser substituted hand hygiene in the current COVID-19 pandemic? A perilous path. J. R. Coll. Physicians Edinb. 2020, 50, 343–350. [Google Scholar] [CrossRef]
- Okazawa, H.; Aihara, M.; Nagatani, T.; Nakajima, H. Allergic contact dermatitis due to ethyl alcohol. Contact Dermat. 1998, 38, 233. [Google Scholar] [CrossRef] [PubMed]
- Widmer, A.F. Replace hand washing with use of a waterless alcohol hand rub? Clin. Infect. Dis. 2000, 31, 136–143. [Google Scholar] [CrossRef]
- Hadaway, A. Handwashing: Clean hands save lives. J. Consum. Health Internet 2020, 24, 43–49. [Google Scholar] [CrossRef]
- Ijaz, M.K.; Nims, R.W.; de Szalay, S.; Rubino, J.R. Soap, water, and severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2): An ancient handwashing strategy for preventing dissemination of a novel virus. PeerJ 2021, 9, e12041. [Google Scholar] [CrossRef] [PubMed]
- Matuschek, C.; Moll, F.; Fangerau, H.; Fischer, J.C.; Zanker, K.; van Griensven, M.; Schneider, M.; Kindgen-Milles, D.; Knoefel, W.T.; Lichtenberg, A.; et al. Face masks: Benefits and risks during the COVID-19 crisis. Eur. J. Med. Res. 2020, 25, 32. [Google Scholar] [CrossRef] [PubMed]
- Sommerstein, R.; Fux, C.A.; Vuichard-Gysin, D.; Abbas, M.; Marschall, J.; Balmelli, C.; Troillet, N.; Harbarth, S.; Schlegel, M.; Widmer, A.; et al. Risk of SARS-CoV-2 transmission by aerosols, the rational use of masks, and protection of healthcare workers from COVID-19. Antimicrob. Resist. Infect. Control 2020, 9, 100. [Google Scholar] [CrossRef] [PubMed]
- Bordea, I.R.; Xhajanka, E.; Candrea, S.; Bran, S.; Onisor, F.; Inchingolo, A.D.; Malcangi, G.; Pham, V.H.; Inchingolo, A.M.; Scarano, A.; et al. Coronavirus (SARS-CoV-2) pandemic: Future challenges for dental practitioners. Microorganisms 2020, 8, 1704. [Google Scholar] [CrossRef]
- Duarte, P.; Santana, V.T. Disinfection measures and control of SARS-COV-2 transmission. Glob. Biosecur. 2020, 2, 1. [Google Scholar] [CrossRef]
- Wilhelm, K.P. Prevention of surfactant-induced irritant contact dermatitis. Curr. Probl. Dermatol. 1996, 25, 78–85. [Google Scholar] [CrossRef] [PubMed]
- Nomura, T.; Nazmul, T.; Yoshimoto, R.; Higashiura, A.; Oda, K.; Sakaguchi, T. Ethanol susceptibility of SARS-CoV-2 and other enveloped viruses. Biocontrol Sci. 2021, 26, 177–180. [Google Scholar] [CrossRef] [PubMed]
- Saha, T.; Khadka, P.; Das, S.C. Alcohol-based hand sanitizer—Composition, proper use and precautions. Germs 2021, 11, 408–417. [Google Scholar] [CrossRef] [PubMed]

| Type | Surface | Survival Time | Virucide | Exposure Duration | Decrease in Infectivity (log10) | Reference |
|---|---|---|---|---|---|---|
| SARS-COV-2 | NR | NR | 80% ethanol | 30 s | ≥3.8 | [37] |
| NR | NR | 75% isopropanol | 30 s | ≥3.8 | [37] | |
| MERS-COV | Steel | 48 h (20 °C) 8–24 h (30 °C) | 80% ethanol | 30 s | >4.0 | [43,46] |
| Plastic | 48 h (20 °C) 8–24 h (30 °C) | 75% isopropanol | 30 s | ≥4.0 | [43] | |
| SARS-COV | Glass | 4 d (RT) | 80% ethanol | 30 s | ≥4.3 | [47,48] |
| Plastic | ≤5 d (22–25 °C) | 85% ethanol | 30 s | ≥5.5 | [49,50] | |
| Wood | 4 d (RT) | 95% ethanol | 30 s | ≥5.5 | [47,50] | |
| Paper | 4–5 d (RT) | 70% isopropanol | 30 s | ≥3.3 | [47,48] | |
| Gown | 2 d (RT) | 75% isopropanol | 30 s | ≥4.0 | [43,51] | |
| Metal | 5 d (RT) | 100% isopropanol | 30 s | ≥3.3 | [47,48] | |
| NR | NR | 45% isopropanol and 30% 1-propanol | 30 s | ≥2.8 | [48] |
| Agent | Mechanism of Action | Benefits | Drawbacks | Adverse Effects | Reference |
|---|---|---|---|---|---|
| Ethanol (>60%) | Denaturation of proteins | Recommended by U.S. FDA against SARS-CoV-2; economical and easy to handle | Disagreeable odor, dryness of skin, possibility of unwanted toxicity in children | Skin: Itching, allergy, dermatitis Liver: Hypocalcemia, hypokalemia, hypomagnesemia, myoglobinuria Others: Vomiting, drowsiness, respiratory arrest, keto acidosis, arrhythmia, cardiac arrest | [42,80,91] |
| Isopropanol (>70%) | Denaturation of proteins | Recommended by U.S. FDA against SARS-CoV-2; economical and easy to handle | Unpleasant odor, dryness of skin, possibility of unwanted toxicity in children | Skin: Rash, itching, irritation, allergy Others: Myoglobinuria, gastritis, respiratory depression | [42,80,91] |
| Quaternary ammonium compounds | Enzymatic inactivation; Degradation of cellular proteins | Minimal human toxicity, better tolerability, no bad odor | Less effective in low pH and in the presence of organic substances | Mild irritation | [91,92] |
| Hydrogen peroxide | Free-radical induced oxidation of cellular components | Relatively less toxic, inexpensive, easy to use | Corrosive | Mild irritation in skin and mucous membrane, vomiting, air embolism | [80,91,93] |
| Iodine compounds | Degradation of cellular proteins, fatty acids, and nucleotides | Non-corrosive, ease of use | Unpleasant odor, staining, irritation | Rash, itching, local swelling | [91,92] |
| Chlorine compounds | Halogenation/oxidation of cellular proteins | Effective in low concentration, low-cost | Corrosive, formation of toxic by-products, irritation | Nausea, coughing, shortness of breath, irritation of mucous membrane, stimulation of the upper airways | [91,94] |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Basak, D.; Deb, S. Sensitivity of SARS-CoV-2 towards Alcohols: Potential for Alcohol-Related Toxicity in Humans. Life 2021, 11, 1334. https://doi.org/10.3390/life11121334
Basak D, Deb S. Sensitivity of SARS-CoV-2 towards Alcohols: Potential for Alcohol-Related Toxicity in Humans. Life. 2021; 11(12):1334. https://doi.org/10.3390/life11121334
Chicago/Turabian StyleBasak, Debasish, and Subrata Deb. 2021. "Sensitivity of SARS-CoV-2 towards Alcohols: Potential for Alcohol-Related Toxicity in Humans" Life 11, no. 12: 1334. https://doi.org/10.3390/life11121334
APA StyleBasak, D., & Deb, S. (2021). Sensitivity of SARS-CoV-2 towards Alcohols: Potential for Alcohol-Related Toxicity in Humans. Life, 11(12), 1334. https://doi.org/10.3390/life11121334







