Do Maternal Stress and Depressive Symptoms in Perinatal Period Predict the Lactation Mastitis Occurrence? A Retrospective Longitudinal Study in Greek Women
Abstract
:1. Introduction
2. Materials and Methods
2.1. Study Population
2.2. Data Collection
2.3. Screening Tools
2.4. Ethical Issues
2.5. Analysis
3. Results
3.1. Study Characteristics
3.2. Mental Health Characteristics
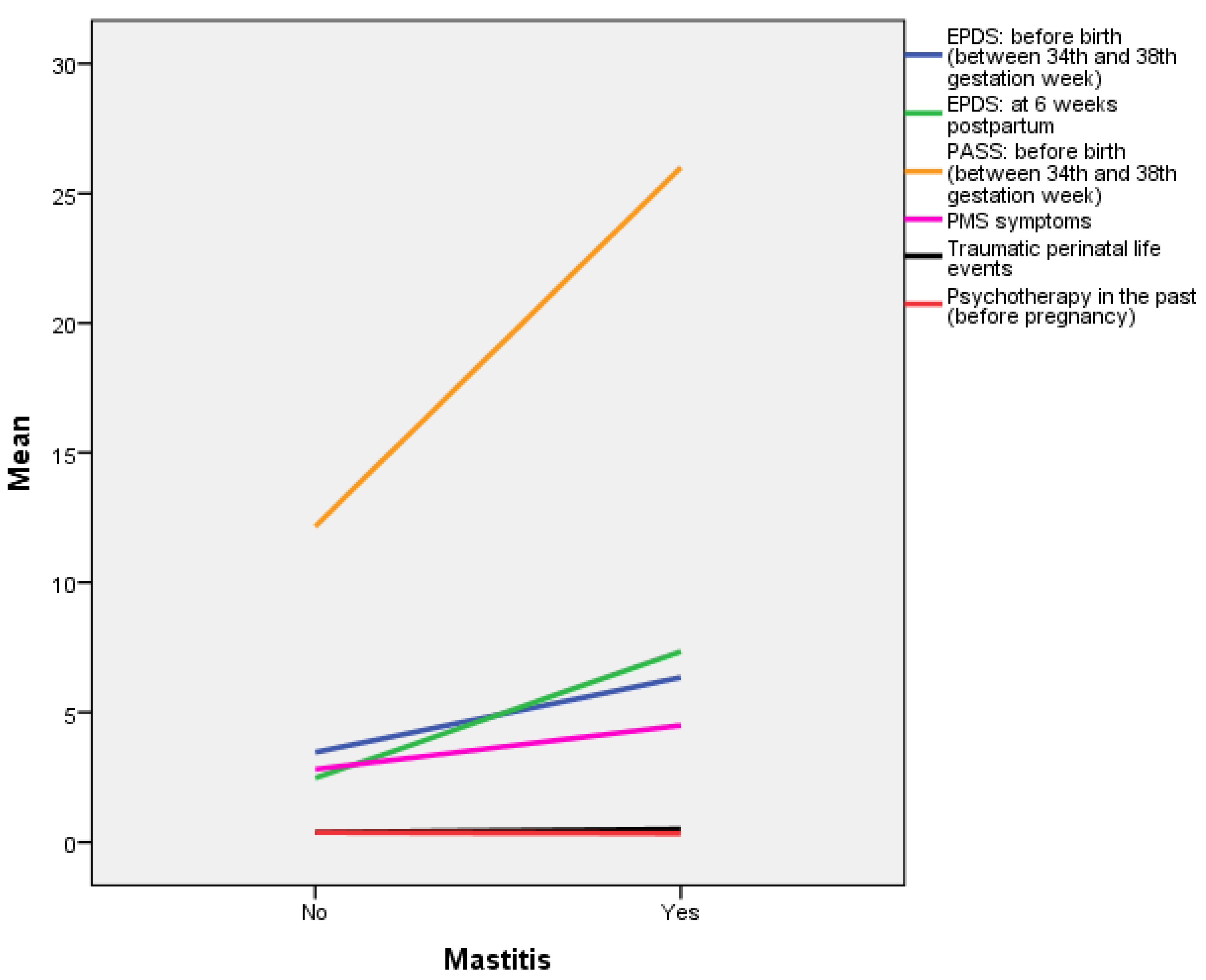
3.3. Multivariate Binary Logistic Regression Analyses
4. Discussion
4.1. The Psycho-Emotional Factors which Predict the Occurrence of Lactation Mastitis
4.2. The Relationship between Perinatal Mental Health Disorders and Lactation Mastitis
4.3. The Benefits of Early Detection for Perinatal Mental Health Disorders
4.4. Limitations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Binns, C.; Lee, M.; Low, W.Y. The Long-Term Public Health Benefits of Breastfeeding. Asia Pac. J. Public Health 2016, 28, 7–14. [Google Scholar] [CrossRef] [Green Version]
- Del Ciampo, L.A.; Del Ciampo, I.R.L. Breastfeeding and the Benefits of Lactation for Women’s Health. Rev. Bras. Ginecol. Obstet. 2018, 40, 354–359. [Google Scholar] [CrossRef] [Green Version]
- Mosca, F.; Giannì, M.L. Human milk: Composition and health benefits. Pediatr. Med. Chir. 2017, 28, 155. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Lamontagne, C.; Hamelin, A.M.; St-Pierre, M. The breastfeeding experience of women with major difficulties who use the services of a breastfeeding clinic: A descriptive study. Int. Breastfeed J. 2008, 3, 17. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Palmer, L.; Carlsson, G.; Mollberg, M.; Nystrom, M. Severe breastfeeding difficulties: Existential lostness as a mother-Women’s lived experiences of initiating breastfeeding under severe difficulties. Int. J. Qual. Stud. Health Well Being 2012, 7, 10846. [Google Scholar] [CrossRef] [PubMed]
- Buck, M.L.; Amir, L.H.; Cullinane, M.; Donath, S.M. The CASTLE Study Team. Nipple pain, damage, and vasospasm in the first 8 weeks postpartum. Breastfeed Med. 2014, 9, 56–62. [Google Scholar] [CrossRef] [Green Version]
- Henshaw, E.J.; Fried, R.; Siskind, E.; Newhouse, L.; Cooper, M. Breastfeeding self-efficacy, mood, and breastfeeding outcomes among primiparous women. J. Hum. Lact. 2015, 31, 511–518. [Google Scholar] [CrossRef]
- Woolhouse, H.; Perlen, S.; Gartland, D.; Brown, S.J. Physical health and recovery in the first 18 months postpartum: Does cesarean section reduce long-term morbidity? Birth 2012, 39, 221–229. [Google Scholar] [CrossRef]
- Marín, M.; Arroyo, R.; Espinosa-Martos, I.; Fernández, L.; Rodríguez, J.M. Identification of emerging human mastitis pathogens by MALDI-TOF and assessment of their antibiotic resistance patterns. Front. Microbiol. 2017, 8, 1258. [Google Scholar] [CrossRef] [Green Version]
- Fetherston, C. Mastitis in lactating women: Physiology or pathology? Breastfeed Rev. 2001, 9, 5–12. [Google Scholar]
- Deng, Y.; Huang, Y.; Ning, P.; Ma, S.-G.; He, P.-Y.; Wang, Y. Maternal Risk Factors for Lactation Mastitis: A Meta-analysis. West. J. Nurs. Res. 2020, 22, 193945920967674. [Google Scholar] [CrossRef]
- Foxman, B.; D’Arcy, H.; Gillespie, B.; Bobo, J.K.; Schwartz, K. Lactation mastitis: Occurrence and medical management among 946 breastfeeding women in the United States. Am. J. Epidemiol. 2002, 155, 103–114. [Google Scholar] [CrossRef]
- Amir, L.H.; Forster, D.A.; Lumley, J.; McLachlan, H. A descriptive study of mastitis in Australian breastfeeding women: Incidence and determinants. BMC Public Health 2007, 7, 62. [Google Scholar] [CrossRef] [Green Version]
- Dixon, J.M.; Khan, L.R. Treatment of breast infection. BMJ 2011, 342, d396. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- World Health Organization. Mastitis: Causes and Management. Available online: http://whqlibdoc.who.int/hq/2000/WHO_FCH_CAH_00.13.pdf (accessed on 20 November 2020).
- Mangesi, L.; Dowswell, T. Treatments for breast engorgement during lactation. Cochrane Database Syst. Rev. 2010, 9, CD006946. [Google Scholar] [CrossRef]
- Labbok, M. Exploration of guilt among mothers who do not breastfeed: The physician’s role. J. Hum. Lact. 2008, 24, 80–84. [Google Scholar] [CrossRef] [PubMed]
- Cooklin, A.R.; Amir, L.H.; Nguyen, C.D.; Buck, M.L.; Cullinane, M.; Fisher, J.R.W.; Donath, S.M. Physical health, breastfeeding problems and maternal mood in the early postpartum: A prospective cohort study. Arch. Womens Ment. Health 2018, 21, 365–374. [Google Scholar] [CrossRef] [PubMed]
- Brown, A.; Rance, J.; Bennett, P. Understanding the relationship between breastfeeding and postnatal depression: The role of pain and physical difficulties. J. Adv. Nurs. 2016, 72, 273–282. [Google Scholar] [CrossRef] [Green Version]
- Howard, L.M.; Khalifeh, H. Perinatal mental health: A review of progress and challenges. World Psychiatry 2020, 19, 313–327. [Google Scholar] [CrossRef] [PubMed]
- Hadi, F.; Shirazi, E.; Soraya, S. Perinatal mental health: A public health concern. Int. J. Fertil. Steril. 2019, 13, 86. [Google Scholar] [CrossRef]
- Khalifeh, H.; Brauer, R.; Toulmin, H.; Howard, L.M. Perinatal mental health: What every neonatologist should know. Early Hum. Dev. 2015, 91, 649–653. [Google Scholar] [CrossRef]
- Zarshenas, M.; Zhao, Y.; Poorarian, S.; Binns, C.W.; Scott, J.A. Incidence and Risk Factors of Mastitis in Shiraz, Iran: Results of a Cohort Study. Breastfeed Med. 2017, 12, 290–296. [Google Scholar] [CrossRef] [PubMed]
- Hahn-Holbrook, J.; Haselton, M.G.; Dunkel Schetter, C.; Glynn, L.M. Does breastfeeding offer protection against maternal depressive symptomatology?: A prospective study from pregnancy to 2 years after birth. Arch. Womens Ment. Health 2013, 16, 411–422. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Ystrom, E. Breastfeeding cessation and symptoms of anxiety and depression: A longitudinal cohort study. BMC Pregnancy Childbirth 2012, 12, 36. [Google Scholar] [CrossRef] [Green Version]
- Dias, C.C.; Figueiredo, B. Breastfeeding and depression: A systematic review of the literature. J. Affect. Disord. 2015, 171, 142–154. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Krishnadas, R.; Cavanagh, J. Depression: An inflammatory illness? J. Neurol. Neurosurg. Psychiatry 2012, 83, 495–502. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Raison, C.L.; Capuron, L.; Miller, A.H. Cytokines sing the blues: Inflammation and the pathogenesis of depression. Trends Immunol. 2006, 27, 24–31. [Google Scholar] [CrossRef] [Green Version]
- Zorrilla, E.P.; Luborsky, L.; McKay, J.R.; Rosenthal, R.; Houldin, A.; Tax, A.; Schmidt, K. The relationship of depression and stressors to immunological assays: A meta-analytic review. Brain. Behav. Immun. 2001, 15, 199–226. [Google Scholar] [CrossRef] [Green Version]
- Gaudet, C.; Wen, S.W.; Walker, M.C. Chronic perinatal pain as a risk factor for postpartum depression symptoms in Canadian women. Can. J. Public Health 2013, 104, 375–387. [Google Scholar] [CrossRef]
- Woolhouse, H.; Gartland, D.; Perlen, S.; Donath, S.; Brown, S.J. Physical health after childbirth and maternal depression in the first 12 months post partum: Results of an Australian nulliparous pregnancy cohort study. Midwifery 2014, 30, 378–384. [Google Scholar] [CrossRef] [PubMed]
- Cox, J.L.; Holden, J.M.; Sagovsky, R. Detection of postnatal depression: Development of the 10-item Edinburgh depression scale. Br. J. Psychiatry 1987, 150, 782–788. [Google Scholar] [CrossRef] [Green Version]
- Leonardou, A.A.; Zervas, Y.M.; Papageorgiou, C.C.; Marks, M.N.; Tsartsara, E.C.; Antsaklis, A.; Christodoulou, G.N.; Soldatos, C.R. Validation of the Edinburgh Postnatal Depression Scale and prevalence of postnatal depression at two months postpartum in a sample of Greek mothers. J. Reprod. Infant. Psychol. 2009, 27, 28–39. [Google Scholar] [CrossRef]
- Somerville, S.; Dedman, K.; Hagan, R.; Oxnam, E.; Wettinger, M.; Byrne, S.; Coo, S.; Doherty, D.; Page, A.C. The Perinatal Anxiety Screening Scale: Development and preliminary validation. Arch. Womens Ment. Health 2014, 17, 443–454. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. Indicators for Assessing Infant and Young Child Feeding Practices, Part 1: Definitions. In Proceedings of the Conclusions of a Consensus Meeting, Washington, DC, USA, 6–8 November 2007; WHO: Geneva, Switzerland, 2008. Available online: http://www.ifpri.org/sites/default/files/publications/childfeeding.pdf (accessed on 20 November 2020).
- Prince, M.; Patel, V.; Saxena, S.; Maj, M.; Maselko, J.; Phillips, M.R.; Rahman, A. No health without mental health. Lancet 2007, 8, 859–877. [Google Scholar] [CrossRef]
- Woolhouse, H.; James, J.; Gartland, D.; McDonald, E.; Brown, S.J. Maternal depressive symptoms at three months postpartum and breastfeeding rates at six months postpartum: Implications for primary care in a prospective cohort study of primiparous women in Australia. Women Birth 2016, 29, 381–387. [Google Scholar] [CrossRef]
- Chaudron, L.H.; Klein, M.H.; Remington, P.; Palta, M.; Allen, C.; Essex, M.J. Predictors, prodromes and incidence of postpartum depression. J. Psychosom. Obstet. Gynaecol. 2001, 22, 103–112. [Google Scholar] [CrossRef]
- Edhborg, M.; Friberg, M.; Lundh, W.; Widstrom, A. “Struggling with life”: Narratives from women with signs of postpartum depression. Scand. J. Public Health 2005, 33, 261–267. [Google Scholar] [CrossRef]
- Lonstein, J.S. Regulation of anxiety during the postpartum period. Front. Neuroendocrinol. 2007, 28, 115–141. [Google Scholar] [CrossRef] [PubMed]
- Stuebe, A.M.; Grewen, K.; Pedersen, C.A.; Propper, C.; Meltzer Brody, S. Failed lactation and perinatal depression: Common problems with shared neuroendocrine mechanisms? J. Womens Health 2012, 21, 264–272. [Google Scholar] [CrossRef] [PubMed]
- Yu, Z.; Sun, S.; Zhang, Y. High-Risk Factors for Suppurative Mastitis in Lactating Women. Med. Sci. Monit. 2018, 19, 4192–4197. [Google Scholar] [CrossRef]
- Slomian, J.; Honvo, G.; Emonts, E.; Reginster, J.Y.; Bruyère, O. Consequences of maternal postpartum depression: A systematic review of maternal and infant outcomes. Womens Health 2019, 15, 1745506519844044. [Google Scholar] [CrossRef] [Green Version]
- Dennis, C.-L.; McQueen, K. The relationship between infant-feeding outcomes and postpartum depression: A qualitative systematic review. Pediatrics 2009, 123, e736–e751. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Schiller, C.E.; Meltzer-Brody, S.; Rubinow, D.R. The role of reproductive hormones in postpartum depression. CNS Spectr. 2015, 20, 48–59. [Google Scholar] [CrossRef] [PubMed]
- Leonard, B.E. The concept of depression as a dysfunction of the immune system. Curr. Immunol. Rev. 2010, 6, 205–212. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Kiecolt-Glaser, J.K.; Glaser, R. Depression and immune function: Central pathways to morbidity and mortality. J. Psychosom. Res. 2002, 53, 873–876. [Google Scholar] [CrossRef]
- The Mental Health Context. Mental Health Policy and Service Guidance Package; World Health Organization: Geneva, Switzerland, 2003; ISBN 92-4-154594-1. [Google Scholar]
- Jardri, R.; Pelta, J.; Maron, M.; Thomas, P.; Delion, P.; Codaccioni, X.; Goudemand, M. Predictive validation study of the Edinburgh Postnatal Depression Scale in the first week after delivery and risk analysis for postnatal depression. J. Affect. Disord. 2006, 93, 169–176. [Google Scholar] [CrossRef]
- Galler, J.; Harrison, R.; Ramsey, F.; Chawla, S.; Taylor, J. Postpartum feeding attitudes, maternal depression, and breastfeeding in Barbados. Infant. Behav. Dev. 2006, 29, 189–203. [Google Scholar] [CrossRef]
- Watkins, S.; Meltzer-Brody, S.; Zolnoun, D.; Stuebe, A. Early breastfeeding experiences and postpartum depression. Obstet. Gynecol. 2011, 118, 214–221. [Google Scholar] [CrossRef]
- Letourneau, N.L.; Dennis, C.-L.; Benzies, K.; Duffett-Leger, L.; Stewart, M.; Tryphonopoulos, P.D.; Este, D.; Watson, W. Postpartum Depression is a Family Affair: Addressing the Impact on Mothers, Fathers, and Children. Issues Ment. Health Nurs. 2012, 33, 445–457. [Google Scholar] [CrossRef]
- Dennis, C.-L.; Schottle, N.; Hodnett, E.; McQueen, K. An all-purpose nipple ointment versus lanolin in treating painful damaged nipples in breastfeeding women: A randomized controlled trial. Breastfeed Med. 2012, 7, 473–479. [Google Scholar] [CrossRef]
- Jackson, K.T.; Mantler, T.; O’Keefe-McCarthy, S. Women’s Experiences of Breastfeeding-Related Pain. MCN Am. J. Matern. Child Nurs. 2019, 44, 66–72. [Google Scholar] [CrossRef] [PubMed]
- Krol, K.M.; Grossmann, T. Psychological effects of breastfeeding on children and mothers. Bundesgesundheitsblatt Gesundh. Gesundheitsschutz 2018, 61, 977–985. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Gentile, S.; Fusco, M.L. Untreated perinatal paternal depression: Effects on offspring. Psychiatry. Res. 2017, 252, 325–332. [Google Scholar] [CrossRef]
- Glover, V.; O’Donnell, K.; O’Connor, T.G.; Ramchandani, P.; Capron, L. Prenatal anxiety and depression, fetal programming and placental function. Psychoneuroendocrinology 2015, 61, 3–4. [Google Scholar] [CrossRef]
- Sanger, C.; Iles, J.E.; Andrew, C.S.; Ranchandani, P.G. Associations between postnatal maternal depression and psychological outcomes in adolescent offspring: A systematic review. Arch. Womens Ment. Health 2015, 18, 147–162. [Google Scholar] [CrossRef]
- Stein, A.; Pearson, R.M.; Goodman, S.H.; Rapa, E.; Rahman, A.; McCallum, M.; Pariante, C.M. Effects of perinatal mental disorders on the fetus and child. Lancet 2014, 384, 1800–1819. [Google Scholar] [CrossRef]
- Raposa, E.; Hammen, C.; Brennan, P.; Najman, J. The long-term effects of maternal depression: Early childhood physical health as a pathway to offspring depression. J. Adolesc. Health 2014, 54, 492–497. [Google Scholar] [CrossRef] [PubMed] [Green Version]

| Demographic Characteristics | N/M | %/SD | Range | |
|---|---|---|---|---|
| Age | 32.9 | 3.9 | 21–41 | |
| Education | ||||
| High School | 110 | 17.7 | ||
| Bachelor’s Degree | 416 | 66.9 | ||
| Master’s/PhD | 96 | 15.4 | ||
| Total | 622 | 100.0 | ||
| Marital Status | ||||
| Married | 524 | 84.2 | ||
| Not Married | 19 | 3.1 | ||
| Single Parent Family | 5 | 0.8 | ||
| Living With a Partner | 74 | 11.9 | ||
| Total | 622 | 100.0 | ||
| Monthly Income | ||||
| 0–500 euros | 158 | 25.4 | ||
| 501–1000 euros | 288 | 46.3 | ||
| >1000 euros | 176 | 28.3 | ||
| Total | 622 | 100.0 | ||
| Perinatal/Health Characteristics | ||||
| Premenstrual Syndrome (PMS) Symptoms | 3.68 | 1.86 | 0–8 | |
| Pregnancy after In Vitro Fertilization (IVF) procedure | ||||
| No | 569 | 91.5 | ||
| Yes | 53 | 8.5 | ||
| Total | 622 | 100.0 | ||
| Smoking Before Pregnancy | ||||
| No | 400 | 64.3 | ||
| Yes | 222 | 35.7 | ||
| Total | 622 | 100.0 | ||
| Smoking During Pregnancy | ||||
| No | 573 | 92.1 | ||
| Yes | 49 | 7.9 | ||
| Total | 622 | 100.0 | ||
| Type of Delivery | ||||
| Vaginal | 312 | 50.2 | ||
| Caesarian Section | 310 | 49.8 | ||
| Total | 622 | 100.0 | ||
| Woman’s Birth Satisfaction | ||||
| Not at all/Little | 66 | 9.6 | ||
| Neither Satisfied nor Dissatisfied | 104 | 15.9 | ||
| Mostly Satisfied | 232 | 35.2 | ||
| Completely Satisfied | 220 | 39.3 | ||
| Total | 622 | 100.0 | ||
| Newborn Weight | ||||
| 1500–2500 | 48 | 7.8 | ||
| 2500–3500 | 421 | 67.8 | ||
| >3500 | 151 | 24.4 | ||
| Total | 622 | 100.0 | ||
| Twins | 14 | 2.3 | ||
| Newborn’s Admission to Neonatal Intensive Care Unit (NICU) | ||||
| No | 529 | 85.0 | ||
| <8 days | 69 | 11.1 | ||
| 8–15 days | 13 | 2.1 | ||
| >15 days | 11 | 1.8 | ||
| Total | 622 | 100.0 | ||
| Breastfeeding Characteristics | ||||
| Newborn Feeding in the Hospital | ||||
| Exclusive Breastfeeding | 444 | 71.4 | ||
| Breastfeeding and Formula | 158 | 25.4 | ||
| Formula | 20 | 3.2 | ||
| Total | 622 | 100.0 | ||
| Newborn Feeding at 1st Month | ||||
| Exclusive Breastfeeding | 472 | 75.9 | ||
| Breastfeeding and Formula | 134 | 21.5 | ||
| Formula | 16 | 2.6 | ||
| Total | 622 | 100.0 | ||
| Any Breastfeeding Duration | 0–30 | |||
| No Breastfeeding | 14 | 2.3 | ||
| ≤6 months | 156 | 25.2 | ||
| 7–24 months | 452 | 72.4 | ||
| Total | 622 | 100.0 | ||
| Exclusive Breastfeeding Duration or Breastfeeding Duration Without any Formula | 0–30 | |||
| No Breastfeeding | 58 | 9.3 | ||
| ≤6 months | 203 | 32.6 | ||
| 7–24 months | 361 | 58.1 | ||
| Total | 622 | 100.0 | ||
| Presence of Mastitis | ||||
| No | 521 | 83.8 | ||
| Yes | 101 | 16.2 | ||
| Total | 622 | 100.0 | ||
| N/M | %/SD | |
|---|---|---|
| Women’s Mental Health Status | ||
| No history of mental health disorders/No risk factors/ Normal Scores on Psychometric Tools | 227 | 36.5 |
| With Risk Factors in Mental Health History | 295 | 47.4 |
| Increased Scores using Psychometric Tools | 100 | 16.1 |
| Total | 622 | 100.0 |
| Symptoms of Mental Health Disorders | ||
| Without | 283 | 45.5 |
| Anxiety Symptoms | 169 | 27.2 |
| Depression Symptoms | 64 | 10.3 |
| Anxiety and Depression | 106 | 17.0 |
| Total | 622 | 100.0 |
| Psychotherapy During Perinatal Period | ||
| No | 549 | 88.4 |
| Yes | 72 | 11.6 |
| Total | 622 | 100.0 |
| Received Psychotropic Medication During Perinatal Period | ||
| No | 617 | 99.2 |
| Yes | 5 | 0.8 |
| Total | 622 | 100.0 |
| Psychotherapy in the Past (Before Pregnancy) | ||
| No | 346 | 55.6 |
| Yes | 276 | 44.4 |
| Total | 622 | 100.0 |
| Presence of Traumatic Life Events in the last year | ||
| No | 492 | 79.1 |
| Yes | 131 | 20.9 |
| Total | 622 | 100.0 |
| B | S.E. | p | Exp(B) | R² | |
|---|---|---|---|---|---|
| EPDS—before Birth (between 34th and 38th gestation week) | 0.114 | 0.046 | 0.014 | 1.120 | 0.044 |
| PASS—before Birth (between 34th and 38th gestation week) | 0.058 | 0.029 | 0.041 | 1.060 | 0.103 |
| EPDS—at 6 Weeks Postpartum | 0.084 | 0.029 | 0.004 | 1.088 | 0.043 |
| PMS Symptoms | 0.132 | 0.059 | 0.025 | 1.141 | 0.014 |
| Traumatic Life Events | 0.940 | 0.418 | 0.025 | 0.391 | 0.024 |
| Psychotherapy in the Past (before pregnancy) | 0.636 | 0.324 | 0.050 | 1.888 | 0.014 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Dagla, M.; Dagla, C.; Mrvoljak-Theodoropoulou, I.; Sotiropoulou, D.; Kavakou, A.-T.; Kontiza, E.; Antoniou, E. Do Maternal Stress and Depressive Symptoms in Perinatal Period Predict the Lactation Mastitis Occurrence? A Retrospective Longitudinal Study in Greek Women. Diagnostics 2021, 11, 1524. https://doi.org/10.3390/diagnostics11091524
Dagla M, Dagla C, Mrvoljak-Theodoropoulou I, Sotiropoulou D, Kavakou A-T, Kontiza E, Antoniou E. Do Maternal Stress and Depressive Symptoms in Perinatal Period Predict the Lactation Mastitis Occurrence? A Retrospective Longitudinal Study in Greek Women. Diagnostics. 2021; 11(9):1524. https://doi.org/10.3390/diagnostics11091524
Chicago/Turabian StyleDagla, Maria, Calliope Dagla, Irina Mrvoljak-Theodoropoulou, Dimitra Sotiropoulou, Aikaterini-Taxiarchoula Kavakou, Eleni Kontiza, and Evangelia Antoniou. 2021. "Do Maternal Stress and Depressive Symptoms in Perinatal Period Predict the Lactation Mastitis Occurrence? A Retrospective Longitudinal Study in Greek Women" Diagnostics 11, no. 9: 1524. https://doi.org/10.3390/diagnostics11091524








