Hybrid Additive Fabrication of a Transparent Liver with Biosimilar Haptic Response for Preoperative Planning
Abstract
:1. Introduction
2. Materials and Methods
2.1. Image Processing and 3D Reconstruction of the Target Anatomy
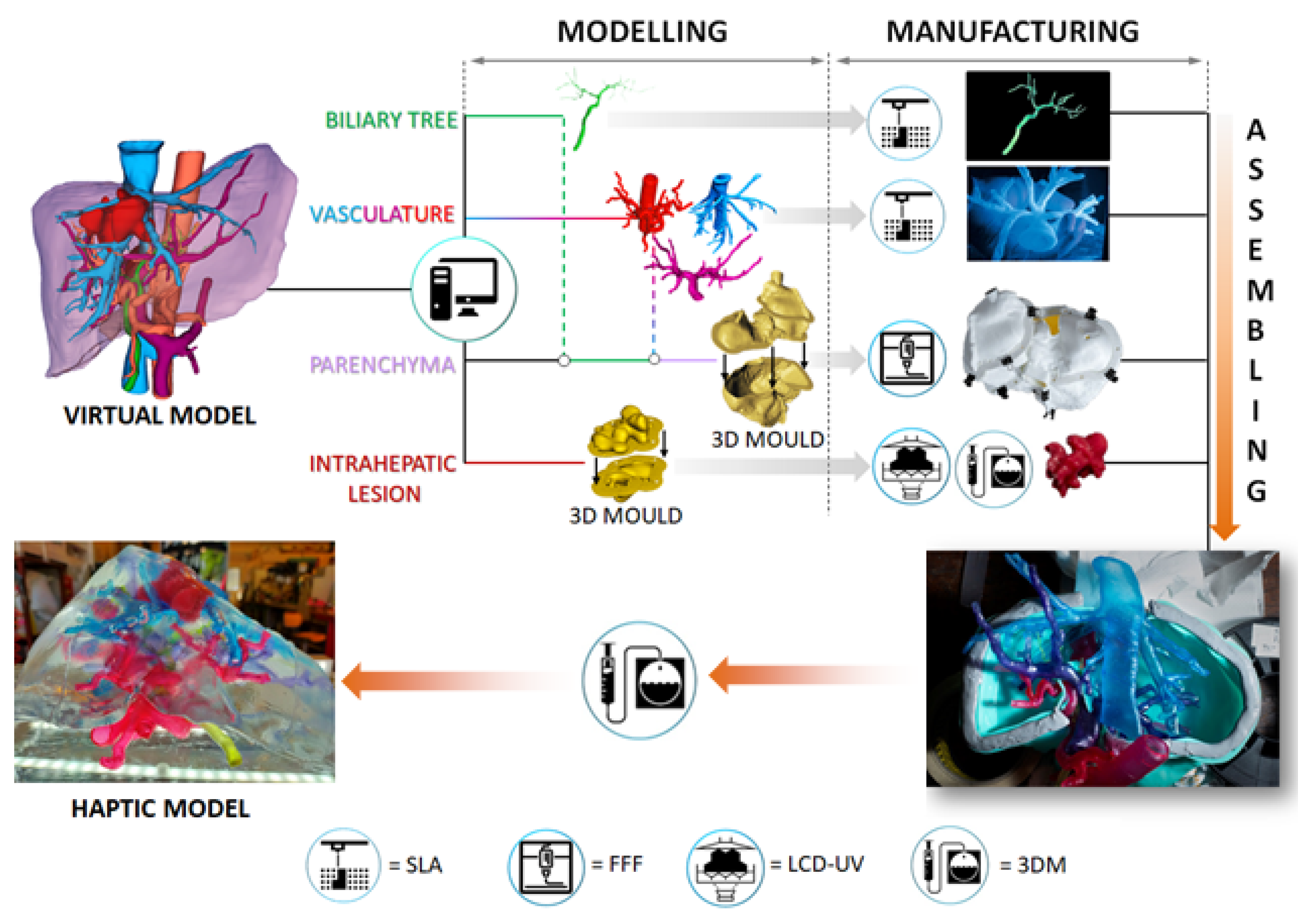
2.2. 3D Haptic Liver Fabrication: Rationale and General Approach
2.3. Phantom Fabrication
2.3.1. Vessels and Biliary Duct 3D Printing
2.3.2. Intrahepatic Lesion Moulding
2.3.3. 3D Assembling and Parenchyma Moulding
2.3.4. Evaluation Methods
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Tejo-Otero, A.; Buj-Corral, I.; Fenollosa-Artés, F. 3D Printing in Medicine for Preoperative Surgical Planning: A Review. Ann. Biomed. Eng. 2020, 48, 536–555. [Google Scholar] [CrossRef] [PubMed]
- Diment, L.E.; Thompson, M.; Bergmann, J.H.M. Clinical efficacy and effectiveness of 3D printing: A systematic review. BMJ Open 2017, 7, e016891. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Garcia, J.; Yang, Z.; Mongrain, R.; Leask, R.L.; Lachapelle, K. 3D printing materials and their use in medical education: A review of current technology and trends for the future. BMJ Simul. Technol. Enhanc. Learn. 2017, 4, 27–40. [Google Scholar] [CrossRef] [PubMed]
- De Montbrun, S.L.; MacRae, H. Simulation in Surgical Education. Clin. Colon Rectal Surg. 2012, 25, 156–165. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Dai, K.-R.; Yan, M.-N.; Zhu, Z.-A.; Sun, Y.-H. Computer-Aided Custom-Made Hemipelvic Prosthesis Used in Extensive Pelvic Lesions. J. Arthroplast. 2007, 22, 981–986. [Google Scholar] [CrossRef]
- Harrysson, O.L.A.; Hosni, Y.A.; Nayfeh, J.F. Custom-designed orthopedic implants evaluated using finite element analysis of patient-specific computed tomography data: Femoral-component case study. BMC Musculoskelet. Disord. 2007, 8, 91. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Jiankang, H.; Dichen, L.; Bingheng, L.; Zhen, W.; Tao, Z. Custom fabrication of composite tibial hemi-knee joint combining CAD/CAE/CAM techniques. Proc. Inst. Mech. Eng. Part H J. Eng. Med. 2006, 220, 823–830. [Google Scholar] [CrossRef]
- Waran, V.; Narayanan, V.; Karuppiah, R.; Pancharatnam, D.; Chandran, H.; Raman, R.; Rahman, Z.A.A.; Owen, S.L.; Aziz, T.Z. Injecting Realism in Surgical Training—Initial Simulation Experience With Custom 3D Models. J. Surg. Educ. 2014, 71, 193–197. [Google Scholar] [CrossRef]
- Dho, Y.-S.; Lee, D.; Ha, T.; Ji, S.Y.; Kim, K.M.; Kang, H.; Kim, M.-S.; Kim, J.W.; Cho, W.-S.; Kim, Y.H.; et al. Clinical application of patient-specific 3D printing brain tumor model production system for neurosurgery. Sci. Rep. 2021, 11, 7005. [Google Scholar] [CrossRef]
- Błaszczyk, M.; Jabbar, R.; Szmyd, B.; Radek, M. 3D Printing of Rapid, Low-Cost and Patient-Specific Models of Brain Vasculature for Use in Preoperative Planning in Clipping of Intracranial Aneurysms. J. Clin. Med. 2021, 10, 1201. [Google Scholar] [CrossRef]
- Zheng, J.; Liu, X.; Chen, X.; Jiang, W.; Abdelrehem, A.; Zhang, S.; Chen, M.; Yang, C. Customized skull base–temporomandibular joint combined prosthesis with 3D-printing fabrication for craniomaxillofacial reconstruction: A preliminary study. Int. J. Oral Maxillofac. Surg. 2019, 48, 1440–1447. [Google Scholar] [CrossRef]
- Du, R.; Su, Y.-X.; Yan, Y.; Choi, W.S.; Yang, W.-F.; Zhang, C.; Chen, X.; Curtin, J.P.; Ouyang, J.; Zhang, B. A Systematic Approach for Making 3D-Printed Patient-Specific Implants for Craniomaxillofacial Reconstruction. Engineering 2020, 6, 1291–1301. [Google Scholar] [CrossRef]
- Atalay, H.A.; Canat, H.L.; Ülker, V.; Alkan, I.; Özkuvanci, Ü.; Altunrende, F. Impact of personalized three-dimensional (3D) printed pelvicalyceal system models on patient information in percutaneous nephrolithotripsy surgery: A pilot study. Int. Braz. J. Urol. 2017, 43, 470–475. [Google Scholar] [CrossRef] [PubMed]
- Westerman, M.E.; Matsumoto, J.M.; Morris, J.M.; Leibovich, B.C. Three-dimensional Printing for Renal Cancer and Surgical Planning. Eur. Urol. Focus 2016, 2, 574–576. [Google Scholar] [CrossRef] [PubMed]
- Meess, K.M.; Izzo, R.L.; Dryjski, M.L.; Curl, R.E.; Harris, L.M.; Springer, M.; Siddiqui, A.H.; Rudin, S.; Ionita, C.N. 3D Printed Abdominal Aortic Aneurysm Phantom for Image Guided Surgical Planning with a Patient Specific Fenestrated Endovascular Graft System. Proc. SPIE Int. Soc. Opt. Eng. 2017, 10138, 101380P. [Google Scholar] [CrossRef] [Green Version]
- Bhatla, P.; Mosca, R.S.; Tretter, J.T. Altering management decisions with gained anatomical insight from a 3D printed model of a complex ventricular septal defect. Cardiol. Young 2016, 27, 377–380. [Google Scholar] [CrossRef]
- RSNA-ACR 3D Printing Registry. Available online: https://www.acr.org/Practice-Management-Quality-Informatics/Registries/3D-Printing-Registry (accessed on 10 August 2021).
- Ballard, D.H.; Wake, N.; Witowski, J.; Rybicki, F.J.; Sheikh, A.; Weadock, W.J.; Ryan, J.R.; Matsumoto, J.S.; Souza, C.; Levine, D.; et al. Radiological Society of North America (RSNA) 3D Printing Special Interest Group (SIG) clinical situations for which 3D printing is considered an appropriate representation or extension of data contained in a medical imaging examination: Abdominal, hepatobiliary, and gastrointestinal conditions. 3D Print. Med. 2020, 6, 13. [Google Scholar] [CrossRef]
- Chepelev, L.; Wake, N.; Ryan, J.; Althobaity, W.; Gupta, A.; Arribas, E.; Santiago, L.; Ballard, D.H.; Wang, K.C.; Weadock, W.; et al. Radiological Society of North America (RSNA) 3D printing Special Interest Group (SIG): Guidelines for medical 3D printing and appropriateness for clinical scenarios. 3D Print. Med. 2018, 4, 11. [Google Scholar] [CrossRef]
- Rengier, F.; Mehndiratta, A.; von Tengg-Kobligk, H.; Zechmann, C.M.; Unterhinninghofen, R.; Kauczor, H.-U.; Giesel, F.L. 3D printing based on imaging data: Review of medical applications. Int. J. Comput. Assist. Radiol. Surg. 2010, 5, 335–341. [Google Scholar] [CrossRef]
- Schoening, W.; Denecke, T.; Neumann, U. Präoperative Bildgebung/Operationsplanung für die Leberchirurgie. Der Chir. 2015, 86, 1167–1182. [Google Scholar] [CrossRef] [PubMed]
- Bailer, R.; Martin, R.C. The effectiveness of using 3D reconstruction software for surgery to augment surgical education. Am. J. Surg. 2019, 218, 1016–1021. [Google Scholar] [CrossRef]
- Majno, P.; Mentha, G.; Toso, C.; Morel, P.; Peitgen, H.O.; Fasel, J.H. Anatomy of the liver: An outline with three levels of complexity—A further step towards tailored territorial liver resections. J. Hepatol. 2014, 60, 654–662. [Google Scholar] [CrossRef] [PubMed]
- Nakamura, T.; Tanaka, K.; Kiuchi, T.; Kasahara, M.; Oike, F.; Ueda, M.; Kaihara, S.; Egawa, H.; Ozden, I.; Kobayashi, N.; et al. Anatomical variations and surgical strategies in right lobe living donor liver transplantation: Lessons from 120 cases 1. Transplantation 2002, 73, 1896–1903. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Zein, N.N.; Hanouneh, I.A.; Bishop, P.D.; Samaan, M.; Eghtesad, B.; Quintini, C.; Miller, C.; Yerian, L.; Klatte, R. Three-dimensional print of a liver for preoperative planning in living donor liver transplantation. Liver Transplant. 2013, 19, 1304–1310. [Google Scholar] [CrossRef]
- Perica, E.R.; Sun, Z. A Systematic Review of Three-Dimensional Printing in Liver Disease. J. Digit. Imaging 2018, 31, 692–701. [Google Scholar] [CrossRef]
- Martelli, N.; Serrano, C.; van den Brink, H.; Pineau, J.; Prognon, P.; Borget, I.; El Batti, S. Advantages and disadvantages of 3-dimensional printing in surgery: A systematic review. Surgery 2016, 159, 1485–1500. [Google Scholar] [CrossRef]
- Valverde, I.; Gomez, G.; Gonzalez, A.; Suárez-Mejías, C.; Adsuar, A.; Coserria, J.F.; Uribe, S.; Gomez-Cia, T.; Hosseinpour, A.R. Three-dimensional patient-specific cardiac model for surgical planning in Nikaidoh procedure. Cardiol. Young 2015, 25, 698–704. [Google Scholar] [CrossRef]
- Soon, D.S.; Chae, M.P.; Pilgrim, C.H.; Rozen, W.; Spychal, R.T.; Hunter-Smith, D. 3D haptic modelling for preoperative planning of hepatic resection: A systematic review. Ann. Med. Surg. 2016, 10, 1–7. [Google Scholar] [CrossRef] [PubMed]
- Rizzetto, F.; Aseni, P.; Vezzulli, F.; Cassin, S.; Rantas, S.; Cereda, A.; Chiara, O.; Vanzulli, A.; Vertemati, M. Grade IV liver injury following mechanical cardiopulmonary resuscitation with postoperative three-dimensional evaluation. J. Emerg. Trauma Shock 2020, 13, 306–308. [Google Scholar] [CrossRef] [PubMed]
- Nalbant, B.; Egeli, T.; Ünek, T.; Altay, C.; Kavur, E.; Selver, A.; Obuz, F.; Ağalar, C.; Özbilgin, M.; Astarcıoğlu, I. Utilizing 3 Dimensional Print of The Liver in Living Donor Liver Transplantation for Preoperative Evaluation. J. Basic Clin. Health Sci. 2020, 4, 85–87. [Google Scholar] [CrossRef]
- Legnani, E.; Gallo, P.; Pezzotta, F.; Padelli, F.; Faragò, G.; Gioppo, A.; Gentili, L.; De Martin, E.; Fumagalli, M.L.; Cavaliere, F.; et al. Additive Fabrication of a Vascular 3D Phantom for Stereotactic Radiosurgery of Arteriovenous Malformations. 3D Print. Addit. Manuf. 2021, 8, 217–226. [Google Scholar] [CrossRef]
- Umale, S.; Chatelin, S.; Bourdet, N.; Deck, C.; Diana, M.; Dhumane, P.; Soler, L.; Marescaux, J.; Willinger, R. Experimental in vitro mechanical characterization of porcine Glisson’s capsule and hepatic veins. J. Biomech. 2011, 44, 1678–1683. [Google Scholar] [CrossRef]
- He, X.-J.; Yu, M.-H.; Li, W.-C.; Wang, H.-Q.; Li, J.; Peng, X.-C.; Tang, J.; Feng, N.; Huang, T.-Z. Morphological and biomechanical remodelling of the hepatic artery in a swine model of portal hypertension. Hepatol. Int. 2012, 6, 631–638. [Google Scholar] [CrossRef]
- Bismuth, H. Surgical anatomy and anatomical surgery of the liver. World J. Surg. 1982, 6, 3–9. [Google Scholar] [CrossRef]
- Couinaud, C. (Ed.) Surgical Anatomy of the Liver Revisited; C. Couinaud: Paris, France, 1989; ISBN 9782903672010. [Google Scholar]
- Witowski, J.S.; Pędziwiatr, M.; Major, P.; Budzyński, A. Cost-effective, personalized, 3D-printed liver model for preoperative planning before laparoscopic liver hemihepatectomy for colorectal cancer metastases. Int. J. Comput. Assist. Radiol. Surg. 2017, 12, 2047–2054. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Pacioni, A.; Carbone, M.; Freschi, C.; Viglialoro, R.M.; Ferrari, V.; Ferrari, M. Patient-specific ultrasound liver phantom: Materials and fabrication method. Int. J. Comput. Assist. Radiol. Surg. 2014, 10, 1065–1075. [Google Scholar] [CrossRef] [PubMed]
- Condino, S.; Montemurro, N.; Cattari, N.; D’Amato, R.; Thomale, U.; Ferrari, V.; Cutolo, F. Evaluation of a Wearable AR Platform for Guiding Complex Craniotomies in Neurosurgery. Ann. Biomed. Eng. 2021, 49, 1–16. [Google Scholar] [CrossRef]
- Zhang, W.; Zhu, W.; Yang, J.; Xiang, N.; Zeng, N.; Hu, H.; Jia, F.; Fang, C. Augmented Reality Navigation for Stereoscopic Laparoscopic Anatomical Hepatectomy of Primary Liver Cancer: Preliminary Experience. Front. Oncol. 2021, 11, 663236. [Google Scholar] [CrossRef] [PubMed]
- Igami, T.; Nakamura, Y.; Hirose, T.; Ebata, T.; Yokoyama, Y.; Sugawara, G.; Mizuno, T.; Mori, K.; Nagino, M. Application of a Three-dimensional Print of a Liver in Hepatectomy for Small Tumors Invisible by Intraoperative Ultrasonography: Preliminary Experience. World J. Surg. 2014, 38, 3163–3166. [Google Scholar] [CrossRef]
- Perica, E.; Sun, Z. Patient-specific three-dimensional printing for pre-surgical planning in hepatocellular carcinoma treatment. Quant. Imaging Med. Surg. 2017, 7, 668–677. [Google Scholar] [CrossRef] [Green Version]
- Witowski, J.; Budzyński, A.; Grochowska, A.; Ballard, D.H.; Major, P.; Rubinkiewicz, M.; Złahoda-Huzior, A.; Popiela, T.J.; Wierdak, M.; Pędziwiatr, M. Decision-making based on 3D printed models in laparoscopic liver resections with intraoperative ultrasound: A prospective observational study. Eur. Radiol. 2019, 30, 1306–1312. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Tejo-Otero, A.; Lustig-Gainza, P.; Fenollosa-Artés, F.; Valls, A.; Krauel, L.; Buj-Corral, I. 3D printed soft surgical planning prototype for a biliary tract rhabdomyosarcoma. J. Mech. Behav. Biomed. Mater. 2020, 109, 103844. [Google Scholar] [CrossRef] [PubMed]
- Blanco, A.M.; Krauel, L.; Artés, F.F. Development of a patients-specific 3D-printed preoperative planning and training tool, with functionalized internal surfaces, for complex oncologic cases. Rapid Prototyp. J. 2019, 25, 363–377. [Google Scholar] [CrossRef]


| Anatomical Details | Spatial Relation of the Venous and Vasculo-Biliary Three | Haptic Properties | |
|---|---|---|---|
| HB surgical team score (total/mean) | 18/3 | 16/2.7 | 12/2.0 |
| Expert radiology team score (total/mean) | 18/3 | 15/2.5 | 13/2.2 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Aseni, P.; Santaniello, T.; Rizzetto, F.; Gentili, L.; Pezzotta, F.; Cavaliere, F.; Vertemati, M.; Milani, P. Hybrid Additive Fabrication of a Transparent Liver with Biosimilar Haptic Response for Preoperative Planning. Diagnostics 2021, 11, 1734. https://doi.org/10.3390/diagnostics11091734
Aseni P, Santaniello T, Rizzetto F, Gentili L, Pezzotta F, Cavaliere F, Vertemati M, Milani P. Hybrid Additive Fabrication of a Transparent Liver with Biosimilar Haptic Response for Preoperative Planning. Diagnostics. 2021; 11(9):1734. https://doi.org/10.3390/diagnostics11091734
Chicago/Turabian StyleAseni, Paolo, Tommaso Santaniello, Francesco Rizzetto, Lorenzo Gentili, Federico Pezzotta, Francesco Cavaliere, Maurizio Vertemati, and Paolo Milani. 2021. "Hybrid Additive Fabrication of a Transparent Liver with Biosimilar Haptic Response for Preoperative Planning" Diagnostics 11, no. 9: 1734. https://doi.org/10.3390/diagnostics11091734







