Challenges in Diagnosis of Uretero–Arterial Fistulas after Complex Pelvic Oncological Procedures—Single Center Experience and Review of the Literature
Abstract
:1. Introduction
2. Materials and Methods
3. Results
4. Discussions
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Kamphorst, K.; Lock, T.M.T.W.; Bergh, R.C.N.V.D.; Moll, F.L.; de Vries, J.-P.P.M.; Lo, R.T.H.; de Kort, G.A.P.; Bruijnen, R.C.G.; Dik, P.; Horenblas, S.; et al. Arterio-Ureteral Fistula: Systematic Review of 445 Patients. J. Urol. 2022, 207, 35–43. [Google Scholar] [CrossRef] [PubMed]
- van den Bergh, R.C.; Moll, F.L.; de Vries, J.P.; Lock, T.M. Arterioureteral fistulas: Unusual suspects-systematic review of 139 cases. Urology 2009, 74, 251–255. [Google Scholar] [CrossRef] [PubMed]
- Heers, H.; Netsch, C.; Wilhelm, K.; Secker, A.; Kurtz, F.; Spachmann, P.; Viniol, S.; Hofmann, R.; Hegele, A. Diagnosis, Treatment, and Outcome of Arterioureteral Fistula: The Urologist’s Perspective. J. Endourol. 2018, 32, 245–251. [Google Scholar] [CrossRef] [PubMed]
- Omran, S.; Schäfer, H.; Kapahnke, S.; Müller, V.; Bürger, M.; Konietschke, F.; Frese, J.P.B.; Neymeyer, J.; Greiner, A. Endovascular and open surgical options in the treatment of uretero-arterial fistulas. Vascular 2020, 29, 672–681. [Google Scholar] [CrossRef]
- van den Bergh, R.C.; Moll, F.L.; de Vries, J.P.; Yeung, K.K.; Lock, T.M. Arterio-ureteral fistula: 11 new cases of a wolf in sheep’s clothing. J. Urol. 2008, 179, 578–581. [Google Scholar] [CrossRef]
- Malgor, R.D.; Oderich, G.S.; Andrews, J.C.; McKusick, M.; Kalra, M.; Misra, S.; Gloviczki, P.; Bower, T.C. Evolution from open surgical to endovascular treatment of ureteral-iliac artery fistula. J. Vasc. Surg. 2012, 55, 1072–1080. [Google Scholar] [CrossRef] [Green Version]
- Hong, S.-Y.; Noh, M.; Ko, G.-Y.; Han, Y.; Kwon, H.; Kwon, T.-W.; Cho, Y.-P. Management Strategy for Ureteral-Iliac Artery Fistula. Ann. Vasc. Surg. 2016, 36, 22–27. [Google Scholar] [CrossRef]
- Krambeck, A.E.; DiMarco, D.S.; Gettman, M.T.; Segura, J.W. Ureteroiliac artery fistula: Diagnosis and treatment algorithm. Urology 2005, 66, 990–994. [Google Scholar] [CrossRef]
- Bergqvist, D.; Parsson, H.; Sherif, A. Arterio-ureteral fistula—A systematic review. Eur. J. Vasc. Endovasc. Surg. 2001, 22, 191–196. [Google Scholar] [CrossRef] [Green Version]
- Ghouti, C.; Leon, G.; Seddik, S.; Said, K.A.; Vaudreuil, L.; Tillou, X. Uretero-arterial fistula: Six new cases and systematic review of the literature. Prog. Urol. 2021, 31, 605–617. [Google Scholar] [CrossRef]
- Matsunaga, F.; Dambaeva, A.; Ponsky, L.E.; Kashyap, V.S.; Tavri, S. Systematic Review of the Management of Ureteroarterial Fistulas After Ileal Conduit Urinary Diversion. Am. J. Roentgenol. 2021, 216, 1452–1461. [Google Scholar] [CrossRef] [PubMed]
- Tselikas, L.; Pellerin, O.; Di Primio, M.; Ben Arfi, M.; Joskin, J.; Beyssen, B.; Thiounn, N.; Sapoval, M. Uretero-iliac fistula: Modern treatment via the endovascular route. Diagn. Interv. Imaging 2013, 94, 311–318. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Moon, E.J.; Kim, D.H.; Chung, J.Y.; Yi, J.W.; Joh, J.H.; Kim, D.H. Endovascular treatment of arterioureteral fistulae involving both external and internal iliac arteries; report of a rare case. Int. J. Clin. Exp. Med. 2016, 9, 12333–12336. [Google Scholar]
- Hernandez, N.; Desroches, B.; Peden, E.; Satkunasivam, R. Uretero-Iliac artery fistula: A rare cause of haematuria. BMJ Case Rep. 2020, 13, e232189. [Google Scholar] [CrossRef] [PubMed]
- Yamasaki, K.; Omori, K.; Takaoka, E.-I.; Sekido, N.; Shigai, M.; Mori, K.; Minami, M.; Watanabe, Y.; Shimazui, T.; Akaza, H. Successful Management by Provocative Angiography and Endovascular Stent of Ureteroarterial Fistula in a Patient with a Long-term Indwelling Ureteral Stent. Jpn. J. Clin. Oncol. 2009, 40, 267–270. [Google Scholar] [CrossRef] [Green Version]
- Madoff, D.C.; Toombs, B.D.; Skolkin, M.D.; Bodurka, D.; Modesitt, S.C.; Wood, C.G.; Hicks, M.E. Endovascular Management of Ureteral-Iliac Artery Fistulae with Wallgraft Endoprostheses. Gynecol. Oncol. 2002, 85, 212–217. [Google Scholar] [CrossRef]
- Batter, S.J.; McGovern, F.J.; Cambria, R.P. Ureteroarterial fistula: Case report and review of the literature. Urology 1996, 48, 481–489. [Google Scholar] [CrossRef]
- Callegari, M.; Thomas, J.; Shekar, A.; Fernstrum, A.; Chen, M.; Bose, S.; Ponsky, L.; Abdel-Azim, A.; Kashyap, V.; Tavri, S. Arterioureteral Fistula in the Setting of an Indwelling Ureteral Stent, Ileal Conduit and History of Pelvic Radiation. Urology 2020, 140, 14–17. [Google Scholar] [CrossRef]
- Shutze, W.P.; Schoenvogel, R.C.; Jacobson, R.M.; Talkington, C.M. Intraoperative transvascular balloon catheter management for arterioureteral fistula. Cardiovasc. Surg. 1993, 1, 731–733. [Google Scholar]
- Horikawa, M.; Saito, H.; Hokotate, H.; Mori, T. Treatment of Ureteroarterial Fistula with an Endoureteral Stent Graft. J. Vasc. Interv. Radiol. 2012, 23, 1241–1243. [Google Scholar] [CrossRef]
- Melegari, S.; Paparella, S.; Follini, M.L.; Cappellano, F.; Ciotti, M.G.; Giollo, A.; Marzorati, G.; Airoldi, F.; Losa, S.; Verweij, F. Bilateral Ureteroarterial Fistula: A Case Report and Review of Literature. Urol. J. 2016, 83, 168–172. [Google Scholar] [CrossRef] [PubMed]
- Okada, T.; Yamaguchi, M.; Muradi, A.; Nomura, Y.; Uotani, K.; Idoguchi, K.; Miyamoto, N.; Kawasaki, R.; Taniguchi, T.; Okita, Y.; et al. Long-term Results of Endovascular Stent Graft Placement of Ureteroarterial Fistula. Cardiovasc. Interv. Radiol. 2012, 36, 950–956. [Google Scholar] [CrossRef] [PubMed]
- Schneider, M.H.; Laturnus, J.M.; Cordes, J. Arterioureteral fistulas in the last 10 years at the University of Lubeck. Urol. A 2019, 58, 666–672. [Google Scholar] [CrossRef]
- Das, A.; Lewandoski, P.; Laganosky, D.; Walton, J.; Shenot, P. Ureteroarterial fistula: A review of the literature. Vascular 2015, 24, 203–207. [Google Scholar] [CrossRef]
- Titomihelakis, G.; Feghali, A.; Nguyen, T.; Salvatore, D.; DiMuzio, P.; Abai, B. Endovascular management and the risk of late failure in the treatment of ureteroarterial fistulas. J. Vasc. Surg. Cases Innov. Tech. 2019, 5, 396–401. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Massmann, A.; Fries, P.; Shayesteh-Kheslat, R.; Buecker, A.; Stöckle, M.; Niklas, C. Life-threatening arterioureteral fistula treatment by endovascular complete anatomic iliac artery bifurcation reconstruction. J. Vasc. Surg. Cases Innov. Tech. 2020, 6, 199–204. [Google Scholar] [CrossRef]
- Simon, B.; Neubauer, J.; Schoenthaler, M.; Hein, S.; Bamberg, F.; Maruschke, L. Management and endovascular therapy of ureteroarterial fistulas: Experience from a single center and review of the literature. CVIR Endovasc. 2021, 4, 36. [Google Scholar] [CrossRef] [PubMed]
- Noh, S.Y.; Shin, J.H.; Yang, W.J.; Chu, H.H.; Park, S.; Chen, C.; Lee, W.H. Arterioureteral fistula: Overview of clinical characteristics, endovascular management, and outcomes. Minim. Invasive Ther. Allied Technol. 2020, 31, 197–205. [Google Scholar] [CrossRef] [PubMed]
- Sherif, A.; Karacagil, S.; Magnusson, A.; Nyman, R.; Norlén, B.J.; Bergqvist, D. Endovascular Approach to Treating Secondary Arterioureteral Fistula. Scand. J. Urol. Nephrol. 2002, 36, 80–82. [Google Scholar] [CrossRef]
- Munoz Guillermo, V.; Carrillo George, C.; Jimenez Peralta, D.; Pietricica, B.N.; Fernandez Aparicio, T. Ureteroiliac Fistula: Bleeding of Unknown Origin—Case Report and Review of the Literature. J. Endourol. Case Rep. 2020, 6, 413–415. [Google Scholar] [CrossRef] [PubMed]
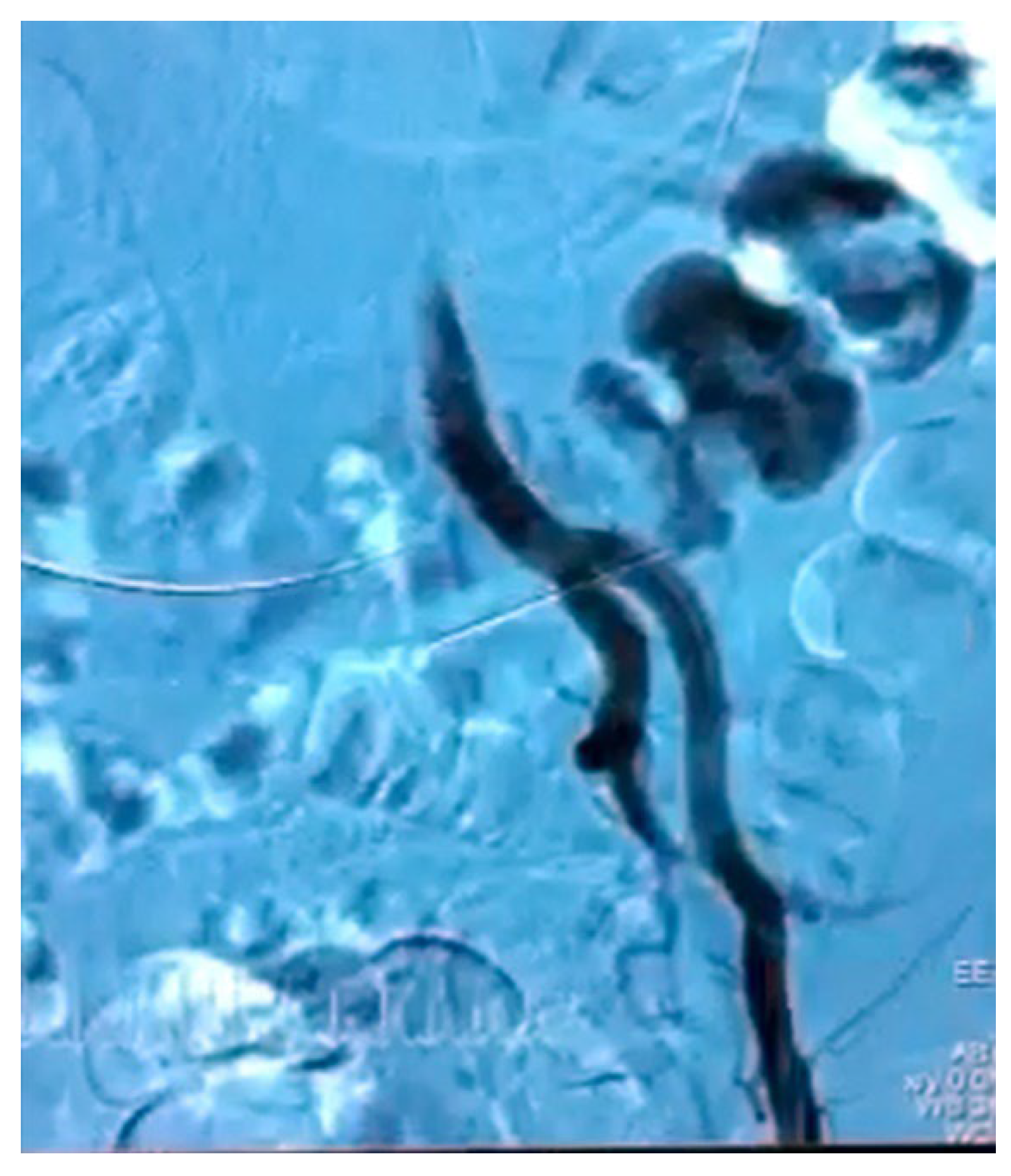

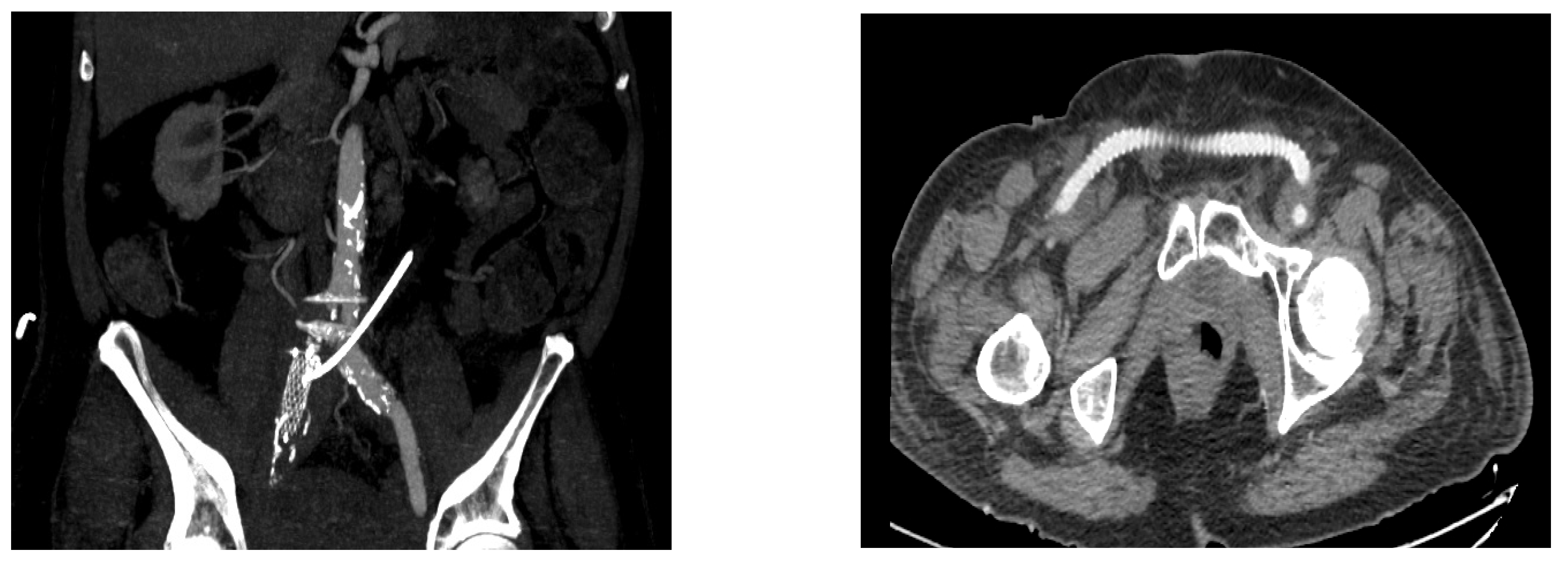
| Mean Age (Yrs, IQR) | 65.3 (51–79) |
|---|---|
| Sex | No, % |
| Male | 2 (22.22) |
| Female | 7 (77.77) |
| Presence of infection | |
| No | 1 (11.11) |
| Multidrug resistant UTI | 6 (66.66) |
| Permanent ureteric stenting | 9 (100) |
| Mean time of permanent stenting to UAF (months, inverval) | 26.8 (8–42.1) |
| Type of surgery for pelvic cancer | |
| Cervical cancer | |
| Hysterectomy | 1 (11.11) |
| Anterior exenteration with cutaneus ureterostomy | 6 (66.66) |
| Bladder cancer | |
| Cystectomy with ileal conduit | 1 (11.11) |
| Colorectal cancer | |
| Total exenteration with ileal conduit | 1 (11.11) |
| Urinay diversion | |
| Cutaneus urinary diversion | 6 (66.66) |
| Ileal conduit | 2 (22.22) |
| Radiotherapy | |
| EBRT only | 2 (22.22) |
| EBRT + brachytherapy | 7 (77.77) |
| Median time from radiotherapy to UAF (months) | 34.6 (11–54.7) |
| Clinical symptoms | |
| Hematuria | 9 (100) |
| Flank pain | 6 (66.66) |
| Hypovolemic shock | 3 (33.33) |
| Mean Hemoglobin at diagnostic (mg/dL, interval) | 7.24 (5.1, 10.8) |
| Mean serum creatinine at diagnostic (mg/dL, interval) | 1.4 (0.6, 2.4) |
| Diagnostic Imaging Procedures | No, % |
|---|---|
| CT scan | 5/9 (55.55) |
| Angiography | 5/7 (71.42) |
| Retrograde pyelography | 1/9 (11.11) |
| Fistula location | |
| Left ureter–left CIA | 6/9 (66.66) |
| Left ureter–abdominal aorta | 1/9 (11.11) |
| Left ureter–EIA–descending colon | 1/9 (11.11) |
| Right ureter–right CIA | 1/9 (11.11) |
| Metacronous UAF | 1/9 (11.11) |
| Pretreatment Diagnostic Imaging | |||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| Year | CT | Angio | Other | Type of Urinary Diversion | UAF Location | Arterial Treatment | Ureteral Treatment | Additional Procedures | Follow-Up (Months) | Status | |
| 1 | 2012 | Negative | Positive | USC | Left ureter- left CIA | Endovascular stent | Nephrostomy | endovascular restenting | 7 | Dead | |
| 2 | 2013 | Negative | N/A | USC | Left ureter- Aorta | Aortic patch | Nephroureterectomy | 1 | Dead | ||
| 3 | 2015 | Positive | Positive | USC | Left ureter- left EIA+ colon | EIA ligation and FFC | ureter ligation +Nephrostomy | Left colectomy | 78 | Dead | |
| 4 | 2016 | Positive | Positive | USC | Left ureter- left CIA | CIA ligation and FFC | ureter ligation +Nephrostomy | 64 | Alive | ||
| 5 | 2018 | Positive | Negative | USC | Left ureter- left CIA | Endovascular stent | Nephrostomy | Nephrectomy | 32 | Alive | |
| 6 | 2019 | Negative | N/A | UPR | None | Left ureter- left CIA | Patch angioplasty | Nephroureterectomy | 27 | Alive | |
| 7 | 2020 | Positive | Negative | Bricker | Left ureter- left CIA | Endovascular stent | Nephrostomy | endovascular restenting | |||
| 2021 | Negative | Negative | Right ureter- right CIA | Endovascular stent | Nephrostomy | Ureter ligation +CIA ligation and FFC | 4 | Dead | |||
| 8 | 2021 | Negative | Positive | Bricker | Left ureter- left CIA | Endovascular stent | Nephrostomy | 10 | Alive | ||
| 9 | 2021 | Positive | Positive | USC | Left ureter- left CIA | Endovascular stent | Nephrostomy | 8 | Alive | ||
| Article, Year | No of Pts | Cystoscopy | CT | Angio | Pyelography | URS | Open Surgery |
|---|---|---|---|---|---|---|---|
| Malgor, 2012 [6] | 20 | 11/14 | 3/8 | 12/14 | |||
| Okada, 2013 [22] | 11 | 6/11 | 6/11 | ||||
| Hong, 2016 [7] | 6 | 4/6 | 1/6 | 1/6 | |||
| Schneider, 2016 [23] | 5 | 2/4 | 2/5 | 2/5 | 1/5 | ||
| Das, 2016 [24] | 61 | 26/34 | 13/36 | 55/76 | 16/24 | 42/45 | |
| Heers, 2018 [3] | 24 | 5/14 | 9/23 | ||||
| Titomihelakis,2019 [25] | 5 | 1/5 | 5/5 | 1/5 | 2/5 | ||
| Massmann, 2020 [26] | 5 | 1/5 | 5/5 | 5/5 | |||
| Simon, 2021 [27] | 17 | 2/10 | 3/17 | ||||
| Omran, 2021 [4] | 25 | 17/25 | 7/23 | 4/21 | |||
| Ghouti, 2021 [10] | 6 | 2/5 | 2/5 | ||||
| Matsunaga, 2021 [11] | 40 | 3/13 | 15/27 | 4/11 | 1/6 | 4/4 | |
| Kamphorst, 2022 [1] | 445 | 40/142 | 68/141 | 169/272 | 60/118 | 40/142 | |
| Our study, 2022 | 9 | 1/9 | 5/9 | 5/7 | 1/9 | ||
| Overall sensitivity | 679 | 97/239 (40.58%) | 134/285 (47.01%) | 292/488 (59.83%) | 85/178 (47.75%) | 43/153 (28.1%) | 48/60 (80%) |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Surcel, C.; Mirvald, C.; Stoica, R.; Cerempei, V.; Heidegger, I.; Labanaris, A.; Tsaur, I.; Baston, C.; Sinescu, I. Challenges in Diagnosis of Uretero–Arterial Fistulas after Complex Pelvic Oncological Procedures—Single Center Experience and Review of the Literature. Diagnostics 2022, 12, 1832. https://doi.org/10.3390/diagnostics12081832
Surcel C, Mirvald C, Stoica R, Cerempei V, Heidegger I, Labanaris A, Tsaur I, Baston C, Sinescu I. Challenges in Diagnosis of Uretero–Arterial Fistulas after Complex Pelvic Oncological Procedures—Single Center Experience and Review of the Literature. Diagnostics. 2022; 12(8):1832. https://doi.org/10.3390/diagnostics12081832
Chicago/Turabian StyleSurcel, Cristian, Cristian Mirvald, Robert Stoica, Vasile Cerempei, Isabel Heidegger, Apostolos Labanaris, Igor Tsaur, Catalin Baston, and Ioanel Sinescu. 2022. "Challenges in Diagnosis of Uretero–Arterial Fistulas after Complex Pelvic Oncological Procedures—Single Center Experience and Review of the Literature" Diagnostics 12, no. 8: 1832. https://doi.org/10.3390/diagnostics12081832







