Diagnosis and Treatment of Inflammatory Pseudotumor with Lower Cranial Nerve Neuropathy by Endoscopic Endonasal Approach: A Systematic Review
Abstract
:1. Introduction
2. Materials and Methods
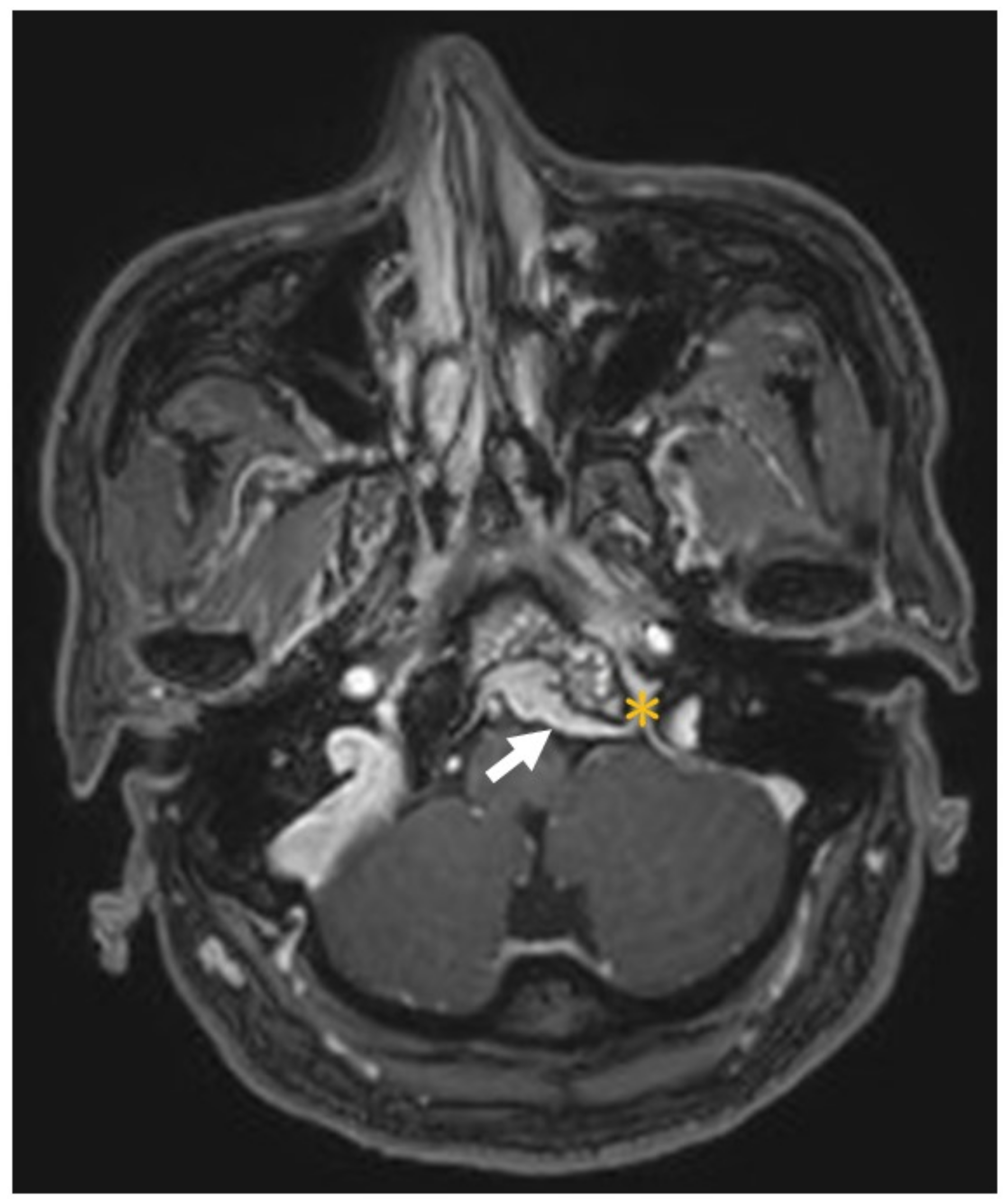
3. Illustrative Case
4. Results
4.1. Demographics and Clinical Presentation
4.2. Diagnostic Tools
4.3. Treatment and Follow-Up Outcomes
5. Discussion
5.1. Etiology
5.2. Demographics and Clinical Presentation
5.3. Diagnostic Tools
5.4. Treatment
5.5. Follow-Up Outcomes
6. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Gandhi, R.H.; Li, L.; Qian, J.; Kuo, Y.H. Intraventricular inflammatory pseudotumor: Report of two cases and review of the literature. Neuropathology 2011, 31, 446–454. [Google Scholar] [CrossRef]
- Eloy, J.A.; Setzen, M.; Liu, J.K. Sinonasal and Ventral Skull Base Malignancies. Otolaryngol. Clin. N. Am. 2017, 50, xxi–xxii. [Google Scholar] [CrossRef]
- Spinazzi, E.F.; Desai, S.V.; Fang, C.H.; Jyung, R.W.; Liu, J.K.; Baredes, S.; Eloy, J.A. Lateral skull base Inflammatory pseudotumor: A systematic review. Laryngoscope 2015, 125, 2593–2600. [Google Scholar] [CrossRef]
- Lin, Y.J.; Yang, T.M.; Lin, J.W.; Song, M.Z.; Lee, T.C. Posterior fossa intracranial inflammatory pseudotumor: A case report and literature review. Surg. Neurol. 2009, 72, 712–716. [Google Scholar] [CrossRef]
- Scott, L.; Blair, G.; Taylor, G.; Dimmick, J.; Fraser, G. Inflammatory pseudotumors in children. J. Pediatr. Surg. 1988, 23, 755–758. [Google Scholar] [CrossRef]
- Vaughan, K.G.; Aziz, A.; Meza, M.P.; Hackam, D.J. Mesenteric inflammatory pseudotumor as a cause of abdominal pain in a teenager: Presentation and literature review. Pediatr. Surg. Int. 2005, 21, 497–499. [Google Scholar] [CrossRef] [PubMed]
- Petrovic, I.; Augustin, G.; Hlupic, L.; Nedic, A.; Romic, I.; Skegro, M. Inflammatory myofibroblastic tumors of the duodenum. Asian J. Surg. 2016, 39, 247–252. [Google Scholar] [CrossRef]
- Carswell, C.; Chataway, J. The successful long-term management of an intracranial inflammatory myofibroblastic tumor with corticosteroids. Clin. Neurol. Neurosurg. 2012, 114, 77–79. [Google Scholar] [CrossRef]
- Puntambekar, P.; Santhakumar, S.; Kupsky, W.J.; Tselis, A.; Mittal, S. Primary intracranial plasma cell granulomas presenting as malignant neoplasms. J. Neurooncol. 2012, 106, 327–337. [Google Scholar] [CrossRef] [PubMed]
- Mendenhall, W.M.; Lessner, A.M. Orbital pseudotumor. Am. J. Clin. Oncol. 2010, 33, 304–306. [Google Scholar] [CrossRef]
- Williamson, R.A.; Paueksakon, P.; Coker, N.J. Inflammatory pseudotumor of the temporal bone. Otol. Neurotol. 2003, 24, 818–822. [Google Scholar] [CrossRef]
- Ajibade, D.V.; Tanaka, I.K.; Paghdal, K.V.; Mirani, N.; Lee, H.J.; Jyung, R.W. Inflammatory pseudotumor (plasma cell granuloma) of the temporal bone. Ear Nose Throat J. 2010, 89, E1–E13. [Google Scholar] [CrossRef] [PubMed]
- Moher, D.; Liberati, A.; Tetzlaff, J.; Altman, D.G. Preferred reporting items for systematic reviews and meta-analyses: The PRISMA statement. PLoS Med. 2009, 6, e1000097. [Google Scholar] [CrossRef] [PubMed]
- Sung, M.W.; Kim, K.H.; Lee, C.H.; Moh, J.H.; Kim, W.H.; Han, M.H. Fibrosing inflammatory pseudotumors of the central skull base. Laryngoscope 1997, 107, 1651–1655. [Google Scholar] [CrossRef] [PubMed]
- Pallini, R.; Liverana, L.; Maria, L.L.; Cesare, C.; Eduardo, F.; Babu, R. Isolated inflammatory pseudotumor of the occipital condyle. Report of two cases. J. Neurosurg. 2002, 97, 248–251. [Google Scholar] [CrossRef] [PubMed]
- Crovetto, M.; Olega, L. Fibrosing inflammatory pseudotumor. Eur. J. Radiol. Extra 2004, 52, 61–64. [Google Scholar] [CrossRef]
- Lee, D.K.; Cho, Y.S.; Hong, S.H.; Chung, W.H.; Ahn, Y.C. Inflammatory pseudotumor involving the skull base: Response to steroid and radiation therapy. Otolaryngol. Head Neck Surg. 2006, 135, 144–148. [Google Scholar] [CrossRef]
- Lu, C.H.; Yang, C.Y.; Wang, C.P.; Yang, C.C.; Liu, H.M.; Chen, Y.F. Imaging of nasopharyngeal inflammatory pseudotumours: Differential from nasopharyngeal carcinoma. Br. J. Radiol. 2010, 83, 8–16. [Google Scholar] [CrossRef] [PubMed]
- Al-Sarraj, S.; Wasserberg, J.; Bartlett, R.; Bridges, L.R. Inflammatory pseudotumour of the central nervous system: Clinicopathological study of one case and review of the literature. Br. J. Neurosurg. 1995, 9, 57–66. [Google Scholar] [CrossRef] [PubMed]
- Chang, Y.; Horoupian, D.S.; Lane, B.; Fross, R.D.; Smyth, L.T., Jr.; Seiling, R.J. Inflammatory pseudotumor of the choroid plexus in Sjögren’s disease. Neurosurgery 1991, 29, 287–290. [Google Scholar] [CrossRef]
- Arber, D.A.; Kamel, O.W.; van de Rijn, M.; Davis, R.E.; Medeiros, L.J.; Jaffe, E.S.; Weiss, L.M. Frequent presence of the Epstein-Barr virus in inflammatory pseudotumor. Hum. Pathol. 1995, 26, 1093–1098. [Google Scholar] [CrossRef]
- Gulley, M.L. Molecular diagnosis of Epstein-Barr virus-related diseases. J. Mol. Diagn. 2001, 3, 1–10. [Google Scholar] [CrossRef]
- Tai, Y.S.; Lin, P.W.; Chen, S.G.; Chang, K.C. Inflammatory pseudotumor of the liver in a patient with human immunodeficiency virus infection. Hepatogastroenterology 1998, 45, 1760–1763. [Google Scholar] [PubMed]
- Geny, C.; Cesaro, P.; Heran, F.; Nguyen, J.P.; Poirier, J.; Degos, J.D. Pseudotumoral neuro-Behçet’s disease. Surg. Neurol. 1993, 39, 374–376. [Google Scholar] [CrossRef]
- Bramwit, M.; Kalina, P.; Rustia-Villa, M. Inflammatory pseudotumor of the choroid plexus. AJNR Am. J. Neuroradiol. 1997, 18, 1307–1309. [Google Scholar] [PubMed]
- Stuti, V.D.; Eleonora, F.S.; Christina, H.F.; Grace, H.; Senja, T.; James, K.L.; Soly, B.; Jean, A.E. Sinonasal and Ventral Skull Base Inflammatory Pseudotumor: A Systematic Review. Laryngoscope 2015, 125, 813–821. [Google Scholar] [CrossRef]
- Nakayama, K.; Inoue, Y.; Aiba, T.; Kono, K.; Wakasa, K.; Yamada, R. Unusual CT and MR findings of inflammatory pseudotumor in the parapharyngeal space: Case report. AJNR Am. J. Neuroradiol. 2001, 22, 1394–1397. [Google Scholar] [PubMed]
- Alyono, J.C.; Shi, Y.; Berry, G.J.; Recht, L.D.; Harsh, G.R.T.; Jackler, R.K.; Corrales, C.E. Inflammatory Pseudotumors of the Skull Base: Meta-Analysis. Otol. Neurotol. 2015, 36, 1432–1438. [Google Scholar] [CrossRef] [PubMed]
- Mombaerts, I.; Schlingemann, R.O.; Goldschmeding, R.; Koornneef, L. Are systemic corticosteroids useful in the management of orbital pseudotumors? Ophthalmology 1996, 103, 521–528. [Google Scholar] [CrossRef]
- Mangiardi, J.R.; Har-El, G. Extraorbital skull base idiopathic pseudotumor. Laryngoscope 2007, 117, 589–594. [Google Scholar] [CrossRef] [PubMed]
- Huang, B.; Liu, H.J.; Liang, C.H. Inflammatory pseudotumor of the skull base involving fissura petrooccipitalis: A rare case with challenging diagnosis. Skull Base Rep. 2011, 1, 105–110. [Google Scholar] [CrossRef] [PubMed]
- McCall, T.; Fassett, D.R.; Lyons, G.; Couldwell, W.T. Inflammatory pseudotumor of the cavernous sinus and skull base. Neurosurg. Rev. 2006, 29, 194–200. [Google Scholar] [CrossRef] [PubMed]
- Shah, S.S.; Lowder, C.Y.; Schmitt, M.A.; Wilke, W.S.; Kosmorsky, G.S.; Meisler, D.M. Low-dose methotrexate therapy for ocular inflammatory disease. Ophthalmology 1992, 99, 1419–1423. [Google Scholar] [CrossRef]






| Year | Author | No. | Age /Sex | Lower Cranial Nerve S/S | Involved Regions | Involved Nerves | MRI Findings | Serology 1 | Biopsy | Treatment Modality | Follow-up Period |
|---|---|---|---|---|---|---|---|---|---|---|---|
| 1997 | Sung et al. [14] | 1 | 57F | Dysphagia | JF, ITF | VII, IX, X, XII | ND | - | Endoscope | Prednisolone (oral): 60–100 mg/d | 6 mo |
| 2 | 41M | Dysphagia, dysarthria, hoarseness | JF | IX, X, XII | T1 hypo T2 hypo | - | Endoscope | Prednisolone (oral): 60–100 mg/d | 6 mo | ||
| 2002 | Pallini et al. [15] | 3 | 49F | Tongue atrophy | FM, clivus | VIII, XII | None | - | nil | Complete resection surgery | 5 y |
| 4 | 46F | Dysphagia, tongue atrophy | FM, clivus, brain stem and upper cervical compression | XI, X, XI, XII | T1 hypo | - | nil | Partial resection surgery | 2 y | ||
| 2004 | Crovetto et al. [16] | 5 | 72M | Dysphagia, tongue atrophy | NP, clivus, HC | IX, X, XII | T1 iso | - | Endoscope | Prednisolone (Total 552 mg IM for 24 days + 30 mg/day oral for 45 days) | 1 y |
| 2006 | Lee et al. [17] | 6 | 63M | Dysphagia, hoarseness | IX, X, XII | ND | - | Transmastoid | Prednisolone (oral): 60 mg/day for 28 days + 10 mg/day for 56 days + RT (2000 cGy) | 6 mo | |
| 2009 | Lin et al. [4] | 7 | 49M | Hoarseness, slow gag reflex, uvula deviation, | CPA | IX, X | enhanced | + | nil | En bloc surgery + whole brain RT (1200 cGy in 6 fractionations) | 2 y |
| 2010 | Lu et al. [18] | 8 | 70M | Dysphagia, hoarseness | NP, HC, JF | II, III, V, VII, IX, X, XII | T1 hypo T2 hypo | - | NP punch | CS (oral) | 1 mo |
| 9 | 32M | Tongue atrophy | NP, Clivus, HC, JF | XII | T1 hypo T2 hypo | - | CT-guided | CS (oral) | 7 mo | ||
| 10 | 37M | Hoarseness | NP, clivus, HC, JF | XII | T1 hypo T2 hypo | - | NP punch | CS (oral) | 8 mo | ||
| Present case | Huang et al. | 48M | Dysphagia, hoarseness, tongue atrophy | JF, Clivus, HC, CA | IX, X, XII | T1 iso T2 hypo | + | nil | Endoscopic decompression surgery + prednisolone (10 mg/day for 100 days, oral) | 3 y |
| Outcomes | All Patients | Treatment Modality | ||||
|---|---|---|---|---|---|---|
| CS Alone | Surgery Alone | CS + RT | Surgery + RT | EEA+ CS | ||
| Symptomatic | ||||||
| Complete resolution | 4 | 3 (50%) | 0 (0%) | 0 (0%) | 0 (0%) | 1 (100%) |
| Partially improved | 3 | 3 (50%) | 0 (0%) | 0 (0%) | 0 (0%) | 0 (0%) |
| Persistent | 4 | 0 (0%) | 2 (100%) | 1 (100%) | 1 (100%) | 0 (0%) |
| Radiographic | ||||||
| Complete resolution | 5 | 3 (50%) | 1 (50%) | 0 (0%) | 0 (0%) | 1 (100%) |
| Remission or stable | 5 | 3 (50%) | 1 (50%) | 0 (0%) | 1 (100%) | 0 (0%) |
| Progression or die | 1 | 0 (0%) | 0 (0%) | 1 (100%) | 0 (0%) | 0 (0%) |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Huang, S.-H.; Chuang, C.-C.; Huang, C.-C.; Jung, S.-M.; Lee, C.-C. Diagnosis and Treatment of Inflammatory Pseudotumor with Lower Cranial Nerve Neuropathy by Endoscopic Endonasal Approach: A Systematic Review. Diagnostics 2022, 12, 2145. https://doi.org/10.3390/diagnostics12092145
Huang S-H, Chuang C-C, Huang C-C, Jung S-M, Lee C-C. Diagnosis and Treatment of Inflammatory Pseudotumor with Lower Cranial Nerve Neuropathy by Endoscopic Endonasal Approach: A Systematic Review. Diagnostics. 2022; 12(9):2145. https://doi.org/10.3390/diagnostics12092145
Chicago/Turabian StyleHuang, Sheng-Han, Chi-Cheng Chuang, Chien-Chia Huang, Shih-Ming Jung, and Cheng-Chi Lee. 2022. "Diagnosis and Treatment of Inflammatory Pseudotumor with Lower Cranial Nerve Neuropathy by Endoscopic Endonasal Approach: A Systematic Review" Diagnostics 12, no. 9: 2145. https://doi.org/10.3390/diagnostics12092145






