Flow-Field Inference for Turbulent Exhale Flow Measurement
Abstract
1. Introduction
2. Related Work
3. Materials and Methods
3.1. Data Acquisition
3.2. Automated Tracking
3.3. Flow Field Generation
3.4. Signal Generation
3.5. Flow Field Modeling
3.6. Flow Field Encoding
3.7. Dataset Creation
3.8. Augmentation
3.9. Model Architecture
3.10. Training
3.11. Flow-Field Interpolation
3.12. Exhale Measures and Unique Signatures
3.13. Exhale Episode Anomaly Detection
3.14. Exhale Segmentation
3.15. Filtering Model
3.16. Anomaly Model
4. Results
4.1. Localized Exhale Flow Prediction
4.2. Individualized Exhale Behaviors
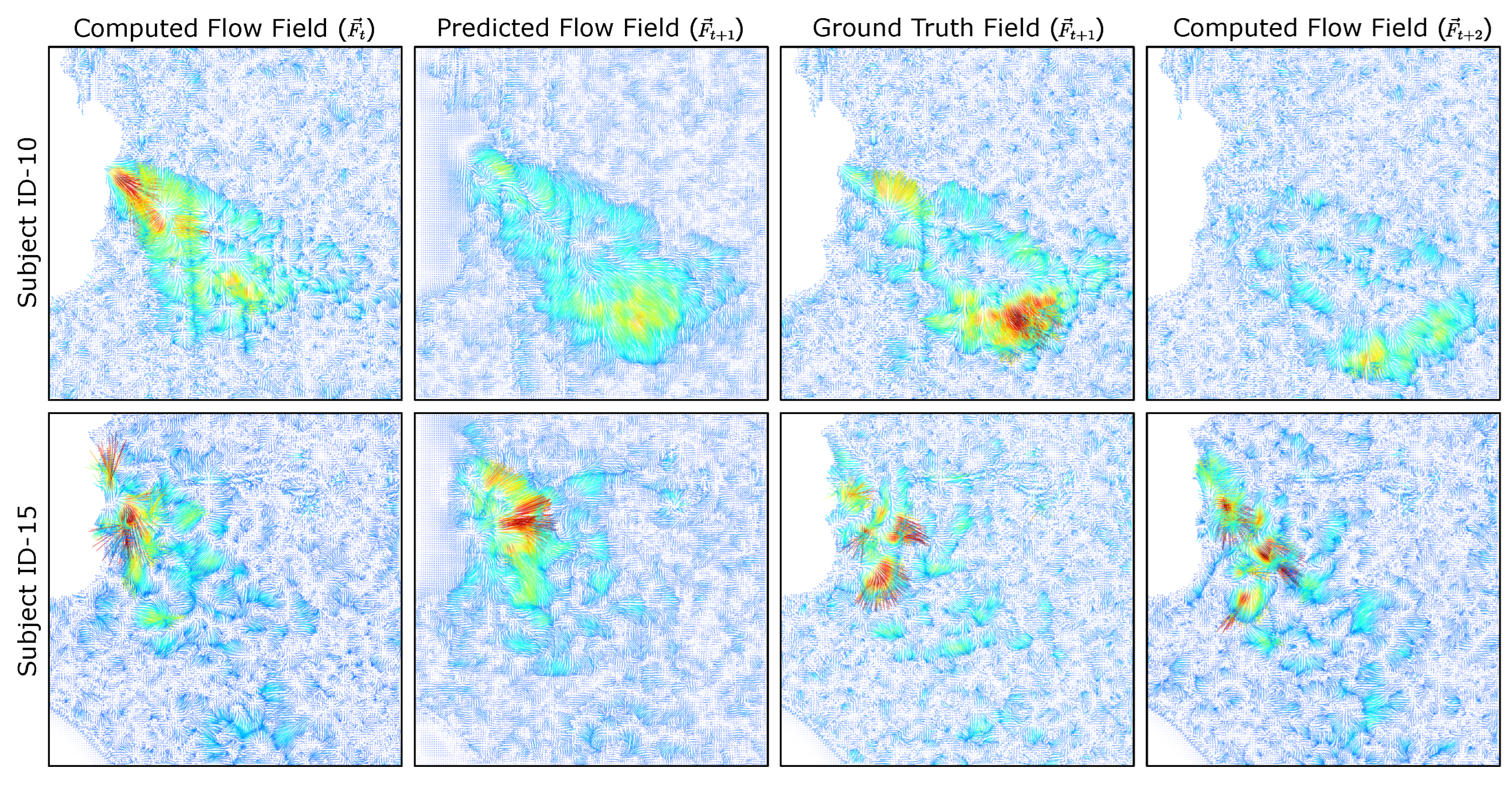

4.3. Anomaly Model Predictions
5. Discussion
6. Future Developments
7. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Lopes, A.J. Advances in spirometry testing for lung function analysis. Expert Rev. Respir. Med. 2019, 13, 559–569. [Google Scholar] [CrossRef] [PubMed]
- Pierce, R. Spirometry: An essential clinical measurement. Aust. Fam. Physician 2005, 34, 535–539. [Google Scholar] [PubMed]
- Barreiro, T.J.; Perillo, I. An approach to interpreting spirometry. Am. Fam. Physician 2004, 69, 1107–1114. [Google Scholar] [PubMed]
- Criée, C.; Sorichter, S.; Smith, H.; Kardos, P.; Merget, R.; Heise, D.; Berdel, D.; Köhler, D.; Magnussen, H.; Marek, W.; et al. Body plethysmography—Its principles and clinical use. Respir. Med. 2011, 105, 959–971. [Google Scholar] [CrossRef] [PubMed]
- Coates, A.; Peslin, R.; Rodenstein, D.; Stocks, J. Measurement of lung volumes by plethysmography. Eur. Respir. J. 1997, 10, 1415–1427. [Google Scholar] [CrossRef] [PubMed]
- Sun, X.; Yang, W.; Gong, S.; Liang, S.; Gu, S.; Lu, H.; Liu, J.; Xu, J. Diagnostic value of volumetric capnography in patients with chronic cough variant asthma. Clinics 2020, 75, e1662. [Google Scholar] [CrossRef] [PubMed]
- Abid, A.; Mieloszyk, R.J.; Verghese, G.C.; Krauss, B.S.; Heldt, T. Model-Based Estimation of Respiratory Parameters from Capnography, with Application to Diagnosing Obstructive Lung Disease. IEEE Trans. Biomed. Eng. 2017, 64, 2957–2967. [Google Scholar] [PubMed]
- John, R.E.S. End-Tidal Carbon Dioxide Monitoring. Crit. Care Nurse 2003, 23, 83–88. [Google Scholar] [CrossRef]
- Bhandary, A.; Prabhu, G.A.; Rajinikanth, V.; Thanaraj, K.P.; Satapathy, S.C.; Robbins, D.E.; Shasky, C.; Zhang, Y.D.; Tavares, J.M.R.; Raja, N.S.M. Deep-learning framework to detect lung abnormality—A study with chest X-Ray and lung CT scan images. Pattern Recognit. Lett. 2020, 129, 271–278. [Google Scholar] [CrossRef]
- Hu, S.; Hoffman, E.; Reinhardt, J. Automatic lung segmentation for accurate quantitation of volumetric X-ray CT images. IEEE Trans. Med. Imaging 2001, 20, 490–498. [Google Scholar] [CrossRef]
- Romei, C.; Turturici, L.; Tavanti, L.; Miedema, J.; Fiorini, S.; Marletta, M.; Wielopolski, P.; Tiddens, H.; Falaschi, F.; Ciet, P. The use of chest magnetic resonance imaging in interstitial lung disease: A systematic review. Eur. Respir. Rev. 2018, 27, 180062. [Google Scholar] [CrossRef]
- Frood, R.; Prestwich, R.; Tsoumpas, C.; Murray, P.; Franks, K.; Scarsbrook, A. Effectiveness of Respiratory-gated Positron Emission Tomography/Computed Tomography for Radiotherapy Planning in Patients with Lung Carcinoma—A Systematic Review. Clin. Oncol. 2018, 30, 225–232. [Google Scholar] [CrossRef]
- Zhu, Z.; Fei, J.; Pavlidis, I. Tracking human breath in infrared imaging. In Proceedings of the Fifth IEEE Symposium on Bioinformatics and Bioengineering (BIBE 2005), Minneapolis, MN, USA, 19–21 October 2005; IEEE: Piscataway, NJ, USA, 2005; pp. 227–231. [Google Scholar]
- Murthy, R.; Pavlidis, I.; Tsiamyrtzis, P. Touchless monitoring of breathing function. In Proceedings of the 26th Annual International Conference of the IEEE Engineering in Medicine and Biology Society, San Francisco, CA, USA, 1–5 September 2004; pp. 1196–1199. [Google Scholar]
- Kakavas, S.; Kotsiou, O.S.; Perlikos, F.; Mermiri, M.; Mavrovounis, G.; Gourgoulianis, K.; Pantazopoulos, I. Pulmonary function testing in COPD: Looking beyond the curtain of FEV1. NPJ Prim. Care Respir. Med. 2021, 31, 23. [Google Scholar] [CrossRef] [PubMed]
- Tomasic, I.; Tomasic, N.; Trobec, R.; Krpan, M.; Kelava, T. Continuous remote monitoring of COPD patients—Justification and explanation of the requirements and a survey of the available technologies. Med. Biol. Eng. Comput. 2018, 56, 547–569. [Google Scholar] [CrossRef]
- Lecompte-Osorio, P.; Pearson, S.D.; Pieroni, C.H.; Stutz, M.R.; Pohlman, A.S.; Lin, J.; Hall, J.B.; Htwe, Y.M.; Belvitch, P.G.; Dudek, S.M.; et al. Bedside estimates of dead space using end-tidal CO2 are independently associated with mortality in ARDS. Crit. Care 2021, 25, 333. [Google Scholar] [CrossRef]
- Li, X.; Ma, X. Acute respiratory failure in COVID-19: Is it “typical” ARDS? Crit. Care 2020, 24, 198. [Google Scholar] [CrossRef]
- Masclans, J.R.; Roca, O.; Muñoz, X.; Pallisa, E.; Torres, F.; Rello, J.; Morell, F. Quality of Life, Pulmonary Function, and Tomographic Scan Abnormalities After ARDS. Chest 2011, 139, 1340–1346. [Google Scholar] [CrossRef] [PubMed]
- An, J.Y.; Shin, H.J.; Yang, M.; Park, D.-Y.; Yang, J.; Kim, H.J. Non-contact diagnosis of sleep breathing disorders using infrared optical gas imaging: A prospective observational study. Sci. Rep. 2022, 12, 21052. [Google Scholar] [CrossRef] [PubMed]
- Jakkaew, P.; Onoye, T. Non-Contact Respiration Monitoring and Body Movements Detection for Sleep Using Thermal Imaging. Sensors 2020, 20, 6307. [Google Scholar] [CrossRef]
- Verwey, C.; Nunes, M.C.; Dangor, Z.; Madhi, S.A. Pulmonary function sequelae after respiratory syncytial virus lower respiratory tract infection in children: A systematic review. Pediatr. Pulmonol. 2020, 55, 1567–1583. [Google Scholar] [CrossRef]
- Ronneberger, O.; Fischer, P.; Brox, T. U-Net: Convolutional Networks for Biomedical Image Segmentation. arXiv 2015, arXiv:1505.04597. [Google Scholar]
- Fischer, P.; Dosovitskiy, A.; Ilg, E.; Häusser, P.; Hazirbas, C.; Golkov, V.; van der Smagt, P.; Cremers, D.; Brox, T. FlowNet: Learning Optical Flow with Convolutional Networks. arXiv 2015, arXiv:1504.06852. [Google Scholar]
- Horn, B.K.; Schunck, B.G. Determining optical flow. Artif. Intell. 1981, 17, 185–203. [Google Scholar] [CrossRef]
- Costanzo, I.; Sen, D.; Rhein, L.; Guler, U. Respiratory Monitoring: Current State of the Art and Future Roads. IEEE Rev. Biomed. Eng. 2022, 15, 103–121. [Google Scholar] [CrossRef] [PubMed]
- Massaroni, C.; Nicolò, A.; Sacchetti, M.; Schena, E. Contactless Methods For Measuring Respiratory Rate: A Review. IEEE Sens. J. 2021, 21, 12821–12839. [Google Scholar] [CrossRef]
- Vanegas, E.; Igual, R.; Plaza, I. Sensing Systems for Respiration Monitoring: A Technical Systematic Review. Sensors 2020, 20, 5446. [Google Scholar] [CrossRef] [PubMed]
- Fekr, A.R.; Radecka, K.; Zilic, Z. Design and Evaluation of an Intelligent Remote Tidal Volume Variability Monitoring System in e-Health Applications. IEEE J. Biomed. Health Informatics 2015, 19, 1532–1548. [Google Scholar] [CrossRef] [PubMed]
- Folke, M.; Cernerud, L.; Ekström, M.; Hök, B. Critical review of non-invasive respiratory monitoring in medical care. Med Biol. Eng. Comput. 2003, 41, 377–383. [Google Scholar] [CrossRef] [PubMed]
- Lucidarme, O.; Coche, E.; Cluzel, P.; Mourey-Gerosa, I.; Howarth, N.; Grenier, P. Expiratory CT scans for chronic airway disease: Correlation with pulmonary function test results. Am. J. Roentgenol. 1998, 170, 301–307. [Google Scholar] [CrossRef]
- Sharma, P.; Hui, X.; Zhou, J.; Conroy, T.B.; Kan, E.C. Wearable radio-frequency sensing of respiratory rate, respiratory volume, and heart rate. npj Digit. Med. 2020, 3, 98. [Google Scholar] [CrossRef]
- Piuzzi, E.; Pisa, S.; Pittella, E.; Podestà, L.; Sangiovanni, S. Wearable Belt With Built-In Textile Electrodes for Cardio—Respiratory Monitoring. Sensors 2020, 20, 4500. [Google Scholar] [CrossRef] [PubMed]
- Vitazkova, D.; Foltan, E.; Kosnacova, H.; Micjan, M.; Donoval, M.; Kuzma, A.; Kopani, M.; Vavrinsky, E. Advances in Respiratory Monitoring: A Comprehensive Review of Wearable and Remote Technologies. Biosensors 2024, 14, 90. [Google Scholar] [CrossRef] [PubMed]
- Deepika, C.; Kandaswamy, A.; Pradeepa, G. An efficient method for detection of inspiration phase of respiration in thermal imaging. J. Sci. Ind. Res. 2016, 75, 40–44. [Google Scholar]
- Hanawa, D.; Ohguchi, T.; Oguchi, K. Basic study on non-contact measurement of human oral breathing by using far infra-red imaging. In Proceedings of the International Conference on Telecommunications and Signal Processing (TSP’16), Vienna, Austria, 27–29 June 2016; pp. 681–684. [Google Scholar]
- Abbas, A.K.; Leonhardt, S. Intelligent neonatal monitoring based on a virtual thermal sensor. BMC Med. Imaging 2014, 14, 9. [Google Scholar] [CrossRef] [PubMed]
- Murthy, J.; Van Jaarsveld, J.; Fei, J.; Pavlidis, I.; Harrykissoon, R.I.; Lucke, J.F.; Faiz, S.; Castriotta, R.J. Thermal Infrared Imaging: A Novel Method to Monitor Airflow during Polysomnography. Sleep 2009, 32, 1521–1527. [Google Scholar] [CrossRef]
- Chekmenev, S.; Rara, H.; Farag, A.A. Non-contact, wavelet-based measurement of vital signs using thermal imaging. In Proceedings of the First International Conference on Graphics, Vision, and Image Processing (GVIP), Cairo, Egypt, 19 December 2005; pp. 107–112. [Google Scholar]
- Adhikari, A.; Hetherington, A.; Sur, S. mmFlow: Facilitating At-Home Spirometry with 5G Smart Devices. In Proceedings of the IEEE (SECON’18), Rome, Italy, 6–9 July 2021; pp. 1–9. [Google Scholar]
- Hillyard, P.; Luong, A.; Abrar, A.S.; Patwari, N.; Sundar, K.; Farney, R.; Burch, J.; Porucznik, C.A.; Pollard, S.H. Comparing Respiratory Monitoring Performance of Commercial Wireless Devices. arXiv 2018, arXiv:1807.06767. [Google Scholar]
- Ponce, M.C.; Sankari, A.; Sharma, S. Pulmonary Function Tests; StatPearls Publishing: Treasure Island, FL, USA, 2023. [Google Scholar]
- Ohno, Y.; Seo, J.B.; Parraga, G.; Lee, K.S.; Gefter, W.B.; Fain, S.B.; Schiebler, M.L.; Hatabu, H. Pulmonary Functional Imaging: Part 1—State-of-the-Art Technical and Physiologic Underpinnings. Radiology 2021, 299, 508–523. [Google Scholar] [CrossRef]
- Gefter, W.B.; Lee, K.S.; Schiebler, M.L.; Parraga, G.; Seo, J.B.; Ohno, Y.; Hatabu, H. Pulmonary Functional Imaging: Part 2—State-of-the-Art Clinical Applications and Opportunities for Improved Patient Care. Radiology 2021, 299, 524–538. [Google Scholar] [CrossRef] [PubMed]
- Huang, Z.; Shi, X.; Zhang, C.; Wang, Q.; Cheung, K.C.; Qin, H.; Dai, J.; Li, H. FlowFormer: A Transformer Architecture for Optical Flow. In Proceedings of the Computer Vision—ECCV 2022; Avidan, S., Brostow, G., Cissé, M., Farinella, G.M., Hassner, T., Eds.; Springer Nature: Cham, Switzerland, 2022; pp. 668–685. [Google Scholar]
- Lin, K.Y.; Chen, D.Y.; Tsai, W.J. Image-based motion-tolerant remote respiratory rate evaluation. IEEE Sens. J. 2016, 16, 3263–3271. [Google Scholar] [CrossRef]
- He, S.; Han, Z.; Iglesias, C.; Mehta, V.; Bolic, M. A Real-Time Respiration Monitoring and Classification System Using a Depth Camera and Radars. Front. Physiol. 2022, 13, 799621. [Google Scholar] [CrossRef]
- Addison, A.P.; Addison, P.S.; Smit, P.; Jacquel, D.; Borg, U.R. Noncontact Respiratory Monitoring Using Depth Sensing Cameras: A Review of Current Literature. Sensors 2021, 21, 1135. [Google Scholar] [CrossRef] [PubMed]
- Maurya, L.; Zwiggelaar, R.; Chawla, D.; Mahapatra, P. Non-contact respiratory rate monitoring using thermal and visible imaging: A pilot study on neonates. J. Clin. Monit. Comput. 2023, 37, 815–828. [Google Scholar] [CrossRef] [PubMed]
- Manullang, M.C.T.; Lin, Y.H.; Lai, S.J.; Chou, N.K. Implementation of Thermal Camera for Non-Contact Physiological Measurement: A Systematic Review. Sensors 2021, 21, 7777. [Google Scholar] [CrossRef]
- Shu, S.; Liang, H.; Zhang, Y.; Zhang, Y.; Yang, Z. Non-contact measurement of human respiration using an infrared thermal camera and the deep learning method. Meas. Sci. Technol. 2022, 33, 075202. [Google Scholar] [CrossRef]
- Yang, F.; He, S.; Sadanand, S.; Yusuf, A.; Bolic, M. Contactless Measurement of Vital Signs Using Thermal and RGB Cameras: A Study of COVID 19-Related Health Monitoring. Sensors 2022, 22, 627. [Google Scholar] [CrossRef] [PubMed]
- Takahashi, Y.; Gu, Y.; Nakada, T.; Abe, R.; Nakaguchi, T. Estimation of Respiratory Rate from Thermography Using Respiratory Likelihood Index. Sensors 2021, 21, 4406. [Google Scholar] [CrossRef] [PubMed]
- Jia, Y.; Du, H.; Wang, H.; Yu, R.; Fan, L.; Xu, G.; Zhang, Q. Automatic early Smoke Segmentation Based on Conditional Generative Adversarial Networks. Optik 2019, 193, 162879. [Google Scholar] [CrossRef]
- Martins, L.; Guede-Fernández, F.; Valente de Almeida, R.; Gamboa, H.; Vieira, P. Real-Time Integration of Segmentation Techniques for Reduction of False Positive Rates in Fire Plume Detection Systems during Forest Fires. Remote Sens. 2022, 14, 2701. [Google Scholar] [CrossRef]
- Nguyen, A.Q.; Nguyen, H.T.; Tran, V.C.; Pham, H.X.; Pestana, J. A Visual Real-Time Fire Detection Using Single Shot MultiBox Detector for UAV-Based Fire Surveillance. In Proceedings of the 2020 IEEE Eighth International Conference on Communications and Electronics (ICCE), Phu Quoc, Vietnam, 13–15 January 2021; pp. 338–343. [Google Scholar]
- Saponara, S.; Elhanashi, A.; Gagliardi, A. Real-time video fire/smoke detection based on CNN in antifire surveillance systems. J. Real-Time Image Process. 2021, 18, 889–900. [Google Scholar] [CrossRef]
- Guo, Y.; Cao, X.; Liu, B.; Gao, M. Cloud Detection for Satellite Imagery Using Attention-Based U-Net Convolutional Neural Network. Symmetry 2020, 12, 1056. [Google Scholar] [CrossRef]
- Xie, W.; Liu, D.; Yang, M.; Chen, S.; Wang, B.; Wang, Z.; Xia, Y.; Liu, Y.; Wang, Y.; Zhang, C. SegCloud: A novel cloud image segmentation model using a deep convolutional neural network for ground-based all-sky-view camera observation. Atmos. Meas. Tech. 2020, 13, 1953–1961. [Google Scholar] [CrossRef]
- Kopaczka, M.; Breuer, L.; Schock, J.; Merhof, D. A Modular System for Detection, Tracking and Analysis of Human Faces in Thermal Infrared Recordings. Sensors 2019, 19, 4135. [Google Scholar] [CrossRef]
- Setjo, C.H.; Achmad, B. Thermal image human detection using Haar-cascade classifier. In Proceedings of the 2017 7th International Annual Engineering Seminar (InAES), Yogyakarta, Indonesia, 1–2 August 2017; pp. 1–6. [Google Scholar]
- Lucas, B.D.; Kanade, T. An iterative image registration technique with an application to stereo vision. In Proceedings of the 7th International Joint Conference on Artificial Intelligence, San Francisco, CA, USA, 28 August 1981; IJCAI’81. Volume 2, pp. 674–679. [Google Scholar]
- Alvarez, L.; Weickert, J.; Sánchez, J. Reliable Estimation of Dense Optical Flow Fields with Large Displacements. Int. J. Comput. Vis. 2000, 39, 41–56. [Google Scholar] [CrossRef]
- Sobel, I. An Isotropic 3 × 3 Image Gradient Operator. In Presentation at Stanford A.I. Project 1968; Academic Press: Cambridge, MA, USA, 2014. [Google Scholar]
- Jakob, W.; Rhinelander, J.; Moldovan, D. Github: PyBind11. Available online: https://github.com/pybind/pybind11 (accessed on 31 May 2024).
- Fortun, D.; Bouthemy, P.; Kervrann, C. Optical flow modeling and computation: A survey. Comput. Vis. Image Underst. 2015, 134, 1–21. [Google Scholar] [CrossRef]
- Chollet, F. Keras: Deep Learning for Humans. Software. 2015. Available online: https://keras.io (accessed on 31 May 2024).
- Abadi, M.; Agarwal, A.; Barham, P.; Brevdo, E.; Chen, Z.; Citro, C.; Corrado, G.S.; Davis, A.; Dean, J.; Devin, M.; et al. TensorFlow: Large-Scale Machine Learning on Heterogeneous Systems. Software. 2015. Available online: https://tensorflow.org (accessed on 31 May 2024).
- Kingma, D.; Ba, J. Adam: A Method for Stochastic Optimization. arXiv 2014, arXiv:1412.6980. [Google Scholar]
- Golgowski, M.; Osowski, S. Anomaly detection in ECG using wavelet transformation. In Proceedings of the 2020 IEEE 21st International Conference on Computational Problems of Electrical Engineering (CPEE’20), Online, 16–19 September 2020; pp. 1–4. [Google Scholar]














Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Transue, S.; Lee, D.-k.; Choi, J.-S.; Choi, S.; Hong, M.; Choi, M.-H. Flow-Field Inference for Turbulent Exhale Flow Measurement. Diagnostics 2024, 14, 1596. https://doi.org/10.3390/diagnostics14151596
Transue S, Lee D-k, Choi J-S, Choi S, Hong M, Choi M-H. Flow-Field Inference for Turbulent Exhale Flow Measurement. Diagnostics. 2024; 14(15):1596. https://doi.org/10.3390/diagnostics14151596
Chicago/Turabian StyleTransue, Shane, Do-kyeong Lee, Jae-Sung Choi, Seongjun Choi, Min Hong, and Min-Hyung Choi. 2024. "Flow-Field Inference for Turbulent Exhale Flow Measurement" Diagnostics 14, no. 15: 1596. https://doi.org/10.3390/diagnostics14151596
APA StyleTransue, S., Lee, D.-k., Choi, J.-S., Choi, S., Hong, M., & Choi, M.-H. (2024). Flow-Field Inference for Turbulent Exhale Flow Measurement. Diagnostics, 14(15), 1596. https://doi.org/10.3390/diagnostics14151596




