The Association of Heart Failure and Liver T1 Mapping in Cardiac Magnetic Resonance Imaging
Abstract
:1. Introduction
2. Materials/Methods
2.1. Primary Study Population
2.2. Baseline Evaluation
2.3. Cardiac Magnetic Resonance Imaging Protocol
2.4. Echocardiography Analysis
2.5. Cardiac MRI Analysis
2.6. Statistical Analysis
3. Results
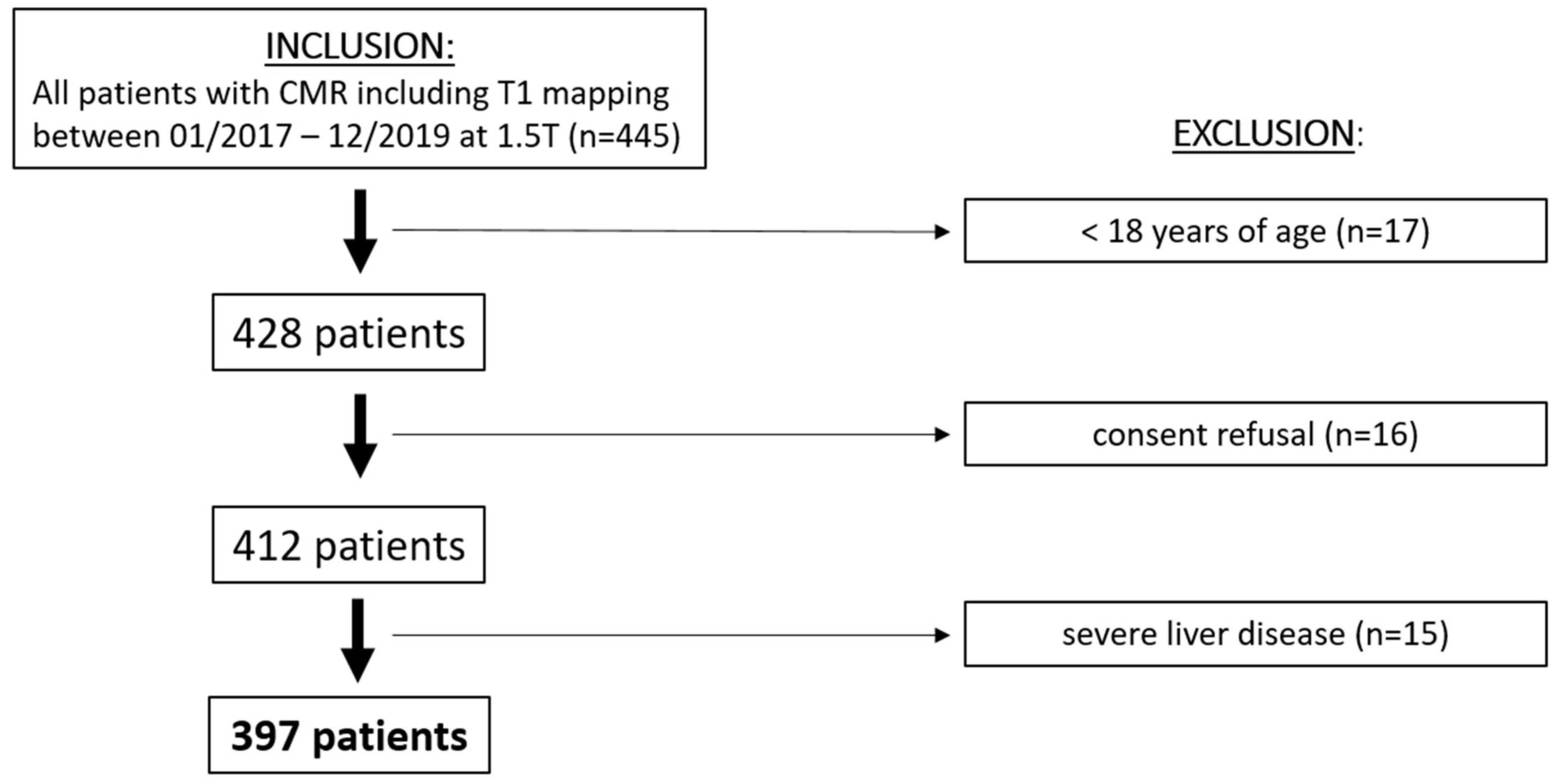
3.1. Final Study Population
3.2. Association of Cardiac MRI and Echocardiography Imaging Parameters with NT-proBNP
3.3. Association of Liver T1 and T2 with NT-proBNP
3.4. Predictive Value of Liver T1 to Determine Elevated NT-proBNP
4. Discussion
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| ALAT | Alanine aminotransferase |
| ASAT | Aspartate aminotransferase |
| BMI | Body mass index |
| CMR | Cardiac magnetic resonance |
| CLD | Chronic liver disease |
| TDI | Tissue Doppler imaging |
| E/A | Mitral inflow early-to-late diastolic flow ratio |
| E’ | Peak early diastolic tissue velocity of mitral annulus |
| ECV | Extracellular volume |
| EF | Ejection fraction |
| GLS | Global longitudinal strain |
| DCM | Dilated cardiomyopathy |
| LAVI | Left atrial volume index |
| MRI | Magnetic resonance imaging |
| NT-proBNP | N-terminal pro-Brain natriuretic peptide |
| NYHA | New York Heart Association |
| ROI | Region of interest |
| RV S’ | Tissue Doppler peak systolic velocity at RV lateral annulus |
| TAPSE | Tricuspid annular plane systolic excursion |
References
- Gonzalez, J.A.; Kramer, C.M. Role of Imaging Techniques for Diagnosis, Prognosis and Management of Heart Failure Patients: Cardiac Magnetic Resonance. Curr. Heart Fail. Rep. 2015, 12, 276–283. [Google Scholar] [CrossRef] [PubMed]
- Møller, J.E.; Pellikka, P.A.; Hillis, G.S.; Oh, J.K. Prognostic importance of diastolic function and filling pressure in patients with acute myocardial infarction. Circulation 2006, 114, 438–444. [Google Scholar] [CrossRef] [PubMed]
- Miyaji, Y.; Iwanaga, Y.; Nakamura, T.; Yasuda, M.; Kawamura, T.; Miyazaki, S. Interrelationship between the Myocardial Mass, Fibrosis, BNP, and Clinical Outcomes in Hypertrophic Cardiomyopathy. Intern. Med. 2016, 55, 1261–1268. [Google Scholar] [CrossRef]
- Katz, D.H.; Beussink, L.; Sauer, A.J.; Freed, B.H.; Burke, M.A.; Shah, S.J. Prevalence, clinical characteristics, and outcomes associated with eccentric versus concentric left ventricular hypertrophy in heart failure with preserved ejection fraction. Am. J. Cardiol. 2013, 112, 1158–1164. [Google Scholar] [CrossRef]
- Magnani, J.W.; Danik, H.J.; Dec, G.W., Jr.; DiSalvo, T.G. Survival in biopsy-proven myocarditis: A long-term retrospective analysis of the histopathologic, clinical, and hemodynamic predictors. Am. Heart J. 2006, 151, 463–470. [Google Scholar] [CrossRef]
- Dahl, J.S.; Videbæk, L.; Poulsen, M.K.; Pellikka, P.A.; Veien, K.; Andersen, L.I.; Haghfelt, T.; Møller, J.E. Noninvasive assessment of filling pressure and left atrial pressure overload in severe aortic valve stenosis: Relation to ventricular remodeling and clinical outcome after aortic valve replacement. J. Thorac. Cardiovasc. Surg. 2011, 142, e77–e83. [Google Scholar] [CrossRef]
- Bredfelt, A.; Rådegran, G.; Hesselstrand, R.; Arheden, H.; Ostenfeld, E. Increased right atrial volume measured with cardiac magnetic resonance is associated with worse clinical outcome in patients with pre-capillary pulmonary hypertension. ESC Heart Fail. 2018, 5, 864–875. [Google Scholar] [CrossRef]
- Weber, M.; Hamm, C. Role of B-type natriuretic peptide (BNP) and NT-proBNP in clinical routine. Heart 2006, 92, 843–849. [Google Scholar] [CrossRef]
- de Lemos, J.A.; McGuire, D.K.; Drazner, M.H. B-type natriuretic peptide in cardiovascular disease. Lancet 2003, 362, 316–322. [Google Scholar] [CrossRef]
- Palazzuoli, A.; Gallotta, M.; Quatrini, I.; Nuti, R. Natriuretic peptides (BNP and NT-proBNP): Measurement and relevance in heart failure. Vasc. Health Risk Manag. 2010, 6, 411–418. [Google Scholar] [CrossRef]
- Dokainish, H. Combining tissue Doppler echocardiography and B-type natriuretic peptide in the evaluation of left ventricular filling pressures: Review of the literature and clinical recommendations. Can. J. Cardiol. 2007, 23, 983–989. [Google Scholar] [CrossRef] [PubMed]
- Seemann, F.; Baldassarre, L.A.; Llanos-Chea, F.; Gonzales, R.A.; Grunseich, K.; Hu, C.; Sugeng, L.; Meadows, J.; Heiberg, E.; Peters, D.C. Assessment of diastolic function and atrial remodeling by MRI—Validation and correlation with echocardiography and filling pressure. Physiol. Rep. 2018, 6, e13828. [Google Scholar] [CrossRef] [PubMed]
- Nauta, J.F.; Hummel, Y.M.; van der Meer, P.; Lam, C.S.P.; Voors, A.A.; van Melle, J.P. Correlation with invasive left ventricular filling pressures and prognostic relevance of the echocardiographic diastolic parameters used in the 2016 ESC heart failure guidelines and in the 2016 ASE/EACVI recommendations: A systematic review in patients with heart failure with preserved ejection fraction. Eur. J. Heart Fail. 2018, 20, 1303–1311. [Google Scholar] [CrossRef] [PubMed]
- Andersen, O.S.; Smiseth, O.A.; Dokainish, H.; Abudiab, M.M.; Schutt, R.C.; Kumar, A.; Sato, K.; Harb, S.; Gude, E.; Remme, E.W.; et al. Estimating Left Ventricular Filling Pressure by Echocardiography. J. Am. Coll. Cardiol. 2017, 69, 1937–1948. [Google Scholar] [CrossRef]
- Puntmann, V.O.; Peker, E.; Chandrashekhar, Y.; Nagel, E. T1 Mapping in Characterizing Myocardial Disease: A Comprehensive Review. Circ. Res. 2016, 119, 277–299. [Google Scholar] [CrossRef]
- Fischer, K.; Guensch, D.P.; Jung, B.; King, I.; von Tengg-Kobligk, H.; Giannetti, N.; Eberle, B.; Friedrich, M.G. Insights Into Myocardial Oxygenation and Cardiovascular Magnetic Resonance Tissue Biomarkers in Heart Failure With Preserved Ejection Fraction. Circ. Heart Fail. 2022, 15, e008903. [Google Scholar] [CrossRef]
- Duca, F.; Zotter-Tufaro, C.; Kammerlander, A.A.; Panzenböck, A.; Aschauer, S.; Dalos, D.; Köll, B.; Börries, B.; Agis, H.; Kain, R.; et al. Cardiac extracellular matrix is associated with adverse outcome in patients with chronic heart failure. Eur. J. Heart Fail. 2017, 19, 502–511. [Google Scholar] [CrossRef]
- Kavoliuniene, A.; Vaitiekiene, A.; Cesnaite, G. Congestive hepatopathy and hypoxic hepatitis in heart failure: A cardiologist’s point of view. Int. J. Cardiol. 2013, 166, 554–558. [Google Scholar] [CrossRef]
- Weisberg, I.S.; Jacobson, I.M. Cardiovascular diseases and the liver. Clin. Liver Dis. 2011, 15, 1–20. [Google Scholar] [CrossRef]
- Giallourakis, C.C.; Rosenberg, P.M.; Friedman, L.S. The liver in heart failure. Clin. Liver Dis. 2002, 6, 947–967. [Google Scholar] [CrossRef]
- Alvarez, A.M.; Mukherjee, D. Liver abnormalities in cardiac diseases and heart failure. Int. J. Angiol. 2011, 20, 135–142. [Google Scholar] [CrossRef]
- Taniguchi, T.; Ohtani, T.; Kioka, H.; Tsukamoto, Y.; Onishi, T.; Nakamoto, K.; Katsimichas, T.; Sengoku, K.; Chimura, M.; Hashimoto, H.; et al. Liver Stiffness Reflecting Right-Sided Filling Pressure Can Predict Adverse Outcomes in Patients With Heart Failure. JACC Cardiovasc. Imaging 2019, 12, 955–964. [Google Scholar] [CrossRef] [PubMed]
- Muthupillai, R.; Lomas, D.J.; Rossman, P.J.; Greenleaf, J.F.; Manduca, A.; Ehman, R.L. Magnetic resonance elastography by direct visualization of propagating acoustic strain waves. Science 1995, 269, 1854–1857. [Google Scholar] [CrossRef] [PubMed]
- Huber, A.T.; Razakamanantsoa, L.; Lamy, J.; Giron, A.; Cluzel, P.; Kachenoura, N.; Redheuil, A. Multiparametric Differentiation of Idiopathic Dilated Cardiomyopathy With and Without Congestive Heart Failure by Means of Cardiac and Hepatic T1-Weighted MRI Mapping. AJR Am. J. Roentgenol. 2020, 215, 79–86. [Google Scholar] [CrossRef]
- McDonagh, T.A.; Metra, M.; Adamo, M.; Gardner, R.S.; Baumbach, A.; Böhm, M.; Burri, H.; Butler, J.; Čelutkienė, J.; Chioncel, O.; et al. 2021 ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure. Eur. Heart J. 2021, 42, 3599–3726. [Google Scholar] [CrossRef]
- Nagueh, S.F.; Smiseth, O.A.; Appleton, C.P.; Byrd, B.F., 3rd; Dokainish, H.; Edvardsen, T.; Flachskampf, F.A.; Gillebert, T.C.; Klein, A.L.; Lancellotti, P.; et al. Recommendations for the Evaluation of Left Ventricular Diastolic Function by Echocardiography: An Update from the American Society of Echocardiography and the European Association of Cardiovascular Imaging. J. Am. Soc. Echocardiogr. 2016, 29, 277–314. [Google Scholar] [CrossRef]
- Ostovaneh, M.R.; Ambale-Venkatesh, B.; Fuji, T.; Bakhshi, H.; Shah, R.; Murthy, V.L.; Tracy, R.P.; Guallar, E.; Wu, C.O.; Bluemke, D.A.; et al. Association of Liver Fibrosis With Cardiovascular Diseases in the General Population: The Multi-Ethnic Study of Atherosclerosis (MESA). Circ. Cardiovasc. Imaging 2018, 11, e007241. [Google Scholar] [CrossRef]
- Mascherbauer, K.; Donà, C.; Koschutnik, M.; Dannenberg, V.; Nitsche, C.; Duca, F.; Heitzinger, G.; Halavina, K.; Steinacher, E.; Kronberger, C.; et al. Hepatic T1-Time Predicts Cardiovascular Risk in All-Comers Referred for Cardiovascular Magnetic Resonance: A Post-Hoc Analysis. Circ. Cardiovasc. Imaging 2022, 15, e014716. [Google Scholar] [CrossRef]
- Langguth, P.; Ravesh, M.S.; Moritz, J.D.; Rinne, K.; Harneit, P.L.; Khodami, J.K.; Graessner, J.; Uebing, A.; Jansen, O.; Both, M.; et al. Non-contrast enhanced magnetic resonance imaging for characterization of Fontan associated liver disease. Int. J. Cardiol. 2021, 349, 48–54. [Google Scholar] [CrossRef]
- Ide, Y.; Gabbert, D.D.; Hansen, J.H.; Uebing, A.; Voges, I. Liver T1 mapping in Fontan patients and patients with biventricular congenital heart disease—Insights into the effects of venous congestions on diffuse liver disease. Int. J. Cardiovasc. Imaging 2025, 4, 347–358. [Google Scholar] [CrossRef]
- Obmann, V.C.; Mertineit, N.; Marx, C.; Berzigotti, A.; Ebner, L.; Heverhagen, J.T.; Christe, A.; Huber, A.T. Liver MR relaxometry at 3T—Segmental normal T(1) and T(2)* values in patients without focal or diffuse liver disease and in patients with increased liver fat and elevated liver stiffness. Sci. Rep. 2019, 9, 8106. [Google Scholar] [CrossRef] [PubMed]
- Gottbrecht, M.; Kramer, C.M.; Salerno, M. Native T1 and Extracellular Volume Measurements by Cardiac MRI in Healthy Adults: A Meta-Analysis. Radiology 2019, 290, 317–326. [Google Scholar] [CrossRef] [PubMed]
- Moon, J.C.; Messroghli, D.R.; Kellman, P.; Piechnik, S.K.; Robson, M.D.; Ugander, M.; Gatehouse, P.D.; Arai, A.E.; Friedrich, M.G.; Neubauer, S.; et al. Myocardial T1 mapping and extracellular volume quantification: A Society for Cardiovascular Magnetic Resonance (SCMR) and CMR Working Group of the European Society of Cardiology consensus statement. J. Cardiovasc. Magn. Reson. 2013, 15, 92. [Google Scholar] [CrossRef] [PubMed]
- Meloni, A.; Martini, N.; Positano, V.; D’Angelo, G.; Barison, A.; Todiere, G.; Grigoratos, C.; Barra, V.; Pistoia, L.; Gargani, L.; et al. Myocardial T1 Values at 1.5 T: Normal Values for General Electric Scanners and Sex-Related Differences. J. Magn. Reson. Imaging 2021, 54, 1486–1500. [Google Scholar] [CrossRef]
- van Kimmenade, R.R.; Januzzi, J.L., Jr.; Bakker, J.A.; Houben, A.J.; Rennenberg, R.; Kroon, A.A.; Crijns, H.J.; van Dieijen-Visser, M.P.; de Leeuw, P.W.; Pinto, Y.M. Renal clearance of B-type natriuretic peptide and amino terminal pro-B-type natriuretic peptide a mechanistic study in hypertensive subjects. J. Am. Coll. Cardiol. 2009, 53, 884–890. [Google Scholar] [CrossRef]
- Bartkowiak, J.; Peters, A.; Seitz, R.; Bernhard, B.; Praz, F.; Graeni, C.; Brugger, N.; Huber, A. Association of heart failure and liver T1 mapping in cardiac magnetic resonance imaging. Eur. Heart J. 2022, 43, ehac544.295. [Google Scholar] [CrossRef]

| Characteristic | Total [n = 397] | Normal NT-proBNP [n = 259] | Elevated NT-proBNP a [n = 138] | p-Value b |
|---|---|---|---|---|
| Age (years) | 56 [37–69] | 53 [33–75] | 61 [51–75] | <0.001 |
| Females (n, %) | 127 [32.0%] | 89 [34.4%] | 40 [29.0%] | 0.313 |
| BMI (kg/m2) | 25 [23–28] | 25 [22–28] | 25 [23–29] | 0.532 |
| Arterial hypertension (n, %) | 196 [49.4%] | 126 [48.6%] | 70 [50.7%] | 0.752 |
| LVEF (%) | 59 [50–63] | 60 [56–64] | 50 [34–62] | <0.001 |
| Pulmonary hypertension (n, %) | 15 [3.8%] | 3 [1.2%] | 12 [8.7%] | <0.001 |
| Atrial fibrillation (n, %) | 37 [9.3%] | 15 [5.8%] | 22 [15.9%] | 0.002 |
| Myocardial infarction (n, %) | 92 [23.3%] | 37 [14.3%] | 55 [39.9%] | <0.001 |
| Diabetes (n, %) | 62 [15.5%] | 23 [8.9%] | 38 [27.5%] | <0.001 |
| ASAT (U/L) | 31 [23–51] | 28 [21–44] | 33 [24–55] | 0.131 |
| ALAT (U/L) | 30 [21–60] | 28 [20–57] | 32 [21–68] | 0.323 |
| Albumin (g/L) | 35 [30–39] | 36 [32–41] | 35 [29–38] | 0.034 |
| CRP (mg/L) | 4 [1–19] | 2 [1–10] | 6 [1–30] | 0.002 |
| Creatinine (µmol/L) | 81 [68–98] | 77 [67–88] | 87 [74–109] | <0.001 |
| Hematocrit | 0.39 [0.36–0.42] | 0.40 [0.36–0.42] | 0.39 [0.35–0.42] | 0.453 |
| Parameter | All Patients [n = 397] | Normal NT-proBNP [n = 259] | Elevated NT-proBNP [n = 138] | p-Value |
|---|---|---|---|---|
| CMR | ||||
| LV EDV index (ml/m2) | 83 [71–99] | 81 [70–94] | 92 [72–112] | <0.001 |
| LV ESV index (ml/m2) | 34 [27–47] | 32 [26–39] | 41 [30–70] | <0.001 |
| LV mass index (g/m2) | 70 [59–83] | 67 [57–77] | 77 [62–93] | <0.001 |
| LVEF (%) | 59 [50–63] | 60 [56–64] | 50 [34–62] | <0.001 |
| RV EDV index (ml/m2) | 78 [64–91] | 78 [67–88] | 77 [54–97] | 0.629 |
| RV ESV index (ml/m2) | 31 [24–40] | 31 [24–37] | 32 [23–50] | 0.171 |
| RVEF (%) | 60 [54–64] | 60 [56–65] | 57 [48–63] | <0.001 |
| Echocardiography | All patients [n = 253] | Normal NT-proBNP [n = 113] | Elevated NT-proBNP [n = 140] | p-value |
| LAVI (ml/m2) | 30 [23–37] | 26 [20–33] | 35 [24–43] | <0.001 |
| E’ mean | 8 [6–11] | 9 [6–12] | 7 [5–9] | <0.001 |
| E/E’ mean | 9 [7–12] | 8 [7–10] | 11 [7–15] | <0.001 |
| RV/RA (mmHg) | 21 [14–27] | 20 [9–25] | 23 [17–33] | 0.011 |
| RAVI (ml/m2) | 26 [20–35] | 25 [20–31] | 29 [19–38] | 0.181 |
| GLS RV (%) | 16 [13–20] | 18 [14–21] | 14 [10–19] | 0.001 |
| VC diameter insp. (mm) | 8 [5–12] | 8 [6–12] | 7 [5–13] | 0.587 |
| VC diameter exp. (mm) | 18 [14–21] | 18 [14–21] | 17 [14–21] | 0.866 |
| Parameter | Normal NT-proBNP [n = 259] | Elevated NT-proBNP [n = 138] | p-Value |
|---|---|---|---|
| T1 relaxation time (ms) | |||
| Left lobe | 568 [530–606] | 571 [536–631] | 0.068 |
| Liver dome | 560 [533–595] | 590 [540–629] | 0.1 |
| Caudate lobe | 598 [578–633] | 664 [640–708] | <0.001 |
| Right lobe | 596 [568–628] | 670 [648–708] | <0.001 |
| T2 relaxation time (ms) | |||
| Left lobe | 50 [47–54] | 50 [46–54] | 0.525 |
| Liver dome | 53 [48–55] | 52 [50–55] | 0.920 |
| Caudate lobe | 52 [49–56] | 54 [47–58] | 0.572 |
| Right lobe | 52 [48–57] | 54 [50–60] | 0.228 |
| Normal LV filling pressure [n = 104] | Elevated LV filling pressure [n = 62] | p-value | |
| T1 relaxation time (ms) | |||
| Left lobe | 570 [532–616] | 583 [536–617] | 0.478 |
| Liver dome | 588 [536–624] | 565 [495–589] | 0.288 |
| Caudate lobe | 596 [572–621] | 654 [615–660] | 0.007 |
| Right lobe | 596 [565–625] | 639 [615–655] | 0.014 |
| VARIABLE | ODDS RATIO | 95% CONFIDENCE INTERVAL | p-VALUE |
|---|---|---|---|
| Hepatic T1 time | |||
| Left lobe | 1.003 | 1.000–1.006 | 0.056 |
| Liver dome | 1.007 | 0.999–1.016 | 0.098 |
| Caudate lobe | 1.016 | 1.007–1.025 | 0.001 |
| Right lobe | 1.015 | 1.007–1.023 | <0.001 |
| Age | 1.027 | 1.015–1.039 | <0.001 |
| LVEF | 0.938 | 0.921–0.955 | <0.001 |
| BMI | 1.025 | 0.990–1.061 | 0.158 |
| Gender | 1.283 | 0.819–2.008 | 0.276 |
| Atrial fibrillation | 3.085 | 1.544–6.166 | 0.001 |
| Creatinine | 1.003 | 0.998–1.008 | 0.241 |
| Multivariate Model 1 | |||
| T1 mapping caudate lobe | 1.013 | 1.004–1.023 | 0.005 |
| Age | 1.004 | 0.968–1.042 | 0.829 |
| Atrial fibrillation | 1.867 | 0.112–31.057 | 0.663 |
| LVEF | 0.958 | 0.915–1.003 | 0.067 |
| Multivariate Model 2 | |||
| T1 mapping right lobe | 1.012 | 1.003–1.021 | 0.009 |
| Age | 1.007 | 0.972–1.044 | 0.692 |
| Atrial fibrillation | 1.598 | 0.090–28.282 | 0.749 |
| LVEF | 0.965 | 0.922–1.009 | 0.119 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Huber, A.T.; Bartkowiak, J.; Seitz, R.; Bernhard, B.; Boscolo Berto, M.; Spano, G.; Wagner, B.; Obmann, V.C.; Ebner, L.; Todorski, I.A.S.; et al. The Association of Heart Failure and Liver T1 Mapping in Cardiac Magnetic Resonance Imaging. Diagnostics 2025, 15, 779. https://doi.org/10.3390/diagnostics15060779
Huber AT, Bartkowiak J, Seitz R, Bernhard B, Boscolo Berto M, Spano G, Wagner B, Obmann VC, Ebner L, Todorski IAS, et al. The Association of Heart Failure and Liver T1 Mapping in Cardiac Magnetic Resonance Imaging. Diagnostics. 2025; 15(6):779. https://doi.org/10.3390/diagnostics15060779
Chicago/Turabian StyleHuber, Adrian T., Joanna Bartkowiak, Robin Seitz, Benedikt Bernhard, Martina Boscolo Berto, Giancarlo Spano, Benedikt Wagner, Verena C. Obmann, Lukas Ebner, Inga A. S. Todorski, and et al. 2025. "The Association of Heart Failure and Liver T1 Mapping in Cardiac Magnetic Resonance Imaging" Diagnostics 15, no. 6: 779. https://doi.org/10.3390/diagnostics15060779
APA StyleHuber, A. T., Bartkowiak, J., Seitz, R., Bernhard, B., Boscolo Berto, M., Spano, G., Wagner, B., Obmann, V. C., Ebner, L., Todorski, I. A. S., Brönnimann, M. P., Fischer, K., Guensch, D. P., Christe, A., Berzigotti, A., Räber, L., Reichlin, T., Pilgrim, T., Praz, F., ... Peters, A. A. (2025). The Association of Heart Failure and Liver T1 Mapping in Cardiac Magnetic Resonance Imaging. Diagnostics, 15(6), 779. https://doi.org/10.3390/diagnostics15060779







