Abstract
The purpose of this review is to address some of the latest aspects regarding molecular features, pathogenic mechanisms, and immune system response to severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), based on recent publications in this field from March 2020 to May 2021. Interpretation keys for periodic re-emergence of coronavirus infections and other lethal viral pandemics are suggested. Antibody-dependent enhancement (ADE) and other potential mechanisms of immune system deception are put forward. Therefore, vaccine development must take into account ADE and other unwanted side effects of immune-based medical intervention. Features reported in our review will allow both clinicians and basic science researchers to take home ideas to improve their knowledge about SARS-CoV-2.
2. Pathogenesis and Different Organ Involvement
Unlike other respiratory viruses, CoVs are well-known to attach to the parenchymal region of the lung, besides the perihilar and stromal areas. This feature is very particular and should draw the attention of researchers to explain this using cellular and molecular mechanisms. The study by Zhou and co-workers has clarified this aspect by demonstrating that SARS-CoV-2 uses the angiotensin-converting enzyme 2 (ACE2) as a specific receptor among the alveolar cells, namely type II alveolar cells (AT2) [20]. Likewise, the pathway followed by SARS-CoV-2 to arrive in the lung alveoli has been elucidated in a recent paper evaluating a particular type of SARS-CoV-2 trans-membrane protease on bronchial cells, TMPRSS2 [21].
In its more severe forms, the clinical course of infection due to the new coronavirus shares many features with sepsis [22]. Among patients who display symptoms, the disease is mild in about 80% of cases, while it is severe or critical in 14% and 5% of patients, respectively [23,24]. Mild disease is characterized by the presence of a flu-like syndrome with fever, fatigue, dry cough, and myalgia. When dyspnea and hypoxia occur, the disease can be considered severe. It becomes critical when acute respiratory distress syndrome (ARDS), shock, or multiple organ dysfunction syndrome (MODS) are presented. Although the three most common symptoms of COVID-19 are fever (99%), fatigue (70%), and dry cough (59%) [25,26,27], it has also been reported that the presence of fever varies according to patient characteristics. Indeed, fever is often more frequent during hospitalization compared to actual hospital admission (89% vs. 44%) [28]. Other symptoms, such as choriza, headache, and enteric manifestations (nausea, vomiting, and diarrhea) may be present, even if in a minimal proportion of cases [27,29]. The occurrence of olfactory and gustatory dysfunctions has been recently reported as frequent symptoms in COVID-19 patients. In a study of 417 patients diagnosed with COVID-19, olfactory and gustatory dysfunctions were reported in 85.6% and 88.0% of patients respectively, with a significant association between both disorders [30]. Finally, neurological manifestations, such as acute cerebrovascular diseases, impaired consciousness, and skeletal muscle injury, have also been reported, especially in patients with a more severe clinical course of infection [31,32].
Aside from this clinical scenario, the association between the many sepsis-like mediators and the severe/late course of SARS-CoV-2 infections is intriguing. Such severe cases have been reported to be related to the enhancement of leucocyte and granulocyte numbers and increased concentrations of D-dimer [33].
It has been demonstrated that the expression of human ACE2 in different organs and tissues would be of relevance regarding clinical susceptibility and prognosis during SARS-CoV-2 infection. The single-cell RNA-seq analysis data suggest that Asian people showed a much higher ACE2 expression cell ratio than Caucasian and African-Americans. This experimental finding supports the different SARS-CoV-2 susceptibility among various human races and may account for the higher sensitivity of Asian people to the new coronavirus [34].
Although the apparent target of SARS-CoV-2 is the lung, research, from the beginning, has made evident the role played by different extra-respiratory tissues and organs, particularly in cases with a more severe clinical course of infection. The digestive tract and liver of humans may be involved in the spreading of this virus within the human body. Recently the putative receptor (ACE2) for SARS-CoV-2 has been found on bile duct epithelial cells. Therefore, an inflammatory response of cholangiocytes and the compensatory proliferation of cholangiocyte-derived hepatocytes may underline the potential mechanism of liver injury by SARS-CoV-2 [35,36]. Accordingly, the presence of SARS-CoV-2 in fecal samples has been recently reported [37].
Such findings have different implications. First, the fecal-oral route of viral transmission could be as crucial as the aerial transmission. Second, the delayed colonization of the digestive tract may suggest a novel pathogenic mechanism and finally, novel clinical and virological assessment (RT-PCR on fecal samples) might be needed in order to follow the natural history of human infection by SARS-CoV-2 [37].
Central nervous system (CNS) involvement has also been recently reported in SARS-CoV-2 infection. Neurological symptoms and signs such as: nausea, vomiting, headache, and reduced consciousness without apparent alterations in head CT scans suggested a diagnosis of encephalitis in some SARS-CoV-2 patients. Molecular tests were carried out on cerebrospinal fluid of some such patients, and SARS-CoV-2 was identified. Coronavirus has been found in the brainstem of both humans and experimental animals. It has also been reported that coronavirus can spread to the medullary cardiorespiratory center from peripheral chemoreceptors and from the lungs through both the blood and synapse routes. This feature might contribute to acute respiratory failure in the most severe cases of SARS-CoV-2 infection [11,38].
The spread of COVID-19 via blood circulation or across the cribriform plate of the ethmoid bone can lead to brain involvement. Such a feature has been reported for SARS-CoV patients. Subsequent budding of the virus from the capillary endothelium and slight injury to the endothelial lining can allow access to the brain. Subsequently, virus interaction with ACE2 receptors found in neurons and glial cells, may then lead to a cycle of viral budding with neuronal damage in the absence of an apparent inflammatory reaction.
Two significant clinical features of the early stage of COVID-19 are hyposmia and ageusia. There is a sharp contradiction regarding the mechanisms of these two symptoms. Some investigators have reported that a change in the mucosal cells of the nasal district might account for such a feature. Indeed, it is very unusual for such a change of feeling, without any overt inflammation and rhinorrhea.
The other possible explanation includes a primary effect of SARS-CoV-2 on the nerve fibers and cells. Many nervous regions, like the raphe nucleus (mesencephalon) and some nuclei of the lobus limbicus, as well as basal nuclei, are significantly involved in olfactory sensitivity. Similarly, ageusia might be explained by an effect on the tongue mucosal cells. Indeed, saliva is a matrix rich in SARS-CoV-2. Moreover, the nervous fiber of peripheral nerves involved in gustatory sensation could be substantially impaired [30,39]. Cerebral involvement alone, with the potential for causing cerebral edema, or small bleeding along with the cerebral microcirculation during COVID-19, may lead to death even before systemic homeostatic deregulation or lung diffuse consolidation. Moreover, entry of SARS-CoV-2 to the central nervous system via the transcriptional route has been reported for other CNS targeting pathogens. Such a route may explain a clinical COVID-19 with hyposmia and the cases of acute respiratory failure in COVID-19. Moriguchi described the first case of meningitis/encephalitis associated with SARS-CoV-2 not detected by nasopharyngeal swab, but confirmed in cerebral-spinal fluid [40].
There is no data which confirms that pregnancy increases the susceptibility of women to COVID-19, and it is still unknown if pregnancy could predispose to a more severe clinical course [41]. Clinical presentations in pregnant women are very similar to non-pregnant ones, and a small case series of women in their third trimester of pregnancy reported no adverse outcomes after delivery [42]. However, some authors suggest performing bimonthly fetal growth monitoring for the possibility of intrauterine growth restriction [43]. One explanation of such findings may be the lack of ACE2 receptors in placental tissue. This is consistent with the lack of SARS-CoV-2 in amniotic fluid, cord blood, and neonatal throat swabs [44].
In children and new-borns, COVID-19 seems to be mild and complications rarely occur [45]. Most children diagnosed with COVID-19 had a benign clinical course, with fewer and mild symptoms [46,47,48]. Reasons why children are not likely to present severe disease are still unknown, although the particular characteristics of the immune system and lower maturity and function of ACE2 receptors in children compared to adults have been suggested as possible underlying mechanisms [49].
3. Immune System Deception by SARS-CoV-2
The S protein has a well-defined composition comprising 14 binding residues that directly interact with human ACE2 receptors. Of these amino acids, eight are conserved in SARS-CoV-2. However, particular changes in some amino acids between S proteins of SARS-CoV and SARS-CoV-2 have been correlated with the enhanced binding affinity of SARS-CoV-2 and ACE2 receptor vs. SARS-CoV [46,50]. The mutations responsible for the greater transmissibility and the corresponding VOCs/VOIs are shown in Table 1.
The S protein binds to CD147, a trans-membrane protein of the immunoglobulin family, known as an entry route in red blood cells for the Malaria parasite. Such a protein could also be used by the new coronavirus [51]. These features may explain the increased human-to-human transmission exhibited by SARS-CoV-2 [46,50].
It has been demonstrated that increased levels of serum IgG antibodies could be proportional to the viral load and enhanced disease severity [52]. SARS-CoV-2 viral load, innate immunity and the several viral replication steps of COVID-19 are of vital importance to better understand the disease scenario. This could help to clarify why some patients remain asymptomatic, while other patients (where SARS-CoV-2 invades the alveoli and replicates in type II pneumocytes) may exhibit pneumonia, often with a fatal outcome [33]. Innate immunity is crucial to control early viral replication before the immune system can generate an effective adaptive immune response and also to establish this adaptive immunity. Innate immunity against SARS-CoV-2 is similar to that against other pathogens and is based on the release of some humoral components and the action of different cellular elements. It would be intriguing to investigate the possible role of endogenous antibiotics, such as magainins, against SARS-CoV-2 in both in vitro and in vivo models [53]. The presence of such innate immunity mediators could account for the significant and timely effect of convalescent plasma transfusions on the severe complications of COVID-19, even in the presence of non-neutralizing antibodies in the transfused plasma [54]. Even Toll-like receptors (TLRs) play a role in pathogenesis of SARS-CoV-2 infection. This feature has been associated with a signal mediated by TLR3, TLR7, or TLR8 leading to immunopathology [55].
Coronaviruses causing severe epidemics may disappear several months after causing deadly pandemics, only to re-emerge after some years to generate another outbreak [56]. Antibodies are primary tools in the protection against respiratory viruses [57]. Historical data regarding periodical re-emergence of the most critical viral respiratory epidemics show undoubtedly that the most studied are the flu epidemics [58]. The study of flu epidemics began with the 1889–1892 Russian Flu, followed by the Spanish Flu (1918–1920). The latter deadly epidemic has recently been analyzed based on the evaluation of antibody titer in survivors and on the direct demonstration of the strong neutralizing effect of such antibodies in an in vivo flu murine model [57]. Strong systemic cytokine reactions of remarkable pathogenic significance followed in this elegant in vivo experimental model of Spanish Flu, reminding us of the immunopathogenesis associated with the most severe COVID-19 clinical cases.
Similarly, in 2002–2003 the first relevant pandemic by a coronavirus causing respiratory pathology, was able to spread over 26 countries with 8096 human cases and 774 deaths [59]. A similar respiratory epidemic emerged again in 2012 spreading over 25 countries [59]. These pandemics have been followed by the present COVID-19 pandemic, which has so far caused more than 170,000,000 cases and more than 3,000,000 fatal outcomes. One traditional interpretation of such periodic behavior of these pandemics is reported as cyclical theory. The lack of population immunity to the previous pathogen would account for the periodicity of such epidemics. Indeed, such immunity would only last while most of the survivors are still alive [60].
However, the reappearance of an epidemic caused by respiratory viruses after only 8–10 years since the previous outbreak, is in contrast with cyclical theory. In this case, a different interpretation must be taken into account to explain such a re-emergence of the same epidemic after such a short period. Dealing with the historical behavior of several flu pandemics, some authors state that previous exposure to the influenza virus has paradoxically enhanced, instead of decreasing, susceptibility to such viral disease [60].
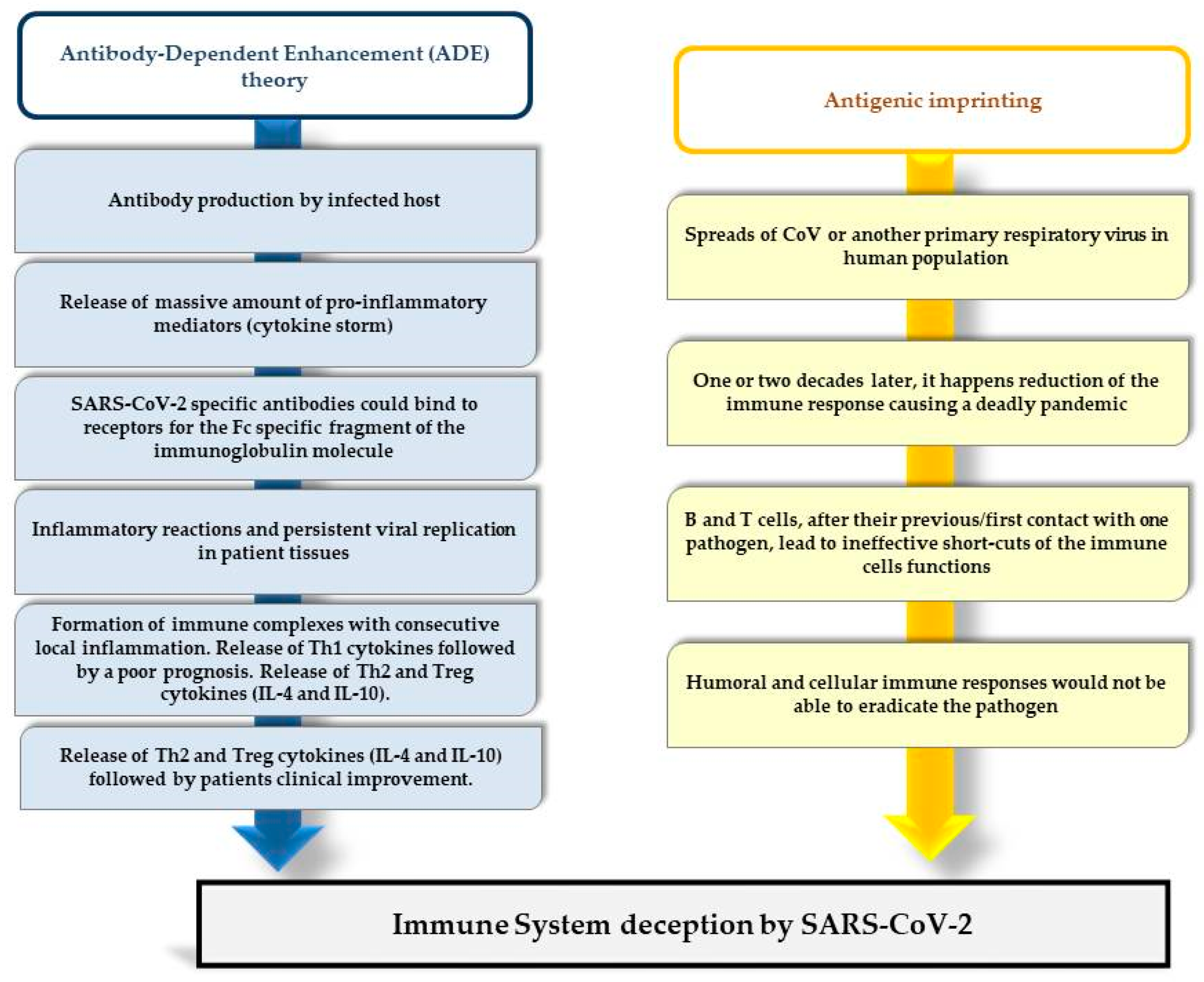
Two possible explanations are reported to account for a second more severe infection based on the same viral etiology of the first one (Figure 1).
Figure 1.
Schematic view of Immune System role during SARS-CoV-2 infection. The antibody-dependent enhancement (ADE) theory is shown in blue, the antigenic imprinting in orange.
The first is explained by the antibody-dependent enhancement (ADE) theory, where antibodies specific to the etiological agent, causing the first epidemic are released.
ADE is the phenomenon in which preexisting, non-neutralizing, or poorly neutralizing antibodies lead to enhanced infection, increasing viral entry into cells. The mechanism of ADE can also occur due to a lower concentration or lesser affinity of neutralizing antibodies. Several factors are involved in ADE such as affinity, concentration, specificity, and isotype of antibodies. It is interesting how high-affinity neutralizing antibodies, even at minimal concentrations, can avoid ADE. In clinical settings, ADE has been reported in several human viruses (HIV, Dengue virus, RSV, Ebola virus, Zika virus, Influenza virus) and veterinary pathogens [55]. On the contrary, according to our knowledge, direct scientific evidence of a clinical impact of ADE during human SARS-CoV-2 infection is lacking. Similarly, ADE emerging after SARS-CoV-2 vaccine administration in humans has not yet been published.
According to Tillett et al., previous exposure to SARS-CoV-2 might not guarantee total immunity. Their findings led to the hypothesis that a mechanism of antibody-dependent enhancement might be the cause of a symptomatic reinfection with SARS-CoV-2 in a 25-year-old man [61].
Focosi et al. collected a number of demographic and clinical data of their patients and evaluated the level of antibodies against antigens of both minor coronaviruses and SARS-CoV-2. Statistical association between the levels of anti-minor coronavirus antibodies and worse clinical outcome was demonstrated. They suggested a possible ADE during SARS-CoV-2 infection due to previous alphacoronavirus (minor coronavirus) immunity and they found that previous antibodies to the seasonal endemic coronaviruses could be associated with a worse clinical outcome in COVID-19 patients [62].
Dengue virus and other viral organisms have been demonstrated to cause ADE. It is a general view that host antibodies play a beneficial role during all viral diseases. Previous studies on SARS-CoV-2 infection showed the peculiar mechanism used by the virus to convert immune cells, such as macrophages and B cells, into weapons against the host. Such a mechanism envisages that SARS-CoV-2-specific antibodies, after engagement with coronavirus or its product, could link receptors specific for the Fc fragment of the immunoglobulin molecule. Such interaction could produce both inflammatory reactions and persistent viral replication in patient tissues [63,64,65]. The formation of immune complexes might lead to the cytokine storm particularly in severe COVID-19 [66]. Some cytokines (IL-1β, IFNγ, IL-8, and IL-4) have been investigated concerning such an atypical viral pathogenic mechanism. Indeed, those patients infected with SARS-CoV-2 were found to exhibit a high concentration of IL-1β, IFNγ, and IP10 (CXCL10), leading to a T-helper-1 (Th1) cascade. This unusual viral pathogenic mechanism has also been reported as a “cytokine storm” [29]. Two relevant aspects should be underlined regarding the cytokine role in SARS-CoV-2 infections. High levels of chemokines like IP10, MCP1, MIP1α, andrelevant concentration of the pro-inflammatory cytokine TNFα found in the severe cases, might explain the intense tissue inflammation and massive consolidation of large lung areas. Moreover, Th17 cells, neutrophils, and granulocytes all produce IL-17, which stimulates production of several pro-inflammatory cytokines [51].
On the contrary, the release of Th2 and Treg cytokines (IL-4 and IL-10), with an anti-inflammatory potential, might account for the many mild cases of SARS-CoV-2 infections [29,67]. Regarding the early release pro-inflammatory cytokines, IL-6 has been reported to be among the main components of the cytokine storm [67].
It is a relevant issue for viral infections that the internalized immune complexes modulate host immune response enhancing viral replication and aggravating disease severity [68]. In the context of SARS-CoV-2, ADE may enhance viral replication in immune cells since the virus might productively infect immune cells including monocytes and B cells both in vivo and ex vivo. Wu et al. studied in vitro ADE of SARS-CoV-2 entry into FcɤRII receptor-bearing cells (Raji cells are lymphoma cells derived from human B lymphocytes) by plasma and antibodies from patients who recovered from COVID-19 [69]. The enhancement of SARS-CoV-2 infection was mediated by IgG and it was more commonly observed in plasma from elderly patients with critical conditions and prolonged disease duration, suggesting a possible association of ADE with worse clinical outcomes in COVID-19 patients [69].
Vaccine development needs to take into account the serious possibility of any potentially dangerous effect which triggers an ADE phenomenon. Due to the very large population that must be vaccinated, the very frequent spread of minor coronavirus infections (HCoV-229E, -NL63, -OC43, -HKU1) throughout the general population should be considered. Such spread probably allows several populations of anti-coronavirus antibodies to be maintained at very low levels for a long time. Thus, the potent trigger of a SARS-CoV-2 vaccine might provoke an uncontrolled ADE with hazardous side effects for the host. Any vaccine must therefore avoid ADE and other unwanted side effects.
A vaccine inducing high titers of neutralizing antibodies is considered safer than one inducing low titers because the new virions are neutralized before the ADE occurs. Furthermore, neutralizing antibodies mediate ADE only at the suboptimal neutralizing concentration. Plasma and antibodies from patients who have recovered from COVID-19 should be tested for potential ADE effects before clinical usage [69]. The development of a vaccine or immunotherapeutic agent targeting only the neutralizing epitopes represents an optimal approach to induce a better immune response reducing the possibility of ADE and hence protecting the host from COVID-19 [55].
Alongside the complex ADE phenomenon, another interpretation which may account for a second more severe infection based on the same viral etiology of the first one is antigenic imprinting. This hypothesis proposes a reduced host immune response against a respiratory virus when such a pathogen comes into contact with the host for the first time early in life. The trend of human immune system B cells and T cells to overly trust on previous/first contact with any given pathogen, leads to ineffective short-cuts of immune cells functions which eventually would not be able to eradicate the pathogen [58,70].
From the ideas reported above, one may hypothesize that the first time a coronavirus or another primary respiratory virus spreads in a human population, a small and limited epidemic would result. However, a second hit, one or two decades later, would cause a deadly pandemic.
The risks due to the ADE phenomenon associated with SARS-CoV-2 have important implications for COVID-19, MIS-C treatment, B-cell vaccines, SARS-CoV-2 antibody therapy, and convalescent plasma therapy for patients. ADE risk for SARS-CoV-2 B-cell vaccines for different subsets of populations, can be associated with various clinical and demographic characteristics such as age, cross-reactive antibodies, variability of antibody levels over time and pregnancy. These new studies place greater emphasis on the need to develop safe SARS-CoV-2 T-cell vaccines that will not be dependent on antibodies [71].
4. Conclusions
The COVID-19 deadly pandemic offers researchers the chance to shed light on many aspects of SARS-CoV-2 and possibly of similar viruses. This virus took advantage of some out-of-the-ordinary social and behavioral aspects within cities with a very large population, during a period of the year when the majority of the community was in transit due to the beginning of the Chinese lunar calendar. In modern times, infectious organisms can exploit the possibility of infecting a large part of the world population due to year-round travel, by air and by cruise ship. On the contrary, until 30 or 40 years ago, very few people could have afforded such frequent trips for either work or leisure. SARS-CoV-2 exploited the quickest and simplest transmission pathway, airborne, instead of slower and less efficient diffusion mechanisms (by contaminated food, by a parenteral route, by specific vectors). Such different and highly efficient transmission patterns of viruses must be thoroughly investigated to avoid other infectious agents from replicating the COVID-19 pandemic. In Table 2 we suggest the main points of SARS-CoV-2 infection for attention.

Table 2.
Take home messages.
Researchers should address the life cycle and biology of SARS-CoV-2, and the molecular mechanisms used to initiate and develop infection in the human host. Such illness begins in the upper airways, but may rapidly progress to the lung tissue and might even spread to several different vital organs, including the brain, liver, heart, kidney, and possibly others. The efficacy of currently available therapeutic strategies against COVID-19 is not yet established. However, different clinical trials are ongoing and preliminary data may be useful in guiding clinicians toward the best management of patients suffering from COVID-19.
Finally, even if the ADE phenomenon is not well addressed in SARS-CoV-2, it is necessary to take into account the side effects of uncontrolled ADE. Hence, investigators should identify effective and safe vaccine strategies to prevent the further spread of this infection and hopefully stop this pandemic.
Future studies dealing with the COVID-19 immune response should address in depth the cellular response of host immunity. Such a response has not been fully addressed to date and would reveal many extremely interesting pathogenic features, as well as suggesting both vaccine and therapeutic improvements.
Author Contributions
Conceptualization, G.M. and M.C.L.; writing—original draft preparation, A.Q. and N.M.; writing—review and editing, G.S.B., L.G., A.G., A.G.L., C.P., E.M.T., P.F., M.M., F.D., G.P., A.S.; supervision, A.Q. and G.M. All authors have read and agreed to the published version of the manuscript.
Funding
This research received no external funding.
Institutional Review Board Statement
Not applicable.
Informed Consent Statement
Not applicable.
Acknowledgments
The authors would like to thank Neill J. Adams, for his valuable scientific and language editing of the manuscript.
Conflicts of Interest
The authors declare no conflict of interest.
References
- de Wit, E.; van Doremalen, N.; Falzarano, D.; Munster, V.J. SARS and MERS: Recent insights into emerging Coronaviruses. Nat. Rev. Microbiol. 2016, 14, 523–534. [Google Scholar] [CrossRef]
- Xu, J.; Zhao, S.; Teng, T.; Abdalla, A.E.; Zhu, W.; Xie, L.; Wang, Y.; Guo, X. Systematic Comparison of Two Animal-to-Human Transmitted Human Coronaviruses: SARS-CoV-2 and SARS-CoV. Viruses 2020, 12, 244. [Google Scholar] [CrossRef] [Green Version]
- Rothan, H.A.; Byrareddy, S.N. The epidemiology and pathogenesis of coronavirus disease (COVID-19) outbreak. J. Autoimmun. 2020, 109, 102433. [Google Scholar] [CrossRef] [PubMed]
- Walls, A.C.; Park, Y.J.; Tortorici, M.A.; Wall, A.; McGuire, A.T.; Veesler, D. Structure, Function, and Antigenicity of the SARS-CoV-2 Spike Glycoprotein. Cell 2020, 181, 281–292.e6. [Google Scholar] [CrossRef]
- Torti, C.; Mazzitelli, M.; Trecarichi, E.M.; Darius, O. Potential Implications of SARS-CoV-2 Epidemic in Africa: Where Are We Going from Now? BMC Infect. Dis. 2020, 20, 412. [Google Scholar] [CrossRef]
- Giovanetti, M.; Benvenuto, D.; Angeletti, S.; Ciccozzi, M. The first two cases of 2019-nCoV in Italy: Where they come from? J. Med. Virol. 2020, 92, 518–521. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Wertheim, J.O. A glimpse into the origins of genetic diversity in the severe acute respiratory syndrome coronavirus 2. Clin. Infect. Dis. 2020, 71, 721–722. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Worobey, M.; Pekar, J.; Larsen, B.B.; Nelson, M.I.; Hill, V.; Joy, J.B.; Rambaut, A.; Suchard, M.A.; Wertheim, J.O.; Lemey, P. The emergence of SARS-CoV-2 in Europe and the US. Version 1. bioRxiv 2020. [Google Scholar] [CrossRef]
- WHO. Coronavirus Disease (COVID-19) Weekly Epidemiological Update and Weekly Operational Update. 2021. Available online: https://go.nature.com/3aahjbg (accessed on 23 August 2021).
- Boehm, E.; Kronig, I.; Neher, R.A.; Eckerle, I.; Vetter, P.; Kaiser, L. Novel SARS-CoV-2 variants: The pandemics within the pandemic. Clin. Microbiol. Infect. 2021, 27, 1109–1117. [Google Scholar] [CrossRef]
- Kim, S.J.; Nguyen, V.G.; Park, Y.H.; Park, B.K.; Chung, H.-C. A Novel Synonymous Mutation of SARS-CoV-2: Is This Possible to Affect Their Antigenicity and Immunogenicity? Vaccines 2020, 14, 220. [Google Scholar] [CrossRef]
- Garcia-Beltran, W.F.; Lam, E.C.; Denis, K.S.; Nitido, A.D.; Garcia, Z.H.; Hauser, B.M.; Feldman, J.; Pavlovic, M.N.; Gregory, D.J.; Poznansky, M.C.; et al. Multiple SARS-CoV-2 variants escape neutralization by vaccine-induced humoral immunity. Cell 2021, 184, 2372–2383. [Google Scholar] [CrossRef]
- Cherian, S.; Potdar, V.; Jadhav, S.; Yadav, P.; Gupta, N.; Das, M.; Rakshit, P.; Singh, S.; Abraham, P.; Panda, S.; et al. SARS-CoV-2 Spike Mutations, L452R, T478K, E484Q and P681R, in the Second Wave of COVID-19 in Maharashtra, India. Microorganisms 2021, 9, 1542. [Google Scholar] [CrossRef] [PubMed]
- Izumi, H.; Nafie, L.A.; Dukor, R.K. Conformational Variability Correlation Prediction of Transmissibility and Neutralization Escape Ability for Multiple Mutation SARS-CoV-2 Strains using SSSCPreds. ACS Omega 2021, 6, 19323–19329. [Google Scholar] [CrossRef]
- Saito, A.; Irie, T.; Suzuki, R.; Maemura, T.; Nasser, H.; Uriu, K.; Kosugi, Y.; Sadamasu, K.S.K.; Kimura, I.; Ito, J.; et al. SARS-CoV-2 spike P681R mutation, a hallmark of the Delta variant, enhances viral fusogenicity and pathogenicity. bioRxiv 2021. [Google Scholar] [CrossRef]
- Zhang, J.; Xiao, T.; Cai, Y.; Lavine, C.L.; Peng, H.; Zhu, H.; Anand, K.; Tong, P.; Gautam, A.; Mayer, M.L.; et al. Membrane fusion and immune evasion by the spike protein of SARS-CoV-2 Delta variant. bioRxiv 2021. [Google Scholar] [CrossRef]
- Rochman, N.D.; Wolf, Y.I.; Faure, G.; Mutz, P.; Zhang, F.; Koonin, E.V. Ongoing global and regional adaptive evolution of SARS-CoV-2. Proc. Natl. Acad. Sci. USA 2021, 118, 2104241118. [Google Scholar] [CrossRef] [PubMed]
- ECDC-European Center for Disease Control. SARS-CoV-2 Variants of Concern as of 6 May 2021. Available online: https://www.ecdc.europa.eu/en/covid-19/variants-concern (accessed on 21 August 2021).
- Li, X.; Geng, M.; Peng, Y.; Meng, L.; Lu, S. Molecular immune pathogenesis and diagnosis of COVID-19. Version 2. J. Pharm. Anal. 2020, 10, 102–108. [Google Scholar] [CrossRef]
- Zhou, P.; Yang, X.-L.; Wang, X.-G.; Hu, B.; Zhang, L.; Zhang, W.; Si, H.-R.; Zhu, Y.; Li, B.; Huang, C.-L.; et al. A pneumonia outbreak associated with a new coronavirus of probable bat origin. Nature 2020, 579, 270–273. [Google Scholar] [CrossRef] [Green Version]
- Lukassen, S.; Chua, R.L.; Trefzer, T.; Kahn, N.C.; Schneider, M.A.; Muley, T.; Winter, H.; Meister, M.; Veith, C.; Boots, A.W.; et al. SARS -CoV-2 receptor ACE 2 and TMPRSS 2 are primarily expressed in bronchial transient secretory cells. EMBO J. 2020, 39, e105114. [Google Scholar] [CrossRef]
- Matera, G.; Quirino, A.; Peronace, C.; Settembre, P.; Marano, V.; Loria, M.T.; Marascio, N.; Galati, L.; Barreca, G.S.; Giancotti, A.; et al. Soluble CD14 Subtype-A New Biomarker in Predicting the Outcome of Critically Ill Septic Patients. Am. J. Med. Sci. 2017, 353, 543–551. [Google Scholar] [CrossRef]
- Pelle, M.C.; Tassone, B.; Ricchio, M.; Mazzitelli, M.; Davoli, C.; Procopio, G.; Cancelliere, A.; La Gamba, V.; Lio, E.; Matera, G.; et al. Late-onset myocardial infarction and autoimmune haemolytic anaemia in a COVID-19 patient without respiratory symptoms, concomitant with a paradoxical increase in inflammatory markers: A case report. J. Med. Case Rep. 2020, 14, 246. [Google Scholar] [CrossRef] [PubMed]
- Wu, Z.; McGoogan, J.M. Characteristics of and Important Lessons from the Coronavirus Disease 2019 (COVID-19) Outbreak in China: Summary of a Report of 72 314 Cases from the Chinese Center for Disease Control and Prevention. JAMA 2020, 323, 1239–1242. [Google Scholar] [CrossRef] [PubMed]
- Spaccarotella, C.; Migliarino, S.; Mongiardo, A.; Curcio, A.; de Rosa, S.; Corcione, N.; Quirino, A.; Barreca, G.S.; Giancotti, A.; Peronace, C.; et al. Fast-track ruling in/out SARS-CoV-2 infection with rapid 0/1.5 h molecular test in patients with acute coronary syndromes. J. Cardiovasc. Med. 2020, 21, 975–979. [Google Scholar] [CrossRef]
- Cancelliere, A.; Procopio, G.; Mazzitelli, M.; Lio, E.; Petullà, M.; Serapide, F.; Pelle, M.C.; Davoli, C.; Trecarichi, E.M.; Torti, C.; et al. A case report of pneumomediastinum in a COVID-19 patient treated with high-flow nasal cannula and review of the literature: Is this a “spontaneous” complication? Clin. Case Rep. 2021, 9, e04007. [Google Scholar] [CrossRef]
- Wang, D.; Hu, B.; Hu, C.; Zhu, F.; Liu, X.; Zhang, J.; Wang, B.; Xiang, H.; Cheng, Z.; Xiong, Y.; et al. Clinical Characteristics of 138 Hospitalized Patients With 2019 Novel Coronavirus-Infected Pneumonia in Wuhan, China. JAMA 2020, 323, 1061–1069. [Google Scholar] [CrossRef] [PubMed]
- Guan, W.J.; Ni, Z.Y.; Hu, Y.; Liang, W.H.; Ou, C.Q.; He, J.X.; Liu, L.; Shan, H.; Lei, C.L.; Hui, D.S.C.; et al. China Medical Treatment Expert Group for COVID-19. Clinical Characteristics of Coronavirus Disease 2019 in China. N. Engl. J. Med. 2020, 382, 1708–1720. [Google Scholar] [CrossRef] [PubMed]
- Huang, C.; Wang, Y.; Li, X.; Ren, L.; Zhao, J.; Hu, Y.; Zhang, L.; Fan, G.; Xu, J.; Gu, X.; et al. Clinical features of patients infected with 2019 novel Coronavirus in Wuhan, China. Lancet 2020, 395, 497–506. [Google Scholar] [CrossRef] [Green Version]
- Lechien, J.R.; Chiesa-Estomba, C.M.; De Siati, D.R.; Horoi, M.; Le Bon, S.D.; Rodriguez, A.; Dequanter, D.; Blecic, S.; El Afia, F.; Distinguin, L.; et al. Olfactory and gustatory dysfunctions as a clinical presentation of mild-to-moderate forms of the Coronavirus disease (COVID-19): A multicenter European study. Eur. Arch. Oto-Rhino-Laryngol. 2020, 277, 2251–2261. [Google Scholar] [CrossRef]
- Mao, L.; Jin, H.; Wang, M.; Hu, Y.; Chen, S.; He, Q.; Chang, J.; Hong, C.; Zhou, Y.; Wang, D.; et al. Neurologic Manifestations of Hospitalized Patients with Coronavirus Disease 2019 in Wuhan, China. JAMA Neurol. 2020, 77, 683–690. [Google Scholar] [CrossRef] [Green Version]
- Trecarichi, E.M.; Mazzitelli, M.; Serapide, F.; Pelle, M.C.; Tassone, B.; Arrighi, E.; Perri, G.; Fusco, P.; Scaglione, V.; Davoli, C.; et al. Clinical characteristics and predictors of mortality associated with COVID-19 in elderly patients from a long-term care facility. Sci. Rep. 2020, 10, 1–7. [Google Scholar] [CrossRef]
- Chen, N.; Zhou, M.; Dong, X.; Qu, J.; Gong, F.; Han, Y.; Qiu, Y.; Wang, J.; Liu, Y.; Wei, Y.; et al. Epidemiological and clinical characteristics of 99 cases of 2019 novel Coronavirus pneumonia in Wuhan, China: A descriptive study. Lancet 2020, 395, 507–513. [Google Scholar] [CrossRef] [Green Version]
- Cao, Y.; Li, L.; Feng, Z.; Wan, S.; Huang, P.; Sun, X.; Wen, F.; Huang, X.; Ning, G.; Wang, W. Comparative genetic analysis of the novel Coronavirus (2019-nCoV/SARS-CoV-2) receptor ACE2 in different populations. Cell Discov. 2020, 6, 11. [Google Scholar] [CrossRef] [Green Version]
- Zhang, C.; Shi, L.; Wang, F.S. Liver injury in COVID-19: Management and challenges. Lancet Gastroenterol. Hepatol. 2020, 5, 428–430. [Google Scholar] [CrossRef]
- Guan, G.W.; Gao, L.; Wang, J.W.; Wen, X.J.; Mao, T.H.; Peng, S.W.; Zhang, T.; Chen, X.M.; Lu, F.M. Exploring the mechanism of liver enzyme abnormalities in patients with novel Coronavirus-infected pneumonia. Zhonghua Gan Zang Bing Za Zhi 2020, 28, 100–106. [Google Scholar]
- Chen, Y.; Chen, L.; Deng, Q.; Zhang, G.; Wu, K.; Ni, L.; Yang, Y.; Liu, B.; Wang, W.; Wei, C.; et al. The presence of SARS-CoV-2 RNA in the feces of COVID-19 patients. J. Med. Virol. 2020, 92, 833–840. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Baig, A.M.; Khaleeq, A.; Ali, U.; Syeda, H. Evidence of the COVID-19-Virus Targeting the CNS: Tissue Distribution, Host–Virus Interaction, and Proposed Neurotropic Mechanisms. ACS Chem. Neurosci. 2020, 11, 995–998. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Lao, W.P.; Imam, S.A.; Nguyen, S.A. Anosmia, hyposmia, and dysgeusia as indicators for positive SARS-CoV-2 infection. World J. Otorhinolaryngol.-Head Neck Surg. 2020, 6, S22–S25. [Google Scholar] [CrossRef]
- Moriguchi, T.; Harii, N.; Goto, J.; Harada, D.; Sugawara, H.; Takamino, J.; Ueno, M.; Sakata, H.; Kondo, K.; Myose, N.; et al. A first Case of Meningitis/Encephalitis associated with SARS-Coronavirus-2. Int. J. Infect. Dis. 2020, 94, 55–58. [Google Scholar] [CrossRef] [PubMed]
- Rasmussen, S.A.; Smulian, J.C.; Lednicky, J.A.; Wen, T.S.; Jamieson, D.J. Coronavirus Disease 2019 (COVID-19) and pregnancy: What obstetricians need to know. Am. J. Obstet. Gynecol. 2020, 222, 415–426. [Google Scholar] [CrossRef] [PubMed]
- Chen, H.; Guo, J.; Wang, C.; Luo, F.; Yu, X.; Zhang, W.; Li, J.; Zhao, D.; Xu, D.; Gong, Q.; et al. Clinical characteristics and intrauterine vertical transmission potential of COVID-19 infection in nine pregnant women: A retrospective review of medical records. Lancet 2020, 395, 809–815. [Google Scholar] [CrossRef] [Green Version]
- Favre, G.; Pomar, L.; Qi, X.; Nielsen-Saines, K.; Musso, D.; Baud, D. Guidelines for pregnant women with suspected SARS-CoV-2 infection. Lancet Infect. Dis. 2020, 20, 652–653. [Google Scholar] [CrossRef] [Green Version]
- Yang, H.; Wang, C.; Poon, L.C. Novel Coronavirus infection and pregnancy. Ultrasound Obstet. Gynecol. 2020, 55, 435–437. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Kam, K.Q.; Yung, C.F.; Cui, L.; Tzer Pin Lin, R.; Mak, T.M.; Maiwald, M.; Li, J.; Chong, C.Y.; Nadua, K.; Tan, N.W.H.; et al. A Well Infant with Coronavirus Disease 2019 (COVID-19) with High Viral Load. Clin. Infect. Dis. 2020, 71, 847–849. [Google Scholar] [CrossRef] [PubMed]
- Lu, X.; Zhang, L.; Du, H.; Zhang, J.; Li, Y.Y.; Qu, J.; Zhang, W.; Wang, Y.; Bao, S.; Li, Y.; et al. Chinese Pediatric Novel Coronavirus Study Team. SARS-CoV-2 Infection in Children. N. Engl. J. Med. 2020, 382, 1663–1665. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- CDC COVID-19 Response Team. Coronavirus Disease 2019 in Children-United States, February 12-April 2, 2020. MMWR Morb. Mortal. Wkly. Rep. 2020, 69, 422–426. [Google Scholar] [CrossRef]
- Choi, S.H.; Kim, H.W.; Kang, J.M.; Kim, D.H.; Cho, E.Y. Epidemiology and clinical features of Coronavirus disease 2019 in children. Clin. Exp. Pediatr. 2020, 63, 125–132. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Dong, Y.; Mo, X.; Hu, Y.; Qi, X.; Jiang, F.; Jiang, Z.; Tong, S. Epidemiology of COVID-19 among Children in China. Pediatrics 2020, 145, e20200702. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Sohrabi, C.; Alsafi, Z.; O’Neill, N.; Khan, M.; Kerwan, A.; Al-Jabir, A.; Iosifidis, C.; Agha, R. World Health Organization declares global emergency: A review of the 2019 novel coronavirus (COVID-19). Int. J. Surg. 2020, 76, 71–76. [Google Scholar] [CrossRef]
- Yazdanpanah, F.; Hamblin, M.R.; Rezaei, N. The immune system and COVID-19: Friend or foe? Life Sci. 2020, 256, 117900. [Google Scholar] [CrossRef]
- Tan, W.; Lu, Y.; Zhang, J.; Wang, J.; Dan, Y.; Tan, Z.; He, X.; Qian, C.; Sun, Q.; Hu, Q.; et al. Viral kinetics and antibody responses in patients with COVID-19. medRxiv 2020. [Google Scholar] [CrossRef] [Green Version]
- Zairi, A.; Tangy, F.; Bouassida, K.; Hani, K. Dermaseptins and magainins:antimicrobial peptides from frogs’ skin-new sources for a promising spermicides microbicides. J. Biomed. Biotechnol. 2009, 2009, 452567. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Casadevall, A.; Pirofski, L.A. The convalescent sera option for containing COVID-19. J. Clin. Investig. 2020, 130, 1545–1548. [Google Scholar] [CrossRef] [Green Version]
- Karthik, K.; Senthilkumar, T.M.A.; Udhayavel, S.; Raj, G.D. Role of antibody-dependent enhancement (ADE) in the virulence of SARS-CoV-2 and its mitigation strategies for the development of vaccines and immunotherapies to counter COVID-19. Hum. Vaccin. Immunother. 2020, 16, 3055–3060. [Google Scholar] [CrossRef] [PubMed]
- Ayukekbong, J.A.; Ntemgwa, M.L.; Ayukekbong, S.A.; Ashu, E.E.; Agbor, T.A. COVID-19 compared to other epidemic coronavirus diseases and the flu. World J. Clin. Infect. Dis. 2020, 10, 1–13. [Google Scholar] [CrossRef]
- Yu, X.; Tsibane, T.; McGraw, P.A.; House, F.S.; Keefer, C.J.; Hicar, M.D.; Tumpey, T.M.; Pappas, C.; Perrone, L.A.; Martinez, O.; et al. Neutralizing antibodies derived from the B cells of 1918 influenza pandemic survivors. Nature 2008, 455, 532–536. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Roncati, L.; Palmieri, B. What about the original antigenic sin of the humans versus SARS-CoV-2? Med. Hypotheses 2020, 142, 109824. [Google Scholar] [CrossRef]
- Shi, Z.; Wang, L.F. Evolution of SARS Coronavirus and the Relevance of Modern Molecular Epidemiology. Genet. Evolut. Infect. Dis. 2011, 711–728. [Google Scholar] [CrossRef]
- Gagnon, A.; Acosta, E.; Hallman, S.; Bourbeau, R.; Dillon, L.Y.; Ouellette, N.; Earn, D.J.D.; Herring, D.A.; Inwood, K.; Madrenas, J.; et al. Pandemic Paradox: Early Life H2N2 Pandemic Influenza Infection Enhanced Susceptibility to Death During the 2009 H1N1 Pandemic. mBio 2018, 9, e02091-17. [Google Scholar] [CrossRef] [Green Version]
- Tillett, R.L.; Sevinsky, J.R.; Hartley, P.D.; Kerwin, H.; Crawford, N.; Gorzalski, A.; Laverdure, C.; Verma, S.C.; Rossetto, C.C.; Jackson, D.; et al. Genomic evidence for reinfection with SARS-CoV-2: A case study. Lancet Infect. Dis. 2021, 21, 52–58. [Google Scholar] [CrossRef]
- Focosi, D.; Genoni, A.; Lucenteforte, E.; Tillati, S.; Tamborini, A.; Spezia, P.G.; Azzi, L.; Baj, A.; Maggi, F. Previous Humoral Immunity to the Endemic Seasonal Alphacoronaviruses NL63 and 229E Is Associated with Worse Clinical Outcome in COVID-19 and Suggests Original Antigenic Sin. Life 2021, 11, 298. [Google Scholar] [CrossRef] [PubMed]
- Jin, Y.; Yang, H.; Ji, W.; Wu, W.; Chen, S.; Zhang, W.; Duan, G. Virology, Epidemiology, Pathogenesis, and Control of COVID-19. Viruses 2020, 12, 372. [Google Scholar] [CrossRef] [Green Version]
- Iwasaki, A.; Yang, Y. The potential danger of suboptimal antibody responses in COVID-19. Nat. Rev. Immunol. 2020, 20, 339–341. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Fu, Y.; Cheng, Y.; Wu, Y. Understanding SARS-CoV-2-Mediated Inflammatory Responses: From Mechanisms to Potential Therapeutic Tools. Virol. Sin. 2020, 35, 266–271. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Fierz, W.; Walz, B. Antibody Dependent Enhancement Due to Original Antigenic Sin and the Development of SARS. Front. Immunol. 2020, 11, 1120. [Google Scholar] [CrossRef]
- Liu, J.; Zheng, X.; Tong, Q.; Li, W.; Wang, B.; Sutter, K.; Trilling, M.; Lu, M.; Dittmer, U.; Yang, D. Overlapping and discrete aspects of the pathology and pathogenesis of the emerging human pathogenic coronaviruses SARS-CoV, MERS-CoV, and 2019-nCoV. J. Med. Virol. 2020, 92, 491–494. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Kulkarni, R. Antibody-Dependent Enhancement of Viral Infections. In Dynamics of Immune Activation in Viral Diseases; Springer Science and Business Media LLC: Berlin/Heidelberg, Germany, 2020; pp. 9–41. [Google Scholar]
- Wu, F.; Yan, R.; Liu, M.; Liu, Z.; Wang, Y.; Luan, D.; Wu, K.; Song, Z.; Sun, T.; Ma, Y.; et al. Antibody-dependent enhancement (ADE) of SARS-CoV-2 infection in recoverehd COVID-19 patients: Studies based on cellular and structural biology analysis. medRxiv 2020. [Google Scholar] [CrossRef]
- Henry, C.; Palm, A.E.; Krammer, F.; Wilson, P.C. From Original Antigenic Sin to the Universal Influenza Virus Vaccine. Trends Immunol. 2018, 39, 70–79. [Google Scholar] [CrossRef] [PubMed]
- Ricke, D.O. Two Different Antibody-Dependent Enhancement (ADE) Risks for SARS-CoV-2 Antibodies. Front. Immunol. 2021, 12, 640093. [Google Scholar] [CrossRef]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).