Postural Stability and Proprioception Abnormalities in Patients with Knee Osteoarthritis
Abstract
:Featured Application
Abstract
1. Introduction
2. Materials and Methods
2.1. Ethical Issues
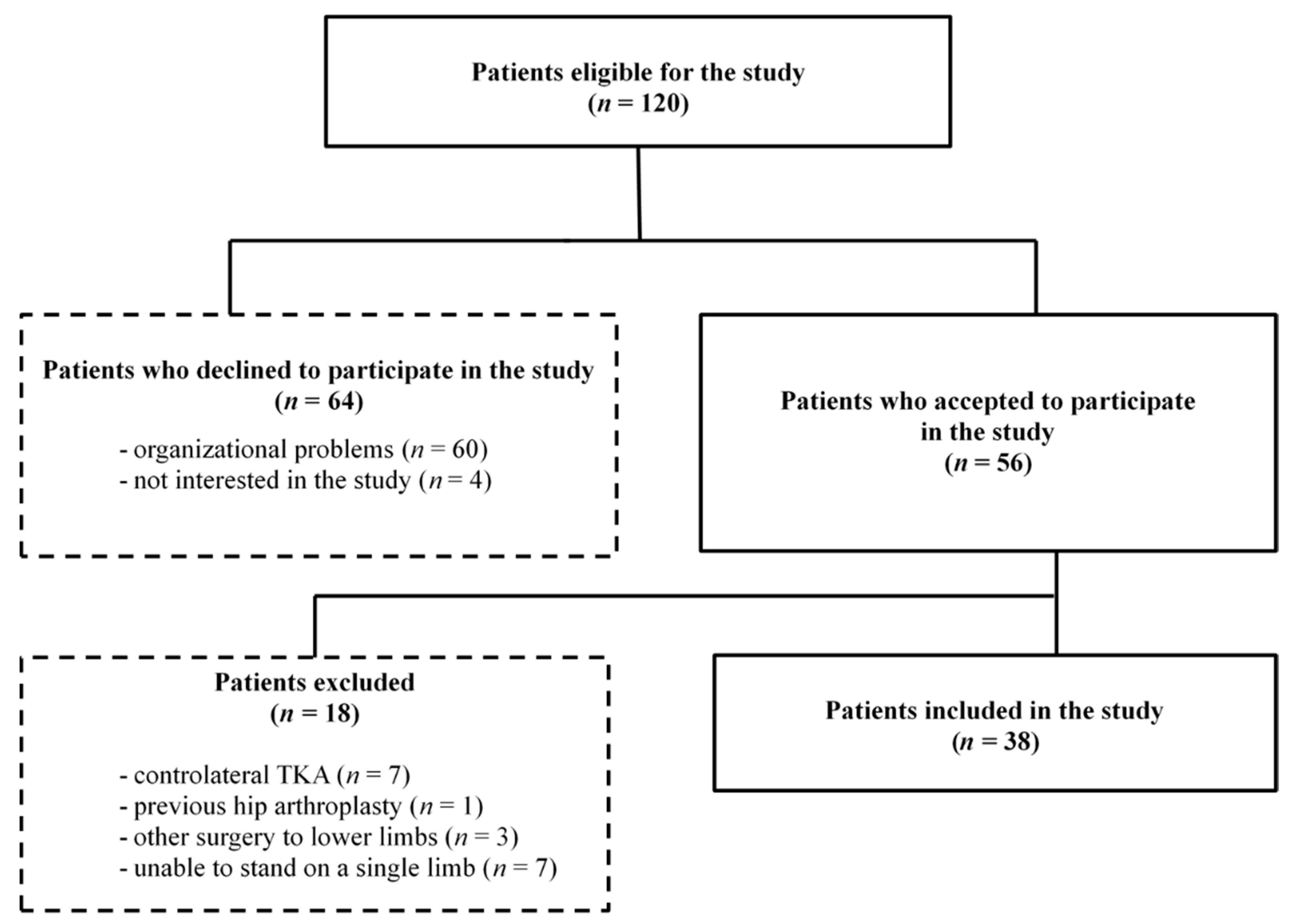
2.2. Participants
2.3. Assessments and Data Analysis
2.4. Statistical Analysis
3. Results
3.1. Postural Stability and Proprioception Assessment
3.1.1. Double-Stance Test
3.1.2. Single-Stance Test
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Appendix A
| Age | BMI | KSS-C | KSS-F | SPPB | ||
|---|---|---|---|---|---|---|
| PI OE | Rho | −0.173 | −0.125 | 0.199 | 0.147 | −0.052 |
| p | 0.314 | 0.467 | 0.246 | 0.393 | 0.765 | |
| PI CE | Rho | −0.114 | −0.186 | −0.067 | 0.058 | −0.044 |
| p | 0.509 | 0.276 | 0.697 | 0.735 | 0.800 | |
| SI OE-KOA limb | Rho | 0.145 | −0.204 | 0.143 | 0.492 | 0.518 |
| p | 0.384 | 0.219 | 0.393 | 0.002 | 0.001 | |
| SI CE-KOA limb | Rho | −0.019 | −0.142 | −0.098 | 0.137 | 0.048 |
| p | 0.912 | 0.396 | 0.557 | 0.413 | 0.776 | |
| SI OE-CONTRALATERAL limb | Rho | 0.181 | −0.131 | −0.027 | 0.246 | 0.121 |
| p | 0.277 | 0.433 | 0.870 | 0.137 | 0.469 | |
| SI CE-CONTRALATERAL limb | Rho | −0.162 | −0.357 | −0.064 | 0.226 | 0.207 |
| p | 0.330 | 0.028 | 0.702 | 0.172 | 0.213 | |
| SI Average (KOA limb and contralateral) OE | Rho | 0.212 | −0.185 | 0.090 | 0.456 | 0.380 |
| p | 0.201 | 0.265 | 0.591 | 0.004 | 0.019 | |
| SI Average (KOA limb and contralateral) OC | Rho | −0.153 | −0.319 | −0.145 | 0.174 | 0.096 |
| p | 0.360 | 0.051 | 0.385 | 0.295 | 0.565 | |
| Kellgren-Lawrence Score | ||
|---|---|---|
| PI OE | tau | 0.218 |
| p | 0.117 | |
| PI CE | tau | 0.150 |
| p | 0.278 | |
| SI OE-KOA limb | tau | −0.277 |
| p | 0.039 | |
| SI CE-KOA limb | tau | −0.160 |
| p | 0.235 | |
| SI OE-CONTRALATERAL limb | tau | −0.237 |
| p | 0.078 | |
| SI CE-CONTRALATERAL limb | tau | 0.004 |
| p | 0.975 | |
| SI Average (KOA limb and contralateral) OE | tau | −0.313 |
| p | 0.020 | |
| SI Average (KOA limb and contralateral) OC | tau | −0.069 |
| p | 0.606 | |
References
- Sowers, M.; Hayes, C.; Jamadar, D.; Capul, D.; Lachance, L.; Jannausch, M.; Welch, G. Magnetic resonance-detected subchondral bone marrow and cartilage defect characteristics associated with pain and X-ray-defined knee osteoarthritis. Osteoarthr. Cartil. 2003, 11, 387–393. [Google Scholar] [CrossRef] [Green Version]
- Davies-Tuck, M.L.; Wluka, A.E.; Wang, Y.; Teichtahl, A.J.; Jones, G.; Ding, C.; Cicuttini, F.M. The natural history of cartilage defects in people with knee osteoarthritis. Osteoarthr. Cartil. 2008, 16, 337–342. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Barrett, D.; Cobb, A.; Bentley, G. Joint proprioception in normal, osteoarthritic and replaced knees. J. Bone Jt. Surg. Br. Vol. 1991, 53–56. [Google Scholar] [CrossRef]
- Sharma, L. Proprioceptive Impairment in Knee Osteoarthritis. Rheum. Dis. Clin. North Am. 1999, 25, 299–314. [Google Scholar] [CrossRef]
- Wada, M.; Kawahara, H.; Shimada, S.; Miyazaki, T.; Baba, H. Joint Proprioception Before and After Total Knee Arthroplasty. Clin. Orthop. Relat. Res. 2002, 403, 161–167. [Google Scholar] [CrossRef]
- Hadamus, A.; Białoszewski, D. Objective assessment of knee proprioception and sensorimotor function in patients with pri-mary gonarthrosis before and after knee replacement. Ortop. Traumatol. Rehabil. 2017, 19, 403–414. [Google Scholar] [CrossRef]
- Sharma, L.; Pai, Y.C.; Holtkamp, K.; Rymer, W.Z. Is knee joint proprioception worse in the arthritic knee versus the unaffected knee in unilateral knee osteoarthritis? Arthritis. Rheum. 1997, 40, 1518–1525. [Google Scholar] [CrossRef] [PubMed]
- Knoop, J.; Steultjens, M.; Van Der Leeden, M.; Van Der Esch, M.; Thorstensson, C.; Roorda, L.; Lems, W.; Dekker, J. Proprioception in knee osteoarthritis: A narrative review. Osteoarthr. Cartil. 2011, 19, 381–388. [Google Scholar] [CrossRef] [Green Version]
- Al-Dadah, O.; Shepstone, L.; Donell, S.T. Proprioception deficiency in articular cartilage lesions of the knee. Knee Surg. Relat. Res. 2020, 32, 1–7. [Google Scholar] [CrossRef] [PubMed]
- Levinger, P.; Menz, H.B.; Wee, E.; Feller, J.A.; Bartlett, J.R.; Bergman, N.R. Physiological risk factors for falls in people with knee osteoarthritis before and early after knee replacement surgery. Knee Surg. Sports Traumatol. Arthrosc. 2010, 19, 1082–1089. [Google Scholar] [CrossRef]
- Doré, A.L.; Golightly, Y.M.; Mercer, X.A.; Renner, J.B.; Jordan, J.M.; Nelson, A.E. Lower-extremity osteoarthritis and the risk of falls in a community based lon-gitudinal study of adults with and without osteoarthritis. Arthr. Care Res. 2015, 67, 633–639. [Google Scholar] [CrossRef]
- Manlapaz, D.; Sole, G.; Jayakaran, P.; Chapple, C.M. Risk Factors for Falls in Adults with Knee Osteoarthritis: A Systematic Review. PM R 2019, 11, 745–757. [Google Scholar] [CrossRef]
- Anderson, M.L.; Allen, K.D.; Golightly, Y.M.; Arbeeva, L.S.; Goode, A.; Huffman, K.M.; Schwartz, T.A.; Hill, C.H. Fall Risk and Utilization of Balance Training for Adults with Symptomatic Knee Osteoarthritis: Secondary Analysis From a Randomized Clinical Trial. J. Geriatr. Phys. Ther. 2019, 42, E39–E44. [Google Scholar] [CrossRef]
- Doma, K.; Grant, A.; Morris, J. The effects of balance training on balance performance and functional outcome measures fol-lowing total knee arthroplasty: A systematic review and meta-analysis. Sports Med. 2018, 48, 2367–2385. [Google Scholar] [CrossRef]
- Hatfield, G.L.; Morrison, A.; Wenman, M.; Hammond, C.A.; Hunt, M.A. Clinical Tests of Standing Balance in the Knee Osteoarthritis Population: Systematic Review and Meta-analysis. Phys. Ther. 2016, 96, 324–337. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Hinman, R.S.; Bennell, K.L.; Metcalf, B.R.; Crossley, K.M. Balance impairments in individuals with symptomatic knee osteoarthritis: A comparison with matched controls using clinical tests. Rheumatology 2002, 41, 1388–1394. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Sazo-Rodriguez, S.; Mendez-Rebolledo, G.; Guzman-Munoz, E.; Rubio-Palma, P. The effects of progressive neuromuscular training on postural balance and functionality in elderly patients with knee ostaeoarthritis: A pilot study. J. Phys. Ther. Sci. 2017, 29, 1229–1235. [Google Scholar] [CrossRef] [Green Version]
- Truszczyńska-Baszak, A.; Dadura, E.; Drzał-Grabiec, J.; Tarnowski, A. Static balance assessment in patients with severe os-teoarthritis of the knee. Knee 2020, 27, 1349–1356. [Google Scholar] [CrossRef]
- Lawson, T.; Morrison, A.; Blaxland, S.; Wenman, M.; Schmidt, C.G.; Hunt, M.A. Laboratory-based measurement of standing balance in individuals with knee os-teoarthritis: A systematic review. Clin. Biomech. 2015, 30, 330–342. [Google Scholar] [CrossRef] [PubMed]
- Kim, H.-S.; Yun, D.H.; Yoo, S.D.; Kim, D.H.; Jeong, Y.S.; Yun, J.-S.; Hwang, D.G.; Jung, P.K.; Choi, S.H. Balance Control and Knee Osteoarthritis Severity. Ann. Rehabil. Med. 2011, 35, 701–709. [Google Scholar] [CrossRef] [Green Version]
- Riva, D.; Mamo, C.; Fanì, M.; Saccavino, P.; Rocca, F.; Momenté, M.; Fratta, M. Single Stance Stability and Proprioceptive Control in Older Adults Living at Home: Gender and Age Differences. J. Aging Res. 2013, 2013, 1–14. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Maktouf, W.; Durand, S.; Boyas, S.; Pouliquen, C.; Beaune, B. Combined effects of aging and obesity on postural control, muscle activity and maximal voluntary force of muscles mobilizing ankle joint. J. Biomech. 2018, 79, 198–206. [Google Scholar] [CrossRef]
- Kohn, M.D.; Sassoon, A.A.; Fernando, N.D. Classifications in Brief: Kellgren-Lawrence Classification of Osteoarthritis. Clin. Orthop. Relat. Res. 2016, 474, 1886–1893. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Treacy, D.; Hassett, L. The Short Physical Performance Battery. J. Physiother. 2018, 64, 61. [Google Scholar] [CrossRef]
- Insall, J.N.; Dorr, L.D.; Scott, R.D.; Norman, W. Rationale, of The Knee Society Clinical Rating System. Clin. Orthop. Relat. Res. 1989, 13–14. [Google Scholar] [CrossRef]
- Riva, D.; Fani, M.; Benedetti, M.G.; Scarsini, A.; Rocca, F.; Mamo, C. Effects of High-Frequency Proprioceptive Training on Single Stance Stability in Older Adults: Implications for Fall Prevention. BioMed Res. Int. 2019, 2019, 2382747. [Google Scholar] [CrossRef] [PubMed]
- Riva, D.; Bianchi, R.; Rocca, F.; Mamo, C. Proprioceptive training and injury prevention in a professional men’s basketball team: A six-year prospective study. J. Strength Cond. Res. 2016, 30, 461–475. [Google Scholar] [CrossRef] [Green Version]
- Le Clair, K.; Riach, C. Postural stability measures: What to measure and for how long. Clin. Biomech. 1996, 11, 176–178. [Google Scholar] [CrossRef]
- Benedetti, M.G.; Coli, M.; Campanacci, L.; Manfrini, M. Postural control skills, proprioception, and risk of fall in long-term survivor patients treated with knee rotationplasty. Int. J. Rehabil. Res. 2019, 42, 68–73. [Google Scholar] [CrossRef]
- Mosca, M.; Caravelli, S.; Massimi, S.; Fuiano, M.; Catanese, G.; Barone, G.; Bragonzoni, L.; Benedetti, M.G. Evaluation of proprioception and postural control at a minimum 1 year follow-up after ankle capsuloligamentous lateralplasty with Brostrom technique: A cohort study. Medicine 2020, 99, e19862. [Google Scholar] [CrossRef]
- Wang, H.; Ji, Z.-Q.; Jiang, G.; Liu, W.; Jiao, X. Correlation among proprioception, muscle strength, and balance. J. Phys. Ther. Sci. 2016, 28, 3468–3472. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Bragonzoni, L.; Rovini, E.; Barone, G.; Cavallo, F.; Zaffagnini, S.; Benedetti, M.G. How proprioception changes before and after total knee arthroplasty: A systematic review. Gait Posture 2019, 72, 1–11. [Google Scholar] [CrossRef]
- Tonelli, S.M.; Rakel, B.A.; Cooper, N.A.; Angstom, W.L.; Sluka, K.A. Women with knee osteoarthritis have more pain and poorer function than men, but similar physical activity prior to total knee replacement. Biol. Sex Differ. 2011, 2, 12. [Google Scholar] [CrossRef] [Green Version]
- Hana, S.; Aicha, B.T.; Selim, D.; Ines, M.; Rawdha, T. Clinical and radiographic features of knee osteoarthritis of elderly patients. Curr. Rheumatol. Rev. 2018, 14, 181–187. [Google Scholar] [CrossRef] [PubMed]
- Lelard, T.; Ahmaidi, S. Effects of physical training on age-related balance and postural control. Neurophysiol. Clin. Neurophysiol. 2015, 45, 357–369. [Google Scholar] [CrossRef] [PubMed]
- Sundstrup, E.; Jakobsen, M.D.; Andersen, J.L.; Randers, M.B.; Petersen, J.; Suetta, C.; Aagaard, P.; Krustrup, P. Muscle function and postural balance in lifelong trained male footballers compared with sedentary elderly men and youngsters. Scand. J. Med. Sci. Sports 2010, 20, 90–97. [Google Scholar] [CrossRef] [PubMed]
- Riis, A.; Rathleff, M.S.; Jensen, M.B.; Simonsen, O. Low grading of the severity of knee osteoarthritis pre-operatively is associated with a lower functional level after total knee replacement: A prospective cohort study with 12 months’ follow-up. Bone Joint J. 2014, 96, 1498–1502. [Google Scholar] [CrossRef]
- Xie, F.; Lo, N.N.; Pullenayegum, E.M.; Tarride, J.-E.; O’Reilly, D.J.; Goeree, R.; Lee, H.-P. Evaluation of health outcomes in osteoarthritis patients after total knee replace-ment: A two-year follow-up. health qual life outcomes. Health Qual. Life Outcomes 2010, 8, 87. [Google Scholar] [CrossRef] [Green Version]
- Meessen, J.M.T.A.; Leichtenberg, C.S.; Tilbury, C.; Kaptein, B.L.; Koster, L.A.; Slagboom, P.E.; Verdegaal, S.H.M.; Onstenk, R.; Zwaag, H.M.J.V.D.L.-V.D.; Kaptijn, H.; et al. Frailty in end-stage hip or knee osteoarthritis: Validation of the Groningen Frailty Indicator (GFI) questionnaire. Rheumatol. Int. 2018, 38, 917–924. [Google Scholar] [CrossRef] [Green Version]
- Van Leeuwen, D.M.; Van De Bunt, F.; De Ruiter, C.J.; Van Schoor, N.M.; Deeg, D.J.; Emanuel, K.S. Functioning Without Cartilage: Older People with Radiographic Knee Osteoarthritis Who Self-Report No Functional Limitations Do Score Lower on a Performance Battery. J. Aging Phys. Act. 2017, 25, 570–575. [Google Scholar] [CrossRef]
- Glover, T.L.; Goodin, B.R.; King, C.; Sibille, K.T.; Herbert, M.S.; Sotolongo, A.; Cruz-Almeida, Y.; Bartley, E.J.; Bulls, H.; Horgas, A.L.; et al. A Cross-sectional Examination of Vitamin D, Obesity, and Measures of Pain and Function in Middle-aged and Older Adults with Knee Osteoarthritis. Clin. J. Pain 2015, 31, 1060–1067. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Mehta, S.P.; Morelli, N.; Prevatte, C.; White, D.; Oliashirazi, A. Validation of physical performance tests in individuals with advanced knee oste-oarthritis. HSS J. 2019, 15, 261–268. [Google Scholar] [CrossRef]
- Gilbert, A.; Song, J.; Cella, D.; Chang, R.W.; Dunlop, D.D. What is an important difference in gait speed in adults with knee osteoarthritis? Arthritis Rheum. 2020, 31. [Google Scholar] [CrossRef]
- Debi, R.; Mor, A.; Segal, O.; Segal, G.; Debbi, E.; Agar, G.; Halperin, N.; Haim, A.; Elbaz, A. Differences in gait patterns, pain, function and quality of life between males and females with knee osteoarthritis: A clinical trial. BMC Musculoskelet. Disord. 2009, 10, 127. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Smith, S.; Woodburn, J.; Steultjens, M.P. Sex- and osteoarthritis-related differences in muscle co-activation during weight-bearing tasks. Gait Posture 2020, 79, 117–125. [Google Scholar] [CrossRef] [PubMed]
- Rice, D.A.; McNair, P.J.; Lewis, G.N. Mechanisms of quadriceps muscle weakness in knee joint osteoarthritis: The effects of prolonged vibration on torque and muscle activation in osteoarthritic and healthy control subjects. Arthritis Res. Ther. 2011, 13, R151. [Google Scholar] [CrossRef] [Green Version]
- Logerstedt, D.S.; Zeni, J., Jr.; Snyder-Mackler, L. Sex differences in patients with different stages of knee osteoarthritis. Arch. Phys. Med. Rehabil. 2014, 95, 2376–2381. [Google Scholar] [CrossRef] [Green Version]
- Culvenor, A.G.; Felson, D.T.; Niu, J.; Wirth, W.; Sattler, M.; Dannhauer, T.; Eckstein, F. Thigh muscle specific-strength and the risk of incident knee osteoarthritis: The in-fluence of sex and greater body mass index. Arthritis Care Res. 2017, 69, 1266–1270. [Google Scholar] [CrossRef]
- Brosseau, L.; Taki, J.; Desjardins, B.; Thevenot, O.; Fransen, M.; A Wells, G.; Imoto, A.M.; Toupin-April, K.; Westby, M.; Gallardo, I.C. Álvarez; et al. The Ottawa panel clinical practice guidelines for the management of knee osteoarthritis. Part two: Strengthening exercise programs. Clin. Rehabil. 2017, 31, 596–611. [Google Scholar] [CrossRef]
- Kolasinski, S.L.; Neogi, T.; Hochberg, M.C.; Oatis, C.; Guyatt, G.; Block, J.; Callahan, L.; Copenhaver, C.; Dodge, C.; Felson, D.; et al. 2019 American College of Rheumatology/Arthritis Foundation Guideline for the Management of Osteoarthritis of the Hand, Hip, and Knee. Arthritis Care Res. 2020, 72, 149–162. [Google Scholar] [CrossRef]

| Mean | SD | p Value | ||
|---|---|---|---|---|
| Age | F | 66.8 | 7.6 | 0.60 |
| M | 69.3 | 3.9 | ||
| all | 67.9 | 6.3 | ||
| BMI | F | 30.6 | 5.1 | 0.11 |
| M | 27.9 | 3.1 | ||
| all | 29.4 | 4.4 | ||
| Kellgren–Lawrence | F | 3.6 | 0.5 | 0.52 |
| M | 3.7 | 0.4 | ||
| all | 3.6 | 0.5 | ||
| KSS-Clinical | F | 57.1 | 19.0 | 0.69 |
| M | 54.8 | 16.5 | ||
| all | 56.1 | 17.7 | ||
| KSS-Functional | F | 55.2 | 12.5 | 0.004 |
| M | 68.5 | 14.3 | ||
| all | 61.1 | 14.7 | ||
| SPPB | F | 6.5 | 2.5 | 0.001 |
| M | 9.3 | 2.0 | ||
| all | 7.7 | 2.6 |
| Mean | SD | n | p Value | ||
|---|---|---|---|---|---|
| PI-OE | F | 0.63 | 0.23 | 21 | <0.0001 |
| M | 0.66 | 0.20 | 17 | <0.0001 | |
| all | 0.63 | 0.22 | 38 | ||
| PI-CE | F | 0.84 | 0.27 | 21 | <0.0001 |
| M | 0.82 | 0.21 | 17 | <0.0001 | |
| all | 0.83 | 0.23 | 38 | ||
| Reference data OE a | F | 0.45 | 0.14 | 117 | |
| M | 0.46 | 0.13 | 119 | ||
| all | n.a. | n.a. | - | ||
| Reference data CE a | F | 0.58 | 0.17 | 117 | |
| M | 0.65 | 0.19 | 119 | ||
| all | n.a. | n.a. | - |
| SI | p Value | AU | p Value | ||||||
|---|---|---|---|---|---|---|---|---|---|
| Mean | SD | n | Mean | SD | n | ||||
| Average (KOA limb and contralateral) OE | F | 64.5 | 12.1 | 21 | <0.0001 | 79.5 | 14.4 | 21 | 0.01 |
| M | 71.2 | 14.2 | 17 | 0.25 | 85.7 | 14.8 | 17 | 0.40 | |
| all | 67.4 | 13.3 | 38 | - | 82.2 | 14.7 | 38 | - | |
| KOA limb OE | F | 59.1 | 17.9 | 21 | <0.0001 | 74.8 | 21.9 | 21 | 0.01 |
| M | 69.1 | 19.7 | 17 | 0.21 | 84.5 | 20.6 | 17 | 0.39 | |
| all | 63.5 | 19.1 | 38 | - | 79.1 | 21.6 | 38 | - | |
| Contralateral Limb OE | F | 65.8 | 19 | 21 | 0.02 | 79.7 | 21.1 | 21 | 0.06 |
| M | 73.2 | 16.1 | 17 | 0.37 | 86.8 | 15.3 | 17 | 0.39 | |
| all | 69.1 | 17.9 | 38 | - | 82.8 | 18.8 | 38 | - | |
| Reference data OE a | F | 74.9 | 20.4 | 119 | 858 | 20.0 | 119 | ||
| M | 76.6 | 17.5 | 117 | 89 | 17.4 | 117 | |||
| all | n.a. | n.a. | - | n.a. | n.a. | - | |||
| Average (KOA limb and contralateral) CE | F | 36.5 | 9.5 | 21 | 0.06 | 47.7 | 13.2 | 21 | 0.11 |
| M | 37.4 | 13.8 | 17 | 0.31 | 50.4 | 17.0 | 17 | 0.40 | |
| all | 36.9 | 11.4 | 38 | - | 48.9 | 14.8 | 38 | - | |
| KOA limb CE | F | 37.8 | 12.9 | 21 | 0.21 | 48.1 | 15.4 | 21 | 0.16 |
| M | 35.3 | 13.3 | 17 | 0.16 | 48.5 | 17.2 | 17 | 0.36 | |
| all | 36.6 | 12.9 | 38 | - | 48.3 | 16 | 38 | - | |
| Contralateral Limb CE | F | 34.4 | 14.1 | 21 | 0.05 | 46.6 | 19.0 | 21 | 0.14 |
| M | 39.6 | 16 | 17 | 0.40 | 52.3 | 19.6 | 17 | 0.37 | |
| all | 36.7 | 15 | 38 | - | 49.1 | 19.2 | 38 | - | |
| Reference data CE a | F | 40 | 14.6 | 119 | 50.5 | 17.9 | 119 | ||
| M | 41.4 | 15.8 | 117 | 53.2 | 19.2 | 117 | |||
| all | n.a. | n.a. | n.a. | n.a. | - | ||||
| Mean | SD | n | p Value | ||
|---|---|---|---|---|---|
| VG-single average | F | 28.0 | 11.1 | 21 | 0.02 |
| M | 33.7 | 13.8 | 17 | 0.39 | |
| all | 30.5 | 12.5 | 38 | - | |
| VG-single reference data a | F | 35.2 | 16.0 | 119 | |
| M | 34.5 | 15.7 | 117 | ||
| all | n.a. | n.a. | - |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Labanca, L.; Barone, G.; Zaffagnini, S.; Bragonzoni, L.; Benedetti, M.G. Postural Stability and Proprioception Abnormalities in Patients with Knee Osteoarthritis. Appl. Sci. 2021, 11, 1469. https://doi.org/10.3390/app11041469
Labanca L, Barone G, Zaffagnini S, Bragonzoni L, Benedetti MG. Postural Stability and Proprioception Abnormalities in Patients with Knee Osteoarthritis. Applied Sciences. 2021; 11(4):1469. https://doi.org/10.3390/app11041469
Chicago/Turabian StyleLabanca, Luciana, Giuseppe Barone, Stefano Zaffagnini, Laura Bragonzoni, and Maria Grazia Benedetti. 2021. "Postural Stability and Proprioception Abnormalities in Patients with Knee Osteoarthritis" Applied Sciences 11, no. 4: 1469. https://doi.org/10.3390/app11041469
APA StyleLabanca, L., Barone, G., Zaffagnini, S., Bragonzoni, L., & Benedetti, M. G. (2021). Postural Stability and Proprioception Abnormalities in Patients with Knee Osteoarthritis. Applied Sciences, 11(4), 1469. https://doi.org/10.3390/app11041469






