Featured Application
A deeper insight into oral lesions potentially detectable in pediatric SARS-CoV-2 positive subjects and following COVID-19 vaccination may enhance clinicians’ preparedness to improve inter-disciplinary pediatric oral and general healthcare.
Abstract
A plethora of systemic manifestations of COVID-19 and adverse reactions to COVID-19 vaccines have been described in pediatric subjects. Therefore, the present systematic review primarily aimed to assess the prevalence and macro-microscopic features of oral lesions following SARS-CoV-2 infection, grading primary oral lesions based on COVID-19 forms, in pediatric subjects. The secondary aim was to evaluate the epidemiology, clinical appearance, and histopathology of oral lesions following the WHO Emergency Use Listing approved and EMA authorized vaccines, in relation to cases and vaccine characteristics. The study protocol was compliant with the PRISMA statement and registered on PROSPERO (CRD42022351821). Case reports, case series, and observational studies were electronically searched till 27 July 2022, on MEDLINE/PubMed, Scopus, and Cochrane library databases, and the PROSPERO register. Data from nine studies describing oral lesions following viral infection and two records reporting oral lesions following vaccine administration, evaluated through the ROBINS-I tool for quality, were independently extracted and qualitatively synthesized, resulting in scarce, jeopardized, and incomplete findings. Since most of the rare lesions recorded were a part of broad-spectrum systemic disorders and syndromes and, thus. undetailed or nonspecific, further studies should assess oral lesions following SARS-CoV-2 infection and vaccination in pediatric subjects, considering novel viral variants and newly developing vaccines.
1. Introduction
The first information regarding COVID-19 dates back to the first cases of SARS-CoV-2 infection, reported in December 2019, in Wuhan, Hubei Province in China. Three months later, on 11 March 2020, the World Health Organization (WHO) proclaimed the status of a global pandemic [1]. Various non-drug preventive measures, such as facial masks and social distancing, were adopted to control the spread of infection, later combined with vaccination. COVID-19 vaccines, although associated with Adverse Drug Reactions (ADRs) [2], similar to all medicinal products, have been effective in reducing the risk of viral transmission and infection, preventing severe forms of COVID-19, and decreasing the rate of hospitalization and death [3].
In the early stages of the COVID-19 pandemic, the number of pediatric SARS-CoV-2 positive subjects appeared to be very small [4]. The evidence suggested, at the time, that pediatric subjects frequently developed an asymptomatic or oligosymptomatic form of SARS-CoV-2 infection [4]. However, subsequent findings revealed that COVID-19 could evolve, in some pediatric cases, into the severe form of the disease. Indeed, cases diagnosed worldwide with a newly characterized syndrome, potentially linked to SARS-CoV-2 infection in children, identified as “Multisystem Inflammatory Syndrome in Children” (MIS-C), or “Paediatric Inflammatory Multisystem Syndrome Temporally Associated with COVID-19” (PIMS-TS), have been described [5,6]. This syndrome shares similar features with other entities already known, also potentially involving the oral cavity, such as Kawasaki Disease (KD), Toxic Shock Syndrome (TSS), Macrophage Activation Syndrome (MAS), and Secondary Hemophagocytic Lymphohistiocytosis (SHLH) [5,6]. However, the lower prevalence of severe COVID-19 observed in pediatric subjects compared to adult ones, and the contrasts with infections caused by other respiratory pathogens, has been partially explained by the age-related differences in viral receptor expression, immune function, and comorbidities rate [6]. Indeed, comorbidities are associated with an increased risk of severe disease, hospitalization, and death, even in pediatric subjects, although most of those hospitalized due to COVID-19 did not have comorbidities [6]. Nevertheless, 14,448,622 pediatric SARS-CoV-2 subjects were recorded in the United States until 24 August 2022 [7], representing 18.4% of all cases.
Consequently, COVID-19 vaccination may be especially beneficial for pediatric subjects at higher risk of severe disease and is thought to be effective in protecting against post-COVID-19 conditions and MIS-C/PIMS-TS [6]. Accordingly, to date, the European Centre for Disease Prevention and Control recommended the COVID-19 vaccination in 12–17 year-olds in all European countries, registering 26.2% of the pediatric population (<18 years of age) as having received at least one dose (on 25 August 2022) [6], with some countries also recommending booster doses for the same age group [6]. The European Medicines Agency (EMA) approved the mRNA BNT162b2 Comirnaty (Pfizer-BioNTech) and the mRNA-1273 Spikevax (Moderna) vaccines for 6–11 year-olds. Similarly, the Centers for Disease Control and Prevention reported that 38% of the pediatric population (<18 years of age) received at least one dose (on 24 August 2022) [7] and approved the mRNA BNT162b2 Comirnaty (Pfizer-BioNTech) vaccine administration in subjects ≥5 years old. The FDA also authorized the use of the mRNA-1273 Spikevax (Moderna) for children <5 years of age.
Therefore, the present systematic review primarily aimed to assess the prevalence and macro-microscopic features of oral lesions following SARS-CoV-2 infection, estimating the degree of association and grading primary oral lesions based on COVID-19 forms in pediatric (<18 years old) subjects. The secondary aim was to evaluate the epidemiology, clinical appearance, and histopathology of oral lesions diagnosed among pediatric subjects who had received at least one dose of the WHO Emergency Use Listing approved [7] and EMA authorized COVID-19 vaccines [8], in relation to the cases’ ages, genders, comorbidities and histories of COVID-19, and vaccine types, and the number of doses administered.
2. Materials and Methods
2.1. Protocol
The study protocol was developed before starting the literature search and analysis and registered with the PROSPERO systematic review registry under CRD42022351821.
The study was performed in accordance with the Preferred Reporting Items for Systematic Reviews and Meta-analyses (PRISMA) statement [9,10], freely available online.
Question formulation, search strategies definition, and study selection criteria were developed according to the PICO model [11].
The study question was “Did SARS-CoV-2 infection and related vaccines cause oral lesions in pediatric patients?”, focusing on:
- P—Population: young subjects (<18 years old) who have tested positive for SARS-CoV-2 or have received at least one dose of the COVID-19 vaccine;
- I—Intervention: SARS-CoV-2 infection and WHO Emergency Use Listing approved [7] and EMA authorized [8] COVID-19 vaccines.
- C—Comparison: adult subjects (>18 years) who tested positive for SARS-CoV-2 or received at least one dose of COVID-19 vaccine;
- O—Outcome(s): oral mucosal lesions associated with SARS-CoV-2 infection or COVID-19 vaccines.
2.2. Search Strategy
An electronic search was independently conducted by two reviewers (FDS, MPDP), on the MEDLINE/PubMed, Scopus, and Cochrane library databases, until 27 July 2022, to retrieve records written in English, without publication date or status restrictions, on oral lesions resulting from SARS-CoV-2 infection, applying the following keywords combined using Boolean operators:
- 1.
- Oral lesion OR oral manifestation OR oral signs
AND
- 2.
- COVID-19 OR SARS-CoV-2 OR Coronavirus disease 2019 OR novel coronavirus
AND
- 3.
- Pediatric OR child OR children.
A further electronic search was conducted with the same methods to obtain records on oral lesions following COVID-19 infection, adding to the previous keywords the following ones preceded by the Boolean operator AND: Vaccine OR vaccination OR anti-SARS-CoV-2.
The reference list of included articles were subsequently screened for potentially relevant articles, as previously described.
2.3. Study Selection Process
Study selection was independently conducted by two reviewers (FDS, MPDP) in compliance with the eligibility criteria applied to the studies on oral lesions in pediatric SARS-CoV-2 positive subjects, described in Table 1, and reported following COVID-19 vaccines, detailed in Table 2, respectively. Any discrepancies were resolved by discussion and consensus with a third reviewer (SM).

Table 1.
Study eligibility criteria for records reporting oral lesions in pediatric SARS-CoV-2 positive subjects.

Table 2.
Study eligibility criteria for records reporting oral lesions in pediatric subjects receiving at least one dose of the COVID-19 vaccine.
All titles and abstracts of articles found through the electronic search were screened. For records considered eligible for this systematic review, and for articles potentially relevant full-texts were obtained and screened.
2.4. Data Extraction and Collection
Data extraction and collection were independently conducted by three reviewers (FDS, MPDP, FDA) on a dedicated form developed considering the proposed models for intervention reviews on RCTs and non-RCTs [12,13]. No attempt to contact authors was performed to obtain or confirm data.
For each record included, concerning oral lesions in pediatric SARS-CoV-2-positive subjects, the following information was extracted and collected:
- -
- author, year and journal of publication, full citation of the article, study design, and funding;
- -
- population sample size, gender, mean age, comorbidities, current therapies for comorbidities, COVID-19 severity and treatment, and the time between disease onset and oral lesion occurrence;
- -
- oral lesion macroscopic and microscopic features, diagnostic procedures and treatment.
For each record included, concerning oral lesions in pediatric subjects receiving at least one dose of the COVID-19 vaccine, the following information was extracted and collected:
- -
- author, year and journal of publication, full citation of the article, study design and funding;
- -
- population sample size, gender, mean age, comorbidities, current therapies for comorbidities, COVID-19, COVID-19 vaccine type and the number of doses administered, and the time between vaccine administration and oral lesion occurrence;
- -
- oral lesion macroscopic and microscopic features, diagnostic procedures and treatment.
2.5. Data Synthesis
Data on primary and other oral lesions reported in pediatric SARS-CoV-2 positive subjects. and following COVID-19 vaccinations, diagnosed through a clinical exam, were exclusively considered for the current analysis. Conversely, data concerning oral lesions self-diagnosed through questionnaires, normal variations, such as fissured and geographic tongue, and likely pre-existing conditions and diseases were not considered. Reported primary oral lesions were classified as previously described [13].
A narrative synthesis focused on the described population, intervention, comparison, and outcome. A descriptive statistical analysis was conducted to qualitatively synthesize extracted data using the Microsoft Excel software 2019, Microsoft Corporation, Redmond, WA, USA):
- -
- to assess the overall prevalence of oral lesions following SARS-CoV-2 infection and COVID-19 vaccination in pediatric subjects;
- -
- to rank primary oral lesions following SARS-CoV-2 infection and COVID-19 vaccination in descending order of occurrence;
- -
- to estimate the frequency and type of primary oral lesions described following SARS-CoV-2 infection in pediatric subjects in relation to age, gender, comorbidities, ongoing treatments, and COVID-19 severity and therapies of the cases;
- -
- to estimate the frequency and type of the primary oral lesions described following COVID-19 vaccination in pediatric subjects in relation to age, gender, comorbidities, ongoing treatments, and history of COVID-19, and to vaccine type and administered dose of the cases.
2.6. Quality Assessment
The risk of bias of the non-randomized studies included in the present systematic review was assessed by three independent reviewers (FDS, MPDP, FDA) through the Risk of Bias in Non-randomized Studies of Interventions (ROBINS-I) [14] tool, considering biases due to confounding, selection of participants, classification of interventions, deviations from intended interventions, missing data, selection of the reported results and biases in the measurement of outcomes.
Accordingly, the risk of bias was judged as:
- -
- Low = low risk of bias for all domains;
- -
- Moderate = low or moderate risk of bias for all domains;
- -
- Serious = serious risk of bias in at least one domain, but not at critical risk of bias in any domain;
- -
- Critical = critical risk of bias in at least one domain.
3. Results
3.1. Study Selection
3.1.1. Oral Lesions in Pediatric SARS-CoV-2 Positive Subjects
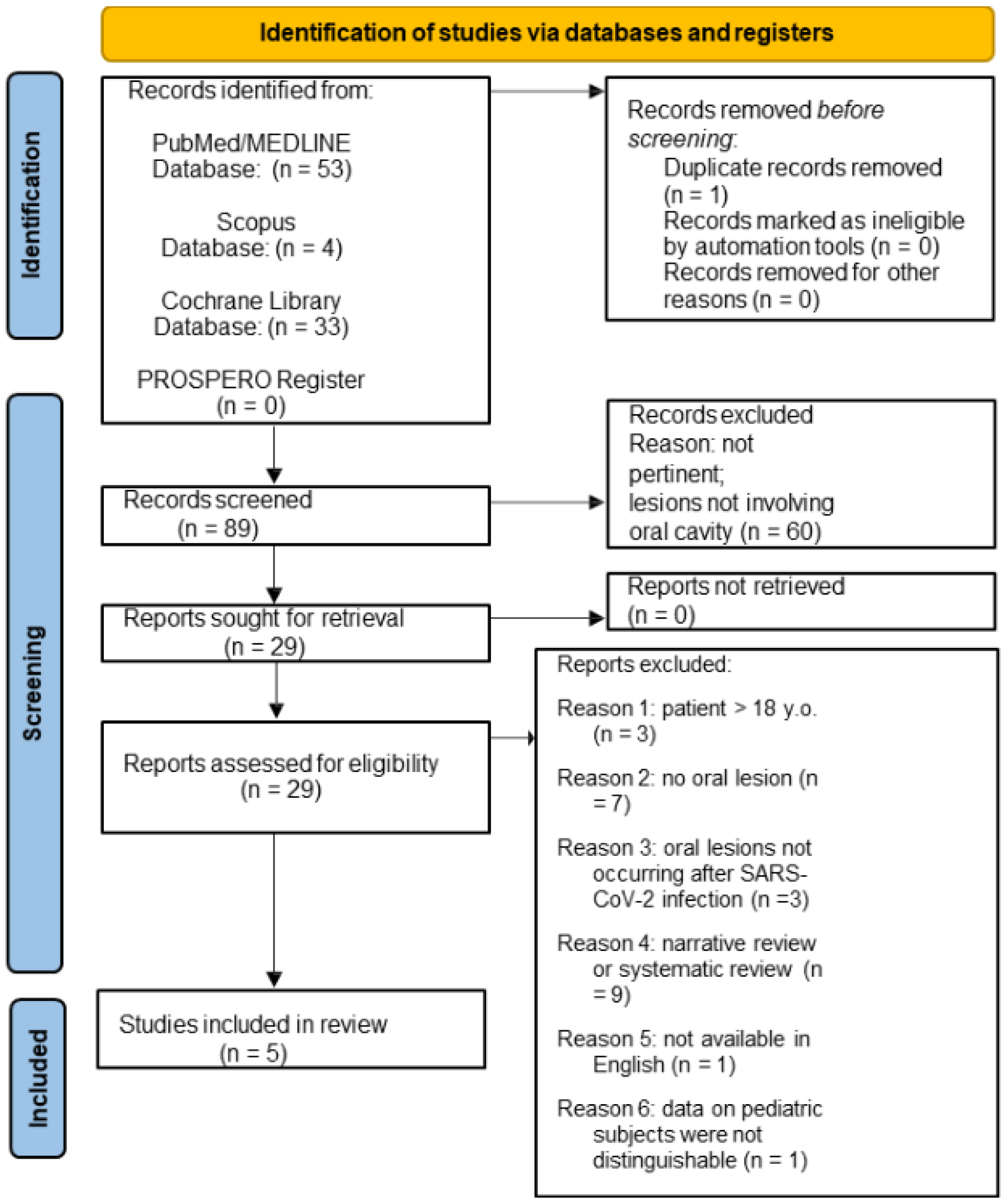
A total of 57 potential titles/abstracts concerning oral lesions in pediatric SARS-CoV-2 positive subjects were obtained from the electronic search, 53 from MEDLINE/PubMed, 4 from Scopus, 33 from Cochrane databases, and 0 from the PROSPERO register. After removing 1 duplicate, the 56 potentially relevant title/abstracts were screened, and 60 were excluded. Of the remaining 29 title/abstracts that were relevant and met the eligibility criteria, the full texts were screened, and an additional 24 records were excluded, specifically because of the following: 3 studies were on patients >18 years of age; 7 studies did not report oral mucosal lesions; 3 studies described oral manifestations not resulting from SARS-CoV-2 infection; 9 studies were narrative and systematic reviews; 1 full-text was not available in English (Chinese); 1 study data on pediatric subjects could not be differentiated from those on adult subjects. In total, 5 studies obtained from the electronic search concerning oral lesions in pediatric SARS-CoV-2-positive subjects were included in this systematic review. The study selection flowchart for electronically retrieved records is shown in Figure 1.
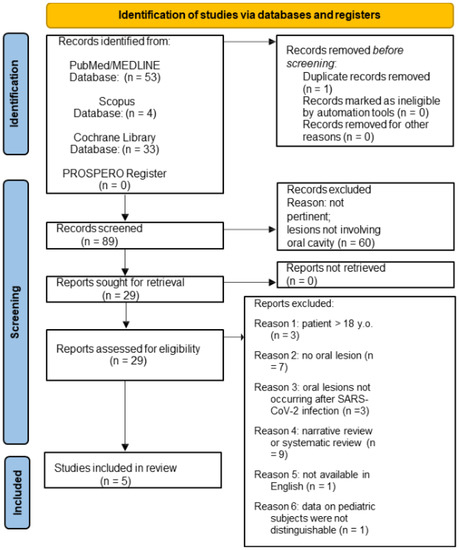
Figure 1.
PRISMA 2020 flow diagram for new systematic reviews which included searches of databases and registers only on oral lesions in pediatric SARS-CoV-2 positive subjects.
Four additional titles [15,16,17,18], retrieved from the manual search of 5 articles included in this systematic review [19,20,21,22,23] and compliant with the eligibility criteria, were also included. Finally, 9 records concerning oral lesions in pediatric SARS-CoV-2 positive patients were included in the present systematic review. All full-texts were freely available, so no contact with the authors had to be arranged.
3.1.2. Oral Lesions in Pediatric Subjects Following COVID-19 Vaccination
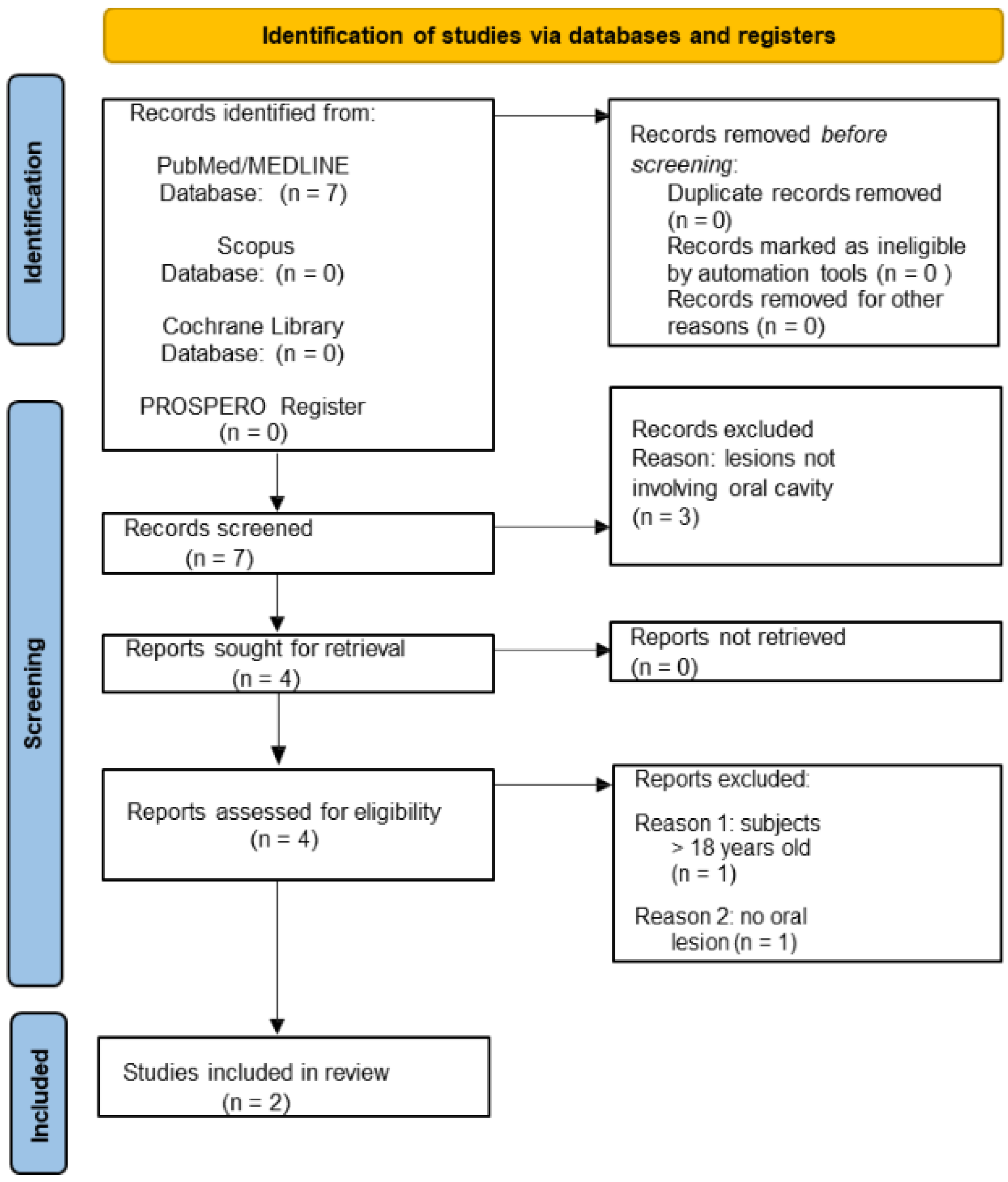
In addition, the study selection flowchart for electronically retrieved records concerning oral lesions diagnosed in pediatric subjects following at least one dose of WHO Emergency Use Listing approved [7] and EMA authorized [8] COVID-19 vaccines (Figure 2) shows that a total of 7 potential title/abstracts were obtained: 7 from the MEDLINE/PubMed, 0 from Scopus, 0 from Cochrane databases, and 0 from the PROSPERO register. The 7 potentially relevant title/abstracts were screened, and 3 records were excluded. Of the remaining 4 relevant abstracts that met the eligibility criteria full-texts were screened, and 2 additional articles were excluded, specifically because of the following: 1 study involved patients >18 years of age; 1 study did not report oral mucosal lesions. A total of 2 studies were obtained from the electronic search concerning oral lesions diagnosed in pediatric subjects following at least one dose of WHO Emergency Use Listing approved [7] and EMA authorized [8] COVID-19 vaccines.
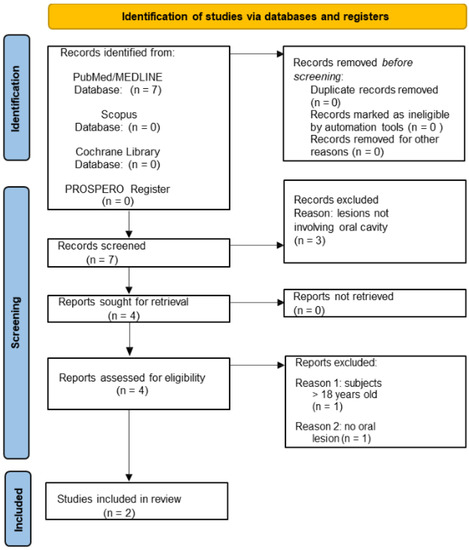
Figure 2.
PRISMA 2020 flow diagram for new systematic reviews which included searches of databases and registers only on oral lesions diagnosed in pediatric subjects following at least one dose of WHO Emergency Use Listing approved [7] and EMA authorized [8] COVID-19 vaccines.
The manual search of the 2 electronically retrieved articles included in the present systematic review resulted in no additional relevant records.
All full-texts were freely available, so no contact with the authors had to be arranged.
3.2. Study Characteristics and Qualitative Synthesis
3.2.1. Oral Lesions in Pediatric SARS-CoV-2 Positive Subjects
Of the 9 studies included on oral lesions in pediatric SARS-CoV-2 positive subjects, 3 were case series [15,18,21], 4 were case reports [16,17,19,23], and 2 were retrospective studies [20,22]. The overall population comprised 50 subjects, but since data concerning pediatric (<18 years) SARS-CoV-2 positive subjects diagnosed with oral lesions were exclusively extracted and analyzed, a total number of 35 cases, constituting 70% of the investigated population, was currently considered.
Table 3 synthesizes the study’s source, characteristics, methods, and oral outcomes, classified based on primary oral lesions [13], with reported diagnosis, therapy, and progression of the oral lesions. Only data compliant with inclusion/exclusion criteria were extracted and synthesized in Table 3; therefore, those concerning subjects >18 years old were not detailed.

Table 3.
Data extracted and collected from the studies included in the present systematic review. General information: First Author, year and journal of publication, reference, study design, funding. Population: sample size, mean age, gender ratio, comorbidities, and related ongoing treatments. COVID-19: severity, treatment, and time to oral lesions onset). Features of the reported primary oral lesions, classified as Erosions and Ulcers (Aphthous-like “Apht.”, Erythema Multiforme-like “EM”, Herpetiform “Herp.”, Plaques (white, red), Vesicles and Bullae, Maculae and Petechiae, others [13]: number (single/multiple); distribution (unilateral/bilateral asymmetrical or symmetrical); location; cyto/histopathology. Reported diagnosis, categorized as Oral Lichen Planus “OLP”, Stevens-Johnson Syndrome “SJS”, Ulcers, others, diagnostic procedure(s) performed, lesions therapy, and progression.
Pediatric SARS-CoV-2 positive subjects diagnosed with oral lesions comprised 20 males and 15 females, aged between 10 days and 14 years, with a mean age of 5.98. Comorbidities, reported in 4 studies [16,19,21,23], were the following: glucose-6-phosphate deficiency and MIS-C mimicking Kawasaki disease in a 13-year-old female [19]; dystonia and epilepsy in a 9-year-old male [16]; cryptorchidism in 15-day-old male [21]; immune thrombocytopenic purpura in 8-year-old female without ongoing treatment [23]. In 4 studies, the data were missing [15,17,18,20], and in 1 study, the patient had no comorbidities [22].
Of the 35 study participants, 17 were hospitalized [15,16,18,19,21,22,23] due to COVID-19, and 2 subsequently died [15,19]. In 1 study [20] reporting 15 cases, data on COVID-19 severity were missing. COVID-19 treatment, not specified in 1 record [20], was reported in 8 studies [15,16,17,18,19,21,22,23]. Specifically, patients had undergone the following: IVIG in 7 studies [15,17,18,19,21,22,23]; plasma therapy in 1 study [22]; artificial ventilation in 3 studies [15,19,22]; vitamin D supplementation in 1 study [21]; antibiotics in 4 studies [15,19,21,22]; antivirals in 3 studies [15,19,22]; antiprotozoals in 1 study [1]; antiemetics in 1 study [19]; monoclonal antibodies in 3 studies [15,19,22]; FAS in 5 studies [15,16,19,22,23]; inotropic therapy in 2 studies [15,22]; anticoagulants in 3 studies [17,19,22]; antiaggregants in 1 study [22]; phosphodiesterase-III inhibitors in 1 study [19]; sympathomimetics in 1 study [19]; stem cell treatment in 1 study [15]; normal saline bolus in 1 study [19]; parenteral nutrition in 1 study [21]; VV-ECMO in 1 study [15]; unspecified creams for topical use in 1 study [21]; eye drops in 1 study [21]. In all 9 studies included in this systematic review, data on time to oral lesion onset were missing.
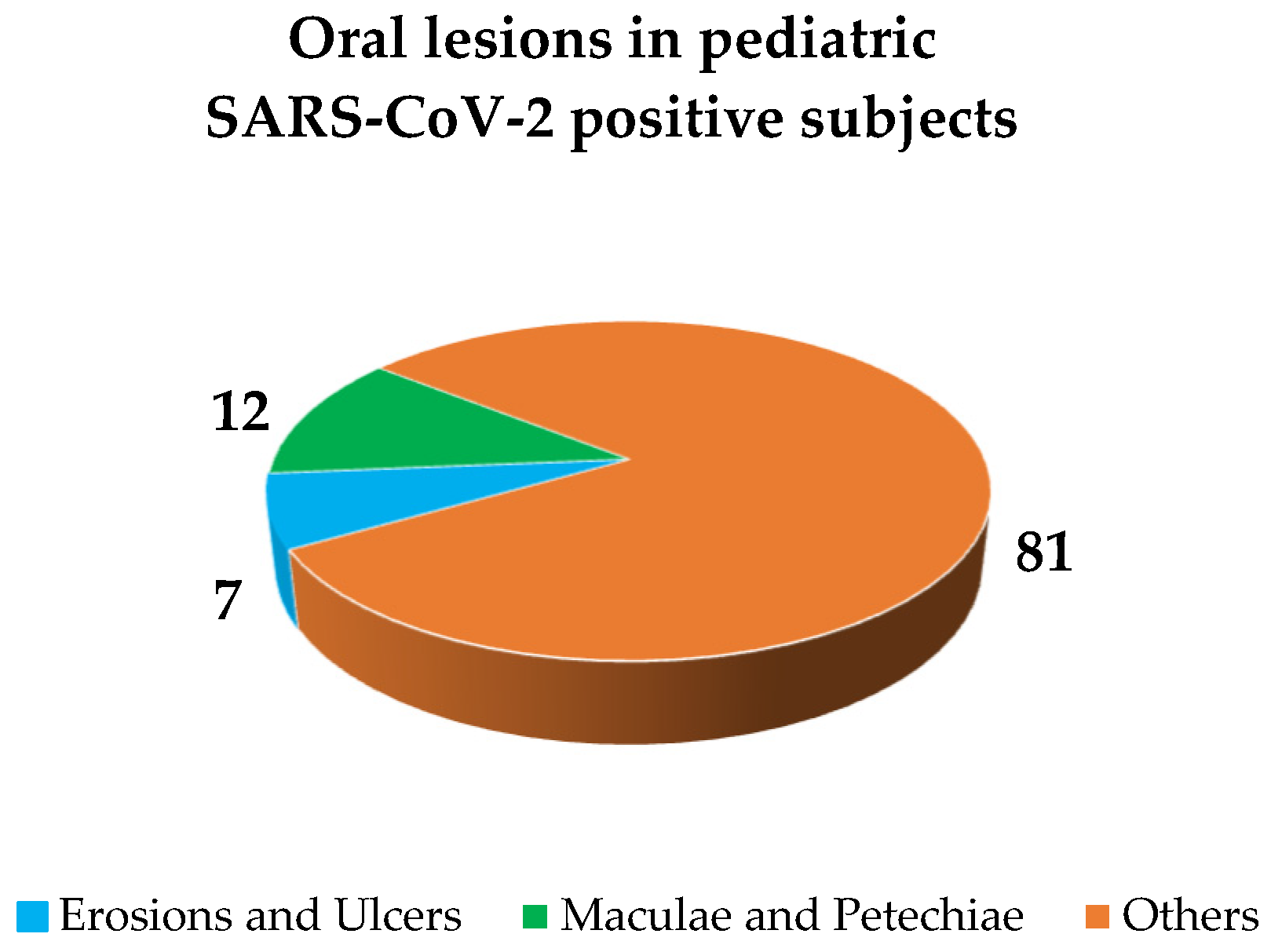
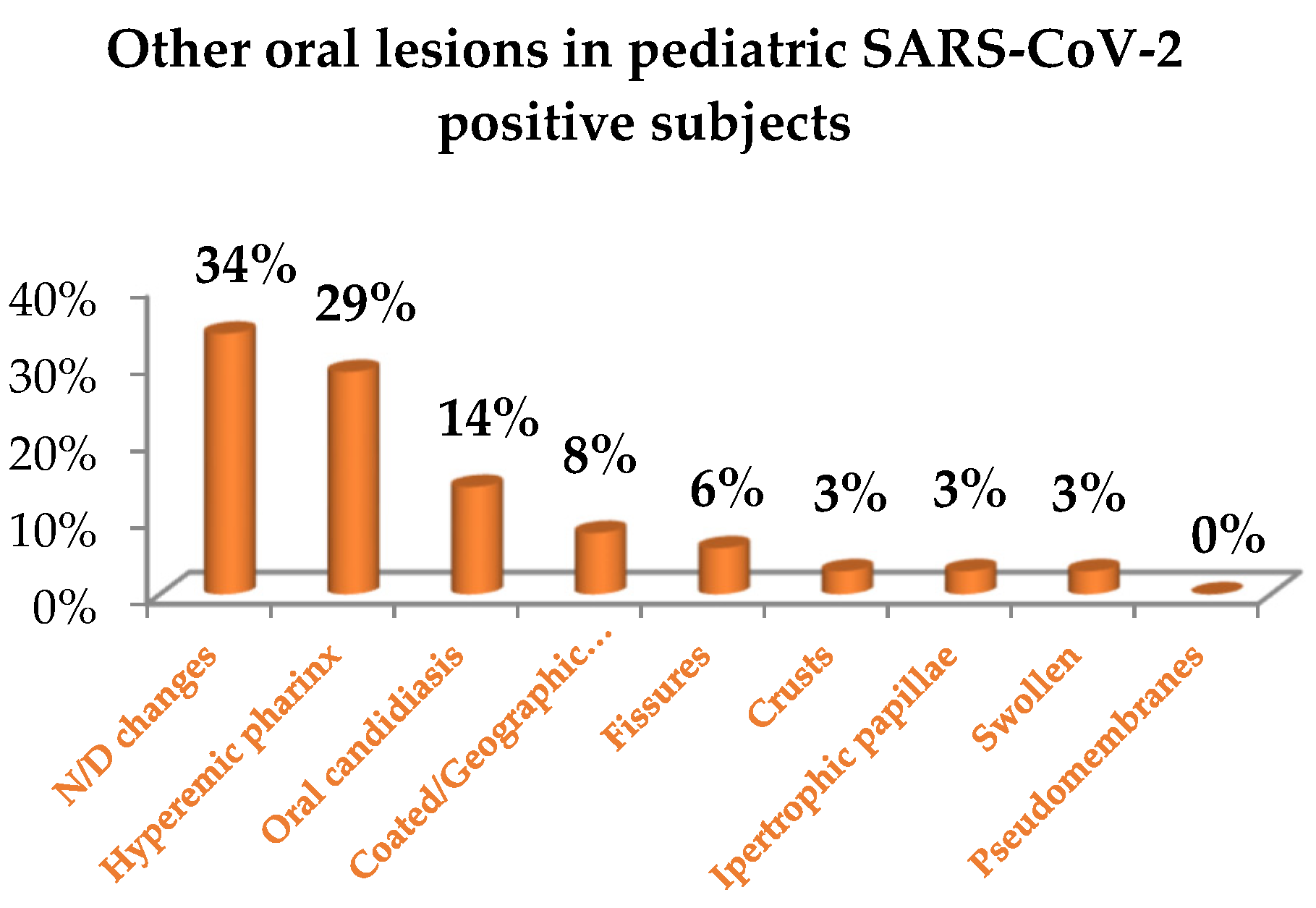
The primary oral lesions, categorized as per a previously proposed classification [13], and accounting for 18.61% of all oral lesions described (Figure 3), were as follows: nonspecific erosions and ulcers in 6.98% (n = 3) [15,16,18]; maculae and petechiae in 11.63% (n = 5), particularly in the form of erythema in 4.65% (n = 2) [15,19], purpura in 2.33% (n = 1) [23], ecchymosis in 2.33% (n = 1) [23] and petechiae in 2.33% (n = 1) [23]. Other oral lesions, detailed in Figure 4, were reported in 81.4% (n = 35) of cases (Figure 3), particularly in the form of: fissures in 4.65% (n = 2) [17,19]; hypertrophic papillae in 2.33% (n = 1) [17]; oral candidiasis in 11.63% (n = 5) [20,21]; geographic tongue in 2.33% (n = 1) [20]; coated tongue in 4.65% (n = 2) [20]; hyperemic pharynx in 23.26% (n = 10) [20]; crusts in 2.33% (n = 1) [18]; swollen in 2.33% (n = 1) [16]; nonspecific oral mucosal changes were reported in 27.91% (n = 12) of cases [15,18,22]. Oral lesions affected in descending order of occurrence the lips [19,22,23], pharynx [20], tongue [17,18,20], and the gingiva [18]; affected site was not better defined for 17 [15,18,22,23] and missing for 6 oral lesions reported [16,20,21]. No cytological nor histological investigations were recorded in any of the 9 studies included in this systematic review.
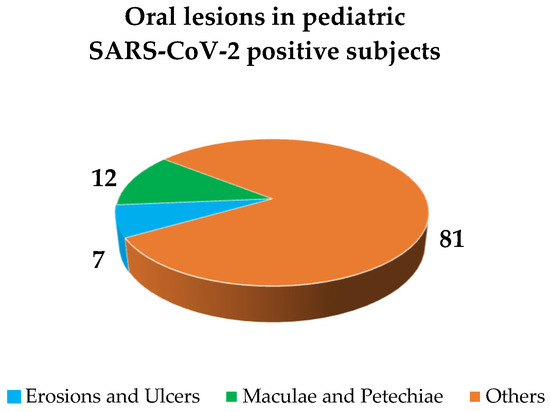
Figure 3.
Frequency of reported oral lesions in pediatric SARS-CoV-2 positive subjects: primary oral lesions and other lesions [13].
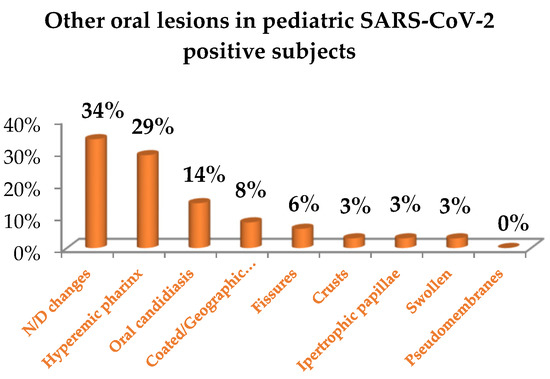
Figure 4.
Other lesions of the oral mucosa in pediatric SARS-CoV-2 positive subjects [13].
The following were reported definitive diagnoses: Kawasaki disease in 12 cases [15,17,18,22], incomplete Kawasaki disease in 1 case [15], oral candidiasis in 5 cases [20,21], ulcer in 1 case [16], erythema multiforme in 1 case [18], immune thrombocytopenic purpura in 1 case [23]. In 15 cases, the final diagnosis was not specified and the reported lesions were: coated tongue (2 cases) [20], swollen tongue (1 case) [16], geographic tongue (1 case) [20], hyperemia of the pharynx (10 cases) [20], erythematous cracked lips (1 case) [19]. Diagnostic procedures, not reported in 1 study [16], were described in 8 studies: RT-PCR for SARS-CoV-2 detection in 7 studies [15,17,18,19,21,22,23]; serological tests in 7 studies [15,17,18,19,21,22,23]; Computed Tomography; in 4 studies [15,18,19,22]; ultrasound investigations in 4 studies [15,17,19,23]; measurements of vital parameters in 5 studies [17,19,20,21,23]; in X-rays in 4 studies [17,19,21,23]; microbiological examinations in 4 studies [17,18,19,23]. The treatment performed for oral lesions was specified in 1 study [21] involving three patients under nystatin, combined in one case with fluconazole iv; in all the remaining studies, the data were missing [15,16,17,18,19,20,22,23]. The data on lesion progression were missing in all 9 studies included in this systematic review.
3.2.2. Oral Lesions Diagnosed in Pediatric Subjects following COVID-19 Vaccination
Of the 2 studies included on diagnosed pediatric subjects receiving at least one dose of WHO Emergency Use Listing approved [7] and EMA authorized [8] COVID-19 vaccines, 1 was a case report [24] and 1 a case series [25], from which only data concerning the pediatric patient were extracted. The number of cases diagnosed with oral lesions following COVID-19 vaccines was 2.
Table 4 synthesizes the study’s source, characteristics, methods, and oral outcomes, classified based on primary oral lesions [13], with reported diagnosis, therapy, and progression of the oral lesions. Only data compliant with inclusion/exclusion criteria were extracted and synthesized in Table 3; therefore, those concerning subjects > 18 years old were not detailed.

Table 4.
Data extracted and collected from the studies included in the present systematic review. General information: First Author, year and journal of publication, study design, reference; funding. Population: sample size, mean age, gender ratio, comorbidities, and related ongoing treatments. Intervention: COVID-19 vaccine type, dose, time to oral lesions onset. Features of the reported primary oral lesions, classified as Erosions and Ulcers (Aphthous-like “Apht.”, Erythema Multiforme-like “EM”, Herpetiform “Herp.”, Plaques (white, red), Vesicles and Bullae, Maculae and Petechiae, others [13]: number (single/multiple); distribution (unilateral/bilateral asymmetrical or symmetrical); location; cyto/histopathology. Reported diagnosis, categorized as Oral Lichen Planus “OLP”, Stevens-Johnson Syndrome “SJS”, Ulcers, others, diagnostic procedure(s) performed, lesions therapy, and progression.
The pediatric study population with oral lesions following COVID-19 vaccines consisted of 2 males, both 15 years old. The reported comorbidities and treatments were aseptic meningitis [24] and West syndrome treated with valproate [25]. In the first case, the patient had a negative history of COVID-19 [24], while in the second case, the data was missing [25].
The vaccine administered in both cases was the COVID-19 mRNA BNT162b2 Comirnaty (Pfizer-BioNTech) [24,25]. Oral lesions occurred 13 days after the second vaccine dose [24] and 7 days after the first vaccine dose administration [25], respectively, with a mean onset time of 10 days.
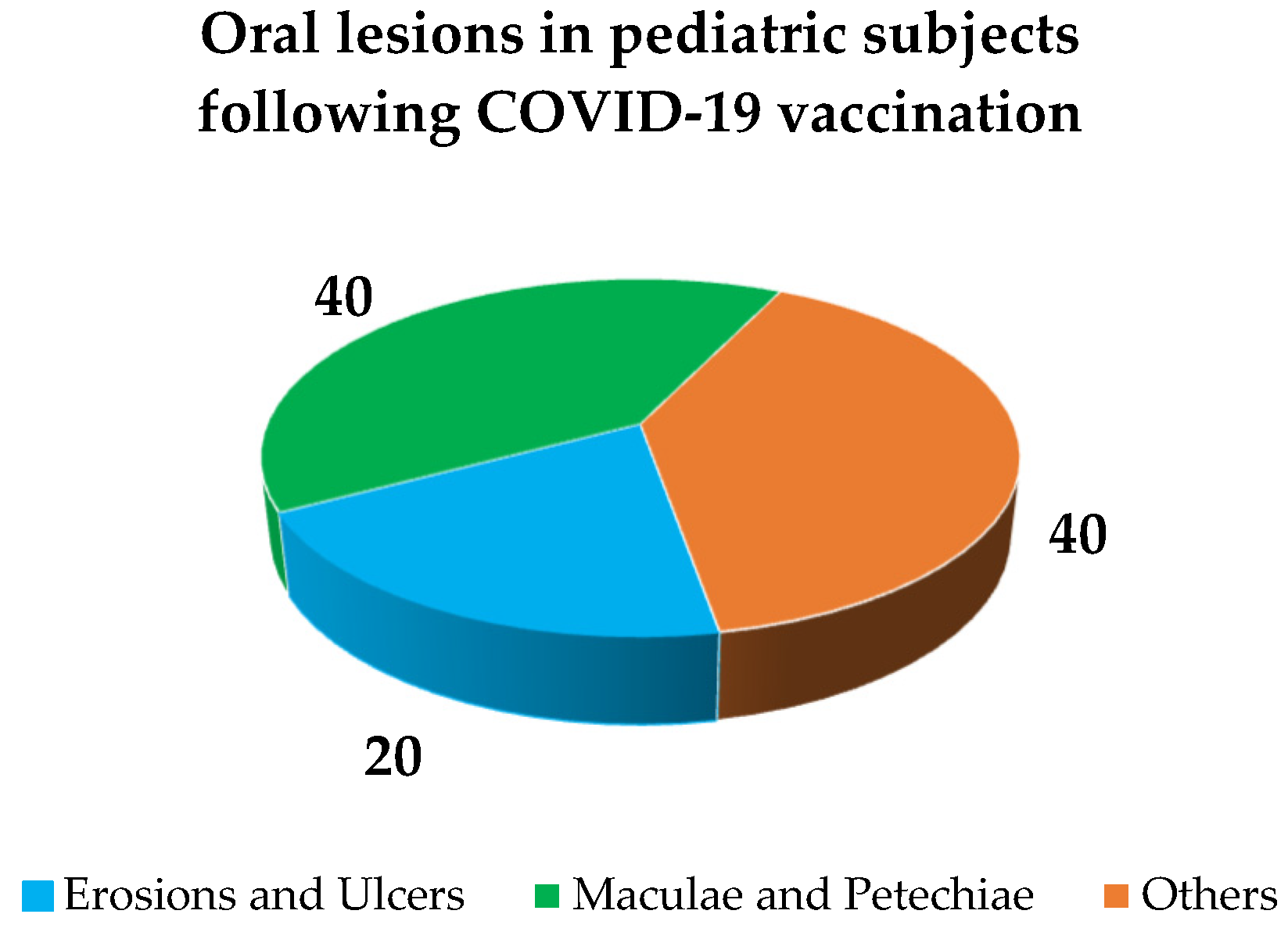
Primary oral lesions reported in pediatric subjects following COVID-19 vaccination, categorized as per a previously proposed classification [13] for 60% of all lesions of the oral mucosa detected (Figure 5) and accounted for were: erosions and ulcers (40%, n = 2) with a herpetiform (50%, n = 1) and unspecified (50%, n = 1) patterns, maculae and petechiae (20%, n = 1). Other lesions were (40%, n = 2), crusts (50%, n = 1) and pseudomembranes (50%, n = 1), as shown in Figure 6. Oral lesions distribution was bilateral and asymmetrical [24] in one case and unspecified in the other case [25], affecting the lips [24,25], cheeks [24], and vermilions [25], along with additional other unspecified intra-oral sites. No cytology/histopathology was recorded.
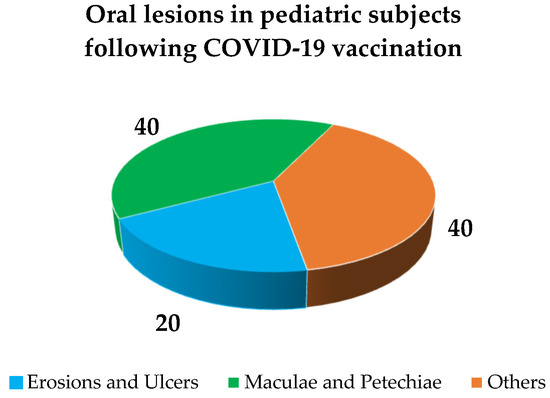
Figure 5.
Frequency of reported oral lesions in pediatric subjects following COVID-19 vaccination: primary oral lesions and other lesions [13].
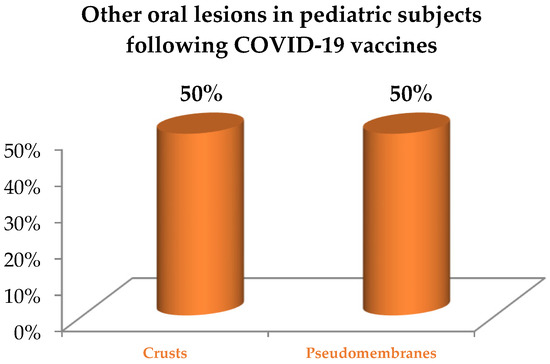
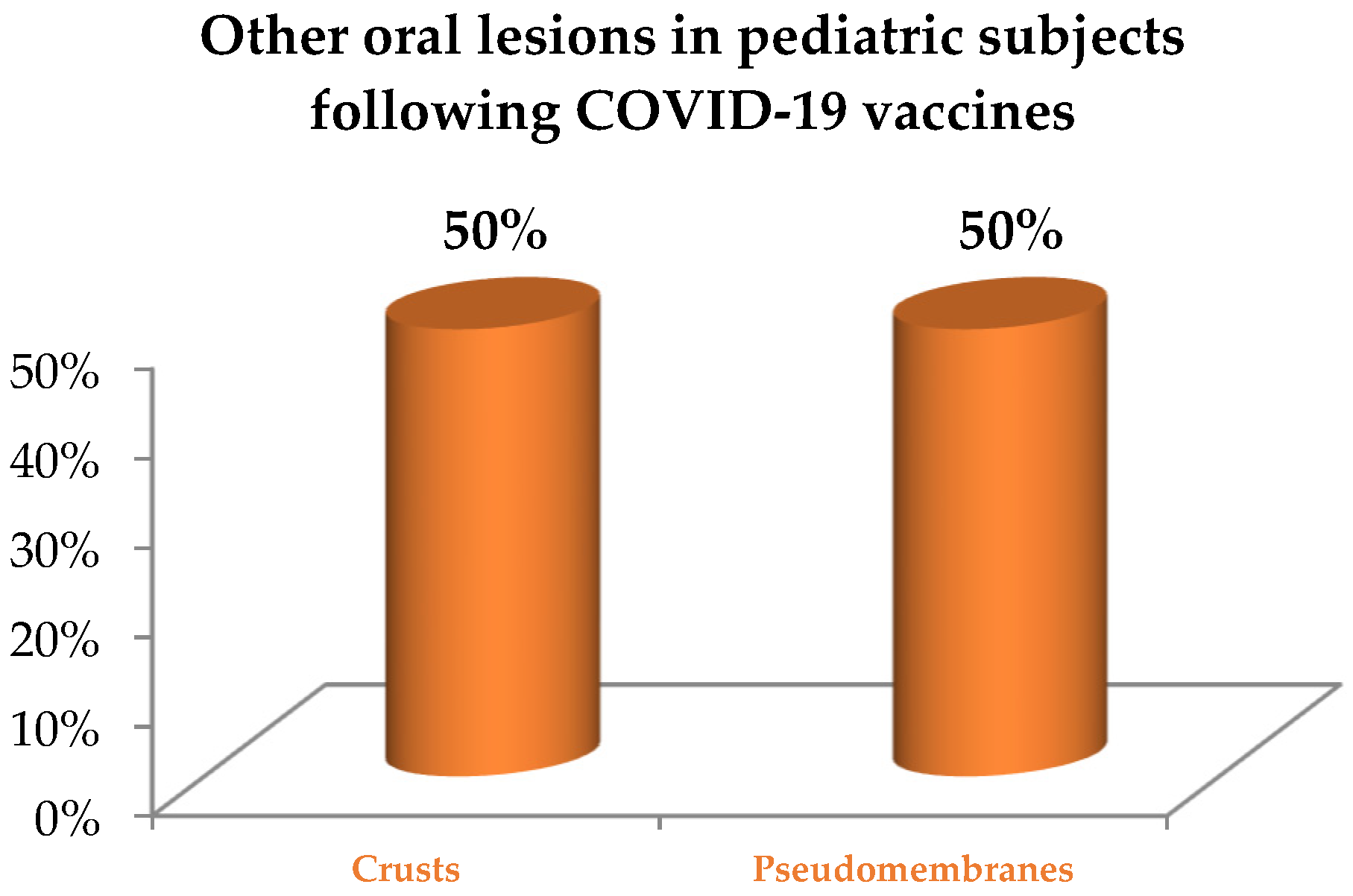
Figure 6.
Other lesions of the oral mucosa in pediatric subjects following COVID-19 vaccination [13].
Reported definitive diagnoses were Behçet’s disease [24] in one case treated for oral lesions with NSAIDs, antivirals, and antibiotics [24], and Erythema Multiforme, in the case treated for oral lesions with FAS [25] showing clinical improvement in 7 days.
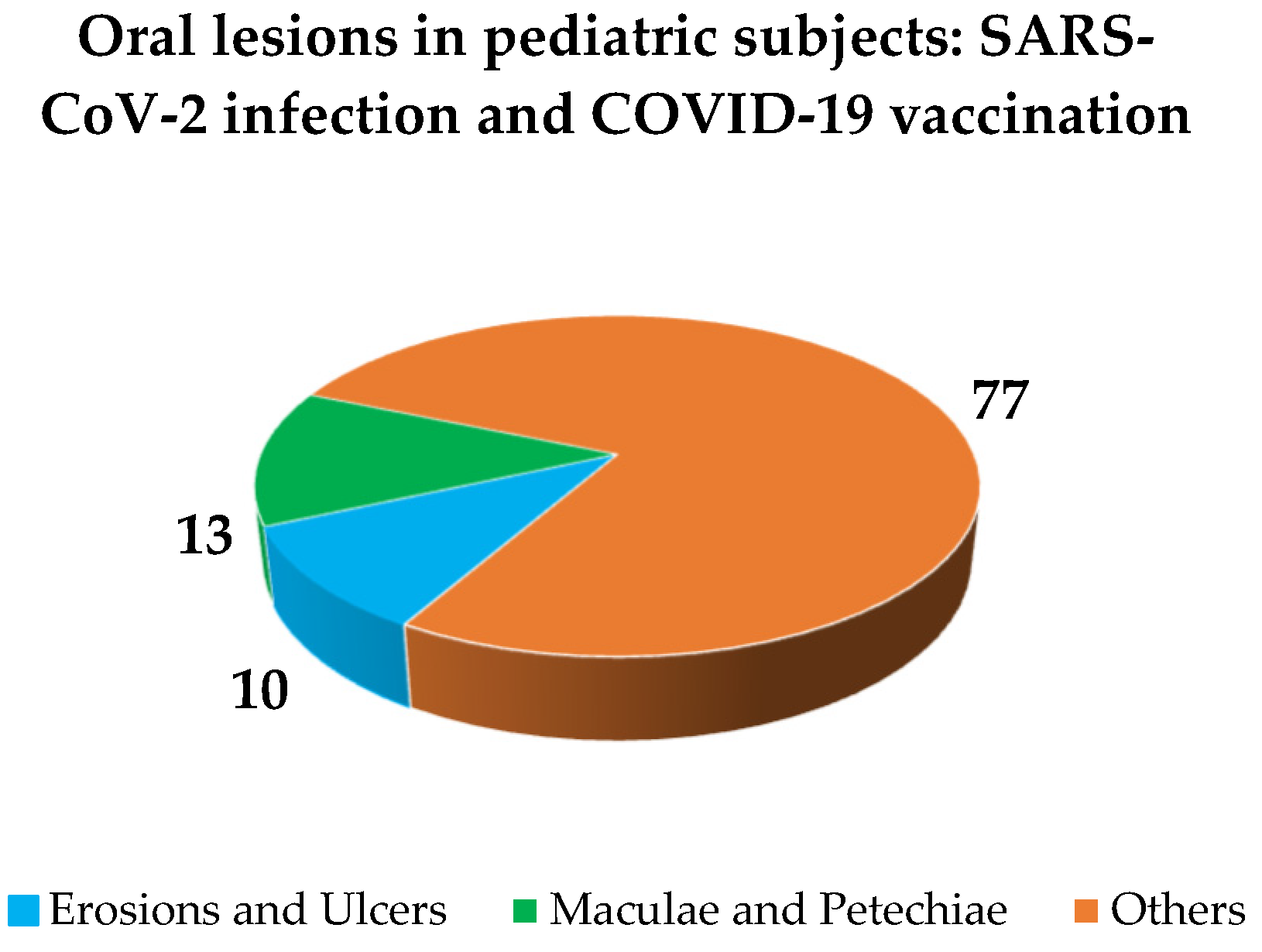
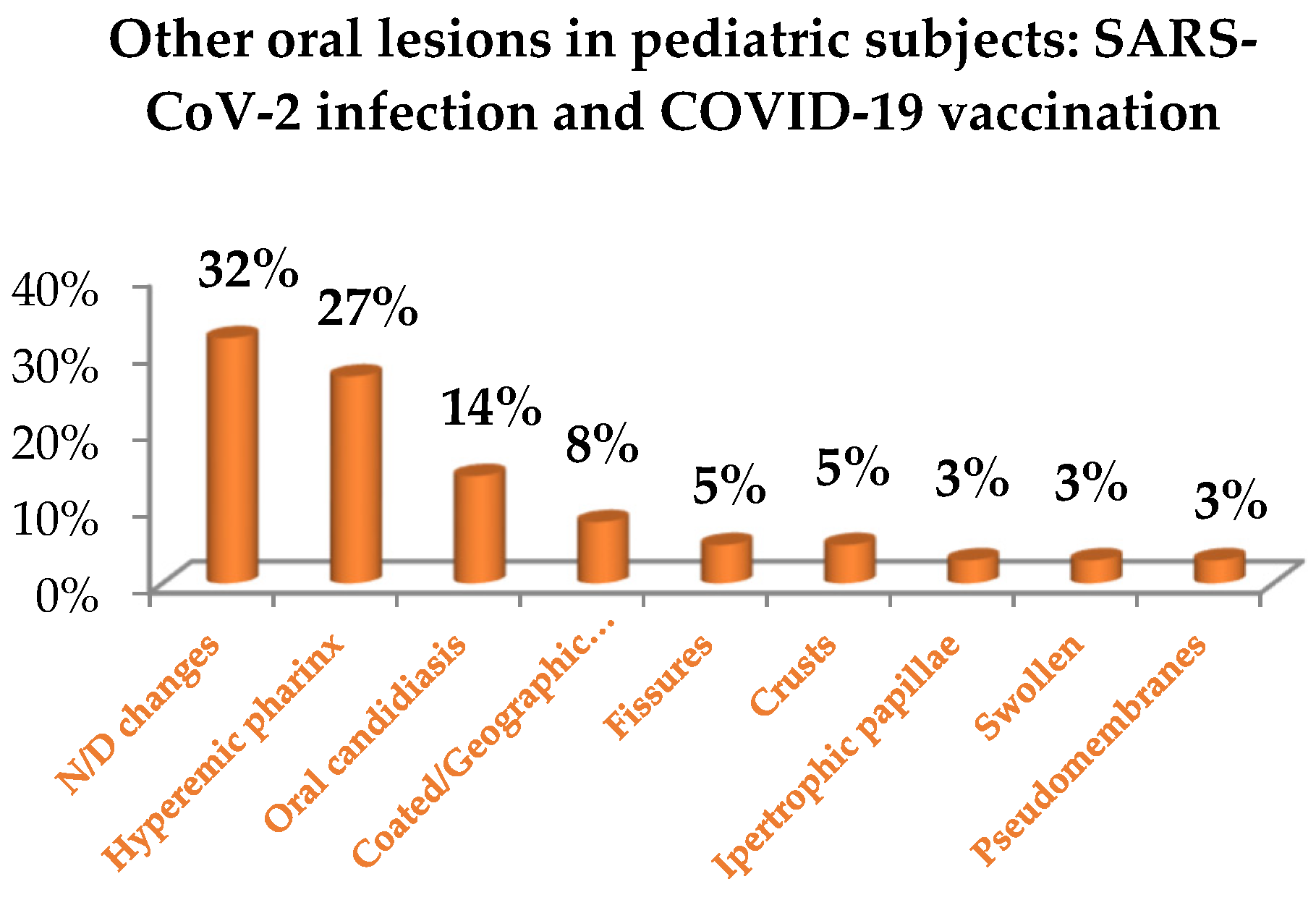
The overall impact of COVID-19 on primary oral lesions, jointly considering those resulting from SARS-CoV-2 infection (Figure 7) and COVID-19 vaccines (Figure 8), in pediatric subjects, was as follows: erosions and ulcers (10%, n = 5); maculae and petechiae (13%, n = 6); other types of oral manifestations (77%, n = 37), specifically: undefined oral mucosal changes (32%, n = 12), hyperemia of pharynx (27%, n = 10), oral candidiasis (14%, n = 5), coated and geographic tongue (8%, n = 3), crusts (5%, n = 2), fissures (5%, n = 2), hypertrophic papilla (3%, n = 1), swollen (3%, n = 1), pseudomembranes (3%, n = 1).
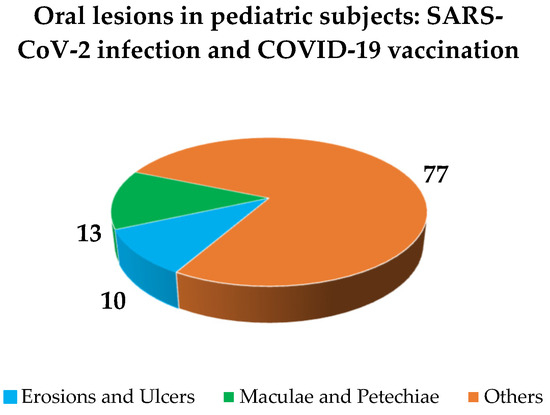
Figure 7.
Frequency of reported oral lesions in pediatric subjects: SARS-CoV-2 infection and COVID-19 vaccination [13].
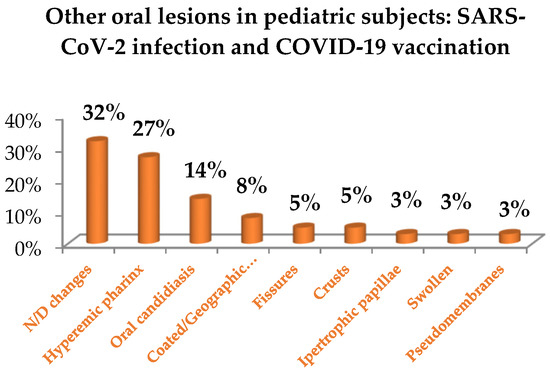
Figure 8.
Other lesions of the oral mucosa in pediatric subjects: SARS-CoV-2 infection and COVID-19 vaccination.
3.3. Quality Assessment
The risk of bias of the non-randomized studies included in the present systematic review is reported in Table 5.

Table 5.
Risk of bias of all the studies included in the systematic review and listed in alphabetical order. For each of the seven domains assessed, Y = low risk of bias (green), PY = a moderate risk of bias (blue); PN = serious risk (orange), N = critical risk of bias (red), and NI = no information (black).
4. Discussion
The primary aim of the present systematic review was to assess the prevalence and macro-microscopic features of oral lesions following SARS-CoV-2 infection, estimating the degree of association and grading primary oral lesions based on COVID-19 forms in pediatric subjects. The secondary aim was to evaluate the epidemiology, clinical appearance, and histopathology of oral lesions diagnosed among pediatric subjects (<18 years old) who had received at least one dose of the WHO Emergency Use Listing approved [7] and EMA authorized COVID-19 vaccines [8], in relation to cases’ ages, genders, comorbidities and histories of COVID-19, and vaccine types and number of doses administered.
Eleven studies were included in the present systematic review, 9 describing 35 cases diagnosed with oral lesions following SARS-CoV-2 infection and 2 reporting 2 cases following vaccination, respectively, thus, involving a total of 37 pediatric subjects.
4.1. Oral Lesions in Pediatric SARS-CoV-2 Positive Subjects
The overall prevalence of cases diagnosed with oral lesions following SARS-CoV-2 infection among pediatric subjects accounted for 35 patients. Although this might seem low, it should actually be considered in line with the low number of infected pediatric subjects, especially in the early stages of the COVID-19 pandemic [1]. Subsequently, the number of reported cases among pediatric SARS-CoV-2 positive subjects spiked, especially during the spread of the Omicron viral variant and the concomitant generalized reduction in public health and social preventive measures. By 24 July 2022, pediatric SARS-CoV-2 positive subjects constituted 26.82% of all cases and 1.38% of deaths worldwide [7]. However, such epidemiologic data may be biased by the frequent asymptomatic presentations and milder symptoms characterizing SARS-CoV-2 infection in pediatric subjects [4], potentially causing underreporting. For the same reason, it may be hypothesized that the presently computed prevalence of oral lesions in SARS-CoV-2 positive pediatric subjects might have been mainly affected by the fact that most of them were a-/oligo-symptomatic [4,5] under domiciliary or self-care, so oral lesions may have been under-acknowledged. As a counterpart, oral lesions in pediatric subjects with severe forms of COVID-19, potentially showing oral and multi-systemic involvement, may have been underdiagnosed, given patients’ life-threatening conditions. Indeed, the attention to the impact of the SARS-CoV-2 infection on children has dramatically increased upon the observation of a hyperinflammatory syndrome, albeit rare, complicating recovery from COVID-19, and known as “Multisystem Inflammatory Syndrome in Children” (MIS-C) or “Paediatric Inflammatory Multisystem Syndrome Temporally Associated with COVID-19” (PIMS-TM) [6]. Furthermore, such a low prevalence of oral lesions in pediatric SARS-CoV-2 positive subjects may also be due to the exclusion of normal variation of the oral mucosa, such as geographic tongue, which is considered the most frequent oral mucosal condition in children [26,27], from the present analysis. Similarly, also self-diagnosed mucosal alterations and pre-existing conditions were not currently considered, in the attempt to point out those lesions likely attributable to either viral direct cytotoxic effect or COVID-19 pathogenesis, complications, and therapies [28].
The higher incidence of oral lesions following viral infection in young males (M:F = 20:15), also observed in adult subjects (M:F = 3156:1769) [13], may be due to the higher prevalence of the severe forms of COVID-19 requiring hospitalization registered in pediatric males. Indeed, according to the study by Peckham et al. [29], involving 3.111.714 cases worldwide, although male and female pediatric subjects have an equivalent risk of becoming infected, males develop severe forms of the disease, requiring hospitalization or, unfortunately, leading to death, more frequently compared to females. Thus, it may be assumed that oral lesions have been diagnosed most in male pediatric subjects compared to female ones due to hospitalization; in fact, oral cavity inspection is hardly conducted in domiciliary and self-care settings. Alternatively, it may be proposed that such oral lesions may occur in the severe forms of the disease, most frequently developing in males. However, given the low number of pediatric cases diagnosed with oral lesions following SARS-CoV-2 infection, their overall prevalence remains under study.
Similarly, since data concerning COVID-19 severity were missing in 15 out of 35 cases, albeit 17 males were hospitalized and 2 of them subsequently died, so the degree of association of oral lesions with SARS-CoV-2 infection, as previously performed for HIV infection [30], could not be computed.
The time between SARS-CoV-2 positivity and the appearance of oral lesions, previously described by Orilisi et al. in an adult population [31], has not been reported in any study concerning pediatric subjects. Nonetheless, it may be proposed that understanding whether the oral lesions may be considered a potential predictor of a-/pre-symptomatic infection, similar to smell and taste alterations [32,33], or an indicator of illness worsening, as suggested for adult subjects [32,33], developing consequent to systemic involvement, could be a crucial wake-up call and aid clinicians in timely therapeutic management, improving patients’ outcomes.
Very heterogeneous denominations on primary oral lesions emerged from the data extracted; this may be partially explained by the fact that oral lesions were reported, in many of the studies included in this systematic review, as an additional sign of systemic syndromes, and were, therefore, detected and described by healthcare workers not specialized in oral medicine [32]. Such a practice may have also led to misdiagnoses with an under-estimation of primary oral lesions, which are characterized by specific macro-microscopic features, and a contextual over-estimate of other oral lesions [13]. Primary oral lesions, specifically erosions and ulcers (6.98%) and maculae and petechiae (11.63%), were diagnosed in only 19% of pediatric cases, while no vesicles and bullae nor plaques were identified. Conversely, data from adult subjects showed a higher prevalence of erosive-ulcerative lesions, 48.96%, and maculae and petechiae (16.44%), along with vesicles and bullae (4.97%), and plaques (0.25%) [14]. In addition, other lesions were the most prevalent ones, reported in 77% of pediatric compared to 20.64% of adult cases [14]. These other lesions most frequently included those not having defined alterations of the oral mucosa (27.91%), nonspecific hyperemic pharynx (23.26%), and oral candidiasis (11.63%). The latter is considered extremely frequent in pediatric subjects and as a co-infection, secondary to immune impairment and general detrimental conditions, and is the most frequent oral manifestation in HIV-positive subjects [34]. However, given the paucity of data concerning primary oral lesions, their final grading based on COVID-19 forms [35] could not be conducted.
4.2. Oral Lesions Pediatric Subjects Following COVID-19 Vaccination
Adverse drug reactions are dangerous sequelae potentially following the administration of medicinal products [1,2] and vaccines [3,36]. The latter, including vaccines against Influenza, Hepatitis-B, Mumps, Measles, Rubella viruses, Clostridium tetani, and others [3,4,5], can be responsible for mucocutaneous reactions that also involve the orofacial district and oral mucous membranes. In particular, orofacial ADRs, with swelling of the face, throat, and tongue, Bell’s facial paralysis, and mucocutaneous lesions of different phenotypes, also comprising lesions of the oral mucosa in the adult population, have been reported following COVID-19 vaccines [37].
Only 2 pediatric subjects were reported in the literature as diagnosed with oral lesions following COVID-19 vaccines. Such a low prevalence may be attributable to the fact that vaccines generally appear to be rarely associated with oral ADRs [38], and these are routinely described together with any skin lesions and, thus, identified as mucocutaneous ADRs. In addition, the detection of oral lesions generally requires appropriate clinical examination. Moreover, epidemiologic data about the overall prevalence of ADRs in the pediatric population, especially outpatients, are highly lacking and often lacunose concerning incidence, clinical manifestations, and the triggering or causative drugs [38]. Therefore, it may be proposed that oral lesions in pediatric subjects who received at least one dose of COVID-19 vaccine may have been misdiagnosed and confused with other clinical pictures frequently found in pediatric patients, such as Candida Albicans or Herpes Simplex virus type-1 oral infections, usually not requiring further diagnostic investigation in routine clinical practice. It is also possible that the involvement of the oral cavity alone and the tendency for resolution, with or without therapy, precluded in some cases the reporting of mild adverse oral reactions, which were, therefore, under-reported. As a counterpart, great attention was given to severe systemic ADRs in the pediatric subjects who have undergone COVID-19 vaccination. Indeed, although rarely described, myocarditis/pericarditis, typically occurring in young males within a few days after administration and responding to treatment, has been recorded [7]. However, a lower risk of occurrence and severity of myocarditis/pericarditis was estimated following COVID-19 vaccination than SARS-CoV-2 infection [7].
Noteworthy, despite the young age of the investigated subjects, reported ADRs were found to be scarce, contrary to what was expected. In fact, due to immunosenescence, the immunogenicity of vaccines is known to be reduced in elderly subjects. On the contrary, young subjects should have higher immune capacity and responsiveness; this finding is also corroborated by the higher sera levels of interferon-gamma detected in youths compared to the elderly following COVID-19 vaccination [39,40].
Unfortunately, no data were retrieved on patients’ comorbidities, related treatments, and history of COVID-19, so it was impossible to understand further the potential interrelationships between general health status, vaccination, and oral lesions occurrence, to point out those factors predisposing or determining such adverse reactions.
Given that only two COVID-19 vaccines have been EMA authorized [8] and one WHO Emergency Use Listing approved [7] for use in all pediatric age groups, both mRNA-based and delivered through lipid nanoparticles, a higher prevalence of oral lesions was anticipated, since oral ADRs in the adult population were more frequently observed following mRNA-based vaccines [2,25,41,42,43,44,45], compared to those with a non-replicating viral vector [46,47,48]. In one case, the oral lesions occurred after the first dose, while in the other, they occurred after administration of the second dose, both at least seven days later and were, therefore, classified as late (<24 h) lesions, as per Hatami et al. [49].
The primary oral lesions described were erosive-ulcerative type (40%), with herpetiform (50%) and unspecified (50%) patterns, followed by macule and petechiae (20%). The failure to detect red and white plaques, as well as vesicles and bullae, may be related to the fact that these lesions are asymptomatic and, thus, could be underacknowledged by the family members of pediatric subjects. Moreover, it may be supposed that erosions and ulcers may be the most prevalent. Along with the primary oral lesions, pseudomembranes and crusts, consistent with the evolution of the above erosive-ulcerative lesions, were also described in the remaining 40% of cases.
The definitive diagnoses in the two cases reported were Behçet’s disease [24] and Erythema Multiforme [25]. Therefore, it may be speculated that clinicians’ attention may have been primarily focused on systemic involvement rather than oral phenomenology, which was not characterized adequately in similar cases described in the literature. However, this finding differs from the adult population with oral ADRs, primarily belonging to lichenoid reactions and Oral Lichen Planus [2,48,50,51], followed by Stevens-Johnson syndrome and Erythema Multiforme [25,42,46]. It may be speculated that lichenoid reactions and Oral Lichen Planus show a predilection for older subjects, and, thus, have not been found, to date, among oral ADRs to COVID-19 vaccines in the study population. Erythema Multiforme, instead, was also commonly diagnosed in pediatric SARS-CoV-2 positive subjects, and is known to be diagnosed with previous Herpes Simplex virus type-1 and Mycoplasma Pneumoniae infections, occurring, in turn, with a higher frequency in adolescents and young adults [52].
Considering oral mucosal lesions potentially related to viral infection and vaccine administration together, erosive-ulcerative lesions (10%) and maculae and petechiae (13%) were the most frequent oral primary lesions, and no case was diagnosed with white or red plaques, nor with vesicles and bullae. Other lesions, accounting for the majority of the total diagnosis (77%), were very heterogeneous and also included normal variations, such as the geographic tongue [31]. In any case, no increase in the detection of oral lesions has been highlighted, to date, as concomitant to the SARS-CoV-2 pandemic, in pediatric subjects. Conversely, a higher identification rate of skin lesions, mainly comprising pseudo-chilblains at the acral regions, which are thought to be among the most peculiar cutaneous manifestations in pediatric SARS-CoV-2 infection, Erythema multiforme, and various types of rashes and urticaria, have been registered [53].
No cyto/histological investigations were performed in any of the studies included in the present systematic review. However, insights into the microscopic characteristics of oral lesions in pediatric subjects may help to identify the pathogenic mechanisms involved in the onset and progression of such lesions. In addition, considering that histopathological findings have been described for adult subjects [54], a comparison between them may indirectly highlight any prevalent pathogenic mechanisms [55], potentially resulting from the different ages and related immune capacity [55].
The study’s main limitations may rely on the fact that besides the very inclusive eligibility criteria and the timeliness of the topic, very few studies were retrieved from the literature. In addition, reported findings were very heterogeneous and incomplete, likely because oral outcomes were often not the focus of the studies included in this systematic review; therefore, a meta-analysis could not be conducted. However, to the best of our knowledge, the present systematic review may be considered the first that qualitatively analyzed data from pediatric subjects on primary oral lesions potentially associated with SARS-CoV-2 infection, estimated the degree of association and grading of primary oral lesions based on COVID-19 forms, and followed COVID-19 vaccines in relation to cases and vaccine type and administered doses. Thus, the presented results, although considered preliminary data for future research, may deepen clinicians’ overall knowledge of oral lesions associated with COVID-19 in pediatric subjects, improving appropriate oral and dental care provision and enhancing multidisciplinary collaboration [13,32,36,51,56].
5. Conclusions
Recently characterized COVID-19-associated syndromes in pediatric subjects, characterized by a plethora of signs and symptoms, have raised the need to examine the impact and, prospectively, the potential causal role of SARS-CoV-2 infection and related vaccines on oral lesions in the pediatric population.
Data from nine studies describing oral lesions following viral infection and two records reporting oral lesions following vaccine administration were extracted and qualitatively synthesized, resulting in scarce, jeopardized, and incomplete findings.
Since most of the rare lesions recorded were a part of broad-spectrum systemic disorders and syndromes, and were, thus, undetailed or nonspecific, further studies should assess the prevalence and macro-microscopic features of oral lesions following SARS-CoV-2 infection, estimating the degree of association and grading primary oral lesions based on COVID-19 forms in pediatric subjects, also considering novel viral variants.
Future investigations should also evaluate the epidemiology, clinical appearance, and histopathology of oral lesions diagnosed among pediatric subjects who received at least one dose of the WHO Emergency Use Listing approved and EMA authorized COVID-19 vaccines in relation to cases’ ages, genders, comorbidities, related treatments, and histories of COVID-19, and vaccine types and the number of doses administered, to point out those factors predisposing, or determining, such adverse reactions, especially considering newly introduced vaccines.
A deeper insight into oral lesions potentially detectable in pediatric SARS-CoV-2 positive subjects and following COVID-19 vaccination may enhance clinicians’ preparedness to improve inter-disciplinary pediatric oral and general healthcare, also introducing oral screening for early diagnosis and appropriate management.
Author Contributions
Conceptualization, F.D.S. and M.P.D.P.; Methodology, F.D.S., A.A. and F.D.; Validation, M.C. (Mario Caggiano) and M.C. (Maria Contaldo); Formal Analysis, S.M. and A.A.; Data Curation, F.D.S., M.P.D.P. and F.D.; Writing—Original Draft Preparation, F.D.S., M.P.D.P., M.C. (Maria Contaldo) and F.D.; Writing–Review & Editing, M.C. (Mario Caggiano) and S.M.; Supervision, S.M. and A.A. All authors have read and agreed to the published version of the manuscript.
Funding
This research received no external funding.
Institutional Review Board Statement
Not applicable.
Informed Consent Statement
Not applicable.
Data Availability Statement
Data are available on MEDLINE/PubMed, Scopus, and Cochrane library databases and on the PROSPERO register.
Conflicts of Interest
The authors declare no conflict of interest.
References
- Rahman, S.; Villagomez Montero, M.T.; Rowe, K.; Kirton, R.; Kunik, F., Jr. Epidemiology, pathogenesis, clinical presentations, diagnosis and treatment of COVID-19: A review of current evidence. Expert Rev. Clin. Pharmacol. 2021, 14, 601–621. [Google Scholar] [CrossRef]
- Caggiano, M.; Amato, M.; Di Spirito, F.; Galdi, M.; Sisalli, L. mRNA COVID-19: Vaccine and Oral Lichen Planus: A case report. Oral Dis. 2022. advance online publication. [Google Scholar] [CrossRef] [PubMed]
- Štefan, M.; Dlouhý, P.; Bezdíčková, L. Vaccinationagainst COVID-19. Klin MikrobiolInfekc Lek 2021, 27, 49–60. [Google Scholar]
- Nikolopoulou, G.B.; Maltezou, H.C. COVID-19 in Children: Where do we Stand? Arch. Med. Res. 2022, 53, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Nakra, N.A.; Blumberg, D.A.; Herrera-Guerra, A.; Lakshminrusimha, S. Multi-System Inflammatory Syndrome in Children (MIS-C) Following SARS-CoV-2 Infection: Review of Clinical Presentation, Hypothetical Pathogenesis, and Proposed Management. Children 2020, 7, 69. [Google Scholar] [CrossRef] [PubMed]
- COVID-19 Vaccine Tracker European Centre for Disease Prevention and Control (europa.eu). Available online: https://www.ecdc.europa.eu/en/publications-data/covid-19-vaccine-tracker (accessed on 2 September 2022).
- Children and COVID-19 Vaccination Trends (aap.org). Available online: https://www.aap.org/en/pages/2019-novel-coronavirus-covid-19-infections/children-and-covid-19-vaccination-trends/ (accessed on 12 August 2022).
- COVID-19 Vaccines: Key Facts. Available online: https://www.ema.europa.eu/en/human-regulatory/overview/public-health-threats/coronavirus-disease-covid-19/treatments-vaccines/vaccines-covid-19/covid-19-vaccines-key-facts#vaccination-in-children-section (accessed on 13 August 2022).
- Moher, D.; Shamseer, L.; Clarke, M.; Ghersi, D.; Liberati, A.; Petticrew, M.; Shekelle, P.; Stewart, L.A.; PRISMA-P Group. Preferred reporting items for systematic review and meta-analysis protocols (PRISMA-P) 2015 statement. Syst. Rev. 2015, 4, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Liberati, A.; Altman, D.G.; Tetzlaff, J.; Mulrow, C.; Gøtzsche, P.C.; Ioannidis, J.P.; Clarke, M.; Devereaux, P.J.; Kleijnen, J.; Moher, D. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate healthcare interventions: Explanation and elaboration. PLoS Med. 2009, 6, e1–e34. [Google Scholar] [CrossRef]
- Richardson, W.S.; Wilson, M.C.; Nishikawa, J.; Hayward, R.S. The well-built clinical question: A key to evidence-based decisions. ACP J. Club 1995, 123, 12–13. [Google Scholar] [CrossRef]
- Data Collection form for Intervention Reviews for RCTs and non-RCTs-Template. Forms, The Cochrane Collaboration. Data Extraction. s.l.: Cochrane Developmental, Psychosocial and Learning Problems, 3 April 2014. Available online: https://view.officeapps.live.com/op/view.aspx?src=https%3A%2F%2Fdplp.cochrane.org%2Fsites%2Fdplp.cochrane.org%2Ffiles%2Fpublic%2Fuploads%2FCDPLPG%2520data%2520collection%2520form%2520for%2520intervention%2520reviews%2520for%2520RCTs%2520and%2520non-RCTs.doc&wdOrigin=BROWSELINK (accessed on 20 July 2022).
- Di Spirito, F.; Iandolo, A.; Amato, A.; Caggiano, M.; Raimondo, A.; Lembo, S.; Martina, S. Prevalence, Features and Degree of Association of Oral Lesions in COVID-19: A Systematic Review of Systematic Reviews. Int. J. Environ. Res. Public Health 2022, 19, 7486. [Google Scholar] [CrossRef]
- Sterne, J.A.; Hernán, M.A.; Reeves, B.C.; Savović, J.; Berkman, N.D.; Viswanathan, M.; Henry, D.; Altman, D.G.; Ansari, M.T.; Boutron, I.; et al. ROBINS-I: A tool for assessing risk of bias in non-randomised studies of interventions. Br. Med. J. 2016, 355, i4919. [Google Scholar] [CrossRef]
- Akca, U.K.; Kesici, S.; Ozsurekci, Y.; Aykan, H.H.; Batu, E.D.; Atalay, E.; Demir, S.; Sag, E.; Vuralli, D.; Bayrakci, B.; et al. Kawasaki like disease in children with COVID 19. Rheumatol. Int. 2020, 40, 2105–2115. [Google Scholar] [CrossRef] [PubMed]
- Cant, A.; Bhujel, N.; Harrison, M. Oral ulceration as presenting feature of paediatric inflammatory multisystem syndrome associated with COVID-19. J. Oral Maxillofac. Surg. 2020, 58, 1052–1063. [Google Scholar] [CrossRef] [PubMed]
- Jones, V.G.; Mills, M.; Suarez, D.; Hogan, C.A.; Yeh, D.; Segal, J.B.; Nguyen, E.L.; Barsh, G.R.; Maskatia, S.; Mathew, R. COVID-19 and Kawasaki Disease: Novel Virus and Novel Case. Hosp. Pediatr. 2020, 10, 537–540. [Google Scholar] [CrossRef]
- Labé, P.; Ly, A.; Sin, C.; Nasser, M.; Chapelon-Fromont, E.; Ben Saïd, P.; Mahé, E. Erythema multiforme and Kawasaki disease associated with COVID-19 infection in children. J. Eur. Acad. Dermatol. Venereol. 2020, 34, 539–541. [Google Scholar] [CrossRef]
- Al Ameer, H.H.; Alkadhem, S.M.; Busaleh, F.; AlKhwaitm, S.; Llaguno, M.B.B. Multisystem Inflammatory Syndrome in Children Temporally Related to COVID-19: A Case Report from Saudi Arabia. Cureus 2020, 12, e10589. [Google Scholar] [CrossRef]
- Bardellini, E.; Bondioni, M.P.; Amadori, F.; Veneri, F.; Lougaris, V.; Meini, A.; Plebani, A.; Majorana, A. Non-specific oral and cutaneous manifestations of Coronavirus Disease 2019 in children. Med. Oral Patol. Oral Y CirugíaBuca 2021, 26, 549–553. [Google Scholar] [CrossRef]
- Dima, M.; Enatescu, I.; Craina, M.; Petre, I.; Iacob, E.R.; Iacob, D. First neonates with severe acute respiratory syndrome coronavirus 2 infection in Romania: Three case reports. Medicine 2020, 99, e21284. [Google Scholar] [CrossRef]
- Falah, N.; Hashmi, S.; Ahmed, Z.; Jaan, A.; Akhtar, A.; Khalid, F.; Frooque, U.; Shera, M.T.; Ali, S.; Javed, A. Kawasaki Disease-Like Features in 10 Pediatric COVID-19 Cases: A Retrospective Study. Cureus 2020, 12, 11–35. [Google Scholar] [CrossRef]
- Marinescu, A.R.; Lazureanu, V.E.; Musta, V.F.; Nicolescu, N.D.; Mocanu, A.; Cut, T.G.; Muresan, C.O.; Tudoran, C.; Licker, M.; Laza, R. Severe Thrombocytopenic Purpura Associated with COVID-19 in a Pediatric Patient. Infect. Drug Resist. 2022, 15, 3405–3415. [Google Scholar] [CrossRef]
- Bogs, T.; Saleh, N.; Yavuz, S.T.; Fazeli, W.; Ganschow, R.; Schreiner, F. Aseptic Meningitis, Mucocutaneous Lesions and Arthritis after COVID-19 Vaccination in a 15-Year-Old Boy. Vaccines 2022, 10, 325. [Google Scholar] [CrossRef]
- Petruzzi, M.; Galleggiante, S.; Messina, S.; Della Vella, F. Oral erythema multiforme after Pfzer-BioNTech COVID-19 vaccination: A report of four cases. BMC Oral Health 2022, 22, 90. [Google Scholar] [CrossRef] [PubMed]
- Riad, A.; Põld, A.; Kateeb, E.; Attia, S. Oral Adverse Events Following COVID-19 Vaccination: Analysis of VAERS Reports. Front. Public Health 2022, 10, 952781. [Google Scholar] [CrossRef] [PubMed]
- Furlanetto, D.L.; Crighton, A.; Topping, G.V. Differences in methodologies of measuring the prevalence of oral mucosal lesions in children and adolescents. Int. J. Paediatr. Dent. 2006, 16, 31–39. [Google Scholar] [CrossRef] [PubMed]
- Iranmanesh, B.; Khalili, M.; Amiri, R.; Zartab, H.; Aflatoonian, M. Oral manifestations of COVID-19 disease: A review article. Dermatol. Ther. 2021, 34, e14578. [Google Scholar] [CrossRef]
- Peckham, H.; de Gruijter, N.M.; Raine, C.; Radziszewska, A.; Ciurtin, C.; Wedderburn, L.R.; Rosser, E.C.; Webb, K.; Deakin, C.T. Male sex identified by global COVID-19 meta-analysis as a risk factor for death and ITU admission. Nat. Commun. 2020, 11, 6317. [Google Scholar] [CrossRef]
- Williams, D.M. Classification and diagnostic criteria for oral lesions in HIV infection. EC-Clearinghouse on Oral Problems Related to HIV Infection and WHO Collaborating Centre on Oral Manifestations of the Immunodeficiency Virus. J. Oral Pathol. Med. 1993, 22, 289–291. [Google Scholar]
- Orilisi, G.; Mascitti, M.; Togni, L.; Monterubbianesi, R.; Tosco, V.; Vitiello, F.; Santarelli, A.; Putignano, A.; Orsini, G. Oral Manifestations of COVID-19 in Hospitalized Patients: A Systematic Review. Int. J. Environ. Res. Public Health 2021, 18, 12511. [Google Scholar] [CrossRef]
- Di Spirito, F.; Pelella, S.; Argentino, S.; Sisalli, L.; Sbordone, L. Oral manifestations and the role of the oral healthcare workers in COVID-19. Oral Dis. 2022, 28, 1003–1004. [Google Scholar] [CrossRef]
- Martín Carreras-Presas, C.; Amaro Sánchez, J.; López-Sánchez, A.F.; Jané-Salas, E.; Somacarrera Pérez, M.L. Oral vesiculobullous lesions associated with SARS-CoV-2 infection. Oral Dis. 2021, 27 (Suppl. 3), 710–712. [Google Scholar] [CrossRef]
- Patton, L.L.; Phelan, J.A.; Ramos-Gomez, F.J.; Nittayananta, W.; Shiboski, C.H.; Mbuguye, T.L. Prevalence and classification of HIV-associated oral lesions. Oral Dis. 2002, 8, 98–109. [Google Scholar] [CrossRef]
- World Health Organization (WHO). Living Guidance for Clinical Management of COVID-19: Living Guidance. Available online: https://www.who.int/publications/i/item/WHO-2019-nCoV-clinical-2021-2 (accessed on 23 November 2021).
- Di Spirito, F.; Amato, A.; Di Palo, M.P.; Contaldo, M.; D’Ambrosio, F.; Lo Giudice, R.; Amato, M. Oral Lesions Following Anti-SARS-CoV-2 Vaccination: A Systematic Review. Int. J. Environ. Res. Public Health 2022, 19, 10228. [Google Scholar] [CrossRef] [PubMed]
- Cirillo, N. Reported orofacial adverse effects of COVID-19 vaccines: The knowns and the unknowns. J. Oral Pathol. Med. 2021, 50, 424–427. [Google Scholar] [CrossRef]
- Riad, A. Oral side effects of COVID-19 vaccine. Br. Dent. J. 2021, 230, 59. [Google Scholar] [CrossRef]
- Smyth, R.M.; Gargon, E.; Kirkham, J.; Cresswell, L.; Golder, S.; Smyth, R.; Williamson, P. Adverse drug reactions in children--a systematic review. PLoS ONE 2012, 7, e24061. [Google Scholar] [CrossRef] [PubMed]
- Moulton, V.R. Sex Hormones in Acquired Immunity and Autoimmune Disease. Front. Immunol. 2018, 9, 2279. [Google Scholar] [CrossRef] [PubMed]
- Calabria, E.; Canfora, F.; Mascolo, M.; Varricchio, S.; Mignogna, M.D.; Adamo, D. Autoimmune mucocutaneous blistering diseases after SARS-CoV-2 vaccination: A Case report of Pemphigus Vulgaris and a literature review. Pathol. Res. Pract. 2022, 232, 153834. [Google Scholar] [CrossRef] [PubMed]
- Borg, L.; Mericieca, L.; Mintoff, D.; Micallef, D.; Pisani, D.; Betts, A.; Scerri, L. Pfizer-BioNTech SARS-CoV-2 mRNA vaccine-associated erythema multiforme. JEADV 2022, 36, 22–24. [Google Scholar] [CrossRef] [PubMed]
- Hertel, M.; Schmidt-Westhausen, A.M.; Wendy, S.; Heiland, M.; Nahles, S.; Preissner, R.; Preissner, S. Onset of Oral Lichenoid Lesions and Oral Lichen Planus Following COVID-19 Vaccination: A Retrospective Analysis of about 300,000 Vaccinated Patients. Vaccines 2022, 10, 480. [Google Scholar] [CrossRef]
- Maeda, K.; Yamashita, D.; Takenobu, T. Ulcers on the bilateral palate mucosa following mRNA-based vaccination for coronavirus disease 2019 (COVID-19): A case report. J. Stomatol. Oral Maxillofac. Surg. 2022, 123, 283–286. [Google Scholar] [CrossRef]
- Saibene, A.M.; Alliata, A.; Cozzi, A.T.; Ottavi, A.; Spagnolini, S.; Pipolo, C.; Maccari, A.; Felisati, G. Erythema Multiforme Major following SARS-CoV-2 vaccine. Clin. Case Rep. 2021, 9, e04947 . [Google Scholar] [CrossRef]
- Dash, S.; Sirka, C.S.; Mishra, S.; Viswan, P. COVID-19 vaccine-induced Stevens–Johnson syndrome. Clin. Exp. Dermatol 2021, 46, 1567–1625. [Google Scholar] [CrossRef] [PubMed]
- Azzi, L.; Toia, M.; Stevanello, N.; Maggi, F.; Forlani, G. An episode of oral mucositis after the first administration of the ChAdOx1 COVID-19 vaccine. Oral Dis. 2021. advance online publication. [Google Scholar] [CrossRef]
- Troeltzsch, M.; Gogl, M.; Berndt, R.; Troeltzsch, M. Oral lichen planus following the administration of vector-based COVID-19 vaccine (Ad26.COV2.S). Oral Dis. 2021. Online ahead of print. [Google Scholar] [CrossRef] [PubMed]
- Hatami, P.; Aryanian, Z.; Niknam Asl, H.; Goodarzi, A. Mucocutaneous adverse effects following COVID-19 vaccination: A case series with a comprehensive review of the literature. Iran. J. Dermatol. 2021, 24, 331–338. [Google Scholar]
- Sharda, P.; Mohta, A.; Ghiya, B.C.; Mehta, R.D. Development of oral lichen planus after COVID-19 vaccination—A rare case report. J. Eur. Acad. Dermatol. Venereol. 2022, 36, 80–157. [Google Scholar] [CrossRef] [PubMed]
- Babazadeh, A.; Miladi, R.; Barary, M.; Shirvani, M.; Ebrahimpour, S.; Aryanian, Z.; Mohseni Afshar, Z. COVID-19 vaccine-related new-onset lichen planus. Clin. Case Rep. 2022, 10, e05323. [Google Scholar] [CrossRef]
- Colonna, C.; Restano, L.; Monzani, N.; Zussino, M.; Ponziani, A.; Cambiaghi, S.; Cavalli, R. Rare and common manifestations of COVID-19 in children. EADV Clin. Pr. 2022, 1, 21–30. [Google Scholar] [CrossRef]
- Dondi, A.; Sperti, G.; Gori, D.; Guaraldi, F.; Montalti, M.; Parini, L.; Piraccini, B.M.; Lanari, M.; Neri, I. Epidemiology and clinical evolution of non-multisystem inflammatory syndrome (MIS-C) dermatological lesions in pediatric patients affected by SARS-CoV-2 infection: A systematic review of the literature. Eur. J. Pediatr. 2022, 10, 1–17. [Google Scholar] [CrossRef]
- Favia, G.; Tempesta, A.; Barile, G.; Brienza, N.; Capodiferro, S.; Vestito, M.C.; Crudele, L.; Procacci, V.; Ingravello, G.; Maiorano, E.; et al. Covid-19 Symptomatic Patients with Oral Lesions: Clinical and Histopathological Study on 123 Cases of the University Hospital Policlinic of Bari with a Purpose of a New Classification. J. Clin. Med. 2021, 10, 757. [Google Scholar] [CrossRef]
- Di Spirito, F.; Contaldo, M.; Amato, A.; Di Palo, M.P.; Pantaleo, G.; Amato, M. COVID-19 Vaccine and Oral Lesions: Putative Pathogenic Mechanisms. Oral Dis. 2022. online ahead of print. [Google Scholar] [CrossRef]
- Di Spirito, F.; Iacono, V.J.; Iandolo, A.; Amato, A.; Sbordone, L. Evidence-based recommendations on periodontal patients during and after the COVID-19 Era: Challenging infectious evidence-based recommendations on periodontal practice and the management of periodontal patients during and after the COVID-19 era: Challenging infectious diseases spread by air-borne transmission. Open Dent. 2021, 15, 325–336. [Google Scholar] [CrossRef]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).