1. Introduction
In the twenty-first century, everyone’s life is determined by aesthetics, which is also one of the goals of dental treatments, regardless of the patient’s age. The aesthetics of the smile influence the appearance, social interactions and psychological well-being of the person [
1]. Contrasts in shapes, colors, lines and textures allow us to distinguish one tooth from another, teeth from gums and the smile from the face [
2].
An aesthetically pleasing smile is associated with intelligence and elevated social status [
3]; therefore, priorities in dental treatments have changed over the years: nowadays, patients themselves stress the aesthetic aspect when setting expectations about dental treatments. Dental professionals should offer high-quality rehabilitation procedures that meet every patient’s biological, physical and aesthetical expectations [
4].
The maxillary anterior teeth are the most influential in terms of smile aesthetics [
5], and one of the variables that influences dental aesthetics seems to be the symmetry of the anterior teeth, considered in terms of dental elements and gingival arches. Regarding these considerations, it is imperative that an ideal treatment plan should include the improvement of this aspect as much as possible to provide the patient with the most aesthetically pleasing restoration [
6,
7,
8,
9,
10].
Creating the perfect smile to match the individual aesthetic of every person represents a challenge for dental professionals and requires a multidisciplinary approach and a meticulous treatment plan [
11]. For years, traditional dental waxing has been the gold standard to represent a preview of dental rehabilitations, even though the quality of the outcome is strongly impacted by the manual skills and knowledge of dental anatomy of the technician [
12]. New digital technologies, diffused in recent years into routine clinical dentistry, are drastically changing the workflow.
The introduction of photography in 1839 led medical professionals to document clinical procedures more and more and paved the way for the development of new digital treatment approaches. In 2002, M. Ackerman and J. Ackerman introduced what was going to become the aesthetical analysis of a patient’s arches performed on patients’ photographs and would, six years later, led to the first Digital Smile Design (DSD) protocol fully based on intraoral and extraoral images [
13,
14].
Given this, it is also important that young clinicians, undergraduates and non-specialized dentists have the opportunities and possibilities to provide their patients with more than one aesthetic analysis and method to create digital and clinical mock-ups [
15,
16,
17].
The Digital Smile Design protocol can be performed on various software, such as Microsoft PowerPoint (version 17, Microsoft Corporation, Redmont, WA, USA), Keynote (Apple Inc., Cupertino, CA, USA) and Photoshop (version 21.x, Adobe Inc., San Jose, CA, USA), or specific apps, such as DSD App (Digital Smile Design, Madrid, Spain), Smile Designer Pro (Tasty Tech Ltd., Toronto, ON, Canada) and Planmeca Romexis Smile Design (Planmeca OY, Helsinki, Finland). Every software package allows the drawing of reference lines and shapes on extra- and intraoral digital photographs. Facial, dento-gingival and dental analyses are carried out to determine the new measurements of the dental elements that are then modified through standard templates or by drawing the elements ex novo [
17,
18,
19]. All of the precise measurements of the modified dental elements obtained from the protocol are then used by a dental technician to produce an accurate wax-up.
The protocol depends on photographic documentation of the case that, if not correctly achieved, could negatively impact the diagnosis and planning of the restorations. Therefore, a learning curve is to be expected for the clinician to be able to use the software [
1].
A digital alternative to 2D digital smile planning is 3D digital smile planning performed on a three-dimensional scan of the patient’s dental arches. This technique allows the clinician to design a digital wax-up of the elements using digital libraries of different three-dimensional shapes and sizes of dental elements [
20]. The digital planning of the restorations can then be 3D printed to obtain a physical model of the restorations.
From digital and traditional wax-ups, a silicone guide can be produced to be used as a guide to print a mock-up in the patient’s mouth, which is an essential part of the treatment plan in order to mimic and validate the planned restorations [
21].
Digital imaging and designing are useful for communicating directly with the patient and showing visual feedback of the possible treatment outcomes of rehabilitations in the aesthetic area, and also improve communication between clinicians who can access the images remotely [
22,
23]. These digital techniques allow the patient to be involved in the design process of the dental elements, which results in a more humanistic and confident smile [
22].
Moceado et al., in their article, reported that the duration of procedures appears to be an important issue concerning the opinion of patients about their care. The perception of a faster procedure was found to be the aspect that pleased most of the patients involved in the study, which reinforces the necessity to pursue further analysis of different types of workflows in terms of working times [
12].
With all this in mind, focused on the purpose to make digital aesthetic planning available in an open-source way and, because various types of workflows can be used to obtain a final mock-up of anterior aesthetic restorations nowadays, the objectives of this experiment were:
Evaluation of the aesthetical opinion of the patient and of a group of external people regarding the three mock-ups obtained with three different types of workflows;
Comparison of the working times of the three workflows;
Comparison of the symmetry between gingival curves and dental elements in every mock-up.
2. Materials and Methods
The patient on whom all the procedures were performed was a 26-year-old woman in treatment at the University Hospital of Verona, Italy. The patient signed an informed consent for all procedures and gave her consent to use her photographs both for clinical aims and for publication.
Ethical Committee approval was not required as the procedures evaluated were part of the clinical routine of the University Hospital of Verona, Italy.
The clinical part of the experiment was carried out in three appointments and, during every procedure, the clinical and laboratory working times were measured in minutes.
All clinical procedures herein reported were performed by the same trained operator and the laboratory procedures were executed by the same technician.
2.1. First Appointment
The patient was positioned at a 1 m distance from a uniform, neutral background and intraoral and extraoral photographs were taken with a Nikon D7000 (Nikon Corp., Shinjuku, Tokyo, Japan) camera and a Nikon Lens AF Micro Nikkor 105 mm 1:2:8D (Nikon Corp., Shinjuku, Tokyo, Japan), as follows:
Extraoral full face pictures: Camera in vertical position, flash off, focus on the cheekbones, ISO auto and aperture f/8;
Intraoral pictures with cheek retractors pulled outwards: Camera in horizontal position, maximum intercuspation, external flash on, focus on canines, ISO auto, aperture f/32 and augmentation ratio 1:3;
Occlusal pictures: external flash on, ISO auto, aperture f/29 and augmentation ratio 1:3;
Overjet pictures with cheek retractors pulled back: maximum intercuspation, external flash on, ISO auto, aperture f/32 and augmentation ratio 1:2.
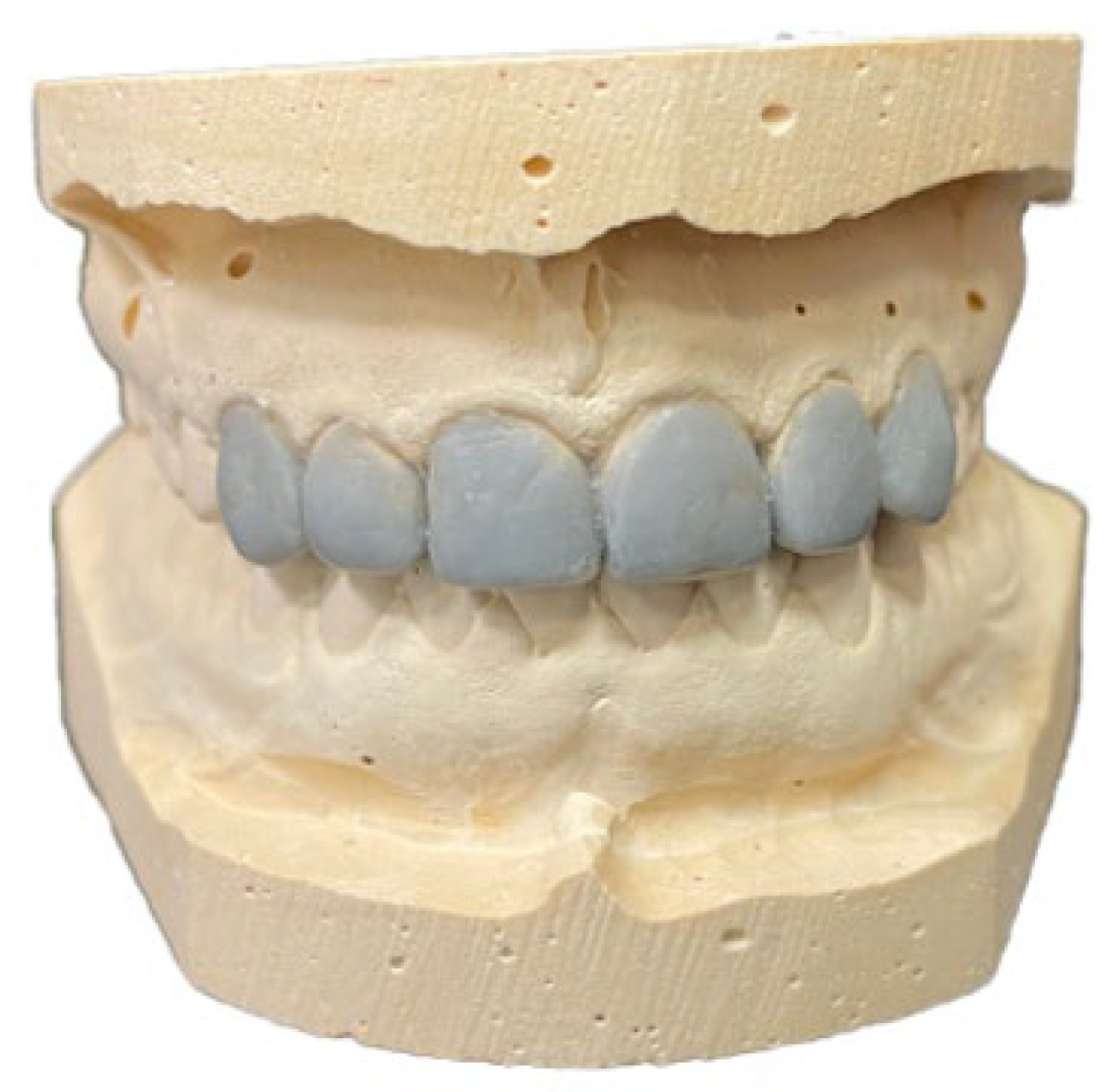
Mandibular and maxillary dental impressions were taken with class A type 1Kromopan Lascode Alginate (Lascode S.p.a, Sesto Fiorentino, Firenze, Italia). The impressions were used to obtain three casts of the patient’s dental arches made with GC Fujirock (GC Europe N. V., Interleuvenlaan, Belgium), a type-4 enhanced plaster (
Figure 1).
Width and length measurements of the upper anterior teeth (canines, lateral incisors and central incisors) were taken with a digital caliper and measured in mm (red lines in
Figure 2). Length was measured from the most coronal point to the most apical point of the clinical crown and width was measured at the equator of each tooth. Measurements of the width and amplitude of the gingival arches of the anterior teeth were also taken using the same caliper and measured in mm. (Yellow lines in
Figure 2)
2.2. Dental Wax-Up Preparation following the Traditional Workflow
The dental casts were used by a dental technician to obtain a dental wax-up without any precise measurements and proportions of the elements given by the clinician. Thowax Yeti Ref. 714-0000 gray wax (Yeti Dental GmbH, Engen, Germany) was used to produce the modified anterior teeth according to the opinion and competence of the dental technician (
Figure 3).
The width and length of the waxed elements and width and amplitude of the corresponding gingival arches were measured with a digital caliper in mm.
2.3. Dental Wax-Up Preparation with a 2D Digital Workflow
To obtain a digital wax-up, an aesthetic and dento-facial analysis was carried out using the Keynote software (Apple Inc., Cupertino, CA, USA). For the dento-facial analysis, the photographs of the smile at rest and with cheek retractors taken during the first appointment were uploaded to Keynote and landmarks were identified.
The frontal full-face smiling photo was used to perform the aesthetic facial analysis, using the following landmarks (
Figure 4):
Green line outlining the facial shape;
Horizontal upper yellow line traced between the pupils;
Horizontal lower yellow line traced between the labial cants;
Central vertical line traced between the middle point of the glabella and the philtrum, indicating the facial midline.
The full-face smiling photograph was also cut to obtain a picture of the smile zone, which was used for the dento-facial analysis (
Figure 5). To describe the lips, the parameters used were fullness, width and symmetry (yellow line).
The frontal photograph in maximum intercuspation with cheek retractors was cut to obtain a photo containing the teeth and used for the dental evaluation (
Figure 6).
The same photograph of the smile zone was uploaded to Keynote to perform the digital smile planning. The upper line of the lower lip and the median line between the upper central incisors were traced. A grid calibrated with the Golden Proportion for dental elements was applied to the picture to guide the mesio-distal rehabilitation of the anterior teeth (
Figure 7).
Two blue lines were traced, one between the two central incisors at their incisal edge and the other along the apex of the papillae between elements 1.2–1.1 and 2.2–2.3 (
Figure 8). The third reference line was the green one, corresponding to the median line.
All the lines traced were grouped and this scheme was applied to the intraoral photograph with cheek retractors, referring to the lines traced before (
Figure 9).
Successively, reference lines were traced and the smile line was modified to obtain the ideal curve. For the central incisors, an 80% width/length ratio was used by positioning a rectangle on each of the upper central incisors.
The smile line was copied and pasted above the maxillary teeth, taking the upper line of the rectangles as a landmark. The line was then modified to obtain the best-fitting curve for the patient (
Figure 10). This new grid was then used as a size guide for the 2D smile design.
A template of six round-shaped teeth produced in Adobe Photoshop
® CS6 (Adobe, San Jose, CA, USA) [
24] was placed inside the grid, with the central incisors and canines touching both upper and lower lines and the lateral incisors not touching both lines (
Figure 11).
A ruler calibrated with the real measurements of the patient’s teeth was used to measure the digitally designed teeth by using the grid (
Figure 12), and the precise values were provided to the dental technician to produce a precise dental wax-up (
Figure 13).
The width and length of the waxed-up upper anterior elements from 1.3 to 2.3 were measured with a digital caliper (mm), and measurements of width and amplitude (mm) of the five corresponding gingival arches were also taken. The values collected were registered.
2.4. Silicone Guides Manufacturing
Two silicone guides were obtained from the two dental wax-ups to produce the dental mock-ups. The silicone used to produce the guides was Elite HD+ Putty Soft by Zhermack (Zhermack S.p.a., Rovigo, Italy).
After the setting time, each silicone guide was shaped with a scalpel by tracing releasing incisions to facilitate resin outflow, and each one was shaped to ease its insertion into the patient’s mouth (
Figure 14).
2.5. Second Appointment
During the second appointment, two mock-ups were produced using the two silicone guides and 3M ESPE Protemp 4 resin, A2 shade (3M Italia S.r.l., Pioltello, Italy).
Photographs of the patient were taken using the same camera and settings as those in the first appointments with the mock-up obtained through the traditional workflow and the mock-up developed through the 2D digital workflow.
2.6. Dental Wax-Up Preparation with a 3D Digital Workflow
The maxillary plaster model was scanned in a dental laboratory with a Sinergia Scan Advanced Plus structured light extraoral scanner (Nobil Metal S.p.a, AT, Italy).
The digital model was opened in Blender software
® (version 2.90, Blender Foundation
®, Amsterdam, The Nederlands), a free software package that was used to design a 3D digital wax-up. Free three-dimensional templates of the maxillary anterior elements from the ”Christian Brenes tooth library” were downloaded for free via subscription to the newsletter of
www.digitaldentistryeducation.com (Blue Sky Bio, LLC, Libertyville, IL, USA) (
Figure 15).
The digital elements were resized and repositioned in order to fit them on the patient’s smile and create the most symmetrical rehabilitation possible.
The digital file was converted in the Preform software (version 2.20.0, Formlabs, Somerville, MA, USA) to obtain a digital print of the modified dental model. The 3D model was printed with a Formlabs 3B printer (Formlabs, Somerville, MA, USA) with Model V3 resin (Formlabs, Somerville, MA, USA) on a printing plate, without a tray, at 0° and with a vertical resolution of 0.1 mm (
Figure 16).
The width and length (mm) of the maxillary anterior elements from 1.3 to 2.3 and width and amplitude (mm) of the five corresponding gingival arches were measured with a digital caliper and registered.
A silicone guide was produced from the three-dimensional printed model following the same procedure described previously.
2.7. Third Appointment
During the third appointment, the mock-up produced through the 3D digital workflow was applied with the silicon guide and 3M ESPE Protemp 4 resin, A2 shade (3M Italia S.r.l., Pioltello, Italy).
Photos of the patient were taken with the same camera and settings as those in the first and second appointments.
The differences between the measurements of the gingival arches and those of the width/length (mm) of the teeth were measured for every type of workflow and descriptive statistical analysis was performed.
2.8. Aesthetical Impact Survey
A survey was created on Google Forms (Alphabet Co., Mountain View, CA, USA), the answers to which were provided online and linked directly to the author’s profile. The survey was anonymous and no personal information was required to ensure the confidentiality of the responders. The title was “Aesthetical Impact Survey” and the compilation time was two minutes. At the beginning of the survey, it was indicated that every person could only respond once. There were no exclusive or inclusive criteria, except for Italian language proficiency. The survey was diffused by sharing the link via WhatsApp™, e-mail and Telegram Messenger to the author’s contacts and collaborators. Every person was invited to share the survey in return to amplify the population sample.
Demographic information was sought in the first section, which included three questions:
Are you a dentistry student or a dental professional? Possible answers “Yes” or “No”;
Age: answer options “15–25 years old”, “25–35 years old”, “35–50 years old”, “over 50 years old”;
Gender: answer options “Male”, “Female”.
Four photos of the patient’s smile were included in the survey:
Initial photograph of the patient’s smile (
Figure 17);
Photograph with the mock-up obtained through the traditional workflow (
Figure 18);
Photograph with the mockup obtained through the 2D digital workflow (
Figure 19);
Photograph with the mock-up obtained through the 3D digital workflow (
Figure 20).
All participants were asked to evaluate every photograph according to their own aesthetic criteria on a discreet scale from 1 to 5, where 1 was the least aesthetically appealing and 5 was the most aesthetically appealing. The patient was also asked to express her opinion on the four photographs using the same scale.
The demographic information was evaluated by descriptive analysis, while the scores assigned to the four pictures were compared using the following statistical analyses:
Mann–Whitney test to compare ratings between the population of dental experts and non-experts;
Mann–Whitney test to compare ratings between the male and female populations;
Kruskal–Wallis test to compare ratings between age groups;
Average scores of every group of people were examined to further analyze what the statistical differences were caused by.
The statistical analysis was performed with the Statistical Package for Social Sciences Version 25.0 (SPSS Inc., Chicago, IL, USA). All tests were considered statistically significant at p ≤ 0.05.
3. Results
The Excel database automatically created by the Google Form was imported into SPSS and used as a calculus sheet, on which the statistical analysis was performed.
In total, 490 people were reached with the survey and 74.3% of those interviewed were experts in the dental field, while the remaining 25.7% were not.
The gender distribution showed that 67.3% of the interviewed people were females and 32.7% were males. A proportion of 41% of the population considered was between 15 and 25 years old, 35.7% was between 25 and 35 years old and 12.2% was over 50 years old.
Upon the request to assign a vote from 1 to 5 to each of the four photographs, people responded as presented in
Figure 21.
The average score for picture 1 was 2.49, that for picture 2 was 3.31, that for picture 3 was 4 and that for picture 4 was 2.9.
The patient herself voted separately on every picture, and the results were:
Photograph 1: 2;
Photograph 2: 3;
Photograph 3: 4;
Photograph 4: 2.
The ratings for every photograph given by the sample are summarized in
Table 1.
3.1. Comparative Analysis of the Samples
The statistical differences between the ratings assigned by dental professionals and non-professionals, males and females and different age groups are presented in
Table 2.
3.2. Symmetrical Analysis of the Three Reconstructions
The measurements of the initial dental cast are reported in
Table 3 and
Table 4.
The measurements taken on the model with the wax-up obtained through traditional workflow are provided in
Table 5 and
Table 6.
The measurements taken on the model with the wax-up obtained through the 2D digital workflow are reported in
Table 7 and
Table 8.
The measurements taken on the model with the wax-up obtained through the 3D digital workflow are reported in
Table 9 and
Table 10.
From the analysis of measurements, it is evident that there was an improvement in the aesthetic parameters in the 2D digital workflow, achieved through the harmonization of measurements of the teeth and soft tissues.
3.3. Working Time Analysis
Through the study, the working times were measured for the three types of workflows and collected in
Table 11.
4. Discussion
The results of this study highlight how recent innovations, such as Digital Smile planning, are progressively changing the dental field for the better; Ref. [
25]. The photograph picturing the patient’s smile modified with the 2D digital workflow, in fact, achieved the highest ratings overall. Experts in the dental field gave an average rating of 3.74, while the average rating for non-experts was 4.06. The statistical analysis showed significant differences between the answers of the two groups; the dental experts voted the 2D digital workflow wax-up as the most aesthetically pleasing; however, they were found to be more critical than non-experts. The same difference was found in the ratings of the other photographs; dental experts rated the patient’s natural smile without a mock-up an average of 2.30, whereas non-experts rated it 2.56, which represents a statistically significant difference as well. Likewise, the ratings of the photograph of the smile reconstructed through the traditional workflow by these two groups of people had similar statistical differences. These differences could be due to the difference in size between the two population groups or to the differences in knowledge and competence within them.
Concerning the differences between ratings given by females and males, there were no statistically significant differences, except for the photograph picturing the smile with the mock-up obtained through the traditional workflow. The results showed a higher average rating in the female group (3.38), whereas the rating in the male group was 3.15.
The differences in the results were also evaluated in relation to the different age groups: for the mock-ups obtained through digital workflows, there was no statistically significant difference. The oldest age group, however, assigned the highest ratings to the patient’s natural smile and the smile modified through the traditional workflow, as opposed to the youngest age group. Individuals in the 15–25 age group assigned photographs 1 and 2 average ratings of 2.37 and 3.25, while individuals in the >50 age group rated the same photographs with higher scores of 3.09 and 3.58, respectively. This difference could be due to the fact that young people are more severe in terms of aesthetics and have stricter standards of beauty [
26,
27], and that older people seem to not be greatly influenced by aesthetic factors [
28]. However, the up-to-date literature provides controversial data when aesthetic perception is analyzed, and this could be linked to the different weight that aesthetics has around the world and among different ages; aesthetic parameters can indeed be influenced by cultural factors, individual preferences and trends of the moment too [
29,
30].
In conclusion, there was a consistent pattern in the aesthetic evaluation between all the population groups included in this survey. In order of appreciation, the pattern was: mockup obtained through Digital Smile planning, mock-up obtained through traditional workflow, mock-up obtained through 3D digital workflow and the patient’s natural smile.
A further possibility for planning and pre-viewing restorations is free-hand mock-ups [
31]; however, the aim of this study was to assess the differences between mock-ups obtained by different workflows. Free-hand mock-up is an interesting technique that is subject to the experience and aesthetic ideal of the operator; this aspect contrasts with the purpose of this study, aiming to identify the most suitable standardizable method; because of this, it was not included in this work.
From the assessment of the measurements taken with the digital caliper and collected in the tables, it is clear that the patient’s teeth and gingival arches were asymmetrical and remained unvaried in the mock-up obtained from the wax-up created by the technician freehand. In opposition to this, the mockups achieved through the digital workflows were symmetrical, except for the gingival arches between elements 1.2–1.3 and 2.2–2.3 in the 2D digital workflow and the dimensions of dental elements 1.1 and 1.2 in the 3D digital workflow. This alteration could be due to the fact that the software for 3D planning was open-source, which implied having no feasibility to substantially adjust the template of teeth to obtain perfect fitting and proportions. It could be interesting to improve this aspect by using professional software and a manageable template of teeth for 3D planning in order to have a more accurate result to measure.
To correct the asymmetry, a gingivectomy would be needed, as shown by the overlapping of white matter on the gingival margin in the digital mock-up. The surgical procedure was not considered by the dental technician, who produced the wax-up without changing the soft tissues’ features. The distinct symmetry in the digital reconstruction could be the reason for the high ratings obtained through the 2D digital reconstruction.
Considering the working times collected in
Table 11, the traditional workflow seemed to be the fastest; however, it must be noted that, in the 3D digital workflow a digital intraoral scanner was not used. If the intraoral scanner had been used, the total working time of 320 min could have been reduced by 50 min, which was the time used to take an alginate impression and produce the plaster model.
In this case, the fastest workflow was the 3D digital workflow, despite it having the worst ratings in the survey. These results could be limited by the use of open-source software that had several limitations compared with paid programs, for example, not allowing to place the two dental arches in occlusion or the lack of digital dental elements to use in the digital wax-up.
The operative times used to produce the mock-up through the 2D digital workflow were the longest (400 min); however, the aesthetic dental and facial analyses were accurately performed with a consequent more customized previsualization and aesthetic result fitting better with the facial features of the patient. Surely, it would also be possible that a trained operator could execute the same procedure in less time.
The authors are well aware that drawing conclusions based on a single case represents a scientific weakness. However, the aesthetic planning of smile restoration is strongly related to the abilities of clinicians and technicians who create wax-ups or digital plans. This aspect is highlighted in our study, where all aspects of the procedures are evaluated, even if they were performed on a single patient. We assumed that knowing the operative times and information about results in terms of symmetry could be an important issue for clinicians and readers, even if they were not drawn from multiple cases.
An important aspect the clinician should take into consideration is the cost differences between the three types of workflows. This aspect greatly affects the feasibility to make reliable mock-ups and full digital rehabilitation; because of this, the authors tested the feasibility of using open-source software, also for allowing young and non-specialized clinicians to use digital tools [
32].
In conclusion, it can be noted that aesthetic digital planning is a useful tool for clinicians and also for communicating with patients [
33]. It is, however, known that, sometimes, it could condition patients into having non-realistic expectations as to what the final result of the rehabilitation could actually be [
17]. The production of the mock-up is certainly an important step that can be included in the course of treatment, especially in rehabilitations in the aesthetic area; it is useful for the patient to have concrete feedback on the modifications that will be applied in the restoration and also for the clinician to have visual feedback of the future restorations in the context of the patient’s smile and face [
34]. It also allows the dentist to further evaluate the relationship between teeth and lips, phonetics and harmony during habitual movements of the perioral soft tissues, which cannot be analyzed realistically in a digital form.
More in-depth analyses should be carried out for the underlying differences in terms of the patient’s satisfaction with both the mock-ups obtained via digital workflows and with the final real aesthetic results. A crucial issue to investigate, in our opinion, is the congruence between the expected results provided by the mock-up and the real aesthetic results obtained after restoration; this aspect may be worth paying more attention to, because it is strictly related to the real usefulness of our planning procedures and the way in which clinicians can show patients the expected results.
The issue of satisfaction with dental aesthetic rehabilitation is of great importance, as well as the excessive expectations raised by unrealistic digital planning. The feasibility of having a good-looking preview could generate an illusory expectation [
17]; therefore, a good explanation of the limitations and proper counseling regarding the final outcome and its advantages and disadvantages by the clinician is essential to obtain authentic informed consent for all phases of work, in addition to the satisfaction of the patients.