Prescribed Versus Taken Polypharmacy and Drug–Drug Interactions in Older Cardiovascular Patients during the COVID-19 Pandemic: Observational Cross-Sectional Analytical Study
Abstract
1. Introduction
2. Materials and Methods
2.1. Ethics
2.2. Inclusion Criteria
2.3. Sample Characteristics
2.4. Medication Lists
2.5. Polypharmacy, DDIs, and DDI Index
2.6. Statistics
2.6.1. Sample Size Calculation
2.6.2. Statistical Processing of Data
3. Results
3.1. EHRs
3.2. Polypharmacy
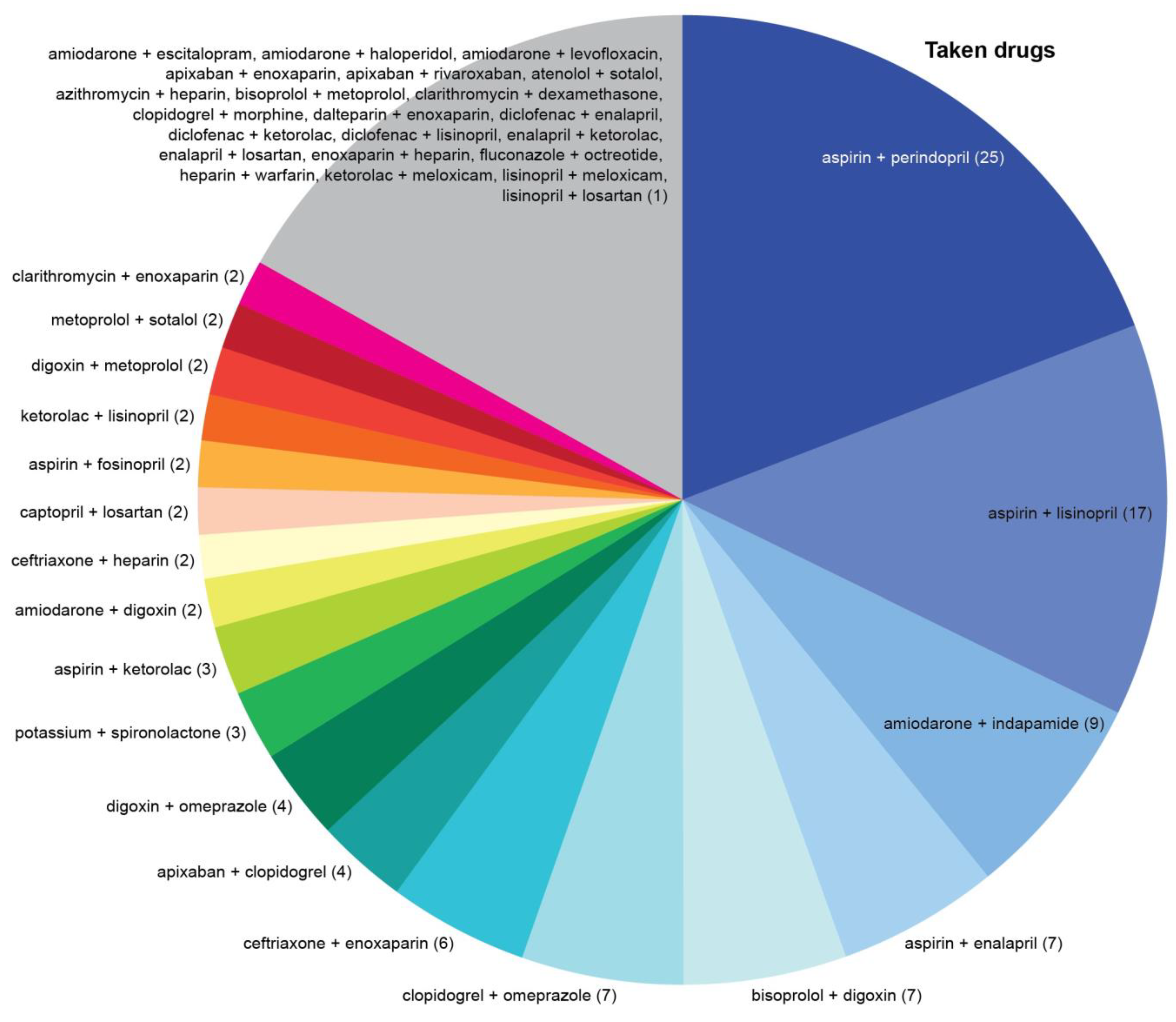
3.3. DDIs
3.4. DDI Index
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Chowdhury, S.R.; Chandra Das, D.; Sunna, T.C.; Beyene, J.; Hossain, A. Global and regional prevalence of multimorbidity in the adult population in community settings: A systematic review and meta-analysis. eClinicalMedicine 2023, 57, 101860. [Google Scholar] [CrossRef] [PubMed]
- Alhumaidi, R.M.; Bamagous, G.A.; Alsanosi, S.M.; Alqashqari, H.S.; Qadhi, R.S.; Alhindi, Y.Z.; Ayoub, N.; Falemban, A.H. Risk of Polypharmacy and Its Outcome in Terms of Drug Interaction in an Elderly Population: A Retrospective Cross-Sectional Study. J. Clin. Med. 2023, 12, 3960. [Google Scholar] [CrossRef] [PubMed]
- Reinhild Haerig, T.; Krause, D.; Klaassen-Mielke, R.; Rudolf, H.; Trampisch, H.J.; Thuermann, P. Potentially inappropriate medication including drug-drug interaction and the risk of frequent falling, hospital admission, and death in older adults—Results of a large cohort study (getABI). Front. Pharmacol. 2023, 14, 1062290. [Google Scholar] [CrossRef] [PubMed]
- Lion, S.; Evrard, P.; Foulon, V.; Spinewine, A. Drug-drug interactions in nursing home residents: Analysis from the COME-ON trial. Age Ageing 2023, 52, afac278. [Google Scholar] [CrossRef]
- Falconi, G.; Kashan, S. Drug Interactions in Palliative Care. In StatPearls; Internet; StatPearls Publishing: Treasure Island, FL, USA, 2023. [Google Scholar]
- Igho-Osagie, E.; Brzozowski, K.; Jin, H.; Brown, J.; Williams, M.G.; Puenpatom, A. Prevalence of Potential Drug-drug Interactions With Ritonavir-containing COVID-19 Therapy in the United States: An Analysis of the National Health and Nutrition Examination Survey. Clin. Ther. 2023, 45, 390–399.e4. [Google Scholar] [CrossRef]
- Makary, M.A.; Daniel, M. Medical error-the third leading cause of death in the US. BMJ 2016, 353, i2139. [Google Scholar] [CrossRef]
- Marincowitz, C.; Preston, L.; Cantrell, A.; Tonkins, M.; Sabir, L.; Mason, S. Factors associated with increased Emergency Department transfer in older long-term care residents: A systematic review. Lancet Healthy Longev. 2022, 3, e437–e447. [Google Scholar] [CrossRef]
- Cerreta, F.; Vučić, K.; Laslop, A. Assessing Medicines for Use in the Geriatric Population. Clin. Pharmacol. Ther. 2023, 113, 536–540. [Google Scholar] [CrossRef]
- Hahn, M.; Roll, S.C. The Influence of Pharmacogenetics on the Clinical Relevance of Pharmacokinetic Drug-Drug Interactions: Drug-Gene, Drug-Gene-Gene and Drug-Drug-Gene Interactions. Pharmaceuticals 2021, 14, 487. [Google Scholar] [CrossRef]
- Malki, M.A.; Pearson, E.R. Drug-drug-gene interactions and adverse drug reactions. Pharmacogenomics J. 2020, 20, 355–366. [Google Scholar] [CrossRef]
- Veiga-Matos, J.; Remião, F.; Motales, A. Pharmacokinetics and Toxicokinetics Roles of Membrane Transporters at Kidney Level. J. Pharm. Pharm. Sci. 2020, 23, 333–356. [Google Scholar] [CrossRef] [PubMed]
- Medscape. Drug Interaction Checker. Available online: https://reference.medscape.com/drug-interactionchecker (accessed on 26 June 2023).
- Vonbach, P.; Dubied, A.; Krähenbühl, S.; Beer, J.H. Evaluation of frequently used drug interaction screening programs. Pharm. World Sci. 2008, 30, 367–374. [Google Scholar] [CrossRef] [PubMed]
- Marcath, L.A.; Xi, J.; Hoylman, E.K.; Kidwell, K.M.; Kraft, S.L.; Hertz, D.L. Comparison of Nine Tools for Screening Drug-Drug Interactions of Oral Oncolytics. J. Oncol. Pract. 2018, 14, e368–e374. [Google Scholar] [CrossRef] [PubMed]
- Hecker, M.; Frahm, N.; Bachmann, P.; Debus, J.L.; Haker, M.C.; Mashhadiakbar, P.; Langhorst, S.E.; Baldt, J.; Streckenbach, B.; Heidler, F.; et al. Screening for severe drug-drug interactions in patients with multiple sclerosis: A comparison of three drug interaction databases. Front. Pharmacol. 2022, 13, 946351. [Google Scholar] [CrossRef]
- Amkreutz, J.; Koch, A.; Buendgens, L.; Trautwein, C.; Eisert, A. Clinical decision support systems differ in their ability to identify clinically relevant drug interactions of immunosuppressants in kidney transplant patients. J. Clin. Pharm. Ther. 2017, 42, 276–285. [Google Scholar] [CrossRef]
- Kheshti, R.; Aalipour, M.; Namazi, S. A comparison of five common drug-drug interaction software programs regarding accuracy and comprehensiveness. J. Res. Pharm. Pract. 2016, 5, 257–263. [Google Scholar] [CrossRef]
- Das, B.; Ramasubbu, S.K.; Agnihotri, A.; Kumar, B.; Rawat, V.S. Leading 20 drug-drug interactions, polypharmacy, and analysis of the nature of risk factors due to QT interval prolonging drug use and potentially inappropriate psychotropic use in elderly psychiatry outpatients. Ther. Adv. Cardiovasc. Dis. 2021, 15. [Google Scholar] [CrossRef]
- Roca, B.; Roca, M. Assessment of Drug Interactions with Online Electronic Checkers in Multi-Pathological Patients. Pharmacology 2022, 107, 111–115. [Google Scholar] [CrossRef]
- Şen, S.; Karahan, E.; Büyükulaş, C.; Polat, Y.O.; Üresin, A.Y. Colchicine for cardiovascular therapy: A drug interaction perspective and a safety meta-analysis. Anatol. J. Cardiol. 2021, 25, 753–761. [Google Scholar] [CrossRef]
- Assefa, Y.A.; Kedir, A.; Kahaliw, W. Survey on Polypharmacy and Drug-Drug Interactions among Elderly People with Cardiovascular Diseases at Yekatit 12 Hospital, Addis Ababa, Ethiopia. Integr. Pharm. Res. Pract. 2020, 9, 1–9. [Google Scholar] [CrossRef]
- Jain, S.; Jain, P.; Sharma, K.; Saraswat, P. A Prospective Analysis of Drug Interactions in Patients of Intensive Cardiac Care Unit. J. Clin. Diagn. Res. 2017, 11, FC01–FC04. [Google Scholar] [CrossRef] [PubMed]
- Yao, X.; Tsang, T.; Sun, Q.; Quinney, S.; Zhang, P.; Ning, X.; Li, L.; Shen, L. Mining and visualizing high-order directional drug interaction effects using the FAERS database. BMC Med. Inform. Decis. Mak. 2020, 20, 50. [Google Scholar] [CrossRef] [PubMed]
- Alrowais, F.; Alotaibi, S.S.; Hilal, A.M.; Marzouk, R.; Mohsen, H.; Osman, A.E.; Alneil, A.A.; Eldesouki, M.I. Clinical Decision Support Systems to Predict Drug-Drug Interaction Using Multilabel Long Short-Term Memory with an Autoencoder. Int. J. Environ. Res. Public Health 2023, 20, 2696. [Google Scholar] [CrossRef]
- Yu, L.; Xu, Z.; Cheng, M.; Lin, W.; Qiu, W.; Xiao, X. MSEDDI: Multi-Scale Embedding for Predicting Drug-Drug Interaction Events. Int. J. Mol. Sci. 2023, 24, 4500. [Google Scholar] [CrossRef]
- Brattig Correia, R.; de Araújo Kohler, L.P.; Mattos, M.M.; Rocha, L.M. City-wide electronic health records reveal gender and age biases in administration of known drug-drug interactions. NPJ Digit. Med. 2019, 2, 74. [Google Scholar] [CrossRef] [PubMed]
- Spanakis, M.; Ioannou, P.; Tzalis, S.; Papakosta, V.; Patelarou, E.; Tzanakis, N.; Patelarou, A.; Kofteridis, D.P. Drug-Drug Interactions among Patients Hospitalized with COVID-19 in Greece. J. Clin. Med. 2022, 11, 7172. [Google Scholar] [CrossRef] [PubMed]
- Ingersgaard, M.V.; Helms Andersen, T.; Norgaard, O.; Grabowski, D.; Olesen, K. Reasons for Nonadherence to Statins—A Systematic Review of Reviews. Patient Prefer. Adherence 2020, 14, 675–691. [Google Scholar] [CrossRef] [PubMed]
- Rochon, P.A.; Petrovic, M.; Cherubini, A.; Onder, G.; O’Mahony, D.; Sternberg, S.A.; Stall, N.M.; Gurwitz, J.H. Polypharmacy, inappropriate prescribing, and deprescribing in older people: Through a sex and gender lens. Lancet Healthy Longev. 2021, 2, e290–e300. [Google Scholar] [CrossRef]
- Chazova, I.E.; Zhernakova, Y.V. Diagnosis and treatment of arterial hypertension [Guidelines]. Syst. Hypertens. 2019, 16, 6–31. [Google Scholar] [CrossRef]
- Dumbreck, S.; Flynn, A.; Nairn, M.; Wilson, M.; Treweek, S.; Mercer, S.W.; Alderson, P.; Thompson, A.; Payne, K.; Guthrie, B. Drug-disease and drug-drug interactions: Systematic examination of recommendations in 12 UK national clinical guidelines. BMJ 2015, 350, h949. [Google Scholar] [CrossRef]
- Tan, Y.Y.; Papez, V.; Chang, W.H.; Mueller, S.H.; Denaxas, S.; Lai, A.G. Comparing clinical trial population representativeness to real-world populations: An external validity analysis encompassing 43,895 trials and 5,685,738 individuals across 989 unique drugs and 286 conditions in England. Lancet Healthy Longev. 2022, 3, e674–e689. [Google Scholar] [CrossRef] [PubMed]
- Tamargo, J.; Kjeldsen, K.P.; Delpón, E.; Semb, A.G.; Cerbai, E.; Dobrev, D.; Savarese, G.; Sulzgruber, P.; Rosano, G.; Borghi, C.; et al. Facing the challenge of polypharmacy when prescribing for older people with cardiovascular disease. A review by the European Society of Cardiology Working Group on Cardiovascular Pharmacotherapy. Eur. Heart J. Cardiovasc. Pharmacother. 2022, 8, 406–419. [Google Scholar] [CrossRef]
- Anfinogenova, N.D.; Trubacheva, I.A.; Popov, S.V.; Efimova, E.V.; Ussov, W.Y. Trends and concerns of potentially inappropriate medication use in patients with cardiovascular diseases. Expert. Opin. Drug Saf. 2021, 20, 1191–1206. [Google Scholar] [CrossRef]
- Anfinogenova, Y.; Grakova, E.V.; Shvedova, M.; Kopieva, K.V.; Teplyakov, A.T.; Popov, S.V. Interdisciplinary approach to compensation of hypoglycemia in diabetic patients with chronic heart failure. Heart Fail. Rev. 2018, 23, 481–497. [Google Scholar] [CrossRef] [PubMed]
- Lyles, C.R.; Nelson, E.C.; Frampton, S.; Dykes, P.C.; Cemballi, A.G.; Sarkar, U. Using Electronic Health Record Portals to Improve Patient Engagement: Research Priorities and Best Practices. Ann. Intern. Med. 2020, 172, S123–S129. [Google Scholar] [CrossRef] [PubMed]






| Parameter | Value |
|---|---|
| Ethnic group, n (%): | |
| White/Caucasian, n (%) | 704 (100%) |
| Sex | |
| Male, n (%) | 268 (38.1%) |
| Female, n (%) | 436 (61.9%) |
| Age, median (IQR), years | 78 (75; 82) |
| Age of men, median (IQR), years | 77.5 (75; 83) |
| Age of women, median (IQR), years | 79 (75; 82) |
| Type of medical care encounter: | |
| Ambulatory visits, n (%) | 458 (65.1) |
| Home visits, n (%) | 118 (16.8) |
| Hospitalizations, n (%) | 110 (15.6) |
| Emergency assessment unit visits, n (%) | 18 (2.56) |
| Time of electronic health record registration | Jan 2019–Aug 2022 |
| Medication List; Sex | Polypharmacy |
|---|---|
| T-List; m, n | 69 *§ |
| T-List; f, n | 146 *§ |
| P-List; m, n | 166 § |
| P-List; f, n | 269 § |
| T-List; m + f, n | 215 § |
| P-List; m + f, n | 435 § |
| Drug Combination | n | Top 10 Serious Drug–Drug Interactions (T-List) |
|---|---|---|
| aspirin + perindopril | 25 | Aspirin, perindopril. Pharmacodynamic antagonism. Avoid or Use Alternate Drug. Co-administration may result in a significant decrease in renal function. NSAIDs may diminish the antihypertensive effect of ACE inhibitors. The mechanism of these interactions is likely related to the ability of NSAIDs to reduce the synthesis of vasodilating renal prostaglandins |
| aspirin + lisinopril | 17 | Aspirin, lisinopril. Pharmacodynamic antagonism. Avoid or Use Alternate Drug. Co-administration may result in a significant decrease in renal function. NSAIDs may diminish the antihypertensive effect of ACE inhibitors. The mechanism of these interactions is likely related to the ability of NSAIDs to reduce the synthesis of vasodilating renal prostaglandins |
| amiodarone + indapamide | 9 | Amiodarone and indapamide both increase QTc interval. Avoid or Use Alternate Drug |
| aspirin + enalapril * | 7 | Aspirin, enalapril. Pharmacodynamic antagonism. Avoid or Use Alternate Drug. Co-administration may result in a significant decrease in renal function. NSAIDs may diminish the antihypertensive effect of ACE inhibitors. The mechanism of these interactions is likely related to the ability of NSAIDs to reduce the synthesis of vasodilating renal prostaglandins |
| bisoprolol + digoxin | 7 | Bisoprolol increases effects of digoxin by pharmacodynamic synergism. Use Caution/Monitor. Enhanced bradycardia |
| clopidogrel + omeprazole | 7 | Omeprazole decreases effects of clopidogrel by affecting hepatic enzyme CYP2C19 metabolism. Avoid or Use Alternate Drug. Clopidogrel efficacy may be reduced by drugs that inhibit CYP2C19. Inhibition of platelet aggregation by clopidogrel is entirely due to an active metabolite. Clopidogrel is metabolized to this active metabolite in part by CYP2C19 |
| ceftriaxone + enoxaparin | 6 | Ceftriaxone increases effects of enoxaparin by anticoagulation. Avoid or Use Alternate Drug. cephalosporins may decrease prothrombin activity |
| apixaban + clopidogrel | 4 | Clopidogrel and apixaban both increase anticoagulation. Avoid or Use Alternate Drug |
| digoxin + omeprazole | 4 | Esomeprazole will increase the level or effect of digoxin by increasing gastric pH. Applies only to oral form of both agents. Avoid or Use Alternate Drug |
| aspirin + ketorolac | 3 | Aspirin, ketorolac. Either increases toxicity of the other by pharmacodynamic synergism. Contraindicated |
| Drug Combination | n | Top 10 Monitor-Closely Drug–Drug Interactions (T-List) |
|---|---|---|
| aspirin + losartan | 104 | Aspirin decreases effects of losartan by pharmacodynamic antagonism. Modify Therapy/Monitor Closely. NSAIDs decrease synthesis of vasodilating renal prostaglandins, and thus affect fluid homeostasis and may diminish antihypertensive effect |
| aspirin + bisoprolol | 94 | Aspirin decreases effects of bisoprolol by pharmacodynamic antagonism. Use Caution/Monitor. Long term (>1 wk) NSAID use. NSAIDs decrease prostaglandin synthesis |
| bisoprolol + losartan | 58 | Bisoprolol, losartan. Mechanism: pharmacodynamic synergism. Use Caution/Monitor. Risk of fetal compromise if given during pregnancy |
| aspirin + spironolactone | 42 | Aspirin decreases effects of spironolactone by unspecified interaction mechanism. Use Caution/Monitor. When used concomitantly, spironolactone dose may need to be titrated to higher maintenance dose and the patient should be observed closely to determine if the desired effect is obtained |
| amiodarone + losartan | 32 | Amiodarone will increase the level or effect of losartan by affecting hepatic enzyme CYP2C9/10 metabolism. Use Caution/Monitor. May inhibit the conversion of losartan to its active metabolite E-3174. Importance of interaction not established; monitor individual therapeutic response to determine losartan dosage |
| aspirin + metoprolol | 32 | Aspirin decreases effects of metoprolol by pharmacodynamic antagonism. Use Caution/Monitor. Long term (>1 wk) NSAID use. NSAIDs decrease prostaglandin synthesis |
| losartan + metoprolol | 32 | Losartan and metoprolol both increase serum potassium. Use Caution/Monitor |
| bisoprolol + torsemide | 31 | Bisoprolol increases and torsemide decreases serum potassium. Effect of interaction is not clear, use caution. Use Caution/Monitor |
| digoxin + spironolactone | 30 | Spironolactone increases levels of digoxin by Other (see comment). Use Caution/Monitor. Comment: Spironolactone may cause false elevation of digoxin assay |
| aspirin + perindopril | 25 | Aspirin, perindopril. pharmacodynamic antagonism. Avoid or Use Alternate Drug. Co-administration may result in a significant decrease in renal function. NSAIDs may diminish the antihypertensive effect of ACE inhibitors. The mechanism of these interactions is likely related to the ability of NSAIDs to reduce the synthesis of vasodilating renal prostaglandins |
| Drug Combination | n | Top 10 Serious Drug–Drug Interactions (P-List) |
|---|---|---|
| aspirin + captopril * | 62 | Aspirin, captopril. Pharmacodynamic antagonism. Avoid or Use Alternate Drug. Co-administration may result in a significant decrease in renal function. NSAIDs may diminish the antihypertensive effect of ACE inhibitors. The mechanism of these interactions is likely related to the ability of NSAIDs to reduce the synthesis of vasodilating renal prostaglandins |
| captopril + losartan | 38 | Losartan, captopril. Either increases toxicity of the other by pharmacodynamic synergism. Avoid or Use Alternate Drug. Dual blockade of renin-angiotensin system increases risks of hypotension, hyperkalemia, and renal impairment |
| aspirin + lisinopril | 34 | Aspirin, lisinopril. pharmacodynamic antagonism. Avoid or Use Alternate Drug. Co-administration may result in a significant decrease in renal function. NSAIDs may diminish the antihypertensive effect of ACE inhibitors. The mechanism of these interactions is likely related to the ability of NSAIDs to reduce the synthesis of vasodilating renal prostaglandins |
| aspirin + perindopril | 34 | Aspirin, perindopril. pharmacodynamic antagonism. Avoid or Use Alternate Drug. Co-administration may result in a significant decrease in renal function. NSAIDs may diminish the antihypertensive effect of ACE inhibitors. The mechanism of these interactions is likely related to the ability of NSAIDs to reduce the synthesis of vasodilating renal prostaglandins |
| clopidogrel + omeprazole | 30 | Omeprazole decreases effects of clopidogrel by affecting hepatic enzyme CYP2C19 metabolism. Avoid or Use Alternate Drug. Clopidogrel efficacy may be reduced by drugs that inhibit CYP2C19. Inhibition of platelet aggregation by clopidogrel is entirely due to an active metabolite. Clopidogrel is metabolized to this active metabolite in part by CYP2C19 |
| amiodarone + indapamide | 9 | Amiodarone and indapamide both increase QTc interval. Avoid or Use Alternate Drug |
| aspirin + enalapril * | 7 | Aspirin, enalapril. pharmacodynamic antagonism. Avoid or Use Alternate Drug. Co-administration may result in a significant decrease in renal function. NSAIDs may diminish the antihypertensive effect of ACE inhibitors. The mechanism of these interactions is likely related to the ability of NSAIDs to reduce the synthesis of vasodilating renal prostaglandins |
| aspirin + fosinopril | 7 | Aspirin, fosinopril. pharmacodynamic antagonism. Avoid or Use Alternate Drug. Co-administration may result in a significant decrease in renal function. NSAIDs may diminish the antihypertensive effect of ACE inhibitors. The mechanism of these interactions is likely related to the ability of NSAIDs to reduce the synthesis of vasodilating renal prostaglandins |
| bisoprolol + digoxin | 6 | Bisoprolol increases effects of digoxin by pharmacodynamic synergism. Use Caution/Monitor. Enhanced bradycardia |
| candesartan + captopril | 6 | Candesartan, captopril. Either increases toxicity of the other by pharmacodynamic synergism. Avoid or Use Alternate Drug. Dual blockade of renin-angiotensin system increases risks of hypotension, hyperkalemia, and renal impairment |
| Drug Combination | n | Top 10 Monitor-Closely Drug–Drug Interactions (P-List) |
|---|---|---|
| aspirin + bisoprolol | 180 | Aspirin decreases effects of bisoprolol by pharmacodynamic antagonism. Use Caution/Monitor. Long term (>1 wk) NSAID use. NSAIDs decrease prostaglandin synthesis |
| aspirin + losartan | 168 | Aspirin decreases effects of losartan by pharmacodynamic antagonism. Modify Therapy/Monitor Closely. NSAIDs decrease synthesis of vasodilating renal prostaglandins, and thus affect fluid homeostasis and may diminish antihypertensive effect |
| aspirin + metoprolol | 86 | Aspirin decreases effects of metoprolol by pharmacodynamic antagonism. Use Caution/Monitor. Long term (>1 wk) NSAID use. NSAIDs decrease prostaglandin synthesis |
| bisoprolol + losartan | 82 | Bisoprolol, losartan. Mechanism: pharmacodynamic synergism. Use Caution/Monitor. Risk of fetal compromise if given during pregnancy |
| aspirin + captopril * | 62 | Aspirin, captopril. pharmacodynamic antagonism. Avoid or Use Alternate Drug. Co-administration may result in a significant decrease in renal function. NSAIDs may diminish the antihypertensive effect of ACE inhibitors. The mechanism of these interactions is likely related to the ability of NSAIDs to reduce the synthesis of vasodilating renal prostaglandins |
| aspirin + spironolactone | 62 | Aspirin decreases effects of spironolactone by unspecified interaction mechanism. Use Caution/Monitor. When used concomitantly, spironolactone dose may need to be titrated to higher maintenance dose and the patient should be observed closely to determine if the desired effect is obtained |
| aspirin + nitroglycerin | 61 | Aspirin increases effects of nitroglycerin sublingual by additive vasodilation. Use Caution/Monitor. Vasodilatory and hemodynamic effects of NTG may be enhanced by co-administration with aspirin (additive effect desirable for emergent treatment) |
| spironolactone + torsemide | 56 | Spironolactone increases and torsemide decreases serum potassium. Effect of interaction is not clear, use caution. Modify Therapy/Monitor Closely |
| bisoprolol + torsemide | 55 | Bisoprolol increases and torsemide decreases serum potassium. Effect of interaction is not clear, use caution. Use Caution/Monitor |
| aspirin + clopidogrel | 46 | Aspirin, clopidogrel. Either increases toxicity of the other by pharmacodynamic synergism. Use Caution/Monitor. The need for simultaneous use of low-dose aspirin and anticoagulant or antiplatelet agents are common for patients with cardiovascular disease; monitor closely |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Anfinogenova, N.D.; Novikova, O.M.; Trubacheva, I.A.; Efimova, E.V.; Chesalov, N.P.; Ussov, W.Y.; Maksimova, A.S.; Shelkovnikova, T.A.; Ryumshina, N.I.; Stepanov, V.A.; et al. Prescribed Versus Taken Polypharmacy and Drug–Drug Interactions in Older Cardiovascular Patients during the COVID-19 Pandemic: Observational Cross-Sectional Analytical Study. J. Clin. Med. 2023, 12, 5061. https://doi.org/10.3390/jcm12155061
Anfinogenova ND, Novikova OM, Trubacheva IA, Efimova EV, Chesalov NP, Ussov WY, Maksimova AS, Shelkovnikova TA, Ryumshina NI, Stepanov VA, et al. Prescribed Versus Taken Polypharmacy and Drug–Drug Interactions in Older Cardiovascular Patients during the COVID-19 Pandemic: Observational Cross-Sectional Analytical Study. Journal of Clinical Medicine. 2023; 12(15):5061. https://doi.org/10.3390/jcm12155061
Chicago/Turabian StyleAnfinogenova, Nina D., Oksana M. Novikova, Irina A. Trubacheva, Elena V. Efimova, Nazary P. Chesalov, Wladimir Y. Ussov, Aleksandra S. Maksimova, Tatiana A. Shelkovnikova, Nadezhda I. Ryumshina, Vadim A. Stepanov, and et al. 2023. "Prescribed Versus Taken Polypharmacy and Drug–Drug Interactions in Older Cardiovascular Patients during the COVID-19 Pandemic: Observational Cross-Sectional Analytical Study" Journal of Clinical Medicine 12, no. 15: 5061. https://doi.org/10.3390/jcm12155061
APA StyleAnfinogenova, N. D., Novikova, O. M., Trubacheva, I. A., Efimova, E. V., Chesalov, N. P., Ussov, W. Y., Maksimova, A. S., Shelkovnikova, T. A., Ryumshina, N. I., Stepanov, V. A., Popov, S. V., & Repin, A. N. (2023). Prescribed Versus Taken Polypharmacy and Drug–Drug Interactions in Older Cardiovascular Patients during the COVID-19 Pandemic: Observational Cross-Sectional Analytical Study. Journal of Clinical Medicine, 12(15), 5061. https://doi.org/10.3390/jcm12155061







