Pediatric Benign Paroxysmal Positional Vertigo: Degree of Nystagmus and Concurrent Dizziness Differs from Adult BPPV
Abstract
1. Introduction
2. Materials and Methods
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Hanley, K.; O’Dowd, T.; Considine, N. A systematic review of vertigo in primary care. Br. J. Gen. Pract. 2001, 51, 666–671. [Google Scholar] [PubMed]
- Bhattacharyya, N.; Gubbels, S.P.; Schwartz, S.R.; Edlow, J.A.; El-Kashlan, H.; Fife, T.; Holmberg, J.M.; Mahoney, K.; Hollingsworth, D.B.; Roberts, R.; et al. Clinical Practice Guideline: Benign Paroxysmal Positional Vertigo (Update). Otolaryngol. Head Neck Surg. 2017, 156 (Suppl. S3), S1–S47. [Google Scholar] [CrossRef] [PubMed]
- Kim, J.S.; Zee, D.S. Clinical practice. Benign paroxysmal positional vertigo. N. Engl. J. Med. 2014, 370, 1138–1147. [Google Scholar] [CrossRef] [PubMed]
- Gioacchini, F.M.; Alicandri-Ciufelli, M.; Kaleci, S.; Magliulo, G.; Re, M. Prevalence and diagnosis of vestibular disorders in children: A review. Int. J. Pediatr. Otorhinolaryngol. 2014, 78, 718–724. [Google Scholar] [CrossRef] [PubMed]
- Lee, J.D.; Kim, C.H.; Hong, S.M.; Kim, S.H.; Suh, M.W.; Kim, M.B.; Shim, D.B.; Chu, H.; Lee, N.H.; Kim, M.; et al. Prevalence of vestibular and balance disorders in children and adolescents according to age: A multi-center study. Int. J. Pediatr. Otorhinolaryngol. 2017, 94, 36–39. [Google Scholar] [CrossRef] [PubMed]
- Davitt, M.; Delvecchio, M.T.; Aronoff, S.C. The Differential Diagnosis of Vertigo in Children: A Systematic Review of 2726 Cases. Pediatr. Emerg. Care 2020, 36, 368–371. [Google Scholar] [CrossRef] [PubMed]
- Lee, H.M.; Park, J.; Lee, B.; Lee, K.H.; Park, S.K.; Chang, J. Etiology and Clinical Characteristics of Pediatric Dizziness. Korean J Otorhinolaryngol. Head Neck Surg. 2018, 61, 459–464. [Google Scholar] [CrossRef]
- Baloh, R.W.; Honrubia, V.; Jacobson, K. Benign positional vertigo: Clinical and oculographic features in 240 cases. Neurology 1987, 37, 371–378. [Google Scholar] [CrossRef] [PubMed]
- D’Agostino, R.; Melagrana, A.; Taborelli, G. Benign positional paroxysmal vertigo of horizontal semicircular canal in the child: Case report. Int. J. Pediatr. Orl. 2003, 67, 549–551. [Google Scholar] [CrossRef]
- Wang, A.; Zhou, G.; Brodsky, J.R. Characteristics of Benign Paroxysmal Positional Vertigo in Young Children. Laryngoscope 2023, 133, 694–699. [Google Scholar] [CrossRef]
- Brodsky, J.R.; Lipson, S.; Wilber, J.; Zhou, G. Benign Paroxysmal Positional Vertigo (BPPV) in Children and Adolescents: Clinical Features and Response to Therapy in 110 Pediatric Patients. Otol. Neurotol. 2018, 39, 344–350. [Google Scholar] [CrossRef] [PubMed]
- Choi, H.G.; Kim, G.; Kim, B.J.; Hong, S.K.; Kim, H.J.; Lee, H.J. How rare is benign paroxysmal positional vertigo in children? A review of 20 cases and their epidemiology. Int. J. Pediatr. Otorhinolaryngol. 2020, 132, 110008. [Google Scholar] [CrossRef] [PubMed]
- Neuhauser, H.K.; Lempert, T. Vertigo: Epidemiologic aspects. Semin. Neurol. 2009, 29, 473–481. [Google Scholar] [CrossRef] [PubMed]
- Ogun, O.A.; Büki, B.; Cohn, E.S.; Janky, K.L.; Lundberg, Y.W. Menopause and benign paroxysmal positional vertigo. Menopause 2014, 21, 886–889. [Google Scholar] [CrossRef] [PubMed]
- Mucci, V.; Hamid, M.; Jacquemyn, Y.; Browne, C.J. Influence of sex hormones on vestibular disorders. Curr. Opin. Neurol. 2022, 35, 135–141. [Google Scholar] [CrossRef] [PubMed]
- Yang, L.; Xu, Y.; Zhang, Y.; Vijayakumar, S.; Jones, S.M.; Lundberg, Y.Y.W. Mechanism Underlying the Effects of Estrogen Deficiency on Otoconia. J. Assoc. Res. Otolaryngol. 2018, 19, 353–362. [Google Scholar] [CrossRef]
- Lyu, H.Y.; Chen, K.G.; Yin, D.M.; Hong, J.; Yang, L.; Zhang, T.Y.; Dai, P.D. The age-related orientational changes of human semicircular canals. Clin. Exp. Otorhinolaryngol. 2016, 9, 109–115. [Google Scholar] [CrossRef] [PubMed]
- Yetiser, S. Review of the pathology underlying benign paroxysmal positional vertigo. J. Int. Med. Res. 2020, 48, 300060519892370. [Google Scholar] [CrossRef] [PubMed]
- Jang, Y.S.; Hwang, C.H.; Shin, J.Y.; Bae, W.Y.; Kin, L.S. Age-related changes on the morphology of the otoconia. Laryngoscope 2006, 116, 996–1001. [Google Scholar] [CrossRef]
- Wang, A.; Zhou, G.; Lipson, S.; Kawai, K.; Corcoran, M.; Brodsky, J.R. Multifactorial characteristics of pediatric dizziness and imbalance. Laryngoscope 2020, 131, E1308–E1314. [Google Scholar] [CrossRef]
- Chu, C.H.; Liu, C.J.; Lin, L.Y.; Chen, T.J.; Wang, S.J. Migraine is associated with an increased risk for benign paroxysmal positional vertigo: A nationwide population-based study. J. Headache Pain 2015, 16, 62. [Google Scholar] [CrossRef] [PubMed]
- Uneri, A. Migraine and benign paroxysmal positional vertigo: An outcome study of 476 patients. Ear Nose Throat J. 2004, 83, 814–815. [Google Scholar] [CrossRef] [PubMed]
- Kim, M.J.; Rhim, G.I. Relationship between orthostatic hypotension and recurrence of benign paroxysmal positional vertigo. Sci. Rep. 2022, 12, 10685. [Google Scholar] [CrossRef] [PubMed]
- Pezzoli, M.; Garzaro, M.; Pecorari, G.; Cena, M.; Giordano, C.; Albera, R. Benign paroxysmal positional vertigo and orthostatic hypotension. Clin. Auton. Res. 2010, 20, 27–31. [Google Scholar] [CrossRef]

| Characteristics | Total Participants | ||
|---|---|---|---|
| Pediatric | Adult | ||
| N | 30 | 264 | |
| Age at visit | |||
| Mean (SD) | 13.60 (4.15) | 60.86 (13.74) | |
| Median (range) | 14.5 (5~18) | 63 (22~90) | |
| Sex, n (%) | |||
| Male | 14 (46.67) | 79 (29.92) | |
| Female | 16 (53.33) | 185 (70.08) | |
| Female-to-Male ratio | 1.14 | 2.34 | |
| Duration of f/up (week) | |||
| Mean (SD) | 7.03 (13.25) | 4.23 (7.32) | |
| Median (range) | 2.5 (0~60) | 2 (0~74) | |
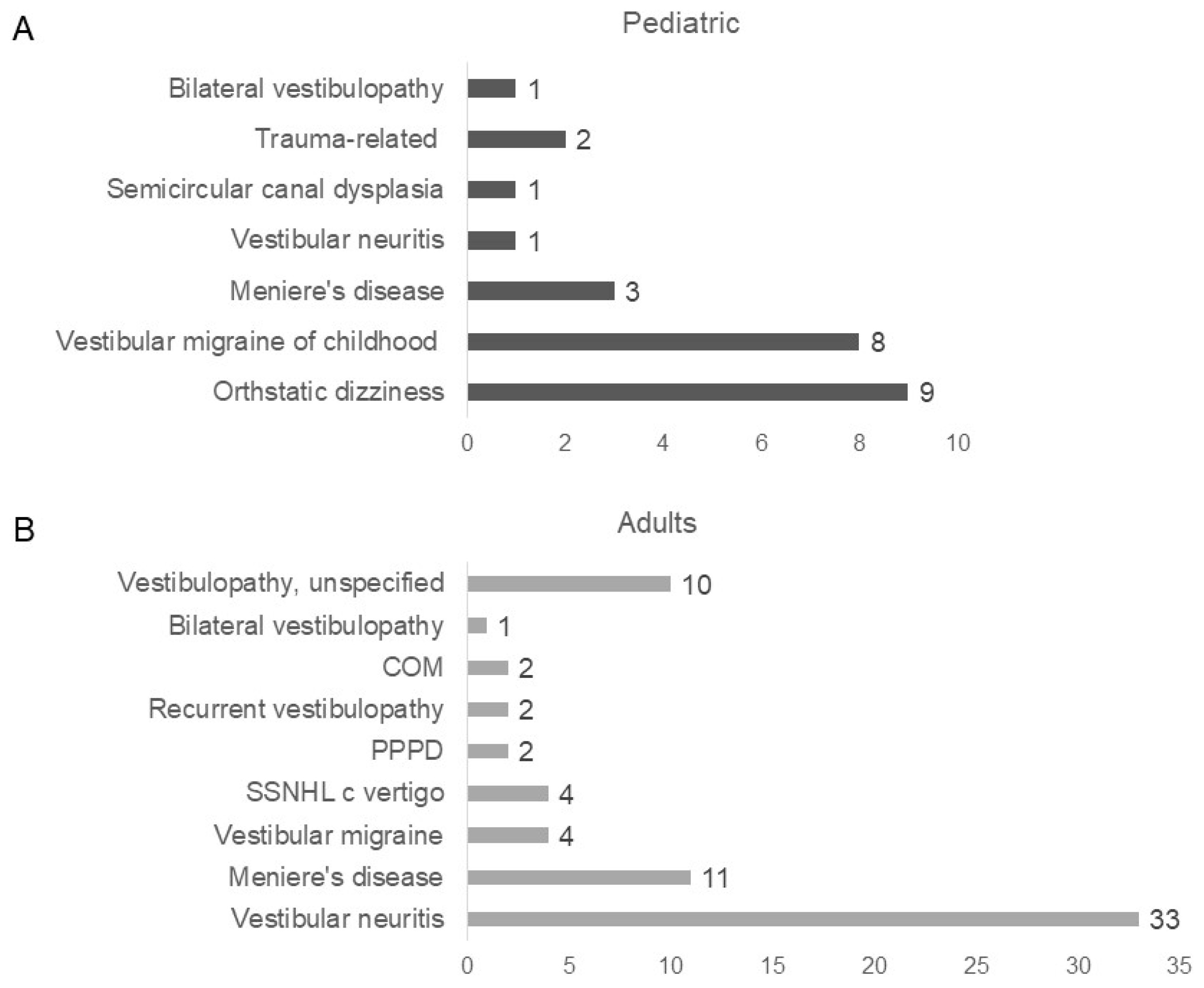
| Concurrent dizziness disorder, n (%) | 19 (63.33) | 69 (26.14) | |
| Comorbid disease (excluding dizziness), n (%) | 1 (3.33) | 120 (45.45) | |
| Characteristics | Total Participants | |||
|---|---|---|---|---|
| Pediatric | Adult | p-Value | ||
| Affected canal, n (%) | 0.007 * | |||
| posterior | 5 (16.67) | 123 (46.59) | ||
| lateral | 24 (80.00) | 131 (49.62) | ||
| superior | 0 (0.00) | 5 (1.89) | ||
| Affected side, n (%) | 0.190 | |||
| right | 18 (60.00) | 154 (58.33) | ||
| left | 10 (33.33) | 105 (39.77) | ||
| both | 2 (6.67) | 5 (1.89) | ||
| Type, n (%) | 0.056 | |||
| canalolithiasis | 18 (60.00) | 209 (79.17) | ||
| cupulolithiasis | 12 (40.00) | 52 (19.70) | ||
| both | 0 (0.00) | 3 (1.14) | ||
| Nyst (deg/sec), mean (SD) | 6.82 (12.09) | 15.58 (20.90) | <0.001 * | |
| Multicanal, n (%) | 3 (10.00) | 27 (10.23) | 1.000 | |
| Number of CRP, mean (SD) | 1.57 (0.94) | 1.88 (1.94) | 0.733 | |
| Recurrent, n (%) | 2 (6.67) | 58 (21.97) | 0.055 | |
| Recurrent number, mean (SD) | 1.00 (0.00) | 1.96 (1.16) | 0.181 | |
| Canal conversion, n (%) | 0 (0.00) | 21 (7.95) | 0.145 | |
| Characteristics | Pediatric | Adults | |||
|---|---|---|---|---|---|
| 20–40 | 41–60 | 61+ | |||
| N | 30 | 23 | 89 | 152 | |
| Sex, n (%) | |||||
| Male | 14 (46.67) | 7 (30.43) | 24 (26.97) | 48 (31.58) | |
| Female | 16 (53.33) | 16 (69.57) | 65 (73.03) | 104 (68.42) | |
| Female-to-Male ratio | 1.14 | 2.29 | 2.71 | 2.17 | |
| Duration of f/up (week) | |||||
| Mean (SD) | 7.03 (13.25) | 5.65 (12.45) | 4.02 (5.40) | 4.14 (7.31) | |
| Median (range) | 2.50 (0~60) | 2 (0~60) | 1 (0~28) | 2 (0~74) | |
| Concurrent dizziness disorder, n (%) | 19 (63.33) | 8 (34.78) | 18 (20.22) | 43 (28.29) | |
| Comorbid disease (excluding dizziness), n (%) | 1 (3.33) | 2 (8.70) | 30 (33.71) | 88 (57.89) | |
| Characteristics | Adults | |||||
|---|---|---|---|---|---|---|
| Pediatric | 20–40 | 41–60 | 61+ | p-Value | ||
| Affected canal, n (%) | 0.096 | |||||
| posterior | 5 (16.67) | 13 (56.52) | 42 (47.19) | 68 (44.74) | ||
| horizontal | 24 (80.00) | 10 (43.48) | 43 (48.31) | 78 (51.32) | ||
| superior | 0 (0.00) | 0 (0.00) | 2 (2.25) | 3 (1.97) | ||
| Affected side, n (%) | 0.417 | |||||
| right | 18 (60.00) | 13 (56.52) | 47 (52.81) | 94 (61.84) | ||
| left | 10 (33.33) | 10 (43.48) | 41 (46.07) | 54 (35.53) | ||
| both | 2 (6.67) | 0 (0.00) | 1 (1.12) | 4 (2.63) | ||
| Type, n (%) | 0.154 | |||||
| canalolithiasis | 18 (60.00) | 18 (78.26) | 74 (83.15) | 117 (76.97) | ||
| cupulolithiasis | 12 (40.00) | 5 (21.74) | 15 (16.85) | 32 (21.05) | ||
| both | 0 (0.00) | 0 (0.00) | 0 (0.00) | 3 (1.97) | ||
| Nyst (deg/sec), mean (SD) | 6.82 (12.09) | 15.96 (35.05) | 13.52 (18.89) | 16.82 (19.53) | <0.001 * | |
| Multicanal, n (%) | 3 (10.00) | 4 (17.39) | 7 (7.87) | 16 (10.53) | 0.560 | |
| Number of CRP, mean (SD) | 1.57 (0.94) | 1.65 (0.98) | 1.88 (1.70) | 1.91 (2.18) | 0.985 | |
| Recurrent, n (%) | 2 (6.67) † | 4 (17.39) | 17 (19.10) | 37 (24.34) † | 0.162 | |
| Recurrent number, mean (SD) | 1.00 (0.00) | 1.75 (0.96) | 1.93 (0.88) | 2.00 (1.29) | 0.591 | |
| Canal conversion, n (%) | 0 (0.00) | 2 (8.70) | 9 (10.11) | 10 (6.58) | 0.286 | |
| Parameter | Estimate | Standard Error | t-Value | Pr > |t| |
|---|---|---|---|---|
| Adult (vs. Pediatric) | 6.206 | 5.816 | 1.07 | 0.287 |
| Effect | Point Estimate | 95% Wald | Confidence Limits | Pr > ChiSq |
|---|---|---|---|---|
| Pediatric (vs. Adult) | 5.413 | 1.559 | 18.793 | 0.008 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
An, J.B.; Kim, J.; Park, S.H.; Yoon, J.; Choo, O.S.; Park, S.-K.; Chang, J. Pediatric Benign Paroxysmal Positional Vertigo: Degree of Nystagmus and Concurrent Dizziness Differs from Adult BPPV. J. Clin. Med. 2024, 13, 1997. https://doi.org/10.3390/jcm13071997
An JB, Kim J, Park SH, Yoon J, Choo OS, Park S-K, Chang J. Pediatric Benign Paroxysmal Positional Vertigo: Degree of Nystagmus and Concurrent Dizziness Differs from Adult BPPV. Journal of Clinical Medicine. 2024; 13(7):1997. https://doi.org/10.3390/jcm13071997
Chicago/Turabian StyleAn, Jun Beom, Jisu Kim, Seok Hyun Park, Joonsung Yoon, Oak Sung Choo, Su-Kyoung Park, and Jiwon Chang. 2024. "Pediatric Benign Paroxysmal Positional Vertigo: Degree of Nystagmus and Concurrent Dizziness Differs from Adult BPPV" Journal of Clinical Medicine 13, no. 7: 1997. https://doi.org/10.3390/jcm13071997
APA StyleAn, J. B., Kim, J., Park, S. H., Yoon, J., Choo, O. S., Park, S.-K., & Chang, J. (2024). Pediatric Benign Paroxysmal Positional Vertigo: Degree of Nystagmus and Concurrent Dizziness Differs from Adult BPPV. Journal of Clinical Medicine, 13(7), 1997. https://doi.org/10.3390/jcm13071997






