The 10-Year Study of the Impact of Particulate Matters on Mortality in Two Transit Cities in North-Eastern Poland (PL-PARTICLES)
Abstract
:1. Introduction
2. Patients and Methods
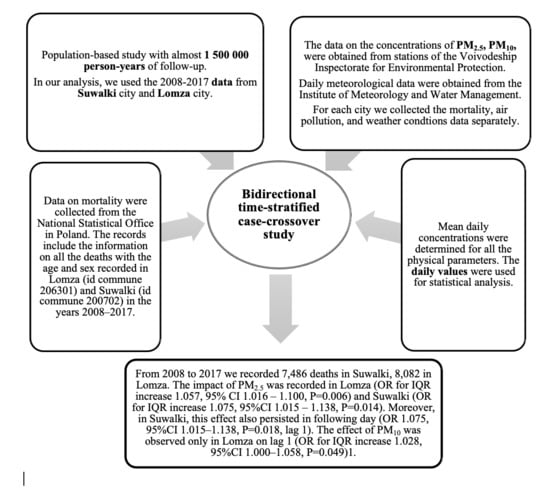
2.1. Study Design
2.2. Region′s Characteristics
2.3. Statistical Analysis
3. Results
4. Discussion
5. Conclusions
6. Limitations
Author Contributions
Funding
Conflicts of Interest
References
- Bae, S.; Kwon, H.J. Current State of Research on the Risk of Morbidity and Mortality Associated with Air Pollution in Korea. Yonsei Med. J. 2019, 60, 243–256. [Google Scholar] [CrossRef] [PubMed]
- Mokoena, K.K.; Ethan, C.J.; Yu, Y.; Shale, K.; Liu, F. Ambient air pollution and respiratory mortality in Xi’an, China: A time-series analysis. Respir. Res. 2019, 20, 139. [Google Scholar] [CrossRef]
- Carugno, M.; Consonni, D.; Randi, G.; Catelan, D.; Grisotto, L.; Bertazzi, P.A.; Biggeri, A.; Baccini, M. Air pollution exposure, cause-specific deaths and hospitalizations in a highly polluted Italian region. Environ. Res. 2016, 147, 415–424. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Sanyal, S.; Rochereau, T.; Maesano, C.N.; Com-Ruelle, L.; Annesi-Maesano, I. Long-Term Effect of Outdoor Air Pollution on Mortality and Morbidity: A 12-Year Follow-Up Study for Metropolitan France. Int. J. Environ. Res. Public Health 2018, 15, 2487. [Google Scholar] [CrossRef] [Green Version]
- Anderson, J.O.; Thundiyil, J.G.; Stolbach, A. Clearing the air: A review of the effects of particulate matter air pollution on human health. J. Med. Toxicol. 2012, 8, 166–175. [Google Scholar] [CrossRef] [Green Version]
- Jiang, X.Q.; Mei, X.D.; Feng, D. Air pollution and chronic airway diseases: What should people know and do? J. Thorac. Dis. 2016, 8, E31–E40. [Google Scholar] [CrossRef]
- Chin, M.T. Basic mechanisms for adverse cardiovascular events associated with air pollution. Heart 2015, 101, 253–256. [Google Scholar] [CrossRef]
- Stanaway, J.D.; Afshin, A.; Gakidou, E.; Lim, S.S.; Abate, D.; Abate, K.H.; Abbafati, C.; Abbasi, N.; Abbastabar, H.; Abd-Allah, F.; et al. Global, regional, and national comparative risk assessment of 84 behavioural, environmental and occupational, and metabolic risks or clusters of risks for 195 countries and territories, 1990-2017: A systematic analysis for the Global Burden of Disease Study 2017. Lancet 2018, 392, 1923–1994. [Google Scholar] [CrossRef] [Green Version]
- Mills, N.L.; Donaldson, K.; Hadoke, P.W.; A Boon, N.; MacNee, W.; Cassee, F.R.; Sandström, T.; Blomberg, A.; E Newby, D. Adverse cardiovascular effects of air pollution. Nat. Clin. Pract. Cardiovasc. Med. 2009, 6, 36–44. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. Revision of the European Standard Population Report of Eurostat’s Task Force. Available online: https://ec.europa.eu/eurostat/documents/3859598/5926869/KS-RA-13-028-EN.PDF/e713fa79-1add-44e8-b23d-5e8fa09b3f8f (accessed on 1 July 2020).
- World Health Organization. Ambient (Outdoor) Air Quality and Health (Updated 2 May 2018). Available online: https://www.who.int/news-room/fact-sheets/detail/ambient-(outdoor)-air-quality-and-health (accessed on 1 July 2020).
- Maclure, M. The case-crossover design: A method for studying transient effects on the risk of acute events. Am. J. Epidemiol. 1991, 133, 144–153. [Google Scholar] [CrossRef]
- Janes, H.; Sheppard, L.; Lumley, T. Case-crossover analyses of air pollution exposure data: Referent selection strategies and their implications for bias. Epidemiology 2005, 16, 717–726. [Google Scholar] [CrossRef] [PubMed]
- Altman, D.G.; Bland, J.M. Statistics Notes Interaction revisited: The difference between two estimates. BMJ 2003, 326, 219. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Von Elm, E.; Altman, D.G.; Egger, M.; Pocock, S.J.; Gøtzsche, P.C.; Vandenbroucke, J.P. The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) statement: Guidelines for reporting observational studies. J. Clin. Epidemiol. 2008, 61, 344–349. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Eurostat: Causes and Occurrence of Deaths in the EU. Available online: https://ec.europa.eu/eurostat/web/products-eurostat-news/-/DDN-20190716-1 (accessed on 5 September 2020).
- Feng, B.; Li, L.; Xu, H. PM 2.5-bound polycyclic aromatic hydrocarbons (PAHs) in Beijing: Seasonal variations, sources, and risk assessment. J. Environ. Sci. 2019, 77, 11–19. [Google Scholar] [CrossRef]
- Al-Naiema, I.M.; Yoon, S.; Wang, Y.Q. Source apportionment of fine particulate matter organic carbon in Shenzhen, China by chemical mass balance and radiocarbon methods. Environ. Pollut. 2018, 240, 34–43. [Google Scholar] [CrossRef] [PubMed]
- Park, C.G.; Cho, H.K.; Shin, H.J. Comparison of Mutagenic Activities of Various Ultra-Fine Particles. Toxicol. Res. 2018, 34, 163–172. [Google Scholar] [CrossRef] [Green Version]
- Cho, H.K.; Park, C.G.; Shin, H.J. Comparison of the in vitro toxicological activity of various particulate matter. Toxicol. Ind. Health 2018, 34, 99–109. [Google Scholar] [CrossRef]
- Campen, M.J.; Lund, A.K.; Doyle-Eisele, M.L. A comparison of vascular effects from complex and individual air pollutants indicates a role for monoxide gases and volatile hydrocarbons. Environ. Health Perspect. 2010, 118, 921–927. [Google Scholar] [CrossRef]
- Yorifuji, T.; Kashima, S.; Doi, H. Fine-particulate Air Pollution from Diesel Emission Control and Mortality Rates in Tokyo: A Quasi-experimental Study. Epidemiology 2016, 27, 769–778. [Google Scholar] [CrossRef]
- Wilker, E.H.; Preis, S.R.; Beiser, A.S. Long-term exposure to fine particulate matter, residential proximity to major roads and measures of brain structure. Stroke 2015, 46, 1161–1166. [Google Scholar] [CrossRef] [Green Version]
- Zeng, W.; Zhang, Y.; Wang, L. Ambient fine particulate pollution and daily morbidity of stroke in Chengdu, China. PLoS ONE 2018, 13, e0206836. [Google Scholar] [CrossRef]
- Zhang, R.; Liu, G.; Jiang, Y. Acute Effects of Particulate Air Pollution on Ischemic Stroke and Hemorrhagic Stroke Mortality. Front. Neurol. 2018, 9, 827. [Google Scholar] [CrossRef] [Green Version]
- Shi, Y.; Matsunaga, T.; Yamaguchi, Y. Long-term trends and spatial patterns of PM 2.5-induced premature mortality in South and Southeast Asia from 1999 to 2014. Sci. Total. Environ. 2018, 631–632, 1504–1514. [Google Scholar] [CrossRef]
- Kowalska, M.; Kocot, K. Short-term exposure to ambient fine particulate matter (PM2.5 and PM10) and the risk of heart rhythm abnormalities and stroke. Postepy Hig. Med. Dosw. 2016, 70, 1017–1025. [Google Scholar] [CrossRef]
- Shah, A.S.; Lee, K.K.; McAllister, D.A. Short term exposure to air pollution and stroke: Systematic review and meta-analysis. BMJ 2015, 350, h1295. [Google Scholar] [CrossRef] [Green Version]
- Li, W.; Cao, Y.; Li, R. The spatial variation in the effects of air pollution on cardiovascular mortality in Beijing, China. J. Expo. Sci. Environ. Epidemiol. 2018, 28, 297–304. [Google Scholar] [CrossRef]
- Pun, V.C.; Kazemiparkouhi, F.; Manjourides, J. Long-Term PM2.5 Exposure and Respiratory, Cancer, and Cardiovascular Mortality in Older US Adults. Am. J. Epidemiol. 2017, 186, 961–969. [Google Scholar] [CrossRef]
- Liu, C.; Chen, R.; Sera, F. Ambient Particulate Air Pollution and Daily Mortality in 652 Cities. N. Engl. J. Med. 2019, 381, 705–715. [Google Scholar] [CrossRef]
- Li, M.H.; Fan, L.C.; Mao, B. Short-term Exposure to Ambient Fine Particulate Matter Increases Hospitalizations and Mortality in COPD: A Systematic Review and Meta-analysis. Chest 2016, 149, 447–458. [Google Scholar] [CrossRef]
- Xing, Y.F.; Xu, Y.H.; Shi, M.H. The impact of PM2.5 on the human respiratory system. J. Thorac. Dis. 2016, 8, E69–E74. [Google Scholar] [CrossRef]
- Wang, L.; Cheng, H.; Wang, D. Airway Microbiome Is Associated with Respiratory Functions and Responses to Ambient Particulate Matter Exposure. Ecotoxicol. Environ. Saf. 2019, 167, 269–277. [Google Scholar] [CrossRef]
- Atkinson, R.W.; Kang, S.; Anderson, H.R. Epidemiological time series studies of PM2.5 and daily mortality and hospital admissions: A systematic review and meta-analysis. Thorax 2014, 69, 660–665. [Google Scholar] [CrossRef] [Green Version]
- Kim, S.Y.; Peel, J.L.; Hannigan, M.P. The temporal lag structure of short-term associations of fine particulate matter chemical constituents and cardiovascular and respiratory hospitalizations. Environ. Health Perspect. 2012, 120, 1094–1099. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Guaita, R.; Pichiule, M.; Maté, T. Short-term impact of particulate matter (PM(2.5)) on respiratory mortality in Madrid. Int. J. Environ. Health Res. 2011, 21, 260–274. [Google Scholar] [CrossRef] [PubMed]
- Meister, K.; Johansson, C.; Forsberg, B. Estimated short-term effects of coarse particles on daily mortality in Stockholm, Sweden. Environ. Health Perspect. 2012, 120, 431–436. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Janssen, N.A.; Fischer, P.; Marra, M. Short-term effects of PM2.5, PM10 and PM2.5-10 on daily mortality in The Netherlands. Sci. Total. Environ. 2013, 463–464, 20–26. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Atkinson, R.W.; Fuller, G.W.; Anderson, H.R. Urban ambient particle metrics and health: A time-series analysis. Epidemiology 2010, 21, 501–511. [Google Scholar] [CrossRef]
- Choi, Y.; Kim, H.; Lee, J.T. Temporal variability of short term effects of PM 10 on mortality in Seoul, Korea. Sci. Total. Environ. 2018, 644, 122–128. [Google Scholar] [CrossRef]
- Renzi, M.; Forastiere, F.; Calzolari, R. Short-term effects of desert and non-desert PM 10 on mortality in Sicily, Italy. Environ. Int. 2018, 120, 472–479. [Google Scholar] [CrossRef]
- Yoo, S.E.; Park, J.S.; Lee, S.H. Comparison of Short-Term Associations between PM 2.5 Components and Mortality across Six Major Cities in South Korea. Int. J. Environ. Res. Public Health 2019, 16, 2872. [Google Scholar] [CrossRef] [Green Version]
- Wang, Y.; Shi, Z.; Shen, F. Associations of daily mortality with short-term exposure to PM2.5 and its constituents in Shanghai, China. Chemosphere 2019, 233, 879–887. [Google Scholar] [CrossRef]
- Liu, M.; Xue, X.; Zhou, B. Population susceptibility differences and effects of air pollution on cardiovascular mortality: Epidemiological evidence from a time-series study. Environ. Sci. Pollut. Res. Int. 2019, 26, 15943–15952. [Google Scholar] [CrossRef] [PubMed]
- Yu, H.; Russell, A.; Mulholland, J. Using cell phone location to assess misclassification errors in air pollution exposure estimation. Environ. Pollut. 2018, 233, 261–266. [Google Scholar] [CrossRef] [PubMed]


| Suwałki | Łomża | p | |
|---|---|---|---|
| Total deaths, N | 7486 | 8082 | |
| Male, % (N) | 54.1 (4055) | 54.5 (4408) | 0.640 |
| Mean age (SD) | 71.7 (16.6) | 72.7 (15.7) | <0.001 |
| CDR (100,000 population/year) | 1079.5 | 1288.1 | <0.001 |
| SDR (100,000 population/year) | 1638.1 | 1944.6 | <0.001 |
| Suwałki | Łomża | p | |
|---|---|---|---|
| All, % (N) | 100 (7486) | 100 (8082) | N/A |
| Cardiovascular deaths, % (N) | 36.4 (2724) | 41.2 (3328) | <0.001 |
| Pulmonary deaths, % (N) | 7.3 (549) | 6.5 (528) | <0.001 |
| Chronic ischemic heart disease, % (N) | 8.5 (633) | 9.1 (733) | 0.176 |
| Cerebral infarction, % (N) | 5.8 (432) | 9.2 (744) | <0.001 |
| Heart disease-unspecified, % (N) | 5.0 (372) | 3.5 (285) | <0.001 |
| Myocardial infarction, % (N) | 3.1 (232) | 3.9 (315) | 0.007 |
| Intracerebral hemorrhage, % (N) | 2.3 (174) | 2.7 (219) | 0.126 |
| Hypertensive heart disease, % (N) | 2.2 (168) | 1.8 (144) | 0.040 |
| Heart failure, % (N) | 1.9 (141) | 3.4 (276) | <0.001 |
| Malignant neoplasm of bronchus and lung, % (N) | 8.0 (597) | 6.4 (518) | <0.001 |
| Instantaneous death, % (N) | 2.6 (196) | 2.8 (225) | 0.524 |
| Chronic obstructive pulmonary disease, % (N) | 2.6 (193) | 3.2 (258) | 0.022 |
| Pneumonia, % (N) | 2.5 (188) | 2.3 (183) | 0.313 |
| Diabetes mellitus, % (N) | 2.1 (160) | 2.6 (206) | 0.090 |
| Malignant neoplasm of breast, % (N) | 2.1 (157) | 1.6 (127) | 0.014 |
| Malignant neoplasm of colon, % (N) | 2.0 (152) | 1.9 (152) | 0.121 |
| Malignant neoplasm of prostate, % (N) | 2.0 (148) | 1.7 (137) | 0.190 |
| Senility, % (N) | 1.9 (139) | 2.2 (176) | 0.155 |
| Suicide, % (N) | 1.8 (132) | 0.8 (62) | <0.001 |
| Atherosclerosis, % (N) | 1.7 (125) | 1.8 (146) | 0.515 |
| Malignant neoplasm of gastric, % (N) | 1.6 (116) | 1.4 (115) | 0.514 |
| Other, % (N) | 40.5 (3031) | 37.9 (3061) | <0.001 |
| Variables | PM2.5 µg/m3 | PM10 µg/m3 | Temp. °C | ||||||
|---|---|---|---|---|---|---|---|---|---|
| Suwałki | Łomża | p | Suwałki | Łomża | p | Suwałki | Łomża | p | |
| Days with observation; N, (%) | 1309 (35.8) | 2230 (61.1) | <0.001 | 3313 (90.7) | 3533 (96.7) | <0.001 | 3653 (100) | 3653 (100) | N/A |
| 2008; mean/day (SD) | N/D | N/D | N/A | 21.5 (11.6) | 31.2 (19.1) | <0.001 | 8.0 (7.2) | 8.5 (7.3) | 0.346 |
| 2009; mean/day (SD) | N/D | N/D | N/A | 23.7 (18.2) | 34.1 (25.1) | <0.001 | 6.9 (8.6) | 7.2 (8.6) | 0.559 |
| 2010; mean/day (SD) | N/D | N/D | N/A | 22.1 (13.3) | 29.9 (19.8) | <0.001 | 6.3 (10.7) | 6.5 (10.5) | 0.754 |
| 2011; mean/day (SD) | N/D | 33.02 (25.6) | N/A | 21.4 (14.2) | 34.0 (23.8) | <0.001 | 7.4 (9.0) | 8.1 (8.9) | 0.346 |
| 2012; mean/day (SD) | N/D | 33.2 (29.4) | N/A | 20.2 (12.8) | 29.9 (20.1) | <0.001 | 6.6 (9.8) | 7.3 (9.9) | 0.350 |
| 2013; mean/day (SD) | N/D | 27.9 (24.7) | N/A | 19.1 (11.2) | 27.1 (15.7) | <0.001 | 7.2 (9.1) | 7.7 (9.0) | 0.535 |
| 2014; mean/day (SD) | 15.1 (8.7) | 28.0 (24.5) | <0.001 | 25.9 (16.8) | 29.4 (18.0) | 0.007 | 7.8 (8.8) | 8.2 (8.7) | 0.551 |
| 2015; mean/day (SD) | 13.2 (10.8) | 26.6 (21.8) | <0.001 | 24.22 (16.72) | 26.1 (15.6) | 0.004 | 8.3 (7.4) | 9.1 (7.7) | 0.218 |
| 2016; mean/day (SD) | 11.6 (8.02) | 25.9 (21.2) | <0.001 | 19.3 (10.0) | 23.6 (14.5) | <0.001 | 7.6 (8.5) | 8.2 (8.4) | 0.272 |
| 2017; mean/day (SD) | 11.4 (8.5) | 25.6 (21.8) | <0.001 | 21.0 (13.2) | 24.8 (16.7) | <0.001 | 7.5 (7.9) | 8.4 (8.1) | 0.108 |
| Total; mean/day (SD) | 12.6 (9.2) | 28.4 (24.3) | <0.001 | 21.7 (14.0) | 29.0 (19.4) | <0.001 | 7.4 (8.8) | 7.9 (8.8) | 0.009 |
| 1st quartile | 6.6 | 12.2 | <0.001 | 12.5 | 16.9 | <0.001 | 1.2 | 1.6 | 0.009 |
| Daily median | 9.9 | 20.0 | <0.001 | 18.1 | 24.0 | <0.001 | 7.2 | 7.7 | 0.009 |
| 3rd quartile | 15.5 | 37.4 | <0.001 | 27.0 | 35.0 | <0.001 | 14.6 | 15.3 | 0.009 |
| IQR | 9.0 | 25.2 | <0.001 | 14.5 | 18.0 | <0.001 | 13.4 | 13.7 | 0.009 |
| Exceed daily mean WHO guideline; N (%) | 110 (8.4) | 908 (40.7) | <0.001 | 139 (4.2) | 345 (9.8) | <0.001 | N/A | N/A | N/A |
| PM2.5 µg/m3 | r = 0.518; p < 0.001 | r = −0.608; p < 0.001 |
| r = 0.668; p < 0.001 | PM10 µg/m3 | r = −0.303; p < 0.001 |
| r = −0.268; p < 0.001 | r = −0.243; p < 0.001 | Temperature °C |
| Variables | Suwałki | Łomża | Ratio of Odds Ratio | |||||
|---|---|---|---|---|---|---|---|---|
| OR (95% CI) | p | OR (95% CI) | p | ROR (95% CI) | p | |||
| Total mortality | LAG 0 | PM2.5 | 1.044 (1.001–1.089) | 0.04 | 1.061 (1.017–1.105) | 0.006 | 0.984 (0.972–1.044) | 0.29 |
| PM10 | 1.024 (0.995–1.054) | 0.10 | 1.018 (0.991–1.047) | 0.21 | 1.005 (0.966–1.047) | 0.38 | ||
| LAG 1 | PM2.5 | 1.027 (0.981–1.075) | 0.27 | 1.029 (0.988–1.071) | 0.17 | 0.998 (0.339–1.061) | 0.48 | |
| PM10 | 1.006 (0.978–1.036) | 0.66 | 1.028 (1.000–1.058) | 0.049 | 0.977 (0.939–1.017) | 0.14 | ||
| LAG 2 | PM2.5 | 1.005 (0.961–1.052) | 0.83 | 1.036 (0.995–1.078) | 0.82 | 0.971 (0.913–1.032) | 0.17 | |
| PM10 | 1.034 (1.005–1.064) | 0.02 | 1.030 (1.001–1.060) | 0.04 | 1.004 (0.965–1.045) | 0.43 | ||
| Cardiovascular mortality | LAG 0 | PM2.5 | 1.085 (1.005–1.171) | 0.04 | 1.086 (1.020–1.156) | 0.01 | 0.999 (0.905–1.103) | 0.50 |
| PM10 | 1.056 (1.006–1.107) | 0.03 | 1.022 (0.979–1.067) | 0.33 | 1.033 (0.972–1.098) | 0.15 | ||
| LAG 1 | PM2.5 | 1.034 (0.957–1.116) | 0.39 | 1.029 (0.967–1.095) | 0.37 | 1.005 (0.910–1.109) | 0.46 | |
| PM10 | 1.004 (0.957–1.054) | 0.86 | 1.034 (0.991–1.080) | 0.13 | 0.971 (0.909–1.036) | 0.19 | ||
| LAG 2 | PM2.5 | 1.014 (0.939–1.094) | 0.73 | 0.992 (0.932–1.056) | 0.80 | 0.981 (0.898–1.071) | 0.33 | |
| PM10 | 1.025 (0.977–1.076) | 0.31 | 1.008 (0.965–1.053) | 0.72 | 1.017 (0.952–1.085) | 0.31 | ||
| Pulmonary mortality | LAG 0 | PM2.5 | 1.161 (0.987–1.365) | 0.072 | 1.130 (0.967–1.320) | 0.12 | 1.027 (0.821–1.286) | 0.41 |
| PM10 | 1.023 (0.916–1.141) | 0.68 | 1.011 (0.906–1.128) | 0.87 | 1.012 (0.866–1.181) | 0.44 | ||
| LAG 1 | PM2.5 | 1.040 (0.885–1.221) | 0.64 | 1.163 (1.021–1.380) | 0.03 | 0.894 (0.717–1.115) | 0.16 | |
| PM10 | 0.979 (0.879–1.091) | 0.69 | 1.013 (0.904–1.135) | 0.82 | 0.966 (0.826–1.131) | 0.33 | ||
| LAG 2 | PM2.5 | 0.898 (0.759–1.062) | 0.21 | 1.073 (0.921–1.251) | 0.37 | 0.837 (0.667–1.050) | 0.06 | |
| PM10 | 0.951 (0.850–1.064) | 0.38 | 1.044 (0.933–1.168) | 0.45 | 0.911 (0.779–1.064) | 0.12 | ||
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Kuźma, Ł.; Dąbrowski, E.J.; Kurasz, A.; Bachórzewska-Gajewska, H.; Dobrzycki, S. The 10-Year Study of the Impact of Particulate Matters on Mortality in Two Transit Cities in North-Eastern Poland (PL-PARTICLES). J. Clin. Med. 2020, 9, 3445. https://doi.org/10.3390/jcm9113445
Kuźma Ł, Dąbrowski EJ, Kurasz A, Bachórzewska-Gajewska H, Dobrzycki S. The 10-Year Study of the Impact of Particulate Matters on Mortality in Two Transit Cities in North-Eastern Poland (PL-PARTICLES). Journal of Clinical Medicine. 2020; 9(11):3445. https://doi.org/10.3390/jcm9113445
Chicago/Turabian StyleKuźma, Łukasz, Emil Julian Dąbrowski, Anna Kurasz, Hanna Bachórzewska-Gajewska, and Sławomir Dobrzycki. 2020. "The 10-Year Study of the Impact of Particulate Matters on Mortality in Two Transit Cities in North-Eastern Poland (PL-PARTICLES)" Journal of Clinical Medicine 9, no. 11: 3445. https://doi.org/10.3390/jcm9113445