Antibiotics 2021, 10(8), 936; https://doi.org/10.3390/antibiotics10080936 - 3 Aug 2021
Cited by 7 | Viewed by 4000
Abstract
Pseudomonas infection is a major determinant of morbidity and mortality in cystic fibrosis (CF). Maintaining optimal lung function in CF patients carrying Pseudomonas remains a challenge. Our study aims to investigate the efficacy of antipseudomonal inhaled antibiotics in CF patients with chronic Pseudomonas
[...] Read more.
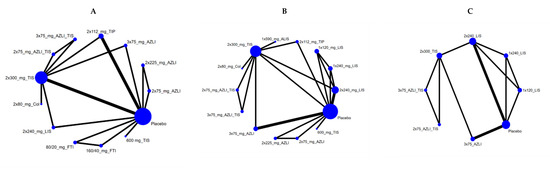
Pseudomonas infection is a major determinant of morbidity and mortality in cystic fibrosis (CF). Maintaining optimal lung function in CF patients carrying Pseudomonas remains a challenge. Our study aims to investigate the efficacy of antipseudomonal inhaled antibiotics in CF patients with chronic Pseudomonas infection. A Bayesian network meta-analysis of randomized controlled trials was conducted. The main outcomes were changes in: (a) forced respiratory volume (FEV1), (b) Pseudomonas aeruginosa sputum density, and (c) CF Questionnaire Revised Respiratory Symptom Score (CFQR-RSS) at 4 weeks follow-up. Eighteen trials which reported on treatment with aztreonam lysine, tobramycin, colistin, levofloxacin, fosfomycin/tobramycin, and amikacin in various dosages were eligible for inclusion. In terms of change in FEV1%, aztreonam lysine (t.i.d., 75 mg) with a 28-day run in the tobramycin phase, aztreonam lysine (b.i.d., 75 mg) with a 28-day run in the tobramycin phase had the highest probability of being the most effective treatment (SUCRAs were 77, 76%, respectively). Regarding change in Pseudomonas sputum density, aztreonam lysine (b.i.d., 75 mg) with a 28-day run in the tobramycin phase, aztreonam lysine (t.i.d., 75 mg) with a 28-day run in the tobramycin phase had the highest probability of being the most effective treatment (SUCRAs were 90, 86%, respectively). Regarding change in CFQR-RSS, aztreonam lysine (t.i.d., 75 mg) and aztreonam lysine (b.i.d., 75 mg) with a 28-day run in the tobramycin inhalation solution phase had the highest probability of being the most effective treatments (SUCRA:74% and 72%, respectively). Regarding changes in FEV1% and Pseudomonas sputum density, aztreonam lysine with a run in tobramycin phase may be the best treatment option in treating chronic Pseudomonas in CF. According to CFQR-RSS no significant differences were found. Given the limitations of the studies included, validation trials are called for.
Full article
(This article belongs to the Special Issue Antibiotic Usage in Acute Situations)
►
Show Figures