Podoplanin Expression Independently and Jointly with Oral Epithelial Dysplasia Grade Acts as a Potential Biomarker of Malignant Transformation in Oral Leukoplakia
Abstract
:1. Introduction
2. Materials and Methods
2.1. Population
2.2. Immunohistochemistry
2.3. Evaluation of Immunohistochemical Expression
2.4. Statistical Analysis
3. Results
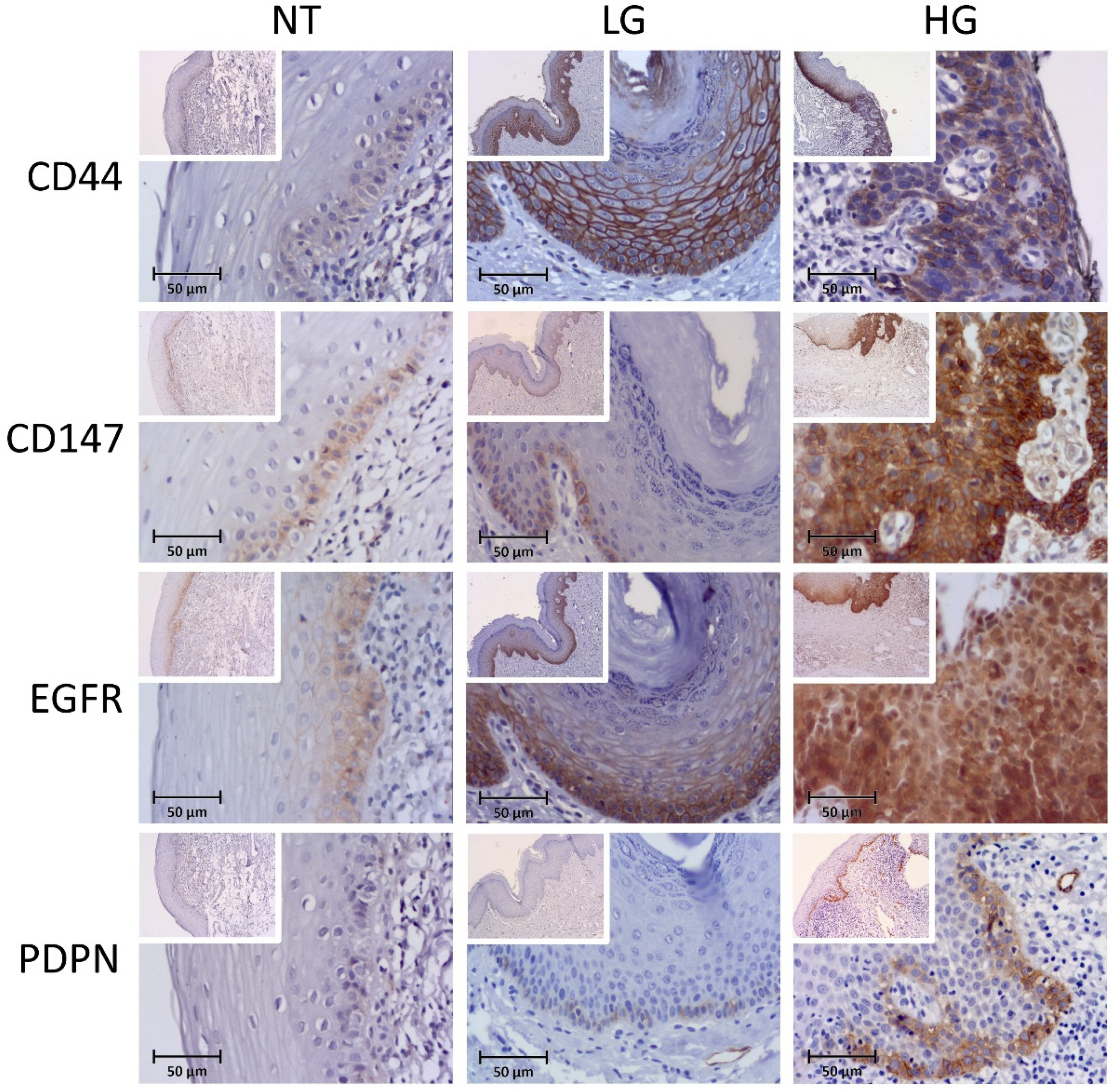
3.1. Protein Analysis
3.1.1. CD44v6
3.1.2. CD147
3.1.3. EGFR
3.1.4. Podoplanin
3.1.5. P53
3.1.6. P63
3.1.7. P73
3.1.8. P16
3.2. Correlation between Markers
3.3. Analysis of Oral Malignant Transformation Free Survival
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Warnakulasuriya, S.; Kujan, O.; Aguirre-Urizar, J.M.; Bagan, J.V.; González-Moles, M.Á.; Kerr, A.R.; Lodi, G.; Mello, F.W.; Monteiro, L.; Ogden, G.R.; et al. Oral potentially malignant disorders: A consensus report from an international seminar on nomenclature and classification, convened by the WHO Collaborating Centre for Oral Cancer. Oral Dis. 2020, 27, 1862–1880. [Google Scholar] [CrossRef] [PubMed]
- Warnakulasuriya, S.; Johnson, N.W.; Van Der Waal, I. Nomenclature and Classification of Potentially Malignant Disorders of the Oral Mucosa. J. Oral Pathol. Med. 2007, 36, 575–580. [Google Scholar] [CrossRef] [PubMed]
- Mello, F.W.; Miguel, A.F.P.; Dutra, K.L.; Porporatti, A.L.; Warnakulasuriya, S.; Guerra, E.N.S.; Rivero, E.R.C. Prevalence of Oral Potentially Malignant Disorders: A Systematic Review and Meta-Analysis. J. Oral Pathol. Med. 2018, 47, 633–640. [Google Scholar] [CrossRef]
- Petti, S. Pooled Estimate of World Leukoplakia Prevalence: A Systematic Review. Oral Oncol. 2003, 39, 770–780. [Google Scholar] [CrossRef]
- Aguirre-Urizar, J.M.; de Mendoza, I.L.-I.; Warnakulasuriya, S. Malignant Transformation of Oral Leukoplakia: Systematic Review and Meta-Analysis of the Last 5 Years. Oral Dis. 2021, 27, 1881–1895. [Google Scholar] [CrossRef] [PubMed]
- Mehanna, H.M.; Rattay, T.; Smith, J.; McConkey, C.C. Treatment and Follow-up of Oral Dysplasia—A Systematic Review and Meta-Analysis. Head Neck 2009, 31, 1600–1609. [Google Scholar] [CrossRef] [PubMed]
- Warnakulasuriya, S.; Ariyawardana, A. Malignant Transformation of Oral Leukoplakia: A Systematic Review of Observational Studies. J. Oral Pathol. Med. 2016, 45, 155–166. [Google Scholar] [CrossRef]
- Speight, P.M.; Khurram, S.A.; Kujan, O. Oral Potentially Malignant Disorders: Risk of Progression to Malignancy. Oral Surg. Oral Med. Oral Pathol. Oral Radiol. 2018, 125, 612–627. [Google Scholar] [CrossRef] [Green Version]
- Warnakulasuriya, K.; Kovacevic, T.; Madden, P.; Coupland, V.H.; Sperandio, M.; Odell, E.; Moller, H. Factors Predicting Malignant Transformation in Oral Potentially Malignant Disorders among Patients Accrued over a 10-Year Period in South East England. J. Oral Pathol. Med. 2011, 40, 677–683. [Google Scholar] [CrossRef]
- Chaturvedi, A.K.; Udaltsova, N.; Engels, E.A.; Katzel, J.A.; Yanik, E.L.; Katki, H.A.; Lingen, M.W.; Silverberg, M.J. Oral Leukoplakia and Risk of Progression to Oral Cancer: A Population-Based Cohort Study. JNCI J. Natl. Cancer Inst. 2020, 112, 1047–1054. [Google Scholar] [CrossRef] [Green Version]
- Kujan, O.; Khattab, A.; Oliver, R.J.; Roberts, S.A.; Thakker, N.; Sloan, P. Why Oral Histopathology Suffers Inter-Observer Variability on Grading Oral Epithelial Dysplasia: An Attempt to Understand the Sources of Variation. Oral Oncol. 2007, 43, 224–231. [Google Scholar] [CrossRef] [PubMed]
- Speight, P.M.; Abram, T.J.; Floriano, P.N.; James, R.; Vick, J.; Thornhill, M.H.; Murdoch, C.; Freeman, C.; Hegarty, A.M.; D’Apice, K.; et al. Interobserver Agreement in Dysplasia Grading: Toward an Enhanced Gold Standard for Clinical Pathology Trials. Oral Surg. Oral Med. Oral Pathol. Oral Radiol. 2015, 120, 474–482.e2. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Hanahan, D.; Weinberg, R.A. Hallmarks of Cancer: The Next Generation. Cell 2011, 144, 646–674. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Chai, A.W.Y.; Lim, K.P.; Cheong, S.C. Translational Genomics and Recent Advances in Oral Squamous Cell Carcinoma. Semin. Cancer Biol. 2020, 61, 71–83. [Google Scholar] [CrossRef]
- Califano, J.; Van Der Riet, P.; Westra, W.; Nawroz, H.; Clayman, G.; Piantadosi, S.; Corio, R.; Lee, D.; Greenberg, B.; Koch, W.; et al. Genetic Progression Model for Head and Neck Cancer: Implications for Field Cancerization. Cancer Res. 1996, 56, 2488–2492. [Google Scholar] [CrossRef]
- Mithani, S.; Mydlarz, W.; Grumbine, F.; Smith, I.; Califano, J. Molecular Genetics of Premalignant Oral Lesions. Oral Dis. 2007, 13, 126–133. [Google Scholar] [CrossRef]
- Nikitakis, N.G.; Pentenero, M.; Georgaki, M.; Poh, C.F.; Peterson, D.E.; Edwards, P.; Lingen, M.; Sauk, J.J.; Nikitakis, N.G.; Pentenero, M.; et al. Molecular Markers Associated with Development and Progression of Potentially Premalignant Oral Epithelial Lesions: Current Knowledge and Future Implications. Oral Surg. Oral Med. Oral Pathol. Oral Radiol. 2018, 125, 650–669. [Google Scholar] [CrossRef] [Green Version]
- Monteiro, L.; Warnakulasuriya, S. Molecular and Signaling Pathways During Oral Carcinogenesis. In Textbook of Oral Cancer: Prevention, Diagnosis and Management; Warnakulasuriya, S., Greenspan, J.S., Eds.; Springer International Publishing: Cham, Switzerland, 2020; pp. 179–194. [Google Scholar]
- Dionne, K.R.; Warnakulasuriya, S.; Zain, R.B.; Cheong, S.C. Potentially Malignant Disorders of the Oral Cavity: Current Practice and Future Directions in the Clinic and Laboratory. Int. J. Cancer 2014, 136, 503–515. [Google Scholar] [CrossRef]
- Lingen, M.; Pinto, A.; Mendes, R.A.; Franchini, R.; Czerninski, R.; Tilakaratne, W.; Woo, S.-B.; Partridge, M.; Peterson, D. Genetics/Epigenetics of Oral Premalignancy: Current Status and Future Research. Oral Dis. 2011, 17, 7–22. [Google Scholar] [CrossRef]
- Monteiro, L.; Mello, F.W.; Warnakulasuriya, S. Tissue Biomarkers for Predicting the Risk of Oral Cancer in Patients Diagnosed with Oral Leukoplakia: A Systematic Review. Oral Dis. 2020, 27, 1977–1992. [Google Scholar] [CrossRef]
- Monteiro, L.S.; Diniz-Freitas, M.; Warnakulasuriya, S.; Garcia-Caballero, T.; Forteza, J.; Fraga, M. An Immunohistochemical Score to Predict the Outcome for Oral Squamous Cell Carcinoma. J. Oral Pathol. Med. 2018, 47, 375–381. [Google Scholar] [CrossRef] [PubMed]
- Monteiro, L.S.; Delgado, M.L.; Ricardo, S.; Amaral, J.; Salazar, F.; Pacheco, J.; Lopes, C.; Bousbaa, H.; Warnakulasuryia, S. Prognostic Significance of Cd44v6, P63, Podoplanin and Mmp-9 in Oral Squamous Cell Carcinomas. Oral Dis. 2016, 22, 303–312. [Google Scholar] [CrossRef] [PubMed]
- Monteiro, L.S.; Delgado, M.L.; Ricardo, S.; Garcez, F.; Amaral, J.; Pacheco, J.; Lopes, C.; Bousbaa, H. EMMPRIN Expression in Oral Squamous Cell Carcinomas: Correlation with Tumor Proliferation and Patient Survival. BioMed Res. Int. 2014, 2014, 905680. [Google Scholar] [CrossRef]
- Kuo, W.P.; Jenssen, T.-K.; Park, P.J.; Lingen, M.W.; Hasina, R.; Ohno-Machado, L. Gene Expression Levels in Different Stages of Progression in Oral Squamous Cell Carcinoma. Proc. AMIA Symp. 2002, 415–419. [Google Scholar]
- Abram, T.J.; Floriano, P.N.; Christodoulides, N.; James, R.; Kerr, A.R.; Thornhill, M.H.; Redding, S.W.; Vigneswaran, N.; Speight, P.M.; Vick, J.; et al. ‘Cytology-on-a-Chip’ Based Sensors for Monitoring of Potentially Malignant Oral Lesions. Oral Oncol. 2016, 60, 103–111. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Villa, A.; Hanna, G.J.; Kacew, A.; Frustino, J.; Hammerman, P.S.; Woo, S. Oral Keratosis of Unknown Significance Shares Genomic Overlap with Oral Dysplasia. Oral Dis. 2019, 25, 1707–1714. [Google Scholar] [CrossRef]
- Woo, S.-B.; Grammer, R.L.; Lerman, M.A. Keratosis of Unknown Significance and Leukoplakia: A Preliminary Study. Oral Surg. Oral Med. Oral Pathol. Oral Radiol. 2014, 118, 713–724. [Google Scholar] [CrossRef]
- Kujan, O.; Oliver, R.J.; Khattab, A.; Roberts, S.A.; Thakker, N.; Sloan, P. Evaluation of a New Binary System of Grading Oral Epithelial Dysplasia for Prediction of Malignant Transformation. Oral Oncol. 2006, 42, 987–993. [Google Scholar] [CrossRef]
- Monteiro, L.; Silva, P.; Delgado, L.; Amaral, B.; Garcês, F.; Salazar, F.; Pacheco, J.J.; Lopes, C.; Bousbaa, H.; Warnakulasuriya, S. Expression of Spindle Assembly Checkpoint Proteins Bubr1 and Mad2 Expression as Potential Biomarkers of Malignant Transformation of Oral Leukoplakia: An Observational Cohort Study. Med. Oral Patol. Oral Cir. Bucal. 2021, 26, e719–e728. [Google Scholar] [CrossRef]
- Kawaguchi, H.; El-Naggar, A.K.; Papadimitrakopoulou, V.; Ren, H.; Fan, Y.-H.; Feng, L.; Lee, J.J.; Kim, E.; Hong, W.K.; Lippman, S.M.; et al. Podoplanin: A Novel Marker for Oral Cancer Risk in Patients with Oral Premalignancy. J. Clin. Oncol. 2008, 26, 354–360. [Google Scholar] [CrossRef]
- Lydiatt, W.M.; Patel, S.G.; O’Sullivan, B.; Brandwein, M.S.; Ridge, J.A.; Migliacci, J.C.; Loomis, A.M.; Shah, J.P. Head and Neck Cancers-Major Changes in the American Joint Committee on Cancer Eighth Edition Cancer Staging Manual. CA Cancer J. Clin. 2017, 67, 122–137. [Google Scholar] [CrossRef] [PubMed]
- Villa, A.; Celentano, A.; Glurich, I.; Wenche, S.; Borgnakke, S.B.J.; Peterson, D.E.; Delli, K.; Ojeda, D.; Vissink, A.; Farah, C.S. World Workshop on Oral Medicine Vii: Prognostic Biomarkers in Oral Leukoplakia: A Systematic Review of Longitudinal Studies. Oral Dis. 2019, 25, 64–78. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Mello, F.W.; Melo, G.; Guerra, E.N.S.; Warnakulasuriya, S.; Garnis, C.; Rivero, E.R.C. Oral Potentially Malignant Disorders: A Scoping Review of Prognostic Biomarkers. Crit. Rev. Oncol. 2020, 153, 102986. [Google Scholar] [CrossRef] [PubMed]
- Celentano, A.; Glurich, I.; Borgnakke, W.S.; Farah, C.S. World Workshop on Oral Medicine Vii: Prognostic Biomarkers in Oral Leukoplakia and Proliferative Verrucous Leukoplakia-a Systematic Review of Retrospective Studies. Oral Dis. 2021, 27, 848–880. [Google Scholar] [CrossRef] [PubMed]
- Kuo, M.Y.-P.; Cheng, S.-J.; Chen, H.-M.; Kok, S.-H.; Hahn, L.-J.; Chiang, C.-P. Expression of Cd44s, Cd44v5, Cd44v6 and Cd44v7-8 in Betel Quid Chewing-Associated Oral Premalignant Lesions and Squamous Cell Carcinomas in Taiwan. J. Oral Pathol. Med. 2007, 27, 428–433. [Google Scholar] [CrossRef] [PubMed]
- Surendran, S.; Siddappa, G.; Mohan, A.; Hicks, W.; Jayaprakash, V.; Mimikos, C.; Mahri, M.; Almarzouki, F.; Morrell, K.; Ravi, R.; et al. Cancer Stem Cell and Its Niche in Malignant Progression of Oral Potentially Malignant Disorders. Oral Oncol. 2017, 75, 140–147. [Google Scholar] [CrossRef] [Green Version]
- González-Moles, M.Á.; González-Ruiz, L.; Ramos-García, P. Cancer Stem Cells in Oral Carcinoma. In Textbook of Oral Cancer: Prevention, Diagnosis and Management; Warnakulasuriya, S., Greenspan, J.S., Eds.; Springer International Publishing: Cham, Switzerland, 2020; pp. 427–437. [Google Scholar]
- Rautava, J.; Soukka, T.; Inki, P.; Leimola-Virtanen, R.; Saloniemi, I.; Happonen, R.-P.; Heikinheimo, K. Cd44v6 in Developing, Dysplastic and Malignant Oral Epithelia. Oral Oncol. 2003, 39, 373–379. [Google Scholar] [CrossRef]
- Godge, P.; Poonja, L.; Py, G.; Ls, P. Quantitative Assessment of Expression of Cell Adhesion Molecule (Cd44) Splice Variants: Cd44 Standard (Cd44s) and V5, V6 Isoforms in Oral Leukoplakias: An Immunohistochemical Study. Indian J. Dent. Res. 2011, 22, 493–494. [Google Scholar] [CrossRef]
- Kahn, H.J.; Marks, A. A New Monoclonal Antibody, D2-40, for Detection of Lymphatic Invasion in Primary Tumors. Lab. Investig. 2002, 82, 1255–1257. [Google Scholar] [CrossRef] [Green Version]
- Atsumi, N.; Ishii, G.; Kojima, M.; Sanada, M.; Fujii, S.; Ochiai, A. Podoplanin, a Novel Marker of Tumor-Initiating Cells in Human Squamous Cell Carcinoma A431. Biochem. Biophys. Res. Commun. 2008, 373, 36–41. [Google Scholar] [CrossRef]
- De Vicente, J.C.; Rodrigo, J.P.; Rodriguez-Santamarta, T.; Lequerica-Fernández, P.; Allonca, E.; García-Pedrero, J.M. Podoplanin Expression in Oral Leukoplakia: Tumorigenic Role. Oral Oncol. 2013, 49, 598–603. [Google Scholar] [CrossRef] [PubMed]
- Saluja, T.S.; Ali, M.; Mishra, P.; Kumar, V.; Singh, S.K. Prognostic Value of Cancer Stem Cell Markers in Potentially Malignant Disorders of Oral Mucosa: A Meta-analysis. Cancer Epidemiol. Biomark. Prev. 2018, 28, 144–153. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Deppa, A.; Janardanan-Nair, B.; Varun, B. Podoplanin Expression in Oral Potentially Malignant Disorders and Oral Squamous Cell Carcinoma. J. Clin. Exp. Dent. 2017, 9, e1418–e1424. [Google Scholar]
- Aiswarya, A.; Suresh, R.; Janardhanan, M.; Savithri, V.; Aravind, T.; Mathew, L. An Immunohistochemical Evaluation of Podoplanin Expression in Oral Leukoplakia and Oral Squamous Cell Carcinoma to Explore Its Potential to Be Used as a Predictor for Malignant Transformation. J. Oral Maxillofac. Pathol. 2019, 23, 159. [Google Scholar] [PubMed]
- Gissi, D.B.; Gabusi, A.; Tarsitano, A.; Luccarini, L.; Morandi, L.; Montebugnoli, L. Podoplanin Expression as a Predictive Marker of Dysplasia in Oral Leukoplakia. J. Cranio-Maxillofac. Surg. 2018, 46, 759–764. [Google Scholar] [CrossRef]
- Grochau, K.J.; Safi, A.F.; Drebber, U.; Grandoch, A.; Zöller, J.E.; Kreppel, M. Podoplanin Expression in Oral Leukoplakia—A Prospective Study. J. Craniomaxillofac. Surg. 2019, 47, 505–509. [Google Scholar] [CrossRef]
- Patil, A.; Patil, K.; Tupsakhare, S.; Gabhane, M.; Sonune, S.; Kandalgaonkar, S. Evaluation of Podoplanin in Oral Leukoplakia and Oral Squamous Cell Carcinoma. Scientifica 2015, 2015, 135298. [Google Scholar] [CrossRef] [Green Version]
- Habiba, U.; Hida, K.; Kitamura, T.; Matsuda, A.Y.; Higashino, F.; Ito, Y.M.; Ohiro, Y.; Totsuka, Y.; Shindoh, M. Aldh1 and Podoplanin Expression Patterns Predict the Risk of Malignant Transformation in Oral Leukoplakia. Oncol. Lett. 2017, 13, 321–328. [Google Scholar] [CrossRef] [Green Version]
- Kreppel, M.; Kreppel, B.; Drebber, U.; Wedemayer, I.; Rothamel, D.; Zöller, J.E.; Scheer, M. Podoplanin Expression in Oral Leukoplakia: Prognostic Value and Clinicopathological Implications. Oral Dis. 2012, 18, 692–699. [Google Scholar] [CrossRef]
- Liu, W.; Zhou, Z.; Yang, X.; Shi, H. Whether Cancer Stem Cell Markers Can Serve as the Markers for Malignant Progression of Oral Potentially Malignant Disorders. Oral Dis. 2021; in press. [Google Scholar] [CrossRef]
- Kumar, M.; Suwasini, S.; Chatterjee, K.; Purkait, S.K.; Samaddar, D.; Chatterjee, A. Expression of P53 Protein and Ki-67 Antigen in Oral Leukoplakia with Different Histopathological Grades of Epithelial Dysplasia. J. Int. Soc. Prev. Community Dent. 2018, 8, 513–522. [Google Scholar] [CrossRef] [PubMed]
- Bascones-Martínez, A.; López-Durán, M.; Cano-Sánchez, J.; Sánchez-Verde, L.; Díez-Rodríguez, A.; Aguirre-Echebarría, P.; Álvarez-Fernández, E.; González-Moles, M.A.; Bascones-Ilundain, J.; Muzio, L.L.; et al. Differences in the Expression of Five Senescence Markers in Oral Cancer, Oral Leukoplakia and Control Samples in Humans. Oncol. Lett. 2012, 3, 1319–1325. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Boaz, K.; Pandya, J.A.; Natarajan, S.; Manaktala, N.; Nandita, K.; Lewis, A.J. A Correlation of Immunohistochemical Expression of Tp53 and Cdkn1a in Oral Epithelial Dysplasia and Oral Squamous Cell Carcinoma. J. Cancer Res. Ther. 2018, 14, 666–670. [Google Scholar] [CrossRef] [PubMed]
- Ramos-García, P.; González-Moles, M.Á.; Warnakulasuriya, S. Significance of P53 Overexpression in the Prediction of the Malignant Transformation Risk of Oral Potentially Malignant Disorders: A Systematic Review and Meta-Analysis. Oral Oncol. 2022, 126, 105734. [Google Scholar] [CrossRef]
- Sundberg, J.; Pandey, S.; Giglio, D.; Holmberg, E.; Kjeller, G.; Kovács, A.; Sand, L.P.; Tokozlu, B.; Öhman, J.; Sapkota, D.; et al. Expression of P53, P63, Podoplanin and Ki-67 in Recurring Versus Non-Recurring Oral Leukoplakia. Sci. Rep. 2021, 11, 1–12. [Google Scholar]
- El-Naggar, A.K.; Lai, S.; Clayman, G.L.; Mims, B.; Lippman, S.M.; Coombes, M.; Luna, M.A.; Lozano, G. P73 Gene Alterations and Expression in Primary Oral and Laryngeal Squamous Carcinomas. Carcinogenesis 2001, 22, 729–735. [Google Scholar] [CrossRef] [Green Version]
- Inoue, H.; Miyazaki, Y.; Kikuchi, K.; Yoshida, N.; Ide, F.; Ohmori, Y.; Tomomura, A.; Sakashita, H.; Kusama, K. Podoplanin Promotes Cell Migration Via the Egf-Src-Cas Pathway in Oral Squamous Cell Carcinoma Cell Lines. J. Oral Sci. 2012, 54, 241–250. [Google Scholar] [CrossRef] [Green Version]
- Mello, F.W.; Kammer, P.V.; Silva, C.A.B.; Parkinson, E.K.; Monteiro, L.D.S.; Warnakulasuriya, S.; Rivero, E.R.C. Prognostic and Clinicopathological Significance of Podoplanin Immunoexpression in Oral and Oropharyngeal Squamous Cell Carcinoma: A Systematic Review. J. Oral Pathol. Med. 2021, 50, 1–9. [Google Scholar] [CrossRef]
- Reed, A.L.; Califano, J.; Cairns, P.; Westra, W.H.; Jones, R.M.; Koch, W.; Ahrendt, S.; Eby, Y.; Sewell, D.; Nawroz, H.; et al. High Frequency of P16 (Cdkn2/Mts-1/Ink4a) Inactivation in Head and Neck Squamous Cell Carcinoma. Cancer Res. 1996, 56, 3630–3633. [Google Scholar]
- Rosin, M.P.; Cheng, X.; Poh, C.; Lam, W.L.; Huang, Y.; Lovas, J.; Berean, K.; Epstein, J.B.; Priddy, R.; Le, N.D.; et al. Use of Allelic Loss to Predict Malignant Risk for Low-Grade Oral Epithelial Dysplasia. Clin. Cancer Res. 2000, 6, 357–362. [Google Scholar]
- Saintigny, P.; El-Naggar, A.K.; Papadimitrakopoulou, V.; Ren, H.; Fan, Y.-H.; Feng, L.; Lee, J.J.; Kim, E.S.; Hong, W.K.; Lippman, S.M.; et al. Deltanp63 Overexpression, Alone and in Combination with Other Biomarkers, Predicts the Development of Oral Cancer in Patients with Leukoplakia. Clin. Cancer Res. 2009, 15, 6284–6291. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Benchekroun, M.T.; Saintigny, P.; Thomas, S.; El-Naggar, A.K.; Papadimitrakopoulou, V.; Ren, H.; Lang, W.; Fan, Y.-H.; Huang, J.; Feng, L.; et al. Epidermal Growth Factor Receptor Expression and Gene Copy Number in the Risk of Oral Cancer. Cancer Prev. Res. 2010, 3, 800–809. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Wu, W.; Wang, Z.; Zhou, Z. Role of the Human Papillomavirus in Malignant Transformation of Oral Leukoplakia Distinct from Oropharyngeal Squamous Cell Carcinoma: A Study of 76 Patients with Internal-Control Specimens. Oral Surg. Oral Med. Oral Pathol. Oral Radiol. 2019, 128, 273–279. [Google Scholar] [CrossRef]
- Zhang, X.; Kim, K.-Y.; Zheng, Z.; Bazarsad, S.; Kim, J. Nomogram for Risk Prediction of Malignant Transformation in Oral Leukoplakia Patients Using Combined Biomarkers. Oral Oncol. 2017, 72, 132–139. [Google Scholar] [CrossRef] [PubMed]
- D’Souza, B.; Nayak, R.; Kotrashetti, V.S. Immunohistochemical Expression of Podoplanin in Clinical Variants of Oral Leukoplakia and Its Correlation With Epithelial Dysplasia. Appl. Immunohistochem. Mol. Morphol. 2018, 26, 132–139. [Google Scholar] [CrossRef]
- Cousins, M.; Carney, K. Can tissue biomarkers be used to determine the prognosis of oral leukoplakia lesions with regards to malignant transformation? Evid. Based Dent. 2022, 23, 18–19. [Google Scholar] [CrossRef]
- Georgaki, M.; Avgoustidis, D.; Theofilou, V.; Piperi, E.; Pettas, E.; Kalyvas, D.; Vlachodimitropoulos, D.; Perisanidis, C.; Lazaris, A.; Nikitakis, N. Recurrence in Oral Premalignancy: Clinicopathologic and Immunohistochemical Analysis. Diagnostics 2021, 11, 872. [Google Scholar] [CrossRef]
- Iocca, O.; Sollecito, T.P.; Alawi, F.; Weinstein, G.S.; Newman, J.G.; de Virgilio, A.; di Maio, P.; Spriano, G.; López, S.P.; Shanti, R.M. Potentially Malignant Disorders of the Oral Cavity and Oral Dysplasia: A Systematic Review and Meta-Analysis of Malignant Transformation Rate by Subtype. Head Neck 2020, 42, 539–555. [Google Scholar] [CrossRef]
- Odell, E.; Kujan, O.; Warnakulasuriya, S.; Sloan, P. Oral Epithelial Dysplasia: Recognition, Grading and Clinical Significance. Oral Dis. 2021, 27, 1947–1976. [Google Scholar] [CrossRef]
- Müller, S. Update from the 4th Edition of the World Health Organization of Head and Neck Tumours: Tumours of the Oral Cavity and Mobile Tongue. Head Neck Pathol. 2017, 11, 33–40. [Google Scholar] [CrossRef]
- Reibel, J.; Gale, N.; Hille, J.; Hunt, J.L.; Lingen, M.; Muller, S.; Sloan, P.; Tilakaratne, W.M.; Westra, W.H.; Willams, M.D. Oral Potentially Malignant Disorders and Oral Epithelial Dysplasias. In Who Classification of Tumours of the Head and Neck. Tumours of the Oral Cavity and Mobile Tongue; El-Naggar, A.K., Chan, J.K.C., Gradis, J.R., Takata, T., Slootweg, P.J., Eds.; IARC Press: Lyon, France, 2017. [Google Scholar]
- Krishnan, H.; Rayes, J.; Miyashita, T.; Ishii, G.; Retzbach, E.; Sheehan, S.A.; Takemoto, A.; Chang, Y.-W.; Yoneda, K.; Asai, J.; et al. Podoplanin: An emerging cancer biomarker and therapeutic target. Cancer Sci. 2018, 109, 1292–1299. [Google Scholar] [CrossRef] [PubMed]


| Primary Antibody | Clone | Dilution | Manufacture |
|---|---|---|---|
| anti-CD44v6 | VFF-7 | 1:120 | Leica Biosystems, Newcastle upon Tyne, UK |
| anti-CD147 | AB1843 | 1:30 | Leica Biosystems, Newcastle upon Tyne, UK |
| anti-EGFR | EGFR.25 | 1/100 | Leica Biosystems, Newcastle upon Tyne, UK |
| anti-p53 | NCLp53 DO7 | 1:20 | Leica Biosystems, Newcastle upon Tyne, UK |
| anti-p63 | 7JUL | 1:25 | Leica Biosystems, Newcastle upon Tyne, UK |
| anti-p73 | 24 | 1:25 | Leica Biosystems, Newcastle upon Tyne, UK |
| anti-p16 | OA315 | prediluted | MTM, Heidelberg, Germany |
| anti-podoplanin | D2-40 | 1:150 | Dako, Carpinteria, CA, USA |
| Variable | N | Oral Malignant Transformation | MTFS a | p-Value b | p-Value c | |
|---|---|---|---|---|---|---|
| CD44 | 0, I II, III | 2 45 | 0 6 | 100 80.1 | 0.510 | 0.803 |
| CD147 | 0, I II, III | 20 24 | 1 3 | 94.7 83.3 | 0.586 | 0.779 |
| EGFR | 0, I II, III | 2 43 | 0 5 | 100 82.7 | 0.610 | 0.461 |
| P53 | 0, I II, III | 14 25 | 1 3 | 92.9 82.1 | 0.574 | 0.642 |
| P73 | 0, I II, III | 11 30 | 2 3 | 75.8 37.5 | 0.582 | 0.526 |
| P63 | 0, I II, III | 1 42 | 0 5 | 100 85.2 | 0.745 | 0.478 |
| P16 | 0, I II, III | 32 8 | 3 3 | 88.4 58.3 | 0.081 | 0.126 |
| P16 TMN | 0–74 >75% | 38 2 | 6 0 | 78.3 100 | 0.550 | - |
| Podoplanin | 0, I II, III | 34 5 | 2 4 | 88.7 20 | <0.001 | <0.001 |
| Podoplanin d | 0, I II, III | 22 16 | 1 5 | 85.7 65.5 | 0.044 | 0.058 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Monteiro, L.; do Amaral, B.; Delgado, L.; Garcês, F.; Salazar, F.; Pacheco, J.J.; Lopes, C.; Warnakulasuriya, S. Podoplanin Expression Independently and Jointly with Oral Epithelial Dysplasia Grade Acts as a Potential Biomarker of Malignant Transformation in Oral Leukoplakia. Biomolecules 2022, 12, 606. https://doi.org/10.3390/biom12050606
Monteiro L, do Amaral B, Delgado L, Garcês F, Salazar F, Pacheco JJ, Lopes C, Warnakulasuriya S. Podoplanin Expression Independently and Jointly with Oral Epithelial Dysplasia Grade Acts as a Potential Biomarker of Malignant Transformation in Oral Leukoplakia. Biomolecules. 2022; 12(5):606. https://doi.org/10.3390/biom12050606
Chicago/Turabian StyleMonteiro, Luís, Barbas do Amaral, Leonor Delgado, Fernanda Garcês, Filomena Salazar, José Júlio Pacheco, Carlos Lopes, and Saman Warnakulasuriya. 2022. "Podoplanin Expression Independently and Jointly with Oral Epithelial Dysplasia Grade Acts as a Potential Biomarker of Malignant Transformation in Oral Leukoplakia" Biomolecules 12, no. 5: 606. https://doi.org/10.3390/biom12050606






