Healthcare Service Efficiency: An Empirical Study on Healthcare Capacity in Various Counties and Cities in Taiwan
Abstract
1. Introduction
1.1. Healthcare in Taiwan
1.2. Measuring Healthcare Efficiency
2. Methodology
2.1. Input-Oriented CCR Model
2.2. Input-Oriented BCC Model
3. Data and Empirical Model
3.1. Samples and Data Sources
3.2. Empirical Model
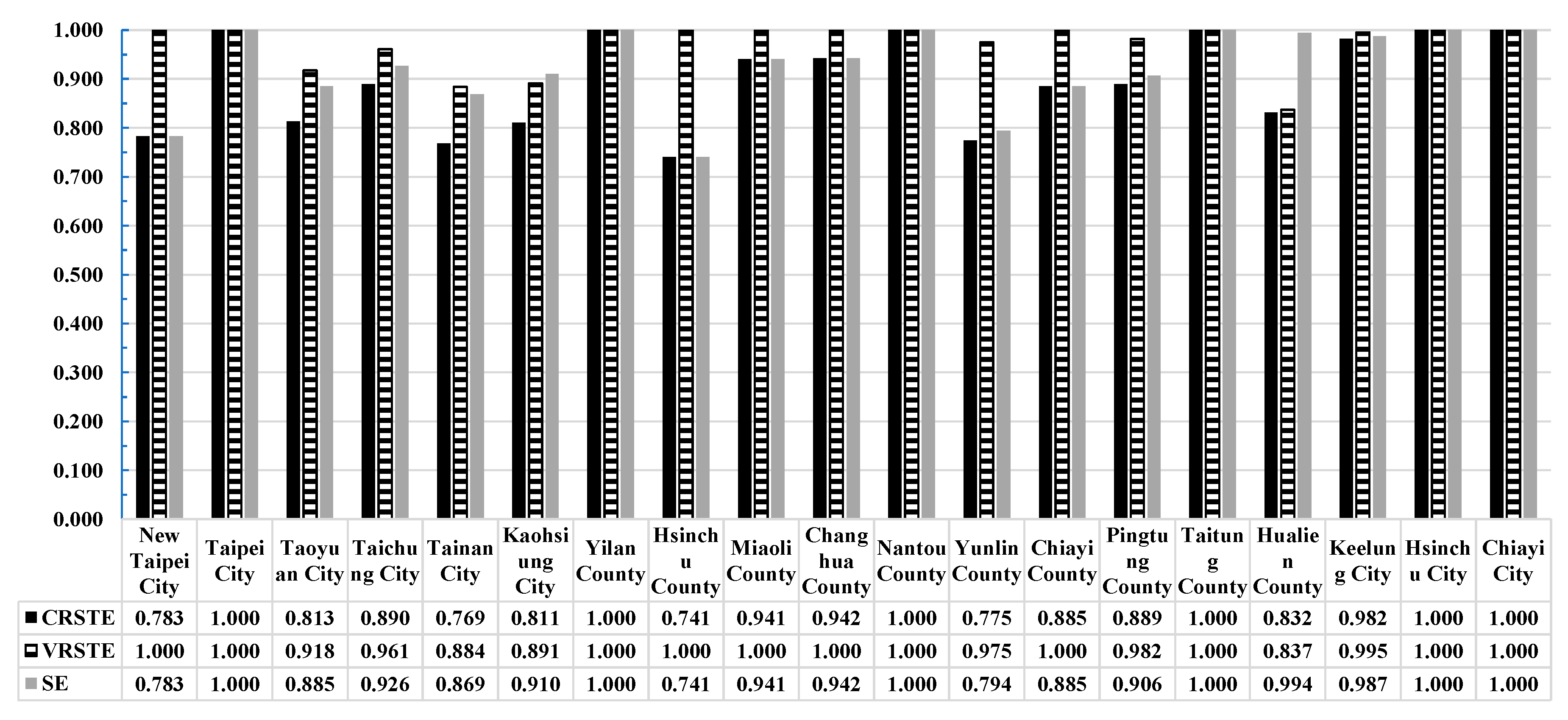
4. Results and Discussion
5. Conclusions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Lee, T.; Propper, C.; Stoye, G. Medical labour supply and the production of healthcare. Fisc. Stud. 2019, 40, 621–661. [Google Scholar] [CrossRef]
- Charlesworth, A.; Firth, Z.; Gerschlick, B.; Watt, T. Future pressures on the NHS and social care. In Securing the Future: Funding Health and Social Care to the 2030s; Charlesworth, A., Johnson, P., Eds.; Institute for Fiscal Studies: London, UK, 2018. [Google Scholar] [CrossRef]
- Kiadaliri, A.A.; Jafari, M.; Gerdtham, U.G. Frontier-based techniques in measuring hospital efficiency in Iran: A systematic review and meta-regression analysis. BMC Health Serv. Res. 2013, 13, 312. [Google Scholar] [CrossRef] [PubMed]
- Zarrin, M.; Schoenfelder, J.; Brunner, J.O. Homogeneity and best practice analyses in hospital performance management: An analytical framework. Health Care Manag. Sci. 2022, 25, 406–425. [Google Scholar] [CrossRef] [PubMed]
- Chu, T.B.; Liu, T.C.; Chen, C.S.; Tsai, Y.W.; Chiu, W.T. Household out-of-pocket medical expenditures and national health insurance in Taiwan: Income and regional inequality. BMC Health Serv. Res. 2005, 5, 60. [Google Scholar] [CrossRef] [PubMed]
- Huang, N.; Yip, W.; Chou, Y.J.; Wang, P.J. The distribution of net benefits under the National Health Insurance programme in Taiwan. Health Policy Plan. 2007, 22, 49–59. [Google Scholar] [CrossRef] [PubMed]
- Marmot, M.; Friel, S.; Bell, R.; Houweling, T.A.; Taylor, S. Closing the gap in a generation: Health equity through action on the social determinants of health. Lancet 2008, 372, 1661–1669. [Google Scholar] [CrossRef]
- Woolf, S.H. Public health implications of government spending reductions. JAMA 2011, 305, 1902–1903. [Google Scholar] [CrossRef]
- Mayberry, R.M.; Nicewander, D.A.; Qin, H.; Ballard, D.J. Improving quality and reducing inequities: A challenge in achieving best care. In Baylor University Medical Center Proceedings; Taylor & Francis: Abingdon, UK, 2006; Volume 19, pp. 103–118. [Google Scholar] [CrossRef]
- Ministry of Health and Welfare. Hospital and Clinic Statistics. 2022. Available online: https://dep.mohw.gov.tw/DOS/lp-5099-113.html (accessed on 29 June 2022).
- Department of Household Registration, Ministry of the Interior. Population Data Statistics. 2022. Available online: https://www.ris.gov.tw/app/portal/346 (accessed on 29 June 2022).
- Nemet, G.F.; Bailey, A.J. Distance and health care utilization among the rural elderly. Soc. Sci. Med. 2000, 50, 1197–1208. [Google Scholar] [CrossRef]
- Guagliardo, M.F. Spatial accessibility of primary care: Concepts, methods and challenges. Int. J. Health Geogr. 2004, 3, 3. [Google Scholar] [CrossRef]
- Arcury, T.A.; Gesler, W.M.; Preisser, J.S.; Sherman, J.; Spencer, J.; Perin, J. The effects of geography and spatial behavior on health care utilization among the residents of a rural region. Health Serv. Res. 2005, 40, 135–156. [Google Scholar] [CrossRef]
- Haynes, R.; Lovett, A.; Sünnenberg, G. Potential accessibility, travel time, and consumer choice: Geographical variations in general medical practice registrations in Eastern England. Environ. Plan. A 2003, 35, 1733–1750. [Google Scholar] [CrossRef]
- McLafferty, S.L. GIS and health care. Annu. Rev. Public Health 2003, 24, 25–42. [Google Scholar] [CrossRef] [PubMed]
- Kohl, S.; Schoenfelder, J.; Fügener, A.; Brunner, J.O. The use of Data Envelopment Analysis (DEA) in healthcare with a focus on hospitals. Health Care Manag. Sci. 2019, 22, 245–286. [Google Scholar] [CrossRef]
- de Almeida Botega, L.; Andrade, M.V.; Guedes, G.R. Brazilian hospitals’ performance: An assessment of the unified health system (SUS). Health Care Manag. Sci. 2020, 23, 443–452. [Google Scholar] [CrossRef] [PubMed]
- Simar, L.; Wilson, P.W. Sensitivity analysis of efficiency scores: How to bootstrap in nonparametric frontier models. Manag. Sci. 1998, 44, 49–61. Available online: https://pubsonline.informs.org/doi/abs/10.1287/mnsc.44.1.49 (accessed on 30 July 2022). [CrossRef]
- Nunamaker, T.R. Measuring routine nursing service efficiency: A comparison of cost per patient day and data envelopment analysis models. Health Serv. Res. 1983, 18, 183–208. Available online: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1068745/pdf/hsresearch00522-0075.pdf (accessed on 30 July 2022).
- Caballer-Tarazona, M.; Moya-Clemente, I.; Vivas-Consuelo, D.; Barrachina-Martínez, I. A model to measure the efficiency of hospital performance. Math. Comput. Model. 2010, 52, 1095–1102. [Google Scholar] [CrossRef]
- Kounetas, K.; Papathanassopoulos, F. How efficient are Greek hospitals? A case study using a double bootstrap DEA approach. Eur. J. Health Econ. 2013, 14, 979–994. [Google Scholar] [CrossRef]
- Stefko, R.; Gavurova, B.; Kocisova, K. Healthcare efficiency assessment using DEA analysis in the Slovak Republic. Health Econ. Rev. 2018, 8, 6. [Google Scholar] [CrossRef]
- Luasa, S.N.; Dineen, D.; Zieba, M. Technical and scale efficiency in public and private Irish nursing homes—A bootstrap DEA approach. Health Care Manag. Sci. 2018, 21, 326–347. [Google Scholar] [CrossRef] [PubMed]
- Chen, Y.; Wang, J.; Zhu, J.; Sherman, H.D.; Chou, S.Y. How the great recession affects performance: A case of Pennsylvania hospitals using DEA. Ann. Oper. Res. 2019, 278, 77–99. [Google Scholar] [CrossRef]
- Berger, M.; Sommersguter-Reichmann, M.; Czypionka, T. Determinants of soft budget constraints: How public debt affects hospital performance in Austria. Soc. Sci. Med. 2020, 249, 112855. [Google Scholar] [CrossRef]
- Lin, C.S.; Chiu, C.M.; Huang, Y.C.; Lang, H.C.; Chen, M.S. Evaluating the operational efficiency and quality of tertiary hospitals in Taiwan: The application of the EBITDA indicator to the DEA method and TOBIT regression. Healthcare 2022, 10, 58. [Google Scholar] [CrossRef] [PubMed]
- Goodarzi, G.; Nasab, M.H.I.; Mehr, N.J.; Rostami, K.; Omidifar, R. Hospital performance assessment of Lorestan University of Medical Sciences. Payesh 2012, 11, 309–315. Available online: http://payeshjournal.ir/article-1-453-en.html (accessed on 30 July 2022).
- Fazria, N.F.; Dhamanti, I. A literature review on the identification of variables for measuring hospital efficiency in the Data Envelopment Analysis (DEA). Unnes J. Public Health 2021, 10, 1–15. [Google Scholar] [CrossRef]
- Farrell, D.J. The measurement of productive efficiency. J. R. Stat. Soc. 1957, 120, 253–290. [Google Scholar] [CrossRef]
- Debreu, G. The coefficient of resource utilization. Econometric 1951, 19, 273–292. [Google Scholar] [CrossRef]
- Koopmans, T.C. Chapter III: An Analysis of Production as an Efficient Combination of Activities, Activity Analysis of Production and Allocation; Cowles Commission for Research in Economics, Monograph; Wiley: New York, NY, USA, 1951; Volume 13, pp. 33–97. Available online: https://cowles.yale.edu/sites/default/files/files/pub/mon/m13-all.pdf (accessed on 30 July 2022).
- Coelli, T.J.; Rao, D.S.P.; O’Donnell, C.J.; Battese, G.E. An Introduction to Efficiency and Productivity Analysis, 2nd ed.; Spinger: New York, NY, USA, 2005. [Google Scholar]
- Charnes, A.; Cooper, W.W.; Rhodes, E. Measuring the efficiency of decision-making units. Eur. J. Oper. Res. 1978, 2, 429–444. [Google Scholar] [CrossRef]
- Banker, R.D.; Charnes, A.; Cooper, W.W. Some models for estimating technical and scale inefficiencies in data envelopment analysis. Manag. Sci. 1984, 30, 1078–1092. [Google Scholar] [CrossRef]
- Seiford, L.M. Data envelopment analysis: The evolution of the State of the Art (1978–1995). J. Product. Anal. 1996, 7, 99–137. Available online: https://www.jstor.org/stable/41770796 (accessed on 30 July 2022). [CrossRef]
- Coelli, T.J. A Guide to DEAP Version 2.1: A Data Encelopment Analysis (Computer) Program; CEPA Working Paper 96/8; Department of Econometrics, University of New England: Armidale, Australia, 1996; Available online: https://www.owlnet.rice.edu/~econ380/DEAP.PDF (accessed on 30 June 2022).


| Items | Variables | Samples | Mean | Std. | Min. | Max. | Median |
|---|---|---|---|---|---|---|---|
| Output Items | Number of outpatient/year | 114 | 5,825,277 | 5,937,610 | 734,488 | 24,246,518 | 2,555,041 |
| Number of emergency departments/year | 114 | 382,517 | 311,772 | 81,936 | 1,121,367 | 203,444 | |
| Number of hospitalizations/year | 114 | 171,084 | 165,403 | 24,755 | 638,412 | 82,314 | |
| Input Items | Total number of beds/year | 114 | 8682 | 7690 | 1496 | 25,526 | 4001 |
| Number of physicians (including Western medicine, Traditional Chinese medicine, and dentistry)/year | 114 | 3590 | 3979 | 380 | 15,764 | 1246 | |
| Number of nurses (nurses and nurse practitioners)/year | 114 | 8564 | 8041 | 1430 | 30,091 | 3685 | |
| Number of other licensed medical practitioners/year | 114 | 3973 | 3975 | 519 | 15,314 | 1595 | |
| The population of each county and city/year | 1,226,564 | 1,106,241 | 215,261 | 4,030,954 | 561,551 | ||
| Item | Counties or Cities (DMUs) | CCR (CRSTE) | BCC (VRSTE) | SE | RTS | Referenced County or City | Number of Times Referenced | |||
|---|---|---|---|---|---|---|---|---|---|---|
| Efficiency Value | Rank | Efficiency Value | Rank | Efficiency Value | Rank | |||||
| 1 | New Taipei City | 0.783 | 16 | 1.000 | 1 | 0.783 | 18 | irs | - | 4 |
| 2 | Taipei City | 1.000 | 1 | 1.000 | 1 | 1.000 | 1 | - | - | - |
| 3 | Taoyuan City | 0.813 | 14 | 0.918 | 16 | 0.885 | 14 | irs | New Taipei City, Yilan County, Chiayi County, Hsinchu City | - |
| 4 | Taichung City | 0.890 | 10 | 0.961 | 15 | 0.926 | 11 | irs | Yilan County, Nantou County, Hsinchu City, Chiayi City | - |
| 5 | Tainan City | 0.769 | 18 | 0.884 | 18 | 0.869 | 16 | irs | New Taipei City, Hsinchu County, Miaoli County, Chiayi County, Hsinchu City | - |
| 6 | Kaohsiung City | 0.811 | 15 | 0.891 | 17 | 0.910 | 12 | irs | New Taipei City, Yilan County, Nantou County, Hsinchu City | - |
| 7 | Yilan County | 1.000 | 1 | 1.000 | 1 | 1.000 | 1 | - | - | 6 |
| 8 | Hsinchu County | 0.741 | 19 | 1.000 | 1 | 0.741 | 19 | irs | - | 3 |
| 9 | Miaoli County | 0.941 | 9 | 1.000 | 1 | 0.941 | 10 | irs | - | 3 |
| 10 | Changhua County | 0.942 | 8 | 1.000 | 1 | 0.942 | 9 | irs | - | - |
| 11 | Nantou County | 1.000 | 1 | 1.000 | 1 | 1.000 | 1 | - | - | 3 |
| 12 | Yunlin County | 0.775 | 17 | 0.975 | 14 | 0.794 | 17 | irs | New Taipei City, Hsinchu County, Miaoli County, Chiayi County, Taitung County, Hsinchu City | - |
| 13 | Chiayi County | 0.885 | 12 | 1.000 | 1 | 0.885 | 14 | irs | - | 4 |
| 14 | Pingtung County | 0.889 | 11 | 0.982 | 13 | 0.906 | 13 | irs | Yilan County, Hsinchu County, Chiayi County, Taitung County, Hsinchu City | - |
| 15 | Taitung County | 1.000 | 1 | 1.000 | 1 | 1.000 | 1 | - | - | 2 |
| 16 | Hualien County | 0.832 | 13 | 0.837 | 19 | 0.994 | 7 | irs | Yilan County, Chiayi City | - |
| 17 | Keelung City | 0.982 | 7 | 0.995 | 12 | 0.987 | 8 | irs | Yilan County, Miaoli County, Nantou County, Hsinchu City | - |
| 18 | Hsinchu City | 1.000 | 1 | 1.000 | 1 | 1.000 | 1 | - | - | 7 |
| 19 | Chiayi City | 1.000 | 1 | 1.000 | 1 | 1.000 | 1 | - | - | 2 |
| Annual average | 0.897 | 0.971 | 0.924 | |||||||
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the author. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Wu, J.-S. Healthcare Service Efficiency: An Empirical Study on Healthcare Capacity in Various Counties and Cities in Taiwan. Healthcare 2023, 11, 1656. https://doi.org/10.3390/healthcare11111656
Wu J-S. Healthcare Service Efficiency: An Empirical Study on Healthcare Capacity in Various Counties and Cities in Taiwan. Healthcare. 2023; 11(11):1656. https://doi.org/10.3390/healthcare11111656
Chicago/Turabian StyleWu, Jih-Shong. 2023. "Healthcare Service Efficiency: An Empirical Study on Healthcare Capacity in Various Counties and Cities in Taiwan" Healthcare 11, no. 11: 1656. https://doi.org/10.3390/healthcare11111656
APA StyleWu, J.-S. (2023). Healthcare Service Efficiency: An Empirical Study on Healthcare Capacity in Various Counties and Cities in Taiwan. Healthcare, 11(11), 1656. https://doi.org/10.3390/healthcare11111656






