An Interprofessional E-Learning Resource to Prepare Students for Clinical Practice in the Operating Room—A Mixed Method Study from the Students’ Perspective
Abstract
:1. Introduction
2. Materials and Methods
2.1. Design
2.2. The E-Learning Resource
2.3. Participants
2.4. Data Collection
2.4.1. Questionnaire
2.4.2. Focus Group Interviews
2.5. Data Analysis
2.5.1. Questionnaire—Quantitative Data
2.5.2. Focus Group Interviews—Qualitative Data
2.6. Ethical Considerations
3. Results
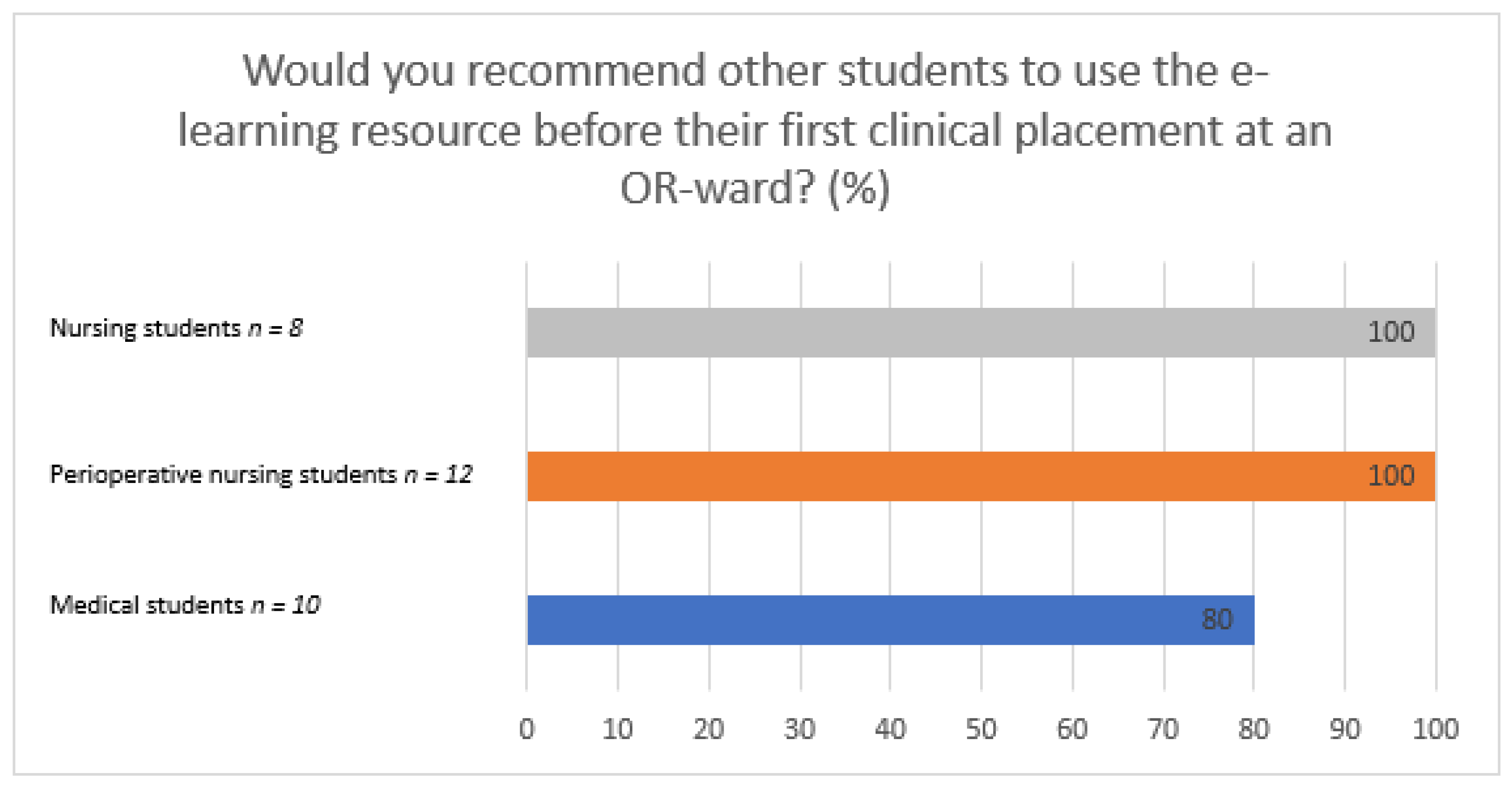
3.1. The E-Learning Resource in Preparation for Clinical Placement at the OR
“You want to be as well prepared as possible when you arrive. Although you may not be able to practice so much practically wearing gloves and such things, you want to be able to see… because then it is good because then you can see it over and over again… and you become a little more confident when you come out if you have seen it…”(Perioperative nurse)
3.2. The Students’ Perception of the Content in the Learning Resource
“Another suggestion is to also inform about what happens when something goes wrong, for example when we get unsterile or similar. So that when and if it happens it will not be so huge but you know what to do if it happens and how to handle this. Takes a little bit of the stress boost…”(Medical student)
3.3. Design and Layout of the E-Learning Resource
“It is confusing the whole arrangement I think... you do not know which (learning activity) one is inside and so you click back, and you end up somewhere else... it is difficult to remember...”(Perioperative nursing student)
3.4. Interprofessional Perspective
“We are lacking an overall picture of what is happening at the operating room, a description of the flow. To be able to prepare even better. A kind of “patient journey” through the flow to the surgery department and also a “staff journey” to gain an increased understanding of other professions in the surgery. That is generally lacking in teaching in general.”(Medical student)
4. Discussion
Limitations
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Meyer, R.; Van Schalkwyk, S.C.; Prakaschandra, R. The operating room as a clinical learning environment: An exploratory study. Nurse Educ. Pract. 2016, 18, 60–72. [Google Scholar] [CrossRef]
- Croghan, S.M.; Phillips, C.; Howson, W. The operating theatre as a classroom: A literature review of medical student learning in the theatre environment. Int. J. Med. Educ. 2019, 10, 75–87. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Zundel, S.; Wolf, I.; Christen, H.-J.; Huwendiek, S. What supports students’ education in the operating room? A focus group study including students’ and surgeons’ views. Am. J. Surg. 2015, 210, 951–959. [Google Scholar] [CrossRef]
- Chapman, S.; Hakeem, A.R.; Marangoni, G.; Prasad, K.R. How can we Enhance Undergraduate Medical Training in the Operating Room? A Survey of Student Attitudes and Opinions. J. Surg. Educ. 2013, 70, 326–333. [Google Scholar] [CrossRef] [PubMed]
- Aliabad, H.B.; Bakhshi, M.; Hassanshahi, G. Students’ perceptions of the academic learning environment in seven medical sciences courses based on DREEM. Adv. Med. Educ. Pract. 2015, 6, 195–203. [Google Scholar] [CrossRef] [Green Version]
- Gillespie, B.M.; Gwinner, K.; Chaboyer, W.; Fairweather, N. Team communications in surgery—Creating a culture of safety. J. Interprof. Care 2013, 27, 387–393. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- West, C.; Graham, L.; Palmer, R.T.; Miller, M.F.; Thayer, E.K.; Stuber, M.L.; Awdishu, L.; Umoren, R.; Wamsley, M.A.; Nelson, E.A.; et al. Implementation of interprofessional education (IPE) in 16 U.S. medical schools: Common practices, barriers and facilitators. J. Interprof. Educ. Pract. 2016, 4, 41–49. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Maertens, H.; Madani, A.; Landry, T.; Vermassen, F.; Van Herzeele, I.; Aggarwal, R. Systematic review of e-learning for surgical training. J. Br. Surg. 2016, 103, 1428–1437. [Google Scholar] [CrossRef] [Green Version]
- Ruiz, J.G.; Mintzer, M.J.; Leipzig, R.M. The Impact of E-Learning in Medical Education. Acad. Med. 2006, 81, 207–212. [Google Scholar] [CrossRef]
- Torbjörnsson, E.; Olivecrona, C.; Sonden, A. An interprofessional initiative aimed at creating a common learning resource for the operating room ward. J. Interprof. Care 2018, 32, 501–504. [Google Scholar] [CrossRef] [PubMed]
- Schoonenboom, J.; Johnson, R.B. How to Construct a Mixed Methods Research Design. KZfSS Kölner Zeitschrift für Soziologie und Sozialpsychologie 2017, 69, 107–131. [Google Scholar] [CrossRef]
- Warfa, A.-R.M. Mixed-Methods Design in Biology Education Research: Approach and Uses. CBE-Life Sci. Educ. 2016, 15, rm5. [Google Scholar] [CrossRef]
- Kitzinger, J. Qualitative Research: Introducing focus groups. BMJ 1995, 311, 299–302. [Google Scholar] [CrossRef] [Green Version]
- Holden, R.R. Face Validity. Corsini Encycl. Psychol. 2010, 1–2. [Google Scholar] [CrossRef]
- Halfens, R.; Meijers, J. Back to basics: An introduction to statistics. J. Wound Care 2013, 22, 248–251. [Google Scholar] [CrossRef] [PubMed]
- Hsieh, H.-F.; Shannon, S.E. Three approaches to qualitative content analysis. Qual. Health Res. 2005, 15, 1277–1288. [Google Scholar] [CrossRef] [PubMed]
- World Medical Association. World Medical Association Declaration of Helsinki: Ethical Principles for Medical Research Involving Human Subjects. JAMA 2013, 310, 2191–2194. [Google Scholar] [CrossRef] [Green Version]
- McNamara, N. Preparing students for clinical placements: The student’s perspective. Nurse Educ. Pract. 2015, 15, 196–202. [Google Scholar] [CrossRef]
- Chu, L.F.; Ngai, L.K.; Young, C.A.; Pearl, R.G.; Macario, A.; Harrison, T.K. Preparing Interns for Anesthesiology Residency Training: Development and Assessment of the Successful Transition to Anesthesia Residency Training (START) E-Learning Curriculum. J. Grad. Med. Educ. 2013, 5, 125–129. [Google Scholar] [CrossRef]
- Haraldseid, C.; Friberg, F.; Aase, K. How can students contribute? A qualitative study of active student involvement in development of technological learning material for clinical skills training. BMC Nurs. 2016, 15, 2. [Google Scholar] [CrossRef] [Green Version]
- Parsell, G.; Bligh, J. Interprofessional learning. Postgrad. Med. J. 1998, 74, 89–95. [Google Scholar] [CrossRef] [PubMed]
- Schuller, M.C.; DaRosa, D.A.; Crandall, M.L. Using Just-in-Time Teaching and Peer Instruction in a Residency Program’s Core Curriculum. Acad. Med. 2015, 90, 384–391. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Leong, C.; Louizos, C.; Currie, C.; Glassford, L.; Davies, N.M.; Brothwell, D.; Renaud, R. Student perspectives of an online module for teaching physical assessment skills for dentistry, dental hygiene, and pharmacy students. J. Interprof. Care 2014, 29, 1–3. [Google Scholar] [CrossRef]
- Stalmeijer, R.E.; McNaughton, N.; Van Mook, W.N.K.A. Using focus groups in medical education research: AMEE Guide No. 91. Med. Teach. 2014, 36, 923–939. [Google Scholar] [CrossRef]
- Côté-Arsenault, D.; Morrison-Beedy, D. Maintaining your focus in focus groups: Avoiding common mistakes. Res. Nurs. Health 2005, 28, 172–179. [Google Scholar] [CrossRef] [Green Version]
- Groves, R.M. Nonresponse Rates and Nonresponse Bias in Household Surveys. Public Opin. Q. 2006, 70, 646–675. [Google Scholar] [CrossRef]



| Learning Outcome | Learning Activity | Format | Running Time (min) |
|---|---|---|---|
| The student shall understand the structure of an operation ward | OR design | Recorded audio lecture | 5.04 |
| The student shall understand the different professions working at the OR and their responsibilities | Professions | Recorded audio lecture | 4.24 |
| The student shall have knowledge regarding the hygiene routine at the OR | Hygiene Routine | Recorded audio lecture | 0.45 |
| The student shall be able to describe the radiation safety at OR | Radiation Safety | Recorded audio lecture | 2.34 |
| The student shall be able to perform a sterile gloving technique | Gloving technique | Recorded audio movie | 1.40 |
| The student shall be able to perform a perioperative surgical hand preparation | Surgical hand preparation | Recorded audio movie | 4.01 |
| All Students n = 52 | 4th Year Medical Students n = 24 | 1st Year Perioperative Nursing Students n = 16 | 3rd Year Nursing Students n = 12 | |
|---|---|---|---|---|
| Age mean (range) | 34.0 (21–55) | 29.5 (22–47) | 38.4 (26–55) | 34.9 (21–52) |
| Gender (%) | ||||
| Male | 33 (63) | 13 (54) | 4 (25) | 2 (17) |
| Female | 19 (37) | 11 (46) | 12 (75) | 10 (83) |
| Previous experience of OR (%) | ||||
| Yes | 31 (60) | 12 (50) | 13 | 6 (50) |
| No | 19 (37) | 10 (42) | 3 | 6 (50) |
| Missing | 2 (3) | 2 (8) | 0 | |
| Had used the e-resource (%) | ||||
| Yes | 34 (65) | 13 (54) | 12 (75) | 9 (75) |
| No | 18 (36) | 11 (46) | 4 (25) | 3 (25) |
| Missing | 0 | 0 | 0 | 0 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Fagerdahl, A.-M.; Torbjörnsson, E.; Sondén, A. An Interprofessional E-Learning Resource to Prepare Students for Clinical Practice in the Operating Room—A Mixed Method Study from the Students’ Perspective. Healthcare 2021, 9, 1028. https://doi.org/10.3390/healthcare9081028
Fagerdahl A-M, Torbjörnsson E, Sondén A. An Interprofessional E-Learning Resource to Prepare Students for Clinical Practice in the Operating Room—A Mixed Method Study from the Students’ Perspective. Healthcare. 2021; 9(8):1028. https://doi.org/10.3390/healthcare9081028
Chicago/Turabian StyleFagerdahl, Ann-Mari, Eva Torbjörnsson, and Anders Sondén. 2021. "An Interprofessional E-Learning Resource to Prepare Students for Clinical Practice in the Operating Room—A Mixed Method Study from the Students’ Perspective" Healthcare 9, no. 8: 1028. https://doi.org/10.3390/healthcare9081028






