Glucometabolism in Kidney Transplant Recipients with and without Posttransplant Diabetes: Focus on Beta-Cell Function
Abstract
:1. Introduction
2. Materials and Methods
2.1. Patients and Experimental Procedure
2.2. Data Analysis
2.3. Statistical Analysis
3. Results
3.1. Basic Characteristics in Patients with PTDM and without PTDM
3.2. Beta-Cell Function Assessed by Indices Based on Insulin or C-Peptide
3.3. Reliability of Beta-Cell Function Assessment through Modeling Analysis
3.4. Beta-Cell Function Assessed by the Model-Based Parameters
3.5. Adjusting the Model-Based Beta-Cell Glucose Sensitivity Parameter in the Comparison between Groups
3.6. Model-Based Beta-Cell Function in Patients Stratified According to Different Criteria
3.7. The COSUGI Index
4. Discussion
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Eide, I.A.; Halden, T.A.; Hartmann, A.; Åsberg, A.; Dahle, D.O.; Reisaeter, A.V.; Jenssen, T. Mortality risk in post-transplantation diabetes mellitus based on glucose and HbA1c diagnostic criteria. Transpl. Int. 2016, 29, 568–578. [Google Scholar] [CrossRef]
- Porrini, E.; Díaz, J.M.; Moreso, F.; Lauzurrica, R.; Ibernon, M.; Torres, I.S.; Ruiz, R.B.; Rodríguez Rodríguez, A.E.; Mallén, P.D.; Bayés-Genís, B.; et al. Prediabetes is a risk factor for cardiovascular disease following renal transplantation. Kidney Int. 2019, 96, 1374–1380. [Google Scholar] [CrossRef]
- Valderhaug, T.G.; Hjelmesæth, J.; Hartmann, A.; Røislien, J.; Bergrem, H.A.; Leivestad, T.; Line, P.D.; Jenssen, T. The association of early post-transplant glucose levels with long-term mortality. Diabetologia 2011, 54, 1341–1349. [Google Scholar] [CrossRef]
- Dos Santos, Q.; Hornum, M.; Terrones-Campos, C.; Crone, C.G.; Wareham, N.E.; Soeborg, A.; Rasmussen, A.; Gustafsson, F.; Perch, M.; Soerensen, S.S.; et al. Posttransplantation Diabetes Mellitus Among Solid Organ Recipients in a Danish Cohort. Transpl. Int. 2022, 35, 10352. [Google Scholar] [CrossRef]
- Kang, E.; Lee, J.; Kang, D.H.; Park, J.; Park, S.; Kim, Y.C.; Kim, D.K.; Joo, K.W.; Kim, Y.S.; Park, M.; et al. Clinical outcomes of posttransplantation diabetes mellitus in kidney transplantation recipients: A nationwide population-based cohort study in Korea. Sci. Rep. 2022, 12, 21632. [Google Scholar] [CrossRef]
- Chakkera, H.A.; Weil, E.J.; Castro, J.; Heilman, R.L.; Reddy, K.S.; Mazur, M.J.; Hamawi, K.; Mulligan, D.C.; Moss, A.A.; Mekeel, K.L.; et al. Hyperglycemia during the immediate period after kidney transplantation. Clin. J. Am. Soc. Nephrol. 2009, 4, 853–859. [Google Scholar] [CrossRef] [PubMed]
- Chakkera, H.A.; Knowler, W.C.; Devarapalli, Y.; Weil, E.J.; Heilman, R.L.; Dueck, A.; Mulligan, D.C.; Reddy, K.S.; Moss, A.A.; Mekeel, K.L.; et al. Relationship between inpatient hyperglycemia and insulin treatment after kidney transplantation and future new onset diabetes mellitus. Clin. J. Am. Soc. Nephrol. 2010, 5, 1669–1675. [Google Scholar] [CrossRef] [PubMed]
- Cheng, C.Y.; Feng, Y.T.; Wang, H.Y. Incidence and relative risk factors in posttransplant diabetes mellitus patients: A retrospective cohort study. Korean J. Transplant. 2020, 34, 213–237. [Google Scholar] [CrossRef] [PubMed]
- Jenssen, T.; Hartmann, A. Post-transplant diabetes mellitus in patients with solid organ transplants. Nat. Rev. Endocrinol. 2019, 15, 172–188. [Google Scholar] [CrossRef]
- Byambasukh, O.; Osté, M.C.J.; Gomes-Neto, A.W.; van den Berg, E.; Navis, G.; Bakker, S.J.L.; Corpeleijn, E. Physical Activity and the Development of Post-Transplant Diabetes Mellitus, and Cardiovascular- and All-Cause Mortality in Renal Transplant Recipients. J. Clin. Med. 2020, 9, 415. [Google Scholar] [CrossRef] [PubMed]
- von Düring, M.E.; Jenssen, T.; Bollerslev, J.; Åsberg, A.; Godang, K.; Eide, I.A.; Dahle, D.O.; Hartmann, A. Visceral fat is better related to impaired glucose metabolism than body mass index after kidney transplantation. Transpl. Int. 2015, 28, 1162–1171. [Google Scholar] [CrossRef]
- Hjelmesæth, J.; Hartmann, A.; Kofstad, J.; Egeland, T.; Stenstrøm, J.; Fauchald, P. Tapering off prednisolone and cyclosporin the first year after renal transplantation: The effect on glucose tolerance. Nephrol. Dial. Transplant. 2001, 16, 829–835. [Google Scholar] [CrossRef] [PubMed]
- Torres, A.; Hernández, D.; Moreso, F.; Serón, D.; Burgos, M.D.; Pallardó, L.M.; Kanter, J.; Díaz Corte, C.; Rodríguez, M.; Diaz, J.M.; et al. Randomized Controlled Trial Assessing the Impact of Tacrolimus Versus Cyclosporine on the Incidence of Posttransplant Diabetes Mellitus. Kidney Int. Rep. 2018, 3, 1304–1315. [Google Scholar] [CrossRef]
- Serna-Higuita, L.M.; Isaza-López, M.C.; Hernández-Herrera, G.N.; Serna-Campuzano, A.M.; Nieto-Rios, J.F.; Heyne, N.; Guthoff, M. Development and Validation of a New Score to Assess the Risk of Posttransplantation Diabetes Mellitus in Kidney Transplant Recipients. Transplant. Direct 2023, 9, e1558. [Google Scholar] [CrossRef] [PubMed]
- Hecking, M.; Werzowa, J.; Haidinger, M.; Hörl, W.H.; Pascual, J.; Budde, K.; Luan, F.L.; Ojo, A.; de Vries, A.P.; Porrini, E.; et al. Novel views on new-onset diabetes after transplantation: Development, prevention and treatment. Nephrol. Dial. Transplant. 2013, 28, 550–566. [Google Scholar] [CrossRef] [PubMed]
- Bergfeld, L.; Werzowa, J.; Säemann, M.; Hecking, M. Correspondence regarding the impact of kidney transplantation on insulin sensitivity. Transpl. Int. 2018, 31, 456–457. [Google Scholar] [CrossRef]
- Sharif, A.; Cohney, S. Post-transplantation diabetes-state of the art. Lancet Diabetes Endocrinol. 2016, 4, 337–349. [Google Scholar] [CrossRef] [PubMed]
- Nam, J.H.; Mun, J.I.; Kim, S.I.; Kang, S.W.; Choi, K.H.; Park, K.; Ahn, C.W.; Cha, B.S.; Song, Y.D.; Lim, S.K.; et al. beta-Cell dysfunction rather than insulin resistance is the main contributing factor for the development of postrenal transplantation diabetes mellitus. Transplantation 2001, 71, 1417–1423. [Google Scholar] [CrossRef]
- Zelle, D.M.; Corpeleijn, E.; Deinum, J.; Stolk, R.P.; Gans, R.O.; Navis, G.; Bakker, S.J. Pancreatic β-cell dysfunction and risk of new-onset diabetes after kidney transplantation. Diabetes Care 2013, 36, 1926–1932. [Google Scholar] [CrossRef]
- Hecking, M.; Kainz, A.; Werzowa, J.; Haidinger, M.; Döller, D.; Tura, A.; Karaboyas, A.; Hörl, W.H.; Wolzt, M.; Sharif, A.; et al. Glucose metabolism after renal transplantation. Diabetes Care 2013, 36, 2763–2771. [Google Scholar] [CrossRef]
- Yates, C.J.; Fourlanos, S.; Colman, P.G.; Cohney, S.J. Divided dosing reduces prednisolone-induced hyperglycaemia and glycaemic variability: A randomized trial after kidney transplantation. Nephrol. Dial. Transplant. 2014, 29, 698–705. [Google Scholar] [CrossRef]
- Hecking, M.; Haidinger, M.; Döller, D.; Werzowa, J.; Tura, A.; Zhang, J.; Tekoglu, H.; Pleiner, J.; Wrba, T.; Rasoul-Rockenschaub, S.; et al. Early basal insulin therapy decreases new-onset diabetes after renal transplantation. J. Am. Soc. Nephrol. 2012, 23, 739–749. [Google Scholar] [CrossRef]
- Schwaiger, E.; Krenn, S.; Kurnikowski, A.; Bergfeld, L.; Pérez-Sáez, M.J.; Frey, A.; Topitz, D.; Bergmann, M.; Hödlmoser, S.; Bachmann, F.; et al. Early Postoperative Basal Insulin Therapy versus Standard of Care for the Prevention of Diabetes Mellitus after Kidney Transplantation: A Multicenter Randomized Trial. J. Am. Soc. Nephrol. 2021, 32, 2083–2098. [Google Scholar] [CrossRef] [PubMed]
- Kurnikowski, A.; Nordheim, E.; Schwaiger, E.; Krenn, S.; Harreiter, J.; Kautzky-Willer, A.; Leutner, M.; Werzowa, J.; Tura, A.; Budde, K.; et al. Criteria for prediabetes and posttransplant diabetes mellitus after kidney transplantation: A 2-year diagnostic accuracy study of participants from a randomized controlled trial. Am. J. Transplant. 2022, 22, 2880–2891. [Google Scholar] [CrossRef] [PubMed]
- American Diabetes Association Professional Practice Committee. 2. Classification and Diagnosis of Diabetes: Standards of Medical Care in Diabetes-2022. Diabetes Care 2022, 45, S17–S38. [Google Scholar] [CrossRef]
- Inker, L.A.; Eneanya, N.D.; Coresh, J.; Tighiouart, H.; Wang, D.; Sang, Y.; Crews, D.C.; Doria, A.; Estrella, M.M.; Froissart, M.; et al. New Creatinine- and Cystatin C–Based Equations to Estimate GFR without Race. N. Engl. J. Med. 2021, 385, 1737–1749. [Google Scholar] [CrossRef] [PubMed]
- Hundemer, G.L.; White, C.A.; Norman, P.A.; Knoll, G.A.; Tangri, N.; Sood, M.M.; Hiremath, S.; Burns, K.D.; McCudden, C.; Akbari, A. Performance of the 2021 Race-Free CKD-EPI Creatinine- and Cystatin C-Based Estimated GFR Equations Among Kidney Transplant Recipients. Am. J. Kidney Dis. 2022, 80, 462–472.e461. [Google Scholar] [CrossRef]
- Phillips, D.I.W.; Clark, P.M.; Hales, C.N.; Osmond, C. Understanding Oral Glucose Tolerance: Comparison of Glucose or Insulin Measurements During the Oral Glucose Tolerance Test with Specific Measurements of Insulin Resistance and Insulin Secretion. Diabet. Med. 1994, 11, 286–292. [Google Scholar] [CrossRef]
- Pacini, G.; Mari, A. Methods for clinical assessment of insulin sensitivity and beta-cell function. Best. Pract. Res. Clin. Endocrinol. Metab. 2003, 17, 305–322. [Google Scholar] [CrossRef]
- Mari, A.; Tura, A.; Gastaldelli, A.; Ferrannini, E. Assessing insulin secretion by modeling in multiple-meal tests: Role of potentiation. Diabetes 2002, 51 (Suppl. S1), S221–S226. [Google Scholar] [CrossRef]
- Mari, A.; Schmitz, O.; Gastaldelli, A.; Oestergaard, T.; Nyholm, B.; Ferrannini, E. Meal and oral glucose tests for assessment of beta -cell function: Modeling analysis in normal subjects. Am. J. Physiol. Endocrinol. Metab. 2002, 283, E1159–E1166. [Google Scholar] [CrossRef] [PubMed]
- Mari, A.; Ferrannini, E. Beta-cell function assessment from modelling of oral tests: An effective approach. Diabetes Obes. Metab. 2008, 10 (Suppl. S4), 77–87. [Google Scholar] [CrossRef] [PubMed]
- Matthews, D.R.; Hosker, J.P.; Rudenski, A.S.; Naylor, B.A.; Treacher, D.F.; Turner, R.C. Homeostasis model assessment: Insulin resistance and beta-cell function from fasting plasma glucose and insulin concentrations in man. Diabetologia 1985, 28, 412–419. [Google Scholar] [CrossRef] [PubMed]
- Tahapary, D.L.; Pratisthita, L.B.; Fitri, N.A.; Marcella, C.; Wafa, S.; Kurniawan, F.; Rizka, A.; Tarigan, T.J.E.; Harbuwono, D.S.; Purnamasari, D.; et al. Challenges in the diagnosis of insulin resistance: Focusing on the role of HOMA-IR and Tryglyceride/glucose index. Diabetes Metab. Syndr. 2022, 16, 102581. [Google Scholar] [CrossRef] [PubMed]
- Tura, A.; Chemello, G.; Szendroedi, J.; Göbl, C.; Færch, K.; Vrbíková, J.; Pacini, G.; Ferrannini, E.; Roden, M. Prediction of clamp-derived insulin sensitivity from the oral glucose insulin sensitivity index. Diabetologia 2018, 61, 1135–1141. [Google Scholar] [CrossRef] [PubMed]
- Rebelos, E.; Honka, M.J. PREDIM index: A useful tool for the application of the euglycemic hyperinsulinemic clamp. J. Endocrinol. Investig. 2021, 44, 631–634. [Google Scholar] [CrossRef] [PubMed]
- Stephenson, J.J.; Raval, A.D.; Kern, D.M.; Bae, J.P. Non-adherence to basal insulin among patients with type 2 diabetes in a US managed care population: Results from a patient survey. Diabetes Obes. Metab. 2018, 20, 2700–2704. [Google Scholar] [CrossRef]
- Perreault, L.; Skyler, J.S.; Rosenstock, J. Novel therapies with precision mechanisms for type 2 diabetes mellitus. Nat. Rev. Endocrinol. 2021, 17, 364–377. [Google Scholar] [CrossRef]
- Lindroos, M.M.; Majamaa, K.; Tura, A.; Mari, A.; Kalliokoski, K.K.; Taittonen, M.T.; Iozzo, P.; Nuutila, P. m.3243A>G mutation in mitochondrial DNA leads to decreased insulin sensitivity in skeletal muscle and to progressive beta-cell dysfunction. Diabetes 2009, 58, 543–549. [Google Scholar] [CrossRef]
- Pascoe, L.; Frayling, T.M.; Weedon, M.N.; Mari, A.; Tura, A.; Ferrannini, E.; Walker, M. Beta cell glucose sensitivity is decreased by 39% in non-diabetic individuals carrying multiple diabetes-risk alleles compared with those with no risk alleles. Diabetologia 2008, 51, 1989–1992. [Google Scholar] [CrossRef]
- Tura, A.; Grassi, A.; Winhofer, Y.; Guolo, A.; Pacini, G.; Mari, A.; Kautzky-Willer, A. Progression to type 2 diabetes in women with former gestational diabetes: Time trajectories of metabolic parameters. PLoS ONE 2012, 7, e50419. [Google Scholar] [CrossRef] [PubMed]
- Tura, A.; Mari, A.; Winzer, C.; Kautzky-Willer, A.; Pacini, G. Impaired beta-cell function in lean normotolerant former gestational diabetic women. Eur. J. Clin. Investig. 2006, 36, 22–28. [Google Scholar] [CrossRef]
- Van Cauter, E.; Mestrez, F.; Sturis, J.; Polonsky, K.S. Estimation of insulin secretion rates from C-peptide levels. Comparison of individual and standard kinetic parameters for C-peptide clearance. Diabetes 1992, 41, 368–377. [Google Scholar] [CrossRef] [PubMed]
- Aoki, Y.; Yanagisawa, Y.; Oguchi, H.; Furuta, S. Contribution of hyperglycemia and renal damage to urinary C-peptide clearance in non-insulin-dependent diabetic patients. Diabetes Res. Clin. Pract. 1991, 14, 85–89. [Google Scholar] [CrossRef] [PubMed]
- Blackman, J.D.; Polonsky, K.S.; Jaspan, J.B.; Sturis, J.; Van Cauter, E.; Thistlethwaite, J.R. Insulin secretory profiles and C-peptide clearance kinetics at 6 months and 2 years after kidney-pancreas transplantation. Diabetes 1992, 41, 1346–1354. [Google Scholar] [CrossRef] [PubMed]
- D’Elia, J.A.; Mulla, C.; Liu, J.; Weinrauch, L.A. Variations in glucose/C-peptide ratio in patients with type 2 diabetes associated with renal function. Diabetes Res. Clin. Pract. 2019, 150, 1–7. [Google Scholar] [CrossRef] [PubMed]
- Robaudo, C.; Zavaroni, I.; Garibotto, G.; Deferrari, G. Renal metabolism of C-peptide in patients with early insulin-dependent diabetes mellitus. Nephron 1996, 72, 395–401. [Google Scholar] [CrossRef]
- ten Dam, M.A.; Werter, C.J.; Popp-Snijders, C.; Donker, A.J.; ten Kate, R.W. Renal handling of insulin and C-peptide in patients with non-insulin-dependent diabetes mellitus. Nephrol. Dial. Transplant. 1993, 8, 134–139. [Google Scholar]
- Zavaroni, I.; Deferrari, G.; Lugari, R.; Bonora, E.; Garibotto, G.; Dall’Aglio, E.; Robaudo, C.; Gnudi, A. Renal metabolism of C-peptide in man. J. Clin. Endocrinol. Metab. 1987, 65, 494–498. [Google Scholar] [CrossRef]
- Ferrannini, E.; Mari, A. Beta cell function and its relation to insulin action in humans: A critical appraisal. Diabetologia 2004, 47, 943–956. [Google Scholar] [CrossRef]
- Tura, A.; Grespan, E.; Göbl, C.S.; Koivula, R.W.; Franks, P.W.; Pearson, E.R.; Walker, M.; Forgie, I.M.; Giordano, G.N.; Pavo, I.; et al. Profiles of Glucose Metabolism in Different Prediabetes Phenotypes, Classified by Fasting Glycemia, 2-Hour OGTT, Glycated Hemoglobin, and 1-Hour OGTT: An IMI DIRECT Study. Diabetes 2021, 70, 2092–2106. [Google Scholar] [CrossRef]
- Defronzo, R.A. Banting Lecture. From the triumvirate to the ominous octet: A new paradigm for the treatment of type 2 diabetes mellitus. Diabetes 2009, 58, 773–795. [Google Scholar] [CrossRef]
- Mannino, G.C.; Mancuso, E.; Sbrignadello, S.; Morettini, M.; Andreozzi, F.; Tura, A. Chemical Compounds and Ambient Factors Affecting Pancreatic Alpha-Cells Mass and Function: What Evidence? Int. J. Environ. Res. Public Health 2022, 19, 16489. [Google Scholar] [CrossRef]
- Banarer, S.; McGregor, V.P.; Cryer, P.E. Intraislet hyperinsulinemia prevents the glucagon response to hypoglycemia despite an intact autonomic response. Diabetes 2002, 51, 958–965. [Google Scholar] [CrossRef]
- Meier, J.J.; Kjems, L.L.; Veldhuis, J.D.; Lefèbvre, P.; Butler, P.C. Postprandial suppression of glucagon secretion depends on intact pulsatile insulin secretion: Further evidence for the intraislet insulin hypothesis. Diabetes 2006, 55, 1051–1056. [Google Scholar] [CrossRef]
- Morettini, M.; Burattini, L.; Göbl, C.; Pacini, G.; Ahrén, B.; Tura, A. Mathematical Model of Glucagon Kinetics for the Assessment of Insulin-Mediated Glucagon Inhibition During an Oral Glucose Tolerance Test. Front. Endocrinol. 2021, 12, 611147. [Google Scholar] [CrossRef] [PubMed]
- Yu, Q.; Shuai, H.; Ahooghalandari, P.; Gylfe, E.; Tengholm, A. Glucose controls glucagon secretion by directly modulating cAMP in alpha cells. Diabetologia 2019, 62, 1212–1224. [Google Scholar] [CrossRef] [PubMed]
- Ekstrand, A.V.; Eriksson, J.G.; Grönhagen-Riska, C.; Ahonen, P.J.; Groop, L.C. Insulin resistance and insulin deficiency in the pathogenesis of posttransplantation diabetes in man. Transplantation 1992, 53, 563–569. [Google Scholar] [CrossRef] [PubMed]
- Midtvedt, K.; Hartmann, A.; Hjelmesaeth, J.; Lund, K.; Bjerkely, B.L. Insulin resistance is a common denominator of post-transplant diabetes mellitus and impaired glucose tolerance in renal transplant recipients. Nephrol. Dial. Transplant. 1998, 13, 427–431. [Google Scholar] [CrossRef] [PubMed]
- Hagen, M.; Hjelmesaeth, J.; Jenssen, T.; Morkrid, L.; Hartmann, A. A 6-year prospective study on new onset diabetes mellitus, insulin release and insulin sensitivity in renal transplant recipients. Nephrol. Dial. Transplant. 2003, 18, 2154–2159. [Google Scholar] [CrossRef] [PubMed]
- Halden, T.A.; Egeland, E.J.; Åsberg, A.; Hartmann, A.; Midtvedt, K.; Khiabani, H.Z.; Holst, J.J.; Knop, F.K.; Hornum, M.; Feldt-Rasmussen, B.; et al. GLP-1 Restores Altered Insulin and Glucagon Secretion in Posttransplantation Diabetes. Diabetes Care 2016, 39, 617–624. [Google Scholar] [CrossRef] [PubMed]
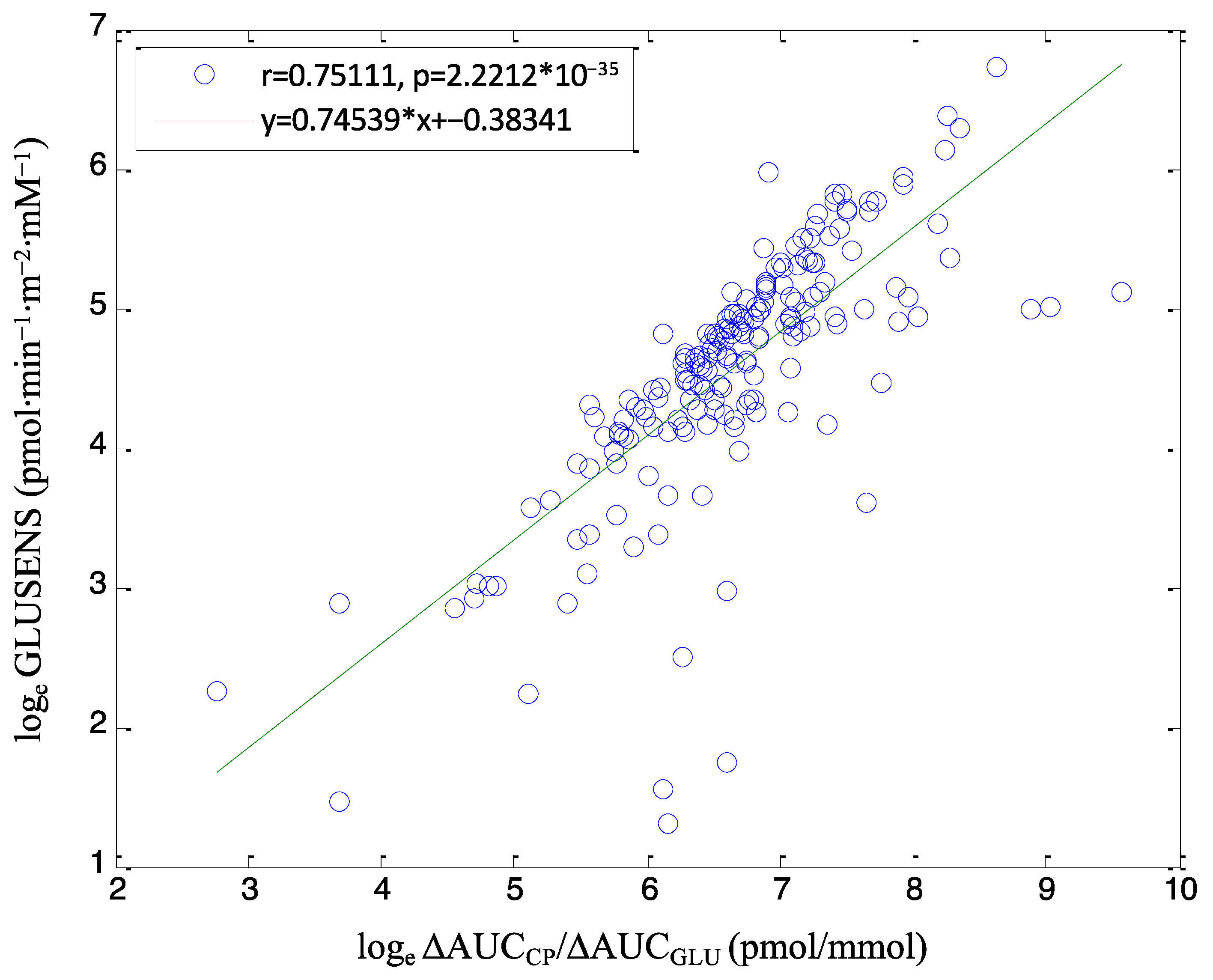

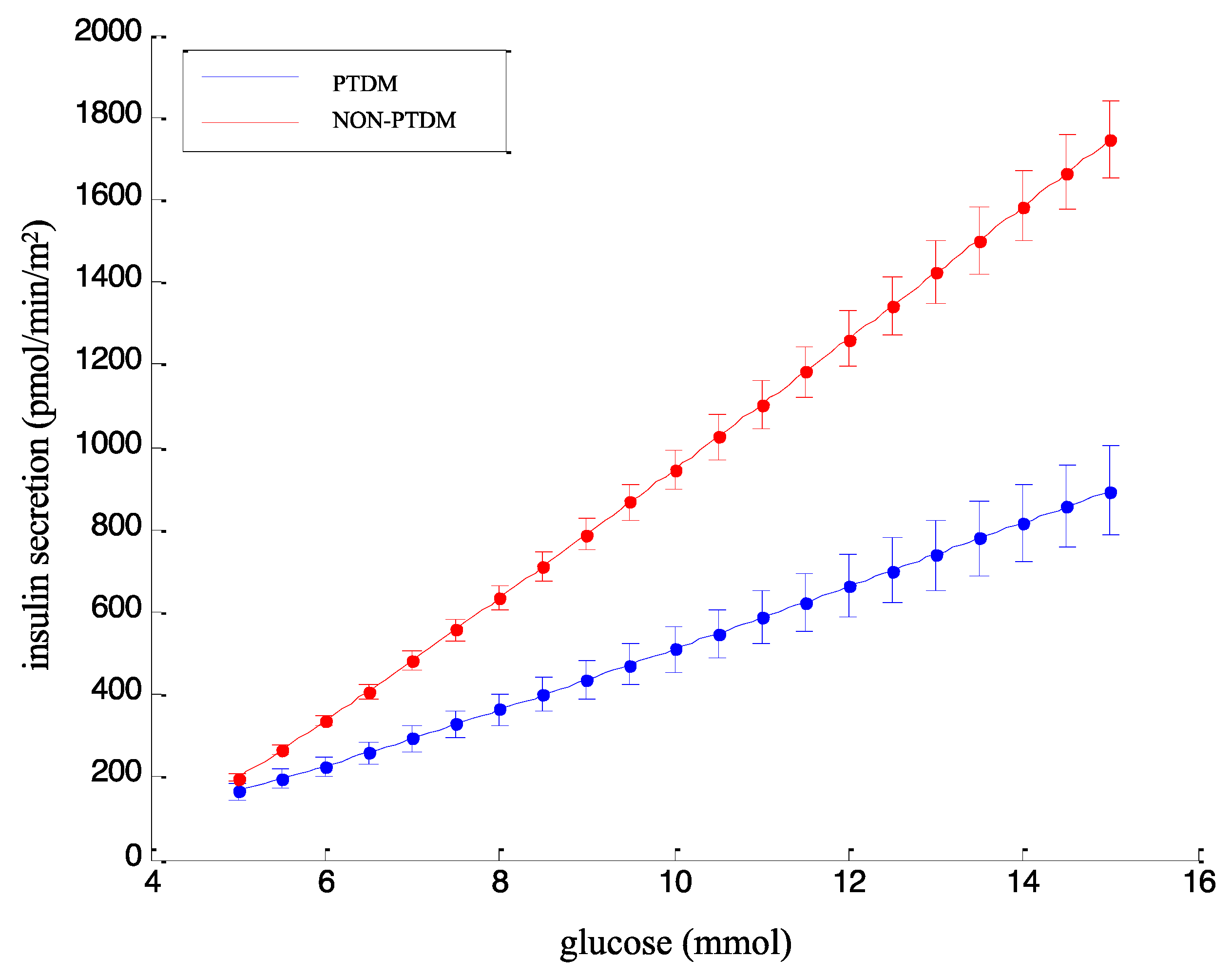

| PTDM | NON-PTDM | |
|---|---|---|
| Baseline | ||
| Sex (Male/Female) | 15/11 | 107/58 |
| Age (years) | 59.88 ± 11.22 | 48.24 ± 14.64 * |
| BMI (kg/m2) | 29.79 ± 6.48 | 25.14 ± 4.75 * |
| Fasting plasma glucose (mg/dL) | 103.52 ± 25.75 | 91.89 ± 16.31 * |
| Fasting serum insulin (µU/mL) | 23.30 ± 27.23 | 14.09 ± 16.44 |
| Fasting serum C-peptide (ng/mL) | 12.67 ± 9.48 | 9.19 ± 5.01 * |
| HbA1c (%) | 5.45 ± 0.46 | 5.10 ± 0.51 * |
| Creatinine (mg/dL) | 7.52 ± 3.72 | 7.67 ± 2.70 |
| eGFR (mL/min/1.73 m2) | 8.23 ± 3.42 | 8.64 ± 4.11 |
| 6-month follow-up | ||
| BMI (kg/m2) | 28.53 ± 6.32 † | 24.87 ± 4.88 * |
| Fasting plasma glucose (mg/dL) | 109.42 ± 21.26 | 95.85 ± 12.46 *,† |
| Fasting serum insulin (µU/mL) | 13.50 ± 9.84 | 10.28 ± 7.19 † |
| Fasting serum C-peptide (ng/mL) | 4.47 ± 2.75 † | 3.63 ± 1.67 † |
| HbA1c (%) | 6.03 ± 0.76 † | 5.45 ± 0.51 *,† |
| Creatinine (mg/dL) | 1.50 ± 0.46 † | 1.51 ± 0.64 † |
| eGFR (mL/min/1.73 m2) | 51.86 ± 15.55 † | 59.73 ± 21.97 † |
| PTDM | NON-PTDM | PTDM–NON-PTDM Relative Difference (%) | |
|---|---|---|---|
| Beta-cell function indices from insulin | |||
| INSf/GLUf (pmol/mmol) | 14.18 ± 12.24 | 11.49 ± 7.45 | 23.40 |
| IGI (pmol/mmol) | 44.78 ± 47.47 | 118.98 ± 114.07 * | −62.37 |
| AUCINS/AUCGLU (pmol/mmol) | 27.33 ± 26.06 | 42.74 ± 25.82 * | −36.05 |
| ΔAUCINS/ΔAUCGLU (pmol/mmol) | 55.18 ± 65.98 | 163.51 ± 200.13 * | −66.25 |
| Beta-cell function indices from C-peptide | |||
| CPf/GLUf (pmol/mmol) | 244.09 ± 139.97 | 224.87 ± 91.71 | 8.54 |
| IGICP (pmol/mmol) | 288.04 ± 264.49 | 581.53 ± 468.72 * | −50.47 |
| AUCCP/AUCGLU (pmol/mmol) | 297.30 ± 159.14 | 414.98 ± 152.09 * | −28.36 |
| ΔAUCCP/ΔAUCGLU (pmol/mmol) | 464.96 ± 547.23 | 1250.28 ± 1519.59 * | −62.81 |
| Beta-cell function parameters from modeling analysis | |||
| GLUSENS (pmol∙min−1∙m−2∙mM−1) | 68.44 ± 57.82 | 143.73 ± 112.91 * | −52.38 |
| RSENS (pmol∙m−2∙mM−1) | 485.87 ± 881.21 | 941.02 ± 1664.61 | −48.37 |
| PFR (dimensionless) | 1.35 ± 0.56 | 1.57 ± 0.90 | −13.96 |
| ISR5 (pmol∙min−1∙m−2) | 165.01 ± 128.14 | 196.99 ± 103.28 | −16.24 |
| ISR6 (pmol∙min−1∙m−2) | 226.51 ± 145.17 | 331.37 ± 172.25 * | −31.64 |
| ISR7 (pmol∙min−1∙m−2) | 293.19 ± 181.12 | 475.58 ± 273.22 * | −38.35 |
| Other glucometabolic indices | |||
| HOMA-IR (dimensionless) | 3.61 ± 2.70 | 2.49 ± 1.93 | 44.66 |
| PREDIM (mg/min/kg) | 3.65 ± 1.68 | 5.46 ± 2.57 * | −33.12 |
| COSUGIINS (dimensionless) | 1.21 ± 0.56 | 0.95 ± 0.51 * | 27.76 |
| COSUGICP (dimensionless) | 1.23 ± 0.41 | 0.95 ± 0.39 * | 29.29 |
| OB | NON-OB | ELDER | NON-ELDER | M | F | |
|---|---|---|---|---|---|---|
| Beta-cell function parameters from modeling analysis | ||||||
| GLUSENS (pmol∙min−1∙m−2∙mM−1) | 120.50 ± 116.34 | 140.18 ± 106.64 | 109.79 ± 84.72 | 154.16 ± 125.03 * | 138.35 ± 106.04 | 123.54 ± 117.95 |
| RSENS (pmol∙m−2∙mM−1) | 459.92 ± 656.91 | 1095.29 ± 1862.34 | 868.25 ± 1779.15 | 888.50 ± 1406.86 | 788.89 ± 1568.99 | 1039.76 ± 1638.98 |
| PFR (dimensionless) | 1.31 ± 0.48 | 1.66 ± 0.90 * | 1.60 ± 0.94 | 1.49 ± 0.71 | 1.54 ± 0.88 | 1.54 ± 0.75 |
| ISR5 (pmol∙min−1∙m−2) | 195.66 ± 117.63 | 191.08 ± 101.70 | 199.04 ± 114.06 | 187.06 ± 101.00 | 188.20 ± 110.23 | 201.50 ± 103.09 |
| ISR6 (pmol∙min−1∙m−2) | 303.37 ± 180.92 | 324.18 ± 167.93 | 300.02 ± 156.42 | 332.01 ± 184.52 | 317.68 ± 169.21 | 316.77 ± 181.17 |
| ISR7 (pmol∙min−1∙m−2) | 420.63 ± 278.31 | 466.29 ± 264.80 | 408.78 ± 226.51 | 487.38 ± 298.54 * | 456.83 ± 262.55 | 439.58 ± 286.66 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Kurnikowski, A.; Salvatori, B.; Krebs, M.; Budde, K.; Eller, K.; Pascual, J.; Morettini, M.; Göbl, C.; Hecking, M.; Tura, A. Glucometabolism in Kidney Transplant Recipients with and without Posttransplant Diabetes: Focus on Beta-Cell Function. Biomedicines 2024, 12, 317. https://doi.org/10.3390/biomedicines12020317
Kurnikowski A, Salvatori B, Krebs M, Budde K, Eller K, Pascual J, Morettini M, Göbl C, Hecking M, Tura A. Glucometabolism in Kidney Transplant Recipients with and without Posttransplant Diabetes: Focus on Beta-Cell Function. Biomedicines. 2024; 12(2):317. https://doi.org/10.3390/biomedicines12020317
Chicago/Turabian StyleKurnikowski, Amelie, Benedetta Salvatori, Michael Krebs, Klemens Budde, Kathrin Eller, Julio Pascual, Micaela Morettini, Christian Göbl, Manfred Hecking, and Andrea Tura. 2024. "Glucometabolism in Kidney Transplant Recipients with and without Posttransplant Diabetes: Focus on Beta-Cell Function" Biomedicines 12, no. 2: 317. https://doi.org/10.3390/biomedicines12020317







