Abstract
Exercise is a cornerstone of diabetes management, but the onset of diabetic foot disease (DFD) can significantly limit its implementation. Meanwhile, physical activity (PA) has been shown to reduce the risk of developing DFD through various mechanisms, and emerging evidence also supports the role of exercise in managing the active phase of the condition. Appropriately tailored PA offers both local and systemic benefits—even in clinical contexts where foot offloading is recommended. The research indicates that selected exercises can be safely incorporated into care plans, providing therapeutic effects without compromising wound healing. Drawing from current knowledge based on basic science, clinical research, and relatively general recommendations, this article summarizes the local and systemic effects of properly selected exercises in patients with DFD. It explains the underlying mechanisms and briefly discusses practical examples, integrating the most recently published findings.
1. Introduction
Exercise is the basis of diabetes mellitus (DM) treatment [1,2,3], as physical activity (PA) plays an important role in regulating glucose levels in the body [4,5,6,7]. Therefore undertaking activity by patients is recommended by all scientific societies dealing with the issue of carbohydrate metabolism disorders. Physical activity refers to any bodily movement produced by skeletal muscles that requires energy expenditure, whereas exercise is a structured and purposeful form of PA designed to improve physical fitness or health outcomes. Difficulties in engaging in PA among patients with DM are common, and stem from numerous issues described in observational studies. These problems arise both from the nature of the disease itself (e.g., glycemic fluctuations, risk of hypoglycemia depending on therapy, presence of complications) as well as from non-disease-related barriers (e.g., socioeconomic status, education, patient age, lack of time, etc.) [8,9,10,11].
Despite ongoing updates, the guidelines regarding recommended PA remain fairly general, and are mostly targeted at patients with DM who do not have significant complications. This is understandable, as the presence of chronic complications (including those affecting the foot) in diabetes requires a highly individualized approach to all recommendations, including those related to exercise. Nonetheless, physical activity remains essential at every stage of diabetes management, although its previous form often requires significant modification.
According to the International Working Group on the Diabetic Foot (IWGD) [12], diabetic foot disease (DFD) is defined as a condition when a patient with diabetes and neuropathy and/or arterial blood flow disorders in the lower limbs develops ulceration, infection, and/or destructive changes in the deep tissues below the ankle. Approximately 4–10% of patients with DM have active foot lesions (such as ulcers, infections, or deformities), while the lifetime risk of developing a foot ulcer reaches 15–25%, meaning that every fourth to sixth person with DM will experience this complication. In Europe, diabetes-related amputations account for 40–70% of all lower-limb amputations [13,14]. The St. Vincent Declaration, an international document developed in 1989 and signed by many European Union countries, outlined ambitious health goals to be achieved within 5–10 years of joining the initiative [15]. Among these cornerstones of health policy was the assumption that the number of lower extremity amputations caused by diabetes should be reduced by half. This particular objective proved to be one of the most difficult to achieve, due to significant regional disparities and limitations within healthcare systems. In regions where multidisciplinary diabetic foot care programs were implemented (including specialist teams, rapid intervention protocols, and patient education), significant reductions in amputation rates were observed—reaching even 50–68%. Unfortunately, on a broader population level, many regions failed to meet the target set by the declaration [16].
There is ample evidence that targeted PA reduces the risk of peripheral neuropathy (prevention stage of DFD) [17]. Adequate exercise improves sole load distribution, skin sensitivity, peripheral nerve conduction, intraepidermal nerve fiber density or joint mobility of the foot which translates into proper gait [18,19], and reduces the risk of pathologies typical of diabetes occurring in that area [20,21,22,23,24,25,26,27]. As in patients without DM, both the reduction of atherosclerosis risk factors and walking have a beneficial effect on peripheral circulation, reducing the risk of clinically significant limb ischemia leading to ulcers and amputations [28,29,30]. At the prevention stage of DFD, patients are educated about the role of exercise and its safety. The condition of the peripheral nervous system (perception of injury) and blood supply to the limbs is assessed.
Although, as mentioned, physical activity is recommended, in some cases, due to overlapping diseases, patients are advised to discontinue or limit their current activities for the duration of treatment. This may have adverse effects not only on the patients’ glycemic control (by increasing insulin resistance) and body weight but on respiratory and cardiovascular systems, and may also contribute to musculoskeletal disorders, which can translate into delayed recovery and poorer functioning after recovery [31,32,33,34,35,36,37,38]. An example of such a situation in the life of a patient with DM is the occurrence of DFD.
In the case of the presence of an unhealed ulcer, current guidelines on the treatment of diabetes and its complications provide only the recommendation to eliminate weight-bearing activity [39,40]. In the presence of Charcot deformity, the role of stretching and muscle-strengthening exercises is noted as potentially helpful [39]. In the Clinical Practice Guideline published in 2023 [41] the authors address this issue and explicitly raise the problem of “Various fitness/exercise routines with various intensities, including aerobic and resistance training” in the context of an expected outcome defined as “Improved mobility in the context of wound healing.” However, even in this document, the lack of precise recommendations regarding which exercises should be prescribed and what their potential benefits are is emphasized. Similarly, in the IWGDF guidelines [40]—the most authoritative document in this field—29 recommendations are provided for managing DFD, but none of them refer to exercise. This situation results from the limited number of RCTs (randomized controlled trials) dedicated to this topic that have included a sufficiently large number of patients in the intervention.
The aim of the article is to highlight the role that exercise, when performed with individualized precautions, can play in improving the condition of a patient with a wound and/or foot deformity due to DFD.
2. Basis for the Narrative Review
The foundation of our narrative review article is a comprehensive systematic review published in 2023 [42], which summarized the limited but growing body of clinical research focused on exercise interventions initiated after a diagnosis of DFD. This review highlighted the potential benefits of various exercise modalities based on the available studies. Following its publication, a new randomized clinical trial was released [43], further supporting the inclusion of exercise in the management of patients with DFD—although it has not yet influenced clinical guidelines [39,40].
In addition to the available clinical studies discussed in the mentioned systematic review and new data from 2024, we have incorporated findings from the basic research, including preclinical experiments (on animals and humans), which provide mechanistic insights into how even simple physical exercises may contribute to both local and systemic improvements in individuals with DFD.
Step by step, we aim to demonstrate that the application of exercise in patients with DFD is safe and may be recommended—even before large-scale, high-quality trials become available—provided it is applied judiciously. In the meantime, clinicians may consider relying on existing evidence from both basic science and clinical research to guide individualized therapeutic decisions.
The authors of the publication have medical (diabetology: ES, AK-B, vascular: ES diseases) and physiotherapeutic (ES, KB) backgrounds, as well as many years of experience in treating patients with DFD.
3. Consequences of Diabetic Foot Disease
Interventions in DFD occur at every stage of the disease and aim to prevent the onset of DFD, treat the condition itself, and prevent its consequences—particularly long-term consequences—that may lead to disability in the patient. The functional and physical consequences of DFD are presented in Table 1. This information has been compiled by the authors based on current knowledge and practical experience in managing patients with diabetic foot disease.
Diabetic foot disease substantially impairs patients’ mobility due to pain, ulcerations, infections, and the mandatory offloading of the affected limb. These limitations often lead to reduced PA, causing muscle weakness and diminished endurance, which further restricts the range of motion (ROM) and the ability to ambulate effectively. Consequently, patients with DFD face a heightened risk of falls and subsequent injuries [44,45]. Furthermore, sensory neuropathy associated with DFD disrupts proprioceptive feedback, resulting in impaired postural control and balance instability. The motor neuropathy contributes to foot deformities and altered biomechanics, exacerbating postural instability and increasing the likelihood of gait abnormalities [46,47]. At the musculoskeletal level, chronic inflammation, immobilization, neuropathic, and ischaemic changes lead to muscle atrophy and joint stiffness, reducing flexibility and strength. Additionally, bone integrity is compromised due to osteopenia or osteoporosis and structural deformities like Charcot foot, which further diminish functional capacity [48,49].
Overall, the combined effects of reduced mobility, impaired postural control, and musculoskeletal deterioration culminate in significant loss of independence. Patients with DFD often require assistance for the activities of daily living and rehabilitation interventions to improve functional outcomes and quality of life [50,51].

Table 1.
Pathomechanisms and Consequences of Diabetic Foot Disease A.
Table 1.
Pathomechanisms and Consequences of Diabetic Foot Disease A.
| Stage/Event | Pathophysiological Description | Physical Consequences | Functional Consequences |
|---|---|---|---|
| 1. Neuropathy (sensory, motor, autonomic) | loss of protective sensation, muscle weakness, dry/cracked skin | foot deformities, skin fissures | increased risk of injury, impaired proprioception, need for rehabilitation |
| 2. Angiopathy (ischemia) | impaired micro- and macrovascular circulation, tissue hypoxia | cold, pale foot, diminished or absent pulses | claudication, poor wound healing, increased risk of amputation revascularization if possible, need for rehabilitation |
| 3. Ulcer formation | due to unnoticed trauma or pressure in insensate areas | chronic wounds, often slow to heal | difficulty walking, need for footwear modification or reduced mobility, need for rehabilitation |
| 4. Infection | rapid bacterial colonization of ulcers, potentially spreading to deep tissues | swelling, redness, abscess, osteomyelitis | hospitalization, immobilization, rehabilitation * |
| 5. Tissue necrosis and gangrene | resulting from uncontrolled infection and/or ischemia | irreversible tissue damage, necrotic areas | surgical intervention or amputation often required, need for rehabilitation |
| 6. Amputation (partial or complete) | removal of necrotic tissue to prevent systemic infection or preserve life/function | loss of limb or part of the limb/foot, postural imbalance | loss of independence, need for rehabilitation, psychological impact, social isolation |
* In cases of sepsis, rehabilitation should be postponed or avoided until the infection is fully controlled. A Sources: Compiled by the authors based on data from [13,40,45,46,47,50,51].
4. The Role of Exercises in the Therapeutic Process of Diabetic Foot Disease
4.1. Multimodal Treatment of DFD
In the event of a complication, such as diabetic foot, the primary goals achieved through appropriate pharmacotherapy include control of glycemia, correction of other risk factors (cholesterol level and blood pressure values), use of antiplatelet drugs, sometimes low doses of anticoagulants (applies to treatment of limb ischemia) and, in justified cases, administration of antibiotics and painkillers.
If necessary, procedures such as revascularization (in the case of vascular lesions), removal of necrotic tissue, or orthopedic interventions should be performed prior to initiating physical exercise [12,17,18,19,20,21,22,23,24,25,26,27,28,29,30]. Physical therapy could also be useful, serving as a complementary approach [52]. Regardless of the above, however, the essential recommended management of ulceration, deformation, and deep tissue inflammation in DFD is the offloading of the affected area [53,54,55]. The goal is to protect damaged tissues from further injury and to promote healing by relieving pressure during loading. Offloading often requires patient immobilization or major activity restriction [53,54], depending on the method used—such as a wheelchair, crutches, special footwear, or a total contact cast (TCC).
Thus, in the described clinical scenario, a therapeutic dilemma emerges. While local pathological changes necessitate offloading—requiring the patient to limit weight-bearing activities such as ambulation and prolonged standing [56]—these same changes, particularly inflammation, simultaneously warrant the implementation of PA, as structured exercise can exert beneficial effects on both the patient’s systemic condition and the local tissue microenvironment [28,29].
In 2023, an expert position was published [57], summarizing the recommended actions for DFD. These actions include an assessment of the usefulness of exercises that the patient may undertake during the treatment of the condition in question. While emphasizing the lack of sufficient evidence that exercise directly accelerates wound healing, the authors recommend performing some of them due to the potential benefits demonstrated both in animals [58,59] and in humans [25].
The possibility of adverse effects is an inherent aspect of any therapy. Improperly conducted exercise may exacerbate local pathological changes and increase the risk of amputation; however, well-organized medical care, adherence to the principles of comprehensive treatment, and timely response to treatment ineffectiveness minimize this risk [31].
The rather modest work on the subject of exercise by patients with diabetic foot to date is supplemented by a recent report [43], released after the publication of the above-mentioned expert study [57]. This study also supported the incorporation of exercise into the therapy of diabetic foot disease. The condition for undertaking exercises is to adhere to the principle of relieving the local change and its surrounding area.
4.2. The Effect of Exercise on the Local Condition in DFD
Prolonged inflammation can lead to bone resorption due to local vasodilation and increased flow in the microcirculation [60]. Long-term offloading can also provoke local osteoporosis and can generate it in other areas of the relieved limb [38]. Each of these disorders has an adverse local impact but also worsens many of the patient’s functions [33,34,35,36,37,38]. The implementation of properly selected exercises can be helpful and have measurable benefits [61,62], preventing further reduction in bone mineral density (BMD), having also a beneficial effect on glycemic control and the patient’s well-being [38].
Even local inflammation [63] causes oxidative stress, which disrupts the repair processes in the wound and has an adverse effect on the entire body, which translates into, for example, increased insulin resistance and, consequently, increased glycemia. This triggers a vicious cycle mechanism as normalization of glycemia is necessary for wound healing. The changes taking place during local infection and their consequences are comprehensively described by Huang et al. [64]. In a hyperglycemic environment, the activity of antioxidant enzymes is reduced, the number of advanced glycation end products (AGEs) increases, which enhances the hypoxia of local tissues, which is further intensified by oxygen-consuming pathogens (in the case of infection) and inflammatory cells [64]. There is data supporting the impact of exercise on the reduction of the severity of local inflammation, regardless of other standard actions taken in this regard [30,65,66,67,68,69]. This is due to the mechanisms activated during exercise, which limit the production of pro-inflammatory cytokines and increase the secretion of anti-inflammatory myokines. The latter also enhances local angiogenesis [70,71], which is essential in the treatment of ischaemic wounds. Lowering excessive blood glucose levels is important at every stage of wound healing, as high glycemia inhibits the proliferation and differentiation of fibroblasts, impairs the secretion of transforming growth factor-β (TGFβ), and reduces collagen synthesis [71].
Additionally, in such a hyperglycemic environment, the activity of endothelial nitric oxide synthase (eNOS) is inhibited, which leads to vascular damage [72]. Hyperglycemia and vascular damage are thus closely related. Moreover, a lack of muscle contraction and joint flexion (natural activities when walking) can cause swelling, which further impedes microcirculatory flow and stiffens joints, reducing their range of motion. Various forms of planned activity, such as Buerger exercises [73,74,75], active range of motion exercises, or stretching [52], contribute to improving local circulation, which creates better conditions for the healing of changes in the foot and prevent muscle atrophy.
Furthermore, improving the ROM is important for the patient’s future [76,77] as its limitation again causes abnormal load on the plantar surface of the foot, callus formation, and an incorrect operation of the muscle pump. However, some of the forms of offloading, such as TCC, may be an obstacle to performing exercises [60]. The necessity of conducting research on an offloading device that does not hinder the involvement of the affected limb in simple exercises was emphasized by the authors of one of the last articles [78].
There is considerable controversy when it comes to exercises during the active phase (open wound or inflammation) [79]. This is understandable considering the fact that most clinical trials are quite old, involve a relatively small number of patients, and are not uniform in their design [55]. This makes them difficult to interpret in terms of patient benefits. Based on the available studies, the existing knowledge is sufficient to consider properly conducted rehabilitation as necessary, even in the acute phase, with the principle of relieving the affected area of the foot and the absence of signs of general infection [80]. Consistent with the above are the aforementioned recently published research results [43], which showed significant improvement in the healing of foot ulcerations in patients with diabetes.
4.3. Impact of Exercises on the General Condition of a Patient with DFD
The benefits of exercise in patients with DFD are both systemic and localized [81,82,83]. Current knowledge about the mechanisms through which various forms of PA regulate different pathological processes or support physiological functions is extensive, and many of these mechanisms are well understood. A detailed summary of this knowledge, including the most recent findings, can be found in the article published by Peng et al. [84], as a detailed discussion of the effects of various forms of PA on patients is beyond the scope of this article.
Overall, the studies confirm that PA in individuals with DM exerts beneficial effects on the cardiovascular and respiratory system [85,86], microcirculation [87,88], or kidneys [89], which is not without significance considering the fact that the correlation between chronic complications and cardiovascular risk has been known for years. Improvements in insulin sensitivity, the patient’s functional and psychological state, and quality of life are also the effects of targeted activity [90].
A key therapeutic principle is the structured implementation of PA, as offloading the foot—provided there are no systemic signs of inflammation—does not necessitate full immobilization of the patient in a bed or a chair.
To perform a large part of daily activities, people involve the lower limbs. When this is limited by a disease, it should be considered whether lower limb muscle activity can be replaced with exercises that exclude the affected area of the foot or include work with the upper limbs or trunk. This is supported by the results of studies that emphasize the role of aerobic exercise in wound healing both in animals [91,92,93,94] and in humans [95], most likely through benefits for the respiratory and cardiovascular systems and improved glucose burning [42,85]. Strength training to prevent atrophy is also helpful in keeping the patient’s muscles in better shape and building muscle mass, which also translates into better glucose utilization and improves muscle tone and coordination of movements [57]. Strengthening the muscles and the patient’s general condition is also of tremendous importance if the treatment of the diabetic foot fails. If amputation and subsequent prosthetics are necessary, the patient’s energy expenditure (EE) when moving is much higher than an able-bodied person [96]. People whose condition indicates a high risk of amputation should be adequately prepared physically so that they can fully use the prosthesis in the future.
4.4. Discussion of Example Exercises for Patients with Diabetic Foot Disease and Contraindications or Precautions for Their Performance
Patients can exercise while sitting or lying down, depending on their overall health and the location of the ulcer. Ankle mobility exercises, such as plantar and dorsal flexion (including toes, separately), pronation and inversion or foot circles are safe and easy to perform, even for elderly people. Their role is to maintain or improve blood flow and joint mobility, they have an antithrombotic and anti-swelling effect. There are also no contraindications to performing simple exercises involving the larger joints of the lower limb (such as alternating flexion/extension at the knee or hip joint or the so-called bicycle exercise while lying on the back). In patients with heel ulcers, a prerequisite during such exercises is the ability to lift the heel during movement, for example, when bending at the knee joint, so that the patient does not rub the affected area on the ground.
Patients with an ischemic foot may also (if they tolerate pain or take pain medication) raise their lower limb and perform the exercises in that position. This is an element of the Buerger [73,74,75] exercises recommended for leg ischemia.
In the absence of contraindications to loading (e.g., when the wound involves the dorsum of the foot) a standing or at least sitting position is recommended. Energy expenditure is approximately 10% higher in the standing position compared to when a person is sitting or lying [97], therefore the change in the patient’s position should be considered beneficial for the degree of glucose utilization.
Exercises can also be performed with the involvement of the upper extremities. Strengthening the muscles of the rim and the free upper limb, apart from its overall impact on the patient’s well-being, respiratory and circulatory systems, is useful due to the patient’s potential need to move in a wheelchair or on crutches if the treatment fails and amputation is necessary [98]. The work of the arms seems to be as burdensome for the body as the work performed using the lower limbs [99], with even better synchronization of breathing with the movements of the upper limbs (vs lower limbs) during submaximal exercises [100]. However, whenever possible, patients should be encouraged to perform dynamic exercises using both the upper and lower extremities (e.g., non-weight bearing combined arm + leg cycling), if only due to the accompanying higher energy expenditure and effect on aerobic conditioning necessary with other limited types of activities [101].
Isometric exercises (alternate tensing and relaxing of muscle parts, without changing the distance of their attachments) are also a frequently used form of rehabilitation when one is unable to move or as a supplement to dynamic exercises. Due to the lack of need for additional movements, they can be performed by people with low physical fitness and poor physical condition, thus easily improving muscle strength and blood flow. Tensing muscles should be avoided in the area where sutures are placed (e.g., to bring the edges of a wound closer or minor amputation) or in the area of fractures (Charcot’s foot) so as not to cause the bones to shift relative to each other due to the tensing of the muscles. The undoubted advantage of the exercises is that they can also be performed in situations of permanent immobilization, with dressings often used for the purpose of offloading.
Learning to walk using crutches remains an element of rehabilitation, both in terms of utility (a way to move around without burdening the affected foot) and EE. Walking on crutches on flat ground or up the stairs is an effort of about 4.5 and 5.0 metabolic equivalents (METs), respectively [102]. Therefore, patients should not be persuaded to use electric wheelchairs for no reason, especially to cover short distances.
Calisthenics strengthens muscles and leads to an additional EE and good heart rate (HR) response [103]. Simple muscle-strengthening exercises, like bedside squats (only when the wound is on the upper part of the foot) [104], sit-ups, or other forms of muscle strengthening using simple instruments, such as stretching rubber bands, squeezing rubber balls, and upper limb exercises with weights, are useful in working with patients. Their role often seems small and is underestimated but the intensity of chair-assisted exercises, for example, could be at least moderate, and these exercises can give about 61% of VO2max, 67% HRmax, and about 3.9 METs loading [104].
In addition to the above-mentioned exercises, patients with foot deformity without ulceration can perform low-intensity aerobic exercises in standing or walking position after fitting an orthotic, if necessary, or with the use of made-to-measure shoes or individual orthotics. If such exercises are performed on a bicycle, the orthosis must be adapted to the foot deformity, and the need to redistribute the pressure of the sole on the pedals should also be taken into account [57]. A good exercise environment for people with deformities without ulceration is water [57].
Table 2 presents examples of simple exercises that can be performed by patients with DFD. The proposed exercises are original and reflect the authors’ clinical approach to rehabilitation in DFD.

Table 2.
Type and examples of exercises that may benefit patients with diabetic foot disease A.
Analyzing the recent reports, it is worth mentioning the possibilities offered by virtual therapy. The impact of some forms of virtual training on aerobic capacity, functional lower-limb strength, reaction time, and pain reduction have been documented [105]. This new and still experimental form of rehabilitation takes advantage of the well-known physiological phenomenon of activating the neural networks of the cerebral cortex and cerebral subcortex, which contain the so-called mirror neurons. After watching an exercise being performed (the element of virtual therapy), its performance is simpler and more correct due to the enhancing adaptive neuroplasticity mechanisms [106]. Although there are no studies for patients with limited mobility due to the diabetic foot, various research using mirror neuron-based therapy have proved its effectiveness on several motor functions in populations with neurological diseases [107,108,109,110], and it seems reasonable to preliminarily extrapolate the obtained results to patients with DM and foot problems until that population is studied. The introduction of virtual reality-based therapy can be an additional tool in the effective use of rehabilitation time in the aforementioned group of people, without the risk of tissue damage or other side effects.
After the ulcer has healed and the inflammation has subsided, the patient may continue the exercises performed during the acute phase of the complication. At this stage, it is also possible to introduce additional exercises with full weight-bearing activities. However, it should be taken into account that the previously affected area remains vulnerable to re-injury. For this reason, patients should protect their feet from mechanical, biological, and thermal factors by special care and by using appropriate insoles or individually fitted footwear. During the recovery phase, it is also advisable to consider vascular procedures—if they could not be performed earlier—as well as orthopedic interventions to correct foot deformities, where possible.
5. Conclusions
Given the absence of evidence indicating harm from properly performed exercises in patients with diabetic foot disease, and considering their documented systemic and, in some cases, local benefits, physical activity should be incorporated into DFD management. Importantly, exercises should not be limited to the affected limb. Activating other body regions can counteract the negative systemic effects of immobilization. Exercise types may include aerobic, anaerobic, isometric, calisthenics, stretching, and active joint mobility exercises, selected based on the location and severity of the foot lesions, offloading method, pain presence, and the patient’s general condition. A clearly structured, individualized exercise plan should be developed at the beginning of treatment and adjusted as the patient’s condition evolves.
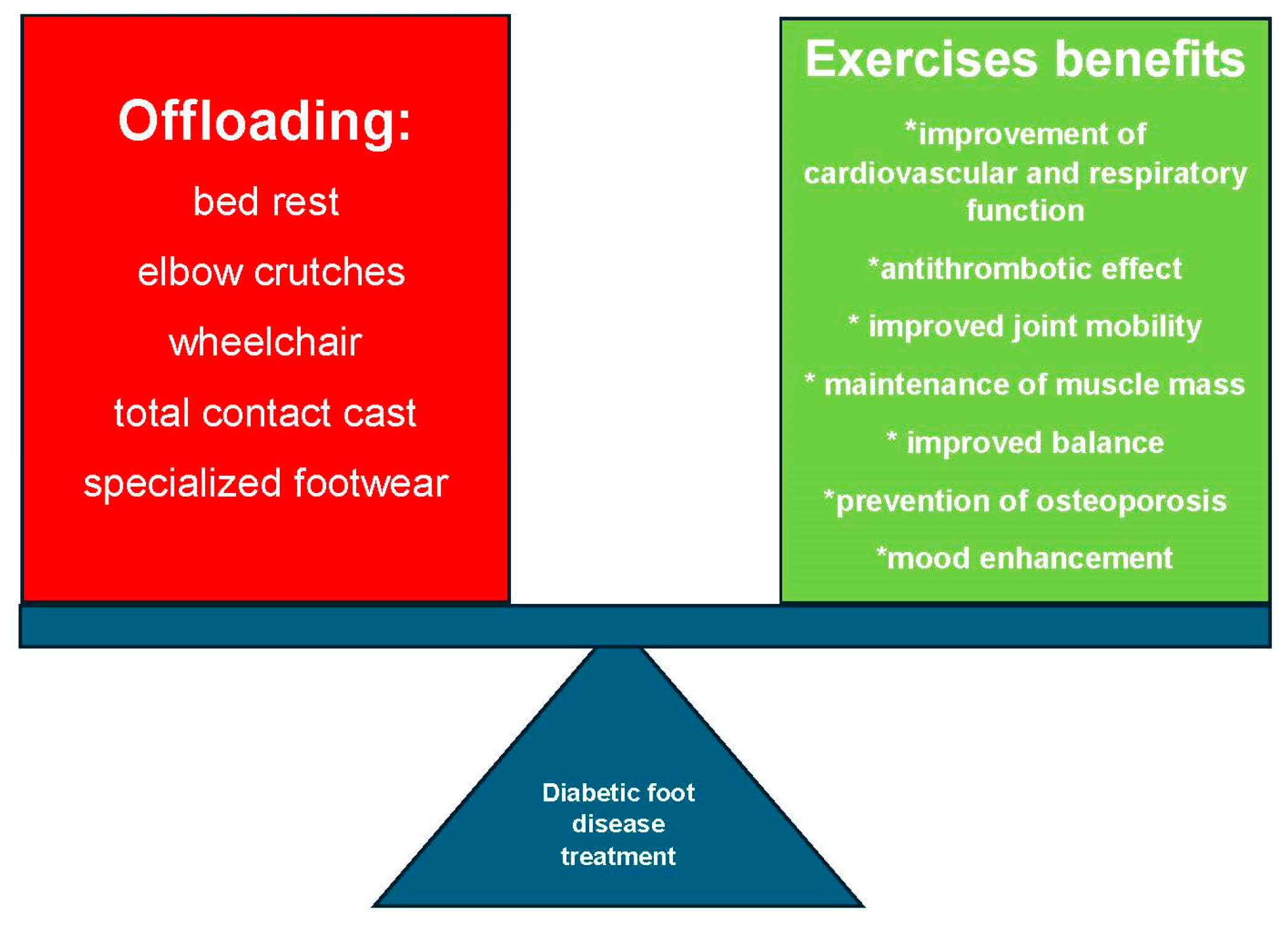
The decision to include exercises and reassurance of their safety by medical staff strongly influences patient engagement. Effective rehabilitation requires an interdisciplinary approach and structured patient education to improve compliance and outcomes while minimizing complications. Figure 1 illustrates the need to balance local offloading with systemic and targeted PA—both essential to optimal DFD therapy.
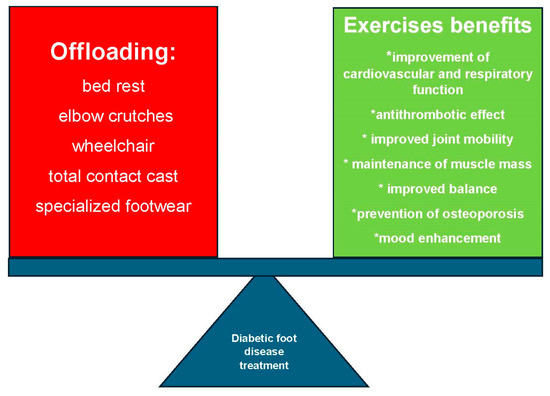
Figure 1.
Balance between Offloading and Exercise in Diabetic Foot Disease (DFD).
Although high-quality RCTs on exercise interventions in DFD remain limited—mainly due to methodological challenges—small, well-designed interventional studies offer valuable insights and can support future meta-analyses.
Author Contributions
E.S.: conceptualization; funding acquisition (publication fee); supervision; writing—original draft; writing—review and editing. A.K.-B.: funding acquisition (publication fee); writing—review and editing. K.B.: writing—original draft. All authors have read and agreed to the published version of the manuscript.
Funding
Wroclaw Medical University and Medical University of Gdansk covered the publication fee.
Conflicts of Interest
The authors declare no conflicts of interest. The funders had no role in the design of the article and its preparation.
References
- Chen, L.; Pei, J.H.; Kuang, J.; Chen, H.-M.; Chen, Z.; Li, Z.-W.; Yang, H. Effect of lifestyle intervention in patients with type 2 diabetes: A meta-analysis. Metabolism 2015, 64, 338–347. [Google Scholar] [CrossRef] [PubMed]
- Thomas, D.E.; Elliott, E.J.; Naughton, G.A. Exercise for type 2 diabetes mellitus. In Cochrane Database of Systematic Reviews; John Wiley & Sons: Hoboken, NJ, USA, 2006. [Google Scholar] [CrossRef]
- American Diabetes Association. Standards of medical care in diabetes—2021. Diabetes Care 2021, 44 (Suppl. S1), S15–S33. [Google Scholar] [CrossRef] [PubMed]
- Hu, F.B. Globalization of Diabetes. Diabetes Care 2011, 34, 1249–1257. [Google Scholar] [CrossRef] [PubMed]
- Little, J.P.; Francois, M.E. High-intensity interval training for improving postprandial hyperglycemia. Res. Q. Exerc. Sport 2014, 85, 451–456. [Google Scholar] [CrossRef] [PubMed]
- Mann, S.; Beedie, C.; Balducci, S.; Zanuso, S.; Allgrove, J.; Bertiato, F.; Jimenez, A. Changes in insulin sensitivity in response to different modalities of exercise: A review of the evidence. Diabetes Metab. Res. Rev. 2014, 30, 257–268. [Google Scholar] [CrossRef] [PubMed]
- Shaban, N.; Kenno, K.A.; Milne, K.J. The effects of a 2 week modified high intensity interval training program on the homeostatic model of insulin resistance (HOMA-IR) in adults with type 2 diabetes. J. Sport. Med. Phys. Fit. 2014, 54, 203–209. [Google Scholar]
- Kilgour, A.H.M.; Rutherford, M.; Higson, J.; Meredith, S.J.; McNiff, J.; Mitchell, S.; Wijayendran, A.; Lim, S.E.R.; Shenkin, S.D. Barriers and motivators to undertaking physical activity in adults over 70—A systematic review of the quantitative literature. Age Ageing 2024, 53, afae080. [Google Scholar] [CrossRef] [PubMed]
- Biernat, K.; Marciniak, D.M.; Mazurek, J.; Kuciel, N.; Hap, K.; Kisiel, M.; Sutkowska, E. The Level and Limitations of Physical Activity in Elderly Patients with Diabetes. J. Clin. Med. 2024, 13, 6329. [Google Scholar] [CrossRef] [PubMed]
- Ajzen, I. The theory of planned behavior. Organ. Behav. Hum. Decis. Process. 1991, 50, 179–211. [Google Scholar] [CrossRef]
- Sutkowska, E.; Biernat, K.; Mazurek, J.; Hap, K.; Kuciel, N.; Sutkowska, M.; Marciniak, D. Level and limitations of physical activity in patients with excess body weight or diabetes. BMJ Open Sport Exerc. Med. 2024, 10, e002041. [Google Scholar] [CrossRef] [PubMed]
- van Netten, J.J.; Bus, S.A.; Apelqvist, J.; Lipsky, B.A.; Hinchliffe, R.J.; Game, F.; Jeffcoate, W.; Jirkovska, A.; Malone, M.; Rasmussen, A.; et al. Definitions and Criteria for Diabetic Foot Disease. IWGDF Guidelines. Available online: https://iwgdfguidelines.org/wp-content/uploads/2019/05/definitions-and-criteria-final.pdf (accessed on 28 May 2025).
- Armstrong, D.G.; Boulton, A.J.M.; Bus, S.A. Diabetic Foot Ulcers and Their Recurrence. N. Engl. J. Med. 2017, 376, 2367–2375. [Google Scholar] [CrossRef] [PubMed]
- Singh, N.; Armstrong, D.G.; Lipsky, B.A. Preventing foot ulcers in patients with diabetes. JAMA 2005, 293, 217–228, International Working Group on the Diabetic Foot (IWGDF) Guidelines. Available online: https://iwgdfguidelines.org/ (accessed on 10 July 2025). [CrossRef] [PubMed]
- WHO/IDF Saint Vincent Declaration Working Group. Diabetes mellitus in Europe: A problem at all ages in all countries. A model for prevention and self care. Acta Diabetol. 1990, 27, 181–183. [Google Scholar]
- Kong, M.F.; Gregory, R. Preventing foot complications in diabetes: The St Vincent Declaration 26 years on. Pract. Diabetes 2016, 33, 154–156. [Google Scholar] [CrossRef]
- Matos, M.; Mendes, R.; Silva, A.B.; Sousa, N. Physical activity and exercise on diabetic foot related outcomes: A systematic review. Diabetes Res. Clin. Pract. 2018, 139, 81–90. [Google Scholar] [CrossRef] [PubMed]
- Mueller, M.J.; Tuttle, L.J.; Lemaster, J.W.; Strube, M.J.; McGill, J.B.; Hastings, M.K.; Sinacore, D.R. Weight-bearing versus nonweight-bearing exercise for persons with diabetes and peripheral neuropathy: A randomized controlled trial. Arch. Phys. Med. Rehabil. 2013, 94, 829–838. [Google Scholar] [CrossRef] [PubMed]
- Sartor, C.D.; Hasue, R.H.; Cacciari, L.P.; Butugan, M.K.; Watari, R.; Pássaro, A.C.; Giacomozzi, C.; Sacco, I.C.N. Effects of strengthening, stretching and functional training on foot function in patients with diabetic neuropathy: Results of a randomized controlled trial. BMC Musculoskelet. Disord. 2014, 15, 137. [Google Scholar] [CrossRef] [PubMed]
- Lemaster, J.W.; Mueller, M.J.; Reiber, G.E.; Mehr, D.R.; Madsen, R.W.; Conn, V.S. Effect of weight-bearing activity on foot ulcer incidence in people with diabetic peripheral neuropathy: Feet first randomized controlled trial. Phys. Ther. 2008, 88, 1385–1398. [Google Scholar] [CrossRef] [PubMed]
- Balducci, S.; Iacobellis, G.; Parisi, L.; Di Biase, N.; Calandriello, E.; Leonetti, F.; Fallucca, F. Exercise training can modify the natural history of diabetic peripheral neuropathy. J. Diabetes Complicat. 2006, 20, 216–223. [Google Scholar] [CrossRef] [PubMed]
- Dixit, S.M.; Maiya, A.G.; Shastry, B.A. Effect of aerobic exercise on peripheral nerve functions of population with diabetic peripheral neuropathy in type 2 diabetes: A single blind, parallel group randomized controlled trial. J. Diabetes Complicat. 2014, 28, 332–339. [Google Scholar] [CrossRef] [PubMed]
- Francia, P.; Anichini, R.; De Bellis, A.; Seghieri, G.; Lazzeri, R.; Paternostro, F. Gulisano, M Diabetic foot prevention: The role of exercise therapy in the treatment of limited joint mobility, muscle weakness and reduced gait speed. Ital. J. Anat. Embryol. 2015, 120, 21–32. [Google Scholar] [PubMed]
- Tran, M.M.; Haley, M.N. Does exercise improve healing of diabetic foot ulcers? A systematic review. J. Foot Ankle Res. 2021, 14, 19. [Google Scholar] [CrossRef] [PubMed]
- Eraydin, S.; Avşar, G. The effect of foot exercises on wound healing in type 2 diabetic patients with a foot ulcer: A randomized control study. J. Wound Ostomy Cont. Nurs. 2018, 45, 123–130. [Google Scholar] [CrossRef] [PubMed]
- Rietz, M.; Lehr, A.; Mino, E.; Lang, A.; Szczerba, E.; Schiemann, T.; Herder, C.; Saatmann, N.; Geidl, W.; Barbaresko, J.; et al. Physical Activity and Risk of Major Diabetes-Related Complications in Individuals with Diabetes: A Systematic Review and Meta-Analysis of Observational Studies. Diabetes Care 2022, 45, 3101–3111. [Google Scholar] [CrossRef] [PubMed]
- Nguyen, V.; Dinh, Q.; Yu, F.; Jia, S.; Wang, X. Interventional effects of exercise on neuropathy in patients with diabetes: A systematic review with meta-analysis. BMC Sports Sci. Med. Rehabil. 2025, 17, 82. [Google Scholar] [CrossRef] [PubMed]
- Lyu, X.; Li, S.; Peng, S.; Cai, H.; Liu, G.; Ran, X. Intensive walking exercise for lower extremity peripheral arterial disease: A systematic review and meta-analysis. J. Diabetes 2016, 8, 363–377. [Google Scholar] [CrossRef] [PubMed]
- Singh, S.; Young, A.; McNaught, C.E. The physiology of wound healing. Surgery 2017, 35, 473–477. [Google Scholar] [CrossRef]
- Cañedo-Dorantes, L.; Cañedo-Ayala, M. Skin acute wound healing: A comprehensive review. Int. J. Inflamm. 2019, 2019, 3706315. [Google Scholar] [CrossRef] [PubMed]
- Aagaard, T.V.; Moeini, S.; Skou, S.T.; Madsen, U.R.; Brorson, S. Benefits and harms of exercise therapy for patients with diabetic foot ulcers: A systematic review. Int. J. Low. Extrem. Wounds 2020, 21, 219–233. [Google Scholar] [CrossRef] [PubMed]
- Otranto, M.; Nascimento, A.P.; Monte-Alto-Costa, A. Insulin resistance impairs cutaneous wound healing in mice. Wound Repair Regen. 2013, 21, 464–472. [Google Scholar] [CrossRef] [PubMed]
- Winget, C.M.; Deroshia, C.W. Psychosocial and Chronophysiological Effects of Inactivity and Immobilization. In Inactivity: Physiological Effects; Sandler, H., Vernikos, J., Eds.; Academic Press: Cambridge, MA, USA, 1986; pp. 123–147. [Google Scholar]
- Garber, C.E.; Blissmer, B.; Deschenes, M.R.; Franklin, B.A.; Lamonte, M.J.; Lee, I.-M.; Nieman, D.C.; Swain, D.P. Quantity and quality of exercise for developing and maintaining cardiorespiratory, musculoskeletal, and neuromotor fitness in apparently healthy adults: Guidance for prescribing exercise. Med. Sci. Sports Exerc. 2011, 43, 1334–1359. [Google Scholar] [CrossRef] [PubMed]
- Bull, F.C.; Al-Ansari, S.S.; Biddle, S.; Borodulin, K.; Buman, M.P.; Cardon, G.; Carty, C.; Chaput, J.-P.; Chastin, S.; Chou, R.; et al. World Health Organization 2020 guidelines on physical activity and sedentary behaviour. Br. J. Sports Med. 2020, 54, 1451–1462. [Google Scholar] [CrossRef] [PubMed]
- Greenleaf, J.E.; Kozlowski, S. Physiological consequences of reduced physical activity during bed rest. Exerc. Sport Sci. Rev. 1982, 10, 84–119. [Google Scholar] [CrossRef] [PubMed]
- Zhang, S.; Huang, X.; Zhao, X.; Li, B.; Cai, Y.; Liang, X.; Wan, Q. Effect of exercise on bone mineral density among patients with osteoporosis and osteopenia: A systematic review and network meta-analysis. J. Clin. Nurs. 2022, 31, 2100–2111. [Google Scholar] [CrossRef] [PubMed]
- Nejatian, M.M.; Sobhi, S.; Sanchez, B.N.; Linn, K.; Manning, L.; Soh, S.-C.; Hiew, J.; Ritter, J.C.; Yeap, B.B.; Hamilton, E.J.; et al. Reduction in femoral neck and total hip bone mineral density following hospitalisation for diabetes-related foot ulceration. Sci. Rep. 2021, 11, 22742. [Google Scholar] [CrossRef] [PubMed]
- Colberg, S.R.; Sigal, R.J.; Yardley, J.E.; Riddell, M.C.; Dunstan, D.W.; Dempsey, P.C.; Horton, E.S.; Castorino, K.; Tate, D.F. Physical Activity/Exercise and Diabetes: A Position Statement of the American Diabetes Association. Diabetes Care 2016, 39, 2065–2079. [Google Scholar] [CrossRef] [PubMed]
- Wound Healing Interventions Guideline (2023 Update). Available online: https://iwgdfguidelines.org/wound-healing-2023/ (accessed on 28 May 2025).
- Wendland, D.M.; Altenburger, E.A.; Swen, S.B.; Haan, J.D. Diabetic Foot Ulcer Beyond Wound Closure: Clinical Practice Guideline. Phys. Ther. 2025, 105, pzae171. [Google Scholar] [CrossRef] [PubMed] [PubMed Central]
- Wendland, D.M.; Kline, P.W.; Simmons, L.; Sinacore, D.R. The effect of exercise, physical activity, stepping characteristics, and loading on diabetic foot ulcer healing: A systematic review. Wounds 2023, 35, 9–17. [Google Scholar] [CrossRef] [PubMed]
- Nayak, D.; Ray, R.; Anand, C.; Baruah, T.D.; Goyal, A. Protocolized Foot Exercises Help in Improvement of Diabetic Foot Ulcers and Quality of Life When Added to Standard Therapy–A Randomized Clinical Trial. Int. J. Low. Extrem. Wounds 2024, 15347346241262591. [Google Scholar] [CrossRef] [PubMed]
- Sekhar, M.S.; Thomas, R.R.; Unnikrishnan, M.K.; Vijayanarayana, K.; Rodrigues, G.S. Impact of diabetic foot ulcer on health-related quality of life: A cross-sectional study. Semin. Vasc. Surg. 2015, 28, 165–171. [Google Scholar] [CrossRef] [PubMed]
- Najafi, B.; Mohseni, H.; Wrobel, J.S. Functional deficits in diabetic foot patients with and without neuropathy. J. Diabetes Res. 2021, 2021, 6636030. [Google Scholar]
- D’Silva, S.; Ziarno, N.; Kluding, P. Postural instability and diabetic peripheral neuropathy: A review. J. Diabetes Complicat. 2020, 34, 107469. [Google Scholar] [CrossRef]
- Morone, G.; Bragazzi, N.L.; Invernizzi, M.; Fusco, A.; Paolucci, T.; Paci, M. Biomechanical alterations in diabetic neuropathic foot: Impact on balance and gait. Clin. Biomech. 2022, 87, 105446. [Google Scholar] [CrossRef]
- Sinacore, D.R.; Riddle, D.L.; Mueller, M.J. Muscle and joint impairments in diabetic neuropathy and their impact on function. J. Am. Podiatr. Med. Assoc. 2018, 108, 205–213. [Google Scholar] [CrossRef]
- Wukich, D.K.; Sung, W. Bone and joint disorders in diabetic foot disease. Diabetes Metab. Res. Rev. 2021, 37, e3402. [Google Scholar] [CrossRef]
- Lavery, L.A.; Armstrong, D.G.; Murdoch, D.P.; Peters, E.J.; Lipsky, B.A. Effect of diabetic foot ulcers on patient independence and quality of life. Diabetes Metab. Res. Rev. 2020, 36, e3294. [Google Scholar] [CrossRef]
- Prompers, L.; Schaper, N.; Apelqvist, J.; Edmonds, M.; Jude, E.; Mauricio, D.; Uccioli, L.; Urbancic, V.; Bakker, K.; Holstein, P.; et al. Functional consequences of diabetic foot disease: A systematic review. Diabetologia 2023, 66, 367–375. [Google Scholar] [CrossRef]
- Turan, Y.; Ertugrul, B.M.; Lipsky, B.A.; Bayraktar, K. Does physical therapy and rehabilitation improve outcomes for diabetic foot ulcers? World J. Exp. Med. 2015, 5, 130–139. [Google Scholar] [CrossRef] [PubMed]
- Ibrahim, A.; Jude, E.; Langton, K.; Martínez-De Jesus, F.R.; Harkless, L.B.; Gawish, H.; Huang, Y.Y.; Labovitz, J.; Xu, Z.; Pendsey, S.; et al. IDF Clinical Practice Recommendations on the Diabetic Foot—2017. A Guide for Healthcare Professionals. Available online: https://idf.org/media/uploads/2023/05/attachments-61.pdf (accessed on 2 August 2024).
- Faglia, E.; Caravaggi, C.; Clerici, G.; Sganzaroli, A.; Curci, V.; Vailati, W.; Simonetti, D.; Sommalvico, F.; Manzoli, L.; Giurato, L.; et al. Effectiveness of removable walker cast versus nonremovable fiberglass off-bearing cast in the healing of diabetic plantar foot ulcer: A randomized controlled trial. Diabetes Care 2010, 33, 1419–1423. [Google Scholar] [CrossRef] [PubMed]
- Jones, K.; Backhouse, M.R.; Bruce, J. Rehabilitation for people wearing offloading devices for diabetes-related foot ulcers: A systematic review and meta-analyses. J. Foot Ankle Res. 2023, 16, 16. [Google Scholar] [CrossRef] [PubMed]
- Najafi, B.; Grewal, G.S.; Bharara, M.; Menzies, R.; Talal, T.K.; Armstrong, D.G. Can’t Stand the Pressure: The Association Between Unprotected Standing, Walking, and Wound Healing in People with Diabetes. J. Diabetes Sci. Technol. 2017, 11, 657–667. [Google Scholar] [CrossRef] [PubMed]
- Gracia-Sánchez, A.; López-Pineda, A.; Lázaro-Martínez, J.L.; Pérez, A.; Pomares-Gómez, F.J.; Fernández-Seguín, L.M.; Martínez-de-Quel, Ó.; Montero, P.; Suso-Ribera, C.; Ortega-Avila, A.J.; et al. Consensus-based recommendations on physical activity and exercise in patients with diabetes at risk of foot ulcerations: A Delphi study. Braz. J. Phys. Ther. 2023, 27, 100500. [Google Scholar] [CrossRef] [PubMed]
- Pence, B.D.; Woods, J.A. Exercise, obesity, and cutaneous wound healing: Evidence from rodent and human studies. Adv. Wound Care 2014, 3, 71–79. [Google Scholar] [CrossRef] [PubMed]
- Keylock, T.; Meserve, L.; Wolfe, A. Low-intensity Exercise Accelerates Wound Healing in Diabetic Mice. Wounds 2018, 30, 68–71. [Google Scholar] [PubMed]
- Rogers, L.C.; Frykberg, R.G.; Armstrong, D.G.; Boulton, A.J.M.; Edmonds, M.; Ha Van, G.; Hartemann, A.; Game, F.; Jeffcoate, W.; Jirkovska, A.; et al. The Charcot foot in diabetes. Diabetes Care 2011, 34, 2123–2129. [Google Scholar] [CrossRef] [PubMed]
- Aitken, E.; Hiew, J.; Hamilton, E.J.; Manning, L.; Ritter, J.C.; Raby, E.; Gittings, P.M. Exercise in adults admitted to hospital with diabetes-related foot ulcers: A pilot study of feasibility and safety. J. Foot Ankle Res. 2023, 16, 18. [Google Scholar] [CrossRef] [PubMed]
- Kanade, R.V.; van Deursen, R.W.; Harding, K.; Price, P. Walking performance in people with diabetic neuropathy: Benefits and threats. Diabetologia 2006, 49, 1747–1754. [Google Scholar] [CrossRef] [PubMed]
- Mathur, N.; Pedersen, B.K. Exercise as a means to control low-grade systemic inflammation. Mediat. Inflamm. 2008, 2008, 109502. [Google Scholar] [CrossRef] [PubMed]
- Huang, H.; Xin, R.; Li, X.; Zhang, X.; Chen, Z.; Zhu, Q.; Tai, Z.; Bao, L. Physical therapy in diabetic foot ulcer: Research progress and clinical application. Int. Wound J. 2023, 20, 3417–3434. [Google Scholar] [CrossRef] [PubMed]
- Pedersen, B.K. Anti-inflammatory effects of exercise: Role in diabetes and cardiovascular disease. Eur. J. Clin. Investig. 2017, 47, 600–611. [Google Scholar] [CrossRef] [PubMed]
- Herder, C.; Peltonen, M.; Koenig, W.; Sütfels, K.; Lindström, J.; Martin, S.; Ilanne-Parikka, P.; Eriksson, J.G.; Aunola, S.; Keinänen-Kiukaanniemi, S.; et al. Anti-inflammatory effect of lifestyle changes in the Finnish Diabetes Prevention Study. Diabetologia 2009, 52, 433–442. [Google Scholar] [CrossRef] [PubMed]
- Yates, T.; Davies, M.J.; Gorely, T.; Talbot, D.; Bull, F.; Sattar, N.; Khunti, K. The effect of increased ambulatory activity on markers of chronic low-grade inflammation: Evidence from the PREPARE programme randomized controlled trial. Diabet. Med. 2010, 27, 1256–1263. [Google Scholar] [CrossRef] [PubMed]
- Zheng, G.; Qiu, P.; Xia, R.; Lin, H.; Ye, B.; Tao, J.; Chen, L.; Zhang, Y.; Wang, Y.; Liu, J.; et al. Effect of aerobic exercise on inflammatory markers in healthy middle-aged and older adults: A systematic review and meta-analysis of randomized controlled trials. Front. Aging Neurosci. 2019, 11, 98. [Google Scholar] [CrossRef] [PubMed]
- Taherkhani, S.; Suzuki, K.; Castell, L. A short overview of changes in inflammatory cytokines and oxidative stress in response to physical activity and antioxidant supplementation. Antioxidants 2020, 9, 886. [Google Scholar] [CrossRef] [PubMed]
- Pedersen, B.K.; Åkerström, T.C.A.; Nielsen, A.R.; Fischer, C.P. Role of myokines in exercise and metabolism. J. Appl. Physiol. 2007, 103, 1093–1098. [Google Scholar] [CrossRef] [PubMed]
- Sharma, S.; Schaper, N.; Rayman, G. Microangiopathy: Is it relevant to wound healing in diabetic foot disease? Diabetes Metab. Res. Rev. 2020, 36, e3244. [Google Scholar] [CrossRef] [PubMed]
- Versey, Z.; da Cruz Nizer, W.S.; Russell, E.; Zigic, S.; DeZeeuw, K.G.; Marek, J.E.; Overhage, J.; Cassol, E. Biofilm-innate immune Interface: Contribution to chronic wound formation. Front. Immunol. 2021, 12, 648554. [Google Scholar] [CrossRef] [PubMed]
- Lin, B.S.; Chang, C.C.; Su, C.L.; Li, J.-R.; Chen, M.-L.; Chen, M.-Y.; Huang, Y.-K. The assessment of Buerger’s exercise on dorsal foot skin circulation in patients with vasculopathic diabetic foot ulcer by using wireless near-infrared spectroscope: A cohort prospective study. Lasers Med. Sci. 2018, 33, 977–982. [Google Scholar] [CrossRef] [PubMed]
- Chang, C.C.; Chen, M.Y.; Shen, J.H.; Lin, Y.B.; Hsu, W.W.; Lin, B.S. A quantitative real-time assessment of Buerger exercise on dorsal foot peripheral skin circulation in patients with diabetes foot. Medicine 2016, 95, e5334. [Google Scholar] [CrossRef] [PubMed]
- Chang, C.F.; Chang, C.C.; Hwang, S.L.; Chen, M.Y. Effects of Buerger Exercise Combined Health-Promoting Program on Peripheral Neurovasculopathy Among Community Residents at High Risk for Diabetic Foot Ulceration. Worldviews Evid.-Based Nurs. 2015, 12, 145–153. [Google Scholar] [CrossRef] [PubMed]
- Chao, C.Y.L.; Zheng, Y.-P.; Cheing, G.L.Y. Epidermal thickness and biomechanical properties of plantar tissues in diabetic foot. Ultrasound Med. Amp. Biol. 2011, 37, 1029–1038. [Google Scholar] [CrossRef] [PubMed]
- Goldsmith, J.R.; Lidtke, R.H.; Shott, S. The effects of range-of-motion therapy on the plantar pressures of patients with diabetes mellitus. J. Am. Podiatr. Med. Assoc. 2002, 92, 483–490. [Google Scholar] [CrossRef] [PubMed]
- Jarl, G.; van Netten, J.J.; Lazzarini, P.A.; Crews, R.T.; Najafi, B.; Mueller, M.J. Should weight-bearing activity be reduced during healing of plantar diabetic foot ulcers, even when using appropriate offloading devices? Diabetes Res. Clin. Pract. 2021, 175, 108733. [Google Scholar] [CrossRef] [PubMed]
- Coombes, B.K.; Sierra-Silvestre, E.; Bisset, L.M.; Mielke, G.I.; Ware, R.S.; Coombes, J.S.; Burton, N.W. Pain exacerbation following physical activity in adults with diabetic neuropathy: Ecological momentary assessment of foot symptoms. Aust. J. Gen. Pract. 2024, 53, 93–98. [Google Scholar] [CrossRef] [PubMed]
- Franklin, B.A.; Eijsvogels, T.M.H.; Pandey, A.; Quindry, J.; Toth, P.P. Physical activity, cardiorespiratory fitness, and cardiovascular health: A clinical practice statement of the ASPC Part I: Bioenergetics, contemporary physical activity recommendations, benefits, risks, extreme exercise regimens, potential maladaptations. Am. J. Prev. Cardiol. 2022, 12, 100424. [Google Scholar] [CrossRef] [PubMed]
- Fiuza-Luces, C.; Garatachea, N.; Berger, N.A.; Lucia, A. Exercise is the real polypill. Physiology 2013, 28, 330–358. [Google Scholar] [CrossRef] [PubMed]
- Lee, I.M.; Shiroma, E.J.; Lobelo, F.; Puska, P.; Blair, S.N.; Katzmarzyk, P.T.; Alkandari, J.R.; Andersen, L.B.; Bauman, A.E.; Brownson, R.C.; et al. Effect of physical inactivity on major non-communicable diseases worldwide: An analysis of burden of disease and life expectancy. Lancet 2012, 380, 219–229. [Google Scholar] [CrossRef] [PubMed]
- Pedersen, B.K.; Saltin, B. Exercise as medicine—Evidence for prescribing exercise as therapy in 26 different chronic diseases. Scand. J. Med. Sci. Sports 2015, 25, 1–72. [Google Scholar] [CrossRef]
- Peng, C.J.; Chen, S.; Yan, S.J.; Zhao, J.N.; Luo, Z.W.; Qian, Y.; Zhao, G.L. Mechanism underlying the effects of exercise against type 2 diabetes: A review on research progress. World J. Diabetes 2024, 15, 1704–1720. [Google Scholar] [CrossRef] [PubMed]
- Lin, X.; Zhang, X.; Guo, J.; Roberts, C.K.; McKenzie, S.; Wu, W.-C.; Liu, S.; Song, Y. Effects of exercise training on cardiorespiratory fitness and biomarkers of cardiometabolic health: A systematic review and meta-analysis of randomized controlled trials. J. Am. Heart Assoc. 2015, 4, e002014. [Google Scholar] [CrossRef] [PubMed]
- Hafstad, A.D.; Lund, J.; Handler-Olsen, E.; Höper, A.C.; Larsen, T.S.; Aasum, E. High- and moderate-intensity training normalizes ventricular function and mechanoenergetics in mice with diet-induced obesity. Diabetes 2013, 62, 2287–2294. [Google Scholar] [CrossRef] [PubMed]
- Laughlin, M.H. Physical activity-induced remodeling of vasculature in skeletal muscle: Role in treatment of type 2 diabetes. J. Appl. Physiol. 2016, 120, 1–16. [Google Scholar] [CrossRef] [PubMed]
- Olver, T.D.; Laughlin, M.H. Endurance, interval sprint, and resistance exercise training: Impact on microvascular dysfunction in type 2 diabetes. Am. J. Physiol. Heart Circ. Physiol. 2016, 310, H337–H350. [Google Scholar] [CrossRef] [PubMed]
- Nataraj, M.; Maiya, G.A.; Nagaraju, S.P.; Shastry, B.A.; Shivashankara, K.N.; Shetty, S.; Mayya, S.S. Effect of exercise-based rehabilitation on functional capacity and renal function in type 2 diabetes mellitus with nephropathy: A randomized controlled trial. Int. Urol. Nephrol. 2024, 56, 2671–2682. [Google Scholar] [CrossRef] [PubMed]
- Amaravadi, S.K.; Maiya, G.A.; Vaishali, K.; Shastry, B.A. Effectiveness of structured exercise program on insulin resistance and quality of life in type 2 diabetes mellitus—A randomized controlled trial. PLoS ONE 2024, 19, e0302831. [Google Scholar] [CrossRef] [PubMed]
- Keylock, K.T.; Vieira, V.J.; Wallig, M.A.; DiPietro, L.; Schrementi, M.; Woods, J.A. Exercise accelerates cutaneous wound healing and decreases wound inflammation in aged mice. Am. J. Physiol. Regul. Integr. Comp. Physiol. 2008, 294, 179–184. [Google Scholar] [CrossRef] [PubMed]
- Zogaib, F.G.; Monte-Alto-Costa, A. Moderate intensity physical training accelerates healing of full-thickness wounds in mice. Braz. J. Med. Biol. Res. 2011, 44, 1025–1035. [Google Scholar] [CrossRef] [PubMed]
- Zhou, W.; Liu, G.H.; Yang, S.H.; Mi, B.B.; Ye, S.N. Low-intensity treadmill exercise promotes rat dorsal wound healing. J. Huazhong Univ. Sci. Technol. Med. Sci. 2016, 36, 121–126. [Google Scholar] [CrossRef] [PubMed]
- Zhang, J.; Yuan, T.; Wang, J.H. Moderate treadmill running exercise prior to tendon injury enhances wound healing in aging rats. Oncotarget 2016, 7, 8498–8512. [Google Scholar] [CrossRef] [PubMed]
- Emery, C.F.; Kiecolt-Glaser, J.K.; Glaser, R.; Malarkey, W.B.; Frid, D.J. Exercise accelerates wound healing among healthy older adults: A preliminary investigation. J. Gerontol. Ser. A 2005, 60, 1432–1436. [Google Scholar] [CrossRef] [PubMed]
- Hoffman, M.D.; Sheldahl, L.M.; Buley, K.J.; Sandford, P.R. Physiological comparison of walking among bilateral above-knee amputee and able-bodied subjects, and a model to account for the differences in metabolic cost. Arch. Phys. Med. Rehabil. 1997, 78, 385–392. [Google Scholar] [CrossRef] [PubMed]
- Amaro-Gahete, F.J.; Sanchez-Delgado, G.; Alcantara, J.M.A.; Martinez-Tellez, B.; Acosta, F.M.; Merchan-Ramirez, E.; Löf, M.; Labayen, I.; Ruiz, J. Energy expenditure differences across lying, sitting, and standing positions in young healthy adults. PLoS ONE 2019, 14, e0217029. [Google Scholar] [CrossRef]
- Keyser, R.E.; Rasch, E.K.; Finley, M.; Rodgers, M.M. Improved upper-body endurance following a 12-week home exercise program for manual wheelchair users. J. Rehabil. Res. Dev. 2003, 40, 501–510. [Google Scholar] [CrossRef] [PubMed]
- Vokac, Z.; Bell, H.; Bautz-Holter, E.; Rodahl, K. Oxygen uptake/heart rate relationship in leg and arm exercise, sitting and standing. J. Appl. Physiol. 1975, 39, 54–59. [Google Scholar] [CrossRef] [PubMed]
- Olivier, N.; Legrand, R.; Rogez, J.; Berthoin, S.; Prieur, F.; Weissland, T. One-leg cycling versus arm cranking: Which is most appropriate for physical conditioning after knee surgery? Arch. Phys. Med. Rehabil. 2008, 89, 508–512. [Google Scholar] [CrossRef] [PubMed]
- Hill, M.; Puddiford, M.; Talbot, C.; Price, M. The validity and reproducibility of perceptually regulated exercise responses during combined arm + leg cycling. Eur. J. Appl. Physiol. 2020, 120, 2203–2212. [Google Scholar] [CrossRef] [PubMed]
- Moran, J.; Murphy, A.; Murphy, D.; Austin, A.; Moran, D.; Cronin, C.; Guinan, E.; Hussey, J. The energy expenditure of non-weight bearing crutch walking on the level and ascending stairs. Gait Posture 2015, 42, 23–26. [Google Scholar] [CrossRef] [PubMed]
- Carter, S.E.; Jones, M.; Gladwell, V.F. Energy expenditure and heart rate response to breaking up sedentary time with three different physical activity interventions. Nutr. Metab. Cardiovasc. Dis. 2015, 25, 503–509. [Google Scholar] [CrossRef] [PubMed]
- Volkers, K.M.; van Dijk, T.C.W.; Eggermont, L.H.; Hollander, A.P.; Scherder, E.J.A. The intensity of chair-assisted exercises in cognitively healthy older adults. J. Aging Phys. Act. 2013, 21, 260–271. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Mollà-Casanova, S.; Muñoz-Gómez, E.; Sempere-Rubio, N.; Inglés, M.; Aguilar-Rodríguez, M.; Page, A.; López-Pascual, J.; Serra-Añó, P. Effect of virtual running with exercise on functionality in pre-frail and frail elderly people: Randomized clinical trial. Aging Clin. Exp. Res. 2023, 35, 1459–1467. [Google Scholar] [CrossRef] [PubMed]
- Kim, J.C.; Lee, H.M. EEG-based evidence of mirror neuron activity from app-mediated stroke patient observation. Medicina 2021, 57, 979. [Google Scholar] [CrossRef] [PubMed]
- Gandhi, D.; Sterba, A.; Khatter, H.; Pandian, J. Mirror therapy in stroke rehabilitation: Current perspectives. Ther. Clin. Risk Manag. 2020, 16, 75–85. [Google Scholar] [CrossRef] [PubMed]
- Maggio, M.G.; Torrisi, M.; Buda, A.; De Luca, R.; Piazzitta, D.; Cannavò, A.; Leo, A.; Milardi, D.; Manuli, A.; Calabrò, R.S.; et al. Effects of robotic neurorehabilitation through Lokomat plus virtual reality on cognitive function in patients with traumatic brain injury: A retrospective case-control study. Int. J. Neurosci. 2020, 130, 117–123. [Google Scholar] [CrossRef] [PubMed]
- Abbruzzese, G.; Marchese, R.; Avanzino, L.; Pelosin, E. Rehabilitation for Parkinson’s disease: Current outlook and future challenges. Park. Relat. Disord. 2016, 22, 60–64. [Google Scholar] [CrossRef] [PubMed]
- Caligiore, D.; Mustile, M.; Spalletta, G.; Baldassarre, G. Action observation and motor imagery for rehabilitation in Parkinson’s disease: A systematic review and an integrative hypothesis. Neurosci. Biobehav. Rev. 2017, 72, 210–222. [Google Scholar] [CrossRef] [PubMed]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).