Linking the Phytochemicals and the α-Glucosidase and α-Amylase Enzyme Inhibitory Effects of Nigella sativa Seed Extracts
Abstract
:1. Introduction
2. Materials and Methods
2.1. Chemicals
2.2. Extracts and Fractions Preparation
2.3. Chemical Characterization
2.3.1. GC–MS Analysis
2.3.2. HPLC–DAD Analysis
2.4. The Effect of N. sativa Seed Extracts and Fractions on the Activity of Digestive Enzymes
2.4.1. In Vitro Intestinal α-Glucosidase Inhibitory Assay
2.4.2. In Vitro Pancreatic α-Amylase Inhibitory Assay
2.5. Inhibition Mechanism Analysis
2.5.1. IC50 Determination
2.5.2. Enzyme Kinetic Parameters Determination
2.5.3. Molecular Docking Analysis
2.6. Acute Toxicity
2.6.1. Experimental Animals
2.6.2. Oral Acute Toxicity in Mice
2.7. Statistical Analysis
3. Results and Discussion
3.1. Extracts and Fractions Characterization
3.1.1. Extraction Yields
3.1.2. GC–MS Characterization
3.1.3. HPLC–DAD Characterization
3.2. The Effect of N. sativa Seed Extracts and Fractions on the Activity of Digestive Enzymes
3.2.1. In Vitro Intestinal α-Glucosidase Inhibition Activity
3.2.2. In Vitro Pancreatic α-Amylase Inhibition Activity
3.2.3. Mechanism and IC50 Determinations
3.2.4. Molecular Docking
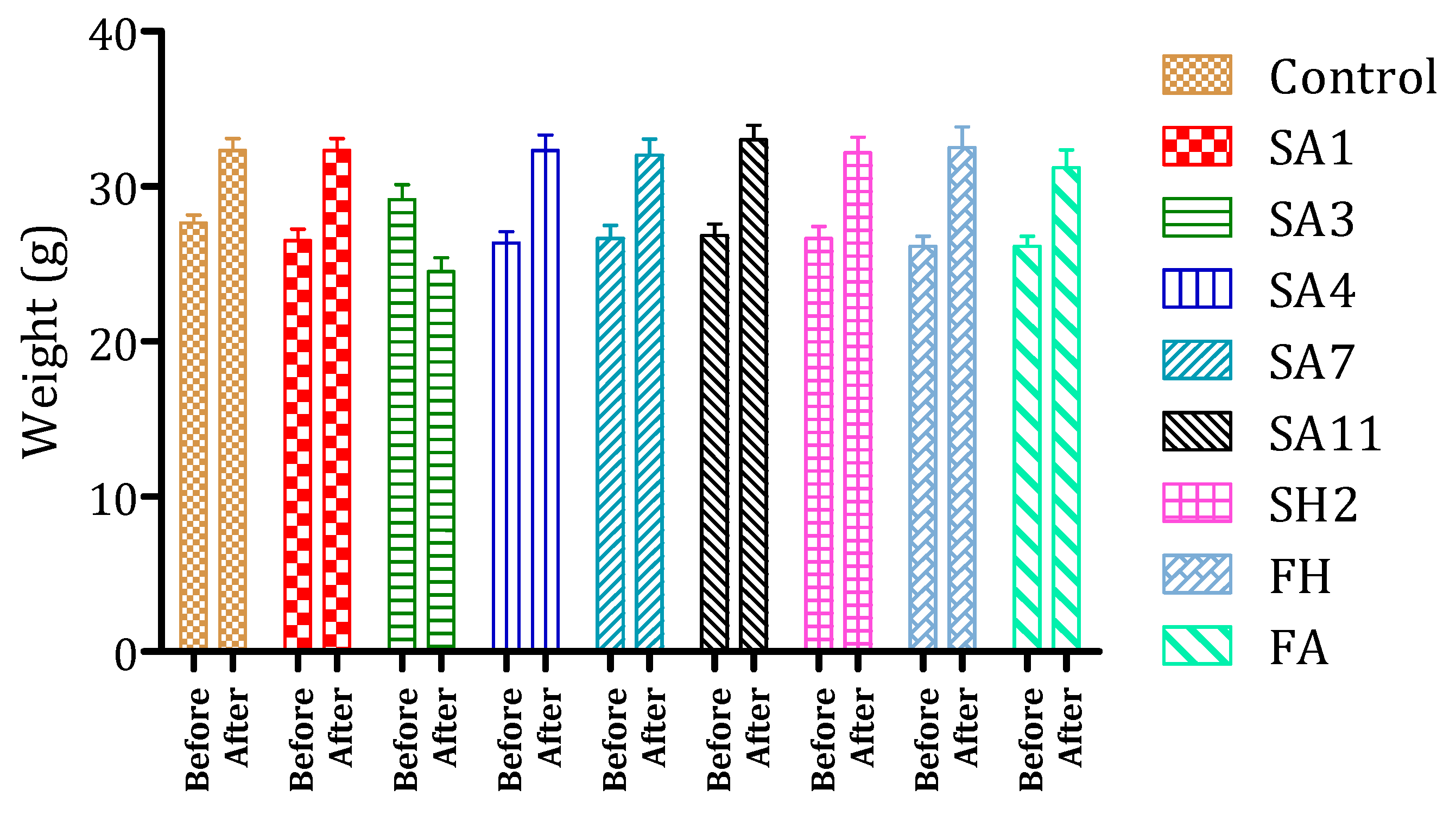
3.3. Evaluation of N. sativa Extracts/Fractions Toxicity in Mice
4. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Data Availability Statement
Conflicts of Interest
References
- Arumugam, G.; Manjula, P.; Paari, N. A review: Anti diabetic medicinal plants used for diabetes mellitus. J. Acute Dis. 2013, 2, 196–200. [Google Scholar] [CrossRef] [Green Version]
- Duarte, A.M.; Guarino, M.P.; Barroso, S.; Gil, M.M. Phytopharmacological strategies in the management of type 2 diabetes mellitus. Foods 2020, 9, 271. [Google Scholar] [CrossRef] [Green Version]
- Bouhrim, M.; Ouassou, H.; Boutahiri, S.; Daoudi, N.E.; Mechchate, H.; Gressier, B.; Eto, B.; Imtara, H.; A Alotaibi, A.; Al-Zharani, M. Opuntia dillenii (Ker Gawl.) haw., seeds oil antidiabetic potential using in vivo, in vitro, in situ, and ex vivo approaches to reveal its underlying mechanism of action. Molecules 2021, 26, 1677. [Google Scholar] [CrossRef] [PubMed]
- Van De Laar, F.A.; Lucassen, P.L.; Akkermans, R.P.; Van De Lisdonk, E.H.; Rutten, G.E.; Van Weel, C. α-Glucosidase inhibitors for patients with type 2 diabetes: Results from a Cochrane systematic review and meta-analysis. Diabetes Care 2005, 28, 154–163. [Google Scholar] [CrossRef] [Green Version]
- Chokki, M.; Cudălbeanu, M.; Zongo, C.; Dah-Nouvlessounon, D.; Ghinea, I.O.; Furdui, B.; Raclea, R.; Savadogo, A.; Baba-Moussa, L.; Avamescu, S.M. Exploring antioxidant and enzymes (α-amylase and β-glucosidase) inhibitory activity of Morinda lucida and Momordica charantia leaves from Benin. Foods 2020, 9, 434. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Xiong, Y.; Ng, K.; Zhang, P.; Warner, R.D.; Shen, S.; Tang, H.-Y.; Liang, Z.; Fang, Z. In vitro α-glucosidase and α-amylase inhibitory activities of free and bound phenolic extracts from the bran and kernel fractions of five Sorghum grain genotypes. Foods 2020, 9, 1301. [Google Scholar] [CrossRef]
- Wang, Z.; Wu, Z.; Zuo, G.; Lim, S.S.; Yan, H. Defatted seeds of oenothera biennis as a potential functional food ingredient for diabetes. Foods 2021, 10, 538. [Google Scholar] [CrossRef] [PubMed]
- Hano, C.; Renouard, S.; Molinié, R.; Corbin, C.; Barakzoy, E.; Doussot, J.; Lamblin, F.; Lainé, E. Flaxseed (Linum usitatissimum L.) extract as well as (+)-secoisolariciresinol diglucoside and its mammalian derivatives are potent inhibitors of α-amylase activity. Bioorg. Med. Chem. Lett. 2013, 23, 3007–3012. [Google Scholar] [CrossRef]
- Zhang, B.; Li, X.; Sun, W.; Xing, Y.; Xiu, Z.; Zhuang, C.; Dong, Y. Dietary flavonoids and acarbose synergistically inhibit α-glucosidase and lower postprandial blood glucose. J. Agric. Food Chem. 2017, 65, 8319–8330. [Google Scholar] [CrossRef]
- Proença, C.; Freitas, M.; Ribeiro, D.; Oliveira, E.F.T.; Sousa, J.L.C.; Tomé, S.M.; Ramos, M.J.; Silva, A.M.S.; Fernandes, P.A.; Fernandes, E. α-Glucosidase inhibition by flavonoids: An in vitro and in silico structure–activity relationship study. J. Enzyme Inhib. Med. Chem. 2017, 32, 1216–1228. [Google Scholar] [CrossRef] [Green Version]
- Proença, C.; Freitas, M.; Ribeiro, D.; Tomé, S.M.; Oliveira, E.F.T.; Viegas, M.F.; Araújo, A.N.; Ramos, M.J.; Silva, A.M.S.; Fernandes, P.A. Evaluation of a flavonoids library for inhibition of pancreatic α-amylase towards a structure–activity relationship. J. Enzyme Inhib. Med. Chem. 2019, 34, 577–588. [Google Scholar] [CrossRef] [Green Version]
- Martinez-Gonzalez, A.I.; Díaz-Sánchez, Á.G.; De La Rosa, L.A.; Bustos-Jaimes, I.; Alvarez-Parrilla, E. Inhibition of α-amylase by flavonoids: Structure activity relationship (SAR). Spectrochim. Acta Part A Mol. Biomol. Spectrosc. 2019, 206, 437–447. [Google Scholar] [CrossRef]
- He, C.; Liu, X.; Jiang, Z.; Geng, S.; Ma, H.; Liu, B. Interaction mechanism of flavonoids and α-glucosidase: Experimental and molecular modelling studies. Foods 2019, 8, 355. [Google Scholar] [CrossRef] [Green Version]
- Ullah, M.A.; Tungmunnithum, D.; Garros, L.; Drouet, S.; Hano, C.; Abbasi, B.H. Effect of ultraviolet-c radiation and melatonin stress on biosynthesis of antioxidant and antidiabetic metabolites produced in in vitro callus cultures of Lepidium sativum L. Int. J. Mol. Sci. 2019, 20, 1787. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Ullah, M.A.; Tungmunnithum, D.; Garros, L.; Hano, C.; Abbasi, B.H. Monochromatic lights-induced trends in antioxidant and antidiabetic polyphenol accumulation in vitro callus cultures of Lepidium sativum L. J. Photochem. Photobiol. B Biol. 2019, 196, 111505. [Google Scholar] [CrossRef]
- Khurshid, R.; Ullah, M.A.; Tungmunnithum, D.; Drouet, S.; Shah, M.; Zaeem, A.; Hameed, S.; Hano, C.; Abbasi, B.H. Lights triggered differential accumulation of antioxidant and antidiabetic secondary metabolites in callus culture of Eclipta alba L. PLoS ONE 2020, 15, e0233963. [Google Scholar] [CrossRef] [PubMed]
- Darand, M.; Darabi, Z.; Yari, Z.; Hedayati, M.; Shahrbaf, M.A.; Khoncheh, A.; Hosseini-Ahangar, B.; Alavian, S.M.; Hekmatdoost, A. The effects of black seed supplementation on cardiovascular risk factors in patients with nonalcoholic fatty liver disease: A randomized, double-blind, placebo-controlled clinical trial. Phyther. Res. 2019, 33, 2369–2377. [Google Scholar] [CrossRef]
- Ahmad, M.F.; Ahmad, F.A.; Ashraf, S.A.; Saad, H.H.; Wahab, S.; Khan, M.I.; Ali, M.; Mohan, S.; Hakeem, K.R.; Athar, M.T. An updated knowledge of Black seed (Nigella sativa Linn): Review of phytochemical constituents and pharmacological properties. J. Herb. Med. 2020, 100404. [Google Scholar] [CrossRef] [PubMed]
- Hamdan, A.; Haji Idrus, R.; Mokhtar, M.H. Effects of Nigella sativa on type-2 diabetes mellitus: A systematic review. Int. J. Environ. Res. Public Health 2019, 16, 4911. [Google Scholar] [CrossRef] [Green Version]
- Kaur, G.; Invally, M.; Khan, M.K.; Jadhav, P. A nutraceutical combination of Cinnamomum cassia & Nigella sativa for Type 1 diabetes mellitus. J. Ayurveda Integr. Med. 2018, 9, 27–37. [Google Scholar]
- Kesen, S.; Amanpour, A.; Tsouli Sarhir, S.; Sevindik, O.; Guclu, G.; Kelebek, H.; Selli, S. Characterization of aroma-active compounds in seed extract of black cumin (Nigella sativa L.) by aroma extract dilution analysis. Foods 2018, 7, 98. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Mazaheri, Y.; Torbati, M.; Azadmard-Damirchi, S.; Savage, G.P. A comprehensive review of the physicochemical, quality and nutritional properties of Nigella sativa oil. Food Rev. Int. 2019, 35, 342–362. [Google Scholar] [CrossRef]
- Kadam, D.; Lele, S.S. Extraction, characterization and bioactive properties of Nigella sativa seedcake. J. Food Sci. Technol. 2017, 54, 3936–3947. [Google Scholar] [CrossRef] [PubMed]
- Sultan, M.T.; Butt, M.S.; Karim, R.; Ahmad, A.N.; Suleria, H.A.R.; Saddique, M.S. Toxicological and safety evaluation of Nigella sativa lipid and volatile fractions in streptozotocin induced diabetes mellitus. Asian Pacific J. Trop. Dis. 2014, 4, S693–S697. [Google Scholar] [CrossRef]
- Heshmati, J.; Namazi, N. Effects of black seed (Nigella sativa) on metabolic parameters in diabetes mellitus: A systematic review. Complement. Ther. Med. 2015, 23, 275–282. [Google Scholar] [CrossRef]
- Jalpa, D.D.; Patel, S.V.; Raval, S.S.; Mandavia, M.K.; Golakiya, B.A. Separation of phytochemicals from Peucedanum Nagpurense by using sepbox and GCMS. J. Cell Tissue Res. 2015, 15, 5275. [Google Scholar]
- Mechraoui, O.; Ladjel, S.; Nedjimi, M.S.; Belfar, M.L.; Moussaoui, Y. Determination of popylphenols content, antioxidant and antibacterial activity of Nigella Sativa L. seed phenolic extracts. Sci. Study Res. Chem. Chem. Eng. Biotechnol. Food Ind. 2018, 19, 411. [Google Scholar]
- Ouassou, H.; Zahidi, T.; Bouknana, S.; Bouhrim, M.; Mekhfi, H.; Ziyyat, A.; Aziz, M.; Bnouham, M. Inhibition of α-glucosidase, intestinal glucose absorption, and antidiabetic properties by Caralluma europaea. Evid. Based Complement. Altern. Med. 2018, 2018, 9589472. [Google Scholar] [CrossRef] [Green Version]
- Daoudi, N.E.; Bouhrim, M.; Ouassou, H.; Legssyer, A.; Mekhfi, H.; Ziyyat, A.; Aziz, M.; Bnouham, M. Inhibitory effect of roasted/unroasted Argania spinosa seeds oil on α-glucosidase, α-amylase and intestinal glucose absorption activities. S. Afr. J. Bot. 2020, 135, 413–420. [Google Scholar] [CrossRef]
- Albus, U. Guide for the Care and Use of Laboratory Animals, 8th ed.; National Academies Press: Washington, DC, USA, 2012. [Google Scholar]
- Naz, H. Nigella sativa: The miraculous herb. Pak. J. Biochem. Mol. Biol 2011, 44, 44–48. [Google Scholar]
- Piras, A.; Rosa, A.; Marongiu, B.; Porcedda, S.; Falconieri, D.; Dessi, M.A.; Ozcelik, B.; Koca, U. Chemical composition and in vitro bioactivity of the volatile and fixed oils of Nigella sativa L. extracted by supercritical carbon dioxide. Ind. Crops Prod. 2013, 46, 317–323. [Google Scholar] [CrossRef]
- Gharby, S.; Harhar, H.; Guillaume, D.; Roudani, A.; Boulbaroud, S.; Ibrahimi, M.; Ahmad, M.; Sultana, S.; Hadda, T.B.; Chafchaouni-Moussaoui, I. Chemical investigation of Nigella sativa L. seed oil produced in Morocco. J. Saudi Soc. Agric. Sci. 2015, 14, 172–177. [Google Scholar] [CrossRef] [Green Version]
- Feuge, R.O.; Vicknair, E.J.; Lovegren, N.V. Modification of vegetable oils. XIII. Some additional properties of acetostearin products. J. Am. Oil Chem. Soc. 1953, 30, 283–287. [Google Scholar] [CrossRef]
- Matthäus, B. Antioxidant activity of extracts obtained from residues of different oilseeds. J. Agric. Food Chem. 2002, 50, 3444–3452. [Google Scholar] [CrossRef]
- Almatroodi, S.A.; Alnuqaydan, A.M.; Alsahli, M.A.; Khan, A.A.; Rahmani, A.H. Thymoquinone, the most prominent constituent of Nigella sativa, attenuates liver damage in streptozotocin-induced diabetic rats via regulation of oxidative stress, inflammation and cyclooxygenase-2 protein expression. Appl. Sci. 2021, 11, 3223. [Google Scholar] [CrossRef]
- Merfort, I.; Wray, V.; Barakat, H.H.; Hussein, S.A.M.; Nawwar, M.A.M.; Willuhn, G. Flavonol triglycosides from seeds of Nigella sativa. Phytochemistry 1997, 46, 359–363. [Google Scholar] [CrossRef]
- Rajkapoor, B.; Anandan, R.; Jayakar, B. Anti-ulcer effect of Nigella sativa Linn. against gastric ulcers in rats. Curr. Sci. 2002, 177–179. [Google Scholar]
- Bourgou, S.; Ksouri, R.; Bellila, A.; Skandrani, I.; Falleh, H.; Marzouk, B. Phenolic composition and biological activities of Tunisian Nigella sativa L. shoots and roots. C. R. Biol. 2008, 331, 48–55. [Google Scholar] [CrossRef] [PubMed]
- Babayan, V.K.; Koottungal, D.; Halaby, G.A. Proximate analysis, fatty acid and amino acid composition of Nigella sativa L. seeds. J. Food Sci. 1978, 43, 1314–1315. [Google Scholar] [CrossRef]
- Choudhary, D.K.; Chaturvedi, N.; Singh, A.; Mishra, A. Characterization, inhibitory activity and mechanism of polyphenols from faba bean (gallic-acid and catechin) on α-glucosidase: Insights from molecular docking and simulation study. Prep. Biochem. Biotechnol. 2020, 50, 123–132. [Google Scholar] [CrossRef] [PubMed]
- Zeng, L.; Zhang, G.; Lin, S.; Gong, D. Inhibitory mechanism of apigenin on α-glucosidase and synergy analysis of flavonoids. J. Agric. Food Chem. 2016, 64, 6939–6949. [Google Scholar] [CrossRef]
- Quan, Y.-S.; Zhang, X.-Y.; Yin, X.-M.; Wang, S.-H.; Jin, L.-L. Potential α-glucosidase inhibitor from Hylotelephium erythrostictum. Bioorg. Med. Chem. Lett. 2020, 30, 127665. [Google Scholar] [CrossRef] [PubMed]
- Xue, N.; Jia, Y.; Li, C.; He, B.; Yang, C.; Wang, J. Characterizations and assays of α-glucosidase inhibition activity on gallic acid cocrystals: Can the cocrystals be defined as a new chemical entity during binding with the α-glucosidase? Molecules 2020, 25, 1163. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Liu, S.; Gao, P.; Zhu, Q.; Luan, F.; Davis, A.R.; Wang, X. Development of cleaved amplified polymorphic sequence markers and a CAPS-based genetic linkage map in watermelon (Citrullus lanatus [Thunb.] Matsum. and Nakai) constructed using whole-genome re-sequencing data. Breed. Sci. 2016, 66, 244–259. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Limanto, A.; Simamora, A.; Santoso, A.W.; Timotius, K.H. Antioxidant, α-glucosidase inhibitory activity and molecular docking study of gallic acid, quercetin and rutin: A comparative study. Mol. Cell. Biomed. Sci. 2019, 3, 67–74. [Google Scholar] [CrossRef]
- Oboh, G.; Ogunsuyi, O.B.; Ogunbadejo, M.D.; Adefegha, S.A. Influence of gallic acid on α-amylase and α-glucosidase inhibitory properties of acarbose. J. Food Drug Anal. 2016, 24, 627–634. [Google Scholar] [CrossRef]
- Dollah, M.A.; Parhizkar, S.; Latiff, L.A.; Hassan, M.H. Bin Toxicity effect of Nigella sativa on the liver function of rats. Adv. Pharm. Bull. 2013, 3, 97. [Google Scholar]
- Liu, S.; Yu, Z.; Zhu, H.; Zhang, W.; Chen, Y. In vitro α-glucosidase inhibitory activity of isolated fractions from water extract of Qingzhuan dark tea. BMC Complement. Altern. Med. 2016, 16, 378. [Google Scholar] [CrossRef] [Green Version]
- Zaoui, A.; Cherrah, Y.; Mahassini, N.; Alaoui, K.; Amarouch, H.; Hassar, M. Acute and chronic toxicity of Nigella sativa fixed oil. Phytomedicine 2002, 9, 69–74. [Google Scholar] [CrossRef] [Green Version]
- Alenzi, F.Q.; El-Bolkiny, Y.E.-S.; Salem, M.L. Protective effects of Nigella sativa oil and thymoquinone against toxicity induced by the anticancer drug cyclophosphamide. Br. J. Biomed. Sci. 2010, 67, 20–28. [Google Scholar] [CrossRef]
- Pourbakhsh, H.; Taghiabadi, E.; Abnous, K.; Hariri, A.T.; Hosseini, S.M.; Hosseinzadeh, H. Effect of Nigella sativa fixed oil on ethanol toxicity in rats. Iran. J. Basic Med. Sci. 2014, 17, 1020–1031. [Google Scholar] [CrossRef] [PubMed]






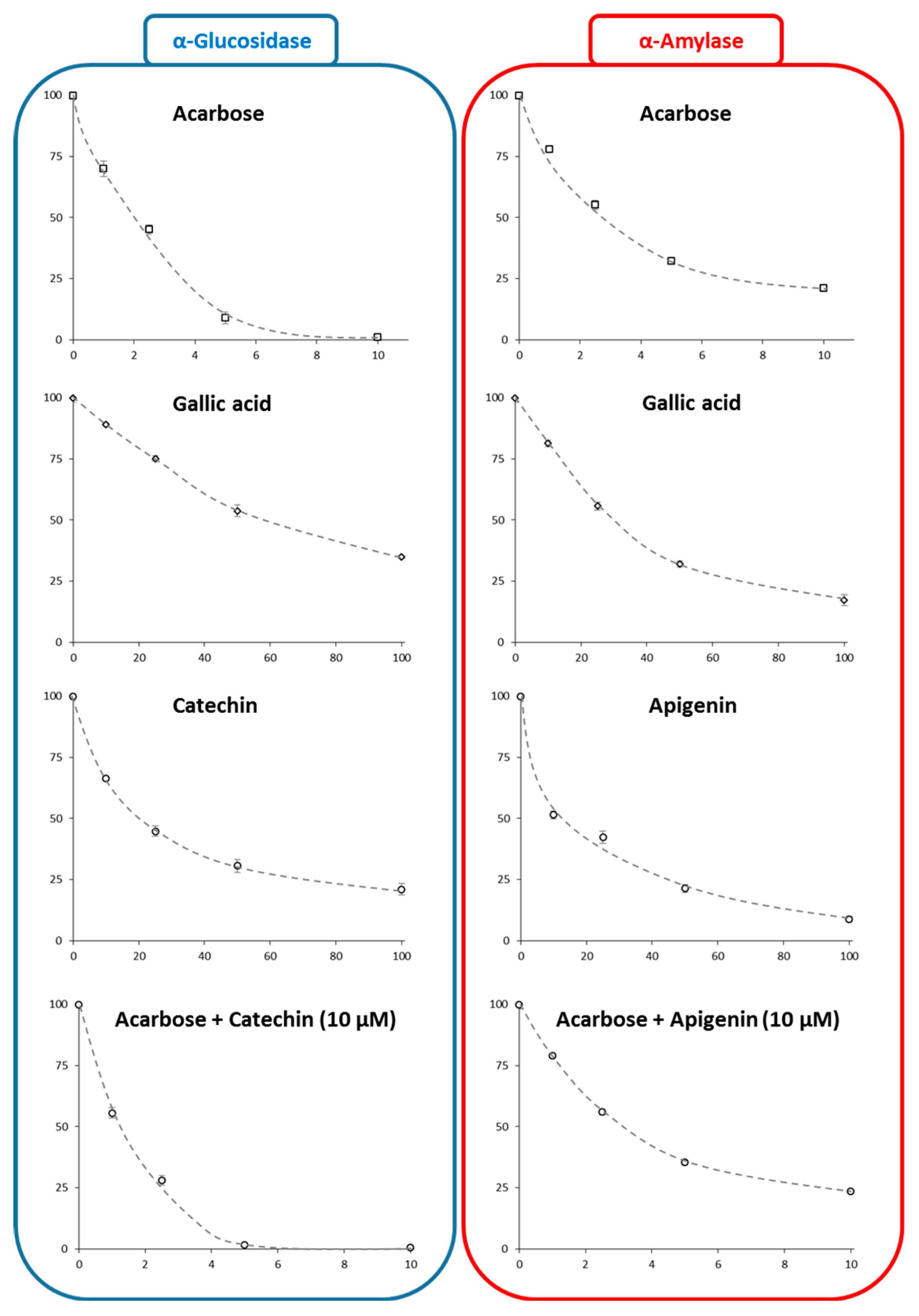


| Ligand | Km (mM) | Vmax (µM/min) | Inhibition Type |
|---|---|---|---|
| intestinal α-glucosidase | |||
| Control 1 | 427.6 ± 1.3 | 14.1 ± 0.7 | - |
| (−)-Catechin | 121.9 ± 1.8 | 13.1 ± 0.9 | Noncompetitive |
| Gallic acid | 202.8 ± 3.1 | 14.7 ± 1.2 | Noncompetitive |
| Acarbose | 426.6 ± 2.4 | 23.9 ± 0.5 | Competitive |
| pancreatic α-amylase | |||
| Control 1 | 82.7 ± 1.6 | 29.6 ± 0.8 | - |
| Apigenin | 82.8 ± 1.3 | 90.1 ± 0.7 | Competitive |
| Gallic acid | 87.3 ± 2.4 | 76.9 ± 1.4 | Competitive |
| Acarbose | 82.7 ± 1.4 | 53.8 ± 1.1 | Competitive |
| Ligand | IC50 (µM) |
|---|---|
| intestinal α-glucosidase | |
| (−)-Catechin | 39.09 ± 1.33 |
| Gallic acid | 13.40 ± 1.85 |
| Acarbose | 1.96 ± 0.18 |
| pancreatic α-amylase | |
| Apigenin | 13.91 ± 2.79 |
| Gallic acid | 27.79 ± 2.06 |
| Acarbose | 3.07 ± 0.03 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Tiji, S.; Bouhrim, M.; Addi, M.; Drouet, S.; Lorenzo, J.M.; Hano, C.; Bnouham, M.; Mimouni, M. Linking the Phytochemicals and the α-Glucosidase and α-Amylase Enzyme Inhibitory Effects of Nigella sativa Seed Extracts. Foods 2021, 10, 1818. https://doi.org/10.3390/foods10081818
Tiji S, Bouhrim M, Addi M, Drouet S, Lorenzo JM, Hano C, Bnouham M, Mimouni M. Linking the Phytochemicals and the α-Glucosidase and α-Amylase Enzyme Inhibitory Effects of Nigella sativa Seed Extracts. Foods. 2021; 10(8):1818. https://doi.org/10.3390/foods10081818
Chicago/Turabian StyleTiji, Salima, Mohamed Bouhrim, Mohamed Addi, Samantha Drouet, Jose Manuel Lorenzo, Christophe Hano, Mohamed Bnouham, and Mostafa Mimouni. 2021. "Linking the Phytochemicals and the α-Glucosidase and α-Amylase Enzyme Inhibitory Effects of Nigella sativa Seed Extracts" Foods 10, no. 8: 1818. https://doi.org/10.3390/foods10081818
APA StyleTiji, S., Bouhrim, M., Addi, M., Drouet, S., Lorenzo, J. M., Hano, C., Bnouham, M., & Mimouni, M. (2021). Linking the Phytochemicals and the α-Glucosidase and α-Amylase Enzyme Inhibitory Effects of Nigella sativa Seed Extracts. Foods, 10(8), 1818. https://doi.org/10.3390/foods10081818








