Abstract
Opportunistic and hospital-acquired infections are common among recipients of solid organ transplantation. New pathogens are increasingly reported in the intensive care unit (ICU) population. We report a case of a patient who developed Trichoderma spp.-related pneumonia (TRP) after heart–lung transplantation. In the absence of antifungal susceptibility testing, TRP was confirmed by histological examination, and empirical therapy with voriconazole and caspofungin was swiftly initiated. Complete resolution of pneumonia was obtained after prolonged combination therapy. Given the lack of guidelines, we conducted a systematic review to elucidate the diagnostic and therapeutic strategies to apply during Trichoderma infection. After deduplication and selection of full texts, we found 42 articles eligible for the systematic review. Pneumonia seems to be the most common clinical manifestation (31.8%). The most used antifungal therapy was amphotericin B, while combination therapy was also reported (27.3%). All the patients were immunocompromised except for one case. Despite the rarity of Trichoderma spp. infection, the increase in invasive fungal infections is of growing importance in ICU, considering their impact on mortality and the emergence of antifungal resistance. In the absence of prospective and multicenter studies, a review can provide useful insight regarding the epidemiology, clinical manifestations, and management of these unexpected challenges.
1. Introduction
Opportunistic and hospital-acquired infections can occur in solid organ transplantation (SOT) recipients. Among them, patients with the highest rate of infectious complications are those undergoing lung transplantation (LTx), especially in the intensive care unit (ICU), where invasive fungal infections (IFIs) are becoming increasingly common [1,2,3,4].
IFIs are a major contributor to nosocomial infection in critically ill patients. Most of them are attributable to Candida spp. (principally bloodstream or abdominal infections) and Aspergillus spp., representing an important cause of morbidity and mortality and being associated with a longer duration of ICU stays [5]. The incidence of IFIs has risen over recent decades. It is continuing to grow both in immunocompetent and immunocompromised hosts, as recently highlighted during the COVID-19 pandemic [6,7]. At the same time, the broadened use of systemic antifungal drugs makes them quite a common component of antimicrobial therapy, with the development of resistance now deserving antifungal stewardship strategies [8,9]. Considering the important limitation in terms of diagnostic tools and turn-around time of traditional tests, risk factor evaluation remains pivotal to guide clinical orientation to treatment [10]. The most common risk factors characterizing ICU admission and predisposing LTx recipients to opportunistic infection are immunosuppressive and immunomodulatory therapy, loss or impairment of cough reflex, CVM co-infection, ischemia of the anastomosis, and ICU-acquired weakness [11,12]. While the best-known opportunistic fungal infections in LTx recipients are those related to Aspergillus spp., infections due to new pathogens, such as molds and filamentous fungi, are on the rise.
Trichoderma spp. is an omnipresent mold, usually present in the soil. Under normal conditions, it does not cause active infections in healthy human hosts [13]. However, nine Trichoderma species have been reported to cause human infection, especially in immunocompromised hosts [14].
Starting from the clinical case of a patient who underwent an en bloc heart–lung transplant and developed a Trichoderma spp.-related pneumonia (TRP) in the first postoperative period despite the antifungal prophylaxis, we conducted a systematic review of the literature to describe clinical characteristics, confirm diagnostic methods, and revise available treatment options and outcomes.
The Clinical Case
A 42-year-old woman was admitted to the cardiosurgical ICU after a heart–lung transplant. Her past medical history was characterized by Eisenmenger Syndrome and patent ductus arterious diagnosed at the age of 3. Her clinical conditions remained stable until the age of 38 when a progressive and symptomatic decline in pulmonary function occurred, and pulmonary fibrosis was diagnosed.
Due to the worsening of her pulmonary and cardiac conditions (increase in pulmonary hypertension and right ventricular dilatation), she underwent a combined heart–lung transplant. Her intraoperative course was complicated by prolonged cardiopulmonary bypass and graft ischemic time (cardiopulmonary bypass time of 285 min and graft ischemic time of 190 min) and by difficulty weaning from the cardiopulmonary bypass itself.
Antimicrobial prophylaxis was started according to our local protocol, including inhaled amphotericin B (amphotericin B lipid complex, 20 mg once daily) and oral nystatin (1 MIE oral drops, TID). Our protocol also included antibacterial prophylaxis (ceftazidime, IV 1 g TID, for the first 72 h), Pneumocystis jirovecii prophylaxis (Trimetoprim-Sulfamethoxazole, PO, once daily), and Citomegalovirus (CMV) prophylaxis according to CMV status (Valganciclovir, PO, 900 mg once daily).
After the patient was successfully weaned from the inotropic support end and extubated on postoperative day 5, her clinical conditions worsened on the ninth postoperative day due to the onset of moderate hypoxemia and clinical signs of pump failure. Leukocytosis appeared associated with an increase in and worsening of tracheal secretion, while a chest X-ray confirmed a left lower lobe consolidation. Additionally, her renal function progressively declined.
Empirical antibiotic coverage with vancomycin and ceftazidime was then initiated. Simultaneously, a chest CT scan confirming parenchymal consolidation and an extensive ground-glass pattern involving both inferior lobes and the lingula and bronchoalveolar lavage (BAL) were obtained. BAL did not find any bacterial growth, but a positive cell culture for Trichoderma spp. and a BAL-Galactomannan assay of weak positivity (EIA 0.60 S/CO) were detected. Hence, antifungal combination therapy with voriconazole and caspofungin was started. A cytological examination was also found positive for hyphal growth. Repeated BALs were performed, as well as culture examination of mucous plug; microscopic examination confirmed Trichoderma spp. and hyphal growth in all the samples, but our laboratory was unable to grow viable cultures, identify Trichoderma species, or perform antimicrobial susceptibilities testing (AST).
After 34 days of antifungal therapy, the resolution of the pneumonia was observed, as confirmed by clinical and chest CT improvement and by a negative BAL culture. Parenteral antifugal therapy was therefore discontinued, and prophylaxis with inhaled amphotericin B alone was maintained. Following surveillance cultures, including subsequent BALs and BAL-Galactomannan assays, were negative for Trichoderma or fungal detection.
The patient suffered ICU-acquired weakness and difficulty weaning from mechanical ventilation. Her clinical course was further complicated by MDR Klebsiella pneumoniae colonization and surgical site infection. Relapsing septic shock despite surgical debridement and end-stage renal failure ensued. The patient died from K. pneumoniae-related septic shock 6 months after transplantation.
While neither Trichoderma nor respiratory failure were direct causes of death, TRP was an early complication that required a prolonged ICU stay, thus hindering the postoperative clinical course.
2. Materials and Methods
2.1. Research Approach
The systematic review protocol was drafted using the Preferred Reporting Items for Systematic Reviews and Meta-analysis Protocols (PRISMA-P), which was revised by the members of our cardiac surgery research team, and the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) statement [15]. The final protocol was prospectively registered with the Open Science Framework on 5 February 2022 (https://osf.io/n63ps, accessed on 1 January 2023).
2.2. Eligibility Criteria and Information Sources
To be included in the review, papers had to focus on human Trichoderma infection. Peer-reviewed articles were included if they were randomized-controlled trials (RCTs) or non-RCT (NRCTs), including case reports, and case series published in English or Italian and retrieved using Pubmed, Scopus, and Embase databases. The search was implemented with the use of registries (clinicaltrials.gov, accessed on 1 January 2023) and gray literature searches (http://greylit.org/, accessed on 1 January 2023).
2.3. Search Strategy
Literature search was carried out using the following search strategies:
- Pubmed: (“trichoderma”[MeSH Terms] OR “trichoderma”[All Fields] OR “trichodermas”[All Fields]) AND ((“human s”[All Fields] OR “humans”[MeSH Terms] OR “humans”[All Fields] OR “human”[All Fields]) AND (“infect”[All Fields] OR “infectability”[All Fields] OR “infectable”[All Fields] OR “infectant”[All Fields] OR “infectants”[All Fields] OR “infected”[All Fields] OR “infecteds”[All Fields] OR “infectibility”[All Fields] OR “infectible”[All Fields] OR “infecting”[All Fields] OR “infection s”[All Fields] OR “infections”[MeSH Terms] OR “infections”[All Fields] OR “infection”[All Fields] OR “infective”[All Fields] OR “infectiveness”[All Fields] OR “infectives”[All Fields] OR “infectivities”[All Fields] OR “infects”[All Fields] OR “pathogenicity”[MeSH Subheading] OR “pathogenicity”[All Fields] OR “infectivity”[All Fields]));
- Embase, Scopus, clinicaltrials.gov, and grey literature: (‘trichoderma’/exp OR trichoderma) AND (‘human infection’ OR ((‘human’/exp OR human) AND (‘infection’/exp OR infection))).
2.4. Selection and Data Collection Process
Search results were exported to EndNote V.X9 (Clarivate Analytics, Philadelphia, PA, USA). Duplicates were automatically removed. The review process was conducted in two steps consisting of evaluating the titles, abstracts, and then full text of all publications identified by our searches for potentially relevant manuscripts. For both levels, two authors (C.B. and E.B.) screened the articles, with conflicts resolved by consensus and discussion with other reviewers (A.C.T. and L.B.). A planned Excel spreadsheet was used to extract data (patients’ characteristics, year of publication, country, type of pathogen, therapy, and outcome measures).
2.5. Data Collection Process and Data Synthesis
We considered as variables the authors, the year of publication, the country where the article was published, the species of fungus that caused the infection, the main pathology from which the patient suffered, the clinical manifestation of the patient’s fungal infection, the treatment of choice, and the outcome.
2.6. Risk of Bias Assessment
Since we found only case reports and case series, it was impossible to apply the risk of bias assessment using the Risk Of Bias In Non-randomized Studies of Interventions (ROBINS-i) tool. Since these were descriptive studies of an infection and therefore not of a specific intervention, we did not deem it appropriate to perform a risk of bias assessment. Where the result has not been reported, we have highlighted this in the results table. Similarly, we decided not to apply a summary of evidence using the Grading of Recommendations, Assessment, Development and Evaluations (GRADE) model for the same reason: (1) there is a lack of comparison group, and (2) the cases are not groupable due to the geographic and temporal uniqueness of each case.
3. Results
3.1. Search Results
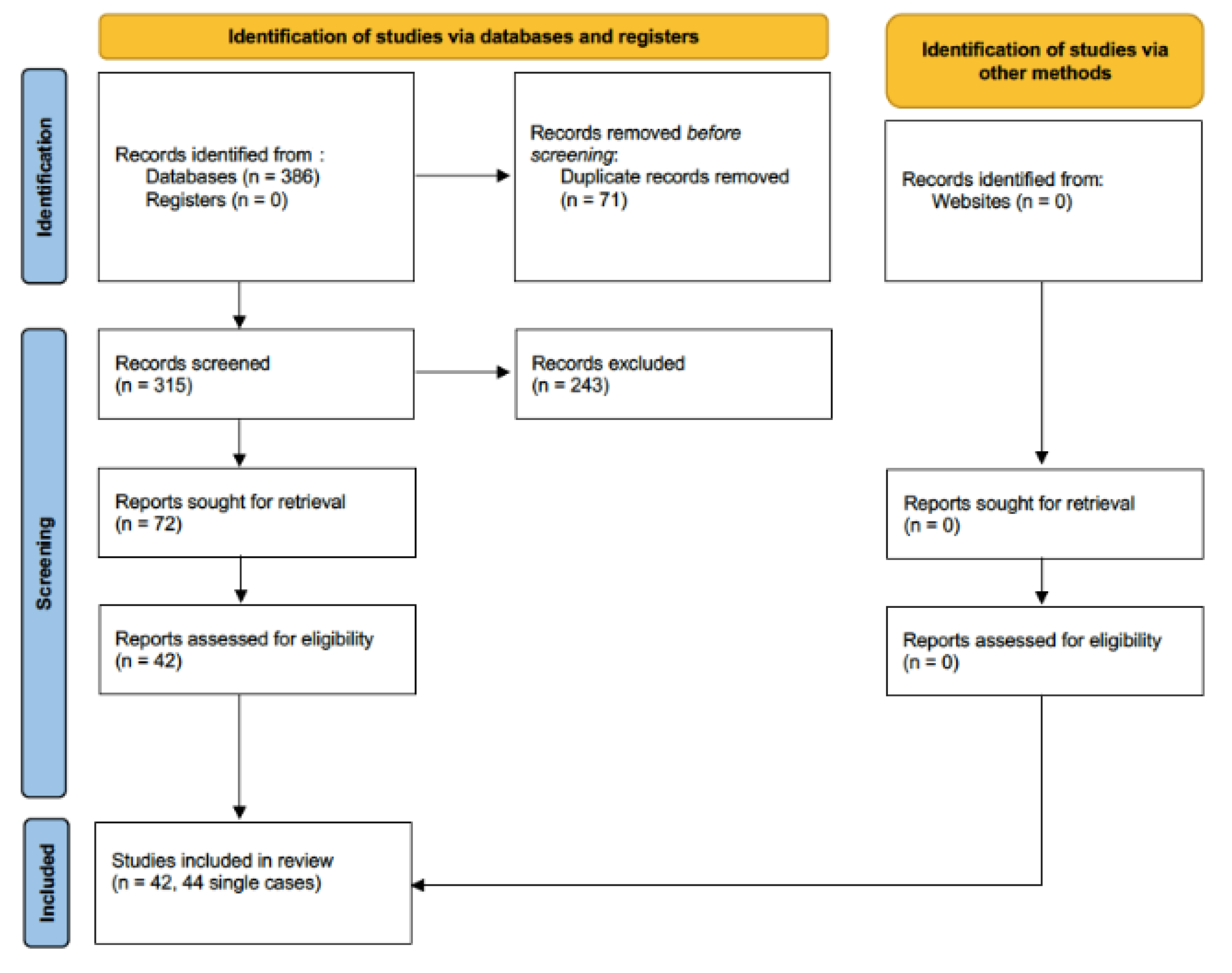
The systematic literature search performed on 11 October 2022 retrieved 386 results. None of them were found from grey literature or clinical trials registers. After deduplication, 72 studies were considered eligible for the full-text evaluation. A total of 42 of them were selected for full-text review and included in the systematic review (Figure 1). The reason for excluding the other full texts is that they did not discuss Trichoderma-related diseases but rather other fungal infections.
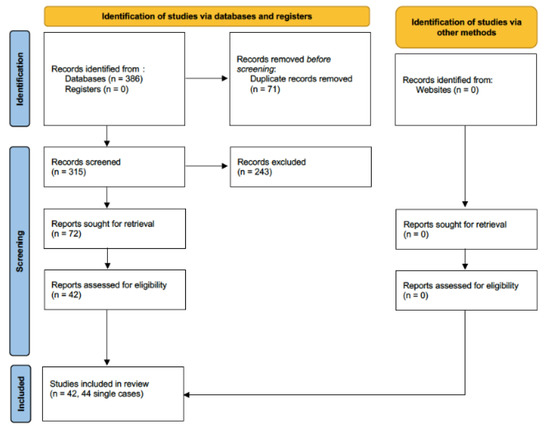
Figure 1.
PRISMA flow diagram.
A total of 50% of the articles were published between 1969 and 1999, 22.5% between 2000 and 2010, and 27.5% from 2011 to the present. The countries of provenance are Spain at 20.5%, France at 18.2%, USA at 15.9%, Japan at 9.1%, Italy at 6.8%, and Saudi Arabia at 2.3% (Table 1).

Table 1.
Summary of findings.
3.2. Trichoderma and the Related Disease
Trichoderma spp. infection is reported in 25% of cases, while Trichoderma was typed in the remaining 75%. A total of 45.5% of the infections were due to T. longibrachiatum and 13.6% to T. viride.
In 31.8% of cases, pneumonia was the highlighted clinical manifestation. We found 12 papers (14 cases) specifically referring to TRP. In all of these cases, TRP affected immunocompromised hosts and in most of them, namely 78.6%, turned out to be non-fatal. However, it should be noted that in 14.3% of cases, it was not possible to determine the outcome, as it was not reported by the authors in the abstract, and the full paper was written in Japanese [21,25].
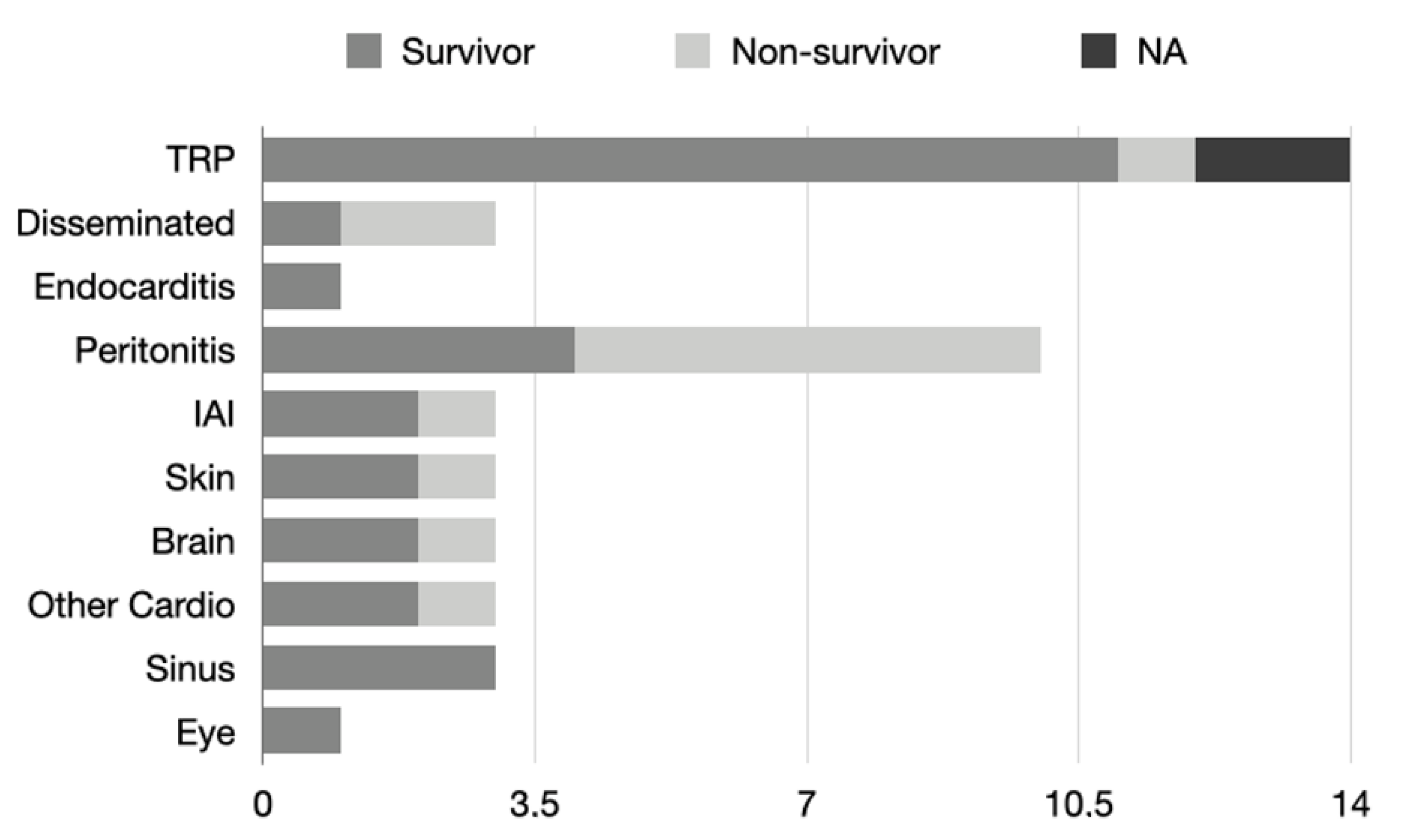
Other clinical manifestations are less common (Figure 2). Trichoderma resulted in peritonitis in 22.7% of cases, and 40% of these subjects survived. Of these patients, 10/12 were patients undergoing outpatient peritoneal dialysis, one was a patient with end-stage renal failure, and one was a patient undergoing kidney transplantation. Intra-abdominal infections without peritonitis accounted for 6.8% of cases, all of them being post-abdominal surgery patients.
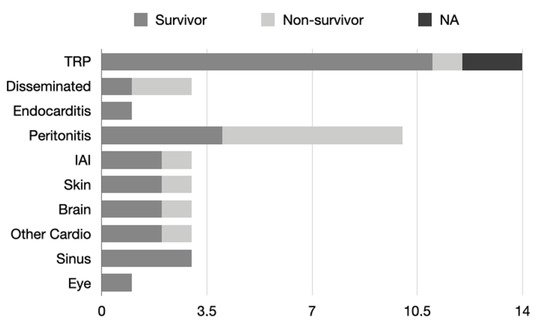
Figure 2.
The graph shows the number of cases in the literature divided by type of Trichoderma infection developed by patients. Each bar is divided according to patient outcome.
Skin infection by Trichoderma accounted for 9.1% of cases, all of them affecting immunocompromised hosts, with a survival rate of 75%.
The reported cases of endocarditis are relatively recent, ranging from 2000 to 2016, representing 6.8% of cases, with 100% mortality. Of these, one patient was receiving home parenteral nutrition [45], one was a patient undergoing aortic surgery [34], and one was a patient undergoing ICD implantation complicated by pneumothorax [48].
There are two cases of brain infection with brain abscess by Trichoderma, and they were reported in 1995 by T. longibrachiatum in Germany in a patient affected by leukemia [24] and in 1999 by T. harzianum in Spain in a kidney transplant patient [32]. Of these, the patient with brain abscess and leukemia, treated with amphotericin B, itraconazole, and surgical debridement, had survived. A case of Trichoderma spp.-related encephalitis was reported in a patient with AIDS, treated with amphotericin B, who survived [35]. Disseminated Trichoderma infection is reported in 6.8% of cases, with a survival rate of 33%. Two of three patients with disseminated Trichoderma infection were bone marrow transplant patients [23,31].
Two cases of sinusitis have been reported, both from T. longibrachiatum, in a liver transplant patient and in an immunocompetent patient [30,46]. Of these two cases, both patients survived with treatment with amphotericin B and surgical debridement. The liver transplant patient had received combination therapy with amphotericin B and itraconazole.
Overall, according to the literature, 27.3% did not survive Trichoderma infection even though, in 4.5% of the articles, the outcome is not reported.
3.3. Diagnostic Tests and Antifungal Susceptibility Testing
A summary of the diagnostic approach and antifungal susceptibility testing is highlighted in Table 2.

Table 2.
Summary of diagnostic approach and antifungal susceptibility testing.
Trichoderma infection was often diagnosed by culture of body fluid involved, being peritoneal fluid in peritonitis or BAL in pulmonary infection. Bioptic examination was rarely employed outside skin infections, in which case it remained the preferred diagnostic test. Regarding AST, data reviewed confirm that Trichoderma spp. maintains elevated MIC toward commonly employed azoles, such as fluconazole and ketokonazole. Most samples analyzed instead reported a significantly low MIC (<1 μg/mL) regarding echinocandins, in most cases caspofungin (MIC < 1 μg/mL in 10 out of 13 samples, 76.9%). Variable resistance patterns can be shown for voriconazole (MIC < 1 μg/mL in nine out of sixteen samples, 56.5%) and amphotericin B (MIC < 1 μg/mL in 10 out of 24 samples, 41.6%).
Furthermore, the diagnostic approach was often more complex in TRP cases. Out of twelve cases, only seven cases were diagnosed by BAL culture and microscopic examination. In two cases with clear clinical respiratory involvement and sepsis, blood cultures were diagnostic for Trichoderma spp.; both of them were neutropenic patients. In one case, transbronchial biopsy was deemed necessary and isolated hyphal growth. Galactomannan assay was performed in only three cases, in one case from BAL material, in a second case from serum analysis, and the last from an unspecified sample; one Serum-Galactomannan assay was positive (EIA = 1.3), while the other two samples were reported negative. Species identification based on PCR amplification and partial DNA sequencing was attempted in six case reports. Trichoderma longibrachiatum was identified in five of these cases. In one case, sequence analysis confirmed Trichoderma species without subspecies identification.
Antifungal susceptibility testing was performed in eight cases of TRP, although the number of antifungal drugs tested varies between studies. Antifungal susceptibility was determined with European Committee on Antimicrobial Susceptibility Testing (EUCAST) standardized methodology. As expected, Trichoderma was vastly resistant to fluconazole and itraconazole, with MIC often >32 μg/mL. Voriconazole showed MIC < 1 μg/mL in four cases and MIC ≥ 1 μg/mL in three cases. Amphotericin B exhibited MIC < 1 μg/mL in three cases and MIC ≥ 1 μg/mL in four cases. Five cases tested Caspofungin susceptibility, and Trichoderma showed clear in vitro susceptibility in all of them, with MIC < 0.5 μg/mL. Finally, one case reported in vitro susceptibility to amphotericin B and resistance to both voriconazole and caspofungin, without disclosing any MIC value.
3.4. Antifungal Management
Antifungal therapy varies among observed cases, depending on timing and site of infection. Most cases relied on amphotericin B, either alone (fifteen cases, 34.1%) or in combination with an azole (eight cases, 18.8%). In eight cases (18.2%), azoles (either itraconazole, ketoconazole, fluconazole, miconazole, or voriconazole) alone were the treatment of choice, while in three cases (6.8%), echinocandin alone was administered. In four cases (9.1%), a combination therapy with echinocandin and voriconazole was deemed necessary. Lastly, in a recent clinical case involving fungal pericarditis, isavuconazole was administered. One paper does not specify the type of antifungal drug used [57].
Concomitant source control procedures, including surgical debridement and catheter removal, were used in 14 cases (35.9%), none of them involving pulmonary infection.
Regarding TRP, the treatment of choice was either amphotericin B plus azole (two patients, 14.3%), amphotericin B in monotherapy (four patients, 28.6%), or echinocandin plus voriconazole (two patients, 14.3%). Amphotericin B plus voriconazole plus caspofungin combination therapy was used in only two cases (14.3%).
Patients who developed Trichoderma spp. infection were reported to be immunocompromised (sixteen cases), onco-hematological (fifteen cases), transplanted (seven cases, two of them lung transplantation), and AIDS (two cases). Among transplant patients, only one lung developed Trichoderma pericarditis [34]. Only in one case [46] did Trichoderma infection affect an immunocompetent patient; in this case, the clinical manifestation was a sinusitis which ended with a resolution of the infection by surgical debridement and antifungal topical therapy.
4. Discussion
Evidence from the scientific literature seems to suggest that Trichoderma spp. represents a re-emerging fungal infection (Table 1). The prolonged use of antifungals and antibacterials in agriculture and medicine has indeed altered the global microbiome, leading to the growth of drug-resistant fungi [58] such as Candida auris, Histoplasma, Cryptococcus, and Aspergillus spp. [2].
Specific risk factors for Trichoderma infection are difficult to detect due to the paucity of cases. The literature review confirmed that Trichoderma spp. infections occur mostly in immunocompromised patients (Table 1). Our patient showed several risk factors for invasive aspergillosis, as her medication regimen included a steroid for immunosuppressive therapy, Anti-Thymocyte Immunoglobulin as induction therapy; notably, no specific environmental factor could be found in the medical history of either the organ donor or the patient other than prolonged pre-transplantation hospitalization of the recipient.
Patients undergoing SOT and hematopoietic stem cell transplantation are likely to develop emerging IFI due to immunosuppressive and immunomodulatory therapy [12]. Furthermore, the widespread use of anti-Aspergillus prophylaxis in SOT recipients may exert selective pressure toward uncommon pathogens [59], such as pathogens generally found in soil (e.g., phaeohyphomycosis), Fusariosis, Scedosporium, and L. prolificans [60]. Given that Trichoderma infection has been found in SOT recipients, namely renal and liver recipients (five cases), it is not surprising to find it in heart–lung recipients as well. Pneumonia is the most reported clinical manifestation, considering both the tendency of these patients to experience pulmonary complications and the fact that the lung is the most common site of infection for uncommon pathogens, such as Trichoderma spp.
There is no doubt that the diagnostic evaluation of TRP is particularly challenging. While typical fungal colonization or disease such as pulmonary Aspergillosis are defined by solid evidence-driven diagnostic criteria [61], the diagnosis of non-Aspergillus invasive mold infection (NAIMI) is based on extrapolated data or expert opinions. Even if the distinction between colonization and active infection is crucial in opportunistic fungal infections [62], this is lacking for NAIMIs [63]. The literature suggests the early use of CT scan, both to diagnose and delineate the disease and to guide invasive procedures aimed at obtaining deep tissue samples (including BAL). Specific markers to identify NAIMI infections [59] are often unavailable [12], and most laboratories do not have adequate expertise to detect and identify rare pathogens. BAL galactomannan (BAL-GM) can be used to evaluate and diagnose Aspergillosis [61]. However, its application in other filamentous fungi infections is controversial, since cross-reactivity of the BAL-GM assay with both Trichoderma pseudokoningii and T. longibrachiatum infections has been reported, with a moderate increase in its values [62]. The weak positivity of the BAL-GM assay that we found is in line with evidence found in the literature. The use of nucleic acid amplification tests (polymerase chain reaction and sequencing on fungal RNA genes) has been described as highly specific and sensitive [12], but their availability is still limited, as in the case of our institution, where is not available. A specific histological investigation to evaluate the presence of hyphae in the BAL confirmed a pulmonary infection, as recommended for unspecified NAIMI.
The clinical status of critically ill patients is frequently not conducive to early lung tissue biopsy. In the case described above, it was not deemed appropriate due to the high risk of reported complications in mechanically ventilated patients. Conversely, the use of BAL together with histological investigation might offer an adequate risk/benefit ratio, being repeatable and easy to perform. From a therapeutic point of view, uncommon IFIs might be affected by antifungal resistance [2]. Antifungal susceptibility testing (AST) has not been routinely performed in all cases of pulmonary Trichoderma infections, mainly due to the difficulty of isolating and growing filamentous fungi (as in the case described) [49,63]. Furthermore, in NAIMI, AST is not recommended, as there are no breakpoints and no established correlation between minimal inhibitory concentration (MIC) and clinical outcome for most uncommon fungal infections [64,65]. This recommendation has been proposed since a correlation between MIC and clinical outcomes in opportunistic mold infections is missing, while a discrepancy between in vitro AST and in vivo infections has been previously reported and suggests poor clinical relevance [59].
Nevertheless, AST for Trichoderma infections is being widely utilized in clinical practice (Table 2), often assuming clinical breakpoints for unspecified mold infection. Our literature review suggests that Trichoderma maintains high in-vitro resistance for azoles, showing MIC often >32 μg/mL. High (>1 μg/mL) MIC values are often reported for voriconazole and amphotericin B as well. Echinocandins instead exhibited MIC < 1 μg/mL in most of the reported cases. These results agree with a previous study regarding in vitro susceptibilities of isolated Trichoderma, including both human and animal samples (however, 40% of samples were collected from the human respiratory tract), which reported mostly low MIC for voriconazole and echinocandins [14].
In the absence of a clinical breakpoint, AST-adjusted antifungal therapy is recommended with low-quality evidence [66]. Although in some cases AST has been obtained and used to guide antifungal therapy [36,39,40,56], no recommendation regarding AST in Trichoderma spp. can be found in the literature.
Treatment for Trichoderma spp. usually consists of amphotericin B or azole (Table 1). In our case, the patient was already receiving amphotericin B aerosol for prophylaxis, raising concerns about a possible breakthrough infection. Possible adverse effects caused by an amphotericin B intravenous course were also considered. Combination therapy with voriconazole and an echinocandin was described to treat Trichoderma-related pulmonary infections with a favorable therapeutic index [40], as in vitro sensitivity of most Trichoderma spp. to both drugs has been reported in previous studies [14] as well as in our literature review (Table 2). In our patient, caspofungin–voriconazole combination therapy was chosen, considering the possibility of amphotericin B resistance in the context of breakthrough infection and the absence of AST, as well as the patient’s comorbidities. Due to concomitant calcineurin inhibitor therapy, a voriconazole-monitoring-driven approach was conducted, as recommended by guidelines [67,68].
Another possible option reported in the literature is represented by liposomal amphotericin B, previously described to treat TRP without further impairment of renal function [49], as well as to treat other Trichoderma infections (Table 1). In animal models, disseminated Trichoderma infection has shown peculiar resistance to most antifungal agents, including amphotericin B and voriconazole; however, combination therapy was not tested in this study [69]. According to the literature, both combination treatment and amphotericin B monotherapy were previously found effective to eradicate the infection.
From the data extracted in the literature, we can suggest with this review to carefully evaluate according to the risk factors (e.g., outpatient peritoneal dialysis patient, immunocompromised patient with unspecified/unresolving pneumonia) the possibility of re-emergent fungal infection, such as Trichoderma. In the absence of universally recognized definitions and diagnostic criteria, careful prompt examination and investigation, based on both a CT scan and BAL with nucleic acid amplification tests, if available, are crucial for early diagnosis. Although laboratory MIC cut-offs are still lacking, AST might be encouraged due to high MIC reported for many antifungal medications, especially considering the global increase in fungal resistance and the need for antifungal stewardship strategies. In the absence of AST, local susceptibilities as well as patient characteristics, including previous prophylaxis or therapies, should be carefully considered to tailor the appropriate antifungal therapy. Both amphotericin B monotherapy and antifungal combination with echinocandin plus voriconazole is reported as effective in Trichoderma spp. infections and can be viable therapies according to the clinical context.
5. Conclusions
Although rare, IFIs caused by uncommon fungi, such as Trichoderma spp. and other NAIMI, are increasingly reported in critically ill patients, especially in SOT recipients, presenting challenges in terms of clinical suspicion, diagnostic methods, and treatment options.
Large and definitive clinical trials involving Trichoderma human infection are unlikely due to the paucity of cases. The topic of re-emerging fungal infections also makes the possibility of an individual patient meta-analysis difficult because of the great differences in the geographic and historical context.
In case of future reports in the literature, we suggest improving the available evidence by reporting in more detail the MIC for antifungals, days of therapy, the outcome, and the concomitant complications developed by the patient.
Author Contributions
Conceptualization, C.B. and A.C.T.; methodology, E.B.; software, E.B.; validation, C.B., A.C.T. and G.M.; formal analysis, E.B.; investigation, C.B. and E.B.; data curation, E.B.; writing—original draft preparation, C.B., E.B., A.C.T. and G.M.; writing—review and editing, L.B., G.M. and S.C.; supervision, G.M. and S.C. All authors have read and agreed to the published version of the manuscript.
Funding
This research received no external funding.
Institutional Review Board Statement
Not applicable.
Informed Consent Statement
Not applicable.
Data Availability Statement
Not applicable.
Conflicts of Interest
The authors declare no conflict of interest.
References
- Neofytos, D.; Fishman, J.A.; Horn, D.; Anaissie, E.; Chang, C.H.; Olyaei, A.; Pfaller, M.; Steinbach, W.J.; Webster, K.M.; Marr, K.A. Epidemiology and outcome of invasive fungal infections in solid organ transplant recipients. Transpl. Infect. Dis. 2010, 12, 220–229. [Google Scholar] [CrossRef] [PubMed]
- Friedman, D.Z.P.; Schwartz, I.S. Emerging Fungal Infections: New Patients, New Patterns, and New Pathogens. J. Fungi 2019, 5, 67. [Google Scholar] [CrossRef] [PubMed]
- Dellière, S.; Rivero-Menendez, O.; Gautier, C.; Garcia-Hermoso, D.; Alastruey-Izquierdo, A.; Alanio, A. Emerging mould infections: Get prepared to meet unexpected fungi in your patient. Med. Mycol. 2020, 58, 156–162. [Google Scholar] [CrossRef] [PubMed]
- Corcione, S.; Lupia, T.; Raviolo, S.; Montrucchio, G.; Trentalange, A.; Curtoni, A.; Cavallo, R.; De Rosa, F.G. Putative invasive pulmonary aspergillosis within medical wards and intensive care units: A 4-year retrospective, observational, single-centre study. Intern. Emerg. Med. 2021, 16, 1619–1627. [Google Scholar] [CrossRef] [PubMed]
- Martin-Loeches, I.; Antonelli, M.; Cuenca-Estrella, M.; Dimopoulos, G.; Einav, S.; De Waele, J.J.; Garnacho-Montero, J.; Kanj, S.S.; Machado, F.R.; Montravers, P.; et al. ESICM/ESCMID task force on practical management of invasive candidiasis in critically ill patients. Intensive Care Med. 2019, 45, 789–805. [Google Scholar] [CrossRef]
- Montrucchio, G.; Lupia, T.; Lombardo, D.; Stroffolini, G.; Corcione, S.; De Rosa, F.G.; Brazzi, L. Risk factors for invasive aspergillosis in ICU patients with COVID-19: Current insights and new key elements. Ann. Intensive Care 2021, 11, 136. [Google Scholar] [CrossRef]
- Timsit, J.F.; Sonneville, R.; Kalil, A.C.; Bassetti, M.; Ferrer, R.; Jaber, S.; Lanternier, F.; Luyt, C.E.; Machado, F.; Mikulska, M.; et al. Diagnostic and therapeutic approach to infectious diseases in solid organ transplant recipients. Intensive Care Med. 2019, 45, 573–591. [Google Scholar] [CrossRef]
- Johnson, M.D.; Lewis, R.E.; Ashley, E.S.D.; Ostrosky-Zeichner, L.; Zaoutis, T.; Thompson, G.R.; Andes, D.R.; Walsh, T.J.; Pappas, P.G.; Cornely, O.A.; et al. Core Recommendations for Antifungal Stewardship: A Statement of the Mycoses Study Group Education and Research Consortium. J. Infect. Dis. 2020, 222, S175–S198. [Google Scholar] [CrossRef]
- De Rosa, F.G.; Corcione, S.; Montrucchio, G.; Brazzi, L.; Di Perri, G. Antifungal Treatment Strategies in the ICU: Beyond Meta-analysis. Turk. J. Anaesthesiol. Reanim. 2016, 44, 283–284. [Google Scholar] [CrossRef]
- Martin-Loeches, I.; Nseir, S.; Rodriguez, A.; Azoulay, E. Disease-specific gaps within fungal respiratory tract infections: Clinical features, diagnosis, and management in critically ill patients. Curr. Opin. Pulm. Med. 2022, 28, 218–224. [Google Scholar] [CrossRef]
- Anesi, J.A.; Baddley, J.W. Approach to the Solid Organ Transplant Patient with Suspected Fungal Infection. Infect. Dis. Clin. N. Am. 2016, 30, 277–296. [Google Scholar] [CrossRef]
- Lockhart, S.R.; Guarner, J. Emerging and reemerging fungal infections. Semin. Diagn. Pathol. 2019, 36, 177–181. [Google Scholar] [CrossRef]
- Harman, G.E.; Howell, C.R.; Viterbo, A.; Chet, I.; Lorito, M. Trichoderma species—Opportunistic, avirulent plant symbionts. Nat. Rev. Microbiol. 2004, 2, 43–56. [Google Scholar] [CrossRef]
- Sandoval-Denis, M.; Sutton, D.A.; Cano-Lira, J.F.; Gené, J.; Fothergill, A.W.; Wiederhold, N.P.; Guarro, J. Phylogeny of the clinically relevant species of the emerging fungus Trichoderma and their antifungal susceptibilities. J. Clin. Microbiol. 2014, 52, 2112–2125. [Google Scholar] [CrossRef]
- Moher, D.; Liberati, A.; Tetzlaff, J.; Altman, D.G. Preferred reporting items for systematic reviews and meta-analyses: The PRISMA statement. PLoS Med. 2009, 6, e1000097. [Google Scholar] [CrossRef]
- Robertson, M.H. Fungi in fluids—A hazard of intravenous therapy. J. Med. Microbiol. 1970, 3, 99–102. [Google Scholar] [CrossRef]
- Gil, M.R.E.; Corral, E.P.; Muñóz, R.M. Pulmonary mycoma cause by Trichoderma viride. Actas Dermosifiliogr. 1976, 67, 673–680. [Google Scholar]
- Loeppky, C.B.; Sprouse, R.F.; Carlson, J.V.; Everett, E.D. Trichoderma viride peritonitis. South. Med. J. 1983, 76, 798–799. [Google Scholar] [CrossRef]
- Ragnaud, J.M.; Marceau, C.; Roche-Bezian, M.C.; Wone, C. Trichoderma koningii peritonitis in continuous ambulatory peritoneal dialysis. Med. Mal. Infect. 1984, 14, 402–405. [Google Scholar] [CrossRef]
- Jacobs, F.; Byl, B.; Bourgeois, N.; Coremans-Pelseneer, J.; Florquin, S.; Depré, G.; Van de Stadt, J.; Adler, M.; Gelin, M.; Thys, J.P. Trichoderma viride infection in a liver transplant recipient. Mycoses 1992, 35, 301–303. [Google Scholar] [CrossRef]
- Imokawa, S.; Sato, A.; Taniguchi, M.; Imamura, M.; Shirai, T.; Suda, T.; Iwata, M.; Gemma, H. Two cases of acute eosinophilic pneumonia with precipitating antibody against Trichosporon cutaneum and Trichoderma viride. Nihon Kyobu Shikkan Gakkai Zasshi 1993, 31, 352–359. [Google Scholar] [PubMed]
- Tanis, B.C.; van der Pijl, H.; van Ogtrop, M.L.; Kibbelaar, R.E.; Chang, P.C. Fatal fungal peritonitis by Trichoderma longibrachiatum complicating peritoneal dialysis. Nephrol. Dial. Transpl. 1995, 10, 114–116. [Google Scholar]
- Gautheret, A.; Dromer, F.; Bourhis, J.H.; Andremont, A. Trichoderma pseudokoningii as a cause of fatal infection in a bone marrow transplant recipient. Clin. Infect. Dis. 1995, 20, 1063–1064. [Google Scholar] [CrossRef] [PubMed]
- Seguin, P.; Degeilh, B.; Grulois, I.; Gacouin, A.; Maugendre, S.; Dufour, T.; Dupont, B.; Camus, C. Successful treatment of a brain abscess due to Trichoderma longibrachiatum after surgical resection. Eur. J. Clin. Microbiol. Infect. Dis. 1995, 14, 445–448. [Google Scholar] [CrossRef]
- Kawaguchi, H.; Yasuba, H.; Yamashita, K.; Fukuma, H.; Misaki, K.; Sumitomo, S.; Kato, M.; Chihara, J. A case of acute eosinophilic pneumonia: Bronchoalveolar lavage findings before and after steroid treatment. Jpn. J. Thorac. Dis. 1995, 33, 738–744. [Google Scholar]
- Guiserix, J.; Ramdane, M.; Finielz, P.; Michault, A.; Rajaonarivelo, P. Trichoderma harzianum peritonitis in peritoneal dialysis. Nephron 1996, 74, 473–474. [Google Scholar] [CrossRef]
- Campos-Herrero, M.I.; Bordes, A.; Perera, A.; Ruiz, M.C.; Fernandez, A. Trichodermia koningii peritonitis in a patient undergoing peritoneal dialysis. Clin. Microbiol. Newsl. 1996, 18, 150–152. [Google Scholar] [CrossRef]
- Munoz, F.M.; Demmler, G.J.; Travis, W.R.; Ogden, A.K.; Rossmann, S.N.; Rinaldi, M.G. Trichoderma longibrachiatum infection in a pediatric patient with aplastic anemia. J. Clin. Microbiol. 1997, 35, 499–503. [Google Scholar] [CrossRef]
- Bren, A. Fungal peritonitis in patients on continuous ambulatory peritoneal dialysis. Eur. J. Clin. Microbiol. Infect. Dis. 1998, 17, 839–843. [Google Scholar] [CrossRef]
- Furukawa, H.; Kusne, S.; Sutton, D.A.; Manez, R.; Carrau, R.; Nichols, L.; Abu-Elmagd, K.; Skedros, D.; Todo, S.; Rinaldi, M.G. Acute invasive sinusitis due to Trichoderma longibrachiatum in a liver and small bowel transplant recipient. Clin. Infect. Dis. 1998, 26, 487–489. [Google Scholar] [CrossRef]
- Richter, S.; Cormican, M.G.; Pfaller, M.A.; Lee, C.K.; Gingrich, R.; Rinaldi, M.G.; Sutton, D.A. Fatal disseminated Trichoderma longibrachiatum infection in an adult bone marrow transplant patient: Species identification and review of the literature. J. Clin. Microbiol. 1999, 37, 1154–1160. [Google Scholar] [CrossRef]
- Guarro, J.; Antolín-Ayala, M.I.; Gené, J.; Gutiérrez-Calzada, J.; Nieves-Díez, C.; Ortoneda, M. Fatal case of Trichoderma harzianum infection in a renal transplant recipient. J. Clin. Microbiol. 1999, 37, 3751–3755. [Google Scholar] [CrossRef]
- Rota, S.; Marchesi, D.; Farina, C.; de Bièvre, C. Trichoderma pseudokoningii peritonitis in automated peritoneal dialysis patient successfully treated by early catheter removal. Perit. Dial. Int. 2000, 20, 91–93. [Google Scholar] [CrossRef]
- Bustamante-Labarta, M.H.; Caramutti, V.; Allende, G.N.; Weinschelbaum, E.; Torino, A.F. Unsuspected embolic fungal endocarditis of an aortic conduit diagnosed by transesophageal echocardiography. J. Am. Soc. Echocardiogr. 2000, 13, 953–954. [Google Scholar] [CrossRef]
- Amato, J.G.; Amato, V.S.; Neto, V.A.; Heins-Vaccari, E.M. An AIDS patient with Trichoderma. Rev. Soc. Bras. Med. Trop. 2002, 35, 269. [Google Scholar] [CrossRef]
- Chouaki, T.; Lavarde, V.; Lachaud, L.; Raccurt, C.P.; Hennequin, C. Invasive infections due to Trichoderma species: Report of 2 cases, findings of in vitro susceptibility testing, and review of the literature. Clin. Infect. Dis. 2002, 35, 1360–1367. [Google Scholar] [CrossRef]
- Myoken, Y.; Sugata, T.; Fujita, Y.; Asaoku, H.; Fujihara, M.; Mikami, Y. Fatal necrotizing stomatitis due to Trichoderma longibrachiatum in a neutropenic patient with malignant lymphoma: A case report. Int. J. Oral Maxillofac. Surg. 2002, 31, 688–691. [Google Scholar] [CrossRef]
- Eşel, D.; Koç, A.N.; Utaş, C.; Karaca, N.; Bozdemir, N. Fatal peritonitis due to Trichoderma sp. in a patient undergoing continuous ambulatory peritoneal dialysis. Mycoses 2003, 46, 71–73. [Google Scholar] [CrossRef]
- De Miguel, D.; Gómez, P.; González, R.; García-Suárez, J.; Cuadros, J.A.; Bañas, M.H.; Romanyk, J.; Burgaleta, C. Nonfatal pulmonary Trichoderma viride infection in an adult patient with acute myeloid leukemia: Report of one case and review of the literature. Diagn. Microbiol. Infect. Dis. 2005, 53, 33–37. [Google Scholar] [CrossRef]
- Alanio, A.; Brethon, B.; de Chauvin, M.F.; de Kerviler, E.; Leblanc, T.; Lacroix, C.; Baruchel, A.; Menotti, J. Invasive pulmonary infection due to Trichoderma longibrachiatum mimicking invasive Aspergillosis in a neutropenic patient successfully treated with voriconazole combined with caspofungin. Clin. Infect. Dis. 2008, 46, e116–e118. [Google Scholar] [CrossRef]
- Kviliute, R.; Paskevicius, A.; Gulbinovic, J.; Stulpinas, R.; Griskevicius, L. Nonfatal Trichoderma citrinoviride pneumonia in an acute myeloid leukemia patient. Ann. Hematol. 2008, 87, 501–502. [Google Scholar] [CrossRef] [PubMed]
- Lagrange-Xélot, M.; Schlemmer, F.; Gallien, S.; Lacroix, C.; Molina, J.M. Trichoderma fungaemia in a neutropenic patient with pulmonary cancer and human immunodeficiency virus infection. Clin. Microbiol. Infect. 2008, 14, 1190–1192. [Google Scholar] [CrossRef] [PubMed]
- Trabelsi, S.; Hariga, D.; Khaled, S. First case of Trichoderma longibrachiatum infection in a renal transplant recipient in Tunisia and review of the literature. Tunis. Med. 2010, 88, 52–57. [Google Scholar] [PubMed]
- Salas, C.F.S.; Joshi, A.Y.; Dhiman, N.; Banerjee, R.; Huskins, W.C.; Wengenack, N.L.; Henry, N.K. Fatal post-operative Trichoderma longibrachiatum mediastinitis and peritonitis in a paediatric patient with complex congenital cardiac disease on peritoneal dialysis. J. Med. Microbiol. 2011, 60, 1869–1871. [Google Scholar] [CrossRef] [PubMed]
- Peralta, L.I.R.; Vera, M.R.M.; Delgado, M.J.G.; de la Cruz, A.J.P. Endocarditis caused by Trichoderma longibrachiatumin a patient receiving home parenteral nutrition. Nutr. Hosp. 2013, 28, 961–964. [Google Scholar] [CrossRef]
- Molnár-Gábor, E.; Dóczi, I.; Hatvani, L.; Vágvölgyi, C.; Kredics, L. Isolated sinusitis sphenoidalis caused by Trichoderma longibrachiatum in an immunocompetent patient with headache. J. Med. Microbiol. 2013, 62, 1249–1252. [Google Scholar] [CrossRef]
- Festuccia, M.; Giaccone, L.; Gay, F.; Brunello, L.; Maffini, E.; Ferrando, F.; Talamo, E.; Boccadoro, M.; Serra, R.; Barbui, A.; et al. Trichoderma species fungemia after high-dose chemotherapy and autologous stem cell transplantation: A case report. Transpl. Infect. Dis. 2014, 16, 653–657. [Google Scholar] [CrossRef]
- Tascini, C.; Cardinali, G.; Barletta, V.; Di Paolo, A.; Leonildi, A.; Zucchelli, G.; Corte, L.; Colabella, C.; Roscini, L.; Consorte, A.; et al. First Case of Trichoderma longibrachiatum CIED (Cardiac Implantable Electronic Device)-Associated Endocarditis in a Non-immunocompromised Host: Biofilm Removal and Diagnostic Problems in the Light of the Current Literature. Mycopathologia 2016, 181, 297–303. [Google Scholar] [CrossRef]
- Akagi, T.; Kawamura, C.; Terasawa, N.; Yamaguchi, K.; Kubo, K. Suspected Pulmonary Infection with Trichoderma longibrachiatum after Allogeneic Stem Cell Transplantation. Intern. Med. 2017, 56, 215–219. [Google Scholar] [CrossRef]
- Carlson, J.; Staiano, P.P.; James, L.R. A rare presentation of an unusual fungus: Trichoderma peritonitis. J. Am. Soc. Nephrol. 2018, 29, 586. [Google Scholar]
- Román-Soto, S.; Álvarez-Rojas, E.; García-Rodríguez, J. Skin infection due to Trichoderma longibrachiatum in a haematological paediatric patient. Clin. Microbiol. Infect. 2019, 25, 1383–1384. [Google Scholar] [CrossRef]
- Sautour, M.; Chrétien, M.L.; Valot, S.; Lafon, I.; Basmaciyan, L.; Legouge, C.; Verrier, T.; Gonssaud, B.; Abou-Hanna, H.; Dalle, F.; et al. First case of proven invasive pulmonary infection due to Trichoderma longibrachiatum in a neutropenic patient with acute leukemia. J. Mycol. Med. 2018, 28, 659–662. [Google Scholar] [CrossRef]
- Recio, R.; Meléndez-Carmona, M.; Martín-Higuera, M.C.; Pérez, V.; López, E.; López-Medrano, F.; Pérez-Ayala, A. Trichoderma longibrachiatum: An unusual pathogen of fungal pericarditis. Clin. Microbiol. Infect. 2019, 25, 586–587. [Google Scholar] [CrossRef]
- Bachu, R.; Hemmings, S.C.; Siddamreddy, S. A rare case of Trichoderma-related peritonitis in a patient on peritoneal dialysis. J. Am. Soc. Nephrol. 2020, 31, 424. [Google Scholar] [CrossRef]
- Zhou, Y.B.; Zhang, G.J.; Song, Y.G.; Sun, L.N.; Chen, Y.H.; Sun, T.T.; Li, R.Y.; Liu, W.; Li, D.M. Application of laser capture microdissection and polymerase chain reaction in the diagnosis of Trichoderma longibrachiatum infection: A promising diagnostic tool for ‘fungal contaminants’ infection. Med. Mycol. 2020, 58, 315–321. [Google Scholar] [CrossRef]
- Georgakopoulou, V.E.; Melemeni, D.; Mantzouranis, K.; Damaskos, C.; Gkoufa, A.; Chlapoutakis, S.; Garmpis, N.; Garmpi, A.; Sklapani, P.; Trakas, N.; et al. Firstcase of pneumonia-parapneumonic effusion due to Trichoderma longibrachiatum. IDCases 2021, 25, e01239. [Google Scholar] [CrossRef]
- Al-Shehri, A.; Aljohani, S.; Semidey, V.A. Bilateral endogenous Trichoderma endophthalmitis in an immunocompromised host. Am. J. Ophthalmol. Case Rep. 2021, 24, 101234. [Google Scholar] [CrossRef]
- Fisher, M.C.; Hawkins, N.J.; Sanglard, D.; Gurr, S.J. Worldwide emergence of resistance to antifungal drugs challenges human health and food security. Science 2018, 360, 739–742. [Google Scholar] [CrossRef]
- Lamoth, F.; Kontoyiannis, D.P. Therapeutic Challenges of Non-Aspergillus Invasive Mold Infections in Immunosuppressed Patients. Antimicrob. Agents Chemother. 2019, 63, e01244-19. [Google Scholar] [CrossRef]
- Shoham, S. Emerging fungal infections in solid organ transplant recipients. Infect. Dis. Clin. N. Am. 2013, 27, 305–316. [Google Scholar] [CrossRef]
- Husain, S.; Camargo, J.F. Invasive Aspergillosis in solid-organ transplant recipients: Guidelines from the American Society of Transplantation Infectious Diseases Community of Practice. Clin. Transplant. 2019, 33, e13544. [Google Scholar] [CrossRef] [PubMed]
- Ascioglu, S.; Rex, J.H.; de Pauw, B.; Bennett, J.E.; Bille, J.; Crokaert, F.; Denning, D.W.; Donnelly, J.P.; Edwards, J.E.; Erjavec, Z.; et al. Defining opportunistic invasive fungal infections in immunocompromised patients with cancer and hematopoietic stem cell transplants: An international consensus. Clin. Infect. Dis. 2002, 34, 7–14. [Google Scholar] [CrossRef] [PubMed]
- Giacobbe, D.R.; Cortegiani, A.; Karaiskos, I.; Mercier, T.; Tejada, S.; Peghin, M.; Grecchi, C.; Rebuffi, C.; Asperges, E.; Zuccaro, V.; et al. Performance of Existing Definitions and Tests for the Diagnosis of Invasive Fungal Diseases other than Invasive Candidiasis and Invasive Aspergillosis in Critically Ill, Adult Patients: A Systematic Review with Qualitative Evidence Synthesis. J. Fungi 2021, 7, 176. [Google Scholar] [CrossRef] [PubMed]
- Cornely, O.A.; Arikan-Akdagli, S.; Dannaoui, E.; Groll, A.H.; Lagrou, K.; Chakrabarti, A.; Lanternier, F.; Pagano, L.; Skiada, A.; Akova, M.; et al. ESCMID and ECMM joint clinical guidelines for the diagnosis and management of mucormycosis 2013. Clin. Microbiol. Infect. 2014, 20 (Suppl. S3), 5–26. [Google Scholar] [CrossRef]
- Tortorano, A.M.; Richardson, M.; Roilides, E.; van Diepeningen, A.; Caira, M.; Munoz, P.; Johnson, E.; Meletiadis, J.; Pana, Z.D.; Lackner, M.; et al. ESCMID and ECMM joint guidelines on diagnosis and management of hyalohyphomycosis: Fusarium spp., Scedosporium spp. and others. Clin. Microbiol. Infect. 2014, 20 (Suppl. S3), 27–46. [Google Scholar] [CrossRef]
- Kidd, S.E.; Crawford, L.C.; Halliday, C.L. Antifungal Susceptibility Testing and Identification. Infect. Dis. Clin. N. Am. 2021, 35, 313–339. [Google Scholar] [CrossRef]
- Husain, B.; Kirchberger, M.C.; Erdmann, M.; Schüpferling, S.; Abolhassani, A.R.; Fröhlich, W.; Berking, C.; Heinzerling, L. Inflammatory markers in autoimmunity induced by checkpoint inhibitors. J. Cancer Res. Clin. Oncol. 2021, 147, 1623–1630. [Google Scholar] [CrossRef]
- Ashbee, H.R.; Barnes, R.A.; Johnson, E.M.; Richardson, M.D.; Gorton, R.; Hope, W.W. Therapeutic drug monitoring (TDM) of antifungal agents: Guidelines from the British Society for Medical Mycology. J. Antimicrob. Chemother. 2014, 69, 1162–1176. [Google Scholar] [CrossRef]
- Lamoth, F.; Lewis, R.E.; Kontoyiannis, D.P. Role and Interpretation of Antifungal Susceptibility Testing for the Management of Invasive Fungal Infections. J. Fungi 2020, 7, 17. [Google Scholar] [CrossRef]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).