Tribomechanical Properties of PVA/Nomex® Composite Hydrogels for Articular Cartilage Repair
Abstract
1. Introduction
2. Results and Discussion
2.1. Morphology
2.2. Chemical and Thermal Characterization
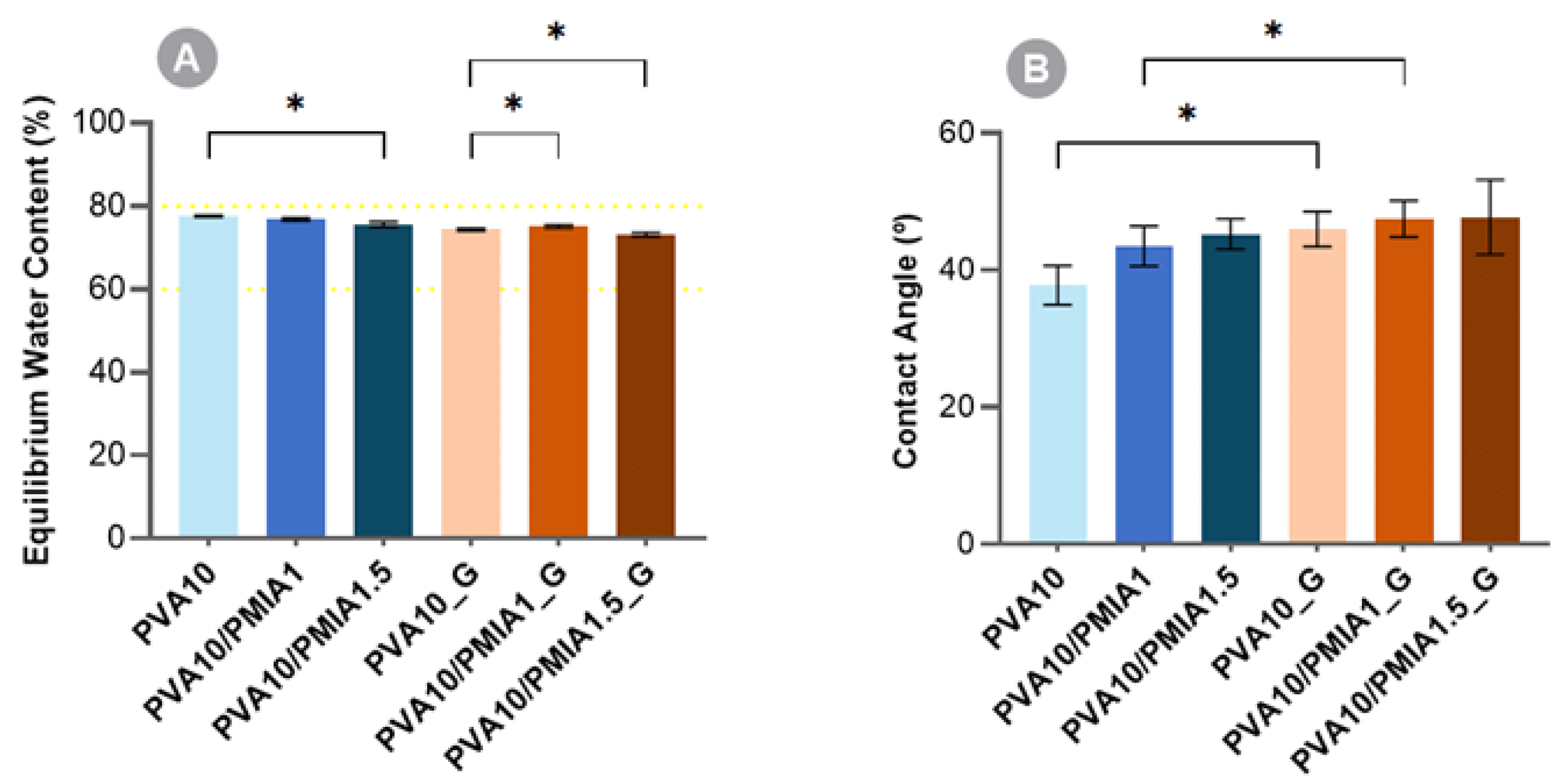
2.3. Equilibrium Water Content and Wettability
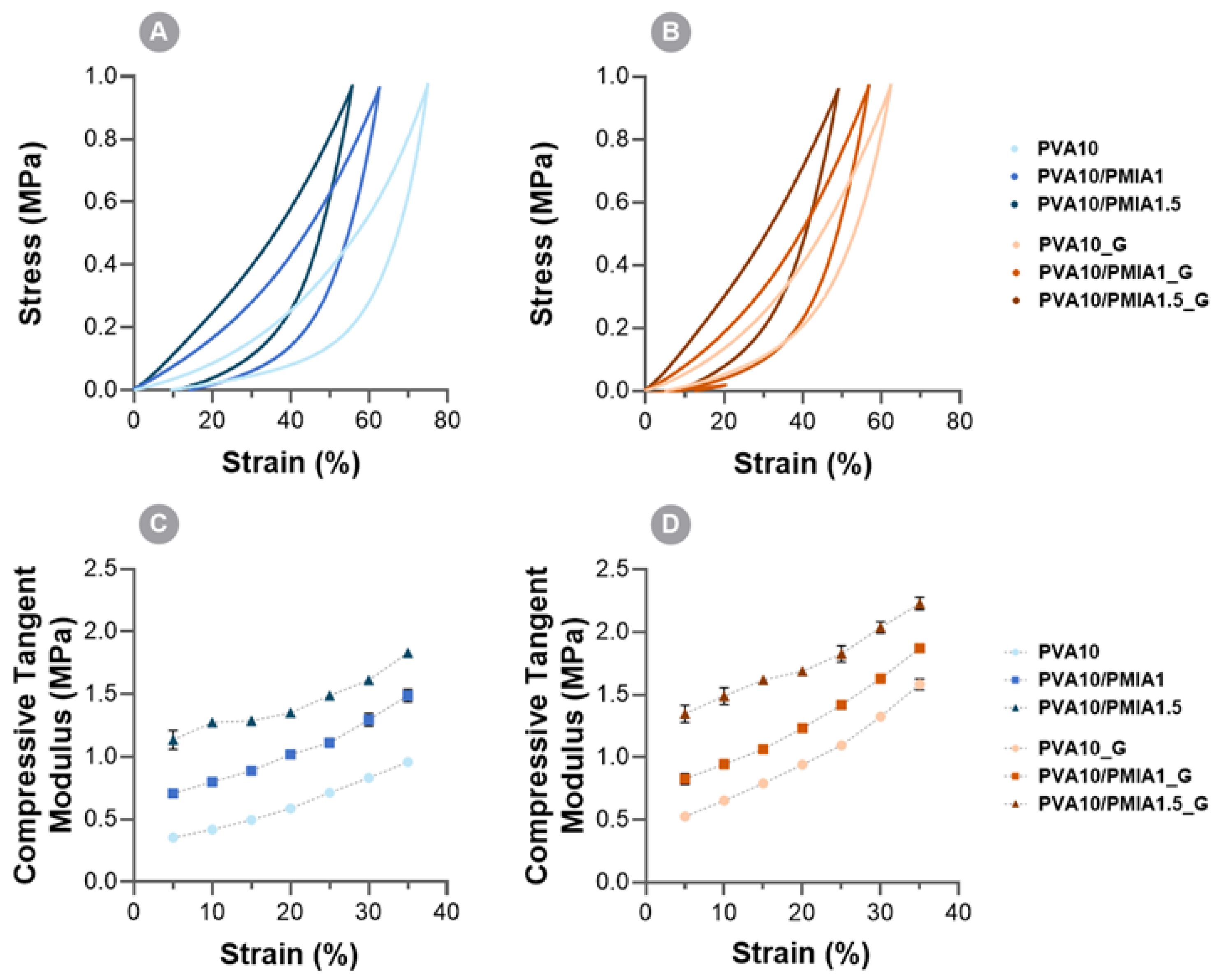
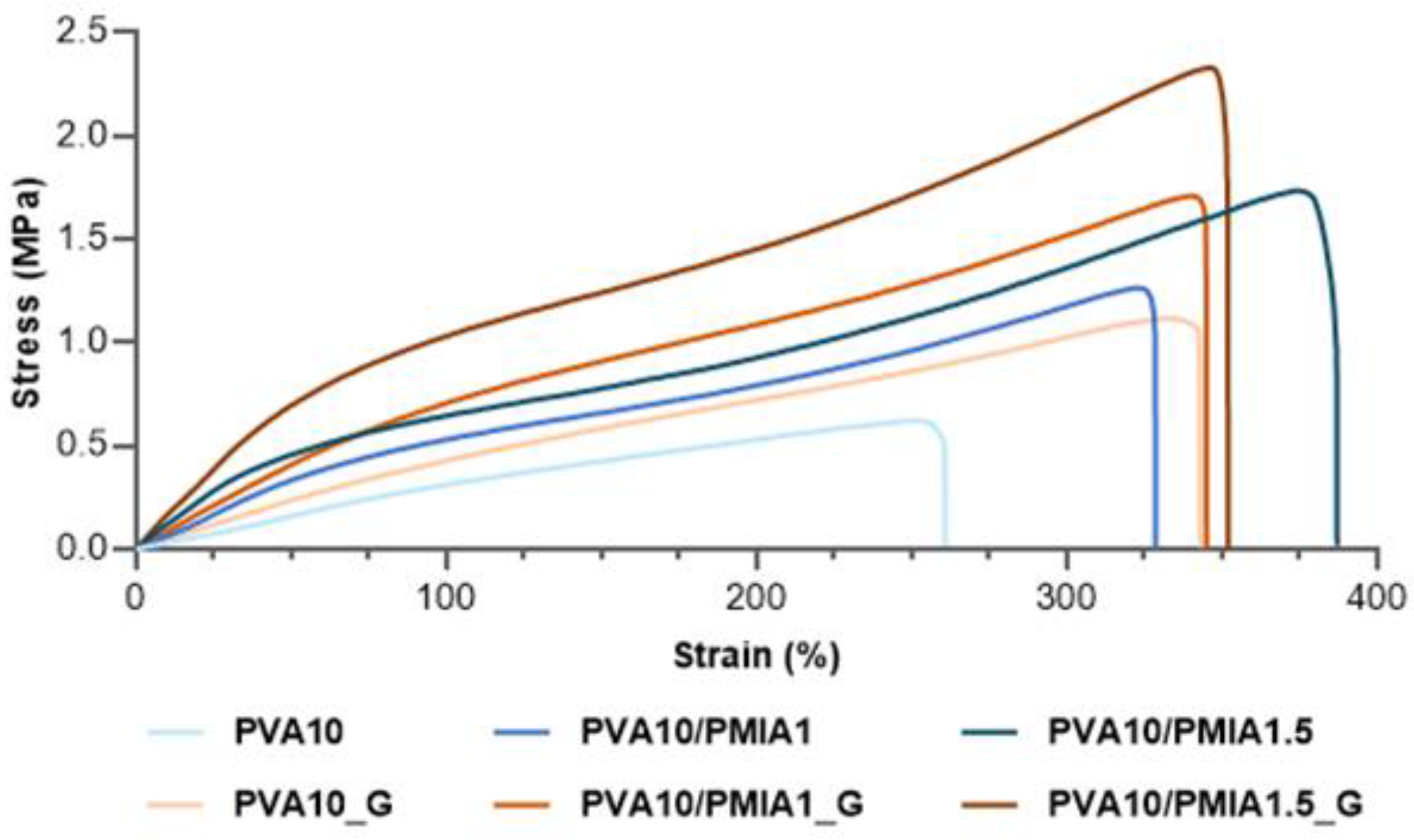
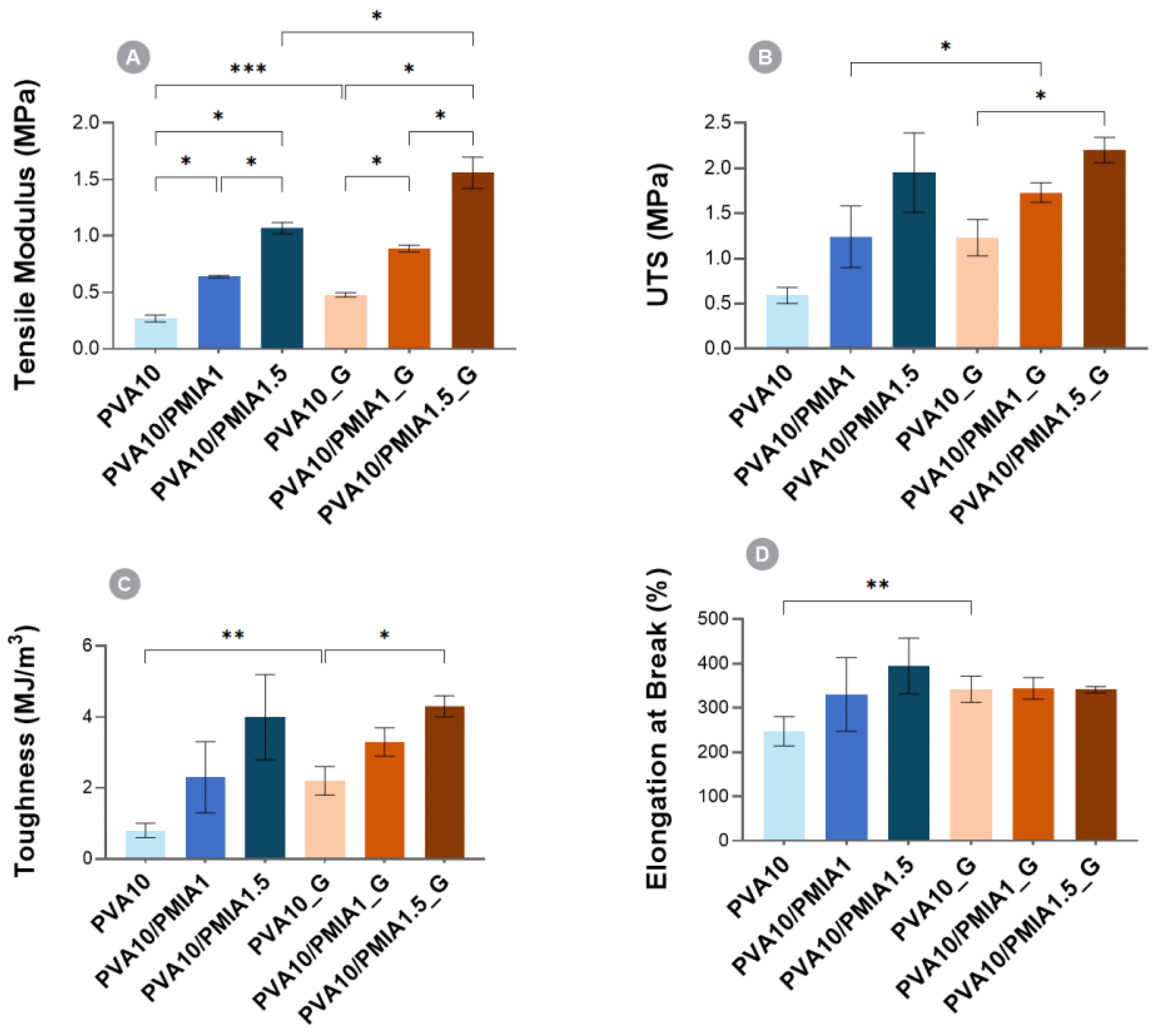
2.4. Mechanical Properties
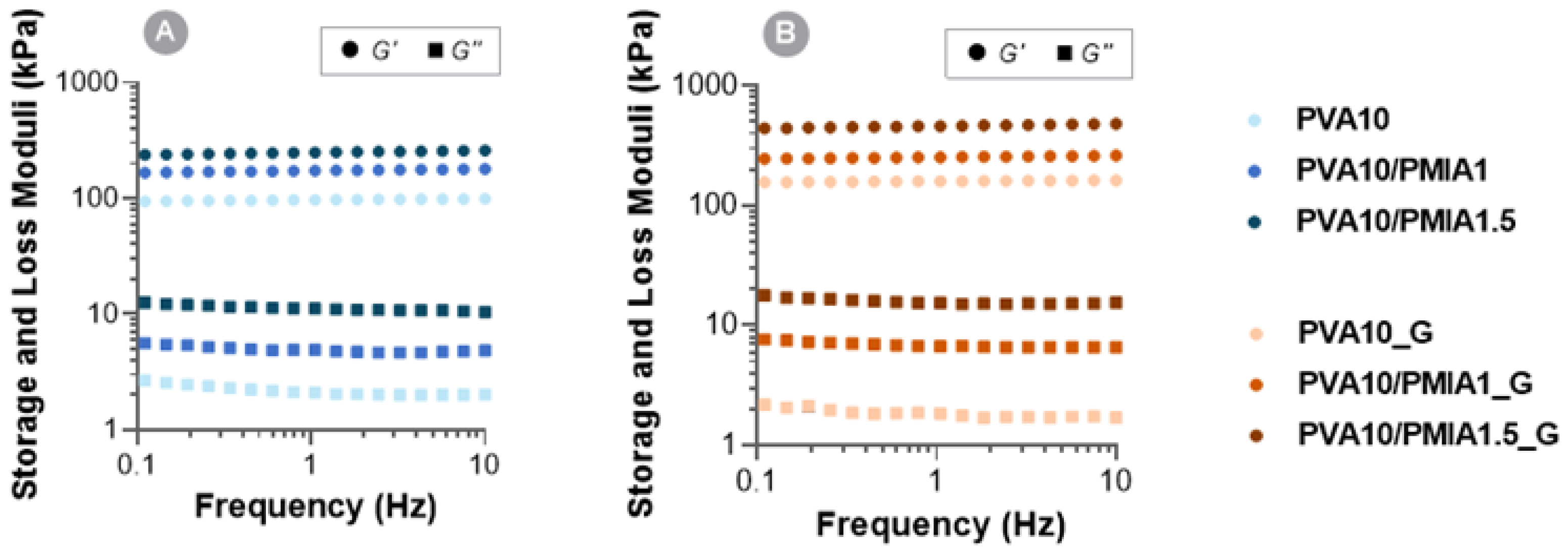
2.5. Rheological Behavior
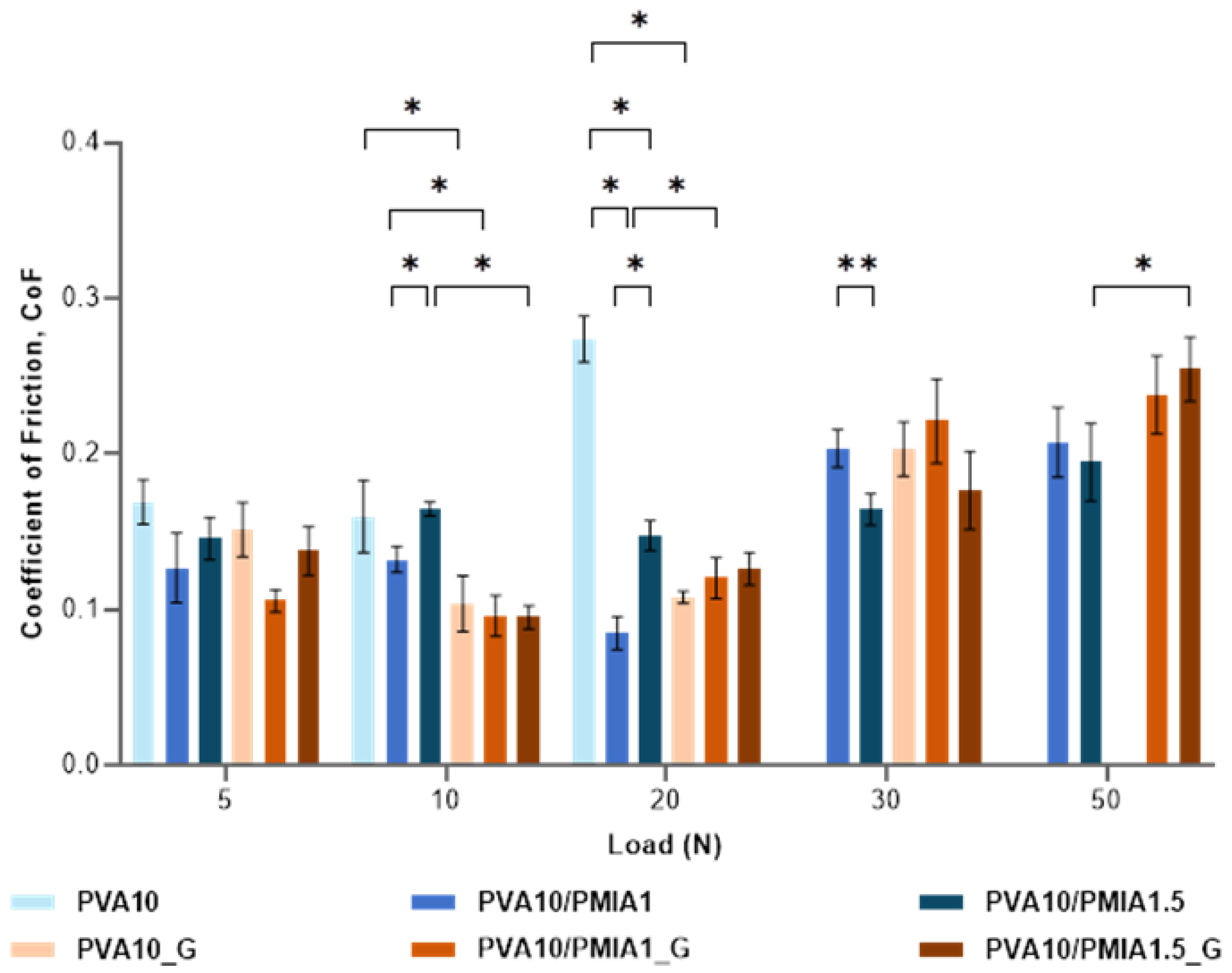
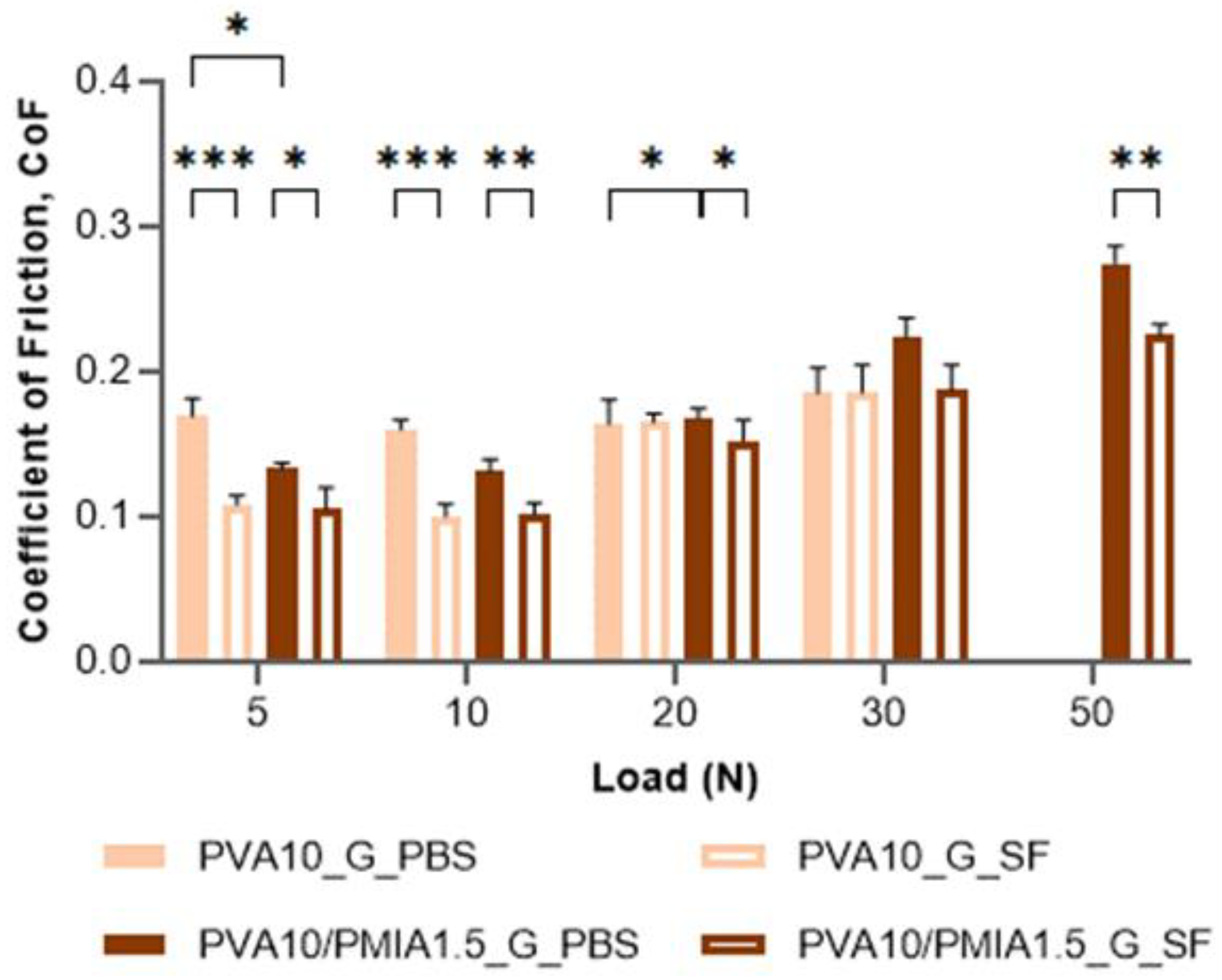
2.6. Tribological Behavior
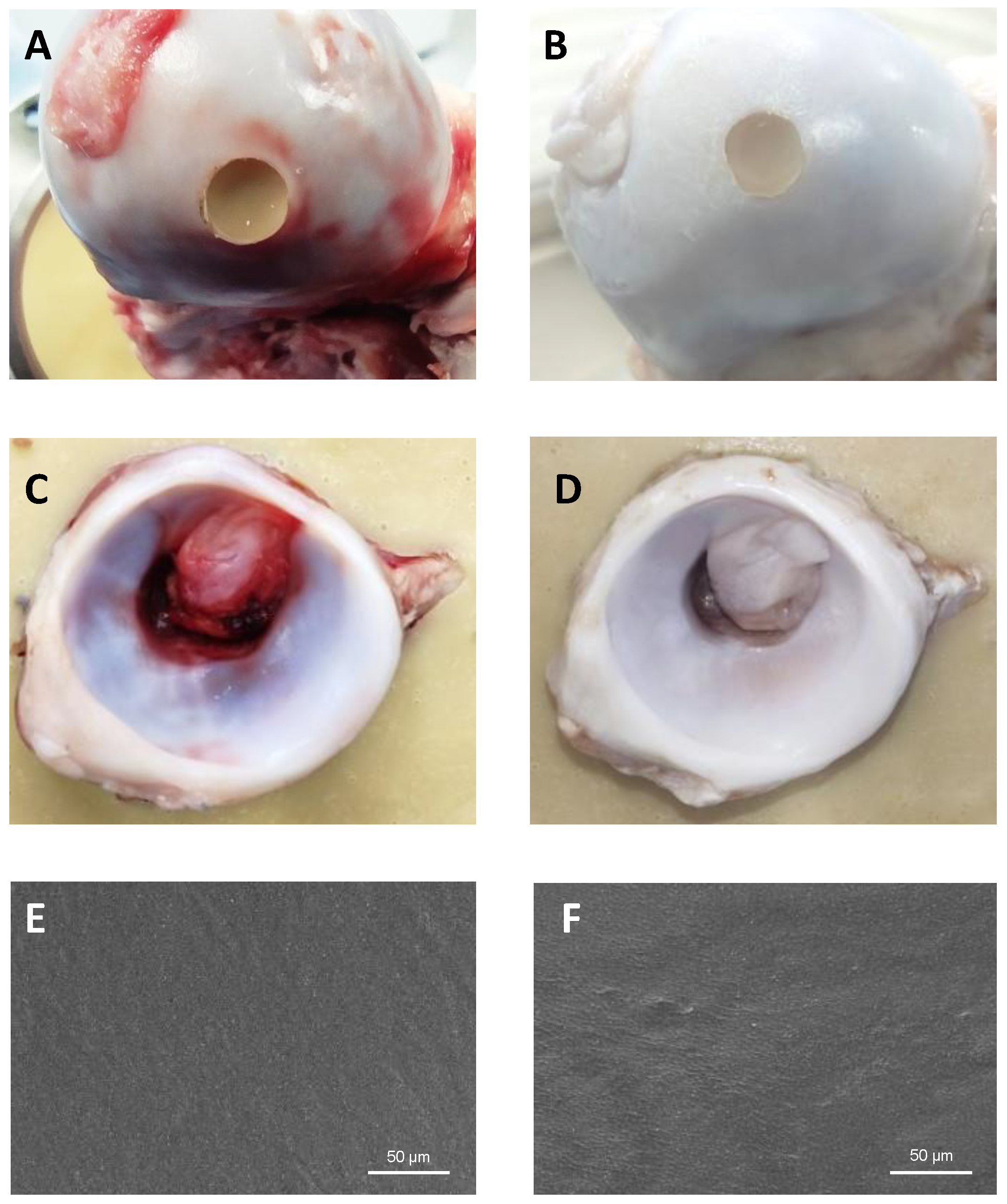
2.7. Proof of Concept Using a Hip Simulator
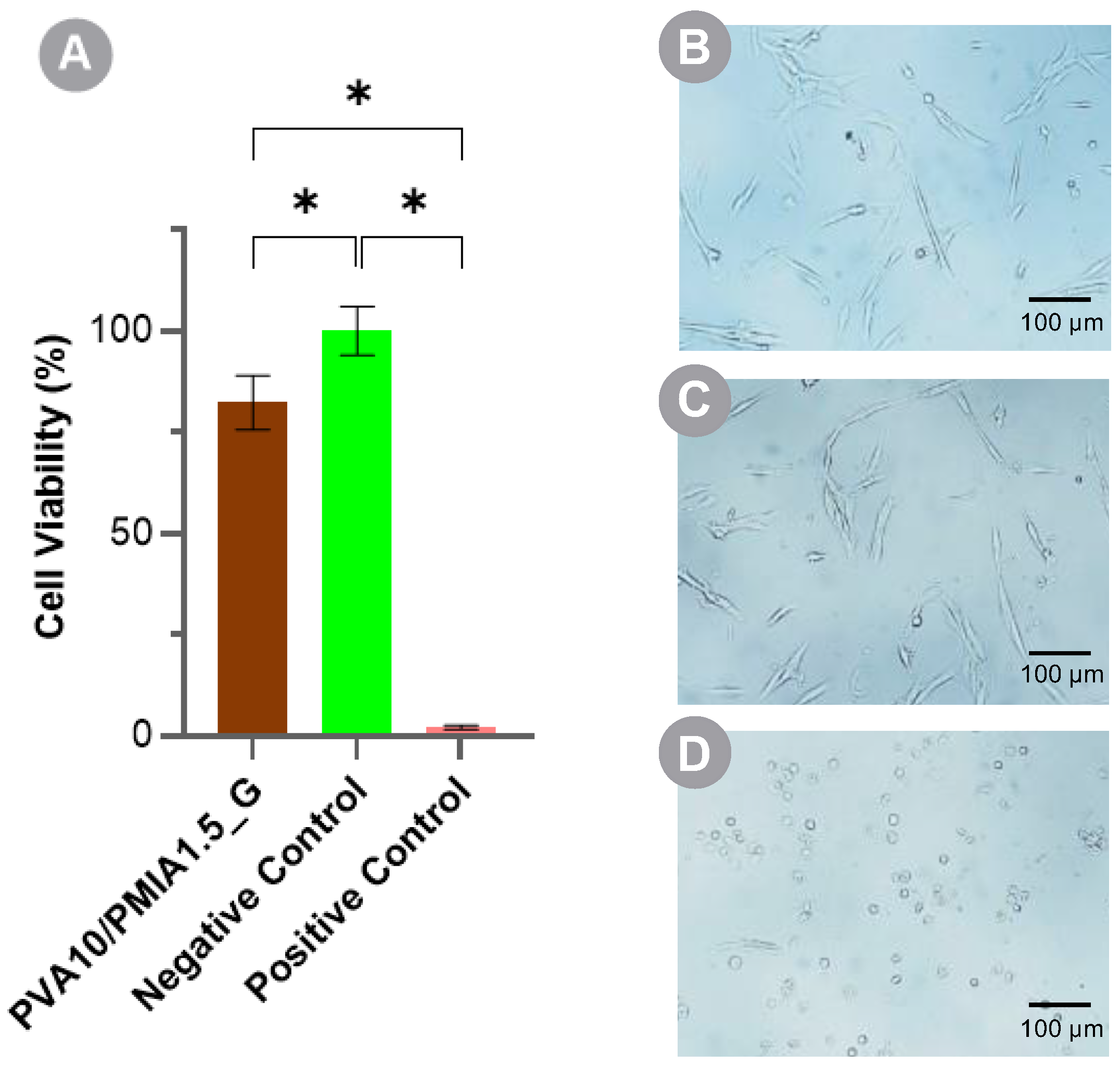
2.8. Cytotoxicity
3. Conclusions
4. Materials and Methods
4.1. Materials
4.2. Preparation of the Materials
4.3. Sterilization
4.4. Morphological Characterization
4.5. Chemical and Thermal Characterization
4.6. Equilibrium Water Content and Wettability
4.7. Mechanical Properties
4.8. Rheological Properties
4.9. Tribological Behavior
4.10. Hip Movement Simulation
4.10.1. Preparation and Fixation of the Hip Joints
4.10.2. Hydrogel Plug Preparation
4.10.3. Experimental Testing: Setup and Parameters
4.11. Cytotoxicity
4.12. Statistical Analysis
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Ledingham, J.; Snowden, N.; Ide, Z. Diagnosis and early management of inflammatory arthritis. BMJ 2017, 358, j3248. [Google Scholar] [CrossRef]
- Katta, J.; Pawaskar, S.S.; Jin, Z.M.; Ingham, E.; Fisher, J. Effect of load variation on the friction properties of articular cartilage. Proc. Inst. Mech. Eng. Part J J. Eng. Tribol. 2007, 221, 175–181. [Google Scholar] [CrossRef]
- Danso, E.; Honkanen, J.; Saarakkala, S.; Korhonen, R. Comparison of nonlinear mechanical properties of bovine articular cartilage and meniscus. J. Biomech. 2014, 47, 200–206. [Google Scholar] [CrossRef]
- Murakami, T.; Yarimitsu, S.; Sakai, N.; Nakashima, K.; Yamaguchi, T.; Sawae, Y.; Suzuki, A. Superior lubrication mechanism in poly(vinyl alcohol) hybrid gel as artificial cartilage. Proc. Inst. Mech. Eng. Part J J. Eng. Tribol. 2017, 231, 1160–1170. [Google Scholar] [CrossRef]
- Katz, J.N.; Arant, K.R.; Loeser, R.F. Diagnosis and Treatment of Hip and Knee Osteoarthritis: A Review. JAMA 2021, 325, 568–578. [Google Scholar] [CrossRef]
- Cross, M.; Smith, E.; Hoy, D.; Nolte, S.; Ackerman, I.; Fransen, M.; Bridgett, L.; Williams, S.; Guillemin, F.; Hill, C.L.; et al. The global burden of hip and knee osteoarthritis: Estimates from the Global Burden of Disease 2010 study. Ann. Rheum. Dis. 2014, 73, 1323–1330. [Google Scholar] [CrossRef]
- Beddoes, C.M.; Whitehouse, M.R.; Briscoe, W.H.; Su, B. Hydrogels as a Replacement Material for Damaged Articular Hyaline Cartilage. Materials 2016, 9, 443. [Google Scholar] [CrossRef]
- Jeuken, R.M.; van Hugten, P.P.; Roth, A.K.; Timur, U.T.; Boymans, T.A.; van Rhijn, L.W.; Bugbee, W.D.; Emans, P.J. A Systematic Review of Focal Cartilage Defect Treatments in Middle-Aged Versus Younger Patients. Orthop. J. Sports Med. 2021, 9, 232596712110312. [Google Scholar] [CrossRef]
- Gowd, A.K.; Weimer, A.E.; Rider, D.E.; Beck, E.C.; Agarwalla, A.; O’brien, L.K.; Alaia, M.J.; Ferguson, C.M.; Waterman, B.R. Cartilage Restoration for Tibiofemoral Bipolar Lesions Results in Promising Failure Rates: A Systematic Review. Arthrosc. Sports Med. Rehabil. 2021, 3, e1227–e1235. [Google Scholar] [CrossRef]
- Orthopaedics, J.R. MaioRegen Ostheochondral Substitute. Available online: https://jri-ltd.com/our-products/orthobiologics/maioregen (accessed on 15 July 2024).
- Stryker. Cartiva Synthetic Cartilage Implant. Available online: https://www.stryker.com/us/en/foot-and-ankle/products/cartiva.html (accessed on 15 July 2024).
- BioPoly. Available online: https://biopolyortho.com/ (accessed on 15 July 2024).
- Brix, M.; Kaipel, M.; Kellner, R.; Schreiner, M.; Apprich, S.; Boszotta, H.; Windhager, R.; Domayer, S.; Trattnig, S. Successful osteoconduction but limited cartilage tissue quality following osteochondral repair by a cell-free multilayered nano-composite scaffold at the knee. Int. Orthop. (SICOT) 2016, 40, 625–632. [Google Scholar] [CrossRef]
- Radcliffe, M.J.; Roukis, T.S. A review of adverse events related to synthetic cartilage implant for the first metatarsophalangeal joint: An analysis of Manufacturer and User Facility Device Experience database from 2016 to 2023. Foot Ankle Surg. Tech. Rep. Cases 2024, 4, 100356. [Google Scholar] [CrossRef]
- Oliveira, A.S.; Silva, J.C.; Loureiro, M.V.; Marques, A.C.; Kotov, N.A.; Colaço, R.; Serro, A.P. Super-Strong Hydrogel Composites Reinforced with PBO Nanofibers for Cartilage Replacement. Macromol. Biosci. 2023, 23, e2200240. [Google Scholar] [CrossRef] [PubMed]
- Zhu, L.; Liu, Y.; Jiang, Z.; Sakai, E.; Qiu, J.; Zhu, P. Highly temperature resistant cellulose nanofiber/polyvinyl alcohol hydrogel using aldehyde cellulose nanofiber as cross-linker. Cellulose 2019, 26, 5291–5303. [Google Scholar] [CrossRef]
- Chronopoulou, L.; Cacciotti, I.; Amalfitano, A.; Di Nitto, A.; D’arienzo, V.; Nocca, G.; Palocci, C. Biosynthesis of innovative calcium phosphate/hydrogel composites: Physicochemical and biological characterisation. Nanotechnology 2021, 32, 095102. [Google Scholar] [CrossRef] [PubMed]
- Mahinroosta, M.; Farsangi, Z.J.; Allahverdi, A.; Shakoori, Z. Hydrogels as intelligent materials: A brief review of synthesis, properties and applications. Mater. Today Chem. 2018, 8, 42–55. [Google Scholar] [CrossRef]
- Branco, A.C.; Oliveira, A.S.; Monteiro, I.; Nolasco, P.; Silva, D.C.; Figueiredo-Pina, C.G.; Colaço, R.; Serro, A.P. PVA-Based Hydrogels Loaded with Diclofenac for Cartilage Replacement. Gels 2022, 8, 143. [Google Scholar] [CrossRef] [PubMed]
- Li, F.; Wang, A.; Wang, C. Analysis of friction between articular cartilage and polyvinyl alcohol hydrogel artificial cartilage. J. Mater. Sci. Mater. Med. 2016, 27, 87. [Google Scholar] [CrossRef] [PubMed]
- Baker, M.I.; Walsh, S.P.; Schwartz, Z.; Boyan, B.D. A review of polyvinyl alcohol and its uses in cartilage and orthopedic applications. J. Biomed. Mater. Res. Part B Appl. Biomater. 2012, 100B, 1451–1457. [Google Scholar] [CrossRef] [PubMed]
- Nečas, D.; Yarimitsu, S.; Rebenda, D.; Shinmori, H.; Vrbka, M.; Sawae, Y.; Murakami, T.; Křupka, I. On the replacement of articular cartilage: The friction of PVA hydrogel layer in hip simulator test. Tribol. Int. 2023, 178, 108100. [Google Scholar] [CrossRef]
- Maiolo, A.S.; Amado, M.N.; Gonzalez, J.S.; Alvarez, V.A. Development and characterization of Poly (vinyl alcohol) based hydrogels for potential use as an articular cartilage replacement. Mater. Sci. Eng. C 2012, 32, 1490–1495. [Google Scholar] [CrossRef]
- Oliveira, A.S.; Schweizer, S.; Nolasco, P.; Barahona, I.; Saraiva, J.; Colaço, R.; Serro, A.P. Tough and Low Friction Polyvinyl Alcohol Hydrogels Loaded with Anti-inflammatories for Cartilage Replacement. Lubricants 2020, 8, 36. [Google Scholar] [CrossRef]
- Zhong, Y.; Lin, Q.; Yu, H.; Shao, L.; Cui, X.; Pang, Q.; Zhu, Y.; Hou, R. Construction methods and biomedical applications of PVA-based hydrogels. Front. Chem. 2024, 12, 1376799. [Google Scholar] [CrossRef]
- Trucco, D.; Vannozzi, L.; Teblum, E.; Telkhozhayeva, M.; Nessim, G.D.; Affatato, S.; Al-Haddad, H.; Lisignoli, G.; Ricotti, L. Graphene Oxide-Doped Gellan Gum–PEGDA Bilayered Hydrogel Mimicking the Mechanical and Lubrication Properties of Articular Cartilage. Adv. Healthc. Mater. 2021, 10, 2001434. [Google Scholar] [CrossRef] [PubMed]
- Jalageri, M.B.; Kumar, G.C.M. Hydroxyapatite Reinforced Polyvinyl Alcohol/Polyvinyl Pyrrolidone Based Hydrogel for Cartilage Replacement. Gels 2022, 8, 555. [Google Scholar] [CrossRef]
- Song, K.; Zhu, W.; Li, X.; Yu, Z. A novel mechanical robust, self-healing and shape memory hydrogel based on PVA reinforced by cellulose nanocrystal. Mater. Lett. 2020, 260, 126884. [Google Scholar] [CrossRef]
- Xu, L.; Zhao, X.; Xu, C.; Kotov, N.A. Water-Rich Biomimetic Composites with Abiotic Self-Organizing Nanofiber Network. Adv. Mater. 2018, 1703343. [Google Scholar] [CrossRef]
- Deopura, B.L.; Padaki, N.V. Synthetic Textile Fibres. In Textiles and Fashion; Elsevier: Amsterdam, The Netherlands, 2015; pp. 97–114. [Google Scholar] [CrossRef]
- Du, W.; Zhang, J.; Zhao, Z.; Zhang, X. Preparation of novel temperature-responsive double-network hydrogel reinforced with aramid nanofibers. Compos. Commun. 2020, 22, 100438. [Google Scholar] [CrossRef]
- Avci, H.; Hassanin, A.; Hamouda, T.; Kiliç, A. High performance fibers: A review on current state of art and future challenges. Eskişehir Osman. Üniversitesi Mühendislik Ve Mimar. Fakültesi Derg. 2019, 27, 130–155. [Google Scholar] [CrossRef]
- Yang, M.; Cao, K.; Sui, L.; Qi, Y.; Zhu, J.; Waas, A.; Arruda, E.M.; Kieffer, J.; Thouless, M.D.; Kotov, N.A. Dispersions of Aramid Nanofibers: A New Nanoscale Building Block. ACS Nano 2011, 5, 6945–6954. [Google Scholar] [CrossRef]
- Guan, Y.; Li, W.; Zhang, Y.; Shi, Z.; Tan, J.; Wang, F.; Wang, Y. Aramid nanofibers and poly (vinyl alcohol) nanocomposites for ideal combination of strength and toughness via hydrogen bonding interactions. Compos. Sci. Technol. 2017, 144, 193–201. [Google Scholar] [CrossRef]
- Guo, Y.; An, X.; Fan, Z. Aramid nanofibers reinforced polyvinyl alcohol/tannic acid hydrogel with improved mechanical and antibacterial properties for potential application as wound dressing. J. Mech. Behav. Biomed. Mater. 2021, 118, 104452. [Google Scholar] [CrossRef] [PubMed]
- Kotov, N.A.; Yang, M.; Cao, K.; Thouless, M.D.; Arruda, E.M.; Waas, A.M.; Siepermann, C.A.P.; Anderson, R.M. Synthesis and Use of Aramid Nanofibers. U.S. Patent 1,016,083,3B2, 26 April 2012. Available online: https://patents.google.com/patent/US10160833B2/en (accessed on 11 November 2023).
- DuPont. Nomex® Fiber Technical Guide. Available online: https://www.dupont.com/content/dam/dupont/amer/us/en/personal-protection/public/documents/en/Nomex(R)%20Fiber%20Technical%20Guide.pdf (accessed on 15 July 2024).
- Kim, S.; Jeong, J.-O.; Lee, S.; Park, J.-S.; Gwon, H.-J.; Jeong, S.I.; Hardy, J.G.; Lim, Y.-M.; Lee, J.Y. Effective gamma-ray sterilization and characterization of conductive polypyrrole biomaterials. Sci. Rep. 2018, 8, 3721. [Google Scholar] [CrossRef] [PubMed]
- dos Santos, V.; Brandalise, R.N.; Savaris, M. Biomaterials Sterilization Methods. In Engineering of Biomaterials; Springer: Cham, Switzerland, 2017; pp. 61–73. [Google Scholar] [CrossRef]
- Sasaki, S.; Suzuki, A. Factors influencing the swelling and elution properties of poly(vinyl alcohol) cast gels. Polym. Adv. Technol. 2016, 27, 318–324. [Google Scholar] [CrossRef]
- Yang, B.; Wang, L.; Zhang, M.; Luo, J.; Ding, X. Timesaving, High-Efficiency Approaches To Fabricate Aramid Nanofibers. ACS Nano 2019, 13, 7886–7897. [Google Scholar] [CrossRef] [PubMed]
- Marrella, A.; Lagazzo, A.; Dellacasa, E.; Pasquini, C.; Finocchio, E.; Barberis, F.; Pastorino, L.; Giannoni, P.; Scaglione, S. 3D Porous Gelatin/PVA Hydrogel as Meniscus Substitute Using Alginate Micro-Particles as Porogens. Polymers 2018, 10, 380. [Google Scholar] [CrossRef] [PubMed]
- Coluccino, L.; Gottardi, R.; Ayadi, F.; Athanassiou, A.; Tuan, R.S.; Ceseracciu, L. Porous Poly(vinyl alcohol)-Based Hydrogel for Knee Meniscus Functional Repair. ACS Biomater. Sci. Eng. 2018, 4, 1518–1527. [Google Scholar] [CrossRef]
- Oliveira, A.S.; Seidi, O.; Ribeiro, N.; Colaço, R.; Serro, A.P. Tribomechanical Comparison between PVA Hydrogels Obtained Using Different Processing Conditions and Human Cartilage. Materials 2019, 12, 3413. [Google Scholar] [CrossRef] [PubMed]
- Oliveira, A.S.; Silva, J.C.; Figueiredo, L.; Ferreira, F.C.; Kotov, N.A.; Colaço, R.; Serro, A.P. High-performance bilayer composites for the replacement of osteochondral defects. Biomater. Sci. 2022, 10, 5856–5875. [Google Scholar] [CrossRef] [PubMed]
- Pires, T.; Oliveira, A.S.; Marques, A.C.; Salema-Oom, M.; Figueiredo-Pina, C.G.; Silva, D.; Serro, A.P. Effects of Non-Conventional Sterilisation Methods on PBO-Reinforced PVA Hydrogels for Cartilage Replacement. Gels 2022, 8, 640. [Google Scholar] [CrossRef]
- Gomaa, M.M.; Hugenschmidt, C.; Dickmann, M.; Abdel-Hady, E.E.; Mohamed, H.F.M.; Abdel-Hamed, M.O. Crosslinked PVA/SSA proton exchange membranes: Correlation between physiochemical properties and free volume determined by positron annihilation spectroscopy. Phys. Chem. Chem. Phys. 2018, 20, 28287–28299. [Google Scholar] [CrossRef]
- Hong, X.; Zou, L.; Zhao, J.; Li, C.; Cong, L. Dry-wet spinning of PVA fiber with high strength and high Young’s modulus. IOP Conf. Ser. Mater. Sci. Eng. 2018, 439, 042011. [Google Scholar] [CrossRef]
- Reguieg, F.; Ricci, L.; Bouyacoub, N.; Belbachir, M.; Bertoldo, M. Thermal characterization by DSC and TGA analyses of PVA hydrogels with organic and sodium MMT. Polym. Bull. 2020, 77, 929–948. [Google Scholar] [CrossRef]
- Jinisha, B.; Anilkumar, K.M.; Manoj, M.; Ashraf, C.M.; Pradeep, V.S.; Jayalekshmi, S. Solid-state supercapacitor with impressive performance characteristics, assembled using redox-mediated gel polymer electrolyte. J. Solid State Electrochem. 2019, 23, 3343–3353. [Google Scholar] [CrossRef]
- Wang, L. Comparison and Analysis of Thermal Degradation Process of Aramid Fibers (Kevlar 49 and Nomex). J. Fiber Bioeng. Inform. 2010, 3, 163–167. [Google Scholar] [CrossRef]
- Ng, H.M.; Saidi, N.M.; Omar, F.S.; Ramesh, K.; Ramesh, S.; Bashir, S. Thermogravimetric Analysis of Polymers. In Encyclopedia of Polymer Science and Technology; Wiley: Hoboken, NJ, USA, 2018; pp. 1–29. [Google Scholar] [CrossRef]
- Radosavljević, A.; Spasojević, J.; Krstić, J.; Kačarević-Popović, Z. Nanocomposite Hydrogels Obtained by Gamma Irradiation. In Cellulose-Based Superabsorbent Hydrogels; Springer: Cham, Switzerland, 2019; pp. 601–623. [Google Scholar] [CrossRef]
- Wang, B.; Kodama, M.; Mukataka, S.; Kokufuta, E. On the intermolecular crosslinking of PVA chains in an aqueous solution by γ-ray irradiation. Polym. Gels Netw. 1998, 6, 71–81. [Google Scholar] [CrossRef]
- Zhang, S.-J.; Yu, H.-Q. Radiation-induced degradation of polyvinyl alcohol in aqueous solutions. Water Res. 2004, 38, 309–316. [Google Scholar] [CrossRef]
- Martínez-Barrera, G.; del Coz-Díaz, J.J.; Álvarez-Rabanal, F.P.; Gayarre, F.L.; Martínez-López, M.; Cruz-Olivares, J. Waste tire rubber particles modified by gamma radiation and their use as modifiers of concrete. Case Stud. Constr. Mater. 2020, 12, e00321. [Google Scholar] [CrossRef]
- Hargreaves, G.; Bowen, J.J. Combined Effects of Gamma and Ultraviolet Radiation Plus Heat on Fibrous Polyamides. Text. Res. J. 1973, 43, 568–576. [Google Scholar] [CrossRef]
- Zhou, Q.; Lyu, J.; Wang, G.; Robertson, M.; Qiang, Z.; Sun, B.; Ye, C.; Zhu, M. Mechanically Strong and Multifunctional Hybrid Hydrogels with Ultrahigh Electrical Conductivity. Adv. Funct. Mater. 2021, 31, 2104536. [Google Scholar] [CrossRef]
- Hsieh, Y.-L.; Yu, B.; Hartzell, M.M. Liquid Wetting, Transport, and Retention Properties of Fibrous Assemblies: Part II: Water Wetting and Retention of 100% and Blended Woven Fabrics. Text. Res. J. 1992, 62, 697–704. [Google Scholar] [CrossRef]
- Zhou, C.; Wu, Q. A novel polyacrylamide nanocomposite hydrogel reinforced with natural chitosan nanofibers. Colloids Surf. B Biointerfaces 2011, 84, 155–162. [Google Scholar] [CrossRef] [PubMed]
- Sasaki, S.; Omata, S.; Murakami, T.; Nagasawa, N.; Taguchi, M.; Suzuki, A. Effect of Gamma Ray Irradiation on Friction Property of Poly(vinyl alcohol) Cast-Drying on Freeze-Thawed Hybrid Gel. Gels 2018, 4, 30. [Google Scholar] [CrossRef] [PubMed]
- Hunt, J.A.; Chen, R.; Van Veen, T.; Bryan, N. Hydrogels for tissue engineering and regenerative medicine. J. Mater. Chem. B 2014, 2, 5319–5338. [Google Scholar] [CrossRef] [PubMed]
- Cacopardo, L.; Guazzelli, N.; Nossa, R.; Mattei, G.; Ahluwalia, A. Engineering hydrogel viscoelasticity. J. Mech. Behav. Biomed. Mater. 2019, 89, 162–167. [Google Scholar] [CrossRef] [PubMed]
- Hao, W.; Yao, X.; Ke, Y.; Ma, Y.; Li, F. Experimental characterization of contact angle and surface energy on aramid fibers. J. Adhes. Sci. Technol. 2013, 27, 1012–1022. [Google Scholar] [CrossRef]
- Pohan, G.; Mattiassi, S.; Yao, Y.; Zaw, A.M.; Anderson, D.E.; Cutiongco, M.F.; Hinds, M.T.; Yim, E.K. Effect of Ethylene Oxide Sterilization on Polyvinyl Alcohol Hydrogel Compared with Gamma Radiation. Tissue Eng. Part A 2020, 26, 1077–1090. [Google Scholar] [CrossRef] [PubMed]
- Shi, Y.; Xiong, D.; Zhang, J. Effect of irradiation dose on mechanical and biotribological properties of PVA/PVP hydrogels as articular cartilage. Tribol. Int. 2014, 78, 60–67. [Google Scholar] [CrossRef]
- El Salmawi, K.M. Gamma Radiation-Induced Crosslinked PVA/Chitosan Blends for Wound Dressing. J. Macromol. Sci. Part A 2007, 44, 541–545. [Google Scholar] [CrossRef]
- Qiao, K.; Zheng, Y.; Guo, S.; Tan, J.; Chen, X.; Li, J.; Xu, D.; Wang, J. Hydrophilic nanofiber of bacterial cellulose guided the changes in the micro-structure and mechanical properties of nf-BC/PVA composites hydrogels. Compos. Sci. Technol. 2015, 118, 47–54. [Google Scholar] [CrossRef]
- Shi, Y.; Xiong, D.; Li, J.; Wang, N. The water-locking and cross-linking effects of graphene oxide on the load-bearing capacity of poly(vinyl alcohol) hydrogel. RSC Adv. 2016, 6, 82467–82477. [Google Scholar] [CrossRef]
- Chen, Y.; Song, J.; Wang, S.; Liu, W. PVA-Based Hydrogels: Promising Candidates for Articular Cartilage Repair. Macromol. Biosci. 2021, 21, 2100147. [Google Scholar] [CrossRef]
- Gaharwar, A.K.; Schexnailder, P.J.; Schmidt, G. Nanocomposite Polymer Biomaterials for Tissue Repair of Bone and Cartilage. In Nanobiomaterials Handbook, 1st ed.; Sitharaman, B., Ed.; CRC Press: Boca Raton, FL, USA, 2011. [Google Scholar] [CrossRef]
- Little, C.J.; Bawolin, N.K.; Chen, X. Mechanical Properties of Natural Cartilage and Tissue-Engineered Constructs. Tissue Eng. Part B Rev. 2011, 17, 213–227. [Google Scholar] [CrossRef] [PubMed]
- Tamaddon, M.; Wang, L.; Liu, Z.; Liu, C. Osteochondral tissue repair in osteoarthritic joints: Clinical challenges and opportunities in tissue engineering. Bio-Design Manuf. 2018, 1, 101–114. [Google Scholar] [CrossRef]
- Athanasiou, K.A.; Darling, E.M.; DuRaine, G.D.; Hu, J.C.; Reddi, A.H. Articular Cartilage, 2nd ed.; Taylor & Francis: Boca Raton, FL, USA, 2013; Volume 53. [Google Scholar]
- Doulabi, A.H.; Mequanint, K.; Mohammadi, H. Blends and Nanocomposite Biomaterials for Articular Cartilage Tissue Engineering. Materials 2014, 7, 5327–5355. [Google Scholar] [CrossRef] [PubMed]
- Stojkov, G.; Niyazov, Z.; Picchioni, F.; Bose, R.K. Relationship between Structure and Rheology of Hydrogels for Various Applications. Gels 2021, 7, 255. [Google Scholar] [CrossRef]
- Dehghan-Niri, M.; Vasheghani-Farahani, E.; Eslaminejad, M.B.; Tavakol, M.; Bagheri, F. Physicomechanical, rheological and in vitro cytocompatibility properties of the electron beam irradiated blend hydrogels of tyramine conjugated gum tragacanth and poly (vinyl alcohol). Mater. Sci. Eng. C 2020, 114, 111073. [Google Scholar] [CrossRef]
- Moore, A.; Burris, D. Tribological rehydration of cartilage and its potential role in preserving joint health. Osteoarthr. Cartil. 2017, 25, 99–107. [Google Scholar] [CrossRef] [PubMed]
- Yang, X.; Zhu, Z.; Liu, Q.; Chen, X.; Ma, M. Effects of PVA, agar contents, and irradiation doses on properties of PVA/ws-chitosan/glycerol hydrogels made by γ-irradiation followed by freeze-thawing. Radiat. Phys. Chem. 2008, 77, 954–960. [Google Scholar] [CrossRef]
- Zainuddin; Cooper-White, J.J.; Hill, D.J.T. Viscoelasticity of radiation-formed PVA/PVP hydrogel. J. Biomater. Sci. Polym. Ed. 2002, 13, 1007–1020. [Google Scholar] [CrossRef]
- Mostakhdemin, M.; Nand, A.; Ramezani, M. Articular and Artificial Cartilage, Characteristics, Properties and Testing Approaches—A Review. Polymers 2021, 13, 2000. [Google Scholar] [CrossRef]
- Boettcher, K.; Grumbein, S.; Winkler, U.; Nachtsheim, J.; Lieleg, O. Adapting a commercial shear rheometer for applications in cartilage research. Rev. Sci. Instrum. 2014, 85, 093903. [Google Scholar] [CrossRef]
- Link, J.M.; Salinas, E.Y.; Hu, J.C.; Athanasiou, K.A. The tribology of cartilage: Mechanisms, experimental techniques, and relevance to translational tissue engineering. Clin. Biomech. 2020, 79, 104880. [Google Scholar] [CrossRef] [PubMed]
- Feng, Y.; Dai, S.-C.; Lim, K.; Ramaswamy, Y.; Jabbarzadeh, A. Tribological and Rheological Properties of Poly(vinyl alcohol)-Gellan Gum Composite Hydrogels. Polymers 2022, 14, 3830. [Google Scholar] [CrossRef] [PubMed]
- Gong, J.P. Friction and lubrication of hydrogels—Its richness and complexity. Soft Matter 2006, 2, 544–552. [Google Scholar] [CrossRef] [PubMed]
- Gong, J.; Iwasaki, Y.; Osada, Y.; Kurihara, K.; Hamai, Y. Friction of Gels. 3. Friction on Solid Surfaces. J. Phys. Chem. B 1999, 103, 6001–6006. [Google Scholar] [CrossRef]
- Chen, K.; Zhang, D.; Cui, X.; Wang, Q. Research on swing friction lubrication mechanisms and the fluid load support characteristics of PVA–HA composite hydrogel. Tribol. Int. 2015, 90, 412–419. [Google Scholar] [CrossRef]
- McCutchen, C. The frictional properties of animal joints. Wear 1962, 5, 1–17. [Google Scholar] [CrossRef]
- Brand, R.A. Joint contact stress: A reasonable surrogate for biological processes? Iowa Orthop. J. 2005, 25, 82–94. [Google Scholar]
- Noguchi, T.; Yamamuro, T.; Oka, M.; Kumar, P.; Kotoura, Y.; Hyonyt, S.; Ikadat, Y. Poly(vinyl alcohol) hydrogel as an artificial articular cartilage: Evaluation of biocompatibility. J. Appl. Biomater. 1991, 2, 101–107. [Google Scholar] [CrossRef]
- Ali, M.; Al-Hajjar, M.; Partridge, S.; Williams, S.; Fisher, J.; Jennings, L.M. Influence of hip joint simulator design and mechanics on the wear and creep of metal-on-polyethylene bearings. Proc. Inst. Mech. Eng. Part H J. Eng. Med. 2016, 230, 389–397. [Google Scholar] [CrossRef]
- Inês, M.; De Sá, M. Tribomechanical Behaviour of Chemically Crosslinked PVA Hydrogels Bioengineering and Nanosystems. Master’s Thesis, Instituto Superior Técnico, University of Lisbon, Lisbon, Portugal, 2019. [Google Scholar]
- Henke, P.; Ruehrmund, L.; Bader, R.; Kebbach, M. Exploration of the Advanced VIVOTM Joint Simulator: An In-Depth Analysis of Opportunities and Limitations Demonstrated by the Artificial Knee Joint. Bioengineering 2024, 11, 178. [Google Scholar] [CrossRef] [PubMed]
- Li, J.; Wang, C.; Han, X.; Liu, S.; Gao, X.; Guo, C.; Wu, X. Aramid Nanofibers-Reinforced Rhein Fibrous Hydrogels as Antibacterial and Anti-Inflammatory Burn Wound Dressings. ACS Appl. Mater. Interfaces 2022, 14, 45167–45177. [Google Scholar] [CrossRef] [PubMed]
- ISO 10993-5:2009(E); Biological Evaluation of Medical Devices—Part 5: Tests for In Vitro Cytotoxicity. ISO: Geneva, Switzerland, 2009.
- Jimenez-Cruz, D.; Dubey, M.; Board, T.; Williams, S. An in vitro methodology for experimental simulation on the natural hip joint. PLoS ONE 2022, 17, e0272264. [Google Scholar] [CrossRef] [PubMed]
- ISO 14242-1:2014; Implants for Surgery—Wear of Total Hip-Joint Prostheses—Part 1: Loading and Displacement Parameters for Wear-Testing Machines and Corresponding Environmental Conditions for Test. ISO: Geneva, Switzerland, 2014.
- ISO 10993-5:2012(E); Biological Evaluation of Medical Devices—Part 12: Sample Preparation and Reference Materials. ISO: Geneva, Switzerland, 2012.

Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Santos, F.; Marto-Costa, C.; Branco, A.C.; Oliveira, A.S.; Galhano dos Santos, R.; Salema-Oom, M.; Diaz, R.L.; Williams, S.; Colaço, R.; Figueiredo-Pina, C.; et al. Tribomechanical Properties of PVA/Nomex® Composite Hydrogels for Articular Cartilage Repair. Gels 2024, 10, 514. https://doi.org/10.3390/gels10080514
Santos F, Marto-Costa C, Branco AC, Oliveira AS, Galhano dos Santos R, Salema-Oom M, Diaz RL, Williams S, Colaço R, Figueiredo-Pina C, et al. Tribomechanical Properties of PVA/Nomex® Composite Hydrogels for Articular Cartilage Repair. Gels. 2024; 10(8):514. https://doi.org/10.3390/gels10080514
Chicago/Turabian StyleSantos, Francisco, Carolina Marto-Costa, Ana Catarina Branco, Andreia Sofia Oliveira, Rui Galhano dos Santos, Madalena Salema-Oom, Roberto Leonardo Diaz, Sophie Williams, Rogério Colaço, Célio Figueiredo-Pina, and et al. 2024. "Tribomechanical Properties of PVA/Nomex® Composite Hydrogels for Articular Cartilage Repair" Gels 10, no. 8: 514. https://doi.org/10.3390/gels10080514
APA StyleSantos, F., Marto-Costa, C., Branco, A. C., Oliveira, A. S., Galhano dos Santos, R., Salema-Oom, M., Diaz, R. L., Williams, S., Colaço, R., Figueiredo-Pina, C., & Serro, A. P. (2024). Tribomechanical Properties of PVA/Nomex® Composite Hydrogels for Articular Cartilage Repair. Gels, 10(8), 514. https://doi.org/10.3390/gels10080514










