Abstract
(1) Background: BioHPP® (Bredent, UK) is a partially crystalline poly ether ether ketone (PEEK) that is strengthened using ceramic. PEEK and its various formulations represent a very interesting alternative, and has been in-depth with its literature in recent years; (2) Methods: A PubMed and Scopus search for the term “BioHPP” yielded 73 results and 42 articles which were included in this short review. Considering the scarce literature on the subject, each article was considered in this review; (3) Results: the articles analyzed are very recent, all published in the last 5 years. Their clinical evaluation of BioHPP® highlights many positive aspects, and few articles have highlighted critical issues in its multiple clinical applications; (4) Conclusions: this material is not only extremely interesting for the future, but possesses characteristics suitable for clinical application today, for endocrowns, small adhesive bridges, temporary prostheses and for immediate loads on implant restorations. The excellent aesthetics and the possibility of simple reprocessing of the restorations made with this material invite its clinical application.
1. Introduction
Innovations in the field of implant prosthetics on materials that can be used both in temporary rehabilitation, such as in immediate loading and definitive restorations, have merged with modern digital techniques, making the use of resins and non-metallic materials increasingly interesting. Although metal prosthetic restorations still represent an extremely recommended solution today for the marginal precision, duration over time, excellent bond of the current alloys with the ceramic coatings, and for the possibility of laser sintering, milling the structure, or to use a casting technique, PEEK and its various formulations represent a very interesting alternative, thoroughly investigated in recent literature.
The purpose of this review is to understand the level of awareness of the mechanical characteristics of BioHPP and its ideal clinical application.
Metals prosthetic rehabilitation have a very different modulus of elasticity from those of bone; these rigid materials discharge important occlusal forces on the prosthetic system, without any cushioning, and therefore, for the application in immediate loading techniques, the need arises to use different materials, equipped with the ability to reduce the load on implants [1]. Since the modulus of elasticity for PEEK at around 12 GPa is similar to that of cortical bone at around 15 GPa, it is particularly suitable for dental implants.
Since the matherial is extremely inert and develops a dense structure as a result of the processing during the compression-molding process, there is good biocompatibility, as has already been proven during the manufacture of plastic abutments [1,2].
Polyetheretherketone (PEEK) has been used in medicine for years, particularly in Orthopedics for more than 40 years [2]. This product, and its novel high-performance evolutions, attracted the attention of researchers for the notable mechanical properties. Over the years, this material has evolved, leading to its reinforcement by inserting fibers or ceramics inside (less than 0.5 µm in diameter) to improve its mechanical capabilities, resistance to stress, and aesthetics [3].
BioHPP® (Bredent, UK) is a partially crystalline poly ether ether ketone (PEEK) that is strengthened using ceramic. The ceramic fillers improve the strength, abrasion properties, and allow it to be veneered. As a result, BioHPP® is the only material to achieve the perfect balance between elasticity and rigidity, with important aesthetic characteristics on its side, thanks to the possibility of being veneered [4].
A BioHPP® prosthesis considerably reduces the maximum values of masticatory forces, both vertically and lateral, compared to titanium, zirconium, or ceramic distributed on the prosthetic structure and in the bone [4,5]. One of the functions of Sharpey fibers is to cushion the distribution of occlusal forces at the bone level. This capacity is often lower on devitalized teeth and completely missing in the case of bone ankylosis/osseointegration at the implant level. From a mechanical point of view, this has unfavorable effects on osseointegration, and from a physiological point of view there are effects on the antagonistic teeth as wear. The interposition of a material such as BioHPP®, often used as an abutment between the bone/implant interface and the prosthesis, guarantees greater safety in immediate loading techniques, thanks to its mechanical characteristics [1,5].
The use of this material is indicated in fixed prostheses for single crowns, bridges with up to two pontics, bonded bridges (Maryland bridges), and in removable prostheses for superstructures with or without friction elements, secondary parts in the presence of bars, individual abutments, Toronto Bridge, or, directly, crowns [6]. Particularly with fixed prostheses in a jaw already restored with metal restorations, the low BioHPP® modulus of elasticity can therefore help achieve normal chewing sensation and reduce the amount of force transmitted with implant-based restorations in the manner of “progressive bone loading”, reducing also the risk of antagonist chipping due to excessive occlusal load during occlusion [4,5]. The possibility that this material has to adapt perfectly to the partially or completely digital workflow and radiation-free diagnostic examination allows for obtaining high levels of aesthetics, and for being able to propose a precise treatment plan for the patient [7,8,9,10,11]. The main solution for its clinical application to date is still represented by cementation, unless intermediate metal components are used that allow it to be screwed, avoiding the various problems of cementation, which, however, can follow traditional techniques without particular differences using adhesive cements, composites, zinc oxide without eugenol, and zinc oxide with eugenol, avoiding only glass ionomer and zinc phosphates cements [12,13].
What makes this material extremely interesting is that it achieves a perfect balance between elasticity (about 4.200–4.800 MPa) and stiffness (flexural strength 180–185 MPa), weight and breaking strength (from 700 N to 1600 N), physiologic integration, and resistance to plaque (bacterial adhesion comparable to that of zirconium oxide or veneering composites, with perfectly polished surface, polishing up to <0.02 µm) [4,6].
Considering the characteristics of this material, it adapts perfectly to the prosthesis on implants, but less so to the one on the tooth. It must be considered that the dental implants alone represent the answer to the medical needs of more than 800,000 individuals in the United States (US), and more than 1.8 million in the European Union (EU). Often, the placement of a limited number of strategic implants makes it possible to propose low-cost implant therapies, which are suitable for a large part of the population, and these materials, resistant, economical, and suitable for immediate loading represent the future of this kind of rehabilitation [5,6].
Several studies have been proposed on the mechanical properties of this interesting material in vitro (less in vivo), but there are still no reviews of these articles that can offer an overview of this product and its possible applications.
2. Materials and Methods
A PubMed search for the term “BioHPP” yielded 29 results. All the articles were selected, evaluated by their titles and subsequently by their abstracts, and were considered valid for the purposes of the comparative and absolute evaluation of the BioHPP compared to other prosthetic materials; only one article not written in English was excluded. 28 articles were included in this review. Considering the scarcity of literature on the subject, each article was considered in this review.
3. Results
The articles taken into consideration indicated that this examination is widely usable and in great progress. The complete search flow is schematized in Figure 1.
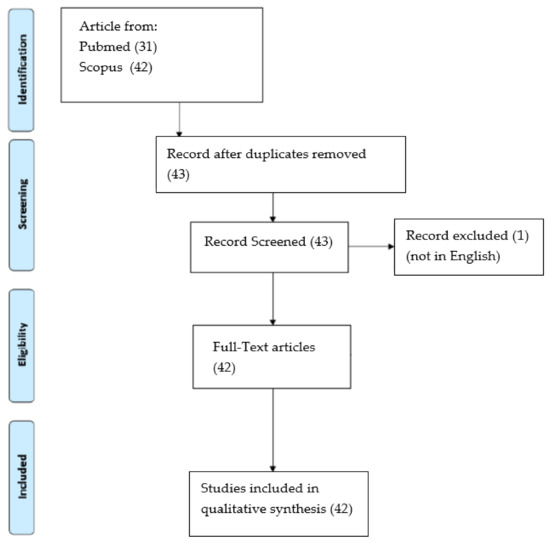
Figure 1.
PRISMA Search flow results [14].
All the articles considered for the study are indicated in Table 1. The number of articles concerning this technique, and their topicality, all very recent, represent a great invitation to continue the research about BioHPP. Only two articles, in their conclusions, underline the negative aspects of this material or the lack of clinical evidence, not considering it to be on par with those conventionally used: Zoidis et al. affirmed “Due to the lack of solid clinical evidence, BioHPP should not be considered as a substitute framework material for a well-designed Cr-Co RDP” and Andrikopoulou et al. “Due to lack of clinical evidence, BioHPP cannot substitute the conventional metal ceramic or all ceramic materials; however, it can be used as an alternative treatment option” [3,15].

Table 1.
Included studies characteristics.
4. Discussion
Peri-implant health is extremely delicate, and strongly correlated with the type of prosthesis, the hygiene of the product and the control of the load distributed at the bone level [10,16]. It is now evident in the literature that the levels of inflammation of the peri implant sulcus, also as a function of the different biological width and therefore of the different implant type, must be maintained and controlled, and to favor this it is necessary that the implant supported prosthesis guarantees excellent marginal closures, cleanable profiles, and does not favor the accumulation of plaque [52,53,54]. The shock absorbance as a feature of this implant material is extremely relevant, and allows for performing an implant rehabilitation, even complete, with interesting mechanical and biological characteristics: It is known that overload cannot directly cause peri-implantitis, but participates as a factor, together with the levels of inflammation that it maintains higher as a stimulus for bone resorption, in the development of implant pathology [20].
CAD/CAM BioHPP® frameworks exhibited not only shock absorbing, but also good marginal fit and fracture resistance and good retention force [4,21].
BioHPP® demonstrates a high biocompatibility, even superior to Zirconia in certain characteristics, and can be superimposed on the materials commonly used for implant restorations [6,22].
Use of different conditioning protocols had a significant effect on the final bond strength of composite resin cement to PEEK surface, but always at an excellent level, guaranteeing a perfect combination between the two materials [12].
Regarding the mechanical characteristics and physical properties of BioHPP®, promising fracture strengths and fracture types were found for the ceramic reinforced PEEK abutments with titanium base [23]. Ardakani et al. researched differently than other authors, but about a different and more complex application of BioHPP®; the state “BioHPP is not a suitable substitute for metal reinforce to enhance the Fracture Strength of PMMA denture base material” [21]. Also, wear behavior of the BioHPP® is extremely suitable for clinical use in dentistry [25]. The main PEEK characteristics are due to its low elastic modulus, similar to that of bone, its low hardness, which will not cause an abrasion of the opposing tooth, which does occur in the case of ceramic [26]. Rasheed et al. state that the shear bond strength of PEEK is similar to that of zirconia, showing the advantage that with the right surface treatments it is also the best adhesive solution [12,27]. Furthermore, the PEEK crowns showed minimal abrasion, better stress modulation through plastic deformation, and good color stability, which makes it a promising alternative to zirconia for fabrication of the crown [28,29,30,31]. PEEK has a low specific weight that permits the fabrication of lighter prostheses, providing high patient satisfaction and comfort during function [32]. For this reason, BioHPP could be used as a promising alternative denture base material with good adaptation, retention, and mechanical properties [33].
The study of Lalama et al. showed that heat-pressed PEEK post and core restorations resulted in higher accuracy when compared to the CAD/CAM method [26]. BioHPP PEEK can be fabricated via CAD/CAM technology by milling PEEK blanks. It can also be pressed by using granular or pellet-shaped PEEK [50,51,52,53,54].
Furthermore, for the application of this material in the production of endocrowns, the evidence is numerous and in agreement. Poly infiltrated ceramics should be considered as a proper material to be used as an endocrown material; furthermore, they allow for easy reprocessing in case of failure [35]. Lithium disilicate showed a better marginal and internal fit compared to PEEK. However, the reinforced PEEK marginal fit is also within the clinical acceptable range [36]. The results are also clinically acceptable in comparison with Zirconia inlay restorations [37]. BioHPP provides very good clinical results due to the structure, but also the polymerization method, namely heat pressing. It has no abrasive effect on the remaining teeth, has white color suitable for fully anatomical use, and insures no ion exchange in the mouth, no discoloration, excellent stability, and optimal polishable properties [45]. However, lithium disilicate remains the gold standard of this type of rehabilitation [38]. Therefore, also for this application, BioHPP® has proven to have excellent characteristics and clinical reliability.
Regarding the retention and wear characteristics of this material, the results are excellent, guaranteeing long-term good results both in terms of resistance and wear [38,39].
PEEK may be a suitable material for removable prosthesis and a telescopic crown technique when used on zirconia crowns [39]. For its future applications, it turns out to be an excellent material also to replace the Cr-Co bars, and considering its positive bond with the composite materials previously highlighted, it turns out to be of a high level [41,42,43].
Regarding Zoidis et al. and Andrikopoulou et al., who expressed less positive comments than other authors, it is also necessary to underline that these are two of the first works published on this topic (5 years ago), and are among the oldest included in the study. This latter fact may be an indication of how the consideration of these materials has changed in just 5 years [3,15].
Furthermore, excellent stability and optimal polishable properties allow the material to have a low affinity for plaque, which hardly aggregates as a biofilm on its mirror-polished surface [45,52,53,54,55].
The limitation of this review is that the presence of a few articles, most of which were published over the last two years, and the little clinical follow-up, did not allow for the execution of a systematic review with meta-analysis.
By improving the aesthetics of this material and its durability with unchanged characteristics greater than that of long-term provisional materials, it could in the near future be used as prosthetic materials for definitive restorations.
The authors, in light of the analysis of the articles included in this review, consider this material to be not only extremely interesting for the future, but with characteristics suitable for clinical application already today, in particular for endocrowns, small adhesive bridges, temporary prostheses, and for immediate loads on implant restorations.
5. Conclusions
BioHPP® is an extremely interesting material both for its mechanical characteristics, for its extreme biocompatibility, and above all for its clinical adaptability in dentistry. The excellent aesthetics, as well as the possibility of simple reprocessing of the restorations made with this material, invite its clinical application. The use of BioHPP® is indicated in fixed prostheses for:
- single crowns
- endocrowns
- bridges with up to two pontics
- bonded bridges (Maryland bridges)
And in removable prostheses for:
- superstructures with or without friction elements
- secondary parts in the presence of bars
- individual abutments
- Toronto Bridge
What makes this material extremely interesting is that it achieves a perfect balance between elasticity, stiffness, weight and breaking strength, physiologic integration, and resistance to plaque with a perfectly polished surface.
In light of the evidence that emerged from this article, the authors suggest the use of this material for temporary prostheses production, especially with immediate loading protocols. The main indication remains the application in implant prosthesis, but increasing attention must be paid to conservative restorations on teeth.
Author Contributions
Conceptualization, R.R. and A.Z.; methodology, M.G.; validation, A.D.B., M.G. and L.T.; formal analysis, A.Z.; investigation, R.R.; resources, R.R.; data curation, A.Z.; writing—original draft preparation, R.R. and D.D.N.; writing—review and editing, L.T.; visualization, A.D.B.; supervision, L.T. All authors have read and agreed to the published version of the manuscript.
Funding
This research received no external funding.
Conflicts of Interest
The authors declare no conflict of interest.
References
- De Bruyn, H.; Raes, S.; Östman, P.-O.; Cosyn, J. Immediate loading in partially and completely edentulous jaws: A review of the literature with clinical guidelines. Periodontology 2000 2014, 66, 153–187. [Google Scholar] [CrossRef] [PubMed]
- Panayotov, I.V.; Orti, V.; Cuisinier, F.; Yachouh, J. Polyetheretherketone (PEEK) for medical applications. J. Mater. Sci. Mater. Med. 2016, 27, 118. [Google Scholar] [CrossRef]
- Zoidis, P.; Papathanasiou, I.; Polyzois, G. The Use of a Modified Poly-Ether-Ether-Ketone (PEEK) as an Alternative Framework Material for Removable Dental Prostheses. A Clinical Report. J. Prosthodont. 2015, 25, 580–584. [Google Scholar] [CrossRef]
- Jin, H.-Y.; Teng, M.-H.; Wang, Z.-J.; Li, X.; Liang, J.-Y.; Wang, W.-X.; Jiang, S.; Zhao, B.-D. Comparative evaluation of BioHPP and titanium as a framework veneered with composite resin for implant-supported fixed dental prostheses. J. Prosthet. Dent. 2019, 122, 383–388. [Google Scholar] [CrossRef] [PubMed]
- Azcarate-Velázquez, F.; Castillo-Oyagüe, R.; Oliveros-López, L.G.; Torres-Lagares, D.; Martínez-González, Á.J.; Pérez-Velasco, A.; Lynch, C.D.; Gutiérrez-Pérez, J.L.; Serrera-Figallo, M.Á. Influence of bone quality on the mechanical interaction between implant and bone: A finite element analysis. J. Dent. 2019, 88, 103161. [Google Scholar] [CrossRef] [PubMed]
- Jovanović, M.; Živić, M.; Milosavljević, M. A Potential Application of Materials Based on a Polymer and CAD/CAM Composite Resins in Prosthetic Dentistry. J. Prosthodont. Res. 2021, 65, 137–147. [Google Scholar] [CrossRef]
- Alhammadi, M.; Al-Mashraqi, A.; Alnami, R.; Ashqar, N.; Alamir, O.; Halboub, E.; Reda, R.; Testarelli, L.; Patil, S. Accuracy and Reproducibility of Facial Measurements of Digital Photographs and Wrapped Cone Beam Computed Tomography (CBCT) Photographs. Diagnostics 2021, 11, 757. [Google Scholar] [CrossRef]
- Perrotti, G.; Baccaglione, G.; Clauser, T.; Scaini, R.; Grassi, R.; Testarelli, L.; Reda, R.; Testori, T.; Del Fabbro, M. Total Face Approach (TFA) 3D Cephalometry and Superimposition in Orthognathic Surgery: Evaluation of the Vertical Dimensions in a Consecutive Series. Methods Protoc. 2021, 4, 36. [Google Scholar] [CrossRef]
- Reda, R.; Zanza, A.; Mazzoni, A.; Cicconetti, A.; Testarelli, L.; Di Nardo, D. An Update of the Possible Applications of Magnetic Resonance Imaging (MRI) in Dentistry: A Literature Review. J. Imaging 2021, 7, 75. [Google Scholar] [CrossRef]
- Patil, S.; Alkahtani, A.; Bhandi, S.; Mashyakhy, M.; Alvarez, M.; Alroomy, R.; Hendi, A.; Varadarajan, S.; Reda, R.; Raj, A.; et al. Ultrasound Imaging versus Radiographs in Differentiating Periapical Lesions: A Systematic Review. Diagnostics 2021, 11, 1208. [Google Scholar] [CrossRef]
- Reda, R.; Zanza, A.; Cicconetti, A.; Bhandi, S.; Miccoli, G.; Gambarini, G.; Di Nardo, D. Ultrasound Imaging in Dentistry: A Literature Overview. J. Imaging 2021, 7, 238. [Google Scholar] [CrossRef] [PubMed]
- Spyropoulos, D.; Kamposiora, P.; Zoidis, P. The Effect of Surface Pretreatment and Water Storage on the Bonding Strength of a Resin Composite Cement to Modified PEEK. Eur. J. Prosthodont. Restor. Dent. 2020, 28, 121–127. [Google Scholar] [PubMed]
- Reda, R.; Zanza, A.; Cicconetti, A.; Bhandi, S.; Guarnieri, R.; Testarelli, L.; Di Nardo, D. A Systematic Review of Cementation Techniques to Minimize Cement Excess in Cement-Retained Implant Restorations. Methods Protoc. 2022, 5, 9. [Google Scholar] [CrossRef] [PubMed]
- Liberati, A.; Altman, D.G.; Tetzlaff, J.; Mulrow, C.; Gøtzsche, P.C.; Ioannidis, J.P.A.; Clarke, M.; Devereaux, P.J.; Kleijnen, J.; Moher, D. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate healthcare interventions: Explanation and elaboration. BMJ 2009, 339, b2700. [Google Scholar] [CrossRef] [Green Version]
- Andrikopoulou, E.; Zoidis, P.; Artopoulou, I.-I.; Doukoudakis, A. Modified PEEK Resin Bonded Fixed Dental Prosthesis for a Young Cleft Lip and Palate Patient. J. Esthet. Restor. Dent. 2016, 28, 201–207. [Google Scholar] [CrossRef]
- Micovic, D.; Mayinger, F.; Bauer, S.; Roos, M.; Eichberger, M.; Stawarczyk, B. Is the high-performance thermoplastic polyetheretherketone indicated as a clasp material for removable dental prostheses? Clin. Oral Investig. 2020, 25, 2859–2866. [Google Scholar] [CrossRef]
- Guo, L.; Smeets, R.; Kluwe, L.; Hartjen, P.; Barbeck, M.; Cacaci, C.; Gosau, M.; Henningsen, A. Cytocompatibility of Titanium, Zirconia and Modified PEEK after Surface Treatment Using UV Light or Non-Thermal Plasma. Int. J. Mol. Sci. 2019, 20, 5596. [Google Scholar] [CrossRef] [Green Version]
- Atsü, S.; Aksan, M.; Bulut, A. Fracture Resistance of Titanium, Zirconia, and Ceramic-Reinforced Polyetheretherketone Implant Abutments Supporting CAD/CAM Monolithic Lithium Disilicate Ceramic Crowns After Aging. Int. J. Oral Maxillofac. Implant. 2019, 34, 622–630. [Google Scholar] [CrossRef]
- Elashmawy, Y.; Elshahawy, W.; Seddik, M.; Aboushelib, M. Influence of fatigue loading on fracture resistance of endodontically treated teeth restored with endocrowns. J. Prosthodont. Res. 2021, 65, 78–85. [Google Scholar] [CrossRef]
- Ramadan, R.; Elsherbeeny, Y.; Ghali, R.; Thabet, Y.; Kandil, B. Retention of a telescopic overdenture on customized abutments after the simulation of 1 year in function. Dent. Med. Probl. 2021, 58, 201–206. [Google Scholar] [CrossRef]
- Ardakani, Z.H.; Giti, R.; Dabiri, S.; Hosseini, A.H.; Moayedi, M. Flexural strength of polymethyl methacrylate reinforced with high-performance polymer and metal mesh. Dent. Res. J. 2021, 18, 30. [Google Scholar]
- Kazi, A.I.; Godil, A.Z.; Wadwan, S.A.; Gandhi, K.Y.; Dugal, R.J.S. Comparative evaluation of marginal and internal fit of endocrowns using lithium disilicate and polyetheretherketone computer-aided design—Computer-aided manufacturing (CAD-CAM) materials: An in vitro study. J. Conserv. Dent. 2021, 24, 198. [Google Scholar] [CrossRef] [PubMed]
- Turksayar, A.A.D.; Hisarbeyli, D.; Kelten, S.; Bulucu, N.B. Wear behavior of current computer-aided design and computer-aided manufacturing composites and reinforced high performance polymers: An in vitro study. J. Esthet. Restor. Dent. 2021. [Google Scholar] [CrossRef]
- Blanch-Martínez, N.; Arias-Herrera, S.; Martínez-González, A. Behavior of polyether-ether-ketone (PEEK) in prostheses on dental implants. A review. J. Clin. Exp. Dent. 2021, 13, e520–e526. [Google Scholar] [CrossRef]
- Reyal, S.S.; Rajamani, V.K.; Gowda, E.M.; Shashidhar, M.P. Comparative prospective clinical evaluation of computer aided design/ computer aided manufacturing milled BioHPP PEEK inlays and Zirconia inlays. J. Indian Prosthodont. Soc. 2021, 21, 240. [Google Scholar] [CrossRef] [PubMed]
- Lalama, M.; Rocha, M.G.; Neill, E.O.; Zoidis, P. Polyetheretherketone (PEEK) Post and Core Restorations: A 3D Accuracy Analysis between Heat-Pressed and CAD-CAM Fabrication Methods. J. Prosthodont. 2021, 1–6. [Google Scholar] [CrossRef]
- Rasheed, M.N.; Sarfaraz, H.; Shetty, S.K.; Prabhu, U.M.; Fernandes, K.; Mohandas, S. Comparison of the bond strength of composite resin to zirconia and composite resin to polyether ether ketone: An in vitro study. J. Pharm. Bioallied Sci. 2020, 12, S504–S509. [Google Scholar] [CrossRef]
- Mayinger, F.; Micovic, D.; Schleich, A.; Roos, M.; Eichberger, M.; Stawarczyk, B. Retention force of polyetheretherketone and cobalt-chrome-molybdenum removable dental prosthesis clasps after artificial aging. Clin. Oral Investig. 2020, 25, 3141–3149. [Google Scholar] [CrossRef]
- Merk, S.; Wagner, C.; Stock, V.; Eichberger, M.; Schmidlin, P.R.; Roos, M.; Stawarczyk, B. Suitability of Secondary PEEK Telescopic Crowns on Zirconia Primary Crowns: The Influence of Fabrication Method and Taper. Materials 2016, 9, 908. [Google Scholar] [CrossRef]
- Abhay, S.S.; Ganapathy, D.; Veeraiyan, D.N.; Ariga, P.; Heboyan, A.; Amornvit, P.; Rokaya, D.; Srimaneepong, V. Wear Resistance, Color Stability and Displacement Resistance of Milled PEEK Crowns Compared to Zirconia Crowns under Stimulated Chewing and High-Performance Aging. Polymers 2021, 13, 3761. [Google Scholar] [CrossRef]
- Porojan, L.; Toma, F.R.; Vasiliu, R.D.; Topală, F.-I.; Porojan, S.D.; Matichescu, A. Optical Properties and Color Stability of Dental PEEK Related to Artificial Ageing and Staining. Polymers 2021, 13, 4102. [Google Scholar] [CrossRef] [PubMed]
- Prechtel, A.; Reymus, M.; Edelhoff, D.; Hickel, R.; Stawarczyk, B. Comparison of various 3D printed and milled PAEK materials: Effect of printing direction and artificial aging on Martens parameters. Dent. Mater. 2019, 36, 197–209. [Google Scholar] [CrossRef] [PubMed]
- Preis, V.; Hahnel, S.; Behr, M.; Bein, L.; Rosentritt, M. In-Vitro fatigue and fracture testing of CAD/CAM-materials in implant-supported molar crowns. Dent. Mater. 2017, 33, 427–433. [Google Scholar] [CrossRef] [PubMed]
- Abdelrehim, A.; Abdelhakim, A.; El Dakkak, S. Influence of different materials on retention behavior of CAD-CAM fabricated bar attachments. J. Prosthet. Dent. 2021. [Google Scholar] [CrossRef]
- Stock, V.; Wagner, C.; Merk, S.; Roos, M.; Schmidlin, P.R.; Eichberger, M.; Stawarczyk, B. Retention force of differently fabricated telescopic PEEK crowns with different tapers. Dent. Mater. J. 2016, 35, 594–600. [Google Scholar] [CrossRef] [Green Version]
- Zoidis, P.; Papathanasiou, I. Modified PEEK resin-bonded fixed dental prosthesis as an interim restoration after implant placement. J. Prosthet. Dent. 2016, 116, 637–641. [Google Scholar] [CrossRef]
- Emera, R.M.K.; Abdallah, R.M. Denture base adaptation, retention, and mechanical properties of BioHPP versus nano-alumina-modified polyamide resins. J. Dent. Res. Dent. Clin. Dent. Prospect. 2021, 15, 239–246. [Google Scholar] [CrossRef]
- Omaish, H.H.M.; Abdelhamid, A.M.; Neena, A.F. Comparison of the strain developed around implants with angled abutments with two reinforced polymeric CAD-CAM superstructure materials: An in vitro comparative study. J. Prosthet. Dent. 2022. [Google Scholar] [CrossRef]
- Popa, D.; Constantiniuc, M.; Earar, K.; Mercut, V.; Scrieciu, M.; Buduru, S.; Luca, E.; Negucioiu, M. Review of Different Materials that can be CAD/CAM Processed Description, chemical composition, indications in dentistry areas. Rev. Chim. 2019, 70, 4029–4034. [Google Scholar] [CrossRef]
- Baciu, S.; Berece, C.; Florea, A.; Tonea, A.V.; Lucaciu, O.; Burde, A.V.; Rusnac, M.; Manole, M.; Saceleanu, A.; Mohan, A.; et al. Comparison of Two Evaluating Methods for Establishing the Marginal Fit on Four Heat—Pressed Resin Inlays. Rev. Chim. 2018, 69, 890–893. [Google Scholar] [CrossRef]
- Biris, C.; Bechir, E.S.; Bechir, A.; Mola, F.C.; Badiu, A.V.; Oltean, C.; Andreescu, C.; Gioga, C. Evaluations of Two Reinforced Polymers Used as Metal-FreeSubstructures in Fixed Dental Restoration. Mater. Plast. 2018, 55, 33–37. [Google Scholar] [CrossRef]
- Baciu, S.; Berece, C.; Florea, A.; Burde, A.V.; Munteanu, A.; Cigu, T.A.; Hosszu, T.; Szuhanek, C.; Manole, M.; Sinescu, C. Three-dimensional Marginal Evaluation of Two Pressed Materials Using Micro-CT Technology. Rev. Chim. 2017, 68, 615–618. [Google Scholar] [CrossRef]
- Pacurar, M.; Bechir, E.S.; Suciu, M.; Bechir, A.; Biris, C.I.; Curt-Mola, F.; Cherana, G.; Dascalu, T.I.; Ormenisan, A. The Benefits of Polyether-Ether-Ketone Polymers in Partial Edentulous Patients. Rev. Chim. 2016, 53, 657–660. [Google Scholar]
- Bechir, S.E.; Bechir, A.; Gioga, C.; Manu, R.; Burcea, A.; Dscalu, I.T. The Advantages of BioHPP Polymer as Superstructure Material in Oral Implantology. Rev. Chim. 2016, 53, 394–398. [Google Scholar]
- Di Iorio, E.; Berardini, M. A new material for fixed implant-supported rehabilitations. Dent. Cadmos 2016, 84, 320–325. [Google Scholar] [CrossRef]
- Amer, M.M.; Elsheikh, M.M.; Haleem, M.M.; Ghoraba, S.F.; Salem, A.A. Short-term comparative evaluation of BioHPP and cast cobalt–chromium as framework for implant supported prostheses: A split mouth clinical randomized trial. J. Int. Oral Health 2021, 13, 564–570. [Google Scholar]
- Odeh, E.; Alansary, H.; Naguib, A.; Taymour, M. Evaluation of biocompatibility of veneered Bio HPP and veneered lithium disilicate crowns in anterior zone (Randomized controlled clinical trial). Braz. Dent. Sci. 2021, 24. [Google Scholar] [CrossRef]
- Kwan, J.; Kwan, N. Clinical Application of PEEK as a Provisional Fixed Dental Prosthesis Retained by Reciprocated Guide Surfaces of Healing Abutments During Dental Implant Treatment. Int. J. Oral Maxillofac. Implant. 2021, 36, 581–586. [Google Scholar] [CrossRef]
- Guarnieri, R.; Zanza, A.; D’Angelo, M.; Di Nardo, D.; Del Giudice, A.; Mazzoni, A.; Reda, R.; Testarelli, L. Correlation between Peri-Implant Marginal Bone Loss Progression and Peri-Implant Sulcular Fluid Levels of Metalloproteinase-8. J. Pers. Med. 2022, 12, 58. [Google Scholar] [CrossRef]
- Sadek, S.A. Comparative Study Clarifying the Usage of PEEK as Suitable Material to Be Used as Partial Denture Attachment and Framework. Open Access Maced. J. Med. Sci. 2019, 7, 1193–1197. [Google Scholar] [CrossRef] [Green Version]
- Bolat, M.; Bosinceanu, D.G.; Sandu, I.G.; Bosinceanu, D.N.; Surlari, Z.; Balcos, C.; Solomon, O.; Vitalariu, A. Comparative Study on the Degree of Bacterial Biofilm Formation of Dental Bridges Made from Three Types of Materials. Mater. Plast. 2019, 56, 144–147. [Google Scholar] [CrossRef]
- Guarnieri, R.; Miccoli, G.; Reda, R.; Mazzoni, A.; Di Nardo, D.; Testarelli, L. Laser microgrooved vs. machined healing abutment disconnection/reconnection: A comparative clinical, radiographical and biochemical study with split-mouth design. Int. J. Implant Dent. 2021, 7, 19. [Google Scholar] [CrossRef]
- Guarnieri, R.; Reda, R.; Di Nardo, D.; Miccoli, G.; Zanza, A.; Testarelli, L. In Vitro Direct and Indirect Cytotoxicity Comparative Analysis of One Pre-Hydrated versus One Dried Acellular Porcine Dermal Matrix. Materials 2022, 15, 1937. [Google Scholar] [CrossRef] [PubMed]
- Guarnieri, R.; Miccoli, G.; Reda, R.; Mazzoni, A.; Di Nardo, D.; Testarelli, L. Sulcus fluid volume, IL-6, and Il-1b concentrations in periodontal and peri-implant tissues comparing machined and laser-microtextured collar/abutment surfaces during 12 weeks of healing: A split-mouth RCT. Clin. Oral Implant. Res. 2022, 33, 94–104. [Google Scholar] [CrossRef]
- Huang, Z.-L.; Shi, J.-Y.; Zhang, X.; Gu, Y.-X.; Lai, H.-C. The influence of the shock-absorbing restorative materials on the stress distributions of short dental implant rehabilitations. Eur. Rev. Med. Pharmacol. Sci. 2021, 25, 24–34. [Google Scholar] [PubMed]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).