Abstract
Malaria is still the most destructive and dangerous parasitic infection in many tropical and subtropical countries. The burden of this disease is getting worse, mainly due to the increasing resistance of Plasmodium falciparum against the widely available antimalarial drugs. There is an urgent need for new, more affordable and accessible antimalarial agents possessing original modes of action. Natural products have played a dominant role in the discovery of leads for the development of drugs to treat human diseases, and this fact anticipates that new antimalarial leads may certainly emerge from tropical plant sources. This present review covers most of the recently-published non-alkaloidal natural compounds from plants with antiplasmodial and antimalarial properties, belonging to the classes of terpenes, limonoids, flavonoids, chromones, xanthones, anthraquinones, miscellaneous and related compounds, besides the majority of papers describing antiplasmodial crude extracts published in the last five years not reviewed before. In addition, some perspectives and remarks on the development of new drugs and phytomedicines for malaria are succinctly discussed.
1. Introduction
Among all parasitic agents causing disease in humans, malaria is undoubtedly the single most destructive and dangerous infectious agent in the developing world [1,2]. This vector-borne infectious disease is a classic example of one that affects the productivity of individuals, families and the whole society, since it causes more energy loss, more debilitation, more loss of work capacity and more economic damage than any other human parasitic diseases [3]. Malaria is commonly associated with poverty, but is also a cause of poverty and a major hindrance to economic development. There were an estimated 247 million malaria cases among 3.3 billion people at risk in 2006, causing nearly a million deaths, mostly of children under 5 years of age. It is widespread in tropical and subtropical regions, including parts of the Americas, Asia and Africa. A total of 109 countries were endemic for malaria in 2008, 45 within the WHO African region [4].
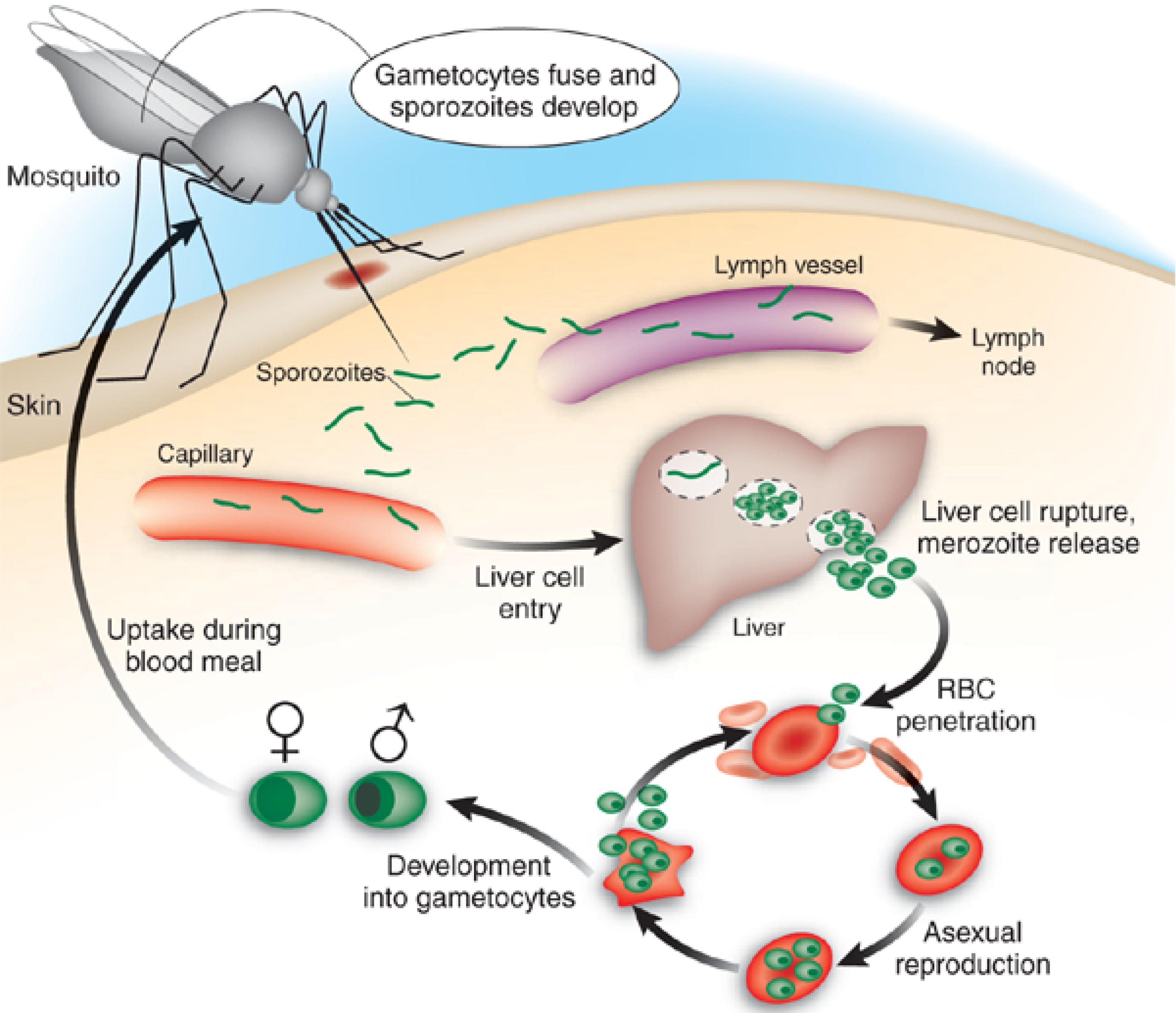
Although human malaria transmitted by female Anopheles mosquitoes has four Plasmodium species as its aetiological agents – P. falciparum, P. vivax, P. ovale and P. malariae, the most widespread and severe disease is caused by P. falciparum, which transiently infects the liver before invading red blood cells of the mammalian host (Figure 1). Clinical manifestations occur at the erythrocytic stage and can include fever, chills, prostration and anaemia, as well as delirium, metabolic acidosis, cerebral malaria and multi-organ system failure, which may be followed by coma and death [5,6,7].
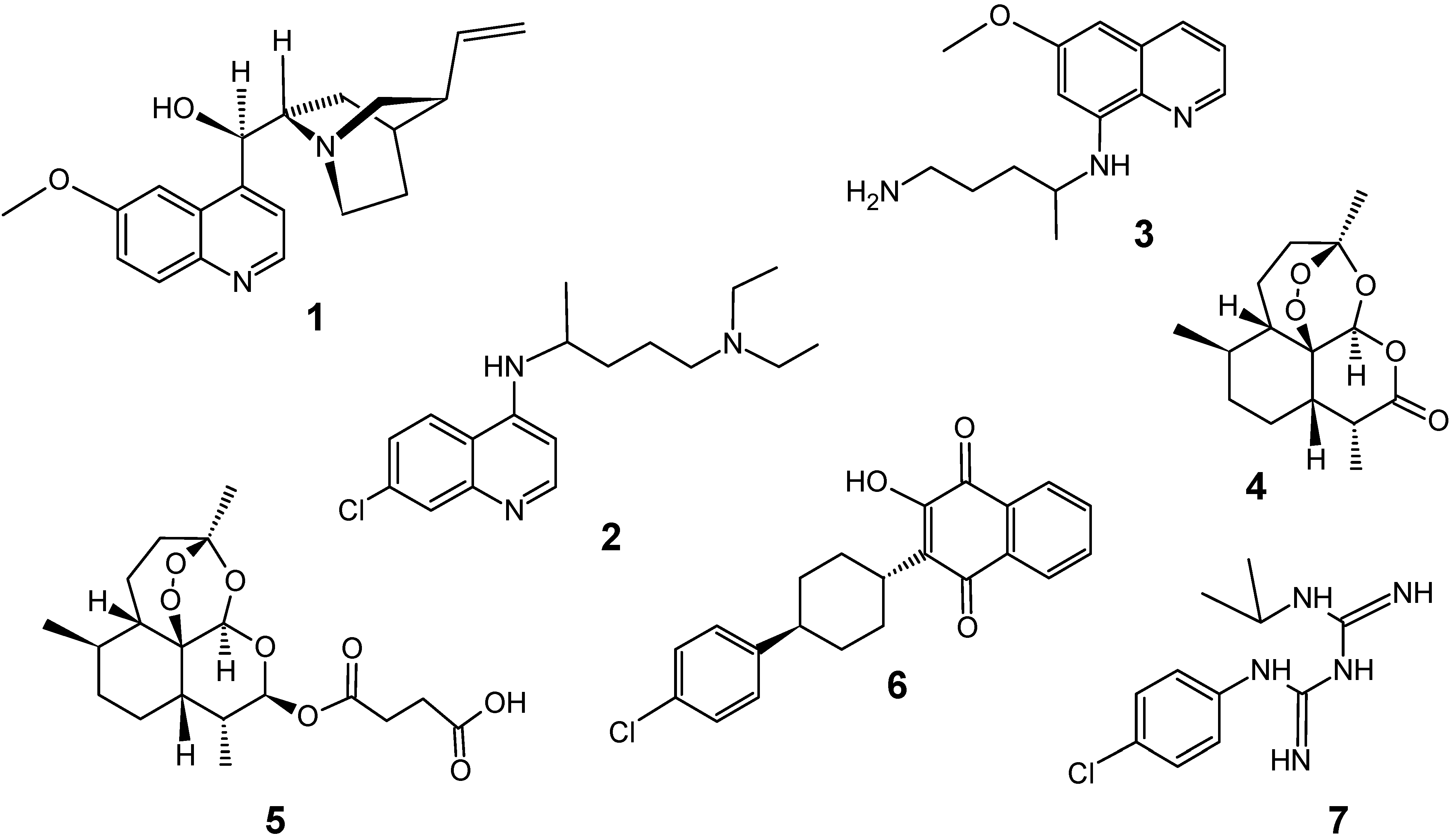
Quinine (1), an aminoquinoline alkaloid isolated from the bark of Cinchona species (Rubiaceae) in 1820 by Pelletier and Caventou, is one of the oldest and most important antimalarial drugs and is still used today. For almost three centuries, this alkaloid was the sole active principle effective against Plamodium falciparum, and it has been considered the responsible, after the Second World War, for the development of synthetic antimalarial drugs belonging to the classes of 4- and 8-aminoquinolines, such as chloroquine (2, 1940) and primaquine (3, 1952), among others. Until recently, chloroquine (2) was the only drug used for the treatment of malaria [8,9].
The appearance of drug-resistance P. falciparum strains since 1960, in particular to chloroquine, has made the treatment of malaria increasingly problematic in virtually all malarious regions of the world [2]. Several researchers have dedicated efforts to the development of new active compounds, especially from artemisinin (4), as an alternative to chloroquine (2). Currently no single drug is effective for treating multi-drug resistant malaria, and effective combination therapy includes artemisinin derivatives such as artesunate (5), or mixtures with older drugs such as the atovaquone (6) – proguanil (7) combination Malarone® [2,10]. Unfortunately first reports on drug resistance to artemisinin-derivatives [11] and to drug combination therapies [12] have already appeared. So, in the absence of a functional, safe and widely available malaria vaccine, efforts to develop new antimalarial drugs continue being urgently needed now.
There is a consensus among the scientific community that natural products have been playing a dominant role in the discovery of leads for the development of drugs for the treatment of human diseases [13]. Indeed, the vast majority of the existing antimalarial chemotherapeutic agents are based on natural products, and this fact anticipates that new leads may certainly emerge from the tropical plant sources, since biological chemodiversity continues to be an important source of molecular templates in the search for antimalarial drugs [14,15,16].
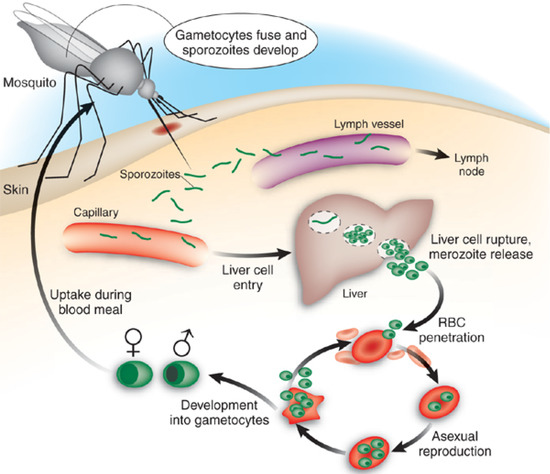
Figure 1.
Schematic life cycle of malaria in humans. Sporozoites are injected into human dermis through the bite of infected Anopheles mosquito. After inoculation, sporozoites migrate to liver cells to establish the first intracellular replicative stage. Merozoites generated from this exoerythrocytic phase then invade erythrocytes (RBCs), and it is during this erythrocytic stage that severe conditions of malaria occur. The life cycle is completed when sexual stages (gametocytes) are ingested by a mosquito. Some sporozoites deposited in the skin eventually penetrate capillaries or lymph vessels. Those entering the lymph vessels will penetrate lymph vascular endothelial cells in lymph nodes to establish a lymph node form, which appears not to continue the life cycle - but may be significant in priming an immune response. Adapted and reproduced by permission from Macmillan Publishers Ltd. [7].
Figure 1.
Schematic life cycle of malaria in humans. Sporozoites are injected into human dermis through the bite of infected Anopheles mosquito. After inoculation, sporozoites migrate to liver cells to establish the first intracellular replicative stage. Merozoites generated from this exoerythrocytic phase then invade erythrocytes (RBCs), and it is during this erythrocytic stage that severe conditions of malaria occur. The life cycle is completed when sexual stages (gametocytes) are ingested by a mosquito. Some sporozoites deposited in the skin eventually penetrate capillaries or lymph vessels. Those entering the lymph vessels will penetrate lymph vascular endothelial cells in lymph nodes to establish a lymph node form, which appears not to continue the life cycle - but may be significant in priming an immune response. Adapted and reproduced by permission from Macmillan Publishers Ltd. [7].
Few reviews focused on natural products with antiplasmodial activities have been reported in the recent literature. Saxena and co-workers published in 2003 a review article providing a critical account of crude extracts, essential oils and antiplasmodial secondary metabolites with diverse chemical structures from higher plants, collected from the period 1993-2003. A total of 127 alkaloids, 18 quassinoids, 23 sesquiterpenes, 27 triterpenoids, 21 flavonoids/xanthones, nine quinones and 25 miscellaneous compounds were highlighted in their work [8]. The review published by Frederich and collaborators in 2008 covers 31 indole alkaloids isolated from natural sources with high antiplasmodial activity (in vitro and in vivo), most of them displaying IC50 values under the micromolar range and with a good selectivity index [17]. Kaur and co-authors published in 2009 a review focusing on antimalarial compounds discovered during 1998-2008 from all natural sources, including crude plant and marine extracts. A total of 266 antiplasmodial natural products pertaining to the classes of alkaloids, terpenes, quassinoids, flavonoids, limonoids, chalcones, peptides, xanthones, quinones, coumarins and miscellaneous compounds, as well as 37 promising semisynthetic antimalarials, were listed in this compilation [18].
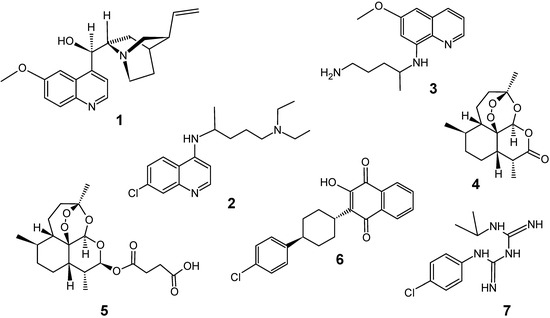
Figure 2.
Some traditional antimalarial drugs.
Figure 2.
Some traditional antimalarial drugs.
Fortunately, an increasing number of articles reporting antiplasmodial natural products from plants have been published recently. Considering that a review submitted by Oliveira and co-workers in 2009 deals with plant-derived antimalarial agents pertaining only to alkaloids [19], this review is intended as a continuation of that work, covering most of all recently-published reports of non-alkaloidal natural compounds with antiplasmodial and antimalarial properties from the period 2008-2009 not reviewed yet, in addition to recently published active crude extracts.
Regarding the criteria for considering the in vitro antiplasmodial activity of a given extract or compound as “good”, “moderate”, “low” or “inactive”, earlier studies by Basco and co-workers [20,21] have adopted the following criteria: IC50 < 10 µg/mL, good activity; IC50 of 10-50 µg/mL, moderate activity; IC50 of 50-100 µg/mL, low activity; and IC50 > 100 µg/mL, inactive. On the other hand, Muriithi and collaborators have expressed their IC50 values in µM and considered as inactive compounds showing IC50 > 100 µM; of limited (moderate?) activity, those with IC50 of 1–20 µM; and of low activity those displayng IC50 of 20–60 µM [22]. In this paper, both criteria have been combined in order to establish the following criteria adopted for all compounds described in this review: IC50 < 1 µM, excellent/potent activity; IC50 of 1-20 µM, good activity; IC50 of 20-100 µM, moderate activity; IC50 of 100-200 µM, low activity; and IC50 > 200 µM, inactive. In addition, Basco and co-workers’ criteria have been used for classifying the antiplasmodial activity of crude extracts.
2. Recently-Published Crude Extracts with Antiplasmodial Activity
Although many crude plant extracts with in vitro and in vivo antiplasmodial activities have been reported in the recent literature, only those which were not referred to in previously published reviews [8,18,23,24] are listed in Table 1. In addition, articles with extensive results [25,26,27,28,29,30,31,32,33,34,35,36,37,38,39,40,41,42] were not included in this Table. As it can be noted, the results often show only modest activity against the parasites in vitro or against malaria in mice, suggesting that the species in question probably have only a limited effect in man and that cure of the disease is unlikely. However, this may not necessarily mean that medicines made from these species are of no value, since partially effective treatments might be beneficial in those cases that the course of the disease is shortened by reducing anaemia and lowering the risk of death or serious illness from other anaemia-related diseases. Moreover, benefits may also include the alleviation of symptoms such as pain and fever and immunomodulation leading to increased immunity [43]. Finally, it is important to stress that plant extracts could also be effective against the parasite on hepatic stage.
As commented before, the more recent development of artemisinin derivatives has re-affirmed the potential of plant species to provide effective drugs for the treatment of malaria. The antiplasmodial activity of all plant extracts depicted in Table 1 confirms this statement and suggests that it would be worthwhile to invest more time and resources into further investigation on active plant species identified in these studies.

Table 1.
Recently-published plant extracts with antiplasmodial activity.
| Family | Species | Extract (part) | Antiplasmodial Activity (IC50, μg/mL) | Strain | Ref. | |
|---|---|---|---|---|---|---|
| Amaranthaceae | Amaranthus spinosus | Water (stem bark) | 789.36 ± 7.19 ¥ | (N.S.) ≠ S | [44] | |
| Annonaceae | Uvariopsis congolana | MeOH* (stem) | 4.47 ± 0.45 | W2 R | [45] | |
| MeOH* (leaves) | 4.57 ± 0.76 | W2 R | ||||
| Polyalthia oliveri | MeOH* (stem bark) | 4.30 ± 0.31 | W2 R | |||
| Enantia chlorantha | MeOH* (stem) | 4.79 ± 1.09 | W2 R | |||
| MeOH* (stem bark) | 2.06 ± 0.01 | W2 R | ||||
| Aphloiaceae | Aphloia theiforms | MeOH (bark) | 13.3 ± 0.8 | 3D7 S | [46] | |
| 11.0 ± 3.1 | W2 R | |||||
| CH2Cl2 (bark) | 16.1 ± 2.7 | 3D7 S | ||||
| 18.2 ± 2.7 | W2 R | |||||
| CH2Cl2 (leaves) | 21.0 ± 1.6 | 3D7S | ||||
| 22.7 ± 2.9 | W2 R | |||||
| Apiaceae | Ferula oopoda | MeOH (roots) | 26.6 | K1 R | [47] | |
| 24.9 | 3D7 S | |||||
| Astrodaucus orientalis | MeOH (aerial parts) | 46.1 | K1 R | |||
| 42.6 | 3D7 S | |||||
| Apocynaceae | Picralima nitida | EtOH (seeds) [115 mg/Kg] | 73.0%** | (N.S.) ≠ S | [48] | |
| Asclepiadaceae | Caralluma tuberculata | Pet. Ether (aerial parts) | 7.94 | K1 R | [49] | |
| Asteraceae | Vernonia amygdalina | EtOH (leaves) | 9.7 ± 2.6 | (N.S.) S | [50] | |
| Pet. Ether (leaves) | 2.5 ± 0.7 | (N.S.) S | ||||
| Isoamyl alcohol (leaves) | 2.7 ± 0.6 | (N.S.) S | ||||
| Psiadia arguta | CH2Cl2 (leaves) | 10.1 ± 2.2 | 3D7 S | [46] | ||
| 8.4 ± 1.1 | W2 R | |||||
| MeOH (leaves) | 22.4 ± 2.2 | 3D7 S | ||||
| 26.1 ± 6.5 | W2 R | |||||
| Centaurea bruguieriana | MeOH (aerial parts) | 36.9 | 3D7 S | [47] | ||
| Centaurea golestanica | MeOH (aerial parts) | 35.6 | K1 R | |||
| 31.6 | 3D7 S | |||||
| Boraginaceae | Heliotropium zeylanicum | MeOH (aerial parts) | 8.41 | K1 R | [49] | |
| Buxaceae | Buxus hyrcana | MeOH (aerial parts) | 4.7 | K1 R | [47] | |
| 7.7 | 3D7 S | |||||
| Caesalpiniaceae | Cassia occidentalis | EtOH (leaves) | 2.8 ± 0.5 | (N.S.) S | [50] | |
| Pet. Ether (leaves) | 1.5 ± 0.7 | (N.S.) S | ||||
| Isoamyl alcohol (leaves) | 18.6 ± 3.6 | (N.S.) S | ||||
| CHCl3 [pH 2-3] (leaves) | 2.9 ± 0.3 | (N.S.) S | ||||
| Capparaceae | Boscia angustifolia | CH2Cl2 (leaves) | 107.9 | 3D7 S | [51] | |
| MeOH (leaves) | 37.6 | 3D7 S | ||||
| Caryophyllaceae | Minuartia lineata | MeOH (aerial parts) | 44.0 | 3D7 S | [47] | |
| Clusiaceae | Croton zambesicus | EtOH (roots) [81 mg/Kg] | 86.18% ** | ANKA ≠ | [52] | |
| n-hexane (root) [57 mg/Kg] | 57.88% ** | ANKA ≠ | ||||
| CHCl 3 (root) [57 mg/Kg] | 75.39% ** | ANKA ≠ | ||||
| AcOEt (root) [57 mg/Kg] | 76.89% ** | ANKA ≠ | ||||
| MeOH (root) [57 mg/Kg] | 77.27% ** | ANKA ≠ | ||||
| Garcinia kola | EtOH (stem bark) | 2.9 ± 0.7 | (N.S.) S | [50] | ||
| Pet. Ether (stem bark) | 1.6 ± 0.2 | (N.S.) S | ||||
| Isoamyl alc. (stem bark) | 41.7 ± 3.2 | (N.S.) S | ||||
| CHCl3 [pH 2-3] (stem bark) | 27.1 ± 2.7 | (N.S.) S | ||||
| Symphonia globulifera | MeOH (leaves) | 4.1±0.5 | K1 R | [53] | ||
| Combretaceae | Terminalia bentzoe L. | MeOH (fresh leaves) | 12.8 ± 2.9 | 3D7 S | [46] | |
| 12.8 ± 3.5 | W2 R | |||||
| CH2Cl2 (leaves) | 42.7 ± 3.2 | 3D7 S | ||||
| 21.0 ± 2.1 | W2 R | |||||
| Cucurbitaceae | Momordica foetida | Water (shoots) | 40.7 ± 11.20 | D10 S | [54] | |
| 50.8 ± 3.00 | K1 R | |||||
| AcOEt (shoots) | 30.0 ± 1.70 | D10 S | ||||
| 29.30 ± 1.47 | K1 R | |||||
| MeOH (shoots) | 75.4 ± 17.50 | D10 S | ||||
| 68.80 ± 5.40 | K1 R | |||||
| Dilleniaceae | Tefracera pogge | EtOH (leaves) | 36.9± 4.2 | (N.S.) S | [50] | |
| Pet. Ether (leaves) | 1.7 ± 0.4 | (N.S.) S | ||||
| Isoamyl alcohol (leaves) | 21.8 ± 5.2 | (N.S.) S | ||||
| Euphorbiaceae | Euphorbia hirta | EtOH (whole plant) | 2.4 ± 0.2 | (N.S.) S | ||
| Pet. Ether (whole plant) | 1.2 ± 0.3 | (N.S.) S | ||||
| Isoamyl alc. (whole plant) | 2.6 ± 1.2 | (N.S.) S | ||||
| Neoboutonia. glabracens | MeOH (leaves) | 5.50 ± 0.20 | W2 R | [45] | ||
| Croton zambesicus | MeOH (stem bark) | 5.69 ± 0.06 | W2 R | |||
| Phyllantus niruri | EtOH (whole plant) | 2.5± 0.1 | (N.S.) S | [50] | ||
| Pet. Ether (whole plant) | 1.3 ± 0.3 | (N.S.) S | ||||
| Isoamyl alc. (whole plant) | 2.3 ± 0.5 | (N.S.) S | ||||
| Fabaceae | Glycyrrhiza glabra | MeOH (aerial parts) | 17.5 | K1 R | [47] | |
| Erythrina fusca | EtOAc (stem bark) | 7.5 | K1 R | [55] | ||
| Stylosanthes erecta | CH2Cl2 (aerial parts) | 21.9 | 3D7 S | [51] | ||
| MeOH (aerial parts) | 23.3 | 3D7 S | ||||
| Tetrapleura tetraptera | EtOH (fruits) [900 mg/Kg] | 76.37%** | (N.S.) ≠ S | [56] | ||
| Geraniaceae | Erodium oxyrrhnchum | MeOH (aerial parts) | 40.3 | K1 R | [47] | |
| 13.0 | 3D7 S | |||||
| Hypericaceae | Harungana madagascariensis | EtOH (stem bark) | 0.052-0.517 | (N.S.) | [57] | |
| MeOH (seeds) | 3.6 ± 0.3 | K1 R | [53] | |||
| Lamiaceae | Otostegia persica | MeOH (fruits + leaves) | 31.1 | K1 R | [47] | |
| Otostegia michauxii | MeOH (aerial parts) | 44.6 | K1 R | |||
| Perovskia abrotanoides | MeOH (aerial parts) | 37.3 | K1 R | |||
| Loganiaceae | Nuxia verticillata | CH2Cl2 (leaves) | 10.9 ± 1.8 | 3D7 S | [46] | |
| 8.8 ± 1.2 | W2 R | |||||
| MeOH (leaves) | 32.7 ± 7.4 | 3D7 S | ||||
| CH2Cl2 (bark) | 27.4 ± 6.6 | 3D7 S | ||||
| MeOH (bark) | 36.9 ± 5.7 | 3D7 S | ||||
| Buddleja salviifolia | CH2Cl2 (bark) | 49.9 ± 9.6 | 3D7 S | |||
| CH2Cl2 (leaves) | 29.7 ± 12.6 | 3D7 S | ||||
| 18.6 ± 5.8 | W2 R | |||||
| Strychnos angolensis | EtOAc (roots) | 17.0 ± 7.6 | FCA20 S | [58] | ||
| Strychnos cocculoides | EtOAc (leaves) | 20.0 ± 11.9 | FCA20 S | |||
| Strychnos gossweileri | EtOAc (roots) | 12.4 ± 4.1 | FCA20 S | |||
| Strychnos henningsii | EtOAc (leaves) | 15.9 ± 3.0 | FCA20 S | |||
| Strychnos johnsonii | EtOAc (stem) | 16.4 ± 1.8 | FCA20 S | |||
| Strychnos mellodora | EtOAc (leaves) | 13.4 | FCA20 S | |||
| MeOH (leaves) | 29.5 | FCA20 S | ||||
| EtOAc (stem) | 14.5 ± 1.5 | FCA20 S | ||||
| EtOAc (roots) | 11.2 ± 3.6 | FCA20 S | ||||
| MeOH (roots) | 25.4 ± 11.0 | FCA20 S | ||||
| Strychnos scheffleri | EtOAc (leaves) | 21.2 | FCA20 S | |||
| Strychnos variabilis | EtOAc (roots) | 2.5 ± 0.2 | FCA20 S | |||
| MeOH (roots) | 2.3 ± 0.5 | FCA20 S | ||||
| Meliaceae | Trichilia emetica | CH2Cl2 (leaves) | 11.9 | 3D7 S | [51] | |
| MeOH (leaves) | 47.6 | 3D7 S | ||||
| Mimosaceae | Cylicodiscus gabunensis | EtOH (stem bark) [60 mg/Kg] | 83.3% ¥ | (N.S.) ≠ S | [59] | |
| Albizia zygia | MeOH (stem bark) | 1.0 ± 0.1 | K1 R | [53] | ||
| Moraceae | Artocarpus communis | MeOH (leaves) | 4.00 ± 0.37 | W2 R | [45] | |
| Nyctagynaceae | Boerhaavia erecta | Water (stem bark) | 564.95 ± 6.23 ¥ | (N.S.) ≠ S | [44] | |
| Polygalaceae | Securidaca longipedunculata | CH2Cl2 (leaves) | 6.9 | 3D7 S | [51] | |
| Rubiaceae | Vangueria infausta | CHCl3 [fr.] (root bark) | 3.8 ± 1.5 | D6 S | [60] | |
| 4.5 ± 2.3 | W2 R | |||||
| Morinda morindoides | EtOH (leaves) | 94.2 ± 3.4 | (N.S.) S | [50] | ||
| Pet. Ether (leaves) | 1.8 ± 0.2 | (N.S.) S | ||||
| Isoamyl alcohol (leaves) | 15.3 ± 3.6 | (N.S.) S | ||||
| CHCl3 [pH 2-3] (leaves) | 8.8 ± 2.5 | (N.S.) S | ||||
| Sapindaceae | Cardiospermum halicacabum | AcOEt (shoots) | 28.60 ± 4.20 | D10 S | [54] | |
| 32.60 ± 2.60 | K1 R | |||||
| MeOH (shoots) | 62.60 ± 9.40 | D10 S | ||||
| 79.00 ± 5.20 | K1 R | |||||
| Solanaceae | Licium shawii | MeOH (aerial parts) | 7.75 | K1 R | [49] | |
| Tamaricaceae | Tamarix aralensis | MeOH (aerial parts) | 43.8 | 3D7 S | [47] | |
| Verbenaceae | Lantana camara | CH2Cl2 (leaves) | 8.7 ± 1.0 | 3D7 S | [46] | |
| 5.7 ± 1.6 | W2 R | |||||
| Vitaceae | Cissus quadrangulari | CH2Cl2 (whole plant) | 23.9 | 3D7 S | [51] | |
| MeOH (whole plant) | 52.8 | 3D7 S | ||||
| Zingiberaceae | Siphonochilus aethiopicus | EtOAc (rhizomes) | 2.90 ± 0.28 | D10 S | [61] | |
| 1.4 | K1 R | |||||
¥ ED50 (mg/Kg); R Chloroquine-resistant strain; S Chloroquine-sensitive strain; *Acetogenine-rich methanol extract; **in vivo chemossupression; (N.S.) – Not specified; ≠ P. berghei berghei, oral administration.
3. Antiplasmodial Non-Alkaloidal Natural Products
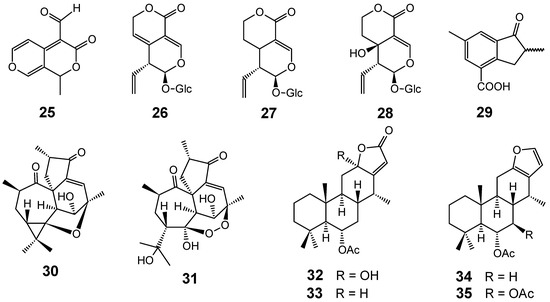
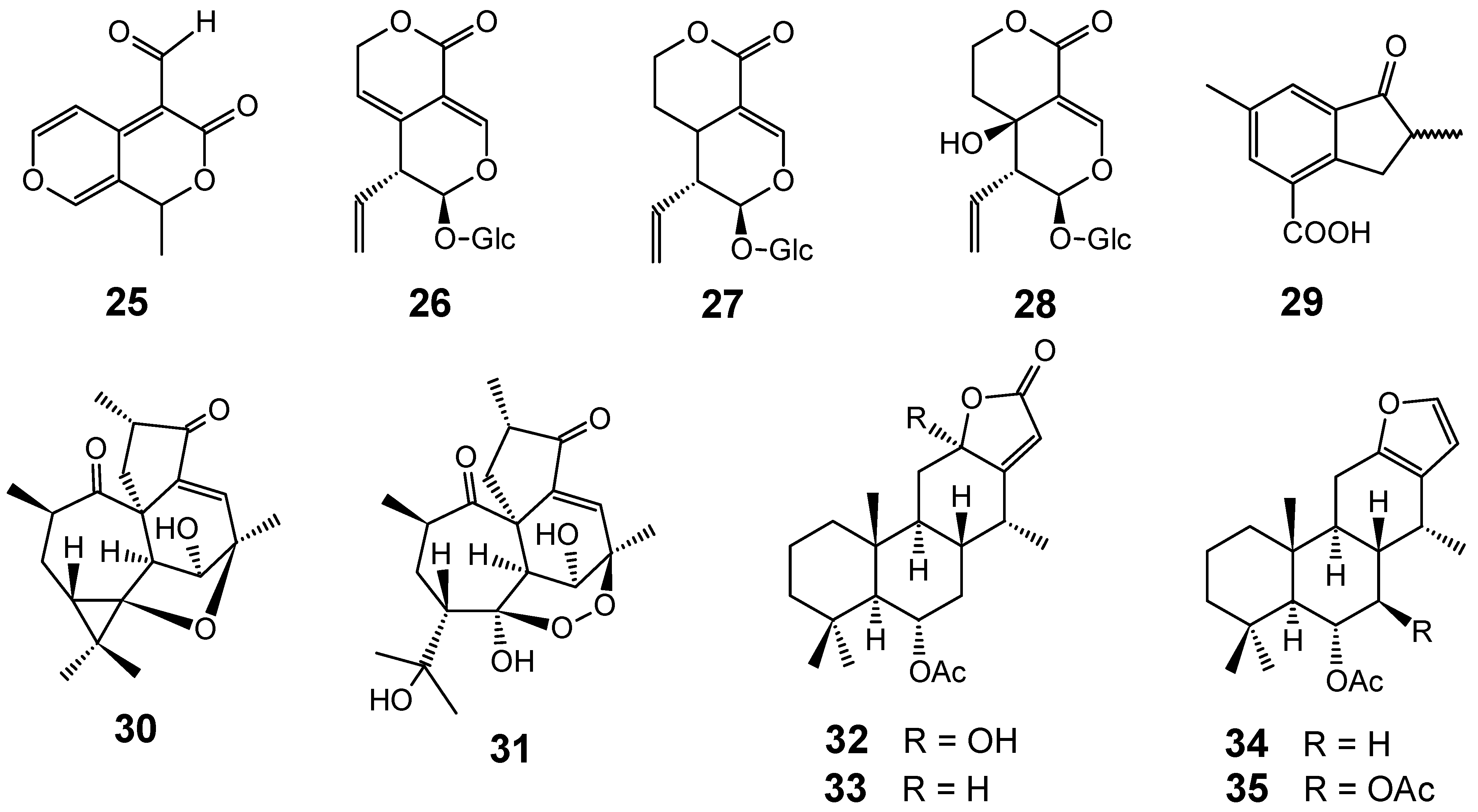
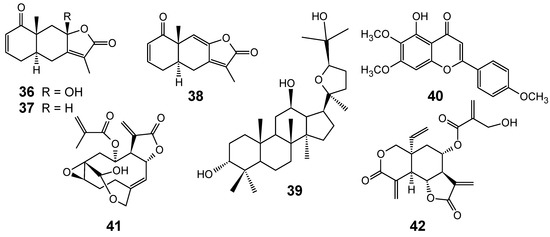
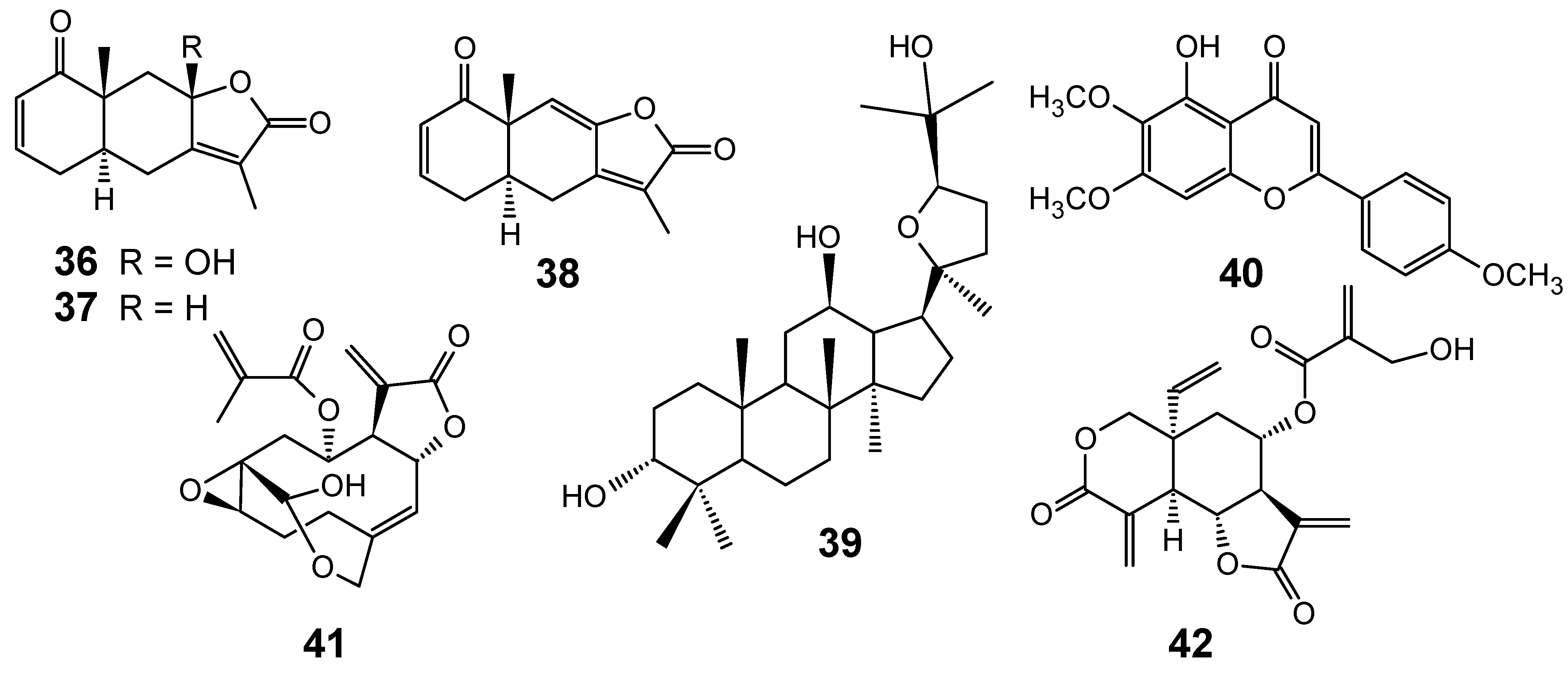
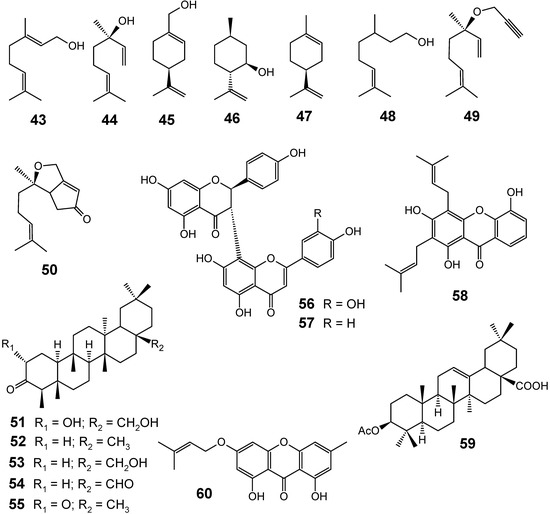
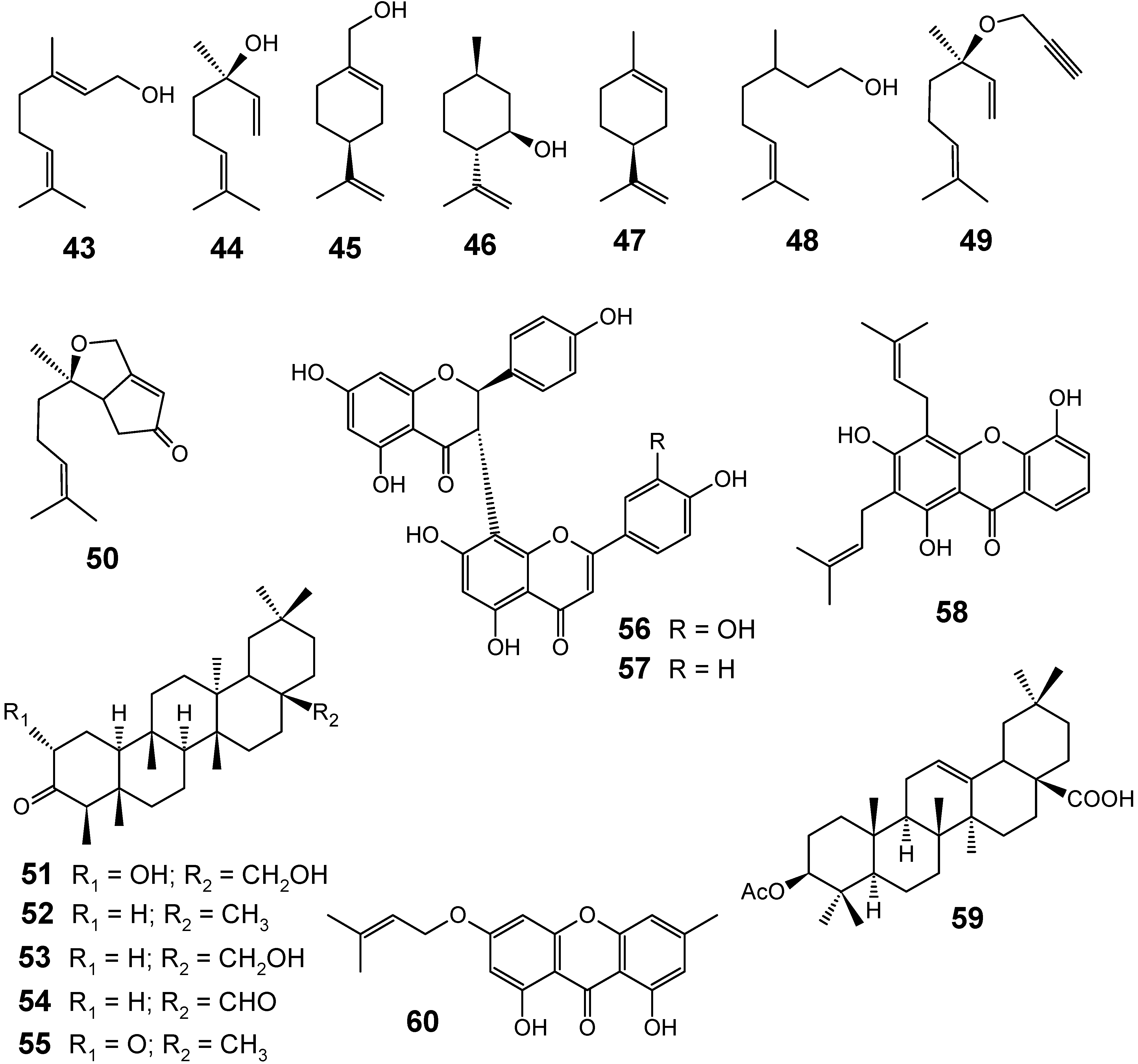
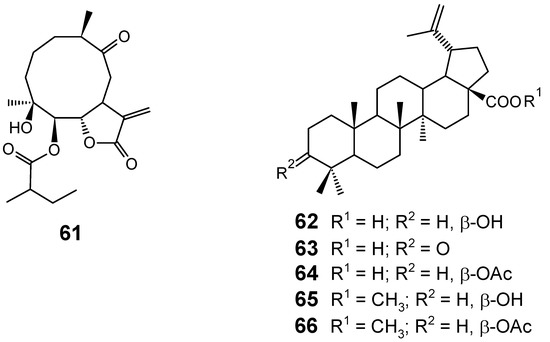
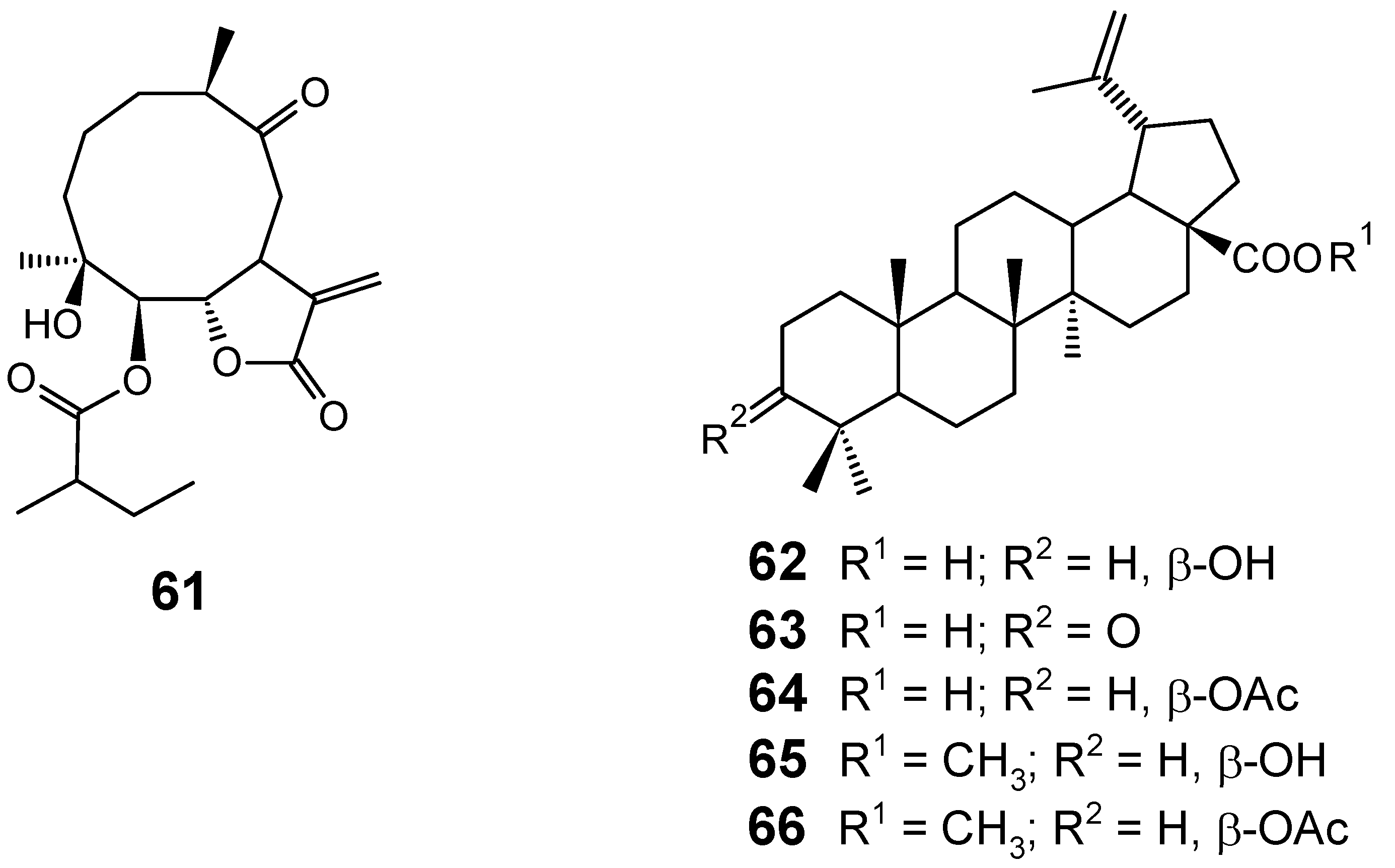
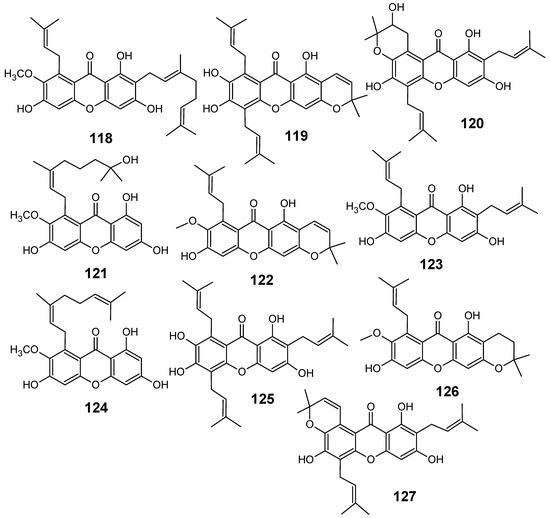
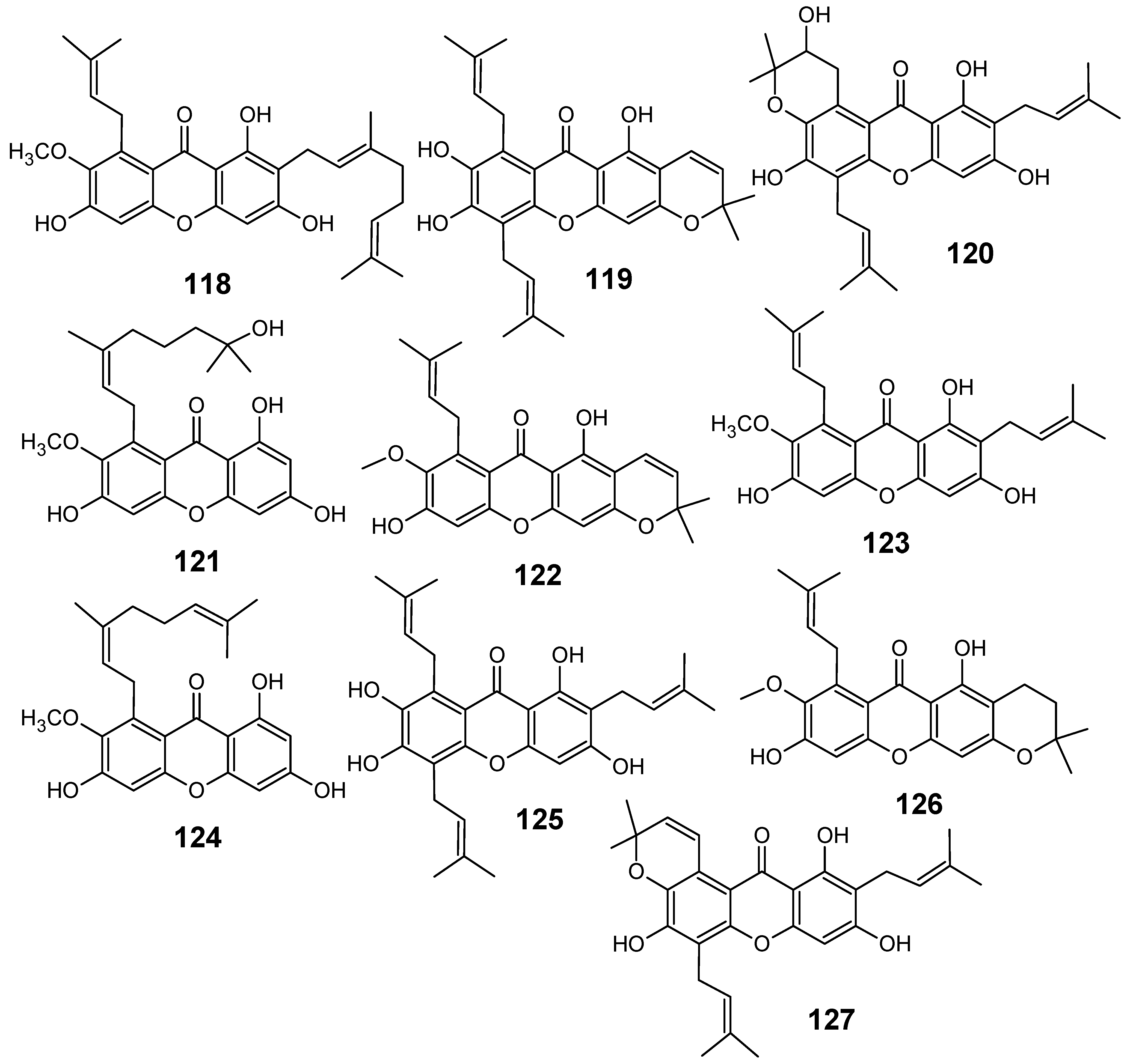
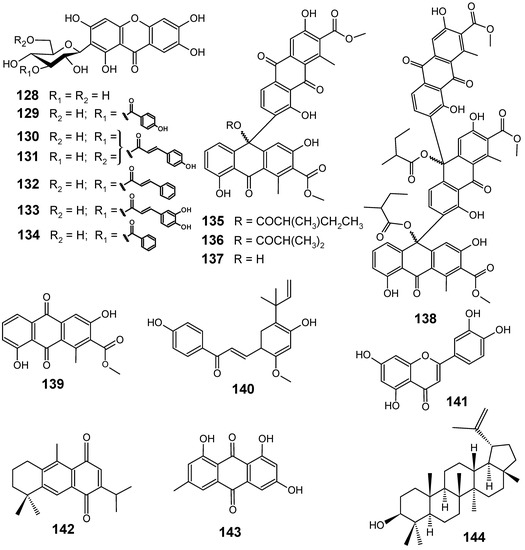
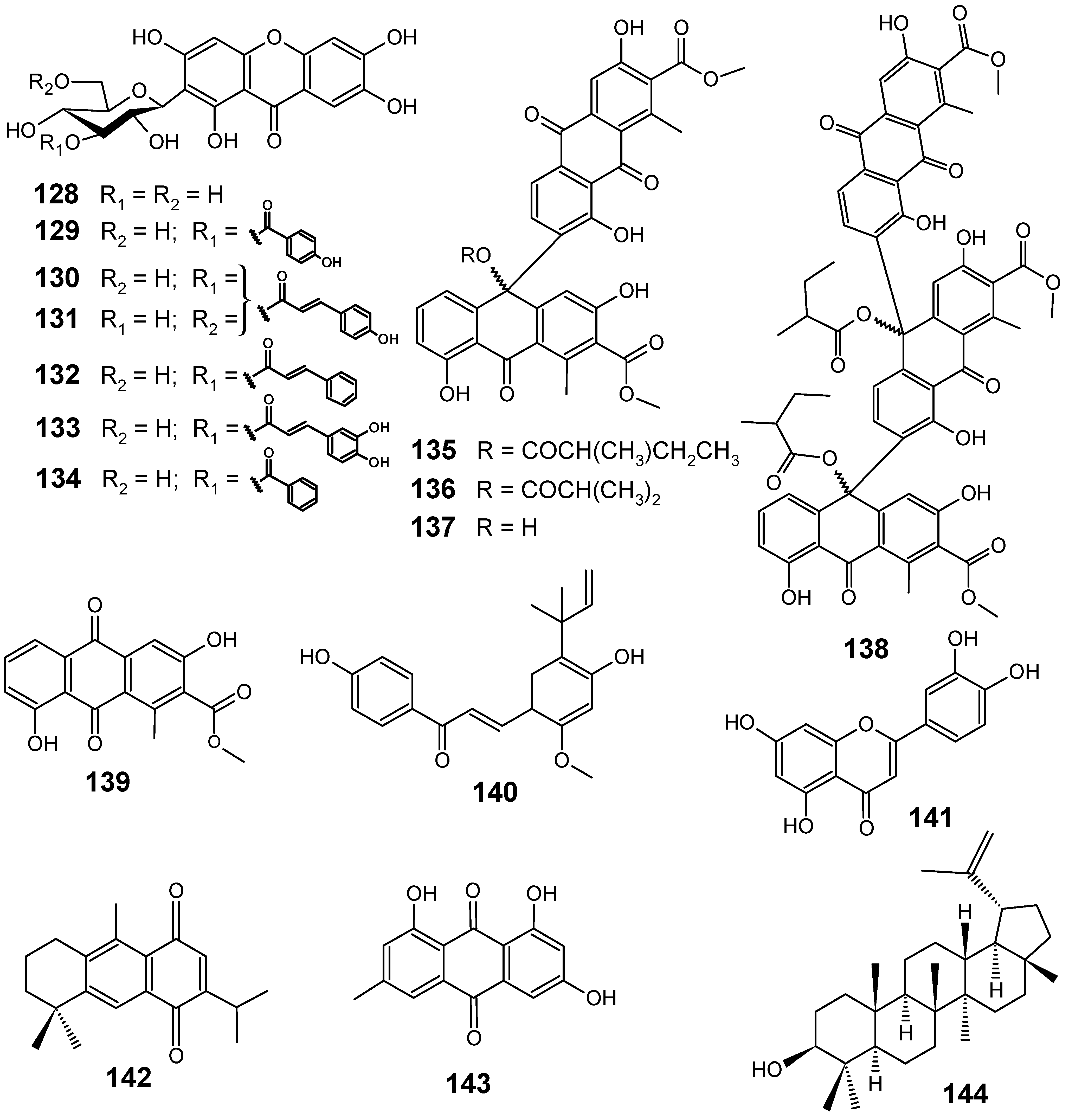
Although several classes of natural products are responsible for the antiplasmodial activity of many plant species used in traditional medicines for the treatment of malaria, the most important and diverse biopotency has been observed in alkaloids, quassinoids and sesquiterpene lactones [8]. Since alkaloids have been recently discussed in the literature [17,19], this review will highlight the majority of antiplasmodial non-alkaloidal natural products published in the period Jan/2008-May/2009 belonging to the classes of terpenes, limonoids, flavonoids, chromones, xanthones, anthraquinones, miscellaneous and related compounds.
3.3. Miscellaneous compounds
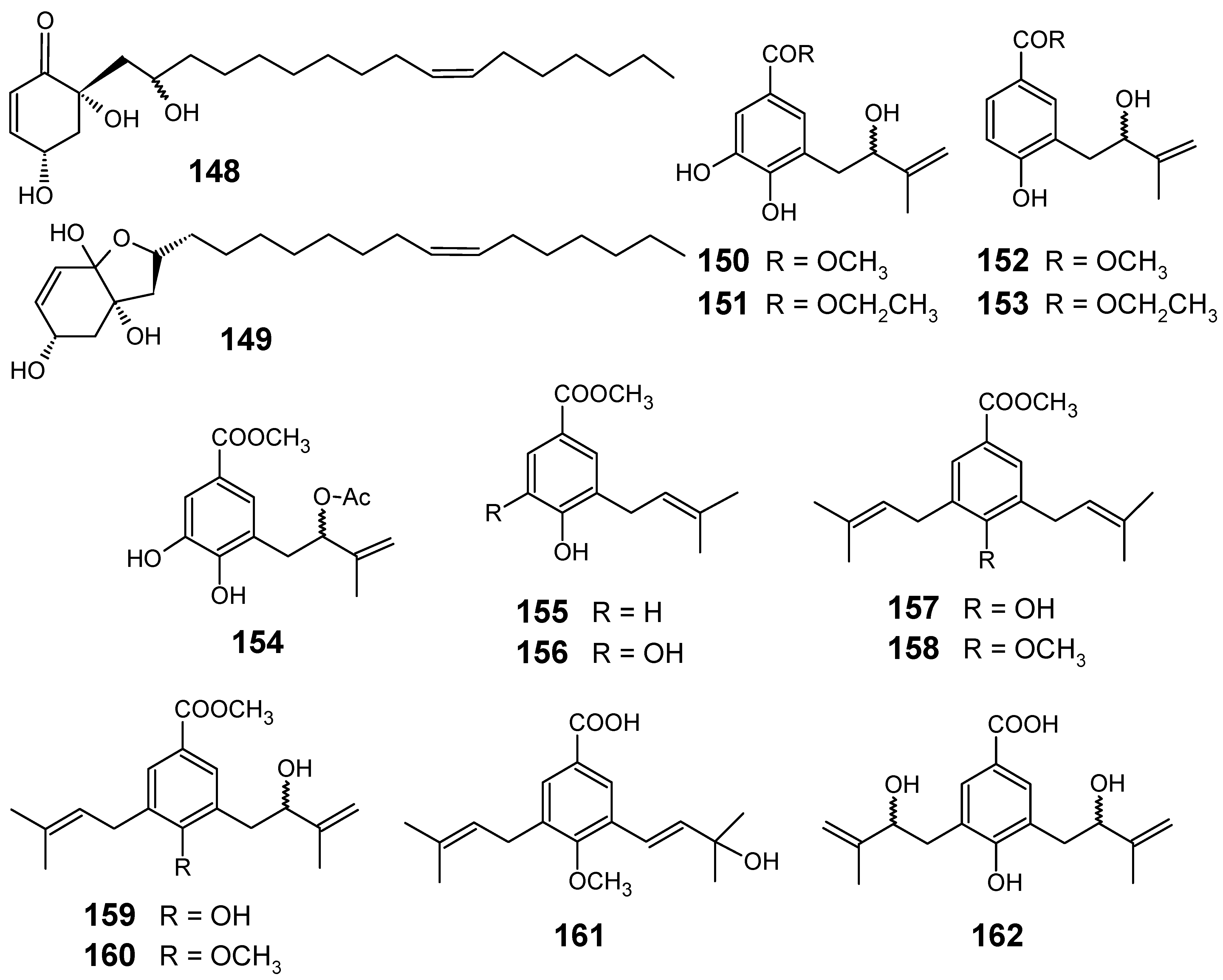
The bioassay-guided purification of CH2Cl2 bark extract of Tapirira guianensis (Anacardiaceae) led to the isolation of cyclic alkyl polyol derivatives 148 and 149 (Figure 16), which were active against the chloroquine-sensitive F32 strain (IC50 = 4.7 µM) and the chloroquine-resistant FcB1 strain (IC50 = 5.4 µM) of P. falciparum. These results show that it is the 148-149 mixture which is mainly responsible for the activities of this plant extract, since other compounds isolated from T. guianensis did not show any interesting activity against the pathogens tested, although they were chemically quite similar [95].
Piper glabratum and P. acutifolium were analyzed for their content of main secondary constituents, affording nine new benzoic acid derivatives (150, 151, 153, 154, 156, and 159-162), in addition to four known compounds (152, 155, 157, and 158) (Figure 16). Compounds 150, 152, 155, 156, 157, 159 and 161 were evaluated in vitro against Leishmania spp., Trypanosoma cruzi and P. falciparum. Among the evaluated compounds, only 155 and 156 exhibited a relative good antiplasmodial activity against F-32 Tanzania (chloroquine sensitive) strains of P. falciparum, with IC50 values of 12.7 and 16.3 μM, respectively. The rest of the compounds were considered less active (IC50 > 16.4 μM). Taking into account the results of the biological activities evaluated, a preliminary structure-activity relationship revealed that the prenylated 4-hydroxybenzoic acid derivatives with one side chain (150, 152, 155 and 156) were substantially more active as potential antiparasitic agents than those with two side chains (157, 158, 159 and 160) [96].
Eleven new polycyclic polyprenylated acylphloroglucinols (PPAPs) (165-170, 172-176) along with the known isogarcinol (163), cycloxanthochymol (164) and garcinol (171) (Figure 17), were isolated from the methanol extract of the trunk latex of Moronobea coccinea (Clusiaceae) which showed 95% inhibitory growth at 10 μg/mL against a chloroquine-resistant strain of P. falciparum (FcB1). Compounds 163-176 exhibited good antiplasmodial activity, being compounds 163-170 the most active ones with their IC50 values ranging from 3.3 to 9.0 μM. These results indicated that the benzophenones with a tetrahydropyran ring are the most potent compounds. In contrast, compounds 171-176 showed lower antiplasmodial activities with IC50 values over 10 μM [97].
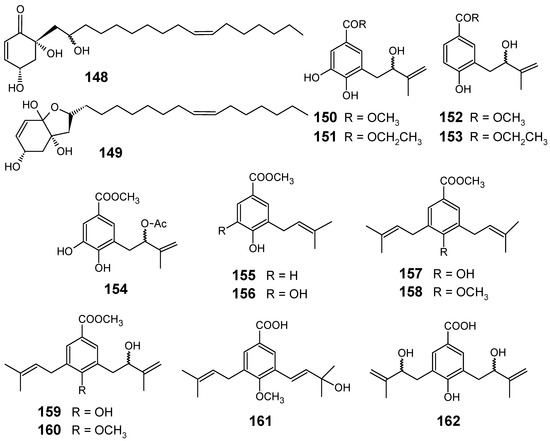
Figure 16.
Antiplasmodial miscellaneous compounds 148-162.
Figure 16.
Antiplasmodial miscellaneous compounds 148-162.
From compounds such as crypthophilic acids A–C (177-179) (Figure 18), which are the first resin glycosides occurring in another family (Scrophulariaceae) that is not Convolvulaceae, along with buddlejasaponin III (180), L-tryptophan and other constituents isolated from the aerial parts of Scrophularia cryptophila, only compounds 179, L-tryptophan and 180 showed antimalarial activity against K1 strain of P. falciparum with IC50 values of 4.0, 81.3 and 24.5 μM, respectively. In target identification studies, none of the three compounds inhibited PfFabI, a key enzyme from the P. falciparum type II fatty acid cascade, FAS-II. In addition, all compounds were found to be selective as they did not possess any cytotoxicity on mammalian L6 cells even at high concentrations (IC50 values >> 470 μM) [98].
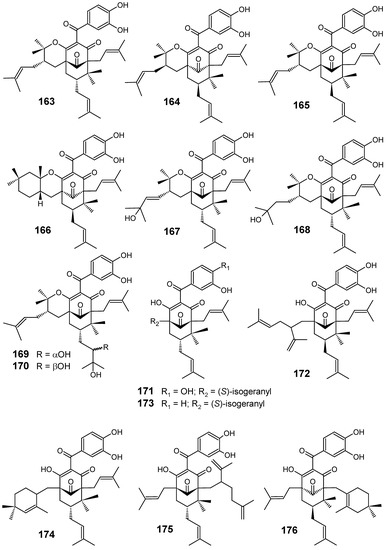
Figure 17.
Antiplasmodial miscellaneous compounds 163-176.
Figure 17.
Antiplasmodial miscellaneous compounds 163-176.
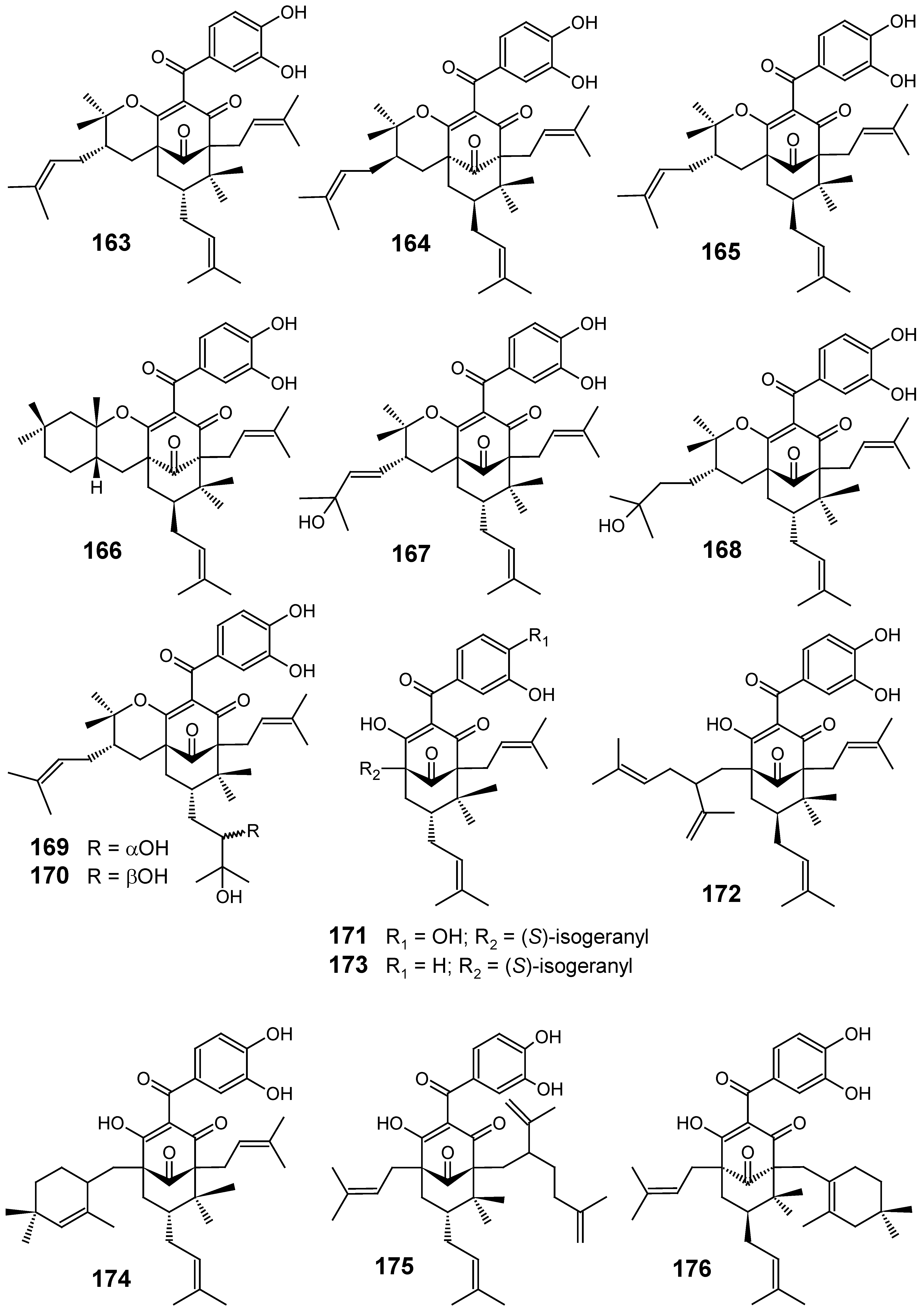
Fractionation of dichloromethane extracts from the leaves of Piper heterophyllum and P. aduncum afforded three new prenylated hydroxybenzoic acids (181-183), along with six known compounds (184-189) (Figure 18). Evaluation of the antiparasitic activity for all isolates showed that all the compounds were considered to be moderately active (IC50 >> 10 µg/mL), except for compound 181, which exhibited a good activity against P. falciparum with an IC50 of 7.0 µM, in comparison with chloroquine used as a positive control (IC50 = 0.3 µM). In conclusion, a geranylgeranyl side chain along with a carboxyl acid group as in 181 seem to be relevant for the antiplasmodial activity [99].
Figure 18.
Antiplasmodial miscellaneous compounds 177-204.
Figure 18.
Antiplasmodial miscellaneous compounds 177-204.
Extracts from Holostylis reniformis were tested in vivo against P. berghei and in vitro against a chloroquine-resistant strain of P. falciparum. The hexane extract of the roots was the most active, causing 67% reduction of parasitemia in vivo. From this extract, six lignans 190-195 (Figure 18), including a new (7’R,8S,8’S)-3’,4’-methylenedioxy-4,5-dimethoxy-2,7’-cyclolignan-7-one (195), were isolated and assayed in vitro against P. falciparum. The three most active lignans (190-192) showed IC50 values of <0.32 µM (<0.12 µg/mL), lignan 192 being the most active compound (IC50 = 0.20 µM). Lignan 194 exhibited a lower activity (IC50 = 8.00 µM), whereas lignan 195 did not exhibit any activity under the same experimental conditions. An evaluation of minimum lethal dose (30%) values showed low toxicity for these lignans in a hepatic cell line (Hep G2A16). Therefore, in vivo assays and clinical studies need to be undertaken with these compounds in order to confirm them as potential candidates for the development of antimalarial drugs [100].
Based on previous work which revealed that petroleum ether extracts of Viola websteri (Violaceae) showed inhibition value of 31.7 as percentage of parasite inhibition at 25 μg/mL, this extract was investigated for its activity against the chloroquine-sensitive D10 strain of P. falciparum. Bioassay-guided fractionation led to the identification of two structurally related compounds (196 and 197) (Figure 18) which were shown to be responsible for the observed activity of the extract. The main antiplasmodial principles, 6-(8’Z-pentadecenyl)-salicylic acid (196) and 6-(8’Z, 11’Z, 14’Z-heptadecatrienyl)-salicylic acid (197), have been isolated from V. websteri for the first time. In addition, this is the first report on the antiplasmodial activity of these compounds. Although compounds 196 (IC50 = 10.1 ± 3.2 µM) and 197 (IC50 = 13.3 ± 6.7 µM) are over 100 times less active than the positive controls, the data suggest that their antiplasmodial activity might not be due to general toxicity [101].
The dichloromethane, methanol and aqueous ethanol extracts of the stem bark of Pycnanthus angolensis (Myristicaceae) were evaluated for their in vitro activity against the 3D7 P. falciparum strain. The CH2Cl2 extract was the most active showing an IC50 = 1.6 μg/mL. From this extract, a new dibenzylbutane lignan, threo-4,4′-dihydroxy-3-methoxylignan (198) named pycnantolol, together with the known lignans (-)-dihydroguaiaretic acid (199), heliobuphthalmin (200), talaumidin (201), hinokinin (202), the labdane type diterpene ozic acid (203) and the steroids stigmast-4-en-6β-ol-3-one (204) (Figure 18), β-sitosterol and stigmasterol were isolated. The antiplasmodial activity of lignans 198–202, ozic acid (203) and stigmast-4-en-6β-ol-3-one (204) was evaluated against 3D7 and Dd2 P. falciparum strains. In contrast with the crude extracts, these isolated compounds have not shown significant antiplasmodial activity against both strains, the lowest IC50 value (60.5 µM) being obtained for talaumidin (201) against the Dd2-chloroquine resistant P. falciparum strain. These results might be explained by synergistic effects between the different constituents of the complex extract and, especially if the antimalarial activity remains being observed in clinical studies and/or animal models, they could suggest that a standardization of the bark extract might be the best solution to a rational use of this traditional antimalarial plant [102].
4. Perspectives and Remarks on the Development of New Drugs and Phytomedicines for Malaria
The research on new antimalarial agents presently faces two distinct challenges: the search for new chemical entities (NCE) of natural or synthetic origin, and the development of phytomedicines [19]. The antiplasmodial/antimalarial natural products focused in this review can be divided into two groups: one of highly active compounds, of complex structures, for which no possibility of practical synthesis can be forseen, and another one, of moderate to low activity but of relative simple structures and, therefore, their synthesis and/or of their analogues could be undertaken. Plant species producing compounds of the first group are potential candidates for the development of phytomedicines, while the second group would represent templates to synthetic drugs.
Will the research on traditional plants contribute for the discovery of new antimalarial drugs? There is no doubt about this possibility. Atovaquone, quinine, artemisinin and its semi-synthetic derivatives are remarkable examples of the diverse contribution of natural products for the development of effective antimalarial drugs, particularly valuable for the treatment of chloroquine-resistant parasites.
Indeed, several potent antiplasmodial natural products have been described, as shown in this review, most of them have only been evaluated by in vitro assays and few of them were evaluated for cytotoxicity and still smaller is the number of those assayed in vivo. Besides, many of them are found in low concentrations in the plant species and usually as part of complex mixtures making their isolation and purification highly expensive. These are typical situations which point to the development of phytomedicines, the known active compounds being useful as chemical-biological markers to guarantee product quality.
Validation of traditional plant remedies presents limitations such as prioritization of plant species for research, lack of informations on ethnobotany of these plants (location and abundance, parts used, form of use, duration of treatment), definition of dosages due to variation on the concentrations of active ingredients in a plant species [103]. It should also be stressed that a basic requirement for the validation of a medicinal plant is the standardization of extracts to be evaluated, including the identification and quantification of chemical and/or biological markers to assure the development of efficient and safe phytomedicines in a short time and at low cost. It is well known that the qualitative and quantitative contents of secondary metabolites in a plant are susceptible to marked variation that is regulated by intrinsic factors (ontogeny and phenology) as well by abiotic (e.g. light, moisture, nutrient availability) and biotic factors such as different physiological and growth stages [104], which make the standardization obligatory.
5. Conclusions
This work reviewed most recently-published non-alkaloidal natural compounds from plants with antiplasmodial and antimalarial properties, besides the majority of antiplasmodial crude extracts published in the last five years. Considering the many antiplasmodial activities observed for all crude extracts and natural compounds described here, it can be stated that in fact there are optimistic perspectives on the continuing investigation of plants used in traditional medicines for the treatment of malaria, and they will certainly lead the scientific community to the discovery of more new efficient molecular templates and phytomedicines for this disease. Malaria and other neglected diseases, such as Chagas’ disease, leishmaniasis and African trypanosomiasis, among others, have a devastating impact on the world’s poor. Unfortunately they have been progressively marginalized by those in charge of making research programme decisions both in public and private sectors, since people suffering from these diseases have not offered a market lucrative enough to attract any notable investment in research and development for new drugs. Thus, this work also intends to stimulate and bring together new and intensive efforts from all research communities of the world to the quest of efficient phytomedicines and novel potential drug candidates both for malaria and other neglected diseases.
Acknowledgements
The authors thank FAPESB, FAPEMIG, CNPq and CAPES for financial supports, as well as Bianca Maia Cezário (UESB) and Eduardo Paulo Gomes for the helpful linguistic assistance. Permission provided by Nature Publishing Group to reproduce Figure 1 is also gratefully acknowledged.
References
- Greenwood, B.M.; Bojang, K.; Whitty, C.J.; Targett, G.A. Malaria. Lancet 2005, 365, 1487–1498. [Google Scholar] [CrossRef]
- Winter, R.W.; Kelly, J.X.; Smilkstein, M.J.; Dodean, R.; Bagby, G.C.; Rathbun, R.K.; Levin, J.I.; Hinrichs, D.; Riscoe, M.K. Evaluation and lead optimization of anti-malarial acridones. Exp. Parasitol. 2006, 114, 47–56. [Google Scholar] [CrossRef]
- Sachs, J.; Malaney, P. The economic and social burden of malaria. Nature 2002, 415, 680–685. [Google Scholar] [CrossRef]
- WHO. World Malaria Report. World Health Organization: Geneva, Switzerland, 2008. Available online: http://apps.who.int/malaria/wmr2008/.
- Fidock, D.A.; Rosenthal, P.J.; Croft, S.L.; Brun, R.; Nwaka, S. Antimalarial drug discovery: efficacy models for compound screening. Nat. Rev. Drug Discov. 2004, 3, 509–520. [Google Scholar] [CrossRef]
- Deprez-Poulain, R.; Melnyk, P. 1,4-Bis(3-aminopropyl)piperazine libraries: from the discovery of classical chloroquine-like antimalarials to the identification of new targets. Comb. Chem. High Throughput Screen. 2005, 8, 39–48. [Google Scholar] [CrossRef]
- Jones, M.K.; Good, M.F. Malaria parasites up close. Nat. Med. 2006, 12, 170–171. [Google Scholar] [CrossRef]
- Saxena, S.; Pant, N.; Jain, D.C.; Bhakuni, R.S. Antimalarial agents from plant sources. Curr. Sci. 2003, 85, 1314–1329. [Google Scholar]
- Viegas Júnior, C.; Bolzani, V.S.; Barreiro, E.J. Os produtos naturais e a química medicinal moderna. Quím. Nova 2006, 29, 326–337. [Google Scholar]
- Taylor, W.R.; White, N.J. Antimalarial drug toxicity: a review. Drug Saf. 2004, 27, 25–61. [Google Scholar] [CrossRef]
- Jambou, R.; Legrand, E.; Niang, M.; Khim, N.; Lim, P.; Volney, B.; Ekala, M.T.; Bouchier, C.; Esterre, P.; Fandeur, T.; Mercereau-Puijalon, O. Resistance of Plasmodium falciparum field isolates to in vitro artemether and point mutations of the SERCA-type PfATPase6. Lancet 2005, 366, 1960–1963. [Google Scholar] [CrossRef]
- Wichmann, O.; Muhlen, M.; Grub, H.; Mockenhaupt, F.P.; Suttorp, N.; Jelinek, T. Malarone treatment failure not associated with previously described mutations in the cytochrome b gene. Malaria J. 2004, 3, 1–3. [Google Scholar] [CrossRef]
- Newman, D.J.; Cragg, G.M.; Snader, K.M. Natural products as sources of new drugs over the period 1981-2002. J. Nat. Prod. 2003, 66, 1022–1037. [Google Scholar] [CrossRef]
- Ziegler, H.L.; Staerk, D.; Christensen, J.; Hviid, L.; Hagerstrand, H.; Jaroszewski, J.W. In vitro Plasmodium falciparum drug sensitivity assay: inhibition of parasite growth by incorporation of stomatocytogenic amphiphiles into the erythrocyte membrane. Antimicrob. Agents Chemother. 2002, 46, 1441–1446. [Google Scholar] [CrossRef]
- Kalauni, S.K.; Awale, S.; Tezuka, Y.; Banskota, A.H.; Linn, T.Z.; Asih, P.B.; Syafruddin, D.; Kadota, S. Antimalarial activity of cassane- and norcassane-type diterpenes from Caesalpinia crista and their structure-activity relationship. Biol. Pharm. Bull. 2006, 29, 1050–1052. [Google Scholar] [CrossRef]
- Portet, B.; Fabre, N.; Roumy, V.; Gornitzka, H.; Bourdy, G.; Chevalley, S.; Sauvain, M.; Valentin, A.; Moulis, C. Activity-guided isolation of antiplasmodial dihydrochalcones and flavanones from Piper hostmannianum var. berbicense. Phytochemistry 2007, 68, 1312–1320. [Google Scholar] [CrossRef]
- Frederich, M.; Tits, M.; Angenot, L. Potential antimalarial activity of indole alkaloids. Trans. R. Soc. Trop. Med. Hyg. 2008, 102, 11–19. [Google Scholar] [CrossRef]
- Kaur, K.; Jain, M.; Kaur, T.; Jain, R. Antimalarials from nature. Bioorg. Med. Chem. 2009, 17, 3229–3256. [Google Scholar] [CrossRef]
- Oliveira, A.B.; Dolabela, M.F.; Braga, F.C.; Jácome, R.L.R.P.; Varotti, F.P.; Póvoa, M.M. Plant-derived antimalarial agents: new leads and efficient phytomedicines. Part I. Alkaloids. Ann. Braz. Acad. Sci. 2009, in press. [Google Scholar]
- Basco, L.; Mitaku, S.; Skaltsounis, A.L.; Ravelomanantsoa, N.; Tillequin, R.; Koch, M.; Le Bras, J. In vitro activities of furoquinoline and acridone alkaloids against Plasmodium falciparum. Antimicrob. Agents Chemother. 1994, 38, 1169–1171. [Google Scholar] [CrossRef]
- Dolabela, M.F.; Oliveira, S.G.; Nascimento, J.M.; Peres, J.M.; Wagner, H.; Póvoa, M.M.; Oliveira, A.B. In vitro antiplasmodial activity of extract and constituents from Esenbeckia febrifuga, a plant traditionally used to treat malaria in the Brazilian Amazon. Phytomedicine 2008, 15, 367–372. [Google Scholar] [CrossRef]
- Muriithi, M.W.; Abraham, W.R.; Addae-Kyereme, J.; Scowen, I.; Croft, S.L.; Gitu, P.M.; Kendrick, H.; Njagi, E.N.M.; Wright, C.W. Isolation and in vitro antiplasmodial activities of alkaloids from Teclea trichocarpa: in vivo antimalarial activity and X-ray crystal structure of normeliopicine. J. Nat. Prod. 2002, 65, 956–959. [Google Scholar] [CrossRef]
- Pillay, P.; Maharaj, V.J.; Smith, P.J. Investigation South African plants as a source of new antimalarial drugs. J. Ethnopharmacol. 2008, 119, 438–454. [Google Scholar] [CrossRef]
- Mariath, I.R.; Falcão, H.S.; Barbosa-Filho, J.M.; Sousa, L.C.F.; Tomaz, A.C.A.; Batista, L.M.; Diniz, M.F.M.F.; Athayde-Filho, P.F.; Tavares, J.F.; Silva, M.S.; Cunha, E.V.L. Plants of the American continent with antimalarial activity. Braz. J. Pharmacogn. 2009, 19, 158–192. [Google Scholar]
- Zirihi, G.N.; Mambu, L.; Guédé-Guina, F.; Bodo, B.; Grellier, P. In vitro antiplasmodial activity and cytotoxicity of 33 West African plants used for treatment of malaria. J. Ethnopharmacol. 2005, 98, 281–285. [Google Scholar] [CrossRef]
- Koch, A.; Tamez, P.; Pezzuto, J.; Soejarto, D. Evaluation of plants used for antimalarial treatment by the Maasai of Kenya. J. Ethnopharmacol. 2005, 101, 95–99. [Google Scholar] [CrossRef]
- Mbatchi, S.F.; Mbatchi, B.; Banzouzi, J.T.; Bansimba, T.; Nsonde Ntandou, G.F.; Ouamba, J.M.; Berry, A.; Benoit-Vical, F. In vitro antiplasmodial activity of 18 plants used in Congo Brazzaville traditional medicine. J. Ethnopharmacol. 2006, 104, 168–174. [Google Scholar] [CrossRef]
- Menan, H.; Banzouzi, J.T.; Hocquette, A.; Pelissier, Y.; Blache, Y.; Kone, M.; Mallie, M.; Assi, L.A.; Valentin, A. Antiplasmodial activity and cytotoxicity of plants used in West African traditional medicine for the treatment of malaria. J. Ethnopharmacol. 2006, 105, 131–136. [Google Scholar] [CrossRef]
- Kvist, L.P.; Christensen, S.B.; Rasmussen, H.B.; Mejia, K.; Gonzalez, A. Identification and evaluation of Peruvian plants used to treat malaria and leishmaniasis. J. Ethnopharmacol. 2006, 106, 390–402. [Google Scholar] [CrossRef]
- Hout, S.; Chea, A.; Bun, S.S.; Elias, R.; Gasquet, M.; Timon-David, P.; Balansard, G.; Azas, N. Screening of selected indigenous plants of Cambodia for antiplasmodial activity. J. Ethnopharmacol. 2006, 107, 12–18. [Google Scholar] [CrossRef]
- Nguyen-Pouplin, J.; Tran, H.; Phan, T.A.; Dolecek, C.; Farrar, J.; Tran, T.H.; Caron, P.; Bodo, B.; Grellier, P. Antimalarial and cytotoxic activities of ethnopharmacologically selected medicinal plants from South Vietnam. J. Ethnopharmacol. 2007, 109, 417–427. [Google Scholar] [CrossRef]
- de Mesquita, M.L.; Grellier, P.; Mambu, L.; de Paula, J.E.; Espindola, L.S. In vitro antiplasmodial activity of Brazilian Cerrado plants used as traditional remedies. J. Ethnopharmacol. 2007, 110, 165–170. [Google Scholar] [CrossRef]
- Muregi, F.W.; Ishih, A.; Miyase, T.; Suzuki, T.; Kino, H.; Amano, T.; Mkoji, G.M.; Terada, M. Antimalarial activity of methanolic extracts from plants used in Kenyan ethnomedicine and their interactions with chloroquine (CQ) against a CQ-tolerant rodent parasite, in mice. J. Ethnopharmacol. 2007, 111, 190–195. [Google Scholar] [CrossRef]
- Osorio, E.; Arango, G.J.; Jimenez, N.; Alzate, F.; Ruiz, G.; Gutierrez, D.; Paco, M.A.; Gimenez, A.; Robledo, S. Antiprotozoal and cytotoxic activities in vitro of Colombian Annonaceae. J. Ethnopharmacol. 2007, 111, 630–635. [Google Scholar] [CrossRef]
- Roumy, V.; Garcia-Pizango, G.; Gutierrez-Choquevilca, A.L.; Ruiz, L.; Jullian, V.; Winterton, P.; Fabre, N.; Moulis, C.; Valentin, A. Amazonian plants from Peru used by Quechua and Mestizo to treat malaria with evaluation of their activity. J. Ethnopharmacol. 2007, 112, 482–489. [Google Scholar] [CrossRef]
- Muthaura, C.N.; Rukunga, G.M.; Chhabra, S.C.; Omar, S.A.; Guantai, A.N.; Gathirwa, J.W.; Tolo, F.M.; Mwitari, P.G.; Keter, L.K.; Kirira, P.G.; Kimani, C.W.; Mungai, G.M.; Njagi, E.N. Antimalarial activity of some plants traditionally used in treatment of malaria in Kwale district of Kenya. J. Ethnopharmacol. 2007, 112, 545–551. [Google Scholar] [CrossRef]
- Soh, P.N.; Benoit-Vical, F. Are West African plants a source of future antimalarial drugs? J. Ethnopharmacol. 2007, 114, 130–140. [Google Scholar] [CrossRef]
- Mesia, G.K.; Tona, G.L.; Nanga, T.H.; Cimanga, R.K.; Apers, S.; Cos, P.; Maes, L.; Pieters, L.; Vlietinck, A.J. Antiprotozoal and cytotoxic screening of 45 plant extracts from Democratic Republic of Congo. J. Ethnopharmacol. 2008, 115, 409–415. [Google Scholar] [CrossRef]
- Benoit-Vical, F.; Soh, P.N.; Salery, M.; Harguem, L.; Poupat, C.; Nongonierma, R. Evaluation of Senegalese plants used in malaria treatment: focus on Chrozophora senegalensis. J. Ethnopharmacol. 2008, 116, 43–48. [Google Scholar] [CrossRef]
- Kaou, A.M.; Mahiou-Leddet, V.; Hutter, S.; Ainouddine, S.; Hassani, S.; Yahaya, I.; Azas, N.; Ollivier, E. Antimalarial activity of crude extracts from nine African medicinal plants. J. Ethnopharmacol. 2008, 116, 74–83. [Google Scholar] [CrossRef]
- Bero, J.; Ganfon, H.; Jonville, M.C.; Frederich, M.; Gbaguidi, F.; DeMol, P.; Moudachirou, M.; Quetin-Leclercq, J. In vitro antiplasmodial activity of plants used in Benin in traditional medicine to treat malaria. J. Ethnopharmacol. 2009, 122, 439–444. [Google Scholar] [CrossRef]
- Celine, V.; Adriana, P.; Eric, D.; Joaquina, A.C.; Yannick, E.; Augusto, L.F.; Rosario, R.; Dionicia, G.; Michel, S.; Denis, C.; Genevieve, B. Medicinal plants from the Yanesha (Peru): evaluation of the leishmanicidal and antimalarial activity of selected extracts. J. Ethnopharmacol. 2009, 123, 413–422. [Google Scholar] [CrossRef]
- Wright, C.W. Plant derived antimalarials agents: new leads and challenges. Phytochem. Rev. 2005, 4, 55–61. [Google Scholar] [CrossRef]
- Hilou, A.; Nacoulma, O.G.; Guiguemde, T.R. In vivo antimalarial activities of extracts from Amaranthus spinosus L. and Boerhaavia erecta L. in mice. J. Ethnopharmacol. 2006, 103, 236–240. [Google Scholar] [CrossRef]
- Boyom, F.F.; Kemgne, E.M.; Tepongning, R.; Mbacham, W.F.; Tsamo, E.; Zollo, P.H.A.; Gut, J.; Rosenthal, P.J. Antiplasmodial activity of extracts from seven medicinal plants used in malaria treatment in Cameroon. J. Ethnopharmacol. 2009, 123, 483–488. [Google Scholar] [CrossRef]
- Jonville, M.C.; Kodja, H.; Humeau, L.; Fournel, J.; De Mol, P.; Cao, M.; Angenot, L.; Frederich, M. Screening of medicinal plants from Reunion Island for antimalarial and cytotoxic activity. J. Ethnopharmacol. 2008, 120, 382–386. [Google Scholar] [CrossRef]
- Esmaeili, S.; Naghibi, F.; Mosaddegh, M.; Sahranavard, S.; Ghafari, S.; Abdullah, N.R. Screening of antiplasmodial properties among some traditionally used Iranian plants. J. Ethnopharmacol. 2009, 121, 400–404. [Google Scholar] [CrossRef]
- Okokon, J.E.; Antia, B.S.; Igboasoiyi, A.C.; Essien, E.E.; Mbagwu, H.O. Evaluation of antiplasmodial activity of ethanolic seed extract of Picralima nitida. J Ethnopharmacol. 2007, 111, 464–467. [Google Scholar] [CrossRef]
- Abdel-Sattar, E.; Harraz, F.M.; Al-Ansari, S.M.; El-Mekkawy, S.; Ichino, C.; Kiyohara, H.; Otoguro, K.; Omura, S.; Yamada, H. Antiplasmodial and antitrypanosomal activity of plants from the Kingdom of Saudi Arabia. Nat. Med. (Tokyo) 2009, 63, 232–239. [Google Scholar]
- Tona, L.; Cimanga, R.K.; Mesia, K.; Musuamba, C.T.; De Bruyne, T.; Apers, S.; Hernans, N.; Van Miert, S.; Pieters, L.; Totté, J.; Vlietinck, A.J. In vitro antiplasmodial activity of extracts and fractions from seven medicinal plants used in the Democratic Republic of Congo. J. Ethnopharmacol. 2004, 93, 27–32. [Google Scholar] [CrossRef]
- Bah, S.; Jager, A.K.; Adsersen, A.; Diallo, D.; Paulsen, B.S. Antiplasmodial and GABA(A)-benzodiazepine receptor binding activities of five plants used in traditional medicine in Mali, West Africa. J. Ethnopharmacol. 2007, 110, 451–457. [Google Scholar] [CrossRef]
- Okokon, J.E.; Nwafor, P.A. Antiplasmodial activity of root extract and fractions of Croton zambesicus. J. Ethnopharmacol. 2009, 121, 74–78. [Google Scholar] [CrossRef]
- Lenta, B.N.; Vonthron-Senecheau, C.; Soh, R.F.; Tantangmo, F.; Ngouela, S.; Kaiser, M.; Tsamo, E.; Anton, R.; Weniger, B. In vitro antiprotozoal activities and cytotoxicity of some selected Cameroonian medicinal plants. J. Ethnopharmacol. 2007, 111, 8–12. [Google Scholar] [CrossRef]
- Waako, P.J.; Gumede, B.; Smith, P.; Folb, P.I. The in vitro and in vivo antimalarial activity of Cardiospermum halicacabum L. and Momordica foetida Schumch. Et Thonn. J. Ethnopharmacol. 2005, 99, 137–143. [Google Scholar] [CrossRef]
- Khaomek, P.; Ichino, C.; Ishiyama, A.; Sekiguchi, H.; Namatame, M.; Ruangrungsi, N.; Saifah, E.; Kiyohara, H.; Otoguro, K.; Omura, S.; Yamada, H. In vitro antimalarial activity of prenylated flavonoids from Erythrina fusca. J. Nat. Med. 2008, 62, 217–220. [Google Scholar] [CrossRef]
- Okokon, J.E.; Udokpoh, A.E.; Antia, B.S. Antimalaria activity of ethanolic extract of Tetrapleura tetraptera fruit. J. Ethnopharmacol. 2007, 111, 537–540. [Google Scholar] [CrossRef]
- Iwalewa, E.O.; Omisore, N.O.; Adewunmi, C.O.; Gbolade, A.A.; Ademowo, O.G. Anti-protozoan activities of Harungana madagascariensis stem bark extract on trichomonads and malaria. J. Ethnopharmacol. 2008, 117, 507–511. [Google Scholar] [CrossRef]
- Phillipe, G.; Angenot, L.; De Mol, P.; Goffin, E.; Hayette, M.P.; Tits, M.; Frédérich, M. In vitro screening of some Strychnos species for antiplasmodial activity. J. Ethnopharmacol. 2005, 97, 535–539. [Google Scholar] [CrossRef]
- Okokon, J.E.; Ita, B.N.; Udokpoh, A.E. Antiplasmodial activity of Cylicodiscus gabunensis. J. Ethnopharmacol. 2006, 107, 175–178. [Google Scholar] [CrossRef]
- Abosl, A.O.; Mbukwa, E.; Majinda, R.R.; Raserok, B.H.; Yenesew, A.; Midiwo, J.O.; Akala, H.; Liyala, P.; Waters, N.C. Vangueria infausta root bark: in vivo and in vitro antiplasmodial activity. Br. J. Biomed. Sci. 2006, 63, 129–133. [Google Scholar]
- Lategan, C.A.; Campbell, W.E.; Seaman, T.; Smith, P.J. The bioactivity of novel furanoterpenoids isolated from Siphonochilus aethiopicus. J. Ethnopharmacol. 2009, 121, 92–97. [Google Scholar] [CrossRef]
- Pedersen, M.M.; Chukwujekwu, J.C.; Lategan, C.A.; Staden, J.; Smith, P.J.; Staerk, D. Antimalarial sesquiterpene lactones from Distephanus angulifolius. Phytochemistry 2009, 70, 601–607. [Google Scholar] [CrossRef]
- Efange, S.M.; Brun, R.; Wittlin, S.; Connolly, J.D.; Hoye, T.R.; McAkam, T.; Makolo, F.L.; Mbah, J.A.; Nelson, D.P.; Nyongbela, K.D.; Wirmum, C.K. Okundoperoxide, a bicyclic cyclo-farnesylsesquiterpene endoperoxide from Scleria striatinux with antiplasmodial activity. J. Nat. Prod. 2009, 72, 280–283. [Google Scholar] [CrossRef]
- Murata, T.; Miyase, T.; Muregi, F.W.; Naoshima-Ishibashi, Y.; Umehara, K.; Warashina, T.; Kanou, S.; Mkoji, G.M.; Terada, M.; Ishih, A. Antiplasmodial triterpenoids from Ekebergia capensis. J. Nat. Prod. 2008, 71, 167–174. [Google Scholar] [CrossRef]
- Jonville, M.C.; Capel, M.; Frederich, M.; Angenot, Luc; Dive, G.; Faure, R.; Azas, N.; Ollivier, E. Fagraldehyde, a secoiridoid isolated from Fagraea fragrans. J. Nat. Prod. 2008, 71, 2038–2040. [Google Scholar] [CrossRef]
- Adelekan, A.M.; Prozesky, E.A.; Hussein, A.A.; Urena, L.D.; van Rooyen, P.H.; Liles, D.C.; Meyer, J.J.; Rodriguez, B. Bioactive diterpenes and other constituents of Croton steenkampianus. J. Nat. Prod. 2008, 71, 1919–1922. [Google Scholar] [CrossRef]
- Matsuno, Y.; Deguchi, J.; Hirasawa, Y.; Ohyama, K.; Toyoda, H.; Hirobe, C.; Ekasari, W.; Widyawaruyanti, A.; Zaini, N.C.; Morita, H. Sucutiniranes A and B, new cassane-type diterpenes from Bowdichia nitida. Bioorg. Med. Chem. Lett. 2008, 18, 3774–3777. [Google Scholar] [CrossRef]
- Kamatou, G.P.P.; Van Zyl, R.L.; Davids, H.; Heerden, F.R.V.; Lourens, A.C.U.; Viljoen, A.M. Antimalarial and anticancer activities of selected South African Salvia species and isolated compounds from S. radula. S. Afr. J. Bot. 2008, 74, 238–243. [Google Scholar] [CrossRef]
- Chukwujekwu, J.C.; Lategan, C.A.; Smith, P.J.; Van Heerden, F.R.; Van Staden, J. Antiplasmodial and cytotoxic activity of isolated sesquiterpene lactones from the acetone leaf extract of Vernonia colorata. S. Afr. J. Bot. 2009, 75, 176–179. [Google Scholar]
- Olagnier, D.; Costes, P.; Berry, A.; Linas, M.D.; Urrutigoity, M.; Dechy-Cabaret, O.; Benoit-Vical, F. Modifications of the chemical structure of terpenes in antiplasmodial and antifungal drug research. Bioorg. Med. Chem. Lett. 2007, 17, 6075–6078. [Google Scholar] [CrossRef]
- Ngouamegne, E.T.; Fongang, R.S.; Ngouela, S.; Boyom, F.F.; Rohmer, M.; Tsamo, E.; Gut, J.; Rosenthal, P.J. Endodesmiadiol, a friedelane triterpenoid, and other antiplasmodial compounds from Endodesmia calophylloides. Chem. Pharm. Bull. (Tokyo) 2008, 56, 374–377. [Google Scholar] [CrossRef]
- Moon, H.I. Antiplasmodial activity of ineupatorolides A from Carpesium rosulatum. Parasitol. Res. 2007, 100, 1147–1149. [Google Scholar] [CrossRef]
- Chung, I.M.; Kim, M.Y.; Moon, H.I. Antiplasmodial activity of sesquiterpene lactone from Carpesium rosulatum in mice. Parasitol. Res. 2008, 103, 341–344. [Google Scholar] [CrossRef]
- de Sa, M.S.; Costa, J.F.; Krettli, A.U.; Zalis, M.G.; Maia, G.L.; Sette, I.M.; Camara, C.D.; Filho, J.M.; Giulietti-Harley, A.M.; Ribeiro Dos Santos, R.; Soares, M.B. Antimalarial activity of betulinic acid and derivatives in vitro against Plasmodium falciparum and in vivo in P. berghei-infected mice. Parasitol. Res. 2009, 105, 275–279. [Google Scholar] [CrossRef]
- Ortet, R.; Prado, S.; Mouray, E.; Thomas, O.P. Sesquiterpene lactones from the endemic Cape Verdean Artemisia gorgonum. Phytochemistry 2008, 69, 2961–2965. [Google Scholar] [CrossRef]
- Afolayan, A.F.; Mann, M.G.; Lategan, C.A.; Smith, P.J.; Bolton, J.J.; Beukes, D.R. Antiplasmodial halogenated monoterpenes from the marine red alga Plocamium cornutum. Phytochemistry 2009, 70, 597–600. [Google Scholar] [CrossRef]
- Zhang, H.; Wang, X.; Chen, F.; Androulakis, X.M.; Wargovich, M.J. Anticancer activity of limonoid from Khaya senegalensis. Phytother. Res. 2007, 21, 731–734. [Google Scholar] [CrossRef]
- Roy, A.; Saraf, S. Limonoids: Overview of significant bioactive triterpenes distributed in plant kingdom. Biol. Pharm. Bull. 2006, 29, 191–201. [Google Scholar] [CrossRef]
- Mohamad, K.; Hirasawa, Y.; Litaudon, M.; Awang, K.; Hadi, A.H.; Takeya, K.; Ekasari, W.; Widyawaruyanti, A.; Zaini, N.C.; Morita, H. Ceramicines B-D, new antiplasmodial limonoids from Chisocheton ceramicus. Bioorg Med Chem 2009, 17, 727–730. [Google Scholar] [CrossRef]
- Banzouzi, J.T.; Soh, P.N.; Mbatchi, B.; Cave, A.; Ramos, S.; Retailleau, P.; Rakotonandrasana, O.; Berry, A.; Benoit-Vical, F. Cogniauxia podolaena: bioassay-guided fractionation of defoliated stems, isolation of active compounds, antiplasmodial activity and cytotoxicity. Planta Med. 2008, 74, 1453–1456. [Google Scholar] [CrossRef]
- Muiva, L.M.; Yenesew, A.; Derese, S.; Heydenreich, M.; Peter, M.G.; Akala, H.M.; Eyase, F.; Waters, N.C.; Mutai, C.; Keriko, J.M.; Walsh, D. Antiplasmodial β-hydroxydihydrochalcone from seedpods of Tephrosia elata. Phytochem. Lett. 2009, in press. [Google Scholar] [CrossRef]
- Kunert, O.; Swamy, R.C.; Kaiser, M.; Presser, A.; Buzzi, S.; Appa-Rao, A.V.N.; Shuhly, W. Antiplasmodial and leishmanicidal activity of biflavonoids from Indian Selaginella bryopteris. Phytochem. Lett. 2008, 1, 171–174. [Google Scholar] [CrossRef]
- Oshimi, S.; Tomizawa, Y.; Hirasawa, Y.; Honda, T.; Ekasari, W.; Widyawaruyanti, A.; Rudyanto, M.; Indrayanto, G.; Zaini, N.C.; Morita, H. Chrobisiamone A, a new bischromone from Cassia siamea and a biomimetic transformation of 5-acetonyl-7-hydroxy-2-methylchromone into cassiarin A. Bioorg. Med. Chem. Lett. 2008, 18, 3761–3763. [Google Scholar] [CrossRef]
- Zelefack, F.; Guilet, D.; Fabre, N.; Bayet, C.; Chevalley, S.; Ngouela, S.; Lenta, B.N.; Valentin, A.; Tsamo, E.; Dijoux-Franca, M.G. Cytotoxic and antiplasmodial xanthones from Pentadesma butyracea. J. Nat. Prod. 2009, 72, 954–957. [Google Scholar] [CrossRef]
- Martin, F.; Hay, A.E.; Cressende, D.; Reist, M.; Vivas, L.; Gupta, M.P.; Carrupt, P.A.; Hostettmann, K. Antioxidant c-glucosylxanthones from the leaves of Arrabidaea patellifera. J. Nat. Prod. 2008, 71, 1887–1890. [Google Scholar] [CrossRef]
- Hou, Y.; Cao, S.; Brodie, P.J.; Callmander, M.W.; Ratovoson, F.; Rakotobe, E.A.; Rasamison, V.E.; Ratsimbason, M.; Alumasa, J.N.; Roepe, P.D.; Kingston, D.G. Antiproliferative and antimalarial anthraquinones of Scutia myrtina from the Madagascar forest. Bioorg. Med. Chem. 2009, 17, 2871–2876. [Google Scholar] [CrossRef]
- Ziegler, H.L.; Hansen, H.S.; Staerk, D.; Christensen, S.B.; Hägerstrand, H.; Jaroszewski, J.W. The antiparasitic compound licochalcone A is a potent echinocytogenic agent that modifies the erythrocyte membrane in the concentration range where antiplasmodial activity is observed. Antimicrob. Agents Chemother. 2004, 48, 4067–4071. [Google Scholar] [CrossRef]
- Mishra, L.C.; Bhattacharya, A.; Bhasin, V.K. Phytochemical licochalcone A enhances antimalarial activity of artemisinin in vitro. Acta Trop. 2009, 109, 194–198. [Google Scholar] [CrossRef]
- Lehane, A.M.; Saliba, K.J. Common dietary flavonoids inhibit the growth of the intraerythrocytic malaria parasite. BMC Res. Notes 2008, 1, 26. [Google Scholar] [CrossRef]
- Moein, M.R.; Pawar, R.S.; Khan, S.I.; Tekwani, B.L.; Khan, I.A. Antileishmanial, antiplasmodial and cytotoxic activities of 12,16-dideoxy aegyptinone B from Zhumeria majdae Rech.f. & Wendelbo. Phytother. Res. 2008, 22, 283–285. [Google Scholar] [CrossRef]
- Ajaiyeoba, E.O.; Oladepo, O.; Fawole, O.I.; Bolaji, O.M.; Akinboye, D.O.; Ogundahunsi, O.A.T.; Falade, C.O.; Gbotosho, G.O.; Itiola, O.A.; Happi, T.C.; Ebong, O.O.; Ononiwu, I.M.; Osowole, O.S.; Oduola, O.O.; Ashidi, J.S.; Oduola, A.M.J. Cultural categorization of febrile illnesses in correlation with herbal remedies for treatment in Southwestern Nigeria. J. Ethnopharmacol. 2003, 85, 179–185. [Google Scholar] [CrossRef]
- Ajaiyeoba, E.O.; Bolaji, O.M.; Akinboye, D.O.; Falade, C.O.; Gbotosho, G.O.; Ashidi, J.S.; Okpako, L.C.; Oduola, O.O.; Falade, M.O.; Itiola, O.A.; Houghton, P.J.; Wright, C.W.; Ogundahunsi, O.A.; Oduola, A.M.J. In vitro antiplasmodial and cytotoxic activities of plants used as antimalarial agents in the southwest Nigerian ethnomedicine. J. Nat. Rem. 2005, 5, 1–6. [Google Scholar]
- Ajaiyeoba, E.O.; Ashidi, J.S.; Okpako, L.C.; Houghton, P.J.; Wright, C.W. Antiplasmodial compounds from Cassia siamea stem bark extract. Phytother. Res. 2008, 22, 254–255. [Google Scholar] [CrossRef]
- Ramanandraibe, V.; Grellier, P.; Martin, M.T.; Deville, A.; Joyeau, R.; Ramanitrahasimbola, D.; Mouray, E.; Rasoanaivo, P.; Mambu, L. Antiplasmodial phenolic compounds from Piptadenia pervillei. Planta Med. 2008, 74, 417–421. [Google Scholar] [CrossRef]
- Roumy, V.; Fabre, N.; Portet, B.; Bourdy, G.; Acebey, L.; Vigor, C.; Valentin, A.; Moulis, C. Four anti-protozoal and anti-bacterial compounds from Tapirira guianensis. Phytochemistry 2009, 70, 305–311. [Google Scholar] [CrossRef]
- Flores, N.; Jimenez, I.A.; Gimenez, A.; Ruiz, G.; Gutierrez, D.; Bourdy, G.; Bazzocchi, I.L. Benzoic acid derivatives from Piper species and their antiparasitic activity. J. Nat. Prod. 2008, 71, 1538–1543. [Google Scholar] [CrossRef]
- Marti, G.; Eparvier, V.; Moretti, C.; Susplugas, S.; Prado, S.; Grellier, P.; Retailleau, P.; Guéritte, F.; Litaudon, M. Antiplasmodial benzophenones from the trunk latex of Moronobea coccinea (Clusiaceae). Phytochemistry 2009, 70, 75–85. [Google Scholar] [CrossRef]
- Tasdemir, D.; Brun, R.; Franzblau, S.G.; Sezgin, Y.; Çalis, I. Evaluation of antiprotozoal and antimycobacterial activities of the resin glycosides and the other metabolites of Scrophularia cryptophila. Phytomedicine 2008, 15, 209–215. [Google Scholar] [CrossRef]
- Flores, N.; Jimenez, I.A.; Gimenez, A.; Ruiz, G.; Gutierrez, D.; Bourdy, G.; Bazzocchi, I.L. Antiparasitic activity of prenylated benzoic acid derivatives from Piper species. Phytochemistry 2009, 70, 621–627. [Google Scholar] [CrossRef]
- de Andrade-Neto, V.F.; da Silva, T.; Lopes, L.M.; do Rosario, V.E.; de Pilla Varotti, F.; Krettli, A.U. Antiplasmodial activity of aryltetralone lignans from Holostylis reniformis. Antimicrob. Agents Chemother. 2007, 51, 2346–2350. [Google Scholar] [CrossRef]
- Lee, S.J.; Park, W.H.; Moon, H.I. Bioassay-guided isolation of antiplasmodial anacardic acids derivatives from the whole plants of Viola websteri Hemsl. Parasitol. Res. 2009, 104, 463–466. [Google Scholar] [CrossRef]
- Abrantes, M.; Mil-Homens, T.; Duarte, N.; Lopes, D.; Cravo, P.; Madureira, M.; Ferreira, M.J. Antiplasmodial activity of lignans and extracts from Pycnanthus angolensis. Planta Med. 2008, 74, 1408–1412. [Google Scholar] [CrossRef]
- Willcox, M.L.; Bodeker, G. Traditional herbal medicines for malaria. Brit. Med. J. 2004, 329, 1156–1159. [Google Scholar] [CrossRef]
- Harborne, J.B. Twenty-five years of chemical ecology. Nat. Prod. Rep. 2001, 18, 361–379. [Google Scholar]
© 2009 by the authors; licensee Molecular Diversity Preservation International, Basel, Switzerland. This article is an open-access article distributed under the terms and conditions of the Creative Commons Attribution license ( http://creativecommons.org/licenses/by/3.0/).