The Increased Dissolution and Oral Absorption of Itraconazole by Nanocrystals with an Endogenous Small-Molecule Surfactant as a Stabilizer
Abstract
1. Introduction
2. Results and Discussion
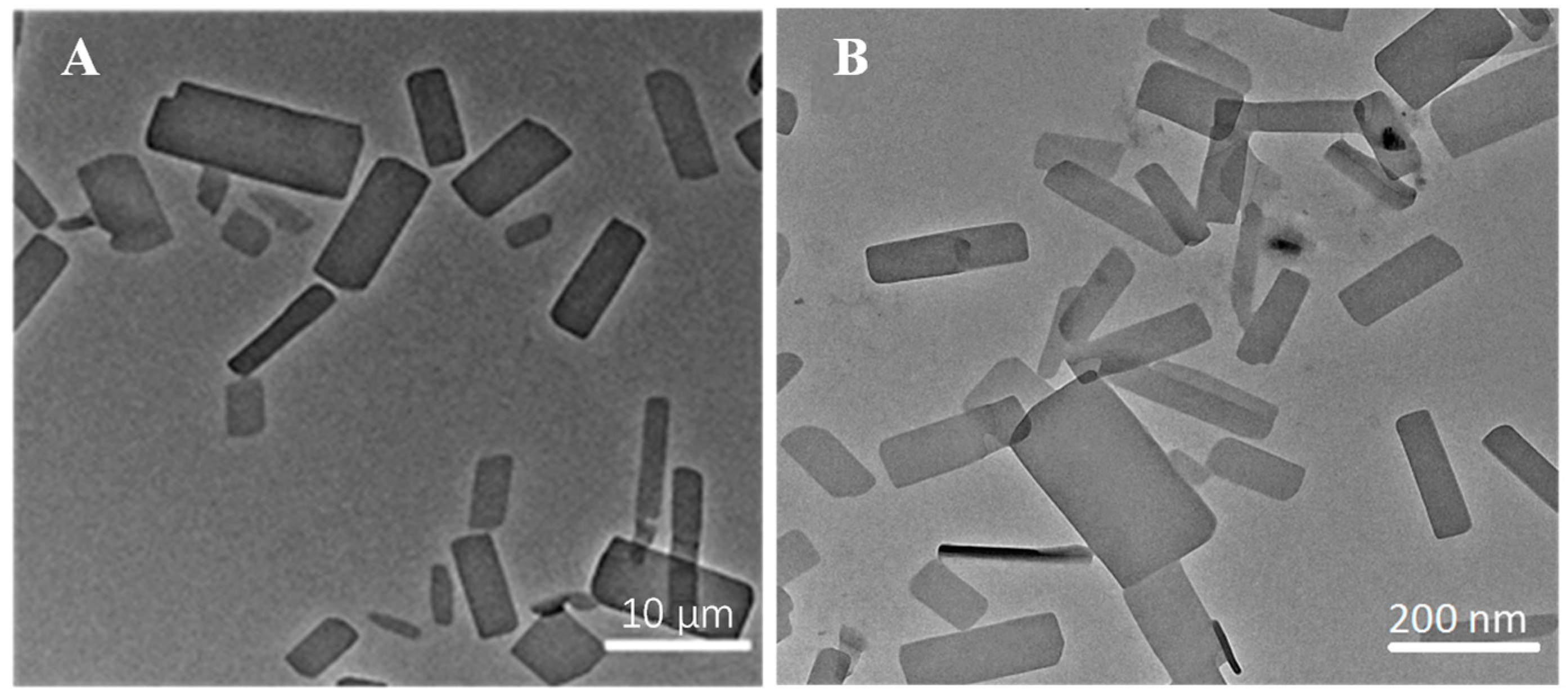
2.1. Preparation and Characterization of the ITZ-Nanos
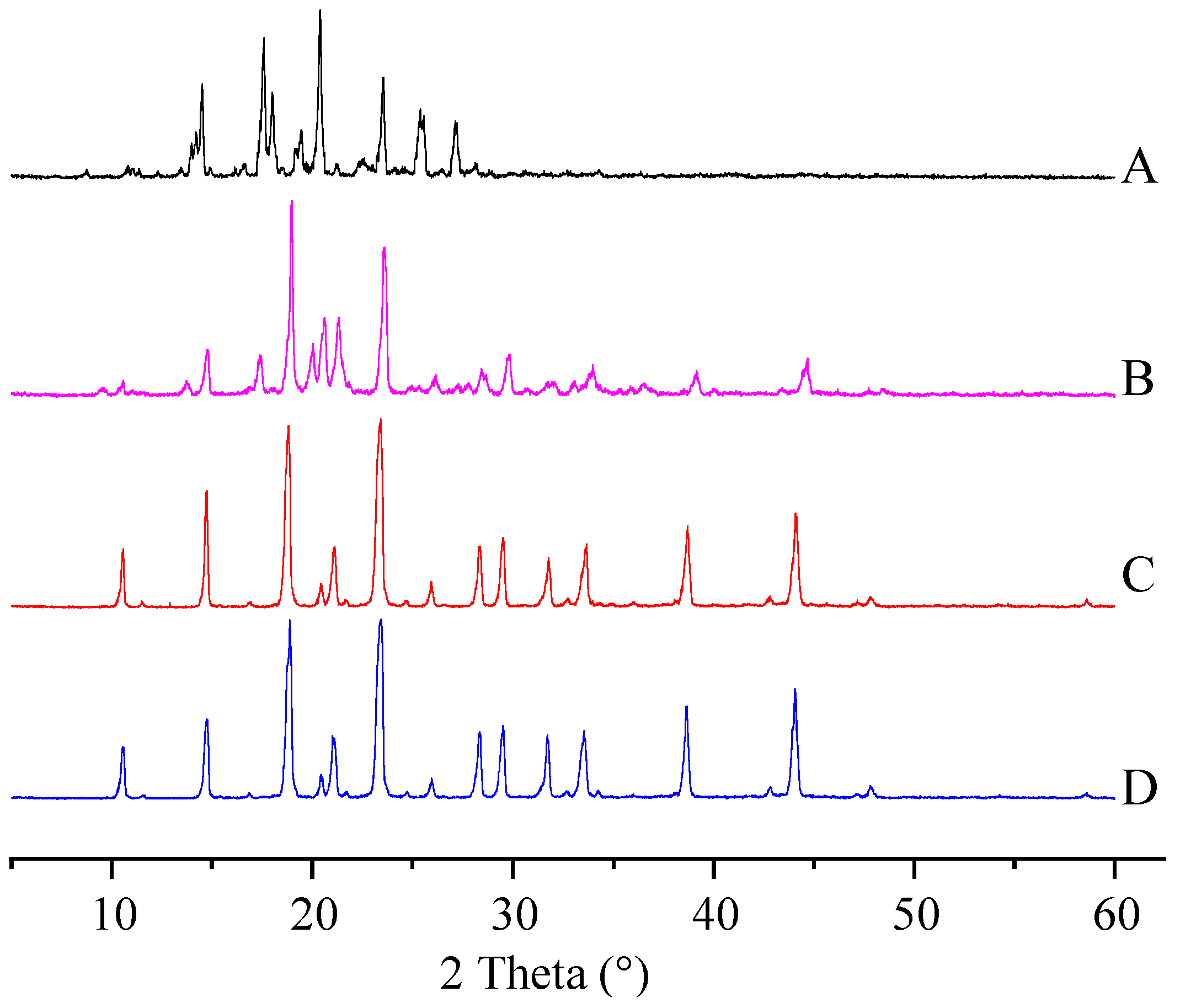
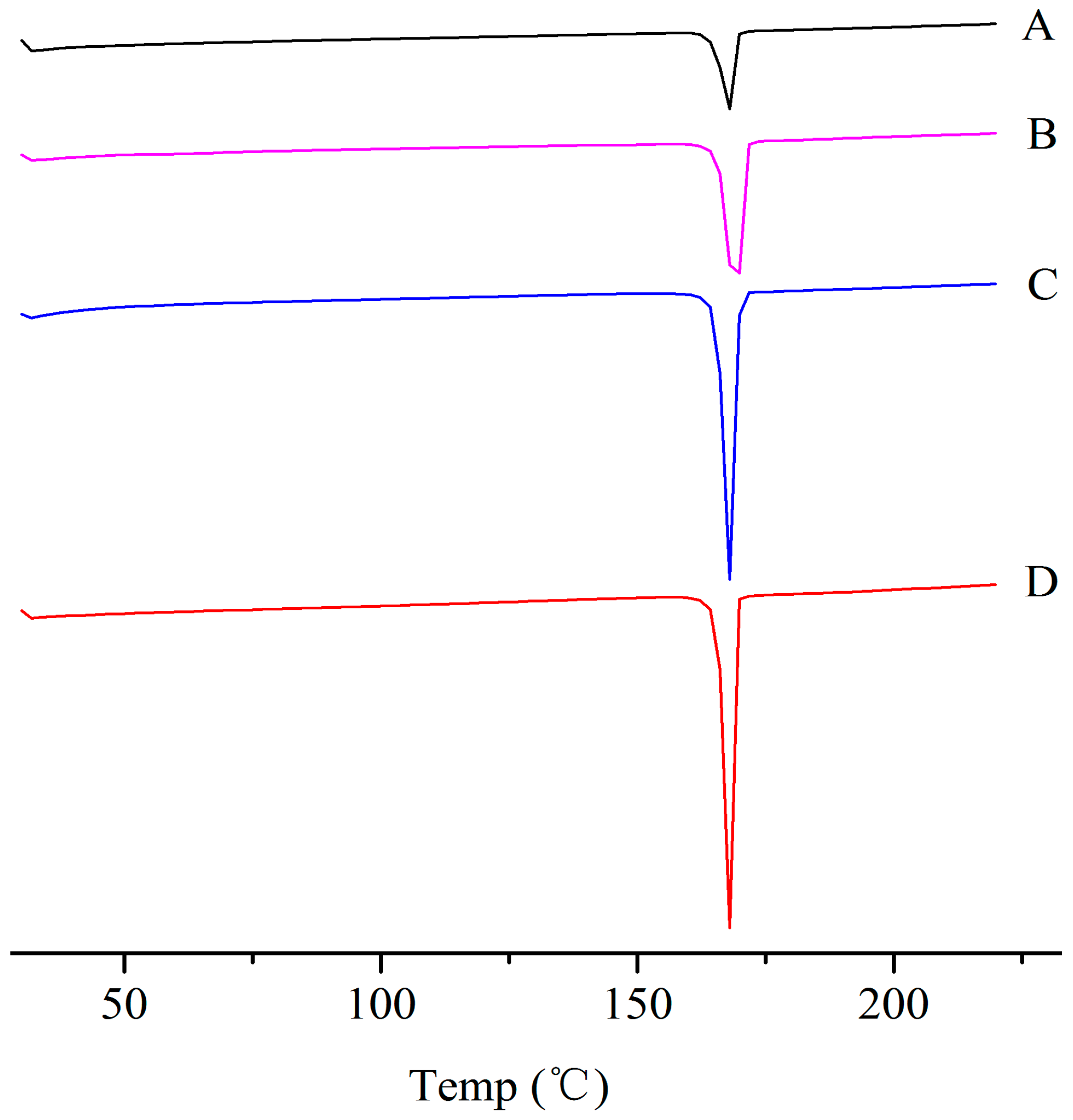
2.2. Crystalline State of the ITZ-Nanos
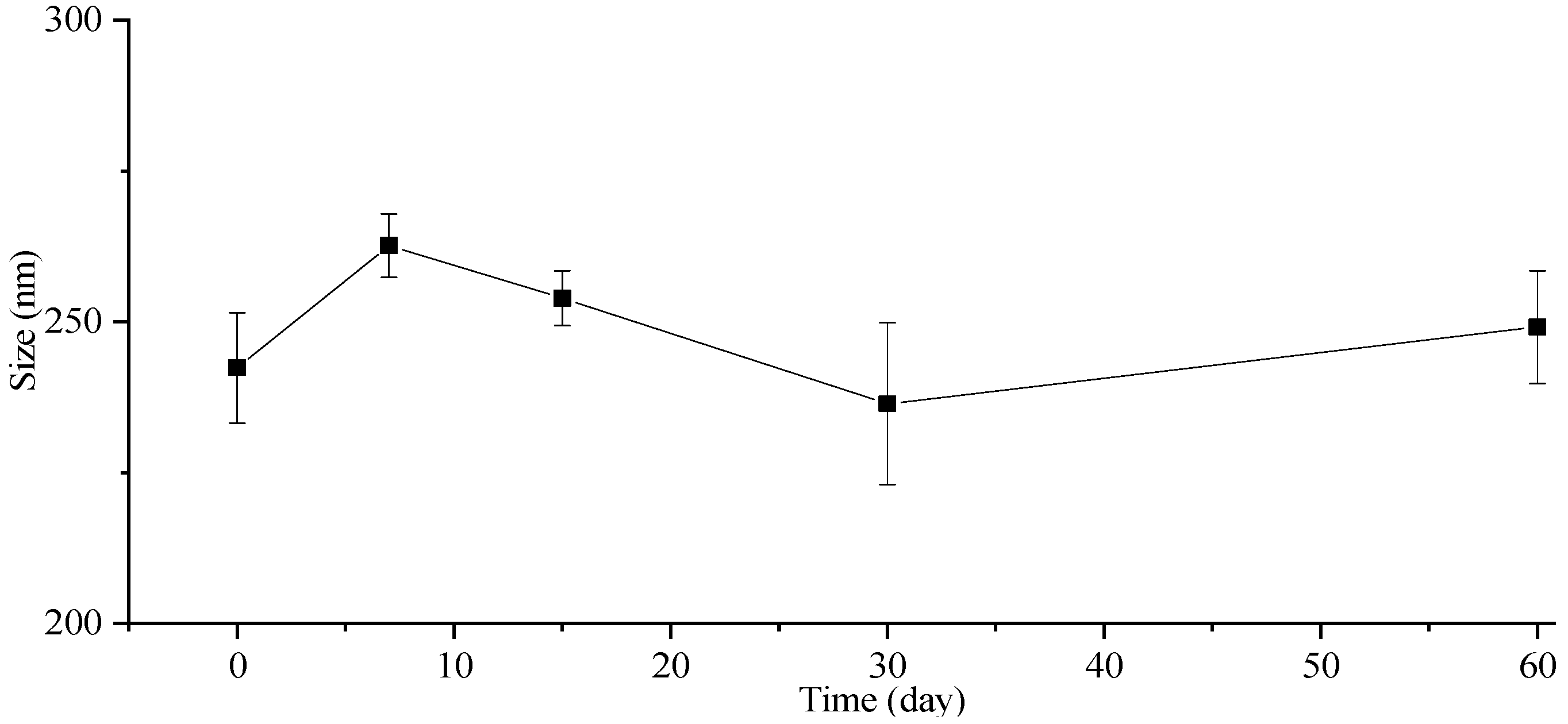
2.3. Stability Study
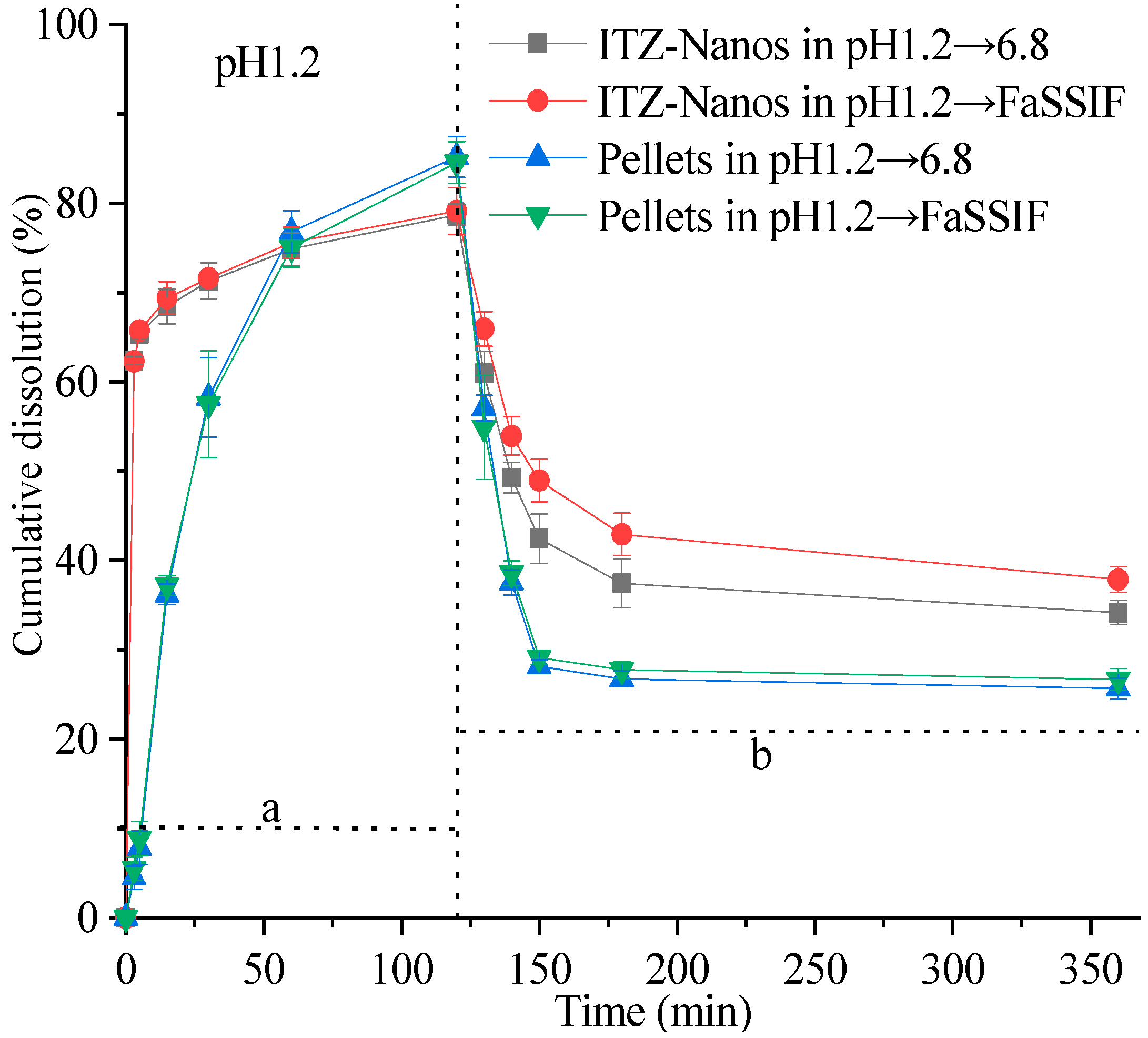
2.4. In Vitro Dissolution under Supersaturating Conditions
2.5. Uptake of ITZ by Caco-2 Cells
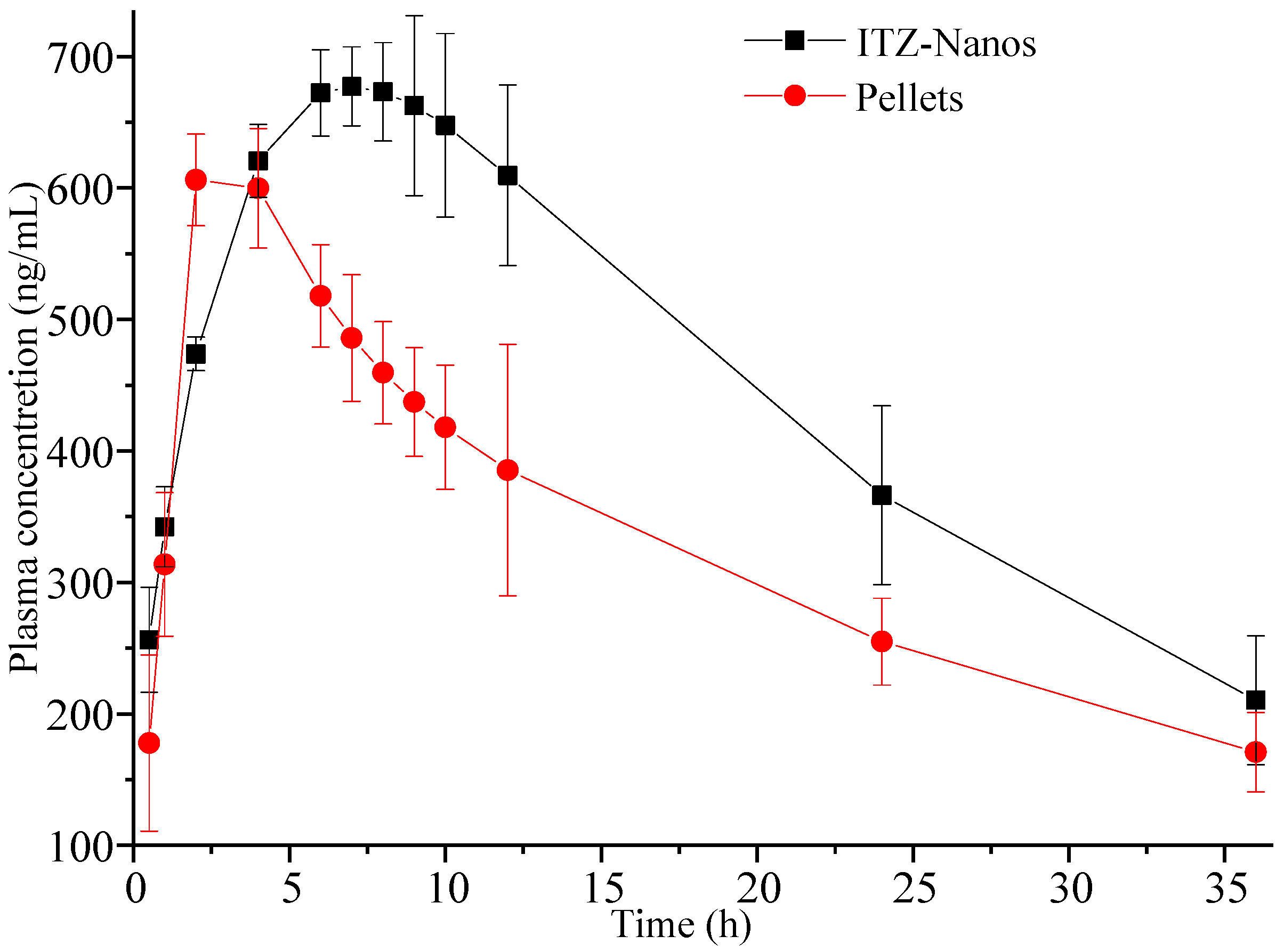
2.6. In Vivo Pharmacokinetics in Rats
3. Materials and Methods
3.1. Preparation of the ITZ-Nanos
3.2. Particle Size Analysis
3.3. Transmission Electron Microscopy
3.4. X-ray Diffraction (XRPD) Measurements
3.5. Differential Scanning Calorimetry
3.6. Supersaturated Dissolution
3.7. Particle Size Stability
3.8. In Vitro Uptake across the Caco-2 Monolayer
3.8.1. Caco-2 Culture
3.8.2. Uptake of ITZ by the Caco-2 Cells
3.9. The In Vivo Pharmacokinetic Study in Rats
3.10. HPLC Analysis
3.11. Data Analysis
4. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Siscar-Lewin, S.; Hube, B.; Brunke, S. Emergence and evolution of virulence in human pathogenic fungi. Trends. Microbiol. 2022, 30, 693–704. [Google Scholar] [CrossRef] [PubMed]
- WHO. WHO Fungal Priority Pathogens List to Guide Research, Development and Public Health Action; WHO: Geneva, Switzerland, 2022. [Google Scholar]
- Janssens, S.; de Armas, H.N.; Remon, J.P.; Van den Mooter, G. The use of a new hydrophilic polymer, Kollicoat IR (R), in the formulation of solid dispersions of Itraconazole. Eur. J. Pharm. Sci. 2007, 30, 288–294. [Google Scholar] [CrossRef] [PubMed]
- Peeters, J.; Neeskens, P.; Tollenaere, J.P.; Van Remoortere, P.; Brewster, M.E. Characterization of the interaction of 2-hydroxypropyl-beta-cyclodextrin with itraconazole at pH 2, 4, and 7. J. Pharm. Sci. 2002, 91, 1414–1422. [Google Scholar] [CrossRef] [PubMed]
- Zong, L.; Li, X.; Wang, H.; Cao, Y.; Yin, L.; Li, M.; Wei, Z.; Chen, D.; Pu, X.; Han, J. Formulation and characterization of biocompatible and stable I.V. itraconazole nanosuspensions stabilized by a new stabilizer polyethylene glycol-poly(beta-Benzyl-l-aspartate) (PEG-PBLA). Int. J. Pharm. 2017, 531, 108–117. [Google Scholar] [CrossRef] [PubMed]
- Yin, Y.J.; Deng, H.L.; Wu, K.; He, B.; Dai, W.B.; Zhang, H.; Fu, J.J.; Le, Y.; Wang, X.Q.; Zhang, Q. A multiaspect study on transcytosis mechanism of sorafenib nanogranules engineered by high-gravity antisolvent precipitation. J. Control. Release 2020, 323, 600–612. [Google Scholar] [CrossRef] [PubMed]
- Li, J.W.; Fu, Q.; Liu, X.H.; Li, M.; Wang, Y.J. Formulation of nimodipine nanocrystals for oral administration. Formulation of nimodipine nanocrystals for oral administration. Arch. Pharm. Res. 2016, 39, 202–212. [Google Scholar] [CrossRef] [PubMed]
- Hong, J.Y.; Kim, J.K.; Song, Y.K.; Park, J.S.; Kim, C.K. A new self-emulsifying formulation of itraconazole with improved dissolution and oral absorption. J. Control. Release 2006, 110, 332–338. [Google Scholar] [CrossRef] [PubMed]
- Hassan, A.; Tang, Y.M.; Ayres, J.W. Itraconazole formation using supercritical carbon dioxide. Drug Dev. Ind. Pharm. 2004, 30, 1029–1035. [Google Scholar] [CrossRef]
- Vaughn, J.M.; Gao, X.; Yacaman, M.J.; Johnston, K.P.; Williams, W.R.O. Comparison of powder produced by evaporative precipitation into aqueous solution (EPAS) and spray freezing into liquid (SFL) technologies using novel Z-contrast STEM and complimentary techniques. Eur. J. Pharm. Biopharm. 2005, 60, 81–89. [Google Scholar] [CrossRef]
- Six, K.; Leuner, C.; Dressman, J.; Verreck, G.; Peeters, J.; Blaton, N.; Augustijns, P.; Kinget, R.; Van den Mooter, G. Thermal properties of hot-stage extrudates of itraconazole and eudragit E100—Phase separation and polymorphism. J. Therm. Anal. Calorim. 2002, 68, 591–601. [Google Scholar] [CrossRef]
- Six, K.; Daems, T.; de Hoon, J.; Van Hecken, A.; Depre, M.; Bouche, M.P.; Prinsen, P.; Verreck, G.; Peeters, J.; Brewster, M.E.; et al. Clinical study of solid dispersions of itraconazole prepared by hot-stage extrusion. Eur. J. Pharm. Sci. 2005, 24, 179–186. [Google Scholar] [CrossRef] [PubMed]
- Yoo, S.D.; Lee, S.H.; Kang, E.; Jun, H.; Jung, J.Y.; Park, J.W.; Lee, K.H. Bioavailability of itraconazole in rats and rabbits after administration of tablets containing solid dispersion particles. Drug Dev. Ind. Pharm. 2000, 26, 27–34. [Google Scholar] [CrossRef] [PubMed]
- Parikh, T.; Sandhu, H.K.; Talele, T.T.; Serajuddin, A.T. Characterization of Solid Dispersion of Itraconazole Prepared by Solubilization in Concentrated Aqueous Solutions of Weak Organic Acids and Drying. Pharm. Res. 2016, 33, 1456–1471. [Google Scholar] [CrossRef] [PubMed]
- Rahman, M.; Radgman, K.; Tarabokija, J.; Ahmad, S.; Bilgili, E. Preparation and Characterization of Spray-Dried Hybrid Nanocrystal-Amorphous Solid Dispersions (HyNASDs) for Supersaturation Enhancement of a Slowly Crystallizing Drug. Nanomaterials. 2023, 13, 2419. [Google Scholar] [CrossRef] [PubMed]
- Kumar, S.; Jog, R.; Shen, J.; Zolnik, B.; Sadrieh, N.; Burgess, D.J. In Vitro and In Vivo Performance of Different Sized Spray-Dried Crystalline Itraconazole. J. Pharm. Sci. 2015, 104, 3018–3028. [Google Scholar] [CrossRef] [PubMed]
- Wlaz, P.; Knaga, S.; Kasperek, K.; Wlaz, A.; Poleszak, E.; Jezewska-Witkowska, G.; Winiarczyk, S.; Wyska, E.; Heinekamp, T.; Rundfeldt, C. Activity and Safety of Inhaled Itraconazole Nanosuspension in a Model Pulmonary Aspergillus fumigatus Infection in Inoculated Young Quails. Mycopathologia. 2015, 180, 35–42. [Google Scholar] [CrossRef] [PubMed]
- Han, X.; Wang, M.; Ma, Z.; Xue, P.; Wang, Y. A new approach to produce drug nanosuspensions CO2-assisted effervescence to produce drug nanosuspensions. Colloids Surf. B 2016, 143, 107–110. [Google Scholar] [CrossRef] [PubMed]
- Karagianni, A.; Peltonen, L. Production of Itraconazole Nanocrystal-Based Polymeric Film Formulations for Immediate Drug Release. Pharmaceutics. 2020, 12, 960. [Google Scholar] [CrossRef]
- Czyz, S.; Wewers, M.; Finke, J.H.; Kwade, A.; van Eerdenbrugh, B.; Juhnke, M.; Bunjes, H. Spray drying of API nanosuspensions: Importance of drying temperature, type and content of matrix former and particle size for successful formulation and process development. Eur. J. Pharm. Biopharm. 2020, 152, 63–71. [Google Scholar] [CrossRef]
- Le Devedec, F.; Strandman, S.; Hildgen, P.; Leclair, G.; Zhu, X.X. PEGylated bile acids for use in drug delivery systems: Enhanced solubility and bioavailability of itraconazole. Mol. Pharm. 2013, 10, 3057–3066. [Google Scholar] [CrossRef]
- Kocbek, P.; Baumgartner, S.; Kristl, J. Preparation and evaluation of nanosuspensions for enhancing the dissolution of poorly soluble drugs. Int. J. Pharma. 2006, 312, 179–186. [Google Scholar] [CrossRef] [PubMed]
- Sarnes, A.; Kovalainen, M.; Hakkinen, M.R.; Laaksonen, T.; Laru, J.; Kiesvaara, J.; Ilkka, J.; Oksala, O.; Rönkkö, S.; Jarvinen, K.; et al. Nanocrystal-based per-oral itraconazole delivery: Superior in vitro dissolution enhancement versus Sporanox® is not realized in in vivo drug absorption. J. Control. Release 2014, 180, 109–116. [Google Scholar] [CrossRef] [PubMed]
- Ikegawa, S.; Okuyama, H.; Oohashi, J.; Murao, N.; Goto, J. Separation and Detection of Bile Acid 24-Glucuronides in Human Urine by Liquid Chromatography Combined with Electrospray Ionization Mass Spectrometry. Anal. Sci. 2005, 15, 625–631. [Google Scholar] [CrossRef][Green Version]
- Vijayalakshmi, N.; Maitra, U. A simple construction of a bile acid based dendritic light harvesting system. Org. Lett. 2005, 7, 2727–2730. [Google Scholar] [CrossRef]
- Kong, W.J.; Wang, J.B.; Xing, X.Y.; Xiao, X.H.; Zhao, Y.L.; Zang, Q.C.; Zhang, P.; Jin, C.; Li, Z.L.; Liu, W. Antifungal evaluation of cholic acid and its derivatives on Candida albicans by microcalorimetry and chemometrics. Anal. Chim. Acta. 2011, 689, 250–256. [Google Scholar] [CrossRef] [PubMed]
- Ghosh, I.; Schenck, D.; Bose, S.; Ruegger, C. Optimization of formulation and process parameters for the production of nanosuspension by wet media milling technique: Effect of Vitamin E TPGS and nanocrystal particle size on oral absorption. Eur. J. Pharm. Sci. 2012, 47, 718–728. [Google Scholar] [CrossRef]
- Singh, S.K.; Srinivasan, K.K.; Gowthamarajan, K.; Singare, D.S.; Prakash, D.; Gaikwad, N.B. Investigation of preparation parameters of nanosuspension by top-down media milling to improve the dissolution of poorly water-soluble glyburide. Eur. J. Pharm. Biopharm. 2011, 78, 441–446. [Google Scholar] [CrossRef]
- Wang, Y.; Zheng, Y.; Zhang, L.; Wang, Q.; Zhang, D. Stability of nanosuspensions in drug delivery. J. Control. Release 2013, 172, 1126–1141. [Google Scholar] [CrossRef] [PubMed]
- Du, J.; Zong, L.L.; Li, M.M.; Yu, K.K.; Qiao, Y.H.; Yuan, Q.; Pu, X.H. Two-pronged anti-tumor therapy by a new polymer paclitaxel Conjugate Micelle with an Anti-Multidrug Resistance Effect. Int. J. Nanomed. 2022, 17, 1323–1341. [Google Scholar] [CrossRef]
- Luo, J.; Giguere, G.; Zhu, X.X. Asymmetric poly(ethylene glycol) star polymers with a cholic acid core and their aggregation properties. Biomacromolecules 2009, 10, 900–906. [Google Scholar] [CrossRef]
- Li, C.C.; Wang, G.J.; Gao, H.Y.; Zhai, M.L.; Li, J.Q. Temperature-, pH-, and Ion- Stimulus- Responsive Swelling Behaviors of Poly( dimethylaminoethyl methacrylate) Gel Containing Cholic Acid. J. Appl. Polym. Sci. 2014, 131, 596–602. [Google Scholar] [CrossRef]
- Sonje, J.; Thakral, S.; Suryanarayanan, R. t-Butanol Enables Dual Functionality of Mannitol: A Cryoprotectant in Frozen Systems and Bulking Agent in Freeze-Dried Formulations. Mol. Pharm. 2020, 17, 3075–3086. [Google Scholar] [CrossRef] [PubMed]
- Chen, J.; Mosquera-Giraldo, L.I.; Ormes, J.D.; Higgins, J.D.; Taylor, L.S. Bile Salts as Crystallization Inhibitors of Supersaturated Solutions of Poorly Water-Soluble Compounds. Cryst. Growth Des. 2015, 15, 2593–2597. [Google Scholar] [CrossRef]
- Tan, E.H.; Parmentier, J.; Low, A.; Moschwitzer, J.P. Downstream drug product processing of itraconazole nanosuspension: Factors influencing tablet material properties and dissolution of compacted nanosuspension-layered sugar beads. Int. J. Pharma. 2017, 532, 131–138. [Google Scholar] [CrossRef] [PubMed]
- Shi, X.; Fan, N.; Zhang, G.; Sun, J.; He, Z.; Li, J. Quercetin amorphous solid dispersions prepared by hot melt extrusion with enhanced solubility and intestinal absorption. Pharm. Dev. Technol. 2020, 25, 472–481. [Google Scholar] [CrossRef] [PubMed]
- Pu, X.H.; Sun, J.; Han, J.H.; Lian, H.; Zhang, P.; Yan, Z.T.; He, Z.G. Nanosuspensions of 10-hydroxycamptothecin that can maintain high and extended supersaturation to enhance oral absorption: Preparation, characterization and in vitro/in vivo evaluation. J. Nanoparticle Res. 2013, 15, 2043–2055. [Google Scholar] [CrossRef]
- Lian, H.; Zhang, T.; Sun, J.; Pu, X.; Tang, Y.; Zhang, Y.; He, Z. Enhanced paracellular and transcellular paclitaxel permeation by chitosan–vitamin E succinate– N -acetyl- l -cysteine copolymer on Caco-2 cell monolayer. J. Nanoparticle Res. 2014, 16, 2355–2370. [Google Scholar] [CrossRef]
- Cao, D.; Wang, Z.J.; Shen, X.T.; Song, X.J.; Zhao, Z.X. Metabolic and Pharmacokinetic Investigation of Ilexsaponin A1 in Normal and Antibiotic-treated Rats. Pharmacogn. Mag. 2023, 20, 245–256. [Google Scholar] [CrossRef]
- Van Speybroeck, M.; Mols, R.; Mellaerts, R.; Do Thi, T.; Martens, A.J.; Van Humbeeck, J.; Annaert, P.; Van den Mooter, G.; Augustijns, P. Combined use of ordered mesoporous silica and precipitation inhibitors for improved oral absorption of the poorly soluble weak base itraconazole. Eur. J. Pharm. Biopharm. 2010, 75, 354–365. [Google Scholar] [CrossRef]
- Matteucci, M.E.; Paguio, J.C.; Miller, M.A.; Williams III, R.O.; Johnston, K.P. Highly supersaturated solutions from dissolution of amorphous itraconazole microparticles at pH 6.8. Mol. Pharm. 2009, 6, 375–385. [Google Scholar] [CrossRef]


| Drug/Stabilizer Ratio | Size (nm) | PDI | Zeta Potential (mV) |
|---|---|---|---|
| 2:1 | 273 ± 25.2 | 0.288 ± 0.027 | −15.2 ± 1.8 |
| 1:1 | 225.7 ± 10.3 | 0.189 ± 0.023 | −28.1 ± 2.3 |
| 1:2 | 262.1 ± 23.5 | 0.268 ± 0.016 | −23.3 ± 2.7 |
| Parameters | Unit | ITZ-Nanos | Pellets |
|---|---|---|---|
| AUC(0–t) | μg·L−1·h−1 | 16,065.68 ± 1514.1 * | 12,084.46 ± 1186.3 |
| AUC(0–∞) | μg·L−1·h−1 | 20,863.45 ± 2917.5 | 17,305.51 ± 2035.7 |
| Cmax | μg·L−1 | 742.49 ± 11.23 ** | 607.35 ± 23.12 |
| Tmax | h | 8.00 ± 0.57 ** | 2.00 ± 0.87 |
| MAT | h | 24.69 ± 1.86 | 30.65 ± 2.36 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Chang, S.; Yang, Q.; Liu, J.; Yin, L.; Han, J.; Zong, L.; Pu, X. The Increased Dissolution and Oral Absorption of Itraconazole by Nanocrystals with an Endogenous Small-Molecule Surfactant as a Stabilizer. Molecules 2024, 29, 1769. https://doi.org/10.3390/molecules29081769
Chang S, Yang Q, Liu J, Yin L, Han J, Zong L, Pu X. The Increased Dissolution and Oral Absorption of Itraconazole by Nanocrystals with an Endogenous Small-Molecule Surfactant as a Stabilizer. Molecules. 2024; 29(8):1769. https://doi.org/10.3390/molecules29081769
Chicago/Turabian StyleChang, Sheng, Qiang Yang, Jiahuan Liu, Li Yin, Jihong Han, Lanlan Zong, and Xiaohui Pu. 2024. "The Increased Dissolution and Oral Absorption of Itraconazole by Nanocrystals with an Endogenous Small-Molecule Surfactant as a Stabilizer" Molecules 29, no. 8: 1769. https://doi.org/10.3390/molecules29081769
APA StyleChang, S., Yang, Q., Liu, J., Yin, L., Han, J., Zong, L., & Pu, X. (2024). The Increased Dissolution and Oral Absorption of Itraconazole by Nanocrystals with an Endogenous Small-Molecule Surfactant as a Stabilizer. Molecules, 29(8), 1769. https://doi.org/10.3390/molecules29081769






