Abstract
Mutation of the tumor suppressor gene, TP53, is associated with abysmal survival outcomes in acute myeloid leukemia (AML). Although it is the most commonly mutated gene in cancer, its occurrence is observed in only 5–10% of de novo AML, and in 30% of therapy related AML (t-AML). TP53 mutation serves as a prognostic marker of poor response to standard-of-care chemotherapy, particularly in t-AML and AML with complex cytogenetics. In light of a poor response to traditional chemotherapy and only a modest improvement in outcome with hypomethylation-based interventions, allogenic stem cell transplant is routinely recommended in these cases, albeit with a response that is often short lived. Despite being frequently mutated across the cancer spectrum, progress and enthusiasm for the development of p53 targeted therapeutic interventions is lacking and to date there is no approved drug that mitigates the effects of TP53 mutation. There is a mounting body of evidence indicating that p53 mutants differ in functionality and form from typical AML cases and subsequently display inconsistent responses to therapy at the cellular level. Understanding this pathobiological activity is imperative to the development of effective therapeutic strategies. This review aims to provide a comprehensive understanding of the effects of TP53 on the hematopoietic system, to describe its varying degree of functionality in tumor suppression, and to illustrate the need for the adoption of personalized therapeutic strategies to target distinct classes of the p53 mutation in AML management.
1. Introduction
The TP53 gene and its protein was first described in 1979 and has since taken center stage due to an avalanche of research after mutations in this gene were identified as the common denominator in more than 50% of human cancers. TP53 mutation associated acute myeloid leukemia represents a distinct molecular cohort with a notorious reputation for uniformly poor prognosis [1]. The TP53 mutation confers a resistant predisposition to current therapeutics regardless of age. In comparison, CR in a non-TP53 mutated cohort is around 80% [2,3,4,5]. A lower variant allele frequency (VAF) of the TP53 mutation is associated with fewer chromosomal losses and a complex karyotype but does not confer a better overall or event free survival to a higher allele frequency [6].
This poor outcome could be substantiated by the crucial role p53 imparts in mediating apoptotic feedback to standard chemotherapy leading to inherent resistance in mutated p53 [2,5,7,8,9].
Li-Fraumeni syndrome, a condition caused by a germline mutation in TP53 in humans born with a single mutant allele of TP53, encompasses a wide variety of early onset cancers, including AML in around 5% of Li Fraumeni related malignancies [10].
Somatic mutations in transcription factor TP53 represent one of the most frequently mutated alterations in human cancers. These mutations are surprisingly observed in only 5–10% of de novo AML but occur in about 25% of older patients with de novo AML with a median age of 60–67 years [3]. In genomic, unstable AML, like t-AML therapy related myelodysplastic syndrome(t-MDS), TP53 mutation is observed in 30–35% of cases. However, in complex-karyotype AML TP53 is mutated in 70% of proportion. Therefore, TP53 represents a powerful adverse indicator of poor prognosis independent of complex karyotype, age and other genetic markers [11,12,13,14,15].
Broadly, TP53 is mutated in all morphological subtypes of the French American British (FAB) classification but is more enriched in erythroleukemia (25–36%) [16,17].
The relative lower prevalence of somatic TP53 mutation in AML compared to solid tumors like ovarian (48%), and colorectal (43%) suggests that other cooperating events are necessary for leukemic progression [3].
2. TP53 Gene, p53 Structure and Cellular Functions
Normal (wild type, WT) p53 protein, which is encoded by the TP53 gene, is located on chromosome 17p13.1. The p53 protein product is a 393 amino acid long phosphoprotein which contains five important hallmark domains: the amino N-terminal transactivation domain, a central DNA-binding domain (DBD), a carboxy-terminal oligomerization domain, and a regulatory domain. (Figure 1) [18]. P53 is known as the guardian of the genome as its official function is to maintain harmony between cell arrest and cell growth during genomic stress [19].

Figure 1.
Functional domain of p53: The N-terminal portion consists of the transactivation domain (TA) and the proline rich domain (PR). TA is required for transactivation of various transcription factors and interaction of MDM2 ubiquitin ligase. The central core is mainly made of the DNA—binding domain (DBD); most of the exons of TP53 are sequenced. The C—terminal consists of the oligomerization domain (OD) and the carboxy- terminal regulatory domain.
TP53 gene is largely a stress response protein with functions ranging from apoptosis to cell cycle control. Therefore, a mutation in the TP53 gene pronounces the effects of oncogenes leading to the uncontrolled proliferation of tumor cells. These mutations are known to give rise to a deleterious gain of function (GOF), a loss of function (LOF) or a non-mutational dysfunction or inactivation of the p53 protein [20,21,22,23]. There are multiple pathways to p53 inactivation resulting in decreased p53 level and subsequent cell proliferation. Half of the time this inactivation is a direct result of TP53 gene mutation in one TP53 allele which eventually can lead to the loss or partial inactivation of the other WT allele over time or during disease progression, owing to loss of heterozygosity (LOH). LOH, in the context of somatic and germline mutation, is considered as a gene alteration that further evolves to tumor progression [24,25,26].
p53 is normally ‘off’ with a short half-life and is tidily regulated at the protein level via post-translational modifications including ubiquitination, phosphorylation, acetylation and methylation [27,28,29,30]. It is activated when cells are stressed [31] or damaged avoiding further proliferation of stressed cells through the G1/S phase of the cell cycle. The continuous ubiquitylation and subsequent degradation allow the unstressed cell to maintain a low level of WT p53. In contrast, p53 ubiquitylation is suppressed under hypoxic conditions, or oncogene activation and DNA damage, leading to its accumulation. p53 is then stabilized in the nucleus in the form of tetrameric complexes and finally undergoes its activation. The formation of tetramers is required for p53 to be fully active and serve as a transcriptional activator of more than 150 target genes [26,32].
The fate of p53 protein in the cell is mainly determined by the rate of degradation rather than the rate of production. p53 is primarily degraded by the interaction of p53 with MDM2 (Double minute 2 Protein).
MDM2 is a ubiquitin E3 ligase that labels p53 with ubiquitin, resulting in p53 degradation by 26S proteasomes [33]. This interaction of p53/MDM2 can be disrupted when stress or DNA damage is detected resulting in the stabilization of p53. Of note, an overexpression of MDM2, which can be observed in many tumors, leads to the deactivation of p53 [26].
Interestingly, primary AML with WT TP53 can overexpress high levels of another important regulator of p53 called MDM4 (also known as MDMX), through binding of p53 AT domain. This finding demonstrates the detrimental consequences of dysfunctional p53 pathways accompanied by inferior survival.
To the contrary, mutant p53 accumulates in tumor cells and is regulated and stabilized by MDM2 in a manner similar to WT p53, which could be secondary to attainting a (GOF) phenotype. Therefore, detection of increased levels of p53 by immunohistochemistry (IHC) correlates with TP53 gene mutation as p53 expression is low in a normal cell [27,28,29,30].
The p53 network is activated primarily by three mechanisms which maintain an increased concentration of p53 protein. This stabilization of higher concentrations of p53 allows for p53 binding to DNA sequences with ensuing transcription of adjacent genes, ultimately resulting in inhibition of cell division or cell death. The first pathway is the activation of kinases like ataxia telangiectasia related (ATR) and casein kinase II on exposure to chemotherapeutic agents and ultraviolet light [34]. Secondly, an increased oncogene expression such as that of Myc or Ras triggers growth signals resulting in the production of p14ARF protein which consequently activates p53 by binding to MDM2 and inhibiting its activity [35,36,37]. Lastly, major kinases like ATM (ataxia telangiectasia mutated) stimulate Chk2 (Checkpoint kinase 2) when triggered by double strand breaks [37]. In summary, significant DNA dependent protein kinases including ATM, Chk1, and Chk2 sense DNA damage, phosphorylate p53 at the AT (amino terminal domain) sites close to the MDM2 binding region and consequently block MDM2 interaction with p53. The end result of this cascade is the stabilization of p53. [38].
p53 encompasses around 18,000 mutations in different cancers. Unlike the majority of the tumor suppressor variants which largely consist of truncation mutations, the predominant p53 mutation in leukemia is a monoallelic missense mutation [39,40]. A missense mutation is a point mutation in the DNA resulting in a single amino acid substitution within the translated protein. This mutation produces a phenotype with increased expression of altered p53 protein, which accumulates in tumor cells contributing to tumor initiation, promotion and chemoresistance [38]. The alternative mutations such as nonsense, splice-site or insertion/deletions are observed in lower frequencies [39,41].
Monoallelic mutation gives rise to mutant p53 full-length protein which are detected in tumors and usually mapped in the DBD affecting sequence specific DNA-binding activity [24].
TP53 mutation in leukemia can occur in the context of somatic and germline mutations, the latter of which is associated with Li-Fraumeni syndrome leads to the development of specific solid tumors and is less likely to arise in diverse tissues [41]. In the sporadic setting, however, TP53 mutations seem to occur when exposed to carcinogens (environmental factors), oncogenic agents or genotoxic insults. This observation further elucidates the robust functionality of p53 in maintaining genomic stability and preventing tumor formation [3].
3. Role of TP53 in Hematopoiesis, Clonal Hematopoiesis and AML
During the development of an organism, each cell acquires a similar set of genes and a template genetic sequence. Differentiation of cells into specific tissues and their function is a byproduct of the activation or silencing of certain genes. With age or as a result of exposure to environmental mutagens, proliferating and differentiating cells may procure somatic mutations. The effects of mutation are many including neutral effects if the variant lies within a non-regulatory region, an increase in proliferation capacity or negative selection against cells if contained within essential genes [42,43].
The hematopoietic system is a complex yet efficient entity responsible for producing a multitude of cells daily. To meet these demands, hematopoietic stem cells (HSCs) have a hierarchical methodology of self-renewal and division into progenitor cells. HSCs can divide giving rise to a progenitor and another HSC or two progenitor cells which will later divide and differentiate into mature cells. Progenitor cells have a limited self-renewal potential. In these cells the acquisition of a mutation will usually end the clonal lineage. However, in some cases a mutation can have a proliferative advantage leading to progenitor cell proliferation. Occasionally, the slowly dividing HSCs may acquire mutations which can influence the HSC compartment and daughter cells. These variants may lead to proliferation and expansion of the HSC clone or one lineage of cells. This constitutes the basis of clonal hematopoiesis (CH) [44,45,46,47].
An important role in the self-renewal and proliferation of normal HSCs is assigned to the TP53 gene and p53 protein [48]. Under biologically functional TP53 HSC self-renewal is decreased when exposed to DNA damaging radiation, oncogene activation and alkylating agents. However, TP53 disruption leads to augmented proliferation and overproduction of pluripotent stem cells [49,50,51]. This suggests that suppression of p53, or its pathway, leads to outgrowth of pluripotent stem cells with subsequent malignant transformation of hematopoietic stem/progenitor cells [52,53,54].
Early studies have shown p53 to be involved in apoptosis, proliferation and differentiation of human HSCs and provides quiescence during steady states of hematopoiesis [55,56]. Intact p53 is integral to the function of bone marrow mesenchymal stromal cells (MSC). This is evidenced by observations that mice with p53 deficient MSCs were unable to support hematopoietic progenitors [57]. Functional p53 is known to contribute to HSC genetic stability and homeostasis by reducing intracellular reactive oxygen species level [58]. In murine HSCs with p53 loss and incorporation of mutant KrasG12D, there was a disposition for indefinite self-renewal and the ability to transform into leukemia cells [51].
With modern techniques, it is now widely understood that aging is ubiquitously associated with mutations and HSC expansion that can harbor mutations in leukemia specific genes without associated hematologic malignancies or cytopenia, commonly referred to as age related clonal hematopoiesis (ARCH) [59,60].
Clonal hematopoiesis of indeterminate potential (CHIP) in leukemia associated genes including DNMT3A, ASXL1, TET2 with a variant allele frequency (VAF) of ≥2% can confer a predisposition for hematological malignancy including overt leukemia, as well as thrombosis, stroke and cardiovascular events [61,62,63,64]. More recently, the utilization of targeted deep sequencing techniques has allowed for the identification of VAFs of >0.5–1%, which have been noted to be associated with an increased odds of AML development [60,63,65]. For this review we will refer to ARCH and CHIP as clonal hematopoiesis (CH)
TP53 somatic mutation is associated with aging, is present in 4% of CH and is believed to play a vital role in CH development along with other associated gene mutations in DNMT3A, TET2, ASXL1, SRSF2, CBL, and SF3B1. There is strong evidence that when the TP53 mutation is present it represents a nearly initiating event and presents as a dominant or founding clone in the development of leukemia whereas DNMT3A and TET2 mutations are sustained over time with no overt association with AML development [11,66].
TP53 mutations are associated with CH development and there is convincing evidence that mutated TP53 can lead to a permissive state of overt leukemia. These findings support the perceived fitness advantage conferred by TP53 through enhancement of HSC self-renewal in light of genotoxic stresses [47]. However, Trp53 mutation induced mouse models exhibit no overt transformation to leukemia, enforcing the idea that Trp53 mutation alone is not sufficient for a foolproof leukemia initiation, but rather multiple additional steps are required [51,67].
Serial acquisition of somatic mutations is known to be involved in the pathogenesis of AML; nevertheless, more definitive studies are needed to address whether these mutations are an initiating or cooperating event. This continues to be a challenge as one third of AML patients harbor no mutations in known leukemia associated genes [68]. Hence, despite the understanding of CH having an effect on survival, there are currently no data supporting the screening of asymptomatic patients.
4. Functional Patterns of TP53 Mutations
In clinical settings, all TP53 mutations are viewed collectively, and therapeutic intervention is not stratified by specific TP53 genotype. However, a plethora of research has enabled us to understand various functional subgroups within p53. Understanding the influence of various forms of TP53 mutations on the clinical characteristics of leukemia is useful in grasping the underlying p53 biology and critical for the development of potent targeted agents [69].
The changes in gene and subsequent protein functionality can be studied based on mutation site in reference to the domain-based structure of p53 protein.
The three main functional regions of p53 protein are the amino terminal region, the centrally situated DNA-binding domain and the oligomerization domain [70]. In AML, TP53 mutations were detected most frequently in the centrally situated DNA-binding domain, followed by the amino terminal domain and the oligomerization domain [70]. The different TP53 domains are distinct in functional activity and under normal circumstances all p53 mutants are inert and behave as LOF mutants. However, exposure to genotoxic stress can have varied effects including GOF and dominant negative (DN) effects (Figure 1) [71,72]. The characterization of the three main functional domains is presented below.
4.1. Amino Terminal Domain Mutants (AT)
The AT domain of the TP53 gene spans through amino acid residues 1-61 and encodes for a transcriptional activator which harbors the transactivation domains (TAD) 1 and 2 and a proline rich domain. Although, the explicit molecular function of TAD1 and TAD2 remains obscure, TAD1 is associated with the induction of a number of genes while TAD2 contributes to tumor suppression. Both TAD1 and TAD2 can independently transactivate genes, however, at least one TAD is required for p53 transcription [73].
AT mutations within the first 40 amino acids are usually insertion or deletion variants and result in the abrogation of full-length p53 expression [74]. The AT domain has several significant regulatory regions, including MDM2. This oncoprotein is a cellular inhibitor of p53 that can bind to the AT domain causing p53 degradation via ubiquitylation and p300 binding resulting in p53 deactivation via acetylation. Some cancers can lead to the amplification of MDM2 resulting in p53 inactivation and unopposed cell growth [75,76].
When a full length p53 formation is disrupted from mutations in the AT domain, initiation of translation from an alternative codon expresses p47. This isoform of p53 is a truncated 47 kDa protein and, when endogenously expressed, serves as a tumor suppressor when p53 lacks TAD1 and TAD2 [77,78].
P47 can induce the expression of selective apoptotic genes and retains some transactivation properties but is unable to encode for cell-cycle arrest genes such as CDKN1A [79,80]. P47 retains a selective apoptotic function despite a flawed G1/S cell cycle checkpoint. Nevertheless, AT domain mutations are prognostically more favorable than p53 DBD mutations.
Hence, expression of high p47 or AT domain TP53 mutations have a better response to therapy which translates into improved overall survival [81]. Theoretically, p47 expression could be used as a biomarker to predict favorable response to therapy
4.2. DNA Binding Domain (DBD)
The centrally located DBD is the most frequently mutated (around 80%) region and spans amino acids 100–200 within exons 5–8 (Figure 1). Mutations to this domain result in the inability to transactivate multiple target genes leading to the functional inactivation of p53 and the loss of DNA binding capacity [71,82]. DBD carries six major mutational hot spots including codons 175, 245, 248, 249, 273, and 282, showing a propensity for arginine residues [83]. The most common hot spot DBD mutations reside in codon 175. The first 42 amino acids at the N-terminal transactivation domain interact with the basal transcriptional machinery serving as a positive regulator of gene expression [69].
As mentioned earlier and contrary to popular belief, mutations often cause various functional defects at a cellular level and not solely LOF via loss of tumor suppressor activity and mitigation of transcriptional activation of the p53 gene [84]. However, in general, DBD mutants are usually LOF variants.
As evident in LFS and mouse models, one DBD mutant TP53 allele confers a predisposition to spontaneous cancer development [85]. The distribution of hot spot residues in germline and sporadic tumors are similar [86]. Thus, the loss or mutation of both TP53 alleles accentuates spontaneous tumor development raising the importance of gene dosage and the enhanced oncogenic potential of the p53 missense mutation [71,87]. Generally, with an underlying DBD mutant p53 allele tumorigenesis is accentuated in the presence of DNA damaging agents. The resulting effects are similar to that of the null p53 allele (TP53 −/−) with decreased transactivation of target genes and limited function of the WT p53 leading mainly to loss of tumor suppression, apoptosis and DNA repair [88,89]. Consequently, DBD mutations are distinguished by complete loss of transactivation potential [90,91], and are resistant to various anticancer therapies resulting in a poor prognosis [77,92,93].
Usually, missense mutations can produce full length mutant p53 which is more stable than WT and present at high levels in tumor cells [94]. These variants attain additional features that inhibit the co-expression of the remaining WT protein encoded in the second allele and are known to have DN effects that support oncogenesis and survival. Of note, DN effects are expressed by the majority of the DBD mutants [29,69,95]. The DBD-DN mutant has an inhibitory effect on the remaining WT p53 protein transgressing to a lower canonical p53 functionality in comparison to LOH of the WT allele or TP53+/− heterozygosity [69,71,96]. Data from multiple studies have concluded that DN effect does not generally lead to tumorigenesis with loss of p53 function. DN is not usually demonstrated at basal levels in mutant p53 protein expression but rather a higher DBD mutant p53 to WT ratio of around 3:1 is required to contribute to tumorigenesis [97,98]. Exposure to DNA damaging agents including radiation and chemotherapy can increase the DBD mutant ratio inducing DN effects by decreasing the WTp53. This implies that therapeutic interventions that decreases mutant p53 could abrogate tumorigenesis in malignancy with one DBD mutant allele [69,71,96].
Often, mutant p53 can initiate new functions independent of WT p53, conferring gain-of-function (GOF) properties that propagate progression, metastasis, drug resistance and survival. GOF capability is achieved by the binding of mutant p53 to the p63 and p73 family of tumor suppressor genes resulting in functional alterations and inhibition of these key transcription factors required for cell cycle arrest [24,88,99,100]. Furthermore, mutant p53 binding to p73 protects cells from chemotherapeutic agents [101]. Thus, GOF effects the ability of the mutant p53 to transactivate novel cell survival genes, [102] which then leads cancer cells to become dependent on mutant p53 for tumorigenesis, [103,104] while resisting cell death on exposure to DNA damaging agents [105]. DBD mutants do not usually possess GOF characteristics, but when present, are commonly seen with mutations in codon 175, 248 and 273 [69]. Hence, targeting the interaction between p53 and p63 and p73 would constitute a promising strategy, thus restoring p73 activity could re-sensitize the cancer cells to therapeutic agents [106]. The aforementioned phenotypic effects of DBD mutations are not mutually exclusive.
4.3. Oligomerization Domain (OD)
The OD, which spans amino acid 325–356, is essential for tetramerization of p53, an important event in tumor suppressor function. Recurrent hotspots with OD mutations are R337H, R342P, and R342. Mutation within the OD is rarely seen in sporadic cancer but commonly encountered with germline mutations [107,108].
Usually, when a mutation affects tetramerization, it is known to diminish DNA binding. Consequently, mutation confers complete or partial loss of transactivation and loss of tumor suppression, thus functionally behaving like LOF p53 proteins [107,109]. Generally, patients with OD mutations lack a response to chemotherapeutic agents as they rely on a p53 mediated cytotoxic effect [69].
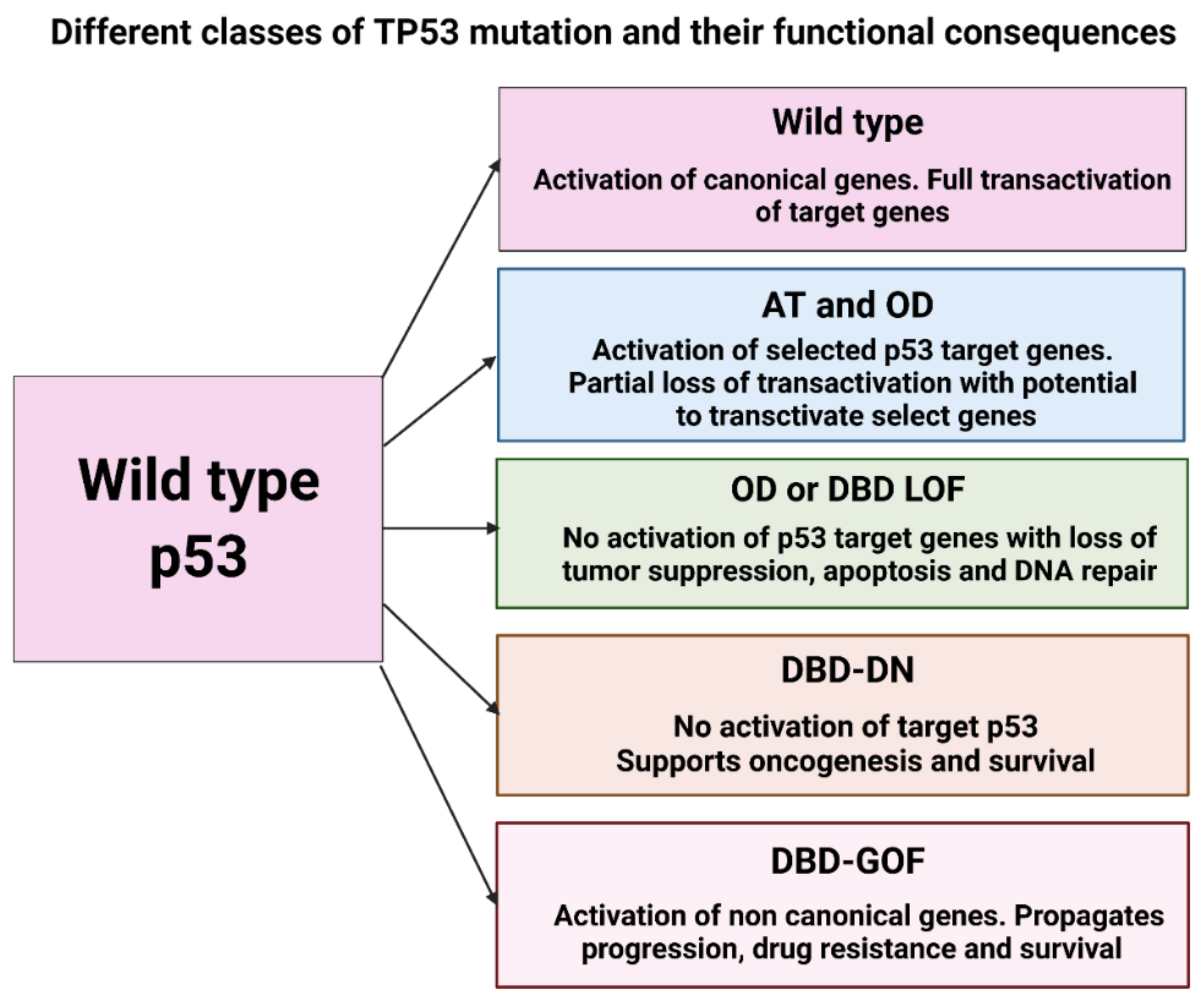
In summary, the mutation of various p53 domains results in a spectrum of functional consequences at a cellular level. Mutation in the AT domain is usually associated with partial loss of transactivation potential with the ability to transactivate select genes.
DBD-LOF variants possess the ability to deliver partial transcriptional function leading to cell death similar to OD mutants while lacking WT p53, while DBD-GOF mutants have the worst functionality with increased cellular survival and metastasis in the p53 null state. Hence, envisaging the different functional classes of the p53 mutant can drastically improve outcomes if therapeutic approaches specific to p53 mutant subtype are adopted (Figure 2) [69].
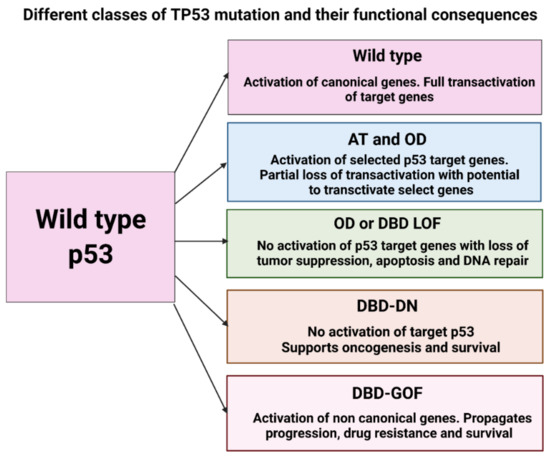
Figure 2.
Classes of TP53 mutations and their functional implication. Amino-terminal (AT), Oligomerization domain (OD), DNA-binding Domain (DBD), Loss of function (LOF), Double negative (DN), Gain of function (GOF).
5. Co-occurring Mutations and Allelic States in TP53 AML
TP53 mutation resulting in loss or alteration of function is seen in approximately 8% of de novo AML. However, these genetic variants are present in 30% of t-AML cases and in patients with complex karyotype, especially in the elderly, they are encountered in around 70% of subjects. Nevertheless, prognosis and overall survival is poor in all subgroups [110,111,112,113]. The 2017 European Leukemic Net (ELN) guidelines was updated to include TP53 mutated leukemia as an unfavorable group. Overall survival for patients with TP53 mutation and complex cytogenetics (i.e., ≥3 cytogenetic abnormalities) is worse in comparison to TP53 WT and complex karyotype or TP53 mutated with no complex cytogenetics [66].
Presence of TP53 mutations as part of CHIP have been observed although mutations in DNMT3A, TET2 and ASXL1 are more common compared to TP53 [59,61,63,114]. Desai et al. evaluated the presence of mutated TP53 in a normal population through prospective study, subjects that harbored a detectable VAF of 1% or more in TP53 or IDH1/2 mutation eventually developed AML. RUNX1 had the shortest latency to develop AML (1.5 years vs. 9.6 years without mutation). Of note, the RUNX1 study was limited by small sample size (only 3 patients), hence more studies are needed to validate this finding. Other mutations with increased odds of developing AML included DNMT3A, TET2, and spliceosome-related genes SRSF2, SF3B1 and U2AF1 [63]. Although, a part of CH it should be noted that a VAF of ≥10% in DNMT3A and TET2 were at increased risk for AML whilst a lower VAF (<10%) was less specific to AML. However, this was not the case with TP53 and IDH mutations, wherein the odds to develop AML was independent of VAF [63].
Mutated TP53 and PPM1D clones were strongly enriched during and after induction chemotherapy. This finding does not necessarily represent the initiation of these mutations but is rather considered to be secondary to preferential expansion of candidate mutations that were present in small frequencies prior to cytotoxic chemotherapy [11,115].
TP53 mutation is commonly associated with complex karyotype, chromothripsis, chromosomal arm losses (especially 5, 7, 17), cytogenetic alterations to copy number (aneuploidy) or some combination of these features [12,66,116]. Usually, TP53 mutations are not associated with low risk aberrations like t (8:21) or inv 16 [12]. An analysis of 40 AML patients demonstrated that copy number alterations with TP53 mutations were associated with trisomy of chromosome 8, gain of chromosome 17 (11.2), 14 (q32.3), 16p (11.2–11.3) and deletion of chromosome 12 (p12.3) [13,117]. Although the mechanism of leukemogenesis in TP53 mutated AML is unknown, the frequent observation of chromosome 5, 7 and 17 aneuploidy with mutated TP53 advocate for their involvement in the transition from CHIP to AML [115].
TP53 mutations are less often linked with alterations in the RAS pathway (4%), FLT3 (6%) or NPM1 (8%), [4,112] and to a lesser frequency can co-exist with single nucleotide variants in recurrent AML genes like TET2, IDH1/2 and DNMT3A [12,13,66,112,116]. A different pattern of co-mutations may be observed within a founding clone compared to a subclone with TP53 mutation. If associated with a founding clone, TP53 mutation usually coexists with transcription factors (RUNX1, CEBPA, NPM1) or epigenetic genes (DNMT3A, TET2, IDH1/2) or can be seen as a subclone in the process of clonal evolution triggered by a poly comb pathway of SF3B1, SRSF2 or a signaling mechanism involving JAK2, RAS, FLT3, PTPN11, or BCOR [59,61,114].
Recent studies have shown the importance of VAF to prognosticate the role of sub-clonal TP53 mutation in AML. In the study TP53 mutations were divided by their VAF into subgroups of >40%, 20–40%, and <20%. VAF of <20%, although considered sub-clonal, had a negative impact on overall survival (OS), complete remission rate and event free survival rates. However, a lower VAF was associated with fewer chromosomal losses and complex karyotype [118]. Similar results were validated with myelodysplasia and secondary AML patients, where in VAF <20% was associated with improved OS compared to VAF >40% which predicted complex karyotype and worse OS [119,120]. TP53 can be associated with diploid cytogenetics but usually the VAF is lower compared to non-diploid cytogenetics.
Short et al. further validated these findings by demonstrating that AML with mutated TP53 VAF of >40% was independently correlated with worse relapse free survival and OS [121].
Furthermore, Sallman et al. describe the striking relationship between an increase in VAF% and worsening karyotype complexity, which again correlated with worsening OS [119].
About 20% of patients with del 5q have TP53 mutation clonal evolution, which is generally associated with resistance to lenalidomide and transformation to AML. As per the world health organization (W) 2016, monitoring for the appearance of clonal evolution or increase in the clone of TP53 predicts disease progression [122,123,124,125].
The extent of TP53 genome instability varies depending on whether it is a monoallelic TP53 hit per single gene mutation or biallelic/multiple hits. Rate of transformation to AML from MDS and overall survival was worse with multiple TP53 hits in comparison to monoallelic TP53 hits- which was very similar to the TP53 WT [126].
6. Current Standard Therapeutic Concepts
Therapy with standard chemotherapy in TP53 mutated AML with loss of TP53 allele displays a lack of chemotherapy induced apoptosis and subsequently a poor response rate (RR), disease-free survival (DFS) and OS while being independent of cytogenetic aberration [5] Decitabine (DAC) has been shown to enhance chemotherapy response in patients harboring TP53 mutations, however, it has not been able to deliver a durable response or clear subclones of TP53 mutations [127,128]. Nevertheless, a higher response was noted in AML patients with TP53 mutations compared to WT TP53 (100 vs. 41%) [127]. The underlying mechanism responsible for the sensitivity of TP53 AML to DAC is currently uncertain. TP53-mutated AML patients receiving a monthly regimen of 5-day DAC had an overall response rate of 62% [12].
Short et al. assessed the efficacy of a 5-day DAC schedule compared to a 10-day regimen in a randomized phase II, open label, single center trial. There was no difference in outcome between the two DAC schedules for those with TP53 mutated status. Intriguingly, response rate did not differ depending on baseline VAF. Four patients had a VAF ≥20% at the time of remission suggesting the presence of TP53 mutation preleukemic clones rather than solely myeloblasts. The two patients that had the longest remission duration had no detectable TP53 mutations present in the remission bone marrow sample [129]. It is widely understood that dominant clone TP53 mutations have poor outcomes but recently sub-clones were noted to have equally poor outcomes [118].
TP53 mutated cells are more sensitive to hypomethylating agents in comparison to cytotoxic agents, providing the impetus for a combination with bcl-2 inhibitor- Venetoclax (VEN) AML study. In patients harboring TP53 mutations, the complete response (CR) + complete remission with incomplete blood count recovery (CRi) rate was 47% while the median OS was 7.2 months. Compared to historical standards of 28% CR rates, the combination displayed promising efficacy. VEN mediated apoptosis appeared TP53 independent [130,131,132,133].
One of the primary and adaptive forms of resistance to VEN-based combination therapy is activated bi-allelic TP53 perturbation. Hence, on disrupting TP53 function within an AML cell line by using CRISPR/Cas9, DiNardo et al. were able to demonstrate an association between TP53 loss and resistance to VEN, hypomethylating agent (HMA) and cytarabine (ARA-C) as a single agent or in combination [134]. Similarly, preclinical studies in leukemic cell lines have displayed an association between VEN resistance and a faulty apoptotic pathway involving TP53 and BAX [135,136].
Allo-SCT with TP53 mutation and complex cytogenetics portend inferior OS in patients with MDS. However, outcomes in patients with complex cytogenetics and WT TP53 are not poor, solidifying the fact TP53 mutation is a critical driver for poor overall survival [137].
7. Newer Molecularly Targeted Therapies
Relapses and primary resistance still occur in TP53 mutated AML, necessitating the dire need for newer therapeutic options. The primary objective of newer therapies is to restore normal TP53 function by either degrading or inactivating mutant p53 or reviving WT p53. (Table 1 and Table 2).

Table 1.
Clinical trials to restore wild type function of p53.

Table 2.
Clinical trials to degrade mutant p53.
7.1. Mutant TP53 Inhibitor-APR-456
For the longest time TP53 was considered undruggable. Eprenetapopt (APR-246), a PRIMA-1 analog, is a novel, first-in-class, small molecule therapeutic agent that binds covalently to cysteine residues in mutant p53 protein and induces a conformational shift to a WT-like structure.
This enables p53 binding to a specific DNA sequence leading to reactivation of pro-apoptotic function by enhancement of target gene transcription [138,139]. APR-246 has activity in cells without detectable TP53 expression and in WT TP53 cells by inducing heightened oxidative stress resulting in cell apoptosis [140] Due to a synergistic effect with azacytidine (AZA) in preclinical AML models, Eprenetapopt is being tested in a phase 1b/2 study in the treatment of naïve high risk myelodysplastic syndrome (HR-MDS) and oligoblastic (20–30% blasts) AML patients. Higher response rates were noted in patients with >10% p53 positivity by IHC and isolated TP53 mutation. Median duration of response was 6.5 months and median time to response was 2 months. Of the 45 patients evaluated, overall response rate was 88% and 53% achieved CR [141].
A European phase 2 study with a similar cohort of HR-MDS and AML showed an overall response rate of 75% and CR of 56% [142]. TP53 VAF clearance correlated with CR in both the studies. On the basis of these encouraging results, APR246 received fast track and orphan drug designation from FDA in April 2020. Results of the randomized phase 3 study of APR-246 and AZA compared to azacytidine alone (NCT03745716) is awaiting full report.
APR346 is being investigated in a phase I study in combination with AZA/VEN for newly diagnosed TP53 mutated myeloid malignancies (NCT04214860) and being assessed in combination with azacitidine following allo-SCT as maintenance therapy in TP53 mutated AML/MDS (NCT03931291).
APR-548, an orally bioavailable derivative of APR-246, is currently being developed to be used in a phase 1 study with AZA in TP53 mutated MDS (NCT04638309). The synergy observed between APR-246 and AZA is hypothesized to be related to down regulation of FLT3 pathway [143].
7.2. MDM2 Inhibitors
p53 pathway dysfunction is highly prevalent in acute myeloid leukemia independent of TP53 mutational status [31] MDM2 and MDM4 are negative regulators of TP53 activity, targeting degradation via ubiquitination. In AML, MDM2 is often overexpressed, hence cells may have low functional TP53 activity without TP53 deletion/mutation. Nutlin-3a is a small molecular inhibitor of the MDM2/p53 interaction, thus this therapeutic provides increased p53 levels secondary to reduced p53 destruction, consequently upregulating apoptosis [144].
RG7388/idasanutlin is an orally bioavailable MDM2 inhibitor which was investigated in the placebo controlled, double blind phase III MIRROS study in combination with cytarabine in the management of relapsed refractory (r/r) AML. Unfortunately, the study had to terminate early as it did not meet primary end point of improved survival in comparison to ARA-C alone [145]. TP53 stabilization, cell cycle arrest and apoptosis were produced in a dose dependent fashion [146]. TP53 mutational status alone did not correlate with CR, although increased expression of MDM2 among HSPC and leukemia blasts was consistent with CR [147,148].
Idasanutlin is currently in clinical trials in combination with Venetoclax in r/r AML (NCT02670044 and NCT04029688). The preliminary results were presented at the 2019 American Society of Hematology annual meeting, and the CR/Cri was reported in 11 of 49 patients [149]. It is in clinical trials for newly diagnosed AML in combination with cytarabine and daunorubicin based induction regimen (NCT03850535).
AMG 232 is a structurally distinct MDM2 inhibitor and interacts with the glycine self-region of the TP53 binding pocket on the surface of MDM2 [150]. AMG 232 is being investigated in r/r AML treatment.
Of the 30 patients evaluated, four achieved a morphological leukemia-free state. Unfortunately, no response was noted in patients with TP53 mutations.
AML possesses high expression of MDMX. Current MDMD2 inhibitors provide a limited effect on other members of the MDM family, including MDMX, which decreases their utility in AML treatment [151]. ALRN-6924 is a stapled peptide with dual inhibition of MDM2/MDM4. Phase I clinical trials utilizing MDM2/MDMX inhibitors in r/r AML and MDS are underway [151,152,153].
7.3. Immunotherapy and Other Agents
Cell surface CD47 interacts with its corresponding receptor on macrophages to inhibit the phagocytosis of normal, healthy cells. CD47 seems to be over expressed in myeloid malignancies, and overexpression of CD47 in myeloid leukemia increases its pathogenicity by allowing for tumor evasion of macrophages. Inhibition of CD47 induces engulfment of leukemic cells [154]. Magrolimab, a CD47 inhibitor, was investigated in a phase 1b study either as single agent in r/r AML or in combination with azacitidine in newly diagnosed AML. Combined Magrolimab and AZA was assessed in the treatment TP53 mutated AML patients (n = 9) resulting in a CR/Cri of 78% and 44%, respectively and negative MRD in 57% of the responders, with a median follow up of 6.9 months. Median duration and survival were not reached [155].
Arsenic trioxide has been shown to inactivate TP53 via 26S proteasome and upregulate WT TP53 functions, thereby inactivating proliferating leukemia cells and promoting apoptosis [156,157]. Furthermore, atorvastatin (statin), a cholesterol lowering drug, was recently investigated as an inducer of the degradation of misfolded or conformational mutant TP53 with minimal effects on WT p53 and DNA contact mutants [158].
8. Conclusions
There is growing evidence of age-related mutations and CH in the HSC and the influence of TP53 on normal HSC self-renewal. The impact of TP53 mutations on CH is indisputable. Improved characterization of the role of TP53 in normal hematopoiesis will lead to a more complete understanding of TP53 mutations in the propagation of CH and leukemogenesis. Pathways leading to TP53 dysregulation represent a common element in non-TP53 mutated AML, hence leveraging WT TP53 in unmutated AML serves as a corner stone in the design of anti-AML therapeutic strategies.
Recently, it has become understood that unaltered TP53 and mutated TP53 within tumor cells can be therapeutically targeted, which has led to the use of novel therapies like, APR-456 which has reported to restore transcriptional activity in mutant p53 or unfolded WT p53, leading to apoptosis or the promising result of anti CD47monoclonal antibody magrolimab in TP53 mutated AML.
This approach is of great precedence, as TP53 mutations in AML are distinctive, although rare, and confer dismal responses to chemotherapeutic agents with very poor outcomes.
Hence, research focused on the exploitation of TP53 pathway activators may yield immense contributions to the management of AML, a pathology associated with a very high risk of therapy failure.
Funding
This research received no external funding.
Conflicts of Interest
The authors declare no conflict of interest.
References
- Sallman, D.A.; McLemore, A.F.; Aldrich, A.L.; Komrokji, R.S.; McGraw, K.L.; Dhawan, A.; Geyer, S.; Hou, H.-A.; Eksioglu, E.A.; Sullivan, A.; et al. TP53 mutations in myelodysplastic syndromes and secondary AML confer an immunosuppressive phenotype. Blood 2020, 136, 2812–2823. [Google Scholar] [CrossRef] [PubMed]
- Williams, A.B.; Schumacher, B. p53 in the DNA-Damage-Repair Process. Cold Spring Harb. Perspect. Med. 2016, 6, a026070. [Google Scholar] [CrossRef] [PubMed]
- Olivier, M.; Hollstein, M.; Hainaut, P. TP53 Mutations in Human Cancers: Origins, Consequences, and Clinical Use. Cold Spring Harb. Perspect. Biol. 2009, 2, a001008. [Google Scholar] [CrossRef] [PubMed]
- Kadia, T.M.; Jain, P.; Ravandi, F.; Garcia-Manero, G.; Andreef, M.; Takahashi, K.; Borthakur, G.; Jabbour, E.; Konopleva, M.; Daver, N.G.; et al. TP53 mutations in newly diagnosed acute myeloid leukemia: Clinicomolecular characteristics, response to therapy, and outcomes. Cancer 2016, 122, 3484–3491. [Google Scholar] [CrossRef] [PubMed]
- Wattel, E.; Preudhomme, C.; Hecquet, B.; Vanrumbeke, M.; Quesnel, B.; Dervite, I.; Morel, P.; Fenaux, P. p53 mutations are associated with resistance to chemotherapy and short survival in hematologic malignancies. Blood 1994, 84, 3148–3157. [Google Scholar] [CrossRef]
- Yan, B.; Claxton, D.; Huang, S.; Qiu, Y. AML chemoresistance: The role of mutant TP53 subclonal expansion and therapy strategy. Exp. Hematol. 2020, 87, 13–19. [Google Scholar] [CrossRef]
- Li, R.; Sutphin, P.D.; Schwartz, D.; Matas, D.; Almog, N.; Wolkowicz, R.; Goldfinger, N.; Pei, H.; Prokocimer, M.; Rotter, V. Mutant p53 protein expression interferes with p53-independent apoptotic pathways. Oncogene 1998, 16, 3269–3277. [Google Scholar] [CrossRef][Green Version]
- Hamada, M.; Fujiwara, T.; Hizuta, A.; Gochi, A.; Naomoto, Y.; Takakura, N.; Takahashi, K.; Roth, J.A.; Tanaka, N.; Orita, K. The p53 gene is a potent determinant of chemosensitivity and radiosensitivity in gastric and colorectal cancers. J. Cancer. Res. Clin. Oncol. 1996, 122, 360–365. [Google Scholar] [CrossRef]
- Eliopoulos, A.G.; Kerr, D.J.; Herod, J.; Hodgkins, L.; Krajewski, S.; Reed, J.C.; Young, L. The control of apoptosis and drug resistance in ovarian cancer: Influence of p53 and Bcl-2. Oncogene 1995, 11, 1217–1228. [Google Scholar]
- Amadou, A.; Achatz, M.I.W.; Hainaut, P. Revisiting tumor patterns and penetrance in germline TP53 mutation carriers: Temporal phases of Li–Fraumeni syndrome. Curr. Opin. Oncol. 2018, 30, 23–29. [Google Scholar] [CrossRef]
- Wong, T.N.; Ramsingh, G.; Young, A.L.; Miller, C.A.; Touma, W.; Welch, J.S.; Lamprecht, T.L.; Shen, D.; Hundal, J.; Fulton, R.S.; et al. Role of TP53 mutations in the origin and evolution of therapy-related acute myeloid leukaemia. Nature 2015, 518, 552–555. [Google Scholar] [CrossRef]
- Seifert, H.; on behalf of the Study Alliance Leukemia (SAL); Mohr, B.; Thiede, C.; Oelschlägel, U.; Schäkel, U.; Illmer, T.; Soucek, S.; Ehninger, G.; Schaich, M. The prognostic impact of 17p (p53) deletion in 2272 adults with acute myeloid leukemia. Leukemia 2009, 23, 656–663. [Google Scholar] [CrossRef]
- Rücker, F.G.; Schlenk, R.F.; Bullinger, L.; Kayser, S.; Teleanu, V.; Kett, H.; Habdank, M.; Kugler, C.-M.; Holzmann, K.; Gaidzik, V.I.; et al. TP53 alterations in acute myeloid leukemia with complex karyotype correlate with specific copy number alterations, monosomal karyotype, and dismal outcome. Blood 2012, 119, 2114–2121. [Google Scholar] [CrossRef]
- Haferlach, C.; Dicker, F.; Herholz, H.; Schnittger, S.; Kern, W. Mutations of the TP53 gene in acute myeloid leukemia are strongly associated with a complex aberrant karyotype. Leukemia 2008, 22, 1539–1541. [Google Scholar] [CrossRef]
- Britt, A.; Mohyuddin, G.R.; McClune, B.; Singh, A.; Lin, T.; Gangul, S.; Abhyankar, S.; Shune, L.; McGuirk, J.; Skikne, B.; et al. Acute myeloid leukemia or myelodysplastic syndrome with chromosome 17 abnormalities and long-term outcomes with or without hematopoietic stem cell transplantation. Leuk. Res. 2020, 95, 106402. [Google Scholar] [CrossRef]
- Hou, H.-A.; Chou, W.-C.; Kuo, Y.-Y.; Liu, C.-Y.; Lin, L.-I.; Tseng, M.-H.; Chiang, Y.-C.; Liu, M.-C.; Liu, C.W.; Tang, J.-L.; et al. TP53 mutations in de novo acute myeloid leukemia patients: Longitudinal follow-ups show the mutation is stable during disease evolution. Blood Cancer J. 2015, 5, e331. [Google Scholar] [CrossRef]
- Rose, D.; Haferlach, T.; Schnittger, S.; Perglerová, K.; Kern, W.; Haferlach, C. Subtype-specific patterns of molecular mutations in acute myeloid leukemia. Leukemia 2017, 31, 11–17. [Google Scholar] [CrossRef]
- Bullock, A.N.; Fersht, A.R. Rescuing the function of mutant p53. Nat. Rev. Cancer 2001, 1, 68–76. [Google Scholar] [CrossRef]
- Brown, C.J.; Lain, S.; Verma, C.S.; Fersht, A.R.; Lane, D. Awakening guardian angels: Drugging the p53 pathway. Nat. Rev. Cancer 2009, 9, 862–873. [Google Scholar] [CrossRef]
- Bejar, R.; Stevenson, K.; Abdel-Wahab, O.; Galili, N.; Nilsson, B.; Garcia-Manero, G.; Kantarjian, H.; Raza, A.; Levine, R.L.; Neuberg, D.; et al. Clinical Effect of Point Mutations in Myelodysplastic Syndromes. N. Engl. J. Med. 2011, 364, 2496–2506. [Google Scholar] [CrossRef] [PubMed]
- Bejar, R.; Levine, R.; Ebert, B.L. Unraveling the Molecular Pathophysiology of Myelodysplastic Syndromes. J. Clin. Oncol. 2011, 29, 504–515. [Google Scholar] [CrossRef] [PubMed]
- Kastenhuber, E.R.; Lowe, S.W. Putting p53 in Context. Cell 2017, 170, 1062–1078. [Google Scholar] [CrossRef]
- Prokocimer, M.; Molchadsky, A.; Rotter, V. Dysfunctional diversity of p53 proteins in adult acute myeloid leukemia: Projections on diagnostic workup and therapy. Blood 2017, 130, 699–712. [Google Scholar] [CrossRef] [PubMed]
- Brosh, R.; Rotter, V. When mutants gain new powers: News from the mutant p53 field. Nat. Rev. Cancer 2009, 9, 701–713. [Google Scholar] [CrossRef]
- Dearth, L.R.; Qian, H.; Wang, T.; Baroni, T.E.; Zeng, J.; Chen, S.W.; Yi, S.Y.; Brachmann, R.K. Inactive full-length p53 mutants lacking dominant wild-type p53 inhibition highlight loss of heterozygosity as an important aspect of p53 status in human cancers. Carcinogenesis 2007, 28, 289–298. [Google Scholar] [CrossRef]
- Bode, A.M.; Dong, Z. Post-translational modification of p53 in tumorigenesis. Nat. Rev. Cancer 2004, 4, 793–805. [Google Scholar] [CrossRef]
- Appella, E.; Anderson, C.W. Post-translational modifications and activation of p53 by genotoxic stresses. Eur. J. Biochem. 2001, 268, 2764–2772. [Google Scholar] [CrossRef]
- Brooks, C.L.; Gu, W. Ubiquitination, phosphorylation and acetylation: The molecular basis for p53 regulation. Curr. Opin. Cell Biol. 2003, 15, 164–171. [Google Scholar] [CrossRef]
- Sigal, A.; Rotter, V. Oncogenic mutations of the p53 tumor suppressor: The demons of the guardian of the genome. Cancer Res. 2000, 60, 6788–6793. [Google Scholar]
- Lee, C.T.; Capodieci, P.; Osman, I.; Fazzari, M.; Ferrara, J.; I Scher, H.; Cordon-Cardo, C. Overexpression of the cyclin-dependent kinase inhibitor p16 is associated with tumor recurrence in human prostate cancer. Clin. Cancer Res. 1999, 5, 977–983. [Google Scholar]
- Quintás-Cardama, A.; Hu, C.; Qutub, A.; Qiu, Y.H.; Zhang, X.; Post, S.M.; Zhang, N.; Coombes, K.; Kornblau, S.M. p53 pathway dysfunction is highly prevalent in acute myeloid leukemia independent of TP53 mutational status. Leukemia 2016, 31, 1296–1305. [Google Scholar] [CrossRef] [PubMed]
- Friedman, P.N.; Chen, X.; Bargonetti, J.; Prives, C. The p53 protein is an unusually shaped tetramer that binds directly to DNA. Proc. Natl. Acad. Sci. USA 1993, 90, 3319–3323. [Google Scholar] [CrossRef] [PubMed]
- Momand, J.; Wu, H.-H.; Dasgupta, G. MDM2—Master regulator of the p53 tumor suppressor protein. Gene 2000, 242, 15–29. [Google Scholar] [CrossRef]
- Meek, D.W. Mechanisms of switching on p53: A role for covalent modification? Oncogene 1999, 18, 7666–7675. [Google Scholar] [CrossRef][Green Version]
- Lowe, S.W.; Lin, A.W. Apoptosis in cancer. Carcinogenesis 2000, 21, 485–495. [Google Scholar] [CrossRef]
- Sherr, C.J.; Weber, J.D. The ARF/p53 pathway. Curr. Opin. Genet. Dev. 2000, 10, 94–99. [Google Scholar] [CrossRef]
- Carr, A.M. Cell cycle. Piecing together the p53 puzzle. Science 2000, 287, 1765–1766. [Google Scholar] [CrossRef]
- Vogelstein, B.; Lane, D.; Levine, A.J. Surfing the p53 network. Nature 2000, 408, 307–310. [Google Scholar] [CrossRef]
- Olivier, M.; Eeles, R.; Hollstein, M.; Khan, M.A.; Harris, C.C.; Hainaut, P. The IARC TP53 database: New online mutation analysis and recommendations to users. Hum. Mutat. 2002, 19, 607–614. [Google Scholar] [CrossRef]
- Weisz, L.; Oren, M.; Rotter, V. Transcription regulation by mutant p53. Oncogene 2007, 26, 2202–2211. [Google Scholar] [CrossRef]
- Petitjean, A.; Achatz, M.I.; Borresen-Dale, A.L.; Hainaut, P.; Olivier, M. TP53 mutations in human cancers: Functional selection and impact on cancer prognosis and outcomes. Oncogene 2007, 26, 2157–2165. [Google Scholar] [CrossRef]
- Collado, M.; Gil, J.; Efeyan, A.; Guerra, C.; Schuhmacher, A.J.; Barradas, M.; Benguria, A.; Zaballos, A.; Flores, J.M.; Barbacid, M.; et al. Tumour biology: Senescence in premalignant tumours. Nature 2005, 436, 642. [Google Scholar] [CrossRef]
- Schreiber, R.D.; Old, L.J.; Smyth, M.J. Cancer immunoediting: Integrating immunity’s roles in cancer suppression and promotion. Science 2011, 331, 1565–1570. [Google Scholar] [CrossRef]
- Signer, R.; Morrison, S.J. Mechanisms that Regulate Stem Cell Aging and Life Span. Cell Stem Cell 2013, 12, 152–165. [Google Scholar] [CrossRef]
- Welch, J.S.; Ley, T.J.; Link, D.C.; Miller, C.; Larson, D.; Koboldt, D.C.; Wartman, L.D.; Lamprecht, T.L.; Liu, F.; Xia, J.; et al. The origin and evolution of mutations in acute myeloid leukemia. Cell 2012, 150, 264–278. [Google Scholar] [CrossRef]
- Orkin, S.H.; Zon, L.I. Hematopoiesis: An Evolving Paradigm for Stem Cell Biology. Cell 2008, 132, 631–644. [Google Scholar] [CrossRef]
- Bowman, R.L.; Busque, L.; Levine, R.L. Clonal Hematopoiesis and Evolution to Hematopoietic Malignancies. Cell Stem Cell 2018, 22, 157–170. [Google Scholar] [CrossRef]
- Liu, Y.; Elf, S.E.; Miyata, Y.; Sashida, G.; Liu, Y.; Huang, G.; Di Giandomenico, S.; Lee, J.M.; Deblasio, A.; Menendez, S.; et al. p53 regulates hematopoietic stem cell quiescence. Cell Stem Cell 2009, 4, 37–48. [Google Scholar] [CrossRef] [PubMed]
- García-Cao, I.; García-Cao, M.; Martín-Caballero, J.; Criado, L.M.; Klatt, P.; Flores, J.M.; Weill, J.-C.; Blasco, M.A.; Serrano, M. “Super p53” mice exhibit enhanced DNA damage response, are tumor resistant and age normally. Embo. J. 2002, 21, 6225–6235. [Google Scholar] [CrossRef] [PubMed]
- Kawamura, T.; Suzuki, J.; Wang, Y.V.; Menendez, S.; Morera, L.B.; Raya, A.; Wahl, G.M.; Belmonte, J.C.I. Linking the p53 tumour suppressor pathway to somatic cell reprogramming. Nature 2009, 460, 1140–1144. [Google Scholar] [CrossRef] [PubMed]
- Zhao, Z.; Zuber, J.; Diaz-Flores, E.; Lintault, L.; Kogan, S.C.; Shannon, K.; Lowe, S.W. p53 loss promotes acute myeloid leukemia by enabling aberrant self-renewal. Genes Dev. 2010, 24, 1389–1402. [Google Scholar] [CrossRef]
- Hong, H.; Takahashi, K.; Ichisaka, T.; Aoi, T.; Kanagawa, O.; Nakagawa, M.; Okita, K.; Yamanaka, S. Suppression of induced pluripotent stem cell generation by the p53-p21 pathway. Nature 2009, 460, 1132–1135. [Google Scholar] [CrossRef]
- Utikal, J.; Polo, J.M.; Stadtfeld, M.; Maherali, N.; Kulalert, W.; Walsh, R.M.; Khalil, A.; Rheinwald, J.G.; Hochedlinger, K. Immortalization eliminates a roadblock during cellular reprogramming into iPS cells. Nature 2009, 460, 1145–1148. [Google Scholar] [CrossRef]
- Pant, V.; Quintás-Cardama, A.; Lozano, G. The p53 pathway in hematopoiesis: Lessons from mouse models, implications for humans. Blood 2012, 120, 5118–5127. [Google Scholar] [CrossRef]
- Chen, S.; Wang, Q.; Yu, H.; Capitano, M.L.; Vemula, S.; Nabinger, S.C.; Gao, R.; Yao, C.; Kobayashi, M.; Geng, Z.; et al. Mutant p53 drives clonal hematopoiesis through modulating epigenetic pathway. Nat. Commun. 2019, 10, 1–14. [Google Scholar] [CrossRef]
- Rivas, C.I.; Wisniewski, D.; Strife, A.; Perez, A.; Lambek, C.; Bruno, S.; Darzynkiewwicz, Z.; Clarkson, B. Constitutive expression of p53 protein in enriched normal human marrow blast cell populations. Blood 1992, 79, 1982–1986. [Google Scholar] [CrossRef]
- Boregowda, S.V.; Krishnappa, V.; Strivelli, J.; Haga, C.L.; Booker, C.N.; Phinney, N.G. Basal p53 expression is indispensable for mesenchymal stem cell integrity. Cell Death Differ. 2018, 25, 679–692. [Google Scholar] [CrossRef]
- Jung, H.; Kim, M.J.; Kim, D.O.; Kim, W.S.; Yoon, S.-J.; Park, Y.-J.; Yoon, S.R.; Kim, T.-D.; Suh, H.-W.; Yun, S.; et al. TXNIP maintains the hematopoietic cell pool by switching the function of p53 under oxidative stress. Cell Metab. 2013, 18, 75–85. [Google Scholar] [CrossRef]
- Xie, M.; Lu, C.; Wang, J.; McLellan, M.D.; Johnson, K.J.; Wendl, M.C.; McMichael, J.F.; Schmidt, H.K.; Yellapantula, V.; Miller, C.A.; et al. Age-related mutations associated with clonal hematopoietic expansion and malignancies. Nat. Med. 2014, 20, 1472–1478. [Google Scholar] [CrossRef]
- Young, A.L.; Challen, G.A.; Birmann, B.; Druley, T.E. Clonal haematopoiesis harbouring AML-associated mutations is ubiquitous in healthy adults. Nat. Commun. 2016, 7, 12484. [Google Scholar] [CrossRef]
- Jaiswal, S.; Fontanillas, P.; Flannick, J.; Manning, A.; Grauman, P.V.; Mar, B.G.; Lindsley, R.C.; Mermel, C.H.; Burtt, N.; Chavez, A.; et al. Age-related clonal hematopoiesis associated with adverse outcomes. N. Engl. J. Med. 2014, 371, 2488–2498. [Google Scholar] [CrossRef] [PubMed]
- Genovese, G.; Kähler, A.K.; Handsaker, R.E.; Lindberg, J.; Rose, S.A.; Bakhoum, S.F.; Chambert, K.; Mick, E.; Neale, B.M.; Fromer, M.; et al. Clonal hematopoiesis and blood-cancer risk inferred from blood DNA sequence. N. Engl. J. Med. 2014, 371, 2477–2487. [Google Scholar] [CrossRef] [PubMed]
- Desai, P.; Trinchant, N.M.; Savenkov, O.; Simon, M.S.; Cheang, G.; Lee, S.; Samuel, M.; Ritchie, E.K.; Guzman, M.L.; Ballman, K.V.; et al. Somatic mutations precede acute myeloid leukemia years before diagnosis. Nat. Med. 2018, 24, 1015–1023. [Google Scholar] [CrossRef]
- Corces-Zimmerman, M.R.; Hong, W.-J.; Weissman, I.L.; Medeiros, B.C.; Majeti, R. Preleukemic mutations in human acute myeloid leukemia affect epigenetic regulators and persist in remission. Proc. Natl. Acad. Sci. USA 2014, 111, 2548–2553. [Google Scholar] [CrossRef]
- Abelson, S.; Collord, G.; Ng, S.W.K.; Weissbrod, O.; Cohen, N.M.; Niemeyer, E.; Barda, N.; Zuzarte, P.C.; Heisler, L.; Sundaravadanam, Y.; et al. Prediction of acute myeloid leukaemia risk in healthy individuals. Nature 2018, 559, 400–404. [Google Scholar] [CrossRef]
- Papaemmanuil, E.; Gerstung, M.; Bullinger, L.; Gaidzik, V.I.; Paschka, P.; Roberts, N.D.; Potter, N.E.; Heuser, M.; Thol, F.; Bolli, N.; et al. Genomic Classification and Prognosis in Acute Myeloid Leukemia. N. Engl. J. Med. 2016, 374, 2209–2221. [Google Scholar] [CrossRef]
- Zhang, J.; Kong, G.; Rajagopalan, A.; Lu, L.; Song, J.; Hussaini, X.Z.; Ranheim, E.A.; Liu, Y.; Wang, J. p53−/− synergizes with enhanced NrasG12D signaling to transform megakaryocyte-erythroid progenitors in acute myeloid leukemia. Blood 2017, 129, 358–370. [Google Scholar] [CrossRef]
- Shen, Y.; Zhu, Y.-M.; Fan, X.; Shi, J.-Y.; Wang, Q.-R.; Yan, X.-J.; Gu, Z.-H.; Wang, Y.-Y.; Chen, B.; Jiang, C.-L.; et al. Gene mutation patterns and their prognostic impact in a cohort of 1185 patients with acute myeloid leukemia. Blood 2011, 118, 5593–5603. [Google Scholar] [CrossRef]
- Sabapathy, K.; Lane, D. Therapeutic targeting of p53: All mutants are equal, but some mutants are more equal than others. Nat. Rev. Clin. Oncol. 2017, 15, 13–30. [Google Scholar] [CrossRef]
- Bieging, K.T.; Mello, S.S.; Attardi, L.D. Unravelling mechanisms of p53-mediated tumour suppression. Nat. Rev. Cancer 2014, 14, 359–370. [Google Scholar] [CrossRef]
- Lee, M.K.; Teoh, W.W.; Phang, B.H.; Tong, W.M.; Wang, Z.Q.; Sabapathy, K. Cell-type, dose, and mutation-type specificity dictate mutant p53 functions in vivo. Cancer Cell 2012, 22, 751–764. [Google Scholar] [CrossRef] [PubMed]
- Hanel, W.; Marchenko, N.D.; Xu, S.; Yu, S.X.; Weng, W.; Moll, U.M. Two hot spot mutant p53 mouse models display differential gain of function in tumorigenesis. Cell Death Differ. 2013, 20, 898–909. [Google Scholar] [CrossRef] [PubMed]
- Suzuki, S.; Tsutsumi, S.; Chen, Y.; Ozeke, C.; Kawase, T.; Aburatani, H.; Ohki, R. Identification and characterization of the binding sequences and target genes of p53 lacking the 1st transactivation domain. Cancer Sci. 2020, 111, 451–466. [Google Scholar] [CrossRef]
- Candau, R.; Scolnick, D.M.; Darpino, P.; Ying, C.Y.; Halazonetis, T.D.; Berger, S. Two tandem and independent sub-activation domains in the amino terminus of p53 require the adaptor complex for activity. Oncogene 1997, 15, 807–816. [Google Scholar] [CrossRef]
- Kussie, P.H.; Gorina, S.; Marechal, V.; Elenbaas, B.; Moreau, J.; Levine, A.J.; Pavletich, N.P. Structure of the MDM2 oncoprotein bound to the p53 tumor suppressor transactivation domain. Science 1996, 274, 948–953. [Google Scholar] [CrossRef]
- Thomaston, J.; Alfonso-Prieto, M.; Woldeyes, R.A.; Fraser, J.; Klein, M.L.; Fiorin, G.; DeGrado, W.F. High-resolution structures of the M2 channel from influenza A virus reveal dynamic pathways for proton stabilization and transduction. Proc. Natl. Acad. Sci. USA 2015, 112, 14260–14265. [Google Scholar] [CrossRef]
- Phang, B.H.; Othman, R.; Bougeard, G.; Chia, R.H.; Frebourg, T.; Tang, C.L.; Cheah, P.Y.; Sabapathy, K. Amino-terminal p53 mutations lead to expression of apoptosis proficient p47 and prognosticate better survival, but predispose to tumorigenesis. Proc. Natl. Acad. Sci. USA 2015, 112, E6349–E6358. [Google Scholar] [CrossRef]
- Courtois, S.; Verhaegh, G.; North, S.; Luciani, M.-G.; Lassus, P.; Hibner, U.; Oren, M.; Hainaut, P. DeltaN-p53, a natural isoform of p53 lacking the first transactivation domain, counteracts growth suppression by wild-type p53. Oncogene 2002, 21, 6722–6728. [Google Scholar] [CrossRef]
- Ohki, R.; Kawase, T.; Ohta, T.; Ichikawa, H.; Taya, Y. Dissecting functional roles of p53 N-terminal transactivation domains by microarray expression analysis. Cancer Sci. 2006, 98, 189–200. [Google Scholar] [CrossRef]
- Yin, Y.; Stephen, C.W.; Luciani, M.G.; Fåhraeus, R. p53 Stability and activity is regulated by Mdm2-mediated induction of alternative p53 translation products. Nat. Cell Biol. 2002, 4, 462–467. [Google Scholar] [CrossRef]
- Hofstetter, G.; Berger, A.; Berger, R.; Zorić, A.; Braicu, E.I.; Reimer, D.; Fiegl, H.; Marth, C.; Zeimet, A.G.; Ulmer, H.; et al. The N-terminally truncated p53 isoform Δ40p53 influences prognosis in mucinous ovarian cancer. Int. J. Gynecol. Cancer 2012, 22, 372–379. [Google Scholar] [CrossRef]
- Olive, K.; Tuveson, D.A.; Ruhe, Z.C.; Yin, B.; Willis, N.A.; Bronson, R.T.; Crowley, D.; Jacks, T. Mutant p53 gain of function in two mouse models of Li-Fraumeni syndrome. Cell 2004, 119, 847–860. [Google Scholar] [CrossRef]
- Terada, K.; Yamaguchi, H.; Ueki, T.; Usuki, K.; Kobayashi, Y.; Tajika, K.; Gomi, S.; Kurosawa, S.; Miyadera, K.; Tokura, T.; et al. Full-length mutation search of the TP53 gene in acute myeloid leukemia has increased significance as a prognostic factor. Ann. Hematol. 2018, 97, 51–61. [Google Scholar] [CrossRef] [PubMed]
- Kato, S.; Han, S.-Y.; Liu, W.; Otsuka, K.; Shibata, H.; Kanamaru, R.; Ishioka, C. Understanding the function-structure and function-mutation relationships of p53 tumor suppressor protein by high-resolution missense mutation analysis. Proc. Natl. Acad. Sci. USA 2003, 100, 8424–8429. [Google Scholar] [CrossRef]
- Donehower, L.A.; Harvey, M.; Slagle, B.L.; McArthur, M.J.; Jr, C.A.M.; Butel, J.; Bradley, A. Mice deficient for p53 are developmentally normal but susceptible to spontaneous tumours. Nature 1992, 356, 215–221. [Google Scholar] [CrossRef]
- Varley, J.M. Germline TP53 mutations and Li-Fraumeni syndrome. Hum. Mutat. 2003, 21, 313–320. [Google Scholar] [CrossRef]
- Kemp, C.J.; Wheldon, T.; Balmain, A. p53-deficient mice are extremely susceptible to radiation-induced tumorigenesis. Nat. Genet. 1994, 8, 66–69. [Google Scholar] [CrossRef]
- Freed-Pastor, W.A.; Prives, C. Mutant p53: One name, many proteins. Genes Dev. 2012, 26, 1268–1286. [Google Scholar] [CrossRef]
- Valente, L.J.; Gray, D.H.; Michalak, E.M.; Pinon-Hofbauer, J.; Egle, A.; Scott, C.L.; Janic, A.; Strasser, A. p53 efficiently suppresses tumor development in the complete absence of its cell-cycle inhibitory and proapoptotic effectors p21, Puma, and Noxa. Cell Rep. 2013, 3, 1339–1345. [Google Scholar] [CrossRef]
- Inga, A.; Cresta, S.; Monti, P.; Aprile, A.; Scott, G.; Abbondandolo, A.; Iggo, R.; Fronza, G.; Challa, A.; Rao, D.R.; et al. Simple identification of dominant p53 mutants by a yeast functional assay. Carcinogenesis 1997, 18, 2019–2021. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Jia, L.Q.; Osada, M.; Ishioka, C.; Gamo, M.; Ikaw, S.; Suzuki, T.; Shimodaira, H.; Niitani, T.; Kudo, T.; Akiyama, M.; et al. Screening the p53 status of human cell lines using a yeast functional assay. Mol Carcinog. 1997, 19, 243–253. [Google Scholar] [CrossRef]
- Pirollo, K.F.; Bouker, K.B.; Chang, E.H. Does p53 status influence tumor response to anticancer therapies? Anticancer. Drugs 2000, 11, 419–432. [Google Scholar] [CrossRef] [PubMed]
- Lu, C.; El-Deiry, W.S. Targeting p53 for enhanced radio- and chemo-sensitivity. Apoptosis 2009, 14, 597–606. [Google Scholar] [CrossRef] [PubMed]
- Vousden, K.H.; Lu, X. Live or let die: The cell’s response to p53. Nat. Rev. Cancer 2002, 2, 594–604. [Google Scholar] [CrossRef]
- Milner, J.; Medcalf, E. Cotranslation of activated mutant p53 with wild type drives the wild-type p53 protein into the mutant conformation. Cell 1991, 65, 765–774. [Google Scholar] [CrossRef]
- Terzian, T.; Suh, Y.-A.; Iwakuma, T.; Post, S.M.; Neumann, M.; Lang, G.A.; Van Pelt, C.S.; Lozano, G. The inherent instability of mutant p53 is alleviated by Mdm2 or p16INK4a loss. Genes Dev. 2008, 22, 1337–1344. [Google Scholar] [CrossRef]
- Chan, W.M.; Siu, W.Y.; Lau, A.; Poon, R.Y. C How many mutant p53 molecules are needed to inactivate a tetramer? Mol. Cell Biol. 2004, 24, 3536–3551. [Google Scholar] [CrossRef]
- Wang, Y.; Suh, Y.-A.; Fuller, M.Y.; Jackson, J.; Xiong, S.; Terzian, T.; Quintás-Cardama, A.; Bankson, J.; El-Naggar, A.K.; Lozano, G. Restoring expression of wild-type p53 suppresses tumor growth but does not cause tumor regression in mice with a p53 missense mutation. J. Clin. Invest. 2011, 121, 893–904. [Google Scholar] [CrossRef]
- Muller, P.A.J.; Vousden, K.H. p53 mutations in cancer. Nat. Cell Biol. 2013, 15, 2–8. [Google Scholar] [CrossRef]
- Sabapathy, K. The Contrived Mutant p53 Oncogene - Beyond Loss of Functions. Front. Oncol. 2015, 5, 276. [Google Scholar] [CrossRef]
- Bergamaschi, D.; Gasco, M.; Hiller, L.; Sullivan, A.; Syed, N.; Trigiante, G.; Yulug, I.; Merlano, M.; Numico, G.; Comino, A.; et al. p53 polymorphism influences response in cancer chemotherapy via modulation of p73-dependent apoptosis. Cancer Cell 2003, 3, 387–402. [Google Scholar] [CrossRef]
- Zhu, J.; Sammons, M.A.; Donahue, G.; Dou, Z.; Vedadi, M.; Getlik, M.; Barsyte-Lovejoy, D.; Al-Awar, R.; Katona, B.W.; Shilatifard, A.; et al. Gain-of-function p53 mutants co-opt chromatin pathways to drive cancer growth. Nature 2015, 525, 206–211. [Google Scholar] [CrossRef] [PubMed]
- Bossi, G.; Lapi, E.; Strano, S.; Rinaldo, C.; Blandino, G.; Sacchi, A. Mutant p53 gain of function: Reduction of tumor malignancy of human cancer cell lines through abrogation of mutant p53 expression. Oncogene 2006, 25, 304–309. [Google Scholar] [CrossRef] [PubMed]
- Vikhanskaya, F.; Lee, M.K.; Mazzoletti, M.; Broggini, M.; Sabapathy, K. Cancer-derived p53 mutants suppress p53-target gene expression--potential mechanism for gain of function of mutant p53. Nucleic Acids Res. 2007, 35, 2093–2104. [Google Scholar] [CrossRef]
- Blandino, G.; Levine, A.J.; Oren, M. Mutant p53 gain of function: Differential effects of different p53 mutants on resistance of cultured cells to chemotherapy. Oncogene 1999, 18, 477–485. [Google Scholar] [CrossRef]
- Di Agostino, S.; Cortese, G.; Monti, O.; Dell’Orso, S.; Sacchi, A.; Eisenstein, M.; Citro, G.; Strano, S.; Blandino, G. The disruption of the protein complex mutantp53/p73 increases selectively the response of tumor cells to anticancer drugs. Cell Cycle 2008, 7, 3440–3447. [Google Scholar] [CrossRef]
- E Lomax, M.; Barnes, D.M.; Hupp, T.R.; Picksley, S.M.; Camplejohn, R.S. Characterization of p53 oligomerization domain mutations isolated from Li-Fraumeni and Li-Fraumeni like family members. Oncogene 1998, 17, 643–649. [Google Scholar] [CrossRef]
- Plummer, S.J.; Santibáñez-Koref, M.; Kurosaki, T.; Liao, S.; Noble, B.; Fain, P.R.; Anton-Culver, H.; Casey, G. A germline 2.35 kb deletion of p53 genomic DNA creating a specific loss of the oligomerization domain inherited in a Li-Fraumeni syndrome family. Oncogene 1994, 9, 3273–3280. [Google Scholar]
- DiGiammarino, E.L.; Lee, A.S.; Cadwell, C.; Zhang, W.; Bothner, B.; Ribeiro, R.C.; Zambetti, G.; Kriwacki, R.W. A novel mechanism of tumorigenesis involving pH-dependent destabilization of a mutant p53 tetramer. Nat. Struct. Biol. 2002, 9, 12–16. [Google Scholar] [CrossRef]
- Christiansen, D.H.; Andersen, M.K.; Pedersen-Bjergaard, J. Mutations with Loss of Heterozygosity of p53 Are Common in Therapy-Related Myelodysplasia and Acute Myeloid Leukemia After Exposure to Alkylating Agents and Significantly Associated With Deletion or Loss of 5q, a Complex Karyotype, and a Poor Prognosis. J. Clin. Oncol. 2001, 19, 1405–1413. [Google Scholar] [CrossRef]
- Pedersenbjergaard, J.; Andersen, M.T.; Christiansen, D.H. Genetics of therapy-related myelodysplasia and acute myeloid leukemia. Leukemia 2008, 22, 240–248. [Google Scholar] [CrossRef]
- Ley, T.J.; Miller, C.; Ding, L.; Raphael, B.J.; Mungall, A.J.; Robertson, A.G.; Hoadley, K.; Triche, T.J.; Laird, P.W.; Batty, J.D.; et al. Genomic and epigenomic landscapes of adult de novo acute myeloid leukemia. N. Engl. J. Med. 2013, 368, 2059–2074. [Google Scholar]
- Bally, C.; Adès, L.; Renneville, A.; Sebert, M.; Eclache, V.; Preudhomme, C.; Mozziconacci, M.-J.; de The, H.; Lehmann-Che, J.; Fenaux, P. Prognostic value of TP53 gene mutations in myelodysplastic syndromes and acute myeloid leukemia treated with azacitidine. Leuk. Res. 2014, 38, 751–755. [Google Scholar] [CrossRef]
- Laurie, C.C.; A Laurie, C.; Rice, K.; Doheny, K.F.; Zelnick, L.; McHugh, C.P.; Ling, H.; Hetrick, K.N.; Pugh, E.W.; Amos, C.; et al. Detectable clonal mosaicism from birth to old age and its relationship to cancer. Nat. Genet. 2012, 44, 642–650. [Google Scholar] [CrossRef]
- Welch, J.S. Patterns of mutations in TP53 mutated AML. Best Pr. Res. Clin. Haematol. 2018, 31, 379–383. [Google Scholar] [CrossRef]
- Rücker, F.G.; Dolnik, A.; Blätte, T.J.; Teleanu, V.; Ernst, A.; Thol, F.; Heuser, M.; Ganser, A.; Döhner, H.; Döhner, K.; et al. Chromothripsis is linked to TP53 alteration, cell cycle impairment, and dismal outcome in acute myeloid leukemia with complex karyotype. Haematologica 2018, 103, e17–e20. [Google Scholar] [CrossRef]
- Svobodova, K.; Zemanova, Z.; Lhotska, H.; Novakova, M.; Podskalska, L.; Belickova, M.; Březinová, J.; Sarova, I.; Izakova, S.; Lizcova, L.; et al. Copy number neutral loss of heterozygosity at 17p and homozygous mutations of TP53 are associated with complex chromosomal aberrations in patients newly diagnosed with myelodysplastic syndromes. Leuk. Res. 2016, 42, 7–12. [Google Scholar] [CrossRef]
- Prochazka, K.T.; Pregartner, G.; Rücker, F.G.; Heitzer, E.; Pabst, G.; Wölfler, A.; Zebisch, A.; Berghold, A.; Döhner, K.; Sill, H. Clinical implications of subclonal TP53 mutations in acute myeloid leukemia. Haematologica 2019, 104, 516–523. [Google Scholar] [CrossRef]
- Sallman, D.A.; Komrokji, R.; Vaupel, C.; Cluzeau, T.; Geyer, S.M.; McGraw, K.L.; Al Ali, N.H.; Lancet, J.; McGinniss, M.J.; Nahas, S.; et al. Impact of TP53 mutation variant allele frequency on phenotype and outcomes in myelodysplastic syndromes. Leukemia 2016, 30, 666–673. [Google Scholar] [CrossRef]
- Dutta, S.; Pregartner, G.; Rücker, F.G.; Heitzer, E.; Zebisch, A.; Bullinger, L.; Berghold, A.; Döhner, K.; Sill, H. Functional Classification of TP53 Mutations in Acute Myeloid Leukemia. Cancers 2020, 12, 637. [Google Scholar] [CrossRef]
- Short, N.J.; Montalban-Bravo, G.; Hwang, H.; Ning, J.; Franquiz, M.J.; Kanagal-Shamanna, R.; Patel, K.P.; Dinardo, C.D.; Ravandi, F.; Garcia-Manero, G.; et al. Prognostic and therapeutic impacts of mutant TP53 variant allelic frequency in newly diagnosed acute myeloid leukemia. Blood Adv. 2020, 4, 5681–5689. [Google Scholar] [CrossRef] [PubMed]
- Martinez-Høyer, S.; Docking, R.; Chan, S.; Jadersten, M.; Parker, J.; Karsan, A. Mechanisms of Resistance to Lenalidomide in Del(5q) Myelodysplastic Syndrome Patients. Blood 2015, 126, 5228. [Google Scholar] [CrossRef]
- Mossner, M.; Jann, J.-C.; Nowak, D.; Platzbercker, U.; Giagounidis, A.; Gotze, K.; Letsch, A.; Shirneshan, K.; Braulke, F. Prevalence, clonal dynamics and clinical impact of TP53 mutations in patients with myelodysplastic syndrome with isolated deletion (5q) treated with lenalidomide: Results from a prospective multicenter study of the german MDS study group (GMDS). Leukemia 2016, 30, 1956–1959. [Google Scholar] [CrossRef] [PubMed]
- Christian, S.; Scharenberg, C.; Giai, V.; Pellagatti, A.; Saft, L.; Dimitriou, M.; Jansson, M.; Jädersten, M.; Grandien, A.; Douagi, I.; et al. Progression in patients with low- and intermediate-1-risk del(5q) myelodysplastic syndromes is predicted by a limited subset of mutations. Haematologica 2017, 102, 498–508. [Google Scholar] [CrossRef]
- Lodé, L.; Ménard, A.; Flet, L.; Richebourg, S.; Loirat, M.; Eveillard, M.; Le Bris, Y.; Godon, C.; Theisen, O.; Gagez, A.L. Emergence and evolution of TP53 mutations are key features of disease progression in myelodysplastic patients with lower-risk del (5q) treated with lenalidomide. Haematologica 2018, 103, e143–e146. [Google Scholar] [CrossRef]
- Bernard, E.; Nannya, Y.; Yoshizato, T.; Hasserjian, R.P.; Saiki, R.; Shiozawa, Y.; Devlin, S.M.; Tuechler, H.; Sarian, A.; Malcovati, L.; et al. TP53 State Dictates Genome Stability, Clinical Presentation and Outcomes in Myelodysplastic Syndromes. Blood 2019, 134, 675. [Google Scholar] [CrossRef]
- Welch, J.S.; Petti, A.A.; Miller, C.; Fronick, C.C.; O’Laughlin, M.; Fulton, R.S.; Wilson, R.K.; Baty, J.D.; Duncavage, E.J.; Tandon, B.; et al. TP53 and Decitabine in Acute Myeloid Leukemia and Myelodysplastic Syndromes. N. Engl. J. Med. 2016, 375, 2023–2036. [Google Scholar] [CrossRef]
- Yi, L.; Sun, Y.; Levine, A. Selected drugs that inhibit DNA methylation can preferentially kill p53 deficient cells. Oncotarget 2014, 5, 8924–8936. [Google Scholar] [CrossRef]
- Short, N.J.; Kantarjian, H.M.; Loghavi, S.; Huang, X.; Qiao, W.; Borthakur, G.; Kadia, T.M.; Daver, N.; Ohanian, M.; Dinardo, C.D.; et al. Treatment with a 5-day versus a 10-day schedule of decitabine in older patients with newly diagnosed acute myeloid leukaemia: A randomised phase 2 trial. Lancet Haematol. 2019, 6, e29–e37. [Google Scholar] [CrossRef]
- Anderson, M.A.; Deng, J.; Seymour, J.F.; Tam, C.; Kim, S.Y.; Fein, J.; Yu, L.; Brown, J.R.; Westerman, D.; Si, E.G.; et al. The BCL2 selective inhibitor venetoclax induces rapid onset apoptosis of CLL cells in patients via a TP53-independent mechanism. Blood 2016, 127, 3215–3224. [Google Scholar] [CrossRef]
- Aldoss, I.; Yang, D.; Aribi, A.; Ali, H.; Sandhu, K.; Al Malki, M.M.; Mei, M.; Salhotra, A.; Khaled, S.; Nakamura, R.; et al. Efficacy of the combination of venetoclax and hypomethylating agents in relapsed/refractory acute myeloid leukemia. Haematologica 2018, 103, e404–e407. [Google Scholar] [CrossRef]
- Dinardo, C.D.; Pratz, K.; Pullarkat, V.; Jonas, B.; Arellano, M.; Becker, P.S.; Frankfurt, O.; Konopleva, M.; Wei, A.H.; Kantarjian, H.M.; et al. Venetoclax combined with decitabine or azacitidine in treatment-naive, elderly patients with acute myeloid leukemia. Blood 2019, 133, 7–17. [Google Scholar] [CrossRef]
- Schiffer, C.A. Promoting Apoptosis with Venetoclax—A Benefit for Older Patients with AML. N. Engl. J. Med. 2020, 383, 677–679. [Google Scholar] [CrossRef]
- DiNardo, C.D.; Tiong, I.S.; Quaglieri, A.; MacRaild, S.; Loghavi, S.; Brown, F.C.; Thijssen, R.; Pomilio, G.; Ivey, A.; Salmon, J.M.; et al. Molecular patterns of response and treatment failure after frontline venetoclax combinations in older patients with AML. Blood 2020, 135, 791–803. [Google Scholar] [CrossRef]
- Chen, X.; Glytsou, C.; Zhou, H.; Narang, S.; Reyna, D.E.; Lopez, A.; Sakellaropoulos, T.; Gong, Y.; Kloetgen, A.; Yap, Y.S.; et al. Targeting Mitochondrial Structure Sensitizes Acute Myeloid Leukemia to Venetoclax Treatment. Cancer Discov. 2019, 9, 890–909. [Google Scholar] [CrossRef]
- Nechiporuk, T.; Kurtz, S.E.; Nikolova, O.; Liu, T.; Jones, C.L.; D’Alessandro, A.; Culp-Hill, R.; D’Almeida, A.; Joshi, S.; Rosenberg, M.; et al. The TP53 Apoptotic Network Is a Primary Mediator of Resistance to BCL2 Inhibition in AML Cells. Cancer Discov. 2019, 9, 910–925. [Google Scholar] [CrossRef]
- Bejar, R.; Stevenson, K.E.; Caughey, B.; Lindsley, C.; Mar, B.; Stojanov, P.; Getz, G.; Steensma, D.P.; Ritz, J.; Soiffer, R.; et al. Somatic mutations predict poor outcome in patients with myelodysplastic syndrome after hematopoietic stem-cell transplantation. J. Clin. Oncol. 2014, 32, 2691–2698. [Google Scholar] [CrossRef]
- Lambert, J.M.; Gorzov, P.; Veprintsev, D.; Söderqvist, M.; Segerbäck, D.; Bergman, J.; Fersht, A.R.; Hainaut, P.; Wiman, K.G.; Bykov, V.N. PRIMA-1 reactivates mutant p53 by covalent binding to the core domain. Cancer Cell 2009, 15, 376–388. [Google Scholar] [CrossRef]
- Zhang, Q.; Bykov, V.J.N.; Wiman, K.G.; Zawacka-Pankau, J. APR-246 reactivates mutant p53 by targeting cysteines 124 and 277. Cell Death Dis. 2018, 9, 1–12. [Google Scholar] [CrossRef]
- Tessoulin, B.; Descamps, G.; Moreau, P.; Maïga, S.; Lodé, L.; Godon, C.; Lambot, S.M.; Oullier, T.; le Gouill, S.; Amiot, M.; et al. PRIMA-1Met induces myeloma cell death independent of p53 by impairing the GSH/ROS balance. Blood 2014, 124, 1626–1636. [Google Scholar] [CrossRef]
- Sallman, D.A.; DeZern, A.E.; Garcia-Manero, G.; Steensma, D.P.; Roboz, G.J.; Sekeres, M.A.; Cluzeau, T.; Sweet, K.; McLemore, A.; McGraw, K.; et al. Phase 2 Results of APR-246 and Azacitidine (AZA) in Patients with TP53 mutant Myelodysplastic Syndromes (MDS) and Oligoblastic Acute Myeloid Leukemia (AML). Blood 2019, 134, 676. [Google Scholar] [CrossRef]
- Cluzeau, T.; Sebert, M.; Rahmé, R.; Cuzzubbo, S.; Lehmann-Che, J.; Madelaine, I.; Peterlin, P.; Bève, B.; Attalah, H.; Chermat, F.; et al. Eprenetapopt Plus Azacitidine in TP53-Mutated Myelodysplastic Syndromes and Acute Myeloid Leukemia: A Phase II Study by the Groupe Francophone des Myélodysplasies (GFM). J. Clin. Oncol. 2021, 39, 1575–1583. [Google Scholar] [CrossRef]
- Maslah, N.; Salomao, N.; Drevon, L.; Verger, E.; Partouche, N.; Ly, P.; Aubin, P.; Naoui, N.; Schlageter, M.H.; Bally, C.; et al. Synergistic effects of PRIMA-1(Met) (APR-246) and 5-azacitidine in TP53-mutated myelodysplastic syndromes and acute myeloid leukemia. Haematologica 2020, 105, 1539–1551. [Google Scholar] [CrossRef]
- Vassilev, L.T.; Vu, B.T.; Graves, B.; Carvajal, D.; Podlaski, F.; Filipovic, Z.; Kong, N.; Kammlott, U.; Lukacs, C.; Klein, C.; et al. In vivo activation of the p53 pathway by small-molecule antagonists of MDM2. Science 2004, 303, 844–848. [Google Scholar] [CrossRef]
- Montesinos, P.; Beckermann, B.M.; Catalani, O.; Esteve, J.; Gamel, K.; Konopleva, M.Y.; Martinelli, G.; Monnet, A.; Papayannidis, C.; Park, A.; et al. MIRROS: A randomized, placebo-controlled, Phase III trial of cytarabine ± idasanutlin in relapsed or refractory acute myeloid leukemia. Future Oncol. 2020, 16, 807–815. [Google Scholar] [CrossRef]
- Ding, Q.; Zhang, Z.; Liu, J.-J.; Jiang, N.; Zhang, J.; Ross, T.M.; Chu, X.-J.; Bartkovitz, D.; Podlaski, F.; Janson, C.; et al. Discovery of RG7388, a potent and selective p53-MDM2 inhibitor in clinical development. J. Med. Chem. 2013, 56, 5979–5983. [Google Scholar] [CrossRef]
- Yee, K.; Martinelli, G.; Vey, N.; Dickinson, M.J.; Seiter, K.; Assouline, S.; Drummond, M.; Yoon, S.-S.; Kasner, M.; Lee, J.-H.; et al. Phase 1/1b Study of RG7388, a Potent MDM2 Antagonist, in Acute Myelogenous Leukemia (AML) Patients (Pts). Blood 2014, 124, 116. [Google Scholar] [CrossRef]
- Martinelli, G.; Pappayannidis, C.; Yee, K.; Vey, N.; Drummond, M.; Kelly, K. Phase 1b Results of Idasanutlin + Cytarabine (ara-c) in Acute Myeloid Leukemia (AML) Patients (PTS). Eur. Hematol. Assoc. 2016, 101, 187. [Google Scholar]
- Daver, N.G.; Garcia, J.S.; Jonas, B.A.; Kelly, K.R.; Assouline, S.; Brandwein, J.M.; Fenaux, P.; Olin, R.L.; Martinelli, G.; Paolini, S.; et al. Updated Results from the Venetoclax (Ven) in Combination with Idasanutlin (Idasa) Arm of a Phase 1b Trial in Elderly Patients (Pts) with Relapsed or Refractory (R/R) AML Ineligible for Cytotoxic Chemotherapy. Blood 2019, 134, 229. [Google Scholar] [CrossRef]
- Rew, Y.; Sun, D. Discovery of a Small Molecule MDM2 Inhibitor (AMG 232) for Treating Cancer. J. Med. Chem. 2014, 57, 6332–6341. [Google Scholar] [CrossRef]
- Erba, H.P.; Becker, P.S.; Shami, P.J.; Grunwald, M.R.; Flesher, D.L.; Zhu, M.; Rasmussen, E.; Henary, H.A.; Anderson, A.A.; Wang, E.S. Phase 1b study of the MDM2 inhibitor AMG 232 with or without trametinib in relapsed/refractory acute myeloid leukemia. Blood Adv. 2019, 3, 1939–1949. [Google Scholar] [CrossRef] [PubMed]
- Carvajal, L.A.; Ben Neriah, D.; Senecal, A.; Benard, L.; Thiruthuvanathan, V.; Yatsenko, T.; Narayanagari, S.-R.; Wheat, J.C.; Todorova, T.I.; Mitchell, K.; et al. Dual inhibition of MDMX and MDM2 as a therapeutic strategy in leukemia. Sci. Transl. Med. 2018, 10, eaao3003. [Google Scholar] [CrossRef] [PubMed]
- Sallman, D.A.; Borate, U.; Cull, E.H.; Donnellan, W.B.; Komrokji, R.S.; Steidl, U.G.; Corvez, M.M.; Payton, M.; Annis, D.A.; Pinchasik, D.; et al. Phase 1/1b Study of the Stapled Peptide ALRN-6924, a Dual Inhibitor of MDMX and MDM2, As Monotherapy or in Combination with Cytarabine for the Treatment of Relapsed/Refractory AML and Advanced MDS with TP53 Wild-Type. Blood 2018, 132, 4066. [Google Scholar] [CrossRef]
- Jaiswal, S.; Jamieson, C.H.; Pang, W.W.; Park, C.Y.; Chao, M.P.; Majeti, R.; Traver, D.; Van Rooijen, N.; Weissman, I.L. CD47 is upregulated on circulating hematopoietic stem cells and leukemia cells to avoid phagocytosis. Cell 2009, 138, 271–285. [Google Scholar] [CrossRef]
- Sallman, D.A.; Asch, A.S.; Al Malki, M.M.; Lee, D.J.; Donnellan, W.B.; Marcucci, G.; Kambhampati, S.; Daver, N.G.; Garcia-Manero, G.; Komrokji, R.S.; et al. The first-in-class anti-CD47 antibody magrolimab (5F9) in combination with azacitidine is effective in MDS and AML patients: Ongoing phase 1b results. In Proceedings of the American Society of Hematology Annual Meeting Oral Presentation, Washington, DC, USA, 5–8 December 2020. [Google Scholar]
- Yan, W.; Zhang, Y.; Zhang, J.; Liu, S.; Cho, S.J.; Chen, X. Mutant p53 protein is targeted by arsenic for degradation and plays a role in arsenic-mediated growth suppression. J. Biol. Chem. 2011, 286, 17478–17486. [Google Scholar] [CrossRef]
- Yan, W.; Jung, Y.-S.; Zhang, Y.; Chen, X. Arsenic trioxide reactivates proteasome-dependent degradation of mutant p53 protein in cancer cells in part via enhanced expression of Pirh2 E3 ligase. PLoS ONE 2014, 9, e103497. [Google Scholar] [CrossRef]
- Parrales, A.; Ranjan, A.; Iyer, S.; Padhye, S.; Weir, S.J.; Roy, A.; Iwakuma, T. DNAJA1 controls the fate of misfolded mutant p53 through the mevalonate pathway. Nat. Cell Biol. 2016, 18, 1233–1243. [Google Scholar] [CrossRef]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).