Narrative Review of New Insight into the Influence of the COVID-19 Pandemic on Cardiovascular Care
Abstract
1. Introduction
2. Materials and Methods
3. Context
4. The Impact of COVID-19 Infection on the Cardiovascular System
4.1. Thromboembolic Condition
4.2. Mechanisms of Coagulopathy Linked with COVID-19
4.3. COVID-19 and Peripheral Venous Diseases
4.4. Cardiovascular Implications of ACE2 Being the SARS-CoV-2 Receptor
4.5. Thromboprophylaxis for the COVID-19
5. COVID-19 Cardiovascular Symptoms
5.1. Ischemia and Non-Ischemia-Related Cardiac Injury
5.2. Cardiomyopathies and Myocarditis
5.3. Arrhythmia and Abrupt Cardiac Death
5.4. Heart Failure
6. Solutions
6.1. Management of Cardiovascular Disease in COVID-19-Exposed Patients
6.2. The Possibility of Using Renin–Angiotensin System Antagonists as a Treatment in COVID-19 Pneumonia
6.3. Additional COVID-19 Therapy Suggestions
6.4. Transplantation of the Heart with Mechanical Circulatory Support
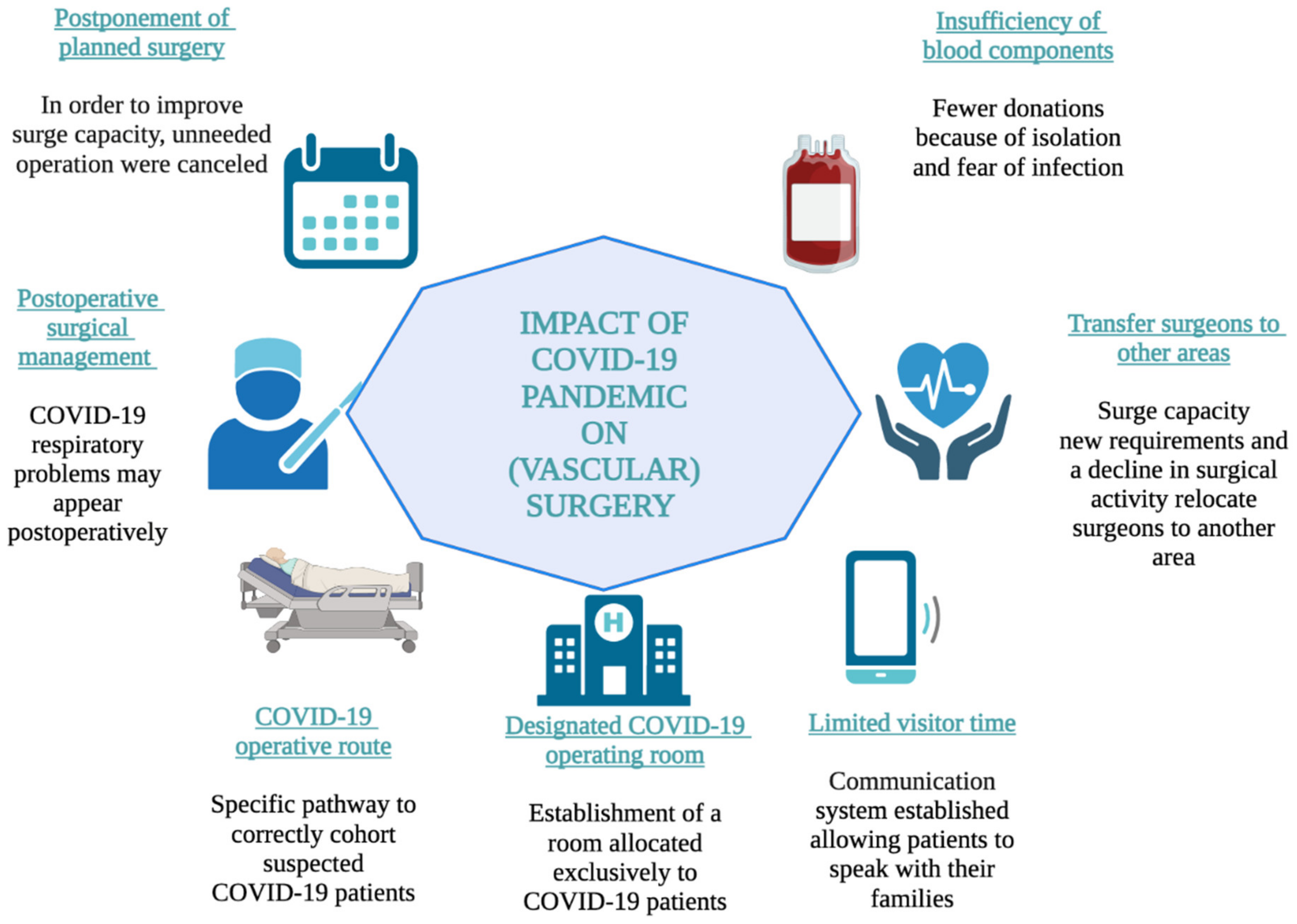
7. Vascular Surgeons and Ethics-Related Factors
8. Transition of Cardiovascular Surgery
Effects Worldwide
9. Residency and COVID-19
10. Short-Term and Long-Term Consequences of the COVID-19 Pandemic Affecting Surgical Care Provision
10.1. The Pandemic’s Effect on Surgical Services
10.2. Reconstructing Surgical Capability following Pandemic
10.3. Getting Ready for the Future
11. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Zhu, N.; Zhang, D.; Wang, W.; Li, X.; Yang, B.; Song, J.; Zhao, X.; Huang, B.; Shi, W.; Lu, R.; et al. A novel Coronavirus from patients with pneumonia in China, 2019. N. Engl. J. Med. 2020, 382, 727–733. [Google Scholar] [CrossRef] [PubMed]
- Weng, L.; Jiao, Y.; Li, Y. First Case of COVID-19 in the United States. N. Engl. J. Med. 2020, 382, e53. [Google Scholar] [PubMed]
- Bhatraju, P.K.; Ghassemieh, B.J.; Nichols, M.; Kim, R.; Jerome, K.R.; Nalla, A.K.; Greninger, A.L.; Pipavath, S.; Wurfel, M.M.; Evans, L.; et al. COVID-19 in critically ill patients in the Seattle region-case series. N. Engl. J. Med. 2020, 382, 2012–2022. [Google Scholar] [CrossRef] [PubMed]
- Driggin, E.; Madhavan, M.V.; Bikdeli, B.; Chuich, T.; Laracy, J.; Biondi-Zoccai, G.; Brown, T.S.; Der Nigoghossian, C.; Zidar, D.A.; Haythe, J.; et al. Cardiovascular considerations for patients, health care workers, and health systems during the COVID-19 pandemic. J. Am. Coll. Cardiol. 2020, 75, 2352–2371. [Google Scholar] [CrossRef]
- Garcia, S.; Albaghdadi, M.S.; Meraj, P.M.; Schmidt, C.; Garberich, R.; Jaffer, F.A.; Dixon, S.; Rade, J.J.; Tannenbaum, M.; Chambers, J.; et al. Reduction in ST-segment elevation cardiac catheterization laboratory activations in the United States during COVID-19 pandemic. J. Am. Coll. Cardiol. 2020, 75, 2871–2872. [Google Scholar] [CrossRef]
- Wood, D.A.; Sathananthan, J.; Gin, K.; Mansour, S.; Ly, H.Q.; Quraishi, A.-U.-R.; Lavoie, A.; Lutchmedial, S.; Nosair, M.; Bagai, A.; et al. Precautions and procedures for coronary and structural cardiac interventions during the COVID-19 pandemic: Guidance from Canadian Association of Interventional Cardiology. Can. J. Cardiol. 2020, 36, 780–783. [Google Scholar] [CrossRef]
- Shah, P.B.; Welt, F.G.P.; Mahmud, E.; Phillips, A.; Anwaruddin, S. Reply: Triage considerations for patients referred for structural heart disease intervention during the Coronavirus disease 2019 (COVID-19) pandemic: An ACC/SCAI consensus statement. JACC Cardiovasc. Interv. 2020, 13, 1607–1608. [Google Scholar] [CrossRef]
- Kirkpatrick, J.N.; Mitchell, C.; Taub, C.; Kort, S.; Hung, J.; Swaminathan, M. ASE statement on protection of patients and echocardiography service providers during the 2019 novel Coronavirus outbreak: Endorsed by the American college of cardiology. J. Am. Soc. Echocardiogr. 2020, 33, 648–653. [Google Scholar] [CrossRef]
- Choi, A.D.; Abbara, S.; Branch, K.R.; Feuchtner, G.M.; Ghoshhajra, B.; Nieman, K.; Pontone, G.; Villines, T.C.; Williams, M.C.; Blankstein, R. Society of Cardiovascular Computed Tomography guidance for use of cardiac computed tomography amidst the COVID-19 pandemic Endorsed by the American College of Cardiology. J. Cardiovasc. Comput. Tomogr. 2020, 14, 101–104. [Google Scholar] [CrossRef]
- Haft, J.W.; Atluri, P.; Ailawadi, G.; Engelman, D.T.; Grant, M.C.; Hassan, A.; Legare, J.F.; Whitman, G.J.R.; Arora, R.C. Adult cardiac surgery during the COVID-19 pandemic: A tiered patient triage guidance statement. J. Thorac. Cardiovasc. Surg. 2020, 160, 452–455. [Google Scholar] [CrossRef]
- Hassan, A.; Arora, R.C.; Adams, C.; Bouchard, D.; Cook, R.; Gunning, D.; Lamarche, Y.; Malas, T.; Moon, M.; Ouzounian, M.; et al. Cardiac surgery in Canada during the COVID-19 pandemic: A guidance statement from the Canadian Society of Cardiac Surgeons. Can. J. Cardiol. 2020, 36, 952–955. [Google Scholar] [CrossRef] [PubMed]
- Mahmud, E.; Dauerman, H.L.; Welt, F.G.P.; Messenger, J.C.; Rao, S.V.; Grines, C.; Mattu, A.; Kirtane, A.J.; Jauhar, R.; Meraj, P.; et al. Management of acute myocardial infarction during the COVID-19 pandemic: A Consensus Statement from the Society for Cardiovascular Angiography and Interventions (SCAI), the American College of Cardiology (ACC), and the American College of Emergency Physicians (ACEP): A Consensus Statement from the Society for Cardiovascular Angiography and Interventions (SCAI), the American College of Cardiology (ACC), and the American College of Emergency Physicians (ACEP). Catheter. Cardiovasc. Interv. 2020, 96, 336–345. [Google Scholar] [CrossRef]
- Pellicori, P.; Doolub, G.; Wong, C.M.; Lee, K.S.; Mangion, K.; Ahmad, M.; Berry, C.; Squire, I.; Lambiase, P.D.; Lyon, A.; et al. COVID-19 and its cardiovascular effects: A systematic review of prevalence studies. Cochrane Database Syst. Rev. 2021, 3, CD013879. [Google Scholar] [CrossRef]
- South, A.M.; Diz, D.I.; Chappell, M.C. COVID-19, ACE2, and the cardiovascular consequences. Am. J. Physiol. Heart Circ. Physiol. 2020, 318, H1084–H1890. [Google Scholar] [CrossRef] [PubMed]
- Zhou, F.; Yu, T.; Du, R.; Fan, G.; Liu, Y.; Liu, Z.; Zhibo, L.; Xiang, J.; Wang, Y.; Song, B.; et al. Clinical course and risk factors for mortality of adult inpatients with COVID-19 in Wuhan, China: A retrospective cohort study. Lancet 2020, 395, 1054–1062. [Google Scholar] [CrossRef]
- Bae, S.; Kim, S.R.; Kim, M.-N.; Shim, W.J.; Park, S.-M. Impact of cardiovascular disease and risk factors on fatal outcomes in patients with COVID-19 according to age: A systematic review and meta-analysis. Heart 2021, 107, 373–380. [Google Scholar] [CrossRef]
- Yang, J.; Zheng, Y.; Gou, X.; Pu, K.; Chen, Z.; Guo, Q.; Ji, R.; Wang, H.; Wang, Y.; Zhou, Y. Prevalence of comorbidities and its effects in patients infected with SARS-CoV-2: A systematic review and meta-analysis. Int. J. Infect. Dis. 2020, 94, 91–95. [Google Scholar] [CrossRef]
- Li, R.; Pei, S.; Chen, B.; Song, Y.; Zhang, T.; Yang, W.; Shaman, J. Substantial undocumented infection facilitates the rapid dissemination of novel coronavirus (SARS-CoV-2). Science 2020, 368, 489–493. [Google Scholar] [CrossRef]
- Wan, Y.; Shang, J.; Graham, R.; Baric, R.S.; Li, F. Receptor recognition by the novel Coronavirus from Wuhan: An analysis based on decade-long structural studies of SARS Coronavirus. J. Virol. 2020, 94, e00127-20. [Google Scholar] [CrossRef]
- Gul, R.; Kim, U.-H.; Alfadda, A.A. Renin-angiotensin system at the interface of COVID-19 infection. Eur. J. Pharmacol. 2021, 890, 173656. [Google Scholar] [CrossRef]
- Tajbakhsh, A.; Gheibi Hayat, S.M.; Taghizadeh, H.; Akbari, A.; Inabadi, M.; Savardashtaki, A.; Johnston, T.P.; Sahebkar, A. COVID-19 and cardiac injury: Clinical manifestations, biomarkers, mechanisms, diagnosis, treatment, and follow up. Expert Rev. Anti-Infect. Ther. 2021, 19, 345–357. [Google Scholar] [CrossRef] [PubMed]
- Mascolo, A.; Scavone, C.; Rafaniello, C.; De Angelis, A.; Urbanek, K.; di Mauro, G.; Cappetta, D.; Berrino, L.; Rossi, F.; Capuano, A. The role of renin-angiotensin-aldosterone system in the heart and lung: Focus on COVID-19. Front. Pharmacol. 2021, 12, 667254. [Google Scholar] [CrossRef] [PubMed]
- Tschöpe, C.; Ammirati, E.; Bozkurt, B.; Caforio, A.L.P.; Cooper, L.T.; Felix, S.B.; Hare, J.M.; Heidecker, B.; Heymans, S.; Hübner, N.; et al. Myocarditis and inflammatory cardiomyopathy: Current evidence and future directions. Nat. Rev. Cardiol. 2021, 18, 169–193. [Google Scholar] [CrossRef]
- Badawi, A.; Ryoo, S.G. Prevalence of comorbidities in the Middle East respiratory syndrome coronavirus (MERS-CoV): A systematic review and meta-analysis. Int. J. Infect. Dis. 2016, 49, 129–133. [Google Scholar] [CrossRef] [PubMed]
- Li, S.S.-L.; Cheng, C.-W.; Fu, C.-L.; Chan, Y.-H.; Lee, M.-P.; Chan, J.W.-M.; Yiu, S.F. Left ventricular performance in patients with severe acute respiratory syndrome: A 30-day echocardiographic follow-up study: A 30-day echocardiographic follow-up study. Circulation 2003, 108, 1798–1803. [Google Scholar] [CrossRef]
- Madjid, M.; Safavi-Naeini, P.; Solomon, S.D.; Vardeny, O. Potential effects of coronaviruses on the cardiovascular system: A review. JAMA Cardiol. 2020, 5, 831–840. [Google Scholar] [CrossRef]
- D’Onofrio, N.; Scisciola, L.; Sardu, C.; Trotta, M.C.; De Feo, M.; Maiello, C.; Mascolo, P.; De Micco, F.; Turriziani, F.; Municinò, E.; et al. Glycated ACE2 receptor in diabetes: Open door for SARS-CoV-2 entry in cardiomyocyte. Cardiovasc. Diabetol. 2021, 20, 99. [Google Scholar] [CrossRef]
- Piazza, G.; Morrow, D.A. Diagnosis, management, and pathophysiology of arterial and venous thrombosis in COVID-19. JAMA 2020, 324, 2548–2549. [Google Scholar] [CrossRef]
- Colling, M.E.; Kanthi, Y. COVID-19-associated coagulopathy: An exploration of mechanisms. Vasc. Med. 2020, 25, 471–478. [Google Scholar] [CrossRef]
- The Lancet Haematology. COVID-19 coagulopathy: An evolving story. Lancet Haematol. 2020, 7, e425. [Google Scholar] [CrossRef]
- Zhang, L.; Yan, X.; Fan, Q.; Liu, H.; Liu, X.; Liu, Z.; Zhang, Z. D-dimer levels on admission to predict in-hospital mortality in patients with COVID-19. J. Thromb. Haemost. 2020, 18, 1324–1329. [Google Scholar] [CrossRef] [PubMed]
- Li, Y.; Zhao, K.; Wei, H.; Chen, W.; Wang, W.; Jia, L.; Liu, Q.; Zhang, J.; Shan, T.; Peng, Z.; et al. Dynamic relationship between D-dimer and COVID-19 severity. Br. J. Haematol. 2020, 190, e24–e27. [Google Scholar] [CrossRef] [PubMed]
- Zhang, Y.; Cao, W.; Jiang, W.; Xiao, M.; Li, Y.; Tang, N.; Liu, Z.; Yan, X.; Zhao, Y.; Li, T.; et al. Profile of natural anticoagulant, coagulant factor and anti-phospholipid antibody in critically ill COVID-19 patients. J. Thromb. Thrombolysis 2020, 50, 580–586. [Google Scholar] [CrossRef] [PubMed]
- Wu, C.; Chen, X.; Cai, Y.; Xia, J.; Zhou, X.; Xu, S.; Huang, H.; Zhang, L.; Zhou, X.; Du, C.; et al. Risk factors associated with acute respiratory distress syndrome and death in patients with Coronavirus disease 2019 pneumonia in Wuhan, China. JAMA Intern. Med. 2020, 180, 934–943. [Google Scholar] [CrossRef] [PubMed]
- Tang, N.; Li, D.; Wang, X.; Sun, Z. Abnormal coagulation parameters are associated with poor prognosis in patients with novel coronavirus pneumonia. J. Thromb. Haemost. 2020, 18, 844–847. [Google Scholar] [CrossRef] [PubMed]
- Avnon, L.S.; Munteanu, D.; Smoliakov, A.; Jotkowitz, A.; Barski, L. Thromboembolic events in patients with severe pandemic influenza A/H1N1. Eur. J. Intern. Med. 2015, 26, 596–598. [Google Scholar] [CrossRef]
- Khan, M.S.; Shahid, I.; Anker, S.D.; Solomon, S.D.; Vardeny, O.; Michos, E.D.; Fonarow, G.C.; Butler, J. Cardiovascular implications of COVID-19 versus influenza infection: A review. BMC Med. 2020, 18, 403. [Google Scholar] [CrossRef]
- Smilowitz, N.R.; Subashchandran, V.; Yuriditsky, E.; Horowitz, J.M.; Reynolds, H.R.; Hochman, J.S.; Berger, J.S. Thrombosis in hospitalized patients with viral respiratory infections versus COVID-19. Am. Heart J. 2021, 231, 93–95. [Google Scholar] [CrossRef]
- Nicolai, L.; Leunig, A.; Brambs, S.; Kaiser, R.; Weinberger, T.; Weigand, M.; Muenchhoff, M.; Hellmuth, J.C.; Ledderose, S.; Schulz, H.; et al. Immunothrombotic dysregulation in COVID-19 pneumonia is associated with respiratory failure and coagulopathy. Circulation 2020, 142, 1176–1189. [Google Scholar] [CrossRef]
- Polak, S.B.; Van Gool, I.C.; Cohen, D.; von der Thüsen, J.H.; van Paassen, J. A systematic review of pathological findings in COVID-19: A pathophysiological timeline and possible mechanisms of disease progression. Mod. Pathol. 2020, 33, 2128–2138. [Google Scholar] [CrossRef]
- Piazza, G.; Campia, U.; Hurwitz, S.; Snyder, J.E.; Rizzo, S.M.; Pfeferman, M.B.; Morrison, R.B.; Leiva, O.; Fanikos, J.; Nauffal, V.; et al. Registry of arterial and venous thromboembolic complications in patients with COVID-19. J. Am. Coll. Cardiol. 2020, 76, 2060–2072. [Google Scholar] [CrossRef] [PubMed]
- Fox, S.E.; Akmatbekov, A.; Harbert, J.L.; Li, G.; Quincy Brown, J.; Vander Heide, R.S. Pulmonary and cardiac pathology in African American patients with COVID-19: An autopsy series from New Orleans. Lancet Respir. Med. 2020, 8, 681–686. [Google Scholar] [CrossRef]
- Nagashima, S.; Mendes, M.C.; Camargo Martins, A.P.; Borges, N.H.; Godoy, T.M.; Miggiolaro, A.F.R.D.S.; da Silva Dezidério, F.; Machado-Souza, C.; de Noronha, L. Endothelial dysfunction and thrombosis in patients with COVID-19-brief report. Arterioscler. Thromb. Vasc. Biol. 2020, 40, 2404–2407. [Google Scholar] [CrossRef]
- Ji, H.-L.; Zhao, R.; Matalon, S.; Matthay, M.A. Elevated plasmin(ogen) as a common risk factor for COVID-19 susceptibility. Physiol. Rev. 2020, 100, 1065–1075. [Google Scholar] [CrossRef] [PubMed]
- Ventura-Santana, E.; Ninan, J.R.; Snyder, C.M.; Okeke, E.B. Neutrophil extracellular traps, sepsis and COVID-19—A tripod stand. Front. Immunol. 2022, 13, 902206. [Google Scholar] [CrossRef] [PubMed]
- Nypaver, T.; Miller, D.; Weaver, M.; Marin, H.; Lee, A.; Griffith, B.; Wang, D.D.; Kabbani, L. Symptomatic extracranial carotid disease in COVID-19 patients is related to thrombus formation. J. Vasc. Surg. 2021, 73, 44–45. [Google Scholar] [CrossRef]
- Ilonzo, N.; Rao, A.; Safir, S.; Vouyouka, A.; Phair, J.; Baldwin, M.; Ting, W.; Soundararajan, K.; Han, D.; Tadros, R.; et al. Acute thrombotic manifestations of coronavirus disease 2019 infection: Experience at a large New York City health care system. J. Vasc. Surg. 2021, 73, 789–796. [Google Scholar] [CrossRef]
- Demelo-Rodríguez, P.; Ordieres-Ortega, L.; Ji, Z.; Del Toro-Cervera, J.; de Miguel-Díez, J.; Álvarez-Sala-Walther, L.A.; Galeano-Valle, F. Long-term follow-up of patients with venous thromboembolism and COVID-19: Analysis of risk factors for death and major bleeding. Eur. J. Haematol. 2021, 106, 716–723. [Google Scholar] [CrossRef]
- Gralinski, L.E.; Baric, R.S. Molecular pathology of emerging coronavirus infections: Molecular pathology of emerging coronavirus infections. J. Pathol. 2015, 235, 185–195. [Google Scholar] [CrossRef]
- Bikdeli, B.; Madhavan, M.V.; Jimenez, D.; Chuich, T.; Dreyfus, I.; Driggin, E.; Nigoghossian, C.; Ageno, W.; Madjid, M.; Guo, Y.; et al. COVID-19 and thrombotic or thromboembolic disease: Implications for prevention, antithrombotic therapy, and follow-up: JACC state-of-the-art review. J. Am. Coll. Cardiol. 2020, 75, 2950–2973. [Google Scholar] [CrossRef]
- Teo, K.-C.; Leung, W.C.Y.; Wong, Y.-K.; Liu, R.K.C.; Chan, A.H.Y.; Choi, O.M.Y.; Kwok, W.M.; Leung, K.K.; Tse, M.Y.; Cheung, R.T.F.; et al. Delays in stroke onset to hospital arrival time during COVID-19. Stroke 2020, 51, 2228–2231. [Google Scholar] [CrossRef] [PubMed]
- Fothergill, R.T.; Smith, A.L.; Wrigley, F.; Perkins, G.D. Out-of-Hospital Cardiac Arrest in London during the COVID-19 pandemic. Resusc. Plus 2021, 5, 100066. [Google Scholar] [CrossRef] [PubMed]
- Lodigiani, C.; Iapichino, G.; Carenzo, L.; Cecconi, M.; Ferrazzi, P.; Sebastian, T.; Kucher, N.; Studt, J.D.; Sacco, C.; Bertuzzi, A.; et al. Venous and arterial thromboembolic complications in COVID-19 patients admitted to an academic hospital in Milan, Italy. Thromb. Res. 2020, 191, 9–14. [Google Scholar] [CrossRef] [PubMed]
- Bhatt, A.S.; Moscone, A.; McElrath, E.E.; Varshney, A.S.; Claggett, B.L.; Bhatt, D.L.; Januzzi, J.L.; Butler, J.; Adler, D.S.; Solomon, S.D.; et al. Fewer hospitalizations for acute cardiovascular conditions during the COVID-19 pandemic. J. Am. Coll. Cardiol. 2020, 76, 280–288. [Google Scholar] [CrossRef]
- Donoghue, M.; Hsieh, F.; Baronas, E.; Godbout, K.; Gosselin, M.; Stagliano, N.; Donovan, M.; Woolf, B.; Robison, K.; Jeyaseelan, R.; et al. A novel angiotensin-converting enzyme-related carboxypeptidase (ACE2) converts angiotensin I to angiotensin 1-9. Circ. Res. 2000, 87, E1–E9. [Google Scholar] [CrossRef]
- Santos, R.A.S.; Sampaio, W.O.; Alzamora, A.C.; Motta-Santos, D.; Alenina, N.; Bader, M.; Campagnole-Santos, M.J. The ACE2/angiotensin-(1–7)/MAS axis of the renin-angiotensin system: Focus on angiotensin-(1–7). Physiol. Rev. 2018, 98, 505–553. [Google Scholar] [CrossRef]
- Turner, A.J.; Tipnis, S.R.; Guy, J.L.; Rice, G.; Hooper, N.M. ACEH/ACE2 is a novel mammalian metallocarboxypeptidase and a homologue of angiotensin-converting enzyme insensitive to ACE inhibitors. Can. J. Physiol. Pharmacol. 2002, 80, 346–353. [Google Scholar] [CrossRef]
- Zhang, Y.; Yan, R.; Zhou, Q. ACE2, B0AT1, and SARS-CoV-2 spike protein: Structural and functional implications. Curr. Opin. Struct. Biol. 2022, 74, 102388. [Google Scholar] [CrossRef]
- Sampaio, W.O.; Henrique de Castro, C.; Santos, R.A.S.; Schiffrin, E.L.; Touyz, R.M. Angiotensin-(1-7) counterregulates angiotensin II signaling in human endothelial cells. Hypertension 2007, 50, 1093–1098. [Google Scholar] [CrossRef]
- Bader, M. ACE2, angiotensin-(1–7), and Mas: The other side of the coin. Pflügers Arch. Eur. J. Physiol. 2013, 465, 79–85. [Google Scholar] [CrossRef]
- Simões e Silva, A.C.; Silveira, K.D.; Ferreira, A.J.; Teixeira, M.M. ACE2, angiotensin-(1-7) and Mas receptor axis in inflammation and fibrosis: Angiotensin-(1-7) in inflammation and fibrosis. Br. J. Pharmacol. 2013, 169, 477–492. [Google Scholar] [CrossRef] [PubMed]
- Gheblawi, M.; Wang, K.; Viveiros, A.; Nguyen, Q.; Zhong, J.-C.; Turner, A.J.; Raizada, M.K.; Grant, M.B.; Oudit, G.Y. Angiotensin-converting enzyme 2: SARS-CoV-2 receptor and regulator of the renin-angiotensin system: Celebrating the 20th anniversary of the discovery of ACE2: Celebrating the 20th anniversary of the discovery of ACE2. Circ. Res. 2020, 126, 1456–1474. [Google Scholar] [CrossRef] [PubMed]
- Touyz, R.M.; Li, H.; Delles, C. ACE2 the Janus-faced protein-from cardiovascular protection to severe acute respiratory syndrome-coronavirus and COVID-19. Clin. Sci. 2020, 134, 747–750. [Google Scholar] [CrossRef] [PubMed]
- Walls, A.C.; Park, Y.-J.; Tortorici, M.A.; Wall, A.; McGuire, A.T.; Veesler, D. Structure, function, and antigenicity of the SARS-CoV-2 spike glycoprotein. Cell 2020, 181, 281–292.e6. [Google Scholar] [CrossRef]
- Yan, R.; Zhang, Y.; Li, Y.; Xia, L.; Guo, Y.; Zhou, Q. Structural basis for the recognition of SARS-CoV-2 by full-length human ACE2. Science 2020, 367, 1444–1448. [Google Scholar] [CrossRef]
- Chen, Y.; Guo, Y.; Pan, Y.; Zhao, Z.J. Structure analysis of the receptor binding of 2019-nCoV. Biochem. Biophys. Res. Commun. 2020, 525, 135–140. [Google Scholar] [CrossRef]
- Hamming, I.; Timens, W.; Bulthuis, M.L.C.; Lely, A.T.; Navis, G.J.; van Goor, H. Tissue distribution of ACE2 protein, the functional receptor for SARS coronavirus. A first step in understanding SARS pathogenesis. J. Pathol. 2004, 203, 631–637. [Google Scholar] [CrossRef]
- Tipnis, S.R.; Hooper, N.M.; Hyde, R.; Karran, E.; Christie, G.; Turner, A.J. A human homolog of angiotensin-converting enzyme: Cloning and functional expression as a captopril-insensitive carboxypeptidase. J. Biol. Chem. 2000, 275, 33238–33243. [Google Scholar] [CrossRef]
- Gao, S.; Zhang, L. ACE2 partially dictates the host range and tropism of SARS-CoV-2. Comput. Struct. Biotechnol. J. 2020, 18, 4040–4047. [Google Scholar] [CrossRef]
- Turner, A.J.; Hiscox, J.A.; Hooper, N.M. ACE2: From vasopeptidase to SARS virus receptor. Trends Pharmacol. Sci. 2004, 25, 291–294. [Google Scholar] [CrossRef]
- Chan, P.K.S.; To, K.-F.; Lo, A.W.I.; Cheung, J.L.K.; Chu, I.; Au, F.W.L.; Tong, J.H.; Tam, J.; Sung, J.J.; Ng, H.K. Persistent infection of SARS coronavirus in colonic cells in vitro. J. Med. Virol. 2004, 74, 1–7. [Google Scholar] [CrossRef] [PubMed]
- McCracken, I.R.; Saginc, G.; He, L.; Huseynov, A.; Daniels, A.; Fletcher, S.; Peghaire, C.; Kalna, V.; Andaloussi-Mäe, M.; Muhl, L.; et al. Lack of evidence of angiotensin-converting enzyme 2 expression and replicative infection by SARS-CoV-2 in human endothelial cells. Circulation 2021, 143, 865–868. [Google Scholar] [CrossRef] [PubMed]
- Fuentes-Prior, P. Priming of SARS-CoV-2 S protein by several membrane-bound serine proteinases could explain enhanced viral infectivity and systemic COVID-19 infection. J. Biol. Chem. 2021, 296, 100135. [Google Scholar] [CrossRef] [PubMed]
- Wei, J.; Alfajaro, M.M.; DeWeirdt, P.C.; Hanna, R.E.; Lu-Culligan, W.J.; Cai, W.L.; Strine, M.S.; Zhang, S.M.; Graziano, V.R.; Schmitz, C.O.; et al. Genome-wide CRISPR screens reveal host factors critical for SARS-CoV-2 infection. Cell 2021, 184, 76–91.e13. [Google Scholar] [CrossRef]
- Geng, Y.-J.; Wei, Z.-Y.; Qian, H.-Y.; Huang, J.; Lodato, R.; Castriotta, R.J. Pathophysiological characteristics and therapeutic approaches for pulmonary injury and cardiovascular complications of coronavirus disease 2019. Cardiovasc. Pathol. 2020, 47, 107228. [Google Scholar] [CrossRef]
- Zeng, J.-H.; Liu, Y.-X.; Yuan, J.; Wang, F.-X.; Wu, W.-B.; Li, J.-X.; Xie, X.J.; Feng, C.; Liu, L. First case of COVID-19 complicated with fulminant myocarditis: A case report and insights. Infection 2020, 48, 773–777. [Google Scholar] [CrossRef]
- Oudit, G.Y.; Kassiri, Z.; Jiang, C.; Liu, P.P.; Poutanen, S.M.; Penninger, J.M.; Butany, J. SARS-coronavirus modulation of myocardial ACE2 expression and inflammation in patients with SARS. Eur. J. Clin. Investig. 2009, 39, 618–625. [Google Scholar] [CrossRef]
- Coperchini, F.; Chiovato, L.; Ricci, G.; Croce, L.; Magri, F.; Rotondi, M. The cytokine storm in COVID-19: Further advances in our understanding the role of specific chemokines involved. Cytokine Growth Factor Rev. 2021, 58, 82–91. [Google Scholar] [CrossRef]
- Petrilli, C.M.; Jones, S.A.; Yang, J.; Rajagopalan, H.; O’Donnell, L.; Chernyak, Y.; Tobin, K.A.; Cerfolio, R.J.; Francois, F.; Horwitz, L.I. Factors associated with hospitalization and critical illness among 4,103 patients with COVID-19 disease in New York City. bioRxiv 2020. [Google Scholar] [CrossRef]
- Vizcaychipi, M.P.; Shovlin, C.L.; McCarthy, A.; Godfrey, A.; Patel, S.; Shah, P.L.; Hayes, M.; Keays, R.T.; Beveridge, I.; Davies, G.; et al. Increase in COVID-19 inpatient survival following detection of Thromboembolic and Cytokine storm risk from the point of admission to hospital by a near real time Traffic-light System (TraCe-Tic). Braz. J. Infect. Dis. 2020, 24, 412–421. [Google Scholar] [CrossRef]
- Kwong, J.C.; Schwartz, K.L.; Campitelli, M.A. Acute myocardial infarction after laboratory-confirmed influenza infection. N. Engl. J. Med. 2018, 378, 2540–2541. [Google Scholar] [CrossRef] [PubMed]
- Solomon, M.D.; McNulty, E.J.; Rana, J.S.; Leong, T.K.; Lee, C.; Sung, S.-H.; Ambrosy, A.P.; Sidney, S.; Go, A.S. The COVID-19 pandemic and the incidence of acute myocardial infarction. N. Engl. J. Med. 2020, 383, 691–693. [Google Scholar] [CrossRef] [PubMed]
- Kam, A.W.; Chaudhry, S.G.; Gunasekaran, N.; White, A., Jr.; Vukasovic, M.; Fung, A.T. Fewer presentations to metropolitan emergency departments during the COVID-19 pandemic. Med. J. Aust. 2020, 213, 370–371. [Google Scholar] [CrossRef] [PubMed]
- Ahmed, T.; Lodhi, S.H.; Kapadia, S.; Shah, G.V. Community and healthcare system-related factors feeding the phenomenon of evading medical attention for time-dependent emergencies during COVID-19 crisis. BMJ Case Rep. 2020, 13, e237817. [Google Scholar] [CrossRef] [PubMed]
- Liu, Y.; Wu, S.; Qin, M.; Jiang, W.; Liu, X. Prevalence of cardiovascular comorbidities in Coronavirus disease 2019, severe acute respiratory syndrome, and Middle East respiratory syndrome: Pooled analysis of published data. J. Am. Heart Assoc. 2020, 9, e016812. [Google Scholar] [CrossRef]
- Wu, Z.; McGoogan, J.M. Characteristics of and important lessons from the Coronavirus disease 2019 (COVID-19) outbreak in China: Summary of a report of 72,314 cases from the Chinese center for disease control and prevention: Summary of a report of 72 314 cases from the Chinese center for disease control and prevention. JAMA 2020, 323, 1239–1242. [Google Scholar] [CrossRef]
- Bonow, R.O.; Fonarow, G.C.; O’Gara, P.T.; Yancy, C.W. Association of Coronavirus disease 2019 (COVID-19) with myocardial injury and mortality. JAMA Cardiol. 2020, 5, 751–753. [Google Scholar] [CrossRef]
- Guo, J.; Huang, Z.; Lin, L.; Lv, J. Coronavirus disease 2019 (COVID-19) and cardiovascular disease: A viewpoint on the potential influence of angiotensin-converting enzyme inhibitors/angiotensin receptor blockers on onset and severity of severe acute respiratory syndrome Coronavirus 2 infection. J. Am. Heart Assoc. 2020, 9, e016219. [Google Scholar] [CrossRef]
- Chen, T.; Wu, D.; Chen, H.; Yan, W.; Yang, D.; Chen, G.; Ma, K.; Xu, D.; Yu, H.; Wang, H.; et al. Clinical characteristics of 113 deceased patients with coronavirus disease 2019: Retrospective study. BMJ 2020, 368, m1091. [Google Scholar] [CrossRef]
- Thachil, J.; Tang, N.; Gando, S.; Falanga, A.; Cattaneo, M.; Levi, M.; Clark, C.; Iba, T. ISTH interim guidance on recognition and management of coagulopathy in COVID-19. J. Thromb. Haemost. 2020, 18, 1023–1026. [Google Scholar] [CrossRef]
- Mahmood, M.M. COVID-19 and Blood Clots: Is it only The Virus to be Blamed? What are new Updates? A Systematic Review. J. Cardiol. Cardiovasc. Res. 2022, 3, 1–19. [Google Scholar] [CrossRef]
- Lei, S.; Jiang, F.; Su, W.; Chen, C.; Chen, J.; Mei, W.; Zhan, L.Y.; Jia, Y.; Zhang, L.; Liu, D.; et al. Clinical characteristics and outcomes of patients undergoing surgeries during the incubation period of COVID-19 infection. EClinicalMedicine 2020, 21, 100331. [Google Scholar] [CrossRef] [PubMed]
- Briscoe, M.; Sykes, R.; Krystofiak, T.; Peck, O.; Mangion, K.; Berry, C. Clinical significance of coronavirus disease 2019 in hospitalized patients with myocardial injury. Clin. Cardiol. 2021, 44, 332–339. [Google Scholar] [CrossRef] [PubMed]
- Dolhnikoff, M.; Ferreira Ferranti, J.; de Almeida Monteiro, R.A.; Duarte-Neto, A.N.; Soares Gomes-Gouvêa, M.; Viu Degaspare, N.; Figueiredo Delgado, A.; Montanari Fiorita, C.; Nunes Leal, G.; Rodrigues, R.M.; et al. SARS-CoV-2 in cardiac tissue of a child with COVID-19-related multisystem inflammatory syndrome. Lancet Child Adolesc. Health 2020, 4, 790–794. [Google Scholar] [CrossRef]
- Al-Mallah, M.H. COVID-19 and the heart. Methodist Debakey Cardiovasc. J. 2021, 17, 1–4. [Google Scholar] [CrossRef]
- Mele, D.; Flamigni, F.; Rapezzi, C.; Ferrari, R. Myocarditis in COVID-19 patients: Current problems. Intern. Emerg. Med. 2021, 16, 1123–1129. [Google Scholar] [CrossRef]
- Sala, S.; Peretto, G.; Gramegna, M.; Palmisano, A.; Villatore, A.; Vignale, D.; De Cobelli, F.; Tresoldi, M.; Cappelletti, A.M.; Basso, C.; et al. Acute myocarditis presenting as a reverse Tako-Tsubo syndrome in a patient with SARS-CoV-2 respiratory infection. Eur. Heart J. 2020, 41, 1861–1862. [Google Scholar] [CrossRef]
- Rovas, A.; Osiaevi, I.; Buscher, K.; Sackarnd, J.; Tepasse, P.-R.; Fobker, M.; Kühn, J.; Braune, S.; Göbel, U.; Thölking, G.; et al. Microvascular dysfunction in COVID-19: The MYSTIC study. Angiogenesis 2021, 24, 145–157. [Google Scholar] [CrossRef]
- Libby, P.; Lüscher, T. COVID-19 is, in the end, an endothelial disease. Eur. Heart J. 2020, 41, 3038–3044. [Google Scholar] [CrossRef]
- Quinaglia, T.; Shabani, M.; Breder, I.; Silber, H.A.; Lima, J.A.C.; Sposito, A.C. Coronavirus disease-19: The multi-level, multi-faceted vasculopathy. Atherosclerosis 2021, 322, 39–50. [Google Scholar] [CrossRef]
- Siddiqi, H.K.; Libby, P.; Ridker, P.M. COVID-19—A vascular disease. Trends Cardiovasc. Med. 2021, 31, 1–5. [Google Scholar] [CrossRef] [PubMed]
- McFadyen, J.D.; Stevens, H.; Peter, K. The emerging threat of (micro)thrombosis in COVID-19 and its therapeutic implications. Circ. Res. 2020, 127, 571–587. [Google Scholar] [CrossRef] [PubMed]
- Mangion, K.; Morrow, A.; Bagot, C.; Bayes, H.; Blyth, K.G.; Church, C.; Corcoran, D.; Delles, C.; Gillespie, L.; Grieve, D.; et al. The chief scientist office cardiovascular and pulmonary imaging in SARS Coronavirus disease-19 (CISCO-19) study. Cardiovasc. Res. 2020, 116, 2185–2196. [Google Scholar] [CrossRef] [PubMed]
- Hegde, S.; Khan, R.; Zordok, M.; Maysky, M. Characteristics and outcome of patients with COVID-19 complicated by Takotsubo cardiomyopathy: Case series with literature review. Open Heart 2020, 7, e001360. [Google Scholar] [CrossRef] [PubMed]
- Finsterer, J.; Stöllberger, C. SARS-CoV-2 triggered Takotsubo in 38 patients. J. Med. Virol. 2021, 93, 1236–1238. [Google Scholar] [CrossRef] [PubMed]
- Mountantonakis, S.E.; Saleh, M.; Fishbein, J.; Gandomi, A.; Lesser, M.; Chelico, J.; Gabriels, J.; Qiu, M.; Epstein, L.M. Atrial fibrillation is an independent predictor for in-hospital mortality in patients admitted with SARS-CoV-2 infection. Heart Rhythm 2021, 18, 501–507. [Google Scholar] [CrossRef] [PubMed]
- Zylla, M.M.; Merle, U.; Vey, J.A.; Korosoglou, G.; Hofmann, E.; Müller, M.; Herth, F.; Schmidt, W.; Blessing, E.; Göggelmann, C.; et al. Predictors and prognostic implications of cardiac arrhythmias in patients hospitalized for COVID-19. J. Clin. Med. 2021, 10, 133. [Google Scholar] [CrossRef]
- Shirazi, S.; Mami, S.; Mohtadi, N.; Ghaysouri, A.; Tavan, H.; Nazari, A.; Kokhazadeh, T.; Mollazadeh, R. Sudden cardiac death in COVID-19 patients, a report of three cases. Future Cardiol. 2021, 17, 113–118. [Google Scholar] [CrossRef]
- Adeghate, E.A.; Eid, N.; Singh, J. Mechanisms of COVID-19-induced heart failure: A short review. Heart Fail. Rev. 2021, 26, 363–369. [Google Scholar] [CrossRef]
- Hadzibegovic, S.; Lena, A.; Churchill, T.W.; Ho, J.E.; Potthoff, S.; Denecke, C.; Rösnick, L.; Heim, K.M.; Kleinschmidt, M.; Sander, L.E.; et al. Heart failure with preserved ejection fraction according to the HFA-PEFF score in COVID-19 patients: Clinical correlates and echocardiographic findings. Eur. J. Heart Fail. 2021, 23, 1891–1902. [Google Scholar] [CrossRef]
- Ata, F.; Montoro-Lopez, M.N.; Awouda, S.; Elsukkar, A.M.A.; Badr, A.M.H.; Patel, A.A.A.H. COVID-19 and heart failure: The big challenge. Heart Views 2020, 21, 187–192. [Google Scholar] [CrossRef] [PubMed]
- Bader, F.; Manla, Y.; Atallah, B.; Starling, R.C. Heart failure and COVID-19. Heart Fail. Rev. 2021, 26, 1–10. [Google Scholar] [CrossRef]
- ISHLT.org. Guidance from the International Society of Heart and Lung Transplantation Regarding the SARS-CoV-2 Pandemic. 2021. Available online: https://ishlt.org/ishlt/media/documents/SARS-CoV-2_Guidance-for-Cardiothoracic-Transplant-and-VAD-center.pdf (accessed on 19 September 2022).
- Gaudriot, B.; Mansour, A.; Thibault, V.; Lederlin, M.; Cauchois, A.; Lelong, B.; Ross, J.T.; Leurent, G.; Tadié, J.M.; Revest, M.; et al. Successful heart transplantation for COVID-19-associated post-infectious fulminant myocarditis. ESC Heart Fail. 2021, 8, 2625–2630. [Google Scholar] [CrossRef] [PubMed]
- Linschoten, M.; Asselbergs, F.W. CAPACITY-COVID: A European Registry to determine the role of cardiovascular disease in the COVID-19 pandemic. Eur. Heart J. 2020, 41, 1795–1796. [Google Scholar] [CrossRef] [PubMed]
- Gerotziafas, G.T.; Catalano, M.; Colgan, M.-P.; Pecsvarady, Z.; Wautrecht, J.C.; Fazeli, B.; Olinic, D.M.; Farkas, K.; Elalamy, I.; Falanga, A.; et al. Guidance for the management of patients with vascular disease or cardiovascular risk factors and COVID-19: Position paper from VAS-European Independent Foundation in Angiology/Vascular Medicine. Thromb. Haemost. 2020, 120, 1597–1628. [Google Scholar] [CrossRef]
- Zhai, Z.; Li, C.; Chen, Y.; Gerotziafas, G.; Zhang, Z.; Wan, J.; Liu, P.; Elalamy, I.; Wang, C. Prevention and treatment of venous thromboembolism associated with Coronavirus disease 2019 infection: A consensus statement before guidelines. Thromb. Haemost. 2020, 120, 937–948. [Google Scholar] [CrossRef]
- Han, D.P.; Penn-Nicholson, A.; Cho, M.W. Identification of critical deter- minants on ACE2 for SARS-CoV entry and development of a potent entry inhibitor. Virology 2006, 350, 15–25. [Google Scholar] [CrossRef]
- Lei, C.; Qian, K.; Li, T.; Zhang, S.; Fu, W.; Ding, M.; Hu, S. Neutralization of SARS-CoV-2 spike pseudotyped virus by recombinant ACE2-Ig. Nat. Commun. 2020, 11, 2070. [Google Scholar] [CrossRef]
- Hernández Prada, J.A.; Ferreira, A.J.; Katovich, M.J.; Shenoy, V.; Qi, Y.; Santos, R.A.S.; Castellano, R.K.; Lampkins, A.J.; Gubala, V.; Ostrov, D.A.; et al. Structure-based identification of small-molecule angiotensin-converting enzyme 2 activators as novel antihypertensive agents. Hypertension 2008, 51, 1312–1317. [Google Scholar] [CrossRef]
- Zhou, P.; Yang, X.-L.; Wang, X.-G.; Hu, B.; Zhang, L.; Zhang, W.; Si, H.R.; Zhu, Y.; Li, B.; Huang, C.L.; et al. A pneumonia outbreak associated with a new coronavirus of probable bat origin. Nature 2020, 579, 270–273. [Google Scholar] [CrossRef]
- Wysocki, J.; Ye, M.; Rodriguez, E.; González-Pacheco, F.R.; Barrios, C.; Evora, K.; Schuster, M.; Loibner, H.; Brosnihan, K.B.; Ferrario, C.M.; et al. Targeting the degradation of angiotensin II with recombinant angiotensin-converting enzyme 2: Prevention of angiotensin II-dependent hypertension: Prevention of angiotensin II-dependent hypertension. Hypertension 2010, 55, 90–98. [Google Scholar] [CrossRef] [PubMed]
- Mancia, G.; Rea, F.; Ludergnani, M.; Apolone, G.; Corrao, G. Renin-angiotensin-aldosterone system blockers and the risk of COVID-19. N. Engl. J. Med. 2020, 382, 2431–2440. [Google Scholar] [CrossRef] [PubMed]
- Zhang, P.; Zhu, L.; Cai, J.; Lei, F.; Qin, J.-J.; Xie, J.; Liu, Y.M.; Zhao, Y.C.; Huang, X.; Lin, L.; et al. Association of inpatient use of angiotensin-converting enzyme inhibitors and angiotensin II receptor blockers with mortality among patients with hypertension hospitalized with COVID-19. Circ. Res. 2020, 126, 1671–1681. [Google Scholar] [CrossRef]
- Xu, J.; Huang, C.; Fan, G.; Liu, Z.; Shang, L.; Zhou, F.; Wang, Y.; Yu, J.; Yang, L.; Xie, K.; et al. Use of angiotensin-converting enzyme inhibitors and angiotensin II receptor blockers in context of COVID-19 outbreak: A retrospective analysis. Front. Med. 2020, 14, 601–612. [Google Scholar] [CrossRef] [PubMed]
- de Abajo, F.J.; Rodríguez-Martín, S.; Lerma, V.; Mejía-Abril, G.; Aguilar, M.; García-Luque, A.; Laredo, L.; Laosa, O.; Centeno-Soto, G.A.; Ángeles Gálvez, M.; et al. Use of renin-angiotensin-aldosterone system inhibitors and risk of COVID-19 requiring admission to hospital: A case-population study. Lancet 2020, 395, 1705–1714. [Google Scholar] [CrossRef]
- Pranata, R.; Permana, H.; Huang, I.; Lim, M.A.; Soetedjo, N.N.M.; Supriyadi, R.; Soeroto, A.Y.; Alkatiri, A.A.; Firman, D.; Lukito, A.A. The use of renin angiotensin system inhibitor on mortality in patients with coronavirus disease 2019 (COVID-19): A systematic review and meta-analysis. Diabetes Metab. Syndr. 2020, 14, 983–990. [Google Scholar] [CrossRef]
- Bean, D.M.; Kraljevic, Z.; Searle, T.; Bendayan, R.; O’Gallagher, K.; Pickles, A.; Folarin, A.; Roguski, L.; Noor, K.; Shek, A.; et al. ACE-inhibitors and Angiotensin-2 Receptor Blockers are not associated with severe SARS-COV-2 infection in a multi-site UK acute Hospital Trust. bioRxiv 2020. [Google Scholar] [CrossRef]
- Oussalah, A.; Gleye, S.; Clerc Urmes, I.; Laugel, E.; Callet, J.; Barbé, F.; Orlowski, S.; Malaplate, C.; Aimone-Gastin, I.; Caillierez, B.M.; et al. Long-term ACE inhibitor/ARB use is associated with severe renal dysfunction and acute kidney injury in patients with severe COVID-19: Results from a referral center cohort in the northeast of France. Clin. Infect. Dis. 2020, 71, 2447–2456. [Google Scholar] [CrossRef]
- Negahdaripour, M. The battle against COVID-19: Where do we stand now? Iran. J. Med. Sci. 2020, 45, 81–82. [Google Scholar] [CrossRef]
- Negahdaripour, M. The rise and fall in therapeutic candidates for COVID-19. Iran. J. Med. Sci. 2020, 45, 231–232. [Google Scholar] [CrossRef]
- Owji, H.; Negahdaripour, M.; Hajighahramani, N. Immunotherapeutic approaches to curtail COVID-19. Int. Immunopharmacol. 2020, 88, 106924. [Google Scholar] [CrossRef]
- Tan, Z.C.; Fu, L.H.; Wang, D.D.; Hong, K. Cardiac manifestations of patients with COVID-19 pneumonia and related treatment recommendations. Zhonghua Xin Xue Guan Bing Za Zhi 2020, 48, E005. [Google Scholar] [CrossRef] [PubMed]
- Jin, Y.-H.; Cai, L.; Cheng, Z.-S.; Cheng, H.; Deng, T.; Fan, Y.-P.; Fang, C.; Huang, D.; Huang, L.Q.; Huang, Q.; et al. A rapid advice guideline for the diagnosis and treatment of 2019 novel coronavirus (2019-nCoV) infected pneumonia (standard version). Mil. Med. Res. 2020, 7, 4. [Google Scholar] [CrossRef] [PubMed]
- Chen, N.; Zhou, M.; Dong, X.; Qu, J.; Gong, F.; Han, Y.; Qiu, Y.; Wang, J.; Liu, Y.; Wei, Y.; et al. Epidemiological and clinical characteristics of 99 cases of 2019 novel coronavirus pneumonia in Wuhan, China: A descriptive study. Lancet 2020, 395, 507–513. [Google Scholar] [CrossRef]
- Wang, D.; Hu, B.; Hu, C.; Zhu, F.; Liu, X.; Zhang, J.; Wang, B.; Xiang, H.; Cheng, Z.; Xiong, Y.; et al. Clinical characteristics of 138 hospitalized patients with 2019 novel Coronavirus-infected pneumonia in Wuhan, China. JAMA 2020, 323, 1061–1069. [Google Scholar] [CrossRef] [PubMed]
- Holshue, M.L.; DeBolt, C.; Lindquist, S.; Lofy, K.H.; Wiesman, J.; Bruce, H.; Spitters, C.; Ericson, K.; Wilkerson, S.; Tural, A.; et al. First case of 2019 novel Coronavirus in the United States. N. Engl. J. Med. 2020, 382, 929–936. [Google Scholar] [CrossRef]
- Zhou, D.; Dai, S.-M.; Tong, Q. COVID-19: A recommendation to examine the effect of hydroxychloroquine in preventing infection and progression. J. Antimicrob. Chemother. 2020, 75, 1667–1670. [Google Scholar] [CrossRef]
- Sarma, P.; Kaur, H.; Kumar, H.; Mahendru, D.; Avti, P.; Bhattacharyya, A.; Prajapat, M.; Shekhar, N.; Kumar, S.; Singh, R.; et al. Virological and clinical cure in COVID-19 patients treated with hydroxychloroquine: A systematic review and meta-analysis. J. Med. Virol. 2020, 92, 776–785. [Google Scholar] [CrossRef]
- Chowdhury, M.S.; Rathod, J.; Gernsheimer, J. A rapid systematic review of clinical trials utilizing chloroquine and hydroxychloroquine as a treatment for COVID-19. Acad. Emerg. Med. 2020, 27, 493–504. [Google Scholar] [CrossRef]
- Singh, A.K.; Singh, A.; Singh, R.; Misra, A. Hydroxychloroquine in patients with COVID-19: A Systematic Review and meta-analysis. Diabetes Metab. Syndr. 2020, 14, 589–596. [Google Scholar] [CrossRef]
- Wu, C.-I.; Postema, P.G.; Arbelo, E.; Behr, E.R.; Bezzina, C.R.; Napolitano, C.; Robyns, T.; Probst, V.; Schulze-Bahr, E.; Remme, C.A.; et al. SARS-CoV-2, COVID-19, and inherited arrhythmia syndromes. Heart Rhythm 2020, 17, 1456–1462. [Google Scholar] [CrossRef] [PubMed]
- Kochi, A.N.; Tagliari, A.P.; Forleo, G.B.; Fassini, G.M.; Tondo, C. Cardiac and arrhythmic complications in patients with COVID-19. J. Cardiovasc. Electrophysiol. 2020, 31, 1003–1008. [Google Scholar] [CrossRef] [PubMed]
- Si, D.; Du, B.; Ni, L.; Yang, B.; Sun, H.; Jiang, N.; Liu, G.; Massé, S.; Jin, L.; Nanthakumar, J.; et al. Death, discharge and arrhythmias among patients with COVID-19 and cardiac injury. CMAJ 2020, 192, E791–E798. [Google Scholar] [CrossRef] [PubMed]
- Khan, I.H.; Zahra, S.A.; Zaim, S.; Harky, A. At the heart of COVID-19. J. Card. Surg. 2020, 35, 1287–1294. [Google Scholar] [CrossRef]
- Melillo, F.; Napolano, A.; Loffi, M.; Regazzoni, V.; Boccellino, A.; Danzi, G.B.; Cappelletti, A.M.; Rovere-Querini, P.; Landoni, G.; Ingallina, G.; et al. Myocardial injury in patients with SARS-CoV-2 pneumonia: Pivotal role of inflammation in COVID-19. Eur. J. Clin. Investig. 2022, 52, e13703. [Google Scholar] [CrossRef]
- Das, R.R.; Jaiswal, N.; Dev, N.; Jaiswal, N.; Naik, S.S.; Sankar, J. Efficacy and safety of anti-malarial drugs (chloroquine and Hydroxy-chloroquine) in treatment of COVID-19 infection: A systematic review and meta-analysis. Front. Med. 2020, 7, 482. [Google Scholar] [CrossRef]
- Li, F.; Cai, J.; Dong, N. First cases of COVID-19 in heart transplantation from China. J. Heart Lung Transplant. 2020, 39, 496–497. [Google Scholar] [CrossRef]
- ELSO.org. ELSO Guidance Document: Use of ECMO in COVID-19 Patients during the PANDEMIC 3/24/2020 1632 EDT ELSO Guidance Document: ECMO for COVID-19 Patients with Severe Cardiopulmonary Failure. n.d. Available online: https://www.elso.org/Portals/0/Files/pdf/ECMO%20for%20COVID%2019%20Guidance%20Document.Final%2003.24.2020.pdf (accessed on 19 September 2022).
- George, I.; Salna, M.; Kobsa, S.; Deroo, S.; Kriegel, J.; Blitzer, D.; Shea, N.J.; D’Angelo, A.; Raza, T.; Kurlansky, P.; et al. The rapid transformation of cardiac surgery practice in the coronavirus disease 2019 (COVID-19) pandemic: Insights and clinical strategies from a centre at the epicentre. Eur. J. Cardiothorac. Surg. 2020, 58, 667–675. [Google Scholar] [CrossRef]
- Tang, P.C.; Haft, J.W.; Romano, M.A.; Bitar, A.; Hasan, R.; Palardy, M.; Aaronson, K.D.; Pagani, F.D. Right ventricular failure following left ventricular assist device implantation is associated with a preoperative pro-inflammatory response. J. Cardiothorac. Surg. 2019, 14, 80. [Google Scholar] [CrossRef]
- Russell, B.; Moss, C.; George, G.; Santaolalla, A.; Cope, A.; Papa, S.; Van Hemelrijck, M. Associations between immune-suppressive and stimulating drugs and novel COVID-19—A systematic review of current evidence. Ecancermedicalscience 2020, 14, 1022. [Google Scholar] [CrossRef]
- Kollmar, J.P.; Colquhoun, D.A.; Huffmyer, J.L. Anesthetic challenges for posterior spine surgery in a patient with left ventricular assist device: A case report: A case report. A A Case Rep. 2017, 9, 77–80. [Google Scholar] [CrossRef] [PubMed]
- Chau, V.Q.; Oliveros, E.; Mahmood, K.; Singhvi, A.; Lala, A.; Moss, N.; Gidwani, U.; Mancini, D.M.; Pinney, S.P.; Parikh, A. The imperfect cytokine storm: Severe COVID-19 with ARDS in a patient on durable LVAD support. JACC Case Rep. 2020, 2, 1315–1320. [Google Scholar] [CrossRef] [PubMed]
- ACS. COVID-19 Guidelines for Triage of Vascular Surgery Patients. Available online: https://www.facs.org/for-medical-professionals/COVID-19/clinical-guidance/elective-case/vascular-surgery/ (accessed on 19 September 2022).
- Fattouch, K.; Corrao, S.; Augugliaro, E.; Minacapelli, A.; Nogara, A.; Zambelli, G.; Argano, C.; Moscarelli, M. Cardiac surgery outcomes in patients with coronavirus disease 2019 (COVID-19): A case-series report. J. Thorac. Cardiovasc. Surg. 2022, 163, 1085–1092.e3. [Google Scholar] [CrossRef] [PubMed]
- Salna, M.; Polanco, A.; Bapat, V.; George, I.; Argenziano, M.; Takeda, K. A case of coronavirus disease 2019 (COVID-19) presenting after coronary artery bypass grafting. J. Thorac. Cardiovasc. Surg. 2020, 160, e193–e195. [Google Scholar] [CrossRef]
- Ad, N.; Luc, J.G.Y.; Nguyen, T.C. COVID-19 North American Cardiac Surgery Survey Working Group. Cardiac surgery in North America and coronavirus disease 2019 (COVID-19): Regional variability in burden and impact. J. Thorac. Cardiovasc. Surg. 2021, 162, 893–903.e4. [Google Scholar] [CrossRef]
- Al-Jabir, A.; Kerwan, A.; Nicola, M.; Alsafi, Z.; Khan, M.; Sohrabi, C.; O’Neill, N.; Iosifidis, C.; Griffin, M.; Mathew, G.; et al. Impact of the Coronavirus (COVID-19) pandemic on surgical practice—Part 1. Int. J. Surg. 2020, 79, 168–179. [Google Scholar] [CrossRef]
- Ng, J.J.; Ho, P.; Dharmaraj, R.B.; Wong, J.C.L.; Choong, A.M.T.L. The global impact of COVID-19 on vascular surgical services. J. Vasc. Surg. 2020, 71, 2182–2183.e1. [Google Scholar] [CrossRef]
- Persad, G.; Wertheimer, A.; Emanuel, E.J. Principles for allocation of scarce medical interventions. Lancet 2009, 373, 423–431. [Google Scholar] [CrossRef]
- White, D.B.; Lo, B. A framework for rationing ventilators and critical care beds during the COVID-19 pandemic. JAMA 2020, 323, 1773–1774. [Google Scholar] [CrossRef]
- Rocha, H.; Silva, I.; Antunes, I.; Veiga, C.; Mendes, D.; Veterano, C.; Castro, J.; Pinelo, A.; Almeida, R. The vascular surgery emergency department in times of COVID-19 pandemic. EJVES Vasc. Forum 2021, 50, 40. [Google Scholar] [CrossRef]
- Mouawad, N.J.; Woo, K.; Malgor, R.D.; Wohlauer, M.V.; Johnson, A.P.; Cuff, R.F.; Coleman, D.M.; Coogan, S.M.; Sheahan, M.G.; Shalhub, S. The impact of the COVID-19 pandemic on vascular surgery practice in the United States. J. Vasc. Surg. 2021, 73, 772–779.e4. [Google Scholar] [CrossRef] [PubMed]
- Mahenthiran, A.K.; Natarajan, J.P.; Bertges, D.J.; Huffman, K.M.; Eldrup-Jorgensen, J.; Lemmon, G.W. Impact of COVID-19 on the Society for Vascular Surgery Vascular Quality Initiative Venous Procedure Registries (varicose vein and inferior vena cava filter). J. Vasc. Surg. Venous Lymphat. Disord. 2021, 9, 1093–1098. [Google Scholar] [CrossRef] [PubMed]
- Lancaster, E.M.; Wu, B.; Iannuzzi, J.; Oskowitz, A.; Gasper, W.; Vartanian, S.; Wick, E.; Hiramoto, J.; Eichler, C.; Lobo, E.; et al. Impact of the coronavirus disease 2019 pandemic on an academic vascular practice and a multidisciplinary limb preservation program. J. Vasc. Surg. 2020, 72, 1850–1855. [Google Scholar] [CrossRef] [PubMed]
- Bozzani, A.; Arici, V.; Ticozzelli, G.; Franciscone, M.M.; Ragni, F.; Sterpetti, A.V. Reduced vascular practice and increased cardiovascular mortality for COVID-19-negative patients. J. Surg. Res. 2022, 272, 146–152. [Google Scholar] [CrossRef]
- Reyes Valdivia, A.; San Norberto, E.; Moreno, R.; Salmerón Febres, L.M.; Miralles, M.; Martínez López, I.; Zanabili, A. Massive drop in elective and urgent aortic procedures during the peak of the COVID-19 outbreak in Spanish multicenter analysis. J. Vasc. Surg. 2021, 73, 349–350. [Google Scholar] [CrossRef] [PubMed]
- Bensaid, A.; Melhaoui, I.; Oujidi, Y.; El Rhalete, A.; El Haddad, I.A.; Bkiyar, H.; Housni, B. Acute limb ischemia in patients with COVID-19 pneumonia. Ann. Med. Surg. 2021, 69, 102747. [Google Scholar] [CrossRef]
- Bozzani, A.; Arici, V.; Tavazzi, G.; Mojoli, F.; Bruno, R.; Sterpetti, A.V.; Ragni, F. Acute thrombosis of lower limbs arteries in the acute phase and after recovery from COVID19. Ann. Surg. 2021, 273, e159–e160. [Google Scholar] [CrossRef]
- Kahlberg, A.; Mascia, D.; Bellosta, R.; Attisani, L.; Pegorer, M.; Socrate, A.M.; Ferraris, M.; Trabattoni, P.; Rinaldi, E.; Melloni, A.; et al. Vascular Surgery during COVID-19 emergency in hub hospitals of Lombardy: Experience on 305 patients. Eur. J. Vasc. Endovasc. Surg. 2021, 61, 306–315. [Google Scholar] [CrossRef]
- Li, T.; Lu, H.; Zhang, W. Clinical observation and management of COVID-19 patients. Emerg. Microbes Infect. 2020, 9, 687–690. [Google Scholar] [CrossRef]
- Arachchillage, D.R.J.; Laffan, M. Abnormal coagulation parameters are associated with poor prognosis in patients with novel coronavirus pneumonia. J. Thromb. Haemost. 2020, 18, 1233–1234. [Google Scholar] [CrossRef]
- Bellosta, R.; Luzzani, L.; Natalini, G.; Pegorer, M.A.; Attisani, L.; Cossu, L.G.; Ferrandina, C.; Fossati, A.; Conti, E.; Bush, R.L.; et al. Acute limb ischemia in patients with COVID-19 pneumonia. J. Vasc. Surg. 2020, 72, 1864–1872. [Google Scholar] [CrossRef] [PubMed]
- Violi, F.; Pastori, D.; Cangemi, R.; Pignatelli, P.; Loffredo, L. Hypercoagulation and antithrombotic treatment in Coronavirus 2019: A new challenge. Thromb. Haemost. 2020, 120, 949–956. [Google Scholar] [CrossRef] [PubMed]
- Lippi, G.; Favaloro, E.J. D-dimer is associated with severity of Coronavirus disease 2019: A pooled analysis. Thromb. Haemost. 2020, 120, 876–878. [Google Scholar] [CrossRef] [PubMed]
- Leong Tan, G.W.; Chandrasekar, S.; Lo, Z.J.; Hong, Q.; Yong, E.; Lingam, P.; Zhang, L.; Quek, L.H.H.; Pua, U. Early experience in the COVID-19 pandemic from a vascular surgery unit in a Singapore tertiary hospital. J. Vasc. Surg. 2020, 72, 12–15. [Google Scholar] [CrossRef]
- Brinster, C.J.; Escousse, G.T.; Rivera, P.A.; Bazan, H.; Parkerson, R.; Leithead, C.; Money, S.R.; Sternbergh, W.C. Drastic increase in hospital labor costs during the COVID-19 pandemic leads to sustained financial loss for an academic vascular surgery division. J. Vasc. Surg. 2022, 75, e17–e18. [Google Scholar] [CrossRef]
- Wang, W.; Gurgone, A.; Martínez, H.; Barbieri Góes, M.C.; Gallo, E.; Kerényi, Á.; Turco, E.M.; Coburger, C.; Andrade, P.D. COVID-19 mortality and economic losses: The role of policies and structural conditions. J. Risk Financ. Manag. 2022, 15, 354. [Google Scholar] [CrossRef]
- Toscano, O.; Cosentino, N.; Campodonico, J.; Bartorelli, A.L.; Marenzi, G. Acute myocardial infarction during the COVID-19 pandemic: An update on clinical characteristics and outcomes. Front. Cardiovasc. Med. 2021, 8, 648290. [Google Scholar] [CrossRef]
- Vascular and Endovascular Research Network (VERN) COVER study collaborative*. Global impact of the first coronavirus disease 2019 (COVID-19) pandemic wave on vascular services. Br. J. Surg. 2020, 107, 1396–1400. [Google Scholar] [CrossRef]
- Pereira-Neves, A.; Domingos, L.F.; Ancetti, S. The impact of the first COVID-19 wave on European vascular education. EJVES Vasc. Forum 2022, 54, 54–57. [Google Scholar] [CrossRef]
- Iborra, E.; Landaluce, M.; Ocaña, J. Home surgical skills training on simulators for vascular surgery trainees during the COVID-19 pandemic on an online basis. EJVES Vasc. Forum 2022, 54, e3–e4. [Google Scholar] [CrossRef]
- COVIDSurg Collaborative. Elective surgery cancellations due to the COVID-19 pandemic: Global predictive modelling to inform surgical recovery plans: Elective surgery during the SARS-CoV-2 pandemic. Br. J. Surg. 2020, 107, 1440–1449. [Google Scholar] [CrossRef]
- Dexter, F.; Parra, M.C.; Brown, J.R.; Loftus, R.W. Perioperative COVID-19 defense: An evidence-based approach for optimization of infection control and operating room management: An evidence-based approach for optimization of infection control and operating room management. Anesth. Analg. 2020, 131, 37–42. [Google Scholar] [CrossRef] [PubMed]
- COVID-19 infection: Implications for perioperative and critical care physicians: Erratum. Anesthesiology 2020, 133, 693. [CrossRef] [PubMed]
- Perioperative management of patients infected with the novel Coronavirus: Recommendation from the joint task force of the Chinese society of anesthesiology and the Chinese association of anesthesiologists: Erratum. Anesthesiology 2020, 133, 693. [CrossRef] [PubMed]
- Herrod, P.J.J.; Adiamah, A.; Boyd-Carson, H.; Daliya, P.; El-Sharkawy, A.M.; Sarmah, P.B.; Hossain, T.; Couch, J.; Sian, T.S.; Wragg, A.; et al. Winter cancellations of elective surgical procedures in the UK: A questionnaire survey of patients on the economic and psychological impact. BMJ Open 2019, 9, e028753. [Google Scholar] [CrossRef]
- Hollander, J.E.; Carr, B.G. Virtually perfect? Telemedicine for COVID-19. N. Engl. J. Med. 2020, 382, 1679–1681. [Google Scholar] [CrossRef]
- Thomas, A.R.; Raats, J.W.; Lensvelt, M.M.A.; de Groot, H.G.W.; Veen, E.J.; van der Laan, L. Conservative treatment in selected patients with severe critical limb ischemia. World J. Surg. 2015, 39, 2090–2095. [Google Scholar] [CrossRef]
- Steunenberg, S.L.; Raats, J.W.; Te Slaa, A.; de Vries, J.; van der Laan, L. Quality of life in patients suffering from critical limb ischemia. Ann. Vasc. Surg. 2016, 36, 310–319. [Google Scholar] [CrossRef]
| Cardiovascular Condition Associated with COVID-19 | Mechanisms Implicated | Therapy/Management | References |
|---|---|---|---|
| Coagulopathy/thrombosis linked with COVID-19 | Reactivity of platelets, with viral-mediated endothelial inflammation and hypercoagulability, higher levels of coagulation factors, accumulated antiphospholipid antibodies, and lowered levels of intrinsic anticoagulant proteins | Antiaggregant/anticoagulant therapy | [42,43,44,45,46,47,48] |
| Peripheral venous diseases | Cytokine storm, systemic immune reaction, hypercoagulable condition, excessive inflammation, platelet activation, endothelial dysfunction, and stasis | Antiaggregant/anticoagulant therapy, venous ablation | [49,50,51,52] |
| Thromboembolism | Disease’s overall severity and its consequences | Low-molecular-weight heparin or fondaparinux instead of straight oral anticoagulants or fractionated heparin | [81] |
| Virus-induced myocarditis and myocardial impairment | Hypoxia or cytokine-mediated systemic inflammation | Depending on the symptomatology | [88] |
| Myocardial infarction | Elevated concentrations of circulating pro-inflammatory cytokines, macrophage involvement inside atherosclerotic plaques, plaque rupture, and thrombosis | Antiaggregant/anticoagulant therapy | [93] |
| Cardiomyopathies and myocarditis | Lymphocytic or eosinophilic infiltration of the heart, cytokine-induced inflammatory myocarditis | Depending on the symptomatology | [97] |
| Takotsubo cardiomyopathy | Direct myocardial damage, inflammation, and stress | Depending on the symptomatology | [104,105] |
| Arrhythmia and abrupt cardiac death | Systemic illness, systemic infection, inflammation, QTc-prolonging drugs, i.e., quinolone antibiotics or hydroxychloroquine | Pharmacological management, i.e., amiodarone and diltiazem | [107,108] |
| Heart failure | Invasion of inflammatory cells, proinflammatory cytokines, endothelial damage, microthrombosis, and hypoxia due to respiratory failure | Pharmacological management | [110,111,112,113,114] |
| Preoperative | Intraoperative | Postoperative |
|---|---|---|
| Constant COVID-19 infection screening prior to 24 to 48 h | Non-COVID surgical suites | Clean recuperation area |
| History of travel and possible exposure | Adaptation of negative-pressure ORs | Considering COVID-19 infection in the event of persistent respiratory distress |
| Accurate CXR evaluation | Airborne measures and PPE must be used by all suppliers | Reduce the risk of renal failure and persistent respiratory distress |
| Avoid unnecessary testing wherever feasible | Non-essential personnel to be absent from room | Protocol for accelerated recuperation, if applicable: Extubation, mobility, and disconnection of chest tubes and pacing wires as quickly is possible |
| Consider using previous test results wherever feasible | Just attending-level medical personnel | Shortly following extubation, patients receive surgical masks |
| Presurgical care delivered through telehealth | Video laryngoscopy to facilitate intubation | Timely collaboration with the family for postoperative recuperation at residence |
| Patients wear surgical masks before arriving at the hospital | Reduce worker turnover inside the room | Early release when clinically stable |
| Prompt intubation before surgery for patients with COVID-19 and respiratory dysfunction | Whenever possible, avoid TEE to prevent pleural invasion and lung harm | Following discharge, frequent and regular digital follow-up |
| Putting off a case if COVID-19 positive | Limit operations that involve CO2 insufflation | Test for COVID-19 if clinical signs are seen |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Axelerad, A.; Stuparu, A.Z.; Muja, L.F.; Docu Axelerad, S.; Petrov, S.G.; Gogu, A.E.; Jianu, D.C. Narrative Review of New Insight into the Influence of the COVID-19 Pandemic on Cardiovascular Care. Medicina 2022, 58, 1554. https://doi.org/10.3390/medicina58111554
Axelerad A, Stuparu AZ, Muja LF, Docu Axelerad S, Petrov SG, Gogu AE, Jianu DC. Narrative Review of New Insight into the Influence of the COVID-19 Pandemic on Cardiovascular Care. Medicina. 2022; 58(11):1554. https://doi.org/10.3390/medicina58111554
Chicago/Turabian StyleAxelerad, Any, Alina Zorina Stuparu, Lavinia Florenta Muja, Silviu Docu Axelerad, Silvia Georgeta Petrov, Anca Elena Gogu, and Dragos Catalin Jianu. 2022. "Narrative Review of New Insight into the Influence of the COVID-19 Pandemic on Cardiovascular Care" Medicina 58, no. 11: 1554. https://doi.org/10.3390/medicina58111554
APA StyleAxelerad, A., Stuparu, A. Z., Muja, L. F., Docu Axelerad, S., Petrov, S. G., Gogu, A. E., & Jianu, D. C. (2022). Narrative Review of New Insight into the Influence of the COVID-19 Pandemic on Cardiovascular Care. Medicina, 58(11), 1554. https://doi.org/10.3390/medicina58111554








