Abstract
Background and Objectives: Inappropriate antibiotic usage in hospitalized patients contributes to microbial resistance. Our study aimed to examine the incidence of clinical bacterial isolates and their antibiotic resistance burden among critically ill patients in different hospital units. Materials and Methods: A single-centered cross-sectional study was conducted in a 120-bed tertiary care hospital that included 221 critically ill patients with hospital-acquired infections. Bacterial cultures and sensitivity reports were obtained and followed by a formal analysis of the antibiogram results to explore recovered isolates’ prevalence and antibiotic susceptibility patterns. Results: Gram-negative bacteria were the most predominant pathogens among recovered isolates from the various hospital units (71%). Klebsiella sp. was the most prevalent microbe, followed by Acinetobacter sp., with an incidence level of 28% and 16.2%, respectively. Among the Gram-positive organisms, the coagulase-negative Staphylococci were the most predominant organism (11.3%), while (6.3%) methicillin-resistant Staphylococcus aureus (MRSA) isolates were recovered from different hospital units. Antibiotic sensitivity testing showed that polymyxin B was the most effective antibiotic against Gram-negative bacteria, whereas vancomycin and linezolid were the most active antibiotics against Gram-positive pathogens. Moreover, 7% of the Gram-negative bacteria isolated from different units showed positive production of extended-spectrum beta-lactamase (ESBL). Conclusions: The current study describes the high antibiotic resistance patterns in various hospital units that need extra legislation to prevent healthcare providers from misprescription and overuse of antibiotics.
1. Introduction
Nosocomial infections are spreading worldwide with millions of patients affected each year [1], especially in developing countries [2,3]. Nosocomial infection is an infection developed 2 to 3 days after admission to any healthcare unit or during a maximum of 3 days after leaving the unit in a condition that the patient was not infected with the same microbe on first admission [4]. Various species of Gram-negative and Gram-positive bacteria are causing nosocomial infections according to several epidemiological analyses [5].
The intensive care unit (ICU) is one of the leading units among healthcare settings in the percentage of the population with nosocomial infections [6], because of its patients who are susceptible to various infections due to immunodeficiency, utilization of invasive medical equipment, administration of various medications, or deformation of normal flora [7,8]. According to the Extended Prevalence of Infection in Intensive Care (EPIC) II, Gram-negative bacteria including Acinetobacter sp., Pseudomonas sp., Escherichia coli (E. coli), Klebsiella sp., and Enterobacter sp. had the highest overall predominance in the ICU, whereas Staphylococcus aureus (S. aureus) was the most predominant microbe among recovered microorganisms [9]. In addition, the high susceptibility of patients in the ICU to microbial infection leads to an increase in the chance of antibiotic resistance among ICU-derived pathogens [7,10].
The excessive use of antimicrobial agents in different healthcare units to combat various infectious diseases is one of the main causes of the emergence of antibiotic resistance in hospitals, leading to more and more nosocomial infections among patients [11,12]. Notably, the COVID-19 pandemic has recently caused a surge in antibiotic resistance, which is one of the most serious health issues affecting individuals worldwide [13]. Self-medication with antibiotics, empirical antibiotic therapy, and antibiotics prescribed by general practitioners were all risk factors for elevated antibiotic resistance levels during the COVID-19 outbreak [14]. In low- and middle-income nations with weak antibiotic control regimes, access to antibiotics without a prescription is directly impacted by both anxiety and improper antibiotic use [15]. Additionally, during the COVID-19 epidemic, the use of biocides greatly expanded on a global scale. The amount of indirect pressure that caused antibiotic resistance was probably increased by these biocides [16].
The predominance of multidrug-resistant (MDR) microorganisms that gain resistance to multiple antibiotics through inherent or acquired mechanisms restricts the choice of antimicrobials in their treatment, leading to a long stay of patients in hospitals and increased healthcare costs [3,17,18]. Thus, it is necessary to determine the prevalence of microbial pathogens and their antibiotic susceptibility patterns to employ an effective therapeutic strategy to combat their spread among patients, especially in healthcare units [3,19,20,21].
It is noteworthy that epidemiological studies investigating the prevalence of microbial pathogens and their resistance pattern are running day after day to help to manage the quick spread of microbial infections with multidrug-resistant bacteria. However, comprehensive updates on the prevalence of microbial pathogens with their susceptibility to different drugs in all healthcare locations are not available [22]. In addition, the microbial species among hospitals vary over time within different hospitals in the same country and even within various units in the same hospital. Furthermore, microbial resistance to antimicrobials is dynamic, with great changes taking place over time in antibiotics sensitivity patterns [3]. Herein, we aimed to examine the frequency of the various bacterial pathogens, including Gram-positive and Gram-negative bacteria, recovered from clinical specimens collected from patients in different hospital units in a tertiary care hospital. Moreover, our study focused on the susceptibility patterns of different microbes to various antibiotics to estimate antibiotic resistance burden and determine the best therapeutic agents available to fight against recovered microorganisms.
2. Materials and Methods
2.1. Study Design and Patients
This was a single-centered cross-sectional study conducted on a 120-bed tertiary care hospital in Cairo, Egypt, between January and July 2021. The study was approved by the Ethics Committee and Institutional Review Board of the Faculty of Pharmacy, Beni-Suef University, with approval number REC-H-PhBSU-22003, 16 February 2021. The study was carried out following the Helsinki Declaration’s principles.
Inclusion criteria included adult patients selected by non-random consecutive sampling technique who were aged >18 years and diagnosed with at least one hospital-acquired infection after 48 h of admissions, such as hospital-acquired pneumonia (HAP), ventilator-associated pneumonia (VAP), urinary tract infections (UTIs), bloodstream infections (BSIs), catheter-related bloodstream infections (CRBSIs), intra-abdominal infections (IAIs), and skin and skin soft tissue infections (SSTIs), within critical care units of the hospital including the general intensive care unit (ICU), intermediate care unit (INT), cardiac care unit (CCU), open-heart surgery unit (OH), and general surgery unit (SUR).
Exclusion criteria included outpatients, pregnancy, lactation, and a patient who started empirical antibiotics before collecting specimens or patients with evidence of infection at the time of hospital admission.
2.2. Isolation and Identification of the Clinical Isolates
Clinical samples of recruited patients (sputum, urine, wound, pus, and blood) were collected in sterile containers followed by isolation and identification of microorganisms from the specimens according to the standard protocols in the laboratory.
Aerobic culture media were used to inoculate the blood samples, while the rest of the clinical specimens were inoculated onto blood agar and cysteine lactose electrolyte deficient (CLED) using a calibrated wire loop (0.001 mL) and then incubated overnight at 37 °C. Gram-positive bacteria were cultured and identified using blood agar due to their hemolytic activity, while Gram-negative bacteria were cultured and identified using CLED based on their lactose fermentation capabilities. Significant colony counts were determined as those over 105 colony-forming units per milliliter (CFU/mL). Culture plates that exhibited no bacterial growth were incubated for a further 48 h.
The confirmation of bacterial identification was accomplished through Gram staining, morphological characterization, and different biochemical tests depending on the type of re-covered microorganisms, such as the catalase reaction, slide and tube coagulase tests, culture on DNase agar, and bile esculin for identification of Gram-positive bacteria, whereas biochemical tests such as oxidase, triple sugar iron, motility indole ornithine, citrate, lysine iron arginine, and urease tests were used to identify Gram-negative bacteria.
2.3. Antimicrobial Susceptibility Testing
All recovered microorganisms were tested for antibiotic susceptibility using the Kirby–Bauer disc diffusion method on Mueller–Hinton agar, and the findings were interpreted according to the Clinical and Laboratory Standard Institute (CLSI) guidelines [23]. The diameter of the zones of inhibition for each antibiotic was measured and interpreted as resistant, intermediate, or susceptible as pre-described in CLSI guidelines [23]. The choice of the tested antibiotics was based on the available drugs that were frequently prescribed in the hospital and on the spectrum of activity of the tested antimicrobials on Gram-positive and Gram-negative bacteria, as illustrated in Table S1.
Further, the clinical isolates of the Gram-positive S. aureus, which were cefoxitin-resistant, were assigned as MRSA as recommended by CSLI [23] and other previous reports [24]. Moreover, the production of ESBL in Gram-negative organisms was detected via the double-disc synergy test on Mueller–Hinton agar media according to the CLSI guidelines [23].
2.4. Statistical Analysis
The patients’ collected specimens and isolated bacterial strains, along with antibiotic sensitivity profiles were registered in the WHONET 5.6 software (WHO, Geneva, Switzerland), a windows-based database for the management and analysis of microbiology laboratory data with a particular focus on antimicrobial resistance surveillance, developed and supported by the WHO Collaborating Centre for Surveillance of Antimicrobial Resistance at the Brigham and Women’s Hospital in Boston, MA, USA [25]. Categorical data are presented as numbers and proportions. Normality testing was conducted using the Shapiro–Walk test. For non-normally distributed continuous data, the median and interquartile range was used. Statistical analyses were carried out using the Statistical Package for Social Sciences (SPSS), version 26 (SPSS Inc., Chicago, IL, USA). All graphs and charts in the study were prepared using EXCEL, (Microsoft Excel 2016 64-Bit Edition, Redmond, WA, USA) whereas the heatmaps were generated using the R-statistical platform (version x 64, 4.1.2, Toulouse, France) [26].
3. Results
3.1. Demographic Data of Included Patients
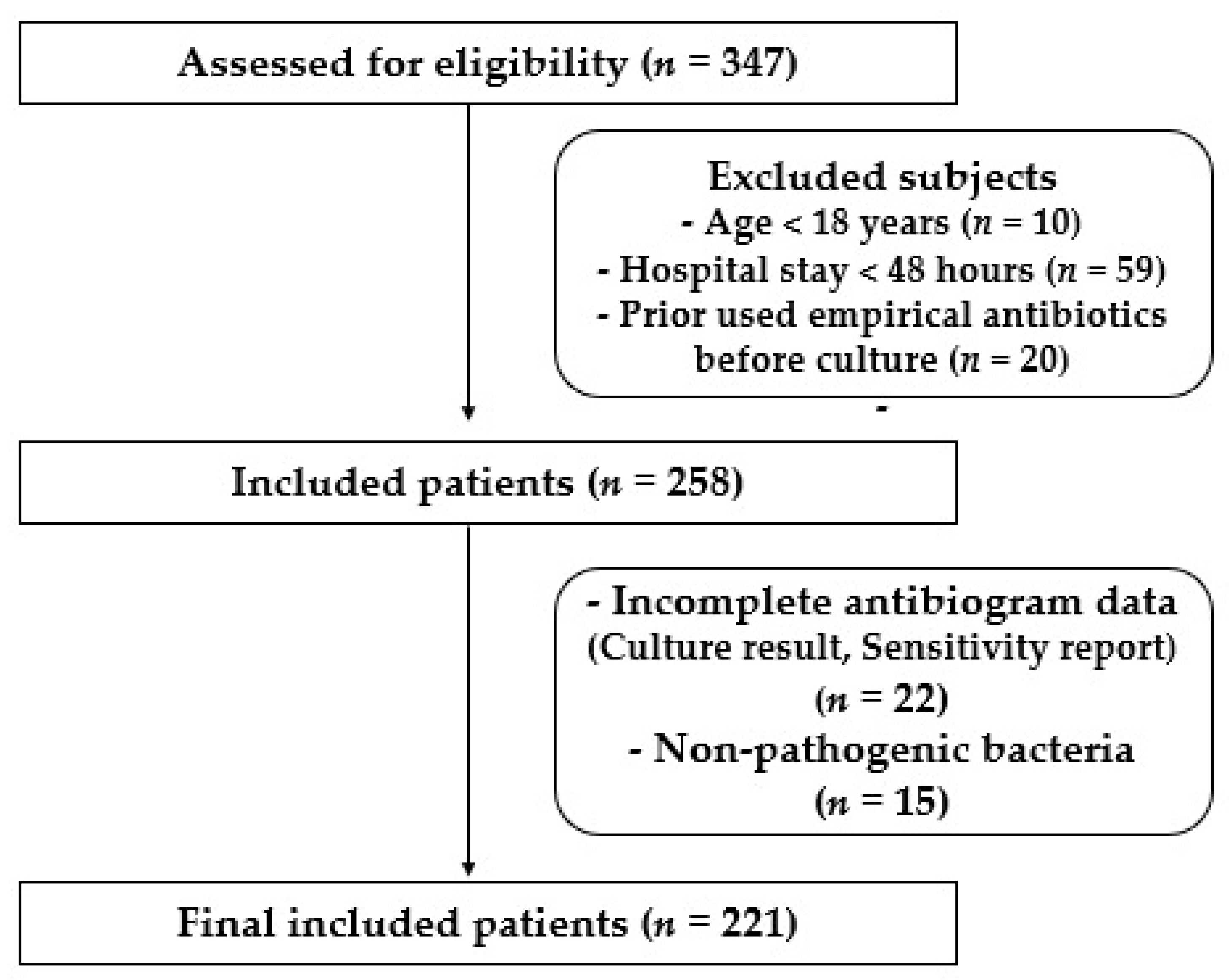
A total of 347 patients were assessed for eligibility; 111 patients did not meet inclusion criteria, while 221 patients with clinical evidence of hospital-acquired infection (HAP, VAP, BSI, CRBSI, IAI, UTI, and SSTI) were enrolled in the study as shown in Figure 1. Among the enrolled subjects, 156 patients (70.6%) were male. The majority (57.5%) of patients were found in the age group of >60 years with a median age of 65 years. Table 1 depicts the demographic characteristics of the patients.
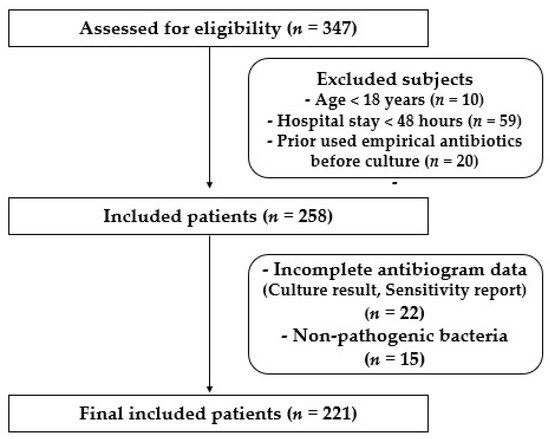
Figure 1.
Flow chart display recruited patients in the study.

Table 1.
Demographic data of included patients.
3.2. Prevalence of the Bacterial Isolates in Different Hospital Units
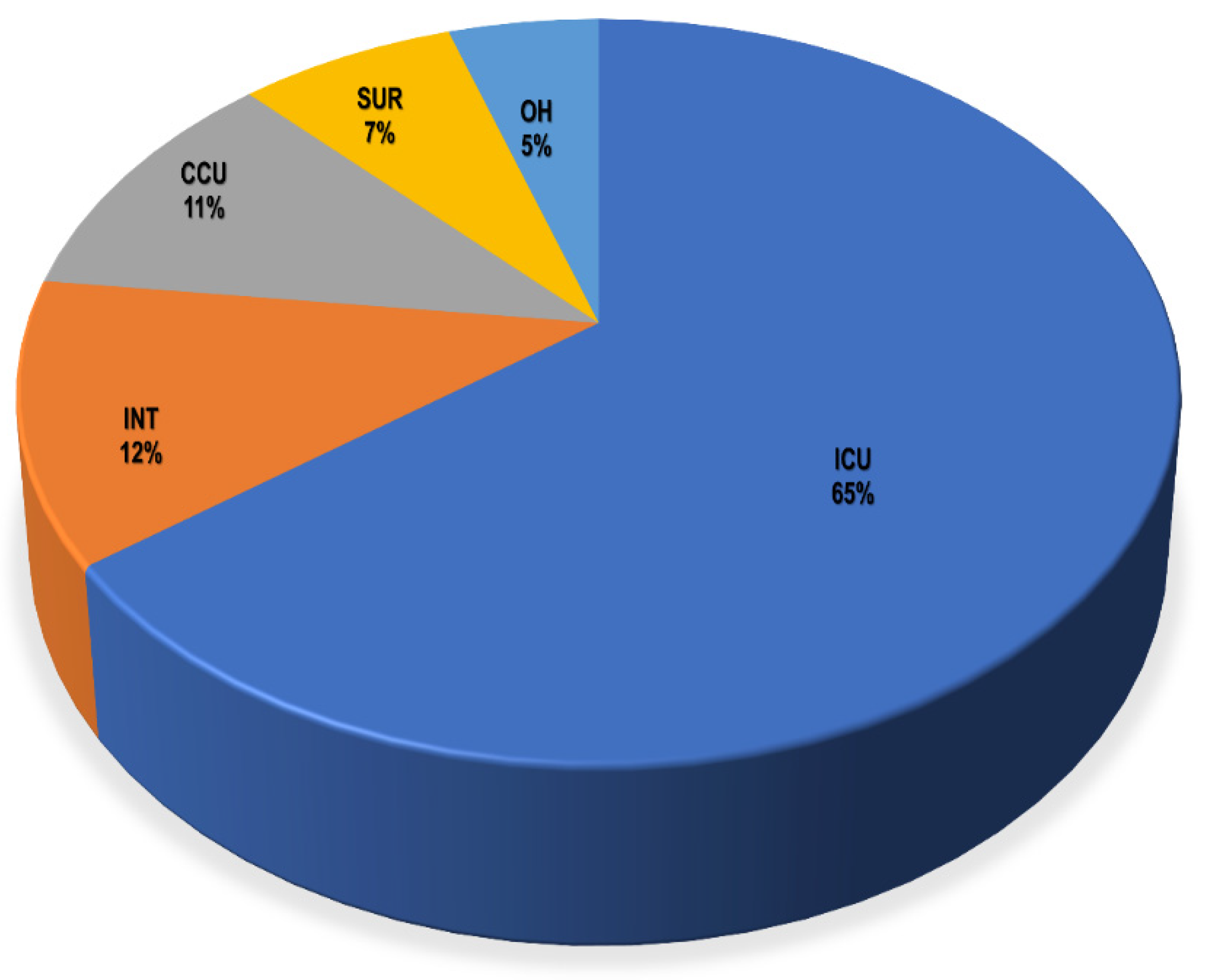
Clinical specimens from recruited patients in the ICU, CCU, INT, SUR, and OH yielded a total of 221 clinical isolates for testing. A total of 157 Gram-negative bacteria and 64 Gram-positive bacteria were isolated from different units (Table S2). The ICU had the biggest share of total isolates with 143 isolates (64.7%), followed by the INT from which 27 bacterial isolates (12.2%) were recovered, whereas the smallest number of recovered isolates was from the OH, with only 11 recovered microorganisms (5%), as shown in Figure 2 and Table S2. Regarding the recovered isolates, the Gram-negative bacteria Klebsiella sp. were the most predominant bacteria among them, with a total of 62 isolates, as presented in Table S3 and Figure S1. Next to Klebsiella sp., Acinetobacter sp., and Pseudomonas sp. as well as the Gram-positive bacteria, coagulase-negative Staphylococcus had total numbers of 36, 31, and 25, respectively.
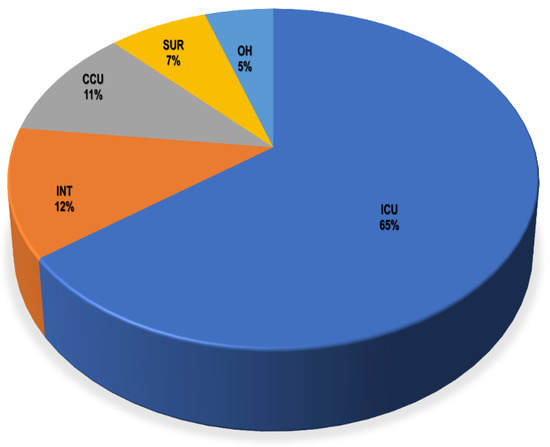
Figure 2.
Percentage of total recovered bacterial isolates from different hospital units. ICU: intensive care unit, INT: intermediate care unit, CCU: cardiac care unit, OH: open-heart surgery unit, SUR: general surgery unit.
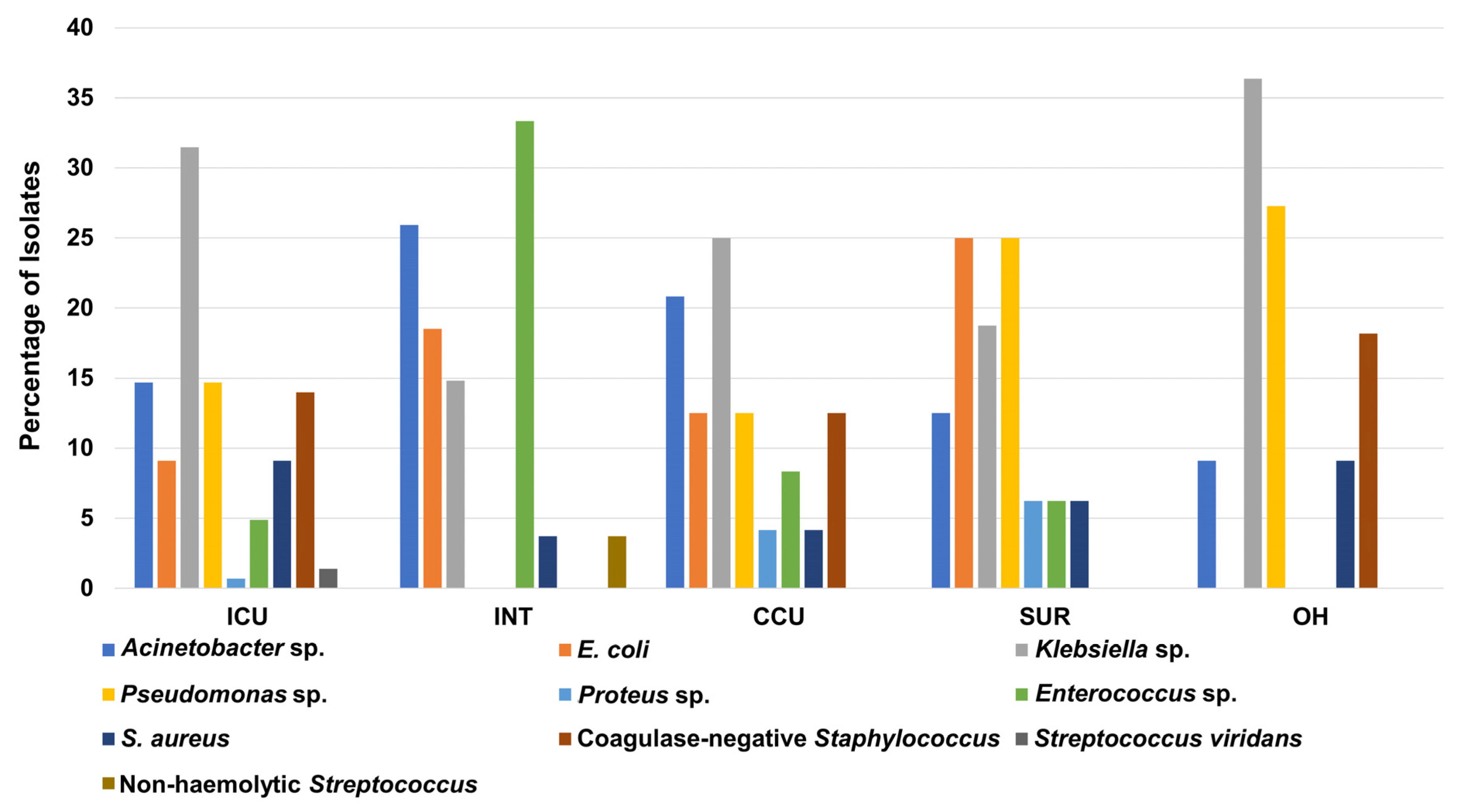
Similarly, Klebsiella sp. had the highest percentage of total isolates in the ICU, CCU, and OH with percentages of 31%, 25%, and 36%, respectively. In contrast, Acinetobacter sp. had the highest percentage in the INT with 26%, whereas E. coli and Pseudomonas sp. showed the biggest share among clinical isolates recovered from the SUR, with a percentage of 25% for both (Figure 3). As expected from the previous statistics, the ICU showed the highest number of bacterial isolates compared to other units for Acinetobacter sp., E. coli, Klebsiella sp., Pseudomonas sp., S. aureus, and coagulase-negative Staphylococcus (Table S4).
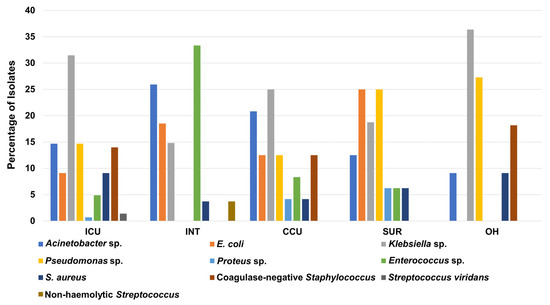
Figure 3.
Percentage of recovered Gram-positive and Gram-negative bacteria from patients in different hospital units. ICU: intensive care unit, INT: intermediate care unit, CCU: cardiac care unit, OH: open-heart surgery unit, SUR: general surgery unit.
On the other hand, extra investigation of the ICU which had the highest share of clinical isolates amongst all hospital units revealed that Klebsiella sp. was the most frequent microorganism among recovered ICU isolates, with a total of 45 isolates (31%), as shown in Table S4. Both Acinetobacter sp. and Pseudomonas sp. were the second most predominant microorganisms recovered from the ICU, with a total number of 21 isolates for both, followed by the Gram-positive bacteria, coagulase-negative Staphylococcus with a total of 20 isolates.
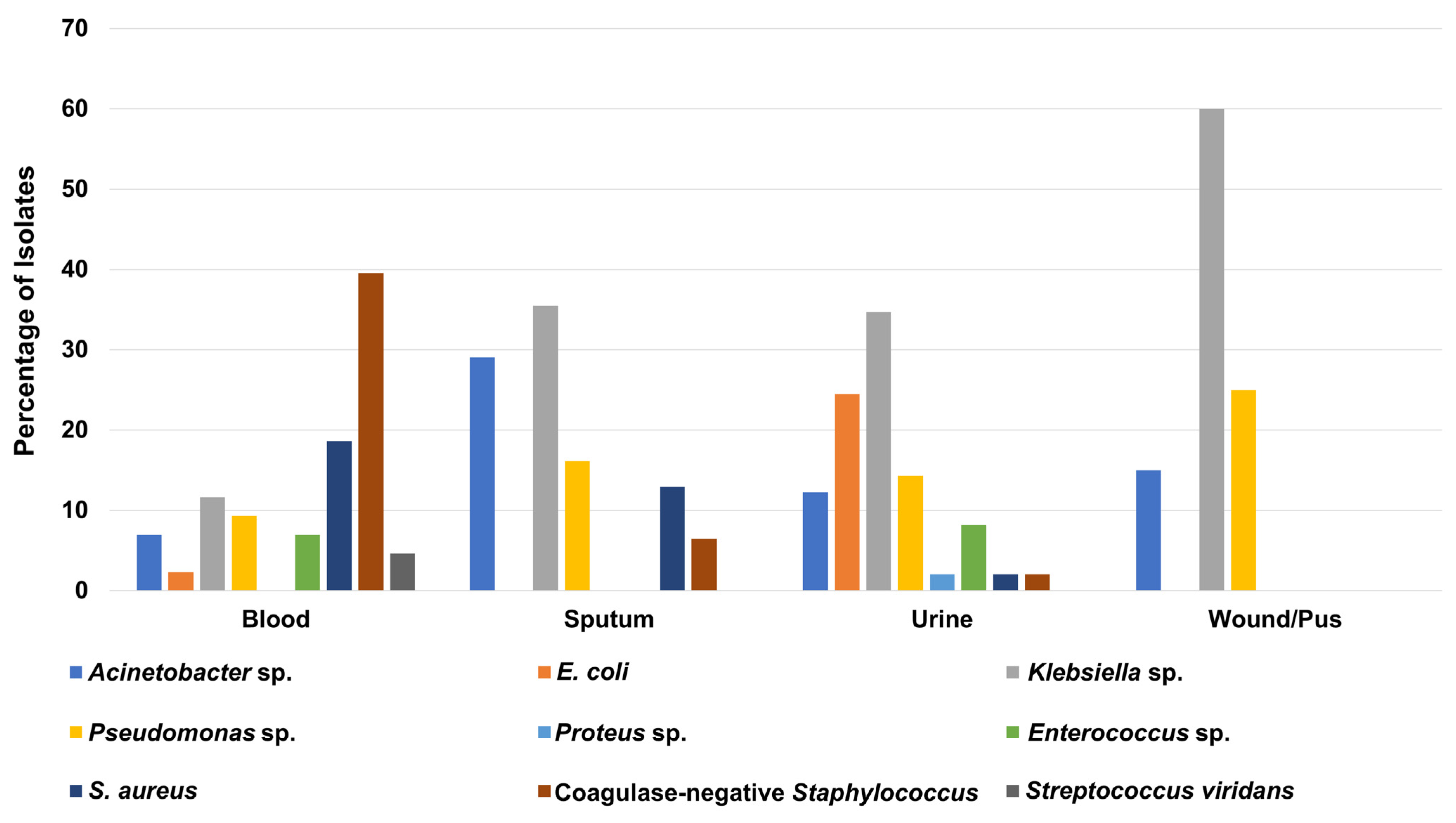
As presented in Table S5, more than one-third of ICU isolates (49 isolates; 34.3%) were recovered from urine samples, while 43 clinical isolates (30%) were isolated from blood samples. Interestingly, Klebsiella sp. was the most frequent microorganism in urine, pus/wound, and sputum samples, with total numbers of 17 (34.7%), 12 (60%), and 11 (35.5%) isolates, respectively (Figure 4 and Table S5). In contrast, the coagulase-negative Staphylococcus was the most predominant microbe among the blood samples collected from ICU patients, with a total of 17 (39.5%) isolates (Figure 4 and Table S5).
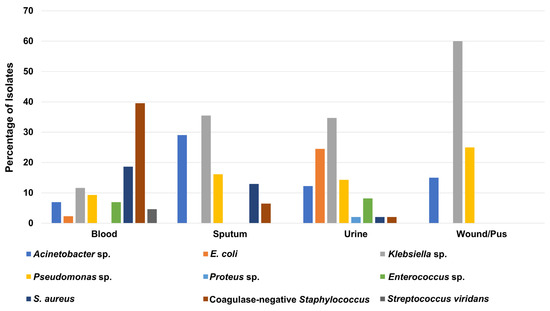
Figure 4.
Percentage of recovered Gram-positive and Gram-negative bacteria from different clinical specimens collected from patients in the intensive care unit.
3.3. Antibiotic Sensitivity Pattern of Recovered Isolates from Different Hospital Units
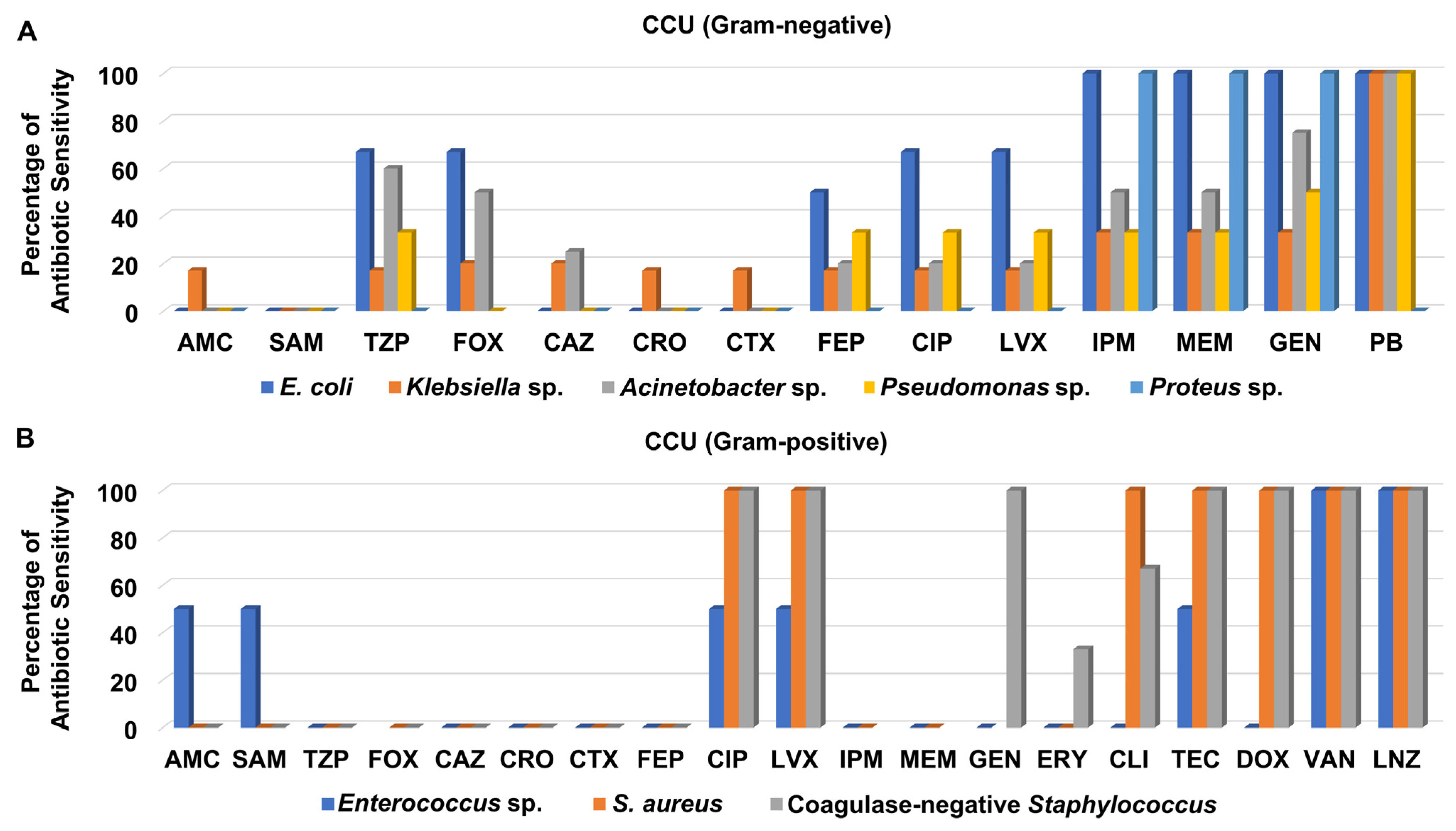
Screening of antibiotic sensitivity patterns of clinical isolates recovered from different specimens from the CCU revealed that most of the Gram-negative bacteria were not sensitive to the cephalosporins; ceftazidime, ceftriaxone, and cefotaxime as well as the aminopenicillins/beta-lactamase inhibitors; amoxicillin/clavulanate, and ampicillin/sulbactam (Figure 5A and Table S6). As presented in Figure 5A, both the carbapenems, imipenem and meropenem, and the aminoglycoside gentamicin exhibited moderate to good antibacterial activity against the Gram-negative bacteria isolated from CCU patients, especially against E. coli, Proteus sp. and Acinetobacter sp., while they showed weaker activity against Pseudomonas sp. and Klebsiella sp. It is noteworthy that polymyxin B displayed the best antimicrobial activity against all Gram-negative bacteria isolated from CCU patients except for Proteus sp.
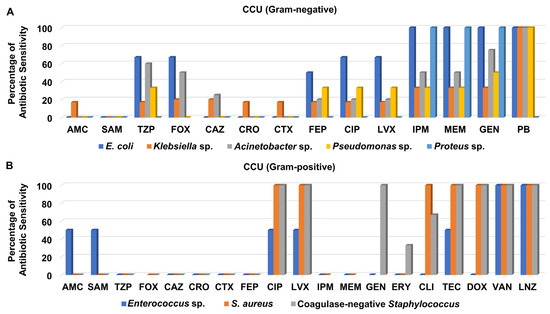
Figure 5.
Percentage of antibiotic sensitivity of different bacterial isolates recovered from the critical cardiac unit. (A) Antibiotic sensitivity pattern of Gram-negative bacteria. (B) Antibiotic sensitivity pattern of Gram-positive bacteria. AMC: amoxicillin/clavulanate, SAM: ampicillin/sulbactam, TZP: piperacillin/tazobactam, FOX: cefoxitin, CAZ: ceftazidime, CRO: ceftriaxone, CTX: cefotaxime, FEP: cefepime, CIP: ciprofloxacin, LVX: levofloxacin, IPM: imipenem, MEM: meropenem, GEN: gentamicin, PB: polymyxin B, ERY: erythromycin, CLI: clindamycin, TEC: teicoplanin, DOX: doxycycline, VAN: vancomycin, LNZ: linezolid.
On the other hand, most of the Gram-positive bacteria recovered from CCU patients were not susceptible to ceftazidime, ceftriaxone, cefotaxime, cefepime, and amoxicillin/clavulanate, ampicillin/sulbactam, piperacillin/tazobactam, and erythromycin (Figure 5B and Table S6). Only one isolate of S. aureus was recovered from CCU patients and assigned as MRSA. The clinical isolates of MRSA, and coagulase-negative Staphylococcus were sensitive to both levofloxacin and ciprofloxacin, whereas neither Enterococcus sp. nor MRSA were susceptible to either imipenem or meropenem. Interestingly, the isolates of MRSA and coagulase-negative Staphylococcus were sensitive to glycylcycline, teicoplanin, and tetracycline, doxycycline, whereas all CCU Gram-positive bacteria were susceptible to the glycopeptide vancomycin and the oxazolidinone linezolid (Figure 5B and Table S6).
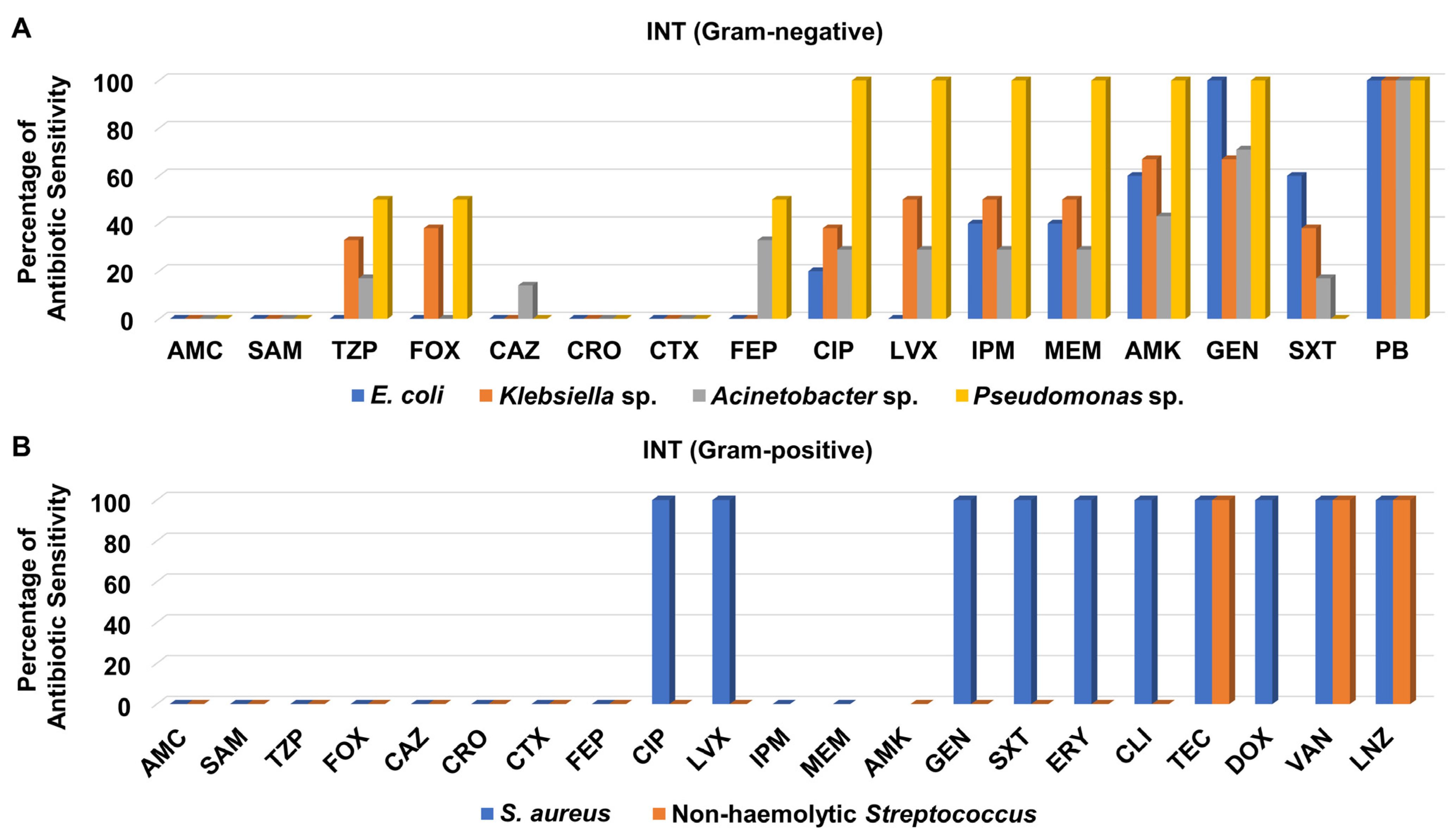
Like the CCU isolates, the Gram-negative bacteria recovered from the INT were not susceptible to ceftazidime, ceftriaxone, cefotaxime, amoxicillin/clavulanate, and ampicillin/sulbactam except for one Acinetobacter sp. isolate which was sensitive to ceftazidime (Figure 6A and Table S7). It is noteworthy that the aminoglycosides amikacin and gentamicin showed good antibacterial activity against most of the Gram-negatives isolates derived from INT patients, while polymyxin B was the best antibacterial agent evaluated with 100% sensitivity of all of them (Figure 6A).
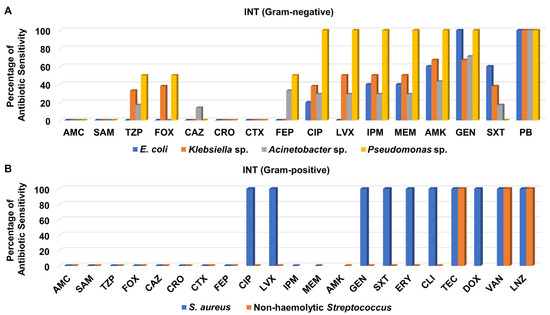
Figure 6.
Percentage of antibiotic sensitivity of different bacterial isolates recovered from the intermediate care unit. (A) Antibiotic sensitivity pattern of Gram-negative bacteria. (B) Antibiotic sensitivity pattern of Gram-positive bacteria. AMC: amoxicillin/clavulanate, SAM: ampicillin/sulbactam, TZP: piperacillin/tazobactam, FOX: cefoxitin, CAZ: ceftazidime, CRO: ceftriaxone, CTX: cefotaxime, FEP: cefepime, CIP: ciprofloxacin, LVX: levofloxacin, IPM: imipenem, MEM: meropenem, GEN: gentamicin, PB: polymyxin B, ERY: erythromycin, CLI: clindamycin, TEC: teicoplanin, DOX: doxycycline, VAN: vancomycin, LNZ: linezolid.
Although only one isolate of S. aureus was recovered from INT patients, it was recorded as MRSA. MRSA and non-hemolytic Streptococcus isolates recovered from the INT did not show any sensitivity to cefoxitin, ceftazidime, ceftriaxone, cefotaxime, cefepime, amoxicillin/clavulanate, ampicillin/sulbactam, and piperacillin/tazobactam (Figure 6B and Table S7). Notably, these isolates were totally sensitive to teicoplanin, vancomycin, and linezolid, as shown in Figure 6B.
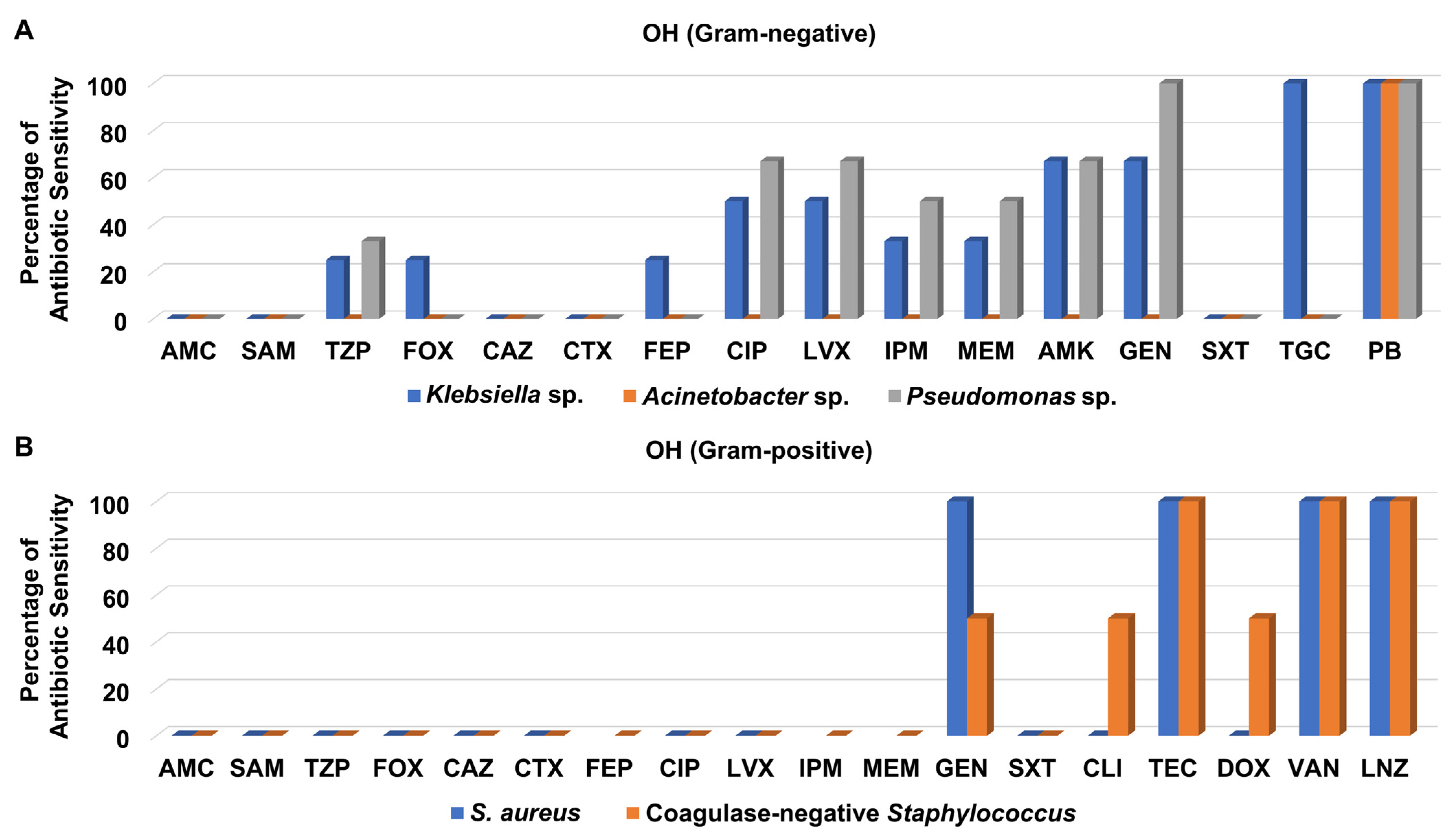
Regarding the Gram-negative bacteria isolated from the OH, they were not susceptible to amoxicillin/clavulanate, ampicillin/sulbactam, ceftazidime, cefotaxime, and trimethoprim/sulfamethoxazole (Figure 7A and Table S8). Notably, Klebsiella sp. and Pseudomonas sp. clinical isolates showed moderate to high sensitivity patterns to levofloxacin, ciprofloxacin, imipenem, meropenem, amikacin, and gentamicin, whereas Acinetobacter sp. isolate was not susceptible to any one of them. It is noteworthy that only Klebsiella sp. isolates were sensitive to tigecycline, while all Gram-negative bacteria isolated from the OH were susceptible to polymyxin B (Figure 7A and Table S8).
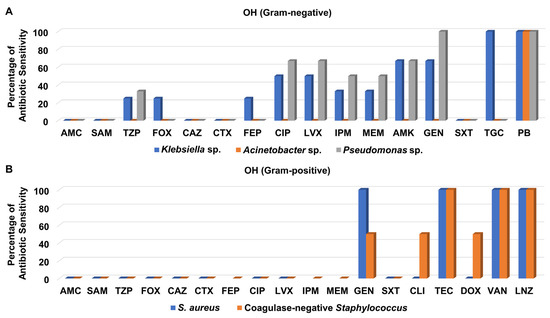
Figure 7.
Percentage of antibiotic sensitivity of different bacterial isolates recovered from the open-heart surgery unit. (A) Antibiotic sensitivity pattern of Gram-negative bacteria. (B) Antibiotic sensitivity pattern of Gram-positive bacteria. AMC: amoxicillin/clavulanate, SAM: ampicillin/sulbactam, TZP: piperacillin/tazobactam, FOX: cefoxitin, CAZ: ceftazidime, CRO: ceftriaxone, CTX: cefotaxime, FEP: cefepime, CIP: ciprofloxacin, LVX: levofloxacin, IPM: imipenem, MEM: meropenem, GEN: gentamicin, PB: polymyxin B, ERY: erythromycin, CLI: clindamycin, TEC: teicoplanin, DOX: doxycycline, VAN: vancomycin, LNZ: linezolid.
Only three Gram-positive bacteria were recovered from the OH, from which one S. aureus isolate was assigned as MRSA; they were not sensitive to amoxicillin/clavulanate, ampicillin/sulbactam, piperacillin/tazobactam, cefoxitin, ceftazidime, cefotaxime, levofloxacin, ciprofloxacin, and trimethoprim/sulfamethoxazole (Figure 7A and Table S8). However, they were all susceptible to teicoplanin, vancomycin, and linezolid, as presented in Figure 7B.
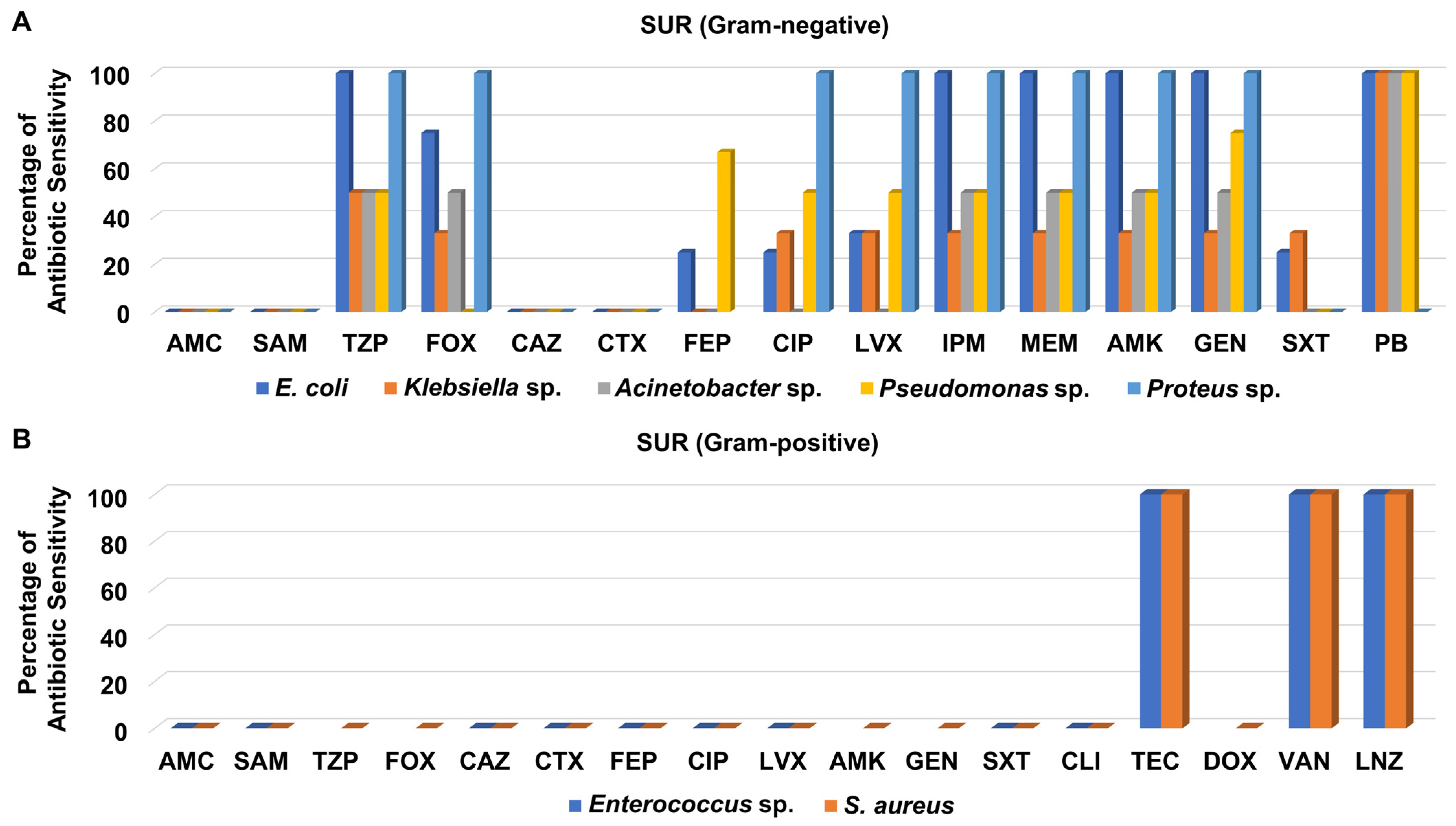
In contrast, the susceptibility of the Gram-negative bacteria isolated from the SUR to different antibiotics was somewhat better than that of isolates from the OH (Figure 8A). All tested Gram-negative isolates recovered from the SUR displayed moderate to high susceptibility to piperacillin/tazobactam, imipenem, meropenem, amikacin, and gentamicin (Figure 8A and Table S9). Like in other units, polymyxin B was the best antibiotic against various SUR-derived Gram-negative bacteria.
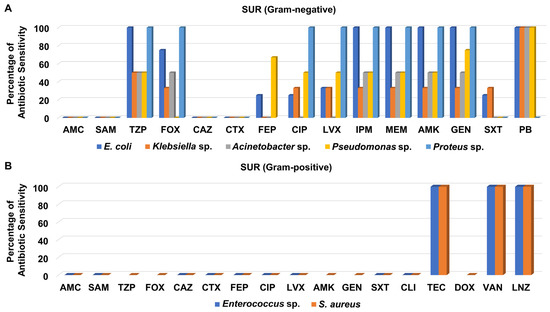
Figure 8.
Percentage of antibiotic sensitivity of different bacterial isolates recovered from the general surgery unit. (A) Antibiotic sensitivity pattern of Gram-negative bacteria. (B) Antibiotic sensitivity pattern of Gram-positive bacteria. AMC: amoxicillin/clavulanate, SAM: ampicillin/sulbactam, TZP: piperacillin/tazobactam, FOX: cefoxitin, CAZ: ceftazidime, CRO: ceftriaxone, CTX: cefotaxime, FEP: cefepime, CIP: ciprofloxacin, LVX: levofloxacin, IPM: imipenem, MEM: meropenem, GEN: gentamicin, PB: polymyxin B, ERY: erythromycin, CLI: clindamycin, TEC: teicoplanin, DOX: doxycycline, VAN: vancomycin, LNZ: linezolid.
On the other hand, the two Gram-positive isolates recovered from the SUR, which were MRSA and Enterococcus sp., were not susceptible to most of the tested antibacterial agents, including amoxicillin/clavulanate, ampicillin/sulbactam, ceftazidime, cefotaxime, cefepime, levofloxacin, ciprofloxacin, and clindamycin, as shown in Figure 8B and Table S9. By contrast, both isolates were only sensitive to teicoplanin, vancomycin, and linezolid.
Interestingly, the Gram-negative bacteria isolated from ICU patients displayed no or weak susceptibility patterns to many tested antibiotics such as ampicillin/sulbactam, amoxicillin/clavulanate, ceftazidime, cefotaxime, ceftriaxone, and cefepime (Table S10 and Figures S2–S7). Notably, many of them displayed moderate to high susceptibility to the aminoglycosides amikacin and gentamicin, as well as the carbapenems imipenem and meropenem. Like other Gram-negative microorganisms in our study, the highest sensitivity pattern of the ICU’s Gram-negative isolates was recorded for polymyxin B (Figure S2).
Investigation of the antibiotic susceptibility patterns of the most predominant bacterial isolates in the ICU, which were Klebsiella sp., revealed that most of them did not show susceptibility to ampicillin/sulbactam, amoxicillin/clavulanate, ceftazidime, ceftriaxone, cefotaxime, cefepime, and trimethoprim/sulfamethoxazole (Table S10 and Figure S3). Markedly, their susceptibility to imipenem, meropenem, amikacin, and gentamicin was better than that of other previously mentioned antibiotics, whereas polymyxin B was the most active antibacterial agent against them (Figure S3).
Regarding Acinetobacter sp. and Pseudomonas sp. Isolates, which were the second most predominant species among Gram-negative microbes recovered from ICU patients, the clinical isolates of Pseudomonas sp. displayed better sensitivity patterns to ciprofloxacin, levofloxacin, amikacin, and gentamicin than Acinetobacter sp., (Table S10 and Figures S4 and S6). By contrast, Acinetobacter sp. isolates showed quite better susceptibility to trimethoprim/sulfamethoxazole for different clinical isolates and nitrofurantoin in urine isolates. Although polymyxin B was not active against one urine isolate of Acinetobacter sp., it was active against all other strains of Acinetobacter sp. and Pseudomonas sp. (Table S10).
Most of the Gram-positive bacteria recovered from ICU patients displayed either no or very weak sensitivity to amoxicillin/clavulanate, ampicillin/sulbactam, piperacillin/tazobactam, cefotaxime, ceftazidime, ceftriaxone, and cefepime (Table S11 and Figures S8–S12). Interestingly, many of them showed either good or high susceptibility to ciprofloxacin, levofloxacin, doxycycline, gentamicin, and nitrofurantoin. Similar to other Gram-positive bacteria recovered in our study, the best antibacterial agents evaluated against various ICU Gram-positive microbes were teicoplanin, vancomycin, and linezolid (Figure S8).
As presented in Table S11 and Figure S9, isolates of the coagulase-negative Staphylococcus recovered from blood and sputum specimens showed moderate susceptibility to the macrolide antibiotics erythromycin and azithromycin, while teicoplanin, vancomycin, and linezolid, and to less extent, doxycycline exhibited the best antibacterial activity when assessed against many coagulase-negative Staphylococcus strains isolated from various clinical samples from ICU patients including urine, blood, and sputum. Similarly, the clinical isolates of S. aureus recovered from ICU patients as the second most predominant Gram-positive microbe among ICU-retrieved bacteria displayed a somewhat comparable susceptibility pattern to the coagulase-negative Staphylococcus (Table S11 and Figure S10). Among the S. aureus isolates detected in the ICU, 10 isolates out of 11 tested against cefoxitin were MRSA (91%), with 3 of them recovered from sputum specimens and 1 recovered from urine specimens, as well as 7 isolates obtained from blood cultures, whereas all MRSA isolates showed high sensitivity to vancomycin and linezolid.
Among the isolated Gram-negative bacteria, 7% (11/157) were ESBL-producing organisms, whereas Klebsiella sp. was the most predominant ESBL producer, with 12.9% of Klebsiella isolates (8/62) having positive production of ESBL. In all, 8% (2/25) of the isolated E. coli and 33.3% (1/3) of Proteus sp. isolates were ESBL-producing microorganisms. Interestingly, 45.4% of the ESBL-producing organisms were isolated from urine specimens followed by sputum specimens (27.2%), wound swabs (18.1%), and blood cultures (9.09%). The highest ESBL producers were isolated from the ICU patients (54.5%) followed by the SUR (27.2%).
Regarding the ESBL-producing organisms, piperacillin/tazobactam, carbapenems, aminoglycosides, and polymyxin B were the most effective antibiotics against the isolates of E. coli, Klebsiella sp., and Proteus sp., while levofloxacin and ciprofloxacin were found least efficacious, especially against Klebsiella sp.
4. Discussion
In this hospital-based analysis of surveillance data from a tertiary care hospital, we surveyed the antibiotic sensitivity profiles of both Gram-positive and Gram-negative nosocomial pathogens isolated from different clinical specimens collected from various healthcare units in the hospital. Our study revealed that the most abundant Gram-negative organisms in all the hospital units were Klebsiella sp., Acinetobacter sp., and Pseudomonas sp., while Staphylococcus sp. was the commonest Gram-positive organism. This agrees with the EPIC II study in African hospitals [27]. Further, our study revealed that the emergence of microbial resistance especially among Gram-negative bacteria has been increasing steadily. These data are in line with trends described from different regions all over the world which are considered threatening issues [28,29].
This big increase in antibiotic resistance could be attributed to different reasons, including the inappropriate use of antibiotics which increased recently during the COVID-19 pandemic, as discussed above. Antibiotics were used during the COVID-19 pandemic to treat bacterial infections that coexisted with COVID-19 infections or to take advantage of their potential antiviral effects; however, the relationship between antibiotic resistance and COVID-19 infection was controversial, as several studies suggested that there had been an increase in antibiotic resistance, while the most prevalent bacteria with high antibiotic resistance were Acinetobacter baumannii and Klebsiella pneumonia from the Gram-negative bacteria in addition to S. aureus and Enterococcus faecalis from the Gram-positive bacteria [3,6,7], which are quite similar to our findings. However, some other studies assumed that the COVID-19 era did not affect antibiotic resistance among microbes [30].
The highest susceptibility rates recorded in most hospital units for Klebsiella sp., Acinetobacter sp., and Pseudomonas sp. were to polymyxin B, which is truly alarming because polymyxin B is one of the last choices in antibiotic therapy. The constant downward trend in piperacillin/tazobactam, imipenem, meropenem, ciprofloxacin, and levofloxacin activity versus Gram-negative pathogens was one of the most important findings of our research, although in many Gram-negative microorganisms, the susceptibility rates of imipenem and meropenem were slightly better than in piperacillin/tazobactam, ciprofloxacin, and levofloxacin. On the other hand, the susceptibility rate to aminoglycosides such as amikacin and gentamicin was noted to be high in different specimens, which may be due to the smaller frequency of usage due to its nephrotoxicity [31]. Additionally, a high pattern of resistance to ampicillin, amoxicillin, ceftriaxone, cefepime, and ceftazidime was recorded. This is consistent with findings from other studies on the antibiotic resistance of Gram-negative bacilli in critically ill individuals [32,33]. These findings of moderate to high resistance patterns of numerous recovered Gram-negative bacteria from different hospital units to several antibiotics from different antibiotic classes such as penicillins, cephalosporins, carbapenems, penicillins/beta-lactamase inhibitors, and quinolones indicate the growing chance of detecting various antibiotic-degrading enzymes such as the b-lactamases carbapenemase, extended-spectrum beta-lactamases, and metallo-beta-lactamases, among others.
Interestingly, 7% of the Gram-negative bacilli recovered in our study were ESBL producers. In other different studies, the percentage of ESBL generation has been found to range from 17% to 70% [34,35]. However, in the investigation by Sharma et al., ESBL production was shown to be 52.49% [36].
Indeed, S. aureus, coagulase-negative Staphylococcus, and Enterococcus species were the most prevalent Gram-positive organisms in our data analysis of this study, while we found a significant sensitivity pattern of most Gram-positive bacteria to linezolid, teicoplanin, and vancomycin. Interestingly, their susceptibility to ciprofloxacin, levofloxacin, doxycycline, gentamicin, erythromycin, azithromycin, clindamycin, and nitrofurantoin has varied between moderate and high among S. aureus and coagulase-negative Staphylococcus isolates, whereas a worse sensitivity pattern was recorded for Enterococci isolates. These results agreed with the antibiogram of the Gram-positive isolates in various studies [37,38,39]. It is noteworthy that 14 isolates out of 15 S. aureus isolates (93%) recovered from different units and tested against cefoxitin were recorded as MRSA, which is an alarming health problem due to limited options for its treatment. By contrast, a previous study conducted by Srikanth et al. found that the MRSA percentage among the coagulase-positive S. aureus was 32.2% [40], while another study by Pai et al. found that out of 237 S. aureus isolates, 69 isolates (29.1%) were recorded as MRSA [41].
In the present study, the antibiogram of our general ICU showed that the Gram-negative organism Klebsiella sp. was the most prevalent bacterium in ICU with a percentage of 31%. This high virulence can be related to the fact that these bacteria are part of the normal flora of the human host’s mouth, oropharynx, GI tracts, skin, and intestines [42]. This finding opposes earlier research, notably a study from the United States, which claimed that Pseudomonas aeruginosa was the most prevalent bacterium (31.6%) [43] whereas another study in Egypt performed by Elkolaly et al. concluded that Pseudomonas sp. was the most prevalent Gram-negative pathogen (37.5%), followed by Klebsiella sp. (25%) [44]. However, a recent study in Egypt by Negm et al. revealed that the incidence of Klebsiella sp. among recovered pathogens was 33.51% [45].
Most of the Klebsiella sp. recovered from the ICU showed low susceptibility to carbapenems, especially in blood cultures (25%), sputum specimens (36%), and wound specimens (27% meropenem and 45% imipenem). This finding is in agreement with the results obtained by Qadeer et al., as carbapenem resistance of Klebsiella was 56% for meropenem and 55% for imipenem [46], while in urine specimens, 62% of Klebsiella sp. isolates were sensitive to meropenem and 67% to imipenem, which is corroborated by Rajan et al. who documented 28.13% carbapenem resistance of Klebsiella [47]. Sheth et al. demonstrated 100% sensitivity of Klebsiella to carbapenems [48]. In addition, Klebsiella sp. recovered from most specimens displayed a low sensitivity pattern to aminoglycosides, which is consistent with results obtained by Gunjal et al., who reported that 60% of Klebsiella were resistant to amikacin, and 80% were resistant to gentamicin [49].
Similarly, clinical isolates of Acinetobacter sp. recovered from blood and sputum exhibited no or bad sensitivity to carbapenems, with a percentage of 0% and 11%, respectively, for imipenem and 0% and 12% for meropenem. Our finding matches the findings obtained by Qadeer et al., who found 0% sensitivity of Acinetobacter to carbapenems [46]. Other findings by Khan reported 79% resistance of Acinetobacter to imipenem [50], whereas Rajan et al. found that 52% of Acinetobacter isolates were resistant to carbapenems [47]. Moreover, most Acinetobacter isolates recovered from blood, pus, and sputum were not sensitive to aminoglycosides and quinolones. Similarly, Negm and coworkers revealed that Acinetobacter was highly resistant to aminoglycosides (82.2% gentamicin and 67.9% amikacin) and fluoroquinolones (91.6% ciprofloxacin and 79.9 levofloxacin) [45].
On the other hand, clinical isolates of Pseudomonas Sp. showed moderate to high susceptibility to carbapenems (50–71% for imipenem and 25–86% for meropenem). Similarly, another study conducted by Rakhee et al. showed that 20.8% of Pseudomonas isolates were resistant to imipenem [51]. In addition, another previous study performed by Rajan et al. showed a high sensitivity pattern of Pseudomonas isolates to carbapenems, as only 12.9% of Pseudomonas isolates were resistant to carbapenems 40 [40]. In contrast, Negm et al.’s study revealed that Pseudomonas isolates were less sensitive to carbapenems (82.7% resistance to imipenem and 84.7% resistance to meropenem) [45]. Moreover, Pseudomonas displayed no or bad sensitivity to most third- and fourth-generation cephalosporins, while they showed moderate to high aminoglycoside susceptibility for most isolates. Radji et al. showed weak sensitivity of Pseudomonas isolates to ceftriaxone (60.9% resistance), and amikacin was seen to be the most efficient antibiotic against Pseudomonas infections, with only 15.6% resistance [52].
Furthermore, E. coli is one of the most prevalent organisms that cause urinary tract infections and it exhibited high sensitivity to carbapenems, with susceptibility rates of 83% for both imipenem and meropenem, confirming the low resistance of E. coli to carbapenems, as shown previously by Qadeer et al., who reported that only 10% of E. coli were carbapenem-resistant [46]. Another study reported that 34% of E. coli isolates were resistant to amikacin. and 53.2% were resistant to gentamicin [44], which is consistent with our results, as 80% of our E. coli isolates were sensitive to amikacin, while 50% were susceptible to gentamicin.
The most common Gram-positive organism in ICU was the coagulase-negative Staphylococcus (14%), which was sensitive to vancomycin and linezolid, with 100% susceptibility. This was followed by S. aureus and Enterococcus, with a prevalence of 9% and 5% in ICU, respectively. Further, their sensitivity to vancomycin and linezolid was 100%. Interestingly, Savanur et al. found similar results in their previous study. Among Gram-positive microbes, the coagulase-negative Staphylococci were the most commonly isolated organisms (15.6%), especially in blood cultures [53]. Indeed, Radha Rani et al. also mentioned that the most prevalent Gram-positive isolates were the coagulase-negative Staphylococci (52.80%), followed by S. aureus (14.40%) and Enterococcus species (10.14%) [54], while Chidambaram et al. showed that among Gram-positive isolates, Enterococcus was the most frequently recovered bacterium (4.79%), followed by S. aureus (3.72%) [55].
In addition, our findings regarding the antibiotic sensitivity pattern of the recovered Gram-positive bacteria were in agreement with earlier studies by Kaur et al., who reported that Gram-positive bacterial isolates showed maximum sensitivity towards vancomycin (100%), whereas the coagulase-negative Staphylococcus and S. aureus were resistant to commonly used antibiotics, including ampicillin, amoxicillin, cloxacillin, and cefoxitin [56]. However, in contrast to our results, Savanur et al. found that the coagulase-negative Staphylococcus isolates were 100% resistant to vancomycin [53].
In the present study, we also observed the consequences of local antibiograms among patients undergoing cardiac surgery, postoperative cardiac surgical patients, and those admitted to the CCU. For instance, Klebsiella, Acinetobacter, and Pseudomonas were the most commonly isolated organisms in the CCU and OH. Klebsiella, Acinetobacter, and Pseudomonas isolates recovered from CCU patients showed low or no sensitivity patterns to many tested antibiotics, including ceftazidime, cefotaxime, cefepime, ciprofloxacin, levofloxacin, meropenem, and imipenem. Davoudi et al. reported the incidence of resistance to ceftazidime, ceftriaxone, and ciprofloxacin among Klebsiella sp. at 71.42%, 57.1%, and 57.1%, respectively [57].
Additionally, we found that 25% of recovered isolates from patients in the CCU were Gram-positive cocci which were extremely sensitive to vancomycin, teicoplanin, and linezolid, except for Enterococci isolates, which were moderately sensitive to teicoplanin (50%). This finding is corroborated by Parameswarappa et al., who showed that Enterococci were sensitive to linezolid (98%), vancomycin (64%), and teicoplanin (59.3%) [58]. Gram-positive bacteria may be prevalent in the CCU due to the incidence of cardiac implanted devices, coronary catheterization, and infectious endocarditis [59].
The prevalence results in the SUR showed that the Gram-negative bacteria were the predominant infectious agents in patients admitted to the general surgery unit, while E. coli and Pseudomonas sp., followed by Klebsiella sp., were the most prevalent organisms. E. coli was found to be less sensitive to ciprofloxacin and levofloxacin, whereas Pseudomonas sp. and Klebsiella sp. showed low and moderate carbapenem resistance, respectively. Like other hospital units, both S. aureus and Enterococcus sp. recovered from the SUR were susceptible to vancomycin, linezolid, and teicoplanin, while they were non-susceptible to trimethoprim/sulfamethoxazole, clindamycin, and ampicillin. These findings are consistent with the study on surgical site wound infections in Mulago and Ugandan [60,61].
Lastly, the high frequency of resistance should raise the alarm and highlight the requirement of regular monitoring of the local prevalence of resistance, which could help to determine the most effective antimicrobial treatment and direct experimental therapy.
Given the high, grave, and frightening occurrence of antimicrobial resistance and the restricted availability of empirical antibiotics, a comprehensive effort to battle this enemy should be a top national priority. This program includes infection control policies, care bundles, an antimicrobial stewardship program (ASP), quality, and education. Until the successful deployment of ASP, the only solutions for our ICUs based on the current antibiogram data will be the combination of antibiotics and the provision of newly available drug generations [62]. The present study has some limitations which should be taken into consideration: first, because other bacterial identification systems were required, we were unable to properly identify most of the bacterial isolates at the species level. Second, the use of non-random consecutive sampling techniques may have led to bias in patient recruitment. Third, the fact that this was a single-center study may limit how well our findings generalize to other centers. However, the study methodology can be translated to other hospitals to ascertain their local susceptibilities, and our simulation data can be applied to other units in a more generalized approach.
5. Conclusions
Most of the infections at the hospital units in our study led to resistance to most available antibiotics. The last-resort antibiotics, polymyxin B for the Gram-negative bacteria and linezolid for the Gram-positive bacteria, were the only sensitive antibiotics in most hospital-acquired infections. This implies an eventual crisis that threatens the healthcare profession and warrants heightened awareness. Extra legislation is required to prevent healthcare providers from misprescribing and overusing antibiotics, and healthcare providers also need to be better educated on how and when to administer antibiotics in both pandemic and everyday settings.
Supplementary Materials
The following supporting information can be downloaded at: https://www.mdpi.com/article/10.3390/medicina58111597/s1, Figure S1. The total number of different Gram-positive and Gram-negative bacteria recovered from various hospital units, Figure S2. Heatmap of the percentage of antibiotic sensitivity of the Gram-negative isolates recovered from intensive care unit, Figure S3. Antibiotic sensitivity pattern of different isolates of Klebsiella sp. recovered from different clinical specimens from intensive care unit, Figure S4. Antibiotic sensitivity pattern of different isolates of Acinetobacter sp. recovered from different clinical specimens from intensive care unit, Figure S5. Antibiotic sensitivity pattern of different isolates of Pseudomonas sp. recovered from different clinical specimens from intensive care unit, Figure S6. Antibiotic sensitivity pattern of different isolates of E. coli recovered from different clinical specimens from intensive care unit, Figure S7. Antibiotic sensitivity pattern of different isolates of Proteus sp. recovered from different clinical specimens from intensive care unit, Figure S8. Heatmap of the percentage of antibiotic sensitivity of the Gram-positive isolates recovered from intensive care unit, Figure S9. Antibiotic sensitivity pattern of different isolates of Coagulase-negative Staphylococcus recovered from different clinical specimens from intensive care unit, Figure S10. Antibiotic sensitivity pattern of different isolates of S. aureus recovered from different clinical specimens from intensive care unit, Figure S11. Antibiotic sensitivity pattern of different isolates of Enterococcus sp. recovered from different clinical specimens from intensive care unit, Figure S12. Antibiotic sensitivity pattern of different isolates of Streptococcus viridans recovered from different clinical specimens from intensive care unit, Table S1. List of antibiotics and their classes used in the antibiotic susceptibility testing of the recovered isolates in the study, Table S2. The total number of recovered bacterial isolates from different hospital units, Table S3. The total numbers of different Gram-positive and Gram-negative bacteria recovered from various hospital units, Table S4. The total numbers of different Gram-positive and Gram-negative bacteria recovered from each hospital unit, Table S5. The total number of different Gram-positive and Gram-negative bacteria recovered from various clinical specimens from patients in intensive care unit, Table S6. Antibiotic sensitivity pattern of different bacterial isolates recovered from the critical cardiac unit in terms of percentage of sensitive isolates, Table S7. Antibiotic sensitivity pattern of different bacterial isolates recovered from the intermediate care unit in terms of percentage of sensitive isolates, Table S8. Antibiotic sensitivity pattern of different bacterial isolates recovered from the open-heart surgery unit in terms of percentage of sensitive isolates, Table S9. Antibiotic sensitivity pattern of different bacterial isolates recovered from the general surgery unit in terms of percentage of sensitive isolates, Table S10. Antibiotic sensitivity pattern of Gram-negative isolates recovered from intensive care unit in terms of percentage of sensitive isolates, Table S11. Antibiotic sensitivity pattern of Gram-positive isolates recovered from intensive care unit in terms of percentage of sensitive isolates.
Author Contributions
R.M.S. and A.E.A.W., study idea and design, methodology, conceptualization, writing, and editing; F.M. and M.S., data processing, analysis, and interpretation, writing, and editing; A.N.M.; G.M.-H., B.F.A. and H.F.S., supervision, drafting of the article, and revision. All authors have read and agreed to the published version of the manuscript.
Funding
This work was funded by the Deanship of Scientific Research at Jouf University under grant No. (DSR-2021-01-0379).
Institutional Review Board Statement
The study was approved by the Ethics Committee and Institutional Review Board of the Faculty of Pharmacy, Beni-Suef University at 16 February 2021, (Approval Number: REC-H-PhBSU-22003). The study was conducted under the principles outlined in the Declaration of Helsinki.
Informed Consent Statement
Written informed consent was obtained from all the participants in the study.
Data Availability Statement
Available upon request from the corresponding author.
Conflicts of Interest
The authors declare no conflict of interest.
References
- World Health Organization. Health Care-Associated Infections Fact Sheet; World Health Organization: Geneva, Switzerland, 2015; p. 4. [Google Scholar]
- Rezai, M.-S.; Bagheri-Nesami, M.; Nikkhah, A. Catheter-related urinary nosocomial infections in intensive care units: An epidemiologic study in North of Iran. Casp. J. Intern. Med. 2017, 8, 76–82. [Google Scholar] [CrossRef]
- Mekonnen, H.; Seid, A.; Fenta, G.M.; Gebrecherkos, T. Antimicrobial resistance profiles and associated factors of Acinetobacter and Pseudomonas aeruginosa nosocomial infection among patients admitted at Dessie comprehensive specialized Hospital, North-East Ethiopia. A cross-sectional study. PLoS ONE 2021, 16, e0257272. [Google Scholar] [CrossRef] [PubMed]
- Horan, T.C.; Andrus, M.; Dudeck, M.A. CDC/NHSN surveillance definition of health care–associated infection and criteria for specific types of infections in the acute care setting. Am. J. Infect. Control. 2008, 36, 309–332. [Google Scholar] [CrossRef]
- Khawaja, A.; Arshad, F.; Munir, S. Acinetobacter species: Prevalence and sensitivity pattern of Acinetobacter species among clinical isolates of tertiary care hospital. Prof. Med. J. 2018, 25, 1949–1953. [Google Scholar]
- Warda, A.E.A.; Sarhan, R.M.; Al-Fishawy, H.S.; Moharram, A.N.; Salem, H.F. Continuous Versus Intermittent Linezolid Infusion for Critically Ill Patients with Hospital-Acquired and Ventilator-Associated Pneumonia: Efficacy and Safety Challenges. Pharmaceuticals 2022, 15, 296. [Google Scholar] [CrossRef]
- Brusselaers, N.; Vogelaers, D.; Blot, S. The rising problem of antimicrobial resistance in the intensive care unit. Ann. Intensiv. Care 2011, 1, 47. [Google Scholar] [CrossRef]
- Marwick, C.; Davey, P. Care bundles: The holy grail of infectious risk management in hospital? Curr. Opin. Infect. Dis. 2009, 22, 364–369. [Google Scholar] [CrossRef]
- Vincent, J.-L.; Sakr, Y.; Singer, M.; Martin-Loeches, I.; Machado, F.R.; Marshall, J.C.; Finfer, S.; Pelosi, P.; Brazzi, L.; Aditianingsih, D.; et al. Prevalence and Outcomes of Infection Among Patients in Intensive Care Units in 2017. JAMA 2020, 323, 1478–1487. [Google Scholar] [CrossRef]
- Carlet, J.; Ali, A.B.; Tabah, A.; Willems, V.; Philippar, F.; Chafine, A.; Misset, B. Multidrug resistant infections in the ICU: Mechanisms, prevention and treatment. In 25 Years of Progress and Innovation in Intensive Care Medicine; Kuhlen, R., Moreno, R., Ranieri, V.M., Rhodes , A., Eds.; Medizinisch Wissenschaftliche Verlagsgesellschaft: Berlin, Germany, 2007; pp. 199–211. [Google Scholar]
- Baym, M.; Stone, L.K.; Kishony, R. Multidrug evolutionary strategies to reverse antibiotic resistance. Science 2016, 351, aad3292. [Google Scholar] [CrossRef]
- Scaglione, V.; Reale, M.; Davoli, C.; Mazzitelli, M.; Serapide, F.; Lionello, R.; La Gamba, V.; Fusco, P.; Bruni, A.; Procopio, D.; et al. Prevalence of Antibiotic Resistance Over Time in a Third-Level University Hospital. Microb. Drug Resist. 2022, 28, 425–435. [Google Scholar] [CrossRef]
- Livermore, D.M. Antibiotic resistance during and beyond COVID-19. JAC-Antimicrob. Resist. 2021, 3, i5–i16. [Google Scholar] [CrossRef] [PubMed]
- Sulayyim, H.J.A.; Ismail, R.; Al Hamid, A.; Ghafar, N.A. Antibiotic Resistance during COVID-19: A Systematic Review. Int. J. Environ. Res. Public Health 2022, 19, 11931. [Google Scholar] [CrossRef] [PubMed]
- Zavala-Flores, E.; Salcedo-Matienzo, J. Medicación prehospitalaria en pacientes hospitalizados por COVID-19 en un hospital público de Lima-Perú. Acta Médica Peru. 2020, 37, 393–395. [Google Scholar] [CrossRef]
- Getahun, H.; Smith, I.; Trivedi, K.; Paulin, S.; Balkhy, H.H. Tackling antimicrobial resistance in the COVID-19 pandemic. Bull. World Health Organ. 2020, 98, 442–442A. [Google Scholar] [CrossRef]
- Morales, E.; Cots, F.; Sala, M.; Comas, M.; Belvis, F.; Riu, M.; Salvadó, M.; Grau, S.; Horcajada, J.P.; Montero, M.M.; et al. Hospital costs of nosocomial multi-drug resistant Pseudomonas aeruginosa acquisition. BMC Health Serv. Res. 2012, 12, 122. [Google Scholar] [CrossRef]
- Huang, H.; Chen, B.; Liu, G.; Ran, J.; Lian, X.; Huang, X.; Wang, N.; Huang, Z. A multi-center study on the risk factors of infection caused by multi-drug resistant Acinetobacter baumannii. BMC Infect. Dis. 2018, 18, 11. [Google Scholar] [CrossRef]
- Hassan, M.A.; El-Aziz, S.A.; Elbadry, H.M.; El-Aassar, S.A.; Tamer, T.M. Prevalence, antimicrobial resistance profile, and characterization of multi-drug resistant bacteria from various infected wounds in North Egypt. Saudi J. Biol. Sci. 2022, 29, 2978–2988. [Google Scholar] [CrossRef]
- Khan, H.A.; Baig, F.K.; Mehboob, R. Nosocomial infections: Epidemiology, prevention, control and surveillance. Asian Pac. J. Trop. Biomed. 2017, 7, 478–482. [Google Scholar] [CrossRef]
- Moghadam, M.T.; Khoshbayan, A.; Chegini, Z.; Farahani, I.; Shariati, A. Bacteriophages, a New Therapeutic Solution for Inhibiting Multidrug-Resistant Bacteria Causing Wound Infection: Lesson from Animal Models and Clinical Trials. Drug Des. Dev. Ther. 2020, 14, 1867–1883. [Google Scholar] [CrossRef]
- Murray, C.J.; Ikuta, K.S.; Sharara, F.; Swetschinski, L.; Aguilar, G.R.; Gray, A.; Han, C.; Bisignano, C.; Rao, P.; Wool, E.; et al. Global burden of bacterial antimicrobial resistance in 2019: A systematic analysis. Lancet 2022, 399, 629–655. [Google Scholar] [CrossRef]
- CLSI M100-S15; Performance Standards for Antimicrobial Susceptibility Testing, 28th Edition. Clinical and Laboratory Standards Institute (CLSI): Wayne, PA, USA, 2018.
- Datta, P.; Gulati, N.; Singla, N.; Vasdeva, H.R.; Bala, K.; Chander, J.; Gupta, V. Evaluation of various methods for the detection of meticillin-resistant Staphylococcus aureus strains and susceptibility patterns. J. Med. Microbiol. 2011, 60, 1613–1616. [Google Scholar] [CrossRef] [PubMed][Green Version]
- WHONET Software. Available online: https://whonet.org/ (accessed on 16 March 2022).
- R-Project. Available online: https://www.r-project.org/about.html (accessed on 22 March 2022).
- Vincent, J.-L.; Rello, J.; Marshall, J.K.; Silva, E.; Anzueto, A.; Martin, C.D.; Moreno, R.; Lipman, J.; Gomersall, C.; Sakr, Y.; et al. International Study of the Prevalence and Outcomes of Infection in Intensive Care Units. JAMA 2009, 302, 2323–2329. [Google Scholar] [CrossRef] [PubMed]
- Tacconelli, E.; Carrara, E.; Savoldi, A.; Harbarth, S.; Mendelson, M.; Monnet, D.L.; Pulcini, C.; Kahlmeter, G.; Kluytmans, J.; Carmeli, Y.; et al. Discovery, research, and development of new antibiotics: The WHO priority list of antibiotic-resistant bacteria and tuberculosis. Lancet Infect. Dis. 2018, 18, 318–327. [Google Scholar] [CrossRef]
- Kaye, K.S.; Pogue, J.M. Infections Caused by Resistant Gram-Negative Bacteria: Epidemiology and Management. Pharmacother. J. Hum. Pharmacol. Drug Ther. 2015, 35, 949–962. [Google Scholar] [CrossRef] [PubMed]
- Ghosh, S.; Bornman, C.; Zafer, M.M. Antimicrobial Resistance Threats in the emerging COVID-19 pandemic: Where do we stand? J. Infect. Public Health 2021, 14, 555–560. [Google Scholar] [CrossRef] [PubMed]
- Paquette, F.; Bernier-Jean, A.; Brunette, V.; Ammann, H.; Lavergne, V.; Pichette, V.; Troyanov, S.; Bouchard, J. Acute Kidney Injury and Renal Recovery with the Use of Aminoglycosides: A Large Retrospective Study. Nephron 2015, 131, 153–160. [Google Scholar] [CrossRef]
- Lockhart, S.R.; Abramson, M.A.; Beekmann, S.E.; Gallagher, G.; Riedel, S.; Diekema, D.; Quinn, J.P.; Doern, G.V. Antimicrobial Resistance among Gram-Negative Bacilli Causing Infections in Intensive Care Unit Patients in the United States between 1993 and 2004. J. Clin. Microbiol. 2007, 45, 3352–3359. [Google Scholar] [CrossRef]
- Morris, S.; Cerceo, E. Trends, Epidemiology, and Management of Multi-Drug Resistant Gram-Negative Bacterial Infections in the Hospitalized Setting. Antibiotics 2020, 9, 196. [Google Scholar] [CrossRef]
- Gopalakrishnan, R.; Sureshkumar, D. Changing trends in antimicrobial susceptibility and hospital acquired infections over an 8 year period in a tertiary care hospital in relation to introduction of an infection control programme. J. Assoc. Physicians India 2010, 58, 25–31. [Google Scholar]
- Patel, B.V.; Patel, P.G.; Raval, P.N.; Patel, M.H.; Patel, P.H.; Vegad, M.M. Bacteriological profile and antibiogram of Gram negative organisms isolated from medical and neurology intensive care unit with special reference to multi-drug resistant organisms. Natl. J. Med. Res. 2012, 2, 335–338. [Google Scholar]
- Sharma, M.; Pathak, S.; Srivastava, P. Prevalence and antibiogram of Extended Spectrum β-Lactamase (ESBL) producing Gram negative bacilli and further molecular characterization of ESBL producing Escherichia coli and Klebsiella spp. J. Clin. Diagn. Res. 2013, 7, 2173. [Google Scholar] [CrossRef] [PubMed]
- Khullar, S.; Rathore, L.; Khatri, P.K.; Parihar, R.S.; Meena, S.; Bora, A.; Maurya, V.; Sharma, N. Identification and Antibiogram of Various Gram Positive Bacterial Isolates from Pyogenic Samples by VITEK® 2 Compact System. Int. J. Curr. Microbiol. Appl. Sci. 2016, 5, 66–77. [Google Scholar] [CrossRef]
- Soltani, R.; Khalili, H.; Abdollahi, A.; Rasoolinejad, M.; Dashti-Khavidaki, S. Nosocomial Gram-positive antimicrobial susceptibility pattern at a referral teaching hospital in Tehran, Iran. Futur. Microbiol. 2012, 7, 903–910. [Google Scholar] [CrossRef]
- Alhumaid, S.; Al Mutair, A.; Al Alawi, Z.; Alzahrani, A.J.; Tobaiqy, M.; Alresasi, A.M.; Bu-Shehab, I.; Al-Hadary, I.; Alhmeed, N.; Alismail, M.; et al. Antimicrobial susceptibility of gram-positive and gram-negative bacteria: A 5-year retrospective analysis at a multi-hospital healthcare system in Saudi Arabia. Ann. Clin. Microbiol. Antimicrob. 2021, 20, 1–18. [Google Scholar] [CrossRef] [PubMed]
- Mir, B.A.; Srikanth. Prevalence and Antimicrobial Susceptibility of methicillin resistant Staphylococcus aureus and coagulase-negative Staphylococci in a tertiary care hospital. Asian J. Pharm. Clin. Res. 2013, 6, 231–234. [Google Scholar]
- Pai, V.; I Rao, V.; Rao, S.P. Prevalence and Antimicrobial Susceptibility Pattern of Methicillin-resistant Staphylococcus Aureus [MRSA] Isolates at a Tertiary Care Hospital in Mangalore, South India. J. Lab. Physicians 2010, 2, 082–084. [Google Scholar] [CrossRef] [PubMed]
- Munoz-Price, L.S.; Poirel, L.; A Bonomo, R.; Schwaber, M.J.; Daikos, G.L.; Cormican, M.; Cornaglia, G.; Garau, J.; Gniadkowski, M.; Hayden, M.K.; et al. Clinical epidemiology of the global expansion of Klebsiella pneumoniae carbapenemases. Lancet Infect. Dis. 2013, 13, 785–796. [Google Scholar] [CrossRef]
- Neuhauser, M.M.; Weinstei, R.A.; Rydman, R.; Danziger, L.H.; Karam, G.; Quinn, J.P. Antibiotic resistance among Gram-negative bacilli in US intensive care units: Implications for fluoroquinolone use. JAMA 2003, 289, 885–888. [Google Scholar] [CrossRef]
- Elkolaly, R.M.; Bahr, H.M.; El-Shafey, B.I.; Basuoni, A.S.; Elber, E.H. Incidence of ventilator-associated pneumonia: Egyptian study. Egypt. J. Bronchol. 2019, 13, 258–266. [Google Scholar] [CrossRef]
- Negm, E.M.; Mowafy, S.M.S.; Mohammed, A.A.; Amer, M.G.; Tawfik, A.E.; Ibrahim, A.E.S.; Hassan, T.H. Antibiograms of intensive care units at an Egyptian tertiary care hospital. Egypt. J. Bronchol. 2021, 15, 1–15. [Google Scholar] [CrossRef]
- Qadeer, A.; Akhtar, A.; Ain, Q.U.; Saadat, S.; Mansoor, S.; Assad, S.; Ishtiaq, W.; Ilyas, A.; Khan, A.Y.; Ajam, Y. Antibiogram of Medical Intensive Care Unit at Tertiary Care Hospital Setting of Pakistan. Cureus 2016, 8, e809. [Google Scholar] [CrossRef] [PubMed]
- Rajan, R.; Rao, A. Antibiogram of Gram-negative bacterial isolates from intensive care unit at a tertiary care hospital. IJAR 2016, 6, 344–347. [Google Scholar]
- Sheth, K.; Patel, T.; Malek, S.; Tripathi, C. Antibiotic Sensitivity Pattern of Bacterial Isolates from the Intensive Care Unit of a Tertiary Care Hospital in India. Trop. J. Pharm. Res. 2013, 11, 991–999. [Google Scholar] [CrossRef]
- Gunjal, P.N.; Gunjal, S.; Kher, S. A Cross-sectional study to determine the profile and antibiotic resistance pattern of gram negative bacilli isolated from intensive care unit patients in a tertiary care hospital in ahmednagar, maharashtra. Int. J. Biomed. Adv. Res. 2012, 3, 281–284. [Google Scholar] [CrossRef]
- Khan, M.A. Bacterial spectrum and susceptibility patterns of pathogens in ICU and IMCU of a secondary care hospital in Kingdom of Saudi Arabia. Int. J. Pathol. 2018, 16, 64–70. [Google Scholar]
- Raakhee, T.; Rao, U.S. Prevalence and resistance pattern of Pseudomonas strains isolated from ICU patients. Int. J. Curr. Microbiol. App. Sci. 2014, 3, 527–534. [Google Scholar]
- Radji, M.; Fauziah, S.; Aribinuko, N. Antibiotic sensitivity pattern of bacterial pathogens in the intensive care unit of Fatmawati Hospital, Indonesia. Asian Pac. J. Trop. Biomed. 2011, 1, 39–42. [Google Scholar] [CrossRef]
- Savanur, S.S.; Gururaj, H. Study of Antibiotic Sensitivity and Resistance Pattern of Bacterial Isolates in Intensive Care Unit Setup of a Tertiary Care Hospital. Indian J. Crit. Care Med. 2019, 23, 547–555. [Google Scholar] [CrossRef]
- Vanitha, R.N.; Gopal, K.; Narendra, M.V.; Vishwakanth, D. A retrospective study on blood stream infections and antibiotic susceptibility patterns in a tertiary care teaching hospital. Int. J. Pharm. Pharm. Sci. 2012, 4, 543–548. [Google Scholar]
- Chidambaram, N.; Ambujam, G.; Rajan, R.; Sasikala, G.; Anandi, V. Antimicrobial profile of clinical isolates in intensive care unit at a tertiary care hospital. Int. J. Med. Res. Health Sci. 2019, 8, 160–166. [Google Scholar]
- Kaur, A.; Singh, V.A. Bacterial isolates and their antibiotic sensitivity pattern in clinically suspected cases of fever of unknown origin. JK Sci. 2014, 16, 105. [Google Scholar]
- Davoudi, A.; Najafi, N.; Alian, S.; Tayebi, A.; Ahangarkani, F.; Rouhi, S.; Heydari, A. Resistance Pattern of Antibiotics in Patient Underwent Open Heart Surgery With Nosocomial Infection in North of Iran. Glob. J. Health Sci. 2015, 8, 288–297. [Google Scholar] [CrossRef] [PubMed]
- Parameswarappa, J.; Metri, B.V.P.B.C. Isolation, identification, and antibiogram of Enterococci isolated from patients with urinary tract infection. Ann. Afr. Med. 2013, 12, 176–181. [Google Scholar] [PubMed]
- Almqvist, M.; Mattsson, G.; Razmi, R.; Magnusson, P. Cardiac Implantable Electronic Device-Related Infections; IntechOpen: London, UK, 2019. [Google Scholar] [CrossRef]
- Seni, J.; Najjuka, C.F.; Kateete, D.P.; Kateete, P.; Joloba, M.L.; Kajumbula, H.; Kapesa, A.; Bwanga, F. Antimicrobial resistance in hospitalized surgical patients: A silently emerging public health concern in Uganda. BMC Res. Notes 2013, 6, 1–7. [Google Scholar] [CrossRef]
- Agaba, P.; Tumukunde, J.; Tindimwebwa, J.V.B.; Kwizera, A. Nosocomial bacterial infections and their antimicrobial susceptibility patterns among patients in Ugandan intensive care units: A cross sectional study. BMC Res. Notes 2017, 10, 1–12. [Google Scholar] [CrossRef] [PubMed]
- Valsamatzi-Panagiotou, A.; Popova, K.B.; Penchovsky, R. Strategies for Prevention and Containment of Antimicrobial Resistance; Sustainable Agriculture Reviews 49; Springer: Cham, Switzerland, 2021; pp. 1–31. [Google Scholar] [CrossRef]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).