Surgical Outcomes of Total Anomalous Pulmonary Venous Connection Repair
Abstract
:1. Introduction
2. Materials and Methods
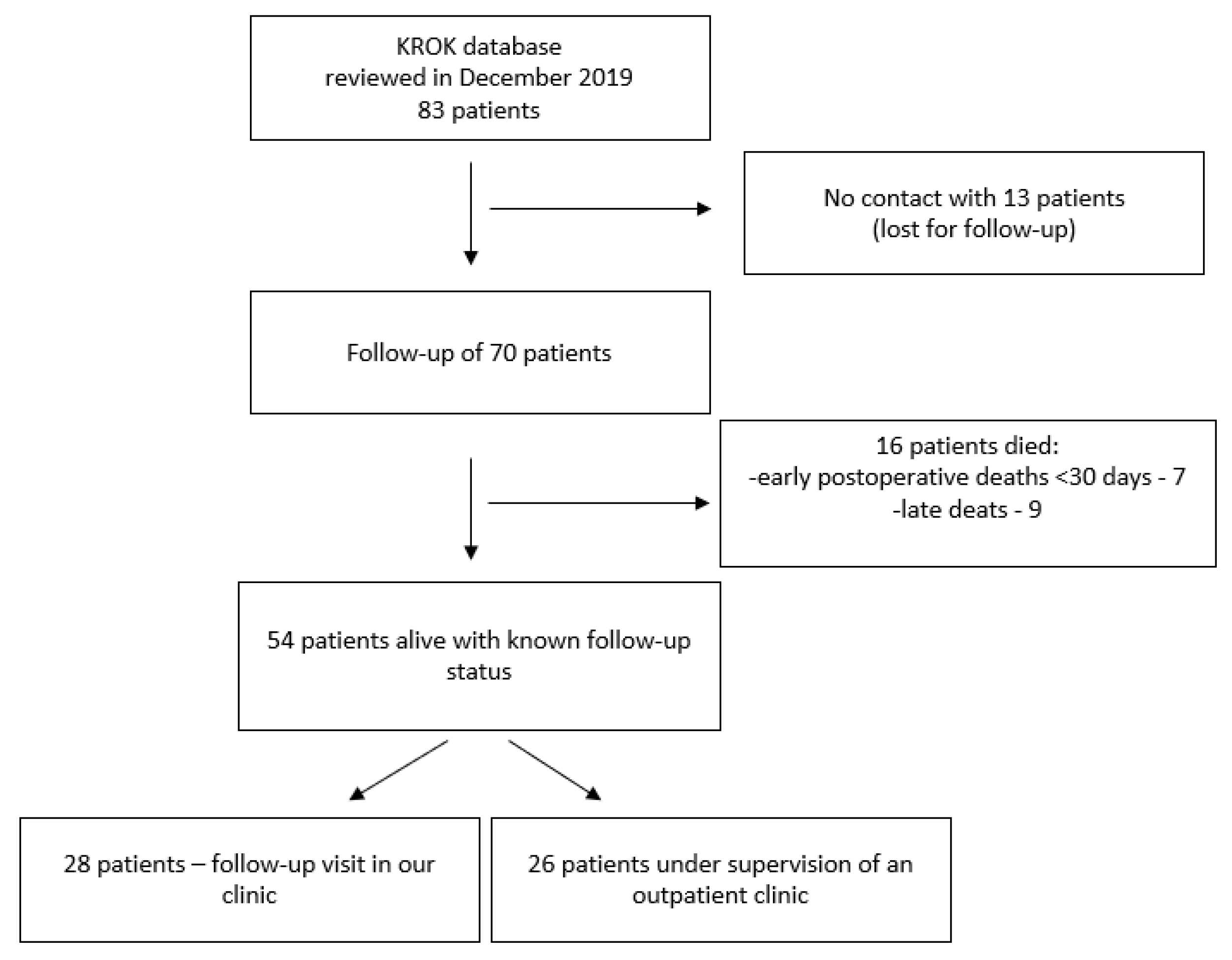
2.1. Study Design
2.2. Patient Cohort
2.3. Surgical Data
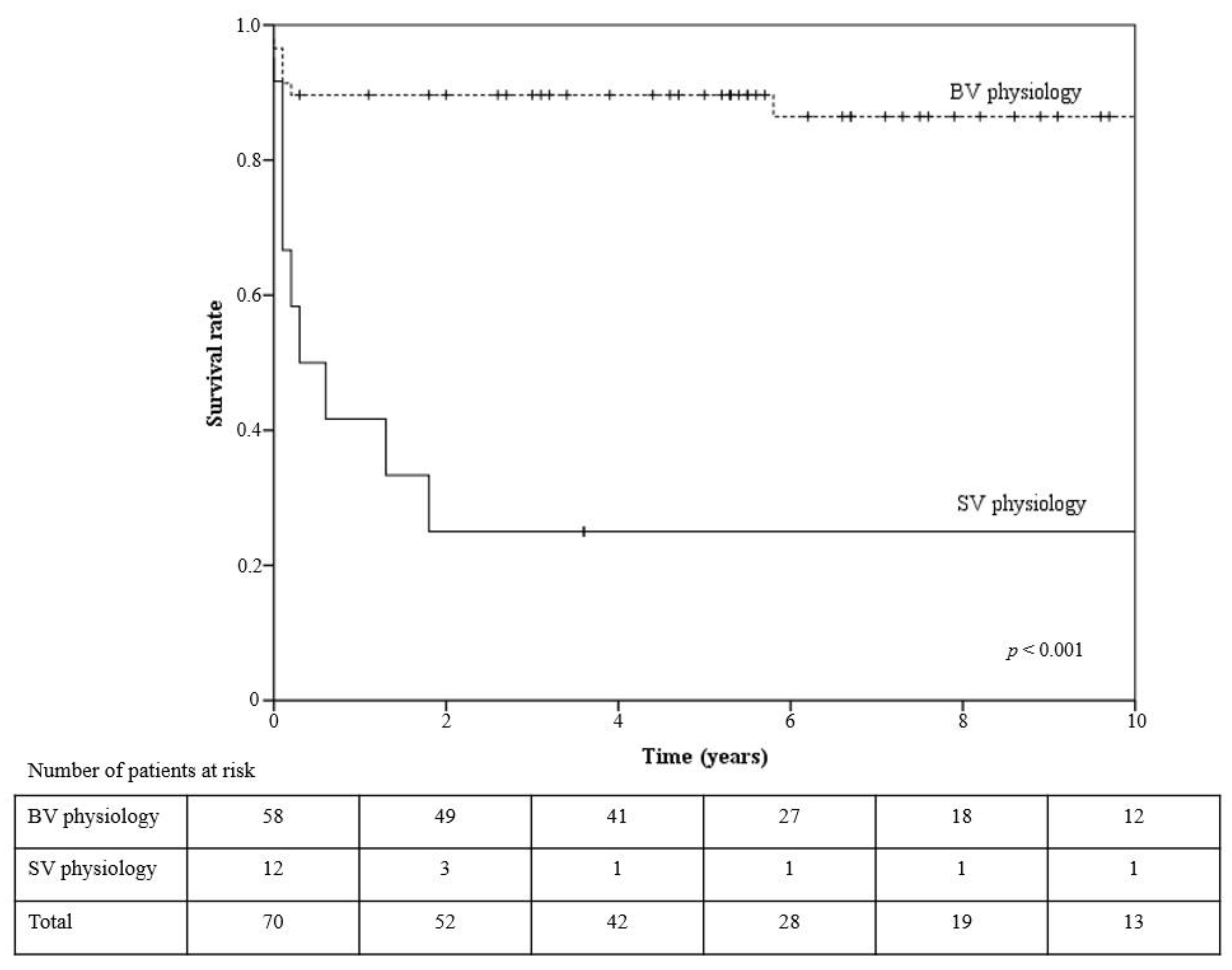
2.4. Statistical Analysis
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Michielon, G.; di Donato, R.M.; Pasquini, L.; Giannico, S.; Brancaccio, G.; Mazzera, E.; Squitieri, C.; Catena, G. Total anomalous pulmonary venous connection: Long-term appraisal with evolving technical solutions. Eur. J. Cardiothorac. Surg. 2002, 22, 184–191. [Google Scholar] [CrossRef] [Green Version]
- European Congenital Heart Surgeons Association Congenital Database. Available online: https://echsacongenitaldb.org/ (accessed on 17 February 2022).
- Craig, J.M.; Darling, R.C.; Rothney, W.B. Total pulmonary venous drainage into the right side of the heart; report of 17 autopsied cases not associated with other major cardiovascular anomalies. Lab. Invest. 1957, 6, 44–64. [Google Scholar] [PubMed]
- Padalino, M.A.; Cavalli, G.; de Franceschi, M.; Mancuso, D.; Maschietto, N.; Vida, V.; Milanesi, O.; Stellin, G. Surgical outcomes of total anomalous pulmonary venous connection repair: A 22-year experience. J. Card. Surg. 2014, 29, 678–685. [Google Scholar] [CrossRef] [PubMed]
- Paladini, D.; Pistorio, A.; Wu, L.H.; Meccariello, G.; Lei, T.; Tuo, G.; Donarini, G.; Marasini, M.; Xie, H.N. Prenatal diagnosis of total and partial anomalous pulmonary venous connection: Multicenter cohort study and meta-analysis. Ultrasound Obstet. Gynecol. 2018, 52, 24–34. [Google Scholar] [CrossRef]
- Sugano, M.; Murata, M.; Ide, Y.; Ito, H.; Kanno, K.; Imai, K.; Ishidou, M.; Fukuba, R.; Sakamoto, K. Midterm results and risk factors of functional single ventricles with extracardiac total anomalous pulmonary venous connection. Gen. Thorac. Cardiovasc. Surg. 2019, 67, 941–948. [Google Scholar] [CrossRef]
- Polish National Registry of Cardiac Surgery Procedures. Available online: http://www.krok.csioz.gov.pl (accessed on 17 February 2022).
- Louis, J.D.S.; Mc Cracken, C.E.; Turk, E.M.; Hancock, H.S.; Menk, J.S.; Harvey, B.A.; Vinocur, J.M.; Oster, M.E.; Moller, J.H.; Spector, L.G.; et al. Long-term transplant-free survival after repair of total anomalous pulmonary venous connection. Ann. Thorac. Surg. 2018, 105, 186–192. [Google Scholar] [CrossRef] [Green Version]
- Lemaire, A.; di Filippo, S.; Parienti, J.J.; Metton, O.; Mitchell, J.; Hénaine, R.; Ninet, J. Total anomalous pulmonary venous connection: A 40 years’ experience analysis. Thorac. Cardiovasc. Surg. 2017, 65, 9–17. [Google Scholar]
- Harada, T.; Nakano, T.; Oda, S.; Kado, H. Surgical results of total anomalous pulmonary venous connection repair in 256 patients. Interact. Cardiovasc. Thorac. Surg. 2019, 28, 421–426. [Google Scholar] [CrossRef] [Green Version]
- Feng, Z.; Yang, Y.; He, F.; Pang, K.; Ma, K.; Zhang, S.; Qi, L.; Wang, G.; Mao, F.; Yuan, J.; et al. Mid-term results of modified L-shaped incision technique for supracardiac total anomalous pulmonary venous connection. Eur. J. Cardiothorac. Surg. 2020, 58, 1261–1268. [Google Scholar] [CrossRef]
- Sakamoto, T.; Nagashima, M.; Umezu, K.; Houki, R.; Ikarashi, J.; Katagiri, J.; Yamazaki, K. Long-term outcomes of total correction for isolated total anomalous pulmonary venous connection: Lessons from 50-years’ experience. Interact. Cardiovasc. Thorac. Surg. 2018, 27, 20–26. [Google Scholar] [CrossRef]
- Karaci, A.R.; Harmandar, B.; Aydemir, N.A.; Sasmazel, A.; Balci, A.Y.; Saritas, T.; Yekeler, I.; Bilal, M.S. Early and intermediate term results for surgical correction of total anomalous pulmonary venous connection. J. Card. Surg. 2012, 27, 376–380. [Google Scholar] [CrossRef] [PubMed]
- Sinzobahamvya, N.; Arenz, C.; Reckers, J.; Photiadis, J.; Murin, P.; Schindler, E.; Hraska, V.; Asfour, B. Poor outcome for patients with totally anomalous pulmonary venous connection and functionally single ventricle. Cardiol. Young. 2009, 19, 594–600. [Google Scholar] [CrossRef] [PubMed]
- Khan, M.S.; Bryant, R., III; Kim, S.H.; Hill, K.D.; Jacobs, J.P.; Jacobs, M.L.; Pasquali, S.K.; Morales, D.L. Contemporary outcomes of surgical repair of total anomalous pulmonary venous connection in patients with heterotaxy syndrome. Ann. Thorac. Surg. 2015, 99, 2134–2139. [Google Scholar] [CrossRef] [PubMed]
- Morales, D.L.; Braud, B.E.; Booth, J.H.; Graves, D.E.; Heinle, J.S.; McKenzie, E.D.; Fraser, C.D., Jr. Heterotaxy patients with total anomalous pulmonary venous return: Improving surgical results. Ann. Thorac. Surg. 2006, 82, 1621–1627. [Google Scholar] [CrossRef]
- Caldarone, C.A.; Najm, H.K.; Kadletz, M.; Smallhorn, J.F.; Freedom, R.M.; Williams, W.G.; Coles, J.G. Surgical management of total anomalous pulmonary venous drainage: Impact of coexisting cardiac anomalies. Ann. Thorac. Surg. 1998, 66, 1521–1526. [Google Scholar] [CrossRef]
- Nakayama, Y.; Hiramatsu, T.; Iwata, Y.; Okamura, T.; Konuma, T.; Matsumura, G.; Suzuki, K.; Hobo, K.; Nakanishi, T.; Kurosawa, H.; et al. Surgical results for functional univentricular heart with total anomalous pulmonary venous connection over a 25-year experience. Ann. Thorac. Surg. 2012, 93, 606–613. [Google Scholar] [CrossRef]
- Yoshimura, N.; Fukahara, K.; Yamashita, A.; Doi, T.; Takeuchi, K.; Yamashita, S.; Homma, T.; Yokoyama, S.; Aoki, M.; Ikeno, Y. Surgery for total anomalous pulmonary venous connection: Primary sutureless repair vs. conventional repair. Gen. Thorac. Cardiovasc. Surg. 2017, 65, 245–251. [Google Scholar] [CrossRef]
- Shi, G.; Zhu, Z.; Chen, J.; Ou, Y.; Hong, H.; Nie, Z.; Zhang, H.; Liu, X.; Zheng, J.; Sun, Q.; et al. Total anomalous pulmonary venous connection: The current management strategies in a pediatric cohort of 768 patients. Circulation 2017, 135, 48–58. [Google Scholar] [CrossRef]
- Karamlou, T.; Gurofsky, R.; Al Sukhni, E.; Coles, J.G.; Williams, W.G.; Caldarone, C.A.; van Arsdell, G.S.; McCrindle, B.W. Factors associated with mortality and reoperation in 377 children with total anomalous pulmonary venous connection. Circulation 2007, 115, 1591–1598. [Google Scholar] [CrossRef] [Green Version]
- Xiang, M.; Wu, C.; Pan, Z.; Wang, Q.; Xi, L. Mixed type of total anomalous pulmonary venous connection: Diagnosis, surgical approach and outcomes. J. Cardiothorac. Surg. 2020, 15, 293. [Google Scholar] [CrossRef]
- Seale, A.N.; Uemura, H.; Webber, S.A.; Partridge, J.; Roughton, M.; Ho, S.Y.; Mc Carthy, K.P.; Jones, S.; Shaughnessy, L.; Sunnegardh, J.; et al. Total anomalous pulmonary venous connection: Morphology and outcome from an international population-based study. Circulation 2010, 122, 2718–2726. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Najm, H.K.; Ahmad, M.; Salam, Y.; Klein, J.; Hasan, S.M.; Majdalany, D.; Stewart, R.D.; Pettersson, G.; Karamlou, T. Early outcomes for in situ pericardial roll repair for distant anomalous pulmonary venous return. Ann. Thorac. Surg. 2021, 111, 169–175. [Google Scholar] [CrossRef] [PubMed]
- Zhao, K.; Wang, H.; Wang, Z.; Zhu, H.; Fang, M.; Zhu, X.; Zhang, N.; Song, H. Early- and intermediate-term results of surgical correction in 122 patients with total anomalous pulmonary venous connection and biventricular physiology. J. Cardiothorac. Surg. 2015, 10, 172. [Google Scholar] [CrossRef]
- Saxena, A.; Fong, L.V.; Lamb, R.K.; Monro, J.L.; Shore, D.F.; Keeton, B.R. Cardiac arrhythmias after surgical correction of total anomalous pulmonary venous connection: Late follow-up. Pediatr. Cardiol. 1991, 12, 89–91. [Google Scholar] [CrossRef]
- Korbmacher, B.; Büttgen, S.; Schulte, H.D.; Hoffmann, M.; Krogmann, O.N.; Rammos, S.; Gams, E. Long-term results after repair of total anomalous pulmonary venous connection. Thorac. Cardiovasc. Surg. 2001, 49, 101–106. [Google Scholar] [CrossRef]
- Emmel, M.; Sreeram, N. Total anomalous pulmonary vein connection: Diagnosis, management, and outcome. Curr. Treat. Options Cardiovasc. Med. 2004, 6, 423–429. [Google Scholar] [CrossRef]
- Bravo-Valenzuela, N.J.; Silva, G.R.; Varella, M.P. Pulmonary vein stenosis in a newborn: A commonly overlooked diagnosis. Case Rep. Cardiol. 2015, 2015, 870257. [Google Scholar] [CrossRef] [Green Version]
- Minich, L.L.; Tani, L.Y.; Breinholt, J.P.; Tuohy, A.M.; Shaddy, R.E. Complete follow-up echocardiograms are needed to detect stenosis of normally connecting pulmonary veins. Echocardiography 2001, 18, 589–592. [Google Scholar] [CrossRef] [PubMed]
- Pazos-López, P.; García-Rodríguez, C.; Guitián-González, A.; Paredes-Galán, E.; Álvarez-Moure, M.Á.; Rodríguez-Álvarez, M.; Baz-Alonso, J.A.; Teijeira-Fernández, E.; Calvo-Iglesias, F.E.; Íñiguez-Romo, A. Pulmonary vein stenosis: Etiology, diagnosis and management. World J. Cardiol. 2016, 8, 81–88. [Google Scholar] [CrossRef]
- Ayabakan, C.; Ozkutlu, S. Normal patterns of flow in the superior caval, hepatic and pulmonary veins as measured using Doppler echocardiography during childhood. Cardiol Young. 2003, 13, 143–151. [Google Scholar] [CrossRef]
| Feature | Total (n = 83); Mean (SD; Range) or Number (%) | Normal Heart Physiology (n = 67); Mean (SD; Range) or Number (%) | Single Ventricle Physiology (n = 16); Mean (SD; Range) or Number (%) | p-Value |
|---|---|---|---|---|
| Gender (male) | 57 (68.7%) | 45 (67.2%) | 12 (75%) | 0.388 |
| Age at operation (days) | 13 (43.9; 1–205) | 15 (47.5; 1–205) | 10.5 (19.3; 3–63) | 0.492 |
| Weight (kg) | 3.4 (0.9; 1.7–6.7) | 3.5 (0.9; 1.8–6.7) | 3 (0.6; 1.7–4) | 0.039 |
| TAPVC subtype: | ||||
| 37 (44.6%) 14 (16.9%) 28 (33.7%) 4 (4.8%) | 30 (44.8%) 13 (19.4%) 20 (29.9%) 4 (6%) | 7 (43.8%) 1 (6.3%) 8 (50%) − (0%) | 0.28 |
| Restrictive TAPVC * | 69 (83.1%) | 57 (85.1%) | 12 (75%) | 0.265 |
| Time from admission to operation (days) | 8.4 (16.2; 0–99) | 6.9 (15; 0–99) | 14.8 (20; 0–61) | 0.162 |
| Feature | Total (n = 83); Mean (SD; Range) or Number (%) | Normal Heart Physiology (n = 67); Mean (SD; Range) or Number (%) | Single Ventricle Physiology (n = 16); Mean (SD; Range) or Number (%) | p-Value |
|---|---|---|---|---|
| CPB time (min.) | 152 (68.3; 45–441) | 147 (70; 45–441) | 176 (57; 74–305) | 0.016 |
| AoX time (min.) | 53.5 (20.4; 21–118) | 56 (20.4; 21–118) | 43 (16.7; 27–78) | 0.015 |
| Use of DHCA | 73 (88%) | 57 (85.1%) | 16 (100%) | 0.102 |
| DHCA time (min.) | 47.9 (18.2; 20–104) | 52 (18.1; 20–104) | 33 (7.2; 22–52) | 0.004 |
| Delayed sternal closure | 36 (43.4%) | 26 (38.8%) | 10 (6.3%) | 0.086 |
| Complications (all): | 50 (60.3%) | 34 (50.8%) | 16 (100%) | <0.001 |
| 45 (54.2%) | 29 (43.3%) | 16 (100%) | <0.001 |
| 31 (37.4%) | 19 (28.4%) | 12 (75%) | 0.001 |
| 13 (15.7%) | 8 (11.9%) | 5 (31.3%) | 0.056 |
| 10 (12.1%) | 6 (9%) | 4 (25%) | 0.095 |
| Postoperative mechanical ventilation time (hours) | 291 (443.8; 1–2750) | 180 (213.6; 1–1080) | 757 (767.7; 4–2750) | <0.001 |
| ICU stay (days) | 17 (29.5; 0–205) | 9 (10.6; 0–49) | 49 (54.3; 0–205) | <0.001 |
| Postoperative hospital stay (days) | 26 (29; 0–206) | 19 (11.9; 1–62) | 54 (52.8; 0–206) | <0.001 |
| Univariate Analysis | Multivariate Analysis | |||||
|---|---|---|---|---|---|---|
| Covariate | HR | 95%CI | p-Value | HR | 95%CI | p-Value |
| Preoperative features | ||||||
| Age (days) | 0.996 | 0.952–1.01 | 0.531 | |||
| Newborn | 1.975 | 0.562–6.939 | 0.289 | |||
| Gender | 0.598 | 0.192–1.857 | 0.374 | |||
| Restrictive TAPVC * | 1.067 | 0.304–3.745 | 0.92 | |||
| TAPVC subtype | 0.742 | 0.442–1.247 | 0.261 | |||
| Supracardiac (I) vs. others (II, III, and IV) subtype of TAPVC | 2.568 | 0.932–7.076 | 0.068 | 3.61 | 1.258–10.356 | 0.017 |
| Intracardiac (II) vs. others (I, III, and IV) subtype of TAPVC | 0.037 | 0–9.201 | 0.241 | |||
| Infracardiac (III) vs. others (I, II, and IV) subtype of TAPVC | 0.8 | 0.278–2.303 | 0.679 | |||
| Mixed (IV) vs. others (I, II, and II subtype) of TAPVC | 0.965 | 0.127–7.308 | 0.972 | |||
| Single ventricle physiology | 9.125 | 3.326–25.04 | <0.001 | 9.126 | 3.259–25.553 | <0.001 |
| Weight (kg) | 0.643 | 0.324–1.277 | 0.207 | |||
| Weight below 3 kg | 2.242 | 0.834–6.025 | 0.109 | 2.064 | 0.737–5.783 | 0.168 |
| Intra- and postoperative features | ||||||
| Time from admission to operation (days) | 1.015 | 0.996–1.034 | 0.114 | 1.657 | 1.273–2.156 | <0.001 |
| Postoperative mechanical ventilation time (hours) | 1.001 | 1–1.002 | 0.001 | 0.999 | 0.998–1.001 | 0.313 |
| ICU stay (days) | 1.013 | 1.005–1.021 | 0.001 | 1.624 | 1.256–2.1 | <0.001 |
| Postoperative hospital stay (days) | 1.014 | 1.006–1.022 | 0.001 | 0.608 | 0.468–0.791 | <0.001 |
| Postoperative complications (overall) | 63.366 | 1.112–3612.041 | 0.044 | 0.122 | 0–146+ | 0.99 |
| Postoperative mechanical ventilation over seven days | 73.552 | 1.297–4141.414 | 0.037 | 14020.79 | 0–146+ | 0.955 |
| Temporary kidney insufficiency requiring dialysis | 34.693 | 4.565–263.661 | 0.001 | 38.376 | 2.976–494.831 | 0.005 |
| Postoperative arrythmia | 2.964 | 1.016–8.645 | 0.047 | 2.534 | 0.445–14.425 | 0.295 |
| Major infections | 0.607 | 0.08–4.595 | 0.628 | |||
| Delayed sternum closure | 1.538 | 0.575–4.114 | 0.392 | |||
| CPB time (min.) | 1.007 | 1.001–1.012 | 0.013 | 1.003 | 0.994–1.011 | 0.544 |
| AoX time (min.) | 1.004 | 0.98–1.029 | 0.741 | |||
| Use of DHCA (min.) | 1.853 | 0.244–14.045 | 0.551 | |||
| DHCA time (min.) | 0.999 | 0.97–1.029 | 0.947 | |||
| Need of reoperation | 2.944 | 0.667–13.007 | 0.154 | 5.906 | 0.74–47.110 | 0.094 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Jaworski, R.; Kansy, A.; Friedman-Gruszczynska, J.; Bieganowska, K.; Mirkowicz-Malek, M. Surgical Outcomes of Total Anomalous Pulmonary Venous Connection Repair. Medicina 2022, 58, 687. https://doi.org/10.3390/medicina58050687
Jaworski R, Kansy A, Friedman-Gruszczynska J, Bieganowska K, Mirkowicz-Malek M. Surgical Outcomes of Total Anomalous Pulmonary Venous Connection Repair. Medicina. 2022; 58(5):687. https://doi.org/10.3390/medicina58050687
Chicago/Turabian StyleJaworski, Radoslaw, Andrzej Kansy, Joanna Friedman-Gruszczynska, Katarzyna Bieganowska, and Malgorzata Mirkowicz-Malek. 2022. "Surgical Outcomes of Total Anomalous Pulmonary Venous Connection Repair" Medicina 58, no. 5: 687. https://doi.org/10.3390/medicina58050687






