One Year on: An Overview of Singapore’s Response to COVID-19—What We Did, How We Fared, How We Can Move Forward
Abstract
:1. Introduction
2. Materials and Methods
3. Results
3.1. Changes in Hospital Practice (210 Articles)
3.2. COVID-19 Pathology (94 Articles)
3.3. Public Health (61 Articles)
3.4. Impact of Pandemic on Clinical Outcomes (45 Articles)
3.5. Psychological Impact (35 Articles)
3.6. Narrative of Events (14 Articles)
3.7. Medical Education (30 Articles)
3.8. Others (15 Articles)
4. Discussion
4.1. Changes to Hospital Practice
4.2. COVID-19 Pathology and Diagnosis
4.3. Public Health
4.4. Impact of COVID-19 Pandemic on Clinical Outcomes
4.5. Psychological Impact
4.6. Medical Education
4.7. Comparison with Similar Studies
4.8. Limitations
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Abdullah, Z.; Salamat, H. Singapore Confirms First Case of Wuhan Virus. Available online: https://www.channelnewsasia.com/singapore/wuhan-virus-pneumonia-singapore-confirms-first-case-786446 (accessed on 25 June 2021).
- Choo, D. Covid-19 Testing Completed for All Migrant Workers in Dormitories, Says MOM, Agencies. TODAY. Available online: https://www.todayonline.com/singapore/covid-19-testing-completed-all-migrant-workers-dormitories-says-mom-agencies (accessed on 25 June 2021).
- Toh, T.W. Singapore’s Measures to Gradually Reopen Borders. The Straits Times. Available online: https://www.straitstimes.com/singapore/transport/singapores-measures-to-gradually-reopen-borders (accessed on 25 June 2021).
- Ang, H.M. NCID Nurse Becomes First Person in Singapore to Receive COVID-19 Vaccine. Channel News Asia. Available online: https://www.channelnewsasia.com/news/singapore/covid-19-first-vaccinations-ncid-healthcare-workers-pfizer-13864346 (accessed on 25 June 2021).
- Teo, J. Singapore Still Ranks High in Covid-19 Vaccination Pace Despite Supply Constraints. The Straits Times. Available online: https://www.straitstimes.com/singapore/health/singapore-still-ranks-high-in-vaccination-pace-despite-supply-constraints (accessed on 25 June 2021).
- Singapore Finds Delta Most Prevalent Among Virus Variants Locally. Reuters. Available online: https://www.reuters.com/world/asia-pacific/singapore-finds-delta-most-prevalent-among-virus-variants-locally-2021-06-09/ (accessed on 25 June 2021).
- Singapore to Advance COVID-19 Research Collaboration with ASEAN and Strengthen Regional Capabilities to Combat Pandemics. Agency for Science, Technology and Research. Available online: https://www.a-star.edu.sg/News-and-Events/a-star-news/news/press-releases/singapore-to-advance-covid-19-research-collaboration-with-asean (accessed on 25 June 2021).
- Moher, D.; Shamseer, L.; Clarke, M.; Ghersi, D.; Liberati, A.; Petticrew, M.; Shekelle, P.; Stewart, L.A. PRISMA-P Group Preferred reporting items for systematic review and meta-analysis protocols (PRISMA-P) 2015 statement. Syst. Rev. 2015, 4, 1. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Tan, S.-M.; Seet, Y.L.M.; Mok, C.W. COVID-19 pandemic: The new normal in breast cancer management—Prioritization of care from a breast surgical unit’s experience in Singapore. Asian J. Surg. 2021, 44, 389–391. [Google Scholar] [CrossRef]
- Mirpuri, T.M.; Wah, M.L.Y.; Siew, S.W.B.; Upadhyaya, V.S. Breast Imaging in the Time of COVID-19: A Singapore-based Breast Center’s Experience in the Midst of a Pandemic. J. Breast Imaging 2020, 2, 478–483. [Google Scholar] [CrossRef]
- Mok, C.W.; Seet, Y.L.M.; Tan, S.-M. Breast Cancer Multidisciplinary Management during COVID-19 Pandemic: Experiences and Strategies Used by a Singapore Breast Surgical Unit. BIO Integr. 2020, 1, 95–100. [Google Scholar] [CrossRef]
- Tan, J.L.; Lim, M.Y.; Lee, S.Y.C.; Yeo, S.B. Impact of COVID-19 on a Tertiary Otolaryngology Practice in Singapore. Ann. Acad. Med. Singap. 2020, 49, 897–901. [Google Scholar] [CrossRef]
- Tan, J.L.; Tay, V.S.-L.; Li, H.; Siow, J.K.; Ang, B.S.P.; Yeo, S.B. Otolaryngology Surgery in Time of COVID-19—What PPE to Use When? Ann. Acad. Med. Singap. 2020, 49, 387–392. [Google Scholar] [CrossRef]
- See, A.; Go, L.K.; Teo, C.; Toh, S.T. Adaptations of a Tertiary Otorhinolaryngology Head and Neck Surgery Department in Singapore During the COVID-19 Outbreak. Authorea 2020, 130, 177–181. [Google Scholar] [CrossRef]
- Lim, M.Y.; Gan, Y.J.; Tan, B.; Kwan, K.; Lim, Q.; Lee, S.; Chong, Y. Practical considerations for the operative team in performing tracheostomy during the COVID-19 pandemic. Singap. Med. J. 2021, 62, 204–206. [Google Scholar] [CrossRef]
- Tan, J.L.; Lim, M.Y.; Lee, C.S.Y.; Yeo, S.B. Resuming otolaryngology services following a COVID-19 lockdown in Singapore. Ann. Acad. Med. Singap. 2021, 50, 99–102. [Google Scholar] [CrossRef] [PubMed]
- Chew, M.; Tan, W.; Ng, C.; Ng, K. Deeply reconsidering elective surgery: Worldwide concerns regarding colorectal surgery in a COVID-19 pandemic and a Singapore perspective. Singap. Med. J. 2020, 61, 509–511. [Google Scholar] [CrossRef]
- Oh, S.L.; Chia, C.; Chen, Y.R.; Goo, T.; Rao, A.D.; Tan, K.Y.; Ong, M.W. Laparoscopic surgery in a patient with atypical presentation of COVID-19: Salient points to reduce the perils of surgery. Singap. Med. J. 2020, 61, 443–444. [Google Scholar] [CrossRef]
- Yau, J.; Tang, K.C.; Tan, H.L.; Teo, L.T. COVID-19 and the Intensive Care Unit: Coordinating a Multisite Intensive Care Unit Ramp-up Strategy in Singapore. Ann. Acad. Med. Singap. 2020, 49, 825–828. [Google Scholar] [CrossRef] [PubMed]
- Goh, S.S.N.; Yeo, D.X.W.; Kaushal, S.A.; Yeong, H.K.; Tan, G.W.L. Surgical and endoscopy protocols for general surgeons during the COVID-19 pandemic: An institutional experience in Singapore. BJS 2020, 107, e249. [Google Scholar] [CrossRef] [PubMed]
- Quek, L.H.H.; Tan, G.W.L.; Pua, U. Managing Endovascular Workload during COVID-19 Outbreak—The Singapore Experience. Ann. Vasc. Surg. 2020, 66, 3–5. [Google Scholar] [CrossRef] [PubMed]
- Ng, A.S.H.; Chew, M.H.; Charn, T.C.; Wong, M.K.; Wong, W.K.; Lee, L.S.; Hua, A.N.S. Keeping a cut above the coronavirus disease: Surgical perspectives from a public health institution in Singapore during Covid-19. ANZ J. Surg. 2020, 90, 666–669. [Google Scholar] [CrossRef]
- Wee, L.E.; Sim, X.Y.J.; Conceicao, E.P.; Aung, M.K.; Wong, H.M.; Teh, Y.E.; Tan, K.Y.; Wijaya, L.; Tan, T.B.H.; Ling, M.L.; et al. Early Recognition of Coronavirus 2019 Disease (COVID-19) Infection in Surgical Inpatients: The Importance of a Risk-Stratified Approach for Early Testing and Isolation. Surg. Infect. 2020, 21, 760–765. [Google Scholar] [CrossRef] [PubMed]
- Chew, M.; Koh, F.; Ng, K. A call to arms: A perspective on safe general surgery in Singapore during the COVID-19 pandemic. Singap. Med. J. 2020, 61, 378–380. [Google Scholar] [CrossRef]
- Goh, S.S.N.; Teo, L.T. Adapting trauma workflows for severely injured trauma patients during the COVID-19 pandemic: Experience in a regional trauma centre in Singapore. Singap. Med. J. 2020, 1, 7. [Google Scholar] [CrossRef]
- Ahmed, S.; Tan, W.L.G.; Chong, Y.-L. Surgical Response to COVID-19 Pandemic: A Singapore Perspective. J. Am. Coll. Surg. 2020, 230, 1074–1077. [Google Scholar] [CrossRef]
- Low, T.-Y.; Hartman, M.; Chee, C.Y.J.; Mohankumar, B.; Ang, S.B.L.; San, M.T.; Shabbir, A.; Madhavan, K.; So, J.B.Y. Restructuring the surgical service during the COVID-19 pandemic: Experience from a tertiary institution in Singapore. Am. J. Surg. 2020, 220, 553–555. [Google Scholar] [CrossRef]
- Leow, L.; Ng, C.S.H.; Mithiran, H. Surgery beyond coronavirus disease. ANZ J. Surg. 2020, 90, 1865–1866. [Google Scholar] [CrossRef]
- Chia, C.L. Being a Surgeon in the Pandemic Era. J. Am. Coll. Surg. 2020, 230, 1077–1079. [Google Scholar] [CrossRef]
- Yeo, D.; Yeo, C.; Kaushal, S.; Tan, G. COVID-19 and the General Surgical Department—Measures to Reduce Spread of SARS-COV-2 Among Surgeons. Ann. Surg. 2020, 272, e3–e4. [Google Scholar] [CrossRef] [PubMed]
- Tan, W.J.; Foo, F.J.; Sivarajah, S.S.; Li, L.H.M.; Koh, F.; Chew, M.H. Safe Colorectal Surgery in the COVID-19 Era—A Singapore Experience. Ann. Coloproctol. 2020, 36, 65–69. [Google Scholar] [CrossRef]
- Tan, Y.Q.; Lu, J.; Wang, Z.; Tiong, H.Y.; Chiong, E. Key Considerations in the Recovery and Resumption of Surgical Services after the COVID-19 Pandemic. Ann. Acad. Med. Singap. 2020, 49, 922–924. [Google Scholar] [CrossRef] [PubMed]
- Hwee, J.; Chiew, J.; Sechachalam, S. The Impact of Coronavirus Disease 2019 (COVID-19) on the Practice of Hand Surgery in Singapore. J. Hand Surg. 2020, 45, 536–541. [Google Scholar] [CrossRef]
- Lo, Y.T.; Teo, N.W.Y.; Ang, B.T. Editorial. Endonasal neurosurgery during the COVID-19 pandemic: The Singapore perspective. J. Neurosurg. 2020, 133, 26–28. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Lee, Z.D.; Yeu, D.L.C.; Ang, B.T.; Ng, W.H.; Seow, W.T. Editorial. COVID-19 and its impact on neurosurgery: Our early experience in Singapore. J. Neurosurg. 2020, 133, 24–25. [Google Scholar] [CrossRef]
- Leong, A.Z.; Lim, J.X.; Tan, C.H.; Teo, K.; Nga, V.D.W.; Lwin, S.; Chou, N.; Yeo, T.T. COVID-19 response measures—A Singapore Neurosurgical Academic Medical Centre experience segregated team model to maintain tertiary level neurosurgical care during the COVID-19 outbreak. Br. J. Neurosurg. 2020, 1–6. [Google Scholar] [CrossRef]
- Lim, Y.H.; Chay, W.Y.; Wong, W.L. Surviving the COVID-19 pandemic: Early response of a gynecologic oncology unit in Singapore. J. Gynecol. Oncol. 2020, 31, e77. [Google Scholar] [CrossRef]
- Chua, M.S.Q.; Lee, J.C.S.; Sulaiman, S.; Tan, H.K. From the frontline of COVID-19—How prepared are we as obstetricians? A commentary. BJOG Int. J. Obstet. Gynaecol. 2020, 127, 786–788. [Google Scholar] [CrossRef]
- Koh, K.M.L.; Mathur, M. Donning the powered air-purifying respirator in an emergency obstetric setting amid the COVID-19 outbreak in Singapore: A balance between safety and urgency. Singap. Med. J. 2020, 26, 3. [Google Scholar] [CrossRef] [PubMed]
- Sim, W.S.; Tan, J.V.; Zhang, V.R.; Chong, G.S.; Ku, C.W.; Tan, K.H.; Tan, H.K.; Yeo, G.S.H.; Tagore, S. Dorscon Orange: An Approach to Challenges in a Busy Antenatal Diagnostic Centre in the Midst of a Global Pandemic. Ann. Acad. Med. Singap. 2020, 49, 677–683. [Google Scholar] [CrossRef]
- Lee, J.; Goy, R.; Sng, B.; Lew, E. Considerations and strategies in the organisation of obstetric anaesthesia care during the 2019 COVID-19 outbreak in Singapore. Int. J. Obstet. Anesthesia 2020, 43, 114–117. [Google Scholar] [CrossRef]
- Tan, S.Q.; Phoon, J.; Chan, M.L.H.; Wong, H.Y.; Durgahshree, M.; Nadarajah, S.; Chan, J.K.Y.; Chan, M.; Chan, J. Providing assisted reproduction treatment during the COVID-19 pandemic in Singapore. Singap. Med. J. 2020. [Google Scholar] [CrossRef] [PubMed]
- Olivia Li, J.P.; Shantha, J.; Wong, T.Y.; Wong, E.Y.; Mehta, J.; Lin, H.; Lin, X.; Strouthidis, N.G.; Park, K.H.; Fung, A.T.; et al. Preparedness among Ophthalmologists: During and Beyond the COVID-19 Pandemic. Ophthalmology 2020, 127, 569–572. [Google Scholar] [CrossRef]
- Khor, W.B.; Yip, L.; Zhao, P.; Foo, V.H.X.; Lim, L.; Ting, D.S.W.; Loon, S.C.; Wong, E.; Yong, V.; Tan, C.; et al. Evolving Practice Patterns in Singapore’s Public Sector Ophthalmology Centers During the COVID-19 Pandemic. Asian J. Ophthalmology. 2020, 9, 285–290. [Google Scholar]
- Lim, L.W.; Yip, L.W.; Tay, H.W.; Ang, X.L.; Lee, L.K.; Chin, C.F.; Yong, V. Sustainable practice of ophthalmology during COVID-19: Challenges and solutions. Graefe’s Arch. Clin. Exp. Ophthalmol. 2020, 258, 1427–1436. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Wong, T.Y.; Bandello, F. Academic Ophthalmology during and after the COVID-19 Pandemic. Ophthalmology 2020, 127, e51–e52. [Google Scholar] [CrossRef]
- Lim, B.X.; Lim, C.H.; Goh, A.Q.; Lim, D.K.; Tan, C.W. Policy recommendations in response to the resurgence of COVID-19 cases for institutional medical practice from an ophthalmic perspective. Asian J. Ophthalmology. 2020, 17, 250–262. [Google Scholar] [CrossRef]
- Jun, I.S.Y.; Hui, K.K.O.; SongBo, P.Z. Perspectives on Coronavirus Disease 2019 Control Measures for Ophthalmology Clinics Based on a Singapore Center Experience. JAMA Ophthalmol. 2020, 138, 435. [Google Scholar] [CrossRef] [Green Version]
- Koh, A.; Chen, Y. Perspective from Singapore and China on the COVID-19 Pandemic: The New World Order for Ophthalmic Practice. Ophthalmology 2020, 127, e49–e50. [Google Scholar] [CrossRef] [PubMed]
- Husain, R.; Zhang, X.; Aung, T. Challenges and Lessons for Managing Glaucoma during COVID-19 Pandemic: Perspectives from Asia. Ophthalmology 2020, 127, e63–e64. [Google Scholar] [CrossRef]
- Zhang, J.; Yam, M.; Chua, I.T. Adapting to the “New Normal” in Orthopaedic Trauma During COVID-19. Ann. Acad. Med. 2020, 49, 613–617. [Google Scholar]
- Liow, M.H.L.; Tay, K.X.K.; Yeo, N.E.M.; Tay, D.K.J.; Goh, S.K.; Koh, J.S.B.; Howe, T.S.; Tan, A.H.C. Ensuring Business Continuity of Musculoskeletal Care During the COVID-19 Pandemic: Experience of a Tertiary Orthopaedic Surgery Department in Singapore. JB JS Open Access. 2020, 5, e0050. [Google Scholar] [CrossRef] [PubMed]
- Decruz, J.; Prabhakar, S.; Ding, B.T.K.; Kunnasegaran, R. The COVID-19 pandemic in Singapore: What does it mean for arthroplasty? Acta Orthop. 2020, 91, 1–5. [Google Scholar] [CrossRef] [PubMed]
- Tay, K.; Kamarul, T.; Lok, W.; Mansor, M.; Li, X.; Wong, J.; Saw, A. COVID-19 in Singapore and Malaysia: Rising to the Challenges of Orthopaedic Practice in an Evolving Pandemic. Malays. Orthop. J. 2020, 14, 7–15. [Google Scholar]
- Chang, L.Z.; Wang, W.; Murphy, D.; Po Hui, J.H. Novel Coronavirus and Orthopaedic Surgery: Early Experiences from Singapore. J. Bone Jt. Surg. Am. 2020, 102, 745–749. [Google Scholar] [CrossRef]
- Thor, J.; Pagkaliwagan, E.; Yeo, A.; Loh, J.; Kon, C. Roadmap Out of COVID-19. Malays. Orthop. J. 2020, 14, 4–9. [Google Scholar]
- Tan, S.H.S.; Hong, C.C.; Saha, S.; Das De, S.; Pearce, C.J. Standing on Your Foot and Ankle During COVID-19: Perspectives from a Singaporean Orthopedic Foot and Ankle Surgery Unit. J. Foot Ankle Surg. 2020, 59, 889–891. [Google Scholar] [CrossRef]
- Lee Ting Soh, T.; Tze Keong Ding, B.; Ming Quan Yap, W.M.Q.; Yoong-Leong Oh, J.; Soh, T.L.T.; Ding, B.T.K.; Yap, W.M.Q.; Oh, J.Y.-L. Spine Surgery and COVID-19: Early Experiences from Singapore. Spine (03622436). 2020, 45, 786–788. [Google Scholar]
- Benjamin Tze, K.; Soh, T.; Bryan Yijia, T.; Jacob Yoong-Leong, O.; Bin Mohd Fadhil, M.F.; Rasappan, K.; Keng Thiam, L.; Ding, B.T.K.; Tan, B.Y.; Oh, J.Y.-L.; et al. Operating in a Pandemic: Lessons and Strategies from an Orthopaedic Unit at the Epicenter of COVID-19 in Singapore. J. Bone Jt. Surg. Am. Vol. 2020, 102, e67(1)–e67(8). [Google Scholar]
- Omar, U.F.; Yein, T.P.; Rajaratnam, V. Managing hand and reconstructive microsurgery service during COVID-19 pandemic: Singapore experience. Postgrad. Med. J. 2020, 96, 379–383. [Google Scholar] [CrossRef]
- Tay, K.; Lee, Y. Trauma and orthopaedics in the COVID-19 pandemic: Breaking every wave. Singap. Med. J. 2020, 61, 396–398. [Google Scholar] [CrossRef] [PubMed]
- Rasappan, K.; Oh, J.Y.L.; Ding, B.T.K.; Fadhil, M.F.M.; Lee, K.T. A surgeon’s role in fighting a medical pandemic: Experiences from the unit at the epicentre of COVID-19 in Singapore—A cohort perspective. Int. J. Surg. 2020, 79, 31–35. [Google Scholar] [CrossRef]
- Barret, J.P.; Chong, S.J.; Depetris, N.; Fisher, M.D.; Luo, G.; Moiemen, N.; Pham, T.; Qiao, L.; Wibbenmeyer, L.; Matsumura, H. Burn center function during the COVID-19 pandemic: An international multi-center report of strategy and experience. Burns 2020, 46, 1021–1035. [Google Scholar] [CrossRef]
- Tan, B.; Teo, H.; Loo, W.; Dinesh, S. Impact of the COVID-19 pandemic on spinal surgery in Singapore. Singap. Med. J. 2020, 61, 624–625. [Google Scholar] [CrossRef] [PubMed]
- Tamara Lee Ting, S.; Sean Wei Loong, H.; Wayne Ming Quan, Y.; Jacob Yoong-Leong, O.; Soh, T.L.T.; Ho, S.W.L.; Yap, W.M.Q.; Oh, J.Y.-L. Spine Surgery and COVID-19: Challenges and Strategies from the Front Lines. J. Bone Jt. Surg. Am. Vol. 2020, 102, e56. [Google Scholar]
- Leow, L.; Ramanathan, K.; Kofidis, T.; Tam, J.K.C.; Mithiran, H. Organization of thoracic surgical services during the COVID pandemic. Surgeon 2021, 19, e1–e8. [Google Scholar] [CrossRef]
- Jheon, S.; Ahmed, A.D.; Fang, V.W.; Jung, W.; Khan, A.Z.; Lee, J.-M.; Nakajima, J.; Sihoe, A.D.; Thongcharoen, P.; Tsuboi, M.; et al. General thoracic surgery services across Asia during the 2020 COVID-19 pandemic. Asian Cardiovasc. Thorac. Ann. 2020, 28, 243–249. [Google Scholar] [CrossRef]
- Chung, S.J.; Tan, E.K.; Kee, T.; Krishnamoorthy, T.L.; Phua, G.C.; Sewa, D.W.; Ong, B.-H.; Tan, T.E.; Sivathasan, C.; Gan, H.L.V.; et al. Practical Considerations for Solid Organ Transplantation During the COVID-19 Global Outbreak: The Experience from Singapore. Transplant. Direct 2020, 6, e554. [Google Scholar] [CrossRef]
- Kee, T.; Hl, V.G.; Shimin, J.C.; Sing, T.P.; Moi, L.Y.; Peng, C.L.; Ht, E.C.; Hoon, L.P.; Hua, Y.J.; Yao, H.Q.; et al. Managing a Renal Transplant Programme During the COVID-19 Pandemic: Practical Experience from a Singapore Transplant Centre. Ann. Acad. Med. Singap. 2020, 49, 652–660. [Google Scholar] [CrossRef]
- Chan, M.-C.; Yeo, S.E.; Chong, Y.-L.; Lee, Y.-M. Stepping Forward: Urologists’ Efforts during the COVID-19 Outbreak in Singapore. Eur. Urol. 2020, 78, e38–e39. [Google Scholar] [CrossRef] [Green Version]
- Tan, Y.Q.; Wu, Q.H.; Chiong, E. Preserving Operational Capability While Building Capacity during the COVID-19 Pandemic: A Tertiary Urology Centre’s Experience; Elsevier: Amsterdam, The Netherlands, 2020; pp. 36–37. [Google Scholar]
- Tiwari, R.V.; Teo, J.S.M.; Sundaram, P.; Cheng, C.W.S. Turning the Tide Against COVID-19: Adaptations of a Urology Department in a Public Hospital in Singapore. Ann. Acad. Med. Singap. 2020, 49, 597–599. [Google Scholar] [CrossRef]
- Chan, M.-C.; Kwok, J.-L.; Yeo, S.E.; Chong, Y.-L. Surgical Precautions for Urologists in the Era of COVID-19. Urology 2020, 143, 11–15. [Google Scholar] [CrossRef]
- Ng, J.J.; Gan, T.R.; Niam, J.Y.; Menon, R.K.; Ho, P.; Dharmaraj, R.B.; Wong, J.C.; Choong, A. Experience from a Singapore tertiary hospital with restructuring of a vascular surgery practice in response to national and institutional policies during the COVID-19 pandemic. J. Vasc. Surg. 2020, 72, 1166–1172. [Google Scholar] [CrossRef]
- Tan, G.W.L.; Chandrasekar, S.; Lo, Z.J.; Hong, Q.; Yong, E.; Lingam, P.; Zhang, L.; Quek, L.H.H.; Pua, U. Early experience in the COVID-19 pandemic from a vascular surgery unit in a Singapore tertiary hospital. J. Vasc. Surg. 2020, 72, 12–15. [Google Scholar] [CrossRef]
- Ng, J.J.; Ho, P.; Dharmaraj, R.B.; Wong, J.C.; Choong, A. The global impact of COVID-19 on vascular surgical services. J. Vasc. Surg. 2020, 71, 2182–2183.e1. [Google Scholar] [CrossRef]
- Khoo, B.Z.E.; See, Y.P.; Koh, T.J.K.; Yeo, S.C. Coronavirus Disease 2019 (COVID-19) and Dialysis: The Experience in Singapore. Kidney Med. 2020, 2, 381–384. [Google Scholar] [CrossRef]
- Chua, H.-R.; MacLaren, G.; Choong, L.H.-L.; Chionh, C.-Y.; Khoo, B.Z.E.; Yeo, S.-C.; Sewa, D.-W.; Ng, S.-Y.; Choo, J.C.-J.; Teo, B.-W.; et al. Ensuring Sustainability of Continuous Kidney Replacement Therapy in the Face of Extraordinary Demand: Lessons From the COVID-19 Pandemic. Am. J. Kidney Dis. 2020, 76, 392–400. [Google Scholar] [CrossRef]
- Lee, M.B.; Chua, H.R.; Wong, W.K.; Chan, G.C.; Leo, C.C.H.; Vathsala, A.; Teo, B.W. Going to war on COVID-19: Mobilizing an academic nephrology group practice. Nephrology 2020, 25, 822–828. [Google Scholar] [CrossRef]
- Ho, Q.Y.; Chung, S.J.; Gan, V.H.L.; Ng, L.G.; Tan, B.H.; Kee, T.Y.S. High-immunological risk living donor renal transplant during the COVID-19 outbreak: Uncertainties and ethical dilemmas. Arab. Archaeol. Epigr. 2020, 20, 1949–1951. [Google Scholar] [CrossRef]
- Chen, D.E.; Tay, E.K.; Tan, P.L.; Su, P.; Koh, M.M.; Ong, P.L.; Chew, E.; Ng, Y.S. The Impact of COVID-19 Pandemic on Rehabilitation in Singapore. Ann. Acad. Med. Singap. 2020, 49, 925–927. [Google Scholar] [CrossRef]
- Chew, L.C.; Yeo, S.I.; Thumboo, J. The Impact of the Off-site Monitoring Clinic (Virtual Monitoring Clinic) on the Practice of Outpatient Rheumatology in a Tertiary Centre during the COVID-19 Pandemic. Ann. Acad. Med. Singap. 2020, 49, 905–908. [Google Scholar] [CrossRef]
- Coffman, T.M.; Chan, C.M.; Choong, L.H.-L.; Curran, I.; Tan, H.K.; Tan, C.C. Perspectives on COVID-19 from Singapore: Impact on ESKD Care and Medical Education. J. Am. Soc. Nephrol. 2020, 31, 2242–2245. [Google Scholar] [CrossRef]
- Ramanathan, K.; Antognini, D.; Combes, A.; Paden, M.; Zakhary, B.; Ogino, M.; MacLaren, G.; Brodie, D.; Shekar, K. Planning and provision of ECMO services for severe ARDS during the COVID-19 pandemic and other outbreaks of emerging infectious diseases. Lancet Respir. Med. 2020, 8, 518–526. [Google Scholar] [CrossRef] [Green Version]
- Htay, H.; Wong, P.M.P.; Choo, R.-E.R.; Dawood, U.S.; Foo, M.W.Y.; Jayaballa, M.; Lee, G.; Lee, M.B.-H.; Liu, Y.L.A.; Low, S.; et al. Strategies for Management of Peritoneal Dialysis Patients in Singapore during COVID-19 Pandemic. Ann. Acad. Med. Singap. 2020, 49, 1025–1028. [Google Scholar] [CrossRef]
- Chia, P.-L.; Tan, K.; Tan, L.W.; Chin, P.S.; Foo, D. Rhythm blues in the time of coronavirus disease 2019 (COVID-19): How the cardiac electrophysiologist adapts to a viral pandemic in Singapore. J. Interv. Card. Electrophysiol. 2020, 58, 269–272. [Google Scholar] [CrossRef]
- Cherian, R.; Poh, K. At the ‘heart’ of the COVID-19 outbreak: Early cardiac implications and mitigating strategies. Singap. Med. J. 2020, 61, 373–374. [Google Scholar] [CrossRef]
- Wong, S.W.; Lee, J.H.; Tan, H.H. Cardiac Catheterisation for ST-Elevation Myocardial Infarction during COVID-19 in Singapore: Protocols and Recommendations. Ann. Acad. Med. Singap. 2020, 49, 602–606. [Google Scholar] [CrossRef]
- Koh, C.H.; Chiong, S.C.; Lee, P.T.; Ding, Z.P.; Ewe, S.H. The Safe Conduct of Echocardiographic Studies During the COVID-19 Pandemic: Perspectives and Experience from a Tertiary Echocardiography Laboratory in Singapore. Cardiovasc. Imaging Asia 2020, 4, 55–59. [Google Scholar] [CrossRef]
- Leow, L.; Papadimas, E.; Subbian, S.K.; MacLaren, G.; Ramanathan, K. Organization of extracorporeal membrane oxygenation services for COVID-19. Asian Cardiovasc. Thorac. Ann. 2021, 29, 165–169. [Google Scholar] [CrossRef]
- Gambaro, A.; Ho, H.H.; Kaier, T.E.; Pires-Morais, G.; Patel, J.A.; Ansari Ramandi, M.M. Management of Acute Coronary Syndrome in the COVID-19 Era: Voices from the Global Cardiology Community. JACC Case Rep. 2020, 2, 1430–1432. [Google Scholar]
- Tan, Z.; Phoon, P.H.Y.; Zeng, L.A.; Fu, J.; Lim, X.T.; Tan, T.E.; Loh, K.W.-T.; Goh, M.H. Response and Operating Room Preparation for the COVID-19 Outbreak: A Perspective from the National Heart Centre in Singapore. J. Cardiothorac. Vasc. Anesthesia 2020, 34, 2331–2337. [Google Scholar] [CrossRef]
- Wee, L.E.; Ruan, W.; Sim, X.Y.J.; Ng, K.; Phoon, P.C.; Conceicao, E.P.; Aung, M.K.; Wong, A.S.-L.; Chua, T.S.J.; Venkatachalam, I. Surveillance for COVID-19 in Cardiac Inpatients: Containing COVID-19 in a Specialized Cardiac Centre. Can. J. Cardiol. 2020, 36, 1327.e3–1327.e4. [Google Scholar] [CrossRef]
- Lim, Z.V.; Lim, Y.L. Impact of COVID-19 on Clinical Operations and Management of Patients in a Singapore Immunodermatology Unit during the’Circuit-Breaker’Period and Beyond. Ann. Acad. Med. Singap. 2020, 49, 919–921. [Google Scholar] [CrossRef] [PubMed]
- Tay, S.; Teh, K.; Wang, L.; Ang, T. Impact of COVID-19: Perspectives from gastroenterology. Singap. Med. J. 2020, 61, 460–462. [Google Scholar] [CrossRef]
- Ong, J.; Cross, G.B.; Dan, Y.Y. Prevention of nosocomial SARS-CoV-2 transmission in endoscopy: International recommendations and the need for a gold standard. Gut 2020, 69, 1145–1148. [Google Scholar] [CrossRef] [PubMed]
- Ang, T.L. Gastrointestinal endoscopy during COVID-19 pandemic. J. Gastroenterol. Hepatol. 2020, 35, 701–702. [Google Scholar] [CrossRef] [Green Version]
- Salazar, E.; Cheah, M.C. Prescribing parenteral nutrition in acute hospital setting during COVID-19: The Singapore experience. Clin. Nutr. 2020, 39, 2321. [Google Scholar] [CrossRef]
- Ang, T.; Li, J.; Vu, C.; Ho, G.; Chang, J.; Chong, C.; Chua, T.; Ong, D.; Yip, B.; Gwee, K. Chapter of Gastroenterologists professional guidance on risk mitigation for gastrointestinal endoscopy during COVID-19 pandemic in Singapore. Singap. Med. J. 2020, 61, 345–349. [Google Scholar] [CrossRef] [PubMed]
- Merchant, R.A.; Chen, M.Z.; Ng, S.E.; Sandrasageran, S.; Wong, L.L.B. The Role of a Geriatrician has Become Even More Important in an Academic Institution during COVID-19. J. Nutr. Health Aging 2020, 24, 681–682. [Google Scholar] [CrossRef] [PubMed]
- Tan, L.F.; Seetharaman, S. Preventing the Spread of COVID-19 to Nursing Homes: Experience from a Singapore Geriatric Centre. J. Am. Geriatr. Soc. 2020, 68, 942. [Google Scholar] [CrossRef] [PubMed]
- Cheong, C.Y.; Yap, P.L.K. Letter to the editor: Staying True to the Calling of Geriatric Medicine Amid the Waves of COVID-19. J. Nutr. Health Aging. 2020, 24, 534–535. [Google Scholar] [CrossRef]
- Tan, W.Y.; Ng, G.C.; Mah, Y.Y.; Law, M.C.; Wong, C.S. Outpatient Management of Patients in Singapore’s National Centre for Infectious Diseases Special Precautions Area Clinic in the COVID-19 Pandemic. Ann. Acad. Med. Singap. 2020, 49, 690–693. [Google Scholar] [CrossRef]
- Wee, L.E.; Venkatachalam, I.; Sim, X.Y.J.; Tan, K.B.-K.; Wen, R.; Tham, C.K.; Gan, W.H.; Ko, K.K.K.; Ho, W.Q.; Kwek, G.T.C.; et al. Containment of COVID-19 and reduction in healthcare-associated respiratory viral infections through a multi-tiered infection control strategy. Infect. Dis. Health 2021, 26, 123–131. [Google Scholar] [CrossRef]
- Ian, W.L.E.; Sim, X.Y.J.; Conceicao, E.P.; Aung, M.K.; Tan, K.Y.; Ko, K.K.K.; Wong, H.M.; Wijaya, L.; Tan, B.H.; Venkatachalam, I.; et al. Containing COVID-19 outside the isolation ward: The impact of an infection control bundle on environmental contamination and transmission in a cohorted general ward. Am. J. Infect. Control 2020, 48, 1056–1061. [Google Scholar]
- Christopher, S.Y.H.; Carol, T.H.; Yu-Lin, W. Challenges in adapting existing hyperacute stroke protocols by a tertiary neuroscience centre for patients with covid 19 in singapore. Int. J. Cerebrovasc. Dis. Stroke 2020. [Google Scholar] [CrossRef]
- De Silva, D.A.; Tan, I.F.; Thilarajah, S. A protocol for acute stroke unit care during the COVID-19 pandemic. J. Stroke Cerebrovasc. Dis. 2020, 29, 105009. [Google Scholar] [CrossRef]
- Lu, Y.; Yan, S.X.; Lan, X.; Zhu, X.; Macapinlac, H.A. Nuclear medicine in responding to global pandemic COVID-19—American College of Nuclear Medicine member experience. Eur. J. Nucl. Med. Mol. Imaging 2020, 47, 1620–1622. [Google Scholar] [CrossRef]
- Lam, W.W.-C.; Loke, K.S.-H.; Wong, W.Y.; Ng, D.C.-E. Facing a disruptive threat: How can a nuclear medicine service be prepared for the coronavirus outbreak 2020? Eur. J. Nucl. Med. Mol. Imaging 2020, 47, 1645–1648. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Tham, W.Y.; Tong, A.K.T.; Loke, K.S.H.; Chio, L.; Lim, G.K.Y.; Seah, X.Y.; Ng, D.C.E.; Yan, S.X.X.; Lam, W.W.-C. Divide and Conquer: Strategies in Singapore to Manage a Nuclear Medicine Department During COVID-19. J. Nucl. Med. Technol. 2020, 48, 98–101. [Google Scholar] [CrossRef]
- Cheng, L.T.J.; Peh, W.M.; Lam, W.W.C. Safeguarding children from coronavirus disease 2019: Practices of nuclear medicine units in Singapore. Proc. Singap. Healthc. 2020, 30, 36–40. [Google Scholar] [CrossRef]
- Ngam, P.I.; Goh, C.X.; Ng, D.C.; Tan, C.J.; Osmany, S.; Tan, A.E.; Kannivelu, A.; Cheng, L.T.; Khor, L.K.; Tong, A.K.; et al. COVID-19: Preparedness in Nuclear Medicine Departments in Singapore and Response to The Global Pandemic. Ann. Acad. Med. Singap. 2020, 49, 496–500. [Google Scholar] [CrossRef]
- Chan, J.J.; Sim, Y.; Ow, S.G.; Lim, J.S.J.; Kusumawidjaja, G.; Zhuang, Q.; Wong, R.X.; Wong, F.Y.; Tan, V.K.M.; Tan, T.J.Y. The impact of COVID-19 on and recommendations for breast cancer care: The Singapore experience. Endocr.-Relat. Cancer 2020, 27, R307–R327. [Google Scholar] [CrossRef]
- Kanesvaran, R.; Chia, C.S.; Yap, S.P.; Wang, M.L.C.; Tham, C.K.; Lim, S.T.; Hwang, W.Y.K.; Kwek, J.W. Cancer Versus COVID-19: A Coordinated Disease Outbreak Response System (DORS) to Combat COVID-19 at the National Cancer Centre Singapore. Ann. Acad. Med. Singap. 2020, 49, 807–809. [Google Scholar] [CrossRef]
- Ngaserin, S.; Chua, H.W.; Chew, M.; Tan, B.K. A tripartite approach can seek to optimize breast cancer management during a pandemic—Real-Time experience of a developing breast oncology unit in Singapore. Breast J. 2020, 26, 1593–1596. [Google Scholar] [CrossRef]
- Ngoi, N.; Lim, J.; Ow, S.; Jen, W.Y.; Lee, M.; Teo, W.; Ho, J.; Sundar, R.; Tung, M.L.; Lee, Y.M.; et al. A segregated-team model to maintain cancer care during the COVID-19 outbreak at an academic center in Singapore. Ann. Oncol. 2020, 31, 840–843. [Google Scholar] [CrossRef]
- Chiang, J.; Yang, V.S.; Han, S.; Zhuang, Q.; Ooi, G.; Sin, I.H.; Chua, G.W.Y.; Tan, S.Y.; Chia, C.S.; Tan, V.K.-M.; et al. Minimizing transmission of COVID-19 while delivering optimal cancer care in a National Cancer Centre. J. Cancer Policy 2020, 25, 100241. [Google Scholar] [CrossRef]
- Vong, E.K.; Chia, P.-L.; Chang, A.Y. Lung cancer management during the COVID-19 pandemic: Experience of a medical oncology unit at a tertiary hospital in Singapore. J. Cancer Metastasis Treat. 2020, 6. [Google Scholar] [CrossRef]
- Tey, J.; Ho, S.; Choo, B.A.; Ho, F.; Yap, S.P.; Tuan, J.K.; Leong, C.N.; Cheo, T.; Sommat, K.; Wang, M.L. Navigating the challenges of the COVID-19 outbreak: Perspectives from the radiation oncology service in Singapore. Radiother. Oncol. 2020, 148, 189–193. [Google Scholar] [CrossRef] [PubMed]
- Tan, B.; Tuan, J.; Yap, S.; Ho, S.; Wang, M. Managing the COVID-19 Pandemic as a National Radiation Oncology Centre in Singapore. Clin. Oncol. 2020, 32, e155–e159. [Google Scholar] [CrossRef] [PubMed]
- Shi, A.H.; Guo, W.; Chng, C.K.; Chan, B.H. Precautions When Providing Dental Care during Coronavirus Disease 2019 (COVID-19) Pandemic. Ann. Acad. Med. Singap. 2020, 49, 312–319. [Google Scholar] [CrossRef] [PubMed]
- Tay, J.R.H.; Ng, E.; Ong, M.M.A.; Sim, C.; Tan, K.; Seneviratne, C.J. A Risk-Based Approach to the COVID-19 Pandemic: The Experience in National Dental Centre Singapore. Front. Med. 2020, 7, 562728. [Google Scholar] [CrossRef]
- Yi, X.; Jamil, N.B.; Gaik, I.T.C.; Fee, L.S. Community nursing services during the COVID-19 pandemic: The Singapore experience. Br. J. Community Nurs. 2020, 25, 390–395. [Google Scholar] [CrossRef]
- Hwang, J.; Yong, E.; Cheong, K.; Ling, Z.J.; Goh, L.H.; Lim, F.S.; Loh, V.; Bagdasarian, N.; Somani, J.; Archuleta, S.; et al. Responding to the COVID-19 pandemic: The role of occupational health services in a tertiary hospital in Singapore. J. Occup. Health 2020, 62, e12172. [Google Scholar] [CrossRef] [PubMed]
- Lim, W.Y.; Wong, P.; Ong, S.G. Reducing droplet spread during airway manipulation. Reply to Au Yong and colleagues. Br. J. Anaesth. 2020, 125, e178–e179. [Google Scholar] [CrossRef]
- Lim, W.Y.; Wong, P.; Teo, L.-M.; Ho, V.K. Resuscitation during the COVID-19 pandemic: Lessons learnt from high-fidelity simulation. Resuscitation 2020, 152, 89–90. [Google Scholar] [CrossRef]
- Ti, L.K.; Ang, L.S.; Foong, T.W.; Ng, B.S.W. What we do when a COVID-19 patient needs an operation: Operating room preparation and guidance. Can. J. Anesth. 2020, 67, 756–758. [Google Scholar] [CrossRef] [Green Version]
- Lim, M.L.; Wong, I.M.; Suhitharan, T.; Kong, A.S.; Goh, Q.Y. A Method to Decrease Exposure to Aerosols for Percutaneous Tracheostomy during the COVID-19 Pandemic. Ann. Acad. Med. Singap. 2020, 49, 608–610. [Google Scholar] [CrossRef]
- Wong, J.; Goh, Q.Y.; Tan, Z.; Lie, S.A.; Tay, Y.C.; Ng, S.Y.; Soh, C.R. Preparing for a COVID-19 pandemic: A review of operating room outbreak response measures in a large tertiary hospital in Singapore. Can. J. Anesth. 2020, 67, 732–745. [Google Scholar] [CrossRef] [Green Version]
- Ong, S.; Khee, T.T.; Tan, T.K. Practical considerations in the anaesthetic management of patients during a COVID-19 epidemic. Anaesthesia 2020, 75, 823–824. [Google Scholar] [CrossRef] [PubMed]
- Au Yong, P.S.A.; Kwa, C.W.X.; Chan, X.H.D. Anaesthetic Considerations for Rationalizing Drug Use in the Operating Theatre: Strategies in a Singapore Hospital during COVID-19. SN Compr. Clin. Med. 2020, 2, 871–873. [Google Scholar] [CrossRef] [PubMed]
- Wong, P.; Lim, W.Y. Aligning difficult airway guidelines with the anesthetic COVID-19 guidelines to develop a COVID-19 difficult airway strategy: A narrative review. J. Anesthesia 2020, 34, 924–943. [Google Scholar] [CrossRef] [PubMed]
- George, J.M.; Xu, Y.; Nursa’Adah, B.J.; Lim, S.F.; Low, L.L.; Chan, D.X. Collaboration between a tertiary pain centre and community teams during the pandemic. Br. J. Community Nurs. 2020, 25, 480–488. [Google Scholar] [CrossRef]
- Thampi, S.; Yap, A.; Fan, L.; Ong, J. Special considerations for the management of COVID-19 pediatric patients in the operating room and pediatric intensive care unit in a tertiary hospital in Singapore. Pediatr. Anesthesia 2020, 30, 642–646. [Google Scholar] [CrossRef] [Green Version]
- Lie, S.A.; Wong, L.T.; Chee, M.; Chong, S.Y. Process-Oriented In Situ Simulation Is a Valuable Tool to Rapidly Ensure Operating Room Preparedness for COVID-19 Outbreak. Simul. Health J. Soc. Simul. Health 2020, 15, 225–233. [Google Scholar] [CrossRef] [PubMed]
- Liew, M.F.; Siow, W.T.; Yau, Y.W.; See, K.C. Safe patient transport for COVID-19. Crit. Care 2020, 24, 1–3. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Ganti, S.; Shanker, S.; Pek, J.H. COVID-19 among Foreign Workers in Dormitories—How One Emergency Department Responded. Ann. Acad. Med. Singap. 2020, 49, 1034–1038. [Google Scholar] [CrossRef]
- Chua, W.L.T.; Quah, L.J.J.; Shen, Y.; Zakaria, D.; Wan, P.W.; Tan, K.; Wong, E. Emergency department € outbreak rostering’ to meet challenges of COVID-19. Emerg. Med. J. 2020, 37, 407–410. [Google Scholar] [CrossRef]
- Anaikatti, P.; Sheth, S.K.; Canlas, A.M.; Shanbhag, N.V.; Goh, M.L.; Lim, H.C. Electronic medical record platform enhancements during COVID-19 to support identify-isolate-inform strategy for initial detection and management of patients. Emerg. Med. Australas. 2021, 33, 164–167. [Google Scholar] [CrossRef]
- Liu, Z.; Teo, T.L.; Lim, M.J.; Nadarajan, G.D.; Segaram, S.S.C.; Thangarajoo, S.; Wee, L.E.; Wee, J.C.P.; Tan, K.B.K. Dynamic emergency department response to the evolving COVID-19 pandemic: The experience of a tertiary hospital in Singapore. J. Am. Coll. Emerg. Physicians Open 2020, 1, 1395–1403. [Google Scholar] [CrossRef] [PubMed]
- Thangayah, J.R.; Tan, K.B.K.; Lim, C.S.; Fua, T.P. Disease Outbreak Surge Response: How a Singapore Tertiary Hospital converted a multi-storey carpark into a Flu Screening Area to respond to the COVID-19 pandemic. Disaster Med. Public Health Prep. 2020, 15, e37–e42. [Google Scholar] [CrossRef]
- Quah, L.J.J.; Tan, B.K.K.; Fua, T.-P.; Wee, C.P.J.; Lim, C.S.; Nadarajan, G.; Zakaria, N.D.; Chan, S.-E.J.; Wan, P.W.; Teo, L.T.; et al. Reorganising the emergency department to manage the COVID-19 outbreak. Int. J. Emerg. Med. 2020, 13, 1–11. [Google Scholar] [CrossRef] [PubMed]
- Wee, L.E.; Fua, T.; Chua, Y.Y.; Ho, F.W.A.; Sim, X.Y.J.; Conceicao, E.P.; Mph, I.V.; Tan, K.B.-K.; Tan, B.H. Containing COVID-19 in the Emergency Department: The Role of Improved Case Detection and Segregation of Suspect Cases. Acad. Emerg. Med. 2020, 27, 379–387. [Google Scholar] [CrossRef]
- Manauis, C.M.; Loh, M.; Kwan, J.; Mingzhou, J.C.; Teo, H.J.; Peng, D.T.K.; Sushilan, S.V.; Leo, Y.S.; Ang Ang Hou, M.B. BCh, BAO (Dublin), MRCS (A&E) (Edinburgh), FAMS, Grad. Dip. Geriatric Medicine (NUS) Bracing for impact: Operational upshots from the National Centre for Infectious Diseases Screening Centre (Singapore) during the COVID-19 outbreak. J. Am. Coll. Emerg. Physicians Open 2020, 1, 549–556. [Google Scholar] [CrossRef]
- Bagdasarian, N.; Mathews, I.; Ng, A.J.Y.; Liu, E.H.; Sin, C.; Mahadevan, M.; Fisher, D.A.; Alexander, N.J.Y.; Choon, E.L.H. A safe and efficient, naturally ventilated structure for COVID-19 surge capacity in Singapore. Infect. Control. Hosp. Epidemiol. 2021, 42, 630–632. [Google Scholar] [CrossRef]
- Siow, W.T.; Tang, S.H.; Agrawal, R.V.; Tan, A.Y.H.; See, K.C. Essential ICU drug shortages for COVID-19: What can frontline clinicians do? Crit. Care 2020, 24, 1–3. [Google Scholar] [CrossRef]
- Liew, M.F.; Siow, W.T.; MacLaren, G.; See, K.C. Preparing for COVID-19: Early experience from an intensive care unit in Singapore. Crit. Care 2020, 24, 1–3. [Google Scholar] [CrossRef] [Green Version]
- Tan, Z.; Phoon, P.H.Y.; Tien, C.J.-C.; Katijo, J.; Ng, S.Y.; Goh, M.H. Practical Considerations for Converting Operating Rooms and Post-anaesthesia Care Units into Intensive Care Units in the COVID-19 Pandemic—Experience from a Large Singapore Tertiary Hospital. Ann. Acad. Med. Singap. 2020, 49, 1009–1012. [Google Scholar] [CrossRef]
- Phua, J.; Weng, L.; Ling, L.; Egi, M.; Lim, C.-M.; Divatia, J.V.; Shrestha, B.R.; Arabi, Y.M.; Ng, J.; Gomersall, C.D.; et al. Intensive care management of coronavirus disease 2019 (COVID-19): Challenges and recommendations. Lancet Respir. Med. 2020, 8, 506–517. [Google Scholar] [CrossRef]
- Anantham, D.; Sewa, D.W.; Ng, S.Y.; Phua, G.C. Triage of ICU Resources in a Pandemic Surge: Good Ethics Depends on Good Data. Ann Acad Med Singap. 2020, 49, 605–607. [Google Scholar] [CrossRef] [PubMed]
- Ho, S.; Tan, Y.Y.; Neo, S.H.S.; Zhuang, Q.; Chiam, M.; Zhou, J.X.; Woong, N.L.; Lee, G.; Krishna, L.K. COVID-19—A Review of the Impact it has made on Supportive and Palliative Care Services Within a Tertiary Hospital and Cancer Centre in Singapore. Ann. Acad. Med. Singap. 2020, 49, 489–495. [Google Scholar] [CrossRef] [PubMed]
- Koh, M.Y.; Yh, M.K. Palliative Care in the Time of COVID-19: Reflections from the Frontline. J. Pain Symptom Manag. 2020, 60, 3–4. [Google Scholar] [CrossRef]
- Poi, C.H.; Koh, M.Y.; Neo, H.Y.; Hum, A.Y. Palliative Care in a COVID-19 Intensive Care Unit (ICU): Challenges and Recommendations for Palliative Care Teams in a Pandemic ICU. Ann. Acad. Med. Singap. 2020, 49, 517–522. [Google Scholar] [CrossRef] [PubMed]
- Khatri, P.; Seetharaman, S.; Phang, C.M.J.; Lee, B.X.A. Home Hospice Services during COVID-19: Ensuring Comfort in Unsettling Times in Singapore. J. Palliat. Med. 2020, 23, 605–606. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Ong, K.J.; Lim, M.Y.Y.; Chng, J.X.R.; Wong, Y.P.; Koh, L.H. Collateral Damage: How the COVID-19 Pandemic Has Affected the Dying Process of Palliative Care Patients in Hospitals-Our Experience and Recommendations. Ann. Acad. Med. Singap. 2020, 49, 618–622. [Google Scholar] [CrossRef]
- Ong, E.K.; Soh, G.T.; Peh, T.Y.; Lo, T.J.; Yee, A.C. Challenges faced by Community Palliative Care Services during the COVID-19 Pandemic-Experiences from a Hospice. Ann. Acad. Med. Singap. 2020, 49, 590–595. [Google Scholar] [CrossRef]
- Tan, S.S.; Yan, B.; Saw, S.; Lee, C.K.; Chong, A.T.; Jureen, R.; Sethi, S. Practical laboratory considerations amidst the COVID-19 outbreak: Early experience from Singapore. J. Clin. Pathol. 2021, 74, 257–260. [Google Scholar] [CrossRef] [Green Version]
- Quek, B.H.; Biswas, A.; Ee, K.T.; Yeo, C.L. Newborn Resuscitation in COVID-19. Ann. Acad. Med. Singap. 2020, 49, 909–912. [Google Scholar] [CrossRef]
- Aishworiya, R.; Biswas, A.; Tan, M.L.N.; Ho, W.L.C.; Joseph, R. COVID-19 Pandemic and Children’s Health—Mitigating Unintended Consequences. Ann. Acad. Med. Singap. 2020, 49, 1031–1033. [Google Scholar] [CrossRef] [PubMed]
- Aishworiya, R.; Chong, S.C.; Kiing, J.S.H. When Life is Put on Hold, How Do We Hold on to Life? Challenges and Opportunities in Developmental and Behavioral Pediatrics during COVID-19. J. Dev. Behav. Pediatr. 2020, 41, 337–339. [Google Scholar] [CrossRef]
- Mulay, K.V.; Aishworiya, R.; Lim, T.S.; Tan, M.Y.; Kiing, J.S.; Chong, S.C.; Kang, Y.Q. Innovations in practice: Adaptation of developmental and behavioral pediatric service in a tertiary center in Singapore during the COVID-19 pandemic. Pediatr. Neonatol. 2021, 62, 70–79. [Google Scholar] [CrossRef]
- Priyadharsini, H.; Chiang, J.J. Embracing telehealth: Supporting young children and families through occupational therapy in Singapore during COVID-19. World Fed. Occup. Ther. Bull. 2020, 76, 90–93. [Google Scholar] [CrossRef]
- Chan, S.M.; Chiong, T.; Chhabra, M.; Koh, C.T.; Wong, Y.L.; Sng, A.A.; Ong, H.T. Early Challenges in Isolation and De-Isolation of Children during the Severe Acute Respiratory Syndrome Coronavirus-2 Pandemic. J. Paediatr. Child. Health 2020, 56, 997–998. [Google Scholar] [CrossRef]
- Wong, J.J.M.; Abbas, Q.; Anantasit, N.; Shimizu, N.; Malisie, R.F.; Dang, H.; Xu, F.; Ong, J.S.M.; Lee, P.C.; Saito, O.; et al. Changes Adopted in Asian Pediatric Hospitals during the COVID-19 Pandemic: A Report from the Pediatric Acute and Critical Care COVID-19 Registry of Asia. J. Pediatr. Intensiv. Care 2021. [Google Scholar] [CrossRef]
- Davis, C.; Ng, K.C.; Oh, J.Y.; Baeg, A.; Rajasegaran, K.; Chew, C.S.E. Caring for Children and Adolescents with Eating Disorders in the Current Coronavirus 19 Pandemic: A Singapore Perspective. J. Adolesc. Health 2020, 67, 131–134. [Google Scholar] [CrossRef]
- Tan, R.M.R.; Ong, G.Y.-K.; Chong, S.-L.; Ganapathy, S.; Tyebally, A.; Lee, K.P. Dynamic adaptation to COVID-19 in a Singapore paediatric emergency department. Emerg. Med. J. 2020, 37, 252–254. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Lam, L.T.M.; Chua, Y.X.; Tan, D.H.Y. Roles and challenges of primary care physicians facing a dual outbreak of COVID-19 and dengue in Singapore. Fam. Pract. 2020, 37, 578–579. [Google Scholar] [CrossRef]
- Wong, S.Y.S.; Tan, D.H.Y.; Zhang, Y.; Ramiah, A.; Zeng, X.; Hui, E.; Young, D.Y.L. A Tale of 3 Asian Cities: How is Primary Care Responding to COVID-19 in Hong Kong, Singapore, and Beijing? Ann. Fam. Med. 2021, 19, 48–54. [Google Scholar] [CrossRef]
- Chen, R.; Chaterji, S.; Moosa, A.S. Responding to the COVID-19 pandemic at a primary care centre in Singapore. Singap. Med. J. 2020. [Google Scholar] [CrossRef]
- Liow, Y.; Loh, V.W.K.; Young, D. 100 days on: The primary care response to COVID-19 in Singapore. Singap. Med. J. 2020. [Google Scholar] [CrossRef]
- Lim, W.H.; Wong, W.M. COVID-19: Notes from the Front Line, Singapore’s Primary Health Care Perspective. Ann. Fam. Med. 2020, 18, 259–261. [Google Scholar] [CrossRef] [PubMed]
- Tor, P.C.; Phu, A.H.; Koh, D.S.H.; Mok, Y.M. Electroconvulsive Therapy in a Time of Coronavirus Disease. J. ECT 2020, 36, 80–85. [Google Scholar] [CrossRef]
- Lim, W.S.; Soh, K.C.; Surej, J.; Goh, K.H. Examining the role of a Psychiatry department in Singapore amidst COVID-19. Asian J. Psychiatry 2020, 54, 102296. [Google Scholar] [CrossRef]
- Poremski, D.; Subner, S.H.; Lam, G.F.; Dev, R.; Mok, Y.M.; Chua, H.C.; Fung, D.S.; Kin, F. Effective infection prevention and control strategies in a large, accredited, psychiatric facility in Singapore. Infect. Control. Hosp. Epidemiol. 2020, 41, 1238–1240. [Google Scholar] [CrossRef] [Green Version]
- H’ng, M.W.; Tan, B.P.; Punamiya, S. Setting up an Interventional Radiology Suite in an Infectious Diseases Centre: Lessons from the Novel Coronavirus (COVID-19) Outbreak. Ann. Acad. Med. Singap. 2020, 49, 684–689. [Google Scholar] [CrossRef] [PubMed]
- Gogna, A.; Punamiya, S.; Gopinathan, A.; Irani, F.; Toh, L.H.W.; Cheong, L.H.W.; Babu, S.; Wee, B.; Goh, P.; Tan, B.P.; et al. Preparing IR for COVID-19: The Singapore Experience. J. Vasc. Interv. Radiol. 2020, 31, 869–875. [Google Scholar] [CrossRef] [PubMed]
- Low, H.M.; Low, E.; Lee, C.H. TTSH and NCID Radiology Services in COVID-19. Ann. Acad. Med. Singap. 2020, 49, 913–914. [Google Scholar] [CrossRef]
- Mossa-Basha, M.; Meltzer, C.C.; Kim, D.C.; Tuite, M.J.; Kolli, K.P.; Tan, B.S. Radiology Department Preparedness for COVID-19: Radiology Scientific Expert Review Panel. Radiology 2020, 296, E106–E112. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Tsou, I.; Liew, C.; Tan, B.; Chou, H.; Wong, S.; Loke, K.; Quah, R.; Tan, A.; Tay, K. Planning and coordination of the radiological response to the coronavirus disease 2019 (COVID-19) pandemic: The Singapore experience. Clin. Radiol. 2020, 75, 415–422. [Google Scholar] [CrossRef]
- Goh, Y.; Chua, W.; Lee, J.K.; Ang, B.W.L.; Liang, C.R.; Tan, C.A.; Choong, D.A.W.; Hoon, H.X.; Ong, M.K.L.; Quek, S.T. Operational Strategies to Prevent Coronavirus Disease 2019 (COVID-19) Spread in Radiology: Experience from a Singapore Radiology Department After Severe Acute Respiratory Syndrome. J. Am. Coll. Radiol. 2020, 17, 717–723. [Google Scholar] [CrossRef] [PubMed]
- Cheng, L.T.E.; Chan, L.P.; Tan, B.H.; Chen, R.C.; Tay, K.H.; Ling, M.L.; Tan, B.S. Deja Vu or Jamais Vu? How the Severe Acute Respiratory Syndrome Experience Influenced a Singapore Radiology Department’s Response to the Coronavirus Disease (COVID-19) Epidemic. Am. J. Roentgenol. 2020, 214, 1206–1210. [Google Scholar] [CrossRef] [PubMed]
- Heng, A.L.; Ooi, C.C.; Eu, B.J.W.; Kiew, Y.S.; Wong, A.S.K.; Da Zhuang, K. The bug stops with me: Prevention of COVID-19 nosocomial transmission during radiographic procedures. J. Med. Imaging Radiat. Sci. 2020, 51, 540–545. [Google Scholar] [CrossRef]
- Chen, R.C.; Tan, T.T.; Chan, L.P. Adapting to a new normal? 5 key operational principles for a radiology service facing the COVID-19 pandemic. Eur. Radiol. 2020, 30, 4964–4967. [Google Scholar] [CrossRef]
- Tay, K.H.; Ooi, C.C.; Bin Mahmood, M.I.; Aw, L.P.; Chan, L.P.; Ng, D.C.E.; Tan, B.S. Reconfiguring the radiology leadership team for crisis management during the COVID-19 pandemic in a large tertiary hospital in Singapore. Eur. Radiol. 2021, 31, 468–474. [Google Scholar] [CrossRef] [PubMed]
- Wong, A.S.K.; Ooi, C.C.; Leow, M.Q.H.; Kiew, Y.S.; Yeo, K.C.W.; Tan, S.G.; Tay, K.H. Adapting Lessons from SARS for the COVID-19 Pandemic—Perspectives from Radiology Nursing in Singapore. J. Radiol. Nurs. 2020, 39, 164–167. [Google Scholar] [CrossRef]
- Tan, B.P.; Lim, K.C.; Goh, Y.G.; Kok, S.S.X.; Teo, S.Y.; Poh, A.C.C.; Kaw, G.J.L.; Quek, S.T.; Wong, S.B.S.; Chan, L.P. Radiology Preparedness in the Ongoing Battle against COVID-19: Experiences from Large to Small Public Hospitals in Singapore. Radiol. Cardiothorac. Imaging 2020, 2, e200140. [Google Scholar] [CrossRef] [Green Version]
- Chen, R.C.; Cheng, L.T.-E.; Lim, J.L.L.; Gogna, A.; Ng, D.C.E.; Teo, L.Z.Y.; Tan, B.S. Touch Me Not: Safe Distancing in Radiology During Coronavirus Disease 2019 (COVID-19). J. Am. Coll. Radiol. 2020, 17, 739–742. [Google Scholar] [CrossRef] [PubMed]
- Too, C.W.; Wen, D.W.; Patel, A.; Syafiq, A.R.A.; Liu, J.; Leong, S.; Gogna, A.; Lo, R.H.G.; Tashi, S.; Lee, K.A.; et al. Interventional Radiology Procedures for COVID-19 Patients: How we Do it. Cardiovasc. Interv. Radiol. 2020, 43, 827–836. [Google Scholar] [CrossRef] [PubMed]
- Da Zhuang, K.; Tan, B.S.; Tan, B.H.; Too, C.W.; Tay, K.H. Old Threat, New Enemy: Is Your Interventional Radiology Service Ready for the Coronavirus Disease 2019? Cardiovasc Intervent Radiol. 2020, 43, 665–666. [Google Scholar] [CrossRef] [Green Version]
- Kok, S.; Shah, M.; Cheong, W.; Cheng, K.; Sng, L.; Salkade, P.; Wong, B. Dealing with COVID-19: Initial perspectives of a small radiology department. Singap. Med. J. 2020, 61, 375–377. [Google Scholar] [CrossRef]
- Quek, L.H.H.; Kannivelu, A.; Pua, U. 90Y Radioembolization: Telemedicine During COVID-19 Outbreak, Opportunity for Prime Time. J. Nucl. Med. 2020, 61, 780. [Google Scholar] [CrossRef] [Green Version]
- Lam, A.Y.; Chan, E.C.; Quek, C.M.; Peng, Y.; Yeo, S.K.; Chang, R.F.; Xin, X.; Goh, S.-Y. Videoconsultation to overcome barriers during COVID-19. Ann. Acad. Med. Singap. 2021, 50, 77–83. [Google Scholar] [CrossRef]
- Kin, W.W. Rapid Transition to a Telemedicine Service at Singapore Community Dialysis Centers during Covid-19. NEJM Catalyst. ScholarBank@NUS Repos. 2020. [Google Scholar] [CrossRef]
- Tan, L.F.; Tee, L.Y.S.; Seetharaman, S.K. Virtual Intergenerational Therapy: New Platforms for Engagement of Older Adults During the COVID-19 Crisis. Am. J. Geriatr. Psychiatry 2020, 28, 1330–1331. [Google Scholar] [CrossRef]
- Poon, N.Y.; Fong, S.P.; Chen, H.Y. Child and adolescent psychiatry telemedicine: A singaporean experience born in Covid-19. Asian J. Psychiatry 2020, 53, 102336. [Google Scholar] [CrossRef] [PubMed]
- Tan, L.L.; Pillay, V.D.; Chia, J.W.; Seah, A.S.; Liu, C.M.; Lim, Y.; Low, J.Y. Using Telemedicine for Outpatient Geriatric Care During the Novel Coronavirus Outbreak: Experience from the First 15 Patients. Ann. Acad. Med. Singap. 2020, 49, 699–703. [Google Scholar] [CrossRef]
- Lim, S.T.; Yap, F.; Chin, X. Bridging the Needs of Adolescent Diabetes Care during COVID-19: A Nurse-Led Telehealth Initiative. J. Adolesc. Health 2020, 67, 615–617. [Google Scholar] [CrossRef] [PubMed]
- Wang, L.Y.; Low, T.T.; Yeo, T.J. Telehealth in COVID-19 and Cardiovascular Disease-Ensuring Equitable Care. Ann. Acad. Med. Singap. 2020, 49, 902–904. [Google Scholar] [CrossRef] [PubMed]
- Lin, Z.; Sim, T.B.; Ong, V.Y.K.; Bin Ab Hamid, Z.; Ho, W.H. Telemedicine in the acute care setting during the COVID-19 pandemic. Intern. Emerg. Med. 2020, 15, 1591–1593. [Google Scholar] [CrossRef] [PubMed]
- Lai, S.H.S.; Tang, C.Q.Y. Telemedicine and COVID-19: Beyond just virtual consultations—The Singapore experience. Bone Jt. Open 2020, 1, 203–204. [Google Scholar] [CrossRef] [PubMed]
- Ong, C.S.H.; Lu, J.; Tan, Y.Q.; Tan, L.G.L.; Tiong, H.Y. Implementation of a Ureteric Colic Telemedicine Service: A Mixed Methods Quality Improvement Study. Urology 2021, 147, 14–20. [Google Scholar] [CrossRef] [PubMed]
- Ko, S.Q.; Hooi, B.M.Y.; Koo, C.-Y.; Chor, D.W.P.; Ling, Z.J.; Chee, Y.-L.; Jen, W.-Y. Remote monitoring of marginalised populations affected by COVID-19: A retrospective review. BMJ Open 2020, 10, e042647. [Google Scholar] [CrossRef]
- Tan, L.F.; Teng, V.H.W.; Seetharaman, S.K.; Yip, A.W. Facilitating telehealth for older adults during the COVID-19 pandemic and beyond: Strategies from a Singapore geriatric center. Geriatr. Gerontol. Int. 2020, 20, 993–995. [Google Scholar] [CrossRef] [PubMed]
- Ong, J.; Young, B.E.; Ong, S. COVID-19 in gastroenterology: A clinical perspective. Gut 2020, 69, 1144–1145. [Google Scholar] [CrossRef]
- Kam, K.-Q.; Ong, J.S.M.; Lee, J.H. Kawasaki disease in the COVID-19 era: A distinct clinical phenotype? Lancet Child. Adolesc. Health 2020, 4, 642–643. [Google Scholar] [CrossRef]
- Kheok, S.W.; Teo, N.W.Y. Olfactory Loss of Function as a Possible Symptom of COVID-19. JAMA Otolaryngol. Neck Surg. 2020, 146, 873–874. [Google Scholar] [CrossRef]
- Chew, M.; Koh, F.; Wu, J.; Ngaserin, S.; Ng, A.; Ong, B.; Lee, V. Clinical assessment of COVID-19 outbreak among migrant workers residing in a large dormitory in Singapore. J. Hosp. Infect. 2020, 106, 202–203. [Google Scholar] [CrossRef]
- Fan, B.E.; Chong, V.C.L.; Chan, S.S.W.; Lim, G.H.; Lim, K.G.E.; Tan, G.B.; Mucheli, S.S.; Kuperan, P.; Ong, K.H. Hematologic parameters in patients with COVID-19 infection. Am. J. Hematol. 2020, 95. [Google Scholar] [CrossRef] [Green Version]
- Wee, L.E.; Chan, Y.F.Z.; Teo, N.W.Y.; Cherng, B.P.Z.; Thien, S.Y.; Wong, H.M.; Wijaya, L.; Toh, S.T.; Tan, T.T. The role of self-reported olfactory and gustatory dysfunction as a screening criterion for suspected COVID-19. Eur. Arch. Oto-Rhino-Laryngol. 2020, 277, 2389–2390. [Google Scholar] [CrossRef] [Green Version]
- Ng, J.J.; Choong, A. Thromboembolic events in patients with SARS-CoV-2. J. Vasc. Surg. 2020, 72, 760–761. [Google Scholar] [CrossRef]
- Tan, C.W.; Low, J.G.H.; Wong, W.H.; Chua, Y.Y.; Goh, S.L.; Ng, H.J. Critically ill COVID -19 infected patients exhibit increased clot waveform analysis parameters consistent with hypercoagulability. Am. J. Hematol. 2020, 95, E156–E158. [Google Scholar] [CrossRef] [PubMed]
- Liew, I.Y.; Mak, T.M.; Cui, L.; Vasoo, S.; Lim, X.R. A Case of Reactive Arthritis Secondary to Coronavirus Disease 2019 Infection. JCR J. Clin. Rheumatol. 2020, 26, 233. [Google Scholar] [CrossRef] [PubMed]
- Yong, M.H.; Chan, Y.F.Z.; Liu, J.; Sanamandra, S.K.; Kheok, S.W.; Lim, K.C.; Sewa, D.W. A Rare Case of Acute Hemorrhagic Leukoencephalitis in a COVID-19 Patient. J. Neurol. Sci. 2020, 416, 117035. [Google Scholar] [CrossRef] [PubMed]
- Chua, A.J.; Charn, T.C.; Chan, E.C.; Loh, J. Acute Olfactory Loss Is Specific for COVID-19 at the Emergency Department. Ann. Emerg. Med. 2020, 76, 550–551. [Google Scholar] [CrossRef] [PubMed]
- Yan, G.; Ang, A.; Tham, S.M.; Ng, A.; Chew, K.L. Relative Bradycardia in Patients with Mild-to-Moderate Coronavirus Disease, Japan. Emerg. Infect. Dis. 2021, 27, 335. [Google Scholar] [CrossRef]
- Ho, J.S.; A Tambyah, P.; Ho, A.F.; Chan, M.Y.; Sia, C.-H. Effect of coronavirus infection on the human heart: A scoping review. Eur. J. Prev. Cardiol. 2020, 27, 1136–1148. [Google Scholar] [CrossRef] [PubMed]
- Chew Lip, N.; Kian Keong, P.; Khoo, H.W.; Hui, T.C.H.; Haja Mohideen, S.M.; Lee, Y.S.; Liew, C.J.Y.; Kok, S.S.X.; Young, B.E.; Ong, S.W.X.; et al. Radiographic features of COVID-19 based on an initial cohort of 96 patients in Singapore. Singap. Med. J. 2020, 61, 501–502. [Google Scholar]
- Koh, J.S.; De Silva, D.A.; Quek, A.M.L.; Chiew, H.J.; Tu, T.M.; Seet, C.Y.H.; Hoe, R.H.M.; Saini, M.; Hui, A.C.-F.; Angon, J.; et al. Corrigendum to ‘Neurology of COVID-19 in Singapore’. J. Neurol. Sci. 2021, 418, 117406. [Google Scholar] [CrossRef]
- Tham, A.C.; Thein, T.-L.; Lee, C.S.; Tan, G.S.E.; Manauis, C.M.; Siow, J.K.; Leo, Y.S.; Lim, M.Y. Olfactory taste disorder as a presenting symptom of COVID-19: A large single-center Singapore study. Eur. Arch. Oto-Rhino-Laryngol. 2021, 278, 1853–1862. [Google Scholar] [CrossRef] [PubMed]
- Sun, Y.; Koh, V.; Marimuthu, K.; Ng, O.T.; Young, B.; Vasoo, S.; Chan, M.; Lee, V.J.M.; De, P.P.; Barkham, T.; et al. Epidemiological and Clinical Predictors of COVID-19. Clin. Infect. Dis. 2020, 71, 786–792. [Google Scholar] [CrossRef] [Green Version]
- Hui, T.C.H.; Khoo, H.W.; Young, B.E.; Mohideen, S.M.H.; Lee, Y.S.; Lim, C.J.; Leo, Y.S.; Kaw, G.J.L.; Lye, D.; Tan, C.H. Clinical utility of chest radiography for severe COVID-19. Quant. Imaging Med. Surg. 2020, 10, 1540–1550. [Google Scholar] [CrossRef]
- Ngiam, J.N.; Chew, N.; Tham, S.M.; Beh, D.L.-L.; Lim, Z.Y.; Li, T.Y.; Cen, S.; Tambyah, P.A.; Santosa, A.; Sia, C.-H.; et al. Demographic shift in COVID-19 patients in Singapore from an aged, at-risk population to young migrant workers with reduced risk of severe disease. Int. J. Infect. Dis. 2021, 103, 329–335. [Google Scholar] [CrossRef]
- Ong, S.W.X.; Young, B.E.; Leo, Y.-S.; Lye, D. Association of Higher Body Mass Index With Severe Coronavirus Disease 2019 (COVID-19) in Younger Patients. Clin. Infect. Dis. 2020, 71, 2300–2302. [Google Scholar] [CrossRef]
- Goh, Y.; Beh, D.L.; Makmur, A.; Somani, J.; Chan, A.C. Pearls & Oy-sters: Facial nerve palsy in COVID-19 infection. Neurology 2020, 95, 364–367. [Google Scholar] [CrossRef] [PubMed]
- Peh, W.M.; Chan, S.K.T.; Lee, Y.L.; Gare, P.S.; Ho, V.K. Lung ultrasound in a Singapore COVID-19 intensive care unit patient and a review of its potential clinical utility in pandemic. J. Ultrason. 2020, 20, e154–e158. [Google Scholar] [CrossRef]
- Sia, C.S.M.; Cheong, S.H.L.; Ngoh, C.L.Y.; Tan, Y.H.; Wong, W.K. Critical Coronavirus Disease 2019 in a Hemodialysis Patient: A Proposed Clinical Management Strategy. Case Rep. Nephrol. Dial. 2020, 10, 86–94. [Google Scholar] [CrossRef] [PubMed]
- Kam, K.-Q.; Yung, C.F.; Cui, L.; Lin, R.T.P.; Mak, T.M.; Maiwald, M.; Li, J.; Chong, C.Y.; Nadua, K.; Tan, N.W.H.; et al. A Well Infant with Coronavirus Disease 2019 With High Viral Load. Clin. Infect. Dis. 2020, 71, 847–849. [Google Scholar] [CrossRef] [PubMed]
- Tan, G.P.; Ho, S.; Fan, B.E.; Chotirmall, S.H.; Tan, C.H.; Lew, S.J.W.; Chia, P.Y.; Young, B.E.; Abisheganaden, J.A.; Puah, S.H. Reversible platypnea-orthodeoxia in COVID-19 acute respiratory distress syndrome survivors. Respir. Physiol. Neurobiol. 2020, 282, 103515. [Google Scholar] [CrossRef]
- Chong, V.C.L.; Lim, K.G.E.; Fan, B.E.; Chan, S.S.W.; Ong, K.H.; Kuperan, P. Reactive lymphocytes in patients with COVID-19. Br. J. Haematol. 2020, 189, 844. [Google Scholar] [CrossRef]
- Ho, Q.Y.; Chung, S.J.; Low, S.C.S.; Chen, R.C.; Teh, S.P.; Chan, F.Z.Y.; Tan, B.H.; Kee, T.Y.S. Evaluating Potential Deceased Donor Renal Transplant Recipients for Asymptomatic COVID-19. Transplant. Direct 2020, 6, e559. [Google Scholar] [CrossRef]
- Zhou, J.C.; Hui, T.C.; Tan, C.H.; Khoo, H.W.; Young, B.E.; Lye, D.C.; Lee, Y.S.; Kaw, G.J. Chest Radiography in Coronavirus Disease 2019 (COVID-19): Correlation with Clinical Course. Ann. Acad. Med. Singap. 2020, 49, 456–461. [Google Scholar] [CrossRef]
- Liew, J.R.P.; Lim, Y.D.; Liew, J.Y.C.; Poh, C.C.A. Clinics in diagnostic imaging (207). Coronavirus disease 2019 (COVID-19) atypical pneumonia. Singap. Med. J. 2020, 61, 363–369. [Google Scholar] [CrossRef]
- Ho, W.Y.B.; Wang, D.; Tan, L.Y.C.; Mahadeorao, B.M.; Tan, C.H.; Lim, H.L.J. Two cases of cutaneous eruptions due to CoVID-19 infection in Singapore: New insights into the spectrum of clinical presentation and histopathology. J. Eur. Acad. Dermatol. Venereol. 2020, 34, E576–E579. [Google Scholar] [CrossRef] [PubMed]
- Lim, L.W.; Tan, G.S.; Yong, V.; Anderson, D.E.; Lye, D.C.; Young, B.; Agrawal, R. Acute Onset of Bilateral Follicular Conjunctivitis in two Patients with Confirmed SARS-CoV-2 Infections. Ocul. Immunol. Inflamm. 2020, 28, 1280–1284. [Google Scholar] [CrossRef] [PubMed]
- Goh, K.J.; Choong, M.C.; Cheong, E.H.; Kalimuddin, S.; Duu Wen, S.; Phua, G.C.; Chan, K.S.; Haja Mohideen, S. Rapid Progression to Acute Respiratory Distress Syndrome: Review of Current Understanding of Critical Illness from COVID-19 Infection. Ann. Acad. Med. Singap. 2020, 49, 108–118. [Google Scholar] [CrossRef] [PubMed]
- Ng, K.; Poon, B.H.; Puar, T.H.K.; Quah, J.L.S.; Loh, W.J.; Wong, Y.-J.; Tan, T.Y.; Raghuram, J. COVID-19 and the Risk to Health Care Workers: A Case Report. Ann. Intern. Med. 2020, 172, 766–767. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Yung, C.F.; Kam, K.Q.; Wong, M.S.Y.; Maiwald, M.; Tan, Y.K.; Tan, B.H.; Thoon, K.C. Environment and Personal Protective Equipment Tests for SARS-CoV-2 in the Isolation Room of an Infant with Infection. Ann. Intern. Med. 2020, 173, 240–242. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Ching-Hui, S.; Ngiam, J.N.; Chew, N.; Beh, D.L.L.; Kian Keong, P.; Sia, C.-H.; Poh, K.K. Educational case series of electrocardiographs during the COVID-19 pandemic and the implications for therapy. Singap. Med J. 2020, 61, 406–412. [Google Scholar]
- Yan, G.; Lee, C.K.; Lam, L.T.M.; Yan, B.; Chua, Y.X.; Lim, A.Y.N.; Phang, K.F.; Kew, G.S.; Teng, H.; Ngai, C.H.; et al. Covert COVID-19 and false-positive dengue serology in Singapore. Lancet Infect. Dis. 2020, 20, 536. [Google Scholar] [CrossRef] [Green Version]
- Lim, Z.; Khoo, H.; Hui, T.; Kok, S.; Kwan, K.; Young, B.; Tan, C.; Kaw, G. Variable computed tomography appearances of COVID-19. Singap. Med. J. 2020, 61, 387–391. [Google Scholar] [CrossRef]
- Young, B.E.; Ong, S.W.X.; Kalimuddin, S.; Low, J.G.; Tan, S.Y.; Loh, J.S.; Ng, O.T.; Marimuthu, K.; Ang, L.W.; Mak, T.M.; et al. Epidemiologic Features and Clinical Course of Patients Infected With SARS-CoV-2 in Singapore. JAMA-J. Am. Med Assoc. 2020, 323, 1488–1494. [Google Scholar] [CrossRef] [Green Version]
- Sim, S.; Teo, S.H.; Kong, J.; Lim, Z.; Ng, M.; Tang, W. COVID-19 in Singapore—A case series from primary care. Singap. Med. J. 2021, 62, 48–51. [Google Scholar] [CrossRef]
- Ong, S.W.X.; Tan, Y.K.; Sutjipto, S.; Chia, P.Y.; Young, B.E.; Gum, M.; Lau, S.K.; Chan, M.; Vasoo, S.; Mendis, S.; et al. Absence of contamination of personal protective equipment (PPE) by severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2). Infect. Control Hosp. Epidemiol. 2020, 41, 614–616. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Chia, P.Y.; Coleman, K.K.; Tan, Y.K.; Ong, S.W.X.; Gum, M.; Lau, S.K.; Lim, X.F.; Lim, A.S.; Sutjipto, S.; Lee, P.H.; et al. Detection of air and surface contamination by SARS-CoV-2 in hospital rooms of infected patients. Nat. Commun. 2020, 11, 2800. [Google Scholar] [CrossRef] [PubMed]
- Seah, I.; Anderson, D.E.; Kang, A.E.Z.; Wang, L.; Rao, P.; Young, B.E.; Lye, D.; Agrawal, R. Assessing Viral Shedding and Infectivity of Tears in Coronavirus Disease 2019 (COVID-19) Patients. Ophthalmology 2020, 127, 977–979. [Google Scholar] [CrossRef] [PubMed]
- Wee, L.E.I.; Thien, S.Y.; Singh, S.R.; Ling, M.L.; Venkatachalam, I. Containing COVID-19 in a specialised neurology centre: The risks of presymptomatic transmission. Neurol. Sci. 2020, 41, 2013–2015. [Google Scholar] [CrossRef]
- Loh, N.-H.W.; Tan, Y.; Taculod, J.; Gorospe, B.; Teope, A.S.; Somani, J.; Tan, A.Y.H. The impact of high-flow nasal cannula (HFNC) on coughing distance: Implications on its use during the novel coronavirus disease outbreak. Can. J. Anesth. 2020, 67, 893–894. [Google Scholar] [CrossRef] [Green Version]
- Ong, S.W.X.; Tan, Y.K.; Chia, P.Y.; Lee, T.H.; Ng, O.T.; Wong, M.S.Y.; Marimuthu, K. Air, Surface Environmental, and Personal Protective Equipment Contamination by Severe Acute Respiratory Syndrome Coronavirus 2 (SARS-CoV-2) from a Symptomatic Patient. JAMA-J. Am. Med Assoc. 2020, 323, 1610–1612. [Google Scholar] [CrossRef] [Green Version]
- Goh, X.L.; Low, Y.F.; Ng, C.H.; Amin, Z.; Ng, Y.P.M. Incidence of SARS-CoV-2 vertical transmission: A meta-analysis. Arch. Dis. Child Fetal. Neonatal. 2021, 106, 112–113. [Google Scholar] [CrossRef]
- Tan, W.Y.T.; Wong, L.Y.; Leo, Y.S.; Toh, M.P.H.S. Does incubation period of COVID-19 vary with age? A study of epidemiologically linked cases in Singapore. Epidemiol. Infect. 2020, 148, 1–16. [Google Scholar] [CrossRef] [PubMed]
- Seneviratne, C.J.; Balan, P.; Ko, K.K.K.; Udawatte, N.S.; Lai, D.; Ng, D.H.L.; Venkatachalam, I.; Lim, K.S.; Ling, M.L.; Oon, L.; et al. Efficacy of commercial mouth-rinses on SARS-CoV-2 viral load in saliva: Randomized control trial in Singapore. Infection 2021, 49, 305–311. [Google Scholar] [CrossRef] [PubMed]
- Ong, S.; Coleman, K.; Chia, P.; Thoon, K.; Pada, S.; Venkatachalam, I.; Fisher, D.; Tan, Y.; Tan, B.; Ng, O.; et al. Transmission modes of severe acute respiratory syndrome coronavirus 2 and implications on infection control: A review. Singap. Med. J. 2020. [Google Scholar] [CrossRef] [PubMed]
- Seah, I.; Agrawal, R. Can the Coronavirus Disease 2019 (COVID-19) Affect the Eyes? A Review of Coronaviruses and Ocular Implications in Humans and Animals. Ocul. Immunol. Inflamm. 2020, 28, 391–395. [Google Scholar] [CrossRef] [PubMed]
- Yeo, C.; Kaushal, S.; Yeo, D. Enteric involvement of coronaviruses: Is faecal-oral transmission of SARS-CoV-2 possible? Lancet Gastroenterol. Hepatol. 2020, 5, 335–337. [Google Scholar] [CrossRef] [Green Version]
- Guo, W.; Chan, B.H.; Chng, C.K.; Shi, A.H. Two Cases of Inadvertent Dental Aerosol Exposure to COVID-19 Patients. Ann. Acad. Med. Singap. 2020, 49, 514–516. [Google Scholar] [CrossRef]
- Amrun, S.N.; Lee, C.Y.P.; Lee, B.E.; Fong, S.W.; Young, B.E.; Chee, R.S.L.; Yeo, N.K.W.; Torres-Ruesta, A.; Carissimo, G.; Poh, C.M.; et al. Linear B-cell epitopes in the spike and nucleocapsid proteins as markers of SARS-CoV-2 exposure and disease severity. Ebiomedicine 2020, 58, 102911. [Google Scholar] [CrossRef]
- Tan, C.W.; Chia, W.N.; Qin, X.; Liu, P.; Chen, M.I.; Tiu, C.; Hu, Z.; Chen, V.C.; Young, B.E.; Sia, W.R.; et al. A SARS-CoV-2 surrogate virus neutralization test based on antibody-mediated blockage of ACE2-spike protein-protein interaction. Nat. Biotechnol. 2020, 38, 1073–1078. [Google Scholar] [CrossRef]
- Sutjipto, S.; Lee, P.H.; Tay, J.Y.; Mendis, S.M.; Abdad, M.Y.; Marimuthu, K.; Ng, O.T.; Cui, L.; Chan, M.; Soon, M.; et al. The Effect of Sample Site, Illness Duration, and the Presence of Pneumonia on the Detection of SARS-CoV-2 by Real-time Reverse Transcription PCR. Open Forum Infect. Dis. 2020, 7, ofaa335. [Google Scholar] [CrossRef]
- Wan, W.Y.; Lim, S.H.; Seng, E.H. Cross-reaction of Sera from COVID-19 Patients with SARS-CoV Assays. Ann. Acad. Med. Singap. 2020, 49, 523–526. [Google Scholar] [CrossRef]
- Tan, G.; Ang, H.; Manauis, C.; Chua, J.; Gao, C.; Ng, F.; Wong, C.; Ng, O.; Marimuthu, K.; Chan, M.; et al. Reducing hospital admissions for COVID-19 at a dedicated screening centre in Singapore. Clin. Microbiol. Infect. 2020, 26, 1278–1279. [Google Scholar] [CrossRef] [PubMed]
- Chan, K.S.; Ko, K.K.; Koh, T.H.; Ho, D.W.; Chan, Y.F.; Tan, T.T.; Le Oon, L. Initial Experiences of Laboratory Diagnosis of Coronavirus Disease 2019 (COVID-19) in Singapore General Hospital. Ann. Acad. Med. Singap. 2020, 49, 415–416. [Google Scholar] [CrossRef]
- Tay, J.-Y.; Lim, P.L.; Marimuthu, K.; Sadarangani, S.P.; Ling, L.M.; Ang, B.S.P.; Chan, M.; Leo, Y.-S.; Vasoo, S. De-isolating Coronavirus Disease 2019 Suspected Cases: A Continuing Challenge. Clin. Infect. Dis. 2020, 71, 883–884. [Google Scholar] [CrossRef] [PubMed]
- Kuo, B.J.; Lai, Y.K.; Tan, M.L.M.; Goh, X.-Y.C. Utility of Screening Chest Radiographs in Patients with Asymptomatic or Minimally Symptomatic COVID-19 in Singapore. Radiology 2021, 298, E131–E140. [Google Scholar] [CrossRef] [PubMed]
- Chew, K.L.; Tan, S.S.; Saw, S.; Pajarillaga, A.; Zaine, S.; Khoo, C.; Wang, W.; Tambyah, P.; Jureen, R.; Sethi, S.K. Clinical evaluation of serological IgG antibody response on the Abbott Architect for established SARS-CoV-2 infection. Clin. Microbiol. Infect. 2020, 26, 1256.e9–1256.e11. [Google Scholar] [CrossRef]
- Lee, C.Y.-P.; Lin, R.T.P.; Renia, L.; Ng, L.F.P. Serological Approaches for COVID-19: Epidemiologic Perspective on Surveillance and Control. Front. Immunol. 2020, 11, 879. [Google Scholar] [CrossRef] [PubMed]
- Lee, A.J.Y.; Chung, C.L.H.; Young, B.E.; Ling, L.M.; Ho, B.C.H.; Puah, S.H.; Iqbal, S.R.; Tan, G.P. Clinical course and physiotherapy intervention in 9 patients with COVID-19. Physiotherapy 2020, 109, 1–3. [Google Scholar] [CrossRef] [PubMed]
- Ng, Z.; Tay, W.C.; Benjamin Ho, C.H. Awake prone positioning for non-intubated oxygen dependent COVID-19 pneumonia patients. Eur. Respir. J. 2020, 56, 2001198. [Google Scholar] [CrossRef]
- Tay, S.S.; Neo, E.J.; Tan, M.M.; Tan, P.L. Post-Critical Care COVID-19 Patient Benefits from a Robotic Patient-Guided Suspension System for Pulmonary Rehabilitation. Ann. Acad. Med. Singap. 2020, 49, 401–404. [Google Scholar] [CrossRef]
- Fan, B.E.; Ong, K.H.; Chan, S.S.W.; Young, B.E.; Chong, V.C.L.; Chen, S.P.C.; Lim, S.P.; Lim, G.P.; Kuperan, P. Blood and blood product use during COVID-19 infection. Am. J. Hematol. 2020, 95, E158–E160. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Lee, R.M.; Tan, G.P.; Puah, S.H.; Ling, L.M.; Choy, C.Y.; Chotirmall, S.H.; Abisheganaden, J.; See, J.J.; Tan, H.L.; Wong, Y.L. Physiological Changes During Prone Positioning in COVID-19 Acute Respiratory Distress Syndrome. Ann. Acad. Med. Singap. 2020, 49, 509–513. [Google Scholar] [CrossRef] [PubMed]
- Pothiawala, S. An approach to a perceived risk of venous thromboembolism in non-ICU COVID-19 patients in Singapore. Proc. Singap. Healthc. 2020, 30, 56–58. [Google Scholar] [CrossRef]
- Lim, J.K.; Qadri, S.K.; Toh, T.S.; Bin Lin, C.; Mok, Y.H.; Lee, J.H. Extracorporeal Membrane Oxygenation for Severe Respiratory Failure During Respiratory Epidemics and Pandemics: A Narrative Review. Ann. Acad. Med. Singap. 2020, 49, 199–214. [Google Scholar] [CrossRef]
- Chew, S.Y.; Lee, Y.S.; Ghimiray, D.; Tan, C.K.; Chua, G.S.W. Characteristics and Outcomes of COVID-19 Patients with Respiratory Failure Admitted to a "Pandemic Ready" Intensive Care Unit—Lessons from Singapore. Ann. Acad. Med. Singap. 2020, 49, 434–448. [Google Scholar] [CrossRef] [PubMed]
- Goldman, J.D.; Lye, D.C.; Hui, D.S.; Marks, K.M.; Bruno, R.; Montejano, R.; Spinner, C.; Galli, M.; Ahn, M.-Y.; Nahass, R.G.; et al. Remdesivir for 5 or 10 Days in Patients with Severe Covid-19. N. Engl. J. Med. 2020, 383, 1827–1837. [Google Scholar] [CrossRef]
- Wong, J.J.-M.; For the Pediatric Acute & Critical Care Medicine Asian Network (PACCMAN); Liu, S.; Dang, H.; Anantasit, N.; Phan, P.H.; Phumeetham, S.; Qian, S.; Ong, J.S.M.; Gan, C.S.; et al. The impact of high frequency oscillatory ventilation on mortality in paediatric acute respiratory distress syndrome. Crit. Care 2020, 24, 1–10. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Pang, J.; Wang, M.X.; Ang, I.Y.H.; Tan, S.H.X.; Lewis, R.F.; Chen, J.I.-P.; Gutierrez, R.A.; Gwee, S.X.W.; Chua, P.E.Y.; Yang, Q.; et al. Potential Rapid Diagnostics, Vaccine and Therapeutics for 2019 Novel Coronavirus (2019-nCoV): A Systematic Review. J. Clin. Med. 2020, 9, 623. [Google Scholar] [CrossRef] [Green Version]
- Le Bert, N.; Tan, A.T.; Kunasegaran, K.; Tham, C.Y.L.; Hafezi, M.; Chia, A.; Chng, M.H.Y.; Lin, M.; Tan, N.; Linster, M.; et al. SARS-CoV-2-specific T cell immunity in cases of COVID-19 and SARS, and uninfected controls. Nature 2020, 584, 457–462. [Google Scholar] [CrossRef]
- Poh, C.M.; Carissimo, G.; Wang, B.; Amrun, S.N.; Lee, C.Y.; Chee, R.S.; Fong, S.W.; Yeo, N.K.; Lee, W.H.; Torres-Ruesta, A.; et al. Two linear epitopes on the SARS-CoV-2 spike protein that elicit neutralising antibodies in COVID-19 patients. Nat. Commun. 2020, 11, 2806. [Google Scholar] [CrossRef] [PubMed]
- Chan, S.S.W.; Christopher, D.; Tan, G.B.; Chong, V.C.L.; Fan, B.E.; Lin, C.Y.; Ong, K.H. Peripheral lymphocyte subset alterations in COVID-19 patients. Int. J. Lab. Hematol. 2020, 42, e199–e203. [Google Scholar] [CrossRef] [PubMed]
- Tan, C.S.; Yeoh, S.F.; Long, C.M. COVID-19: Critical Role of Angiotensin 1-7 in ACE2 Modulation. Ann. Acad. Med. Singap. 2020, 49, 398–400. [Google Scholar] [CrossRef]
- Tay, M.Z.; Poh, C.M.; Rénia, L.; Macary, P.A.; Ng, L.F.P. The trinity of COVID-19: Immunity, inflammation and intervention. Nat. Rev. Immunol. 2020, 20, 363–374. [Google Scholar] [CrossRef] [PubMed]
- Young, B.E.; Ong, S.W.X.; Ng, L.F.P.; Anderson, D.E.; Chia, W.N.; Chia, P.Y.; Ang, L.W.; Mak, T.M.; Kalimuddin, S.; Chai, L.Y.; et al. Viral dynamics and immune correlates of COVID-19 disease severity. Clin. Infect. Dis. 2020. [Google Scholar] [CrossRef]
- Young, B.E.; Fong, S.-W.; Chan, Y.-H.; Mak, T.-M.; Ang, L.W.; Anderson, D.E.; Lee, C.Y.-P.; Amrun, S.N.; Lee, B.; Goh, Y.S.; et al. Effects of a major deletion in the SARS-CoV-2 genome on the severity of infection and the inflammatory response: An observational cohort study. Lancet 2020, 396, 603–611. [Google Scholar] [CrossRef]
- Lim, T.K. The Facts, Fallacies and Uncertainties about Coronavirus Disease 2019 (COVID-19). Ann. Acad. Med. Singap. 2020, 49, 343–345. [Google Scholar] [CrossRef]
- Wong, S.; Leong, K.; Ng, K.; Tan, S.; Lo, P.; Chan, K. An elderly couple with COVID-19 pneumonia treated in Singapore: Contrasting clinical course and management. Singap. Med. J. 2020, 61, 392–394. [Google Scholar] [CrossRef]
- Ong, J.S.M.; Tosoni, A.; Kim, Y.; Kissoon, N.; Murthy, S. Coronavirus Disease 2019 in Critically Ill Children: A Narrative Review of the Literature*. Pediatr. Crit. Care Med. 2020, 21, 662–666. [Google Scholar] [CrossRef] [PubMed]
- Zhang, J.J.Y.; Lee, K.S.; Ang, L.W.; Leo, Y.S.; Young, B.E. Risk Factors for Severe Disease and Efficacy of Treatment in Patients Infected With COVID-19: A Systematic Review, Meta-Analysis, and Meta-Regression Analysis. Clin. Infect. Dis. 2020, 71, 2199–2206. [Google Scholar] [CrossRef]
- Sun, L.J.; Wong, S.X.L.; Gollamudi, S. A Case of HIV and SARS-CoV-2 Co-infection in Singapore. JAIDS-J. Acquir. Immune Defic. Syndr. 2020, 84, E23–E24. [Google Scholar] [CrossRef]
- Choy, C.Y.; Wong, C.S. SARS-CoV-2 and Advanced HIV Infection. Ann. Acad. Med. Singap. 2020, 49, 1042–1043. [Google Scholar] [CrossRef]
- Fan, B.E.; Lim, K.G.E.; Chong, V.C.L.; Chan, S.S.W.; Ong, K.H.; Kuperan, P. COVID-19 and mycoplasma pneumoniae coinfection. Am. J. Hematol. 2020, 95, 723–724. [Google Scholar] [CrossRef]
- Wong, J.E.L.; Leo, Y.S.; Tan, C.C. COVID-19 in Singapore-Current Experience Critical Global Issues That Require Attention and Action. JAMA-J. Am. Med. Assoc. 2020, 323, 1243–1244. [Google Scholar] [CrossRef] [PubMed]
- Wee, L.E.; Cherng, B.P.Z.; Conceicao, E.P.; Goh, K.C.-M.; Wan, W.Y.; Ko, K.K.K.; Aung, M.K.; Sim, X.Y.J.; Wijaya, L.; Ling, M.L.; et al. Experience of a Tertiary Hospital in Singapore with Management of a Dual Outbreak of COVID-19 and Dengue. Am. J. Trop. Med. Hyg. 2020, 103, 2005–2011. [Google Scholar] [CrossRef] [PubMed]
- Tan, S.H.; Ng, T.M.; Tay, H.L.; Yap, M.Y.; Heng, S.T.; Loo, A.Y.X.; Teng, C.B.; Lee, T.H. A point prevalence survey to assess antibiotic prescribing in patients hospitalized with confirmed and suspected coronavirus disease 2019 (COVID-19). J. Glob. Antimicrob. Resist. 2021, 24, 45–47. [Google Scholar] [CrossRef] [PubMed]
- Tan, S.H.S.; Hong, C.C.; Saha, S.; Murphy, D.; Hui, J.H. Medications in COVID-19 patients: Summarizing the current literature from an orthopaedic perspective. Int. Orthop. 2020, 44, 1599–1603. [Google Scholar] [CrossRef]
- Chotirmall, S.H.; Wang, L.; Abisheganaden, J.A. Letter from Singapore: The clinical and research response to COVID-19. Respirology 2020, 25, 1101–1102. [Google Scholar] [CrossRef]
- Wee, L.E.; Hsieh, J.Y.C.; Phua, G.C.; Tan, Y.; Conceicao, E.P.; Wijaya, L.; Tan, T.T.; Tan, B.H. Respiratory surveillance wards as a strategy to reduce nosocomial transmission of COVID-19 through early detection: The experience of a tertiary-care hospital in Singapore. Infect. Control Hosp. Epidemiol. 2020, 41, 820–825. [Google Scholar] [CrossRef]
- Wee, L.E.; Sim, J.X.Y.; Conceicao, E.P.; Aung, M.K.; Ng, I.M.; Ling, M.L. Re: ’Personal protective equipment protecting healthcare workers in the Chinese epicenter of COVID-19’ by Zhao et al. Clin. Microbiol. Infect. 2020, 26, 1719–1721. [Google Scholar] [CrossRef]
- Wong, L.Y.; Tan, A.L.; Leo, Y.; Lee, V.J.M.; Toh, M.P.H.S. Healthcare workers in Singapore infected with COVID-19: 23 January-17 April. Influ. Other Respir. Viruses 2021, 15, 218–226. [Google Scholar] [CrossRef]
- Ong, J.J.Y.; Bharatendu, C.; Goh, Y.; Tang, J.Z.Y.; Sooi, K.W.X.; Tan, Y.L.; Tan, B.Y.Q.; Teoh, H.L.; Ong, S.T.; Allen, D.M.; et al. Headaches Associated with Personal Protective Equipment – A Cross-Sectional Study Among Frontline Healthcare Workers During COVID-19. Headache J. Head Face Pain 2020, 60, 864–877. [Google Scholar] [CrossRef] [Green Version]
- Seah, I.; Su, X.; Lingam, G. Revisiting the dangers of the coronavirus in the ophthalmology practice. Eye 2020, 34, 1155–1157. [Google Scholar] [CrossRef] [Green Version]
- Tan, G.S.E.; Linn, K.Z.; Soon, M.M.L.; Vasoo, S.; Chan, M.; Poh, B.F.; Ng, O.-T.; Ang, B.S.-P.; Leo, Y.-S.; Marimuthu, K. Effect of extended use N95 respirators and eye protection on personal protective equipment (PPE) utilization during SARS-CoV-2 outbreak in Singapore. Antimicrob. Resist. Infect. Control 2020, 9, 86. [Google Scholar] [CrossRef]
- Chua, J.X.; Ong, L.; Tan, C.H. Innovative Face Shields Help Frontliners Face-off COVID-19 Pandemic. Ann. Acad. Med. Singap. 2020, 49, 1044–1047. [Google Scholar] [CrossRef]
- Gan, W.H.; Lim, J.W.; Koh, D. Preventing Intra-hospital Infection and Transmission of Coronavirus Disease 2019 in Health-care Workers. Saf. Health Work. 2020, 11, 241–243. [Google Scholar] [CrossRef]
- Wee, L.E.; Sim, X.Y.J.; Conceicao, E.P.; Aung, M.K.; Goh, J.Q.; Yeo, D.W.T.; Gan, W.H.; Chua, Y.Y.; Wijaya, L.; Tan, T.T.; et al. Containment of COVID-19 cases among healthcare workers: The role of surveillance, early detection, and outbreak management. Infect. Control Hosp. Epidemiol. 2020, 41, 765–771. [Google Scholar] [CrossRef] [PubMed]
- Lee, H.C.; Goh, C.L. Occupational dermatoses from Personal Protective Equipment during the COVID-19 pandemic in the tropics—A Review. J. Eur. Acad. Dermatol. Venereol. 2020, 35, 589–596. [Google Scholar] [CrossRef] [PubMed]
- Tan, S.W.; Oh, C.C. Contact Dermatitis from Hand Hygiene Practices in the COVID-19 Pandemic. Ann. Acad. Med. Singap. 2020, 49, 674–676. [Google Scholar] [CrossRef]
- Zihui, T.; Deborah Wen Shi, K.; Ling Antonia, Z.; Jong-Chie Claudia, T.; Aaron Kwang Yang, L.; Yee Yian, O.; Miqi Mavis, T.; Hairil Rizal, A.; Tan, Z.; Khoo, D.W.S.; et al. Protecting health care workers in the front line: Innovation in COVID-19 pandemic. J. Glob. Health 2020, 10, 010357. [Google Scholar]
- Rajamani, A.; Subramaniam, A.; Shekar, K.; Haji, J.; Luo, J.; Bihari, S.; Wong, W.T.; Gullapalli, N.; Renner, M.; Alcancia, C.M.; et al. Personal protective equipment preparedness in Asia-Pacific intensive care units during the coronavirus disease 2019 pandemic: A multinational survey. Aust. Crit. Care 2021, 34, 135–141. [Google Scholar] [CrossRef]
- Htun, H.L.; Lim, D.W.; Kyaw, W.M.; Loh, W.-N.J.; Lee, L.T.; Ang, B.; Chow, A. Responding to the COVID-19 Outbreak in Singapore: Staff Protection and Staff Temperature and Sickness Surveillance Systems. Clin. Infect. Dis. 2020, 71, 1947–1952. [Google Scholar] [CrossRef]
- Ng, Y.; Li, Z.; Chua, Y.X.; Chaw, W.L.; Zhao, Z.; Er, B.; Pung, R.; Chiew, C.J.; Lye, D.; Heng, D.; et al. Evaluation of the Effectiveness of Surveillance and Containment Measures for the First 100 Patients with COVID-19 in Singapore—January 2–February 29. MMWR Morb. Mortal. Wkly. Rep. 2020, 69, 307–311. [Google Scholar] [CrossRef] [PubMed]
- Teo, W.-Y. Implications for border containment strategies when COVID-19 presents atypically. Public Health 2020, 186, 193–196. [Google Scholar] [CrossRef]
- Dickens, B.L.; Koo, J.R.; Lim, J.T.; Park, M.; Quaye, S.; Sun, H.; Sun, Y.; Pung, R.; Wilder-Smith, A.; Chai, L.Y.A. Modelling lockdown and exit strategies for COVID-19 in Singapore. Lancet Reg. Health-West. Pac. 2020, 1, 100004. [Google Scholar] [CrossRef]
- Koo, J.R.; Cook, A.R.; Park, M.; Sun, Y.X.H.; Sun, H.Y.; Lim, J.T. Interventions to mitigate early spread of SARS-CoV-2 in Singapore: A modelling study. Lancet Infect. Dis. 2020, 20, 678–688. [Google Scholar] [CrossRef] [Green Version]
- Han, E.; Tan, M.M.J.; Turk, E.; Sridhar, D.; Leung, G.M.; Shibuya, K.; Asgari, N.; Oh, J.; García-Basteiro, A.L.; Hanefeld, J.; et al. Lessons learnt from easing COVID-19 restrictions: An analysis of countries and regions in Asia Pacific and Europe. Lancet 2020, 396, 1525–1534. [Google Scholar] [CrossRef]
- Lee, V.J.; Chiew, C.J.; Khong, W.X. Interrupting transmission of COVID-19: Lessons from containment efforts in Singapore. J. Travel Med. 2020, 27. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Ng, W.T. COVID-19: Protection of Workers at the Workplace in Singapore. Saf. Health Work. 2021, 12, 133–135. [Google Scholar] [CrossRef]
- Chiew, C.J.; Li, Z.; Lee, V.J. Reducing onward spread of COVID-19 from imported cases: Quarantine and ‘stay at home’ measures for travellers and returning residents to Singapore. J. Travel Med. 2020, 27, taaa049. [Google Scholar] [CrossRef] [Green Version]
- Lee, W.C.; Ong, C.Y. Overview of rapid mitigating strategies in Singapore during the COVID-19 pandemic. Public Health 2020, 185, 15–17. [Google Scholar] [CrossRef]
- Chia, M.L.; Chau, D.H.H.; Lim, K.S.; Liu, C.W.Y.; Tan, H.K.; Tan, Y.R. Managing COVID-19 in a Novel, Rapidly Deployable Community Isolation Quarantine Facility. Ann. Intern. Med. 2021, 174, 247–251. [Google Scholar] [CrossRef]
- Lee, G.L.; Lee, W.T.; Kok, W.L. Deployment of a Forward Medical Post to Provide Medical Support in a Purpose-built Dormitory during the COVID-19 Pandemic. Ann. Acad. Med. Singap. 2020, 49, 928–930. [Google Scholar] [CrossRef]
- Pung, R.; Park, M.; Cook, A.R.; Lee, V.J. Age-related risk of household transmission of COVID-19 in Singapore. Influenza Other Respir. Viruses 2020, 15, 206–208. [Google Scholar] [CrossRef]
- de Souza, T.H.; Lanziotti, V.S.; Lee, J.H. COVID-19 and Children: Many Questions Yet to Be Answered. Ann. Acad. Med. Singap. 2020, 49, 527–529. [Google Scholar] [CrossRef]
- Bagdasarian, N.; Fisher, D. Heterogenous COVID-19 transmission dynamics within Singapore: A clearer picture of future national responses. BMC Med. 2020, 18, 164. [Google Scholar] [CrossRef]
- Yung, C.F.; Kam, K.-Q.; Chong, C.Y.; Nadua, K.D.; Li, J.; Tan, N.W.H.; Ganapathy, S.; Lee, K.P.; Ng, K.C.; Chan, Y.H.; et al. Household Transmission of Severe Acute Respiratory Syndrome Coronavirus 2 from Adults to Children. J. Pediatr. 2020, 225, 249–251. [Google Scholar] [CrossRef]
- Ng, O.-T.; Marimuthu, K.; Chia, P.-Y.; Koh, V.; Chiew, C.J.; De Wang, L.; Young, B.E.; Chan, M.; Vasoo, S.; Ling, L.M.; et al. SARS-CoV-2 Infection among Travelers Returning from Wuhan, China. N. Engl. J. Med. 2020, 382, 1476–1478. [Google Scholar] [CrossRef] [Green Version]
- Ng, O.T.; Marimuthu, K.; Koh, V.; Pang, J.; Linn, K.Z.; Sun, J.; De Wang, L.; Chia, W.N.; Tiu, C.; Chan, M.; et al. SARS-CoV-2 seroprevalence and transmission risk factors among high-risk close contacts: A retrospective cohort study. Lancet Infect. Dis. 2020, 21. [Google Scholar] [CrossRef]
- Li, J.H.; Thoon, K.C.; Chong, C.Y.; Maiwald, M.; Kam, K.Q.; Nadua, K.; Tan, N.W.; Yung, C.F. Comparative Analysis of Symptomatic and Asymptomatic SARS-CoV-2 Infection in Children. Ann. Acad. Med. Singap. 2020, 49, 530–537. [Google Scholar] [CrossRef]
- Yeung, W.; Ng, K.; Fong, J.M.N.; Sng, J.; Tai, B.C.; Chia, S.E. Assessment of Proficiency of N95 Mask Donning Among the General Public in Singapore. JAMA Netw. Open 2020, 3, e209670. [Google Scholar] [CrossRef]
- Wei, W.E.; Li, Z.; Chiew, C.J.; Yong, S.E.; Toh, M.P.; Lee, V.J. Presymptomatic transmission of SARS-CoV-2—Singapore, January 23–March 16. Morb. Mortal. Wkly. Rep. 2020, 69, 411–415. [Google Scholar] [CrossRef] [Green Version]
- Yong, S.E.F.; Anderson, D.E.; Wei, W.; Pang, J.; Ni Chia, W.; Tan, C.W.; Teoh, Y.L.; Rajendram, P.; Toh, M.P.H.S.; Poh, C.; et al. Connecting clusters of COVID-19: An epidemiological and serological investigation. Lancet Infect. Dis. 2020, 20, 809–815. [Google Scholar] [CrossRef]
- Tan, L.F.; Seetharaman, S.K. COVID-19 outbreak in nursing homes in Singapore. J. Microbiol. Immunol. Infect. 2021, 54, 123–124. [Google Scholar] [CrossRef]
- Pung, R.; Chiew, C.J.; Young, B.E.; Chin, S.; Chen, M.I.; Clapham, H.E.; Cook, A.R.; Maurer-Stroh, S.; Toh, M.P.H.S.; Poh, C.; et al. Investigation of three clusters of COVID-19 in Singapore: Implications for surveillance and response measures. Lancet 2020, 395, 1039–1046. [Google Scholar] [CrossRef]
- Gorny, A.W.; Bagdasarian, N.; Koh, A.H.K.; Lim, Y.C.; Ong, J.S.M.; Ng, B.S.W.; Hooi, B.; Tam, W.J.; Kagda, F.H.; Chua, G.S.W.; et al. SARS-CoV-2 in migrant worker dormitories: Geospatial epidemiology supporting outbreak management. Int. J. Infect. Dis. 2021, 103, 389–394. [Google Scholar] [CrossRef]
- Ho, H.J.; Zhang, Z.X.; Huang, Z.; Aung, A.H.; Lim, W.-Y.; Chow, A. Use of a Real-Time Locating System for Contact Tracing of Health Care Workers During the COVID-19 Pandemic at an Infectious Disease Center in Singapore: Validation Study. J. Med. Internet Res. 2020, 22, e19437. [Google Scholar] [CrossRef] [PubMed]
- Saw, Y.E.; Tan, E.Y.; Liu, J.S.; Liu, J. Predicting public take-up of digital contact tracing during the COVID-19 crisis: Results of a national survey in Singapore. J. Med. Internet Res. 2021, 15, 15. [Google Scholar]
- Huang, Z.; Guo, H.; Lee, Y.-M.; Ho, E.C.; Ang, H.; Chow, A. Performance of Digital Contact Tracing Tools for COVID-19 Response in Singapore: Cross-Sectional Study. JMIR mHealth uHealth 2020, 8, e23148. [Google Scholar] [CrossRef]
- Huang, Z.; Guo, H.; Lim, H.Y.; Chow, A. Awareness, acceptance, and adoption of the national digital contact tracing tool post COVID-19 lockdown among visitors to a public hospital in Singapore. Clin. Microbiol. Infect. 2021, 19, 1046–1048. [Google Scholar] [CrossRef]
- Lai, S.H.S.; Tang, C.Q.Y.; Kurup, A.; Thevendran, G. The experience of contact tracing in Singapore in the control of COVID-19: Highlighting the use of digital technology. Int. Orthop. 2021, 45, 65–69. [Google Scholar] [CrossRef] [PubMed]
- Goggin, G. COVID-19 apps in Singapore and Australia: Reimagining healthy nations with digital technology. Media Int. Aust. 2020, 177, 61–75. [Google Scholar] [CrossRef]
- Koh, D.; Cunningham, A.C. Counting Coronavirus Disease 2019 (COVID-19) Cases: Case Definitions, Screened Populations and Testing Techniques Matter. Ann. Acad. Med. Singap 2020, 49, 161–165. [Google Scholar] [CrossRef]
- Lee, T.H.; Junhao Lin, R.; Lin, R.T.P.; Barkham, T.; Rao, P.; Leo, Y.S.; Chien Lye, D.; Young, B. Testing for SARS-CoV-2: Can We Stop at 2? Clin. Infect. Dis. 2020, 71, 2246–2248. [Google Scholar] [CrossRef] [PubMed]
- Huang, W.; Chai, G.T.; Thong, Y.H.B.; Chan, P.C.M.; Ang, S.P.B.; Chow, L.P.A. Pneumonia surveillance and its attendant clinical risk stratification for COVID-19 in low-risk patients. Public Health 2021, 190, 89–92. [Google Scholar] [CrossRef]
- Shanker, S.; Chia, D.W.J.; Ganti, S. Difficulties faced by a medical team based at a COVID-19 quarantine facility. Singap. Med. J. 2020. [Google Scholar] [CrossRef] [PubMed]
- Lim, J.T.; Dickens, B.L.; Cook, A.R.; Khoo, A.L.; Dan, Y.Y.; Fisher, D.A.; Tambyah, P.A.; Chai, L.Y.A. The costs of an expanded screening criteria for COVID-19: A modelling study. Int. J. Infect. Dis. 2020, 100, 490–496. [Google Scholar] [CrossRef] [PubMed]
- Koon, O.E. The Impact of Sociocultural Influences on the COVID-19 Measures—Reflections From Singapore. J. Pain Symptom Manag. 2020, 60, e90–e92. [Google Scholar] [CrossRef]
- Ozdemir, S.; Ng, S.; Chaudhry, I.; Finkelstein, E.A. Adoption of Preventive Behaviour Strategies and Public Perceptions about COVID-19 in Singapore. Int. J. Health Policy Manag. 2020. [Google Scholar] [CrossRef]
- Long, V.; Tan, B.Y.S.; Tan, L.F. Knowledge and Perceptions of COVID-19 among the General Public in Singapore: A Cross-sectional Online Survey. Ann. Acad. Med. Singap. 2020, 49, 1048–1051. [Google Scholar] [CrossRef]
- Sun, H.; Dickens, B.L.; Cook, A.; Clapham, H.E. Importations of COVID-19 into African countries and risk of onward spread. BMC Infect. Dis. 2020, 20, 1–13. [Google Scholar] [CrossRef]
- Pung, R.; Cook, A.R.; Chiew, C.J.; Clapham, H.E.; Sun, Y.; Li, Z.; Dickens, B.L.; Ma, S.; Mak, K.; Tan, C.C.; et al. Effectiveness of Containment Measures Against COVID-19 in Singapore: Implications for Other National Containment Efforts. Epidemiology 2021, 32, 79–86. [Google Scholar] [CrossRef]
- Yung, C.F.; Saffari, E.; Liew, C. Time to Rt <1 for COVID-19 public health lockdown measures. Epidemiol. Infect. 2020, 148, 1–8. [Google Scholar] [CrossRef]
- Goei, A.; Tiruchittampalam, M. Community care facility-a novel concept to deal with the Covid-19 pandemic: A Singaporean institution’s experience. J. Public Health Manag. Pract. 2020, 26, 613–621. [Google Scholar] [CrossRef]
- Soh, E.F. Building for the Known Unknown-Development of the National Centre for Infectious Diseases. Ann. Acad. Med. Singap. 2020, 49, 582–587. [Google Scholar] [CrossRef]
- Toyoda, H.; Huang, D.Q.; Le, M.; Nguyen, M.H. Liver Care and Surveillance: The Global Impact of the COVID-19 Pandemic. Hepatol. Commun. 2020, 4, 1751–1757. [Google Scholar] [CrossRef]
- Yeo, T.J.; Wang, Y.-T.L.; Low, T.T. Have a heart during the COVID-19 crisis: Making the case for cardiac rehabilitation in the face of an ongoing pandemic. Eur. J. Prev. Cardiol. 2020, 27, 903–905. [Google Scholar] [CrossRef] [Green Version]
- Ho, J.S.Y.; Tambyah, P.A.; Sia, C.-H. A Call for Vaccine Against COVID-19: Implications for Cardiovascular Morbidity and Healthcare Utilization. Cardiovasc. Drugs Ther. 2020, 34, 585–587. [Google Scholar] [CrossRef]
- Wee, L.E.; Conceicao, E.P.; Tan, J.Y.; Chan, L.L.-H.; Phoon, P.C.; Sim, X.Y.J.; Venkatachalam, I. Reduction in heart failure admissions with concomitant respiratory viral infections during the novel coronavirus disease-2019 pandemic: Unintended consequence of public health measures in Singapore. J. Card. Fail. 2021, 27, 117–119. [Google Scholar] [CrossRef]
- Lim, S.L.; Woo, K.L.; Lim, E.; Ng, F.; Chan, M.Y.; Gandhi, M. Impact of COVID-19 on health-related quality of life in patients with cardiovascular disease: A multi-ethnic Asian study. Health Qual. Life Outcomes 2020, 18, 1–7. [Google Scholar] [CrossRef]
- Chew, N.W.; Sia, C.-H.; Wee, H.-L.; Benedict, L.J.-D.; Rastogi, S.; Kojodjojo, P.; Chor, W.P.D.; Leong, B.S.-H.; Koh, B.C.-P.; Tam, H.; et al. Impact of the COVID-19 Pandemic on Door-to-Balloon Time for Primary Percutaneous Coronary Intervention—Results from the Singapore Western STEMI Network. Circ. J. 2021, 85, 139–149. [Google Scholar] [CrossRef]
- Malhotra, C.; Chaudhry, I.; Ozdemir, S.; Finkelstein, E.A. Reduced health-care utilization among people with chronic medical conditions during coronavirus disease 2019. Proc. Singap. Healthc. 2020. [Google Scholar] [CrossRef]
- Ho, J.S.; I Fernando, D.; Chan, M.Y.; Sia, C.-H. Obesity in COVID-19: A Systematic Review and Meta-analysis. Ann. Acad. Med. Singap. 2020, 49, 996–1008. [Google Scholar] [CrossRef]
- Chang, P.; Wong, Y.-J.; Yang, W.; Lim, K.; Tan, P.; Ho, G.; Yip, B.; Li, J.; Chong, C.; Ong, D.; et al. Chapter of Gastroenterologists professional guidance for management of patients with liver disease in Singapore during the COVID-19 pandemic. Singap. Med. J. 2020, 61, 619–623. [Google Scholar] [CrossRef]
- Cheong, C.Y.; Yap, P.L.K. Timely Reminders from COVID-19 for Dementia Care. Ann. Acad. Med. Singap. 2020, 49, 801–803. [Google Scholar] [CrossRef]
- Lim, W.S.; Liang, C.; Assantachai, P.; Auyeung, T.W.; Kang, L.; Lee, W.; Lim, J.-Y.; Sugimoto, K.; Akishita, M.; Chia, S.; et al. COVID-19 and older people in Asia: Asian Working Group for Sarcopenia calls to action. Geriatr. Gerontol. Int. 2020, 20, 547–558. [Google Scholar] [CrossRef]
- Rais, N.C.; Au, L.; Tan, M. COVID-19 Impact in Community Care—A Perspective on Older Persons with Dementia in Singapore. J. Am. Med. Dir. Assoc. 2020, 21, 997. [Google Scholar] [CrossRef]
- Chow, A.; Hein, A.A.; Kyaw, W.M. Unintended Consequence: Influenza plunges with public health response to COVID-19 in Singapore. J. Infect. 2020, 81, e68–e69. [Google Scholar] [CrossRef]
- Wee, L.E.I.; Conceicao, E.P.; Tan, J.Y.; Magesparan, K.D.; Amin, I.B.M.; Ismail, B.B.S.; Toh, H.X.; Jin, P.; Zhang, J.; Wee, E.G.L.; et al. Unintended consequences of infection prevention and control measures during COVID-19 pandemic. Am. J. Infect. Control 2021, 49, 469–477. [Google Scholar] [CrossRef]
- Tham, S.M.; Lim, W.Y.; Lee, C.K.; Loh, J.; Premkumar, A.; Yan, B.; Kee, A.; Chai, L.; Tambyah, P.A.; Yan, G. Four Patients with COVID-19 and Tuberculosis, Singapore, April–May 2020. Emerg. Infect. Dis. 2020, 26, 2763–2765. [Google Scholar] [CrossRef]
- Wee, L.E.; Conceicao, E.P.; Sim, J.X.-Y.; Aung, M.K.; Venkatachalam, I. The impact of visitor restrictions on health care-associated respiratory viral infections during the COVID-19 pandemic: Experience of a tertiary hospital in Singapore. Am. J. Infect. Control 2021, 49, 134–135. [Google Scholar] [CrossRef]
- Wee, L.E.; Conceicao, E.P.; Sim, J.X.Y.; Aung, M.K.; Venkatachalam, I. Impact of infection prevention precautions on adenoviral infections during the COVID-19 pandemic: Experience of a tertiary hospital in Singapore. Infect. Control. Hosp. Epidemiol. 2020, 1–9, 969944. [Google Scholar] [CrossRef]
- Lim, R.H.; Chow, A.; Ho, H.J. Decline in pneumococcal disease incidence in the time of COVID-19 in Singapore. J. Infect. 2020, 81, e19–e21. [Google Scholar] [CrossRef] [PubMed]
- Tan, J.; Conceicao, E.; Sim, X.; Wee, L.; Aung, M.; Venkatachalam, I. Public health measures during COVID-19 pandemic reduced hospital admissions for community respiratory viral infections. J. Hosp. Infect. 2020, 106, 387–389. [Google Scholar] [CrossRef] [PubMed]
- Liew, Y.; Lee, W.H.L.; Tan, L.; Kwa, A.L.H.; Thien, S.Y.; Cherng, B.P.Z.; Chung, S.J. Antimicrobial stewardship programme: A vital resource for hospitals during the global outbreak of coronavirus disease 2019 (COVID-19). Int. J. Antimicrob. Agents 2020, 56, 106145. [Google Scholar] [CrossRef]
- Lim, J.T.; Dickens, B.S.L.; Chew, L.Z.X.; Choo, E.L.W.; Koo, J.R.; Aik, J.; Ng, L.C.; Cook, A.R. Impact of sars-cov-2 interventions on dengue transmission. PLOS Negl. Trop. Dis. 2020, 14, e0008719. [Google Scholar] [CrossRef]
- Wee, L.E.; Ko, K.K.K.; Ho, W.Q.; Kwek, G.T.C.; Tan, T.T.; Wijaya, L. Community-acquired viral respiratory infections amongst hospitalized inpatients during a COVID-19 outbreak in Singapore: Co-infection and clinical outcomes. J. Clin. Virol. 2020, 128, 104436. [Google Scholar] [CrossRef]
- Wee, L.; Conceicao, E.; Tan, J.; Venkatachalam, I.; Ling, M. Zero healthcare-associated respiratory viral infections among haematology inpatients: Unexpected consequence of heightened infection control during COVID-19 outbreak. J. Hosp. Infect. 2021, 107, 1–4. [Google Scholar] [CrossRef]
- Paliwal, P.R.; Tan, B.Y.Q.; Leow, A.S.T.; Sibi, S.; Chor, D.W.P.; Chin, A.X.Y.; Yau, Y.-W.; Cross, G.B.; Wong, L.Y.H.; Chia, M.L.J.; et al. Impact of the COVID-19 pandemic on hyperacute stroke treatment: Experience from a comprehensive stroke centre in Singapore. J. Thromb. Thrombolysis 2020, 50, 596–603. [Google Scholar] [CrossRef]
- Riandini, T.; Tan, K.B.; De Silva, D.A. Lessons from Severe Acute Respiratory Syndrome Coronavirus 2003 Pandemic as Evidence to Advocate for Stroke Public Education During the Current Coronavirus Disease 2019 Pandemic. Ann. Acad. Med. Singap. 2020, 49, 538–542. [Google Scholar] [CrossRef]
- Singh, T.; Ngoh, C.L.Y.; Wong, W.K.; Khan, B.A. Impact of Telemedicine on Hospitalisation and Mortality Rates in Community-Based Haemodialysis Centres in Singapore during the COVID-19 Pandemic. Ann. Acad. Med. Singap. 2020, 49, 756–763. [Google Scholar] [CrossRef]
- Wee, L.; Conceicao, E.; Sim, X.; Ko, K.; Ling, M.; Venkatachalam, I. Reduction in healthcare-associated respiratory viral infections during a COVID-19 outbreak. Clin. Microbiol. Infect. 2020, 26, 1579–1581. [Google Scholar] [CrossRef] [PubMed]
- Soo, R.J.J.; Chiew, C.J.; Ma, S.; Pung, R.; Lee, V. Decreased Influenza Incidence under COVID-19 Control Measures, Singapore. Emerg. Infect. Dis. 2020, 26, 1933–1935. [Google Scholar] [CrossRef]
- Chan, D.K.H.; Keh, C.H.L.; Seow, C.S.; Iau, P.T.C. Maintaining quality of care in colorectal cancer surgery during the COVID-19 pandemic. BJS 2020, 107, e422–e423. [Google Scholar] [CrossRef]
- Chia, C.L.K.; Oh, H.B.; Kabir, T.; Tan, Y.P.; Thiruchelvam, N.; Pang, N.Q.; Chan, K.S.; Koh, Y.X. Impact of COVID-19 Pandemic on Management of Acute Cholecystitis in Singapore. Ann. Acad. Med. Singap. 2020, 49, 817–824. [Google Scholar] [CrossRef]
- Yeo, K.T.; Oei, J.L.; De Luca, D.; Schmölzer, G.M.; Guaran, R.; Palasanthiran, P.; Kumar, K.; Buonocore, G.; Cheong, J.; Owen, L.S.; et al. Review of guidelines and recommendations from 17 countries highlights the challenges that clinicians face caring for neonates born to mothers with COVID-19. Acta Paediatr. 2020, 109, 2192–2207. [Google Scholar] [CrossRef]
- Mattar, C.N.Z.; Kalimuddin, S.; Sadarangani, S.P.; Tagore, S.; Thain, S.; Thoon, K.C.; Hong, E.Y.; Kanneganti, A.; Ku, C.W.; Chan, G.M.F.; et al. Pregnancy Outcomes in COVID-19: A Prospective Cohort Study in Singapore. Ann. Acad. Med. Singap. 2020, 49, 857–869. [Google Scholar] [CrossRef]
- Wong, K.C.; Cheok, J.W.G.; Tay, K.; Koh, S.B.; Howe, T.S. Where have all the hip fractures gone? Osteoporos. Int. 2020, 31, 2057–2058. [Google Scholar] [CrossRef] [PubMed]
- Ding, B.T.K.; Ng, J.; Tan, K.G. Enhanced Recovery after Surgery for Knee Arthroplasty in the Era of COVID-19. J. Knee Surg. 2020. [Google Scholar] [CrossRef]
- Tan, E.K.; Koh, Y.X.; Kee, T.; Juhari, J.B.; Tan, T.E.; Sim, D.K.L.; Ho, A.Y.L.; Krishnan, L.; Tee, P.S.; Krishnamoorthy, T.L.; et al. Waitlisted Transplant Candidates’ Attitudes and Concerns Toward Transplantation During COVID-19. Ann. Transplant. 2020, 25, 1–12. [Google Scholar] [CrossRef] [PubMed]
- Lim, T.; Tan, M.Y.; Aishworiya, R.; Kang, Y.Q. Autism Spectrum Disorder and COVID-19: Helping Caregivers Navigate the Pandemic. Ann. Acad. Med. Singap. 2020, 49, 384–386. [Google Scholar] [CrossRef]
- Yung, C.F.; Nadua, K.D.; Oh, B.K.; Thoon, K.C. Epidemiological trends in Kawasaki disease during COVID-19 in Singapore. J. Pediatrics 2020, 226, 314–315. [Google Scholar] [CrossRef] [PubMed]
- Zhong, Y.; Clapham, H.E.; Aishworiya, R.; Chua, Y.X.; Mathews, J.; Ong, M.; Wang, J.; Murugasu, B.; Chiang, W.C.; Lee, B.W.; et al. Childhood vaccinations: Hidden impact of COVID-19 on children in Singapore. Vaccine 2021, 39, 780–785. [Google Scholar] [CrossRef] [PubMed]
- Chong, S.-L.; Soo, J.S.L.; Ganapathy, S.; Lee, K.P.; Tyebally, A.; Yung, C.F.; Thoon, K.C.; Ng, Y.H.; Oh, J.Y. Impact of COVID-19 on pediatric emergencies and hospitalizations in Singapore. BMC Pediatr. 2020, 20, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Wong, F.P.Y.; Wong, J.L.J.; Mok, Y.M.; Chandwani, N. Adapting and Delivering Care during the COVID-19 Pandemic: Staff Diary from the Mood Disorders Unit in Singapore. Ann. Acad. Med. Singap. 2020, 49, 804–806. [Google Scholar] [CrossRef]
- How, G.Y.; Pua, U. Trends of interventional radiology procedures during the COVID-19 pandemic: The first 27 weeks in the eye of the storm. Insights Imaging 2020, 11, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Lateef, F. The impact of the COVID 19 pandemic on emergency department attendance: What seems to be keeping the patients away? J. Emergencies Trauma Shock 2020, 13, 246. [Google Scholar] [CrossRef]
- Chan, D.X.; Lin, X.F.; George, J.M.; Liu, C.W. Clinical Challenges and Considerations in Management of Chronic Pain Patients During a COVID-19 Pandemic. Ann. Acad. Med. Singap. 2020, 49, 669–673. [Google Scholar] [CrossRef]
- Tan, B.Y.; Kanneganti, A.; Lim, L.J.; Tan, M.; Chua, Y.X.; Tan, L.; Sia, C.H.; Denning, M.; Goh, E.T.; Purkayastha, S.; et al. Burnout and Associated Factors Among Health Care Workers in Singapore During the COVID-19 Pandemic. J. Am. Med. Dir. Assoc. 2020, 21, 1751–1758.e5. [Google Scholar] [CrossRef]
- Teo, W.Z.Y.; Soo, Y.E.; Yip, C.; Lizhen, O.; Chun-Tsu, L. The psychological impact of COVID-19 on ’hidden’ frontline healthcare workers. Int. J. Soc. Psychiatry 2020, 11, 20764020950772. [Google Scholar] [CrossRef]
- Lee, J.; Venugopal, V.; Latha, P.; Alhadad, S.; Leow, C.; Goh, N.; Tan, E.; Kjellstrom, T.; Morabito, M.; Lee, J. Heat Stress and Thermal Perception amongst Healthcare Workers during the COVID-19 Pandemic in India and Singapore. Int. J. Environ. Res. Public Health 2020, 17, 8100. [Google Scholar] [CrossRef] [PubMed]
- Wong, K.C.; Han, X.A.; Tay, K.S.; Koh, S.B.; Howe, T.S. The psychological impact on an orthopaedic outpatient setting in the early phase of the COVID-19 pandemic: A cross-sectional study. J. Orthop. Surg. Res. 2020, 15, 1–7. [Google Scholar] [CrossRef]
- Lau, J.; Tan, D.H.-Y.; Wong, G.J.; Lew, Y.-J.; Chua, Y.-X.; Low, L.-L.; Ho, H.-K.; Kwek, T.-S.; Toh, S.-A.E.-S.; Tan, K.-K. Prepared and highly committed despite the risk of COVID-19 infection: A cross-sectional survey of primary care physicians’ concerns and coping strategies in Singapore. BMC Fam. Pract. 2021, 22, 1–9. [Google Scholar] [CrossRef]
- Ng, K.Y.Y.; Zhou, S.; Tan, S.H.; Ishak, N.D.B.; Goh, Z.Z.S.; Chua, Z.Y.; Chia, J.M.X.; Chew, E.L.; Shwe, T.; Mok, J.K.Y.; et al. Understanding the Psychological Impact of COVID-19 Pandemic on Patients with Cancer, Their Caregivers, and Health Care Workers in Singapore. JCO Glob. Oncol. 2020, 6, 1494–1509. [Google Scholar] [CrossRef]
- Goh, Y.; Yong, Q.Y.J.O.; Chen, T.H.; Ho, S.H.C.; Chee, Y.I.C.; Chee, T.T. The Impact of COVID-19 on nurses working in a University Health System in Singapore: A qualitative descriptive study. Int. J. Ment. Health Nurs. 2021, 30, 643–652. [Google Scholar] [CrossRef]
- Lee, M.C.; Thampi, S.; Chan, H.P.; Khoo, D.; Chin, B.Z.; Foo, D.P.; Lua, C.B.; Lewin, B.; Jacob, R. Psychological distress during the COVID-19 pandemic amongst anaesthesiologists and nurses. Br. J. Anaesth. 2020, 125, e384–e386. [Google Scholar] [CrossRef] [PubMed]
- Chew, Q.H.; Chia, F.L.-A.; Ng, W.K.; Lee, W.C.I.; Tan, P.L.L.; Wong, C.S.; Puah, S.H.; Shelat, V.; Seah, E.-J.D.; Huey, C.W.T.; et al. Psychological and coping responses to COVID-19 amongst residents in training across ACGME-I accredited specialties in Singapore. Psychiatry Res. 2020, 290, 113146. [Google Scholar] [CrossRef] [PubMed]
- Seow, J.W.; Lin, S.; Khor, Y.P.; Hey, D.H.; Kagda, F.H. Stress and Strain in an Orthopaedic Department on the Frontlines during the COVID-19 Pandemic: An Analysis of Burnout and the Factors Influencing It. Ann. Acad. Med. Singap. 2020, 49, 814–816. [Google Scholar] [CrossRef]
- Tan, Y.Q.; Chan, M.T.; Chiong, E. Psychological health among surgical providers during the COVID-19 pandemic: A call to action. BJS 2020, 107, e459–e460. [Google Scholar] [CrossRef]
- Goh, S.S.N.; Chia, M.Y.C. Anxiety and Morale in Front-Line Healthcare Workers During the Coronavirus Disease 2019 (COVID-19) Outbreak at the National Screening Centre in Singapore. Ann. Acad. Med. Singap. 2020, 49, 259–262. [Google Scholar] [CrossRef]
- Ng, Q.X.; De Deyn, M.L.Z.Q.; Lim, D.Y.; Chan, H.W.; Yeo, W.S. The wounded healer: A narrative review of the mental health effects of the COVID-19 pandemic on healthcare workers. Asian J. Psychiatry 2020, 54, 102258. [Google Scholar] [CrossRef]
- Lim, W.P.; Seet, X.Y.; Rahman, H. Designing a psychological preparedness toolkit for healthcare workers in the wake of COVID-19: A Singapore perspective. Asian J. Psychiatry 2020, 53, 102204. [Google Scholar] [CrossRef]
- Tng, J.; Chew, Q.H.; Sim, K. Psychological sequelae within different populations during the COVID-19 pandemic: A rapid review of extant evidence. Singap. Med. J. 2020. [Google Scholar] [CrossRef]
- Chew, N.W.S.; Lee, G.K.H.; Tan, B.Y.Q.; Jing, M.; Goh, Y.; Ngiam, N.J.H.; Yeo, L.L.L.; Ahmad, A.; Ahmed Khan, F.; Napolean Shanmugam, G.; et al. A multinational, multicentre study on the psychological outcomes and associated physical symptoms amongst healthcare workers during COVID-19 outbreak. Brain Behav. Immun. 2020, 88, 559–565. [Google Scholar] [CrossRef]
- Tan, B.; Chew, N.W.; Lee, G.K.; Jing, M.; Goh, Y.; Yeo, L.L.; Zhang, K.; Chin, H.-K.; Ahmad, A.; Khan, F.A.; et al. Psychological Impact of the COVID-19 Pandemic on Health Care Workers in Singapore. Ann. Intern. Med. 2020, 173, 317–320. [Google Scholar] [CrossRef] [Green Version]
- Yong, L.M.O.; Xin, X.; Wee, J.M.L.; Poopalalingam, R.; Kwek, K.Y.C.; Thumboo, J. Perception survey of crisis and emergency risk communication in an acute hospital in the management of COVID-19 pandemic in Singapore. BMC Public Health 2020, 20, 1–12. [Google Scholar] [CrossRef]
- Ng, Q.X.; Chee, K.T.; De Deyn, M.L.Z.Q.; Chua, Z. Staying connected during the COVID-19 pandemic. Int. J. Soc. Psychiatry 2020, 66, 519–520. [Google Scholar] [CrossRef]
- Ng, Q.J.; Koh, K.M.; Tagore, S.; Mathur, M. Perception and Feelings of Antenatal Women during COVID-19 Pandemic: A Cross-Sectional Survey. Ann. Acad. Med. Singap. 2020, 49, 543–552. [Google Scholar] [CrossRef]
- Lee, R.W.K.; Loy, S.L.; Yang, L.; Chan, J.K.Y.; Tan, L.K. Attitudes and precaution practices towards COVID-19 among pregnant women in Singapore: A cross-sectional survey. BMC Pregnancy Childbirth 2020, 20, 1–10. [Google Scholar] [CrossRef] [Green Version]
- Woong, N.L.; Ekstrom, V.S.M.; Xin, X.; Lim, C.; Boon, E.S.K.; Teo, S.W.J.; Ng, P.C.S.; Ang, T.P.S.; Lim, S.H.; Lam, A.Y.R.; et al. Empower to connect and connect to empower: Experience in using a humanistic approach to improve patients’ access to, and experience of, care in isolation wards during the COVID-19 outbreak in Singapore. BMJ Open Qual. 2021, 10, e000996. [Google Scholar] [CrossRef]
- Sim, H.; How, C. Mental health and psychosocial support during healthcare emergencies—COVID-19 pandemic. Singap. Med. J. 2020, 61, 357–362. [Google Scholar] [CrossRef]
- Lim, J.; Leow, Z.; Ong, J.; Pang, L.S.; Lim, E. The effects of online group mindfulness training on stress and sleep quality during the COVID-19 pandemic in Singapore: A retrospective equivalence analysis. JMIR Ment. Health 2021, 19, 19. [Google Scholar] [CrossRef]
- Khng, J. Managing the impact of COVID-19 on cancer survivors in Singapore. Asia Pac. J. Soc. Work. Dev. 2020, 31, 147–151. [Google Scholar] [CrossRef]
- Lateef, F. Face to face with coronavirus disease 19: Maintaining motivation, psychological safety, and wellness. J. Emergencies Trauma Shock 2020, 13, 116–123. [Google Scholar] [CrossRef]
- Ho, C.S.; Chee, C.Y.; Ho, R.C. Mental health strategies to combat the psychological impact of COVID-19 beyond paranoia and panic. Ann. Acad. Med. Singap. 2020, 49, 155–160. [Google Scholar] [CrossRef]
- Chew, N.W.S.; Ngiam, J.N.; Khan, F.A.; Marmin, M.; Hassan, F.B.; Sharon, T.M.-L.; Lim, C.H.; Bin Mohaini, M.I.; Danuaji, R.; Nguyen, T.H.; et al. Asian-Pacific perspective on the psychological well-being of healthcare workers during the evolution of the COVID-19 pandemic. BJPsych Open 2020, 6, e116. [Google Scholar] [CrossRef]
- Lim, J.M.; Tun, Z.M.; Kumar, V.; Quaye, S.E.D.; Offeddu, V.; Cook, A.R.; Lwin, M.O.; Jiang, S.; Tam, C.C. Population anxiety and positive behaviour change during the COVID-19 epidemic: Cross-sectional surveys in Singapore, China and Italy. Influ. Other Respir. Viruses 2021, 15, 45–55. [Google Scholar] [CrossRef]
- Liu, J.C.J.; Tong, E.M.W. The Relation Between Official WhatsApp-Distributed COVID-19 News Exposure and Psychological Symptoms: Cross-Sectional Survey Study. J. Med. Internet Res. 2020, 22, e22142. [Google Scholar] [CrossRef]
- Chan, L.G.; Kuan, B. Mental health and holistic care of migrant workers in Singapore during the COVID-19 pandemic. J. Global Health 2020, 10, 1–5. [Google Scholar] [CrossRef]
- Chew, Q.H.; Wei, K.C.; Vasoo, S.; Chua, H.C.; Sim, K. Narrative synthesis of psychological and coping responses towards emerging infectious disease outbreaks in the general population: Practical considerations for the COVID-19 pandemic. Singap. Med. J. 2020, 61, 350–356. [Google Scholar] [CrossRef]
- Luo, Y.; Chua, C.R.; Xiong, Z.; Ho, R.C.; Ho, C.S.H. A Systematic Review of the Impact of Viral Respiratory Epidemics on Mental Health: An Implication on the Coronavirus Disease 2019 Pandemic. Front. Psychiatry 2020, 11, 565098. [Google Scholar] [CrossRef]
- Renjan, V.; Fung, D.S.S. Debate: COVID-19 to the under 19-a Singapore school mental health response. Child Adolesc. Ment. Health 2020, 25, 260–262. [Google Scholar] [CrossRef]
- Subramaniam, M.; Lee, Y.Y.; Chong, S.A. Mental Health for All, Greater Investment—Greater Access. Ann. Acad. Med. Singap 2020, 49, 720–722. [Google Scholar] [CrossRef]
- Hsu, L.Y.; Chia, P.Y.; Lim, J.F. The Novel Coronavirus (SARS-CoV-2) Epidemic. Ann. Acad. Med. Singap. 2020, 49, 1–3. [Google Scholar] [CrossRef]
- Ngiam, N.; Tham, S.M.; Vasoo, S.; Poh, K.-K. COVID-19: Local lessons from a global pandemic. Singap. Med. J. 2020, 61, 341–342. [Google Scholar] [CrossRef]
- Tan, T.H.Y.; Toh, M.; Vasoo, S.; Lye, D.C.B.; Ang, B.S.P.; Leo, Y.S.; Lee, V.J.M.; Puah, S.H.; Kurup, A. Coronavirus Disease 2019 (COVID-19): The Singapore Experience. A Review of the First Eight Months. Ann. Acad. Med. Singap. 2020, 49, 764–778. [Google Scholar] [CrossRef]
- Chen, J.I.P.; Yap, J.C.H.; Hsu, L.Y.; Teo, Y.Y. COVID-19 and Singapore: From Early Response to Circuit Breaker. Ann. Acad. Med. Singap. 2020, 49, 561–572. [Google Scholar] [CrossRef]
- Ong, S.E. Singapore and Covid-19: In the forefront of response efforts? Round Table 2020, 109, 334–335. [Google Scholar] [CrossRef]
- Lee, P.H.; Vasoo, S. COVID-19—Where do we go from here? Singap. Med. J. 2020, 61, 343–344. [Google Scholar] [CrossRef]
- Lum, L.H.W.; Tambyah, P.A. Outbreak of COVID-19—An urgent need for good science to silence our fears? Singap. Med. J. 2020, 61, 55–57. [Google Scholar] [CrossRef]
- Woo, J.J. Policy capacity and Singapore’s response to the COVID-19 pandemic. Policy Soc. 2020, 39, 345–362. [Google Scholar] [CrossRef]
- Lin, R.J.; Lee, T.H.; Lye, D.C. From SARS to COVID-19: The Singapore journey. Med. J. Aust. 2020, 212, 497–502.e1. [Google Scholar] [CrossRef]
- Vidyarthi, A.R.; Bagdasarian, N.; Esmaili, A.M.; Archuleta, S.; Monash, B.; Sehgal, N.L.; Green, A.; Lim, A. Understanding the Singapore COVID-19 Experience: Implications for Hospital Medicine. J. Hosp. Med. 2020, 15, 281–283. [Google Scholar] [CrossRef] [Green Version]
- Wilder-Smith, A.; Chiew, C.J.; Lee, V.J. Can we contain the COVID-19 outbreak with the same measures as for SARS? Lancet Infect. Dis. 2020, 20, e102–e107. [Google Scholar] [CrossRef] [Green Version]
- Román, R.G.; Wang, L.-F.; Lee, B.; Halpin, K.; de Wit, E.; Broder, C.C.; Rahman, M.; Kristiansen, P.; Saville, M. Nipah@20: Lessons Learned from Another Virus with Pandemic Potential. mSphere 2020, 5, e00602-20. [Google Scholar] [CrossRef]
- De Deyn, M.; Ng, O.X.; Loke, W.; Yeo, W.S. A tale of two cities: A comparison of Hong Kong and Singapore’s early strategies for the Coronavirus Disease 2019 (COVID-19). J. Infect. 2020, 81, E51–E52. [Google Scholar] [CrossRef]
- Hsu, L.; Chia, P.; Vasoo, S. A midpoint perspective on the COVID-19 pandemic. Singap. Med. J. 2020, 61, 381–383. [Google Scholar] [CrossRef]
- Cleland, J.; Tan, E.C.P.; Tham, K.Y.; Low-Beer, N. How Covid-19 opened up questions of sociomateriality in healthcare education. Adv. Health Sci. Educ. 2020, 25, 479–482. [Google Scholar] [CrossRef]
- Dong, C.; Lee, D.W.C.; Aw, D.C.W. Tips for medical educators on how to conduct effective online teaching in times of social distancing. Proc. Singap. Healthc. 2020, 30, 59–63. [Google Scholar] [CrossRef]
- Evans, D.J.; Bay, B.H.; Wilson, T.D.; Smith, C.F.; Lachman, N.; Pawlina, W. Going Virtual to Support Anatomy Education: A STOPGAP in the Midst of the Covid-19 Pandemic. Anat. Sci. Educ. 2020, 13, 279–283. [Google Scholar] [CrossRef] [Green Version]
- Srinivasan, D.K. Medical Students’ Perceptions and an Anatomy Teacher’s Personal Experience Using an e-Learning Platform for Tutorials during the Covid-19 Crisis. Anat. Sci. Educ. 2020, 13, 318–319. [Google Scholar] [CrossRef]
- Samarasekera, D.; Goh, D.L.M.; Lau, T.C. Medical School Approach to Manage the Current COVID-19 Crisis. Acad. Med. 2020, 95, 1126–1127. [Google Scholar] [CrossRef] [PubMed]
- Liang, Z.C.; Ooi, S.B.S.; Wang, W. Pandemics and Their Impact on Medical Training: Lessons from Singapore. Acad. Med. 2020, 95, 1359–1361. [Google Scholar] [CrossRef] [PubMed]
- Tay, Y.X.; Chow, H.C.; Ooi, C.C. Impact on clinical learning during coronavirus disease 2019 pandemic: From disruption to recovery and the new norms. Korean J. Med. Educ. 2020, 32, 297–305. [Google Scholar] [CrossRef]
- Cleland, J.; Chu, J.; Lim, S.; Low, J.; Low-Beer, N.; Kwek, T.K. COVID 19: Designing and conducting an online mini-multiple interview (MMI) in a dynamic landscape. Med. Teach. 2020, 42, 776–780. [Google Scholar] [CrossRef]
- Teo, L.W.; Pang, T.; Ong, Y.J.; Lai, C. Coping with COVID-19: Perspectives of Student Radiographers. J. Med. Imaging Radiat. Sci. 2020, 51, 358–360. [Google Scholar] [CrossRef]
- Tay, Y.X.; Sng, L.H.; Chow, H.C.; Zainuldin, M.R. Clinical placements for undergraduate diagnostic radiography students amidst the COVID-19 pandemic in Singapore: Preparation, challenges and strategies for safe resumption. J. Med. Imaging Radiat. Sci. 2020, 51, 560–566. [Google Scholar] [CrossRef]
- Samarasekera, D.; Goh, D.L.M.; Yeo, S.P.; Ngiam, N.S.P.; Aw, M.M.; Lim, M.M.; Pillai, S.; Lee, S.S.; Mahadevan, M.; Kow, A.; et al. Response and Lessons Learnt Managing the COVID-19 Crisis by School of Medicine, National University of Singapore. MedEdPublish 2020, 9, 92. [Google Scholar] [CrossRef]
- Ashokka, B.; Ong, S.Y.; Tay, K.H.; Loh, N.H.W.; Gee, C.F.; Samarasekera, D. Coordinated responses of academic medical centres to pandemics: Sustaining medical education during COVID-19. Med. Teach. 2020, 42, 762–771. [Google Scholar] [CrossRef] [PubMed]
- Boursicot, K.; Kemp, S.; Ong, T.H.; Wijaya, L.; Goh, S.H.; Freeman, K.J.; Curran, I. Conducting a high-stakes OSCE in a COVID-19 environment. MedEdPublish 2020, 9. [Google Scholar] [CrossRef] [Green Version]
- Compton, S.; Sarraf-Yazdi, S.; Rustandy, F.; Krishna, L.K.R. Medical students’ preference for returning to the clinical setting during the COVID-19 pandemic. Med. Educ. 2020, 54, 943–950. [Google Scholar] [CrossRef]
- Sia, C.-H.; Tan, B.Y.-Q.; Ooi, S.B.S. Impact of the coronavirus disease 2019 pandemic on postgraduate medical education in a Singaporean academic medical institution. Korean J. Med. Educ. 2020, 32, 97–100. [Google Scholar] [CrossRef]
- Chan, G.M.F.; Kanneganti, A.; Yasin, N.; Ismail-Pratt, I.; Logan, S.J.S. Well-being, obstetrics and gynaecology and COVID-19: Leaving no trainee behind. Aust. N. Z. J. Obstet. Gynaecol. 2020, 60, 983–986. [Google Scholar] [CrossRef]
- Chowdhury, A.; Tan, Y.Q.; Wang, Z.; Tiong, H.Y.; Chiong, E. Right Place, Right Time: Serendipitous Opportunities in a Urology Fellowship Disrupted by the COVID-19 Pandemic. Urology 2020, 143, 269. [Google Scholar] [CrossRef] [PubMed]
- Lim, Y.; Chook, S.; Low, T.-T.; Yeo, W.T.; Tay, E. Cardiology Training in Singapore During the COVID-19 Pandemic. Acad. Med. 2020, 95, e2. [Google Scholar] [CrossRef] [PubMed]
- Cheong, M.A.; Chee, Y.; Ng, H.J.; Jen, W. Keeping the bloodline of haematology medical education flowing during a pandemic. Int. J. Lab. Hematol. 2020, 42, e196–e198. [Google Scholar] [CrossRef]
- Tan, Y.Q.; Pek, X.W.G.; Wang, Z.; Tiong, H.Y.; Chiong, E. Impact of the COVID-19 Pandemic on the Urology Residency Match in Singapore. Urology 2020, 143, 272–273. [Google Scholar] [CrossRef]
- Tan, Y.Q.; Wang, Z.; Tiong, H.Y.; Chiong, E. The Good, the Bad, and the Ugly of the COVID-19 Pandemic in a Urology Residency Program in Singapore. Urology 2020, 142, 244–245. [Google Scholar] [CrossRef] [PubMed]
- Tay, Y.H.; Lim, L.; Cheng, A.; Sim, K. Disrupting the disruption: Using digital tools to support psychiatry residency training in Singapore during the COVID-19 pandemic. Psychiatry Res. 2020, 289, 113063. [Google Scholar] [CrossRef]
- Wong, C.S.; Tay, W.; Hap, X.; Chia, F. Love in the time of coronavirus: Training and service during COVID-19. Singap. Med. J. 2020, 61, 384–386. [Google Scholar] [CrossRef]
- Kee, A.; Archuleta, S.; Dan, Y.Y. Internal Medicine Residency Training in the COVID-19 Era—Reflections from Singapore. J. Grad. Med. Educ. 2020, 12, 406–408. [Google Scholar] [CrossRef] [PubMed]
- Wittayanakorn, N.; Nga, V.D.W.; Sobana, M.; Bahuri, N.F.A.; Baticulon, R.E. Impact of COVID-19 on Neurosurgical Training in Southeast Asia. World Neurosurg. 2020, 144, e164–e177. [Google Scholar] [CrossRef] [PubMed]
- Yong, X.; Chew, C.W.; Chin, C.Y.; Ong, C.Y.M.; Tan, H.K.; Lee, J.C.S. COVID-19 in Singapore: Graduate Medical Education in The Face of a Global Pandemic. MedEdPublish 2020, 9. [Google Scholar] [CrossRef]
- Foong, W.-S.; Teo, H.L.T.; Wang, D.H.B.; Loh, S.Y.J. Challenges and adaptations in training during pandemic COVID-19: Observations by an orthopedic resident in Singapore. Acta Orthop. 2020, 91, 562–566. [Google Scholar] [CrossRef] [PubMed]
- Lee, J.; Chan, J.; Ithnin, F.; Goy, R.; Sng, B. Resilience of the restructured obstetric anaesthesia training programme during the COVID-19 outbreak in Singapore. Int. J. Obstet. Anesthesia 2020, 43, 89–90. [Google Scholar] [CrossRef] [PubMed]
- Kanneganti, A.; Lim, K.M.X.; Chan, G.M.F.; Choo, S.; Choolani, M.; Ismail-Pratt, I.; Logan, S.J.S. Pedagogy in a pandemic—COVID-19 and virtual continuing medical education (vCME) in obstetrics and gynecology. Acta Obstet. Gynecol. Scand. 2020, 99, 692–695. [Google Scholar] [CrossRef] [PubMed]
- Chew, Q.H.; Chia, F.L.-A.; Ng, W.K.; Lee, W.C.I.; Tan, P.L.L.; Wong, C.S.; Puah, S.H.; Shelat, V.G.; Seah, E.-J.D.; Huey, C.W.T.; et al. Perceived Stress, Stigma, Traumatic Stress Levels and Coping Responses amongst Residents in Training across Multiple Specialties during COVID-19 Pandemic—A Longitudinal Study. Int. J. Environ. Res. Public Health 2020, 17, 6572. [Google Scholar] [CrossRef]
- Seneviratne, C.J.; Lau, M.W.J.; Goh, B.T. The Role of Dentists in COVID-19 Is Beyond Dentistry: Voluntary Medical Engagements and Future Preparedness. Front. Med. 2020, 7, 566. [Google Scholar] [CrossRef]
- Sirisena, D.; Zhang, M.; Li, J.Z.; Chew, K. Impact of COVID-19: Perspectives from Sport and Exercise Medicine. Ann. Acad. Med. Singap. 2020, 49, 596–598. [Google Scholar]
- Goh, O.Q.; Islam, A.M.; Lim, J.C.; Chow, W.-C. Towards health market systems changes for migrant workers based on the COVID-19 experience in Singapore. BMJ Glob. Health 2020, 5, e003054. [Google Scholar] [CrossRef] [PubMed]
- Rajaraman, N.; Yip, T.-W.; Kuan, B.Y.H.; Lim, J.F.Y. Exclusion of Migrant Workers from National UHC Systems—Perspectives from HealthServe, a Non-profit Organisation in Singapore. Asian Bioeth. Rev. 2020, 12, 363–374. [Google Scholar] [CrossRef] [PubMed]
- Tee, L.Y.; Alhamid, S.M.; Tan, J.L.; Di Oo, T.; Chien, J.; Galinato, P.; Tan, S.Y.; Humaira, S.; Fong, R.K.C.; Puar, T.H.; et al. COVID-19 and Undiagnosed Pre-diabetes or Diabetes Mellitus Among International Migrant Workers in Singapore. Front. Public Health 2020, 8, 584249. [Google Scholar] [CrossRef]
- Chia, C.L.K. Leading a COVID-19 cohort ward without blades: A surgeon’s perspectives. Br. J. Surg. 2020, 107, e298–e299. [Google Scholar] [CrossRef]
- Lim, C.; Zhou, J.X.; Woong, N.L.; Chiam, M.; Krishna, L.K.R. Addressing the Needs of Migrant Workers in ICUs in Singapore. J. Med. Educ. Curric. Dev. 2020, 7. [Google Scholar] [CrossRef]
- Goh, E.F.; Tan, C.N.; Pek, K.; Leong, S.; Wong, W.C.; Lim, W.S. Not Wasting a Crisis: How Geriatrics Clinical Research Can Remain Engaged During COVID-19. J. Am. Geriatr. Soc. 2020, 68, 1676–1677. [Google Scholar] [CrossRef] [PubMed]
- Liu, N.; Chee, M.L.; Niu, C.; Pek, P.P.; Siddiqui, F.J.; Ansah, J.P.; Matchar, D.B.; Lam, S.S.W.; Abdullah, H.R.; Chan, A.; et al. Coronavirus disease 2019 (COVID-19): An evidence map of medical literature. BMC Med. Res. Methodol. 2020, 20, 1–11. [Google Scholar] [CrossRef] [PubMed]
- Seah, I. Striving as a nation to become an academic leader in the COVID-19 crisis. Singap. Med. J. 2020, 61, 370–372. [Google Scholar] [CrossRef] [PubMed]
- Loh, T.P.; Horvath, A.R.; Wang, C.-B.; Koch, D.; Adeli, K.; Mancini, N.; Ferrari, M.; Hawkins, R.; Sethi, S.; Lippi, G. Operational considerations and challenges of biochemistry laboratories during the COVID-19 outbreak: An IFCC global survey. Clin. Chem. Lab. Med. 2020, 58, 1441–1449. [Google Scholar] [CrossRef] [PubMed]
- Chia, E.W.Y.; Tay, K.T. Critical-care resource allocation during the coronavirus disease 2019 pandemic in Singapore: A brief narrative review. Proc. Singap. Healthc. 2020, 30, 76–79. [Google Scholar] [CrossRef]
- Lateef, F.B.A. Through the Ethical Lenses: There is Really More than Meets the Eye with Covid-19. Arch. Emerg. Med. Intensiv. Care 2020, 3, 6–16. [Google Scholar] [CrossRef]
- Krishna, L.K.R.; Neo, H.Y.; Chia, E.W.Y.; Tay, K.T.; Chan, N.; Neo, P.S.H.; Goh, C.; Peh, T.Y.; Chiam, M.; Low, J.A.Y.H. The role of palliative medicine in ICU bed allocation in COVID-19: A joint position statement of the Singapore Hospice Council and the Chapter of Palliative Medicine Physicians. Asian Bioeth. Rev. 2020, 12, 205–211. [Google Scholar] [CrossRef]
- Yi, H.; Ng, S.T.; Farwin, A.; Low, A.P.T.; Chang, C.M.; Lim, J. Health equity considerations in COVID-19: Geospatial network analysis of the COVID-19 outbreak in the migrant population in Singapore. J. Travel Med. 2021, 28, taaa159. [Google Scholar] [CrossRef] [PubMed]
- Faria, G.; Onubogu, I.K.; Tadros, B.J.; Relwani, J. Change in practice due to COVID-19—Early experiences of a United Kingdom district general hospital in trauma & orthopaedics. J. Orthop. 2020, 22, 288–290. [Google Scholar] [CrossRef]
- De Santo, L.S.; Rubino, A.S.; Torella, M.; Galbiati, D.; Iannelli, G.; Iesu, S.; Tritto, F.P.; Fiorani, B.; Chiariello, L.; De Bellis, A.; et al. Cardiac surgery practice during the COVID-19 outbreak: A regionwide survey. J. Thorac. Dis. 2021, 13, 125–132. [Google Scholar] [CrossRef] [PubMed]
- Bhargava, S.; Sarkar, R. Impact of COVID-19 Pandemic on Dermatology Practice in India. Indian Dermatol. Online J. 2020, 11, 712–719. [Google Scholar] [PubMed]
- Kamdar, H.A.; Senay, B.; Mainali, S.; Lee, V.; Gulati, D.K.; Greene-Chandos, D.; Hinduja, A.; Strohm, T. Clinician’s Perception of Practice Changes for Stroke During the COVID-19 Pandemic. J. Stroke Cerebrovasc. Dis. 2020, 29, 105179. [Google Scholar] [CrossRef]
- Jeong, A.; Sagong, M. Changes in the Clinical Practice of Ophthalmology during the Coronavirus Disease 2019 (COVID-19) Outbreak: An Experience from Daegu, Korea. Infect. Chemother. 2020, 52, 226–230. [Google Scholar] [CrossRef]
- Teo, J. TTSH Covid-19 cluster sparked by new variant that originated in India. The Straits Times. Available online: https://www.straitstimes.com/singapore/health/ttsh-covid-19-cluster-five-patients-have-india-variant-of-virus (accessed on 25 June 2021).
- Taiwan to Put 5000 into Quarantine over Hospital COVID-19 Cluster. Reuters. Available online: https://www.reuters.com/article/us-health-coronavirus-taiwan-idUSKBN29T0CN (accessed on 25 June 2021).
- In-Depth Analysis Identifies Causes and Mitigation Efforts in COVID-19 Cluster. Brigham and Women’s Hospital. Available online: https://www.eurekalert.org/pub_releases/2021-02/bawh-iai020821.php (accessed on 25 June 2021).
- Gooch, K. COVID-19 Cluster at Kentucky Hospital Prompts Testing of 100 Employees. Becker’s Hospital Review. Available online: https://www.beckershospitalreview.com/workforce/covid-19-cluster-at-kentucky-hospital-prompts-testing-of-100-employees.html (accessed on 25 June 2021).
- Bearne, L.M.; Gregory, W.J.; Hurley, M.V. Remotely delivered physiotherapy: Can we capture the benefits beyond COVID-19? Rheumatology 2021, 60, 1582–1584. [Google Scholar] [CrossRef] [PubMed]
- Di Carlo, F.; Sociali, A.; Picutti, E.; Pettorruso, M.; Vellante, F.; Verrastro, V.; Martinotti, G.; di Giannantonio, M. Telepsychiatry and other cutting-edge technologies in COVID-19 pandemic: Bridging the distance in mental health assistance. Int. J. Clin. Pract. 2021, 75, e13716. [Google Scholar] [CrossRef]
- Appleby, E.; Gill, S.T.; Hayes, L.K.; Walker, T.L.; Walsh, M.; Kumar, S. Effectiveness of telerehabilitation in the management of adults with stroke: A systematic review. PLoS ONE 2019, 14, e0225150. [Google Scholar] [CrossRef] [Green Version]
- Qing, A. Around 1 in 3 Students Collected TraceTogether Tokens in School: MOE. The Straits Times. Available online: https://www.straitstimes.com/singapore/around-1-in-3-students-collected-tracetogether-tokens-in-school-moe (accessed on 25 June 2021).
- Confirmed Cases of COVID-19 Variants Identified in UK. Public Health England. Available online: https://www.gov.uk/government/news/confirmed-cases-of-covid-19-variants-identified-in-uk (accessed on 25 June 2021).
- Dobson, H.; Malpas, C.B.; Burrell, A.J.; Gurvich, C.; Chen, L.; Kulkarni, J.; Winton-Brown, T. Burnout and psychological distress amongst Australian healthcare workers during the COVID-19 pandemic. Australas. Psychiatry 2021, 29, 26–30. [Google Scholar] [CrossRef]
- Nishimura, Y.; Miyoshi, T.; Hagiya, H.; Kosaki, Y.; Otsuka, F. Burnout of Healthcare Workers amid the COVID-19 Pandemic: A Japanese Cross-Sectional Survey. Int. J. Environ. Res. Public Health 2021, 18, 2434. [Google Scholar] [CrossRef] [PubMed]
- Torrente, M.; Sousa, P.A.; Sánchez-Ramos, A.; Pimentao, J.; Royuela, A.; Franco, F.; Collazo-Lorduy, A.; Menasalvas, E.; Provencio, M. To burn-out or not to burn-out: A cross-sectional study in healthcare professionals in Spain during COVID-19 pandemic. BMJ Open 2021, 11, e044945. [Google Scholar] [CrossRef]
- Khasne, R.W.; Dhakulkar, B.S.; Mahajan, H.C. Burnout among Healthcare Workers during COVID-19 Pandemic in India: Results of a Questionnaire-based Survey. Indian J. Crit. Care Med. 2020, 24, 664–671. [Google Scholar] [CrossRef] [PubMed]
- Alzueta, E.; Perrin, P.; Baker, F.C.; Caffarra, S.; Ramos-Usuga, D.; Yuksel, D.; Arango-Lasprilla, J.C. How the COVID-19 pandemic has changed our lives: A study of psychological correlates across 59 countries. J. Clin. Psychol. 2021, 77, 556–570. [Google Scholar] [CrossRef] [PubMed]
- Dawson, D.L.; Golijani-Moghaddam, N. COVID-19: Psychological flexibility, coping, mental health, and wellbeing in the UK during the pandemic. J. Context. Behav. Sci. 2020, 17, 126–134. [Google Scholar] [CrossRef]
- Holingue, C.; Badillo-Goicoechea, E.; Riehm, K.E.; Veldhuis, C.B.; Thrul, J.; Johnson, R.M.; Fallin, M.D.; Kreuter, F.; Stuart, E.A.; Kalb, L.G. Mental distress during the COVID-19 pandemic among US adults without a pre-existing mental health condition: Findings from American trend panel survey. Prev. Med. 2020, 139, 106231. [Google Scholar] [CrossRef]
- Mazza, C.; Ricci, E.; Biondi, S.; Colasanti, M.; Ferracuti, S.; Napoli, C.; Roma, P. A Nationwide Survey of Psychological Distress among Italian People during the COVID-19 Pandemic: Immediate Psychological Responses and Associated Factors. Int. J. Environ. Res. Public Health 2020, 17, 3165. [Google Scholar] [CrossRef]
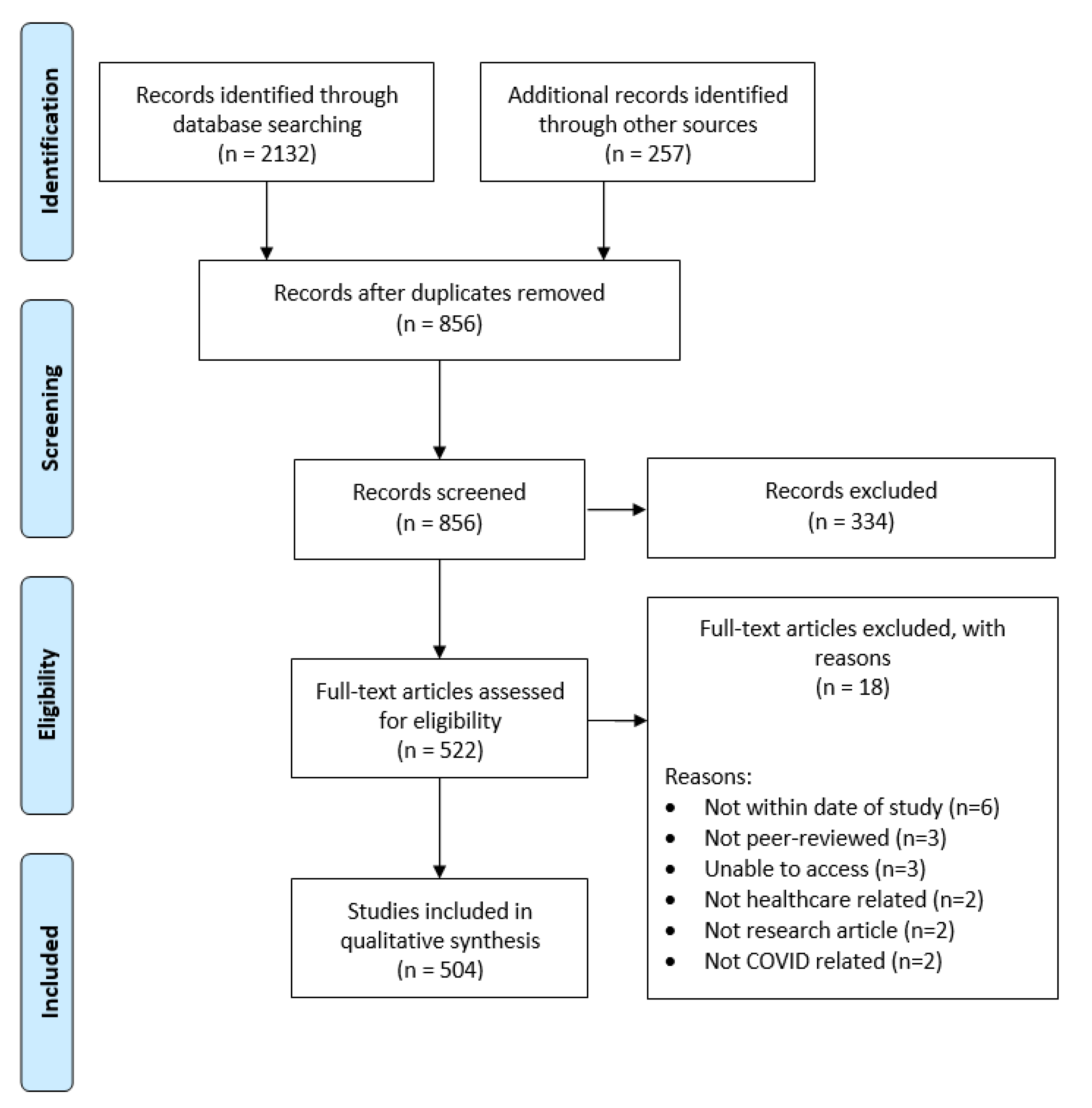
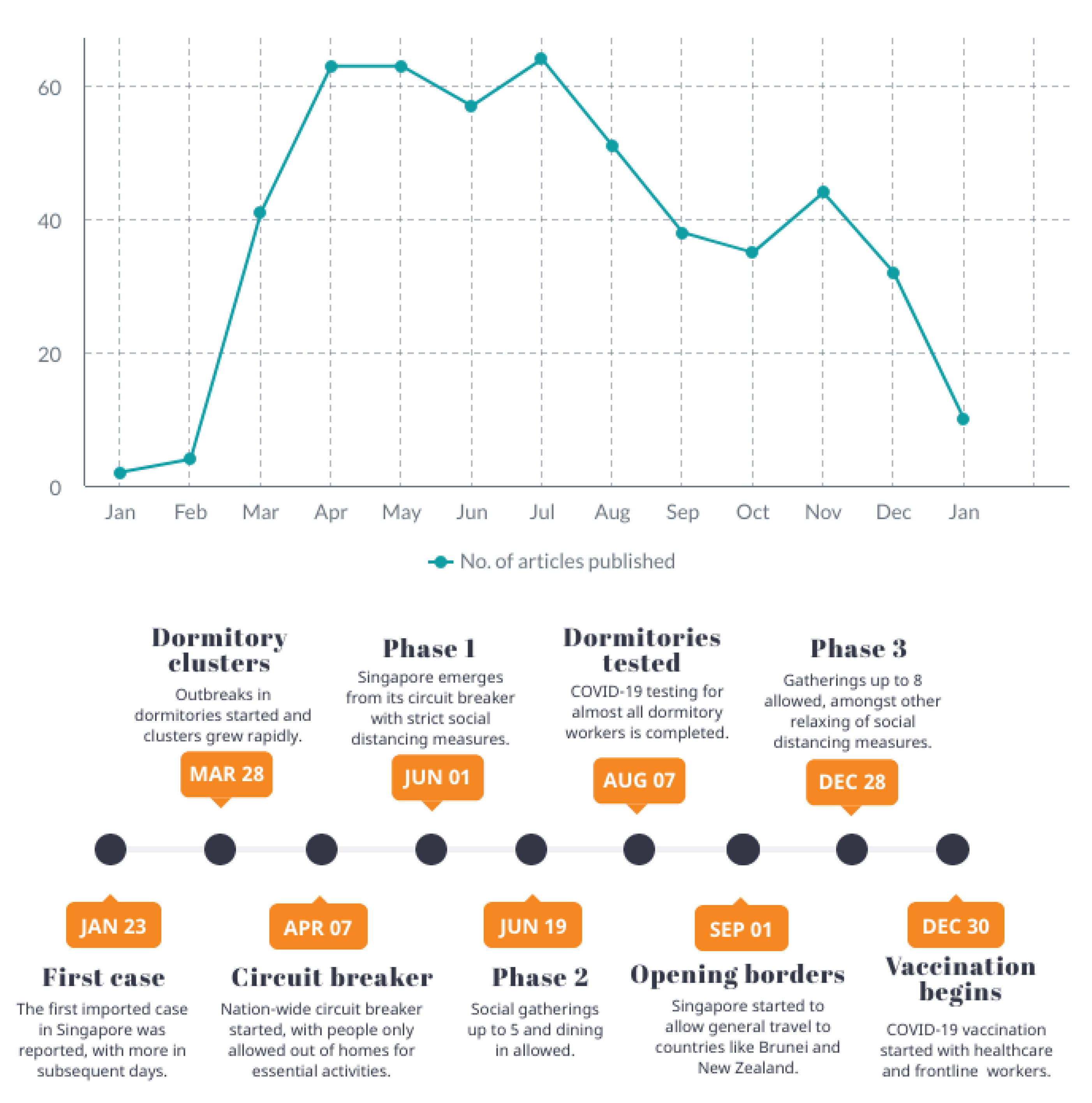

| Theme | No. of Articles | Theme | No. of Articles | Theme | No. of Articles |
|---|---|---|---|---|---|
| Changes in hospital practice | 210 | COVID-19 Pathology | 94 | Public Health | 61 |
| General changes to practice | 14 | Case reports, symptoms and complications | 39 | Healthcare worker safety | 13 |
| Telemedicine | 13 | Viral transmission modalities | 14 | Containment | 11 |
| Internal Medicine | 46 | Testing | 10 | Transmission across population | 8 |
| Surgical | 69 | Treatment | 11 | Contact Tracing | 6 |
| Other specialties | 64 | Molecular pathology | 7 | Clusters | 5 |
| Allied Health/Dentistry | 4 | General | 4 | Screening and Testing | 5 |
| Co-infection | 3 | Compliance | 3 | ||
| Impact of pandemic on clinical outcomes | 45 | Others | 6 | Modelling | 3 |
| Internal Medicine | 28 | Others | 7 | ||
| Surgical | 7 | Narrative of events | 14 | ||
| Other specialties | 10 | Summary of events | 7 | Others | 15 |
| Comparison with previous pandemics | 5 | Study of a population | 7 | ||
| Psychological impact | 35 | Comparison with other countries | 2 | Impact on research | 4 |
| Healthcare workers | 18 | Ethics | 4 | ||
| Patients | 7 | Medical education | 30 | ||
| General population | 10 | Undergraduate | 14 | ||
| Residency training | 16 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Anand, S.V.; Shuy, Y.K.; Lee, P.S.S.; Lee, E.S. One Year on: An Overview of Singapore’s Response to COVID-19—What We Did, How We Fared, How We Can Move Forward. Int. J. Environ. Res. Public Health 2021, 18, 9125. https://doi.org/10.3390/ijerph18179125
Anand SV, Shuy YK, Lee PSS, Lee ES. One Year on: An Overview of Singapore’s Response to COVID-19—What We Did, How We Fared, How We Can Move Forward. International Journal of Environmental Research and Public Health. 2021; 18(17):9125. https://doi.org/10.3390/ijerph18179125
Chicago/Turabian StyleAnand, S Vivek, Yao Kang Shuy, Poay Sian Sabrina Lee, and Eng Sing Lee. 2021. "One Year on: An Overview of Singapore’s Response to COVID-19—What We Did, How We Fared, How We Can Move Forward" International Journal of Environmental Research and Public Health 18, no. 17: 9125. https://doi.org/10.3390/ijerph18179125
APA StyleAnand, S. V., Shuy, Y. K., Lee, P. S. S., & Lee, E. S. (2021). One Year on: An Overview of Singapore’s Response to COVID-19—What We Did, How We Fared, How We Can Move Forward. International Journal of Environmental Research and Public Health, 18(17), 9125. https://doi.org/10.3390/ijerph18179125






