Abstract
We aimed to provide an overview of how work environment and occupational health are affected, and describe interventions designed to improve the work environment during epidemics and pandemics. The guidelines on Preferred Reporting Items for Systematic reviews and Meta-Analyses (PRISMA) were followed. The databases Cinahl, Medline, PsycInfo, and Web of Science were searched for population: working population; exposure: coronavirus epidemic or pandemic; and outcome: work environment, in articles published until October 2020. Quality assessment was based on a modified version of the Mixed Methods Appraisal Tool (MMAT). After deduplication 3711 articles remained, of which 530 were selected for full-text screening and 119 for quality assessment. After the exclusion of studies that were low quality, 95 remained, of which 85 focused on healthcare personnel and 10 on employees in other industries; 73 used quantitative methods and 22 used qualitative or mixed methods; the majority were based on cross-sectional data. Healthcare staff experienced increased job demands, poor leadership, and lack of resources (personal protective equipment, personnel, and competence). High demands and work with infected patients were associated with negative mental health outcomes. There was a lack of studies assessing interventions, studies from industries other than healthcare, and studies of high quality.
1. Introduction
The outbreak of SARS-CoV-2 virus in China in late 2019 rapidly developed into an epidemic, and in March 2020, the World Health Organization declared a state of global pandemic [1]. The spread of disease and restrictions to counteract the spread affected all of society, including working life, educational systems, and healthcare organizations. COVID-19 developed to be a major occupational health risk for employees not only in healthcare [2] but also in the service, manufacturing, and agriculture industries [3,4]. Previous coronavirus epidemics, such as severe acute respiratory syndrome (SARS) with an outbreak in 2003 and Middle East respiratory syndrome (MERS) with an outbreak in 2012, had a similar impact on working life and health, although not as widespread throughout societies worldwide. The COVID-19 pandemic is likely to be followed by new epidemics and pandemics affecting working life and employees in the decades to come, and employers and society need to be prepared to handle new health crises. The establishment of occupational safety policies to counteract the negative health effects of new epidemics and pandemics need to be based on scientific evidence. Therefore, there is a need to systematically review the current research on how corona epidemics and pandemics impacted working life and employee health, and what measures aimed at counteracting negative health effects on employees were effective. Several reviews of the work environment during the COVID-19 pandemic have been published [5,6,7,8,9,10,11,12]. However, most reviews focused solely on the impact on healthcare organizations [6,7,8,10,11,12], and it is important to include studies describing other labor market industries and how they are affected by epidemics and pandemics. Two reviews had a broader scope: an umbrella review from Canada [9] and a systematic review from Brazil [5]. However, the umbrella review did not evaluate the methodological quality of the included studies, and the systematic review did not include intervention studies targeting work environment factors. Moreover, previous research reviews only included studies of the work environment during COVID-19, possibly missing important knowledge drawn from previous coronavirus epidemics. With the present systematic review of studies, focusing on how the work environment and employee health are affected during an epidemic or pandemic caused by coronavirus (COVID-19, SARS, and MERS), and the effect of interventions to improve work environment and employee health, we intend to fill this knowledge gap. This work is based on a systematic review commissioned by the Swedish Agency for Work Environment Expertise.
Aim
The aim of the present study was to systematically review research on work environments and employee health during coronavirus epidemics or pandemics. The specific research questions were: During an epidemic or pandemic caused by a coronavirus,
- How is the work environment affected?
- What are the associations between work environment factors and employee health?
- What are the effects of interventions to improve the work environment or health?
2. Methods
We followed the guidelines on Preferred Reporting Items for Systematic reviews and Meta-Analyses (PRISMA) [13]. A professional at the University Library at Uppsala University, Sweden, conducted the literature search in the start of October 2020 and a protocol was registered in Prospero on the 29th March 2021 (no CRD42021229165). A principal investigator (AN) and two additional researchers (ID, KR) made up the core review team and two research assistants (YL, WL) and an expert on qualitative research (UW) provided input in particular parts of the review process.
2.1. Search Strategy and Study Selection
The search strategy was developed by the core review team in collaboration with a librarian at Uppsala University. The databases Cinahl, Medline, PsycInfo, and Web of Science were searched for articles published up until October 2020. The search strategy was based on a combination of terms identifying exposure (healthcare epidemic or pandemic), population (working population), and outcome (work environment). The full search strategy is given in Appendix A.
The inclusion criteria for the present study were:
- (1)
- Language: Swedish or English;
- (2)
- Population: The working population;
- (3)
- Exposure: Corona virus epidemic or pandemic; and
- (4)
- Outcome: Work environment. Only original articles published in peer-review journals were considered.
First, the titles and abstracts identified by the search were screened against our inclusion criteria by two researchers or research assistants in the review team. Discrepancies or uncertainties were discussed and resolved in the core review team. In case the titles and abstracts did not provide enough information, the articles were moved forward to the next step of the selection process. Next, full-text articles were screened by two members of the core review team according to the same procedure as for the previous step. Reasons for exclusion of an article were noted. We used the software tool Covidence (www.covidence.org, accessed on 29 September 2020) for the selection of abstracts and full-text articles. Next, the data of the selected articles were extracted to Excel sheets.
2.2. Quality Assessment
The data extracted from the full-text articles to the Excel sheets were author, journal, year of publication, country of origin, population, response rate, research question, study design, exposure, outcome, confounders considered, follow-up time, analytical strategy, and main results. The quality assessment was based on a slightly modified version of the Mixed Methods Appraisal Tool (MMAT) [14]. Different assessment criteria were considered for the different study designs. One researcher was responsible for the quality assessment of each study, but calibration between assessors and studies was carried out continuously throughout the assessment process. When uncertainties arose, assessment was conducted by discussion between the three members of the core review team. Each study was given a score between one and four or between one and five, depending on the study design. Based on this score, the study was further assessed to be of low, medium, or high quality. See Appendix A for a full description of the quality assessment process. Only studies of medium or high quality were considered in the summary of results, discussion, and conclusion, but low-quality studies are also listed in the tables.
2.3. Summary of Study Results
The majority of studies were based either on cross-sectional or qualitative data. Given the quality of the evidence and the diversity of studies included in the present systematic literature review, a meta-analysis was not feasible. The results are instead carefully presented in seven exhaustive tables. Work environment factors that were reported in several quantitative and qualitative studies are described and highlighted in the discussion section.
3. Results
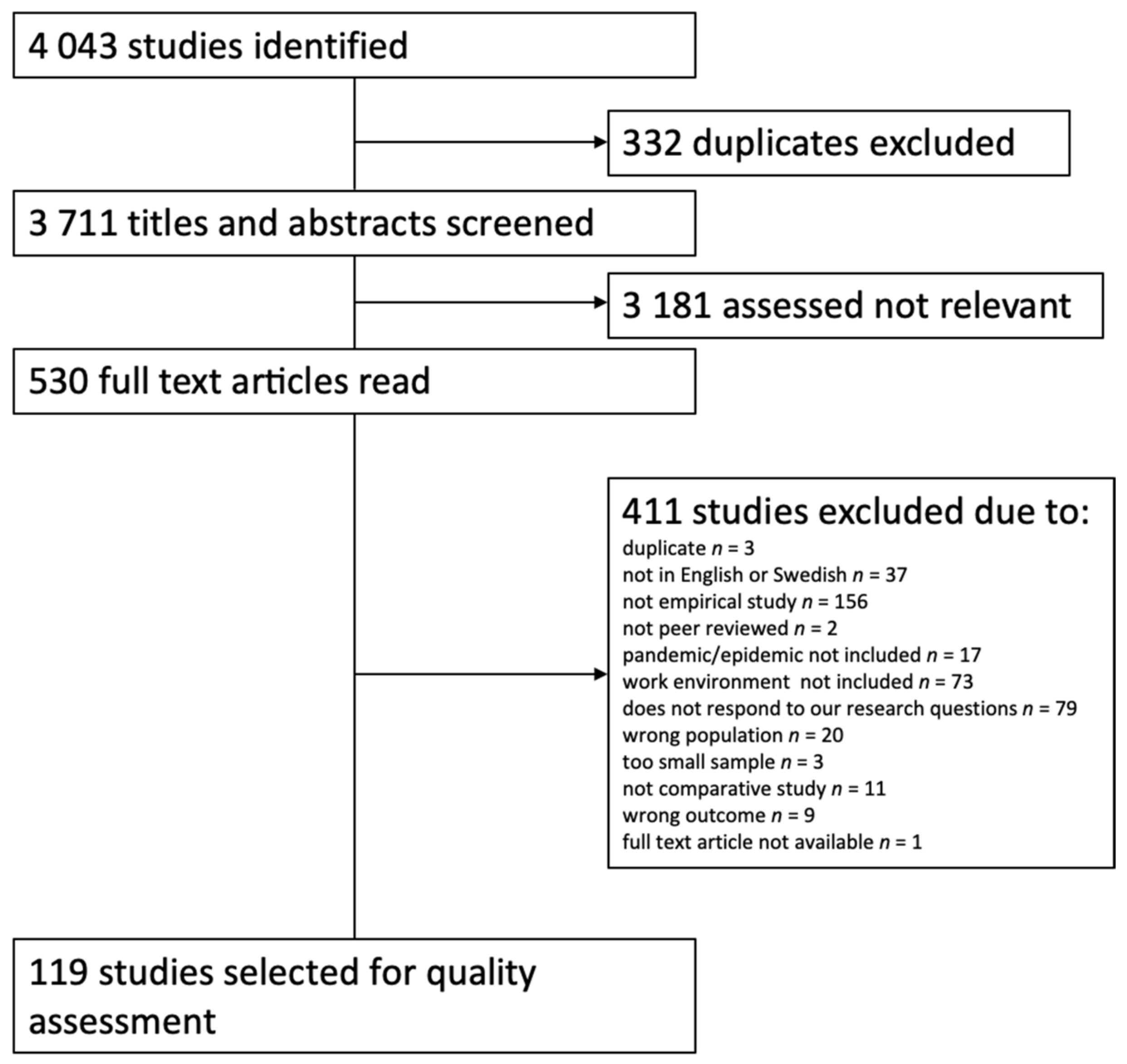
In the literature search 4043 hits were recorded, of which 3711 remained after deduplication. The titles and abstracts of these articles were screened for eligibility and 530 were moved forward for full-text screening. During this step of the process, an additional 411 articles were excluded (primarily because of not being an empirical study) and 119 were passed on to the stage of quality assessment (see Figure 1).
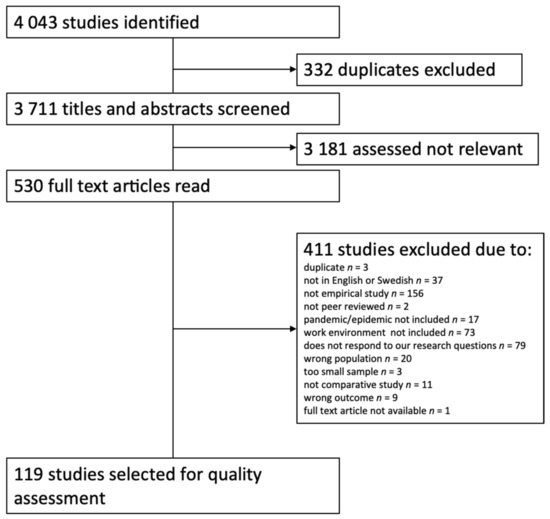
Figure 1.
Flowchart of the selection and exclusion of articles.
Of the 119 selected articles, 24 were excluded due to low quality [15,16,17,18,19,20,21,22,23,24,25,26,27,28,29,30,31,32,33,34,35,36,37,38]. Of the remaining 95 studies, 85 investigated the healthcare industry and 10 studies focused on other industries. The results are presented separately for the healthcare industry and other industries below.
3.1. The Healthcare Industry
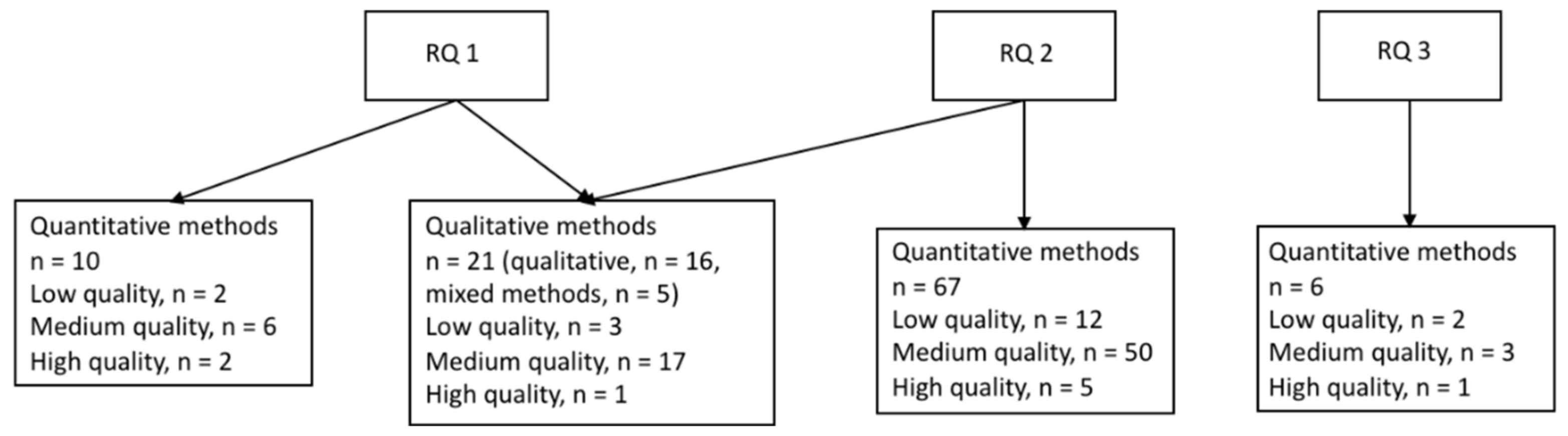
Of the 85 studies focusing on healthcare workers (HCWs, reported in Table 1, Table 2, Table 3 and Table 4), 67 studies were based on quantitative data (Table 1, Table 2 and Table 3) and 18 on qualitative or mixed-methods designs (Table 4). The quantitative studies are presented separately for research question 1, 2, and 3 below followed by the results from the qualitative and mixed-methods studies, which were combined for research question 1 and 2 as they were often assessed simultaneously and were not possible to separate in the synthesis of the results (see Figure 2). We did not identify any qualitative or mixed-methods studies assessing research question 3.

Table 1.
Overview of quantitative studies assessing how the work environment is affected by an epidemic or pandemic (COVID-19, SARS, or MERS) in the healthcare industry (research question 1).

Table 2.
Overview of quantitative studies assessing the associations between work environment factors and health (research question 2) in the healthcare industry during an epidemic or pandemic (COVID-19, SARS, or MERS).

Table 3.
Overview of quantitative studies assessing interventions to change the work environment or health in the healthcare industry during an epidemic or pandemic (COVID-19, SARS, or MERS, research question 3).

Table 4.
Overview of qualitative and mixed-methods studies exploring how the work environment in the healthcare sector is affected by an epidemic or pandemic (research question 1) and studies investigating the associations between the work environment and health during an epidemic or pandemic (research question 2).
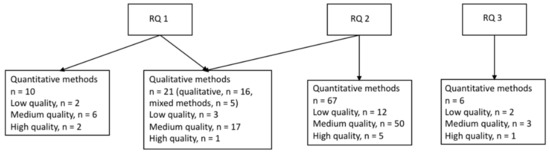
Figure 2.
Studies of the healthcare industry sorted by research question and methodology. Research questions (RQs): During an epidemic or pandemic caused by a coronavirus: (1) How is the work environment affected? (2) What are the associations between work environment factors and employee health? (3) What are the effects of interventions to improve the work environment or health?
3.1.1. Results from Quantitative Studies
RQ 1: How is the work environment affected by an epidemic or pandemic?
There were eight studies of medium or high quality that used quantitative methodology to investigate how the work environment was affected by a pandemic or epidemic [39,40,41,42,43,44,45,46] (see Table 1). One of them included data from four continents: four studies were from Europe, one from North America, one from Australia, and one from Asia. Six focused on the work environment during COVID-19 and two during SARS.
In several studies, workload was reported to be increased during the pandemic [39,41,42,44], particularly in high-risk sectors [39], by those working close to infected patients [41], by nurses [42], and by women [39]. In contrast, primary healthcare nurses in Australia reported decreased work hours and threats of termination since the onset of the COVID-19 pandemic [40]. One study from the UK reported that telemedicine was efficient and without an associated increased workload [43]. Differences in personnel shortage problems, provision of personal protective equipment (PPE) and PPE training, and staff diagnosed with COVID-19 were reported between Asia, Europe, North America, and South America [45]. Nurses reported more negative factors in the work environment, such as poor information, insufficient infection control measures, and lack of appreciation by employer, than doctors [42,46].
RQ2: Associations between work environment and health during an epidemic or pandemic.
Of the 55 quantitative studies of medium to high quality that investigated associations with health outcomes, 44 investigated associations with mental ill-health [47,48,49,50,51,52,53,54,55,56,57,58,59,60,61,62,63,64,65,66,67,68,69,70,71,72,73,74,75,76,77,78,79,80,81,82,83,84,85,86,87,88,89,90], 4 associations with physical complaints due to PPE [91,92,93,94], and 7 associations with risk of healthcare infection [95,96,97,98,99,100,101] (see Table 2). One of the studies was global, 12 were from Europe, 12 from North America, 26 from Asia, 1 from South America, and 3 from the Middle East. Most studies, 36 of them, investigated the work environment and health during COVID-19, 15 during SARS, and 4 during MERS. Three studies compared mental ill-health between healthcare workers and workers in other professions and found that healthcare workers reported increased mental ill-health in comparison [47,53,88]. A large number of the studies focusing on mental health outcomes reported associations between working in the frontline (i.e., working with patients infected or suspected to be infected) and symptoms of depression, anxiety, emotional exhaustion, burnout, sleep disturbances, or post-traumatic stress syndrome [48,50,54,55,57,63,65,67,70,75,81,82,84,86,89,90]. Among these employees, several work stressors were found to be associated with mental health outcomes. For example, longer working hours or overtime work [50,53,68,77,87,88] and type of shift/higher frequency of night shifts [60,64,87] were associated with increased symptoms of mental ill-health. Other factors associated with mental health symptoms were not having adequate knowledge and training to meet the work demands [50,62,67,70,71,83], lack of PPE [61,65,70,77,80,85], fear of being infected by healthcare [61,83], and experiencing stigmatization for working with infected patients [59,69,74]. Lastly, lack of organizational resources, such as manpower [83] or hospital resources for the treatment of infected patients [60] and lack of organizational and social support at work [50,52,62,65,67,84], was associated with negative mental health outcomes.
Seven studies focused on the risk of healthcare infection in healthcare personnel in relation to exposure to infected patients [95,96,97,98,99,100,101]. Higher risk of infection was found to be associated with working within a meter of an exposed patient [99], intubating [96,97], or performing chest compression [101] on a patient, having contact with respiratory secretion of an infected patient [100,101], inadequate training in infection control [95,101], and not using adequate PPE [95,96,100,101].
Four studies of medium or high quality [91,92,93,94] investigated the association between use of PPE and skin injuries or headaches. In three studies [91,92,93], an association between use of PPE and skin injuries was reported and in one study [94], an association with headaches was found.
RQ3: Interventions to improve the work environment during an epidemic or pandemic.
Four studies that measured the effects of interventions to improve the work environment and health were assessed to be of medium or high quality [102,103,104,105]. Three of these [103,104,105] focused on infection control, of which two investigated the effects of infection control training and one compared infection rates between hospitals with and without certain infection control measures. All interventions showed effects on infection. The fourth study [102] evaluated the mental health effects of an intervention targeting several organizational factors such as training, resources, infection control, and support teams. The intervention was found to protect the mental health of healthcare staff.
3.1.2. Results from Qualitative Studies
RQ1 and 2: The work environment during an epidemic or pandemic and its association with employee health.
There were 18 studies of medium to high quality that explored healthcare staffs’ experiences using a qualitative or mixed-methods designs [106,107,108,109,110,111,112,113,114,115,116,117,118,119,120,121,122,123]. Two studies were performed in Europe, nine in Asia, five in North America, and two in the Middle East. Twelve of the studies were performed during the COVID-19 pandemic, four during SARS, and two during MERS (see Table 4). All studies included a thematic analysis of qualitative data based on interviews or open-ended questionnaire items. The mixed-methods studies also included some quantitative elements.
Healthcare staff described high quantitative demands in terms of increased workload, intense work, large patient volumes, increased work shifts, and more administration [106,107,110,111,113,114,122] causing distress or burnout. In a mixed-methods study, self-reported burnout symptoms were found in 10–18% of 468 emergency physicians during the first 10 weeks of the COVID-19 pandemic [107]. Staff also described high qualitative demands, expressed as difficult tasks [108,111,123], new routines [107], collaborating with inexperienced staff [123], and working in a totally new context [113]. They struggled to stay updated on new, constantly changing guidelines [110] and to manage uncertainty [112,115]. Additional themes related to working with infected patients were feeling powerless [113], anxiety and suffering in staff working with seriously ill and dying patients [111,122], and decreased quality of care [108,116]. In several studies, healthcare staff reported a lack of PPE and a fear of becoming infected [106,107,108,110,111,112,114,115,121]. Among staff using PPE, there were reports about exhaustion and discomfort caused by the equipment [113,120,122]. Social stigma and being avoided by family and others due to patient contact was also described [108,117,120,121]. Several studies included staff’s descriptions of deficits in work organization: a chaotic workplace [110], insufficient preparedness for the pandemic [121], lack of information provided to staff [109,118,119], mismatch of nursing competencies and tasks [109], and an unfair work distribution [108]. Other studies included descriptions of healthcare staff’s suggestions for future improvements: involving all actors in developing communication strategies and being open about risk communication [118]. Furthermore, the development of effective work routines [108,109,122], increased attention given to staff’s mental and physical health [109], and disaster rescue training were suggested [114]. Among psychotherapists working remotely, this was perceived as challenging by 80%; nonetheless, 65% considered this to be the future core business for them [116].
Some positive aspects were described: healthcare staff experienced satisfaction and professional development during the SARS epidemic [106] and the COVID-19 pandemic [113,114,122]. Increased flexibility and less family–work conflict, thanks to remote work, were described by psychotherapists [116]. Social support [113,122] and working towards a common goal [106] were described as positive.
3.2. Industries Other Than Healthcare
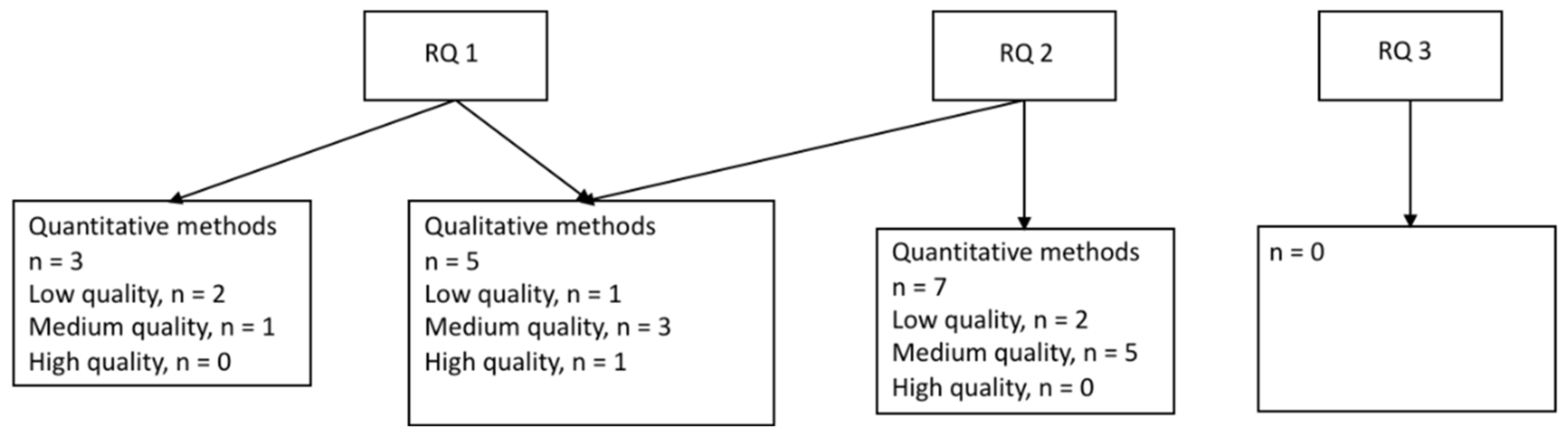
Of the ten studies focusing on industries other than the healthcare industry (reported in Table 5, Table 6 and Table 7), six studies were based on quantitative data (Table 5 and Table 6) and four on qualitative or mixed-methods designs (Table 7). The quantitative studies are presented separately for research question 1 and 2 below, followed by the results from the qualitative and mixed-methods studies presented together for the same research questions (see Figure 3). No studies of interventions aiming to improve the work environment or employee health in industries outside healthcare were identified.

Table 5.
Overview of quantitative studies assessing how the work environment in organizations outside the healthcare sector is affected by an epidemic or pandemic (research question 1). All studies are in the context of COVID-19.

Table 6.
Overview of quantitative studies assessing the associations between work environment factors and health in organizations outside the healthcare sector during an epidemic or pandemic (research question 2). All studies are in the context of COVID-19.

Table 7.
Overview of qualitative and mixed-methods studies exploring how the work environment outside the healthcare sector is affected by an epidemic or pandemic (research question 1) and studies investigating the associations between the work environment and health during an epidemic or pandemic (research question 2).
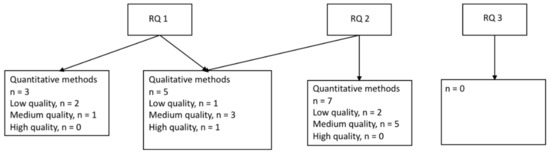
Figure 3.
Studies of industries other than healthcare, sorted by research question and methodology. Research questions (RQs): During an epidemic or pandemic caused by a coronavirus: (1) How is the work environment affected? (2) What are the associations between work environment factors and employee health? (3) What are the effects of interventions to improve the work environment or health?
3.2.1. Results from Quantitative Studies
RQ1: How is the work environment affected by a pandemic or epidemic?
Only one study of high enough quality matched the inclusion criteria [124]. The study was from Brazil and investigated changes in working conditions among a variety of professions, such as teachers, social workers, psychologists, physicians, and lawyers, working with child health and security. The results showed that their working hours had decreased during the COVID-19 pandemic compared to before.
RQ2: Associations between the work environment and health during an epidemic or pandemic
Five studies, all with a cross-sectional research design, performed in Asia, and assessed to be of medium quality, met the inclusion criteria [125,126,127,128,129]. The samples and research questions were heterogenous. In male police officers in Pakistan during the COVID-19 pandemic, an association between work–family conflict and work-related stress was found [125]. In a Chinese study, no association between where the employees worked (at home, at the office, or both) and mental ill-health was found, with the exception that those who alternated between the office and home reported less somatization symptoms [127]. Another Chinese study reported an association between improved hygiene routines during COVID-19 and lower levels of self-reported stress among employees [128]. A Japanese study found a positive association between the number of preventive infection measures implemented at the workplace, and the level of fear and anxiety related to COVID-19, a result that the authors stated may be due to a higher awareness about the disease at workplaces with a larger number of preventive measures [126]. Last, a study from Hong Kong found associations between dissatisfaction with infection control measures, perceived infection risk, and lower health-related quality of life [129].
3.2.2. Results from Qualitative Studies
RQ1 and 2: The work environment during an epidemic or pandemic and its association with employee health
Four studies of medium or high quality explored experiences among staff in industries other than healthcare using a qualitative or mixed-methods design: three in the educational system [130,131,132] and one in social work [133]. Two studies were performed in North America (SARS and COVID-19, respectively), one in Europe (COVID-19), and one in Australia (COVID-19) (see Table 7). The teachers described how the quick transition to remote teaching during the COVID-19 pandemic increased their workload [132] and introduced uncertainty [130] and techno stress [131]. Furthermore, they reported how they lost the opportunity to teach hands-on skills [131,132] and worried about students’ learning outcomes [130,132] and wellbeing [130]. The transition to remote teaching was perceived as “demanding” or “very demanding” by 49% of the educators at a physician assistant program in North America [131]. However, they also described how they adjusted and found positive aspects of remote teaching such as using new pedagogies and synchronous teaching across remote sites [132] and increased flexibility, sometimes at the cost of difficulties in home–work balance, during the workday [130]. Social workers at a hospital described how the SARS epidemic influenced their professional roles by increasing the emotional awareness of patients’ families and other professionals and problems regarding information about guidelines and their implementation [133].
4. Discussion
To the best of our knowledge, this is the first systematic review of studies describing the impact of healthcare epidemics and pandemics (COVID-19, MERS, and SARS) on the work environment and employee health, and the effect of interventions, including industries within and outside healthcare organizations. Previous reviews have reported healthcare to be the most thoroughly studied industry [5,9] and the present review confirms this is still the case.
Based on the findings in 95 original studies (85 within healthcare and 10 in other industries), we found unambiguous evidence for a negative impact on healthcare staff in terms of increased demands such as excessive workload and difficult tasks. Healthcare staff reported that they needed to adapt quickly to new routines and collaborations, managing insecurity and a lack of resources. There was a need for strong communicative leadership and provision of social support. Mental ill-health among healthcare staff was associated with exposure to infected patients, high demands, lack of PPE, lack of competence, lack of social support at work, feeling stigmatized, and perceiving a high risk of becoming infected. Nurses reported worse mental health compared to other healthcare professions. A few intervention studies, all within healthcare organizations, were identified. They evaluated training and new routines to reduce the risk of disease transmission and reported positive results. The small number of studies performed in industries outside healthcare found mental ill-health to be associated with insufficient preventive measures at the workplace, high workload, work–family conflict, and not being able to work remotely. A few studies exploring teachers’ experiences reported an increased workload due to the quick transition to remote teaching but also positive aspects of learning new teaching methods that they wished to integrate in their regular teaching after the pandemic.
Several original articles focusing on the COVID-19 pandemic, published after the search in October, 2020, support the findings in the present review: increased working hours and occupational stigma were associated with worse mental health and intention to leave among Taiwanese nurses [134]; mental health among primary healthcare workers in China was negatively affected by pandemic-related work stress; however, such stress was attenuated by social support and resilience [135]; and, finally, a Swedish longitudinal study found negative changes in healthcare staff’s working conditions and their possibility to recover after comparing their ratings before and after the first wave of COVID-19 [136].
4.1. Overall Strength of the Evidence
The large number of articles published since COVID-19 started to spread demonstrate the immediate response in the research community to the pandemic. Evidence started to accumulate within a few months from the outbreak, and a picture is emerging of how the work environment and employees’ health have been affected so far. The evidence from the healthcare sector shows a coherent picture from quantitative and qualitative data from studies worldwide of a strong impact on this industry.
4.2. Limitations of the Current Evidence
The weak study designs and overall low methodological quality of the included studies indicate that quantity was prioritized ahead of quality during the first few months of the COVID-19 pandemic but also during previous healthcare epidemics. The speed of the review and publication process, indicated by the dates of the reception, acceptance, and publication of articles, suggests that the peer-review process may have been less stringent than what is normally the case. Most of the studies that met the inclusion criteria for the present systematic review were based on convenience samples and cross-sectional designs. Furthermore, most studies used non-validated measures of exposure and also of the outcomes, and potential confounders were often not considered in the analyses. These methodological flaws prevent any conclusions about the causality between the work environment factors and employee health. The SARS and MERS epidemics were included in the present review because, with time having passed, we expected that studies with longitudinal designs and of higher quality had been published, providing an opportunity to learn from previous healthcare epidemics. However, few longitudinal follow-up studies of the previous healthcare epidemics were identified in our literature search, demonstrating a missed opportunity to learn about the long-term consequences of such epidemics.
4.3. Overall Gaps in Knowledge and Research
Longitudinal studies are needed to follow changes over time, accumulating knowledge that may enable conclusions about the causality and effects in different groups. Furthermore, it is important to develop and evaluate interventions using experimental designs to establish effective measures to enhance the work environment and health as new epidemics and pandemics evolve. In healthcare, employees report experiencing stigma for working with infected patients. More research is needed on this topic, and how to protect healthcare workers from such an extra burden during a health crisis. There is a paucity of studies from industries other than healthcare investigating the work environment and employee health during and after epidemics and pandemics. There is, for example, a need to study the long-term effect of remote work to evaluate both positive and negative impacts. There has, in general, been a larger focus on risks and stressors in the work environment and less research on possible positive changes to the work environment that can inform the development of the new working life past COVID-19.
4.4. Strengths and Limitations of the Current Review
The present review was conducted in accordance with the PRISMA guidelines for developing and reporting systematic research reviews. The search strategy was developed in a collaboration between researchers and a search specialist at Uppsala University library. A large number of studies about the work environment and health during the outbreaks of COVID-19, SARS, and MERS had been published by the search date in October 2020. The authors of the present review screened, together with two research assistants, the 4043 hits and each study was independently evaluated by at least two people in the team. Many full-text articles were read and discussed in the core assessment team. An updated search was conducted at the end of January 2021, generating an additional 2915 hits, which was too large a number of extra articles to be handled with sustained methodological stringency within the time frame of the commission by the Swedish Agency for Work Environment Expertise. A quick assessment of the new hits gave us the primary impression that most of the literature that had been published between October 2020 and January 2021 suffered from similar methodological limitations to the studies published until October 2020 and included in this review. Nevertheless, it cannot be ruled out that we could have identified additional relevant studies of higher quality had we had the possibility of prolonging the time frame for our literature search.
The search strategy was developed carefully, with consideration of capturing relevant studies while simultaneously obtaining an amount of hits in the search result that was feasible to handle within the given time frame. We used MESH terms and search terms for work environment but not for specific work environment risks. We tried to develop such search terms, but because it was impossible to draw the line between which ones to include and which ones to leave out, we decided to only use broader terms. Although this was the most feasible solution, it means that if a study did not include search terms for work environment while still investigating an aspect of this, it was not included in the present review (see the search strategy in Appendix A).
The inclusion of different study designs in the present review provided a nuanced picture of current research but made the evidence more difficult to synthesize. The results across studies with different designs, however, were overall coherent and pointed in the same direction. Using the MMAT meant that an assessment of studies with different designs was parsimonious but possibly not thorough enough to capture all important aspects of methodological quality. It did not, for example, include an assessment of causality. While this assessment tool matched the quality of the evidence of the research field at the time the search was conducted, it also means that the bar for a study to qualify as medium or high quality was quite low.
4.5. Implications for Future Research
Based on the identified knowledge gaps, longitudinal studies are needed to assess the work environment and employee health over time during and after epidemics or pandemics. It is evident that the work environment and employee mental health were affected among healthcare personnel during the acute phases of the pandemic, particularly those working in the frontline, but research on the long-term effects on health after the pandemic is over appears crucial. Preferably, studies could make use of data on work environment factors and health collected before epidemics and follow the samples during and after pandemics, building up longitudinal data to study changes in these measures over time. Intervention studies aimed at mitigating the negative effects on the work environment and employee health are important to inform policy development in case of future epidemics and pandemics. To increase the quality and comparability of studies of the work environment during pandemics and epidemics, validated measures of work exposure and health outcomes need to be used and confounders carefully accounted for in statistical analyses. Finally, more research focusing on industries other than healthcare is needed. Examples are the educational industry, also widely affected by the pandemic, and the service and culture sectors (that were affected economically) and many white-collar industries in which workers quickly transitioned from office to remote work.
5. Conclusions
During the first months of the COVID-19 pandemic, a large number of cross-sectional studies, quantitative and qualitative, on the work environment and health, mainly within the healthcare industry, were published. The weak study designs and overall low methodological quality limited the opportunity to learn about the long-term health effects of changes in the work environment during the pandemic. However, there was a remarkable accordance in the results of the situation in the healthcare industry from studies spanning several continents and using different methodologies, painting a picture of increased quantitative and qualitative demands, lack of personal and organizational resources to meet these demands, fear among personnel of being infected, and experienced stigma related to work with infected patients.
5.1. Practical Implications
The possible long-term health effects of the increased demands and limited resources that have characterized the work environment for healthcare employees during acute phases of the COVID-19 pandemic need to be followed up clinically and in research.
5.2. Key Messages
- The work environment and mental health were strongly affected in healthcare employees during the first months of the COVID-19 pandemic.
- Longitudinal studies are needed to evaluate the possible long-term consequences of severe and long-lasting stressors in the work environment during the COVID-19 pandemic within healthcare.
- Studies evaluating the effects of interventions aiming to improve the work environment and mitigate negative health effects are needed to prepare for future pandemics.
- Studies of higher quality with regards to sampling strategies, exposure and outcome measurements, control of possible confounders, etc. are needed to move the research field forward.
- Studies from industries outside healthcare are needed to obtain a broader picture of how pandemics affect the work environment of entire labor markets.
Author Contributions
A.N. was the PI of the study, lead the work, participated in all phases of the systematic review, and drafted the manuscript together with I.D. K.R. took part in all phases of the systematic review, developed the Excel sheets for the selection process and quality assessment, contributed with methodological expertise, and read and commented on early drafts of the manuscript. I.D. took part in all phases of the systematic review, was responsible for the quality assessment of qualitative and mixed methods studies, and drafted the manuscript together with A.N. All authors have read and agreed to the published version of the manuscript.
Funding
The systematic review was commissioned by the Swedish Agency for Work Environment Expertise (no 20/00187).
Institutional Review Board Statement
Not applicable.
Informed Consent Statement
Not applicable.
Data Availability Statement
Not applicable.
Acknowledgments
We would like to thank Agnes Kotka at the University Library at Uppsala University for support in developing the search strategy, conducting the database searches and delivering the selected studies to the review team. Ylva Lindberg and Wilhelm Linder contributed in the early phase of the systematic review process by assessing articles in the search results for inclusion and exclusion criteria. Ulrika Winblad consulted the core review team in the quality assessment of qualitative and mixed methods studies.
Conflicts of Interest
The authors declare that there is no conflict of interest.
Appendix A. Search Strategy

Table A1.
Database: Cinahl (via Ebsco) Date: 5 October 2020.
Table A1.
Database: Cinahl (via Ebsco) Date: 5 October 2020.
| Search nr | Search Term | Results |
|---|---|---|
| Population: working population | ||
| #1 | Employees [MH+] | 678 |
| #2 | Industry [MH+] | 49,859 |
| #3 | Health Occupations [MH+] | 755,520 |
| #4 | Occupations and Professions [MH+] | 97,601 |
| #5 | Women, Working [MH+] | 4309 |
| #6 | Work [MH+] | 7345 |
| #7 | Company OR Employ * OR Industry OR Job OR “Occupational group *” OR Occupations OR Personnel OR Staff OR Work * [Title/Abstract] | 710,991 |
| #8 | #1 OR #2 OR #3 OR #4 OR #5 OR #6 OR #7 | 1,647,557 |
| Intervention: Occupational health in the context of coronavirus | ||
| #9 | Coronavirus [MH+] | 10,073 |
| #10 | Coronavirus Infections [MH+] | 17,917 |
| #11 | COVID-19 [MH+] | 8752 |
| #12 | Middle East Respiratory Syndrome Coronavirus [MH+] | 425 |
| #13 | SARS Virus [MH+] | 312 |
| #14 | Severe Acute Respiratory Syndrome [MH+] | 2293 |
| #15 | Corona OR Coronavirus OR cov2 OR COVID19 OR COVID-19 OR MERS OR SARS OR 2019-nCoV * OR “2019-nCoV infection *” [Title/Abstract] | 22,197 |
| #16 | #9 OR #10 OR #11 OR #12 OR #13 OR #14 OR #15 | 26,523 |
| #17 | Occupational Diseases [MH+] | 39,966 |
| #18 | Occupational Health [MH+] | 62,588 |
| #19 | Occupational Health Nursing [MH+] | 4552 |
| #20 | Occupational Health Services [MH+] | 7659 |
| #21 | Occupational Medicine [MH+] | 459 |
| #22 | Occupational Safety [MH+] | 20,833 |
| #23 | Psychosocial Factors [MH+] | 722 |
| #24 | Psychosocial Aspects of Illness [MH+] | 197,113 |
| #25 | Work Environment [MH+] | 33,011 |
| #26 | Workload [MH+] | 15,717 |
| #27 | Work Related Illnesses [MH+] | 476 |
| #28 | Occupational Disease * OR Occupational Health OR Occupational Medicine OR Psychosocial OR Psycho-social OR Stressor * OR (Work OR Working) N3 (Condition * OR Environment * OR Related OR Load) OR Workload [Title/Abstract] | 125,105 |
| #29 | 17 OR 18 OR 19 OR 20 OR 21 OR 22 OR 23 OR 24 OR 25 OR 26 OR 27 OR 28 | 883,355 |
| #30 | #8 AND #16 AND #29 | 2451 |
[MH+] = Subject heading, exploded. [Title/Abstract] = Title or abstract. * = Truncation.

Table A2.
Database: PsycInfo (via Ebsco) Date: 20201005.
Table A2.
Database: PsycInfo (via Ebsco) Date: 20201005.
| Search nr | Search Term | Results |
|---|---|---|
| Population: working population | ||
| #1 | Occupations [DE] | 12,145 |
| #2 | Personnel [DE] | 10,757 |
| #3 | Work Teams [DE] | 5151 |
| #4 | Working Women [DE] | 6477 |
| #5 | Company OR Employ * OR Industry OR Job OR “Occupational group *” OR Occupations OR Personnel OR Staff OR Work * [Title/Abstract] | 1,042,507 |
| #6 | #1 OR #2 OR #3 OR #4 OR #5 | 1,290,435 |
| Intervention: Occupational health in the context of coronavirus | ||
| #7 | Coronavirus [DE] | 1006 |
| #8 | Middle East Respiratory Syndrome [DE] | 24 |
| #9 | Severe Acute Respiratory Syndrome [DE] | 260 |
| #10 | corona OR coronavirus OR cov2 OR COVID19 OR COVID-19 OR MERS OR SARS OR 2019-nCoV * OR “2019-nCoV infection *” [Title/Abstract] | 3503 |
| #11 | #7 OR #8 OR #9 OR #10 | 4164 |
| #12 | Occupational Health [DE] | 5907 |
| #13 | Occupational Safety [DE] | 3649 |
| #14 | Psychosocial Factors [DE] | 34,687 |
| #15 | Psychosocial Outcomes [DE] | 233 |
| #16 | Working Conditions [DE] | 23,362 |
| #17 | Work Related Illnesses [DE] | 1070 |
| #18 | Occupational disease * OR Occupational Health OR Occupational Medicine OR Psychosocial OR Psycho-social OR Stressor * OR (Work OR Working) N3 (Condition * OR Environment * OR Related OR Load) OR Workload [Title/Abstract] | 172,647 |
| #19 | 12 OR 13 OR 14 OR 15 OR 16 OR 17 OR 18 | 350,431 |
| #20 | #6 AND #11 #AND #19 | 235 |
[DE] = Thesaurus of Psychological Index Term. [Title/Abstract] = Title or abstract. * = Truncation.

Table A3.
Database: Pubmed (via NCBI) Date: 2020105.
Table A3.
Database: Pubmed (via NCBI) Date: 2020105.
| Search nr | Search Term | Results |
|---|---|---|
| Population: working population | ||
| #1 | Employment [MeSH Terms] | 87,290 |
| #2 | Industry [MeSH Terms] | 316,795 |
| #3 | Occupational Groups [MeSH Terms] | 610,845 |
| #4 | Occupations [MeSH Terms] | 34,444 |
| #5 | Women, working [MeSH Terms] | 5375 |
| #6 | Work [MeSH Terms] | 63,870 |
| #7 | Workplace [MeSH Terms] | 23,230 |
| #8 | Company OR Employ * OR Industry OR Job OR “Occupational group *” OR Occupations OR Personnel OR Staff OR Work * [Title/Abstract] | 2,340,428 |
| #9 | #1 OR #2 OR #3 OR #4 OR #5 OR #6 OR #7 OR #8 | 3,057,511 |
| Intervention: Occupational health in the context of coronavirus | ||
| #10 | Coronavirus Infections [MeSH Terms] | 38,313 |
| #11 | SARS Virus [MeSH Terms] | 3555 |
| #12 | Corona OR Coronavirus OR cov2 OR COVID19 OR COVID-19 OR MERS OR SARS OR 2019-nCoV * OR “2019-nCoV infection *” [Title/Abstract] | 83,910 |
| #13 | #10 OR #11 OR #12 | 87,768 |
| #14 | Occupational Diseases [MeSH Terms] | 132,343 |
| #15 | Occupational Health [MeSH Terms] | 33,662 |
| #16 | Occupational Health Services [MeSH Terms] | 10,554 |
| #17 | Occupational Medicine [MeSH Terms] | 23,330 |
| #18 | Occupational Health Nursing [MeSH Terms] | 4390 |
| #19 | Workload [MeSH Terms] | 21,538 |
| #20 | Occupational disease * OR Occupational Health OR Occupational Medicine OR Psychosocial OR Psycho-social OR Stressor * OR Work Condition * OR Working Condition * OR Work Environment * OR Working Environment * OR Workload OR Work load OR Work related [Title/Abstract] | 232,828 |
| #21 | #14 OR #15 OR #16 OR #17 OR #18 OR #19 OR #20 | 395,316 |
| #22 | #9 AND #13 AND #21 | 1043 |
[MeSH] = Term from the Medline controlled vocabulary, including terms found below this term in the MeSH hierarchy. Title/Abstract] = Title or abstract. * = Truncation.

Table A4.
Database: Web of Science Date: 2020105.
Table A4.
Database: Web of Science Date: 2020105.
| Population: working population | ||
| #1 | Company OR Employ * OR Industry OR Job OR “Occupational group *” OR Occupations OR Personnel OR Staff OR Work * [Topic] | 6,936,326 |
| Intervention: Occupational health in the context of coronavirus | ||
| #2 | Corona OR Coronavirus OR cov2 OR COVID19 OR COVID-19 OR MERS OR SARS OR 2019-nCoV * OR “2019-nCoV infection *” [Topic] | 133,497 |
| #3 | Occupational Disease * OR Occupational Health OR Occupational Medicine OR Psychosocial OR Psycho-social OR Stressor * OR (“Work” or “Working”) NEAR/3 (Condition * OR Environment * OR Related OR Load) OR Workload [Topic] | 459,304 |
| #4 | #1 AND #2 AND #3 | 844 |
[Topic] = Title, Abstract, Author Keywords, Keywords Plus. * = Truncation.
Quality assessment
Mixed Methods Appraisal Tool (MMAT) 2018, [14], an instrument developed for the quality assessment in systematic reviews including original articles with different research designs, was used. The criteria are listed below.
For quantitative non-randomized studies:
(1) If the participants are representative of the target population, (2) if the measurements for outcome and exposure are appropriate, (3) if outcome data is complete (referring to dropout), (4) if relevant confounders are accounted for, and (5) during the study period, if intervention/exposure occurred as intended.
For quantitative randomized controlled trials:
(1) If randomization was appropriately performed, (2) if the groups are comparable at baseline, (3) if there is complete outcome data, (4) if outcome assessors are blinded to the intervention provided, and (5) if the participants adhered to the assigned intervention.
For qualitative studies:
(1) If the qualitative approach is appropriate to answer the research questions, (2) if the data collection methods are adequate to address the research question, (3) if the findings are adequately derived from the data, (4) if the interpretation of the results is sufficiently substantiated by the data, and (5) if there is coherence between qualitative data sources, collection, analysis, and interpretation
For mixed-methods studies:
(1) If there is an adequate rationale for using a mixed-methods design to address the research questions, (2) if the different components of the study are effectively integrated to answer the research question, (3) if the outputs of the integration of qualitative and quantitative components are adequately interpreted, (4) if divergences and inconsistencies between quantitative and qualitative results are adequately addressed, and (5) if the different components of the study adhere to the quality criteria of each tradition of the methods involved.
We adjusted the quality assessment criteria for quantitative non-randomized studies. Because the last criterium (during the study period, if intervention/exposure occurred as intended) was not relevant for cross-sectional studies, which is the majority of the included studies, we did not consider this criterion in our quality assessment. Thus, only four criteria were used for quantitative non-randomized studies.
The core research team developed a procedure to rate the overall quality of each study as low, medium, or high. The aim was both to identify studies of low quality to exclude these from our analysis and conclusions, and to obtain an overall picture of the quality of the included research. In this procedure, we considered each study design separately and came to the following criteria for the overall study quality.
For quantitative non-randomized studies:
High quality = 4 yes, Medium quality = 2–3 yes, Low quality = 1 yes.
For quantitative randomized controlled trials:
High quality = 5 yes, Medium quality = 3–4 yes, Low quality = 1–2 yes.
For qualitative and mixed methods studies:
High quality = 5 yes, Medium quality = 3–4 yes, Low quality = 1–2 yes.
References
- WHO Director-General’s Opening Remarks at the Media Briefing on COVID-19—11 March 2020. Available online: https://www.who.int/director-general/speeches/detail/who-director-general-s-opening-remarks-at-the-media-briefing-on-COVID-19---11-march-2020 (accessed on 1 February 2021).
- Bandyopadhyay, S.; Baticulon, R.E.; Kadhum, M.; Alser, M.; Ojuka, D.K.; Badereddin, Y.; Kamath, A.; Parepalli, S.A.; Brown, G.; Iharchane, S.; et al. Infection and mortality of healthcare workers worldwide from COVID-19: A systematic review. BMJ Glob. Health 2020, 5, e003097. [Google Scholar] [CrossRef] [PubMed]
- Chen, Y.H.; Glymour, M.; Riley, A.; Balmes, J.; Duchowny, K.; Harrison, R. Excess mortality associated with the COVID-19 pandemic among Californians 18-65 years of age, by occupational sector and occupation: March through November 2020. PLoS ONE 2021, 16, e0252454. [Google Scholar] [CrossRef] [PubMed]
- Burdorf, A.; Porru, F.; Rugulies, R. The COVID-19 pandemic: One year later—An occupational perspective. Scand. J. Work. Environ. Health 2021, 47, 245–247. [Google Scholar] [CrossRef] [PubMed]
- Sigahi, T.F.A.C.; Kawasaki, B.C.; Bolis, I.; Morioka, S.N. A systematic review on the impacts of Covid-19 on work: Contributions and a path forward from the perspectives of ergonomics and psychodynamics of work. Hum. Factors Ergon. Manuf. Serv. Ind. 2021, 31, 375–388. [Google Scholar] [CrossRef]
- Gualano, M.R.; Sinigaglia, T.; Lo Moro, G.; Rousset, S.; Cremona, A.; Bert, F. The Burden of Burnout among Healthcare Profes-sionals of Intensive Care Units and Emergency Departments during the COVID-19 Pandemic: A Systematic Review. Int. J. Environ. Res. Public Health 2021, 18, 8172. [Google Scholar] [CrossRef]
- Galanis, P.; Vraka, I.; Fragkou, D.; Bilali, A.; Kaitelidou, D. Impact of personal protective equipment use on health care workers’ physical health during the COVID-19 pandemic: A systematic review and meta-analysis. Am. J. Infect. Control 2021, 49, 1305–1315. [Google Scholar] [CrossRef]
- Rieckert, A.; Schuit, E.; Bleijenberg, N.; Cate, D.T.; De Lange, W.; Ginkel, J.M.D.M.-V.; Mathijssen, E.; Smit, L.C.; Stalpers, D.; Schoonhoven, L.; et al. How can we build and maintain the resilience of our health care professionals during COVID-19? Recommendations based on a scoping review. BMJ Open 2021, 11, e043718. [Google Scholar] [CrossRef]
- Fan, J.; Senthanar, S.; Macpherson, R.; Sharpe, K.; Peters, C.; Koehoorn, M.; McLeod, C. An Umbrella Review of the Work and Health Impacts of Working in an Epidemic/Pandemic Environment. Int. J. Environ. Res. Public Health 2021, 18, 6828. [Google Scholar] [CrossRef]
- Turner, S.; Botero-Tovar, N.; Herrera, M.A.; Kuhlmann, J.P.B.; Ortiz, F.; Ramírez, J.C.; Maldonado, L.F. Systematic review of experiences and perceptions of key actors and organisations at multiple levels within health systems internationally in responding to COVID-19. Implement. Sci. 2021, 16, 50. [Google Scholar] [CrossRef]
- Sharifi, M.; Asadi-Pooya, A.A.; Mousavi-Roknabadi, R.S. Burnout among Healthcare Providers of COVID-19; A Systematic Review of Epidemiology and Recommendations: Burnout in healthcare providers. Arch. Acad. Emerg. Med. 2020, 9, e7. [Google Scholar] [CrossRef]
- Gross, J.V.; Mohren, J.; Erren, T.C. COVID-19 and healthcare workers: A rapid systematic review into risks and preventive measures. BMJ Open 2021, 11, e042270. [Google Scholar] [CrossRef] [PubMed]
- Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA). Available online: www.prisma-statement.org (accessed on 5 October 2020).
- Hong, Q.N.; Fàbregues, S.; Bartlett, G.; Boardman, F.; Cargo, M.; Dagenais, P.; Gagnon, M.-P.; Griffiths, F.; Nicolau, B.; O’Cathain, A.; et al. The Mixed Methods Appraisal Tool (MMAT) version 2018 for information professionals and researchers. Educ. Inf. 2018, 34, 285–291. [Google Scholar] [CrossRef]
- Hoffman, K.E.; Garner, D.; Koong, A.C.; Woodward, W.A. Understanding the Intersection of Working from Home and Burnout to Optimize Post-COVID19 Work Arrangements in Radiation Oncology. Int. J. Radiat. Oncol. 2020, 108, 370–373. [Google Scholar] [CrossRef] [PubMed]
- Xie, H.; Cheng, X.; Song, X.; Wu, W.; Chen, J.; Xi, Z.; Shou, K. Investigation of the Psychological disorders in the healthcare nurses during a coronavirus disease 2019 outbreak in China. Medicine 2020, 99, e21662. [Google Scholar] [CrossRef] [PubMed]
- Khalid, I.; Khalid, T.J.; Qabajah, M.R.; Barnard, A.G.; Qushmaq, I.A. Healthcare Workers Emotions, Perceived Stressors and Coping Strategies During a MERS-CoV Outbreak. Clin. Med. Res. 2016, 14, 7–14. [Google Scholar] [CrossRef] [PubMed]
- Koksal, E.; Dost, B.; Terzi, Ö.; Ustun, Y.B.; Özdin, S.; Bilgin, S. Evaluation of Depression and Anxiety Levels and Related Factors Among Operating Theater Workers During the Novel Coronavirus (COVID-19) Pandemic. J. PeriAnesthesia Nurs. 2020, 35, 472–477. [Google Scholar] [CrossRef]
- Kuo, F.; Yang, P.; Hsu, H.; Su, C.; Chen, C.; Yeh, I.; Wu, Y.; Chen, L. Survey on perceived work stress and its influencing factors among hospital staff during the COVID -19 pandemic in Taiwan. Kaohsiung J. Med Sci. 2020, 36, 944–952. [Google Scholar] [CrossRef]
- Maraqa, B.; Nazzal, Z.; Zink, T. Palestinian Health Care Workers’ Stress and Stressors during COVID-19 Pandemic: A Cross-Sectional Study. J. Prim. Care Community Health 2020, 11, 2150132720955026. [Google Scholar] [CrossRef]
- Rodriguez, R.M.; Medak, A.J.; Baumann, B.M.; Lim, S.; Chinnock, B.; Frazier, R. Academic Emergency Medicine Physicians’ Anxiety Levels, Stressors, and Potential Stress Mitigation Measures During the Acceleration Phase of the COVID-19 Pandemic. Acad. Emerg. Med. 2020, 27, 700–707. [Google Scholar] [CrossRef]
- Bhatnagar, S.; Sarma, R.; Vig, S.; Rathore, P.; Pushpam, D.; Mishra, S.; Gupta, N.; Garg, R.; Kumar, V.; Bharati, S.J. Concerns of health care professionals managing non-COVID patients during the COVID-19 pandemic: A descriptive cross-sectional study. Indian J. Palliat. Care 2020, 26, S21–S26. [Google Scholar] [CrossRef]
- Semaan, A.; Audet, C.; Huysmans, E.; Afolabi, B.; Assarag, B.; Banke-Thomas, A.; Blencowe, H.; Caluwaerts, S.; Campbell, O.M.R.; Cavallaro, F.L.; et al. Voices from the frontline: Findings from a thematic analysis of a rapid online global survey of maternal and newborn health professionals facing the COVID-19 pandemic. BMJ Glob. Health 2020, 5, e002967. [Google Scholar] [CrossRef]
- Shalhub, S.; Mouawad, N.J.; Malgor, R.D.; Johnson, A.P.; Wohlauer, M.V.; Coogan, S.M. Global vascular surgeons experience, stressors, and coping during the COVID-19 pandemic. J. Vasc. Surg. 2020, 73, 762–771.e4. [Google Scholar] [CrossRef] [PubMed]
- Singh, M.; Pawar, M.; Bothra, A.; Maheshwari, A.; Dubey, V.; Tiwari, A. Personal protective equipment induced facial der-matoses in healthcare workers managing Coronavirus disease 2019. J. Eur. Acad. Dermatol. Venereol. 2020, 34, e378–e380. [Google Scholar] [CrossRef] [PubMed]
- Tabah, A.; Ramanan, M.; Laupland, K.B.; Buetti, N.; Cortegiani, A.; Mellinghoff, J.; Conway Morris, A.; Camporota, L.; Zappella, N.; Elhadi, M.; et al. Personal protective equipment and intensive care unit healthcare worker safety in the COVID-19 era (PPE-SAFE): An international survey. J. Crit. Care 2020, 59, 70–75. [Google Scholar] [CrossRef]
- Zhang, M.; Zhou, M.; Tang, F.; Wang, Y.; Nie, H.; Zhang, L.; You, G. Knowledge, attitude, and practice regarding COVID-19 among healthcare workers in Henan, China. J. Hosp. Infect. 2020, 105, 183–187. [Google Scholar] [CrossRef]
- Zhang, S.X.; Sun, S.; Afshar Jahanshahi, A.; Alvarez-Risco, A.; Ibarra, V.G.; Li, J. Developing and testing a measure of COVID-19 organizational support of healthcare workers—Results from Peru, Ecuador, and Bolivia. Psychiatry Res. 2020, 291, 113174. [Google Scholar] [CrossRef] [PubMed]
- Zhang, Y.; Wei, L.; Li, H.; Pan, Y.; Wang, J.; Li, Q.; Wu, Q.; Wei, H. The Psychological Change Process of Frontline Nurses Caring for Patients with COVID-19 during Its Outbreak. Issues Ment. Health Nurs. 2020, 41, 525–530. [Google Scholar] [CrossRef] [PubMed]
- Algunmeeyn, A.; El-Dahiyat, F.; Altakhineh, M.M.; Azab, M.; Babar, Z.U. Understanding the factors influencing healthcare pro-viders’ burnout during the outbreak of COVID-19 in Jordanian hospitals. J. Pharm. Policy Pract. 2020, 13, 53. [Google Scholar] [CrossRef]
- Craig, L.; Churchill, B. Dual-earner parent couples’ work and care during COVID-19. Gend. Work. Organ. 2020, 28, 66–79. [Google Scholar] [CrossRef]
- Deguchi, M.; Chie, M. Voices of Sanitation Workers in Japan amidst the COVID-19 Pandemic. Asia-Pac. J. Jpn. Focus. 2020, 18, 5485. [Google Scholar]
- Molino, M.; Ingusci, E.; Signore, F.; Manuti, A.; Giancaspro, M.L.; Russo, V.; Zito, M.; Cortese, C.G. Wellbeing Costs of Technology Use during Covid-19 Remote Working: An Investigation Using the Italian Translation of the Technostress Creators Scale. Sustainability 2020, 12, 5911. [Google Scholar] [CrossRef]
- Moretti, A.; Menna, F.; Aulicino, M.; Paoletta, M.; Liguori, S.; Iolascon, G. Characterization of Home Working Population during COVID-19 Emergency: A Cross-Sectional Analysis. Int. J. Environ. Res. Public Health 2020, 17, 6284. [Google Scholar] [CrossRef] [PubMed]
- Saqib, A.; Rampal, T. Quality improvement report: Setting up a staff well-being hub through continuous engagement. BMJ Open Qual. 2020, 9, e001008. [Google Scholar] [CrossRef] [PubMed]
- Sethi, B.A.; Sethi, A.; Ali, S.; Aamir, H.S. Impact of Coronavirus disease (COVID-19) pandemic on health professionals. Pak. J. Med. Sci. 2020, 36, S6–S11. [Google Scholar] [CrossRef]
- Stirling, B.V.; Harmston, J.; Alsobayel, H. An educational programme for nursing college staff and students during a MERS- coronavirus outbreak in Saudi Arabia. BMC Nurs. 2015, 14, 20. [Google Scholar] [CrossRef] [PubMed]
- Yildirim, T.M.; Eslen-Ziya, H. The differential impact of COVID-19 on the work conditions of women and men academics during the lockdown. Gender Work Organ. 2020, 28, 243–249. [Google Scholar] [CrossRef]
- Felice, C.; Di Tanna, G.L.; Zanus, G.; Grossi, U. Impact of COVID-19 Outbreak on Healthcare Workers in Italy: Results from a National E-Survey. J. Community Health 2020, 45, 675–683. [Google Scholar] [CrossRef]
- Halcomb, E.; McInnes, S.; Williams, A.; Ashley, C.; James, S.; Fernandez, R.; Calma, K. The Experiences of Primary Healthcare Nurses during the COVID-19 Pandemic in Australia. J. Nurs. Sch. 2020, 52, 553–563. [Google Scholar] [CrossRef]
- Koh, D.; Lim, M.K.; Chia, S.E.; Ko, S.M.; Qian, F.; Ng, V. Risk perception and impact of Severe Acute Respiratory Syndrome (SARS) on work and personal lives of healthcare workers in Singapore: What can we learn? Med. Care 2005, 43, 676–682. [Google Scholar] [CrossRef]
- Kramer, V.; Papazova, I.; Thoma, A.; Kunz, M.; Falkai, P.; Schneider-Axmann, T.; Hierundar, A.; Wagner, E.; Hasan, A. Subjective burden and perspectives of German healthcare workers during the COVID-19 pandemic. Eur. Arch. Psychiatry Clin. Neurosci. 2020, 271, 271–281. [Google Scholar] [CrossRef]
- Smrke, A.; Younger, E.; Wilson, R.; Husson, O.; Farag, S.; Merry, E.; Macklin-Doherty, A.; Cojocaru, E.; Arthur, A.; Benson, C.; et al. Telemedicine During the COVID-19 Pandemic: Impact on Care for Rare Cancers. JCO Glob. Oncol. 2020, 6, 1046–1051. [Google Scholar] [CrossRef]
- Spiller, T.R.; Méan, M.; Ernst, J.; Sazpinar, O.; Gehrke, S.; Paolercio, F. Development of health care workers’ mental health during the SARS-CoV-2 pandemic in Switzerland: Two cross-sectional studies. Psychol. Med. 2020, 1–4. [Google Scholar] [CrossRef] [PubMed]
- Teoh, J.Y.-C.; Ong, W.L.K.; González, D.; Castellani, D.; Dubin, J.M.; Esperto, F.; Campi, R.; Gudaru, K.; Talwar, R.; Okhunov, Z.; et al. A Global Survey on the Impact of COVID-19 on Urological Services. Eur. Urol. 2020, 78, 265–275. [Google Scholar] [CrossRef]
- Tolomiczenko, G.S.; Kahan, M.; Ricci, M.; Strathern, L.; Jeney, C.; Patterson, K.; Wilson, L. SARS: Coping with the impact at a community hospital. J. Adv. Nurs. 2005, 50, 101–110. [Google Scholar] [CrossRef]
- Bai, Y.; Lin, C.C.; Lin, C.Y.; Chen, J.Y.; Chue, C.M.; Chou, P. Survey of stress reactions among health care workers involved with the SARS outbreak. Psychiatr. Serv. 2004, 55, 1055–1057. [Google Scholar] [CrossRef] [PubMed]
- Buselli, R.; Corsi, M.; Baldanzi, S.; Chiumiento, M.; Del Lupo, E.; Dell’Oste, V.; Bertelloni, C.A.; Massimetti, G.; Dell’Osso, L.; Cristaudo, A.; et al. Professional Quality of Life and Mental Health Outcomes among Health Care Workers Exposed to Sars-Cov-2 (Covid-19). Int. J. Environ. Res. Public Health 2020, 17, 6180. [Google Scholar] [CrossRef] [PubMed]
- De Sio, S.; Buomprisco, G.; La Torre, G.; Lapteva, E.; Perri, R.; Greco, E. The impact of COVID-19 on doctors’ well-being: Results of a web survey during the lockdown in Italy. Eur. Rev. Med. Pharmacol. Sci. 2020, 24, 7869–7879. [Google Scholar] [PubMed]
- Elbay, R.Y.; Kurtulmuş, A.; Arpacıoğlu, S.; Karadere, E. Depression, anxiety, stress levels of physicians and associated factors in Covid-19 pandemics. Psychiatry Res. 2020, 290, 113130. [Google Scholar] [CrossRef]
- Evanoff, B.A.; Strickland, J.R.; Dale, A.M.; Hayibor, L.; Page, E.; Duncan, J.G. Work-Related and Personal Factors Associated with Mental Well-Being During the COVID-19 Response: Survey of Health Care and Other Workers. J. Med. Internet Res. 2020, 22, e21366. [Google Scholar] [CrossRef]
- Fiksenbaum, L.; Greenglass, E.R.; Marjanovic, Z.; Coffey, S. Emotional Exhaustion and State Anger in Nurses Who Worked During the Sars Outbreak: The Role of Perceived Threat and Organizational Support. Can. J. Community Ment. Health 2006, 25, 89–103. [Google Scholar] [CrossRef]
- Hacimusalar, Y.; Kahve, A.C.; Yasar, A.B.; Aydin, M.S. Anxiety and hopelessness levels in COVID-19 pandemic: A comparative study of healthcare professionals and other community sample in Turkey. J. Psychiatr. Res. 2020, 129, 181–188. [Google Scholar] [CrossRef] [PubMed]
- Han, L.; Wong, F.K.Y.; She, D.L.M.; Li, S.Y.; Yang, Y.F.; Jiang, M.Y.; Ruan, Y.; Su, Q.; Ma, Y.; Chung, L.Y.F. Anxiety and Depression of Nurses in a North West Province in China During the Period of Novel Coronavirus Pneumonia Outbreak. J. Nurs. Sch. 2020, 52, 564–573. [Google Scholar] [CrossRef]
- Hoseinabadi, T.S.; Kakhki, S.; Teimori, G.; Nayyeri, S. Burnout and its influencing factors between frontline nurses and nurses from other wards during the outbreak of Coronacvirus Disease—COVID-19 in Iran. Nurs. Res. Educ. 2020, 38, e03. [Google Scholar]
- Huang, L.; Wang, Y.; Liu, J.; Ye, P.; Chen, X.; Xu, H.; Qu, H.; Ning, G. Factors Influencing Anxiety of Health Care Workers in the Radiology Department with High Exposure Risk to COVID-19. Med Sci. Monit. 2020, 26, e926008-1. [Google Scholar] [CrossRef]
- Jung, H.; Jung, S.Y.; Lee, M.H.; Kim, M.S. Assessing the Presence of Post-Traumatic Stress and Turnover Intention among Nurses Post–Middle East Respiratory Syndrome Outbreak: The Importance of Supervisor Support. Work. Health Saf. 2020, 68, 337–345. [Google Scholar] [CrossRef] [PubMed]
- Khalafallah, A.M.; Lam, S.; Gami, A.; Dornbos, D.L.; Sivakumar, W.; Johnson, J.N. Burnout and career satisfaction among attending neurosurgeons during the COVID-19 pandemic. Clin. Neurol. Neurosurg. 2020, 198, 106193. [Google Scholar] [CrossRef] [PubMed]
- Khanal, P.; Devkota, N.; Dahal, M.; Paudel, K.; Joshi, D. Mental health impacts among health workers during COVID-19 in a low resource setting: A cross-sectional survey from Nepal. Glob. Health 2020, 16, 89. [Google Scholar] [CrossRef]
- Kim, J.-S.; Choi, J.S. Factors Influencing Emergency Nurses’ Burnout during an Outbreak of Middle East Respiratory Syndrome Coronavirus in Korea. Asian Nurs. Res. 2016, 10, 295–299. [Google Scholar] [CrossRef]
- Lam, S.C.; Arora, T.; Grey, I.; Suen, L.K.P.; Huang, E.Y.-Z.; Li, D.; Lam, K.B.H. Perceived Risk and Protection From Infection and Depressive Symptoms Among Healthcare Workers in Mainland China and Hong Kong During COVID-19. Front. Psychiatry 2020, 11, 686. [Google Scholar] [CrossRef]
- Lancee, W.J.; Maunder, R.G.; Goldbloom, D.S. Prevalence of psychiatric disorders among Toronto hospital workers one to two years after the SARS outbreak. Psychiatr. Serv. 2008, 59, 91–95. [Google Scholar] [CrossRef]
- Lee, S.M.; Kang, W.S.; Cho, A.-R.; Kim, T.; Park, J.K. Psychological impact of the 2015 MERS outbreak on hospital workers and quarantined hemodialysis patients. Compr. Psychiatry 2018, 87, 123–127. [Google Scholar] [CrossRef] [PubMed]
- Luceño-Moreno, L.; Talavera-Velasco, B.; García-Albuerne, Y.; Martín-García, J. Symptoms of Posttraumatic Stress, Anxiety, Depression, Levels of Resilience and Burnout in Spanish Health Personnel during the COVID-19 Pandemic. Int. J. Environ. Res. Public Health 2020, 17, 5514. [Google Scholar] [CrossRef] [PubMed]
- Marjanovic, Z.; Greenglass, E.R.; Coffey, S. The relevance of psychosocial variables and working conditions in predicting nurses’ coping strategies during the SARS crisis: An online questionnaire survey. Int. J. Nurs. Stud. 2007, 44, 991–998. [Google Scholar] [CrossRef] [PubMed]
- Matsuo, T.; Kobayashi, D.; Taki, F.; Sakamoto, F.; Uehara, Y.; Mori, N.; Fukui, T. Prevalence of Health Care Worker Burnout during the Coronavirus Disease 2019 (COVID-19) Pandemic in Japan. JAMA Netw. Open 2020, 3, e2017271. [Google Scholar] [CrossRef] [PubMed]
- Maunder, R.G.; Lancee, W.J.; Balderson, K.E.; Bennett, J.P.; Borgundvaag, B.; Evans, S.; Fernandes, C.M.; Goldbloom, D.S.; Gupta, M.; Hunter, J.J.; et al. Long-term psychological and occupa-tional effects of providing hospital healthcare during SARS outbreak. Emerg. Infect. Dis. 2006, 12, 1924–1932. [Google Scholar] [CrossRef]
- Mo, Y.; Deng, L.; Zhang, L.; Lang, Q.; Liao, C.; Wang, N.; Qin, M.; Huang, H. Work stress among Chinese nurses to support Wuhan in fighting against COVID-19 epidemic. J. Nurs. Manag. 2020, 28, 1002–1009. [Google Scholar] [CrossRef]
- Monterrosa-Castro, A.; Redondo-Mendoza, V.; Lara, M.F.M. Psychosocial factors associated with symptoms of generalized anxiety disorder in general practitioners during the COVID-19 pandemic. J. Investig. Med. 2020, 68, 1228–1234. [Google Scholar] [CrossRef]
- Morgantini, L.A.; Naha, U.; Wang, H.; Francavilla, S.; Acar, Ö.; Flores, J.M.; Crivellaro, S.; Moreira, D.; Abern, M.; Eklund, M.; et al. Factors contributing to healthcare professional burnout during the COVID-19 pandemic: A rapid turnaround global survey. PLoS ONE 2020, 15, e0238217. [Google Scholar] [CrossRef]
- Mosheva, M.; Hertz-Palmor, N.; Dorman Ilan, S.; Matalon, N.; Pessach, I.M.; Afek, A.; Ziv, A.; Kreiss, Y.; Gross, R.; Gothelf, D. Anxiety, pandemic-related stress and resilience among physicians during the COVID-19 pandemic. Depress. Anxiety 2020, 37, 965–971. [Google Scholar] [CrossRef]
- Nickell, L.A.; Crighton, E.J.; Tracy, C.S.; Al-Enazy, H.; Bolaji, Y.; Hanjrah, S.; Hussain, A.; Makhlouf, S.; Upshur, R.E. Psychosocial effects of SARS on hospital staff: Survey of a large tertiary care institution. Can. Med. Assoc. J. 2004, 170, 793–798. [Google Scholar] [CrossRef]
- Pratt, M.; Kerr, M.; Wong, C. The impact of ERI, burnout, and caring for SARS patients on hospital nurses’ self-reported compliance with infection control. Can. J. Infect. Control 2009, 24, 167–172. [Google Scholar] [PubMed]
- Ramaci, T.; Barattucci, M.; Ledda, C.; Rapisarda, V. Social Stigma during COVID-19 and its Impact on HCWs Outcomes. Sustainability 2020, 12, 3834. [Google Scholar] [CrossRef]
- Rossi, R.; Socci, V.; Pacitti, F.; Di Lorenzo, G.; Di Marco, A.; Siracusano, A.; Rossi, A. Mental Health Outcomes Among Frontline and Second-Line Health Care Workers During the Coronavirus Disease 2019 (COVID-19) Pandemic in Italy. JAMA Netw. Open 2020, 3, e2010185. [Google Scholar] [CrossRef] [PubMed]
- Ruiz-Fernandez, M.D.; Ramos-Pichardo, J.D.; Ibanez-Masero, O.; Cabrera-Troya, J.; Carmona-Rega, M.I.; Ortega-Galan, A.M. Com-passion fatigue, burnout, compassion satisfaction and perceived stress in healthcare professionals during the COVID-19 health crisis in Spain. J. Clin. Nurs. 2020, 29, 4321–4330. [Google Scholar] [CrossRef] [PubMed]
- Sampaio, F.; Sequeira, C.; Teixeira, L. Nurses’ Mental Health during the COVID-19 Outbreak: A Cross-Sectional Study. J. Occup. Environ. Med. 2020, 62, 783–787. [Google Scholar] [CrossRef] [PubMed]
- Saricam, M. COVID-19-Related anxiety in nurses working on front lines in Turkey. Nurs. Midwifery Stud. 2020, 9, 178. [Google Scholar] [CrossRef]
- Shah, N.; Raheem, A.; Sideris, M.; Velauthar, L.; Saeed, F. Mental health amongst obstetrics and gynaecology doctors during the COVID-19 pandemic: Results of a UK-wide study. Eur. J. Obstet. Gynecol. Reprod. Biol. 2020, 253, 90–94. [Google Scholar] [CrossRef]
- Smith, P.M.; Oudyk, J.; Potter, G.; Mustard, C. The Association between the Perceived Adequacy of Workplace Infection Control Procedures and Personal Protective Equipment with Mental Health Symptoms: A Cross-sectional Survey of Canadian Health-care Workers during the COVID-19 Pandemic: L’association entre le caractère adéquat perçu des procédures de con-trôle des infections au travail et de l’équipement de protection personnel pour les symptômes de santé mentale. Un sondage transversal des travailleurs de la santé canadiens durant la pandémie COVID-19. Can. J. Psychiatry 2020, 66, 17–24. [Google Scholar]
- Styra, R.; Hawryluck, L.; Robinson, S.; Kasapinovic, S.; Fones, C.; Gold, W.L. Impact on health care workers employed in high-risk areas during the Toronto SARS outbreak. J. Psychosom. Res. 2008, 64, 177–183. [Google Scholar] [CrossRef]
- Su, T.-P.; Lien, T.-C.; Yang, C.-Y.; Su, Y.L.; Wang, J.-H.; Tsai, S.-L.; Yin, J.-C. Prevalence of psychiatric morbidity and psychological adaptation of the nurses in a structured SARS caring unit during outbreak: A prospective and periodic assessment study in Taiwan. J. Psychiatr. Res. 2007, 41, 119–130. [Google Scholar] [CrossRef]
- Suryavanshi, N.; Kadam, A.; Dhumal, G.; Nimkar, S.; Mave, V.; Gupta, A.; Cox, S.R.; Gupte, N. Mental health and quality of life among healthcare professionals during the COVID-19 pandemic in India. Brain Behav. 2020, 10, e01837. [Google Scholar] [CrossRef] [PubMed]
- Tam, C.W.C.; Pang, E.P.F.; Lam, L.C.W.; Chiu, H.F.K. Severe acute respiratory syndrome (SARS) in Hong Kong in 2003: Stress and psychological impact among frontline healthcare workers. Psychol. Med. 2004, 34, 1197–1204. [Google Scholar] [CrossRef] [PubMed]
- Xiao, X.; Zhu, X.; Fu, S.; Hu, Y.; Li, X.; Xiao, J. Psychological impact of healthcare workers in China during COVID-19 pneumonia epidemic: A multi-center cross-sectional survey investigation. J. Affect. Disord. 2020, 274, 405–410. [Google Scholar] [CrossRef] [PubMed]
- Zerbini, G.; Ebigbo, A.; Reicherts, P.; Kunz, M.; Messman, H. Psychosocial burden of healthcare professionals in times of COVID-19—A survey conducted at the University Hospital Augsburg. GMS Ger. Med. Sci. 2020, 18, Doc05. [Google Scholar] [PubMed]
- Zhan, Y.-X.; Zhao, S.-Y.; Yuan, J.; Liu, H.; Liu, Y.-F.; Gui, L.-L.; Zheng, H.; Zhou, Y.-M.; Qiu, L.-H.; Chen, J.-H.; et al. Prevalence and Influencing Factors on Fatigue of First-line Nurses Combating with COVID-19 in China: A Descriptive Cross-Sectional Study. Curr. Med Sci. 2020, 40, 625–635. [Google Scholar] [CrossRef]
- Zhou, Y.; Wang, W.; Sun, Y.; Qian, W.; Liu, Z.; Wang, R. The prevalence and risk factors of psychological disturbances of frontline medical staff in china under the COVID-19 epidemic: Workload should be concerned. J. Affect. Disord. 2020, 26, 510–514. [Google Scholar] [CrossRef] [PubMed]
- Wang, H.; Huang, D.; Huang, H.; Zhang, J.; Guo, L.; Liu, Y.; Ma, H.; Geng, Q. The psychological impact of COVID-19 pandemic on medical staff in Guangdong, China: A cross-sectional study. Psychol. Med. 2020, 52, 884–892. [Google Scholar] [CrossRef]
- Wang, H.; Liu, Y.; Hu, K.; Zhang, M.; Du, M.; Huang, H.; Yue, X. Healthcare workers’ stress when caring for COVID-19 patients: An altruistic perspective. Nurs. Ethic 2020, 27, 1490–1500. [Google Scholar] [CrossRef]
- I Foo, C.C.; Goon, A.T.J.; Leow, Y.-H.; Goh, C.-L. Adverse skin reactions to personal protective equipment against severe acute respiratory syndrome? A descriptive study in Singapore. Contact Dermat. 2006, 55, 291–294. [Google Scholar] [CrossRef]
- Jiang, Q.; Song, S.; Zhou, J.; Liu, Y.; Chen, A.; Bai, Y.; Wang, J.; Jiang, Z.; Zhang, Y.; Liu, H.; et al. The Prevalence, Characteristics, and Prevention Status of Skin Injury Caused by Personal Protective Equipment among Medical Staff in Fighting COVID-19: A Multicenter, Cross-Sectional Study. Adv. Wound Care 2020, 9, 357–364. [Google Scholar] [CrossRef]
- Lan, J.; Song, Z.; Miao, X.; Li, H.; Li, Y.; Dong, L.; Yang, J.; An, X.; Zhang, Y.; Yang, L.; et al. Skin damage among health care workers managing coronavirus disease-2019. J. Am. Acad. Dermatol. 2020, 82, 1215–1216. [Google Scholar] [CrossRef] [PubMed]
- Ong, J.J.; Bharatendu, C.; Goh, Y.; Tang, J.Z.; Sooi, K.W.; Tan, Y.L.; Tan, B.Y.; Teoh, H.; Ong, S.T.; Allen, D.M.; et al. Headaches Associated With Personal Protective Equipment—A Cross-Sectional Study Among Frontline Healthcare Workers During COVID-19. Headache: J. Head Face Pain 2020, 60, 864–877. [Google Scholar] [CrossRef] [PubMed]
- Alraddadi, B.M.; Al-Salmi, H.S.; Jacobs-Slifka, K.; Slayton, R.B.; Estivariz, C.F.; Geller, A.I.; Al-Turkistani, H.H.; Al-Rehily, S.S.; Alserehi, H.A.; Wali, G.Y.; et al. Risk Factors for Middle East Respiratory Syndrome Coronavirus Infection among Healthcare Personnel. Emerg. Infect. Dis. 2016, 22, 1915–1920. [Google Scholar] [CrossRef] [PubMed]
- Chatterjee, P.; Anand, T.; Singh, K.J.; Rasaily, R.; Singh, R.; Das, S. Healthcare workers & SARS-CoV-2 infection in India: A case-control investigation in the time of COVID-19. Indian J. Med. Res. 2020, 151, 459–467. [Google Scholar]
- Loeb, M.; McGeer, A.; Henry, B.; Ofner, M.; Rose, D.; Hlywka, T.; Levie, J.; McQueen, J.; Smith, S.; Moss, L.; et al. SARS among Critical Care Nurses, Toronto. Emerg. Infect. Dis. 2004, 10, 251–255. [Google Scholar] [CrossRef]
- Morcuende, M.; Guglielminotti, J.; Landau, R. Anesthesiologists’ and Intensive Care Providers’ Exposure to COVID-19 Infection in a New York City Academic Center: A Prospective Cohort Study Assessing Symptoms and COVID-19 Antibody Testing. Anesth. Analg. 2020, 131, 669–676. [Google Scholar] [CrossRef]
- Reynolds, M.G.; Anh, B.H.; Thu, V.H.; Montgomery, J.M.; Bausch, D.G.; Shah, J.J.; Maloney, S.; Leitmeyer, K.C.; Huy, V.Q.; Horby, P.; et al. Factors associated with nosocomial SARS-CoV transmission among healthcare workers in Hanoi, Vietnam, 2003. BMC Public Health 2006, 6, 207. [Google Scholar] [CrossRef]
- Teleman, M.D.; Boudville, I.C.; Heng, B.H.; Zhu, D.; Leo, Y.S. Factors associated with transmission of severe acute respiratory syndrome among health-care workers in Singapore. Epidemiol. Infect. 2004, 132, 797–803. [Google Scholar] [CrossRef]
- Liu, W.; Tang, F.; Fang, L.-Q.; De Vlas, S.J.; Ma, H.-J.; Zhou, J.-P.; Looman, C.W.N.; Richardus, J.H.; Cao, W.-C. Risk factors for SARS infection among hospital healthcare workers in Beijing: A case control study. Trop. Med. Int. Health 2009, 14, 52–59. [Google Scholar] [CrossRef]
- Chen, R.; Chou, K.R.; Huang, Y.J.; Wang, T.S.; Liu, S.Y.; Ho, L.Y. Effects of a SARS prevention programme in Taiwan on nursing staff’s anxiety, depression and sleep quality: A longitudinal survey. Int. J. Nurs. Stud. 2006, 43, 215–225. [Google Scholar] [CrossRef]
- Rogers, B.; Buckheit, K.; Ostendorf, J. Development of Competencies for Respiratory Protection for Health Care Workers. Work. Health Saf. 2018, 67, 56–67. [Google Scholar] [CrossRef] [PubMed]
- Suppan, L.; Abbas, M.; Stuby, L.; Cottet, P.; Larribau, R.; Golay, E.; Iten, A.; Harbarth, S.; Gartner, B.; Suppan, M. Effect of an E-Learning Module on Personal Protective Equipment Proficiency Among Prehospital Personnel: Web-Based Randomized Controlled Trial. J. Med. Internet Res. 2020, 22, e21265. [Google Scholar] [CrossRef] [PubMed]
- Yen, M.-Y.; Lin, Y.; Su, I.-J.; Huang, F.-Y.; Ho, M.-S.; Chang, S.-C.; Tan, K.-H.; Chen, K.-T.; Chang, H.; Liu, Y.-C.; et al. Using an integrated infection control strategy during outbreak control to minimize nosocomial infection of severe acute respiratory syndrome among healthcare workers. J. Hosp. Infect. 2006, 62, 195–199. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Bergeron, S.M.; Cameron, S.; Armstrong-Stassen, M.; Pare, K. Diverse implications of a national health crisis: A qualitative ex-ploration of community nurses’ SARS experiences. Can. J. Nurs. Res. Rev. Can. De Rech. En Sci. Infirm. 2006, 38, 42–54. [Google Scholar]
- De Wit, K.; Mercuri, M.; Wallner, C.; Clayton, N.; Archambault, P.; Ritchie, K. Canadian emergency physician psychological distress and burnout during the first 10 weeks of COVID-19: A mixed-methods study. J. Am. Coll. Emerg. Physicians Open 2020, 1, 1030–1038. [Google Scholar] [CrossRef]
- Kackin, O.; Ciydem, E.; Aci, O.S.; Kutlu, F.Y. Experiences and psychosocial problems of nurses caring for patients diagnosed with COVID-19 in Turkey: A qualitative study. Int. J. Soc. Psychiatry 2020, 67, 158–167. [Google Scholar] [CrossRef]
- Gao, X.; Jiang, L.; Hu, Y.; Li, L.; Hou, L. Nurses’ experiences regarding shift patterns in isolation wards during the COVID-19 pandemic in China: A qualitative study. J. Clin. Nurs. 2020, 29, 4270–4280. [Google Scholar] [CrossRef]
- Kang, H.S.; Son, Y.D.; Chae, S.-M.; Corte, C. Working experiences of nurses during the Middle East respiratory syndrome outbreak. Int. J. Nurs. Pract. 2018, 24, e12664. [Google Scholar] [CrossRef]
- Karimi, Z.; Fereidouni, Z.; Behnammoghadam, M.; Alimohammadi, N.; Mousavizadeh, A.; Salehi, T.; Mirzaee, M.S.; Mirzaee, S. The Lived Experience of Nurses Caring for Patients with COVID-19 in Iran: A Phenomenological Study. Risk Manag. Health Policy 2020, 13, 1271–1278. [Google Scholar] [CrossRef]
- Lee, J.Y.; Hong, J.H.; Park, E.Y. Beyond the fear: Nurses’ experiences caring for patients with Middle East respiratory syndrome: A phenomenological study. J. Clin. Nurs. 2020, 29, 3349–3362. [Google Scholar] [CrossRef]
- Liu, Q.; Luo, D.; Haase, J.E.; Guo, Q.; Wang, X.Q.; Liu, S.; Xia, L.; Liu, Z.; Yang, J.; Yang, B.X. The experiences of health-care providers during the COVID-19 crisis in China: A qualitative study. Lancet Glob. Health 2020, 8, e790–e798. [Google Scholar] [CrossRef]
- Liu, Y.E.; Zhai, Z.C.; Han, Y.H.; Liu, Y.L.; Liu, F.P.; Hu, D.Y. Experiences of front-line nurses combating coronavirus disease-2019 in China: A qualitative analysis. Public Health Nurs. 2020, 37, 757–763. [Google Scholar] [CrossRef] [PubMed]
- Mahendran, K.; Patel, S.; Sproat, C. Psychosocial effects of the COVID-19 pandemic on staff in a dental teaching hospital. Br. Dent. J. 2020, 229, 127–132. [Google Scholar] [CrossRef] [PubMed]
- McBeath, A.G.; Du Plock, S.; Bager-Charleson, S. The challenges and experiences of psychotherapists working remotely during the coronavirus* pandemic. Couns. Psychother. Res. 2020, 20, 394–405. [Google Scholar] [CrossRef]
- Mohindra, R.; Soni, R.K.; Suri, V.; Bhalla, A.; Singh, S.M. The experience of social and emotional distancing among health care providers in the context of COVID-19: A study from North India. J. Hum. Behav. Soc. Environ. 2020, 31, 173–183. [Google Scholar] [CrossRef]
- O’Connor, E.; O’Sullivan, T.; Amaratunga, C.; Thille, P.; Phillips, K.P.; Carter, M. Risk communication with nurses during in-fectious disease outbreaks: Learning from SARS. J. Emerg. Manag. 2009, 7, 48–56. [Google Scholar] [CrossRef]
- O’Sullivan, T.L.; Amaratunga, C.; Phillips, K.P.; Corneil, W.; O’Connor, E.; Lemyre, L.; Dow, D. If Schools Are Closed, Who Will Watch Our Kids? Family Caregiving and Other Sources of Role Conflict among Nurses during Large-Scale Outbreaks. Prehospital Disaster Med. 2009, 24, 321–325. [Google Scholar] [CrossRef]
- Robertson, E.; Hershenfield, K.; Grace, S.; Stewart, D.E. The Psychosocial Effects of Being Quarantined following Exposure to SARS: A Qualitative Study of Toronto Health Care Workers. Can. J. Psychiatry 2004, 49, 403–407. [Google Scholar] [CrossRef]
- Sadati, A.K.; Zarei, L.; Shahabi, S.; Heydari, S.T.; Taheri, V.; Jiriaei, R.; Ebrahimzade, N.; Lankarani, K.B. Nursing experiences of COVID-19 outbreak in Iran: A qualitative study. Nurs. Open 2020, 8, 72–79. [Google Scholar] [CrossRef]
- Sun, N.; Wei, L.; Shi, S.; Jiao, D.; Song, R.; Ma, L.; Wang, H.; Wang, C.; Wang, Z.; You, Y.; et al. A qualitative study on the psychological experience of caregivers of COVID-19 patients. Am. J. Infect. Control 2020, 48, 592–598. [Google Scholar] [CrossRef]
- Xu, C.; Zhang, X.; Wang, Y. Mapping of Health Literacy and Social Panic via Web Search Data during the COVID-19 Public Health Emergency: Infodemiological Study. J. Med. Internet Res. 2020, 22, e18831. [Google Scholar] [CrossRef]
- Priolo Filho, S.R.; Goldfarb, D.; Zibetti, M.R.; Aznar-Blefari, C. Brazilian Child Protection Professionals’ Resilient Behavior during the COVID-19 Pandemic. Child Abus. Negl. 2020, 110, 104701. [Google Scholar] [CrossRef] [PubMed]
- Sadiq, M. Policing in pandemic: Is perception of workload causing work-family conflict, job dissatisfaction and job stress? J. Public Aff. 2020, 22, e2486. [Google Scholar] [CrossRef]
- Sasaki, N.; Kuroda, R.; Tsuno, K.; Kawakami, N. Workplace responses to COVID-19 associated with mental health and work performance of employees in Japan. J. Occup. Health 2020, 62, e12134. [Google Scholar] [CrossRef] [PubMed]
- Song, L.; Wang, Y.; Li, Z.; Yang, Y.; Li, H. Mental Health and Work Attitudes among People Resuming Work during the COVID-19 Pandemic: A Cross-Sectional Study in China. Int. J. Environ. Res. Public Health 2020, 17, 5059. [Google Scholar] [CrossRef]
- Tan, W.; Hao, F.; McIntyre, R.S.; Jiang, L.; Jiang, X.; Zhang, L.; Zhao, X.; Zou, Y.; Hu, Y.; Luo, X.; et al. Is returning to work during the COVID-19 pandemic stressful? A study on immediate mental health status and psychoneuroimmunity prevention measures of Chinese workforce. Brain Behav. Immun. 2020, 87, 84–92. [Google Scholar] [CrossRef] [PubMed]
- Wong, E.L.-Y.; Ho, K.-F.; Wong, S.Y.-S.; Cheung, A.W.-L.; Yau, P.S.-Y.; Dong, D.; Yeoh, E.-K. Views on Workplace Policies and its Impact on Health-Related Quality of Life during Coronavirus Disease (COVID-19) Pandemic: Cross-Sectional Survey of Employees. Int. J. Health Policy Manag. 2020, 11, 344–353. [Google Scholar] [CrossRef]
- Kim, L.E.; Asbury, K. ‘Like a rug had been pulled from under you’: The impact of COVID-19 on teachers in England during the first six weeks of the UK lockdown. Br. J. Educ. Psychol. 2020, 90, 1062–1083. [Google Scholar] [CrossRef]
- Neary, S.; Van Rhee, J.; Roman, C. The Effect of the Coronavirus Pandemic on Physician Assistant Educators. J. Physician Assist. Educ. 2020, 31, 121–125. [Google Scholar] [CrossRef]
- Pather, N.; Blyth, P.; Chapman, J.A.; Dayal, M.R.; Flack, N.A.; Fogg, Q.A.; Green, R.A.; Hulme, A.; Johnson, I.; Meyer, A.J.; et al. Forced Disruption of Anatomy Education in Australia and New Zealand: An Acute Response to the Covid-19 Pandemic. Anat. Sci. Educ. 2020, 13, 284–300. [Google Scholar] [CrossRef]
- Gearing, R.; Saini, M.; McNeill, T. Experiences and implications of social workers practicing in a pediatric hospital environment affected by SARS. Health Soc. Work 2007, 32, 17–27. [Google Scholar] [CrossRef] [PubMed]
- Li, T.; Pien, L.; Kao, C.; Kubo, T.; Cheng, W. Effects of work conditions and organisational strategies on nurses’ mental health during the COVID-19 pandemic. J. Nurs. Manag. 2021, 30, 71–78. [Google Scholar] [CrossRef] [PubMed]
- Shi, L.-S.; Xu, R.H.; Xia, Y.; Chen, D.-X.; Wang, D. The Impact of COVID-19-Related Work Stress on the Mental Health of Primary Healthcare Workers: The Mediating Effects of Social Support and Resilience. Front. Psychol. 2022, 12, 800183. [Google Scholar] [CrossRef] [PubMed]
- Alexiou, E.; Steingrimsson, S.; Akerstrom, M.; Jonsdottir, I.H.; Ahlstrom, L.; Finizia, C.; Wijk, H.; Degl’Innocenti, A. A Survey of Psychiatric Healthcare Workers’ Perception of Working Environment and Possibility to Recover Before and After the First Wave of COVID-19 in Sweden. Front. Psychiatry 2021, 12, 770955. [Google Scholar] [CrossRef]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).