Abstract
Increased use of electronic nicotine delivery systems (ENDS) and improper disposal after use pose a public health and an environmental justice (EJ) concern if use prevalence is disproportionately high among minorities and people of low socioeconomic status (SES) (broadly termed “EJ populations” for the purposes of this review). This review synthesizes literature on demographic patterns of use prevalence, susceptibility, advertisement exposure, and access to ENDS, and extrapolates environmental tobacco exposure (ETE) from ENDS among EJ populations. Seven electronic databases were searched using ENDS-related terms. We included studies published between 2017 and May 2020 that described ENDS use prevalence, susceptibility to ENDS use, advertisement exposure, and access to ENDS by race, ethnicity, or SES. Data synthesis was based on the assumptions that ETE increases with high use prevalence, susceptibility may influence future use, and advertisement exposure and access may impact demographic differences in use. We identified 32 studies describing use prevalence, susceptibility, advertisement exposure, or access to vape shops and other tobacco retail outlets by race/ethnicity or SES. We found higher prevalence of ENDS use among non-Hispanic Whites and inconclusive use patterns by SES. Patterns of susceptibility to use, advertisement exposure, and access were also mixed, with slightly higher outcomes observed among low SES youth. However, the evidence base on advertisement exposure was limited, with limited generalizability. Our findings indicate low prevalence of ENDS use among EJ populations. While this suggests low potential ETE among these groups, mixed outcomes on susceptibility, advertisement exposure, and access to ENDS among low SES groups may affect future ENDS use and ETE. Educational campaigns that discourage ENDS uptake should target EJ youth. Initiatives aimed at managing vape shop presence in EJ communities and monitoring targeted advertisement are also needed.
1. Introduction
A sustained decrease in the prevalence of combustible tobacco smoking has been reported over recent decades [1]. However, disparities in tobacco use persist among racial/ethnic minorities and across groups defined by educational level and socioeconomic status (SES) [2]. Many studies have investigated the potential for electronic nicotine delivery systems (ENDS) to offer an alternative for those who struggle to quit, including smokers from socioeconomically disadvantaged backgrounds [3,4]. However, evidence from systematic reviews makes it difficult to draw firm conclusions about ENDS impact on smoking inequalities. Current ENDS use among United States (U.S.) adults declined from 3.7% in 2014 to 2.8% in 2017 and increased to 4.5% in 2019 [5,6]. A rapid increase in use among high/middle school students during 2017–2018 (11.7% to 20.8%/3.3% to 4.9%) prompted the Surgeon General to declare ENDS use among youth and young adults a public health epidemic [7,8]. The estimated 2021 current e-cigarette use among high and middle school students is 11.3% and 2.8%, respectively [9].
Increased use of ENDS presents the potential for environmental exposure to toxic chemicals from secondhand and thirdhand aerosols and ENDS waste, posing a public health concern. The presence of toxic chemical constituents in ENDS aerosols is well-documented. Ultrafine particles, nicotine, glycerin, and toxicants created by the oxidation or dehydration of vegetable glycerin and polyethylene glycol including formaldehyde and acetaldehyde are present in secondhand aerosols (SHA) from ENDS [10,11,12,13]. Recent literature suggests that SHA pollutant levels are generally lower than those in secondhand smoke (SHS). However, ENDS are still a source of indoor air pollutants because SHA toxicant levels are above background levels [13,14,15,16,17,18]. Much like thirdhand smoke, SHA can form residues on indoor surfaces; one study found SHA constituents from a vape shop traveled to form deposits on indoor surfaces in adjacent businesses [19].
The disposal of ENDS components may also pose a public health concern. Littered or improperly discarded ENDS can leach heavy metals, battery acids, and organic chemicals, potentially affecting humans and other organisms [20,21,22]. Small components (e.g., pods, cartridges) can pose choking hazards for small children and may be eaten by birds and other animals. Exploding ENDS batteries can cause severe burns and start fires.
These environmental tobacco exposure (ETE) scenarios may present an environmental justice (EJ) concern if ENDS use prevalence is disproportionately high among minorities and low-income populations (broadly termed “EJ populations” herein). EJ assessment was mandated under the National Environmental Policy Act (NEPA) by Executive Order (EO) 12,898 in 1994 to ensure equitable protection from environmental and human health hazards resulting from federal agency actions. The EO and associated Presidential Memorandum ordered the creation of the Interagency Working Group on Environmental Justice, which provides guidance to federal agencies on criteria to identify and address potential disproportionate human health, economic, and social effects, including effects on minority and low-income communities through the NEPA process [23].
Racial and ethnic disparities in ETE resulting from combustible tobacco product use are well-documented [24,25,26]. However, studies reporting sociodemographic differences in ETE from ENDS use are limited. This review synthesizes available scientific literature on use prevalence, susceptibility, advertisement exposure, and access to ENDS in the U.S. to address two questions: (1) Are use prevalence, susceptibility, advertisement exposure, and access to ENDS disproportionately high among EJ populations? (2) Are EJ populations likely to have disproportionately high environmental exposure to ENDS aerosols and wastes?
2. Methods
2.1. Search Strategy
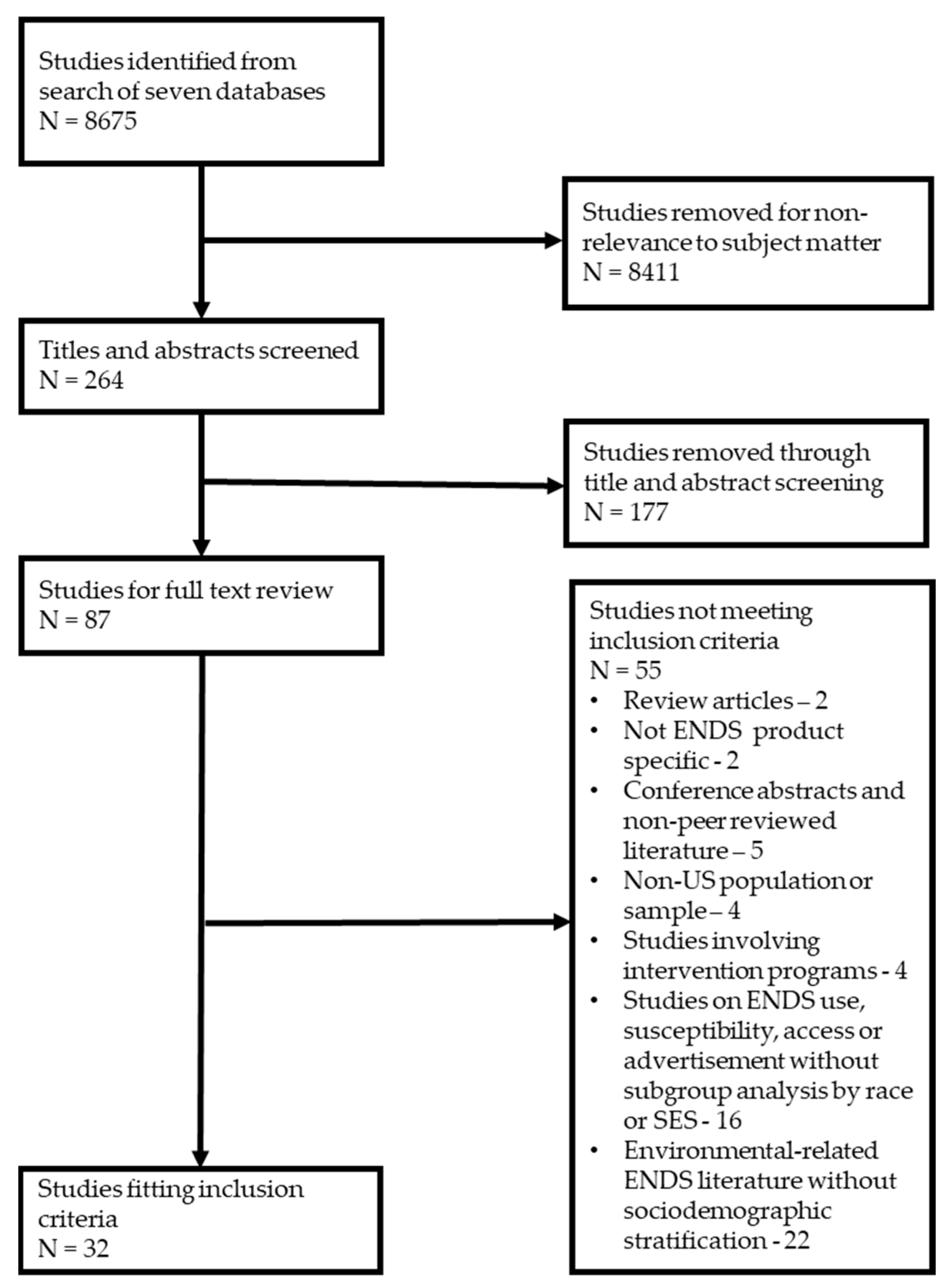
The literature search covered seven databases of peer-reviewed articles using terms for all available ENDS data (Supplementary File S1). Initially, 8675 studies were identified between 2017 and May 2020. We screened titles and abstracts for articles focused on use prevalence, susceptibility, advertisement exposure, or access to ENDS, resulting in 264 abstracts.
2.2. Study Selection
Studies were selected to answer the two questions noted above. We limited the review to publications from 2017 onwards, reflecting the period of a general increase in ENDS use [27]. No limits were set on the study design or scale, but we restricted our search to articles available in English. To meet our inclusion criteria, studies had to report use prevalence, susceptibility, advertisement exposure, or access to ENDS or a combination of those measures by race/ethnicity or an appropriate SES indicator (household income, user’s educational attainment, parent education, school setting) in a population or sample. We excluded non-peer-reviewed articles, studies involving intervention programs, review articles, and books. We also excluded non-U.S. studies to reflect NEPA’s reach. We assessed titles and abstracts against eligibility criteria after initial screening and removal of irrelevant references. A full-text review was conducted for 87 studies, including independent assessment by all authors and a secondary review of all exclusions. Discrepancies were resolved by discussion among authors. Our final evidence base comprised 32 studies (Figure 1).
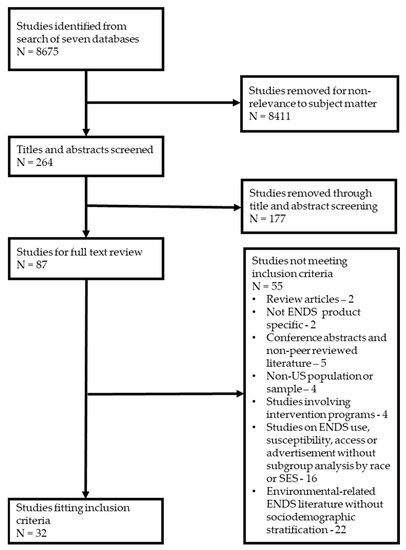
Figure 1.
PRISMA flow diagram.
2.3. Data Extraction
Data on the following factors were extracted: article and publication information, research questions, description of study population group with inclusion or exclusion criteria if applicable, demographics, SES indicators, study design, method summary, measured outcomes and results, study strengths and limitations including those listed by the authors, and risk of bias (Supplementary File S2).
2.4. Data Analysis
The review findings were summarized via narrative synthesis of selected studies. Racial/ethnic minorities were classified as all races other than non-Hispanic Whites (NHW). Meta-analyses were not performed due to study design diversity (longitudinal, cross-sectional, cross-sectional from longitudinal data, quantitative) and heterogeneity of study settings (national, state, county, local). We characterized potential exposure to SHA and chemicals from ENDS wastes as ETE. Direct estimation of ETE was not possible because studies directly describing ENDS-related ETE by race/ethnicity and SES are limited.
ETE was extrapolated from study findings based on three assumptions. First, potential ETE increases with use prevalence, and ENDS users are likely to use products in homes and vehicles around people of similar racial/ethnic and socioeconomic backgrounds. The literature supports this assumption: EJ populations have higher SHS exposure partly due to smoking rates and places of domicile and employment [28,29,30]. Second, ENDS use susceptibility may influence future use among non-users and experimental ENDS users. Longitudinal studies show that ENDS susceptibility among youth is a predictor of subsequent ENDS initiation and use [31,32,33,34]. Third, exposure to ENDS advertisements and access to vape shops and other tobacco retail outlets may impact demographic differences in ENDS use. Several factors are associated with future ENDS use, including product advertising, cigarette smoking, age, and being NHW [35]. Significant associations have also been reported between receptivity to tobacco advertising and progression toward use [34].
High ETE was identified when use prevalence, susceptibility, advertisement exposure, or access to ENDS was higher among at least one racial/ethnic minority group than among NHW, and among people of a low SES background. Low ETE was identified when use prevalence, susceptibility, advertisement exposure, or access to ENDS among racial/ethnic minority groups was less than or equal to exposure among NHW, and low among people of low SES backgrounds. Contradictory or complex use patterns, susceptibility, advertisement exposure, and access to ENDS were classified as unclear with respect to potential ETE.
3. Results
We identified 32 studies describing use prevalence, susceptibility, advertisement exposure, access to ENDS by race/ethnicity, or SES (Figure 1). Articles reviewed included studies analyzing cross-sectional and longitudinal data from national, state, and local surveys. All studies used self-reported outcome measures of unknown validity or reliability due to the lack of research to date on such measures. Various terms were used to describe the racial/ethnic makeup of study participants; for the purposes of this study, NHW represents all non-Hispanic Whites, non-Hispanic Black (NHB) represents Blacks and African Americans, and Hispanic represents Hispanics and Latinos. Other racial groups included Asians and Native Americans or Alaskan Natives. Key findings are summarized in Table 1.

Table 1.
Key findings from the articles.
Sixteen studies reported use prevalence among youth (12–17), young adults (18–25), and adults (18 and older). Fifteen of those studies reported subgroup analysis by race/ethnicity and ten by SES. Five studies reported these for “ever use” and seven for “current, past month, or past 30-day use.” Two studies reported ENDS use among current smokers. Definitions of “current use” and “ever use” were not consistent; “current use” was mostly defined as daily use or any use within the past 30 days or past month, while “ever use” was defined variously from any use in the past 12 months to ever lifetime use.
Nine studies evaluated ENDS susceptibility; seven reported on susceptibility by race/ethnicity and six by SES. In studies reporting subgroup analysis by race/ethnicity, one study reported results for ENDS and polysubstance use, one for ENDS and other tobacco products, and one for ENDS and cigarette use. One study evaluated harm perception as a factor in ENDS susceptibility by race/ethnicity and SES.
Thirteen studies evaluated advertisement exposure and ENDS access. Of these, four reported on both advertising and access, four reported advertising only, and five reported access only. For advertising, five studies reported subgroup analysis by race/ethnicity, and five studies by SES. For access, nine studies reported subgroup analysis by race/ethnicity and seven studies by SES.
3.1. Race/Ethnicity
3.1.1. Prevalence of Use
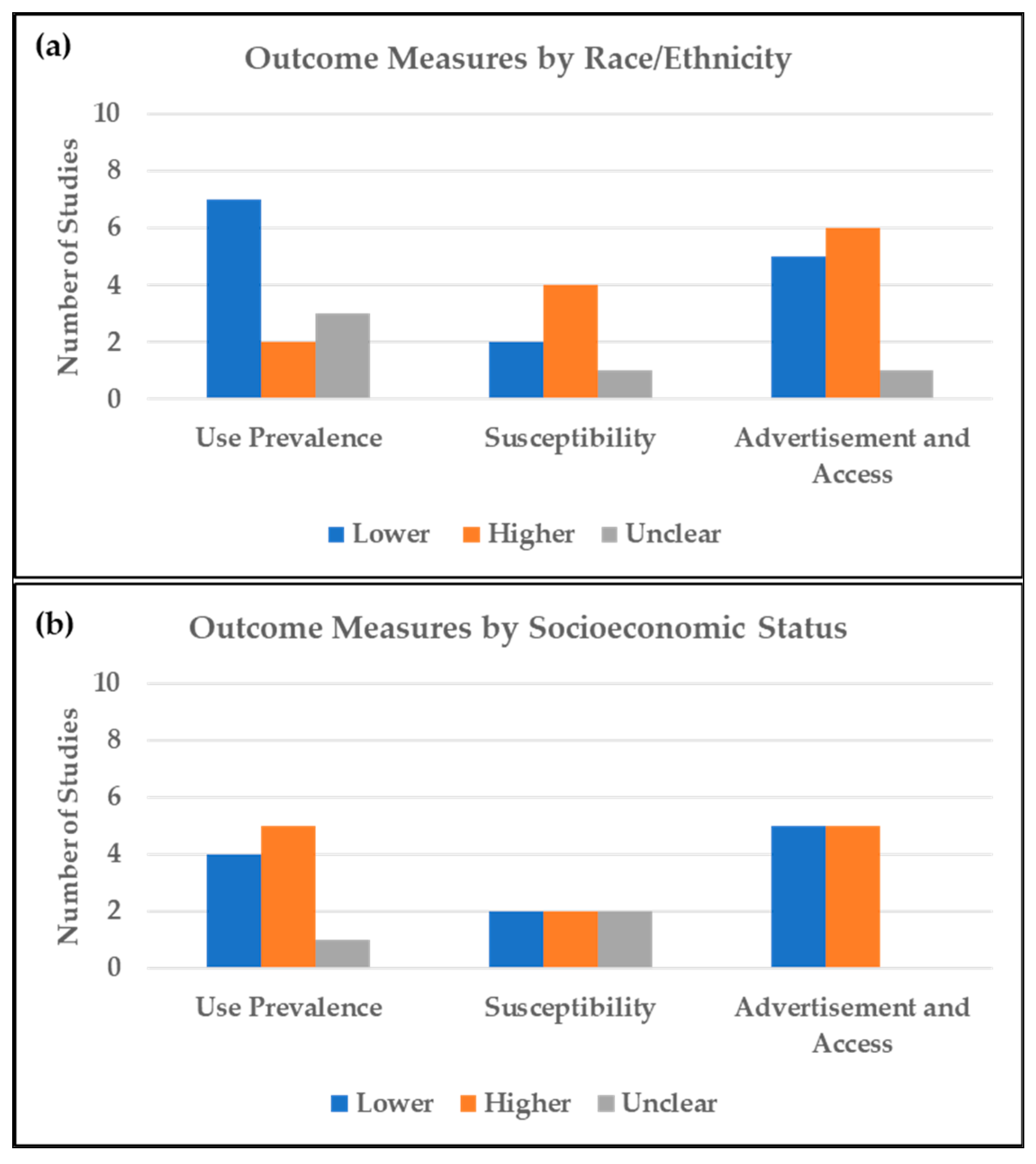
Studies describing use prevalence by race/ethnicity generally showed lower prevalence among minorities compared to NHW (Figure 2a). Outcomes from surveys involving adult participants were similar to those involving youth with respect to use prevalence among racial/ethnic minorities. Seven studies reported lower use prevalence among racial/ethnic minorities [36,37,38,39,40]. Data from the 2014 and 2018 National Health Interview Survey (NHIS) showed an increase in ENDS ever use prevalence among U.S. adults for all races (13.0% to 15.7%), with the highest prevalence in 2018 observed among NHW (19.1%) [36]. Results from a national survey of high school students showed that schools with a higher percentage of NHW students (14.4% for tenth grade, 17.1% for twelfth grade) and schools with a higher prevalence of past-month cigarette smoking (adjusted odds ratio (AOR) = 6.82; 95% confidence interval (CI) = 5.68–7.96) had significantly higher past-month ENDS use [38]. Similarly, a nationally-representative youth survey found lower odds of ENDS poly-use (tobacco, alcohol, or cannabis) among all other racial/ethnic groups (odds ratios (ORs) = 0.18–0.61) compared to NHW [37]. Other studies reporting lower ENDS use among minorities involved data from local and regional surveys [39,40]. A study involving Los Angeles County adults reported the highest prevalence of ENDS ever use among NHW adults (12.8%) followed by Asian adults (8.9%); NHB had the lowest prevalence (5.8%) [39]. A study assessing JUUL use among ever and past-30-day ENDS users reported a positive association between JUUL use and being NHW [40]. Four studies reported higher use prevalence among minorities; one of these analyzed data from a national survey [41,42,43]. Three of those studies reported higher odds of ENDS ever use among Hispanic adolescents compared to NHW (3% vs. 1.5%, p = 0.003; 34.5% vs. 24.9%, p < 0.001; and OR = 1.30, 95%CI = 1.17–1.45) [41,42,43] and one reported the highest ENDS use among non-Hispanic “other” adults (OR = 9.3, 95%CI = 6.0–12.6) compared to non-Hispanic Whites [6]. However, lower odds of ENDS ever use were reported among NHB (OR = 0.72, 95%CI = 0.63–0.83) and Asian (OR = 0.64, 95%CI = 0.50–0.81) students compared to NHW [41]. Results from three nationally representative studies were mixed [5,44,45]. JUUL ever use prevalence among participants aged 15–34 was comparable between Hispanic and NHW ENDS ever users (14.6% vs. 14.4%) [44]. Similarly, self-reported current and regular e-cigarette use were the highest among non-Hispanic whites and persons of “other” races [5,45].
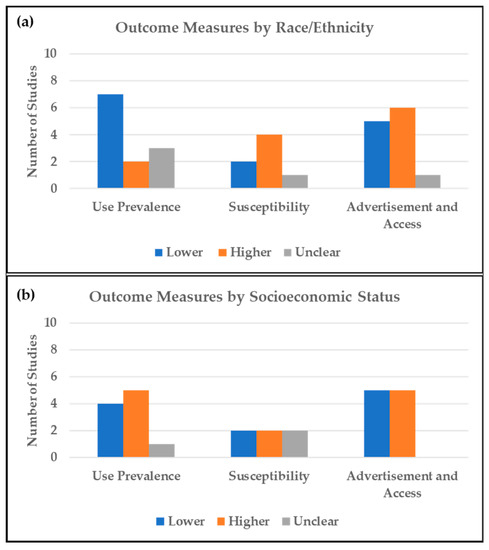
Figure 2.
Distribution of studies showing the direction of potential environmental tobacco exposure (ETE) from ENDS among (a) racial/ethnic minorities compared to non-Hispanic whites, and (b) low socioeconomic status compared to high socioeconomic status. Higher: refers to higher potential for ETE among minorities and low SES groups. Lower: refers to lower potential for ETE among minorities and low SES groups. Unclear: contradictory or complex patterns of potential ETE.
3.1.2. Susceptibility to ENDS Use
Studies examining the susceptibility by race/ethnicity generally reported higher susceptibility among minority youth and lower susceptibility among minority adults (Figure 2a). Four studies reported higher susceptibility among racial/ethnic minorities. Results from a study analyzing a nationally representative sample of participants aged 13–18 revealed that perceived health risks of nicotine and toxins in ENDS products were 34% lower in NHB compared to NHW [46]. A study following use patterns in adolescents reported that baseline ENDS ever use was higher for Hispanics than NHW (34.5% vs. 24.9%; p < 0.001) but lower at a 12-month follow-up for past 30-day use (17.3% vs. 13.2%; p < 0.001) [42]. Susceptibility was significantly higher among Hispanic compared to NHW youth in two studies in Nevada (AOR = 1.89; 95%CI = 1.27–2.83) and in central Texas (38.7% vs. 29.7%; p < 0.0001) [43,47]. Two studies reported lower susceptibility among minorities; both involved national surveys (OR (NHB) = 0.27, 95%CI = 0.09–0.77; OR (Hispanic) = 0.26, 95%CI = 0.09–0.70) [37,48]. Evidence from one study indicated mixed or unclear outcomes with respect to susceptibility. The results revealed that, among current users of noncigarette combustible tobacco, Hispanics and NHB adults were more likely to use ENDS (OR (NHB) = 2.7, 95%CI = 1.0–4.3; OR (Hispanic) = 3.3, 95%CI = 1.2–5.4). However, among current cigarette smokers, racial groups other than NHB were more likely to use ENDS, indicating that susceptibility among racial groups may differ by combustible product use status [49].
3.1.3. Advertisement Exposure and Access to ENDS
Outcomes from studies describing advertisement exposure and access to ENDS by race/ethnicity were mixed (Figure 2a). Five studies reported on advertising or marketing strategies by race/ethnicity [48,50,51,52,53]; two analyzed data from national surveys [48,51]; and three involved data from county and state surveys [50,52,53]. Nine studies reported ENDS access by race/ethnicity [50,52,53,54,55,56,57,58,59]; six analyzed state and local data [50,52,53,54,55,59]; and three analyzed nationally representative data [56,57,58].
For advertising, a study analyzing data from Los Angeles County reported that marketing strategies differed by race/ethnicity, and exterior advertising was less prominent in Hispanic/Latino (OR = 0.36, 95%CI = 0.17–0.72) and Korean American (OR = 0.28, 95%CI = 0.10–0.74) communities compared to NHW communities [50]. ENDS advertising was significantly lower in neighborhoods with majority NHB (20.3%, adjusted prevalence ratio (aPR) = 0.63(0.41,0.99)) and Hispanic (22.9%, aPR = 0.62(0.40,0.98)) populations in New York City (NYC) [53]. E-cigarette advertising declined in retail stores close to high schools in NJ including districts with >50% non-White students, between 2015 and 2016 [52]. In two national studies, NHB youth reported higher ENDS use following higher exposure to advertising or marketing strategies at rates over 2.5 and 3 times higher than Hispanic and NHW youth, respectively [51]. Among adults, NHB (30.10%, p < 0.05) and “other” (non-Hispanic other) (17.42%, p < 0.05) users reported higher use due to appealing advertising [48].
Studies on access were mostly at state and county levels and revealed mixed results. ENDS were less likely to be placed in proximity to youth-friendly items in African American (OR = 0.32, 95%CI = 0.16–0.65), Korean American (OR = 0.20, 95%CI = 0.07–0.59), and Hispanic/Latino (OR = 0.07, 95%CI = 0.02–0.26) communities in Southern California, and retailers were less likely to sell and advertise ENDS, compared to NHW communities [50]. In NJ, e-cigarette availability near high schools, including school districts with >50% non-White students, decreased over a one-year period (2015–2016) [52]. Austin, Texas had lower proportions of NHB (5.7%) and Hispanic (32.7%) residents in census tracts with a vape shop compared to NHW residents (77.7%). Though the odds of finding a vape shop in Hispanic areas was high, the odds were low for NHB areas (AOR = 0.90; 95%CI = 0.815–0.997) and decreased with an increasing percentage of NHB residents [54]. However, results from a study in Orange County, California revealed that census tracts with at least one vape shop had a higher percentage of Asians (mean = 20.1%, p = 0.030), Hispanics (mean = 35.8%, p = 0.001), and people born outside the U.S. (mean = 31.8%, p = 0.004) [55]. Tobacco retailers in NYC had the lowest ENDS availability in high percent NHB (28.7%, aPR = 0.71(0.51,0.98)) and Hispanic (28.3%, aPR = 0.75(0.53,1.05)) neighborhoods [53]. Vape shops were more likely to be located in neighborhoods with high Hispanic populations across Virginia [59]. Similarly, national studies on vape shop proximity to public middle and high schools revealed that vape shop density was higher and vape shops were closer to schools in districts with higher proportions of Asian and NHB populations [56]. Another national study found vape shops were more likely to be in urban areas with high Hispanic (adjusted risk ratio (aRR) = 3.3, p < 0.0001) and Asian (aRR = 2.0, p < 0.0001) populations, and non-urban areas with high African American (aRR = 3.9, p = 0.0009) and Hispanic (aRR = 7.4, p < 0.0001) populations [58]. Xiao et al. suggested that increasing ENDS prices may decrease demand more among other non-Hispanic ethnicities compared to NHWs due to potential affordability-driven use (AOR = 2.684, 95%CI = 1.044–6.899) [57]. However, non-Hispanic “other” (89.30%), NHW (78.79%), and Hispanic (76.59%) youth reported higher ENDS use due to appealing flavors than NHB youth (53.62%) [57].
3.2. Socioeconomic Status
3.2.1. Prevalence of Use
Outcomes from studies describing ENDS use prevalence by SES were mixed (Figure 2b) [39,40,44,60,61,62]. Four studies reported lower use prevalence among low SES groups [39,40,44], five studies reported higher prevalence among low SES groups [60,61,62], and one study reported unclear results [45]. Among the studies reporting low prevalence among low SES groups, one study reported higher ENDS ever use among adults with a household income ≥300% of the federal poverty level (FPL) compared to those = 0–99% FPL (10.7% vs. 6.3%), and among adults with some college education or higher compared to those with less than high school education (10.2% vs. 4.6%) [39]. Self-reported current e-cigarette use significantly increased from 2017 to 2018 among U.S. young adults and adults with income four times the FPL or greater (difference = 4.3%, 95%CI = 0.6–8.0%, p = 0.008) [5]. JUUL use was reportedly highest among ENDS ever users with high SES backgrounds and among people living in the northeast (17.1% ever users, 7.8% current users) [40,44]. Among studies reporting high prevalence among low SES groups, a national survey showed higher odds of use among individuals with less than high school education (OR = 1.47, 95%CI = 1.08–2.00) and among people with income below FPL (OR = 1.31, 95%CI = 1.01–1.69) [60]. Results from a 2019 national survey showed the highest ENDS use among those in the lowest income bracket (OR = 5.0, 95%CI = 4.4–5.6) and those with no more than a high school education (OR = 7.8, 95%CI = 5.5–10.1) [6]. Higher education was linked with lower odds of using ENDS, with the significant inverse association observed among NHW but not NHB adults (OR = 0.76, 95%CI = 0.61–0.95) [61]. Compared to non-users in a 2013–2014 national survey, e-cigarette users were more likely to be less educated or have a lower income [63]. A study describing poly-product use among adolescents showed that lower parental education was associated with increased odds of past ENDS use (OR = 1.30, 95%CI = 1.12–1.51), and lower school subjective social status was associated with increased odds of past (OR = 1.11, 95%CI = 1.03–1.20) or current use (OR = 1.25, 95%CI = 1.08–1.44) of ENDS compared to never use [62]. Results from a 2014 national survey indicated that regular e-cigarette use varied by educational level but had no significant association with income [45].
3.2.2. Susceptibility to ENDS Use
Studies examining ENDS susceptibility by SES are inconclusive (Figure 2b). Two studies reported higher susceptibility among low SES youth, two reported lower susceptibility among low SES adults, and two reported unclear results [43,46,48,49,61,64]. Studies reporting higher susceptibility among low SES youth revealed lower health risk perceptions of nicotine and ENDS toxins or chemicals among youth with lower parental education (OR = 0.69, 95%CI = 0.55–0.87) and low-income status (OR = 0.72, 95%CI = 0.58–0.91). Additionally, students in lower SES schools had significantly higher odds of susceptibility compared with students at higher SES schools (AOR = 2.01, 95%CI = 1.49–2.71) [43,46]. Studies reporting lower susceptibility among low SES participants revealed that lower income smokers were more likely to believe ENDS are more harmful than cigarettes (OR = 1.40, 95%CI = 1.08–1.82) [48]. Lower SES was associated with a reduced overall likelihood of ENDS use among adults (OR = 1.01, 95%CI = 0.83–1.24) and higher education was associated with a 0.9% increase in the likelihood of switching from conventional cigarette smoking to ENDS compared to those without any higher education (95%CI = 0.0–1.9) among ever smokers [48,64] Evidence from one study analyzing nationally representative data revealed that among current cigarette smokers, those living at or above the FPL with higher education were more likely to use ENDS (OR = 60.7, 95%CI = 57.9–65.3, OR = 61.7, 95%CI = 58.4–64.9). However, results also revealed that among current users of noncigarette combustible tobacco, those living in poverty were more likely to have ever used ENDS (OR = 4.1, 95%CI = 1.5–6.8) [49]. Another study revealed an inverse association between education attainment and ENDS use in NHW but not in NHB adults (OR = 1.63, 95%CI = 1.04–2.56) [61].
3.2.3. Advertisement Exposure and Access to ENDS
Studies examining ENDS advertisement exposure and access by SES generally reported higher exposure and lower access among low SES youth (Figure 2b). Three studies reported on ENDS advertising and marketing strategies by SES [51,57,65], and three described access by SES [54,55,56].
For ENDS advertising, a survey of Connecticut high school students reported higher potential for high SES youth to experience greater recent advertising exposure, indirectly influencing e-cigarette use (indirect effect: β = 0.01, standard error (SE) = 0.00, 95%CI = 0.001–0.010, p = 0.02) [65]. However, a study analyzing nationally representative data revealed that low SES youth were also more likely to report using ENDS because people in the media or other public figures used them than those in higher SES groups (52.3%, 95%CI = 40.21–64.13) [51]. Similarly, a later study reported that those with household income <$50,000 were more likely to use ENDS because the advertising appeals to them (~58%) [57].
For access to ENDS, three studies revealed that increased poverty correlated with increased odds of vape shop presence in Austin, TX (AOR = 1.07, 95%CI = 1.010–1.125), Orange County, CA (%poverty in areas with at least one vape shop (12.4%) vs. areas with none (8.8%), p < 0.001), and in neighborhoods across Virginia with low household income, a higher percentage of renter-occupied housing, lower gross rent cost, and a higher percentage of vacant houses [54,55]. However, studies assessing the nationwide distribution of vape shops revealed that shops were further away from schools in school districts in higher-poverty areas [56], or that poverty was not a significant determinant of vape shop density [58]. In NYC and NJ, ENDS availability was highest in high-income neighborhoods (64.3%, aPR = 1.00 (reference)) [53], and in retail stores close to mid-to-high income school districts, respectively [52].
4. Discussion
Studies directly describing environmental exposure to secondhand and thirdhand ENDS aerosols and chemicals from ENDS waste on EJ populations are limited. This narrative review attempts to extrapolate demographic differences in potential ETE from use prevalence, susceptibility, advertising exposure, and access to ENDS. We synthesized available studies to assess use prevalence among minorities compared to NHW, and people of low vs. high SES backgrounds. Susceptibility to ENDS use, advertisement exposure, and access was also reviewed, since susceptibility may influence future use among non-users and experimental users, and advertising and access may influence demographic differences in ENDS use. The potential for ETE was extrapolated from reviewed data based on those assumptions.
Generally, our review showed lower potential ETE among racial/ethnic minorities compared to NHW with respect to ENDS use prevalence. This is consistent with findings from studies showing a higher likelihood of exposure to SHS and SHA among NHW youth [66,67,68]. Similarly, a recent review on sociodemographic differences in ENDS awareness and use showed that ENDS appear to have gained greater reach among NHW than other racial/ethnic groups, and among people with higher educational attainment [69]. However, our review revealed inconclusive results on use prevalence and SES. Lucherin et al. reviewed the potential for non-combustible nicotine products to reduce socioeconomic inequities from smoking and reported a positive association between ENDS use prevalence and high SES; they acknowledged that the evidence suggests a potential flattening of the SES gradient over time [2]. The mixed outcomes revealed in our review may also be indicative of a potential leveling of the SES gradient. Lower use prevalence among minorities presents a positive outlook on potential ETE from ENDS and does not show disproportionately high ETE among those groups. However, mixed outcomes observed with respect to use prevalence by SES and the potential flattening of the SES gradient may affect the future ETE outlook among these groups.
We found mixed results from studies assessing ENDS use susceptibility. While these studies were more likely to suggest higher susceptibility among low SES and minority youth, the opposite was reported for low SES and minority adults. High susceptibility among minority youth is concerning, because ENDS susceptibility is a potential predictor of future ENDS use and use of products such as marijuana and alcohol [70]. Though ENDS susceptibility trends cannot be compared to ENDS use trends with cross-sectional data, longitudinal studies have found that ENDS susceptibility predicts subsequent use at follow-up [7,31,32,34]. Longitudinal data would clearly characterize the influence of susceptibility on ENDS use and associated demographic factors.
Advertising exposure and access were higher among racial/ethnic minority youth and adults. However, differential advertisement exposure and access to ENDS were mostly reported at state and local levels, though these data may lack generalizability. Advertisement exposure and access also appeared to be influenced by SES. However, the current evidence on sociodemographic differences in advertisement exposure and access was limited; additional studies can help better understand ENDS use resulting from advertisement exposure and access, and associated ETE among EJ groups. Initiatives aimed at controlling advertising may help curb youth e-cigarette use [35]. FDA’s youth tobacco prevention campaigns [71] and the surgeon general’s call for aggressive state and local actions (e.g., restricting youth access to ENDS in retail stores, including ENDS in smoke-free indoor air policies) [8] are important steps to reduce initiation, use, and ETE potential. FDA’s enforcement policy on flavored cartridge-based ENDS [72] and flavored ENDS bans by state and local governments [73] may also curb future initiation.
5. Limitations
To our knowledge, our review is the first to infer sociodemographic patterns of potential ETE from ENDS use, susceptibility, advertising, and access. However, several limitations exist. We did not assess study quality. As studies directly examining ENDS-related ETE are limited, we relied on several assumptions to extrapolate ETE from the studies reviewed. The direct assessment of ETE through surveys and measurement of biomarkers of exposure could provide more reliable data to inform EJ assessments through the NEPA process. As with all reviews, we were limited by the evidence available and its reporting. For instance, most studies involved self-reported surveys; therefore, recall bias and other individual study limitations may have impacted our results. Heterogeneity in study design and settings made meta-analysis impossible. Some studies included local and regional surveys; sociodemographic characteristics differ widely across regions and observations in any one region may not be generalizable. Furthermore, differences in exposure and use pattern measurement made it difficult to draw conclusions. For example, some studies assessed ENDS use only while others assessed dual, or poly-use across subgroups. Many studies did not consider differences in ENDS product preferences by brand, type, flavor, nicotine concentration, cost, or other characteristics, potentially skewing subgroup results. Finally, the ENDS landscape is quickly changing; the sociodemographic patterns reported may have evolved beyond our search time frame.
6. Conclusions
Our review extrapolates the potential for disproportionately high ETE among EJ populations resulting from ENDS use prevalence, susceptibility, advertisement exposure, and access. The findings indicate that ENDS use is less prevalent among EJ populations. While this suggests a low potential for ETE among these groups, mixed outcomes on susceptibility, advertisement exposure, and access among low SES groups show a potential flattening of the SES gradient over time, which may affect future ENDS ETE. These findings underscore the importance of educational campaigns to prevent initiation and subsequent addiction among non-users of tobacco products and initiatives aimed at managing vape shop presence in EJ communities and monitoring targeted advertisements.
Supplementary Materials
The following supporting information can be downloaded at: https://www.mdpi.com/article/10.3390/ijerph192013585/s1, Supplementary File S1: ENDS literature search terms; Supplementary File S2: Full-text extraction table.
Author Contributions
Conceptualization, S.A.N.; methodology, S.A.N.; validation, S.A.N., B.M. and Y.T.-Z.; formal analysis, S.A.N., B.M. and Y.T.-Z.; investigation, S.A.N., B.M. and Y.T.-Z.; data curation, S.A.N.; writing—original draft preparation, S.A.N., B.M. and Y.T.-Z.; writing—review and editing, S.A.N., B.M. and Y.T.-Z.; visualization, S.A.N.; project administration, S.A.N. All authors have read and agreed to the published version of the manuscript.
Funding
This research received no external funding.
Informed Consent Statement
Not applicable.
Conflicts of Interest
The authors have no potential conflict of interest to declare.
Disclaimer
The findings and conclusions in this report are those of the authors and do not necessarily represent the official position of the Food and Drug Administration.
References
- Thun, M.; Peto, R.; Boreham, J.; Lopez, A.D. Stages of the cigarette epidemic on entering its second century. Tob. Control 2012, 21, 96–101. [Google Scholar] [CrossRef]
- Lucherini, M.; Hill, S.; Smith, K. Potential for non-combustible nicotine products to reduce socioeconomic inequalities in smoking: A systematic review and synthesis of best available evidence. BMC Public Health 2019, 19, 1469. [Google Scholar] [CrossRef] [PubMed]
- El Dib, R.; Suzumura, E.A.; Akl, E.A.; Gomaa, H.; Agarwal, A.; Chang, Y.; Prasad, M.; Ashoorion, V.; Heels-Ansdell, D.; Maziak, W.; et al. Electronic nicotine delivery systems and/or electronic non-nicotine delivery systems for tobacco smoking cessation or reduction: A systematic review and meta-analysis. BMJ Open 2017, 7, e012680. [Google Scholar] [CrossRef]
- Hartmann-Boyce, J.; McRobbie, H.; Bullen, C.; Begh, R.; Stead, L.F.; Hajek, P. Electronic cigarettes for smoking cessation. Cochrane Database Syst. Rev. 2016, 2016, 1–244. [Google Scholar] [CrossRef] [PubMed]
- Dai, H.; Leventhal, A.M. Prevalence of e-cigarette use among adults in the United States, 2014–2018. JAMA 2019, 322, 1824–1827. [Google Scholar] [CrossRef]
- Cornelius, M.E.; Wang, T.W.; Jamal, A.; Loretan, C.G.; Neff, L.J. Tobacco product use among adults—United States, 2019. MMWR Morb. Mortal. Wkly. Rep. 2020, 69, 1736–1742. [Google Scholar] [CrossRef]
- Cullen, K.A.; Ambrose, B.K.; Gentzke, A.S.; Apelberg, B.J.; Jamal, A.; King, B.A. Notes from the field: Use of electronic cigarettes and any tobacco product among middle and high school students—United States, 2011–2018. MMWR Morb. Mortal. Wkly. Rep. 2018, 67, 1276–1277. [Google Scholar] [CrossRef] [PubMed]
- Surgeon General’s Advisory on E-Cigarette Use among Youth. Available online: https://e-cigarettes.surgeongeneral.gov/documents/surgeon-generals-advisory-on-e-cigarette-use-among-youth-2018.pdf (accessed on 21 May 2021).
- Park-Lee, E.; Ren, C.; Sawdey, M.D.; Gentzke, A.S.; Cornelius, M.; Jamal, A.; Cullen, K.A. Notes from the field: E-cigarette use among middle and high school students—National Youth Tobacco Survey, United States, 2021. MMWR Morb. Mortal. Wkly. Rep. 2021, 70, 1387–1389. [Google Scholar] [CrossRef]
- Shearston, J.; Lee, L.; Eazor, J.; Meherally, S.; Park, S.H.; Vilcassim, M.R.; Weitzman, M.; Gordon, T. Effects of exposure to direct and secondhand hookah and e-cigarette aerosols on ambient air quality and cardiopulmonary health in adults and children: Protocol for a panel study. BMJ Open 2019, 9, e029490. [Google Scholar] [CrossRef]
- Martuzevicius, D.; Prasauskas, T.; Setyan, A.; O’Connell, G.; Cahours, X.; Julien, R.; Colard, S. Characterization of the Spatial and Temporal Dispersion Differences Between Exhaled E-Cigarette Mist and Cigarette Smoke. Nicotine Tob. Res. 2019, 21, 1371–1377. [Google Scholar] [CrossRef]
- Logue, J.M.; Sleiman, M.; Montesinos, V.N.; Russell, M.L.; Litter, M.I.; Benowitz, N.L.; Gundel, L.A.; Destaillats, H. Emissions from electronic cigarettes: Assessing vapers’ intake of toxic compounds, secondhand exposures, and the associated health impacts. Environ. Sci. Technol. 2017, 51, 9271–9279. [Google Scholar] [CrossRef] [PubMed]
- Li, L.; Lin, Y.; Xia, T.; Zhu, Y. Effects of electronic cigarettes on indoor air quality and health. Annu. Rev. Public Health 2020, 41, 363–380. [Google Scholar] [CrossRef] [PubMed]
- Lampos, S.; Kostenidou, E.; Farsalinos, K.; Zagoriti, Z.; Ntoukas, A.; Dalamarinis, K.; Savranakis, P.; Lagoumintzis, G.; Poulas, K. Real-time assessment of e-cigarettes and conventional cigarettes emissions: Aerosol size distributions, mass and number concentrations. Toxics 2019, 7, 45. [Google Scholar] [CrossRef]
- Savdie, J.; Canha, N.; Buitrago, N.; Almeida, S.M. Passive exposure to pollutants from a new generation of cigarettes in real life scenarios. Int. J. Environ. Res. Public Health 2020, 17, 3455. [Google Scholar] [CrossRef]
- Palmisani, J.; Di Gilio, A.; Palmieri, L.; Abenavoli, C.; Famele, M.; Draisci, R.; de Gennaro, G. Evaluation of second-hand exposure to electronic cigarette vaping under a real scenario: Measurements of ultrafine particle number concentration and size distribution and comparison with traditional tobacco smoke. Toxics 2019, 7, 59. [Google Scholar] [CrossRef]
- Son, Y.; Giovenco, D.P.; Delnevo, C.; Khlystov, A.; Samburova, V.; Meng, Q. Indoor air quality and passive e-cigarette aerosol exposures in vape-shops. Nicotine Tob. Res. 2020, 22, 1772–1779. [Google Scholar] [CrossRef]
- Amalia, B.; Liu, X.; Lugo, A.; Fu, M.; Odone, A.; van den Brandt, P.A.; Semple, S.; Clancy, L.; Soriano, J.B.; Fernández, E.; et al. Exposure to secondhand aerosol of electronic cigarettes in indoor settings in 12 European countries: Data from the TackSHS survey. Tob. Control 2021, 30, 49–56. [Google Scholar] [CrossRef]
- Khachatoorian, C.; Jacob Iii, P.; Benowitz, N.L.; Talbot, P. Electronic cigarette chemicals transfer from a vape shop to a nearby business in a multiple-tenant retail building. Tob. Control 2018, 28, 519–525. [Google Scholar] [CrossRef]
- Mock, J.; Hendlin, Y.H. Notes from the field: Environmental contamination from e-cigarette, cigarette, cigar, and cannabis products at 12 high schools—San Francisco Bay Area, 2018–2019. MMWR Morb. Mortal. Wkly. Rep. 2019, 68, 897–899. [Google Scholar] [CrossRef]
- Hendlin, Y.H. Alert: Public health implications of electronic cigarette waste. Am. J. Public Health 2018, 108, 1489–1490. [Google Scholar] [CrossRef]
- Krause, M.J.; Townsend, T.G. Hazardous waste status of discarded electronic cigarettes. Waste Manag. 2015, 39, 57–62. [Google Scholar] [CrossRef]
- Executive Order 12898–Federal Actions to Address Environmental Justice in Minority Populations and Low-Income Populations. 1994. Available online: https://www.archives.gov/federal-register/executive-orders/1994.html#12898 (accessed on 29 April 2021).
- Yao, T.; Sung, H.-Y.; Wang, Y.; Lightwood, J.; Max, W. Sociodemographic differences among U.S. children and adults exposed to secondhand smoke at home: National health interview surveys 2000 and 2010. Public Health Rep. 2016, 131, 357–366. [Google Scholar] [CrossRef] [PubMed]
- Shenassa, E.D.; Rossen, L.M.; Cohen, J.; Morello-Frosch, R.; Payne-Sturges, D.C. Income inequality and US children’s secondhand smoke exposure: Distinct associations by race–ethnicity. Nicotine Tob. Res. 2016, 19, 1292–1299. [Google Scholar] [CrossRef] [PubMed]
- Homa, D.M.; Neff, L.J.; King, B.A.; Caraballo, R.S.; Bunnell, R.E.; Babb, S.D.; Garrett, B.E.; Sosnoff, C.S.; Wang, L.; Centers for Disease, C.; et al. Vital signs: Disparities in nonsmokers’ exposure to secondhand smoke—United States, 1999–2012. MMWR Morb. Mortal. Wkly. Rep. 2015, 64, 103–108. [Google Scholar]
- Cullen, K.A.; Gentzke, A.S.; Sawdey, M.D.; Chang, J.T.; Anic, G.M.; Wang, T.W.; Creamer, M.R.; Jamal, A.; Ambrose, B.K.; King, B.A. E-Cigarette use among youth in the United States, 2019. JAMA 2019, 322, 2095. [Google Scholar] [CrossRef]
- Tsai, J.; Homa, D.M.; Gentzke, A.S.; Mahoney, M.; Sharapova, S.R.; Sosnoff, C.S.; Caron, K.T.; Wang, L.; Melstrom, P.C.; Trivers, K.F. Exposure to secondhand smoke among nonsmokers—United States, 1988–2014. MMWR Morb. Mortal. Wkly. Rep. 2018, 67, 1342–1346. [Google Scholar] [CrossRef] [PubMed]
- Walton, K.; Gentzke, A.S.; Murphy-Hoefer, R.; Kenemer, B.; Neff, L.J. Exposure to secondhand smoke in homes and vehicles among US youths, United States, 2011-2019. Prev. Chronic Dis. 2020, 17, E103. [Google Scholar] [CrossRef] [PubMed]
- Su, C.P.; Syamlal, G.; Tamers, S.; Li, J.; Luckhaupt, S.E. Workplace secondhand tobacco smoke exposure among U.S. nonsmoking workers, 2015. MMWR Morb. Mortal. Wkly. Rep. 2015, 68, 604–607. [Google Scholar] [CrossRef]
- Bold, K.W.; Kong, G.; Cavallo, D.A.; Camenga, D.R.; Krishnan-Sarin, S. E-cigarette susceptibility as a predictor of youth initiation of e-cigarettes. Nicotine Tob. Res. 2016, 20, 140–144. [Google Scholar] [CrossRef]
- Carey, F.R.; Wilkinson, A.V.; Harrell, M.B.; Cohn, E.A.; Perry, C.L. Measurement and predictive value of susceptibility to cigarettes, e-cigarettes, cigars, and hookah among Texas adolescents. Addict. Behav. Rep. 2018, 8, 95–101. [Google Scholar] [CrossRef]
- Strong, D.R.; Hartman, S.J.; Nodora, J.; Messer, K.; James, L.; White, M.; Portnoy, D.B.; Choiniere, C.J.; Vullo, G.C.; Pierce, J. Predictive validity of the expanded susceptibility to smoke index. Nicotine Tob. Res. 2014, 17, 862–869. [Google Scholar] [CrossRef] [PubMed]
- Pierce, J.P.; Sargent, J.D.; Portnoy, D.B.; White, M.; Noble, M.; Kealey, S.; Borek, N.; Carusi, C.; Choi, K.; Green, V.R.; et al. Association between receptivity to tobacco advertising and progression to tobacco use in youth and young adults in the PATH study. JAMA Pediatr. 2018, 172, 444–451. [Google Scholar] [CrossRef] [PubMed]
- Camenga, D.; Gutierrez, K.M.; Kong, G.; Cavallo, D.; Simon, P.; Krishnan-Sarin, S. E-cigarette advertising exposure in e-cigarette naive adolescents and subsequent e-cigarette use: A longitudinal cohort study. Addict. Behav. 2018, 81, 78–83. [Google Scholar] [CrossRef] [PubMed]
- QuickStats. Age-adjusted percentage of adults who had ever used an e-cigarette, by race and ethnicity—National health interview survey, United States, 2014 and 2018. MMWR Morb. Mortal. Wkly. Rep. 2019, 68, 1102. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Gilbert, P.A.; Kava, C.M.; Afifi, R. High school students rarely use e-cigarettes alone: A socio-demographic analysis of poly-substance use among adolescents in the USA. Nicotine Tob. Res. 2020, 23, 505–510. [Google Scholar] [CrossRef] [PubMed]
- McCabe, S.E.; Boyd, C.J.; Evans-Polce, R.J.; McCabe, V.V.; Veliz, P.T. School-level prevalence and predictors of e-cigarette use in 8th, 10th, and 12th grade U.S. youth: Results from a national survey (2015–2016). J. Adolesc. Health 2020, 67, 531–541. [Google Scholar] [CrossRef] [PubMed]
- Du, Y.; Shih, M.; Shah, M.D.; Weber, M.D.; Lightstone, A.S. Prevalence and sociodemographic disparities in ever e-cigarette use among adults in Los Angeles County. Prev. Med. Rep. 2019, 15, 100904. [Google Scholar] [CrossRef]
- Roberts, M.E.; Keller-Hamilton, B.; Ferketich, A.K.; Berman, M.L. Juul and the upsurge of e-cigarette use among college undergraduates. J. Am. Coll. Health 2020, 70, 9–12. [Google Scholar] [CrossRef]
- Yu, E.; Lippert, A.M. Race/ethnicity modifies the association between school prevalence of e-cigarette use and student-level use: Results from the 2014 US national youth tobacco survey. Health Place 2017, 46, 114–120. [Google Scholar] [CrossRef]
- Barrington-Trimis, J.L.; Bello, M.S.; Liu, F.; Leventhal, A.M.; Kong, G.; Mayer, M.; Cruz, T.B.; Krishnan-Sarin, S.; McConnell, R. Ethnic differences in patterns of cigarette and e-cigarette use over time among adolescents. J. Adolesc. Health 2019, 65, 359–365. [Google Scholar] [CrossRef]
- Springer, A.E.; Davis, C.; Van Dusen, D.; Grayless, M.; Case, K.R.; Craft, M.; Kelder, S.H. School socioeconomic disparities in e-cigarette susceptibility and use among central Texas middle school students. Prev. Med. Rep. 2018, 11, 105–108. [Google Scholar] [CrossRef] [PubMed]
- Vallone, D.M.; Cuccia, A.F.; Briggs, J.; Xiao, H.; Schillo, B.A.; Hair, E.C. Electronic cigarette and JUUL use among adolescents and young adults. JAMA Pediatr. 2020, 174, 277–286. [Google Scholar] [CrossRef] [PubMed]
- Levy, D.T.; Yuan, Z.; Li, Y. The prevalence and characteristics of e-cigarette users in the U.S. Int. J. Environ. Res. Public Health 2017, 14, 1200. [Google Scholar] [CrossRef]
- Vu, T.T.; Groom, A.; Hart, J.L.; Tran, H.; Landry, R.L.; Ma, J.Z.; Walker, K.L.; Giachello, A.L.; Kesh, A.; Payne, T.J.; et al. Socioeconomic and demographic status and perceived health risks of e-cigarette product contents among youth: Results from a national survey. Health Promot. Pract. 2020, 21, 148s–156s. [Google Scholar] [CrossRef] [PubMed]
- Williams, L.M.; Clements-Nolle, K.; Lensch, T.; Yang, W. Exposure to adverse childhood experiences and early initiation of electronic vapor product use among middle school students in Nevada. Addict. Behav. Rep. 2020, 11, 100266. [Google Scholar] [CrossRef]
- Harlow, A.F.; Stokes, A.; Brooks, D.R. Socioeconomic and racial/ethnic differences in e-cigarette uptake among cigarette smokers: Longitudinal analysis of the population assessment of tobacco and health (PATH) study. Nicotine Tob. Res. 2019, 21, 1385–1393. [Google Scholar] [CrossRef]
- Spears, C.A.; Jones, D.M.; Weaver, S.R.; Huang, J.; Yang, B.; Pechacek, T.F.; Eriksen, M.P. Sociodemographic correlates of electronic nicotine delivery systems (ENDS) use in the United States, 2016–2017. Am. J. Public Health 2019, 109, 1224–1232. [Google Scholar] [CrossRef]
- Escobedo, P.; Garcia, R.; Soto, C.; Rodriguez, Y.; Barahona, R.; Baezconde-Garbanati, L. Comparison of e-cigarette marketing and availability in tobacco retail outlets among diverse low-income communities in California. Tob. Control 2019, 29, 469–471. [Google Scholar] [CrossRef]
- Moran, M.B.; Heley, K.; Pierce, J.P.; Niaura, R.; Strong, D.; Abrams, D. Ethnic and socioeconomic disparities in recalled exposure to and self-reported impact of tobacco marketing and promotions. Health Commun. 2017, 34, 280–289. [Google Scholar] [CrossRef]
- Giovenco, D.P.; Ackerman, C.; Hrywna, M.; Delnevo, C.D. Changes in the availability and promotion of non-cigarette tobacco products near high schools in New Jersey, USA. Tob. Control 2018, 27, 578–579. [Google Scholar] [CrossRef]
- Giovenco, D.P.; Spillane, T.E.; Merizier, J.M. Neighborhood differences in alternative tobacco product availability and advertising in New York City: Implications for health disparities. Nicotine Tob. Res. 2018, 21, 896–902. [Google Scholar] [CrossRef] [PubMed]
- Chido-Amajuoyi, O.G.; Ozigbu, C.E.; Zhang, K. School proximity and census tract correlates of e-cigarette specialty retail outlets (vape shops) in central Texas. Prev. Med. Rep. 2020, 18, 101079. [Google Scholar] [CrossRef] [PubMed]
- Bostean, G.; Sanchez, L.; Lippert, A.M. Sociodemographic disparities in e-cigarette retail environment: Vape stores and census tract characteristics in Orange County, CA. Health Place 2018, 50, 65–72. [Google Scholar] [CrossRef] [PubMed]
- Venugopal, P.D.; Morse, A.L.; Tworek, C.; Chang, H.W. Socioeconomic disparities in vape shop density and proximity to public schools in the conterminous United States, 2018. Health Promot. Pract. 2020, 21, 9s–17s. [Google Scholar] [CrossRef] [PubMed]
- Xiao, C.; Heley, K.; Kennedy, R.D.; Lagasse, L.; Moran, M.B. Sociodemographic differences in reasons for ENDS use among US youth within Wave 2 of the PATH study. Tob. Induc. Dis. 2019, 17, 04. [Google Scholar] [CrossRef] [PubMed]
- Dai, H.; Hao, J.; Catley, D. Vape shop density and socio-demographic disparities: A U.S. census tract analysis. Nicotine Tob. Res. 2017, 19, 1338–1344. [Google Scholar] [CrossRef] [PubMed]
- Wheeler, D.C.; Do, E.K.; Hayes, R.B.; Fugate-Laus, K.; Fallavollita, W.L.; Hughes, C.; Fuemmeler, B.F. Neighborhood disadvantage and tobacco retail outlet and vape shop outlet rates. Int. J. Environ. Res. Public Health 2020, 17, 2864. [Google Scholar] [CrossRef]
- Stallings-Smith, S.; Ballantyne, T. Ever use of e-cigarettes among adults in the United States: A cross-sectional study of sociodemographic factors. Inquiry 2019, 56, 46958019864479. [Google Scholar] [CrossRef]
- Assari, S.; Mistry, R.; Bazargan, M. Race, educational attainment, and e-cigarette use. J. Med. Res. Innov. 2020, 4, e000185. [Google Scholar] [CrossRef]
- Bello, M.S.; Khoddam, R.; Stone, M.D.; Cho, J.; Yoon, Y.; Lee, J.O.; Leventhal, A.M. Poly-product drug use disparities in adolescents of lower socioeconomic status: Emerging trends in nicotine products, marijuana products, and prescription drugs. Behav. Res. Ther. 2019, 115, 103–110. [Google Scholar] [CrossRef]
- Jaber, R.M.; Mirbolouk, M.; Defilippis, A.P.; Maziak, W.; Keith, R.; Payne, T.; Stokes, A.; Benjamin, E.; Bhatnagar, A.; Blankstein, R.; et al. Electronic cigarette use prevalence, associated factors, and pattern by cigarette smoking status in the United States from NHANES (National health and nutrition examination survey) 2013–2014. J. Am. Heart Assoc. 2018, 7, e008178. [Google Scholar] [CrossRef] [PubMed]
- Friedman, A.S.; Horn, S.J.L. Socioeconomic disparities in electronic cigarette use and transitions from smoking. Nicotine Tob. Res. 2019, 21, 1363–1370. [Google Scholar] [CrossRef] [PubMed]
- Simon, P.; Camenga, D.; Morean, M.; Kong, G.; Bold, K.W.; Cavallo, D.A.; Krishnan-Sarin, S. Socioeconomic status and adolescent e-cigarette use: The mediating role of e-cigarette advertisement exposure. Prev. Med. 2018, 112, 193–198. [Google Scholar] [CrossRef] [PubMed]
- Tan, A.S.L.; Bigman, C.A.; Mello, S.; Sanders-Jackson, A. Trends in the prevalence of exposure to e-cigarette aerosol in public places among US middle and high school students, 2015 to 2018. JAMA Netw. Open 2019, 2, e1910184. [Google Scholar] [CrossRef] [PubMed]
- Gentzke, A.S.; Wang, T.W.; Marynak, K.L.; Trivers, K.F.; King, B.A. Exposure to secondhand smoke and secondhand e-cigarette aerosol among middle and high school students. Prev. Chronic Dis. 2019, 16, E42. [Google Scholar] [CrossRef]
- Wang, T.W.; Marynak, K.L.; Agaku, I.T.; King, B.A. Secondhand exposure to electronic cigarette aerosol among US youths. JAMA Pediatr. 2017, 171, 490–492. [Google Scholar] [CrossRef]
- Hartwell, G.; Thomas, S.; Egan, M.; Gilmore, A.; Petticrew, M. E-cigarettes and equity: A systematic review of differences in awareness and use between sociodemographic groups. Tob. Control 2016, 26, e85–e91. [Google Scholar] [CrossRef]
- Nicksic, N.E.; Barnes, A.J. Is susceptibility to e-cigarettes among youth associated with tobacco and other substance use behaviors one year later? Results from the PATH study. Prev. Med. 2019, 121, 109–114. [Google Scholar] [CrossRef]
- U.S. Food and Drug Administration. FDA Launches New Campaign: “The Real Cost” Youth E-Cigarette Prevention Campaign. 2019. Available online: https://www.fda.gov/tobacco-products/youth-and-tobacco/fda-launches-new-campaign-real-cost-youth-e-cigarette-prevention-campaign (accessed on 8 June 2021).
- U.S. Food and Drug Administration. FDA Finalizes Enforcement Policy on Unauthorized Flavored Cartridge-Based E-Cigarettes That Appeal to Children, including Fruit and Mint. 2020. Available online: https://www.fda.gov/news-events/press-announcements/fda-finalizes-enforcement-policy-unauthorized-flavored-cartridge-based-e-cigarettes-appeal-children (accessed on 8 June 2021).
- Campaign for Tobacco Free Kids. States and Localities That Have Restricted the Sale of Flavored Tobacco Products. 2021. Available online: https://www.tobaccofreekids.org/assets/factsheets/0398.pdf (accessed on 29 April 2021).
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).