Outcomes of COVID-19 Patients under Cytotoxic Cancer Chemotherapy in Brazil
Abstract
:Simple Summary
Abstract
1. Introduction
2. Results
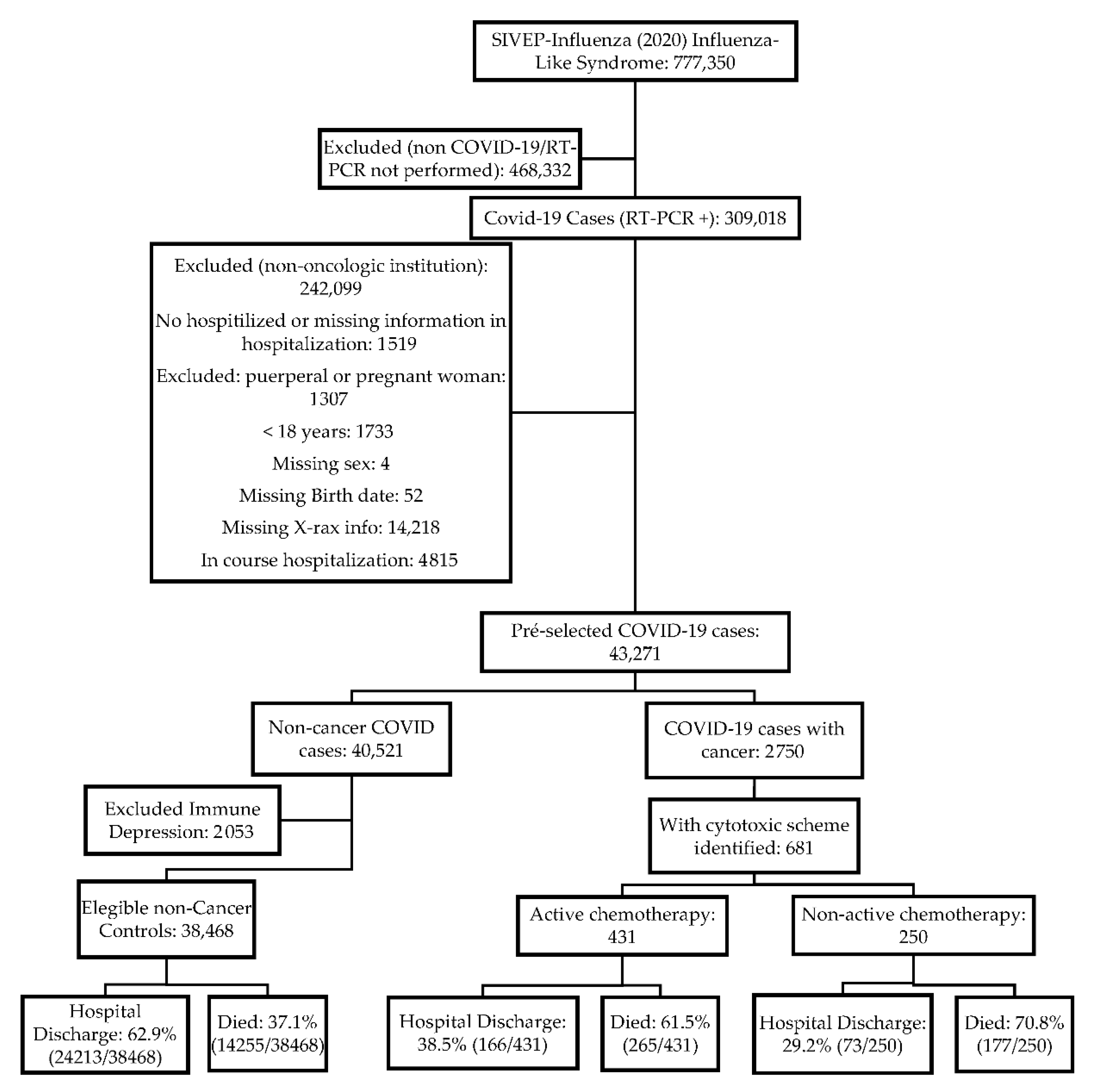
2.1. Participants
2.2. Descriptive Data
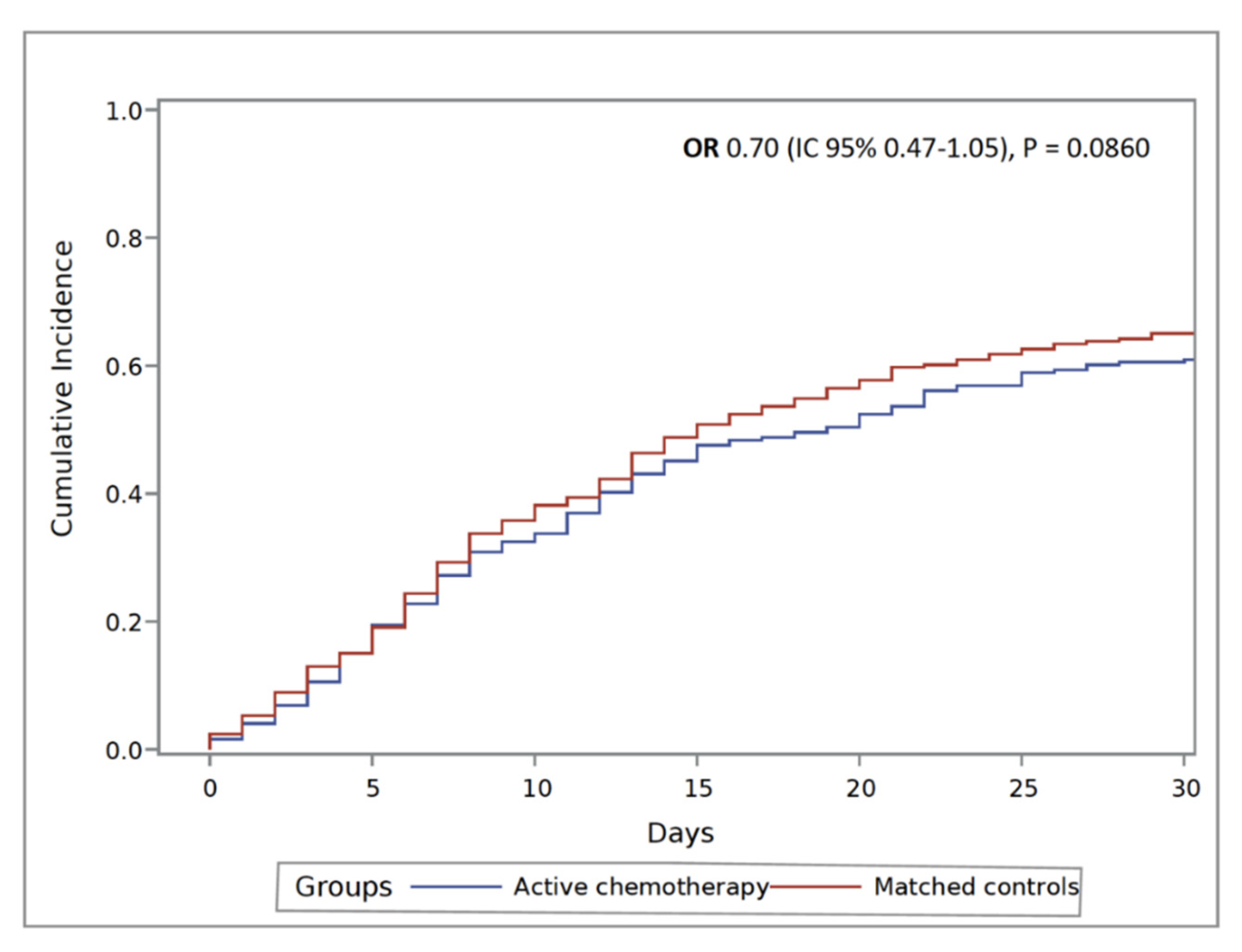
2.3. Outcome Data
3. Discussion
4. Materials and Methods
4.1. Study Design
4.2. Participants and Data Collection
4.3. Variables Analyzed
4.4. Analysis
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Conflicts of Interest
References
- WHO. Coronavirus Disease (COVID-19) Dashboard. Available online: https://covid19.who.int/ (accessed on 26 August 2020).
- Zhang, H.; Han, H.; He, T.; Labbe, K.E.; Hernandez, A.V.; Chen, H.; Velcheti, V.; Stebbing, J.; Wong, K.-K. Clinical Characteristics and Outcomes of COVID-19-Infected Cancer Patients: A Systematic Review and Meta-Analysis. JNCI J. Natl. Cancer Inst. 2020. [Google Scholar] [CrossRef] [PubMed]
- Zheng, Z.; Peng, F.; Xu, B.; Zhao, J.; Liu, H.; Peng, J.; Li, Q.; Jiang, C.; Zhou, Y.; Liu, S.; et al. Risk factors of critical mortal COVID-19 cases: A systematic literature review and meta-analysis. J. Infect. 2020, 81, e16–e25. [Google Scholar] [CrossRef] [PubMed]
- Giannakoulis, V.G.; Papoutsi, E.; Siempos, I.I. Effect of Cancer on Clinical Outcomes of Patients With COVID-19: A Meta-Analysis of Patient Data. JCO Glob. Oncol. 2020, 799–808. [Google Scholar] [CrossRef] [PubMed]
- Saini, K.S.; Tagliamento, M.; Lambertini, M.; McNally, R.; Romano, M.; Leone, M.; Curigliano, G.; de Azambuja, E. Mortality in patients with cancer and COVID-19: A systematic review and pooled analysis of 52 studies. Eur. J. Cancer 2020, 703, 135577. [Google Scholar] [CrossRef]
- De Azambuja, E.; Brandão, M.; Wildiers, H.; Laenen, A.; Aspeslagh, S.; Fontaine, C.; Collignon, J.; Lybaert, W.; Verheezen, J.; Rutten, A.; et al. Impact of solid cancer on in-hospital mortality overall and among different subgroups of patients with COVID-19: A nationwide, population-based analysis. ESMO Open 2020, 5, 1–11. [Google Scholar] [CrossRef]
- Mulvey, T.M.; Jacobson, J.O. COVID-19 and Cancer Care: Ensuring Safety While Transforming Care Delivery. J. Clin. Oncol. 2020. [Google Scholar] [CrossRef]
- Addeo, A.; Friedlaender, A. Cancer and COVID-19: Unmasking their ties. Cancer Treat. Rev. 2020, 88, 102041. [Google Scholar] [CrossRef]
- Rivera, D.R.; Peters, S.; Panagiotou, O.A.; Shah, D.P.; Kuderer, N.M.; Hsu, C.-Y.; Rubinstein, S.M.; Lee, B.J.; Choueiri, T.K.; de Lima Lopes, G.; et al. Utilization of COVID-19 Treatments and Clinical Outcomes among Patients with Cancer: A COVID-19 and Cancer Consortium (CCC19) Cohort Study. Cancer Discov. 2020, 10, 1514–1527. [Google Scholar] [CrossRef]
- Tian, J.; Yuan, X.; Xiao, J.; Zhong, Q.; Yang, C.; Liu, B.; Cai, Y.; Lu, Z.; Wang, J.; Wang, Y.; et al. Clinical characteristics and risk factors associated with COVID-19 disease severity in patients with cancer in Wuhan, China: A multicentre, retrospective, cohort study. Lancet Oncol. 2020, 21, 893–903. [Google Scholar] [CrossRef]
- Yang, K.; Sheng, Y.; Huang, C.; Jin, Y.; Xiong, N.; Jiang, K.; Lu, H.; Liu, J.; Yang, J.; Dong, Y.; et al. Clinical characteristics, outcomes, and risk factors for mortality in patients with cancer and COVID-19 in Hubei, China: A multicentre, retrospective, cohort study. Lancet Oncol. 2020, 21, 904–913. [Google Scholar] [CrossRef]
- Lee, L.Y.W.; Cazier, J.-B.; Starkey, T.; Briggs, S.E.W.; Arnold, R.; Bisht, V.; Booth, S.; Campton, N.A.; Cheng, V.W.T.; Collins, G.; et al. COVID-19 prevalence and mortality in patients with cancer and the effect of primary tumour subtype and patient demographics: A prospective cohort study. Lancet Oncol. 2020, 2045, 1–8. [Google Scholar] [CrossRef]
- Jee, J.; Foote, M.B.; Lumish, M.; Stonestrom, A.J.; Wills, B.; Narendra, V.; Avutu, V.; Murciano-Goroff, Y.R.; Chan, J.E.; Derkach, A.; et al. Chemotherapy and COVID-19 Outcomes in Patients with Cancer. J. Clin. Oncol. 2020. [Google Scholar] [CrossRef] [PubMed]
- Kuderer, N.M.; Choueiri, T.K.; Shah, D.P.; Shyr, Y.; Rubinstein, S.M.; Rivera, D.R.; Shete, S.; Hsu, C.-Y.; Desai, A.; de Lima Lopes, G.; et al. Clinical impact of COVID-19 on patients with cancer (CCC19): A cohort study. Lancet 2020, 395, 1907–1918. [Google Scholar] [CrossRef]
- Fillmore, N.R.; La, J.; Szalat, R.E.; Tuck, D.P.; Nguyen, V.; Yildirim, C.; Do, N.V.; Brophy, M.T.; Munshi, N.C. Prevalence and outcome of COVID-19 infection in cancer patients: A national Veterans Affairs study. JNCI J. Natl. Cancer Inst. 2020. [Google Scholar] [CrossRef] [PubMed]
- Brar, G.; Pinheiro, L.C.; Shusterman, M.; Swed, B.; Reshetnyak, E.; Soroka, O.; Chen, F.; Yamshon, S.; Vaughn, J.; Martin, P.; et al. COVID-19 Severity and Outcomes in Patients With Cancer: A Matched Cohort Study. J. Clin. Oncol. 2020. [Google Scholar] [CrossRef] [PubMed]
- Garassino, M.C.; Whisenant, J.G.; Huang, L.-C.; Trama, A.; Torri, V.; Agustoni, F.; Baena, J.; Banna, G.; Berardi, R.; Bettini, A.C.; et al. COVID-19 in patients with thoracic malignancies (TERAVOLT): First results of an international, registry-based, cohort study. Lancet Oncol. 2020, 21, 914–922. [Google Scholar] [CrossRef]
- Yekedüz, E.; Utkan, G.; Ürün, Y. A systematic review and meta-analysis: The effect of active cancer treatment on severity of COVID-19. Eur. J. Cancer 2020, 141, 92–104. [Google Scholar] [CrossRef]
- Park, R.; Lee, S.A.; Kim, S.Y.; de Melo, A.C.; Kasi, A. Association of active oncologic treatment and risk of death in cancer patients with COVID-19: A systematic review and meta-analysis of patient data. Acta Oncol. 2020, 1–7. [Google Scholar] [CrossRef]
- Lee, L.Y.W.; Cazier, J.-B.; Angelis, V.; Arnold, R.; Bisht, V.; Campton, N.A.; Chackathayil, J.; Cheng, V.W.; Curley, H.M.; Fittall, M.W.; et al. COVID-19 mortality in patients with cancer on chemotherapy or other anticancer treatments: A prospective cohort study. Lancet 2020, 395, 1919–1926. [Google Scholar] [CrossRef]
- Baqui, P.; Bica, I.; Marra, V.; Ercole, A.; van der Schaar, M. Ethnic and regional variations in hospital mortality from COVID-19 in Brazil: A cross-sectional observational study. Lancet Glob. Health 2020, 8, e1018–e1026. [Google Scholar] [CrossRef]
- Passamonti, F.; Cattaneo, C.; Arcaini, L.; Bruna, R.; Cavo, M.; Merli, F.; Angelucci, E.; Krampera, M.; Cairoli, R.; Della Porta, M.G.; et al. Clinical characteristics and risk factors associated with COVID-19 severity in patients with haematological malignancies in Italy: A retrospective, multicentre, cohort study. Lancet Haematol. 2020, 3026, 1–9. [Google Scholar] [CrossRef]
- García-Suárez, J.; de la Cruz, J.; Cedillo, Á.; Llamas, P.; Duarte, R.; Jiménez-Yuste, V.; Hernández-Rivas, J.Á.; Gil-Manso, R.; Kwon, M.; Sánchez-Godoy, P.; et al. Impact of hematologic malignancy and type of cancer therapy on COVID-19 severity and mortality: Lessons from a large population-based registry study. J. Hematol. Oncol. 2020, 13, 133. [Google Scholar] [CrossRef] [PubMed]
- Glanz, A.; Chawla, K.; Fabry, S.; Subramanian, G.; Garcia, J.; Jay, B.; Ciricillo, J.; Chakravarti, R.; Taylor, R.T.; Chattopadhyay, S. High throughput screening of FDA-approved drug library reveals the compounds that promote IRF3-mediated pro-apoptotic pathway inhibit virus replication. Viruses 2020, 12, 442. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Meyer-Almes, F.-J. Repurposing approved drugs as potential inhibitors of 3CL-protease of SARS-CoV-2: Virtual screening and structure based drug design. Comput. Biol. Chem. 2020, 88, 107351. [Google Scholar] [CrossRef]
- Al-Motawa, M.; Abbas, H.; Wijten, P.; de la Fuente, A.; Xue, M.; Rabbani, N.; Thornalley, P. Vulnerabilities of the SARS-CoV-2 Virus to Proteotoxicity—Opportunity for Repurposed Chemotherapy of COVID-19 Infection. SSRN Electron. J. 2020. [Google Scholar] [CrossRef]
- Revannasiddaiah, S.; Kumar Devadas, S.; Palassery, R.; Kumar Pant, N.; Maka, V.V. A potential role for cyclophosphamide in the mitigation of acute respiratory distress syndrome among patients with SARS-CoV-2. Med. Hypotheses 2020, 144, 109850. [Google Scholar] [CrossRef]
- Brocato, R.L.; Principe, L.M.; Kim, R.K.; Zeng, X.; Williams, J.A.; Liu, Y.; Li, R.; Smith, J.M.; Golden, J.W.; Gangemi, D.; et al. Disruption of Adaptive Immunity Enhances Disease in SARS-CoV-2-Infected Syrian Hamsters. J. Virol. 2020, 94, 1–13. [Google Scholar] [CrossRef]
- Fedele, P.; Ferro, A.; Sanna, V.; La Verde, N.; Paris, I.; Chiari, R. Exploring metastatic breast cancer treatment changes during COVID-19 pandemic. J. Chemother. 2020, 1–6. [Google Scholar] [CrossRef]
- Brunetti, O.; Derakhshani, A.; Baradaran, B.; Galvano, A.; Russo, A.; Silvestris, N. COVID-19 Infection in Cancer Patients: How Can Oncologists Deal With These Patients? Front. Oncol. 2020, 10. [Google Scholar] [CrossRef]
- Plataforma Integrada de Vigilância em Saúde Ministerio da Saúde. Available online: http://plataforma.saude.gov.br/ (accessed on 8 October 2020).

| Characteristic | Non-Matched | Pair Matched | Standardized Mean Difference | ||||||
|---|---|---|---|---|---|---|---|---|---|
| Active Chemo. n = 431 | Non-Active Chemo. n = 250 | p | Active Chemo. n = 246 | Non-Active Chemo. n = 246 | p | All | Region | Matched | |
| Age | 0.0182 | 0.9893 | |||||||
| <50 years | 121 (28.1) | 46 (18.4) | 49 (19.9) | 46 (18.7) | 0.23058 | 0.19103 | 0.02907 | ||
| 50 to 64 years | 172 (39.9) | 102 (40.8) | 99 (40.2) | 101 (41.1) | −0.01820 | −0.00805 | −0.01657 | ||
| 65 to 79 years | 122 (28.3) | 93 (37.2) | 89 (36.2) | 90 (36.6) | −0.19036 | −0.16575 | −0.00870 | ||
| ≥80 years | 16 (3.7) | 9 (3.6) | 9 (3.7) | 9 (3.7) | 0.00598 | 0.00661 | 0.00000 | ||
| Sex | 0.1849 | 0.7183 | −0.10541 | −0.10407 | 0.03268 | ||||
| Male | 186 (43.2) | 121 (48.4) | 122 (49.6) | 118 (48) | |||||
| Female | 245 (56.8) | 129 (51.6) | 124 (50.4) | 128 (52) | |||||
| Comorbidities | |||||||||
| Heart Disease | 83 (19.3) | 60 (24) | 0.1430 | 60 (24.4) | 57 (23.2) | 0.7507 | −0.11538 | −0.08634 | 0.02967 |
| Diabetes | 66 (15.3) | 38 (15.2) | 0.9684 | 38 (15.5) | 38 (15.5) | 1.0000 | 0.00315 | −0.00225 | 0.00000 |
| Neurologic disease | 5 (1.2) | 8 (3.2) | 0.0608 | 5 (2) | 6 (2.4) | 0.7604 | −0.14003 | −0.08629 | −0.02790 |
| Chronic lung disease | 17 (3.9) | 12 (4.8) | 0.5940 | 11 (4.5) | 12 (4.9) | 0.8309 | −0.04186 | −0.04203 | −0.01988 |
| Nephropathy | 23 (5.3) | 16 (6.4) | 0.5648 | 15 (6.1) | 15 (6.1) | 1.0000 | −0.04526 | −0.02810 | 0.00000 |
| Critical Presentation | 97 (22.5) | 61 (24.4) | 0.5724 | 59 (24) | 61 (24.8) | 0.8337 | −0.04472 | −0.05520 | −0.01919 |
| Southeast | 281 (65.2) | 138 (55.2) | 0.0097 | 138 (56.1) | 137 (55.7) | 0.9277 | 0.20531 | 0.18656 | 0.00835 |
| Clinical Stage | 0.0747 | 0.9835 | |||||||
| I/II | 64 (14.9) | 42 (16.8) | 41 (16.7) | 42 (17.1) | 0.01846 | 0.02824 | −0.03477 | ||
| III/IV | 272 (63.1) | 172 (68.8) | 170 (69.1) | 168 (68.3) | 0.12211 | 0.09351 | 0.00000 | ||
| Unknown | 27 (6.3) | 7 (2.8) | 8 (3.3) | 7 (2.9) | −0.16690 | −0.14763 | −0.01958 | ||
| Other | 68 (15.8) | 29 (11.6) | 27 (11) | 29 (11.8) | −0.12157 | −0.09036 | 0.02366 | ||
| Mult. Drug Regimen | 237 (55) | 132 (52.8) | 0.5806 | 135 (54.9) | 130 (52.9) | 0.6511 | −0.04391 | −0.03066 | −0.04078 |
| Drug Class | |||||||||
| Anti-Metabolic | 169 (39.2) | 96 (38.4) | 0.8342 | 97 (39.4) | 94 (38.2) | 0.7814 | 0.01665 | 0.00663 | 0.02503 |
| Microtubule inhib. | 153 (35.5) | 86 (34.4) | 0.7721 | 82 (33.3) | 84 (34.2) | 0.8488 | 0.02305 | 0.01766 | −0.01705 |
| Alkylating | 115 (26.7) | 53 (21.2) | 0.1097 | 56 (22.8) | 53 (21.5) | 0.7447 | 0.12874 | 0.11029 | 0.02864 |
| Cisplatin | 186 (43.2) | 127 (50.8) | 0.0537 | 127 (51.6) | 125 (50.8) | 0.8568 | −0.15362 | −0.14223 | 0.01634 |
| Type 1 topois. inhib. | 36 (8.4) | 10 (4) | 0.0291 | 13 (5.3) | 10 (4.1) | 0.5217 | 0.18156 | 0.11641 | 0.05087 |
| Type 2 topois. inhib. | 94 (21.8) | 40 (16) | 0.0660 | 40 (16.3) | 40 (16.3) | 1.0000 | 0.14879 | 0.11031 | 0.00000 |
| Treatment | 0.0077 | 0.4682 | |||||||
| Palliative 1st Line | 193 (44.8) | 105 (42) | 119 (48.4) | 103 (41.9) | −0.05602 | −0.07571 | −0.13108 | ||
| Palliative 2nd Line | 36 (8.4) | 22 (8.8) | 16 (6.5) | 22 (8.9) | 0.01595 | 0.02385 | 0.08697 | ||
| Hematological cancer | 111 (25.8) | 44 (17.6) | 41 (16.7) | 44 (17.9) | −0.25943 | −0.21717 | −0.02354 | ||
| Neoadj./Definit./Adjuv. | 91 (21.1) | 79 (31.6) | 70 (28.5) | 77 (31.3) | 0.23933 | 0.22339 | 0.06494 | ||
| Primary Site | 0.0694 | 0.9995 | |||||||
| GI | 121 (28.1) | 78 (31.2) | 83 (33.7) | 78 (31.7) | −0.06849 | −0.08101 | 0.00894 | ||
| Head and Neck | 18 (4.2) | 17 (6.8) | 15 (6.1) | 16 (6.5) | −0.11539 | −0.10312 | −0.01795 | ||
| Lung | 30 (7) | 21 (8.4) | 17 (6.9) | 21 (8.5) | −0.05408 | −0.04458 | −0.04600 | ||
| Others | 15 (3.5) | 14 (5.6) | 14 (5.7) | 12 (4.9) | −0.10195 | −0.06780 | 0.00000 | ||
| Breast | 66 (15.3) | 24 (9.6) | 25 (10.2) | 24 (9.8) | 0.17366 | 0.16172 | 0.06203 | ||
| Gynecological | 42 (9.7) | 33 (13.2) | 33 (13.4) | 32 (13) | −0.10858 | −0.10351 | −0.02565 | ||
| Prostate | 9 (2.1) | 8 (3.2) | 7 (2.9) | 8 (3.3) | −0.06934 | −0.07311 | 0.00000 | ||
| Cent. Nervous Syst. | 8 (1.9) | 4 (1.6) | 4 (1.6) | 4 (1.6) | 0.01966 | 0.01748 | 0.00000 | ||
| Hematologic | 111 (25.8) | 44 (17.6) | 41 (16.7) | 44 (17.9) | 0.19887 | 0.19157 | 0.00995 | ||
| Sarcomas | 11 (2.6) | 7 (2.8) | 7 (2.9) | 7 (2.9) | −0.01535 | −0.01853 | −0.02529 | ||
| Logit Prop. Score | 0.57261 | 0.48064 | 0.06873 | ||||||
| Outcome | 0.0141 | 0.3322 | |||||||
| Hospital Discharge | 166 (38.5) | 73 (29.2) | 83 (33.9) | 73 (29.8) | |||||
| Death | 265 (61.5) | 177 (70.8) | 162 (66.1) | 172 (70.2) | |||||
| Characteristic | Events/Number at Risk | Univariate Analysis | Multivariate Analysis | ||
|---|---|---|---|---|---|
| OR (95% CI) | p | OR (95% CI) | p | ||
| Age | |||||
| <65 years | 277/441 | Reference (A) | |||
| ≥65 years | 165/240 | 1.3 (0.93–1.82) | 0.1213 | ||
| Sex | |||||
| Male | 206/307 | Reference (B) | |||
| Female | 236/374 | 0.84 (0.61–1.15) | 0.2768 | ||
| Comorbidities | |||||
| Heart Disease | 101/143 | 1.39 (0.93–2.07) | 0.1075 | ||
| Diabetes | 70/104 | 1.14 (0.73–1.77) | 0.5771 | ||
| Neurologic disease | 9/13 | 1.22 (0.37–4.01) | 0.7418 | ||
| Chronic lung disease | 19/29 | 1.03 (0.47–2.25) | 0.9439 | ||
| Nephropathy | 29/39 | 1.61 (0.77–3.36) | 0.2066 | ||
| Southeast Brazilian Region | 261/419 | 0.74 (0.53–1.03) | 0.0712 | 0.74 (0.53–1.03) | 0.0777 |
| Clinical Stage | |||||
| I/II | 61/106 | Reference (C) | |||
| III/IV | 293/444 | 1.43 (0.93–2.21) | 0.1039 | ||
| Unknown | 21/34 | 1.19 (0.54–2.63) | 0.6642 | ||
| Other | 67/97 | 1.65 (0.93–2.94) | 0.0903 | ||
| Mult. Drug Regimen | 238/369 | 0.96 (0.7–1.32) | 0.8094 | ||
| Drug Class | |||||
| Anti-Metabolic | 175/265 | 1.09 (0.79–1.5) | 0.6210 | ||
| Microtubule inhibitor | 154/239 | 0.97 (0.7–1.35) | 0.8501 | ||
| Alkylating | 95/168 | 0.62 (0.44–0.89) | 0.0092 | ||
| Cisplatin | 216/313 | 1.4 (1.02–1.92) | 0.0388 | ||
| Type 1 topois. inhib. | 29/46 | 0.92 (0.49–1.71) | 0.7842 | ||
| Type 2 topois. inhib. | 69/134 | 0.5 (0.34–0.73) | 0.0003 | 0.55 (0.36–0.85) | 0.0070 |
| Chemotherapy setting | |||||
| Neoadj./Definit./Adjuv. | 94/170 | Reference (D) | |||
| Palliative 1st Line | 209/298 | 1.9 (1.28–2.81) | 0.0013 | 1.83 (1.22–2.74) | 0.0038 |
| Palliative 2nd Line | 43/58 | 2.32 (1.2–4.49) | 0.0127 | 2.26 (1.15–4.45) | 0.0180 |
| Hematological cancer | 96/155 | 1.32 (0.84–2.05) | 0.2253 | 1.68 (1.05–2.7) | 0.0310 |
| Primary Site | |||||
| GI | 126/199 | Reference (E) | |||
| Head and Neck | 18/35 | 0.61 (0.3–1.26) | 0.1852 | ||
| Lung | 38/51 | 1.69 (0.85–3.39) | 0.1360 | ||
| Others | 25/29 | 3.62 (1.21–10.81) | 0.0212 | ||
| Breast | 51/90 | 0.76 (0.46–1.26) | 0.2832 | ||
| Gynecological | 55/75 | 1.59 (0.89–2.87) | 0.1201 | ||
| Prostate | 13/17 | 1.88 (0.59–5.99) | 0.2838 | ||
| Cent. Nervous Syst. | 7/12 | 0.81 (0.25–2.65) | 0.7288 | ||
| Hematologic | 96/155 | 0.94 (0.61–1.46) | 0.7898 | ||
| Sarcomas | 13/18 | 1.51 (0.52–4.4) | 0.4534 | ||
| Active chemotherapy | 265/431 | 0.66 (0.47–0.92) | 0.0144 | 0.66 (0.46–0.93) | 0.0169 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Duarte, M.B.O.; Leal, F.; Argenton, J.L.P.; Carvalheira, J.B.C. Outcomes of COVID-19 Patients under Cytotoxic Cancer Chemotherapy in Brazil. Cancers 2020, 12, 3490. https://doi.org/10.3390/cancers12123490
Duarte MBO, Leal F, Argenton JLP, Carvalheira JBC. Outcomes of COVID-19 Patients under Cytotoxic Cancer Chemotherapy in Brazil. Cancers. 2020; 12(12):3490. https://doi.org/10.3390/cancers12123490
Chicago/Turabian StyleDuarte, Mateus Bringel Oliveira, Frederico Leal, Juliana Luz Passos Argenton, and José Barreto Campello Carvalheira. 2020. "Outcomes of COVID-19 Patients under Cytotoxic Cancer Chemotherapy in Brazil" Cancers 12, no. 12: 3490. https://doi.org/10.3390/cancers12123490





